The misplacement of external ventricular drain by freehand method in emergent neurosurgery
|
|
|
- Willis Richards
- 5 years ago
- Views:
Transcription
1 Acta Neurol. Belg., 2011, 111, Original articles The misplacement of external ventricular drain by freehand method in emergent neurosurgery Cheng-Ta HsieH 1,2, Guann-Juh CHen 1, Hsin-i Ma 1, Cheng-Fu CHanG 1, Cheng-Ma CHenG 1, Yih-Huei su 1, Da-Tong Ju 1, Chung-Ching Hsia 1, Yuan-Hao CHen 1, Hao-Yiang Wu 1 and Ming-Ying Liu 1 1 Department of neurological surgery, Tri-service General Hospital, national Defense Medical Center, Taipei, Taiwan, Republic of China; 2 Department of neurosurgery, sijhih Cathy General Hospital, new Taipei, Taiwan, Republic of China Abstract External ventricular drain (EVD) placement is one of the most basic and common neurosurgical procedure which most was performed by young neurosurgical trainees. This study is conducted to determinate the safe and accuracy of EVD placement by freehand method. About 129 EVD placements were evaluated in this study. Eighty-three catheters (64.3%) were located in the ipsilateral frontal horn or third ventricle. The functional accuracy was 86%. Of eighteen misplaced catheters, only 4 (3.1%) catheters were nonfunctional, requiring a replacement or reposition. The higher misplaced rate was significantly observed in patients whose head CT scans revealed the lower hydrocephalus ratio (28.85%) and the smaller ventricular size (5.6mm). Twenty-one (16.2%) new hemorrhages associated with EVD placements were observed. Using the freehand method, EVD placement is a safe and effective procedure in management of these emergent neurosurgical diseases. Key words: Hydrocephalus; traumatic brain injury; ventri - culostomy; subarachnoid hemorrhages; stroke. Introduction external ventricular drain (evd) placement is one of the most important and common emergent procedures in neurosurgery. The goal of evd is indicated in monitoring intracranial pressure and therapeutic drainage of cerebrospinal fluid which are secondary to multiple intracranial disorders including traumatic brain injury, intracranial hemorrhage, hydrocephalus, intracranial hypertension, ventriculitis, other intracranial neoplasms or vascular malformations. evd is a catheter inserted into the ventricular system and connected to an external tube and collection bag. since Dandy introduced the ventriculostomy, the evd placement by freehand method is a wellestablished basic procedure in neurosurgery and mostly performed by young neurosurgical trainees (Gardner et al. 2009). The incidence, prevention and management of infection and hemorrhage secondary to evd placement have been well investigated (anderson et al. 2004; Gardner et al. 2009). However, the accuracy of evd placement by freehand method is rarely discussed especially when the frontal horn of lateral ventricle was dislocated or compressed. in our hospital, the evd placement is a basic neurosurgical technique and performed by neurosurgical trainees using the freehand method. We retrospectively reviewed 129 evd insertions. The relevant risk factors and accuracy were also analyzed. Patients and methods PaTienTs Between January 2008 and august 2009, a total of 266 patients admitted to Tri-service General Hospital after sustaining head trauma, intracerebral hemorrhage, subarachnoid hemorrhage or acute hydrocephalus were met criteria for emergent insertion of evds. Criteria for external ventricular drains were (1) Glasgow Coma scale score of less than 9, (2) evidence of hydrocephalus, (3) monitoring intracranial pressure. all patients in whom no subsequent head computed tomographic (CT) scan was obtained after evd placement were excluded. study MeTHoDoLoGY We retrospectively reviewed patients hospital charts, surgical indications, operative procedure, operator s experience and the pre-operative and post-operative head CT scans. The location of catheter tip of evd shown on the postoperative head
2 THe MisPLaCeMenT of external VenTRiCuLaR DRain 23 CT scan was recorded. Midline shift was defined as the deviated distance from septum pellucidum to the midline. Hydrocephalus ratio was represented as the ratio of maximum width of the frontal horns to the maximum width of the inner table of the cranium. The ventricular size was defined as the width of ipsilateral frontal horn. Hemorrhage attributable to the insertion of the catheter was defined as a new area of hemorrhage along the device, which could be demonstrated on the postoperative head CT scan. The combined surgery was defined as if the evd placement was the only one part of whole procedure such as clipping of aneurysms or removal of subdural hematomas, especially when the head was tilting. surgical PRoCeDuRe The emergent evd placement was all performed in operative room under general anesthesia. neither image navigator nor a Ghaja guide device was used during the whole procedure. The frontal trephination performed with a 3 mm diameter twist drill was made 1 cm frontal to coronal suture and 2.5 cm lateral to midline, after making a 4 cm skin incision. The direction of ventriculostomy was aimed toward the ipsilateral inner canthus and external auditory meatus. The exact direction was modified based on the pre-operative head CT scan and the experience of operators. The ventricular metal needle was inserted with a depth of 5 cm below the brain surface. after cerebrospinal fluid (CsF) flew out through the ventricular needle, the catheter of evd was inserted into the previous tract and attached to a trocar and was tunneled away about 5 cm from the skin incision. Then the catheter was connected to a sterile external drainage bag. The skin was closed as standard procedure. statistics Results are given as mean ± standard error mean. The student s t-test was used to compare continuous data in two categories. Qualitative variables were compared between groups using the Fischer s exact test or chi-square test. a p value less than 0.05 within a confidence interval of 95% was taken as statistically significant. The level of statistical significance was set at Results 125 patients including 84 men (67%) and 41 women (33%) were enrolled in our study. The mean age was 55.7 years, ranging from 16 to 93 years. a total of 129 evds were emergently Table 1 The summary of the tip locations of 129 evd placements Tip location no (%) ipsilateral Contralateral Frontal horn 70 (54.3) Body of lateral ventricle 8 (6.2) Basal ganglion 6 (4.7) Thalamus 2 (1.6) Cerebrum 1 (0.8) Frontal horn 17 (13.2) Body of lateral ventricle 3 (2.3) Basal ganglion 1 (0.8) Thalamus 3 (2.3) Cerebrum 2 (1.6) Third ventricle 13 (10) Corpus callosum 1 (0.8) suprasellar region 2 (1.6) placed. Four patients received bilateral evd placements simultaneously due to the severe intraventricular hemorrhages resulting into the compartment-like ventricles. Forty-five patients (35%) presented with intracerebral hemorrhage, 41 (32%) with trauma, 37 (29%) with subarachnoid hemorrhage, and 6 (4%) with neoplasm. 79 evds (61%) were inserted from the right trephination, where 50 evds (39%) were made from left approach. The final location of catheter tip was summarized as Table 1. The most common locations were ipsilateral frontal horn (54.3%), contralateral frontal horn (13.2%) and third ventricle (10%). 83 catheters (64.3%) were located in the ipsilateral frontal horn (Fig. 1) or third ventricle. There were 18 misplaced catheters in 14% of 129 evd placements, including 7 basal ganglion, 5 thalamus, 3 cerebrum (Fig. 2), 2 suprasellar cistern and 1 corpus callosum. only four (3.1%) catheters were nonfunctional, requiring a replacement or reposition. There were no known neurological complications from the misplaced catheters. Because the 18 misplacements were all in eloquent area, we compared these cases (the misplaced group) with other 111 evd insertions (the control group) for further analysis. as shown on Table 2, the difference of surgical indications including the trauma, intra cerebral hemorrhage, sub - arachnoid hemorrhage or neoplasm between the misplaced group and control group did not reach the
3 24 C.-T. HsieH et al. FiG. 2. The head computed tomographic scan revealed the catheter was located in the contralateral cerebrum. FiG. 1. The head computed tomographic scan revealed the catheter was located in the ipsilateral frontal horn above the Foramen of Monro, as known as the ideal target. significance. Considering the radiological parameters in the head CT scan, the higher misplaced rate was significantly observed in patients whose head CT scans revealed the lower hydro cephalus ratio and the smaller ventricular size (P = and 0.05, respectively). in the misplaced group, the mean hydrocephalus ratio was 28.85% (range, 20.8 ~ 38.2%) and the mean ventricular size was 5.6 mm (range, 0.6 ~ 15.5 mm). The midline shift and the site of ventriculostomy were not attributable to the misplacement of evd (P = 0.54 and 0.441, respectively). otherwise, the operator s experiences and combined surgery did not affect the accuracy of placement (P = and 0.899, respectively). Twenty-one (16.2%) new hemorrhages associated with evd placements were observed on subsequent head CT scans (Fig. 3). no patients experienced this associated hemorrhages required a craniotomy. The occurrence of new hemorrhages between the misplaced group and control group didn t reach the significant differences. Discussion The evd placement is one of the most effective and most frequently used therapeutic procedures in neurosurgery. evd allows not only continuous drainage of CsF but also the measurement of intracranial pressure, acquisition of ventricular fluid and administration of antibiotics, chemotherapeutic agents and thrombrolytic medication. The frontal horn anterior to the foramen of Monro is ideal target for ventricular catheter placement because there is no choroid plexus anterior to the foramen of Monro (Lind et al., 2008). The freehand method using surface landmark remains the most common and practical method for neurosurgeons. The frontal approach used the trajectory landmarks of the line of intersection of a coronal plane with the medial canthus of ipsilateral eye and a sagittal plane with ipsilateral external auditory meatus. The landmark of trephination is identified at the 2.5 cm lateral to the midline and 1cm anterior to the coronal suture. However, in case of brain shifting and ventricular compression, the exact direction of trajectory should be adapted according to the the pre-operative head CT scan and the operator s experience (stangl et al., 1998). The complications of evd placement are wellestablished, including dislocation, infection and hemorrhages (Khan et al., 1998). Most studies emphasized the infection and hemorrhage, as known as the two most common complications of evd placement (Gardner et al., 2009). only few studies discussed the accuracy of evd placement (Bogdahn et al., 1992; Khanna et al., 1995; stangl et al., 1998; o Leary et al., 2000; anderson et al., 2004; Huyette et al., 2008; Kakarla et al., 2008; Lind et al., 2008; ngo et al., 2009). Conventionally, the correct loca-
4 THe MisPLaCeMenT of external VenTRiCuLaR DRain 25 Table 2 The summary of clinical features in patients with misplacement of external ventricular drain placement and in controls *Value : mean ± standard error mean. Control group Misplaced group P no of procedures indications Trauma Yes no ich Yes no sah Yes no Tumor Yes 6 0 no Midline shift (mm)* 3.69 ± ± Hydrocephalus ratio (%)* ± ± Ventricle size (mm) * 7.7 ± ± Ventriculoostomy stie Right Left 45 5 Combined surgery Yes no operator experiences 3-4 years years new hemorrhage Yes no tion for the distal end of catheter is at or just above the foramen of Monro(saladino et al., 2009). When the ipsilateral frontal horn or third ventricle is considered as the final location of the catheter, the inaccuracy ranged from 20% to 36% in the published literatures (Khanna et al., 1995; Kakarla et al., 2008). in this study, the inaccuracy was 35.7%, which was consistent with previous findings. However, compared to conventional definition, functional accuracy also has been described (Kakarla et al., 2008). The catheter was considered as misplacement when it was intraparenchymal or in extraventricular space. Based on different reference point of catheter tip, the overall inaccuracy of evd placement varies, ranging from 6.3% to 36% (Table 3). of these studies, most failed to describe the exact location of the misplaced catheters (Bogdahn et al., 1992; stangl et al., 1998; o Leary et al., 2000; anderson et al., 2004). The relevant risk factors contributing to the final location of catheter placed by freehand method were also infrequently discussed (Khanna et al., 1995; Kakarla et al., 2008; saladino et al., 2009). in a retrospective review of 346 patients received freehand ventriculostomy placed by neurosurgical trainees over an 11-month period in a single institute, Kakarla et al. reported the overall functional accuracy was 87% (Kakarla et al., 2008). Depended on their new grading system, the misplacement in the eloquent parenchyma such as brainstem, cerebellum, internal capsule, basal ganglia, thalamus, occipital cortex and basal cisterns occurred in 46 occasions (13%). in the subgroup, the rate of misplaced evds was highest in patients with trauma, midline shift and absent subarachnoid hemorrhage. They concluded that the dislocated or compressed ventricles were the keystone resulting into these misplacements. according to the new grading system reported by Kakarla et al. (Kakarla et al., 2008), the functional accuracy in current study was 86%. in the subgroup, the misplaced evds didn t significantly occur in patients experienced trauma or absent subarachnoid hemorrhage. neither midline shift nor combined surgery contributed the misplacement. only the hydrocephalus ratio and the ventricular size
5 26 C.-T. HsieH et al. FiG. 3. The head computed tomographic scan revealed the new hemorrhage around the catheter along the tract. statistically and significantly affected the accuracy. in the misplaced group, the mean of hydrocephalus ratio and ventricular size were 28.8% and 5.6 mm, respectively. except the brain shifting (midline shift), we concur with Kakarla et al. that the small ventricle was considered as the main reason contributing for the misplaced evds (Kakarla et al., 2008). of the 212 catheters analyzed, saladino et al. reported 12.3% was considered misplaced (saladino et al., 2009). The most misplaced catheter was intraparenchymal, where the contralateral or ipsilateral basal ganglia was the most common misplaced location. However, no detail description was mentioned. in current study, 7 (43.8%) of 16 intraparenchymal misplacement occurred in the ipsilataeral or contralateral basal ganglia. otherwise, surprisingly, the previous studies also demonstrated the rare immediate neurological complications were associated with these misplaced catheters (anderson et al., 2004; Kakarla et al., 2008). The overall replaced rate has been estimated approximately about 3% in the literature (Roitberg et al., 2001; Kakarla et al., 2008; ngo et al., 2009; saladino et al., 2009). in our study, although the 18 catheters were misplaced, no known neurological complications from the misplaced catheters were found. otherwise, only four (3.1%) of them required a replacement or reposition. our result was consisted with the previous findings. Hemorrhage was another immediate complication associated with evd placement. The rate of evdrelated hemorrhages ranges from 0 to 41% (stangl et al., 1998; anderson et al., 2004; Kakarla et al., 2008; Gardner et al., 2009). some severe hemorrhages such as acute subdural hemorrhages, epidural hemorrhages or intracerebral hemorrhegas have been Table 3 summarized the accuracy of ventriculostomy by freehand method in the published literatures author Year inaccuracy Reference point Bogdahn et al. (2) % unknown Khanna et al. (8) % Frontal horn stangl et al. (17) % unknown o Leary et al. (13) % 8 (33.3%) of 24 insertion crossed the midline but only two required replacement. anderson et al. (1) % unknown *Kakarla et al. (6) % Brainstem/cerebellum/internal capsule/basal ganglia/thalamus/ occipital cortex/ basal cisterns Huyette et al. (5) % nonventricular spaces. Lind et al. (11) % outside frontal horn and third ventricle ngo et al. (12) % intraparenchyma and basal ganglia saladino et al. (16) % intraparenchyma / extraventricular spaces Current study 14% Basal ganglia/thalamus/cerebrum/corpus Callosum/basal cistern *The inaccuracy was 23.1% when the catheter was outside ipsilateral frontal horn or third ventricle.
6 THe MisPLaCeMenT of external VenTRiCuLaR DRain 27 described and some of them required a craniotomy (Huyette et al., 2008; Gardner et al., 2009; Lind et al., 2009; ngo et al., 2009; saladino et al., 2009). in this study, 21 (16.2%) new hemorrhages were observed on subsequent head CT scans. no patients experienced these evd-related hemorrhages required a craniotomy. However, the difference of occurrence of new hemorrhages between the misplaced group and control group didn t reach the significances. Despite the freehand method, several devices such as the Ghajar guide (Ghajar, 1985) have been developed to improve the accuracy of ventriculostomy (o Leary et al., 2000). except the surface landmarks, it provides to guide a catheter in a path perpendicular to the skull surface into the frontal horn of the lateral ventricle. However, in cases of compressed or dislocated ventricles, the ventriculostomy is difficult based on conventional surface landmarks or these assisted devices. The ideal direction should be still modified according to the pre-operative head CT scans and the operator s experience (stangl et al., 1998; anderson et al., 2004). With the development of equipments and techniques, the stereotactic system, frameless neuronavigation or CT-guidance offer the neurosurgeons in localizing the optimal site of catheter and in selecting the proper trajectory (Krotz et al., 2004; Prat et al., 2009). However, some disadvantages such the more expansive price, more required equipment, more technique requirement and the increase of the procedure time are not acceptable in an emergent situation. There are some limitations in our study. First, it is a retrospective study and we only include the patients who have the subsequent head CT scans after evd placements. The misplaced rate in current study can t reflect the overall situation. The further prospective study with regular subsequent head CT scans should be conducted to estimate the exact misplaced rate. secondary, the majority of these misplaced evds didn t cause clinically immediate sequelaes. The long-term deficits also should be investigated. Third, we didn t record the number of passes required to achieve the successful ventricular puncture. otherwise, the possibility of coagulopathy did not investigated in these emergent situations. These may be the main reason that we have the higher new hemorrhage rate after catheters insertion. Conclusion in this study, the functional accuracy of evd placement was about 86%. only 3.1% of misplaced evds required a replacement or reposition surgery. although the new hemorrhage associated with evd placement was higher about 16.2%, no patients required a craniotomy. using the freehand method, evd placement is a safe and effective procedure in management of these emergent neurosurgical diseases. ReFeRenCes anderson RC, Kan P, Klimo P, Brockmeyer DL, Walker ML. et al. Complications of intracranial pressure monitoring in children with head trauma. J neurosurg. 2004;101:53-8. Bogdahn u, Lau W, Hassel W, Gunreben G, Mertens HG. et al. Continuous-pressure controlled, external ventricular drainage for treatment of acute hydrocephalus evaluation of risk factors. neurosurgery. 1992;31: ; discussion Gardner Pa, engh J, atteberry D, Moossy JJ. Hemorrhage rates after external ventricular drain placement. J neurosurg. 2009;110: Ghajar JB. a guide for ventricular catheter placement. Technical note. J neurosurg. 1985;63: Huyette DR, Turnbow BJ, Kaufman C, Vaslow DF, Whiting BB. et al. accuracy of the freehand pass technique for ventriculostomy catheter placement: retrospective assessment using computed tomography scans. J neurosurg. 2008;108: Kakarla uk, Kim LJ, Chang sw, Theodore n, spetzler RF. safety and accuracy of bedside external ventricular drain placement. neurosurgery. 2008;63:ons162-6; discussion ons Khan sh, Kureshi iu, Mulgrew T, Ho sy, onyiuke HC. Comparison of percutaneous ventriculostomies and intraparenchymal monitor: a retrospective evaluation of 156 patients. acta neurochir suppl. 1998; 71:50-2. Khanna RK, Rosenblum ML, Rock JP, Malik GM. Prolonged external ventricular drainage with percutaneous long-tunnel ventriculostomies. J neuro surg. 1995;83: Krotz M, Linsenmaier u, Kanz KG, Pfeifer KJ, Mutschler W. et al. evaluation of minimally invasive percutaneous CT-controlled ventriculostomy in patients with severe head trauma. eur Radiol. 2004;14: Lind CR, Correia Ja, Law aj, Kejriwal R. a survey of surgical techniques for catheterising the cerebral lateral ventricles. J Clin neurosci. 2008;15: Lind CR, Tsai am, Lind CJ, Law aj. Ventricular catheter placement accuracy in non-stereotactic shunt surgery for hydrocephalus. J Clin neurosci. 2009; 16: ngo Qn, Ranger a, singh Rn, Kornecki a, seabrook Ja. et al. external ventricular drains in pediatric patients. Pediatr Crit Care Med. 2009;10: o Leary st, Kole MK, Hoover Da, Hysell se, Thomas a. et al. efficacy of the Ghajar Guide revisited:a prospective study. J neurosurg. 2000;92:801-3.
7 28 C.-T. HsieH et al. Prat R, Galeano i. endoscopic biopsy of foramen of Monro and third ventricle lesions guided by frameless neuronavigation: usefulness and limitations. Clin neurol neurosurg. 2009;111: Roitberg BZ, Khan n, alp Ms, Hersonskey T, Charbel FT. et al. Bedside external ventricular drain placement for the treatment of acute hydrocephalus. Br J neurosurg. 2001;15: saladino a, White JB, Wijdicks ef, Lanzino G. Malplacement of ventricular catheters by neurosurgeons: a single institution experience. neurocrit Care. 2009; 10: stangl ap, Meyer B, Zentner J, schramm J. Continuous external CsF drainage a perpetual problem in neurosurgery. surg neurol. 1998;50: Dr. Ming-Ying Liu, Department of neurological surgery, Tri-service General Hospital, no. 325, sec. 2, Cheng-Kung Road, Taipei, Taiwan nogor@mail2000.com.tw
Accuracy of the Free Hand Placement of an External Ventricular Drain (EVD)
 KOR J CEREBROVASCULAR SURGERY June 2O10 Vol. 12 No 2, page 82-6 Accuracy of the Free Hand Placement of an External Ventricular Drain (EVD) Department of Neurosurgery, Gachon University of Medicine & Science,
KOR J CEREBROVASCULAR SURGERY June 2O10 Vol. 12 No 2, page 82-6 Accuracy of the Free Hand Placement of an External Ventricular Drain (EVD) Department of Neurosurgery, Gachon University of Medicine & Science,
Accuracy and Safety of Bedside External Ventricular Drain Placement at Two Different Cranial Sites : Kocher s Point versus Forehead
 online ML Comm www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2011.50.4.317 J Korean Neurosurg Soc 50 : 317-321, 2011 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2011 The Korean Neurosurgical
online ML Comm www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2011.50.4.317 J Korean Neurosurg Soc 50 : 317-321, 2011 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2011 The Korean Neurosurgical
Do Iatrogenic Factors Bias the Placement of External Ventricular Catheters? A Single Institute Experience and Review of the Literature
 Neurol Med Chir (Tokyo) 5, 8 86, Do Iatrogenic Factors Bias the Placement of External Ventricular Catheters? A Single Institute Experience and Review of the Literature Christoph M. WOERNLE, Jan-Karl BURKHARDT,
Neurol Med Chir (Tokyo) 5, 8 86, Do Iatrogenic Factors Bias the Placement of External Ventricular Catheters? A Single Institute Experience and Review of the Literature Christoph M. WOERNLE, Jan-Karl BURKHARDT,
Freehand insertion of external ventricular drains
 CLINICAL ARTICLE Utilizing preprocedural CT scans to identify patients at risk for suboptimal external ventricular drain placement with the freehand insertion technique Mitchell P. Wilson, MD, 1 Cian O
CLINICAL ARTICLE Utilizing preprocedural CT scans to identify patients at risk for suboptimal external ventricular drain placement with the freehand insertion technique Mitchell P. Wilson, MD, 1 Cian O
Perioperative Management Of Extra-Ventricular Drains (EVD)
 Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
External ventricular drain (EVD) placement for cerebrospinal. FOCUS Neurosurg Focus 43 (5):E5, 2017
 NEUROSURGICAL FOCUS Neurosurg Focus 43 (5):E5, 2017 Real-time ultrasound-guided external ventricular drain placement: technical note James H. Manfield, MBBS, MSc, MRCS, 1 and Kenny K. H. Yu, MBBS, MRCS,
NEUROSURGICAL FOCUS Neurosurg Focus 43 (5):E5, 2017 Real-time ultrasound-guided external ventricular drain placement: technical note James H. Manfield, MBBS, MSc, MRCS, 1 and Kenny K. H. Yu, MBBS, MRCS,
Accurate placement of a ventricular catheter is crucial
 clinical article J Neurosurg 124:1429 1433, 2016 Calvarial slope affecting accuracy of Ghajar Guide technique for ventricular catheter placement Jaechan Park, MD, PhD, 1,2 Wonsoo Son, MD, 1,2 Ki-Su Park,
clinical article J Neurosurg 124:1429 1433, 2016 Calvarial slope affecting accuracy of Ghajar Guide technique for ventricular catheter placement Jaechan Park, MD, PhD, 1,2 Wonsoo Son, MD, 1,2 Ki-Su Park,
Hemorrhage Rates Associated with Two Methods of Ventriculostomy: External Ventricular Drainage vs. Ventriculoperitoneal Shunt Procedure
 ORIGINAL ARTICLE Neurol Med Chir (Tokyo) 54, 545 551, 2014 doi: 10.2176/nmc.oa.2013-0178 Online February 10, 2014 Hemorrhage Rates Associated with Two Methods of Ventriculostomy: External Ventricular Drainage
ORIGINAL ARTICLE Neurol Med Chir (Tokyo) 54, 545 551, 2014 doi: 10.2176/nmc.oa.2013-0178 Online February 10, 2014 Hemorrhage Rates Associated with Two Methods of Ventriculostomy: External Ventricular Drainage
Multiple Intracranial High Density Foci after Brain Parenchymal Catheterization
 CLINICL RTICLE Korean J Neurotrauma 2016;12(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/10.13004/kjnt.2016.12.2.118 Multiple Intracranial High Density Foci after rain Parenchymal Catheterization
CLINICL RTICLE Korean J Neurotrauma 2016;12(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/10.13004/kjnt.2016.12.2.118 Multiple Intracranial High Density Foci after rain Parenchymal Catheterization
An approach using the occipital parietal point for placement of ventriculoperitoneal catheters in adults. Abstract Introduction Methods Results
 An approach using the occipital parietal point for placement of ventriculoperitoneal catheters in adults. Jason Duong, DO 1, Dan Miulli DO 1, Fanglong Dong, PhD 2, Andrew Sumida MSIV 3, 1 Neurosurgery
An approach using the occipital parietal point for placement of ventriculoperitoneal catheters in adults. Jason Duong, DO 1, Dan Miulli DO 1, Fanglong Dong, PhD 2, Andrew Sumida MSIV 3, 1 Neurosurgery
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS.
 External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS. External Ventricular Drain Indications: Therapeutic (To relieve raised
External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS. External Ventricular Drain Indications: Therapeutic (To relieve raised
Traumatic brain Injury- An open eye approach
 Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
The use of intracranial pressure (ICP) monitoring in the
 Training Protocol for Intracranial Pressure Monitor Placement by Nonneurosurgeons: 5-Year Experience Kathryn Ko, MD, and Alicia Conforti, RN Background: This report evaluates a protocol for training nonneurosurgeon
Training Protocol for Intracranial Pressure Monitor Placement by Nonneurosurgeons: 5-Year Experience Kathryn Ko, MD, and Alicia Conforti, RN Background: This report evaluates a protocol for training nonneurosurgeon
The Hydrocephalus Clinical Research Network
 J Neurosurg Pediatrics 14:173 178, 2014 AA, 2014 Factors associated with ventricular catheter movement and inaccurate catheter location: post hoc analysis of the Hydrocephalus Clinical Research Network
J Neurosurg Pediatrics 14:173 178, 2014 AA, 2014 Factors associated with ventricular catheter movement and inaccurate catheter location: post hoc analysis of the Hydrocephalus Clinical Research Network
SOP: Cerebral Ultrasound
 SOP: Cerebral Ultrasound Version Author(s) Date Changes Approved by 1.0 Cornelia Hagmann Manon Benders 29.5.2012 Initial Version Gorm Greisen 1.1 Cornelia Hagmann 18.6.2012 Minor changes Gorm Greisen 1.2
SOP: Cerebral Ultrasound Version Author(s) Date Changes Approved by 1.0 Cornelia Hagmann Manon Benders 29.5.2012 Initial Version Gorm Greisen 1.1 Cornelia Hagmann 18.6.2012 Minor changes Gorm Greisen 1.2
Slide 1. Slide 2. Slide 3. Tomography vs Topography. Computed Tomography (CT): A simplified Topographical review of the Brain. Learning Objective
 Slide 1 Computed Tomography (CT): A simplified Topographical review of the Brain Jon Wheiler, ACNP-BC Slide 2 Tomography vs Topography Tomography: A technique for displaying a representation of a cross
Slide 1 Computed Tomography (CT): A simplified Topographical review of the Brain Jon Wheiler, ACNP-BC Slide 2 Tomography vs Topography Tomography: A technique for displaying a representation of a cross
Effect of Electromagnetic Navigated Ventriculoperitoneal Shunt Placement on Failure Rates
 www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2013.53.3.150 J Korean Neurosurg Soc 53 : 150-154, 2013 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2013 The Korean Neurosurgical Society Clinical
www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2013.53.3.150 J Korean Neurosurg Soc 53 : 150-154, 2013 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2013 The Korean Neurosurgical Society Clinical
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
The significance of traumatic haematoma in the
 Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
Complex Hydrocephalus
 2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
Insertion of an external ventricular drain (EVD) is a
 Short Communication Intracerebral Hemorrhage With Severe Ventricular Involvement Lumbar Drainage for Communicating Hydrocephalus Hagen B. Huttner, MD; Simon Nagel, MD; Elena Tognoni; Martin Köhrmann, MD;
Short Communication Intracerebral Hemorrhage With Severe Ventricular Involvement Lumbar Drainage for Communicating Hydrocephalus Hagen B. Huttner, MD; Simon Nagel, MD; Elena Tognoni; Martin Köhrmann, MD;
Brain Meninges, Ventricles and CSF
 Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Moron General Hospital Ciego de Avila Cuba. Department of Neurological Surgery
 Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
The management of ICH when to operate when not to?
 The management of ICH when to operate when not to? Intracranial Hemorrhage High Incidence o Accounts for 10-15% of all strokes 1,2,5 o 80,000 cases in US; 2 million WW 2,5 o Incidence doubles for African-
The management of ICH when to operate when not to? Intracranial Hemorrhage High Incidence o Accounts for 10-15% of all strokes 1,2,5 o 80,000 cases in US; 2 million WW 2,5 o Incidence doubles for African-
Placement and revision of ventricular shunts for hydrocephalus
 J Neurosurg 120:684 696, 2014 AANS, 2014 Improvement in clinical outcomes following optimal targeting of brain ventricular catheters with intraoperative imaging Clinical article Christopher G. Janson,
J Neurosurg 120:684 696, 2014 AANS, 2014 Improvement in clinical outcomes following optimal targeting of brain ventricular catheters with intraoperative imaging Clinical article Christopher G. Janson,
Ventriculostomy is one of the most common procedures. Revisiting the rules for freehand ventriculostomy: a virtual reality analysis
 CLINICAL ARTICLE J Neurosurg 128:1250 1257, 2018 Revisiting the rules for freehand ventriculostomy: a virtual reality analysis Clemens Raabe, 1,2 Jens Fichtner, MD, 2 Jürgen Beck, MD, 2 Jan Gralla, MD,
CLINICAL ARTICLE J Neurosurg 128:1250 1257, 2018 Revisiting the rules for freehand ventriculostomy: a virtual reality analysis Clemens Raabe, 1,2 Jens Fichtner, MD, 2 Jürgen Beck, MD, 2 Jan Gralla, MD,
A Simple, Fast and Fully Automated Approach for Midline Shift Measurement on Brain Computed Tomography
 A Simple, Fast and Fully Automated Approach for Midline Shift Measurement on Brain Computed Tomography Huan-Chih Wang, Shih-Hao Ho, Furen Xiao, Jen-Hai Chou 2 Mar 2017 Abstract: Brain CT has become a standard
A Simple, Fast and Fully Automated Approach for Midline Shift Measurement on Brain Computed Tomography Huan-Chih Wang, Shih-Hao Ho, Furen Xiao, Jen-Hai Chou 2 Mar 2017 Abstract: Brain CT has become a standard
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score
 Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
HIROSHI NAKAGUCHI, M.D., PH.D., TAKEO TANISHIMA, M.D., PH.D., Clinical Material and Methods
 J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Quality Metrics. Stroke Related Procedure Outcomes
 Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Researcher 2018;10(3)
 Comparative study between frontal and posterior parietal ventriculo-peritoneal shunts in management of hydrocephalus Prof. Dr. Abdelhalim Moasa, Dr. Mohamed Hasan and Mohamed Abdelrazek Department of Neurosurgery,
Comparative study between frontal and posterior parietal ventriculo-peritoneal shunts in management of hydrocephalus Prof. Dr. Abdelhalim Moasa, Dr. Mohamed Hasan and Mohamed Abdelrazek Department of Neurosurgery,
NEURORADIOLOGY DIL part 3
 NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
Intracranial air on computerized tomography ANNE G. OSBORN, M.D., JONATHAN H. DAINES, M.D., S. DOUGLAS WING, M.D., AND ROBERT E. ANDERSON, M.D.
 J Neurosurg 48:355-359, 1978 Intracranial air on computerized tomography ANNE G. OSBORN, M.D., JONATHAN H. DAINES, M.D., S. DOUGLAS WING, M.D., AND ROBERT E. ANDERSON, M.D. Department of Radiology, University
J Neurosurg 48:355-359, 1978 Intracranial air on computerized tomography ANNE G. OSBORN, M.D., JONATHAN H. DAINES, M.D., S. DOUGLAS WING, M.D., AND ROBERT E. ANDERSON, M.D. Department of Radiology, University
Stereotactic Burr Hole Aspiration Surgery for Spontaneous Hypertensive Cerebellar Hemorrhage
 Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2012.14.3.170 Original Article Stereotactic Burr Hole Aspiration Surgery for Spontaneous
Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2012.14.3.170 Original Article Stereotactic Burr Hole Aspiration Surgery for Spontaneous
Tyler Carson D.O., Vladamir Cortez D.O., Dan E. Miulli D.O.
 Bedside Intracranial Hematoma Evacuation and Intraparenchymal Drain Placement for Spontaneous Intracranial Hematoma Larger than 30 cc in Volume: Institutional Experience and Patient Outcomes Tyler Carson
Bedside Intracranial Hematoma Evacuation and Intraparenchymal Drain Placement for Spontaneous Intracranial Hematoma Larger than 30 cc in Volume: Institutional Experience and Patient Outcomes Tyler Carson
Extent of subarachnoid hemorrhage and development of hydrocephalus
 Clinical Science Extent of subarachnoid hemorrhage and development of hydrocephalus Mirsad Hodžić, Mirza Moranjkić, Zlatko Ercegović, Harun Brkić Department of neurosurgery, University Clinical Center
Clinical Science Extent of subarachnoid hemorrhage and development of hydrocephalus Mirsad Hodžić, Mirza Moranjkić, Zlatko Ercegović, Harun Brkić Department of neurosurgery, University Clinical Center
Stroke & Neurovascular Center of New Jersey. Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center
 Stroke & Neurovascular Center of New Jersey Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center Past, present and future Past, present and future Cerebral Blood Flow Past, present and future
Stroke & Neurovascular Center of New Jersey Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center Past, present and future Past, present and future Cerebral Blood Flow Past, present and future
2/20/2019 BRAIN DISSECTION CODING AND DOCUMENTATION OBJECTIVES INTRODUCTION
 BRAIN DISSECTION CODING AND DOCUMENTATION Diana R. Phelps, CPC, CPC-I, CEMC OBJECTIVES Identify general structure of the human brain Describe how the different parts work Recognized the two hemispheres
BRAIN DISSECTION CODING AND DOCUMENTATION Diana R. Phelps, CPC, CPC-I, CEMC OBJECTIVES Identify general structure of the human brain Describe how the different parts work Recognized the two hemispheres
For Emergency Doctors. Dr Suzanne Smallbane November 2011
 For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D.
 J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
Pterional-subolfactory Approach for Treatment of High Positioned Anterior Communicating Artery Aneurysms
 Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2013.15.3.177 Clinical Article Pterional-subolfactory Approach for Treatment of
Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2013.15.3.177 Clinical Article Pterional-subolfactory Approach for Treatment of
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
Attenuation value in HU From -500 To HU From -10 To HU From 60 To 90 HU. From 200 HU and above
 Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
intracranial anomalies
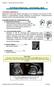 Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES
 PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES INTRODUCTION: Traumatic Brain Injury (TBI) is an important clinical entity in acute care surgery without well-defined guidelines
PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES INTRODUCTION: Traumatic Brain Injury (TBI) is an important clinical entity in acute care surgery without well-defined guidelines
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT. G. Tamburrini, Rome
 INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
Distal anterior cerebral artery (DACA) aneurysms are. Case Report
 248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
APP Placement of ICP Monitors. Sanjay Patra, MD
 APP Placement of ICP Monitors Sanjay Patra, MD Can midlevel providers place external ventricular drains safely and accurately? Sanjay Patra MD MSc Director Epilepsy Surgery Director Brain Trauma Spectrum
APP Placement of ICP Monitors Sanjay Patra, MD Can midlevel providers place external ventricular drains safely and accurately? Sanjay Patra MD MSc Director Epilepsy Surgery Director Brain Trauma Spectrum
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Complications of intracranial pressure monitoring in children with head trauma
 J Neurosurg (Pediatrics 2) 101:53 58, 2004 Complications of intracranial pressure monitoring in children with head trauma RICHARD C. E. ANDERSON, M.D., PETER KAN, M.D., PAUL KLIMO, M.D., M.P.H., DOUGLAS
J Neurosurg (Pediatrics 2) 101:53 58, 2004 Complications of intracranial pressure monitoring in children with head trauma RICHARD C. E. ANDERSON, M.D., PETER KAN, M.D., PAUL KLIMO, M.D., M.P.H., DOUGLAS
Ultrasound examination of the neonatal brain
 Ultrasound examination of the neonatal brain Guideline for the performance and reporting of neonatal and preterm brain ultrasound examination, by the Finnish Perinatology Society and the Paediatric Radiology
Ultrasound examination of the neonatal brain Guideline for the performance and reporting of neonatal and preterm brain ultrasound examination, by the Finnish Perinatology Society and the Paediatric Radiology
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Radiological evaluation of ventriculoperitoneal shunt systems
 Radiological evaluation of ventriculoperitoneal shunt systems Poster No.: C-702 Congress: ECR 2009 Type: Educational Exhibit Topic: Neuro Authors: T. Rodt, C. von Falck, C. Tschan, M. Diensthuber, J. Zajaczek,
Radiological evaluation of ventriculoperitoneal shunt systems Poster No.: C-702 Congress: ECR 2009 Type: Educational Exhibit Topic: Neuro Authors: T. Rodt, C. von Falck, C. Tschan, M. Diensthuber, J. Zajaczek,
Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions
 https://doi.org/10.1007/s12028-017-0487-3 ORIGINAL ARTICLE Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions Sherri A. Braksick
https://doi.org/10.1007/s12028-017-0487-3 ORIGINAL ARTICLE Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions Sherri A. Braksick
Lumbar Catheter for Monitoring of Intracranial Pressure in Patients with Post-Hemorrhagic Communicating Hydrocephalus
 DOI 1.17/s1228-1-949-6 ORIGINAL ARTICLE Lumbar Catheter for Monitoring of Intracranial Pressure in Patients with Post-Hemorrhagic Communicating Hydrocephalus Verena Speck Dimitre Staykov Hagen B. Huttner
DOI 1.17/s1228-1-949-6 ORIGINAL ARTICLE Lumbar Catheter for Monitoring of Intracranial Pressure in Patients with Post-Hemorrhagic Communicating Hydrocephalus Verena Speck Dimitre Staykov Hagen B. Huttner
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER
 CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
Treatment of Acute Hydrocephalus After Subarachnoid Hemorrhage With Serial Lumbar Puncture
 19 Treatment of Acute After Subarachnoid Hemorrhage With Serial Lumbar Puncture Djo Hasan, MD; Kenneth W. Lindsay, PhD, FRCS; and Marinus Vermeulen, MD Downloaded from http://ahajournals.org by on vember,
19 Treatment of Acute After Subarachnoid Hemorrhage With Serial Lumbar Puncture Djo Hasan, MD; Kenneth W. Lindsay, PhD, FRCS; and Marinus Vermeulen, MD Downloaded from http://ahajournals.org by on vember,
A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage
 July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN
 Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN History of Marshall scale Proposed by Marshall, et al in 1991 to classify head
Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN History of Marshall scale Proposed by Marshall, et al in 1991 to classify head
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage
 Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
PA SYLLABUS. Syllabus for students of the FACULTY OF MEDICINE No.2
 Approved At the meeting of the Faculty Council Medicine No. of Approved At the meeting of the chair of Neurosurgery No. of Dean of the Faculty Medicine No.2 PhD, associate professor M. Betiu Head of the
Approved At the meeting of the Faculty Council Medicine No. of Approved At the meeting of the chair of Neurosurgery No. of Dean of the Faculty Medicine No.2 PhD, associate professor M. Betiu Head of the
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries. Goes to 6N
 Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Adult - Cerebrovascular. Adult - Cranio-Cervical Junction. Adult - Epilepsy. Adult - Hydrocephalus
 list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
Suprasellar Arachnoid Cysts. Wan Tew SEOW FRACS Singapore
 Suprasellar Arachnoid Cysts Wan Tew SEOW FRACS Singapore Distribution Intracranial Arachnoid Cysts Sylvian fissure 49% CPA 11% Quadrigeminal 10% Vermian 9% Sellar and suprasellar 9% Interhemispheric 5%
Suprasellar Arachnoid Cysts Wan Tew SEOW FRACS Singapore Distribution Intracranial Arachnoid Cysts Sylvian fissure 49% CPA 11% Quadrigeminal 10% Vermian 9% Sellar and suprasellar 9% Interhemispheric 5%
Integra B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE
 Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Neurosonography: State of the art
 Neurosonography: State of the art Lisa H Lowe, MD, FAAP Professor and Academic Chair, University MO-Kansas City Pediatric Radiologist, Children s Mercy Hospitals and Clinics Learning objectives After this
Neurosonography: State of the art Lisa H Lowe, MD, FAAP Professor and Academic Chair, University MO-Kansas City Pediatric Radiologist, Children s Mercy Hospitals and Clinics Learning objectives After this
Although neuroendoscopy was originally devised. Small-ventricle neuroendoscopy for pediatric brain tumor management.
 J Neurosurg Pediatrics 7:000 000, 7:104 110, 2011 Small-ventricle neuroendoscopy for pediatric brain tumor management Clinical article Robert P. Naftel, M.D., 1 Chevis N. Shannon, M.B.A., M.P.H., Dr.P.H.,
J Neurosurg Pediatrics 7:000 000, 7:104 110, 2011 Small-ventricle neuroendoscopy for pediatric brain tumor management Clinical article Robert P. Naftel, M.D., 1 Chevis N. Shannon, M.B.A., M.P.H., Dr.P.H.,
PRIVILEGE APPLICATION FORM - [Mercy Medical Center]
![PRIVILEGE APPLICATION FORM - [Mercy Medical Center] PRIVILEGE APPLICATION FORM - [Mercy Medical Center]](/thumbs/89/98821167.jpg) Current Privilege Status Key Practitioner's Current Privilege status is signified in ( ) preceding each privilege. G = W = Withdrawn T = Temporary P = With Proctor A = Assist with C = With Consult E =
Current Privilege Status Key Practitioner's Current Privilege status is signified in ( ) preceding each privilege. G = W = Withdrawn T = Temporary P = With Proctor A = Assist with C = With Consult E =
Serial Brain CT Scans in Severe Head Injury without Intracranial Pressure Monitoring
 online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(1):26-30 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.1.26 Serial Brain CT Scans in Severe Head Injury without
online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(1):26-30 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.1.26 Serial Brain CT Scans in Severe Head Injury without
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
CSF MANAGEMENT REIMBURSEMENT GUIDE
 CSF MANAGEMENT REIMBURSEMENT GUIDE TABLE OF CONTENTS Cerebrospinal Fluid Shunts ICD-10-CM diagnosis Codes...2 ICD-10-PCS Codes...4 Physician and Hospital Outpatient Coding...6 Hospital Inpatient DRG Assignments...7
CSF MANAGEMENT REIMBURSEMENT GUIDE TABLE OF CONTENTS Cerebrospinal Fluid Shunts ICD-10-CM diagnosis Codes...2 ICD-10-PCS Codes...4 Physician and Hospital Outpatient Coding...6 Hospital Inpatient DRG Assignments...7
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
The incidence of CT scan use is drastically on the
 J Neurosurg Pediatrics 12:406 410, 2013 AANS, 2013 Low-dose head computed tomography in children: a single institutional experience in pediatric radiation risk reduction Clinical article Ryan P. Morton,
J Neurosurg Pediatrics 12:406 410, 2013 AANS, 2013 Low-dose head computed tomography in children: a single institutional experience in pediatric radiation risk reduction Clinical article Ryan P. Morton,
Brain Arteriovenous Malformations Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos
 Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos Neuroradiology Department Hospital de Santa Maria University of Lisbon CEREBRAL AVM CLINICAL / EPIDEMIOLOGY Brain
Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos Neuroradiology Department Hospital de Santa Maria University of Lisbon CEREBRAL AVM CLINICAL / EPIDEMIOLOGY Brain
Analysis of Prognostic Factors for Chronic Subdural Hematoma
 online ML Comm 0CLINICAL ARTICLE0 J Kor Neurotraumatol Soc 2008;4:14-18 ISSN 1738-8708 Analysis of Prognostic Factors for Chronic Subdural Hematoma Young-Il Kim, MD, Jung-Hoon Lee, MD, Seung-Won Park,
online ML Comm 0CLINICAL ARTICLE0 J Kor Neurotraumatol Soc 2008;4:14-18 ISSN 1738-8708 Analysis of Prognostic Factors for Chronic Subdural Hematoma Young-Il Kim, MD, Jung-Hoon Lee, MD, Seung-Won Park,
Short Communications. Alcoholic Intracerebral Hemorrhage
 Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
North Oaks Trauma Symposium Friday, November 3, 2017
 Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
Extradural hematoma (EDH) accounts for 2% of all head injuries (1). In
 CASE REPORT Conservative management of extradural hematoma: A report of sixty-two cases A. Rahim H. Zwayed 1, Brandon Lucke-Wold 2 Zwayed ARH, Lucke-wold B. Conservative management of extradural hematoma:
CASE REPORT Conservative management of extradural hematoma: A report of sixty-two cases A. Rahim H. Zwayed 1, Brandon Lucke-Wold 2 Zwayed ARH, Lucke-wold B. Conservative management of extradural hematoma:
Hypertensive Caudate Hemorrhage Prognostic Predictor, Outcome, and Role of External Ventricular Drainage
 Hypertensive Caudate Hemorrhage Prognostic Predictor, Outcome, and Role of External Ventricular Drainage Po-Chou Liliang, MD; Cheng-Loong Liang, MD; Cheng-Hsien Lu, MD; Hsueh-Wen Chang, PhD; Ching-Hsiao
Hypertensive Caudate Hemorrhage Prognostic Predictor, Outcome, and Role of External Ventricular Drainage Po-Chou Liliang, MD; Cheng-Loong Liang, MD; Cheng-Hsien Lu, MD; Hsueh-Wen Chang, PhD; Ching-Hsiao
Residence of Discipline of Neurosurgery of Hospital da Santa Casa de Misericórdia of Sao Paulo Sao Paulo, Brazil
 Cronicon OPEN ACCESS NEUROLOGY Research Article Efficacy of the Lamina Terminalis Fenestration Associated With the Liliequist Membrane Fenestration in Reducing Shunt-Dependent Hydrocephalus Following Aneurysm
Cronicon OPEN ACCESS NEUROLOGY Research Article Efficacy of the Lamina Terminalis Fenestration Associated With the Liliequist Membrane Fenestration in Reducing Shunt-Dependent Hydrocephalus Following Aneurysm
Surgical techniques and procedures for cerebrovascular surgery. Surgery for the AVF at the cranio-cervical junction and high cervical spine
 VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
Keyhole craniectomy in the surgical management of spontaneous intracerebral hematoma
 Neurology Asia 2007; 12 : 21 27 Keyhole craniectomy in the surgical management of spontaneous intracerebral hematoma S Balaji Pai, RG Varma, JKBC Parthiban, KN Krishna, RM Varma, *R Srinivasa,*PT Acharya,*BP
Neurology Asia 2007; 12 : 21 27 Keyhole craniectomy in the surgical management of spontaneous intracerebral hematoma S Balaji Pai, RG Varma, JKBC Parthiban, KN Krishna, RM Varma, *R Srinivasa,*PT Acharya,*BP
Lothian Audit of the Treatment of Cerebral Haemorrhage (LATCH)
 1. INTRODUCTION Stroke physicians, emergency department doctors, and neurologists are often unsure about which patients they should refer for neurosurgical intervention. Early neurosurgical evacuation
1. INTRODUCTION Stroke physicians, emergency department doctors, and neurologists are often unsure about which patients they should refer for neurosurgical intervention. Early neurosurgical evacuation
Concurrent Subarachnoid Hemorrhage and Acute Myocardial Infarction: A Case Report
 Concurrent subarachnoid hemorrhage and AMI 155 Concurrent Subarachnoid Hemorrhage and Acute Myocardial Infarction: A Case Report Chen-Chuan Cheng 1, Wen-Shiann Wu 1, Chun-Yen Chiang 1, Tsuei-Yuang Huang
Concurrent subarachnoid hemorrhage and AMI 155 Concurrent Subarachnoid Hemorrhage and Acute Myocardial Infarction: A Case Report Chen-Chuan Cheng 1, Wen-Shiann Wu 1, Chun-Yen Chiang 1, Tsuei-Yuang Huang
A Less Invasive Approach for Ruptured Aneurysm with Intracranial Hematoma: Coil Embolization Followed by Clot Evacuation
 A Less Invasive Approach for Ruptured Aneurysm with Intracranial Hematoma: Coil Embolization Followed by Clot Evacuation Je Hoon Jeong, MD 1 Jun Seok Koh, MD 1 Eui Jong Kim, MD 2 Index terms: Endovascular
A Less Invasive Approach for Ruptured Aneurysm with Intracranial Hematoma: Coil Embolization Followed by Clot Evacuation Je Hoon Jeong, MD 1 Jun Seok Koh, MD 1 Eui Jong Kim, MD 2 Index terms: Endovascular
The "Keyhole": A Sign of
 473 The "Keyhole": A Sign of Herniation of a Trapped Fourth Ventricle and Other Posterior Fossa Cysts Barbara J. Wolfson' Eric N. Faerber' Raymond C. Truex, Jr. 2 When a cystic structure in the posterior
473 The "Keyhole": A Sign of Herniation of a Trapped Fourth Ventricle and Other Posterior Fossa Cysts Barbara J. Wolfson' Eric N. Faerber' Raymond C. Truex, Jr. 2 When a cystic structure in the posterior
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT
 SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury
 Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases
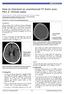 How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Original Article. Abstract. Jason Raj Johnson 3, Zamzuri Idris 1,2, Jafri Malin Abdullah 1,2,
 Original Article Prevalence of Shunt Dependency and Clinical Outcome in Patients with Massive Intraventricular Haemorrhage Treated with Endoscopic Washout and External Ventricular Drainage Jason Raj Johnson
Original Article Prevalence of Shunt Dependency and Clinical Outcome in Patients with Massive Intraventricular Haemorrhage Treated with Endoscopic Washout and External Ventricular Drainage Jason Raj Johnson
 www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
