Imaging in the Evaluation of Children with Suspected Craniosynostosis
|
|
|
- Cori Murphy
- 6 years ago
- Views:
Transcription
1 4 Imaging in the Evaluation of Children with Suspected Craniosynostosis Daniel N. Vinocur and L. Santiago Medina I. What is the role of imaging in the diagnosis of craniosynostosis? II. What is the cost and cost-effectiveness of imaging in children with suspected craniosynostosis? III. Is imaging required when the clinical diagnosis has clearly been made? IV. How often and what intracranial abnormalities are seen in craniosynostosis? V. What is the role of imaging in the prenatal diagnosis of craniosynostosis? Issues Plain skull radiography demonstrates moderate to high sensitivity and specificity in craniosynostosis. Numerous publications support 3D-CT as the imaging modality with the best diagnostic performance, with reported sensitivities of %. CT also detects associated intracranial pathology. Higher diagnostic performance is obtained with plain films and CT if the studies are of good quality and interpreted by an experienced reviewer. Cranial sonography shows preliminary promise as a diagnostic test for craniosynostosis. The evidence is based on small cohorts; hence, larger series are needed before it is routinely used. Imaging strategies for children with suspected craniosynostosis should be based on their risk group. In healthy children with head deformity including posterior plagiocephaly, skull radiography is recommended. Syndromes such as Apert, Crouzon, and Pfeiffer nearly always have associated craniosynostosis and hence require 3D imaging for surgical planning. Key Points D.N. Vinocur ( ) Department of Radiology, Children s Hospital Boston. Harvard Medical School. Boston, Massachusetts daniel.vinocur@childrens.harvard.edu L.S. Medina et al. (eds.), Evidence-Based Imaging in Pediatrics, DOI / _4, Springer Science+Business Media, LLC
2 44 D.N. Vinocur and L.S. Medina Imaging is not necessary for diagnosis or preoperative planning in isolated craniosynostosis with unequivocal clinical findings. However, in countries with high medicolegal issues, imaging may still be required. Intracranial anomalies can be seen in some patients with craniosynostosis but the exact incidence is not well known. Small retrospective US and MRI studies demonstrate the feasibility of prenatal diagnosis of craniosynostosis. However, large prospective studies are still required to understand the prenatal role of imaging in craniosynostosis and their effect on postnatal outcome. Definition and Pathophysiology Craniosynostosis is the premature fusion of the skull sutures. The resulting asymmetric calvarial growth causes characteristic cranial deformities. The clinical outcome varies between minor cosmetic deformity to severe head growth restriction with mental retardation and cranial palsies (1). Craniosynostosis cases can be classified as non-syndromic (isolated) and syndromic. The exact etiology of this disorder is unknown; however, in several syndromic cases, genetic disorders have been documented (2 4). Epidemiology The overall prevalence of craniosynostosis in the general population ranges from 34 to 48 per 100,000 live births (5, 6). Higher incidence has been reported in the state of Colorado, USA (7), but the reason for this difference is unclear. In the general population, syndromic cases of synostosis are less common than non-syndromic cases (8 11). Sagittal followed by coronal synostosis are the most frequent type, accounting for 56 and 22% of the cases, respectively (6). In children with syndromic craniosynostotic disorders, such as Crouzon, Apert, and Pfeiffer syndromes, synostosis is almost universally present (8 11) Deformational plagiocephaly is defined as the asymmetric flattening of the head due to repeated pressure. Since 1992, there has been an exponential increase in the number of infants seen with deformational posterior plagiocephaly (positional molding) (12, 13). The most likely explanations are the 1992 American Academy of Pediatrics recommendation that infants sleep in the supine position to decrease the risk of sudden infant death syndrome (SIDS) and the increased awareness among pediatricians and other primary care providers of plagiocephaly (14 18). This specific entity usually presents some time after birth, progresses until 6 months of age, and remains stable thereafter (13). The skull deformity is generally considered to be only of cosmetic significance, and in the vast majority of cases it will respond to conservative measures such as changing sleep position or corrective helmets (3, 14). Overall Cost to Society We are not aware of studies documenting national costs of diagnosis or treatment of craniosynostosis or deformational plagiocephaly before or after the 1992 recommendations from the American Academy of Pediatrics. The cost of imaging studies and cost-effectiveness analysis are discussed in detail below. Goals The overall goal of neuroimaging for infants with suspected craniosynostosis is the early detection and characterization of this entity to enable appropriate treatment. Delayed diagnosis and treatment may lead to (1) cosmetic calvarial deformity which may be difficult to correct or may require more extensive cranioplasty and (2) potentially irreversible neurological impairment (18). Specific imaging goals include detailed characterization of the number of sutures, extent of suture involvement, and complexity of 3D calvarial deformity. Secondary goals include uncovering underlying brain anomalies associated with syndromic
3 Chapter 4 Imaging in the Evaluation of Children 45 synostotic disorders. More recently, there has been growing interest in the prenatal diagnosis of this disorder. Methodology Scientific article search was performed using the Medline/PubMed electronic database (National Library of Medicine, Bethesda, MD) and Ovid (Wolters Klumer, New York, New York) for original research publications discussing the diagnostic performance and effectiveness of imaging strategies in craniosynostosis. The search for neuroimagingrelated publications covered the period 1980 November The search strategy employed different combinations of the following terms: (1) Craniosynostosis, (2)Sensitivity, (3)Specificity, and (4) Diagnosis. This review was limited to human studies and the English language literature. The authors performed an initial review of the titles and abstracts of the identified articles followed by full text detailed review of relevant articles. Discussion of Issues I. What Is the Role of Imaging in the Diagnosis of Craniosynostosis? Summary of Evidence: Plain skull radiography demonstrates moderate to high sensitivity and specificity in craniosynostosis (limited to moderate evidence). Numerous publications show 3D-CT as the test with the best diagnostic performance, with reported sensitivities of % (limited to moderate evidence). Additionally CT allows the detection of associated intracranial pathology. Higher diagnostic performance is obtained when radiographs and CT are of good quality and interpreted by experienced reviewers (limited to moderate evidence). An imaging diagnostic algorithm is summarized in Fig The diagnostic algorithm is based on the clinical differentiation between syndromic and isolated craniosynostosis. In isolated (non-syndromic) cases, we advocate starting with plain radiographs. If the radiographs are negative, clinical follow-up would be indicated. In equivocal cases, or when the radiographs are positive, further characterization with 3D-CT is recommended. Syndromic cases are best evaluated directly with 3D-CT, with surgical consultation indicated in positive cases. Head sonography shows preliminary promise as a diagnostic test for craniosynostosis. The evidence is based on small cohorts; hence, larger series are needed before routine use in medical practice (limited evidence). Bone scintigraphy has fallen out of use, mainly due to its low accuracy, estimated at 66%. In addition, interpretation of images is complex and requires great expertise (limited evidence). Supporting Evidence Skull Radiographs Plain radiographs are classically considered the first-line imaging modality in craniosynostosis (19, 20). The standard series includes an anteroposterior view, Towne projection, and both lateral views. The low cost per study, low radiation, and universal availability have made it an attractive diagnostic choice (21). However, large prospective studies addressing the diagnostic accuracy of plain radiographs for the detection of craniosynostosis are lacking. In a retrospective study by Cerovac and colleagues, the overall diagnostic accuracy of plain radiography was estimated to be 91% (20) (limited evidence). Vannier and colleagues (22) reported wide ranges of diagnostic accuracies depending on the suture evaluated, ranging from 56% for the metopic suture to 88% for the sagittal suture. Overall sensitivity and specificity were reported between 57 and 80% and 54 and 100%, respectively (limited to moderate evidence). Pilgram et al. showed poor quality radiographic studies had significant decrease in sensitivity and specificity estimated at 60 and 78%, respectively (23) (Table 4.1) (limited to moderate evidence). In an older study from 1985 with 36 patients (18), plain radiography was reported to have an accuracy rate of 89% when compared to surgical inspection and pathologic examination (limited evidence). Computed Tomography (CT) The introduction of computed tomography revolutionized the imaging of craniosynostosis. This modality not only depicts the
4 46 D.N. Vinocur and L.S. Medina osseous pathology exquisitely but also allows for the detection of associated intracranial abnormalities, including hydrocephalus and brain developmental anomalies, such as agenesis of the corpus callosum (24). In addition, CT can identify alternative causes for asymmetric cranial morphology, such as brain hemiatrophy and chronic subdural collections (19). Numerous studies have been published in the literature demonstrating the high diagnostic performance of CT (Table 4.1). Agrawal et al. (25) reported an overall sensitivity of 100% for CT diagnosis of synostosis in 12 infants (limited evidence). A blinded study performed on a relatively small cohort (25 infants) reported that the sensitivity of CT with 3D surface-rendered reconstructions to be in the range of % (limited evidence) (26). An older study from 1985 using thicker axial slices and no 3D reconstructions (18) reported an overall accuracy for CT diagnosis of 94%. CT reviewer experience and image quality play an important role in the achieved diagnostic performance. Vannier et al. demonstrated sensitivity and specificity of 96.4 and 100%, respectively, for experienced CT reviewers (limited to moderate evidence) (27). They also revealed that less experienced CT reviewers had a significant drop in specificity of the test to 83% (limited to moderate evidence) (Table 4.1) (27). Pilgram et al. demonstrated that poor quality CT studies had a significant decrease in sensitivity and specificity estimated at 73 and 78%, respectively (limited to moderate evidence) (23). The use and risks of sedation or general anesthesia to perform CT examinations in children have been considered by several authors (20, 21). The overall risk of death from sedation is very low and has been estimated at 1 in one million (28 30). Furthermore, with the advent of spiral and multidetector CT, imaging time has been reduced drastically; hence, most children no longer need sedation for routine head CT. Imaging post-processing also has an impact on the diagnostic performance of CT. Vannier et al. (22) compared and concluded that 3D shaded rendering of the skull was superior to the combined information from 2D- CT and plain radiography (limited to moderate evidence). In a technical note, Medina (31) reported from a small group of 10 patients the advantages of 3D maximum intensity projections (MIP) in the comprehensive assessment of craniosynostosis (limited evidence). Ultrasound (US) Lately growing interest has been placed on ultrasonographic examination for craniosynostosis given its lack of ionizing radiation and need for sedation. However, sonography is operator dependent, requires special technologist training, and is not feasible in infants older than 13 months (32). Technically the examination consists in scanning the sutures with highfrequency transducers (typically 7.5 MHz), utilizing gel as contact medium. In 2006, Jan Regelsberger and colleagues from Hamburg, Germany, published a small series of 26 patients in which the diagnosis of craniosynostosis was established by ultrasound and confirmed later with CT. The study reported US sensitivity of 100% relative to CT (limited evidence) (32). Plagiocephaly is a common problem with an estimated prevalence of 20% at 8 months of age (33). There was a sharp increase in posterior plagiocephaly over the last 25 years (13), after the widespread adoption of the AAP infant positioning recommendations to decrease the incidence of SIDS (34). A few articles addressed the use of ultrasound for this specific clinical concern (i.e., unilateral occipital craniosynostosis versus deformational molding) (32, 35). Sze and colleagues (35) published a prospective study of 41 subjects (including controls) to understand the role of US in characterizing posterior plagiocephaly (limited to moderate evidence). Their study correlated ultrasonographic findings with CT results. The overall sensitivity for US diagnosis was 100% and the specificity was 89% (limited to moderate evidence). Bone Scintigraphy Older literature emphasized the role of Tc99mbased bone scintigraphy for the diagnosis of craniosynostosis. The literature estimates the overall accuracy of scintigraphy to be approximately 66% (18), which renders it essentially valueless for current practice use. In addition, interpretation of this modality requires expert knowledge regarding the different normal phases of activity along calvarial bone maturation (36).
5 Chapter 4 Imaging in the Evaluation of Children 47 II. What Is the Cost and Cost-Effectiveness of Imaging in Children with Suspected Craniosynostosis? Summary of Evidence: Selection of children with suspected craniosynostosis based on their risk group and use of the most appropriate evaluation strategy could maximize clinical and economic outcomes for these patients. A comprehensive cost-effectiveness analysis comparing different imaging strategies in the diagnosis of craniosynostosis was performed by Medina et al. (21) (moderate to strong evidence). In healthy children with head deformity, including posterior plagiocephaly, the skull radiographic strategy had the most reasonable cost per quality-adjusted life year (QALY) gained. Three-dimensional CT was more effective but had a high cost per QALY gained. In children with syndromic craniofacial disorders (high risk), 3D-CT was the most effective strategy and had a reasonable cost per QALY gained. Figure 4.1 summarizes the best imaging approach in suspected craniosynostosis. Supporting Evidence: Medina et al. (21) performed formal cost-effectiveness analysis (CEA) on diagnostic strategies in children with suspected craniosynostosis (moderate to strong evidence). Three risk groups were analyzed on the basis of the prevalence (pretest probability) of disease: low (completely healthy children; prevalence, 34/100,000), intermediate (healthy children with head deformity; prevalence, 1/115), and high risk (children with syndromic craniofacial disorders (i.e., Crouzon ssyndrome or Apert s syndrome); prevalence, 9 10/10). The analysis was based on cost (not charge) expressed in 1999 U.S. dollars. Cost data for the study are shown in Table 4.2. In the low-risk group, the radiographic plus 3D-CT strategies resulted in a cost per qualityadjusted life year (QALY) gained of more than $560,000. In the intermediate risk group, the radiographic strategy resulted in a cost per QALY gained of $54,600. Three-dimensional CT was more effective than the two other strategiesbutatahighercost,withacostperqaly gained of $374,200. In the high-risk group, 3D- CT (without initial radiographs) was the most effective strategy with a cost per QALY gained of $33,800. Less experienced radiologists and poor-quality studies increased the evaluation cost per QALY gained for all of the risk groups because of decreased effectiveness. The authors concluded that radiologic screening of completely healthy children (low risk for synostosis) is not warranted because of the high cost per QALY gained for any imaging. In healthy children with head deformity (intermediate risk), the initial workup with radiographs is the most cost-effective choice. Threedimensional CT is more effective but more expensive. In children with syndromic craniofacial disorders (high risk), 3D-CT was the most cost-effective imaging approach. III. Is Imaging Required When the Clinical Diagnosis Has Clearly Been Made? Summary of Evidence: Isolated craniosynostosis with unequivocal clinical findings probably does not warrant preoperative imaging for diagnostic correlation and preoperative planning (moderate evidence), though imaging may be important for medicolegal considerations. Supporting Evidence: In the setting of growing concern regarding radiation exposure (37), Agrawal et al. (25) studied the usefulness of preoperative imaging of clinically diagnosed isolated sagittal craniosynostosis. In their retrospective study of 114 cases, they correlated clinical diagnosis and pre-surgical imaging (plain radiography and CT) with surgical and pathologic findings and found a correlation of 100% for clinical diagnosis (moderate evidence). Both imaging studies also had a 100% correlation with surgical pathology results. In this preliminary work, they concluded that clinically typical isolated sagittal craniosynostosis does not warrant imaging. Similarly, Cerovac and colleagues from the Great Ormond Street Hospital for Children in UK (20) published a retrospective series of 109 clinically diagnosed cases of isolated craniosynostosis (non-syndromic) and correlated them with pre-surgical imaging (CT and radiography) and surgical findings. They also demonstrated 100% confirmation of clinical and CT diagnosis (moderate evidence). Furthermore,
6 48 D.N. Vinocur and L.S. Medina they reported no additional treatment benefit from CT in screening for intracranial abnormalities or change in surgical planning. IV. How Often and What Intracranial Abnormalities Are Seen in Craniosynostosis? Summary of Evidence: There are few studies addressing this question and those published have been small and without well-defined cohorts. Therefore, intracranial anomalies can be seen in some patients with craniosynostosis but the exact incidence is not well known. Supporting Evidence: The exact incidence of associated intracranial anomalies in craniosynostosis is not well known. In a study from 1982, Goldstein and Kidd (38) reported on a heterogeneous group of patients with a variety of syndromic and isolated craniosynostosis (limited evidence). In this group, 5 out of 13 patients (38%) demonstrated an associated intracranial abnormality, most commonly hydrocephalus. However, only 1 of the 5 patients with an intracranial abnormality led to change in therapy (insertion of a shunt for hydrocephalus). On the other hand, Hayward et al. (39) published a selective study of 30 patients with severe craniosynostosis and complex clinical syndromes who had MR imaging. The authors found more associated pathologies with the following prevalence: hindbrain herniation 19/30; syringomyelia 1/30; hydrocephalus 12/30; and non-specified anomalies of cerebral white matter 4/30. The association of intracranial anomalies with syndromic craniosynostosis has been well established. Crouzon syndrome is associated with chronic tonsillar herniation (Chiari I malformation) in approximately 70% of cases and syringomyelia in 20% of cases. Other associations include hydrocephalus and absent corpus callosum (40). Apert syndrome has been associated with megalencephaly and stable ventriculomegaly. Interestingly, progressive hydrocephalus appears to be relatively uncommon (20%) (41). Additional associations include agenesis of the corpus callosum/septum pellucidum, encephalocele (42), limbic and gyral malformations, and heterotopic gray matter among others (24, 41). Finally, Pfeiffer syndrome demonstrates considerable heterogeneity, with subgroups of patients with mild phenotypes without mental retardation (43) to more severe phenotypes associated with mental retardation, hydrocephalus, and Arnold Chiari II malformation (40). V. What Is the Role of Imaging in the Prenatal Diagnosis of Craniosynostosis? Summary of Evidence: Small retrospective US and MRI studies in the prenatal diagnosis of craniosynostosis have been published (limited evidence). However, large prospective studies are still required to understand the prenatal role of imaging in craniosynostosis and their effect on parental counseling, surgical planning, and postnatal outcome of these fetuses. Supporting Evidence: Recently, there has been increasing interest in the antenatal diagnosis of craniosynostosis. Early detection could potentially allow for different interventions, including elective termination of pregnancy in severe syndromic synostosis, elective cesarean section, early postnatal surgery, and perhaps fetal surgery (44). Ultrasound (US) In the largest series found in the literature, Delahaye and colleagues (4) performed a retrospective study in 40 fetuses with high risk of craniosynostosis. The inclusion criteria included (1) patients with positive family history of craniosynostosis and (2) those with an abnormal screening obstetrical ultrasound. Abnormal screening ultrasounds were based on altered head measurements and indices. Reported sensitivity and specificity was 100 and 97%, respectively, for this retrospective study (4) (limited evidence). Miller and colleagues used screening ultrasound (non-targeted) in the second and third trimesters to compile a heterogeneous retrospective cohort of 21 fetuses with craniosynostosis. In this study, the authors correlated postnatal diagnosis with indirect signs of craniosynostosis on screening ultrasound
7 Chapter 4 Imaging in the Evaluation of Children 49 examinations (cranial geometry and indices). Their study demonstrated poor correlation between routine parameters of a non-dedicated prenatal ultrasound in the proper identification of synostosis (limited evidence). Using cranial geometry and indices, only 15 of the 26 (estimated sensitivity 58%) cases were diagnostic of postnatally documented craniosynostosis (limited evidence) (44). MRI Fjortoft and colleagues reviewed the imaging in a small group of 15 fetuses that demonstrated abnormal screening US during the second and third trimesters and were subsequently referred to fetal MRI imaging with the specific suspicion of craniosynostosis. In this cohort, MRI demonstrated 100% sensitivity and specificity when correlated to follow-up postnatal medical records (limited evidence) (45). No prospective MR imaging studies were found. Take Home Figures and Tables Figure 4.1 is an algorithm with a suggested diagnostic approach for suspected craniosynostosis. Tables 4.1 and 4.2 discuss the performance of imaging tests for suspected craniosynostosis and the costs of imaging tests, respectively. Child with skull asymmetry Non-syndromic Syndromic Plain radiographs + or equivocal 3-D CT Figure 4.1. Suggested diagnostic approach algorithm. Summary of the best imaging approach according to suspected syndromic versus non-syndromic skull deformity. Clinical Follow-up + Surgical Consultation Table 4.1. Diagnostic performance of imaging tests Diagnostic test Sensitivity (%) Range References Radiographs (good quality) Sensitivity (%) (22) Specificity (%) (22) Radiographs (poor quality) Sensitivity (%) (23) Specificity (%) (23) CT a,b (experienced reviewer) Sensitivity (%) (26) Specificity (%) (26) CT a,b (less experienced reviewers) Sensitivity (%) (26) Specificity (%) (26) CT (poor quality) Sensitivity (%) (23) Specificity (%) (23) a CT with 3D reconstructions. Good quality. Modified with permission of the ARRS from Medina et al. (21)
8 50 D.N. Vinocur and L.S. Medina Table 4.2. Cost of imaging tests Variable Direct cost ($) Total cost a ($) Medicaid b ($) Skull radiography D-CT Sedation c CT plus sedation a Medical center cost estimates include direct (fixed and variable) and indirect (overhead) costs. b Medicaid reimbursement (Ohio). This cost was used for the case-based study. c Sedation by nonanesthesiologist is not reimbursed by Medicaid. Modified with permission of the ARRS from Medina et al. (21) Imaging Case Studies Figures 4.2, 4.3, and 4.4 illustrate representative cases of non-syndromic and syndromic craniosynostosis. In addition, a case of the commonly seen non-synostotic plagiocephaly is presented. Figure 4.2. Case 1. Another case of isolated sagittal craniosynostosis. Superior view from a 3D-CT reconstruction demonstrating fusion of the sagittal suture (star) with associated dolichocephaly.
9 Chapter 4 Imaging in the Evaluation of Children 51 Figure 4.3. Case 2. Non-synostotic occipital plagiocephaly (positional molding or deformational plagiocephaly). A: Superior projection from a 3D-CT reconstruction demonstrating the skull deformity. B: Posterior projection from a 3D-CT reconstruction demonstrating patent lamboid sutures (stars). CT Spiral or MDCT with surface rendering and maximum intensity projections. Axial acquisition with the following suggested parameters. 120 kvp 200 ma Thickness 2.5 mm Parenchymal reconstruction: 5 mm with soft tissue algorithm 3D Images: mm high-resolution bone reconstruction using 3D volume rendering and high-definition maximum intensity projection. Future Research Figure 4.4. Case 3. Apert syndrome. Anterior oblique projection from a 3D-CT reconstruction demonstrating coronal (star) and squamosal (ˆ) sutures synostosis. Also note the facial hypoplasia. Suggested Imaging Protocol for Craniosynostosis Plain Radiographs Excellent quality plain films including anteroposterior, Towne, and both lateral radiographs. Large studies are needed to evaluate the role of ultrasound in the diagnosis of craniosynostosis, particularly in the differentiation between this entity and deformational plagiocephaly. Further research is required to establish the role of MRI and US in the antenatal diagnosis of craniosynostosis. Better-defined cohorts should be studied to determine the incidence of intracranial abnormalities based on the type of synostotic disorder.
10 52 D.N. Vinocur and L.S. Medina References 1. Fernbach SK. Pediatr Radiol 1998 Sep; 28(9): Blaumeiser B, Loquet P, Wuyts W, Nothen MM. Prenat Diagn 2004 Aug; 24(8): Van Vlimmeren LA, Helders PJ, van Adrichem LN, Engelbert RH. Euro J Pediatr 2004 Apr; 163(4 5): Delahaye S, Bernard JP, Renier D, Ville Y. Ultrasound Obstet Gynecol 2003 Apr; 21(4): Lajeunie E, Le Merrer M, Bonaïti-Pellie C, Marchac D, Renier D. Am J Med Genet Feb 13; 55(4): Cohen MM Jr. In Cohen MM Jr (ed.): Craniosynostosis: Diagnosis, Evaluation and Management, 2nd ed. New York: Oxford University Press, 2000; Alderman BW, Fernbach SK, Greene C, Mangione EJ, Ferguson SW. Arch Pediatr Adolesc Med 1997 Feb; 151(2): Cohen MM Jr. In Cohen MM Jr (ed.): Craniosynostosis: Diagnosis, Evaluation, and Management, 2nd ed. New York: Oxford University Press, 2000; Cohen MM Jr. In: Cohen MM Jr (ed.): Craniosynostosis: Diagnosis Evaluation, and Management, 2nd ed. New York: Oxford University Press, 2000; Cohen MM Jr, MacLean RE In Cohen MM Jr (ed.): Craniosynostosis: Diagnosis, Evaluation, and Management, 2nd ed. New York: Oxford University Press, 2000; Blank CE. Ann Hum Genet 1960;24: Mulliken JB, Vander Woude DL, Hansen M, LaBrie RA, Scott RM. Plast Reconstr Surg 1999;103: Jones BM, Hayward R, Evans R, Britto J. BMJ 1997 Sep 20; 315(7110): Argenta LC, David LR, Wilson JA, Bell WO. J Craniofac Surg 1996;7: Kane AA, Mitchell LE, Craven KP, Marsh JF. Pediatrics 1996;89: Turk AE, McCarthy JG, Thorn CHM, Wissoff JH. J Craniofac Surg 1996;7: Willinger M, Hoffman JH, Hartford RB. Pediatrics 1994;93: Gellad FE, Haney PJ, Sun JC, Robinson WL, Rao KC et al. Pediatr Radiol 1985; 15(5): Abrahams JJ, Eklund JA. Clin Plast Surg 1995 Jul; 22(3): Cerovac S, Neil-Dwyer JG, Rich P, Jones BM, Hayward RD. Br J Neurosurg 2002 Aug; 16(4): Medina LS, Richardson RR, Crone K. Am J Roentgenol 2002 Jul; 179(1): Vannier MW, Hildebolt CF, Marsh JL, Pilgram TK, McAlister WH, Shackelford GD et al. Radiology 1989 Dec; 173(3): Pilgram TK, Vannier MW, Hildebolt CF et al. Radiology 1989;173: de León GA, de León G, Grover WD, Zaeri N, Alburger PD. Ach Neurol 1987; 44(9): Agrawal D, Steinbok P, Cochrane DD. Child s Nerv Syst 2006 Apr; 22(4): Vannier MW, Pilgram TK, Marsh JL, Kraemer BB, Rayne SC, Gado MH et al. Am J Neuroradiol 1994 Nov; 15(10): Vannier MW, Pilgram TK, Marsh JL et al. AJNR 1994;15: Cote CJ. Pediatr Clin North Am 1994;41: Holzman RS. Pediatr Clin North Am 1994;41: dedombal F. J R Coll Physicians Lond 1975;9: Medina LS. Am J Neuroradiol 2000 Nov Dec; 21(10): Regelsberger J, Delling G, Helmke K, Tsokos M, Kammler G, Kranzlein H et al. J Craniofac Surg 2006 Jul; 17(4): ; discussion Hutchison BL, Hutchison LA, Thompson JM, Mitchell EA. Pediatrics 2004 Oct;114(4): AAP Task Force on Infant Positioning and SIDS Positioning and SIDS Pediatrics. Pediatrics 1992 Jun; 89: Sze RW, Parisi MT, Sidhu M, Paladin AM, Ngo AV, Seidel KD et al. Pediatr Radiol 2003 Sep; 33(9): Fernbach SK, Feinstein KA. Neurosurg Clin N Am 1991 Jul; 2(3): Slovis TL. Pediatrics 2003; 112: Goldstein SJ, Kidd RC. Comput Radiol 1982 Nov Dec; 6(6): Hayward R, Harkness W, Kendall B, Jones B. Scand J Plast Reconstr Surg Hand Surg 1992; 26(3): Lachman R. Taybi and Lachman s Radiology of Syndromes, Metabolic Disorders, and Skeletal Dysplasias, 5th ed. St. Louis: Mosby, Cohen MM Jr, Kreiborg S. Am J Med Genet 1990; 35: Gershoni-Baruch R, Nachlieli T, Guilburd JN. Child s Nerv Syst 1991; 7: Teebi AS, Kennedy S, Chun K, Ray PN. Am J Med Genet 2002; 107: Miller C, Losken HW, Towbin R, Bowen A, Mooney MP, Towbin A et al. Cleft Palate- Craniofac J 2002; Jan 39(1): Fjortoft MI, Sevely A, Boetto S, Kessler S, Sarramon MF et al. Neuroradiology 2007 Jun; 49(6):
11
Interesting Case Series. The Danger of Posterior Plagiocephaly
 Interesting Case Series The Danger of Posterior Plagiocephaly Susan Orra, BA, a,b Kashyap Komarraju Tadisina, BS, a Bahar Bassiri Gharb, MD, PhD, a Antonio Rampazzo, MD, PhD, a Gaby Doumit, MD, a and Francis
Interesting Case Series The Danger of Posterior Plagiocephaly Susan Orra, BA, a,b Kashyap Komarraju Tadisina, BS, a Bahar Bassiri Gharb, MD, PhD, a Antonio Rampazzo, MD, PhD, a Gaby Doumit, MD, a and Francis
High-frequency ultrasound confirmation of positional plagiocephaly
 J Neurosurg (5 Suppl Pediatrics) 105:413 417, 2006 High-frequency ultrasound confirmation of positional plagiocephaly JAN REGELSBERGER, M.D., GÜNTER DELLING, M.D., MICHAEL TSOKOS, M.D., KNUTH HELMKE, M.D.,
J Neurosurg (5 Suppl Pediatrics) 105:413 417, 2006 High-frequency ultrasound confirmation of positional plagiocephaly JAN REGELSBERGER, M.D., GÜNTER DELLING, M.D., MICHAEL TSOKOS, M.D., KNUTH HELMKE, M.D.,
MEDICAL POLICY MEDICAL POLICY DETAILS POLICY STATEMENT POLICY GUIDELINES. Page: 1 of 5. Medical Policy Title CRANIAL ORTHOTICS Policy Number 1.01.
 Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title CRANIAL ORTHOTICS Policy Number 1.01.32 Category Equipment/Supplies Effective Date 10/18/01 Revised Date 06/27/02, 07/24/03, 06/24/04,
Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title CRANIAL ORTHOTICS Policy Number 1.01.32 Category Equipment/Supplies Effective Date 10/18/01 Revised Date 06/27/02, 07/24/03, 06/24/04,
Research Article Human Anatomy Case Report Bathrocephaly: a case report of a head shape associated with a persistent mendosal suture
 IJAE Vol. 119, n. 3: 263-267, 2014 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research Article Human Anatomy Case Report Bathrocephaly: a case report of a head shape associated with a persistent mendosal
IJAE Vol. 119, n. 3: 263-267, 2014 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research Article Human Anatomy Case Report Bathrocephaly: a case report of a head shape associated with a persistent mendosal
Occipital flattening in the infant skull
 Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Nonsurgical, nonorthotic treatment of occipital plagiocephaly: what is the natural history of the misshapen neonatal head?
 Nonsurgical, nonorthotic treatment of occipital plagiocephaly: what is the natural history of the misshapen neonatal head? S. David Moss, M.D. Phoenix Children's Hospital, Phoenix, Arizona Plagiocephaly
Nonsurgical, nonorthotic treatment of occipital plagiocephaly: what is the natural history of the misshapen neonatal head? S. David Moss, M.D. Phoenix Children's Hospital, Phoenix, Arizona Plagiocephaly
Prevention Diagnosis
 Prevention and Management of Positional Skull Deformities in Infants John Persing, MD, Hector James, MD, Jack Swanson, MD, John Kattwinkel, MD, Committee on Practice and Ambulatory Medicine, Section on
Prevention and Management of Positional Skull Deformities in Infants John Persing, MD, Hector James, MD, Jack Swanson, MD, John Kattwinkel, MD, Committee on Practice and Ambulatory Medicine, Section on
International Journal of Current Research and Academic Review ISSN: Volume 3 Number 1 (January-2015) pp
 International Journal of Current Research and Academic Review ISSN: 47 Volume Number (January) pp. 66 www.ijcrar.com Clinical Profile of Patients with Craniosynostosis: A Descriptive Study Nagaraj V. Gadwal*
International Journal of Current Research and Academic Review ISSN: 47 Volume Number (January) pp. 66 www.ijcrar.com Clinical Profile of Patients with Craniosynostosis: A Descriptive Study Nagaraj V. Gadwal*
Department of Neurosurgery. Differentiating Craniosynostosis from Positional Plagiocephaly
 Department of Neurosurgery Differentiating Craniosynostosis from Positional Plagiocephaly The number of infants with head shape deformities has risen over the past several years, likely due to increased
Department of Neurosurgery Differentiating Craniosynostosis from Positional Plagiocephaly The number of infants with head shape deformities has risen over the past several years, likely due to increased
CNS Embryology 5th Menstrual Week (Dorsal View)
 Imaging of the Fetal Brain; Normal & Abnormal Alfred Abuhamad, M.D. Eastern Virginia Medical School CNS Embryology 5th Menstrual Week (Dorsal View) Day 20 from fertilization Neural plate formed in ectoderm
Imaging of the Fetal Brain; Normal & Abnormal Alfred Abuhamad, M.D. Eastern Virginia Medical School CNS Embryology 5th Menstrual Week (Dorsal View) Day 20 from fertilization Neural plate formed in ectoderm
4.1 Classification of Craniosynostosis: Therapeutical implications.
 ISPN course 23 rd Nov, 2015 Cranial & Craniofacial disorders 4.1 Classification of Craniosynostosis: Therapeutical implications. Kazuaki Shimoji, Masakazu Miyajima and Hajime Arai Department of Neurosurgery,
ISPN course 23 rd Nov, 2015 Cranial & Craniofacial disorders 4.1 Classification of Craniosynostosis: Therapeutical implications. Kazuaki Shimoji, Masakazu Miyajima and Hajime Arai Department of Neurosurgery,
MP Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses. Related Policies None
 Medical Policy BCBSA Ref. Policy: 1.01.11 Last Review: 03/29/2018 Effective Date: 03/29/2018 Section: Durable Medical Equipment Related Policies None DISCLAIMER Our medical policies are designed for informational
Medical Policy BCBSA Ref. Policy: 1.01.11 Last Review: 03/29/2018 Effective Date: 03/29/2018 Section: Durable Medical Equipment Related Policies None DISCLAIMER Our medical policies are designed for informational
Policy #: 008 Latest Review Date: May 2007 Category: Durable Medical Equipment
 Name of Policy: Dynamic Orthotic Cranioplasty (DOC) Policy #: 008 Latest Review Date: May 2007 Category: Durable Medical Equipment Policy Grade: D Background: As a general rule, benefits are payable under
Name of Policy: Dynamic Orthotic Cranioplasty (DOC) Policy #: 008 Latest Review Date: May 2007 Category: Durable Medical Equipment Policy Grade: D Background: As a general rule, benefits are payable under
Children with Metopic Ridge
 DOI: 10.5137/1019-5149.JTN.16886-15.2 Received: 28.12.2015 / Accepted: 04.03.2016 Published Online: 25.04.2016 Original Investigation Children with Metopic Ridge Tufan HICDONMEZ Dr. Lutfi Kirdar Education
DOI: 10.5137/1019-5149.JTN.16886-15.2 Received: 28.12.2015 / Accepted: 04.03.2016 Published Online: 25.04.2016 Original Investigation Children with Metopic Ridge Tufan HICDONMEZ Dr. Lutfi Kirdar Education
Craniosynostosis - making the head fit the hat
 Craniosynostosis - making the head fit the hat Poster No.: R-0173 Congress: 2014 CSM Type: Scientific Exhibit Authors: S. Constantine, B. Clark; NORTH ADELAIDE/AU Keywords: Head and neck, Bones, Pediatric,
Craniosynostosis - making the head fit the hat Poster No.: R-0173 Congress: 2014 CSM Type: Scientific Exhibit Authors: S. Constantine, B. Clark; NORTH ADELAIDE/AU Keywords: Head and neck, Bones, Pediatric,
Spectrum of Cranio-facial anomalies during 2 Ultrasound. trimester on
 Spectrum of Cranio-facial anomalies during 2 Ultrasound nd trimester on Poster No.: C-0378 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. Dave, S. Solanki; Ahmedabad/IN Keywords: Obstetrics (Pregnancy
Spectrum of Cranio-facial anomalies during 2 Ultrasound nd trimester on Poster No.: C-0378 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. Dave, S. Solanki; Ahmedabad/IN Keywords: Obstetrics (Pregnancy
Han-Sung Kwon M.D. Department of Obstetrics and Gynecology Konkuk University School of Medicine Seoul, Korea
 Han-Sung Kwon M.D. Department of Obstetrics and Gynecology Konkuk University School of Medicine Seoul, Korea Embryologic features of the developing hindbrain Embryologic features of the developing hindbrain
Han-Sung Kwon M.D. Department of Obstetrics and Gynecology Konkuk University School of Medicine Seoul, Korea Embryologic features of the developing hindbrain Embryologic features of the developing hindbrain
Length of synostosis and segmented intracranial volume correlate with age in patients with non-syndromic sagittal synostosis
 https://helda.helsinki.fi Length of synostosis and segmented intracranial volume correlate with age in patients with non-syndromic sagittal synostosis Heliövaara, Arja 2018-03 Heliövaara, A, Leikola, J,
https://helda.helsinki.fi Length of synostosis and segmented intracranial volume correlate with age in patients with non-syndromic sagittal synostosis Heliövaara, Arja 2018-03 Heliövaara, A, Leikola, J,
Craniosynostosis. Diagnosis and Treatment
 Craniosynostosis Diagnosis and Treatment 2015 For more information about the Weill Cornell Craniofacial Program ABOUT The Weill Cornell Craniofacial Program takes a multidisciplinary approach to treating
Craniosynostosis Diagnosis and Treatment 2015 For more information about the Weill Cornell Craniofacial Program ABOUT The Weill Cornell Craniofacial Program takes a multidisciplinary approach to treating
A New Ultrasound Method for Assessment of Head Shape Change in Infants With Plagiocephaly Jin Kyung Kim, MD, Dong Rak Kwon, MD, Gi-Young Park, MD
 Original Article Ann Rehabil Med 2014;38(4):541-547 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.4.541 Annals of Rehabilitation Medicine A New Ultrasound Method for Assessment
Original Article Ann Rehabil Med 2014;38(4):541-547 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.4.541 Annals of Rehabilitation Medicine A New Ultrasound Method for Assessment
Determination of the Chronological Age of Skull Base Suture Closure Using Computed Tomography
 Journal of Basic & Applied Sciences, 2012, 8, 247-252 247 Determination of the Chronological Age of Skull Base Suture Closure Using Computed Tomography Sattam S. Lingawi* Associate Professor of Radiology,
Journal of Basic & Applied Sciences, 2012, 8, 247-252 247 Determination of the Chronological Age of Skull Base Suture Closure Using Computed Tomography Sattam S. Lingawi* Associate Professor of Radiology,
Craniosynostosis and Plagiocephaly
 Craniosynostosis and Plagiocephaly Andrew Jea MD MHA FAAP Professor and Chief Section of Pediatric Neurosurgery Riley Hospital for Children Department of Neurosurgery Indiana University School of Medicine
Craniosynostosis and Plagiocephaly Andrew Jea MD MHA FAAP Professor and Chief Section of Pediatric Neurosurgery Riley Hospital for Children Department of Neurosurgery Indiana University School of Medicine
Effective Treatment of Craniosynostosis and Deformational Plagiocephaly Improves with Early Diagnosis:
 Effective Treatment of Craniosynostosis and Deformational Plagiocephaly Improves with Early Diagnosis: Watchful Waiting May Not Be the Best Option for Evaluating Abnormal Head Shape in Infants April, 2016
Effective Treatment of Craniosynostosis and Deformational Plagiocephaly Improves with Early Diagnosis: Watchful Waiting May Not Be the Best Option for Evaluating Abnormal Head Shape in Infants April, 2016
CURRICULUM VITAE. SPR in Neurosurgery North Thames Rotation Scheme. 1. Royal Free Hospital RFH ( ; 18 months ) Specialist Registrar
 CURRICULUM VITAE Name Title Present Position Address : -Jesus Lafuente : -MD, FRCSEd, PhD : -CONSULTANT NEUROSURGEON : -HOSPÌTAL DEL MAR PASEO MARITIMO 23 BARCELONA 08003 E-mail : jlbspine@gmail.com Phone
CURRICULUM VITAE Name Title Present Position Address : -Jesus Lafuente : -MD, FRCSEd, PhD : -CONSULTANT NEUROSURGEON : -HOSPÌTAL DEL MAR PASEO MARITIMO 23 BARCELONA 08003 E-mail : jlbspine@gmail.com Phone
Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy
 Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy File name: Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses File code:
Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy File name: Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses File code:
Neurodevelopment in Children with Single-Suture Craniosynostosis and Plagiocephaly without Synostosis
 Neurodevelopment in Children with Single-Suture Craniosynostosis and Plagiocephaly without Synostosis Jayesh Panchal, M.B.B.S., F.R.C.S., M.B.A., Hamid Amirsheybani, M.D., Robin Gurwitch, Ph.D., Vicki
Neurodevelopment in Children with Single-Suture Craniosynostosis and Plagiocephaly without Synostosis Jayesh Panchal, M.B.B.S., F.R.C.S., M.B.A., Hamid Amirsheybani, M.D., Robin Gurwitch, Ph.D., Vicki
De f o r m at i o n a l or positional plagiocephaly is the
 J Neurosurg Pediatrics 5:000 000, 5:368 374, 2010 Comparison of perceptions and treatment practices between neurosurgeons and plastic surgeons for infants with deformational plagiocephaly Clinical article
J Neurosurg Pediatrics 5:000 000, 5:368 374, 2010 Comparison of perceptions and treatment practices between neurosurgeons and plastic surgeons for infants with deformational plagiocephaly Clinical article
CASE REPORT Pan-Suture Synostosis After Posterior Vault Distraction
 CASE REPORT Pan-Suture Synostosis After Posterior Vault Distraction Katrina F. Chu, BA, a Stephen R. Sullivan, MD, MPH, a,b and Helena O. Taylor, MD, PhD a,b a Warren Alpert Medical School of Brown University;
CASE REPORT Pan-Suture Synostosis After Posterior Vault Distraction Katrina F. Chu, BA, a Stephen R. Sullivan, MD, MPH, a,b and Helena O. Taylor, MD, PhD a,b a Warren Alpert Medical School of Brown University;
Authors: Shitel Patel, Rami R Hallac, Pang-yun Chou, Min-Jeong Cho, Neil Stewart, Ana Nava, James Seaward, Alex Kane, Christopher Derderian
 Authors: Shitel Patel, Rami R Hallac, Pang-yun Chou, Min-Jeong Cho, Neil Stewart, Ana Nava, James Seaward, Alex Kane, Christopher Derderian Title: Location and Time of Maximal Head Shape Change in Strip
Authors: Shitel Patel, Rami R Hallac, Pang-yun Chou, Min-Jeong Cho, Neil Stewart, Ana Nava, James Seaward, Alex Kane, Christopher Derderian Title: Location and Time of Maximal Head Shape Change in Strip
Deformational Plagiocephaly
 Deformational Plagiocephaly A GUIDE TO DIAGNOSIS AND TREATMENT Introduction In 1992, the American Academy of Pediatrics began to recommend supine sleeping for infants to reduce the incidence of Sudden
Deformational Plagiocephaly A GUIDE TO DIAGNOSIS AND TREATMENT Introduction In 1992, the American Academy of Pediatrics began to recommend supine sleeping for infants to reduce the incidence of Sudden
Clinical Guide. Pediatric Cranial Deformities using STAR Cranial Remolding Orthoses
 Clinical Guide Orthotic Management of Pediatric Cranial Deformities using STAR Cranial Remolding Orthoses STARband Clinical Guide By Dulcey Lima, CO, OTR/L Introduction The number of skull deformities
Clinical Guide Orthotic Management of Pediatric Cranial Deformities using STAR Cranial Remolding Orthoses STARband Clinical Guide By Dulcey Lima, CO, OTR/L Introduction The number of skull deformities
Subject: Brain CT. Original Effective Date: 11/7/2017. Policy Number: MCR: 600. Revision Date(s): Review Date:
 Subject: Brain CT Policy Number: MCR: 600 Revision Date(s): MHW Original Effective Date: 11/7/2017 Review Date: DISCLAIMER This Molina Clinical Review (MCR) is intended to facilitate the Utilization Management
Subject: Brain CT Policy Number: MCR: 600 Revision Date(s): MHW Original Effective Date: 11/7/2017 Review Date: DISCLAIMER This Molina Clinical Review (MCR) is intended to facilitate the Utilization Management
What is Craniosynostosis?
 What is Craniosynostosis? Craniosynostosis is defined as the premature closure of the cranial sutures (what some people refer to as soft spots). This results in restricted and abnormal growth of the head.
What is Craniosynostosis? Craniosynostosis is defined as the premature closure of the cranial sutures (what some people refer to as soft spots). This results in restricted and abnormal growth of the head.
Imaging the Premature Brain- New Knowledge
 Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
JBI Database of Systematic Reviews & Implementation Reports 2013;11(11) 54-63
 Risk factors for developing recurrent raised intracranial pressure post cranial vault remodelling in nonsyndromic craniosynostosis in children: a systematic review protocol Xenia Doorenbosch MBBS 1,2 Jared
Risk factors for developing recurrent raised intracranial pressure post cranial vault remodelling in nonsyndromic craniosynostosis in children: a systematic review protocol Xenia Doorenbosch MBBS 1,2 Jared
Multidisciplinary care of craniosynostosis
 Journal of Multidisciplinary Healthcare open access to scientific and medical research Open Access Full Text Article Multidisciplinary care of craniosynostosis Review edward P Buchanan 1 Yunfeng Xue 1
Journal of Multidisciplinary Healthcare open access to scientific and medical research Open Access Full Text Article Multidisciplinary care of craniosynostosis Review edward P Buchanan 1 Yunfeng Xue 1
Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy
 Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy File name: Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses File code:
Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy File name: Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses File code:
Supplementary Online Content
 Supplementary Online Content Honein MA, Dawson AL, Petersen E, et al; US Zika Pregnancy Registry Collaboration. Birth Defects Among Fetuses and Infants of US Women With Laboratory Evidence of Possible
Supplementary Online Content Honein MA, Dawson AL, Petersen E, et al; US Zika Pregnancy Registry Collaboration. Birth Defects Among Fetuses and Infants of US Women With Laboratory Evidence of Possible
Motion of bones and volume changes in the neurocranium after craniectomy in Crouzon's disease
 J Neurosurg 50:494-498, 1979 Motion of bones and volume changes in the neurocranium after craniectomy in Crouzon's disease A roentgen stereometrie study BODIL RUNE, D.D.S., GORAN SELVIK, M.D., SVEN KREmORG,
J Neurosurg 50:494-498, 1979 Motion of bones and volume changes in the neurocranium after craniectomy in Crouzon's disease A roentgen stereometrie study BODIL RUNE, D.D.S., GORAN SELVIK, M.D., SVEN KREmORG,
Evaluation of Staggered Osteotomy in Surgical Treatment of Trigonocephaly
 Evaluation of Staggered Osteotomy... Hassanpour et al. 28 Original 28 Evaluation of Staggered Osteotomy in Surgical Treatment of Trigonocephaly Seyed Esmail Hassanpour¹ Mohammad Reza Hadi Sichani 2 Mohammadreza
Evaluation of Staggered Osteotomy... Hassanpour et al. 28 Original 28 Evaluation of Staggered Osteotomy in Surgical Treatment of Trigonocephaly Seyed Esmail Hassanpour¹ Mohammad Reza Hadi Sichani 2 Mohammadreza
Practical CT and MRI Anthony J. Fischetti, DVM, MS, DACVR Department Head of Diagnostic Imaging The Animal Medical Center, New York OBJECTIVE:
 Practical CT and MRI Anthony J. Fischetti, DVM, MS, DACVR Department Head of Diagnostic Imaging The Animal Medical Center, New York OBJECTIVE: This lecture describes the most common indications for referred
Practical CT and MRI Anthony J. Fischetti, DVM, MS, DACVR Department Head of Diagnostic Imaging The Animal Medical Center, New York OBJECTIVE: This lecture describes the most common indications for referred
Surgery for craniosynostosis has evolved rapidly
 Surgical Treatment of Craniosynostosis: Outcome Analysis of 250 Consecutive Patients Gerald M. Sloan, MD*; Karin C. Wells, MD ; Corey Raffel, MD, PhD ; and J. Gordon McComb, MD ABSTRACT. Objective. Surgery
Surgical Treatment of Craniosynostosis: Outcome Analysis of 250 Consecutive Patients Gerald M. Sloan, MD*; Karin C. Wells, MD ; Corey Raffel, MD, PhD ; and J. Gordon McComb, MD ABSTRACT. Objective. Surgery
Unilateral fusion of the coronal suture is the most. Isolated frontosphenoidal synostosis: a rare cause of synostotic frontal plagiocephaly
 J Neurosurg Pediatrics 13:553 558, 2014 AANS, 2014 Isolated frontosphenoidal synostosis: a rare cause of synostotic frontal plagiocephaly Clinical aicle Tina M. Sauerhammer, M.D., Albe K. Oh, M.D., Michael
J Neurosurg Pediatrics 13:553 558, 2014 AANS, 2014 Isolated frontosphenoidal synostosis: a rare cause of synostotic frontal plagiocephaly Clinical aicle Tina M. Sauerhammer, M.D., Albe K. Oh, M.D., Michael
T HERE is an unusual and interesting variety of craniosynostosis in
 SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
intracranial anomalies
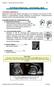 Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Emerging Surgical Technologies: Open vs. Endoscopic Craniosynostosis Repair
 Emerging Surgical Technologies: Open vs. Endoscopic Craniosynostosis Repair Petra M. Meier, MD, DEAA Senior Associate of the Department of Anesthesiology, Perioperative and Pain Medicine, Boston Children
Emerging Surgical Technologies: Open vs. Endoscopic Craniosynostosis Repair Petra M. Meier, MD, DEAA Senior Associate of the Department of Anesthesiology, Perioperative and Pain Medicine, Boston Children
EVALUATION OF CHRONIC HEADACHE BY COMPUTED TOMOGRAPHY: A RETROSPECTIVE STUDY
 EVALUATION OF CHRONIC HEADACHE BY COMPUTED TOMOGRAPHY: A RETROSPECTIVE STUDY Abstract: Anish Subedee Objective: To find out the proportion of intracranial abnormalities in patients with chronic headache
EVALUATION OF CHRONIC HEADACHE BY COMPUTED TOMOGRAPHY: A RETROSPECTIVE STUDY Abstract: Anish Subedee Objective: To find out the proportion of intracranial abnormalities in patients with chronic headache
Cranial Base Changes Following. Surgical Treatment of Craniosynostosis. JEFFREY L. MARSH, M.D. MicHaAeL W. VaAnniEer, M.D.
 Cranial Base Changes Following Surgical Treatment of Craniosynostosis JEFFREY L. MARSH, M.D. MicHaAeL W. VaAnniEer, M.D. Three-dimensional osseous surface images from CT scans have been used to study the
Cranial Base Changes Following Surgical Treatment of Craniosynostosis JEFFREY L. MARSH, M.D. MicHaAeL W. VaAnniEer, M.D. Three-dimensional osseous surface images from CT scans have been used to study the
Original Research THE USE OF REFORMATTED CONE BEAM CT IMAGES IN ASSESSING MID-FACE TRAUMA, WITH A FOCUS ON THE ORBITAL FLOOR FRACTURES
 DOI: 10.15386/cjmed-601 Original Research THE USE OF REFORMATTED CONE BEAM CT IMAGES IN ASSESSING MID-FACE TRAUMA, WITH A FOCUS ON THE ORBITAL FLOOR FRACTURES RALUCA ROMAN 1, MIHAELA HEDEȘIU 1, FLOAREA
DOI: 10.15386/cjmed-601 Original Research THE USE OF REFORMATTED CONE BEAM CT IMAGES IN ASSESSING MID-FACE TRAUMA, WITH A FOCUS ON THE ORBITAL FLOOR FRACTURES RALUCA ROMAN 1, MIHAELA HEDEȘIU 1, FLOAREA
(i) Family 1. The male proband (1.III-1) from European descent was referred at
 1 Supplementary Note Clinical descriptions of families (i) Family 1. The male proband (1.III-1) from European descent was referred at age 14 because of scoliosis. He had normal development. Physical evaluation
1 Supplementary Note Clinical descriptions of families (i) Family 1. The male proband (1.III-1) from European descent was referred at age 14 because of scoliosis. He had normal development. Physical evaluation
Optimized phase contrast MRV technique outperforms timeof-flight in the diagnosis of cerebral venous thrombosis
 Optimized phase contrast MRV technique outperforms timeof-flight in the diagnosis of cerebral venous thrombosis Poster No.: C-3377 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Scientific Exhibit
Optimized phase contrast MRV technique outperforms timeof-flight in the diagnosis of cerebral venous thrombosis Poster No.: C-3377 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Scientific Exhibit
Case MDCT 3D reconstructed features of posterior urethral valve
 Case 12688 MDCT 3D reconstructed features of posterior urethral valve Hidayatullah Hamidi Third year Resident of Radiology French medical institute for children Radiology Department; Kabul, Afghanistan;
Case 12688 MDCT 3D reconstructed features of posterior urethral valve Hidayatullah Hamidi Third year Resident of Radiology French medical institute for children Radiology Department; Kabul, Afghanistan;
Sagittal craniosynostosis is the most common of the. Combined metopic and sagittal craniosynostosis: is it worse than sagittal synostosis alone?
 Neurosurg Focus 31 (2):E2, 2011 Combined metopic and sagittal craniosynostosis: is it worse than sagittal synostosis alone? Jordan S. Terner, B.A., 1 Roberto Travieso, B.A., 1 Su-shin Lee, M.D., 2 Antonio
Neurosurg Focus 31 (2):E2, 2011 Combined metopic and sagittal craniosynostosis: is it worse than sagittal synostosis alone? Jordan S. Terner, B.A., 1 Roberto Travieso, B.A., 1 Su-shin Lee, M.D., 2 Antonio
Neurodevelopmental Implications of Deformational Plagiocephaly
 0196-206X/05/2605-0379 Developmental and Behavioral Pediatrics Vol. 26, No. 5, October 2005 Copyright # 2005 by Lippincott Williams & Wilkins, Inc. Printed in U.S.A. Review Article Neurodevelopmental Implications
0196-206X/05/2605-0379 Developmental and Behavioral Pediatrics Vol. 26, No. 5, October 2005 Copyright # 2005 by Lippincott Williams & Wilkins, Inc. Printed in U.S.A. Review Article Neurodevelopmental Implications
Cleidocranial Dysplasia
 BRIEF REPORTS Cleidocranial Dysplasia Anita Sharma Rohtash Yadav Kuldip Ahlawat Cleidocranial dysplasia (CCD), is characterized by short stature, typical facial features and variable degree of pan-skeletal
BRIEF REPORTS Cleidocranial Dysplasia Anita Sharma Rohtash Yadav Kuldip Ahlawat Cleidocranial dysplasia (CCD), is characterized by short stature, typical facial features and variable degree of pan-skeletal
Reassessment of Sphenoid Dysplasia Associated with Neurofibromatosis Type 1
 AJNR Am J Neuroradiol 23:644 648, April 2002 Reassessment of Sphenoid Dysplasia Associated with Neurofibromatosis Type 1 Claude Jacquemin, Thomas M. Bosley, Don Liu, Helena Svedberg, and Amal Buhaliqa
AJNR Am J Neuroradiol 23:644 648, April 2002 Reassessment of Sphenoid Dysplasia Associated with Neurofibromatosis Type 1 Claude Jacquemin, Thomas M. Bosley, Don Liu, Helena Svedberg, and Amal Buhaliqa
REVIEW ARTICLE Egypt. J. Hum. Genet. Vol. 8, No. 2, Nov Dandy-Walker Malformation
 REVIEW ARTICLE Egypt. J. Hum. Genet. Vol. 8, No. 2, Nov. 2007 Medical Genetics Center, Ain Shams University INTRODUCTION Dandy-Walker malformation is a rare congenital malformation and involves the cerebellum
REVIEW ARTICLE Egypt. J. Hum. Genet. Vol. 8, No. 2, Nov. 2007 Medical Genetics Center, Ain Shams University INTRODUCTION Dandy-Walker malformation is a rare congenital malformation and involves the cerebellum
Cleft-Craniofacial Center
 Cleft-Craniofacial Center A Pioneering T eam 2 Welcome to the Cleft-Craniofacial Center at Children s Hospital of Pittsburgh The Cleft-Craniofacial Center at Children s Hospital of Pittsburgh has been
Cleft-Craniofacial Center A Pioneering T eam 2 Welcome to the Cleft-Craniofacial Center at Children s Hospital of Pittsburgh The Cleft-Craniofacial Center at Children s Hospital of Pittsburgh has been
ECMUS The Safety Committee of EFSUMB : Tutorial
 Neonatal cranial ultrasound Safety Aspects (2013) Prepared for ECMUS by B.J. van der Knoop, M.D. 1, J.I.P. de Vries, M.D., PhD 1, I.A. Zonnenberg, M.D. 2, J.I.M.L. Verbeke, M.D. 3 R.J. Vermeulen, M.D.,
Neonatal cranial ultrasound Safety Aspects (2013) Prepared for ECMUS by B.J. van der Knoop, M.D. 1, J.I.P. de Vries, M.D., PhD 1, I.A. Zonnenberg, M.D. 2, J.I.M.L. Verbeke, M.D. 3 R.J. Vermeulen, M.D.,
Characteristics, head shape measurements and developmental delay in 287 consecutive infants attending a plagiocephaly clinic
 Acta Pædiatrica ISSN 0803 5253 REGULAR ARTICLE Characteristics, head shape measurements and developmental delay in 287 consecutive infants attending a plagiocephaly clinic BL Hutchison (bl.hutchison@auckland.ac.nz),
Acta Pædiatrica ISSN 0803 5253 REGULAR ARTICLE Characteristics, head shape measurements and developmental delay in 287 consecutive infants attending a plagiocephaly clinic BL Hutchison (bl.hutchison@auckland.ac.nz),
High spatial resolution reveals excellent detail in pediatric neuro imaging
 Publication for the Philips MRI Community Issue 46 2012/2 High spatial resolution reveals excellent detail in pediatric neuro imaging Achieva 3.0T with 32-channel SENSE Head coil has become the system
Publication for the Philips MRI Community Issue 46 2012/2 High spatial resolution reveals excellent detail in pediatric neuro imaging Achieva 3.0T with 32-channel SENSE Head coil has become the system
Skull base growth in children with Chiari malformation Type I
 See the corresponding editorial in this issue, pp 187. J Neurosurg (3 Suppl Pediatrics) 107:188 192, 2007 Skull base growth in children with Chiari malformation Type I SPYROS SGOUROS, M.D., F.R.C.S.(SN),
See the corresponding editorial in this issue, pp 187. J Neurosurg (3 Suppl Pediatrics) 107:188 192, 2007 Skull base growth in children with Chiari malformation Type I SPYROS SGOUROS, M.D., F.R.C.S.(SN),
The prevalence of deformational plagiocephaly PEDIATRIC/CRANIOFACIAL
 PEDIATRIC/CRANIOFACIAL Effectiveness of Conservative Therapy and Helmet Therapy for Positional Cranial Deformation Jordan P. Steinberg, M.D., Ph.D. Roshni Rawlani, B.A. Laura S. Humphries, M.D. Vinay Rawlani,
PEDIATRIC/CRANIOFACIAL Effectiveness of Conservative Therapy and Helmet Therapy for Positional Cranial Deformation Jordan P. Steinberg, M.D., Ph.D. Roshni Rawlani, B.A. Laura S. Humphries, M.D. Vinay Rawlani,
abstract ARTICLE BACKGROUND: Radiography, typically the first-line imaging study for diagnosis of
 Cranial Ultrasound as a First- Line Imaging Examination for Craniosynostosis Katya Rozovsky, MD, a,b Kristin Udjus, MD, a Nagwa Wilson, MD, PhD, a Nicholas James Barrowman, PhD, c Natalia Simanovsky, MD,
Cranial Ultrasound as a First- Line Imaging Examination for Craniosynostosis Katya Rozovsky, MD, a,b Kristin Udjus, MD, a Nagwa Wilson, MD, PhD, a Nicholas James Barrowman, PhD, c Natalia Simanovsky, MD,
Occipital plagiocephaly
 ritish Journal of Plastic Surgery (2000), 53, 367 377 9 2000 The ritish ssociation of Plastic Surgeons doi:10.1054/bjps.2000.3329 RITISH JOURNL OF [ ~ ] PLSTIC SURGERY Occipital plagiocephaly D. J. David
ritish Journal of Plastic Surgery (2000), 53, 367 377 9 2000 The ritish ssociation of Plastic Surgeons doi:10.1054/bjps.2000.3329 RITISH JOURNL OF [ ~ ] PLSTIC SURGERY Occipital plagiocephaly D. J. David
Corporate Medical Policy
 Corporate Medical Policy Invasive Prenatal (Fetal) Diagnostic Testing File Name: Origination: Last CAP Review: Next CAP Review: Last Review: invasive_prenatal_(fetal)_diagnostic_testing 12/2014 3/2018
Corporate Medical Policy Invasive Prenatal (Fetal) Diagnostic Testing File Name: Origination: Last CAP Review: Next CAP Review: Last Review: invasive_prenatal_(fetal)_diagnostic_testing 12/2014 3/2018
Fetal Medicine. Case Presentations. Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital. October 2003
 Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
Advances in Emergency Imaging
 Hampton Symposium,, October 16 th, 2010 Advances in Emergency Imaging Robert A. Novelline, MD Professor of Radiology, Harvard Medical School Director of Emergency Radiology, Massachusetts General Hospital
Hampton Symposium,, October 16 th, 2010 Advances in Emergency Imaging Robert A. Novelline, MD Professor of Radiology, Harvard Medical School Director of Emergency Radiology, Massachusetts General Hospital
RE: CHILD S NAME DOB: XXXXXXX Denial of DOC Band coverage XXXXXXXXX Care First Blue Cross Blue Shield Contract #: XXXXXX Group #: XXXXXXXXXXXXXX
 YOUR ADDRESS Oct. 9, 2002 Care First Blue Cross Blue Shield Attention: Appeals/Supervisor Control Plan Claims Unit P.O. Box 1739 Cumberland, Maryland 21501 RE: CHILD S NAME DOB: XXXXXXX Denial of DOC Band
YOUR ADDRESS Oct. 9, 2002 Care First Blue Cross Blue Shield Attention: Appeals/Supervisor Control Plan Claims Unit P.O. Box 1739 Cumberland, Maryland 21501 RE: CHILD S NAME DOB: XXXXXXX Denial of DOC Band
Prenatal Diagnosis of Cleft Lip
 Commentary Prenatal Diagnosis of Cleft Lip What the Sonologist Needs to Tell the Surgeon John. Mulliken, MD, eryl R. enacerraf, MD Division of Plastic Surgery, Children s Hospital (J..M.) Department of
Commentary Prenatal Diagnosis of Cleft Lip What the Sonologist Needs to Tell the Surgeon John. Mulliken, MD, eryl R. enacerraf, MD Division of Plastic Surgery, Children s Hospital (J..M.) Department of
Fetal MRI. Page 1 of 69
 Fetal MRI Poster No.: C-0878 Congress: ECR 2015 Type: Educational Exhibit Authors: Y. Kocaba# Köksel, M. A. Oztek, C. Y. Sanhal, S. Toru, #. Mendilcio#lu, M. #im#ek, K. Karaali; Antalya/TR Keywords: Obstetrics,
Fetal MRI Poster No.: C-0878 Congress: ECR 2015 Type: Educational Exhibit Authors: Y. Kocaba# Köksel, M. A. Oztek, C. Y. Sanhal, S. Toru, #. Mendilcio#lu, M. #im#ek, K. Karaali; Antalya/TR Keywords: Obstetrics,
Table 1: Helmet vs Conservative Treatment
 Table 1: Helmet vs Conservative Treatment Author (Year) Title Study Description Data Class, Quality, and Van Wijk et al (2014) Helmet Therapy in Infants with Positional Skull Deformation: Randomized Controlled
Table 1: Helmet vs Conservative Treatment Author (Year) Title Study Description Data Class, Quality, and Van Wijk et al (2014) Helmet Therapy in Infants with Positional Skull Deformation: Randomized Controlled
Interactions of the endocrine system, bone and oral health
 Interactions of the endocrine system, bone and oral health All bones are not equal! Dense high proportion of cortical bone High proportion of trabecular bone Mandible Functions: mastication, respiration,
Interactions of the endocrine system, bone and oral health All bones are not equal! Dense high proportion of cortical bone High proportion of trabecular bone Mandible Functions: mastication, respiration,
Craniosynostosis : Updates in Radiologic Diagnosis
 www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2016.59.3.219 J Korean Neurosurg Soc 59 (3) : 219-226, 2016 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2016 The Korean Neurosurgical Society Pediatric
www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2016.59.3.219 J Korean Neurosurg Soc 59 (3) : 219-226, 2016 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2016 The Korean Neurosurgical Society Pediatric
2016 Congress of Neurological Surgeons 1
 CONGRESS OF NEUROLOGICAL SURGEONS SYSTEMATIC REVIEW AND EVIDENCE-BASED GUIDELINE FOR THE DIAGNOSIS OF PATIENTS WITH POSITIONAL PLAGIOCEPHALY: THE ROLE OF IMAGING Sponsored by Congress of Neurological Surgeons
CONGRESS OF NEUROLOGICAL SURGEONS SYSTEMATIC REVIEW AND EVIDENCE-BASED GUIDELINE FOR THE DIAGNOSIS OF PATIENTS WITH POSITIONAL PLAGIOCEPHALY: THE ROLE OF IMAGING Sponsored by Congress of Neurological Surgeons
Central Nervous System Congenital Abnormalities
 Central Nervous System Congenital Abnormalities Eva Brichtova, M.D., Ph.D., Department of Pediatric Sugery, Orthopaedics and Traumatology, University Hospital Brno Neural tube defects Dysraphism uncomplete
Central Nervous System Congenital Abnormalities Eva Brichtova, M.D., Ph.D., Department of Pediatric Sugery, Orthopaedics and Traumatology, University Hospital Brno Neural tube defects Dysraphism uncomplete
INFANTILE EXOTROPIA. Lionel Kowal
 INFANTILE EXOTROPIA Lionel Kowal INFANTILE XT Usage often imprecise Variation in definitions number of investigators? onset day 1 of life? constant / intermittent Any / large angle? Associated systemic
INFANTILE EXOTROPIA Lionel Kowal INFANTILE XT Usage often imprecise Variation in definitions number of investigators? onset day 1 of life? constant / intermittent Any / large angle? Associated systemic
Romanian Neurosurgery Volume XXXI Number April-June. Article
 Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Association of abnormal metopic suture causing hypertelorism, interfrontal encephalocele with craniofacial cosmetic deformity associated
Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Association of abnormal metopic suture causing hypertelorism, interfrontal encephalocele with craniofacial cosmetic deformity associated
RADIOLOGIC TECHNOLOGY (526)
 RADIOLOGIC TECHNOLOGY (526) 526-133 DMS General Procedures 2 Radiologic Technology (526) 1 526-130 Introduction to Diagnostic Medical Sonography This course introduces the student to the history of ultrasound
RADIOLOGIC TECHNOLOGY (526) 526-133 DMS General Procedures 2 Radiologic Technology (526) 1 526-130 Introduction to Diagnostic Medical Sonography This course introduces the student to the history of ultrasound
Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment
 Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment Poster No.: C-1753 Congress: ECR 2011 Type: Scientific Exhibit Authors: E.
Ureteropelvic Junction Obstruction (UPJO) syndrome: imaging with Multidetector CT (MDCT) prior to minimally invasive treatment Poster No.: C-1753 Congress: ECR 2011 Type: Scientific Exhibit Authors: E.
Original Date: February 2006 PLAIN FILM X-RAYS
 Magellan Healthcare Clinical guidelines Original Date: February 2006 PLAIN FILM X-RAYS Page 1 of 5 Adopted Date 1 : April 2016 Physical Medicine Clinical Decision Making Last Review Date: August 2015 Guideline
Magellan Healthcare Clinical guidelines Original Date: February 2006 PLAIN FILM X-RAYS Page 1 of 5 Adopted Date 1 : April 2016 Physical Medicine Clinical Decision Making Last Review Date: August 2015 Guideline
Original Date: February 2006 PLAIN FILM X-RAYS
 Magellan Healthcare Clinical guidelines Original Date: February 2006 PLAIN FILM X-RAYS Page 1 of 5 Adopted Date 1 : April 2016 Physical Medicine Clinical Decision Making Last Review Date: August 2016 Guideline
Magellan Healthcare Clinical guidelines Original Date: February 2006 PLAIN FILM X-RAYS Page 1 of 5 Adopted Date 1 : April 2016 Physical Medicine Clinical Decision Making Last Review Date: August 2016 Guideline
SWISS SOCIETY OF NEONATOLOGY. Cantrell s pentalogy: an unusual midline defect
 SWISS SOCIETY OF NEONATOLOGY Cantrell s pentalogy: an unusual midline defect October 2004 2 Cevey-Macherel MN, Meijboom EJ, Di Bernardo S, Truttmann AC, Division of Neonatology and Division of Pediatric
SWISS SOCIETY OF NEONATOLOGY Cantrell s pentalogy: an unusual midline defect October 2004 2 Cevey-Macherel MN, Meijboom EJ, Di Bernardo S, Truttmann AC, Division of Neonatology and Division of Pediatric
4.3 Surgical Management of anterior skull synostosis
 ISPN course 23 rd Nov, 2015 Cranial & Craniofacial disorders 4.3 Surgical Management of anterior skull synostosis Kazuaki Shimoji, Masakazu Miyajima and Hajime Arai Department of Neurosurgery, Juntendo
ISPN course 23 rd Nov, 2015 Cranial & Craniofacial disorders 4.3 Surgical Management of anterior skull synostosis Kazuaki Shimoji, Masakazu Miyajima and Hajime Arai Department of Neurosurgery, Juntendo
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
An important indication for imaging the anterior skull base
 ORIGINAL RESEARCH D.C. Hughes M.J. Kaduthodil D.J.A. Connolly P.D. Griffiths Dimensions and Ossification of the Normal Anterior Cranial Fossa in Children BACKGROUND AND PURPOSE: Interpretation of CT of
ORIGINAL RESEARCH D.C. Hughes M.J. Kaduthodil D.J.A. Connolly P.D. Griffiths Dimensions and Ossification of the Normal Anterior Cranial Fossa in Children BACKGROUND AND PURPOSE: Interpretation of CT of
Debate continues to rage over the significance PEDIATRIC/CRANIOFACIAL. Neurodevelopmental Delays in Children with Deformational Plagiocephaly
 PEDIATRIC/CRANIOFACIAL Neurodevelopmental Delays in Children with Rouzbeh K. Kordestani, M.D., M.P.H. Shaurin Patel, M.D. David E., Bard, M.S. Robin Gurwitch, Ph.D. Jayesh Panchal, M.D., M.B.A. Oklahoma
PEDIATRIC/CRANIOFACIAL Neurodevelopmental Delays in Children with Rouzbeh K. Kordestani, M.D., M.P.H. Shaurin Patel, M.D. David E., Bard, M.S. Robin Gurwitch, Ph.D. Jayesh Panchal, M.D., M.B.A. Oklahoma
LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS
 POLSKI PRZEGLĄD CHIRURGICZNY 2009, 81, 1, 23 27 10.2478/v10035-009-0004-2 LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS PRADEEP JAIN, ANAND AGARWAL, ARVIND SRIVASTAVA Department of Plastic
POLSKI PRZEGLĄD CHIRURGICZNY 2009, 81, 1, 23 27 10.2478/v10035-009-0004-2 LATERAL CEPHALOMETRIC EVALUATION IN CLEFT PALATE PATIENTS PRADEEP JAIN, ANAND AGARWAL, ARVIND SRIVASTAVA Department of Plastic
Lumbosacral Transitional Vertebrae
 Lumbosacral Transitional Vertebrae Poster No.: C-073 Congress: ECR 206 Type: Educational Exhibit Authors: M. Mustapic, R. Vukojevi#, M. Gulin, D. Marjan, I. Boric ; 2 2 Zagreb/HR, Zabok/HR Keywords: Congenital,
Lumbosacral Transitional Vertebrae Poster No.: C-073 Congress: ECR 206 Type: Educational Exhibit Authors: M. Mustapic, R. Vukojevi#, M. Gulin, D. Marjan, I. Boric ; 2 2 Zagreb/HR, Zabok/HR Keywords: Congenital,
Clinical utility of tomosynthesis in suspected scaphoid fracture: Preliminary results evaluating the VolumeRad technique
 Clinical utility of tomosynthesis in suspected scaphoid fracture: Preliminary results evaluating the VolumeRad technique Poster No.: C-2193 Congress: ECR 2010 Type: Scientific Exhibit Topic: Musculoskeletal
Clinical utility of tomosynthesis in suspected scaphoid fracture: Preliminary results evaluating the VolumeRad technique Poster No.: C-2193 Congress: ECR 2010 Type: Scientific Exhibit Topic: Musculoskeletal
Craniosynostosis. chapter. Jeffrey Weinzweig, MD / Stephen B. Baker, MD, DDS / Mitchel Seruya, MD AQ1
 chapter 16 AQ1 Craniosynostosis Jeffrey Weinzweig, MD / Stephen B. Baker, MD, DDS / Mitchel Seruya, MD AQ2 PATIENT EVALUATION AND SELECTION Craniosynostosis is defined as the premature closure of a cranial
chapter 16 AQ1 Craniosynostosis Jeffrey Weinzweig, MD / Stephen B. Baker, MD, DDS / Mitchel Seruya, MD AQ2 PATIENT EVALUATION AND SELECTION Craniosynostosis is defined as the premature closure of a cranial
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Craniosynostosis is a disorder of skull development,
 Accuracy of Craniofacial Measurements: Computed Tomography and Three-Dimensional Computed Tomography Compared With Stereolithographic Models Julia Frühwald, MD,* Kurt A. Schicho, MD,1 Michael Figl, MD,2
Accuracy of Craniofacial Measurements: Computed Tomography and Three-Dimensional Computed Tomography Compared With Stereolithographic Models Julia Frühwald, MD,* Kurt A. Schicho, MD,1 Michael Figl, MD,2
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study
 Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Assessment of Pentalogy of Cantrell using 3D Multidetector Computed Tomography
 Assessment of Pentalogy of Cantrell using 3D Multidetector Computed Tomography Margaret H. Yew, B.A., Philip J. Spevak, M.D., Elliot K. Fishman, M.D., and Jens Vogel-Claussen, M.D. Citation: Yew MH, Spevak
Assessment of Pentalogy of Cantrell using 3D Multidetector Computed Tomography Margaret H. Yew, B.A., Philip J. Spevak, M.D., Elliot K. Fishman, M.D., and Jens Vogel-Claussen, M.D. Citation: Yew MH, Spevak
Radiological investigations
 Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Relationship of brain and skull in pre- and postoperative
 J. Anat. (2005) 206, pp373 385 Relationship of brain and skull in pre- and postoperative Blackwell Publishing, Ltd. sagittal synostosis Kristina Aldridge, 1 Alex A. Kane, 2 Jeffrey L. Marsh, 3 Peng Yan,
J. Anat. (2005) 206, pp373 385 Relationship of brain and skull in pre- and postoperative Blackwell Publishing, Ltd. sagittal synostosis Kristina Aldridge, 1 Alex A. Kane, 2 Jeffrey L. Marsh, 3 Peng Yan,
Role of the Radiologist
 Diagnosis and Treatment of Blunt Cerebrovascular Injuries NORDTER Consensus Conference October 22-24, 2007 Clint W. Sliker, M.D. University of Maryland Medical Center R Adams Cowley Shock Trauma Center
Diagnosis and Treatment of Blunt Cerebrovascular Injuries NORDTER Consensus Conference October 22-24, 2007 Clint W. Sliker, M.D. University of Maryland Medical Center R Adams Cowley Shock Trauma Center
