Diagnostics of ulcus cruris venosum
|
|
|
- Randolf McGee
- 6 years ago
- Views:
Transcription
1 Review Article 85 Diagnostics of ulcus cruris venosum M. Stücker; A. Pljakic; M. Dörler Klinik für Dermatologie, Venerologie und Allergologie der Ruhr-Universität Bochum, Venenzentrum der dermatologischen und gefäßchirurgischen Kliniken der Ruhr-Universität Bochum, Germany Keywords Ulcer, Ulcus cruris venosum, CVI, duplex ultrasound Summary Clinical diagnostics of venous leg ulcers set the course for efficient therapy. Precise clinical findings with an objectification of signs and symptoms of chronic venous insufficiency are essential. Duplex ultrasound investigations of the leg veins are necessary in the very early stages after the appearance of leg ulcers. Furthermore, not only a clinical investigation of the arterial perfusion but also the determination of the ankle-brachial-index is obligatory. Microbiological diagnostics are currently seen as useful in Germany, due to discussions on MRSA, even though they don t have an immediate therapeutic consequence without the presence of clinical signs of infection. Therapeutic achievements can be objectified by a continuous documentation of the wound size, the wound bed, the wound exudate and signs of infection as well as the life quality of patients with chronic wounds. Correspondence to Prof. Dr. Markus Stücker Venenzentrum der dermatologischen und gefäßchirurgischen Kliniken Kliniken der Ruhr-Universität Bochum Hiltroper Landwehr 1113, Bochum, Germany Tel. 49/234/ od. 378, Fax m.stuecker@klinikum-bochum.de Gravitational ulcer is the most common cause of chronic wounds of the lower limb. It accounts for up to 70 % of all chronic wounds on the leg (1). Gravitational ulcer is defined as ulceration of the leg or foot in an area with venous hypertension. Venous hypertension is caused by refluxes or obstructions. Schlüsselwörter Ulkus, Ulcus cruris venosum, CVI, Duplexsonografie Zusammenfassung Die Diagnostik des Ulcus cruris venosum stellt die Weichen für eine erfolgreiche Therapie. Entscheidend ist eine präzise klinische Befunderhebung mit der Objektivierung der Zeichen einer chronischen Veneninsuffizienz. Sehr frühzeitig bei dem Auftreten eines Ulcus cruris ist eine duplexsonografische Untersuchung der Beinvenen zur Therapieplanung erforderlich. Obligatorisch ist ferner nicht nur die klinische Untersuchung der arteriellen Durchblutung, sondern auch die Bestimmung des Knöchel-Arm-Index. Eine mikrobiologische Diagnostik wird derzeit in Deutschland aufgrund der MRSA-Diskussion für sinnvoll erachtet, obwohl sie ohne das Vorliegen klinischer Infektionszeichen keine direkte therapeutische Konsequenz hat. Durch eine laufende Dokumentation der Wundgröße, des Wundgrunds, des Wundexsudats und der Infektzeichen sowie der Lebensqualität des Patienten mit chronischen Wunden können Therapieerfolge objektiviert werden. Diagnostik des Ulcus cruris venosum Phlebologie 2016; 45: Received: January 27, 2016 Accepted: January 28, 2016 However, other exceptional situations, such as arthrogenic congestion syndrome or functional chronic venous insufficiency in obesity-associated dependency syndrome, can also lead to signs of chronic venous insufficiency, sometimes progressing to gravitational ulcer (2). When analysing the causes of gravitational ulcer, impaired venous function in not only the leg, but also in the pelvis in the area of the iliac vein or the inferior vena cava should be considered. In addition to impaired venous function, other pathogenetically relevant mechanisms exist, such as activation of inflammatory cascades. However, as these are currently poorly accessible to routine diagnostics, they are not further considered in this article. The purpose of diagnostics in gravitational ulcer must be to define, as efficiently as possible, the pathogenetically relevant factors that are accessible to therapy. An essential step here is to decide whether the ulcer is a purely gravitational ulcer or whether other pathogenetic factors also play a part. Here, particular consideration should be given to peripheral arterial occlusive disease and other pathological conditions, such as scarring, lymphoedema, autoimmune diseases, infections and trauma (3). If other pathogenetically relevant factors beyond those of purely venous origin are present, protracted healing is likely. The main differential diagnoses for lower leg ulcers are listed in Table 1. The following specific steps are of proven efficacy in the diagnosis of gravitational ulcer: Medical history The medical history of patients with gravitational ulcer can be complicated by the limitations associated with the patients advanced age, their very long medical history and complex concomitant diseases. It has therefore proven effective to concentrate on a few questions that are particularly important for the management of gravitational ulcer. Of relevance in this context are the patients possibilities of independent actions in therapy and their social circumstances, in order to estimate to what extent supportive measures, such as a mobile nursing service, may be necessary. They should be asked about any concomi- Schattauer 2016 Phlebologie 2/2016
2 86 M. Stücker, A. Pljakic; M. Doerler: Diagnosis of gravitational ulcer Tab. 1 Differential diagnosis of gravitational ulcer (according to 4). Vascular disorders Neuropathic Metabolic Haematological Exogenous Neoplasia Infection Drug Genetic defect Veins Arteries Lymph drainage disorder Vasculitis Microangiopathy Peripheral CNS Erythrocytes Leukocytes Platelets Dysproteinaemia Coagulation Primary cutaneous malignancy Bacteria Viruses Fungi Protozoa Chronic venous insufficiency: postthrombotic syndrome, varicosis, dysplasia Peripheral arterial occlusive disease, hypertension, arteriovenous fistula, arterial thrombosis, embolism, dysplasia, thromboangiitis obliterans, aneurysm Lymphoedema, dysplasia Rheumatoid arthritis, leukocytoclastic vasculitis, polyarteritis nodosa, Wegener s granulomatosis, Churg- Strauss syndrome, Bazin s disease, lupus erythematosus, Sjögren s syndrome, scleroderma, Behçet s disease Diabetes mellitus, livedoid vasculopathy Diabetes mellitus, alcohol, medicines Tabetic neurosyphilis, myelodysplasia, syringomyelia, spina bifida, poliomyelitis, multiple sclerosis Diabetes mellitus, gout, prolidase deficiency, Gaucher s disease, amyloidosis, calciphylaxis, porphyrias, hyperhomocysteinaemia Sickle cell anaemia, thalassaemia, polycythaemia vera Leukaemia Thrombocythaemia Cryoglobulinaemia, lymphoma Plasmatic coagulation factors (factors I-XIII), coagulation inhibitors (antithrombin III, APC resistance, proteins C and S), fibrinolysis factors (t-pa, PAI, plasmin) Heat, cold, pressure, ionising radiation, artefacts, chemical noxae, allergens Basal cell carcinoma, squamous cell carcinoma (Marjolin s ulcer), malignant melanoma, (angio)sarcoma, cutaneous lymphoma Furuncle, ecthyma, mycobacteriosis, syphilis, erysipelas, anthrax, diphtheria, chronic vegetative pyoderma, tropical ulcer Herpes, smallpox virus, cytomegalovirus infection Sporotrichosis, histoplasmosis, blastomycosis, coccidioidomycosis Leishmaniasis Hydroxycarbamide, leflunomide, methotrexate, halogens, Marcumar [phenprocoumon], vaccinations, ergotamine, paravasal cytostatics Klinefelter s syndrome, Felty s syndrome, TAP 1 mutation, leukocyte adhesion deficiency tant disease and their vaccination status (tetanus protection?). The questions should focus on the venous disease itself and the ulceration. Cf. Table 2 and Table 3. Clinical investigation Gravitational ulcer has a typical morphology. It is more frequently located on the medial malleolus than on the fibular malleolus. Other signs of chronic venous insufficiency are typically found around the gravitational ulcer, such as spider-burst veins, reticular veins, varicoses of the smaller leg veins, oedema, hyperpigmentation, stasis eczema, white atrophy, lipodermatosclerosis, scarred changes associated with status post ulcer healing. In the event of multiple ulcerations and an atypical location, further factors have to be considered, which, in addition to venous hypertension, can lead to the development and persistence of the ulceration or which are solely responsible for the ulceration. Early recognition of malignant tumours as the cause or sequelae of ulceration is important (5). One significant indication of a malignant transformation is a treatmentresistant course, in which the assumed gravitational ulcer has shown no healing tendency over 68 weeks, despite adequate compression therapy. Already at the initial examination, there will be further criteria that are indicative of a malignant tumour in the ulcerated area: atypical morphology with atypical position, form and wound surroundings, nodular proliferation, darkly livid colour of the granular tissue and a long duration with a small wound size. In the event of any clinical or anamnestic indications of malignant tumour growth in the ulcerated area, sufficiently large biopsies should be taken from various sites. Typical biopsy sites are the wound edge and areas of nodular proliferation in the various ulcerated areas. If ulcerated areas are biopsied, the biopsies must be deep enough to avoid obtaining only Phlebologie 2/2016 Schattauer 2016
3 M. Stücker, A. Pljakic; M. Doerler: Diagnosis of gravitational ulcer 87 superficial wound detritus or pathological granulation tissue and leaving behind the possibly underlying cancerous process. Microbiology It is often considered unnecessary to start a routine microbiological culture for venous ulcerations. A microbiological culture should only be started in the presence of clinical signs of wound infections (3). By contrast, in many health care institutions, particularly in hospitals, meticillin-resistant Staphylococcus aureus (MRSA) screening is performed at admission, if MRSA risk factors are present. Skin ulcerations are assessed as MRSA risk factors. In such patients, a combined throat/nose swab and a swab from the wound area should be taken. Independently of this, a microbiological culture should be obtained from patients showing clinical signs of infection, such as fever, increasing pain, increased redness, increased wound exudate, an offensive wound odour, biofilm formation, tissue necrosis or ulcer progression (3). In specialised centres, in which patients present with secondary or tertiary disease, crural ulcerations often show such features, so that primary microbiological diagnostics are frequently indicated in such centres. For this, a bacterial swab should be obtained by guiding the swab in a spiral circular motion from the outside to the inside, covering as large an area of the wound as possible (6). Peripheral arterial occlusive disease In all patients with chronic crural wounds, the ankle-brachial index should be determined. Whereas only 3 % of patients below 60 years of age suffer from peripheral arterial occlusive disease, there is a dramatic rise in the frequency of this disease in later years, increasing to over 20 % in those aged 75 years and above (7). The ankle-brachial index is determined with the patient lying down using a blood pressure cuff and a continuous wave (CW) Doppler probe. The blood pressure cuff should be placed immediately above the ankle, as the Tab. 2 Basic medical history in gravitational ulcer Tab. 3 Specific history in gravitational ulcer Weight, height, BMI Concomitant disease, particularly Allergies Angiological risk factors Social history Mobility Duration of current ulceration Current symptoms Last therapy Recurrent ulceration Previous interventions on the legs affecting the ulceration Epicutaneous testing History of multiresistant pathogens Tetanus protection pressure is recorded under the cuff during the measurement. The ulceration will often have to be covered appropriately, in order to achieve a sufficiently distal measure- Peripheral polyneuropathy Vasculitis Diabetes mellitus Heart failure and other cardiac diseases Current internal medication Nicotine abuse Hypercholesterolaemia Arterial hypertension Marital status: Children: Occupation: Residence: 1= standing up independently (if necessary, with walking aid) and walking at least 50 m, 2= standing up with outside help and walking at least 50 m, 3= moving at least 50 m in a wheelchair, 4= moving <50 m Pain, discharge, increase in size of the ulceration Intermittent claudication with a maximum painless walking distance in metres Cramps in the calf muscles, tendency to swelling of the legs, sensation of heaviness in the legs Wound dressing Wound débridement Compression therapy Dressing change previously performed by: How many recurrences First occurrence of ulceration Varicose vein surgery Sclerotherapy Percutaneous transluminal angioplasty (PTA) Bypass surgery Split-skin graft No allergy pass available/ Allergy pass available MRSA/extended-spectrum beta-lactamases (ESBL) / multiresistant pseudomonads ment. Placing the blood pressure cuff further proximal to the wound can result in distal arterial occlusions or stenoses being overlooked. The Doppler probe records the Schattauer 2016 Phlebologie 2/2016
4 88 M. Stücker, A. Pljakic; M. Doerler: Diagnosis of gravitational ulcer 1. Deep veins: patency and reflux 2. Junctions in the groin and knee: Refluxes (terminal valve and preterminal valve) 3. Main branches: measurement of diameter and reflux (in the saphenous compartment): 4. Lateral branches: if incompetent 5. Non-saphenous veins: if incompetent 6. Perforating vein: measurement of diameter and reflux Common femoral vein Popliteal vein Saphenofemoral junction Saphenopopliteal junction Great saphenous vein Anterior accessory saphenous vein Posterior accessory saphenous vein Small saphenous vein Thigh extension of the small saphenous vein/giacomini vein Tab. 4 Examination sites of venous duplex ultrasound according to the UIP consensus document 2011 (9) systolic pressure over the posterior tibial artery and the dorsal artery of the foot on each leg and is set in proportion to the pressure of the brachial artery in the arm that is used to calculate the ankle-brachial index. Peripheral arterial occlusive disease is assumed if the ankle-brachial index is <0.90 at rest. An ankle-brachial index of 0.50 usually corresponds to critical ischaemia. Compression therapy should not be performed if malleolar artery pressures are below 60 mmhg. At malleolar artery pressures between 60 and 80 mmhg, compression therapy should be attempted, but this may cause excessive pain for the patient. At malleolar artery pressures above 80 mmhg, Fig. 1 Questionnaire Wound QoL (11) Phlebologie 2/2016 Schattauer 2016
5 M. Stücker, A. Pljakic; M. Doerler: Diagnosis of gravitational ulcer 89 compression therapy can be performed, even in the presence of pathological anklebrachial indices. In the event of pathological ankle-brachial indices, particularly in patients with critical ischaemia, the option of arterial revascularisation should be investigated. Venous function measurements Using venous plethysmography, such as strain-gauge plethysmography, air plethysmography or photoplethysmography, it is possible to objectify functional impairment of the venous outflow. Venous reflux, impaired outflow and impaired muscle pump function correlate well with the findings of duplex ultrasound and can objectify changes in venous function through therapeutic measures on the venous system. Venous duplex ultrasound Venous duplex ultrasound is considered to be an indispensable reference standard in the examination of patients with gravitational ulcer. The examination should be performed directly at the outset of diagnostic tests. Although CW Doppler examinations yield important indications of venous disorders, duplex ultrasonography is essential when planning invasive treatment measures and is often suggested as the first-line diagnostic test (3). In patients with gravitational ulcer, duplex ultrasonography follows the general principles of duplex ultrasound diagnostics in chronic venous insufficiency in accordance with the UIP consensus document of 2006 (8). The following information is taken from this consensus document. Ultrasonic probes of MHz are proposed and only in the case of very voluminous and oedematous legs may 3.55 MHz probes be advisable. In order to standardise the measurements of venous diameters and refluxes, the UIP consensus recommends performing the examination with the patient standing up. Refluxes lasting longer than 0.5 seconds are considered to be pathological. The refluxes can be triggered by various measures, such as manual compression/decompression of the lower leg, the inner side of the thigh or varicose veins, but also by active dorsiflexion and relaxation of the foot or by the classic Valsalva manoeuvre. The main examination sites are presented in Table 4. Venous imaging Diagnostic investigation of the deep veins of the legs is currently gaining in importance. Obstructions in the deep veins of the legs as the cause of severe chronic venous insufficiency, sometimes progressing to gravitational ulcer, have probably been underestimated for a long time. Frequently, duplex ultrasound only provides insufficient information about the iliocaval veins, so that supplementary procedures are required, if insufficiency of the deep leg veins in the pelvic area is suspected. In such cases, CT angiograms and MRI angiograms are helpful and can be followed by targeted phlebography. As a practical procedure, it has proved advisable to conduct an initial analysis of the superficial and deep venous system of the leg, as already described, and to treat superficial refluxes. If the ulcerations fail to heal, duplex ultrasound should be repeated, in order to detect any untreated refluxes of the superficial leg veins and reflux Tab. 5 Diagram of wound documentation based on (12) < Wound bed score A B C D Wound exudate score Infection score k d i treatment should be repeated, if necessary. If an ulceration fails to heal despite sufficient reflux treatment or if no superficial refluxes occur despite apparent signs of chronic venous insufficiency, imaging of the deep pelvic veins should be considered. If occlusions or stenoses of the deep pelvic veins are evident, stenting of these veins can accelerate healing of the gravitational ulcer (10). Quality of life Evaluation of the quality of life of patients with chronic wounds is generally recommended. As quality of life questionnaires are often very extensive, a shorter, onepage quality of life questionnaire was specifically developed for patients with chronic wounds and reduced to 17 questions. This so-called Wound QoL ( Fig. 1) covers the three subscales of life, body and psyche (11). The form can be used in routine clinical practice. Contractual agreement with the creators of the form is only required for use in studies (Dr. Christine Blome, CVderm, Universitätsklinik Hamburg-Eppendorf, Martinistraße 52, Hamburg, Germany). Quality of life should be evaluated at regular intervals. Particularly in long-term diseases, it is an important follow-up par- Characterisation of the wound bed Granulation tissue 100 % % < 50 % Unlimited extension Amount of exudate no exudate/minimal moderate very heavy Signs of infection Wound area: Length x breadth in mm Fibrinous coatings no signs of infection signs of an imminent wound infection manifest wound infection Scabbing Schattauer 2016 Phlebologie 2/2016
6 90 M. Stücker, A. Pljakic; M. Doerler: Diagnosis of gravitational ulcer ameter for monitoring treatment and evaluating the course of disease. Wound documentation After the documentation at initial presentation, wound documentation should be conducted at regular intervals, at least once a month, in order to objectify the effect of therapy on the healing process. The number and position of the individual ulcers are particularly important parameters of wound documentation. The size of each individual wound (at least its length and breadth), the amount of exudate, the area of granulation and the wound coating and any signs of wound infection should be documented. This can be conducted, for example, on the basis of a proposal by Falanga from 2000 (12) ( Table 5). Conflict of interest The author declares that no conflict of interest exists. Ethical guidelines The article was written in accordance with national guidelines and the current Declaration of Helsinki. References 1. Tatsioni A, Balk E, OADonnell TF Jr, Lau J. Usual care in the management of chronic wounds: A review of the recent literature. J Am Coll Surg 2007; 205: Dörler M, Altmeyer P, Stücker M. Venous leg ulcer caused by obesity-associated dependency syndrome. Phlebologie 2013; 43: O Donnell TF Jr, Passman MA, Marston WA, et al.; Society for Vascular Surgery; American Venous Forum. Management of venous leg ulcers: clinical practice guidelines of the Society for Vascular Surgery and the American Venous Forum. J Vasc Surg 2014 Aug; 60(2 Suppl): 3S-59S. 4. Dissemond J, Körber A, Grabbe S. Differentialdiagnosen des Ulcus cruris. J Dtsch Dermatol Ges 2006; 4(8): Reich-Schupke S, Dörler M, Wollina U, et al. Squamous cell carcinomas in chronic venous leg ulcers. Data of the German Marjolin Registry and review. J Dtsch Dermatol Ges 2015; 13(10): Al Ghazal P, Körber A, Klode J, et al. Evaluation of the Essen Rotary as a new technique for bacterial swabs: results of a prospective controlled clinical investigation in 50 patients with chronic leg ulcers. Int Wound J 2014; 11(1): Criqui MH, Fronek A, et al. The prevalence of peripheral arterial disease in a defined population. Circulation 1985; 71(3): Coleridge-Smith P, Labropoulos N, Partsch H, et al. Duplex ultrasound investigation of the veins in chronic venous disease of the lower limbs--uip consensus document. Part I. Basic principles. Eur J Vasc Endovasc Surg 2006 Jan; 31(1): De Maeseneer M, Pichot O, Cavezzi A, et al. Duplex ultrasound investigation of the veins of the lower limbs after treatment for varicose veins UIP consensus document. Eur J Vasc Endovasc Surg 2011; 42(1): Verma H, Tripathi RK. Algorithm-based approach to management of venous leg ulceration. Semin Vasc Surg 2015 Mar; 28(1): Blome C, Baade K, Debus ES, Price P, Augustin M. The Wound-QoL : A short questionnaire measuring quality of life in patients with chronic wounds based on three established disease-specific instruments. Wound Rep Reg 2014; 22: Falanga V. Classifications for wound bed preparation and stimulation of chronic wounds. Wound Repair Regen 2000 Sep-Oct; 8(5): Phlebologie 2/2016 Schattauer 2016
Venous Reflux Duplex Exam
 Venous Reflux Duplex Exam GWENDOLYN CARMEL, RVT PHYSIOLOGIST, DEPARTMENT OF VASCULAR SURGERY NEW JERSEY VETERANS HEALTHCARE CENTER EAST ORANGE, NJ PURPOSE: To identify patterns of incompetence and which
Venous Reflux Duplex Exam GWENDOLYN CARMEL, RVT PHYSIOLOGIST, DEPARTMENT OF VASCULAR SURGERY NEW JERSEY VETERANS HEALTHCARE CENTER EAST ORANGE, NJ PURPOSE: To identify patterns of incompetence and which
chronic venous disorders, varicose vein, CEAP classification, lipodermatosclerosis, Klippel- Trenaunay syndrome DVT CVD
 Online publication August 27, 2009 chronic venous disorders: CVD CEAP 4 CEAP CVD J Jpn Coll Angiol, 2009, 49: 201 205 chronic venous disorders, varicose vein, CEAP classification, lipodermatosclerosis,
Online publication August 27, 2009 chronic venous disorders: CVD CEAP 4 CEAP CVD J Jpn Coll Angiol, 2009, 49: 201 205 chronic venous disorders, varicose vein, CEAP classification, lipodermatosclerosis,
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
Segmental GSV reflux
 Segmental GSV reflux History of presentation A 43 year old female presented with right lower extremity varicose veins and swelling. She had symptoms of aching, heaviness and tiredness in the right leg.
Segmental GSV reflux History of presentation A 43 year old female presented with right lower extremity varicose veins and swelling. She had symptoms of aching, heaviness and tiredness in the right leg.
Starting with deep venous treatment
 Starting with deep venous treatment Carsten Arnoldussen, MD Interventional Radiologist Maastricht University Medical Centre, Maastricht VieCuri Medical Centre, Venlo The Netherlands Background Maastricht
Starting with deep venous treatment Carsten Arnoldussen, MD Interventional Radiologist Maastricht University Medical Centre, Maastricht VieCuri Medical Centre, Venlo The Netherlands Background Maastricht
Clinical/Duplex Evaluation of Varicose Veins: Who to Treat?
 Clinical/Duplex Evaluation of Varicose Veins: Who to Treat? Sanjoy Kundu MD, FASA, FCIRSE, FSIR The Vein Institute of Toronto Scarborough Vascular Group Scarborough Vascular Ultrasound Scarborough Vascular
Clinical/Duplex Evaluation of Varicose Veins: Who to Treat? Sanjoy Kundu MD, FASA, FCIRSE, FSIR The Vein Institute of Toronto Scarborough Vascular Group Scarborough Vascular Ultrasound Scarborough Vascular
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
DISORDERS OF VENOUS SYSTEM
 DISORDERS OF VENOUS SYSTEM Varicose Veins Any dilated, elongated and tortuous vein irrespective of size Varicose veins are common in the superficial veins of the leg which are subject to high pressure
DISORDERS OF VENOUS SYSTEM Varicose Veins Any dilated, elongated and tortuous vein irrespective of size Varicose veins are common in the superficial veins of the leg which are subject to high pressure
Determine the patients relative risk of thrombosis. Be confident that you have had a meaningful discussion with the patient.
 Patient Assessment :Venous History, Examination and Introduction to Doppler and PPG Dr Louis Loizou The 11 th Annual Scientific Meeting and Workshops of the Australasian College of Phlebology Tuesday 18
Patient Assessment :Venous History, Examination and Introduction to Doppler and PPG Dr Louis Loizou The 11 th Annual Scientific Meeting and Workshops of the Australasian College of Phlebology Tuesday 18
Dr Paul Thibault. Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology
 Dr Paul Thibault Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology Prescribing Effective Compression and PTS Dr Paul Thibault Phlebologist, Newcastle,
Dr Paul Thibault Phlebologist & Assistant Editor Phlebology (International Journal) Australasian College of Phlebology Prescribing Effective Compression and PTS Dr Paul Thibault Phlebologist, Newcastle,
Promoting best practice in leg ulcer management
 Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Promoting best practice in leg ulcer management Sylvie Hampton MA BSc (Hons) DpSN RGN Independent Tissue Viability Consultant Nurse Leg Ulcers - What are the causes? Chronic leg ulcers are defined as those
Selection and work up for the right patients suspected of deep venous disease
 Selection and work up for the right patients suspected of deep venous disease R A G H U K O L L U R I, M S, M D, R V T S Y S T E M M E D I C A L D I R E C T O R V A S C U L A R M E D I C I N E / V A S
Selection and work up for the right patients suspected of deep venous disease R A G H U K O L L U R I, M S, M D, R V T S Y S T E M M E D I C A L D I R E C T O R V A S C U L A R M E D I C I N E / V A S
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
Lower Limb Venous Ultrasound. Colin P. Griffin MSc, BSc (Hons)
 Lower Limb Venous Ultrasound Colin P. Griffin MSc, BSc (Hons) Peripheral Vessels Lower Limb Peripheral Vessels Lower Limb Venous Deep System Common Iliac External/Internal Iliac Common Femoral Femoral
Lower Limb Venous Ultrasound Colin P. Griffin MSc, BSc (Hons) Peripheral Vessels Lower Limb Peripheral Vessels Lower Limb Venous Deep System Common Iliac External/Internal Iliac Common Femoral Femoral
Etiology of chronic leg ulcers in 31,619 patients in Germany analyzed by an expert survey
 DOI: 10.1111/j.1610-0387.2010.07535.x Original Article 1 Etiology of chronic leg ulcers in 31,619 patients in Germany analyzed by an expert survey Andreas Körber 1, Joachim Klode 1, Samy Al-Benna 2, Caroline
DOI: 10.1111/j.1610-0387.2010.07535.x Original Article 1 Etiology of chronic leg ulcers in 31,619 patients in Germany analyzed by an expert survey Andreas Körber 1, Joachim Klode 1, Samy Al-Benna 2, Caroline
Priorities Forum Statement
 Priorities Forum Statement Number 9 Subject Varicose Vein Surgery Date of decision September 2014 Date refreshed March 2017 Date of review September 2018 Relevant OPCS codes: L841-46, L848-49, L851-53,
Priorities Forum Statement Number 9 Subject Varicose Vein Surgery Date of decision September 2014 Date refreshed March 2017 Date of review September 2018 Relevant OPCS codes: L841-46, L848-49, L851-53,
Lower Extremity Venous Insufficiency Evaluation
 VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Lower Extremity Venous Insufficiency Evaluation This Protocol was prepared by members of the Society for Vascular Ultrasound (SVU) as a template
VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Lower Extremity Venous Insufficiency Evaluation This Protocol was prepared by members of the Society for Vascular Ultrasound (SVU) as a template
How to manage leg ulcers in the elderly
 How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
Venous Ulcers. A Little Basic Science. An Aggressive Prescription to Aid Healing. Why do venous ulcers occur? Ambulatory venous hypertension!
 UCSF Vascular Symposium April 26-28, 2012 San Francisco, California True statements about the management of venous ulcers include: An Aggressive Prescription to Aid Healing Anthony J. Comerota, MD, FACS,
UCSF Vascular Symposium April 26-28, 2012 San Francisco, California True statements about the management of venous ulcers include: An Aggressive Prescription to Aid Healing Anthony J. Comerota, MD, FACS,
Healthy Legs For Life! Prevention is better then cure
 Healthy Legs For Life! Prevention is better then cure Ellie Lindsay Independent Specialist Practitioner Associate Lecturer, CRICP, London Visiting Fellow, Queensland University of Technology Occurrence
Healthy Legs For Life! Prevention is better then cure Ellie Lindsay Independent Specialist Practitioner Associate Lecturer, CRICP, London Visiting Fellow, Queensland University of Technology Occurrence
Step by step ultrasound examination of varicose veins. Dr. Özgün Sensebat Vascular Surgeon Private Vascular Clinic Dorsten & Borken, Germany
 Step by step ultrasound examination of varicose Dr. Özgün Sensebat Vascular Surgeon Private Vascular Clinic Dorsten & Borken, Germany Required technical setup: B-mode vessel imaging combined with color
Step by step ultrasound examination of varicose Dr. Özgün Sensebat Vascular Surgeon Private Vascular Clinic Dorsten & Borken, Germany Required technical setup: B-mode vessel imaging combined with color
Leg ulcer assessment and management
 Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Chronic Venous Insufficiency
 Chronic Venous Insufficiency None Disclosures Lesley Enfinger, MSN,NP-C Chronic Venous Insufficiency Over 24 Million Americans affected by Chronic Venous Insufficiency (CVI) 10 x More Americans suffer
Chronic Venous Insufficiency None Disclosures Lesley Enfinger, MSN,NP-C Chronic Venous Insufficiency Over 24 Million Americans affected by Chronic Venous Insufficiency (CVI) 10 x More Americans suffer
Chronic Venous Insufficiency Compression and Beyond
 Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
Deep Venous Pathology. Eberhard Rabe Department of Dermatology University of Bonn Germany
 Deep Venous Pathology Eberhard Rabe Department of Dermatology University of Bonn Germany Disclosures None for this presentation Consultant: Sigvaris, EUROCOM Speakers bureau: Bayer Vital, Aspen, Boehringer,
Deep Venous Pathology Eberhard Rabe Department of Dermatology University of Bonn Germany Disclosures None for this presentation Consultant: Sigvaris, EUROCOM Speakers bureau: Bayer Vital, Aspen, Boehringer,
Management of Post-Thrombotic Syndrome
 Management of Post-Thrombotic Syndrome Thanainit Chotanaphuti Phramongkutklao College of Medicine Bangkok, Thailand President of CAOS Asia President of Thai Hip & Knee Society President of ASEAN Arthroplasty
Management of Post-Thrombotic Syndrome Thanainit Chotanaphuti Phramongkutklao College of Medicine Bangkok, Thailand President of CAOS Asia President of Thai Hip & Knee Society President of ASEAN Arthroplasty
New Guideline in venous ulcer treatment: dressing, medication, intervention
 New Guideline in venous ulcer treatment: dressing, medication, intervention Kittipan Rerkasem, FRCS(T), PhD Department of Surgery Faculty of Medicine Chiang Mai University Topic Overview venous ulcer treatment
New Guideline in venous ulcer treatment: dressing, medication, intervention Kittipan Rerkasem, FRCS(T), PhD Department of Surgery Faculty of Medicine Chiang Mai University Topic Overview venous ulcer treatment
Clinical case. Symptomatic anterior accessory great saphenous vein (AAGSV) reflux
 Clinical case Symptomatic anterior accessory great saphenous vein (AAGSV) reflux A 70 year-old female presents with symptomatic varicose veins on left leg for more than 10 years. She complains of heaviness,
Clinical case Symptomatic anterior accessory great saphenous vein (AAGSV) reflux A 70 year-old female presents with symptomatic varicose veins on left leg for more than 10 years. She complains of heaviness,
Conflict of Interest. None
 Conflict of Interest None American Venous Forum Guidelines on Superficial Venous Disease TOP 10 GUIDELINES 10. We recommend using the CEAP classification to describe chronic venous disorders. (GRADE 1B)
Conflict of Interest None American Venous Forum Guidelines on Superficial Venous Disease TOP 10 GUIDELINES 10. We recommend using the CEAP classification to describe chronic venous disorders. (GRADE 1B)
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Interactive Learning Session
 Chronic Venous Disease - Part I Interactive Learning Session 2011 Ali Sabbour Prof of Vascular Surgery http://mic.shams.edu.eg/moodle6 Login as a guest Surgery 2 Ali Sabbour - Chronic Venous Disease Intended
Chronic Venous Disease - Part I Interactive Learning Session 2011 Ali Sabbour Prof of Vascular Surgery http://mic.shams.edu.eg/moodle6 Login as a guest Surgery 2 Ali Sabbour - Chronic Venous Disease Intended
Post-Thrombotic Syndrome(PTS) Conservative Treatment Options
 Post-Thrombotic Syndrome(PTS) Conservative Treatment Options Dr. S. Kundu Scarborough Hospital-General Division Scarborough Vascular Group Toronto Endovascular Centre The Vein Institute of Toronto Scarborough
Post-Thrombotic Syndrome(PTS) Conservative Treatment Options Dr. S. Kundu Scarborough Hospital-General Division Scarborough Vascular Group Toronto Endovascular Centre The Vein Institute of Toronto Scarborough
Diameter reduction of the great saphenous vein and the common femoral vein after CHIVA
 Original article 1 Diameter reduction of the great saphenous vein and the common femoral vein after CHIVA Long-term results E. Mendoza Private Practice, Wunstorf Keywords Varicose veins, CHIVA, vein diameter,
Original article 1 Diameter reduction of the great saphenous vein and the common femoral vein after CHIVA Long-term results E. Mendoza Private Practice, Wunstorf Keywords Varicose veins, CHIVA, vein diameter,
Protocols for the evaluation of lower extremity venous reflux: supine, sitting, or standing?
 Protocols for the evaluation of lower extremity venous reflux: supine, sitting, or standing? Susan Whitelaw RVT, RDMS PURPOSE Duplex imaging of the lower extremity veins is performed to assess the deep
Protocols for the evaluation of lower extremity venous reflux: supine, sitting, or standing? Susan Whitelaw RVT, RDMS PURPOSE Duplex imaging of the lower extremity veins is performed to assess the deep
Additional Information S-55
 Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
Peripheral Arterial Disease Extremity
 Peripheral Arterial Disease Lower Extremity 05 Contributor Dr Steven Chong Advisors Dr Ashish Anil Dr Tay Jam Chin Introduction Risk Factors Clinical Presentation Classification History PHYSICAL examination
Peripheral Arterial Disease Lower Extremity 05 Contributor Dr Steven Chong Advisors Dr Ashish Anil Dr Tay Jam Chin Introduction Risk Factors Clinical Presentation Classification History PHYSICAL examination
Classification for elastic tubes, medical socks and soft bandaging?
 Classification for elastic tubes, medical socks and soft bandaging? Dr. Martin Abel Head of Medical & Regulatory Affairs, Lohmann & Rauscher GmbH & Co KG Copenhagen, 17.05.2013 1 Standard Bandages in UK
Classification for elastic tubes, medical socks and soft bandaging? Dr. Martin Abel Head of Medical & Regulatory Affairs, Lohmann & Rauscher GmbH & Co KG Copenhagen, 17.05.2013 1 Standard Bandages in UK
Venous drainage of the lower limb
 Venous drainage of the lower limb INTRODUCTION It is of immense clinical and surgical importance. The venous blood against gravity. FACTORS HELPING THE VENOUS DRAINAGE OF THE LOWER LIMB The contraction
Venous drainage of the lower limb INTRODUCTION It is of immense clinical and surgical importance. The venous blood against gravity. FACTORS HELPING THE VENOUS DRAINAGE OF THE LOWER LIMB The contraction
How to best approach chronic venous occlusions?
 How to best approach chronic venous occlusions? Prof. Nils Kucher Director Venous Thromboembolism Reseach Group University Hospital Bern nilskucher.com Disclosure Speaker name: Nils Kucher X X I have the
How to best approach chronic venous occlusions? Prof. Nils Kucher Director Venous Thromboembolism Reseach Group University Hospital Bern nilskucher.com Disclosure Speaker name: Nils Kucher X X I have the
Ms Prudence Lennox. Director of Nursing IHC President of the NZ Wound Care Society Auckland. 8:45-9:15 Wound Management in Primary Care
 Ms Prudence Lennox Director of Nursing IHC President of the NZ Wound Care Society Auckland 8:45-9:15 Wound Management in Primary Care Wound management in primary care L I Z M I L N E R N U R S E M A N
Ms Prudence Lennox Director of Nursing IHC President of the NZ Wound Care Society Auckland 8:45-9:15 Wound Management in Primary Care Wound management in primary care L I Z M I L N E R N U R S E M A N
A A U
 PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
Venous Insufficiency Ulcers. Patient Assessment: Superficial varicosities. Evidence of healed ulcers. Dermatitis. Normal ABI.
 Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Ms Prudence Lennox. Ms Liz Milner. 15:30-16:00 Wound Management in Primary Care. Nurse Manager Healthcare Rehabilitation Auckland
 Ms Liz Milner Nurse Manager Healthcare Rehabilitation Auckland Ms Prudence Lennox President NZ Wound Care Society 15:30-16:00 Wound Management in Primary Care Overview Wounds we see in primary care Flap
Ms Liz Milner Nurse Manager Healthcare Rehabilitation Auckland Ms Prudence Lennox President NZ Wound Care Society 15:30-16:00 Wound Management in Primary Care Overview Wounds we see in primary care Flap
SVS AVF Clinical Practice Guidelines Venous Ulcer
 Venous Ulcer SVS AVF Venous Ulcer Clinical Practice Guidelines Task Force Multispecialty committee members Thomas F. O Donnell, Jr., MD (Chair), Marc A. Passman, MD (Vice Chair), William A. Marston, MD,
Venous Ulcer SVS AVF Venous Ulcer Clinical Practice Guidelines Task Force Multispecialty committee members Thomas F. O Donnell, Jr., MD (Chair), Marc A. Passman, MD (Vice Chair), William A. Marston, MD,
DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS
 TOKUDA HOSPITAL SOFIA DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS MILENA STANEVA, MD, PhD Department of vascular surgery and angiology Venous thromboembolic disease continues to cause significant morbidity
TOKUDA HOSPITAL SOFIA DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS MILENA STANEVA, MD, PhD Department of vascular surgery and angiology Venous thromboembolic disease continues to cause significant morbidity
Imaging for Peripheral Vascular Disease
 Imaging for Peripheral Vascular Disease James G. Jollis, MD Director, Rex Hospital Cardiovascular Imaging Imaging for Peripheral Vascular Disease 54 year old male with exertional calf pain in his right
Imaging for Peripheral Vascular Disease James G. Jollis, MD Director, Rex Hospital Cardiovascular Imaging Imaging for Peripheral Vascular Disease 54 year old male with exertional calf pain in his right
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS
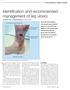 Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Identification and recommended management of leg ulcers Jill Robson RGN and Gerard Stansby MA, MChir, FRCS thickened skin, lipodermatosclerosis skin stained haemosiderin shallow ulcer irregular shape Our
Fig MHz cm/s. Table 1 Fig. 2. Fig. 3, 4. Fig. 5
 GE Fig. 1 3. 5 MHz 7 10 MHz 3. 5 5. 0 MHz B 10 20 cm/s Table 1 Fig. 2 Fig. 1 1 2 3 3 3 : 1 2 3 Fig. 3, 4 Fig. 5 Table 1 a b c Fig. 2 a B b B c Fig. 6 Table 1 Fig. 7 a b c Fig. 3 a AV b A VV c 1 cm 2 1
GE Fig. 1 3. 5 MHz 7 10 MHz 3. 5 5. 0 MHz B 10 20 cm/s Table 1 Fig. 2 Fig. 1 1 2 3 3 3 : 1 2 3 Fig. 3, 4 Fig. 5 Table 1 a b c Fig. 2 a B b B c Fig. 6 Table 1 Fig. 7 a b c Fig. 3 a AV b A VV c 1 cm 2 1
Venous Insufficiency Ulcer
 Disclosure NOTHING Venous Insufficiency Ulcer Venous Insufficiency Ulcer Also know as Venous Stasis Ulcer Ulcerative Venous Reflux Disease Statistics / Clinical Frequency Affects 2-5 % of the population
Disclosure NOTHING Venous Insufficiency Ulcer Venous Insufficiency Ulcer Also know as Venous Stasis Ulcer Ulcerative Venous Reflux Disease Statistics / Clinical Frequency Affects 2-5 % of the population
High Level Overview: Venous Anatomy of Lower Extremities. Anatomy of a Vein 5/11/2015. Barbara Deusterman, RN
 High Level Overview: Venous Anatomy of Lower Extremities Barbara Deusterman, RN What does this anatomy lecture have to do with visually guided sclerotherapy (VGS)? May 11, 2015 2 Anatomy of a Vein Almeida,
High Level Overview: Venous Anatomy of Lower Extremities Barbara Deusterman, RN What does this anatomy lecture have to do with visually guided sclerotherapy (VGS)? May 11, 2015 2 Anatomy of a Vein Almeida,
Physician s Vascular Interpretation Examination Content Outline
 Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Varicose Vein Information Sheet
 Neil Goldstein, MD Joseph Hewett, MD Board- Certified Physicians in Interventional, Diagnostic, and Vascular Radiology, Surgery, Vascular Surgery and Phlebology Varicose Vein Information Sheet PREVALENCE
Neil Goldstein, MD Joseph Hewett, MD Board- Certified Physicians in Interventional, Diagnostic, and Vascular Radiology, Surgery, Vascular Surgery and Phlebology Varicose Vein Information Sheet PREVALENCE
RECOGNITION AND ENDOVASCULAR TREATMENT OF CHRONIC VENOUS INSUFFICIENCY
 RECOGNITION AND ENDOVASCULAR TREATMENT OF CHRONIC VENOUS INSUFFICIENCY Paul Kramer, MD, FACC, FSCAI Liberty Cardiovascular Specialists Liberty Regional Heart and Vascular Center DISCLOSURES NONE Venous
RECOGNITION AND ENDOVASCULAR TREATMENT OF CHRONIC VENOUS INSUFFICIENCY Paul Kramer, MD, FACC, FSCAI Liberty Cardiovascular Specialists Liberty Regional Heart and Vascular Center DISCLOSURES NONE Venous
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Non-invasive examination
 Non-invasive examination Segmental pressure and Ankle-Brachial Index (ABI) The segmental blood pressure (SBP) examination is a simple, noninvasive method for diagnosing and localizing arterial disease.
Non-invasive examination Segmental pressure and Ankle-Brachial Index (ABI) The segmental blood pressure (SBP) examination is a simple, noninvasive method for diagnosing and localizing arterial disease.
A short review of diagnosis and compression therapy of chronic venous. insufficiency, Clinical picture and diagnosis A B S T R A C T WORDS
 A short review of diagnosis and compression therapy of chronic venous insufficiency N. Kecelj Leskovec, M. D. Pavlovi}, and T. Lunder A B S T R A C T Introduction: Chronic venous insufficiency (CVI) is
A short review of diagnosis and compression therapy of chronic venous insufficiency N. Kecelj Leskovec, M. D. Pavlovi}, and T. Lunder A B S T R A C T Introduction: Chronic venous insufficiency (CVI) is
Independent evaluation of BEMER physical vascular regulation therapy
 of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
Management of Lower Limb Ulcers. D. NAIK MBChB FRACS DDU
 Management of Lower Limb Ulcers D. NAIK MBChB FRACS DDU Ulcer A defect in the epithelium A failure to heal Ulcer Aetiology of Leg Ulcers Venous insufficiency Macrovascular arterial insufficiency Infectious
Management of Lower Limb Ulcers D. NAIK MBChB FRACS DDU Ulcer A defect in the epithelium A failure to heal Ulcer Aetiology of Leg Ulcers Venous insufficiency Macrovascular arterial insufficiency Infectious
Information about minimally-invasive vein therapy
 Information about minimallyinvasive vein therapy Table of Contents 2 Healthy Legs... 3 Modern Examination... 6 Compression Therapy... 7 Sclerotherapy... 8 MiniPhlebectomy... 10 Laser Therapy (Endolaser)...
Information about minimallyinvasive vein therapy Table of Contents 2 Healthy Legs... 3 Modern Examination... 6 Compression Therapy... 7 Sclerotherapy... 8 MiniPhlebectomy... 10 Laser Therapy (Endolaser)...
Vein Disease Treatment
 MP9241 Covered Service: Yes when meets criteria below Prior Authorization Required: Yes as indicated in 2.0, 3.0, 4.0 and 5.0 Additional Information: None Prevea360 Health Plan Medical Policy: Vein disease
MP9241 Covered Service: Yes when meets criteria below Prior Authorization Required: Yes as indicated in 2.0, 3.0, 4.0 and 5.0 Additional Information: None Prevea360 Health Plan Medical Policy: Vein disease
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
All WALES LYMPHOEDEMA GUIDANCE:
 All WALES LYMPHOEDEMA GUIDANCE: Lymphoedema Vascular Assessment Policy (Toe Brachial Pressure Index / TBPI) April 2013 Created by the All Wales Lymphoedema Service Leads 1 Background The presence of peripheral
All WALES LYMPHOEDEMA GUIDANCE: Lymphoedema Vascular Assessment Policy (Toe Brachial Pressure Index / TBPI) April 2013 Created by the All Wales Lymphoedema Service Leads 1 Background The presence of peripheral
Clinico-Anatomical and Radiological Correlation of Varicose Veins of Lower Limb A Cross-sectional Study
 ORIGINAL RESEARCH www.ijcmr.com Clinico-Anatomical and Radiological Correlation of Varicose Veins of Lower Limb A Cross-sectional Study Lalatendu Swain 1, Mamata Singh 2, Prabhat Nalini Rautray 3 ABSTRACT
ORIGINAL RESEARCH www.ijcmr.com Clinico-Anatomical and Radiological Correlation of Varicose Veins of Lower Limb A Cross-sectional Study Lalatendu Swain 1, Mamata Singh 2, Prabhat Nalini Rautray 3 ABSTRACT
Management of Lower Limb Ulcers. D. NAIK MBChB FRACS DDU
 Management of Lower Limb Ulcers D. NAIK MBChB FRACS DDU Ulcer A defect in the epithelium Ulcer A failure to heal Aetiology of Leg Ulcers Arterial Venous Neuropathic Vasculitic Infectious Neoplastic Lymphoedema
Management of Lower Limb Ulcers D. NAIK MBChB FRACS DDU Ulcer A defect in the epithelium Ulcer A failure to heal Aetiology of Leg Ulcers Arterial Venous Neuropathic Vasculitic Infectious Neoplastic Lymphoedema
Doppler ultrasound in the evaluation of chronic venous insufficiency: A step-by-step morphological and hemodynamic review
 Doppler ultrasound in the evaluation of chronic venous insufficiency: A step-by-step morphological and hemodynamic review Poster No.: C-3206 Congress: ECR 2010 Type: Educational Exhibit Topic: Vascular
Doppler ultrasound in the evaluation of chronic venous insufficiency: A step-by-step morphological and hemodynamic review Poster No.: C-3206 Congress: ECR 2010 Type: Educational Exhibit Topic: Vascular
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound
 Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
NCVH. Ultrasongraphy: State of the Art Vein Forum 2015 A Multidisciplinary Approach to Otptimizing Venous Circulation From Wounds to WOW
 Ultrasongraphy: State of the Art 2015 NCVH New Cardiovascular Horizons Vein Forum 2015 A Multidisciplinary Approach to Otptimizing Venous Circulation From Wounds to WOW Anil K. Chagarlamudi, M.D. Cardiovascular
Ultrasongraphy: State of the Art 2015 NCVH New Cardiovascular Horizons Vein Forum 2015 A Multidisciplinary Approach to Otptimizing Venous Circulation From Wounds to WOW Anil K. Chagarlamudi, M.D. Cardiovascular
Surgical Options for revascularisation P E T E R S U B R A M A N I A M
 Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Patient assessment and strategy making for endovenous treatment
 Patient assessment and strategy making for endovenous treatment Raghu Kolluri, MD Director Vascular Medicine OhioHealth Riverside Methodist Hospital Columbus, OH Disclosures Current Medtronic Consultant/
Patient assessment and strategy making for endovenous treatment Raghu Kolluri, MD Director Vascular Medicine OhioHealth Riverside Methodist Hospital Columbus, OH Disclosures Current Medtronic Consultant/
Appendix 1 to Direct Vision Sclerotherapy AUSTRALASIAN COLLEGE OF PHLEBOLOGY CLINICAL PROCEDURES. CP Direct Vision Sclerotherapy Clinical procedure
 Appendix 1 to Direct Vision Sclerotherapy AUSTRALASIAN COLLEGE OF PHLEBOLOGY CLINICAL PROCEDURES CP Direct Vision Sclerotherapy Clinical procedure 1 PURPOSE This procedure summarises the actions required
Appendix 1 to Direct Vision Sclerotherapy AUSTRALASIAN COLLEGE OF PHLEBOLOGY CLINICAL PROCEDURES CP Direct Vision Sclerotherapy Clinical procedure 1 PURPOSE This procedure summarises the actions required
Prevention and Management of Leg Ulcers
 EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Materials and Methods
 Veins and Lymphatics 2017; volume 6:6757 Initial patterns of unilateral great saphenous vein reflux in women with telangiectasias and varicose veins Carlos A. Engelhorn, 1,2 Ana Luiza D.V. Engelhorn, 1,2
Veins and Lymphatics 2017; volume 6:6757 Initial patterns of unilateral great saphenous vein reflux in women with telangiectasias and varicose veins Carlos A. Engelhorn, 1,2 Ana Luiza D.V. Engelhorn, 1,2
2017 Florida Vascular Society
 Current Management of Venous Leg Ulcers: How to Identify Patients with Correctable Venous Disease and Interventional Procedures to Heal and Prevent Recurrence 2017 Florida Vascular Society Bill Marston
Current Management of Venous Leg Ulcers: How to Identify Patients with Correctable Venous Disease and Interventional Procedures to Heal and Prevent Recurrence 2017 Florida Vascular Society Bill Marston
Schedule of Benefits. for Professional Fees Vascular Procedures
 Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
Wound Assessment Report
 Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Clinical Examination of VASCULAR PATIENTS. Stephanie Hirst & Alexander Sunde
 Clinical Examination of VASCULAR PATIENTS Stephanie Hirst & Alexander Sunde Goals of Medical History To record the patient s symptoms at time of presentation. To organize the events which have lead to
Clinical Examination of VASCULAR PATIENTS Stephanie Hirst & Alexander Sunde Goals of Medical History To record the patient s symptoms at time of presentation. To organize the events which have lead to
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2)
 Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
The role of ultrasound duplex in endovenous procedures
 The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device
 VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
VeinOPlus Vascular Peripheral Vascular & Wound Therapy Device Calf Muscle Pump Dysfunction Therapy Increases blood flow, accelerates wound healing, and improves CVD and PAD symptoms Tomorrow s Technology
Efficacy of Velcro Band Devices in Venous and. Mixed Arterio-Venous Patients
 Efficacy of Velcro Band Devices in Venous and Mixed Arterio-Venous Patients T. Noppeney Center for Vascular Diseases: Outpatient Dept. Obere Turnstrasse, Dept. for Vascular Surgery Martha-Maria Hospital
Efficacy of Velcro Band Devices in Venous and Mixed Arterio-Venous Patients T. Noppeney Center for Vascular Diseases: Outpatient Dept. Obere Turnstrasse, Dept. for Vascular Surgery Martha-Maria Hospital
The Peripheral Vascular System
 The Peripheral Vascular System Anatomy and Physiology Arteries Arteries contain 3 concentric layers of tissue: - the intima - the media - the adventitia The intima The endothelium of the intima has metabolic
The Peripheral Vascular System Anatomy and Physiology Arteries Arteries contain 3 concentric layers of tissue: - the intima - the media - the adventitia The intima The endothelium of the intima has metabolic
Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS
 Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS Asymptomatic mass - 38-40%will develop symptoms at a rate of 14%/yr Intermittent claudic ation (chronic ischemia) - 25%-40%
Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS Asymptomatic mass - 38-40%will develop symptoms at a rate of 14%/yr Intermittent claudic ation (chronic ischemia) - 25%-40%
OHTAC Recommendation. Endovascular Laser Treatment for Varicose Veins. Presented to the Ontario Health Technology Advisory Committee in November 2009
 OHTAC Recommendation Endovascular Laser Treatment for Varicose Veins Presented to the Ontario Health Technology Advisory Committee in November 2009 April 2010 Issue Background The Ontario Health Technology
OHTAC Recommendation Endovascular Laser Treatment for Varicose Veins Presented to the Ontario Health Technology Advisory Committee in November 2009 April 2010 Issue Background The Ontario Health Technology
When general causes such as cardiac or renal failure and hypoproteinaemia (which tend to affect both legs) have
 Part One: Assessment and Diagnosis THE REDISTRIBUTION OF FLUID FROM THE ARTERIAL END OF THE CAPILLARY TO THE VENOUS END (STARLING'S LAW) IS THE MECHANISM UNDERLYING ALMOST ALL CASES OF LIMB OEDEMA. This
Part One: Assessment and Diagnosis THE REDISTRIBUTION OF FLUID FROM THE ARTERIAL END OF THE CAPILLARY TO THE VENOUS END (STARLING'S LAW) IS THE MECHANISM UNDERLYING ALMOST ALL CASES OF LIMB OEDEMA. This
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship
 Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
How does compression really work?
 How does compression really work? Felizitas Pannier Private Practice Phlebology & Dermatology, Bonn, Germany Many thanks to Hugo Partsch, Horst Gerlach and Hans-Jürgen Thomä for some of the pictures Compression
How does compression really work? Felizitas Pannier Private Practice Phlebology & Dermatology, Bonn, Germany Many thanks to Hugo Partsch, Horst Gerlach and Hans-Jürgen Thomä for some of the pictures Compression
Prospective evaluation of chronic venous insufficiency based on foot venous pressure measurements and air plethysmography findings
 Prospective evaluation of chronic venous insufficiency based on foot venous pressure measurements and air plethysmography findings Masato Fukuoka, MD, Takaki Sugimoto, MD, and Yutaka Okita, MD, Kobe, Japan
Prospective evaluation of chronic venous insufficiency based on foot venous pressure measurements and air plethysmography findings Masato Fukuoka, MD, Takaki Sugimoto, MD, and Yutaka Okita, MD, Kobe, Japan
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS
 HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
Appendix D: Leg Ulcer Assessment Form
 Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Nursing Best Practice Guideline Appendix D: Ulcer Assessment Form Person Completing Assessment: Date: Client Name: Caf # CM# VON ID #: District CCAC ID # Address Telephone Home: Work: Date of Birth Y/M/D:
Arterial & Venous Ulcers. A Comprehensive Review Assessment & Management
 Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Arterial & Venous Ulcers A Comprehensive Review Assessment & Management 1 Objectives Understand Arterial & Venous disease Understand the etiology of lower extremities ulcers Understand assessment of lower
Progression of reflux patterns in saphenous veins of women with chronic venous valvular insufficiency
 Progression of reflux patterns in saphenous veins of women with chronic venous valvular insufficiency C A Engelhorn*, R Manetti*, M M Baviera*, G M Bombonato*, M Lonardoni*, M F Cassou, A L Engelhorn*
Progression of reflux patterns in saphenous veins of women with chronic venous valvular insufficiency C A Engelhorn*, R Manetti*, M M Baviera*, G M Bombonato*, M Lonardoni*, M F Cassou, A L Engelhorn*
Chronic Venous Disease: A Complex Disorder. A N Nicolaides
 Chronic Venous Disease: A Complex Disorder A N Nicolaides Emeritus Professor of Vascular Surgery, Imperial College, London. Hon. Professor of Surgery, University of Nicosia Medical School, Cyprus Disclosures
Chronic Venous Disease: A Complex Disorder A N Nicolaides Emeritus Professor of Vascular Surgery, Imperial College, London. Hon. Professor of Surgery, University of Nicosia Medical School, Cyprus Disclosures
Jordan M. Garrison, MD FACS, FASMBS
 Jordan M. Garrison, MD FACS, FASMBS Peripheral Arterial Disease (PAD) Near or Complete obstruction of > 1 Peripheral Artery Peripheral Venous reflux Disease Varicose Veins Chronic Venous Stasis Ulcer Disease
Jordan M. Garrison, MD FACS, FASMBS Peripheral Arterial Disease (PAD) Near or Complete obstruction of > 1 Peripheral Artery Peripheral Venous reflux Disease Varicose Veins Chronic Venous Stasis Ulcer Disease
Anatomy. Patterns of reflux. Technique. Testing Reflux time Patient position. Difficult! Learning. NOT system optimisation. Clinical Assesment
 Anatomy Patterns of reflux Awareness Technique Testing Reflux time Patient position Difficult! Learning NOT system optimisation Enlarged Clinical Assesment Twisted Where are the symptoms? Why they are
Anatomy Patterns of reflux Awareness Technique Testing Reflux time Patient position Difficult! Learning NOT system optimisation Enlarged Clinical Assesment Twisted Where are the symptoms? Why they are
Prof. Nabil CHAKFE et coll.
 Prof. Nabil CHAKFE et coll. For the Department of Vascular Surgery and Kidney Transplantation University Hospital of Strasbourg, FRANCE Popliteal artery entrapment: misdiagnosed Epidemiology Prevalence:
Prof. Nabil CHAKFE et coll. For the Department of Vascular Surgery and Kidney Transplantation University Hospital of Strasbourg, FRANCE Popliteal artery entrapment: misdiagnosed Epidemiology Prevalence:
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
