Perforation of the esophagus results in significant morbidity
|
|
|
- Derek Evans
- 5 years ago
- Views:
Transcription
1 Primary Repair of Esophageal Perforation David T. Cooke, MD,* and Christine L. Lau, MD Perforation of the esophagus results in significant morbidity and potential mortality. Determinants of morbidity and mortality are the cause of the injury, location of the injury along the esophagus, and delay in diagnosis and treatment. Spontaneous perforation, such as postemetic Boerhaave s syndrome, accounts for up to 36% of esophageal perforation, 19% of iatrogenic injuries, and 7% of external trauma. 1 Delay in diagnosis greater than 24 hours doubles the resultant mortality. However, regardless of time to diagnosis, in the absence of associated malignancy, severe esophageal dysmotility, or gastroesophageal reflux stricture, several reports indicate the advantages and success of primarily repairing esophageal injuries. 2-4 Causes of esophageal perforation can be divided into instrumental and noninstrumental. Instrumental causes include endoscopy, both rigid and flexible, dilation of strictures or the esophagogastric junction (EGJ) by pneumatic balloon dilation or bouginage, and airway intubation. Noninstrumental causes include barogenic, penetrating, and operative trauma. The most common etiology of barogenic trauma is Boerhaave s syndrome. In 1723, Dr. Hermann Boerhaave detailed in his report, History of a Grievous Disease Not Previously Described, a postmortem on the Dutch admiral, Baron Jan Germit von Wassenaer. 5 The Baron had a habit of self-inducing emesis after heavy meals. After a dinner of duck and beer, the Baron vomited, experienced an acute ripping sensation, and died 18 hours later. A postmortem found a transverse tear of the distal esophagus, just proximal to the EGJ. Although esophageal perforation may occur anywhere, certain types of esophageal injuries have a predilection to occurring at key anatomic areas. These areas correspond to *Division of Cardiothoracic Surgery, University of California, Davis, Sacramento, California. Division of Thoracic and Cardiovascular Surgery, University of Virginia, Charlottesville, Virginia. Address reprint requests to Christine L. Lau, MD, University of Virginia, Division of Thoracic and Cardiovascular Surgery, PO Box , Charlottesville, VA cll2y@virginia.edu natural points of narrowing, specifically, the criopharyngeus muscle of the cervical esophagus, the area of broncho-aortic constriction at the proximal one-third of the esophagus, and the distal EGJ (Fig. 1). Iatrogenic cervical esophageal injuries, especially endoscopy, commonly occur at Killian s triangle, an area lacking posterior esophageal muscularis (Fig. 2). This narrow area is bordered by the horizontal cricopharyngeus muscle inferiorly and the oblique inferior constrictor muscles superiorly. Ingested foreign bodies often become lodged at the broncho-aortic constriction, causing localized injury. Barogenic trauma occurs most frequently near the EGJ. In cervical esophageal perforation, patients often present with symptoms of neck pain, dysphagia, odynophagia, dysphonia, and subcutaneous emphysema. Symptoms of intrathoracic esophageal perforation are often more extreme and include chest pain, tachycardia, fever, leukocytosis, and hypotension. Intrathoracic esophageal perforation may rapidly contaminate the mediastinum, causing chemical irritation, inflammation, and sepsis. Chemical injury from the disrupted esophagus may cause the overlying pleura to rupture, and negative intrathoracic pressure draws saliva, gastric juice, and bacteria from the esophageal lumen into the pleural space, eventually leading to marked fluid shifts and shock. Several diagnostic tests play important roles in identifying esophageal perforation. A chest radiograph should be obtained, looking for subcutaneous emphysema and pneumomediastinum. Contrast esophagography is the gold standard. Water-soluble gastrograffin should be avoided, as it is hypertonic and aspiration may lead to pneumonitis. 6 Thin barium is an effective and safe contrast agent for esophagography and detects even small defects. 7 Chest computed tomography identifies pneumomediastinum, pneumoperitoneum, pleural effusions, and esophageal thickening. Flexible endoscopy is valuable and may identify a high-grade stricture or malignancy that would steer the surgeon from primary repair to esophagectomy. Once the diagnosis of esophageal injury is confirmed, prompt surgical treatment is mandatory. In the following sections, we describe primary repair of the cervical and intrathoracic esophageal perforation /08/$-see front matter 2008 Elsevier Inc. All rights reserved. doi: /j.optechstcvs
2 Primary repair of esophageal perforation 127 Figure 1 The esophagus has anatomical points of narrowing or constriction that make the organ prone to injury at these areas. The areas are the cricopharyngeus muscle of the cervical esophagus, the area of broncho-aortic constriction at the proximal one-third of the esophagus, and the distal esophagogastric junction. m. muscle.
3 128 D.T. Cooke and C.L. Lau Figure 2 Iatrogenic cervical esophageal injuries commonly occur at Killian s triangle, which is a narrow area bordered by the horizontal cricopharyngeus muscle inferiorly and the oblique inferior constrictor muscles superiorly. The area within the triangle lacks posterior esophageal muscularis and is easily penetrated, as illustrated by the flexible esophagoscope. m. muscle.
4 Primary repair of esophageal perforation 129 Operative Technique Cervical Exploration Neck exploration is the correct approach for cervical esophageal injuries as well as injuries to the proximal one-third of the thoracic esophagus down to the level of the carina. The majority of cervical esophageal injuries should be approached via the left neck. The patient is placed in the supine position and a shoulder roll is placed beneath the scapulae to extend the neck, and the arms are tucked to the sides. The patient s head is rotated slightly to the right to provide optimal exposure of the left neck (Fig. 3). In the absence of distal obstruction, it is not necessary to repair a difficult to expose cervical esophageal injury, as the lesion will likely heal with adequate external drainage. However, the perforation should be primarily repaired if it is readily identified. For repair, a 40- or 46-F Maloney bougie is passed to prevent narrowing of the esophagus; a vertical esophageal myotomy is performed to expose the entire extent of the mucosal injury. The mucosal tear is repaired with interrupted 4-0 absorbable suture, and the muscularis is reapproximated with a running or interrupted 3-0 suture. The bougie is removed, and a nasogastric tube is inserted just proximal to the repair. The repair Figure 3 (A) The left neck is entered through a 5- to 7-cm incision along the anterior border of the sternocleidomastoid muscle (dashed line). The cricoid prominence is palpated as an external landmark, and one-third of the incision is made above the level of the cricoid cartilage, and two-thirds of the incision is extended below. If the esophageal injury involves the proximal one-third of the thoracic esophagus, the neck incision can be extended onto the sternum (dotted line), and the manubrium can be partially split to provide better access to the superior mediastinum. (B) The plane of the dissection is carried medial to the sternocleidomastoid muscle and carotid sheath, and lateral to the thyroid gland and trachea (bold line). a. artery; m. muscle; v. vein.
5 130 D.T. Cooke and C.L. Lau Figure 4 The incision is carried down through the platysma muscle, identifying the sternohyoid and omohyoid strap muscles, while the sternocleidomastoid muscle is retracted laterally with an Army Navy retractor. The omohyoid muscle is divided, and its cut belly is followed down to the carotid sheath. m. muscle. is tested with the wound submerged under saline, and air is insufflated through the nasogastric tube while the distal esophagus is occluded by the surgeon s fingers. The nasogastric tube is then advanced past the repair and into the stomach (Figs. 4-9). If the cervical esophagus could not be primarily repaired, the wound is left partially open, packed, and allowed to granulate close. The nasogastric tube is removed on postoperative day 3 and the patient is started on a clear liquid diet. A thin barium esophagogram is performed on postoperative day 7. Figure 5 If necessary, the middle thyroid vein and inferior thyroid artery are divided if those vessels are in the surgeon s view. The trachea and thyroid gland are retracted medially by the assistant s finger, exposing the esophagus. Note a finger is used for retraction in the tracheoesophageal groove and not a metal retractor. A metal retractor such as an Army Navy increases the risk of injury to the recurrent laryngeal nerve. Although care must be taken when placing retraction on the tracheoesophageal groove, identification of the recurrent laryngeal nerve is not necessary. a. artery; v. vein.
6 Primary repair of esophageal perforation 131 Figure 6 Although the trachea is retracted medially and the carotid is retracted laterally, the surgeon mobilizes the esophagus by encircling it with his or her finger, starting at the medial border of the esophagus and extending down posteriorly to the prevertebral fascia. This mobilization is performed using a combination of blunt dissection with a finger and sharp dissection with Metzabaum scissors. The mobilized esophagus is then encircled with a ¼-inch Penrose drain for easy traction. Figure 7 The mucosal injury is generally more extensive than the apparent muscularis defect. A longitudinal myotomy is performed with cautery until the full extent of the mucosal tear is apparent, and the mucosa is debrided, as necessary, to fresh edges.
7 132 D.T. Cooke and C.L. Lau Figure 8 After the esophageal repair, a finger is passed down posterior to the esophagus and anterior to the prevertebral fascia down into the superior mediastinum, followed by a sucker, to remove any fluid or effluent. A flat Blake drain is then placed into the superior mediastinum along this path and externalized, for closed drainage. Figure 9 After the wound is copiously irrigated, the platysma muscle is closed with widely spaced interrupted 4-0 Vicryl sutures, and the skin is closed with a running 4-0 nylon suture.
8 Primary repair of esophageal perforation 133 Figure 10 Injuries to the distal third of the esophagus are managed through the left side of the chest, via the seventh intercostal space. The patient is placed in the right lateral decubitus position, and a roll is placed just bellow the axilla, to protect the brachial plexus. The table is flexed to increase the intercostal spaces, and reverse Trendelenberg tilting of the table is provided until the thorax is parallel to the floor. Figure 11 In harvesting an intercostal muscle flap for a reinforced repair, the muscle of the seventh interspace is carefully cauterized off of the seventh rib, and the neurovascular bundle is gently levered off of the rib with a periosteal elevator. The muscle is then cauterized off of the eighth rib. The muscle is divided anteriorly and mobilized posteriorly as a pedicle. It is wrapped in moist gauze and set aside until the end of the case.
9 134 D.T. Cooke and C.L. Lau Figure 12 After the chest is entered, any effusion, succus, or debris is evacuated. The lung is retracted anteriorly with a cloth-covered Harrington retractor, or other type of lung retractor. Beginning near the esophageal hiatus of the diaphragm and between the aorta and the pericardium, the esophagus is mobilized with the surgeon s finger. Thoracic Exploration Perforations of the middle third of the esophagus are approached from the right side through the fourth through sixth intercostal space, depending on location, while injuries to the distal third of the esophagus are managed from the left side of the chest, through the seventh intercostal space (Fig.10). Single lung ventilation with a double lumen endotracheal tube may improve exposure; however, this is not necessary as the lung usually can be retracted aside. Reinforcement of the primary repair with an intercostal muscle flap, pericardial fat pad, pleural patch (Grillo patch), or omentum is not necessary but may be performed. The decision to reinforce the primary repair with an intercostal muscle flap must be made before thoracotomy (Figs ). As mentioned in the cervical exploration section, the mucosal injury is usually more extensive than the apparent muscularis defect. A longitudinal myotomy is performed until the full extent of the mucosal tear is apparent, and the mucosa edges are debrided. The mucosa can be repaired with interrupted 4-0 Vicryl sutures. Whyte and coworkers described an effective technique of primary repair, where the mucosal edges are grasped and approximated with Allis clamps, and the mucosa is closed with a 3.5-mm load gastrointestinal anastomotic (GIA) surgical stapler (AutoSuture, Inc., Norwalk, CT) 4 (Fig. 14). The second layer of muscularis is closed with an interrupted or running 4-0 absorbable suture. At this time, the repair may be reinforced with the intercostal muscle pedicled flap (Fig.15). If the repair is to be reinforced with a pleural patch, only thickened inflamed parietal pleural is to be used. Normal parietal pleural is too thin and falls apart once harvested. Alternatively in some cases the pericardial fat pad provides good coverage. A nasogastric tube is inserted to just above the repair; while the closure is submerged under saline, it is tested by insufflating air and occluding the distal esophagus. The nasogastric tube is then advanced into the stomach. The mediastinum and chest are thoroughly irrigated; an angled 28-F chest tube is positioned over the diaphragm, and a straight 28-F chest tube is placed along the posterior thorax. Draining gastrostomy and feeding jejunostomy tubes are generally not necessary. The nasogastric tube is left to low wall suction for 3 days and then removed. The patient is started on a clear liquid diet and slowly advanced. A thin barium swallow study is obtained on postoperative day 7. Esophageal Stenting Recently some groups have reported success in managing esophageal perforations with removable esophageal stents. Kiev and colleagues 8 have described their use of removable Polyflex esophageal stents (Rush, Inc., Teleflex Medical, Duluth, GA) in the treatment of 14 patients with esophageal perforations (5 of whom had continued leaks documented on contrast studies after primary surgical repair). All 14 patients had successful healing of the perforation without the need for additional surgical intervention. Oral intake in the majority was quickly resumed. In all patients,
10 Primary repair of esophageal perforation 135 Figure 13 The esophagus is then encircled with a Penrose drain for easy manipulation.
11 136 D.T. Cooke and C.L. Lau Figure 14 With a 40-F or 46-F Maloney bougie inserted into the lumen, the esophageal mucosal edges are grasped and approximated with Allis clamps, and the mucosa is closed with a 3.5-mm load GIA surgical stapler (AutoSuture, Inc., Norwalk, CT).
12 Primary repair of esophageal perforation 137 Figure 15 The second layer of muscularis is closed with an interrupted or running 4-0 absorbable suture. The repair may be reinforced with the intercostal muscle pedicled flap sewn in place with interrupted mattress sutures around the circumference of the flap. this group placed percutaneous gastrostomy tubes to aid in nutrition as well as to keep the stomach decompressed. In general their patients were discharged with the stents in place and returned for reevaluation; usually the stent was removed within the 30-day period after stent deployment. Stent migration was a noted problem that required prompt identification and repositioning. Of note, the site of perforation is important in determining stent deployment with efforts made if possible to avoid stenting at or above the upper esophageal sphincter or across the gastroesophageal sphincter. Conclusions Successful outcomes for primary repair of esophageal perforation can be obtained even in delays in diagnosis greater than 24 hours. Wright and coworkers reported on 28 patients who underwent reinforced primary repair of thoracic esophageal injuries, with a total mortality of 14%. 3 Thirteen patients were treated 24 hours after their injury; of these 13 patients, there was a 31% mortality and a 54% leak rate. Whyte and coworkers described 22 patients with thoracic esophageal perforations who underwent primary repair. 4 The mortality rate for all patients was 5%. Nine patients underwent repair 24 hours after their initial injury, and 33% of those patients developed a postoperative leak. Iannettoni and coworkers examined the long-term results of 42 patients treated for esophageal perforation. 9 The mean follow-up was 3.7 years, and the overall mortality was 16.7%. Of the 42 patients, 25 underwent primary repair of their esophageal perforation. Five of the patients who underwent primary repair (20%) developed postoperative leaks, and all five had preexisting gastroesophageal reflux disease (GERD) with peptic strictures. Forty percent of the primary repair patients required postoperative dilations for dysphagia, and five of those patients ultimately required esophagectomy for intractable GERD-related strictures. Primary repair of esophageal perforations can be accomplished with favorable results. However, perforations due to instrumentation of GERD-related stricture may be better suited by esophagectomy at initial presentation, as postoperative dilation of these strictures to eliminate dysphagia is usually unsuccessful. Perforation as a result of instrumentation of achalasia can be treated by primary repair of the injury, long myotomy, and a Belsey antireflux operation. In the absence of primary malignancy or severe peptic stricture, primary repair of esophageal perforation is the optimal therapeutic approach. In the near future esophageal stenting for perforation may become the preferred treatment especially in cases without significant mediastinal soiling. References 1. Brinster CJ, Singhal S, Lee L, et al: Evolving options in the management of esophageal perforation. Ann Thorac Surg 77: , Grillo HC, Wilkins EW Jr: Esophageal repair following late diagnosis of intrathoracic perforation. Ann Thorac Surg 20: , Wright CD, Mathisen DJ, Wain JC, et al: Reinforced primary repair of thoracic esophageal perforation. Ann Thorac Surg 60: , Whyte RI, Iannettoni MD, Orringer MB: Intrathoracic esophageal perforation. The merit of primary repair. J Thorac Cardiovasc Surg 109: , Boerhaave H: Atrocis, nec descripti prima, morbid historia. Derbes V, Mitchell R, translators. Bull Med Libr Assoc 43:217, Reich SB: Production of pulmonary edema by aspiration of water-soluble nonabsorbable contrast media. Radiology 92: , Gollub MJ, Bains MS: Barium sulfate: a new (old) contrast agent for diagnosis of postoperative esophageal leaks. Radiology 202: , Kiev J, Amendola M, Bouhaidar D, et al: A management algorithm for esophageal perforation. Am J Surg 194: , Iannettoni MD, Vlessis AA, Whyte RI, et al: Functional outcome after surgical treatment of esophageal perforation. Ann Thorac Surg 64: , 1997
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Alexander C Vlantis. Total Laryngectomy 57
 07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
Case Presentation Surgery Grand Round. Amid Keshavarzi, MD UCHSC 4/9/2006
 Case Presentation Surgery Grand Round Amid Keshavarzi, MD UCHSC 4/9/2006 Case Presentation 12 y/o female Presented to OSH after accidental swallowing of plastic fork in the bus, CXR/AXR form OSH did not
Case Presentation Surgery Grand Round Amid Keshavarzi, MD UCHSC 4/9/2006 Case Presentation 12 y/o female Presented to OSH after accidental swallowing of plastic fork in the bus, CXR/AXR form OSH did not
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Esophageal perforation remains a diagnostic and therapeutic
 Esophageal Diversion Daniel P. Raymond, MD, and Thomas J. Watson, MD Division of Thoracic and Foregut Surgery, Department of Surgery, University of Rochester Medical Center, Rochester, New York. Address
Esophageal Diversion Daniel P. Raymond, MD, and Thomas J. Watson, MD Division of Thoracic and Foregut Surgery, Department of Surgery, University of Rochester Medical Center, Rochester, New York. Address
ESOPHAGEAL PERFORATION. Anju Sidhu MD University of Louisville Gastroenterology, Hepatology, and Nutrition January 24, 2013
 ESOPHAGEAL PERFORATION Anju Sidhu MD University of Louisville Gastroenterology, Hepatology, and Nutrition January 24, 2013 OUTLINE Risk factors Diagnosis Management GOALS Make sure you don t miss it If
ESOPHAGEAL PERFORATION Anju Sidhu MD University of Louisville Gastroenterology, Hepatology, and Nutrition January 24, 2013 OUTLINE Risk factors Diagnosis Management GOALS Make sure you don t miss it If
Achalasia is a primary esophageal motility disorder of unknown
 Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Esophageal injuries. Pre-test /11/10. 新光急診張志華醫師 Facebook.com/jack119. O What is the most common cause of esophageal injuries?
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 O What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic 1 Pre-test 2 O Which contrast
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 O What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic 1 Pre-test 2 O Which contrast
Tracheo-innominate artery fistula (TIF) is an uncommon
 Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
AATS Focus on Thoracic Surgery: Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017?
 AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
Combined Collis-Nissen Reconstruction. of the esophagogastric junction at. Mark B. Orringer, M.D., and Herbert Sloan, M.D.
 Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
Esophageal injuries. 新光急診張志華醫師 Facebook.com/jack119
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Uniportal video-assisted thoracic surgery for esophageal cancer
 Surgical Technique on Esophageal Surgery Uniportal video-assisted thoracic surgery for esophageal cancer Hasan F. Batirel Thoracic Surgery Department, Marmara University Hospital, Istanbul, Turkey Correspondence
Surgical Technique on Esophageal Surgery Uniportal video-assisted thoracic surgery for esophageal cancer Hasan F. Batirel Thoracic Surgery Department, Marmara University Hospital, Istanbul, Turkey Correspondence
Acquired pediatric esophageal diseases Imaging approaches and findings. M. Mearadji International Foundation for Pediatric Imaging Aid
 Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Departement of Surgery Faculty of Medicine University Sumatera Utara
 SSS EESOPHAGEAL HPOSAGEAL DISORDERS IN SURGICAL PERSPECTIVE Departement of Surgery Faculty of Medicine University Sumatera Utara CONTENT 1. Esophageal Atresia 2. Achalasia 3. Esophageal Rupture 4. Tumor
SSS EESOPHAGEAL HPOSAGEAL DISORDERS IN SURGICAL PERSPECTIVE Departement of Surgery Faculty of Medicine University Sumatera Utara CONTENT 1. Esophageal Atresia 2. Achalasia 3. Esophageal Rupture 4. Tumor
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Thyroidectomy. Siu Kwan Ng. Modified Radical Neck Dissection Type II 47
 06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Esophageal Diverticulum. Ahmed Hozain, PGY III Kings County Hospital University Hospital of Brooklyn, Surgery Grand Rounds May 18 th, 2017
 Esophageal Diverticulum Ahmed Hozain, PGY III Kings County Hospital University Hospital of Brooklyn, Surgery Grand Rounds May 18 th, 2017 Case Presentation 53 YOF presented to KCHC with sx of dysphagia
Esophageal Diverticulum Ahmed Hozain, PGY III Kings County Hospital University Hospital of Brooklyn, Surgery Grand Rounds May 18 th, 2017 Case Presentation 53 YOF presented to KCHC with sx of dysphagia
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
THE DESCENDING THORACIC AORTA
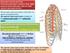 Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
PLEURAE and PLEURAL RECESSES
 PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
Anatomy notes-thorax.
 Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
STERNUM. Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts:
 STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
Surgical Management of Subglottic Stenosis
 Surgical Management of Subglottic Stenosis Cameron D. Wright, MD ubglottic stenosis is usually due to either endotracheal S tube ischemic necrosis or idiopathic larygotracheal stenosis. The ischemic area
Surgical Management of Subglottic Stenosis Cameron D. Wright, MD ubglottic stenosis is usually due to either endotracheal S tube ischemic necrosis or idiopathic larygotracheal stenosis. The ischemic area
Transthoracic esophagectomy and an intrathoracic esophagogastric
 General Thoracic Surgery Transhiatal Esophagectomy without Thoracotomy Mark B. Orringer, MD Transthoracic esophagectomy and an intrathoracic esophagogastric anastomosis was the standard surgical approach
General Thoracic Surgery Transhiatal Esophagectomy without Thoracotomy Mark B. Orringer, MD Transthoracic esophagectomy and an intrathoracic esophagogastric anastomosis was the standard surgical approach
Reinforced Primary Repair of Thoracic Esophageal Perforation
 Reinforced Primary Repair of Thoracic Esophageal Perforation Cameron D. Wright, MD, Douglas J. Mathisen, MD, John C. Wain, MD, Ashby C. Moncure, MD, Alan D. Hilgenberg, MD, and Hermes C. Grillo, MD General
Reinforced Primary Repair of Thoracic Esophageal Perforation Cameron D. Wright, MD, Douglas J. Mathisen, MD, John C. Wain, MD, Ashby C. Moncure, MD, Alan D. Hilgenberg, MD, and Hermes C. Grillo, MD General
The left thoracoabdominal and left neck approach to
 Esophagectomy: Left Thoracoabdominal and Left Neck Thomas W. Rice, MD *, The left thoracoabdominal and left neck approach to esophagectomy offers flexibility, versatility, and options. In the western world,
Esophagectomy: Left Thoracoabdominal and Left Neck Thomas W. Rice, MD *, The left thoracoabdominal and left neck approach to esophagectomy offers flexibility, versatility, and options. In the western world,
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
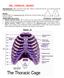 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
Intrathoracic esophageal. perforation. The merit of primary repair
 Intrathoracic esophageal The merit of primary repair perforation Between 1976 and 1993, 22 patients with intrathoracic esophageal perforations, none associated with carcinoma, underwent primary repair
Intrathoracic esophageal The merit of primary repair perforation Between 1976 and 1993, 22 patients with intrathoracic esophageal perforations, none associated with carcinoma, underwent primary repair
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Surgical Repair of Iatrogenic Cervical Tracheal Stenosis
 Surgical Repair of Iatrogenic Cervical Tracheal Stenosis Nirmal K. Veeramachaneni, MD, and Bryan F. Meyers, MD, MPH he advent of intensive care unit management has increased the potential opportunities
Surgical Repair of Iatrogenic Cervical Tracheal Stenosis Nirmal K. Veeramachaneni, MD, and Bryan F. Meyers, MD, MPH he advent of intensive care unit management has increased the potential opportunities
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Mediastinum and pericardium
 Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Penetrating Wounds of the Esophagus
 Panagiotis N. Symbas, M.D., Denis H. Tyras, M.D., Charles R. Hatcher, Jr., M.D., and Byron Perry, M.D. ABSTRACT The histories of 22 patients with perforation of the esophagus from bullet or stab wounds
Panagiotis N. Symbas, M.D., Denis H. Tyras, M.D., Charles R. Hatcher, Jr., M.D., and Byron Perry, M.D. ABSTRACT The histories of 22 patients with perforation of the esophagus from bullet or stab wounds
Anatomy of thoracic wall
 Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
4/16/2017. Learning Objectives. Interpretation of the Chest Radiograph. Components. Production of the Radiograph. Density & Appearance
 Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
T treat empyema, although modern day thoracic
 The Schede and Modern Thoracoplasty Benjamin J. Pomerantz, Joseph C. Cleveland, Jr, and Marvin Pomerantz THORACOPLASTY-GENERAL CONSIDERATIONS horacoplasty evolved as a procedure designed to T treat empyema,
The Schede and Modern Thoracoplasty Benjamin J. Pomerantz, Joseph C. Cleveland, Jr, and Marvin Pomerantz THORACOPLASTY-GENERAL CONSIDERATIONS horacoplasty evolved as a procedure designed to T treat empyema,
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Resection of malignant tumors invading the thoracic inlet
 Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Imaging of Thoracic Trauma: Tips and Traps. Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania
 Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Esophageal perforations are challenging to manage and are
 Endoscopic Techniques for the Management of Esophageal Perforation Karen Joanna Dickinson, MBBS, BSc, MD, FRCS, and Shanda H. Blackmon, MD, MPH Esophageal perforations or leaks can be spontaneous, iatrogenic,
Endoscopic Techniques for the Management of Esophageal Perforation Karen Joanna Dickinson, MBBS, BSc, MD, FRCS, and Shanda H. Blackmon, MD, MPH Esophageal perforations or leaks can be spontaneous, iatrogenic,
Idiopathic laryngotracheal stenosis
 Surgical Technique Idiopathic laryngotracheal stenosis Christina L. Costantino, Douglas J. Mathisen Massachusetts General Hospital, Boston, MA 02114, USA Correspondence to: Douglas J. Mathisen, MD. Massachusetts
Surgical Technique Idiopathic laryngotracheal stenosis Christina L. Costantino, Douglas J. Mathisen Massachusetts General Hospital, Boston, MA 02114, USA Correspondence to: Douglas J. Mathisen, MD. Massachusetts
The left thoracoabdominal incision provides excellent
 Left Thoracoabdominal Incision Sudhir Sundaresan The left thoracoabdominal incision provides excellent exposure for operations dealing with the distal esophagus or proximal stomach. It is particularly
Left Thoracoabdominal Incision Sudhir Sundaresan The left thoracoabdominal incision provides excellent exposure for operations dealing with the distal esophagus or proximal stomach. It is particularly
Chapter 16. Thoracic Injuries
 Thoracic Injuries Chapter 16 Thoracic Injuries Introduction About 15% of war injuries involve the chest. Of those, 10% are superficial (soft tissue only) requiring only basic wound treatment. The remaining
Thoracic Injuries Chapter 16 Thoracic Injuries Introduction About 15% of war injuries involve the chest. Of those, 10% are superficial (soft tissue only) requiring only basic wound treatment. The remaining
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
Evaluation & Management of Penetrating Wounds to the NECK
 Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Chapter 5: Other mediastinal structures. The Large Arteries. The Aorta. Ascending aorta
 Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
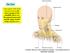 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions
 Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions John L. Cameron, M.D., Richard F. Kieffer, M.D., Thomas R. Hendrix, M.D., Denis G. Mehigan, M.., and R. Robinson aker,
Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions John L. Cameron, M.D., Richard F. Kieffer, M.D., Thomas R. Hendrix, M.D., Denis G. Mehigan, M.., and R. Robinson aker,
Lung & Pleura. The Topics :
 Lung & Pleura The Topics : The Trachea. The Bronchi. The Brochopulmonary Segments. The Lungs. The Hilum. The Pleura. The Surface Anatomy Of The Lung & Pleura. The Root & Hilum. - first of all, the lung
Lung & Pleura The Topics : The Trachea. The Bronchi. The Brochopulmonary Segments. The Lungs. The Hilum. The Pleura. The Surface Anatomy Of The Lung & Pleura. The Root & Hilum. - first of all, the lung
Physical Exam. Vitals stable on room air Abdomen soft, non-distented Normal external genitalia Patent anus No limb anomalies
 Case Presentation 1 day-old full-term baby girl noted to have drooling of saliva and increased secretions at birth Fetal US @32wks had shown polyhydramnios Birth weight 3515g Apgar 7@1min and 8@5min Unable
Case Presentation 1 day-old full-term baby girl noted to have drooling of saliva and increased secretions at birth Fetal US @32wks had shown polyhydramnios Birth weight 3515g Apgar 7@1min and 8@5min Unable
01/26/2010 GENERAL SURGERY ABSITE ANATOMY ANATOMY. Yvonne M. Carter, MD Georgetown University Medical Center. Layers. mucosa. squamous epithelium
 GENERAL SURGERY ABSITE REVIEW: ESOPHAGUS Yvonne M. Carter, MD Georgetown University Medical Center ANATOMY Layers mucosa muscle squamous epithelium columnar epithelium (distal 2cm) inner = circular outer
GENERAL SURGERY ABSITE REVIEW: ESOPHAGUS Yvonne M. Carter, MD Georgetown University Medical Center ANATOMY Layers mucosa muscle squamous epithelium columnar epithelium (distal 2cm) inner = circular outer
Trauma operating room
 Section 1 Chapter 1 Operating Room General Conduct Trauma operating room Kenji Inaba and Lisa L. Schlitzkus Operating room A large operating room (OR) situated near the emergency department, elevators,
Section 1 Chapter 1 Operating Room General Conduct Trauma operating room Kenji Inaba and Lisa L. Schlitzkus Operating room A large operating room (OR) situated near the emergency department, elevators,
Yara saddam & Dana Qatawneh. Razi kittaneh. Maher hadidi
 1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
Dana Alrafaiah. - Moayyad Al-Shafei. -Mohammad H. Al-Mohtaseb. 1 P a g e
 - 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
- 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 3 Cricothyroidotomy LESSON ASSIGNMENT Paragraphs 3-1 through 3-7. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Define cricothyroidotomy. 3-2. Identify
LESSON ASSIGNMENT LESSON 3 Cricothyroidotomy LESSON ASSIGNMENT Paragraphs 3-1 through 3-7. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Define cricothyroidotomy. 3-2. Identify
Esophageal Stent Placement for the Treatment of Acute Intrathoracic Anastomotic Leak After Esophagectomy
 ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
Proceedings of the World Small Animal Veterinary Association Mexico City, Mexico 2005
 Close this window to return to IVIS Proceedings of the World Small Animal Veterinary Association Mexico City, Mexico 2005 Hosted by: Reprinted in the IVIS website with the permission of the WSAVA Surgery
Close this window to return to IVIS Proceedings of the World Small Animal Veterinary Association Mexico City, Mexico 2005 Hosted by: Reprinted in the IVIS website with the permission of the WSAVA Surgery
The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control
 ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Positioning and Accesses
 5 2 Positioning and Accesses Yvonne Knoblauch, Dieter Hahnloser Positioning Correct and stable positioning of the patient is the first step for a successful operation. Safe positioning of the arm and leg
5 2 Positioning and Accesses Yvonne Knoblauch, Dieter Hahnloser Positioning Correct and stable positioning of the patient is the first step for a successful operation. Safe positioning of the arm and leg
ANATOMY OF THE PLEURA. Dr Oluwadiya KS
 ANATOMY OF THE PLEURA Dr Oluwadiya KS www.oluwadiya.sitesled.com Introduction The thoracic cavity is divided mainly into: Right pleural cavity Mediastinum Left Pleural cavity Pleural cavity The pleural
ANATOMY OF THE PLEURA Dr Oluwadiya KS www.oluwadiya.sitesled.com Introduction The thoracic cavity is divided mainly into: Right pleural cavity Mediastinum Left Pleural cavity Pleural cavity The pleural
The supraclavicular approach to scalenectomy and first rib resection: Description of technique
 The supraclavicular approach to scalenectomy and first rib resection: Description of technique Richard J. Sanders, M.D., and Susan Raymer, Denver, Colo. Supraclavicular first rib resection has been performed
The supraclavicular approach to scalenectomy and first rib resection: Description of technique Richard J. Sanders, M.D., and Susan Raymer, Denver, Colo. Supraclavicular first rib resection has been performed
Penetrating Neck Trauma. Herve J. LeBoeuf, MD Francis B. Quinn, MD
 Penetrating Neck Trauma Herve J. LeBoeuf, MD Francis B. Quinn, MD Introduction 5-10% of all trauma Overall mortality rate as high as 11% Major vessel injury fatal in 65%, including prehospital deaths Attending
Penetrating Neck Trauma Herve J. LeBoeuf, MD Francis B. Quinn, MD Introduction 5-10% of all trauma Overall mortality rate as high as 11% Major vessel injury fatal in 65%, including prehospital deaths Attending
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Pneumothorax. Defined as air in the pleural space which can occur through a number of mechanisms
 Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
9/18/2015. Disclosures. Objectives. Dysphagia Sherri Ekobena PA-C. I have no relevant financial interests to disclose I have no conflicts of interest
 Dysphagia Sherri Ekobena PA-C Disclosures I have no relevant financial interests to disclose I have no conflicts of interest Objectives Define what dysphagia is Define types of dysphagia Define studies
Dysphagia Sherri Ekobena PA-C Disclosures I have no relevant financial interests to disclose I have no conflicts of interest Objectives Define what dysphagia is Define types of dysphagia Define studies
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
It passes through the diaphragm at the level of the 10th thoracic vertebra to join the stomach
 The esophagus is a tubular structure (muscular, collapsible tube ) about 10 in. (25 cm) long that is continuous above with the laryngeal part of the pharynx opposite the sixth cervical vertebra The esophagus
The esophagus is a tubular structure (muscular, collapsible tube ) about 10 in. (25 cm) long that is continuous above with the laryngeal part of the pharynx opposite the sixth cervical vertebra The esophagus
LECTURE -I. Intercostal Spaces & Its Content. BY Dr Farooq Khan Aurakzai. Date:
 LECTURE -I Intercostal Spaces & Its Content BY Dr Farooq Khan Aurakzai Date: 18.04.18 Layers of IC space: Following are the layers of the thoracic region: Skin Subcutaneous CT External IC muscle and membrane
LECTURE -I Intercostal Spaces & Its Content BY Dr Farooq Khan Aurakzai Date: 18.04.18 Layers of IC space: Following are the layers of the thoracic region: Skin Subcutaneous CT External IC muscle and membrane
Gastric transposition in infants and children
 DOI 10.1007/s00383-010-2736-9 REVIEW ARTICLE Gastric transposition in infants and children Robert A. Cowles Arnold G. Coran Accepted: 6 September 2010 Ó Springer-Verlag 2010 Abstract The loss of esophageal
DOI 10.1007/s00383-010-2736-9 REVIEW ARTICLE Gastric transposition in infants and children Robert A. Cowles Arnold G. Coran Accepted: 6 September 2010 Ó Springer-Verlag 2010 Abstract The loss of esophageal
Surgical anatomy of thyroid and parathyroid glands
 Head & Neck Surgery Course Surgical anatomy of thyroid and parathyroid glands Dr Pierfrancesco PELLICCIA Pr Benjamin LALLEMANT Service ORL et CMF CHU de Nîmes CH de Arles Thyroid glands Dr Pierfrancesco
Head & Neck Surgery Course Surgical anatomy of thyroid and parathyroid glands Dr Pierfrancesco PELLICCIA Pr Benjamin LALLEMANT Service ORL et CMF CHU de Nîmes CH de Arles Thyroid glands Dr Pierfrancesco
Traditionally, surgical antireflux therapy has been
 Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
Nissen Fundoplication
 Nissen Fundoplication By Donna Weldon Nissen fundoplication is a surgical procedure used to treat gastroesophageal reflux disease, or GERD, and hiatus hernias. For GERD, is it usually performed when medical
Nissen Fundoplication By Donna Weldon Nissen fundoplication is a surgical procedure used to treat gastroesophageal reflux disease, or GERD, and hiatus hernias. For GERD, is it usually performed when medical
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL. September 17, Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous
 Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Subglottic stenosis, with involvement of the lower larynx
 Laryngotracheal Resection and Reconstruction John D. Mitchell, MD n, Subglottic stenosis is being recognized with increasing frequency in adults, and may be the most frequent indication for airway intervention
Laryngotracheal Resection and Reconstruction John D. Mitchell, MD n, Subglottic stenosis is being recognized with increasing frequency in adults, and may be the most frequent indication for airway intervention
Thoracoabdominal Esophagectomy for Cancer of the Gastroesophageal Junction
 Thoracoabdominal Esophagectomy for Cancer of the Gastroesophageal Junction Douglas J. Mathisen The left thoracoabdominal esophagogastrectomy has for many years been the standard approach for resection
Thoracoabdominal Esophagectomy for Cancer of the Gastroesophageal Junction Douglas J. Mathisen The left thoracoabdominal esophagogastrectomy has for many years been the standard approach for resection
Mediastinum It is a thick movable partition between the two pleural sacs & lungs. It contains all the structures which lie
 Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Surface anatomy of Cardiovascular system
 Surface anatomy of Cardiovascular system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The lines cover the front, side, and back of the thorax Midsternal
Surface anatomy of Cardiovascular system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The lines cover the front, side, and back of the thorax Midsternal
THYROID & PARATHYROID. By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy
 THYROID & PARATHYROID By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy 1 OBJECTIVES By the end of the lecture, the student should be able to: Describe the shape, position, relations and structure of
THYROID & PARATHYROID By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy 1 OBJECTIVES By the end of the lecture, the student should be able to: Describe the shape, position, relations and structure of
Robotic-assisted McKeown esophagectomy
 Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
Carinal resections. Leonidas Tapias, Michael Lanuti. Clinical vignette
 Masters of Cardiothoracic Surgery Carinal resections Leonidas Tapias, Michael Lanuti Division of Thoracic Surgery, Massachusetts General Hospital, Boston, MA, USA Correspondence to: Michael Lanuti, MD.
Masters of Cardiothoracic Surgery Carinal resections Leonidas Tapias, Michael Lanuti Division of Thoracic Surgery, Massachusetts General Hospital, Boston, MA, USA Correspondence to: Michael Lanuti, MD.
T ageal fistulas result from complications of mechanical
 Management of Acquired Nonmalignant Tracheoesophageal Fistula Douglas J. Mathisen, MD, Hermes C. Grillo, MD, John C. Wain, MD, and Alan D. Hilgenberg, MD Department of Surgery, Massachusetts General Hospital,
Management of Acquired Nonmalignant Tracheoesophageal Fistula Douglas J. Mathisen, MD, Hermes C. Grillo, MD, John C. Wain, MD, and Alan D. Hilgenberg, MD Department of Surgery, Massachusetts General Hospital,
