Prone Position in Percutaneous Nephrolithotomy and Postoperative Visual Loss
|
|
|
- Andrea Laureen Hill
- 5 years ago
- Views:
Transcription
1 Endourology and Stone Disease Prone Position in Percutaneous Nephrolithotomy and Postoperative Visual Loss Mahvash Agah, 1 Mahshid Ghasemi, 2 Fatemeh Roodneshin, 3 Badiozaman Radpay, 3 Siamak Moradian 4 Keywords: intraocular pressure, percutaneous nephrolithotomy, prone position, vision acuity 1 Anesthesiology Research Center, Shahid Labbafinejad Medical Center, Shahid Beheshti University of Medical Sciences,Tehran, Iran 2 Taleghani Medical Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran 3 Urology and Nephrology Research Center, Shahid Labbafinejad Medical Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran 4 Shahid Labbafinejad Medical Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran Corresponding Author: Fatemeh Roodneshin, MD Urology and Nephrology Research Center, Shahid Labbafinejad Medical Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran Tel/Fax: Dr_roodneshin_f07@yahoo.com Received December 10 Accepted March 11 Purpose: To study the simultaneous effects of prone position and anesthesia on intraocular pressure (IOP) and the time impact on post anesthesia visual loss development in percutaneous nephrolithotomy (PCNL). Materials and Methods: Twenty patients who were candidates for PCNL were recruited in this study. Intraocular pressure was measured in five occasions: 1. Base line; 2. Ten minutes after anesthesia (Supine-I); 3. Ten minutes after position change to prone (Prone-I); 4. At the end of the operation (Prone-II); and 5. Ten minutes after position change to supine (Supine-II). The data were analyzed by SPSS software using repeated measures ANOVA and paired t test. Results: The participants consisted of 17 (85%) men and 3 (15%) women, with the mean age of 44 years. The duration of the prone position was ± minutes. Intraocular pressure changed significantly in five positions (P =.000). It was lower in supine-i than baseline, higher in prone-i than base line and supine-i, lower in supine-ii than prone-ii, and highest in prone-ii (P =.000). There was a linear relationship between IOP and prone position duration (r = 0.67; P =.001). Conclusion: Intraocular pressure dropped significantly after anesthesia and increased in prone position. There was a linear relationship between IOP rise and the prone position duration, doubled within two hours. Therefore, in PCNL carried out in prone position, it is recommended to observe safety measures and necessary precautions for IOP rise and possible post anesthesia visual loss, particularly in glaucoma. INTRODUCTION Of peri-operative complications, post anesthesia visual loss (PVL) is one of the most important ones reported in numerous articles. (1-6) Post anesthesia visual loss is an unfortunate, horrifying, and rare complication that is among the legal complaints. (7) It has been mostly reported in spinal surgeries and the prone position. (3) Urol J. 11;8: Several factors, including hypotension, anemia, and the pressure on the eyes may lead to PVL. (2) However, some researchers have suggested that hemorrhage, changes in blood pressure, hematocrit level alterations, and the volume of fluid replacement during the operation might not be contributory factors in development of PVL. (7) Reduction Urology Journal Vol 8 No 3 Summer
2 in eye s perfusion, the volume of blood loss, and the replacement fluids have been mentioned as the most common factors that lead to PVL. Ischemic optic neuropathy (ION), in which either the anterior (AION) or the posterior (PION) section of the nerve is involved, is the most common cause of PVL. (6) Ho and colleagues studied the ION after the spinal cord surgeries in prone position and reported that mostly the external part of the nerve was affected by ischemia and was frequently bilateral (40% for AION and 47% for PION). (8) Unfortunately, nowadays, the routine check of the optic nerve blood flow is not carried out. (7) The anterior and posterior sections of the nerve are supplied separately by the posterior branches of the ciliary artery and perforating arteries, respectively. Over % of normal populations have abnormal autoregulation that is undetectable clinically. (9) Blood vessels are compressible easily at the posterior section of the optic nerve and with the alteration in the eye perfusion pressure, some patients become susceptible to ION, (10,11) and atherosclerosis worsens the situation. (11) In normal patients, reduction in the eye perfusion in the range of autoregulation is tolerable, but in the existence of atherosclerosis, there is a possibility of blood flow reduction in the nerve, (12) and patients with vascular impairment are at higher risk of developing ION. (10,11) Optic nerve is sensitive to acute bleeding; nonetheless, acute hemodilution is not precarious and therefore there is no need to extra blood. (6,7) Hemodilution and hypotension are routine in open heart surgery, but PVL is rare. (7) Generally, PVL is not caused by direct pressure on the eye globe, but the main factor is the effect of hemodynamic alterations on ocular perfusion pressure (OPP) that is the result of subtracting the intraocular pressure (IOP) from mean arterial pressure (MAP); OPP = MAP IOP. (13) Yet in ocular perfusion, the attention has been focused more on holding MAP normal or high, and IOP has been left relatively unnoticed, since even if MAP is steady, a high IOP prevents a proper OPP. Hypotension also decreases IOP, which in turn reduces OPP. (14) In a study on the effect of position on IOP in awake patients, the pressure raised from 13.5 mmhg in supine position to mmhg in the prone position. (15) Prone position causes an increase in the peritoneal pressure with subsequent increase in IOP, peak inspiratory pressure (PIP), and central vein pressure. In the patients not suffering from glaucoma, the peritoneal pressure during the laparoscopic surgery did not yield increased IOP in the lithotomy position, (16) but IOP increased in glaucomatous rabbits. (17) Intraocular pressure showed an increase in the anesthetized patients and the awake volunteers in the supine position with low head placement (Trendelenburg). The mechanism is the rise in the episcleral venous pressure. (9) Furthermore, general anesthesia reduces IOP. (18) The rise in PaCO 2 could increase IOP during the general anesthesia in the supine position, (19) but PaCO 2 does not change substantially during general anesthesia. () In a study, the rises of PaCO 2 and end-tidal carbon dioxide concentration (ETCO2) in the prone position were reported. (21) The balance between the prone position and general anesthesia plays an important role in OPP. Percutaneous nephrolithotomy (PCNL) is relatively a new technique and the treatment of choice for removing stones in the kidney, proximal ureter, inferior pole of the kidney, or infundibulopelvic and the stones accompanied by the evidence of obstruction. This operation usually results in low blood loss and the overall need for blood transfusion is less than 10%. (22) To carry out this operation, there is mostly a need to general anesthesia. Although PCNL is usually completed in prone position, performing it in the supine and flank positions is still under debate. (23-26) The aim of this study was to investigate the simultaneous effects of anesthesia and prone position on IOP during PCNL and the risk of developing PVL. MATERIALS AND METHODS This study was a non-controlled, nonrandomized, and non-blinded (pre post quasiexperimental design) clinical trial that was carried out on patients candidate for PCNL. All of them were in American Society of Anesthesiologists (ASA) class I to III. The written 192 Urology Journal Vol 8 No 3 Summer 11
3 informed consents were obtained from each participant. Patients with a history of either eye disease or eye surgery were excluded from the study. The demographic and clinical data were collected using a questionnaire. All the patients had hematocrits above 30% and the duration of patients fasting was 8 hours. First, electrocariography monitors, non-invasive sphygmomanometer, pulse oximetry, and nerve stimulator were connected to the patient. Both eyes were anesthetized by 0.5% tetracaine. Before prescription of any premedication, the pressures of both eyes were measured in supine position by Tono-Pen XL hand-held applanation tonometer (Baseline). The mean of 4 measurements with the right standard deviation of less than 5% was acceptable that otherwise the measurement was repeated. Anesthesia protocol was the same for all the patients and achieved as follows: Premedication with xylocaine 1.5 mg/kg and fentanyl 1 to 2 μg/ kg. Induction with nesdonal 3 to 5 mg/kg and atracurium 0.5 mg/kg and the continuation of the anesthesia by fentanyl 1 to 2 μg/kg/h infusion, halothane 0.5% to 0.6%, and N 2 O 50%. Mean arterial pressure was regulated at the range of % of wakefulness and ventilation on the basis of ETCO 2 30 to 35 mmhg. In order to maintain the intravascular volume during the operation, in addition to the precise compensation of the hemorrhage, 5 ml/kg normal saline was prescribed for each patient. Any subject with the hemorrhage of greater than 1000 cc was excluded from the study. By controlling train of four, the timing for intubation and the re-prescription of the muscle relaxants were determined that in the case of the existence of more than one twitch, muscle relaxant (0.1 mg/kg) was repeated. Particularly, at the time of the position change, patient was sustained flaccid and in deep anesthesia. The IOP was measured in the following stages: 1. Awakeness and in supine position (Baseline) 2. Ten minutes after induction and in supine position (Supine-I) 3. Ten minutes into acquiring prone position (Prone-I) 4. At the end of the operation in prone position (Prone-II) 5. Ten minutes into acquiring supine position (Supine-II) before the reverse injection and the change in depth of anesthesia Simultaneously, in the above-mentioned stages, PIP, end-tidal halothane (ET Hal), ETCO 2, pulse rate, saturation of peripheral oxygen (SPO 2 ), and MAP were measured as well. The XL hand-held tonometer was calibrated after each use. The change of position was carried out by the same team, considering all necessary precautions gently for all the patients. Applying pressure on the eyes was avoided during the prone position and a gelatinous head ring was placed under the patient s head without any contact with the eyes. The method of operation was unchanged. The surgeon, surgical equipment, the evaluators, and persons who collected the data were the same for all the patients. The patients were questioned concerning the visual acuity or any other visual disturbances in both eyes in the recovery room. Pre and postoperative hematocrit level as well as urine output and blood loss were measured. The data were analyzed by SPSS software (the Statistical Package for the Social Sciences, version 11.0, SPSS Inc., Chicago, Illinois, USA) using repeated measures ANOVA and paired t test. P values less than.05 were considered significant. RESULTS The participants consisted of 17 (85%) men and 3 (15%) women, with the mean age of 44 years. The duration of the prone position was ± minutes. No significant differences were observed regarding PIP, ETCO 2, MAP, SPO 2, and ET Hal in the five stages. Since the statistical differences were unavailable between the right-eye and the left-eye IOPs, we considered the left-eye IOP in our calculations. The measured IOP ranged between 12 and 40 mmhg and it was observed that IOP changed Urology Journal Vol 8 No 3 Summer
4 Patients mean intraocular pressures in five occasions Base line Supine I Prone I Prone II Supine II Total N 100 Mean (Range), mm/hg (14.00 to 17.00) (12.00 to 13.00) (.00 to 28.00) (37.00 to 40.00) (13.00 to 14.00) (12.00 to 40.00) Std. Deviation Std. Error E % Confidence Interval for Mean to to to to to to % Confidence Interval of Intraocular Pressure N - Base Line Supine I Prone I Prone II Supine II GROUPS Patients mean intraocular pressures in five positions in percutaneous nephrolithotomy significantly in the five positions (P =.000). The IOP in supine I (12.5 ± 0.5 mmhg) was lower than the baseline (15.42 ± 0.9 mmhg) (P =.000). The intraocular pressure in prone I (25.5 ± 1.5 mmhg) was higher than supine I and the baseline (P =.000). The IOP in prone II (38.9 ± 0.9 mmhg) was higher than all previous measurements (P =.000). The IOP in supine II (13.7 ± 0.4 mmhg) was lower than prone II (P = 0.000) (Table and Figure). There was a linear relationship between the IOP and duration of the prone position (r = 0.67; P = 0.001) that the IOP rose as the time elapsed. DISCUSSION To the best of our knowledge, this study is the first one on the IOP in PCNL and the effect of the duration of the prone position on the anesthetized patients. In this study, anesthesia reduced the IOP, which is in line with other studies showing that administration of anesthetic drugs, such as nesdonal and atracurium, resulted in reduction of the IOP. (27) The other finding is that the position change to prone leads to alteration of the IOP in a way that not only it compensates the reducing effects of the anesthetic drugs in 10 minutes, but also exceeds the baseline. The effects of the prone position have also been demonstrated in a study by Lam and Douthwaite, in which the IOP raised within 8 minutes after the change of position to prone. (15) They carried out the trial on awake volunteers. Our study showed that the increasing effect of the prone position on IOP is stronger than the reducing effects of general anesthesia on IOP. The most accurate method of measuring IOP over the time is its continuous and invasive measurement. This type of recording IOP has been reported in two groups of patients by implanting a probe into the anterior chamber of the eye for 96 hours. (28) However, we utilized Tono-Pen XL similar to the study by Lam and Douthwaite. (15) The accuracy of this device in comparison with the invasive method of probe implantation has been demonstrated by Setogawa and Kawai. (29) Rises in PaCO 2 and EtCO 2 have been reported in the prone position. (21) Since the rise of the PaCO 2 could increase the IOP, (21) we kept PaCO 2 unchanged from the beginning to the end of the anesthesia in order to abolish its interfering effects. A number of researchers induced a rise in the IOP by increasing the acute fluid administration. (25) In our study, we compensated not only the fluid loss, but also the patients received 5cc/ kg/h of fluid. The point that the intravascular volume change is capable of changing the IOP requires prospective studies. (27) Nonetheless, we maintained the fluid balance and the intravascular volume in a steady state in order to prevent the possible effects of the intravascular volume. Unlike the study by Pillunat and colleagues, 194 Urology Journal Vol 8 No 3 Summer 11
5 our patients were in a position completely in parallel to the horizontal surface, and therefore, the effects of increase or decrease in episcleral intravenous pressure due to the Trendelenburg position could not be measured in our study. (9) Fortunately, we did not observe any visual loss after anesthesia, but the first reported case of PVL after PCNL in the Labbafinejad Medical Center was a 75-year-old man with the history of diabetes mellitus, hyperlipidemia, and mild anemia. The patient had painless PVL in both eyes limited to light perception immediately after the operation. In ophthalmologic examination, the optic disc was pink without swelling and visual fields were severely affected; however, neuroimaging was normal. The visual fields and acuity improved dramatically in a matter of three months, but optic disc turned slightly pale and this was the first report of PION after PCNL. (30) According to the report by Roth and Barach, there is a possibility of PVL in the prone position, with hypotension, anemia, and direct pressure to the eyeball as risk factors. (7) In our study, we have avoided all the three mentioned factors and the fact that whether or not it is the reason for no visual loss after anesthesia is not assessable with this number of patients and it requires further studies. On the other hand, it does not seem that acute hemodilution is precarious. Since hemodilution occurs frequently in open heart surgery, but visual loss usually occurs after the spinal surgeries in prone position. (22) In a study on anesthetized patients in spinal surgery in prone position, Hunt and coworkers reported the rise in the IOP. Nevertheless, the duration of the operation, age, and body mass index have been mentioned as non-contributory factors. (31) According to the report of Ho and colleagues in assessing the reasons for ION duration, the prone position has been lengthy in all the subjects with the average of 450 minutes, which points to the time factor in the development of ION in prone position. (8) Also the reduction of OPP, intra-operative bleeding, anemia or hemodilution, and the infusion of large amounts of intravascular fluids are among the aggravating factors in ION. (8) In healthy volunteers, IOP increases with the acute rise in the fluid load, (25) and dehydration due to physical exercise reduces IOP. (32) The reduction in osmolarity during dialysis also increases IOP. (33) Prospective studies are required in order to demonstrate the relationship between the fluid balance and IOP in prone position. (27) In a comprehensive literature review on visual loss after non-ocular surgeries, it has been reported that risk of decrease in visual acuity and visual ability rises in case of preexisting diseases, such as hypertension, diabetes mellitus, sickle cell anemia, renal failure, gastrointestinal ulcer, narrow-angle glaucoma, vascular occlusive disease, cardiac disease, arteriosclerosis, polycythemia vera, and collagen vascular disorders. Furthermore, the precipitating factors for ION include prolonged hypotension, anemia, surgery, trauma, gastrointestinal bleeding, hemorrhage, shock, prone position, direct pressure on the globe, and long operation time. (34) In our study, the effect of the duration of the prone position on the rise of IOP was significant and other factors were ruled out. All the patients had the blood pressures of above 1 mmhg during the operation. By maintaining other conditions unchanged, it was tried to study the effect of the duration of the prone position on IOP in PCNL. After doubling the IOP from the normal level, (35) the risk of damage to the optic nerve starts, and according to our study the IOP was doubled and reached up to 40 mmhg after two hours. CONCLUSION Since in PCNL the rise of IOP in the prone position has a linear relationship with time and doubles within two hours, it is recommended that in the prone position surgeries, special attention has to be focused on the IOP. Prospective larger studies on the IOP with different setting are needed to confirm our results. CONFLICT OF INTEREST None declared. REFERENCES 1. Stoelting RK. APSF survey results identify safety issues priorities. Anesthesia Patient Safety Fouodation Urology Journal Vol 8 No 3 Summer
6 Newslett. 1999;14: Brown RH, Schauble JF, Miller NR. Anemia and hypotension as contributors to perioperative loss of vision. Anesthesiology. 1994;80: Cheng MA, Sigurdson W, Tempelhoff R, Lauryssen C. Visual loss after spine surgery: a survey. Neurosurgery. 00;46:625-30; discussion Myers MA, Hamilton SR, Bogosian AJ, Smith CH, Wagner TA. Visual loss as a complication of spine surgery. A review of 37 cases. Spine (Phila Pa 1976). 1997;22: Stevens WR, Glazer PA, Kelley SD, Lietman TM, Bradford DS. Ophthalmic complications after spinal surgery. Spine (Phila Pa 1976). 1997;22: Williams EL, Hart WM, Jr., Tempelhoff R. Postoperative ischemic optic neuropathy. Anesth Analg. 1995;80: Roth S, Barach P. Postoperative visual loss: still no answers--yet. Anesthesiology. 01;95: Ho VT, Newman NJ, Song S, Ksiazek S, Roth S. Ischemic optic neuropathy following spine surgery. J Neurosurg Anesthesiol. 05;17: Pillunat LE, Anderson DR, Knighton RW, Joos KM, Feuer WJ. Autoregulation of human optic nerve head circulation in response to increased intraocular pressure. Exp Eye Res. 1997;64: Hayreh SS. Posterior ischemic optic neuropathy. Ophthalmologica. 1981;182: Isayama Y, Hiramatsu K, Asakura S, Takahashi T. Posterior ischemic optic neuropathy. I. Blood supply of the optic nerve. Ophthalmologica. 1983;186: Hayreh SS, Bill A, Sperber GO. Effects of high intraocular pressure on the glucose metabolism in the retina and optic nerve in old atherosclerotic monkeys. Graefes Arch Clin Exp Ophthalmol. 1994;232: Hayreh SS. Anterior ischemic optic neuropathy. Clin Neurosci. 1997;4: Tsamparlakis J, Casey TA, Howell W, Edridge A. Dependence of intraocular pressure on induced hypotension and posture during surgical anaesthesia. Trans Ophthalmol Soc U K. 1980;100: Lam AK, Douthwaite WA. Does the change of anterior chamber depth or/and episcleral venous pressure cause intraocular pressure change in postural variation? Optom Vis Sci. 1997;74: Lentschener C, Benhamou D, Niessen F, Mercier FJ, Fernandez H. Intra-ocular pressure changes during gynaecological laparoscopy. Anaesthesia. 1996;51: Lentschener C, Leveque JP, Mazoit JX, Benhamou D. The effect of pneumoperitoneum on intraocular pressure in rabbits with alpha-chymotrypsin-induced glaucoma. Anesth Analg. 1998;86: Murphy DF. Anesthesia and intraocular pressure. Anesth Analg. 1985;64: Hvidberg A, Kessing SV, Fernandes A. Effect of changes in PCO2 and body positions on intraocular pressure during general anaesthesia. Acta Ophthalmol (Copenh). 1981;59: Pelosi P, Croci M, Calappi E, et al. The prone positioning during general anesthesia minimally affects respiratory mechanics while improving functional residual capacity and increasing oxygen tension. Anesth Analg. 1995;80: Wahba RW, Tessler MJ, Kardash KJ. Carbon dioxide tensions during anesthesia in the prone position. Anesth Analg. 1998;86: Thueroff JW, Gillitzer R. Percutaneous endourology and ureterorenoscopy. In: Tanagho EA, McAninch JW, eds. Smith s general Urology. 17 ed. New York: McGraw-Hill; 08: Liu L, Zheng S, Xu Y, Wei Q. Systematic review and meta-analysis of percutaneous nephrolithotomy for patients in the supine versus prone position. J Endourol. 10;24: Wu P, Wang L, Wang K. Supine versus prone position in percutaneous nephrolithotomy for kidney calculi: a meta-analysis. Int Urol Nephrol. 11;43: Miano R, Scoffone C, De Nunzio C, et al. Position: prone or supine is the issue of percutaneous nephrolithotomy. J Endourol. 10;24: Karami H, Rezaei A, Mohammadhosseini M, Javanmard B, Mazloomfard M, Lotfi B. Ultrasonography-guided percutaneous nephrolithotomy in the flank position versus fluoroscopy-guided percutaneous nephrolithotomy in the prone position: a comparative study. J Endourol. 10;24: Cheng MA, Todorov A, Tempelhoff R, McHugh T, Crowder CM, Lauryssen C. The effect of prone positioning on intraocular pressure in anesthetized patients. Anesthesiology. 01;95: Hoh H, Schwanengel M. [Continuous intraocular pressure measurement over several days with the Codman Microsensor--a case report]. Klin Monbl Augenheilkd. 1999;215: Setogawa A, Kawai. Measurement of intraocular pressure by both invasive and noninvasive techniques in rabbits exposed to head-down tilt. Jpn J Physiol. 1998;48: Pakravan M, Kiavash V, Moradian S. Posterior Ischemic Optic Neuropathy Following Percutaneous Nephrolithotomy. JOVR. 08;2: Hunt K, Bajekal R, Calder I, Meacher R, Eliahoo J, Acheson JF. Changes in intraocular pressure in anesthetized prone patients. J Neurosurg Anesthesiol. 04;16: Martin B, Harris A, Hammel T, Malinovsky V. Mechanism of exercise-induced ocular hypotension. Invest Ophthalmol Vis Sci. 1999;40: Tawara A. [Intraocular pressure during hemodialysis]. J UOEH. 00;22: Rupp-Montpetit K, Moody ML. Visual loss as a complication of nonophthalmologic surgery: a review of the literature. AANA J. 04;72: Salmon JF. Glaucoma. In: Riordan-Eva P, ed. Vaughan and Asbury s general ophthalmology. 17 ed. New York: Lange Medical Books/McGraw-Hill; 08: Urology Journal Vol 8 No 3 Summer 11
Materials and Methods
 Anesthesiology 2001; 95:1351 5 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. The Effect of Prone Positioning on Intraocular Pressure in Anesthetized Patients Mary
Anesthesiology 2001; 95:1351 5 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. The Effect of Prone Positioning on Intraocular Pressure in Anesthetized Patients Mary
The Effect of Head Inclination on Intraocular Pressure in the Prone Position
 Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 11-11-2017 The
Rhode Island College Digital Commons @ RIC Master's Theses, Dissertations, Graduate Research and Major Papers Overview Master's Theses, Dissertations, Graduate Research and Major Papers 11-11-2017 The
The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery
 The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery The Case: Upon awakening from anesthesia, he is blind in both eyes After Non-Ocular Surgeries Nancy J. Newman,
The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery The Case: Upon awakening from anesthesia, he is blind in both eyes After Non-Ocular Surgeries Nancy J. Newman,
Perioperative Visual Loss
 Perioperative Visual Loss Associated with Spine Surgery Agina M. Kempen, CRNA Chief Nurse Anesthetist St. Clair Hospital Pittsburgh, PA Website/Resources: www.asaclosedclaims.org Miller s s Anesthesia
Perioperative Visual Loss Associated with Spine Surgery Agina M. Kempen, CRNA Chief Nurse Anesthetist St. Clair Hospital Pittsburgh, PA Website/Resources: www.asaclosedclaims.org Miller s s Anesthesia
POSTOPERATIVE vision loss after spine surgery is a
 Effects of Crystalloid versus Colloid and the -2 Agonist Brimonidine versus Placebo on Intraocular Pressure during Prone Spine Surgery A Factorial Randomized Trial Ehab Farag, M.D., F.R.C.A.,* Daniel I.
Effects of Crystalloid versus Colloid and the -2 Agonist Brimonidine versus Placebo on Intraocular Pressure during Prone Spine Surgery A Factorial Randomized Trial Ehab Farag, M.D., F.R.C.A.,* Daniel I.
Vision loss is a devastating perioperative complication
 Intraocular Pressure in Pediatric Patients During Prone Surgery Peter Szmuk, MD,* Jeffrey W. Steiner, DO,* Radu B. Pop, MS,* Jing You, MS, David R. Weakley, Jr., MD, Dale M. Swift, MD, and Daniel I. Sessler,
Intraocular Pressure in Pediatric Patients During Prone Surgery Peter Szmuk, MD,* Jeffrey W. Steiner, DO,* Radu B. Pop, MS,* Jing You, MS, David R. Weakley, Jr., MD, Dale M. Swift, MD, and Daniel I. Sessler,
Bilateral Posterior Ischemic Optic Neuropathy in a Patient with Severe Diabetic Ketoacidosis
 Bilateral Posterior Ischemic Optic Neuropathy in a Patient with Severe Diabetic Ketoacidosis The Harvard community has made this article openly available. Please share how this access benefits you. Your
Bilateral Posterior Ischemic Optic Neuropathy in a Patient with Severe Diabetic Ketoacidosis The Harvard community has made this article openly available. Please share how this access benefits you. Your
A,kCetazolamide lowers intraocular pressure
 Ocular and systemic effects of acetazolamide in nephrectomized rabbits Zvi Friedman,* Theodore Krupin, and Bernard Becker The effects of acetazolamide on intraocular pressure (IOP) were studied on rabbits
Ocular and systemic effects of acetazolamide in nephrectomized rabbits Zvi Friedman,* Theodore Krupin, and Bernard Becker The effects of acetazolamide on intraocular pressure (IOP) were studied on rabbits
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion
 Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006.
 Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006 Introduction Laparoscopic surgery started in the mid 1950s. In recent
Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006 Introduction Laparoscopic surgery started in the mid 1950s. In recent
Respiratory Depression and Considerations for Monitoring Following Ophthalmologic Surgery
 Respiratory Depression and Considerations for Monitoring Following Ophthalmologic Surgery Athir Morad, M.D. Division of Neurocritical care Departments of Anesthesiology/ Critical Care Medicine and Neurology
Respiratory Depression and Considerations for Monitoring Following Ophthalmologic Surgery Athir Morad, M.D. Division of Neurocritical care Departments of Anesthesiology/ Critical Care Medicine and Neurology
ISSN X (Print) Research Article. India 3,4 Research Assistant, Institute of Nephro-Urology, Bangalore, India
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(1A):8-12 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(1A):8-12 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Observational study evaluating variation of intra-ocular pressure (IOP) with positional change during colorectal laparoscopic surgery
 Observational study evaluating variation of intra-ocular pressure (IOP) with positional change during colorectal laparoscopic surgery Abstract Background The incidence of perioperative visual loss following
Observational study evaluating variation of intra-ocular pressure (IOP) with positional change during colorectal laparoscopic surgery Abstract Background The incidence of perioperative visual loss following
General Versus Spinal Anesthesia in Percutaneous Nephrolithotomy
 ENDOUROLOGY AND STONE DISEASE General Versus Spinal Anesthesia in Percutaneous Nephrolithotomy Sadrollah Mehrabi, 1 Ali Mousavi Zadeh, 1 Mehdi Akbartabar Toori, 1 Farhad Mehrabi 2 1 Social Determinants
ENDOUROLOGY AND STONE DISEASE General Versus Spinal Anesthesia in Percutaneous Nephrolithotomy Sadrollah Mehrabi, 1 Ali Mousavi Zadeh, 1 Mehdi Akbartabar Toori, 1 Farhad Mehrabi 2 1 Social Determinants
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Efficacy of the Valsalva Maneuver on Needle Projection Pain and Hemodynamic Responses During Spinal Puncture
 156 Research Paper International Journal of Medical Sciences 2011; 8(2):156-160 Ivyspring International Publisher. All rights reserved. Efficacy of the Valsalva Maneuver on Needle Projection Pain and Hemodynamic
156 Research Paper International Journal of Medical Sciences 2011; 8(2):156-160 Ivyspring International Publisher. All rights reserved. Efficacy of the Valsalva Maneuver on Needle Projection Pain and Hemodynamic
Perioperative Ischemic Optic Neuropathy
 Anesthesiology 2009; 110:246 53 Copyright 2009, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Perioperative Ischemic Optic Neuropathy A Case Control Analysis of 126,666
Anesthesiology 2009; 110:246 53 Copyright 2009, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Perioperative Ischemic Optic Neuropathy A Case Control Analysis of 126,666
CLASS-y Laser Treats Glaucoma
 Article # 404 Comments About the Author Released: Author: Category: March 12th, 2014 Issue #0314 Ehud Assia Feature S S S S S CLASS-y Laser Treats Glaucoma Transforming complex, invasive and risky glaucoma
Article # 404 Comments About the Author Released: Author: Category: March 12th, 2014 Issue #0314 Ehud Assia Feature S S S S S CLASS-y Laser Treats Glaucoma Transforming complex, invasive and risky glaucoma
Anaesthetic considerations for laparoscopic surgery in canines
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Anaesthetic considerations for laparoscopic surgery in canines Author : Chris Miller Categories : Canine, Companion animal,
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Anaesthetic considerations for laparoscopic surgery in canines Author : Chris Miller Categories : Canine, Companion animal,
Disclosures. Closed Claims Reports: Review of Anesthetic Complications. ASA Closed Claims Database. Outline
 Closed Claims Reports: Review of Anesthetic Complications Disclosures Funded by NHLBI & Hamilton Endowment Funds (UCSF Department of Anesthesia). Jae-Woo Lee, MD Associate Professor in Residence University
Closed Claims Reports: Review of Anesthetic Complications Disclosures Funded by NHLBI & Hamilton Endowment Funds (UCSF Department of Anesthesia). Jae-Woo Lee, MD Associate Professor in Residence University
Anesthesia for Total Hip and Knee Arthroplasty
 Anesthesia for Total Hip and Knee Arthroplasty Typical approach Describe anesthesia technique Rather Describe issues with THA and TKA How anesthesia can modify Issues Total Hip Total Knee Blood Loss ++
Anesthesia for Total Hip and Knee Arthroplasty Typical approach Describe anesthesia technique Rather Describe issues with THA and TKA How anesthesia can modify Issues Total Hip Total Knee Blood Loss ++
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
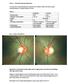 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
3 years experience of working in OB&GYN, general surgery operating room of the Ershad hospital, Karaj
 ALIREZA JAFARI APT#4.N#14.Sarab Ave,Azarshahr St, Shariati St Tehran,IRAN PHONE;00982122887568 00989123021232(cell) alirezajaffari@sbmu.ac.ir Personal Information Marital status :married Nationality :Iranian
ALIREZA JAFARI APT#4.N#14.Sarab Ave,Azarshahr St, Shariati St Tehran,IRAN PHONE;00982122887568 00989123021232(cell) alirezajaffari@sbmu.ac.ir Personal Information Marital status :married Nationality :Iranian
10/27/2013. Optic Red Herrings
 Optic Red Herrings 1 Optic neuropathy Compressive Inflammatory Toxic Glaucomatous Ischemic Post traumatic GLAUCOMATOUS OPTIC NEUROPATHY Glaucoma: Traditionally defined as a progressive optic neuropathy
Optic Red Herrings 1 Optic neuropathy Compressive Inflammatory Toxic Glaucomatous Ischemic Post traumatic GLAUCOMATOUS OPTIC NEUROPATHY Glaucoma: Traditionally defined as a progressive optic neuropathy
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
General surgery. Thyroid surgery. Physiological response to pneumoperitoneum. Bowel resection
 General surgery Thyroid surgery Physiological response to pneumoperitoneum Bowel resection General surgery 3.D.9.1 James Mitchell (December 24, 2003) Thyroid surgery Preoperative Assessment Routine, plus
General surgery Thyroid surgery Physiological response to pneumoperitoneum Bowel resection General surgery 3.D.9.1 James Mitchell (December 24, 2003) Thyroid surgery Preoperative Assessment Routine, plus
25. Fluid Management and Renal Function During a Laparoscopic Case Done Under CO 2 Pneumoperitoneum
 25. Fluid Management and Renal Function During a Laparoscopic Case Done Under CO 2 Pneumoperitoneum Gamal Mostafa, M.D. Frederick L. Greene, M.D. Minimally invasive surgery aims to attenuate the stress
25. Fluid Management and Renal Function During a Laparoscopic Case Done Under CO 2 Pneumoperitoneum Gamal Mostafa, M.D. Frederick L. Greene, M.D. Minimally invasive surgery aims to attenuate the stress
The American Society of Anesthesiologists Postoperative Visual Loss Registry
 CLINICAL INVESTIGATIONS Anesthesiology 2006; 105:652 9 Copyright 2006, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. The American Society of Anesthesiologists Postoperative
CLINICAL INVESTIGATIONS Anesthesiology 2006; 105:652 9 Copyright 2006, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. The American Society of Anesthesiologists Postoperative
9/25/2017 CASE. 67 years old On 2 topical meds since 3 years. Rx: +3.0 RE LE
 CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
Management of Traumatic Brain Injury (and other neurosurgical emergencies)
 Management of Traumatic Brain Injury (and other neurosurgical emergencies) Laurel Moore, M.D. University of Michigan 22 nd Annual Review February 7, 2019 Greetings from Michigan! Objectives for Today s
Management of Traumatic Brain Injury (and other neurosurgical emergencies) Laurel Moore, M.D. University of Michigan 22 nd Annual Review February 7, 2019 Greetings from Michigan! Objectives for Today s
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study
 Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University.
 Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Study Of Effects Of Varying Durations Of Pre-Oxygenation. J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh
 ISPUB.COM The Internet Journal of Anesthesiology Volume 20 Number 1 J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh Citation J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 20 Number 1 J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh Citation J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh.. The Internet
Anterior Ischemic Optic Neuropathy (AION)
 Anterior Ischemic Optic Neuropathy (AION) Your doctor thinks you have suffered an episode of anterior ischemic optic neuropathy (AION). This is the most common cause of sudden decreased vision in patients
Anterior Ischemic Optic Neuropathy (AION) Your doctor thinks you have suffered an episode of anterior ischemic optic neuropathy (AION). This is the most common cause of sudden decreased vision in patients
1/31/2018. Course Objectives. Diagnostic Testing. Optic Nerve Damage ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY TECHNICIAN: -SDP
 ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY KNOW THE DISEASE PROCESS TECHNICIAN: EXPLAIN PROCESS OF EXAMINATION Presenters: Dana McMahan, COA Nicole Smith, COA Engage with patient s, help alleviate
ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY KNOW THE DISEASE PROCESS TECHNICIAN: EXPLAIN PROCESS OF EXAMINATION Presenters: Dana McMahan, COA Nicole Smith, COA Engage with patient s, help alleviate
Anesthetic Management of Laparoscopic Surgery for a Patient with
 Anesthetic Management of Laparoscopic Surgery for a Patient with a Ventriculoperitoneal shunt Abstract With the advances in the management of hydrocephalus, patients with ventriculoperitoneal shunt are
Anesthetic Management of Laparoscopic Surgery for a Patient with a Ventriculoperitoneal shunt Abstract With the advances in the management of hydrocephalus, patients with ventriculoperitoneal shunt are
General OR Rotations GOALS & OBJECTIVES
 General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
ANESTHESIA EXAM (four week rotation)
 SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
MA HOSSAIN. Summary: Journal of Bangladesh College of Physicians and Surgeons Vol. 29, No. 2, April 2011
 Journal of Bangladesh College of Physicians and Surgeons Vol. 29, No. 2, April 2011 Comparative Study of Stone Pulverization and Clearance Rate between Patients Treated by ESWL Under Spinal Anesthesia
Journal of Bangladesh College of Physicians and Surgeons Vol. 29, No. 2, April 2011 Comparative Study of Stone Pulverization and Clearance Rate between Patients Treated by ESWL Under Spinal Anesthesia
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Relationship between Diabetes and Intraocular Pressure
 Relationship between Diabetes and Intraocular Pressure Mohammad Khalaj, Sajjad Fereydooni, and Ameneh Barikani Children Growth Research Center, Qazvin University of Medical Sciences, Qazvin, Iran ORIGINAL
Relationship between Diabetes and Intraocular Pressure Mohammad Khalaj, Sajjad Fereydooni, and Ameneh Barikani Children Growth Research Center, Qazvin University of Medical Sciences, Qazvin, Iran ORIGINAL
Original Article Influence of butorphanol on the postoperative remifentanil hyperalgesia
 Int J Clin Exp Med 2016;9(2):4685-4689 www.ijcem.com /ISSN:1940-5901/IJCEM0017991 Original Article Influence of butorphanol on the postoperative remifentanil hyperalgesia Chen Lv, Hui Zheng, Mingyang Wei,
Int J Clin Exp Med 2016;9(2):4685-4689 www.ijcem.com /ISSN:1940-5901/IJCEM0017991 Original Article Influence of butorphanol on the postoperative remifentanil hyperalgesia Chen Lv, Hui Zheng, Mingyang Wei,
10. Severe traumatic brain injury also see flow chart Appendix 5
 10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
Anesthesia Final Exam
 Anesthesia Final Exam 1) For a patient who is chronically taking the following medications, which two should be withheld on the day of surgery? a) Lasix b) Metoprolol c) Glucophage d) Theodur 2) A 51 year
Anesthesia Final Exam 1) For a patient who is chronically taking the following medications, which two should be withheld on the day of surgery? a) Lasix b) Metoprolol c) Glucophage d) Theodur 2) A 51 year
Neuropathy (NAION) and Avastin. Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013
 Non Arteritic Ischemic Optic Neuropathy (NAION) and Avastin Shalom Kelman, MD Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013 Anterior Ischemic Optic Neuropathy Acute, painless, visual loss,
Non Arteritic Ischemic Optic Neuropathy (NAION) and Avastin Shalom Kelman, MD Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013 Anterior Ischemic Optic Neuropathy Acute, painless, visual loss,
MD (Anaesthesiology) Title (Plan of Thesis) (Session )
 S.No. 1. COMPARATIVE STUDY OF CENTRAL VENOUS CANNULATION USING ULTRASOUND GUIDANCE VERSUS LANDMARK TECHNIQUE IN PAEDIATRIC CARDIAC PATIENT. 2. TO EVALUATE THE ABILITY OF SVV OBTAINED BY VIGILEO-FLO TRAC
S.No. 1. COMPARATIVE STUDY OF CENTRAL VENOUS CANNULATION USING ULTRASOUND GUIDANCE VERSUS LANDMARK TECHNIQUE IN PAEDIATRIC CARDIAC PATIENT. 2. TO EVALUATE THE ABILITY OF SVV OBTAINED BY VIGILEO-FLO TRAC
Original Article Comparison of General versus Spinal Anesthesia in Patients undergoing Percutaneous Nephrolithotomy: A Prospective Randomized Study
 ISSN: 2091-2331 (PRINT) 2091-234X (ONLINE) Journal of Nobel Medical College Available Online: www.nepjol.info, www.nobelmedicalcollege.com.np Volume 5, Number 1, Issue 8, January-July 2016, 37-42 Original
ISSN: 2091-2331 (PRINT) 2091-234X (ONLINE) Journal of Nobel Medical College Available Online: www.nepjol.info, www.nobelmedicalcollege.com.np Volume 5, Number 1, Issue 8, January-July 2016, 37-42 Original
CEA and cerebral protection Volodymyr labinskyy, MD
 CEA and cerebral protection Volodymyr labinskyy, MD VA Hospital 7/26/2012 63 year old male presents for the vascular evaluation s/p TIA in January 2012 PMH: HTN, long term active smoker, Hep C PSH: None
CEA and cerebral protection Volodymyr labinskyy, MD VA Hospital 7/26/2012 63 year old male presents for the vascular evaluation s/p TIA in January 2012 PMH: HTN, long term active smoker, Hep C PSH: None
INTRACEREBRAL HEMORRHAGE FOLLOWING ENUCLEATION: A RESULT OF SURGERY OR ANESTHESIA?
 INTRACEREBRAL HEMORRHAGE FOLLOWING ENUCLEATION: A RESULT OF SURGERY OR ANESTHESIA? - A Case Report - DIDEM DAL *, AYDIN ERDEN *, FATMA SARICAOĞLU * AND ULKU AYPAR * Summary Choroidal melanoma is the most
INTRACEREBRAL HEMORRHAGE FOLLOWING ENUCLEATION: A RESULT OF SURGERY OR ANESTHESIA? - A Case Report - DIDEM DAL *, AYDIN ERDEN *, FATMA SARICAOĞLU * AND ULKU AYPAR * Summary Choroidal melanoma is the most
Pilot Of Spontaneous Breathing Vs. Ventilated Model For Hemorrhage And Resuscitation In The Rabbit
 Article ID: WMC001137 Pilot Of Spontaneous Breathing Vs. Ventilated Model For Hemorrhage And Resuscitation In The Rabbit Author(s):Dr. Jonathan S. Jahr, MD, Dr. Robert A. Gunther, PhD, Dr. Bernd Driessen,
Article ID: WMC001137 Pilot Of Spontaneous Breathing Vs. Ventilated Model For Hemorrhage And Resuscitation In The Rabbit Author(s):Dr. Jonathan S. Jahr, MD, Dr. Robert A. Gunther, PhD, Dr. Bernd Driessen,
Spine surgeons are concerned about uncontrollable
 The Effect of Patient Positioning on Intraabdominal Pressure and Blood Loss in Spinal Surgery Chang Kil Park, MD Department of Anesthesiology, Eulji University School of Medicine, Taejon, Korea Intraabdominal
The Effect of Patient Positioning on Intraabdominal Pressure and Blood Loss in Spinal Surgery Chang Kil Park, MD Department of Anesthesiology, Eulji University School of Medicine, Taejon, Korea Intraabdominal
Postoperative cognitive dysfunction a neverending story
 Postoperative cognitive dysfunction a neverending story Adela Hilda Onuţu, MD, PhD Cluj-Napoca, Romania adela_hilda@yahoo.com No conflict of interest Contents Postoperative cognitive dysfunction (POCD)
Postoperative cognitive dysfunction a neverending story Adela Hilda Onuţu, MD, PhD Cluj-Napoca, Romania adela_hilda@yahoo.com No conflict of interest Contents Postoperative cognitive dysfunction (POCD)
POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO
 POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO MD (ANAESTHESIOLOGY) FINAL EXAMINATION AUGUST 2013 Date : 2 nd August 2013 Time : 1.00 p.m. 4.00 p.m. Answer any three questions. Answer each question
POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO MD (ANAESTHESIOLOGY) FINAL EXAMINATION AUGUST 2013 Date : 2 nd August 2013 Time : 1.00 p.m. 4.00 p.m. Answer any three questions. Answer each question
The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus
 The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus Received: 25/4/2016 Accepted: 8/12/2016 Introduction Diabetic papillopathy is an atypical form of non-arteritic anterior ischemic
The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus Received: 25/4/2016 Accepted: 8/12/2016 Introduction Diabetic papillopathy is an atypical form of non-arteritic anterior ischemic
福島県立医科大学学術成果リポジトリ. Title laparoscopic adrenalectomy in patie pheochromocytoma. Midori; Iida, Hiroshi; Murakawa, Ma
 福島県立医科大学学術成果リポジトリ Examination of the usefulness of no Title variation monitoring for adjusting laparoscopic adrenalectomy in patie pheochromocytoma Isosu, Tsuyoshi; Obara, Shinju; Oha Author(s) Atsuyuki;
福島県立医科大学学術成果リポジトリ Examination of the usefulness of no Title variation monitoring for adjusting laparoscopic adrenalectomy in patie pheochromocytoma Isosu, Tsuyoshi; Obara, Shinju; Oha Author(s) Atsuyuki;
Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
NEPTUNE RED BANK BRICK
 NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
ICU treatment of the trauma patient. Intensive Care Training Program Radboud University Medical Centre Nijmegen
 ICU treatment of the trauma patient Intensive Care Training Program Radboud University Medical Centre Nijmegen Christian Kleber Surgical Intensive Care Unit - The trauma surgery Perspective Langenbecks
ICU treatment of the trauma patient Intensive Care Training Program Radboud University Medical Centre Nijmegen Christian Kleber Surgical Intensive Care Unit - The trauma surgery Perspective Langenbecks
NEOVASCULAR GLAUCOMA IN A NIGERIAN AFRICAN POPULATION
 October 2006 E AST AFRICAN MEDICAL JOURNAL 559 East African Medical Journal Vol. 83 No. 10 October 2006 NEOVASCULAR GLAUCOMA IN A NIGERIAN AFRICAN POPULATION: A.O. Ashaye, FWACS, MSc, Department of Ophthalmology,
October 2006 E AST AFRICAN MEDICAL JOURNAL 559 East African Medical Journal Vol. 83 No. 10 October 2006 NEOVASCULAR GLAUCOMA IN A NIGERIAN AFRICAN POPULATION: A.O. Ashaye, FWACS, MSc, Department of Ophthalmology,
Science & Technologies
 STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
Disclosures. Anesthesia for Endovascular Treatment of Acute Ischemic Stroke. Acute Ischemic Stroke. Acute Stroke = Medical Emergency!
 Disclosures Anesthesia for Endovascular Treatment of Acute Ischemic Stroke I have nothing to disclose. Chanhung Lee MD, PhD Associate Professor Anesthesia and perioperative Care Acute Ischemic Stroke 780,000
Disclosures Anesthesia for Endovascular Treatment of Acute Ischemic Stroke I have nothing to disclose. Chanhung Lee MD, PhD Associate Professor Anesthesia and perioperative Care Acute Ischemic Stroke 780,000
Ureteroscopic and Extracorporeal Shock Wave Lithotripsy for Rather Large Renal Pelvis Calculi
 Endourology and Stone Disease Ureteroscopic and Extracorporeal Shock Wave Lithotripsy for Rather Large Renal Pelvis Calculi Kamyar Tavakkoli Tabasi, Mehri Baghban Haghighi Introduction: The aim of this
Endourology and Stone Disease Ureteroscopic and Extracorporeal Shock Wave Lithotripsy for Rather Large Renal Pelvis Calculi Kamyar Tavakkoli Tabasi, Mehri Baghban Haghighi Introduction: The aim of this
Paediatric neuraxial anaesthesia asleep or awake, what is the best for safety?
 ISPUB.COM The Internet Journal of Anesthesiology Volume 21 Number 1 Paediatric neuraxial anaesthesia asleep or awake, what is the best for safety? A Shabana, A Shorrab Citation A Shabana, A Shorrab. Paediatric
ISPUB.COM The Internet Journal of Anesthesiology Volume 21 Number 1 Paediatric neuraxial anaesthesia asleep or awake, what is the best for safety? A Shabana, A Shorrab Citation A Shabana, A Shorrab. Paediatric
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Activated partial thromboplastin time abnormality, perioperative approach to, 104 105 Acute kidney injury, perioperative, 89 99 early
Index Note: Page numbers of article titles are in boldface type. A Activated partial thromboplastin time abnormality, perioperative approach to, 104 105 Acute kidney injury, perioperative, 89 99 early
How to maintain optimal perfusion during Cardiopulmonary By-pass. Herdono Poernomo, MD
 How to maintain optimal perfusion during Cardiopulmonary By-pass Herdono Poernomo, MD Cardiopulmonary By-pass Target Physiologic condition as a healthy person Everything is in Normal Limit How to maintain
How to maintain optimal perfusion during Cardiopulmonary By-pass Herdono Poernomo, MD Cardiopulmonary By-pass Target Physiologic condition as a healthy person Everything is in Normal Limit How to maintain
Diabetic Retinopathy and its Impact on Ocular Heamodynamics during Local Anesthesia Comparing Peribulbar and Subtenon in Phacoemulsification
 Med. J. Cairo Univ., Vol. 84, No. 2, December: 169-173, 2016 www.medicaljournalofcairouniversity.net Diabetic Retinopathy and its Impact on Ocular Heamodynamics during Local Anesthesia Comparing Peribulbar
Med. J. Cairo Univ., Vol. 84, No. 2, December: 169-173, 2016 www.medicaljournalofcairouniversity.net Diabetic Retinopathy and its Impact on Ocular Heamodynamics during Local Anesthesia Comparing Peribulbar
Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD
 Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD July 26, 2010 Chief Complaint: New floaters in both eyes. History of Present
Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD July 26, 2010 Chief Complaint: New floaters in both eyes. History of Present
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Changes in intraocular pressure during low dose intravenous sedation with propofol before cataract
 British Journal of Ophthalmology 1995; 79: 1093-1097 Department of Ophthalmology, Indiana University School ofmedicine, and Roudebush Veteran's Hospital of Indianapolis, Indiana, USA S Neel R Deitch Jr
British Journal of Ophthalmology 1995; 79: 1093-1097 Department of Ophthalmology, Indiana University School ofmedicine, and Roudebush Veteran's Hospital of Indianapolis, Indiana, USA S Neel R Deitch Jr
Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant
 Original Article Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant Mirmohammad Taghi Mortazavi, 1 Masood Parish, 1 Naghi Abedini, 2
Original Article Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant Mirmohammad Taghi Mortazavi, 1 Masood Parish, 1 Naghi Abedini, 2
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
Postural effects on intraocular pressure and ocular perfusion pressure in patients with non-arteritic anterior ischemic optic neuropathy
 Yang et al. BMC Ophthalmology (2017) 17:47 DOI 10.1186/s12886-017-0441-3 RESEARCH ARTICLE Open Access Postural effects on intraocular pressure and ocular perfusion pressure in patients with non-arteritic
Yang et al. BMC Ophthalmology (2017) 17:47 DOI 10.1186/s12886-017-0441-3 RESEARCH ARTICLE Open Access Postural effects on intraocular pressure and ocular perfusion pressure in patients with non-arteritic
VISUAL LOSS AFTER ANESTHESIA DIFFERENT CAUSES: DIFFERENT SOLUTIONS
 VISUAL LOSS AFTER ANESTHESIA DIFFERENT CAUSES: DIFFERENT SOLUTIONS - A Review - Elizabeth A.M. Frost * Historical Introduction It has long been recognized that visual damage may follow the administration
VISUAL LOSS AFTER ANESTHESIA DIFFERENT CAUSES: DIFFERENT SOLUTIONS - A Review - Elizabeth A.M. Frost * Historical Introduction It has long been recognized that visual damage may follow the administration
VI.2.2 Summary of treatment benefits
 EU-Risk Management Plan for Bimatoprost V01 aetiology), both OAG and ACG can be secondary conditions. Secondary glaucoma refers to any case in which another disorder (e.g. injury, inflammation, vascular
EU-Risk Management Plan for Bimatoprost V01 aetiology), both OAG and ACG can be secondary conditions. Secondary glaucoma refers to any case in which another disorder (e.g. injury, inflammation, vascular
Health Tech Symposium Fall, Dan Sommers P.E. EMT-P
 Health Tech Symposium Fall, 2009 Dan Sommers P.E. EMT-P Human Physiological Signals Simple Explanations for Complicated Systems Ref: Atlas of Human Anatomy, 4 th Edition Simple Schematic RA LA RV LV PCR
Health Tech Symposium Fall, 2009 Dan Sommers P.E. EMT-P Human Physiological Signals Simple Explanations for Complicated Systems Ref: Atlas of Human Anatomy, 4 th Edition Simple Schematic RA LA RV LV PCR
3/30/12. Luke J. Gasowski BS, BSRT, NREMT-P, FP-C, CCP-C, RRT-NPS
 Luke J. Gasowski BS, BSRT, NREMT-P, FP-C, CCP-C, RRT-NPS 1) Define and describe ETCO 2 2) Explain methods of measuring ETCO 2 3) Describe various clinical applications of ETCO 2 4) Describe the relationship
Luke J. Gasowski BS, BSRT, NREMT-P, FP-C, CCP-C, RRT-NPS 1) Define and describe ETCO 2 2) Explain methods of measuring ETCO 2 3) Describe various clinical applications of ETCO 2 4) Describe the relationship
Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical Trial
 J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
Rocuronium versus Vecuronium for laparoscopic cholecystectomy
 Original Article, Vol. 2, No. 4, Issue 6, Oct.-Dec., 2013 Rocuronium versus Vecuronium for laparoscopic cholecystectomy Tabdar S 1, Kadariya ER 2 1 Sushila Tabdar, Assistant Professor, Department of Anaesthesiology
Original Article, Vol. 2, No. 4, Issue 6, Oct.-Dec., 2013 Rocuronium versus Vecuronium for laparoscopic cholecystectomy Tabdar S 1, Kadariya ER 2 1 Sushila Tabdar, Assistant Professor, Department of Anaesthesiology
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Sign up to receive ATOTW weekly
 PERIPHERAL NERVE BLOCKS GETTING STARTED ANAESTHESIA TUTORIAL OF THE WEEK 134 PUBLICATION DATE 18/05/09 Dr Kim Russon, Consultant Anaesthetist Dr Helen Findley, ST3 Anaesthetics Dr Zoe Harclerode, ST3 Anaesthetics
PERIPHERAL NERVE BLOCKS GETTING STARTED ANAESTHESIA TUTORIAL OF THE WEEK 134 PUBLICATION DATE 18/05/09 Dr Kim Russon, Consultant Anaesthetist Dr Helen Findley, ST3 Anaesthetics Dr Zoe Harclerode, ST3 Anaesthetics
Journal of Anesthesia & Clinical
 Journal of Anesthesia & Clinical Research ISSN: 2155-6148 Journal of Anesthesia & Clinical Research Balasubramanian and Menaha, J Anesth Clin Res 2017, 8:12 DOI: 10.4172/2155-6148.1000791 Research Article
Journal of Anesthesia & Clinical Research ISSN: 2155-6148 Journal of Anesthesia & Clinical Research Balasubramanian and Menaha, J Anesth Clin Res 2017, 8:12 DOI: 10.4172/2155-6148.1000791 Research Article
Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy
 Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy Department of Anaesthesia University Children s Hospital Zurich Switzerland Epidemiology Herniotomy needed in
Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy Department of Anaesthesia University Children s Hospital Zurich Switzerland Epidemiology Herniotomy needed in
Advanced Cardiac Life Support (ACLS) Science Update 2015
 1 2 3 4 5 6 7 8 9 Advanced Cardiac Life Support (ACLS) Science Update 2015 What s New in ACLS for 2015? Adult CPR CPR remains (Compressions, Airway, Breathing Chest compressions has priority over all other
1 2 3 4 5 6 7 8 9 Advanced Cardiac Life Support (ACLS) Science Update 2015 What s New in ACLS for 2015? Adult CPR CPR remains (Compressions, Airway, Breathing Chest compressions has priority over all other
Percutaneous nephrolithotomy for staghorn kidney stones in elderly patients
 Int Urol Nephrol (2011) 43:639 643 DOI 10.1007/s11255-010-9885-6 UROLOGY ORIGINAL PAPER Percutaneous nephrolithotomy for staghorn kidney stones in elderly patients Baris Kuzgunbay Tahsin Turunc Ozgur Yaycioglu
Int Urol Nephrol (2011) 43:639 643 DOI 10.1007/s11255-010-9885-6 UROLOGY ORIGINAL PAPER Percutaneous nephrolithotomy for staghorn kidney stones in elderly patients Baris Kuzgunbay Tahsin Turunc Ozgur Yaycioglu
Original Article. Retinal effects of Sildenafil in diabetic patients. Summary: 8; Vol.50, No.1. J Fac Med Baghdad 63
 Retinal effects of Sildenafil in diabetic patients Original Article * (B.Sc. D.Sc. M.Sc) Summary: Fac Med Baghdad 8; Vol.50, No.1 200 Results: Received Dec 2006 Accepted Jun.2007 Background Sildenafil
Retinal effects of Sildenafil in diabetic patients Original Article * (B.Sc. D.Sc. M.Sc) Summary: Fac Med Baghdad 8; Vol.50, No.1 200 Results: Received Dec 2006 Accepted Jun.2007 Background Sildenafil
CAN TIGHT NECKTIE BE A RISK FACTOR IN DEVELOPMENT AND PROGRESSION OF PRIMARY- OPEN ANGLE GLAUCOMA (POAG)?
 CAN TIGHT NECKTIE BE A RISK FACTOR IN DEVELOPMENT AND PROGRESSION OF PRIMARY- OPEN ANGLE GLAUCOMA (POAG)? BY AJAYI, O. B., AKPOROBARO, N. AND AKINLABI, A. G. DEPARTMENT OF OPTOMETRY, UNIVERSITY OF BENIN,
CAN TIGHT NECKTIE BE A RISK FACTOR IN DEVELOPMENT AND PROGRESSION OF PRIMARY- OPEN ANGLE GLAUCOMA (POAG)? BY AJAYI, O. B., AKPOROBARO, N. AND AKINLABI, A. G. DEPARTMENT OF OPTOMETRY, UNIVERSITY OF BENIN,
RVO RETINAL VEIN OCCLUSION
 RVO RETINAL VEIN OCCLUSION A guide to understanding RVO Take some time to learn about RVO - it may help you hold on to your vision Retinal vein occlusion is a common disorder of the retina and a leading
RVO RETINAL VEIN OCCLUSION A guide to understanding RVO Take some time to learn about RVO - it may help you hold on to your vision Retinal vein occlusion is a common disorder of the retina and a leading
Evolution of the Definition of Primary Open-Angle Glaucoma
 OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D.
 Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D. Cleveland Clinic, Cleveland OH 1 Complications during central venous catheterization (CVC) occur 2% -15% of the
Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D. Cleveland Clinic, Cleveland OH 1 Complications during central venous catheterization (CVC) occur 2% -15% of the
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
SHOCK. Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital
 SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
Physiologic Based Management of Circulatory Shock Kuwait 2018
 Physiologic Based Management of Circulatory Shock Kuwait 2018 Dr. Yasser Elsayed, MD, PhD Director of the Targeted Neonatal Echocardiography, Point of Care and Hemodynamics Program Staff Neonatologist
Physiologic Based Management of Circulatory Shock Kuwait 2018 Dr. Yasser Elsayed, MD, PhD Director of the Targeted Neonatal Echocardiography, Point of Care and Hemodynamics Program Staff Neonatologist
8th Annual NKY TBI Conference 3/28/2014
 Closed Head Injury: Headache to Herniation A N T H O N Y T. K R A M E R U N I V E R S I T Y O F C I N C I N N A T I B L U E A S H E M S T E C H N O L O G Y P R O G R A M Objectives Describe the pathological
Closed Head Injury: Headache to Herniation A N T H O N Y T. K R A M E R U N I V E R S I T Y O F C I N C I N N A T I B L U E A S H E M S T E C H N O L O G Y P R O G R A M Objectives Describe the pathological
Ischaemic optic neuropathy: the Singapore scene
 O r i g i n a l A r t i c l e Singapore Med J 2007; 48 (4) : 281 Ischaemic optic neuropathy: the Singapore scene Cullen J F, Por Y M Abstract The commonest cause of an optic neuropathy in Singapore is
O r i g i n a l A r t i c l e Singapore Med J 2007; 48 (4) : 281 Ischaemic optic neuropathy: the Singapore scene Cullen J F, Por Y M Abstract The commonest cause of an optic neuropathy in Singapore is
Comparison of the Hemodynamic Responses with. with LMA vs Endotracheal Intubation
 Original article Comparison of the Hemodynamic Responses 10.5005/jp-journals-10045-0060 with LMA vs Endotracheal Intubation Comparison of the Hemodynamic Responses with Laryngeal Mask Airway vs Endotracheal
Original article Comparison of the Hemodynamic Responses 10.5005/jp-journals-10045-0060 with LMA vs Endotracheal Intubation Comparison of the Hemodynamic Responses with Laryngeal Mask Airway vs Endotracheal
Pet owners are often very anxious about veterinary procedures that involve anesthesia. This handout attempts to alleviate some of these concerns.
 Printable Version Anesthesia for Cats Pet owners are often very anxious about veterinary procedures that involve anesthesia. This handout attempts to alleviate some of these concerns. The word anesthesia
Printable Version Anesthesia for Cats Pet owners are often very anxious about veterinary procedures that involve anesthesia. This handout attempts to alleviate some of these concerns. The word anesthesia
INVOS System Inservice Guide for Pediatric Use. INVOS System Inservice Guide for Pediatric Use
 INVOS System Inservice Guide for Pediatric Use INVOS System Inservice Guide for Pediatric Use The INVOS System: A Window to Perfusion Adequacy The noninvasive INVOS System reports the venous- weighted
INVOS System Inservice Guide for Pediatric Use INVOS System Inservice Guide for Pediatric Use The INVOS System: A Window to Perfusion Adequacy The noninvasive INVOS System reports the venous- weighted
Correspondence should be addressed to Emre Ayintap;
 Ophthalmology, Article ID 696302, 4 pages http://dx.doi.org/10.1155/2014/696302 Research Article The Injection of Air/Oxygen Bubble into the Anterior Chamber of Rabbits as a Treatment for Hyphema in Patients
Ophthalmology, Article ID 696302, 4 pages http://dx.doi.org/10.1155/2014/696302 Research Article The Injection of Air/Oxygen Bubble into the Anterior Chamber of Rabbits as a Treatment for Hyphema in Patients
Respiratory Effects of IV CR845 - A Peripherally Acting, Selective Kappa Opioid Receptor Agonist
 Respiratory Effects of IV CR845 - A Peripherally Acting, Selective Kappa Opioid Receptor Agonist Eugene R. Viscusi, 1 Marc C. Torjman, 1 Joseph W. Stauffer, 2 Catherine L. Munera, 2 Beatrice S. Setnik,
Respiratory Effects of IV CR845 - A Peripherally Acting, Selective Kappa Opioid Receptor Agonist Eugene R. Viscusi, 1 Marc C. Torjman, 1 Joseph W. Stauffer, 2 Catherine L. Munera, 2 Beatrice S. Setnik,
