Chronic diarrhea, defined as the production of liquid or
|
|
|
- Lenard Ross
- 5 years ago
- Views:
Transcription
1 Mastocytic Enterocolitis Increased Mucosal Mast Cells in Chronic Intractable Diarrhea Shriram Jakate, MD, FRCPath; Mark Demeo, MD; Rohan John, MD; Mary Tobin, MD; Ali Keshavarzian, MD Context. In some adult patients with chronic intractable diarrhea, the diagnosis remains elusive even after detailed evaluations, and colonic or duodenal biopsy specimens may appear unremarkable on routine hematoxylineosin staining. Objectives. To assess the concentration of mast cells in colonic or duodenal biopsy specimens by immunohistochemical analysis for mast cell tryptase from patients with chronic intractable diarrhea and to evaluate their response to drugs affecting mast cell function. Design. Mast cells per high-power field were assessed in biopsy specimens from 47 patients with chronic intractable diarrhea, from 50 control subjects, and from 63 patients with other specific diseases that cause chronic diarrhea (inflammatory bowel disease, celiac disease, collagenous colitis, and lymphocytic colitis). Patients with chronic intractable diarrhea who had more than 20 mast cells per high-power field were administered drugs affecting mast cell mediator function and release. Results. The mean SD concentration of mast cells in the 50 control subjects was cells per high-power field; hence, patients with more than 20 mast cells per high-power field were considered to have increased mast cells. Thirty-three (70%) of 47 patients with chronic intractable diarrhea had increased mast cells, and symptoms were controlled by drug therapy in 22 (67%) of the 33 patients. No patient had systemic or cutaneous mastocytosis. No increase in mast cells was seen in patients with other common causes of chronic diarrhea. Conclusions. In chronic intractable diarrhea, colonic or duodenal biopsy specimens may appear unremarkable on routine hematoxylin-eosin staining, but increased mast cells may be demonstrated by immunohistochemistry for mast cell tryptase, with the novel term mastocytic enterocolitis describing this condition. Similar increases in mast cells are not apparent in control populations or in patients with other specific diseases that cause chronic diarrhea. The cause of the increased mast cells remains to be elucidated. (Arch Pathol Lab Med. 2006;130: ) Chronic diarrhea, defined as the production of liquid or loose stools for more than 4 weeks, has an approximate prevalence of 5% among the US population. 1 The causes of chronic diarrhea vary widely by age and by socioeconomic status of the population surveyed. The most frequent diagnoses in patients with chronic diarrhea in developed countries include irritable bowel syndrome (IBS), inflammatory bowel disease, malabsorption syndrome (including celiac disease or gluten-sensitive enteropathy), chronic infections, and idiopathic secretory diarrhea. 1 Most of these conditions can be diagnosed by following the guidelines for evaluation recommended by the American Gastroenterological Association, 2 which include a detailed 14-point history, physical examination, routine laboratory tests, therapeutic trials, stool analysis, and further evaluations such as culture studies, radiography, en- Accepted for publication October 28, From the Departments of Pathology (Drs Jakate and John) and Medicine (Drs Demeo, Tobin, and Keshavarzian), Rush University Medical Center, Chicago, Ill. The authors have no relevant financial interest in the products or companies described in this article. Presented at the 94th Annual Meeting of the United States and Canadian Academy of Pathology, San Antonio, Tex, February 28, Reprints: Shriram Jakate, MD, FRCPath, Department of Pathology, Rush University Medical Center, 1653 W Congress Pkwy, Chicago, IL ( shriram jakate@rush.edu). doscopy, and biopsies. Management strategies also include concurrent testing and empiric treatment. 3 However, in some patients, no cause is clinically apparent even after these guidelines are followed, and the diagnosis remains indeterminate and the treatment frustrating. Mucosal mast cells are key regulators of intestinal sensory and motor function and may be involved in chronic functional diarrhea. We observed increased mast cells in the gut mucosa as the principal morphologic abnormality in a subset of patients with chronic functional diarrhea. We consider this a distinctive morphologic disorder that is revealed by immunohistochemical analysis for mast cell tryptase (MCT) and term this condition mastocytic enterocolitis. The increase in mast cells is not associated with systemic or cutaneous mastocytosis. Most patients with this condition respond to drugs affecting mast cell mediator function and release such as histamine H 1 and H 2 receptor antagonists and granule membrane stabilizing agents. An increase in enterocolonic mucosal mast cells is postulated to be a reactive and gut-specific phenomenon resulting from unknown stimuli. This increase is presumed to enhance mast cell mediator release, which results in diarrhea and abdominal pain through paracrine interaction with the enteric nervous system and its effector motor response. In our affected patients, no consistent underlying clinical determinants were obvious, and many cases would be classified as diarrhea-predominant IBS for 362 Arch Pathol Lab Med Vol 130, March 2006 Mastocytic Enterocolitis Jakate et al
2 lack of a more specific diagnosis. To calibrate the increase in mast cells, we determined the baseline concentration of mast cells in adult colonic and duodenal mucosa in incidentally biopsied tissue from control subjects. To estimate the specificity of increased mast cells in chronic intractable diarrhea, the mucosal concentration of mast cells was investigated in other common disorders that cause chronic diarrhea, such as inflammatory bowel disease, gluten-sensitive enteropathy, collagenous colitis, and lymphocytic colitis. MATERIALS AND METHODS Forty-seven patients (32 women and 15 men; age range, years) were diagnosed as having chronic persistent diarrhea of unknown cause at our institution between 2000 and All patients underwent the investigational protocol recommended by the American Gastroenterological Association. A comprehensive history was obtained that included the onset, pattern, and duration of symptoms, as well as the presence or absence of fecal incontinence, abdominal pain, weight loss, medication use, recent travel, diet, and stress. A physical examination was conducted to assess the extent of fluid loss, as well to evaluate rashes, flushing, oral ulcers, edema, perianal skin, anal sphincter tone, abdominal masses, and ascites. Complete blood counts and a basic metabolic panel (serum sodium, potassium, chloride, carbon dioxide, glucose, calcium, urea nitrogen, and creatinine) were performed. A stool analysis assessed the type and severity of diarrhea and the presence of ova and parasites. In addition, the patients underwent full colonoscopy (22/47 patients), upper endoscopy (20 patients), or both (5 patients), with random biopsy samples taken from the colon and from the second part of the duodenum. The random colonic biopsies included 4 to 10 pieces taken from the right and left colon and submitted in one container, and the random duodenal biopsies included 2 to 5 pieces taken mainly from the second part of the duodenum and submitted in one container. The colonic and duodenal biopsy specimens were processed for routine histologic examination with standard formalin fixation and paraffin embedding, and 5- m-thin sections were stained with hematoxylin-eosin. In addition, all sections were immunohistochemically stained for MCT as follows: 4- m-thin sections were cut, dried, and deparaffinized before placing them on the Ventana NexES autostainer (Ventana Medical Systems Inc, Tucson, Ariz), where they were treated with protease 1 for 4 minutes and then incubated with monoclonal mouse anti-human MCT (clone AA1, code M 7052; DAKO, Carpinteria, Calif; dilution 1: 1600) for 32 minutes. A recommended negative control was used. Visualization was performed using the iview DAB detection kit (Ventana Medical Systems Inc). To establish the baseline concentration of mucosal mast cells, similar immunohistochemical staining was performed on 50 incidentally obtained duodenal (n 25) and colonic (n 25) biopsy specimens from patients with conditions unrelated to diarrhea (such as duodenal biopsies for gastroesophageal reflux, Helicobacter gastritis, gastric fundic gland polyps, and mucosa adjacent to duodenal adenomatous polyps; and colonic biopsies for melanosis and mucosa adjacent to adenomatous polyps). The baseline concentration was presumed to be the distribution of mast cells in a control population of comparable age and sex (age range, years; female-male ratio, 27:23) as the study population. The sources of the control biopsy specimens included the duodenal bulb, second part of the duodenum, random or unspecified duodenum, random colon, right colon, left colon, descending colon, sigmoid, and rectum. In addition, biopsy specimens from 63 patients with chronic diarrhea caused by the following specific diseases were immunostained for MCT: collagenous colitis (4 patients), lymphocytic colitis (3 patients), Crohn colitis (9 patients), ulcerative colitis (12 patients), and gluten-sensitive enteropathy (35 patients). Endoscopic mucosal biopsies in these patients were initial diagnostic specimens demonstrating active inflammation and were not posttherapeutic or surveillance samples. Mast cells (representing 2 separate biopsy pieces and random parts of the mucosa that filled the entire visual field) were counted per high-power field (original magnification 400, objective 40, and eyepiece 10) and were averaged per 10 high-power fields. Muscularis mucosa and submucosa were excluded from mast cell counts. In the duodenum, only the closely arranged villi that filled the entire visual field were included. In addition, only the intact mast cells with visible nuclei and darkly staining cytoplasm were counted. Wisps of extracellular, apparently degranulated tryptase were excluded from counts. In 40 of 47 study patients, concurrent toluidine blue staining was used to demonstrate metachromasia in mast cells. Levels of serum tryptase were determined in 3 of 47 patients. Among the 47 patients with chronic intractable diarrhea, 33 patients had increased mast cells ( 20 mast cells per high-power field) and were administered a 2-week regimen of 10 mg/d of cetirizine hydrochloride (an H 1 receptor antagonist) and 300 mg twice a day of ranitidine hydrochloride (an H 2 receptor antagonist). In 8 of the 33 patients, a third drug, 200 mg (in 10 ml) of cromolyn sodium (a mast cell mediator release inhibitor) was given 4 times daily for 4 to 6 weeks. The patients were followed up for resolution, improvement, or persistence of symptoms. The patients who did not have increased mast cells were not given these drugs. RESULTS All 47 study patients had chronic diarrhea of unknown cause, and no specific underlying disorder could be identified after conducting the recommended history, physical examination, routine laboratory tests, and stool analysis. Twenty-one of the 47 patients also had variable and intermittent abdominal pain and were diagnosed as having possible diarrhea-predominant IBS, based on Rome II diagnostic criteria. 4 No patient had documented systemic or cutaneous mastocytosis. Assessment of serum tryptase levels in the 3 patients analyzed showed no elevation. On endoscopy, the colon and duodenum were described as being normal in 43 of 47 patients and as showing mild edema in the other 4 patients. In 34 of 47 patients, the colonic and duodenal mucosa appeared normal on routine hematoxylin-eosin staining (Figure 1) or showed a mild and focal increase in mixed inflammatory cells in the lamina propria (Figure 2). In the other 13 patients, there was a mild increase in eosinophils in the lamina propria, without any other abnormality (Figure 3). In particular, there were no specific pathologic features such as crypt distortion or mucin depletion, cryptitis, crypt abscesses, granulomas, thickened collagen band, excessive eosinophils, increased intraepithelial lymphocytes, shortened duodenal villi, parasites, or viral inclusions. In the 40 samples stained with toluidine blue, 30% to 60% fewer mast cells were highlighted than with MCT, because only the heavily granulated mast cells showed metachromasia. Hence, the results of toluidine blue staining were eliminated from the analysis. Immunostaining for MCT revealed intracytoplasmic brown staining that was highly specific for mast cells. The staining was so consistently strong that it was read as positive or as negative for mast cells, without assessing the intensity of staining. The mean SD concentration of mucosal mast cells in the control population was cells per high-power field (colon, cells; and duodenum, cells) (Figure 4). When other tissue such as duodenal bulb, stomach, and ileum was included with colon or duodenum, the variation in mast cell counts was no Arch Pathol Lab Med Vol 130, March 2006 Mastocytic Enterocolitis Jakate et al 363
3 Figure 1. Histologically normal appearing colonic (A) and duodenal (B) mucosa (hematoxylin-eosin, original magnification 200). Figure 2. Mild nonspecific increase in mixed inflammatory cells in the lamina propria of colonic (A) and duodenal (B) mucosa (hematoxylineosin, original magnification 200). greater than 2 SD. However, only the colonic and duodenal tissue counts were considered baseline values for comparison with colonic and duodenal samples in the study patients with chronic intractable diarrhea. The presence of more than 20 mast cells per high-power field was considered an increase in mast cells because this represented 2 SD beyond the normal values for colon and duodenum. Among the 63 samples from patients with other specific diseases that cause chronic diarrhea, the mean SD mast cell count of cells per high-power field was close to that of the control population. Thirty-three (70%) of 47 study patients with chronic intractable diarrhea had increased mast cells (mean SD, cells per highpower field) (Figure 5). Figure 6 illustrates the mean SD concentrations of mast cells in the control subjects, in the patients with diarrhea caused by specific diseases, and in the study patients with chronic intractable diarrhea. Among the 5 patients who underwent both colonic and duodenal biopsies, the increase in mast cells observed in 3 patients was seen in both organs, suggesting a diffuse enterocolonic mucosal increase. Among all biopsy samples in which there was an increase in mast cells, the increase was generally diffuse in the mucosa, with little elevation in the concentration of submucosal mast cells (Figure 7), with no sex differences observed in the control versus the affected populations. At follow-up, 22 (67%) of 33 study patients who received H 1 and H 2 receptor antagonists with or without mast cell mediator release inhibitor showed cessation of diarrhea or significant reduction in diarrhea (defined as 50% reduction in stool frequency or as 50% improvement in stool consistency). COMMENT Mast cells, functionally and morphologically distinct cells of hematopoietic origin, are distributed throughout many tissues 5 and are rich in gastrointestinal mucosa, enabling their immune function in response to a diversity of environmental substances in the gut lumen. Mast cells are unique granulocytes because they are absent in peripheral blood and develop in situ from CD34-positive or c-kit positive progenitor cells. 6 Within the gut, the following 2 distinct subpopulations of mast cells are distinguishable by their neutral protease content: (1) the mucosal reactive mast cells, which may increase dramatically in response to immune stimuli and are dependent on T lymphocytes (termed the Tmastcellphenotype because it contains tryptase) and (2) the submucosal constitutive mast cells, which are more static, are related to angiogenesis 364 Arch Pathol Lab Med Vol 130, March 2006 Mastocytic Enterocolitis Jakate et al
4 Figure 5. Increased mast cells visualized by immunohistochemical staining for mast cell tryptase in patients with chronic intractable diarrhea in colonic (A) and duodenal (B) mucosa (original magnification 400). Figure 3. Mild increase in eosinophils in the lamina propria of colonic mucosa (hematoxylin-eosin, original magnification 200). Figure 4. Distribution of mast cells visualized by immunohistochemical staining for mast cell tryptase in control samples in colonic (A) and duodenal (B) mucosa (original magnification 400). and tissue remodeling, and are unrelated to the immune system (termed the TC mast cell phenotype because it contains tryptase and chymase). 7,8 Mast cells are best known for their classic role in the allergic hypersensitivity type I reaction, in which binding of multivalent allergen to membrane-bound immunoglobulin E causes activation and release of stored inflammatory mediators in secretory granules, including histamine, neutral proteases, cytokines, lipid mediators, and others. However, mast cells may have an equal or greater role in the gastrointestinal tract in immune response to complement components 9 against various microbial and other agents, in excitability on central nervous system stimuli such as stress, 10 and as strategic connector between the gut lumen and the integrated enteric nervous system. 11 The contribution of mast cells to gastrointestinal symptoms is exemplified by the frequency of gastrointestinal complaints in systemic mastocytosis (commonly abdominal pain and diarrhea and less frequently nausea and vomiting) Patients with systemic mastocytosis have shown abnormally increased visceral sensitivity to rectal balloon distension, which may explain diarrhea, urgency, and fecal incontinence. 15 Mast cell degranulation has been shown to mediate postoperative ileus in a murine model, 16 indicative of the role of mast cells in hypomotility and hypermotility of the gut. In many gastrointestinal diseases that may cause chronic diarrhea, the role of mast cells and their mediators is being investigated, although with increasing controversy. There have been several reports of increased, normal, or Arch Pathol Lab Med Vol 130, March 2006 Mastocytic Enterocolitis Jakate et al 365
5 Figure 6. Chart illustrating the distribution of mast cells in control subjects, patients with diarrhea caused by specific diseases, and patients with chronic intractable diarrhea. Figure 7. Microphotograph showing preferential mucosal increase of mast cells compared with the static submucosal mast cells in the duodenum (immunohistochemical staining for mast cell tryptase, original magnification 100). decreased concentrations of mast cells in inflammatory bowel disease, increased MCT secretion in ulcerative colitis, 21 mast cell mediated ion transport in inflammatory bowel disease, 22 increased mast cell activation in collagenous colitis, 23,24 and increased or decreased mast cell concentrations in gluten-sensitive enteropathy Some contribution of mast cells in the pathogenesis of these diseases appears inevitable by virtue of their diffuse residence in the gastrointestinal mucosa, their role as potent mediators, and their close collaboration with the enteric nervous system. Among the gastrointestinal diseases that may cause chronic diarrhea, IBS is intriguing because the diagnosis is based on symptoms and on exclusion of other diseases. Irritable bowel syndrome has an overall prevalence in the United States of about 2.9% among the adult population, and the symptoms include pain, constipation, or predominant diarrhea. 28 Predominant diarrhea is the least frequent of the 3 symptoms, with no published incidence rates, but probably comprising fewer than 20% of IBS cases. Twenty-one (45%) of our 47 study patients had abdominal pain and were initially presumed to have diarrheapredominant IBS. In patients with IBS, increased mast cells have been demonstrated in the cecum, 29 terminal ileum, 30 and colon. 31 Although mast cells may be altered in all forms of IBS, patients with presumed diarrhea-predominant IBS are more easily evaluated, as more of these patients undergo endoscopy and biopsy compared with patients with other forms of presumed IBS. Herein, we describe a group of patients with clinically intractable chronic diarrhea and the sole abnormality of an increase in mast cells observed on immunohistochemical staining for MCT. Unlike urticaria pigmentosa or cutaneous mastocytoma, in which dense collections of mast cells are easily visualized on routine hematoxylin-eosin staining, the enterocolonic mucosa in mastocytic enterocolitis appears unremarkable. This is because the increased mast cells are diffusely scattered and are masked by the usual population of histiocytes, lymphocytes, and 366 Arch Pathol Lab Med Vol 130, March 2006 Mastocytic Enterocolitis Jakate et al
6 plasma cells within the lamina propria. Histologically, this increased mast cell population is of the mucosal reactive T mast cell phenotype because there is no simultaneous increase in the submucosal constitutive TC mast cell phenotype. This fortuitous mucosal diffuse distribution perfectly suits the type of tissue sample obtainable on random endoscopic biopsy specimens. Increased mast cells may produce symptoms through an increase in mast cell mediator release and local or paracrine signals to the enteric nervous system. 11 Although the cause of increased mast cells in chronic intractable diarrhea is unknown, mast cell mediator release is a typical response to adaptive and innate immunologic stimuli and to brain-gut interactions. Recognition of the released mast cell mediators by sensory neurons and interneurons of the enteric nervous system activates a programmed stereotypic defense reaction from the motor neurons (resulting in hypersecretion and power propulsion) and from the effector systems (causing diarrhea and abdominal pain). We propose the novel term mastocytic enterocolitis to describe the increased gut mucosal mast cells that are revealed by immunohistochemical demonstration of MCT in patients with chronic intractable diarrhea. This term is not meant to imply a specific diagnosis but rather to reflect the clinical setting of chronic intractable diarrhea with negative results on laboratory workup, unremarkable histologic appearances on routine staining, and more effective treatment availability compared with diarrhea-predominant IBS. Drugs affecting mast cell function are commonly prescribed and are widely used for conditions such as allergies and peptic ulcer but are not ordinarily prescribed for diarrhea. The primary objective of this study was to assess the concentration of mast cells in colonic or duodenal biopsy specimens from patients with chronic intractable diarrhea, and evaluation of the clinical and therapeutic aspects of the disease will require additional research. Physicians managing patients with chronic intractable diarrhea are encouraged to incorporate endoscopy, random colonic or duodenal mucosal sampling, and MCT immunostaining as part of their investigational protocol, and if increased mast cells are found, they should consider therapeutic options that alter mast cell mediator release and function. Because the mast cell population can demonstrate dynamic fluctuations, investigations are best performed during periods of active symptoms and before treatment. Although MCT, a neutral serine protease, is the most abundant mediator stored in mast cell granules, 32 serum tryptase level measurement may not be diagnostic in chronic intractable diarrhea because the effect of mast cell mediator release is immediately local or paracrine. Further studies in this area should elucidate clinical subclasses of disorders with distinct immunologic or central nervous system triggers for mucosal mast cell proliferation and mediator release. This work was funded by the Department of Pathology, Rush University Medical Center. References 1. Fine KD, Schiller LR. AGA technical review on the evaluation and management of chronic diarrhea. Gastroenterology. 1999;116: American Gastroenterological Association medical position statement: guidelines for the evaluation and management of chronic diarrhea. Gastroenterology. 1999;116: Schiller LR. Chronic diarrhea. Gastroenterology. 2004;127: Olden KW. Diagnosis of irritable bowel syndrome. Gastroenterology. 2002; 122: Stevens RL, Austen KF. Recent advances in the cellular and molecular biology of mast cells. Immunol Today. 1989;10: Kirshenbaum AS, Goff JP, Semere T, Foster B, Scott LM, Metcalfe DD. Demonstration that human mast cells arise from a progenitor cell population that is CD34, c-kit, and expresses aminopeptidase N (CD13). Blood. 1999;94: Irani AA, Schechter NM, Craig SS, DeBlois G, Schwartz LB. Two types of human mast cells that have distinct neutral protease compositions. Proc Natl Acad Sci U S A. 1986;83: Friend DS, Ghildyal N, Austen KF, Gurish MF, Matsumoto R, Stevens RL. Mast cells that reside at different locations in the jejunum of mice infected with Trichinella spiralis exhibit sequential changes in their granule ultrastructure and chymase phenotype. J Cell Biol. 1996;135: Marshall JS, Jawdat DM. Mast cells in innate immunity. J Allergy Clin Immunol. 2004;114: Santos J, Saperas E, Nogueiras C, et al. Release of mast cell mediators into the jejunum by cold pain stress in humans. Gastroenterology. 1998;114: Wood JD. Enteric neuroimmunophysiology and pathophysiology. Gastroenterology. 2004;127: Castells MC. Mastocytosis: classification, diagnosis, and clinical presentation. Allergy Asthma Proc. 2004;25: Miner PB Jr. The role of the mast cell in clinical gastrointestinal disease with special reference to systemic mastocytosis. J Invest Dermatol. 1991;96:40S 44S. 14. Cherner JA, Jensen RT, Dubois A, O Dorisio TM, Gardner JD, Metcalfe DD. Gastrointestinal dysfunction in systemic mastocytosis. Gastroenterology. 1988;95: Libel R, Biddle WL, Miner PB Jr. Evaluation of anorectal physiology in patients with increased mast cells. Dig Dis Sci. 1993;38: de Jonge WJ, The FO, van der Coelen D, et al. Mast cell degranulation during abdominal surgery initiates postoperative ileus in mice. Gastroenterology. 2004;127: Stoyanova II, Gulubova MV. Mast cells and inflammatory mediators in chronic ulcerative colitis. Acta Histochem. 2002;104: He SH. Key role of mast cells and their major secretory products in inflammatory bowel disease. World J Gastroenterol. 2004;10: Minocha A, Thomas C, Omar R. Lack of crucial role of mast cells in pathogenesis of experimental colitis in mice. Dig Dis Sci. 1995;40: Bischoff SC, Wedemeyer J, Herrmann A, et al. Histopathology. 1996;28: Raithel M, Winterkamp S, Pacurar A, Ulrich P, Hochberger J, Hahn EG. Release of mast cell tryptase from human colorectal mucosa in inflammatory bowel disease. Scand J Gastroenterol. 2001;36: Crowe SE, Luthra GK, Perdue MH. Mast cell mediated ion transport in intestine from patients with and without inflammatory bowel disease. Gut. 1997; 41: Schwab D, Raithel M, Hahn EG. Evidence for mast cell activation in collagenous colitis. Inflamm Res. 1998;47(suppl 1):S64 S Nishida Y, Murase K, Isomoto H, et al. Different distribution of mast cells and macrophages in colonic mucosa of patients with collagenous colitis and inflammatory bowel disease. Hepatogastroenterology. 2002;49: Wingren U, Hallert C, Norrby K, Enerback L. Histamine and mucosal mast cells in gluten enteropathy. Agents Actions. 1986;18: Horvath K, Simon K, Horn G, Bodanszky H. Mast cell degranulation after a single dose of gliandin in the jejunum of patients with celiac disease. Acta Paediatr Hung. 1986;27: Suranyi Y, Freier S, Faber J, Dollberg L. Intestinal mast cells in different stages of celiac disease. Isr J Med Sci. 1986;22: Drossman DA, Camilleri M, Mayer EA, Whitehead WE. AGA technical review on irritable bowel syndrome. Gastroenterology. 2002;123: O Sullivan M, Clayton N, Breslin NP, et al. Increased mast cells in the irritable bowel syndrome. Neurogastroenterol Motil. 2000;12: Weston AP, Biddle WL, Bhatia PS, Miner PB. Terminal ileal mucosal mast cells in irritable bowel syndrome. Dig Dis Sci. 1993;38: Chadwick VS, Chen W, Shu D, et al. Activation of the mucosal immune system in irritable bowel syndrome. Gastroenterology. 2002;122: Payne V, Kam PC. Mast cell tryptase: a review of its physiology and clinical significance. Anaesthesia. 2004;59: Arch Pathol Lab Med Vol 130, March 2006 Mastocytic Enterocolitis Jakate et al 367
How I Handle Mast Cells in GI Biopsies
 How I Handle Mast Cells in GI Biopsies Dora Lam-Himlin, MD Mayo Clinic Scottsdale, AZ Rodger C. Haggitt Gastrointestinal Pathology Society Forum United States and Canadian Academy of Pathologists Seattle,
How I Handle Mast Cells in GI Biopsies Dora Lam-Himlin, MD Mayo Clinic Scottsdale, AZ Rodger C. Haggitt Gastrointestinal Pathology Society Forum United States and Canadian Academy of Pathologists Seattle,
How I Handle Mast Cells in GI Biopsies
 How I Handle Mast Cells in GI Biopsies Dora Lam-Himlin, MD Rodger C. Haggitt Gastrointestinal Pathology Society Forum United States and Canadian Academy of Pathologists Seattle, Washington, March 12, 2016
How I Handle Mast Cells in GI Biopsies Dora Lam-Himlin, MD Rodger C. Haggitt Gastrointestinal Pathology Society Forum United States and Canadian Academy of Pathologists Seattle, Washington, March 12, 2016
TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON
 TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON Gurjeet Kaur 1, S Mahendra Raj 2 and Nyi Nyi Naing 3 Departments of 1 Pathology and 2 Medicine and the 3 Epidemiology and Medical Statistics
TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON Gurjeet Kaur 1, S Mahendra Raj 2 and Nyi Nyi Naing 3 Departments of 1 Pathology and 2 Medicine and the 3 Epidemiology and Medical Statistics
Mast cells have an important immunoregulatory function,
 Mast Cells in Gastrointestinal Disease David B. Ramsay, MD, Sindu Stephen, MD, Marie Borum, MD, EdD, MPH, Lysandra Voltaggio, MD, and David B. Doman, MD, FACP, FACG Drs. Ramsay and Stephen are Gastroenterology
Mast Cells in Gastrointestinal Disease David B. Ramsay, MD, Sindu Stephen, MD, Marie Borum, MD, EdD, MPH, Lysandra Voltaggio, MD, and David B. Doman, MD, FACP, FACG Drs. Ramsay and Stephen are Gastroenterology
Activation of the Mucosal Immune System in Irritable Bowel Syndrome
 GASTROENTEROLOGY 2002;122:1778 1783 Activation of the Mucosal Immune System in Irritable Bowel Syndrome VINTON S. CHADWICK,* WANGXUE CHEN,* DAIRU SHU,* BARBARA PAULUS,* PETER BETHWAITE, ANDY TIE, and IAN
GASTROENTEROLOGY 2002;122:1778 1783 Activation of the Mucosal Immune System in Irritable Bowel Syndrome VINTON S. CHADWICK,* WANGXUE CHEN,* DAIRU SHU,* BARBARA PAULUS,* PETER BETHWAITE, ANDY TIE, and IAN
Case History B Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment
 Case History B-1325945 Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment Case History B-1325945 Pathology Submucosa & Muscularis Endometriosis
Case History B-1325945 Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment Case History B-1325945 Pathology Submucosa & Muscularis Endometriosis
Are Gastrointestinal Mucosal Mast Cells Increased in Patients With Systemic Mastocytosis?
 Anatomic Pathology / GASTRODUODENAL MAST CELLS IN MASTOCYTOSIS Are Gastrointestinal Mucosal Mast Cells Increased in Patients With Systemic Mastocytosis? Sabine I. Siegert, MD, 1 Joachim Diebold, MD, PhD,
Anatomic Pathology / GASTRODUODENAL MAST CELLS IN MASTOCYTOSIS Are Gastrointestinal Mucosal Mast Cells Increased in Patients With Systemic Mastocytosis? Sabine I. Siegert, MD, 1 Joachim Diebold, MD, PhD,
These studies were made at a time when it was not. yet fully established that mast cells could react with
 Gut, 1975, 16, 861-866 Mast cells and immunoglobulin E in inflammatory bowel disease G. LLOYD1, F. H. Y. GREEN, H. FOX, V. MANI2, AND L. A. TURNBERG2 From the Department ofpathology, University of Manchester,
Gut, 1975, 16, 861-866 Mast cells and immunoglobulin E in inflammatory bowel disease G. LLOYD1, F. H. Y. GREEN, H. FOX, V. MANI2, AND L. A. TURNBERG2 From the Department ofpathology, University of Manchester,
The Role of Food in the Functional Gastrointestinal Disorders
 The Role of Food in the Functional Gastrointestinal Disorders H. Vahedi, MD. Gastroentrologist Associate professor of medicine DDRI 92.4.27 vahedi@ams.ac.ir Disorder Sub-category A. Oesophageal disorders
The Role of Food in the Functional Gastrointestinal Disorders H. Vahedi, MD. Gastroentrologist Associate professor of medicine DDRI 92.4.27 vahedi@ams.ac.ir Disorder Sub-category A. Oesophageal disorders
... SELECTED ABSTRACTS...
 ... SELECTED ABSTRACTS... The following abstracts, from medical journals containing literature on irritable bowel syndrome, were selected for their relevance to this supplement. A Technical Review for
... SELECTED ABSTRACTS... The following abstracts, from medical journals containing literature on irritable bowel syndrome, were selected for their relevance to this supplement. A Technical Review for
Lymphocytic Gastritis, Isolated Type Occurring in Family Members. A Case Report.
 Lymphocytic Gastritis, Isolated Type Occurring in Family Members. A Case Report. Alan Shienbaum, DO; AndriyPavlenko, MD; Jun Liu, MD, PhD; Janusz J Godyn, MD. Pathology Department, Kennedy University Hospitals,
Lymphocytic Gastritis, Isolated Type Occurring in Family Members. A Case Report. Alan Shienbaum, DO; AndriyPavlenko, MD; Jun Liu, MD, PhD; Janusz J Godyn, MD. Pathology Department, Kennedy University Hospitals,
Kids Like to Break the Rules: Gastrointestinal Pathology in Children
 Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
Gastroenterology. Certification Examination Blueprint. Purpose of the exam
 Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University
 CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
HDF Case CRYPTOSPORIDIOSE
 HDF Case 986949 CRYPTOSPORIDIOSE 45 yo male with severe diarrhea. Known HIV positive. Endoscopic biopsy of duodenum, the colon and ileum. EXUDATIVE CHANGES GRANULAR BASOPHILIC BODIES Colonic biopsy shows
HDF Case 986949 CRYPTOSPORIDIOSE 45 yo male with severe diarrhea. Known HIV positive. Endoscopic biopsy of duodenum, the colon and ileum. EXUDATIVE CHANGES GRANULAR BASOPHILIC BODIES Colonic biopsy shows
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST QUESTIONS. Ver. #
 SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding
 Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding Allergic Colitis is an inflammatory disorder of the colon which occurs mainly in preschool children. It is caused by an
Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding Allergic Colitis is an inflammatory disorder of the colon which occurs mainly in preschool children. It is caused by an
Fecal incontinence causes 196 epidemiology 8 treatment 196
 Subject Index Achalasia course 93 differential diagnosis 93 esophageal dysphagia 92 95 etiology 92, 93 treatment 93 95 work-up 93 Aminosalicylates, pharmacokinetics and aging effects 36 Antibiotics diarrhea
Subject Index Achalasia course 93 differential diagnosis 93 esophageal dysphagia 92 95 etiology 92, 93 treatment 93 95 work-up 93 Aminosalicylates, pharmacokinetics and aging effects 36 Antibiotics diarrhea
IBD. Crohn s. Outline. Ulcerative colitis versus Crohn s disease: is biopsy useful? UC vs. Crohn s? Is it easy? Biopsy settings 21/07/2017 IBD
 Outline Ulcerative colitis versus Crohn s disease: is biopsy useful? Roger Feakins Colorectal biopsies Ileal and upper GI biopsies Special situations New techniques Summary Inflammatory bowel disease (IBD)
Outline Ulcerative colitis versus Crohn s disease: is biopsy useful? Roger Feakins Colorectal biopsies Ileal and upper GI biopsies Special situations New techniques Summary Inflammatory bowel disease (IBD)
A Chronic or Recurring Pattern of Esophagitis Resembling Allergic Contact Dermatitis
 Anatomic Pathology / Lymphocytic Esophagitis Lymphocytic Esophagitis A Chronic or Recurring Pattern of Esophagitis Resembling Allergic Contact Dermatitis Julianne K. Purdy, MD, Henry D. Appelman, MD, Christopher
Anatomic Pathology / Lymphocytic Esophagitis Lymphocytic Esophagitis A Chronic or Recurring Pattern of Esophagitis Resembling Allergic Contact Dermatitis Julianne K. Purdy, MD, Henry D. Appelman, MD, Christopher
A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis
 doi: 10.2169/internalmedicine.1607-18 http://internmed.jp CASE REPORT A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis Rumiko Tsuboi,
doi: 10.2169/internalmedicine.1607-18 http://internmed.jp CASE REPORT A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis Rumiko Tsuboi,
A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue
 A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue UCSF Liver and Gastrointestinal Pathology Update Sept. 4, 2009 How to Go Wrong When Evaluating Small Bowel Biopsies, Based on
A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue UCSF Liver and Gastrointestinal Pathology Update Sept. 4, 2009 How to Go Wrong When Evaluating Small Bowel Biopsies, Based on
ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK. Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center
 ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center 1 ST ADMISSION - 2015 38 y/o female Abdominal pain, diarrhea - intermittent
ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center 1 ST ADMISSION - 2015 38 y/o female Abdominal pain, diarrhea - intermittent
Overview of digestion or, gut reactions - to food
 Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions - to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology e-mail: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions - to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology e-mail: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
Histological and immunological characteristics of colitis associated with anti-ctla 4 antibody therapy
 Histological and immunological characteristics of colitis associated with anti-ctla 4 antibody therapy M. Perdiki 2, G. Bamias 1, D. Pouloudi 2, H. Gogas 3, I. Delladetsima 2 1 Academic Dpt. of Gastroenterology,
Histological and immunological characteristics of colitis associated with anti-ctla 4 antibody therapy M. Perdiki 2, G. Bamias 1, D. Pouloudi 2, H. Gogas 3, I. Delladetsima 2 1 Academic Dpt. of Gastroenterology,
Overview of digestion or, gut reactions - to food
 1 Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology email: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
1 Key concepts in Digestion. Indigestion module Overview of digestion or, gut reactions to food Prof. Barry Campbell Gastroenterology Cellular & Molecular Physiology email: bjcampbl@liv.ac.uk http://pcwww.liv.ac.uk/~bjcampbl
Histopathology: gastritis and peptic ulceration
 Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
INTRODUCTION TO GASTROINTESTINAL FUNCTIONS
 1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint
 GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
하부위장관비종양성질환의 감별진단 주미인제의대일산백병원
 하부위장관비종양성질환의 감별진단 주미인제의대일산백병원 Solutions for diagnostic problems in Colitis : Please ask yourself five questions Normal or Inflamed? Acute or Chronic? IBD or Other chronic colitis? Ulcerative colitis or
하부위장관비종양성질환의 감별진단 주미인제의대일산백병원 Solutions for diagnostic problems in Colitis : Please ask yourself five questions Normal or Inflamed? Acute or Chronic? IBD or Other chronic colitis? Ulcerative colitis or
Small intestine. Small intestine
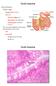 General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report
 Showa Univ J Med Sci 29 3, 315 319, September 2017 Case Report Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report Kodai TOMIOKA 1
Showa Univ J Med Sci 29 3, 315 319, September 2017 Case Report Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report Kodai TOMIOKA 1
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Role of Mast Cells in Appendicitis Dr. Jyoti Sharma 1*, Dr. Nitin Chaudhary 2*, Dr. Sunita
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Role of Mast Cells in Appendicitis Dr. Jyoti Sharma 1*, Dr. Nitin Chaudhary 2*, Dr. Sunita
children Crohn s disease in MR enterography for GI Complications Microscopy Characterization Primary sclerosing cholangitis Anorectal fistulae
 MR enterography for Crohn s disease in children BOAZ KARMAZYN, MD PEDIATRIC RADIOLOGY ASSOCIATE PROFESSOR Characterization Crohn disease Idiopathic chronic transmural IBD Increasing incidence Age 7/100,000
MR enterography for Crohn s disease in children BOAZ KARMAZYN, MD PEDIATRIC RADIOLOGY ASSOCIATE PROFESSOR Characterization Crohn disease Idiopathic chronic transmural IBD Increasing incidence Age 7/100,000
(b) Stomach s function 1. Dilution of food materials 2. Acidification of food (absorption of dietary Fe in small intestine) 3. Partial chemical digest
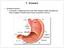 (1) General features a) Stomach is widened portion of gut-tube: between tubular and spherical; Note arranged of smooth muscle tissue in muscularis externa. 1 (b) Stomach s function 1. Dilution of food
(1) General features a) Stomach is widened portion of gut-tube: between tubular and spherical; Note arranged of smooth muscle tissue in muscularis externa. 1 (b) Stomach s function 1. Dilution of food
Irritable bowel syndrome (IBS) is a ... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome
 ... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome Based on a presentation by Marvin M. Schuster, MD Presentation Summary Approximately 20% of the general population has irritable bowel
... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome Based on a presentation by Marvin M. Schuster, MD Presentation Summary Approximately 20% of the general population has irritable bowel
DIGESTIVE TRACT ESOPHAGUS
 DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
HDF Case Whipple s disease
 HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
Supplemental Digital Content 1. Endoscopic and histolological findings in INR and FR study subjects
 Supplemental Digital Content 1. Endoscopic and histolological findings in INR and FR study subjects Patient Group Macroscopic examination Ileum Histology Colon/rectum Histology 1 INR Normal Acute and chronic
Supplemental Digital Content 1. Endoscopic and histolological findings in INR and FR study subjects Patient Group Macroscopic examination Ileum Histology Colon/rectum Histology 1 INR Normal Acute and chronic
Diarrhea may be: Acute (short-term, usually lasting several days), which is usually related to bacterial or viral infections.
 Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Frequency and Distribution of Microscopic Findings in Patients with Chronic Non-Bloody Diarrhea and Normal Colonoscopy
 IJMS Vol 33, No 2, June 2008 Original Article Frequency and Distribution of Microscopic Findings in Patients with Chronic Non-Bloody Diarrhea and Normal Colonoscopy H. Tabrizchie, M.J. Zahedie 1, M. Hayatbakhsh
IJMS Vol 33, No 2, June 2008 Original Article Frequency and Distribution of Microscopic Findings in Patients with Chronic Non-Bloody Diarrhea and Normal Colonoscopy H. Tabrizchie, M.J. Zahedie 1, M. Hayatbakhsh
Digestion: Small and Large Intestines Pathology
 Digestion: Small and Large Intestines Pathology Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one onone relationship with a qualified health
Digestion: Small and Large Intestines Pathology Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one onone relationship with a qualified health
Gastrooesophageal reflux disease. Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia
 Gastrooesophageal reflux disease Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia Reflux esophagitis (RE) GERD: a spectrum of clinical conditions and histologic alterations resulting
Gastrooesophageal reflux disease Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia Reflux esophagitis (RE) GERD: a spectrum of clinical conditions and histologic alterations resulting
What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you)
 What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you) Jonathan N. Glickman MD PhD Director, GI Pathology, Caris Diagnostics, Newton, MA Associate Professor of Pathology,
What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you) Jonathan N. Glickman MD PhD Director, GI Pathology, Caris Diagnostics, Newton, MA Associate Professor of Pathology,
HASPI Medical Anatomy & Physiology 15a Lab Activity
 HASPI Medical Anatomy & Physiology 15a Lab Activity Name(s): Period: Date: The Digestive System Digestion is an important process that involves breaking down food and drink into small molecules that can
HASPI Medical Anatomy & Physiology 15a Lab Activity Name(s): Period: Date: The Digestive System Digestion is an important process that involves breaking down food and drink into small molecules that can
Soft palate elevates, closing off the nasopharynx. Hard palate Tongue Bolus Epiglottis. Glottis Larynx moves up and forward.
 The Cephalic Phase Chemical and mechanical digestion begins in the mouth Saliva is an exocrine secretion Salivary secretion is under autonomic control Softens and lubricates food Chemical digestion: salivary
The Cephalic Phase Chemical and mechanical digestion begins in the mouth Saliva is an exocrine secretion Salivary secretion is under autonomic control Softens and lubricates food Chemical digestion: salivary
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
Allergic disorders of the gastrointestinal tract
 Allergic disorders of the gastrointestinal tract Christopher Justinich, MD Introduction The patient with presumed food hypersensitivity continues to present a challenge for the clinician. In certain instances,
Allergic disorders of the gastrointestinal tract Christopher Justinich, MD Introduction The patient with presumed food hypersensitivity continues to present a challenge for the clinician. In certain instances,
Case: The patient is a 73 year old woman with vague complaints of dyspepsia and abdominal pain. Upper endoscopy showed features of gastritis and a
 Case: The patient is a 73 year old woman with vague complaints of dyspepsia and abdominal pain. Upper endoscopy showed features of gastritis and a nodular lesion in the body of the stomach. The patient
Case: The patient is a 73 year old woman with vague complaints of dyspepsia and abdominal pain. Upper endoscopy showed features of gastritis and a nodular lesion in the body of the stomach. The patient
Imaging Evaluation of Polyps. CT Colonography: Sessile Adenoma. Polyps, DALMs & Megacolon Objectives
 Polyps, DALMs & Megacolon: Pathology and Imaging of the Colon and Rectum Angela D. Levy and Leslie H. Sobin Washington, DC Drs. Levy and Sobin have indicated that they have no relationships which, in the
Polyps, DALMs & Megacolon: Pathology and Imaging of the Colon and Rectum Angela D. Levy and Leslie H. Sobin Washington, DC Drs. Levy and Sobin have indicated that they have no relationships which, in the
Physiological processes in the GI tract:
 Gastrointestinal physiology for medical students General principal of gastrointestinal function Motility, nervous control and blood circulation Physiological processes in the GI tract: Motility Secretion
Gastrointestinal physiology for medical students General principal of gastrointestinal function Motility, nervous control and blood circulation Physiological processes in the GI tract: Motility Secretion
Ingestion Digestion- Absorption- Elimination
 DIGESTIVE SYSTEM 1 FUNCTIONS Organization GI tract==mouth anus Accessory organs Salivary glands, liver, pancreas, gallbladder Major Functions: Ingestion-mouth, teeth, tongue Digestion- chemical and mechanical
DIGESTIVE SYSTEM 1 FUNCTIONS Organization GI tract==mouth anus Accessory organs Salivary glands, liver, pancreas, gallbladder Major Functions: Ingestion-mouth, teeth, tongue Digestion- chemical and mechanical
INTERNATIONAL COURSE ON THE PATHOLOGY OF THE DIGESTIVE SYSTEM VICTOR BABES NATIONAL INSTITUTE OF PATHOLOGY BUCHAREST 7-8 BUCHAREST 2014
 INTERNATIONAL COURSE ON THE PATHOLOGY OF THE DIGESTIVE SYSTEM VICTOR BABES NATIONAL INSTITUTE OF PATHOLOGY BUCHAREST 7-8 BUCHAREST 2014 Endoscopic biopsy samples of naïve colitides patients: Role of basal
INTERNATIONAL COURSE ON THE PATHOLOGY OF THE DIGESTIVE SYSTEM VICTOR BABES NATIONAL INSTITUTE OF PATHOLOGY BUCHAREST 7-8 BUCHAREST 2014 Endoscopic biopsy samples of naïve colitides patients: Role of basal
SAM PROVIDER TOOLKIT
 THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
embedded tissue-sections has the advantage of permanence of the sections and is more suitable for
 Gut, 1980, 21, 941-947 Immunoglobulin containing cells in inflammatory bowel disease of the colon: a morphometric and immunohistochemical study P C M ROSEKRANS,* C J L M MEIJER, A M VAN DER WAL, C J CORNELISSE,
Gut, 1980, 21, 941-947 Immunoglobulin containing cells in inflammatory bowel disease of the colon: a morphometric and immunohistochemical study P C M ROSEKRANS,* C J L M MEIJER, A M VAN DER WAL, C J CORNELISSE,
Pitfalls in the Diagnosis of Inflammatory Bowel Disease
 Pitfalls in the Diagnosis of Inflammatory Bowel Disease Robert H Riddell MD Mt Sinai Hospital Toronto Prof of Lab. Medicine and Pathobiology University of Toronto Atypical gross / endoscopic distribution
Pitfalls in the Diagnosis of Inflammatory Bowel Disease Robert H Riddell MD Mt Sinai Hospital Toronto Prof of Lab. Medicine and Pathobiology University of Toronto Atypical gross / endoscopic distribution
Bloating, Flatulence, and
 A 45-Year-Old Man With Recurrent Abdominal Pain, Bloating, Flatulence, and Intermittent Loose Stools Anthony J. Lembo, MD Associate Professor of Medicine Harvard Medical School Director, GI Motility Laboratory
A 45-Year-Old Man With Recurrent Abdominal Pain, Bloating, Flatulence, and Intermittent Loose Stools Anthony J. Lembo, MD Associate Professor of Medicine Harvard Medical School Director, GI Motility Laboratory
Helicobacter and gastritis
 1 Helicobacter and gastritis Dr. Hala Al Daghistani Helicobacter pylori is a spiral-shaped gram-negative rod. H. pylori is associated with antral gastritis, duodenal (peptic) ulcer disease, gastric ulcers,
1 Helicobacter and gastritis Dr. Hala Al Daghistani Helicobacter pylori is a spiral-shaped gram-negative rod. H. pylori is associated with antral gastritis, duodenal (peptic) ulcer disease, gastric ulcers,
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
General Structure of Digestive Tract
 Dr. Nabil Khouri General Structure of Digestive Tract Common Characteristics: Hollow tube composed of a lumen whose diameter varies. Surrounded by a wall made up of 4 principal layers: Mucosa Epithelial
Dr. Nabil Khouri General Structure of Digestive Tract Common Characteristics: Hollow tube composed of a lumen whose diameter varies. Surrounded by a wall made up of 4 principal layers: Mucosa Epithelial
Functional Dyspepsia. Norbert Welkovics Heine van der Walt
 Norbert Welkovics Heine van der Walt Characteristics: Central abdomen Pain or discomfort Not associated with bowel movements No structural or biochemical abnormalty Definition Part of Gastroduodenal disorders
Norbert Welkovics Heine van der Walt Characteristics: Central abdomen Pain or discomfort Not associated with bowel movements No structural or biochemical abnormalty Definition Part of Gastroduodenal disorders
David Leff, DO. April 13, Disclosure. I have the following financial relationships to disclosure:
 David Leff, DO AOMA 94 th Annual Convention April 13, 2016 Disclosure I have the following financial relationships to disclosure: Speaker s Bureau: Allergan Labs, Takeda Pharmaceutical, Valeant Pharmaceutical
David Leff, DO AOMA 94 th Annual Convention April 13, 2016 Disclosure I have the following financial relationships to disclosure: Speaker s Bureau: Allergan Labs, Takeda Pharmaceutical, Valeant Pharmaceutical
What is your diagnosis? a. Lymphocytic colitis. b. Collagenous colitis. c. Common variable immunodeficiency (CVID) associated colitis
 Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
Food Choices and Alternative Techniques in Management of IBS: Fad Versus Evidence
 Food Choices and Alternative Techniques in Management of IBS: Fad Versus Evidence Maria Vazquez Roque, MD, MSc Assistant Professor Gastroenterology and Hepatology 2010 MFMER slide-1 Objectives Gluten-free
Food Choices and Alternative Techniques in Management of IBS: Fad Versus Evidence Maria Vazquez Roque, MD, MSc Assistant Professor Gastroenterology and Hepatology 2010 MFMER slide-1 Objectives Gluten-free
Collagenous gastritis and collagenous colitis: a report with sequential histological and ultrastructural findings
 Gut 1999;44:881 885 881 CASE REPORTS Wellcome Trust Research Laboratory, Christian Medical College and Hospital, Vellore 632004, India A B Pulimood B S Ramakrishna M M Mathan Correspondence to: Dr A B
Gut 1999;44:881 885 881 CASE REPORTS Wellcome Trust Research Laboratory, Christian Medical College and Hospital, Vellore 632004, India A B Pulimood B S Ramakrishna M M Mathan Correspondence to: Dr A B
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A
 HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
Gastroenterology Fellowship Program
 Gastroenterology Fellowship Program Outpatient Clinical Rotations I. Overview A. Three Year Continuity Clinic Experience All gastroenterology fellows will be required to have a ½ day continuity clinic
Gastroenterology Fellowship Program Outpatient Clinical Rotations I. Overview A. Three Year Continuity Clinic Experience All gastroenterology fellows will be required to have a ½ day continuity clinic
Department of Pathology and Laboratory Medicine, University of Florida College of Medicine-Jacksonville, Jacksonville, FL 32209, USA
 International Scholarly Research Network ISRN Dermatology Volume 2012, Article ID 759630, 5 pages doi:10.5402/2012/759630 Research Article A Comparative Analysis of Mast Cell Quantification in Five Common
International Scholarly Research Network ISRN Dermatology Volume 2012, Article ID 759630, 5 pages doi:10.5402/2012/759630 Research Article A Comparative Analysis of Mast Cell Quantification in Five Common
HISTOPATHOLOGICAL STUDY OF ENDOSCOPIC BIOPSIES OF STOMACH
 HISTOPATHOLOGICAL STUDY OF ENDOSCOPIC BIOPSIES OF STOMACH Pages with reference to book, From 177 To 179 Javed Iqbal Kazi, Syed Mahmood Alam ( Departments of Pathology, Jinnah Postgraduate Medical Centre,
HISTOPATHOLOGICAL STUDY OF ENDOSCOPIC BIOPSIES OF STOMACH Pages with reference to book, From 177 To 179 Javed Iqbal Kazi, Syed Mahmood Alam ( Departments of Pathology, Jinnah Postgraduate Medical Centre,
Chapter 12: Training in Pathology. DDSEP Chapter 13: Question 19
 DDSEP Chapter 13: Question 19 A 70 year-old male with a history of celiac disease diagnosed in his forties reports abdominal pain, dark stools, and 20-pound weight loss. He reports complete compliance
DDSEP Chapter 13: Question 19 A 70 year-old male with a history of celiac disease diagnosed in his forties reports abdominal pain, dark stools, and 20-pound weight loss. He reports complete compliance
RADIATION INDUCED SMALL BOWEL DISEASE. Dr Mnguni Supervisor: Dr Lohlun Radiation Oncology
 RADIATION INDUCED SMALL BOWEL DISEASE Dr Mnguni Supervisor: Dr Lohlun Radiation Oncology INTRODUCTION Radiation therapy is not regularly indicated in the treatment of small bowel disease. Reasons are complex
RADIATION INDUCED SMALL BOWEL DISEASE Dr Mnguni Supervisor: Dr Lohlun Radiation Oncology INTRODUCTION Radiation therapy is not regularly indicated in the treatment of small bowel disease. Reasons are complex
Unexpected Findings at Endoscopy
 The Endoscopic Incidentaloma: What to Tell Your Patient t with Unexpected Endoscopic Findings: Gastric Intestinal Metaplasia, Silent Ileitis, Carcinoid David Greenwald, MD Montefiore Medical Center Albert
The Endoscopic Incidentaloma: What to Tell Your Patient t with Unexpected Endoscopic Findings: Gastric Intestinal Metaplasia, Silent Ileitis, Carcinoid David Greenwald, MD Montefiore Medical Center Albert
For the past 40 years, it has been standard practice to obtain
 ORIGINAL ARTICLE: GASTROENTEROLOGY Good Agreement Between Endoscopic Findings and Biopsy Reports Supports Limited Tissue Sampling During Pediatric Colonoscopy Michael A. Manfredi, Hongyu Jiang, Lawrence
ORIGINAL ARTICLE: GASTROENTEROLOGY Good Agreement Between Endoscopic Findings and Biopsy Reports Supports Limited Tissue Sampling During Pediatric Colonoscopy Michael A. Manfredi, Hongyu Jiang, Lawrence
Small Bowel Cases. Introduction. Introduction, Continued 12/7/2011. Lesions Found on endoscopic biopsies Just Like Signing Out
 Small Bowel Cases Lesions Found on endoscopic biopsies Just Like Signing Out Introduction Small intestinal biopsies have a few special pitfalls, for example: Neuroendocrine tumors are readily mistaken
Small Bowel Cases Lesions Found on endoscopic biopsies Just Like Signing Out Introduction Small intestinal biopsies have a few special pitfalls, for example: Neuroendocrine tumors are readily mistaken
Eosinophilic GI Diseases: Shining a light on Eosinophils Beyond the Esophagus
 Food Allergy Track 4 Non-IgE-Dependent Food Sensitization Eosinophilic GI Diseases: Shining a light on Eosinophils Beyond the Esophagus Dan Atkins, MD Chief, Allergy Section Co-Director, Gastrointestinal
Food Allergy Track 4 Non-IgE-Dependent Food Sensitization Eosinophilic GI Diseases: Shining a light on Eosinophils Beyond the Esophagus Dan Atkins, MD Chief, Allergy Section Co-Director, Gastrointestinal
Surgical Management of IBD. Val Jefford Grand Rounds October 14, 2003
 Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
What do we need for diagnosis of IBD
 What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
MAST CELLS IN ORAL LICHEN PLANUS
 MAST CELLS IN ORAL LICHEN PLANUS Mahija Janardhanan* V.Ramesh. ** *Reader, Department of Oral Pathology & Microbiology, Amrita school of Dentistry, Kochi. **Professor & HOD, Department of Oral Pathology
MAST CELLS IN ORAL LICHEN PLANUS Mahija Janardhanan* V.Ramesh. ** *Reader, Department of Oral Pathology & Microbiology, Amrita school of Dentistry, Kochi. **Professor & HOD, Department of Oral Pathology
11/1/2017. Tetyana Mettler, MD Department of Laboratory Medicine and Pathology University of Minnesota. Cerilli & Greenson
 Tetyana Mettler, MD Department of Laboratory Medicine and Pathology University of Minnesota Acute infectious (self-limited) colitis Focal active colitis Pseudomembranous colitis Ischemic colitis Collagenous
Tetyana Mettler, MD Department of Laboratory Medicine and Pathology University of Minnesota Acute infectious (self-limited) colitis Focal active colitis Pseudomembranous colitis Ischemic colitis Collagenous
The Morphologic Profile of Inflammatory Bowel Disease and the Diagnostic Problem of Crohn s Disease versus TB Colitis A Case Series
 OPEN ACCESS CASE REPORT The Morphologic Profile of Inflammatory Bowel Disease and the Diagnostic Problem of Crohn s Disease versus TB Colitis A Case Series Maria Lourdes Tilbe, Francia Victoria De Los
OPEN ACCESS CASE REPORT The Morphologic Profile of Inflammatory Bowel Disease and the Diagnostic Problem of Crohn s Disease versus TB Colitis A Case Series Maria Lourdes Tilbe, Francia Victoria De Los
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT.
 PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
DIVISION OF GASTROENTEROLOGY
 DR. Lloyd Mayer T H E H E N R Y D. J A N O W I T Z DIVISION OF GASTROENTEROLOGY Mount Sinai is consistently ranked among the top five gastroenterology centers in the nation. The irresistible combination
DR. Lloyd Mayer T H E H E N R Y D. J A N O W I T Z DIVISION OF GASTROENTEROLOGY Mount Sinai is consistently ranked among the top five gastroenterology centers in the nation. The irresistible combination
Endoscopic mucosal biopsies are useful in distinguishing granulomatous colitis due to Crohn s disease from tuberculosis
 Gut 1999;45:537 541 537 Wellcome Research Unit, Department of Gastrointestinal Sciences, Christian Medical College and Hospital, Vellore 632 004, Tamilnadu, India A B Pulimood B S Ramakrishna G Kurian
Gut 1999;45:537 541 537 Wellcome Research Unit, Department of Gastrointestinal Sciences, Christian Medical College and Hospital, Vellore 632 004, Tamilnadu, India A B Pulimood B S Ramakrishna G Kurian
Original Article The Frequency of Lymphocytic and Reflux Esophagitis in Non-Human Primates
 www.ijcep.com/ijcep710008 Original Article The Frequency of Lymphocytic and Reflux Esophagitis in Non-Human Primates Carlos A. Rubio, Edward J. Dick Jr, Abiel Orrego and Gene B. Hubbard Southwest National
www.ijcep.com/ijcep710008 Original Article The Frequency of Lymphocytic and Reflux Esophagitis in Non-Human Primates Carlos A. Rubio, Edward J. Dick Jr, Abiel Orrego and Gene B. Hubbard Southwest National
Disclosure. Learning Objectives 4/25/2014. I have no disclosures
 Alka Goyal MD Division of Pediatric Gastroenterology Hepatology and Nutrition Children s Hospital of Pittsburgh of UPMC Disclosure I have no disclosures Learning Objectives Diagnosis of Eosinophilic Esophagitis
Alka Goyal MD Division of Pediatric Gastroenterology Hepatology and Nutrition Children s Hospital of Pittsburgh of UPMC Disclosure I have no disclosures Learning Objectives Diagnosis of Eosinophilic Esophagitis
The revised Porto criteria for diagnosing
 R E S E A R C H P A P E R Long-term Outcome of Inflammatory Bowel Disease Unclassified in Children SIBA PROSAD PAUL AND BHUPINDER KAUR SANDHU From Bristol Royal Hospital for Children, Upper Maudlin Street,
R E S E A R C H P A P E R Long-term Outcome of Inflammatory Bowel Disease Unclassified in Children SIBA PROSAD PAUL AND BHUPINDER KAUR SANDHU From Bristol Royal Hospital for Children, Upper Maudlin Street,
Treatment of Inflammatory Bowel Disease. Michael Weiss MD, FACG
 Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Alimentary Canal (I)
 Alimentary Canal (I) Esophagus and Stomach (Objectives) By the end of this lecture, the student should be able to discuss the microscopic structure in correlation with the function of the following organs:
Alimentary Canal (I) Esophagus and Stomach (Objectives) By the end of this lecture, the student should be able to discuss the microscopic structure in correlation with the function of the following organs:
Chronic immune colitis in rabbits
 Chronic immune colitis in rabbits A. S. MEE, J. E. McLAUGHLIN, H. J. F. HODGSON, AND D. P. JEWELL Gut, 1979, 20, 1-5 From the Academic Department of Medicine and Department of Histopathology, Royal Free
Chronic immune colitis in rabbits A. S. MEE, J. E. McLAUGHLIN, H. J. F. HODGSON, AND D. P. JEWELL Gut, 1979, 20, 1-5 From the Academic Department of Medicine and Department of Histopathology, Royal Free
Chapter 5: Common Digestive Problems from The Kansas State University Human Nutrition (HN 400) Flexbook by Brian Lindshield is in the public domain
 Chapter 5: Common Digestive Problems from The Kansas State University Human Nutrition (HN 400) Flexbook by Brian Lindshield is in the public domain in the United States. 5 Common Digestive Problems Before
Chapter 5: Common Digestive Problems from The Kansas State University Human Nutrition (HN 400) Flexbook by Brian Lindshield is in the public domain in the United States. 5 Common Digestive Problems Before
INNATE IMMUNITY Non-Specific Immune Response. Physiology Unit 3
 INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
Primary mucinous adenocarcinoma developing in an ileostomy stoma
 Gut, 1988, 29, 1607-1612 Primary mucinous adenocarcinoma developing in an ileostomy stoma P J SMART, S SASTRY, AND S WELLS From the Departments of Histopathology and Surgery, Bolton General Hospital, Fan
Gut, 1988, 29, 1607-1612 Primary mucinous adenocarcinoma developing in an ileostomy stoma P J SMART, S SASTRY, AND S WELLS From the Departments of Histopathology and Surgery, Bolton General Hospital, Fan
Faecal Calprotectin. Reliable Non-Invasive Discrimination Between Inflammatory Bowel Disease (IBD) & Irritable Bowel Syndrome (IBS)
 Faecal Calprotectin Reliable Non-Invasive Discrimination Between Inflammatory Bowel Disease (IBD) & Irritable Bowel Syndrome (IBS) Reliable, Non Invasive Identification of IBD vs IBS Available from Eurofins
Faecal Calprotectin Reliable Non-Invasive Discrimination Between Inflammatory Bowel Disease (IBD) & Irritable Bowel Syndrome (IBS) Reliable, Non Invasive Identification of IBD vs IBS Available from Eurofins
Refractory celiac disease (RCD) KASSEM BARADA LEBANESE SOCIETY OF GASTROENTEROLOGY NOVEMBER, 2014
 Refractory celiac disease (RCD) KASSEM BARADA LEBANESE SOCIETY OF GASTROENTEROLOGY NOVEMBER, 2014 Case scenario (1) A 49 year woman presents with intermittent watery diarrhea and bloating of two years
Refractory celiac disease (RCD) KASSEM BARADA LEBANESE SOCIETY OF GASTROENTEROLOGY NOVEMBER, 2014 Case scenario (1) A 49 year woman presents with intermittent watery diarrhea and bloating of two years
INVESTIGATIONS OF GASTROINTESTINAL DISEAS
 INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
MAST-CELLS are present in the digestive tract of all classes of vertebrates
 The Distribution of Mast-Cells in the Digestive Tract of Laboratory Animals: Its Bearings on the Problem of the Location of Histamine in Tissues By I. MOTA, A. G. FERRI, AND S. YONEDA 251 (From the Laboratory
The Distribution of Mast-Cells in the Digestive Tract of Laboratory Animals: Its Bearings on the Problem of the Location of Histamine in Tissues By I. MOTA, A. G. FERRI, AND S. YONEDA 251 (From the Laboratory
University of Buea. Faculty of Health Sciences. Programme in Medicine
 Faculty of Health Sciences University of Buea Wednesday, 28 th January 2009 Time: 8 00-10 00 Programme in Medicine MED 303 (Gastrointestinal Physiology) EXAMS (2008-2009) Identify the letter of the choice
Faculty of Health Sciences University of Buea Wednesday, 28 th January 2009 Time: 8 00-10 00 Programme in Medicine MED 303 (Gastrointestinal Physiology) EXAMS (2008-2009) Identify the letter of the choice
A Guide to Gastrointestinal Motility Disorders
 A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord André Smout Jan Tack A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord Gastroenterology and Hepatology Academic Medical
A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord André Smout Jan Tack A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord Gastroenterology and Hepatology Academic Medical
Eosinophilic Esophagitis (EoE)
 Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
