TNF- and IFN- are overexpressed in the bone marrow of Fanconi anemia patients and TNF- suppresses erythropoiesis in vitro
|
|
|
- Byron Lucas
- 5 years ago
- Views:
Transcription
1 HEMATOPOIESIS TNF- and IFN- are overexpressed in the bone marrow of Fanconi anemia patients and TNF- suppresses erythropoiesis in vitro Carlo Dufour, Anna Corcione, Johanna Svahn, Riccardo Haupt, Vincenzo Poggi, Albert Nandor Béka ssy, Rosanna Scimè, Angela Pistorio, and Vito Pistoia In Fanconi anemia (FA) C mice tumor necrosis factor (TNF- ) and interferon (IFN- ) have key roles in the pathogenesis of bone marrow failure. In FA subjects TNF- was found to be increased in the serum and overproduced by patientderived B-cell lines. In acquired aplastic anemia, a disease in which, similarly to FA, marrow failure occurs, TNF- and IFN- act as late mediators of the stem cell damage and are overexpressed in patient marrow lymphocytes. This study evaluated in marrow mononuclear cells Introduction (MNCs) of patients with FA, the expression of negative modulators of the hematopoiesis, such as TNF-, IFN-, macrophage inflammatory protein 1 (MIP-1 ), and surface Fas ligand, and the role of TNF- on FA erythropoiesis in vitro. TNF- and IFN- were significantly overexpressed in stimulated marrow MNCs of FA patients as compared to healthy controls. MIP-1 and Fas ligand were undetectable in patients and controls. In bone marrow cultures, the addition of anti TNF- increased the size and significantly increased the number of erythroid colony-forming units and erythroid burstforming units grown from FA patients but not from healthy controls. This indicates that FA subjects have a marrow TNF- activity that inhibits erythropoiesis in vitro. TNF- has a relevant role in the pathogenesis of erythroid failure in FA patients. (Blood. 2003;102: ) 2003 by The American Society of Hematology Fanconi anemia (FA) is a rare genetic disease characterized by bone marrow (BM) failure, somatic abnormalities, susceptibility to cancer, and chromosomal fragility. At least 8 complementation groups have been identified (A, B, C, D1, D2, E, F, G) and 7 genes (A, C, D2, E, F, G, and BRCA2, which has been reported to correspond to B and D1) have been cloned so far. 1-3 FA gene products interact and form an intracellular complex that is mainly involved in DNA damage cell repair machinery. 2 BM failure represents the major cause of morbidity and mortality in patients with FA. The currently available information on its pathogenesis is mostly derived from Fanconi anemia C (FANCC) mice models. 4-6 These data indicate that the myelosuppressive cytokines interferon (IFN- ) and tumor necrosis factor (TNF- ) induce the death of hematopoietic progenitor cells through increased apoptosis, which occurs at very low cytokine concentrations 4-6 and is, in part, mediated by Fas. 6,7 The scanty information available in humans indicates that TNF- is increased in the serum of FA patients 8,9 and overproduced by lymphoblastoid cell lines derived from the patients themselves. 9 TNF- and IFN- are known to be the late effectors of the damage of the hematopoietic stem cell compartment that occurs in aplastic anemia (AA), an acquired disease that shares with FA the development of BM failure The expression of myelosuppressive cytokines in BM cells from FA patients has not yet been investigated nor has the role of these cytokines in the pathogenesis of BM failure been addressed. In the present study we assessed whether negative modulators of hematopoiesis, such as TNF-, IFN-, macrophage inflammatory protein 1 (MIP-1 ), and surface Fas ligand, were involved in the pathogenesis of BM failure in FA. To this end we tested, by flow cytometric analysis, the expression of TNF-, IFN-, MIP-1, and Fas ligand, in mononuclear cells (MNCs) isolated from the BM of 7 FA patients and 8 healthy controls. We also investigated the in vitro effects of TNF- neutralization on the growth of erythroid progenitors from BM MNCs of FA patients and controls. Patients, materials, and methods Study subjects Patients were recruited between December 1999 and February Patients were eligible if they had a confirmed diagnosis of FA, did not previously receive a BM transplant, and were infection free 4 weeks before and after the study. Controls were selected over the same time span among voluntary BM donors who had to match the same infection-free criteria as did the patients. The study protocol was approved by the Ethics Committee of the G. Gaslini Children s Hospital and by the committees of the other institutions who participated in the project. From the Hematology Unit, Department of Pediatric Hemato-Oncology, G. Gaslini Children s Hospital, Genova, Italy; Laboratory of Oncology, G. Gaslini Children s Hospital, Genova, Italy; Epidemiology and Biostatistics Section, Scientific Directorate, G. Gaslini Children s Hospital, Genova, Italy; Pediatric Hematology Unit, Pausillipon Hospital, Napoli, Italy; University Hospital Lund, Department of Pediatric Hematology-Oncology, Lund, Sweden; and Department of Hematology and BMT Unit, V. Cervello Hospital, Palermo, Italy. Submitted January 15, 2003; accepted April 22, Prepublished online as Blood First Edition Paper, May 15, 2003; DOI /blood Supported in part by Associazione Italiana per la Ricerca sull Anemia di Fanconi (AIRFA), Associazione Bambino Emopatico ed Oncologico (ABEO), Barncancerfonden, Sweden, Stiftelsen Samariten Stockholm, Sweden, and SAAR depositi oleari portuali Genova, Italy. Reprints: Carlo Dufour, Hematology Unit, Department of Pediatric Hematology- Oncology, G. Gaslini Children s Hospital, Largo G Gaslini 5, Genova, Italy; carlodufour@ospedale-gaslini.ge.it. The publication costs of this article were defrayed in part by page charge payment. Therefore, and solely to indicate this fact, this article is hereby marked advertisement in accordance with 18 U.S.C. section by The American Society of Hematology BLOOD, 15 SEPTEMBER 2003 VOLUME 102, NUMBER
2 2054 DUFOUR et al BLOOD, 15 SEPTEMBER 2003 VOLUME 102, NUMBER 6 BM sampling BM cells were obtained from patients and controls after informed consent was given either by the parents or, whenever applicable, by the study subjects themselves in conformity with the Declaration of Helsinki principles. BM samples from the patients were taken at routine diagnostic investigation or follow-up evaluation as required by the disease. In most cases marrow aspiration was performed with the patients under deep sedation. No marrow aspirations were ever performed for the purpose of this study. Normal BM samples from voluntary healthy donors were obtained, under general anesthesia, during the procedure of marrow harvest for marrow donation. No marrow aspirations were ever performed for the purpose of this study. BM cell collection and processing BM MNCs from both patients and healthy controls were isolated on Ficoll-Hypaque density gradients (Pharmacia, Uppsala, Sweden). Approximately cells/ml were obtained at the end of this procedure from FA patients. After washing in phosphate-buffered saline (PBS; Sigma, St Louis, MO) supplemented with 1% fetal bovine serum (FBS; Sigma), MNCs were frozen in a solution containing 50% RPMI 1640 medium, 40% FBS, and 10% dimethyl sulfoxide (DMSO; Sigma), stored in liquid nitrogen, and then thawed. Flow cytometric detection of intracellular cytokines BM MNCs were cultured for 5 hours at 37 C ina5%co 2 atmosphere in RPMI 1640 medium supplemented with 10% FBS in the presence of 50 ng/ml phorbol 12-myristate 13-acetate (PMA; Sigma), 250 ng/ml calcium ionophore (A23187; Sigma), and 5 g/ml brefeldin A (Sigma), which inhibits intracellular transport of cytokines into the Golgi complex thus impeding the release of cytokines in the extracellular environment. The choice of PMA and calcium ionophore for cell stimulation was dictated by the need to activate all cell types present in the BM MNC fraction, irrespective of the CD3 or CD3 immunophenotype, to assess their contribution to the production/expression of tested hematopoietic modulators. After culture, cells were washed twice in PBS with 1% FBS and subsequently stained for 30 minutes at 4 C with the following murine monoclonal antibodies (mabs): anti-cd3 tricolor (Caltag, Burlingame, CA) and unconjugated anti-cd178 (Fas ligand; BD Pharmingen, San Diego, CA). Fluorescein isothiocyanate (FITC) conjugated antimouse IgG secondary mab was purchased from BD Pharmingen. In all the experiments, to minimize background staining, Fc receptor blockade was achieved by incubation of cells with excess purified human immunoglobulin before staining. Stained cells were resuspended for 20 minutes at 4 Cin Cytofix/Cytoperm fixation/permeabilization solution (Caltag), according to the manufacturer s instructions. Once permeabilized, cells were washed twice and stained for intracellular cytokines with the following mabs: mouse anti-ifn phycoerythrin (PE; Caltag), rat anti TNF- PE (Caltag), and mouse anti MIP-1 PE (BD Pharmingen). Negative controls were PE-conjugated isotype-matched mabs of irrelevant specificity and a ligand-blocking control in which fluorochrome-conjugated antibodies were preincubated with appropriate concentrations of matched recombinant cytokines, according to the manufacturer s instructions. In some experiments freshly isolated BM MNCs from patients and controls were tested for intracellular expression of TNF- and IFN- omitting incubation with PMA, calcium ionophore, and brefeldin A. Immunophenotypic dissection of BM MNCs according to the expression of the CD 3 marker was carried out because CD3 T cells are known to elaborate the tested cytokines, in healthy individuals and in patients with other BM failure diseases, like AA Flow cytometric analysis was performed using a FACScan cytometer (Becton Dickinson, San Jose, CA). Gates were selected on the basis of the CD3 staining. Results were expressed as: (1) percentage of CD3 cells and CD3 cells and (2) mean ratio of relative fluorescence intensity (MRFI), calculated on the same cell fractions, as follows: mean fluorescence intensity (MFI) of cytokine staining/mfi of irrelevant isotype-matched mab staining. MRFI was used to roughly quantitate the amount of target antigen expressed. Clonogenic assay The in vitro assay for the growth of erythroid colony- and burst-forming units (CFU-Es and BFU-Es, respectively) was performed using methyl cellulose media (MethoCult; StemCell Technologies, Vancouver, BC, Canada). In brief, BM MNCs/dish were tested in triplicate (ie, a total of seeded BM MNCs) in semisolid cultures containing 0.9% methyl cellulose, 30% FBS, 1% bovine serum albumin, 10 4 M 2-mercaptoethanol, and 2 mm L-glutamine. To support erythroid colony growth, 50 ng/ml recombinant human stem cell factor (rhscf), 20 ng/ml recombinant human granulocyte-macrophage colony-stimulating factor (rhgm-csf), 20 ng/ml recombinant human interleukin 3 (rhil-3), 20 ng/ml rhil-6, 20 ng/ml recombinant human granulocyte colony-stimulating factor (rhg- CSF), and 3 U/mL erythropoietin were added to the culture system (StemCell). Cultures were incubated for 7 to 9 days (CFU-Es) and 14 to 16 days (BFU-Es) under humidified conditions in a 5% CO 2 atmosphere at 37 C, in the presence and in the absence of 1 or 10 g/ml of the recombinant soluble human tumor necrosis factor (TNF) receptor-fc fusion protein etanercept (Immunex, Seattle, WA). In this protein, the human p75 TNF receptor is fused with the Fc portion of human IgG1. Control cultures were carried out in the presence of the purified Fc fragment of human IgG1 (Alexis, Del Mar, CA). CFU-Es and BFU-Es from both patients and controls were counted at the indicated times. The term CFU-E was used to identify progenitors that give rise to isolated single or paired clusters of 5 to approximately 100 sufficiently hemoglobinized erythroblasts. These colony numbers peak after 7 to 9 days of incubation and were scored at this time. The term BFU-E was used to identify more immature progenitors that give rise to larger, burst-configured erythroid colonies made up of 3 to 8 closely arranged clusters of hemoglobinized erythroblasts per colony, whose number peaks after 14 to 16 days of incubation. Statistical analysis Because of the small sample size of the groups of FA patients and of healthy controls, the nonparametric Mann-Whitney U test was used to compare the 2 groups for BM intracytoplasmic cytokine expression. The same test was also used to compare cases and controls for the increase of the CFU-Es and BFU-Es (expressed as percentage of increase with respect to baseline) after the addition of anti TNF- fusion protein to the cultures. Furthermore, the Wilcoxon test was used to evaluate the effect of the addition of anti TNF- on the growth of CFU-Es and BFU-Es expressed as number of colonies after 7 and 14 days, both in cases and controls. For each subject the percentage of increment of CFU-E and BFU-E growth with respect to baseline conditions was calculated by subtracting the baseline number of colonies from the number obtained after the addition of TNF- fusion protein. This figure was subsequently divided by the baseline number of colonies and then multiplied by 100. The median value for patients and controls was calculated and reported. The Cohen K coefficient was used to evaluate the degree of concordance between intracytoplasmic TNF- expression and colony growth after addition of anti TNF-. 13,14 Statistical significance was defined as P.05. All the statistical tests were 2-sided. The Statistica Version 6.0 software was used to perform all the analyses (StatSoft, Statistica, Tulsa, OK). Results Eight FA patients entered the study; one of them developed an infection a week after the sampling and was then excluded from the analysis. This left 1 boy and 6 girls with FA eligible and evaluable for the study. Their median age was 8 years (mean, 9 years; range, 2-16 years) and their complementation group was A in 4 patients (UPN 1, 3, 5, 6), C in 1 (UPN 7) and unknown in the remaining 2
3 BLOOD, 15 SEPTEMBER 2003 VOLUME 102, NUMBER 6 TNF- AND IFN- IN BM OF FANCONI ANEMIA PATIENTS 2055 Table 1. Hematologic values of the FA patients at the time of the study UPN Age, y, sex Complementation group WBC count, 10 3 / L PMN count, 10 3 / L Hb level, g/dl Platelet count, 10 3 / L BM cellularity, % BM cytogenetics 1 6, F A ,XX 2 16, F ND ND 46,XX 3 5, F A ND 46,XX 4 12, F ND ND 46,XX11q- 5 2, F A ND 46,XX 6 8, F A ,XX 7 14, M C ND 46,XY ND indicates not determined. (UPN 2 and 4). Table 1 reports on their most relevant hematologic characteristics at the time of the study. During the same period, 8 voluntary BM donors (3 boys, 5 girls) agreed to be included in the study. At study entry their median age was 3 years (mean, 6.3 years; minimum, 1 year; maximum, 16 years). Their median hematologic values were within the normal range for their age (white blood cell [WBC] count, / L; polymorphonuclear [PMN] cell count, / L; hemoglobin [Hb] level, 13.2 g/dl; platelet count, / L). The 2 groups were comparable for age at study entry (P.29). TNF- and IFN- intracytoplasmic expression Table 2 reports on TNF- and IFN- expression in stimulated marrow MNCs from FA patients and controls. Data are presented both as percentage of positive cells and as MRFI in all analyzed subsets of marrow MNCs ( Flow cytometric detection of intracellular cytokines ). In the FA patients the TNF- content of all tested marrow MNC subsets, both if expressed as percentage of positive cells and as MRFI, were increased as compared to the control group in whom almost no cytokine was detectable. The difference was statistically significant in all the combinations (P.006 for TNF- /CD3 cells both as percentage of positive cells and as MRFI; P.016 for TNF- /CD3 cells as percentage of positive cells; P.045 for TNF- /CD3 cells as MRFI; Table 2). The expression of IFN- in the patient group was higher than that found in the controls in all tested marrow cellular subsets. Statistical significance was achieved in 3 of the 4 assessed combinations: IFN- /CD3 cells/percent of positive cells (P.013); IFN- /CD3 cells/mrfi (P.021); IFN- /CD3 cells/percent of positive cells (P.014; Table 2). Representative scattergrams of TNF- and IFN- expression in CD3 BM MNCs obtained from 2 patients and 2 controls are shown in Figure 1. Detailed results of percentages of positive cells and MRFI values of individual patients are provided in Figure 2. Intracellular cytokine expression in uncultured BM MNCs from 5 patients (UPN 1, 4-7) and 5 healthy controls was also investigated. The results of these experiments were consistently negative. MIP-1 intracytoplasmic and Fas ligand surface expression Neither the patients nor the controls expressed intracytoplasmic MIP-1 or surface Fas ligand in stimulated CD3 and CD3 marrow cells. This occurred both when cytokine expression was evaluated as percentage of positive cells and as MRFI. Colony studies CFU-Es. In the patients, the mean number of CFU-Es (colonies/ seeded BM MNCs) grown in the absence of anti TNF- was 12.0 (median, 9.0; minimum, 0; maximum, 37; SE, 4.8), whereas in the normal control group it was (median, 353.5; minimum, 102; maximum, 522; SE, 47.3). In both groups no differences were seen when colonies were grown in the presence of purified Fc fragment of human IgG1 (data not shown). When low-dose (LD 1 g/ml) and high-dose (HD 10 g/ ml) anti TNF- fusion protein was added to the culture samples from the FA patients, the mean number of CFU-Es significantly increased to 34.7 (median, 19.0; minimum, 0; maximum, 100; SE, 14.1; P.043) (Figure 3A) and 38.1 (median, 15.0; minimum, 0; maximum, 96; SE, 15.0; P.028), respectively. On the other hand, in the control group, the addition of anti TNF- fusion protein did not increase the mean number of colonies as compared Table 2. TNF- and IFN- intracytoplasmic expression in marrow MNCs in 7 FA patients and 8 controls FA patients Controls Mean (SD) Median Min-Max Mean (SD) Median Min-Max P* TNF- TNF- /CD3 cells, % 9.57 (8.68) (0.00) TNF- /CD3 cells, MRFI 3.71 (3.09) (0.00) TNF- /CD3,% 6.29 (6.57) (0.53) TNF- /CD3, MRFI 1.86 (0.90) (0.18) IFN- IFN- /CD3 cells, % 8.57 (7.91) (0.71) IFN- /CD3 cells, MRFI 2.29 (1.25) (0.35) IFN- /CD3,% 5.57 (7.07) (0.74) IFN- /CD3, MRFI 2.00 (2.65) (0.00) Min indicates minimum; max, maximum. *Mann-Whitney U test; only statistically significant P values are shown. CD3 phenotypically defined cells were chosen because they contain the cell fraction that is known to produce these cytokines in healthy subjects and in marrow failure disease such as AA
4 2056 DUFOUR et al BLOOD, 15 SEPTEMBER 2003 VOLUME 102, NUMBER 6 Figure 1. Examples of intracytoplasmic expression of TNF- and IFN- in CD3 BM MNCs from 2 representative FA patients (UPN 1 and 7) and 2 representative healthy control subjects. As shown in Table 2 and Figure 2, TNF- and IFN- were also expressed in CD3 cells. In the top right corner of each scattergram the percentage of positive BM cells is represented. UPN 1: (A) CD3 /TNF- cells, 7%; (B) CD3 /IFN- cells, 9%. UPN 7: (C) CD3 /TNF- cells, 17%; (D) CD3 /IFN- cells, 20%. Healthy control 1: (E) CD3 /TNF- cells, less than 1%; (F) CD3 /IFN- cells, 2%. Healthy control 2: (G) CD3 /TNF- cells, less than 1%; (H) CD3 /IFN- cells, less than 1%. to baseline values (362.2) both at LD (362.0; median, 349.0; minimum, 96; maximum, 525; SE, 48.0; Figure 3A) and at HD (340.0; median, 346.0; minimum, 81; maximum, 528; SE, 62.7; P.944 and P.075, respectively). The mean percentage of increment with respect to baseline observed in the patients after the addition of both LD (206%; median, 89.2%) and HD (257.7%; median, 66.7%) anti TNF- fusion protein was significantly greater than the no increment ( 0.60%; median, 0.51% with LD; 4.41%; median, 1.85% with HD) seen in the healthy controls (P.011 and P.0043 for LD and HD anti TNF-, respectively). Noteworthy, the addition of LD and HD anti TNF- also resulted in an increase of the size of the erythroid colonies grown at day 7 (Figure 4A), whereas this effect was not seen in healthy controls. BFU-Es. In the patients, the mean number of BFU-Es (colonies/ seeded BM MNCs) grown in the absence of anti TNF- was 7.3 (median, 6.0; minimum, 0; maximum, 24; SE, 3.1), whereas in the healthy controls the mean number of colonies was (median, 336.5; minimum, 66; maximum, 691; SE, 60.9). In both groups no differences were seen when colonies were grown in the presence of purified Fc fragment of human IgG1. The addition of anti TNF- fusion protein to the culture of the patients resulted in a significant increase of the mean number of BFU-Es to 19.3 (median, 12.0; minimum, 0; maximum, 45; SE, 6.9) with LD (Figure 3B) and to 16.1 with HD (median, 12.0; minimum, 0; maximum, 49; SE, 6.7) anti TNF- fusion protein (P.043). On the other hand, in the healthy controls the addition of anti TNF- fusion protein did not significantly increase the mean number of the colonies as compared to baseline values (343.1) both at LD (mean, 350.6; median, 332.5; minimum, 142; maximum, 695; SE, 55.7; Figure 3B) and at HD (mean, 369.0; median, 326.5; minimum, 199; maximum, 689; SE, 68.6). In the patients, the mean percentage of increment observed after the addition of both LD (175.8%; median, 71.4%) and HD (92.4%; median, 100%) anti TNF- was significantly greater for both LD (P.028) and HD (P.045) than that seen in the healthy controls (13.7%; median, 1.17% for LD; 32.2%; median, 1.06% for HD). Moreover, anti TNF- was also able to induce a remarkable increase in the size of BFU-Es (Figure 4B), an effect not seen in healthy controls. In the patient group the growth of granulocyte-macrophage colony-forming units (CFU-GMs) in baseline conditions was notably reduced in comparison to that of erythroid-committed progenitors. This impeded the use of CFU-GM data for appropriate comparisons with anti TNF- conditions and with healthy controls. When looking at patients individually, the observed degree of agreement between the intracytoplasmic TNF- expression and the colony growth with anti TNF- was 71.4% (5 of 7 concordant and 2 of 7 nonconcordant), corresponding to a fair degree of concordance (k 0.30). In particular, in 4 patients (UPN 1, 2, 3, 7) the increase of intracytoplasmic TNF- was associated with an enhancement in the number of erythroid colonies grown in the presence of either LD or HD anti TNF-. In another patient (UPN 4) with undetectable intracytoplasmic TNF- in BM MNCs, the addition of anti TNF- had no effect on erythroid colony growth. Finally there were 2 nonconcordant patients. In one patient (UPN 6) the increase of intracellular TNF- was not accompanied by a rise in the colony growth with anti TNF-. This patient had advanced marrow failure and severely reduced hematopoiesis that led him to marrow transplantation shortly after the test. In the remaining nonconcordant patient (UPN 5), no intracytoplasmic TNF- was detected, but a rise of colony growth with anti TNF- was observed. Discussion Our study provides the first evidence that in vitro-stimulated BM MNCs from FA patients overexpress TNF- and IFN- and that in marrow cultures of FA patients there is a TNF- activity that inhibits erythropoiesis in vitro. We have also found that other negative modulators of hematopoiesis, such as MIP-1 and surface Fas ligand, are not overexpressed in stimulated BM MNC fractions from FA patients. TNF- and IFN- were not detected in uncultured and unstimulated BM MNCs. This finding may indicate that an additional stress/stimulus is required to detect increased intracellular cytokines. Another possible explanation might be that uncultured BM MNCs, differently from stimulated cells, were not treated with
5 BLOOD, 15 SEPTEMBER 2003 VOLUME 102, NUMBER 6 TNF- AND IFN- IN BM OF FANCONI ANEMIA PATIENTS 2057 Figure 2. TNF- and IFN- intracytoplasmic expression in BM MNCs in individual FA patients. CD3 phenotypically defined MNCs were chosen because they contain T cells that in healthy individuals and in other marrow failure diseases such as AA are known to elaborate the tested cytokines. TNF- and IFN- expression are provided for each patient, both as percentage of positive cells and as MRFI, in each analyzed marrow cellular subset ( CD3 cells, o CD3 cells). (A) TNF- intracytoplasmic expression shown as percentage of cells in the cellular subsets (CD3, CD3 cells) expressing this cytokine. (B) TNF- intracytoplasmic expression shown as MRFI of cells in the cellular subsets (CD3, CD3 cells) expressing this cytokine. (C) IFN- intracytoplasmic expression shown as percentage of cells in the cellular subsets (CD3, CD3 cells) expressing this cytokine. (D) IFN- intracytoplasmic expression shown as MRFI of cells in the cellular subsets (CD3, CD3 cells) expressing this cytokine. Figure 3. Effect of anti TNF- on the growth of erythroid committed progenitors in FA patients and controls. (A) Each column represents mean values; error bars indicate the SE of the estimate. We also reported in brackets median, minimum, and maximum values. In the patients, CFU-Es (mean, 34.7; median, 19.0; minimum, 0; maximum, 100) grown after the addition of LD anti TNF- (1 g/ml) significantly outnumbered (P.043) that grown in the absence of anti TNF- (mean, 12.0; median, 9.0; minimum, 0; maximum, 37; left side). A similar significant difference was obtained with HD anti-tnf- (10 g/ml; P.028; diagram not shown). The addition of anti TNF- had no effect on the growth of CFU-Es in healthy controls (mean number of colonies without LD anti TNF-, 362.2; median, 353.5; minimum, 102; maximum, 522; mean number of colonies with LD anti TNF-, 362.0; median, 349.0; minimum, 96; maximum, 525; right side). (B) Each column represents mean values; error bars indicate the SE of the estimate. We also reported in brackets median, minimum, and maximum values. In the patients, BFU-Es grown after the addition of LD anti TNF- (mean, 19.3; median, 12.0; minimum, 0; maximum, 45) significantly outnumbered (P.043) that grown in the absence of anti TNF- (mean, 7.3; median, 6.0; minimum, 0; maximum, 24; left side). The same held true, with the identical significance (P.043), also for HD anti TNF- (diagram not shown). The addition of anti TNF- had no effect on the growth of BFU-Es in healthy controls (mean number of colonies without LD anti TNF-, 343.1; median, 336.5; minimum, 66; maximum, 691; mean number of colonies with LD anti TNF-, 350.6; median, 332.5; minimum, 142; maximum, 695; right side). indicates no anti TNF- ;, with anti TNF- (1 g/ml). brefeldin A, whose function is that of blocking the release of cytokines outside the cells. Thus it cannot be excluded that, in the absence of brefeldin A, newly synthesized TNF- and IFN- were rapidly secreted in the extracellular milieu and were not detectable intracellularly. Because all analyzed patients had not had transfusions and were infection free at least 4 weeks before and after the study, the increased expression of IFN- and TNF- after PMA stimulation in the BM cannot be linked to infections and transfusion and should therefore be considered as a disease-related characteristic. A previous study demonstrated that the IFN- mrna was not increased in unstimulated BM MNCs from FA patients. 12 It is possible that the short-term stimulation that cells underwent in our experiments may account for the IFN- overexpression we detected in our study. It has to be noted, however, that normal BM MNCs stimulated under the same conditions did not accumulate IFN- in their cytoplasm. The marrow overexpression of TNF- we demonstrated following stimulation agrees with previous data showing that this cytokine is increased in the serum of FA patients 8,9 and overproduced by lymphoblastoid cells derived from patients themselves. 9 It is unknown whether this increased TNF- BM content reflects the condition of increased apoptosis of FA cells or is a consequence of the genetic defect. Whatever the mechanism responsible for TNF- and IFN- excess in stimulated FA marrow cells, it is of note that these cytokines are overexpressed in marrow lymphocytes from acquired AA, 10 a disease that shares with FA the occurrence of BM failure. In acquired AA, autoreactive T cells are activated by an antigenic stimulus and release, among other cytokines, TNF- and IFN- that act as the late effectors of the damage on the stem cell compartment. 11 No evidence so far indicates that in FA an immune activation stimulates marrow MNCs to hyperproduce IFN- and TNF-. Nevertheless, their presence in the marrow seems consistent with a possible role for these cytokines in the pathogenesis of marrow failure also in FA. To further investigate this issue, we grew marrow-committed progenitor cells in semisolid assay in the presence and in the absence of etanercept, an anti TNF- fusion protein used in the
6 2058 DUFOUR et al BLOOD, 15 SEPTEMBER 2003 VOLUME 102, NUMBER 6 Figure 4. Effect of anti TNF- on erythroid-committed progenitor growth in FA patients. (A) CFU-Es grown in the absence of anti TNF- are shown (i,ii; medium alone). The size of CFU-Es cultured in the absence of anti TNF- but in the presence of purified Fc fragment of human IgG1 were not different (not shown). The addition of LD (1 g/ml) anti TNF- (iii,iv) increased the size of CFU-Es grown from marrow MNCs of FA patients. A similar effect was seen with HD (10 g/ml) anti TNF- (not shown). (B) BFU-Es grown in the absence of anti TNF- are shown (i,ii; medium alone). The size of BFU-Es cultured in the absence of anti TNF- but in the presence of purified Fc fragment of human IgG1 were not different (not shown). Panel Bii shows a minor nonhemoglobinized component at the periphery. The addition of LD anti TNF- (iii,iv) increased the size of BFU-Es grown from BM MNCs of FA patients. A similar effect was seen with HD anti TNF- (not shown). treatment of autoimmune diseases. 15 The shortage of cells allowed us to grow only erythroid-committed progenitors and only with an anti TNF- but not with an anti-ifn- antagonist. In the patients, at variance from controls, we found that etanercept provoked a significant rise of erythropoiesis in vitro, as shown both by the increase of the number and of the size of CFU-Es and BFU-Es with respect to values detected in the absence of anti TNF-. FA subjects had many fewer baseline colonies than healthy individuals, but the increase after TNF- neutralization indicated that in FA marrow cells there was a TNF- effect, lacking in healthy controls, that significantly inhibited erythropoiesis in vitro. We did not measure TNF- production from FA marrow cultures; therefore whether this effect reflects an overproduction or an increased sensitivity to TNF- of FA versus normal marrow progenitor cells still remains an open question. The fair concordance between TNF- intracellular expression and recovery of erythroid colony growth following etanercept may suggest that the TNF- activity is, to some extent, attributable to the TNF- production by marrow MNCs. In the single patient (UPN 5) in whom the rise of BFU-Es and CFU-Es with anti TNF- was not associated with an increase of intracytoplasmic TNF- in the BM cells, we can hypothesize that etanercept blocked TNF-, which binds to the same receptors as TNF-. 16 Another plausible explanation for UPN 5 s responsiveness to anti TNF- resides in the differences between the intracytoplasmic assay (5 hours of treatment with PMA and heterogeneous cell population read-out) versus progenitor assay (7-14 days of stimulatory cytokines and progenitor read-out). All together, the TNF- results indicate that this cytokine has a relevant role in the pathogenesis of erythropoietic failure of FA. We did not test the growth of myeloid- and megakaryocytic-committed progenitors, but it is possible that TNF- has a similar suppressive effect on these marrow lineages as well as on the stem cell compartment. We could not test whether there was a similar IFN- mediated myelosuppressive effect, which seems logical to hypothesize given that IFN- was also overexpressed in stimulated marrow MNCs. References This marrow TNF- activity may have some clinical implications. Indeed the demonstration of the TNF- myelosuppressive effect in vitro may identify those FA subjects with marrow failure who, through treatment with anti TNF-, may have a positive effect on erythroid and possibly other hematopoietic lineages. However, the potential value of anti TNF- needs to be confirmed in other studies before entering the established care of FA patients. As for the other negative modulators of the hematopoiesis we have assessed, MIP-1 and surface Fas ligand were not detectable in patients or healthy controls. Very low concentrations of MIP-1 exerted a myelosuppressive effect in FANCC mice. 6 Although this cytokine was not expressed in stimulated BM MNCs from patients, a role for MIP-1 in the origin of BM failure in FA subjects cannot be excluded, because it is still possible that FA cells are hypersensitive to amounts of MIP-1 below the threshold of detection of our experimental setting. The lack of expression of surface Fas ligand on marrow MNCs does not exclude the existence of a Fas-mediated apoptosis in FA cells 4,7 because CD 34 cells from FA patients have been shown to express constitutively Fas ligand. 4 In our study, failure to detect surface Fas ligand plus MNCs is most likely due to the paucity of CD34 cells in patients with FA. In summary, our study shows that in stimulated BM MNCs of patients with FA there is an overexpression of the myelosuppressive cytokines TNF- and IFN- and that marrow cultures from FA subjects produce a TNF- activity that suppresses erythropoiesis in vitro. These data provide further insight into the pathogenesis of marrow failure in FA and may represent an experimental support for future clinical trials investigating the possibility of treating selected FA patients with anti TNF-. Acknowledgments Ms Sara Calmanti and Ms Francesca Garaventa are acknowledged for secretarial assistance in the preparation of the tables and figures of this manuscript. 1. Siddique MA, Nakanishi K, Taniguchi T, Grompe M, D Andrea AD. Function of the Fanconi anemia complementation group F and D1 cells. Exp Hematol. 2001;29: Garcia-Higuera I, Taniguchi T, Ganesan S, et al. Interaction of the Fanconi anemia proteins and BRCA1 in a common pathway. Mol Cell. 2001;7: Howlett NG, Taniguchi T, Olson S, et al. Biallelic inactivation of BRCA2 in Fanconi anemia. Science. 2002;297: Rathbun RK, Faulkner GR, Ostroski MH, et al. Inactivation of the Fanconi anemia group C gene augments interferon- - induced apoptotic responses in hematopoietic cells. Blood. 1997;90: Whitney MA, Royle G, Low MJ, et al. Germ cell defects and hematopoietic hypersensitivity to
7 BLOOD, 15 SEPTEMBER 2003 VOLUME 102, NUMBER 6 TNF- AND IFN- IN BM OF FANCONI ANEMIA PATIENTS 2059 INF- in mice with a targeted disruption of the Fanconi anemia C gene. Blood. 1996;88: Haneline LS, Broxmeyer HE, Cooper S, et al. Multiple inhibitory cytokines induce deregulated progenitor growth and apoptosis in hematopoietic cells from Fac / mice. Blood. 1998;91: Otsuki T, Nagakura S, Wang J, et al. Tumor necrosis factor and CD-95 ligation suppress erythropoiesis in Fanconi anemia C gene knockout mice. J Cell Physiol. 1999;179: Shulz JC, Shahidi NT. Tumor necrosis factor-alpha overproduction in Fanconi s anemia. Am J Hematol. 1993;42: Rosselli F, Sancean J, Gluckman E, et al. Abnormal lymphokine production: a novel feature of the genetic disease Fanconi anemia. In vitro and in vivo spontaneous overproduction of tumor necrosis factor. Blood. 1994;83: Dufour C, Corcione A, Svahn J, et al. Interferon and tumor necrosis factor are over-expressed in bone marrow T lymphocytes from pediatric patients with aplastic anaemia. Br J Hematol. 2001; 115: Young NS. Hematopoietic cell destruction by immune mechanisms in acquired aplastic anemia. Semin Hematol. 2000;37: Nisticò A, Young NS. IFN- gene expression in the bone marrow of patients with aplastic anemia. Ann Intern Med. 1994;120: Cohen J. A coefficient of agreement for nominal scales. Educ Psychol Meas. 1960;20: Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977;33: Moreland LW, Baumgartner SW, Schiff MH, et al. Treatment of rheumatoid arthritis with a recombinant human tumor necrosis factor receptor (p75)-fc fusion protein. N Engl J Med. 1997;337: Paul NL, Ruddle NH. Lymphotoxin. Annual Rev Immunol. 1987;6:
Effect of Interleukin 10 on the Hematopoietic Progenitor Cells from Patients with Aplastic Anemia
 Effect of Interleukin 10 on the Hematopoietic Progenitor Cells from Patients with Aplastic Anemia YOSHINOBU ASANO, SHOICHIRO SHIBATA, SHINJI KOBAYASHI, SEIICHI OKAMURA, YOSHIYUKI NIHO First Department
Effect of Interleukin 10 on the Hematopoietic Progenitor Cells from Patients with Aplastic Anemia YOSHINOBU ASANO, SHOICHIRO SHIBATA, SHINJI KOBAYASHI, SEIICHI OKAMURA, YOSHIYUKI NIHO First Department
McAb and rhil-2 activated bone marrow on the killing and purging of leukemia cells
 Effects of McAb and rhil-2 activated bone marrow on the killing and purging of leukemia cells X.C. Wei, D.D. Yang, X.R. Han, Y.A. Zhao, Y.C. Li, L.J. Zhang and J.J. Wang Institute of hematological research,
Effects of McAb and rhil-2 activated bone marrow on the killing and purging of leukemia cells X.C. Wei, D.D. Yang, X.R. Han, Y.A. Zhao, Y.C. Li, L.J. Zhang and J.J. Wang Institute of hematological research,
Detailed step-by-step operating procedures for NK cell and CTL degranulation assays
 Supplemental methods Detailed step-by-step operating procedures for NK cell and CTL degranulation assays Materials PBMC isolated from patients, relatives and healthy donors as control K562 cells (ATCC,
Supplemental methods Detailed step-by-step operating procedures for NK cell and CTL degranulation assays Materials PBMC isolated from patients, relatives and healthy donors as control K562 cells (ATCC,
THE INFLUENCE OF SODIUM FLUORIDE ON THE CLONOGENECITY OF HUMAN HEMATOPOIETIC PROGENITOR CELLS: PRELIMINARY REPORT
 168 Fluoride Vol. 33 No. 4 168-173 2 Research Report THE INFLUENCE OF SODIUM FLUORIDE ON THE CLONOGENECITY OF HUMAN HEMATOPOIETIC PROGENITOR CELLS: PRELIMINARY REPORT Boguslaw Machaliński, a Maria Zejmo,
168 Fluoride Vol. 33 No. 4 168-173 2 Research Report THE INFLUENCE OF SODIUM FLUORIDE ON THE CLONOGENECITY OF HUMAN HEMATOPOIETIC PROGENITOR CELLS: PRELIMINARY REPORT Boguslaw Machaliński, a Maria Zejmo,
Technical Resources. BD Immunocytometry Systems. FastImmune Intracellular Cytokine Staining Procedures
 FastImmune Intracellular Cytokine Staining Procedures BD has developed protocols for the detection of intracellular cytokines in activated lymphocytes and in activated monocytes. The procedures have been
FastImmune Intracellular Cytokine Staining Procedures BD has developed protocols for the detection of intracellular cytokines in activated lymphocytes and in activated monocytes. The procedures have been
Feasibility of hyperthermia as a purging modality in autologous bone marrow transplantation Wierenga, Pieter Klaas
 University of Groningen Feasibility of hyperthermia as a purging modality in autologous bone marrow transplantation Wierenga, Pieter Klaas IMPORTANT NOTE: You are advised to consult the publisher's version
University of Groningen Feasibility of hyperthermia as a purging modality in autologous bone marrow transplantation Wierenga, Pieter Klaas IMPORTANT NOTE: You are advised to consult the publisher's version
BCR-ABL - LSK BCR-ABL + LKS - (%)
 Marker Clone BCR-ABL + LSK (%) BCR-ABL + LKS - (%) BCR-ABL - LSK (%) P value vs. BCR-ABL + LKS - P value vs. BCR-ABL - LSK CD2 RM2-5 12.9 ± 3.6 36.7 ± 6.5 19.3 ± 2.4 0.01 0.10 CD5 53-7.3 13.9 ± 3.2 20.8
Marker Clone BCR-ABL + LSK (%) BCR-ABL + LKS - (%) BCR-ABL - LSK (%) P value vs. BCR-ABL + LKS - P value vs. BCR-ABL - LSK CD2 RM2-5 12.9 ± 3.6 36.7 ± 6.5 19.3 ± 2.4 0.01 0.10 CD5 53-7.3 13.9 ± 3.2 20.8
Organic dust-induced interleukin-12 production activates T- and natural killer cells
 Eur Respir J 22; 2: 686 69 DOI:.1183/931936.2.222 Printed in UK all rights reserved Copyright #ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Organic dust-induced interleukin-12 production
Eur Respir J 22; 2: 686 69 DOI:.1183/931936.2.222 Printed in UK all rights reserved Copyright #ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Organic dust-induced interleukin-12 production
Optimizing Intracellular Flow Cytometry
 Optimizing Intracellular Flow Cytometry Detection of Cytokines, Transcription Factors, and Phosphoprotein by Flow Cytometry Presented by Erika O Donnell, PhD, BD Biosciences 23-14876-00 Outline Basic principles
Optimizing Intracellular Flow Cytometry Detection of Cytokines, Transcription Factors, and Phosphoprotein by Flow Cytometry Presented by Erika O Donnell, PhD, BD Biosciences 23-14876-00 Outline Basic principles
Supplemental Information. T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism
 Immunity, Volume 33 Supplemental Information T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism Franziska Petermann, Veit Rothhammer, Malte
Immunity, Volume 33 Supplemental Information T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism Franziska Petermann, Veit Rothhammer, Malte
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
Optimizing Intracellular Flow Cytometry:
 Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
Hematology 101. Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD
 Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Supplementary Figures
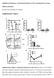 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Supplementary Materials for
 www.sciencesignaling.org/cgi/content/full/8/381/ra59/dc1 Supplementary Materials for Analysis of single-cell cytokine secretion reveals a role for paracrine signaling in coordinating macrophage responses
www.sciencesignaling.org/cgi/content/full/8/381/ra59/dc1 Supplementary Materials for Analysis of single-cell cytokine secretion reveals a role for paracrine signaling in coordinating macrophage responses
Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD-
 Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
The Adaptive Immune Responses
 The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
Immunofluorescent Staining of Intracellular Cytokines for Flow Cytometric Analysis
 Immunofluorescent Staining of Intracellular Cytokines for Flow Cytometric Analysis I. Introduction Improved methods have continually been sought to analyze single-cell cytokine production by human and
Immunofluorescent Staining of Intracellular Cytokines for Flow Cytometric Analysis I. Introduction Improved methods have continually been sought to analyze single-cell cytokine production by human and
Predictive role of cutaneous lymphocyteassociated antigen (CLA) in TNF-α inhibitor treatment of psoriasis
 Predictive role of cutaneous lymphocyteassociated antigen (CLA) in TNF-α inhibitor treatment of psoriasis Thesis of doctoral (PhD) dissertation Dr. Jókai Hajnalka, MD Semmelweis University School of Doctoral
Predictive role of cutaneous lymphocyteassociated antigen (CLA) in TNF-α inhibitor treatment of psoriasis Thesis of doctoral (PhD) dissertation Dr. Jókai Hajnalka, MD Semmelweis University School of Doctoral
From the Diagnostic Immunology Laboratories
 Immunology Laboratories ISSUE 9 SPRING 2012 PAGE 1 Spring Meetings Please stop by and say hello in May at this year s American Society of Pediatric Hematology/Oncology (ASPHO) Annual Meeting in New Orleans
Immunology Laboratories ISSUE 9 SPRING 2012 PAGE 1 Spring Meetings Please stop by and say hello in May at this year s American Society of Pediatric Hematology/Oncology (ASPHO) Annual Meeting in New Orleans
CD34+ Cells: A Comparison of Stem and Progenitor Cells in Cord Blood, Peripheral Blood, and the Bone Marrow
 White Paper September 2016 CD34+ Cells: A Comparison of Stem and Progenitor Cells in Cord Blood, Peripheral Blood, and the Bone Marrow Lily C. Trajman, PhD Introduction: Hematopoietic Stem Cells (HSCs)
White Paper September 2016 CD34+ Cells: A Comparison of Stem and Progenitor Cells in Cord Blood, Peripheral Blood, and the Bone Marrow Lily C. Trajman, PhD Introduction: Hematopoietic Stem Cells (HSCs)
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Fas/FasL in the immune pathogenesis of severe aplastic anemia
 Fas/FasL in the immune pathogenesis of severe aplastic anemia C.Y. Liu, R. Fu, H.Q. Wang, L.J. Li, H. Liu, J. Guan, T. Wang, W.W. Qi, E.B. Ruan, W. Qu, G.J. Wang, H. Liu, Y.H. Wu, J. Song, L.M. Xing and
Fas/FasL in the immune pathogenesis of severe aplastic anemia C.Y. Liu, R. Fu, H.Q. Wang, L.J. Li, H. Liu, J. Guan, T. Wang, W.W. Qi, E.B. Ruan, W. Qu, G.J. Wang, H. Liu, Y.H. Wu, J. Song, L.M. Xing and
Pearson r = P (one-tailed) = n = 9
 8F4-Specific Lysis, % 1 UPN1 UPN3 8 UPN7 6 Pearson r =.69 UPN2 UPN5 P (one-tailed) =.192 4 UPN8 n = 9 2 UPN9 UPN4 UPN6 5 1 15 2 25 8 8F4, % Max MFI Supplementary Figure S1. AML samples UPN1-UPN9 show variable
8F4-Specific Lysis, % 1 UPN1 UPN3 8 UPN7 6 Pearson r =.69 UPN2 UPN5 P (one-tailed) =.192 4 UPN8 n = 9 2 UPN9 UPN4 UPN6 5 1 15 2 25 8 8F4, % Max MFI Supplementary Figure S1. AML samples UPN1-UPN9 show variable
Bead Based Assays for Cytokine Detection
 Bead Based Assays for Cytokine Detection September 27, 2014 6 th EFIS-EJI South East European Immunology School SEEIS 2014 Timisoara, Romania The Cells of the Immune System The Immune Reaction (Th2) (Th1)
Bead Based Assays for Cytokine Detection September 27, 2014 6 th EFIS-EJI South East European Immunology School SEEIS 2014 Timisoara, Romania The Cells of the Immune System The Immune Reaction (Th2) (Th1)
Apoptosis of lymphocytes in SLE: the level, correlation with dosage prednisolone and lymphocyte phenotypes
 Apoptosis of lymphocytes in SLE: the level, correlation with dosage prednisolone and lymphocyte phenotypes ABDELMAROUF MOHIELDEIN 1, NATALIA BELUSHKINA 2, ULIANA PETROVA 3. 1,2 Department of Biochemistry,
Apoptosis of lymphocytes in SLE: the level, correlation with dosage prednisolone and lymphocyte phenotypes ABDELMAROUF MOHIELDEIN 1, NATALIA BELUSHKINA 2, ULIANA PETROVA 3. 1,2 Department of Biochemistry,
The Immune System. A macrophage. ! Functions of the Immune System. ! Types of Immune Responses. ! Organization of the Immune System
 The Immune System! Functions of the Immune System! Types of Immune Responses! Organization of the Immune System! Innate Defense Mechanisms! Acquired Defense Mechanisms! Applied Immunology A macrophage
The Immune System! Functions of the Immune System! Types of Immune Responses! Organization of the Immune System! Innate Defense Mechanisms! Acquired Defense Mechanisms! Applied Immunology A macrophage
Fluorochrome Panel 1 Panel 2 Panel 3 Panel 4 Panel 5 CTLA-4 CTLA-4 CD15 CD3 FITC. Bio) PD-1 (MIH4, BD) ICOS (C398.4A, Biolegend) PD-L1 (MIH1, BD)
 Additional file : Table S. Antibodies used for panel stain to identify peripheral immune cell subsets. Panel : PD- signaling; Panel : CD + T cells, CD + T cells, B cells; Panel : Tregs; Panel :, -T, cdc,
Additional file : Table S. Antibodies used for panel stain to identify peripheral immune cell subsets. Panel : PD- signaling; Panel : CD + T cells, CD + T cells, B cells; Panel : Tregs; Panel :, -T, cdc,
Data Sheet TIGIT / NFAT Reporter - Jurkat Cell Line Catalog #60538
 Data Sheet TIGIT / NFAT Reporter - Jurkat Cell Line Catalog #60538 Background: TIGIT is a co-inhibitory receptor that is highly expressed in Natural Killer (NK) cells, activated CD4+, CD8+ and regulatory
Data Sheet TIGIT / NFAT Reporter - Jurkat Cell Line Catalog #60538 Background: TIGIT is a co-inhibitory receptor that is highly expressed in Natural Killer (NK) cells, activated CD4+, CD8+ and regulatory
M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology
 Code : AS-2246 M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology A. Select one correct option for each of the following questions:- 2X10=10 1. (b)
Code : AS-2246 M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology A. Select one correct option for each of the following questions:- 2X10=10 1. (b)
T H 1, T H 2 and T H 17 polarization of naïve CD4 + mouse T cells
 A complete workflow for cell preparation, isolation, polarization and analysis T H 1, T H 2 and T H 17 polarization of naïve CD4 + mouse T cells Introduction Workflow CD4 + T helper (T H) cells play a
A complete workflow for cell preparation, isolation, polarization and analysis T H 1, T H 2 and T H 17 polarization of naïve CD4 + mouse T cells Introduction Workflow CD4 + T helper (T H) cells play a
Anaemia & Cancer. John de Vos Consultant Haematologist RSCH
 Anaemia & Cancer John de Vos Consultant Haematologist RSCH overview Definitions & setting the scene Causes Consequences Biology Treatment Personal approach Patient Clinical team Anaemia - Definition :
Anaemia & Cancer John de Vos Consultant Haematologist RSCH overview Definitions & setting the scene Causes Consequences Biology Treatment Personal approach Patient Clinical team Anaemia - Definition :
Difference in Cytokine Production and Cell Activation between Adenoidal Lymphocytes and Peripheral Blood Lymphocytes of Children with Otitis Media
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Sept. 2005, p. 1130 1134 Vol. 12, No. 9 1071-412X/05/$08.00 0 doi:10.1128/cdli.12.9.1130 1134.2005 Copyright 2005, American Society for Microbiology. All
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Sept. 2005, p. 1130 1134 Vol. 12, No. 9 1071-412X/05/$08.00 0 doi:10.1128/cdli.12.9.1130 1134.2005 Copyright 2005, American Society for Microbiology. All
Nature Medicine: doi: /nm.2109
 HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Rapid antigen-specific T cell enrichment (Rapid ARTE)
 Direct ex vivo characterization of human antigen-specific CD154+CD4+ T cell Rapid antigen-specific T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central role
Direct ex vivo characterization of human antigen-specific CD154+CD4+ T cell Rapid antigen-specific T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central role
CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads (Miltenyi Biotec) for depletion of CD25 +
 Supplements Supplemental Materials and Methods Depletion of CD25 + T-cells from PBMC. Fresh or HD precultured PBMC were stained with the conjugate CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads
Supplements Supplemental Materials and Methods Depletion of CD25 + T-cells from PBMC. Fresh or HD precultured PBMC were stained with the conjugate CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads
Development of Natural Killer Cells from Lymphohematopoietic Progenitors of Murine Fetal Liver
 Development of Natural Killer Cells from Lymphohematopoietic Progenitors of Murine Fetal Liver YUKHI AIBA, MAKIO OGAWA Ralph H. Johnson Department of Veterans Affairs Medical Center, Department of Medicine,
Development of Natural Killer Cells from Lymphohematopoietic Progenitors of Murine Fetal Liver YUKHI AIBA, MAKIO OGAWA Ralph H. Johnson Department of Veterans Affairs Medical Center, Department of Medicine,
CHAPTER 3 LABORATORY PROCEDURES
 CHAPTER 3 LABORATORY PROCEDURES CHAPTER 3 LABORATORY PROCEDURES 3.1 HLA TYPING Molecular HLA typing will be performed for all donor cord blood units and patients in the three reference laboratories identified
CHAPTER 3 LABORATORY PROCEDURES CHAPTER 3 LABORATORY PROCEDURES 3.1 HLA TYPING Molecular HLA typing will be performed for all donor cord blood units and patients in the three reference laboratories identified
BD Cytofix/Cytoperm Plus Fixation/Permeabilization Kit (with BD GolgiStop protein transport inhibitor containing monensin) (Cat. No.
 Kit Manual BD Cytofix/Cytoperm Fixation/Permeabilization Kit (Cat. No. 554714) BD Cytofix/Cytoperm Plus Fixation/Permeabilization Kit (with BD GolgiStop protein transport inhibitor containing monensin)
Kit Manual BD Cytofix/Cytoperm Fixation/Permeabilization Kit (Cat. No. 554714) BD Cytofix/Cytoperm Plus Fixation/Permeabilization Kit (with BD GolgiStop protein transport inhibitor containing monensin)
Optimizing Intracellular Flow Cytometry:
 Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors Presented by Jurg Rohrer, PhD, BD Biosciences 23-10780-00 Outline Introduction Cytokines Transcription
Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors Presented by Jurg Rohrer, PhD, BD Biosciences 23-10780-00 Outline Introduction Cytokines Transcription
were isolated from the freshly drawn blood of healthy donors and ACS patients using the
 Supplemental Figure 1. Quality control of CD4 + T-cell purification. CD4 + T cells were isolated from the freshly drawn blood of healthy donors and ACS patients using the RosetteSep CD4 + T Cell Enrichment
Supplemental Figure 1. Quality control of CD4 + T-cell purification. CD4 + T cells were isolated from the freshly drawn blood of healthy donors and ACS patients using the RosetteSep CD4 + T Cell Enrichment
Hematopoiesis. Hematopoiesis. Hematopoiesis
 Chapter. Cells and Organs of the Immune System Hematopoiesis Hematopoiesis- formation and development of WBC and RBC bone marrow. Hematopoietic stem cell- give rise to any blood cells (constant number,
Chapter. Cells and Organs of the Immune System Hematopoiesis Hematopoiesis- formation and development of WBC and RBC bone marrow. Hematopoietic stem cell- give rise to any blood cells (constant number,
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Interferon γ regulates idiopathic pneumonia syndrome, a. Th17 + CD4 + T-cell-mediated GvH disease
 Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
An intrinsic thyrotropin-mediated pathway of TNF- production by bone marrow cells
 HEMATOPOIESIS An intrinsic thyrotropin-mediated pathway of TNF- production by bone marrow cells Heuy-Ching Wang, Jolene Dragoo, Qin Zhou, and John R. Klein Recent studies have identified a role for thyroid-stimulating
HEMATOPOIESIS An intrinsic thyrotropin-mediated pathway of TNF- production by bone marrow cells Heuy-Ching Wang, Jolene Dragoo, Qin Zhou, and John R. Klein Recent studies have identified a role for thyroid-stimulating
Supplementary Figure 1. Efficient DC depletion in CD11c.DOG transgenic mice
 Supplementary Figure 1. Efficient DC depletion in CD11c.DOG transgenic mice (a) CD11c.DOG transgenic mice (tg) were treated with 8 ng/g body weight (b.w.) diphtheria toxin (DT) i.p. on day -1 and every
Supplementary Figure 1. Efficient DC depletion in CD11c.DOG transgenic mice (a) CD11c.DOG transgenic mice (tg) were treated with 8 ng/g body weight (b.w.) diphtheria toxin (DT) i.p. on day -1 and every
Supplementalgfigureg1gSchematicgdiagramgofgtumor1modellingg
 SChinjectionh F:LuchLCLsh IVhinjectionh T:cellsh Monitorhforhtumorh growthhandhxeno: reactivehgvhd GVLgexperimentg kcbgvsgpbgt1cellse Xeno1reactiveg experimentg kcbgvsgpbgt1cellse IVhinjectionh 5xh,N^6
SChinjectionh F:LuchLCLsh IVhinjectionh T:cellsh Monitorhforhtumorh growthhandhxeno: reactivehgvhd GVLgexperimentg kcbgvsgpbgt1cellse Xeno1reactiveg experimentg kcbgvsgpbgt1cellse IVhinjectionh 5xh,N^6
Automated and Standardized Counting of Mouse Bone Marrow CFU Assays
 Automated and Standardized Counting of Mouse Bone Marrow CFU Assays 2 Automated and Standardized Colony Counting Table of Contents 4 Colony-Forming Unit (CFU) Assays for Mouse Bone Marrow 5 Automated Assay
Automated and Standardized Counting of Mouse Bone Marrow CFU Assays 2 Automated and Standardized Colony Counting Table of Contents 4 Colony-Forming Unit (CFU) Assays for Mouse Bone Marrow 5 Automated Assay
Generation of monocytederived Dendritic Cells (modcs)
 monocytederived Dendritic (modcs) Application Note Background Dendritic (DCs) are so called because of their characteristic cell surface projections that resemble the dendrites of neurons (see Fig 1 and
monocytederived Dendritic (modcs) Application Note Background Dendritic (DCs) are so called because of their characteristic cell surface projections that resemble the dendrites of neurons (see Fig 1 and
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the author to give readers additional information about his work. Supplement to: Olnes MJ, Scheinberg P, Calvo KR, et al. Eltrombopag and improved
Supplementary Appendix This appendix has been provided by the author to give readers additional information about his work. Supplement to: Olnes MJ, Scheinberg P, Calvo KR, et al. Eltrombopag and improved
Hemopoietic Precursors in Human Bone Marrow Transplantation
 International Journal of Cell Cloning 4: 11-18 Suppl 1 (1986) Hemopoietic Precursors in Human Bone Marrow Transplantation H.A. Messner Ontario Cancer Institute, University of Toronto, Toronto, Ontario,
International Journal of Cell Cloning 4: 11-18 Suppl 1 (1986) Hemopoietic Precursors in Human Bone Marrow Transplantation H.A. Messner Ontario Cancer Institute, University of Toronto, Toronto, Ontario,
In vitro bactericidal assay Fig. S8 Gentamicin protection assay Phagocytosis assay
 In vitro bactericidal assay Mouse bone marrow was isolated from the femur and the tibia. Cells were suspended in phosphate buffered saline containing.5% BSA and 2 mm EDTA and filtered through a cell strainer.
In vitro bactericidal assay Mouse bone marrow was isolated from the femur and the tibia. Cells were suspended in phosphate buffered saline containing.5% BSA and 2 mm EDTA and filtered through a cell strainer.
SUPPLEMENTARY INFORMATION. CXCR4 inhibitors could benefit to HER2 but not to Triple-Negative. breast cancer patients
 SUPPLEMENTARY INFORMATION CXCR4 inhibitors could benefit to HER2 but not to Triple-Negative breast cancer patients Lefort S. 1,2, Thuleau A. 3, Kieffer Y. 1,2, Sirven P. 1,2, Bieche I. 4, Marangoni E.
SUPPLEMENTARY INFORMATION CXCR4 inhibitors could benefit to HER2 but not to Triple-Negative breast cancer patients Lefort S. 1,2, Thuleau A. 3, Kieffer Y. 1,2, Sirven P. 1,2, Bieche I. 4, Marangoni E.
S-NITROSOGLUTATHIONE MODULATES CXCR4 AND ICOS EXPRESSION
 CELLULAR & MOLECULAR BIOLOGY LETTERS Volume 11, (2006) pp 30 36 http://www.cmbl.org.pl Received: 01 August 2005 Revised form accepted: 17 November 2005 DOI: 10.2478/s11658-006-0003-9 2006 by the University
CELLULAR & MOLECULAR BIOLOGY LETTERS Volume 11, (2006) pp 30 36 http://www.cmbl.org.pl Received: 01 August 2005 Revised form accepted: 17 November 2005 DOI: 10.2478/s11658-006-0003-9 2006 by the University
Hematopoietic Growth Factors Colony Stimulating Factors. Erythropoietin (Epoetin alfa). Granulocyte-macrophage colonystimulating factor (G-CSF).
 Hematopoietic Growth Factors Colony Stimulating Factors. Erythropoietin (Epoetin alfa). Granulocyte colony-stimulating factor(g-csf). Granulocyte-macrophage colonystimulating factor (G-CSF). Interleukin-11
Hematopoietic Growth Factors Colony Stimulating Factors. Erythropoietin (Epoetin alfa). Granulocyte colony-stimulating factor(g-csf). Granulocyte-macrophage colonystimulating factor (G-CSF). Interleukin-11
Rapid Decline of Clonogenic Hemopoietic Progenitors in Semisolid Cultures of Bone Marrow Samples Derived from Patients with Chronic Myeloid Leukemia
 Original Manuscript International Journal of Cell Cloning 7314-321 (1989) Rapid Decline of Clonogenic Hemopoietic Progenitors in Semisolid Cultures of Bone Marrow Samples Derived from Patients with Chronic
Original Manuscript International Journal of Cell Cloning 7314-321 (1989) Rapid Decline of Clonogenic Hemopoietic Progenitors in Semisolid Cultures of Bone Marrow Samples Derived from Patients with Chronic
Stem cells: units of development and regeneration. Fernando D. Camargo Ph.D. Whitehead Fellow Whitehead Institute for Biomedical Research.
 Stem cells: units of development and regeneration Fernando D. Camargo Ph.D. Whitehead Fellow Whitehead Institute for Biomedical Research Concepts 1. Embryonic vs. adult stem cells 2. Hematopoietic stem
Stem cells: units of development and regeneration Fernando D. Camargo Ph.D. Whitehead Fellow Whitehead Institute for Biomedical Research Concepts 1. Embryonic vs. adult stem cells 2. Hematopoietic stem
Myelodysplastic scoring system with flow cytometry. G Detry B Husson
 Myelodysplastic scoring system with flow cytometry G Detry B Husson Myelodysplastic syndroms Clonal haematopoietic stem cell disease characterized by dysplasia in one or more of the myeloid cell lines
Myelodysplastic scoring system with flow cytometry G Detry B Husson Myelodysplastic syndroms Clonal haematopoietic stem cell disease characterized by dysplasia in one or more of the myeloid cell lines
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
The system Fas/Fas-L in SLE
 The system Fas/Fas-L in SLE NATALIA BELUSHKINA 1, ABDELMAROUF MOHIELDEIN 2, ULIANA PETROVA 3. 1,2 Department of Biochemistry, 3 Deparment of immunology 1 Sechenov Moscow Medical Academy, Research Institute
The system Fas/Fas-L in SLE NATALIA BELUSHKINA 1, ABDELMAROUF MOHIELDEIN 2, ULIANA PETROVA 3. 1,2 Department of Biochemistry, 3 Deparment of immunology 1 Sechenov Moscow Medical Academy, Research Institute
Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel:
 Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Understand the physiological
Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Understand the physiological
Supplementary Figure 1. Generation of knockin mice expressing L-selectinN138G. (a) Schematics of the Sellg allele (top), the targeting vector, the
 Supplementary Figure 1. Generation of knockin mice expressing L-selectinN138G. (a) Schematics of the Sellg allele (top), the targeting vector, the targeted allele in ES cells, and the mutant allele in
Supplementary Figure 1. Generation of knockin mice expressing L-selectinN138G. (a) Schematics of the Sellg allele (top), the targeting vector, the targeted allele in ES cells, and the mutant allele in
Targeting tumour associated macrophages in anti-cancer therapies. Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018
 Targeting tumour associated macrophages in anti-cancer therapies Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018 Macrophages: Professional phagocytes of the myeloid lineage APC,
Targeting tumour associated macrophages in anti-cancer therapies Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018 Macrophages: Professional phagocytes of the myeloid lineage APC,
Chemotherapeutic Susceptibility of Human Bone Marrow Progenitor Cells and Human Myelogenous Leukemia Cells (HMO) in Co-Culture: Preliminary Report
 International Journal of Cell Cloning 2: 254-262 (1984) Chemotherapeutic Susceptibility of Human Bone Marrow Progenitor Cells and Human Myelogenous Leukemia Cells (HMO) in Co-Culture: Preliminary Report
International Journal of Cell Cloning 2: 254-262 (1984) Chemotherapeutic Susceptibility of Human Bone Marrow Progenitor Cells and Human Myelogenous Leukemia Cells (HMO) in Co-Culture: Preliminary Report
Supporting Information
 Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
Human and mouse T cell regulation mediated by soluble CD52 interaction with Siglec-10. Esther Bandala-Sanchez, Yuxia Zhang, Simone Reinwald,
 Human and mouse T cell regulation mediated by soluble CD52 interaction with Siglec-1 Esther Bandala-Sanchez, Yuxia Zhang, Simone Reinwald, James A. Dromey, Bo Han Lee, Junyan Qian, Ralph M Böhmer and Leonard
Human and mouse T cell regulation mediated by soluble CD52 interaction with Siglec-1 Esther Bandala-Sanchez, Yuxia Zhang, Simone Reinwald, James A. Dromey, Bo Han Lee, Junyan Qian, Ralph M Böhmer and Leonard
and follicular helper T cells is Egr2-dependent. (a) Diagrammatic representation of the
 Supplementary Figure 1. LAG3 + Treg-mediated regulation of germinal center B cells and follicular helper T cells is Egr2-dependent. (a) Diagrammatic representation of the experimental protocol for the
Supplementary Figure 1. LAG3 + Treg-mediated regulation of germinal center B cells and follicular helper T cells is Egr2-dependent. (a) Diagrammatic representation of the experimental protocol for the
SUPPLEMENTARY INFORMATION. Involvement of IL-21 in the epidermal hyperplasia of psoriasis
 SUPPLEMENTARY INFORMATION Involvement of IL-21 in the epidermal hyperplasia of psoriasis Roberta Caruso 1, Elisabetta Botti 2, Massimiliano Sarra 1, Maria Esposito 2, Carmine Stolfi 1, Laura Diluvio 2,
SUPPLEMENTARY INFORMATION Involvement of IL-21 in the epidermal hyperplasia of psoriasis Roberta Caruso 1, Elisabetta Botti 2, Massimiliano Sarra 1, Maria Esposito 2, Carmine Stolfi 1, Laura Diluvio 2,
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION
 CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Data Sheet. NFAT Reporter (Luc) Jurkat Cell line Catalog #: 60621
 Data Sheet NFAT Reporter (Luc) Jurkat Cell line Catalog #: 60621 Background The nuclear factor of activator T cells (NFAT) family of transcription factors plays an important role in immune response. T
Data Sheet NFAT Reporter (Luc) Jurkat Cell line Catalog #: 60621 Background The nuclear factor of activator T cells (NFAT) family of transcription factors plays an important role in immune response. T
Cooperation of germ line JAK2 mutations E846D and R1063H leads to erythroid hyperplasia with megakaryocytic atypia
 Cooperation of germ line JAK2 mutations E846D and R1063H leads to erythroid hyperplasia with megakaryocytic atypia Katarina Kapralova, Ph.D. Department of Biology Faculty of Medicine and Dentistry Palacký
Cooperation of germ line JAK2 mutations E846D and R1063H leads to erythroid hyperplasia with megakaryocytic atypia Katarina Kapralova, Ph.D. Department of Biology Faculty of Medicine and Dentistry Palacký
Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE)
 Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central
Direct ex vivo characterization of human antigen-specific CD154 + CD4 + T cells Rapid antigen-reactive T cell enrichment (Rapid ARTE) Introduction Workflow Antigen (ag)-specific T cells play a central
Cytokines, adhesion molecules and apoptosis markers. A comprehensive product line for human and veterinary ELISAs
 Cytokines, adhesion molecules and apoptosis markers A comprehensive product line for human and veterinary ELISAs IBL International s cytokine product line... is extremely comprehensive. The assays are
Cytokines, adhesion molecules and apoptosis markers A comprehensive product line for human and veterinary ELISAs IBL International s cytokine product line... is extremely comprehensive. The assays are
The CD40/CD40 ligand interactions exert pleiotropic effects on bone marrow granulopoiesis
 Article The / ligand interactions exert pleiotropic effects on bone marrow granulopoiesis Irene Mavroudi,*, Vassiliki Papadaki,* Katerina Pyrovolaki,* Pavlos Katonis, Aristides G. Eliopoulos,, and Helen
Article The / ligand interactions exert pleiotropic effects on bone marrow granulopoiesis Irene Mavroudi,*, Vassiliki Papadaki,* Katerina Pyrovolaki,* Pavlos Katonis, Aristides G. Eliopoulos,, and Helen
EML Erythroid and Neutrophil Differentiation Protocols Cristina Pina 1*, Cristina Fugazza 2 and Tariq Enver 3
 EML Erythroid and Neutrophil Differentiation Protocols Cristina Pina 1*, Cristina Fugazza 2 and Tariq Enver 3 1 Department of Haematology, University of Cambridge, Cambridge, UK; 2 Dipartimento de Biotecnologie
EML Erythroid and Neutrophil Differentiation Protocols Cristina Pina 1*, Cristina Fugazza 2 and Tariq Enver 3 1 Department of Haematology, University of Cambridge, Cambridge, UK; 2 Dipartimento de Biotecnologie
Aplastic anemia. Case report. Effect of antithymocyte globulin on erythroid colony formation
 Case report Aplastic anemia Effect of antithymocyte globulin on erythroid colony formation Susan A. Rothmann Hamburger, Ph.D. Department of Laboratory Hematology and Blood Banking James H. Finke, Ph.D.
Case report Aplastic anemia Effect of antithymocyte globulin on erythroid colony formation Susan A. Rothmann Hamburger, Ph.D. Department of Laboratory Hematology and Blood Banking James H. Finke, Ph.D.
In vitro expansion of mouse CD4 + T cells
 Direct ex vivo isolation, cultivation and expansion of CD4 + T cells from mouse spleen In vitro expansion of mouse CD4 + T cells Introduction CD4 + T helper (TH) cells play a central role in the adaptive
Direct ex vivo isolation, cultivation and expansion of CD4 + T cells from mouse spleen In vitro expansion of mouse CD4 + T cells Introduction CD4 + T helper (TH) cells play a central role in the adaptive
Immunopathology. 2-Patterned hemodynamic responses, cell surface associated and soluble mediator systems (e.g., complement and coagulation systems).
 Immunopathology The chief role of the immune system is to protect the host from invasion by foreign agents. Immune responses can be elicited by a wide range of agents including toxins, drugs, chemicals,
Immunopathology The chief role of the immune system is to protect the host from invasion by foreign agents. Immune responses can be elicited by a wide range of agents including toxins, drugs, chemicals,
in MDS Amit Verma Albert Einstein College of Medicine
 Signal Transduction Inhibitors in MDS Amit Verma Albert Einstein College of Medicine Ineffective Hematopoiesis in MDS Hypercellular marrows with decreased peripheral blood counts Increased Cell death (Apoptosis/Cell
Signal Transduction Inhibitors in MDS Amit Verma Albert Einstein College of Medicine Ineffective Hematopoiesis in MDS Hypercellular marrows with decreased peripheral blood counts Increased Cell death (Apoptosis/Cell
UMR CNRS 6101, Service d Hématologie Clinique, Service de Pédiatrie, CHU Dupuytren, Limoges, France
 Stem Cells Original Article Membrane and Intracellular Platelet-Activating Factor Receptor Expression in Leukemic Blasts of Patients with Acute Myeloid and Lymphoid Leukemia M. DONNARD, L. GUGLIELMI, P.
Stem Cells Original Article Membrane and Intracellular Platelet-Activating Factor Receptor Expression in Leukemic Blasts of Patients with Acute Myeloid and Lymphoid Leukemia M. DONNARD, L. GUGLIELMI, P.
BD Pharmingen. Human Th1/Th2/Th17 Phenotyping Kit. Technical Data Sheet. Product Information. Description Components:
 Technical Data Sheet Human Th1/Th2/Th17 Phenotyping Kit Product Information Material Number: Size: Description Components: 560751 50 Tests BD Pharmingen 51-9006615 Human Th1/Th2/Th17 Phenotyping Cocktail
Technical Data Sheet Human Th1/Th2/Th17 Phenotyping Kit Product Information Material Number: Size: Description Components: 560751 50 Tests BD Pharmingen 51-9006615 Human Th1/Th2/Th17 Phenotyping Cocktail
SUPPLEMENTARY INFORMATION
 Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to
 Class II tetramer staining Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to PE were combined with dominant HIV epitopes (DRB1*0101-DRFYKTLRAEQASQEV, DRB1*0301- PEKEVLVWKFDSRLAFHH,
Class II tetramer staining Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to PE were combined with dominant HIV epitopes (DRB1*0101-DRFYKTLRAEQASQEV, DRB1*0301- PEKEVLVWKFDSRLAFHH,
Effects of Mast Cell Growth Factor on Ara-C Mediated Acute Myeloid Leukemia Cell Killing
 Effects of Mast Cell Growth Factor on Ara-C Mediated Acute Myeloid Leukemia Cell Killing A. Tafuri, L. De Felice, M. G. Mascolo, T. Valentini, M. T. Petrucci, M. C. Petti University La Sapienza of Rome,
Effects of Mast Cell Growth Factor on Ara-C Mediated Acute Myeloid Leukemia Cell Killing A. Tafuri, L. De Felice, M. G. Mascolo, T. Valentini, M. T. Petrucci, M. C. Petti University La Sapienza of Rome,
HCV core protein interaction with gc1q receptor inhibits Th1 differentiation of CD4 T cells via suppression of dendritic cell IL-12 production
 HCV core protein interaction with gcq receptor inhibits Th differentiation of CD T cells via suppression of dendritic cell IL- production Stephen N. Waggoner,*, Caroline H. T. Hall,* and Young S. Hahn*,,
HCV core protein interaction with gcq receptor inhibits Th differentiation of CD T cells via suppression of dendritic cell IL- production Stephen N. Waggoner,*, Caroline H. T. Hall,* and Young S. Hahn*,,
Principles of Adaptive Immunity
 Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
ImageStream cytometer analysis. Cells were cultured as described above in vented-cap
 ImageStream cytometer analysis. Cells were cultured as described above in vented-cap polypropylene tubes, stained with αcd66b-fitc, αm-dc8-pe and αcd56-pe-cy5.5 mabs, washed and fixed with 4 % (w/v) paraformaldehyde.
ImageStream cytometer analysis. Cells were cultured as described above in vented-cap polypropylene tubes, stained with αcd66b-fitc, αm-dc8-pe and αcd56-pe-cy5.5 mabs, washed and fixed with 4 % (w/v) paraformaldehyde.
January 25, 2017 Scientific Research Process Name of Journal: ESPS Manuscript NO: Manuscript Type: Title: Authors: Correspondence to
 January 25, 2017 Scientific Research Process Name of Journal: World Journal of Gastroenterology ESPS Manuscript NO: 31928 Manuscript Type: ORIGINAL ARTICLE Title: Thiopurine use associated with reduced
January 25, 2017 Scientific Research Process Name of Journal: World Journal of Gastroenterology ESPS Manuscript NO: 31928 Manuscript Type: ORIGINAL ARTICLE Title: Thiopurine use associated with reduced
Immunology Lecture 4. Clinical Relevance of the Immune System
 Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
IL-3. Alternative names. Structure. Discovery. Main activities and pathophysiological roles. John W. Schrader * SUMMARY BACKGROUND
 IL-3 John W. Schrader * The Biomedical Research Centre, University of British Columbia, 2222 Health Sciences Mall, Vancouver, British Columbia, Canada V6T 1Z3 * corresponding author tel: 604-822-7810,
IL-3 John W. Schrader * The Biomedical Research Centre, University of British Columbia, 2222 Health Sciences Mall, Vancouver, British Columbia, Canada V6T 1Z3 * corresponding author tel: 604-822-7810,
Childhood hematopoiesis and hematological features. Yongmin Tang Dept. Hematology-oncology Chidlren s Hospital Zhejiang University School of medicine
 Childhood hematopoiesis and hematological features Yongmin Tang Dept. Hematology-oncology Chidlren s Hospital Zhejiang University School of medicine Questions: How much have you known about our hematopoietic
Childhood hematopoiesis and hematological features Yongmin Tang Dept. Hematology-oncology Chidlren s Hospital Zhejiang University School of medicine Questions: How much have you known about our hematopoietic
Gladstone Institutes, University of California (UCSF), San Francisco, USA
 Fluorescence-linked Antigen Quantification (FLAQ) Assay for Fast Quantification of HIV-1 p24 Gag Marianne Gesner, Mekhala Maiti, Robert Grant and Marielle Cavrois * Gladstone Institutes, University of
Fluorescence-linked Antigen Quantification (FLAQ) Assay for Fast Quantification of HIV-1 p24 Gag Marianne Gesner, Mekhala Maiti, Robert Grant and Marielle Cavrois * Gladstone Institutes, University of
Supplement Material. Spleen weight (mg) LN cells (X106) Acat1-/- Acat1-/- Mouse weight (g)
 Supplement Material A Spleen weight (mg) C Mouse weight (g) 1 5 1 2 9 6 3 2 5 2 1 5 Male LN cells (X16) 4 ** ** Female B 3 2 1 Supplemental Figure I. Spleen weight (A), Inguinal lymph node (LN) cell number
Supplement Material A Spleen weight (mg) C Mouse weight (g) 1 5 1 2 9 6 3 2 5 2 1 5 Male LN cells (X16) 4 ** ** Female B 3 2 1 Supplemental Figure I. Spleen weight (A), Inguinal lymph node (LN) cell number
HD1 (FLU) HD2 (EBV) HD2 (FLU)
 ramer staining + anti-pe beads ramer staining a HD1 (FLU) HD2 (EBV) HD2 (FLU).73.11.56.46.24 1.12 b CD127 + c CD127 + d CD127 - e CD127 - PD1 - PD1 + PD1 + PD1-1 1 1 1 %CD127 + PD1-8 6 4 2 + anti-pe %CD127
ramer staining + anti-pe beads ramer staining a HD1 (FLU) HD2 (EBV) HD2 (FLU).73.11.56.46.24 1.12 b CD127 + c CD127 + d CD127 - e CD127 - PD1 - PD1 + PD1 + PD1-1 1 1 1 %CD127 + PD1-8 6 4 2 + anti-pe %CD127
Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer
 Supplementary Information Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer Gi-Hoon Nam, Eun-Jung Lee, Yoon Kyoung Kim, Yeonsun Hong, Yoonjeong Choi,
Supplementary Information Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer Gi-Hoon Nam, Eun-Jung Lee, Yoon Kyoung Kim, Yeonsun Hong, Yoonjeong Choi,
PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human
 Anti-CD19-CAR transduced T-cell preparation PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human AB serum (Gemini) and 300 international units/ml IL-2 (Novartis). T cell proliferation
Anti-CD19-CAR transduced T-cell preparation PBMC from each patient were suspended in AIM V medium (Invitrogen) with 5% human AB serum (Gemini) and 300 international units/ml IL-2 (Novartis). T cell proliferation
Data Sheet PD-1 / NFAT Reporter - Jurkat Cell Line Catalog #: 60535
 Data Sheet PD-1 / NFAT Reporter - Jurkat Cell Line Catalog #: 60535 Product Description Recombinant Jurkat T cell expressing firefly luciferase gene under the control of NFAT response elements with constitutive
Data Sheet PD-1 / NFAT Reporter - Jurkat Cell Line Catalog #: 60535 Product Description Recombinant Jurkat T cell expressing firefly luciferase gene under the control of NFAT response elements with constitutive
Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2*
 Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2* 1 Department of Laboratory Medicine - Laboratory of Hematology, Radboud University
Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2* 1 Department of Laboratory Medicine - Laboratory of Hematology, Radboud University
