Chronic Prostatitis/Chronic Pelvic Pain Syndrome and Male Bladder Pain Syndrome/Interstitial Cystitis: How Are They Related?
|
|
|
- Elvin Stevenson
- 5 years ago
- Views:
Transcription
1 Review ISSN (Print) / ISSN: (Online) Urogenit Tract Infect 2017;12(1): Chronic Prostatitis/Chronic Pelvic Pain Syndrome and Male Bladder Pain Syndrome/Interstitial Cystitis: How Are They Related? Sang Wook Lee Department of Urology, Kangwon National University School of Medicine, Chuncheon, Korea To date, the heterogeneous pathophysiology of chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS) and bladder pain syndrome/interstitial cystitis (BPS/IC) has not been fully elucidated. Thus, it is difficult to make a full comparison between CP/CPPS and male BPS/IC. Controversy and confusion surrounding the terminologies and classifications of CP/CPPS and BPS/IC complicates the issue. CP/CPPS and male BPS/IC are not mutually exclusive conditions, in that they have similarities in their pathogenesis and clinical presentation. Based on the working definitions of these terms, it would be correct to say that male BPS/IC is subsumed by CP/CPPS, and that male BPS/IC can be regarded as CP/CPPS with clear bladder-specific features. Although the term CP/CPPS may be inappropriate, especially since CP may be misleading, the perspective that CP/CPPS and male BPS/IC are male urological chronic pain syndromes could enhance the understanding of the relationship between the two. The European Association of Urology classification for chronic pelvic pain is systematic and corresponds well with our knowledge of chronic pain. Therefore, this classification might be the solution to the problems associated with the existing terminologies and taxonomy of CP/CPPS and BPS/IC. In the management of urological chronic pelvic pain in men, clinical phenotyping systems (the UPOINT or UPOINTs system) profile patients and indicate how tailored treatment could be achieved as individualized, multimodal therapeutic regimens. It would be prudent to include bladder-specific features, such as painful filling or painful urgency, in the criteria for the organ-specific domain of the UPOINT(s) system. Keywords: Classification; Diagnosis; Male; Pelvic pain; Syndrome Copyright 2017, Korean Association of Urogenital Tract Infection and Inflammation. All rights reserved. This is an open access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Received: 12 March, 2017 Revised: 3 April, 2017 Accepted: 3 April, 2017 Correspondence to: Sang Wook Lee Department of Urology, Kangwon National University Hospital, 156 Baengnyeong-ro, Chuncheon 24289, Korea Tel: , Fax: paulee@kangwon.ac.kr INTRODUCTION Traditionally, chronic pelvic pain accompanied by lower urinary tract symptoms in men was believed to arise from an inflammation of the prostate gland [1]. Men with these symptoms are usually diagnosed with chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS). Although bladder pain syndrome/interstitial cystitis (BPS/IC) is also characterized by pelvic pain associated with lower urinary tract symptoms, such as increased frequency of urination, it was believed to occur primarily in women. Until recently, male BPS/IC has received scant attention. However, contemporary studies suggest that male BPS/IC is much more common than was previously thought [2-5]; there has been increasing interest in male patients exhibiting symptoms and signs suggestive of BPS/IC. 15
2 16 Sang Wook Lee. CP/CPPS and Male BPS/IC Male BPS/IC is often initially diagnosed as CP/CPPS [6,7]. Evidence suggests that many men diagnosed with CP/CPPS could instead have been diagnosed with BPS/IC [1,7]. While some previous reports highlight the differences between CP/CPPS and male BPS/IC, there is substantial overlap in the clinical presentation and pathogenesis [1,6]. Moreover, the complex, heterogeneous pathophysiology of CP/CPPS and BPS/IC is poorly understood [8,9]. Therefore, it is difficult to compare and contrast CP/CPPS and male BPS/IC. Controversy and confusion surrounding the terms and taxonomy of CP/CPPS and BPS/IC complicates the issue. CP/CPPS and BPS/IC are now considered as chronic pain syndromes, rather than prostate or bladder diseases [10,11]. Regarding CP/CPPS and BPS/IC as urological chronic pain syndromes could promote better understanding of the relationship between CP/CPPS and male BPS/IC. This article outlines the relationship between CP/CPPS and male BPS/IC, presenting a prudent approach to male chronic pelvic pain. Herein, the definitions of CP/CPPS and BPS/IC are reviewed, and problems with the existing terminologies are discussed. The European Association of Urology (EAU) chronic pelvic pain classification system is suggested as a solution to these problems. Bladder-specific features in BPS/IC are also addressed. TERMS AND DEFINITIONS 1. CP/CPPS In the late 1990s, the National Institutes of Health (NIH) established a consensus on the definition and classification system for prostatitis syndromes, which has become the accepted international norm in both clinical practice and research [12]. The NIH classification of prostatitis syndromes includes four categories: (I) acute bacterial prostatitis, (II) chronic bacterial prostatitis, (III) CP/CPPS, and (IV) asymptomatic inflammatory prostatitis. More than 90% of symptomatic patients with prostatitis syndrome fall under the third category, CP/CPPS, which is described as chronic genitourinary pain in the absence of uropathogenic bacteria localized to the prostate gland using standard methodology. A detailed definition of CP/CPPS is urologic pain or discomfort in the pelvic region, associated with urinary symptoms or sexual dysfunction with a duration of at least 3 of the last 6 months [9]. The differential diagnoses of pelvic pain, such as urinary tract infection, malignancy, anatomic abnormalities, or neurologic disorders, need to be excluded. CP/CPPS is subclassified into either the inflammatory (NIH category IIIA) type or the noninflammatory (NIH category IIIB) type, based on the presence of leukocytes in the prostate samples [9,12]. The pain of CP/CPPS is most commonly localized to the perineum, suprapubic area, and penis; however, it can also be present in the testes, groin, or lower back [13]. In many patients, one of the most prominent, important, and bothersome features is pain during or after ejaculation [14]. In many patients diagnosed with CP/CPPS, the evidence of inflammation of the prostate cannot be found. There are no clinically relevant diagnostic or therapeutic consequences arising from differentiating between the inflammatory and non-inflammatory CP/CPPS [15]. It is also likely that the cause of CP/CPPS is multifactorial [16,17]. Organs other than the prostate gland may be more important in the genesis of this syndrome [12]. Even pelvic pain may be independent of the prostate, at least in some patients with CP/CPPS. Therefore, the term CP/CPPS appears to be inappropriate, and chronic prostatitis (CP) is especially misleading. We also should consider whether it is appropriate to classify CP/CPPS under prostatitis syndromes. Unlike BPS/IC, the name and working definition of CP/CPPS have remained stable for the past 20 years. It is my humble opinion to replace the name, CP/CPPS, with a more appropriate term, since it not only confuses clinicians but it also seems to hamper the research advancement in this area. 2. BPS/IC The nomenclature and taxonomy of BPS or IC have been evolving for many years and remain controversial [18,19]. IC, originally considered as a bladder disease, is now considered as a chronic pain syndrome [11]. Hanno [20] stated that the term IC did not describe the clinical syndrome or pathology in many cases. Moreover, the term IC seems to be misleading as it directs attention only to the urinary bladder and inflammation [18]. The meetings of the European Society for the Study of Interstitial Cystitis (ESSIC) in 2005 and 2006 arrived at a consensus: the term bladder pain syndrome (BPS) better complies with our present knowledge and current nomenclature of other pain syndromes than the terms interstitial cystitis (IC) and painful bladder syndrome
3 Sang Wook Lee. CP/CPPS and Male BPS/IC 17 (PBS). BPS can be diagnosed based on chronic (more than 6 months) pelvic pain, pressure, or discomfort, perceived to be related to the urinary bladder and accompanied by at least one other urinary symptom, such as persistent urge to void or frequency. Other confusable diseases must be excluded as the cause. Further documentation and classification of BPS, according to the findings of cystoscopy with hydrodistention and morphological findings of bladder biopsies, are encouraged. The presence of symptoms in other organs, as well as cognitive, behavioral, emotional, and sexual symptoms should be addressed [18]. The discontinuation of using the term, IC, might cause serious issues for healthcare systems, potentially affecting the reimbursement and the likelihood of patients receiving disability benefits, and so forth. Therefore, to promote a more straightforward change in nomenclature, the ESSIC agreed that the term BPS/IC could be used in parallel with BPS, at least for the time being [18]. Some clinicians preferred minor modifications, as expressed at the meeting held under the auspices of the Society for Urodynamics and Female Urology (SUFU). The SUFU definition was adopted in the guidelines of the American Urological Association, along with the nomenclature of IC/BPS [21]. RELATIONSHIP BETWEEN CP/CPPS AND MALE BPS/IC CP/CPPS and male BPS/IC are not mutually exclusive. There is a considerable overlap in the pathogenesis and clinical presentation between CP/CPPS and male BPS/IC [1,4,6,22-24]. CP/CPPS and BPS/IC are now considered as chronic pain syndromes, rather than prostate or bladder diseases [10,11]. Chronic pain that characterizes both CP/CPPS and BPS/IC is thought to be a consequence of neural sensitization [13,19]. Based on the definitions of the terms, it may be correct to say that male BPS/IC is a subset of CP/CPPS, or that male BPS/IC is subsumed by CP/CPPS. Pelvic pain, pressure, or discomfort perceived to be related to the urinary bladder, included in the definition of BPS/IC, is covered by urologic pain or discomfort in the pelvic region, included in the definition of CP/CPPS. In a detailed description of 488 men with CP/CPPS, the most frequently reported region of pain or discomfort was in perineum, followed by the suprapubic region [25]. Considering male BPS/IC as CP/CPPS with clear bladder-specific features could clarify the relationship between these two conditions. It is problematic to postulate that male BPS/IC is subsumed by CP/CPPS, as this contradicts the fact that CP/CPPS is a prostatitis syndrome. If the proposition that male BPS/IC is encompassed under CP/CPPS is true, then the proposition that male BPS/IC is included under prostatitis syndromes should also be true, as CP/CPPS is considered to be a prostatitis syndrome. This apparent contradiction is caused by the misleading term CP/CPPS and the current classification of prostatitis syndrome. To eliminate such a cognitive dissonance and resolve the confusion regarding terminologies and taxonomies, it may be necessary to change the nomenclature of CP/CPPS and establish a new consensus on the classification system for chronic pelvic pain and prostatitis syndromes. BLADDER-SPECIFIC FEATURES AND DIAGNOSIS OF BPS/IC Painful bladder filling and painful urgency (or painful urge to void) are main bladder-specific symptoms in BPS/IC. Painful filling is described as pain that worsens with the degree of bladder filling. The pain may be relieved at least partially by urination [26-28]. Painful urgency is described as the urge to urinate due mainly to pain, pressure, or discomfort, but not to fear of incontinence [26]. Painful urgency in BPS/IC differs from urgency in overactive bladder (OAB). Urgency is the key symptom of OAB and is defined as a sudden compelling desire to pass urine, which is difficult to defer [29]. Urgency in OAB is characterized by a sudden-onset fear of leakage, whereas painful urgency in BPS/IC has a persistent nature and is associated with fear of intensifying pain, pressure, or discomfort [30]. Severe storage symptoms are also bladder-specific symptoms, such as increased frequency of urination or nocturia. Here, voiding diary might serve as a useful tool. A recent study showed that patients with BPS/IC had a greater urinary frequency, a lower and more constant voided volume, and a narrower range of voided volume compared with patients with OAB [31]. Urinalysis results are usually normal in BPS/IC [32]. Numerous diagnostic biomarkers for BPS/IC have been explored, including antiproliferative factor, urinary and serum nerve growth factors, and urinary and serum
4 18 Sang Wook Lee. CP/CPPS and Male BPS/IC proinflammatory cytokines or chemokines. However, none of these putative biomarkers have been validated [33]. Potassium chloride bladder permeability test is no longer recommended, as it lacks sufficient evidence in its effectiveness [15]. Cystoscopy with hydrodistention, and biopsy under anesthesia, can be performed if indicated. According to the findings (Hunner lesions or glomerulations) of cystoscopy with hydrodistention and morphological findings of bladder biopsies, BPS/IC can further be classified [15,18]. Office cystoscopy is useful in that it can detect or exclude diseases, such as bladder cancer, and reproduce painful bladder filling in patients with BPS/IC. Hunner lesions or mucosal/submucosal bleeding may also be observed during the office cystoscopy, although the bladder cannot be filled as much as in cystoscopy under anesthesia. It is important to examine the bladder mucosa from the early phase of filling, as Hunner lesions might be obscured soon after bladder distention [32]. The lesions are more readily recognized by a narrow-band imaging cystoscopy [34]. A typical Hunner lesion is a circumscribed, reddened mucosal area with small vessels that radiate towards a central scar, with a fibrin deposit or coagulum attached to this area [18,35]. This site ruptures with increasing bladder distention, with petechial oozing of blood occurring from the lesion and the mucosal margins in a waterfall manner. It is important to detect these Hunner lesions because patients with these lesions have specific characteristics, such that this subgroup can be treated successfully [36]. PRUDENT APPROACH TO CHRONIC PELVIC PAIN IN MALES Patients with CP/CPPS or BPS/IC are an inhomogeneous group, with diverse etiologies and different responses to therapy. To classify patients with urological chronic pelvic pain (CP/CPPS and BPS/IC) and to direct appropriate therapy, a six-point clinical phenotyping system (the UPOINT system) had been proposed in the late 2000s [17,28,37,38]. The UPOINT system profiles patients and indicates how tailored treatment could be achieved as individualized multimodal therapeutic regimens. The clinical domains of UPOINT are Urinary symptoms, Psychosocial dysfunction, Organ-specific findings, Infection, Neurologic/systemic conditions, and Tenderness of muscles, providing mnemonic UPOINT. With sexual dysfunction affecting 40-70% of all men with CP/CPPS [39-41], the inclusion of an additional domain for sexual dysfunction was proposed, and a modified UPOINT algorithm (UPOINTs) has been suggested [42-44]. The original organ-specific domain for CP/CPPS is related only to the prostate, while the organ-specific domain for BPS/IC is related only to the bladder. For CP/CPPS, the organ-specific domain is considered to be positive if there is a specific prostate tenderness on examination, leukocytes on microscopic examination of the prostatic fluid, hematospermia, or extensive prostatic calcification [38]. In the UPOINT system for BPS/IC, the criteria for organ-specific domain include pain with bladder recycling (typically pain on bladder filling and temporary relief on voiding), pain on bladder filling with low volumes of irrigation fluid, glomerulations or Hunner lesions noted during cystoscopy, and typical inflammation confirmed by a bladder biopsy [28]. Recent studies suggest that the prevalence of BPS/IC in men might be higher than previously thought [2-5]. Men diagnosed with CP/CPPS may also have bladder-specific symptoms. Therefore, it would be more prudent to include bladder-specific features in addition to prostate-specific findings in the criteria for organ-specific domain when performing UPOINT-based evaluations in men suspected of having chronic pelvic pain. Samplaski et al. [27] characterized patients diagnosed with CP/CPPS using UPOINT domains and subdomains, and the organ-specific domain was subdivided into bladder (organ specific-bladder) and prostate (organ specific-prostate). The organ specific-bladder domain was positive in 33% of their patients. A research network study showed that 75% of all men with BPS/IC or CP/CPPS had painful filling or painful urgency [26]. EAU CLASSIFICATION OF CHRONIC PELVIC PAIN: SHOULD THE TERM CP/CPPS BE REPLACED? The first EAU guidelines on chronic pelvic pain were published in 2003 [45]. In 10 years, an updated version was accepted for publication in 2012 by the International Association for the Study of Pain Council [15]. The EAU classification defines chronic pelvic pain as chronic or persistent pain perceived in the structures related
5 Sang Wook Lee. CP/CPPS and Male BPS/IC 19 to the pelvis in either men or women. It is often associated with negative cognitive, behavioral, sexual, and emotional consequences, as well as with symptoms suggestive of lower urinary tract, sexual, bowel, pelvic floor, or gynecological dysfunction [15]. Chronic pelvic pain syndrome (CPPS) is a subgroup of chronic pelvic pain. CPPS is defined as the occurrence of chronic pelvic pain with no proven infection or other obvious pathology accounting for pain. In the EAU classification, CPPS is an umbrella term that includes non-urological CPPS, and it should be differentiated from CP/CPPS. The pain perceived in CPPS may be localized within a single organ, or may be experienced in more than one pelvic organ; moreover, it can even be associated with systemic symptoms, as seen in chronic fatigue syndrome, fibromyalgia, or Sjogren s syndrome. When pain is localized to a single organ, some specialists may wish to consider using an end-organ term, such as bladder pain syndrome (BPS), prostate pain syndrome (PPS), or urethral pain syndrome. When pain is localized to more than one organ, or pain cannot be clearly ascribed to one organ, the term CPPS should be used [15]. The definition and subtypes of BPS in this classification follow the proposal set forth by ESSIC. Consequently, BPS in the EAU classification is on par with BPS/IC (or BPS) in the ESSIC proposal. PPS is defined as the occurrence of persistent or recurrent episodic pain in the region of the prostate during at least 3 of the previous 6 months, which is convincingly reproduced by prostate palpation [15]. CP/CPPS is generally classified as CPPS in the EAU classification, although some cases of CP/CPPS could be classified as PPS. The EAU classification of chronic pelvic pain is logical and systematic, and it concurs with our knowledge of chronic pain. It could also resolve the problems associated with the current terminologies and taxonomies of CP/CPPS and BPS/IC. Of course, it is difficult to change the terms with a wide currency, and there are many obstacles to changing the existing system. Furthermore, reaching a consensus on new terminologies and classifications is a challenging and time-consuming task. Nevertheless, a change is necessary for the improvement in clinical practice and communication. Whether or not we accept the EAU classification of chronic pelvic pain on an international scale, it seems appropriate to replace the misleading name Fig. 1. Conceptualization of the classification of male chronic pelvic pain syndrome. The Venn diagram shows the relationship between chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS), male bladder pain syndrome/interstitial cystitis (BPS/IC), and male chronic pelvic pain syndrome (CPPS). It seems appropriate to replace the misleading term CP/CPPS with male urological CPPS (UCPPS). The CPPS in male CPPS is an umbrella term that includes non-urological CPPS and should be differentiated from CP/CPPS. CP/CPPS with male CPPS or male urological CPPS (Fig. 1). CONCLUSIONS CP/CPPS and male BPS/IC are not mutually exclusive conditions, as they have much in common with respect to their pathogenesis and clinical presentations. Based on the working definitions of these terms, it would be correct to say that male BPS/IC is included under CP/CPPS, and that male BPS/IC may be regarded as CP/CPPS with clear bladder-specific features. Although the term CP/CPPS may be inappropriate and misleading, considering CP/CPPS and male BPS/IC as male urological chronic pain syndromes could help us better understand the relationship between them. The EAU classification of chronic pelvic pain might solve the problems associated with the existing terminology and taxonomy for CP/CPPS and BPS/IC. A multimodal therapeutic approach addressing the clinical phenotypic profile on an individual basis is recommended to manage male cases of chronic pelvic pain. It would be prudent to also include bladder-specific features, such as painful filling or painful urgency in the criteria for organ-specific domain of the UPOINT(s) system. CONFLICT OF INTEREST No potential conflict of interest relevant to this article was reported.
6 20 Sang Wook Lee. CP/CPPS and Male BPS/IC REFERENCES 1. Forrest JB, Nickel JC, Moldwin RM. Chronic prostatitis/chronic pelvic pain syndrome and male interstitial cystitis: enigmas and opportunities. Urology 2007;69(4 Suppl): Forrest JB, Vo Q. Observations on the presentation, diagnosis, and treatment of interstitial cystitis in men. Urology 2001;57(6 Suppl 1): Clemens JQ, Meenan RT, Rosetti MC, Gao SY, Calhoun EA. Prevalence and incidence of interstitial cystitis in a managed care population. J Urol 2005;173: Forrest JB, Schmidt S. Interstitial cystitis, chronic nonbacterial prostatitis and chronic pelvic pain syndrome in men: a common and frequently identical clinical entity. J Urol 2004;172: Suskind AM, Berry SH, Ewing BA, Elliott MN, Suttorp MJ, Clemens JQ. The prevalence and overlap of interstitial cystitis/ bladder pain syndrome and chronic prostatitis/chronic pelvic pain syndrome in men: results of the RAND Interstitial Cystitis Epidemiology male study. J Urol 2013;189: Arora HC, Shoskes DA. The enigma of men with interstitial cystitis/bladder pain syndrome. Transl Androl Urol 2015;4: Parsons CL, Rosenberg MT, Sassani P, Ebrahimi K, Koziol JA, Zupkas P. Quantifying symptoms in men with interstitial cystitis/ prostatitis, and its correlation with potassium-sensitivity testing. BJU Int 2005;95: Hanno P, Lin A, Nordling J, Nyberg L, van Ophoven A, Ueda T, et al. Bladder pain syndrome international consultation on incontinence. Neurourol Urodyn 2010;29: Magistro G, Wagenlehner FM, Grabe M, Weidner W, Stief CG, Nickel JC. Contemporary management of chronic prostatitis/ chronic pelvic pain syndrome. Eur Urol 2016;69: Hanno P, Andersson KE, Birder L, Elneil S, Kanai A, Pontari M. Chronic pelvic pain syndrome/bladder pain syndrome: taking stock, looking ahead: ICI-RS Neurourol Urodyn 2012;31: Janicki TI. Chronic pelvic pain as a form of complex regional pain syndrome. Clin Obstet Gynecol 2003;46: Krieger JN, Nyberg L Jr, Nickel JC. NIH consensus definition and classification of prostatitis. JAMA 1999;282: Nickel JC. Inflammatory and pain conditions of the male genitourinary tract. In: Wein AJ, Kavoussi LR, Partin AW, Peters C, Campbell MF, Walsh PC, editors. Campbell-Walsh urology. 11th ed. Philadelphia: Elsevier; p Shoskes DA, Landis JR, Wang Y, Nickel JC, Zeitlin SI, Nadler R; Chronic Prostatitis Collaborative Research Network Study Group. Impact of post-ejaculatory pain in men with category III chronic prostatitis/chronic pelvic pain syndrome. J Urol 2004;172: Engeler D, Baranowski AP, Borovicka J, Cottrell A, Dinis- Oliveira P, Elneil S, et al; The European Association of Urology. Guidelines on chronic pelvic pain [Internet]. Available from: nic-pelvic-pain-2015.pdf. 16. Shoskes DA, Katz E. Multimodal therapy for chronic prostatitis/ chronic pelvic pain syndrome. Curr Urol Rep 2005;6: Shoskes DA, Nickel JC, Dolinga R, Prots D. Clinical phenotyping of patients with chronic prostatitis/chronic pelvic pain syndrome and correlation with symptom severity. Urology 2009;73: van de Merwe JP, Nordling J, Bouchelouche P, Bouchelouche K, Cervigni M, Daha LK, et al. Diagnostic criteria, classification, and nomenclature for painful bladder syndrome/interstitial cystitis: an ESSIC proposal. Eur Urol 2008;53: Hanno PM. Bladder pain syndrome (interstitial cystitis) and related disorders. In: Wein AJ, Kavoussi LR, Partin AW, Peters C, Campbell MF, Walsh PC, editors. Campbell-Walsh urology. 11th ed. Philadelphia: Elsevier; p Hanno PM. Re-imagining interstitial cystitis. Urol Clin North Am 2008;35: Hanno PM, Burks DA, Clemens JQ, Dmochowski RR, Erickson D, Fitzgerald MP, et al. AUA guideline for the diagnosis and treatment of interstitial cystitis/bladder pain syndrome. J Urol 2011;185: Pontari MA. Chronic prostatitis/chronic pelvic pain syndrome and interstitial cystitis: are they related? Curr Urol Rep 2006;7: Eisenberg ER, Moldwin RM. Etiology: where does prostatitis stop and interstitial cystitis begin? World J Urol 2003;21: Parsons CL. Prostatitis, interstitial cystitis, chronic pelvic pain, and urethral syndrome share a common pathophysiology: lower urinary dysfunctional epithelium and potassium recycling. Urology 2003;62: Schaeffer AJ, Landis JR, Knauss JS, Propert KJ, Alexander RB, Litwin MS, et al. Demographic and clinical characteristics of men with chronic prostatitis: the national institutes of health chronic prostatitis cohort study. J Urol 2002;168: Lai HH, Krieger JN, Pontari MA, Buchwald D, Hou X, Landis JR; MAPP Research Network. Painful bladder filling and painful urgency are distinct characteristics in men and women with urological chronic pelvic pain syndromes: a MAPP research network study. J Urol 2015;194: Samplaski MK, Li J, Shoskes DA. Clustering of UPOINT domains and subdomains in men with chronic prostatitis/ chronic pelvic pain syndrome and contribution to symptom severity. J Urol 2012;188: Nickel JC, Shoskes D, Irvine-Bird K. Clinical phenotyping of women with interstitial cystitis/painful bladder syndrome: a key to classification and potentially improved management. J Urol 2009;182: Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U, et al. The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Neurourol Urodyn
7 Sang Wook Lee. CP/CPPS and Male BPS/IC ;21: Homma Y. Hypersensitive bladder: a solution to confused terminology and ignorance concerning interstitial cystitis. Int J Urol 2014;21 Suppl 1: Kim SH, Oh SA, Oh SJ. Voiding diary might serve as a useful tool to understand differences between bladder pain syndrome/ interstitial cystitis and overactive bladder. Int J Urol 2014;21: Homma Y, Ueda T, Tomoe H, Lin AT, Kuo HC, Lee MH, et al. Clinical guidelines for interstitial cystitis and hypersensitive bladder updated in Int J Urol 2016;23: Kuo HC. Potential urine and serum biomarkers for patients with bladder pain syndrome/interstitial cystitis. Int J Urol 2014;21 Suppl 1: Ueda T, Nakagawa M, Okamura M, Tanoue H, Yoshida H, Yoshimura N. New cystoscopic diagnosis for interstitial cystitis/painful bladder syndrome using narrow-band imaging system. Int J Urol 2008;15: Fall M, Johansson SL, Aldenborg F. Chronic interstitial cystitis: a heterogeneous syndrome. J Urol 1987;137: Nordling J, Fall M, Hanno P. Global concepts of bladder pain syndrome (interstitial cystitis). World J Urol 2012;30: Shoskes DA, Nickel JC, Rackley RR, Pontari MA. Clinical phenotyping in chronic prostatitis/chronic pelvic pain syndrome and interstitial cystitis: a management strategy for urologic chronic pelvic pain syndromes. Prostate Cancer Prostatic Dis 2009;12: Shoskes DA, Nickel JC, Kattan MW. Phenotypically directed multimodal therapy for chronic prostatitis/chronic pelvic pain syndrome: a prospective study using UPOINT. Urology 2010;75: Trinchieri A, Magri V, Cariani L, Bonamore R, Restelli A, Garlaschi MC, et al. Prevalence of sexual dysfunction in men with chronic prostatitis/chronic pelvic pain syndrome. Arch Ital Urol Androl 2007;79: Lee SW, Liong ML, Yuen KH, Leong WS, Cheah PY, Khan NA, et al. Adverse impact of sexual dysfunction in chronic prostatitis/ chronic pelvic pain syndrome. Urology 2008;71: Mehik A, Hellstrom P, Sarpola A, Lukkarinen O, Jarvelin MR. Fears, sexual disturbances and personality features in men with prostatitis: a population-based cross-sectional study in Finland. BJU Int 2001;88: Magri V, Wagenlehner F, Perletti G, Schneider S, Marras E, Naber KG, et al. Use of the UPOINT chronic prostatitis/chronic pelvic pain syndrome classification in European patient cohorts: sexual function domain improves correlations. J Urol 2010;184: Davis SN, Binik YM, Amsel R, Carrier S. Is a sexual dysfunction domain important for quality of life in men with urological chronic pelvic pain syndrome? Signs "UPOINT" to yes. J Urol 2013;189: Samplaski MK, Li J, Shoskes DA. Inclusion of erectile domain to UPOINT phenotype does not improve correlation with symptom severity in men with chronic prostatitis/chronic pelvic pain syndrome. Urology 2011;78: Fall M, Baranowski AP, Fowler CJ, Lepinard V, Malone-Lee JG, Messelink EJ, et al. EAU guidelines on chronic pelvic pain. Eur Urol 2004;46:681-9.
Clinical Significance of National Institutes of Health Classification in Patients With Chronic Prostatitis/Chronic Pelvic Pain Syndrome
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.4.276 Original Article - Infection/Inflammation http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.4.276&domain=pdf&date_stamp=2014-04-17
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.4.276 Original Article - Infection/Inflammation http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.4.276&domain=pdf&date_stamp=2014-04-17
INTERSTITIAL CYSTITIS (IC) MANAGEMENT
 INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
Prostatitis: overview and assessment of pain outcomes and implications for inclusion criteria. Michel Pontari IMMPACT-XX Meeting July 13, 2017
 Prostatitis: overview and assessment of pain outcomes and implications for inclusion criteria Michel Pontari IMMPACT-XX Meeting July 13, 2017 NIDDK Classification of Prostatitis 1 Type I: Acute Bacterial
Prostatitis: overview and assessment of pain outcomes and implications for inclusion criteria Michel Pontari IMMPACT-XX Meeting July 13, 2017 NIDDK Classification of Prostatitis 1 Type I: Acute Bacterial
Addendum 1: International Consultation
 Reprinted with Permission of the International Consultation on Urological Diseases and the International Continence Society Hanno PM, Cervigni M, Dinis P, Lin A, Nickel JC, Nordling J, van Ophoven A, Ueda
Reprinted with Permission of the International Consultation on Urological Diseases and the International Continence Society Hanno PM, Cervigni M, Dinis P, Lin A, Nickel JC, Nordling J, van Ophoven A, Ueda
Is Urethral Pain Syndrome Really Part of Bladder Pain Syndrome?
 Review ISSN 2465-8243(Print) / ISSN: 2465-8510(Online) https://doi.org/10.14777/uti.2017.12.1.22 Urogenit Tract Infect 2017;12(1):22-27 http://crossmark.crossref.org/dialog/?doi=10.14777/uti.2017.12.1.&domain=pdf&date_stamp=2017-04-25
Review ISSN 2465-8243(Print) / ISSN: 2465-8510(Online) https://doi.org/10.14777/uti.2017.12.1.22 Urogenit Tract Infect 2017;12(1):22-27 http://crossmark.crossref.org/dialog/?doi=10.14777/uti.2017.12.1.&domain=pdf&date_stamp=2017-04-25
Dr. Krithika Doshi. Chronic Pelvic Pain: Headache in the Pelvis Pelvic Pain in Men- Are they all Noncyclical?
 Chronic Pelvic Pain: Headache in the Pelvis Pelvic Pain in Men- Are they all Noncyclical? Dr Kritika Doshi Introduction: Chronic pelvic and urogenital pain syndromes have recently been recognized as a
Chronic Pelvic Pain: Headache in the Pelvis Pelvic Pain in Men- Are they all Noncyclical? Dr Kritika Doshi Introduction: Chronic pelvic and urogenital pain syndromes have recently been recognized as a
The three As of chronic prostatitis therapy: antibiotics, a-blockers and anti-inflammatories. What is the evidence?
 Rev Article CHRONIC PROSTATITIS THERAPY NICKEL The three As of chronic prostatitis therapy: antibiotics, a-blockers and anti-inflammatories. What is the evidence? J. CURTIS NICKEL Department of Urology,
Rev Article CHRONIC PROSTATITIS THERAPY NICKEL The three As of chronic prostatitis therapy: antibiotics, a-blockers and anti-inflammatories. What is the evidence? J. CURTIS NICKEL Department of Urology,
Interstitial Cystitis:
 Diagnosis and Definition ESSIC approach Jørgen Nordling, chairman ESSIC Professor of Urology University of Copenhagen Denmark Interstitial Cystitis: A painful, potentially disabling, inflammatory disease
Diagnosis and Definition ESSIC approach Jørgen Nordling, chairman ESSIC Professor of Urology University of Copenhagen Denmark Interstitial Cystitis: A painful, potentially disabling, inflammatory disease
BPS/IC: evolution of definition and prevalence
 BPS/IC: evolution of definition and prevalence ame in history Tic doloureux of the bladder 1836 Interstitial cystitis 1878 Cystitis parenchymatosa 197 unner s ulcer 1915 Panmural ulcerative cystitis 192
BPS/IC: evolution of definition and prevalence ame in history Tic doloureux of the bladder 1836 Interstitial cystitis 1878 Cystitis parenchymatosa 197 unner s ulcer 1915 Panmural ulcerative cystitis 192
Role of cystoscopy and hydrodistention in the diagnosis of interstitial cystitis/bladder pain syndrome
 Review Article Role of cystoscopy and hydrodistention in the diagnosis of interstitial cystitis/bladder pain syndrome Gisela Ens, Gustavo L. Garrido Voiding Dysfunction and Urodynamic Section, Division
Review Article Role of cystoscopy and hydrodistention in the diagnosis of interstitial cystitis/bladder pain syndrome Gisela Ens, Gustavo L. Garrido Voiding Dysfunction and Urodynamic Section, Division
Hypersensitive bladder: A solution to confused terminology and ignorance concerning interstitial cystitis
 bs_bs_banner International Journal of Urology (2014) 21 (Suppl 1), 43 47 doi: 10.1111/iju.12314 Review Article Hypersensitive bladder: A solution to confused terminology and ignorance concerning interstitial
bs_bs_banner International Journal of Urology (2014) 21 (Suppl 1), 43 47 doi: 10.1111/iju.12314 Review Article Hypersensitive bladder: A solution to confused terminology and ignorance concerning interstitial
Rawal Medical Journal
 Rawal Medical Journal An official publication of Pakistan Medical Association Rawalpindi Islamabad branch Established 1975 Volume 36 Number 4 October - December 2011 Original Article Role of alpha blockers
Rawal Medical Journal An official publication of Pakistan Medical Association Rawalpindi Islamabad branch Established 1975 Volume 36 Number 4 October - December 2011 Original Article Role of alpha blockers
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Disease State Prostatitis Indicator Classification Disease Management Strength of Recommendation
 Client HMSA: PQSR 2009 Measure Title DIAGNOSTIC WORKUP OF CHRONIC PROSTATITIS Disease State Prostatitis Indicator Classification Disease Management Strength of Recommendation B Organizations Providing
Client HMSA: PQSR 2009 Measure Title DIAGNOSTIC WORKUP OF CHRONIC PROSTATITIS Disease State Prostatitis Indicator Classification Disease Management Strength of Recommendation B Organizations Providing
CHRONIC PELVIC PAIN SYNDROME. Jay Lee, MD, FRCSC Clinical Assistant Professor, University of Calgary
 CHRONIC PELVIC PAIN SYNDROME Jay Lee, MD, FRCSC Clinical Assistant Professor, University of Calgary Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
CHRONIC PELVIC PAIN SYNDROME Jay Lee, MD, FRCSC Clinical Assistant Professor, University of Calgary Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective?
 Original Article In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective? Hikaru Tomoe Department of Urology and Pelvic Reconstructive Surgery, Tokyo
Original Article In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective? Hikaru Tomoe Department of Urology and Pelvic Reconstructive Surgery, Tokyo
The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence
 european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
In evaluating a patient with lower urinary tract symptoms (LUTS), urologists
 CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS Interstitial Cystitis and Lower Urinary Tract Symptoms in Males and Females The Combined Role of Potassium and Epithelial Dysfunction C. Lowell Parsons, MD
CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS Interstitial Cystitis and Lower Urinary Tract Symptoms in Males and Females The Combined Role of Potassium and Epithelial Dysfunction C. Lowell Parsons, MD
Chronic pelvic pain-when surgery fails
 Chronic pelvic pain-when surgery fails Sherif Tawfeek FRANZCOG, FRCOG, FICS, MSc, Dip-Endoscopy Consultant in Obstetrics and Gynaecology Senior lecturer at University of Otago Objectives Identify the common
Chronic pelvic pain-when surgery fails Sherif Tawfeek FRANZCOG, FRCOG, FICS, MSc, Dip-Endoscopy Consultant in Obstetrics and Gynaecology Senior lecturer at University of Otago Objectives Identify the common
DELAYED DIAGNOSIS. Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >60%
 DELAYED DIAGNOSIS Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >6% 1 PREVALENCE 1,, 9,, 8,, 7,, 6,, 5,, 4,, 3,, 2,, 1,, NHS "Prostatitis" "Endometriosis" The
DELAYED DIAGNOSIS Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >6% 1 PREVALENCE 1,, 9,, 8,, 7,, 6,, 5,, 4,, 3,, 2,, 1,, NHS "Prostatitis" "Endometriosis" The
BLADDER HEALTH. Painful Bladder AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION
 BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Studies Few But Promising at 2010 AUA Meeting
 Studies Few But Promising at 2010 AUA Meeting The 2010 American Urological Association s annual meeting brought fewer studies of chronic prostatitis/chronic pelvic pain (CP/CPPS) than in the past. That
Studies Few But Promising at 2010 AUA Meeting The 2010 American Urological Association s annual meeting brought fewer studies of chronic prostatitis/chronic pelvic pain (CP/CPPS) than in the past. That
Bladder pain syndrome / Interstitial cystitis
 Bladder pain syndrome / Interstitial cystitis Terminology The term bladder pain syndrome/interstitial cystitis (BPS/IC) is defined as the presence of chronic pain, pressure, or pelvic discomfort lasting
Bladder pain syndrome / Interstitial cystitis Terminology The term bladder pain syndrome/interstitial cystitis (BPS/IC) is defined as the presence of chronic pain, pressure, or pelvic discomfort lasting
Chronic Prostatitis/Chronic Pelvic Pain Syndrome: Basing a Treatment Strategy on Randomized Placebo Controlled Trials 2012
 Chronic Prostatitis/Chronic Pelvic Pain Syndrome: Basing a Treatment Strategy on Randomized Placebo Controlled Trials 2012 J. Curtis Nickel Professor of Urology, Queen s University Canada CIHR Canada Research
Chronic Prostatitis/Chronic Pelvic Pain Syndrome: Basing a Treatment Strategy on Randomized Placebo Controlled Trials 2012 J. Curtis Nickel Professor of Urology, Queen s University Canada CIHR Canada Research
Effect of Low-Dose Amitriptyline Treatment for Interstitial Cystitis/Bladder Pain Syndrome
 ORIGINAL ARTICLE Effect of Low-Dose Amitriptyline Treatment for Interstitial Cystitis/Bladder Pain Syndrome Weiguo Chen 1, Donghua Xie 2, Guolu Liu 1, Yifan Chen 1, Zongqiang Cai 1 1 Department of Urology,
ORIGINAL ARTICLE Effect of Low-Dose Amitriptyline Treatment for Interstitial Cystitis/Bladder Pain Syndrome Weiguo Chen 1, Donghua Xie 2, Guolu Liu 1, Yifan Chen 1, Zongqiang Cai 1 1 Department of Urology,
INTRODUCTION. Original Article - Lower Urinary Tract Dysfunction. Aram Kim 1, Kyeong-Ok Hoe 2, Jung Hyun Shin 2, Myung-Soo Choo 2 1
 Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:353-358. pissn 2466-0493 eissn 2466-054X Evaluation of the incidence and risk factors associated with persistent frequency
Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:353-358. pissn 2466-0493 eissn 2466-054X Evaluation of the incidence and risk factors associated with persistent frequency
Novel research approaches for interstitial cystitis/bladder pain syndrome: thinking beyond the bladder
 Review Article Novel research approaches for interstitial cystitis/bladder pain syndrome: thinking beyond the bladder Chris Mullins, Tamara Bavendam, Ziya Kirkali, John W. Kusek National Institute of Diabetes
Review Article Novel research approaches for interstitial cystitis/bladder pain syndrome: thinking beyond the bladder Chris Mullins, Tamara Bavendam, Ziya Kirkali, John W. Kusek National Institute of Diabetes
REVIEW. International Journal of Surgery
 International Journal of Surgery 11 (2013) 233e237 Contents lists available at SciVerse ScienceDirect International Journal of Surgery journal homepage: www.theijs.com Review The evil twin syndrome in
International Journal of Surgery 11 (2013) 233e237 Contents lists available at SciVerse ScienceDirect International Journal of Surgery journal homepage: www.theijs.com Review The evil twin syndrome in
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Prevalence of sexual dysfunction in men with chronic prostatitis/ chronic pelvic pain syndrome: a meta analysis
 DOI 10.1007/s00345-015-1720-3 ORIGINAL ARTICLE Prevalence of sexual dysfunction in men with chronic prostatitis/ chronic pelvic pain syndrome: a meta analysis Hong Jun Li 1 De Ying Kang 2 Received: 25
DOI 10.1007/s00345-015-1720-3 ORIGINAL ARTICLE Prevalence of sexual dysfunction in men with chronic prostatitis/ chronic pelvic pain syndrome: a meta analysis Hong Jun Li 1 De Ying Kang 2 Received: 25
How does interstitial cystitis begin?
 Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
32 OBG Management July 2010 Vol. 22 No. 7 obgmanagement.com
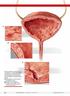 A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
EUROPEAN UROLOGY 63 (2013)
 EUROPEAN UROLOGY 63 (2013) 953 959 available at www.sciencedirect.com journal homepage: www.europeanurology.com Pelvic Pain National Institutes of Health Chronic Prostatitis Symptom Index (NIH-CPSI) Symptom
EUROPEAN UROLOGY 63 (2013) 953 959 available at www.sciencedirect.com journal homepage: www.europeanurology.com Pelvic Pain National Institutes of Health Chronic Prostatitis Symptom Index (NIH-CPSI) Symptom
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE?
 PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
Diagnosis and Mangement of Nocturia in Adults
 Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
TADALAFIL THERAPY IN PATIENTS WITH CHRONIC PROSTATITIS/CHRONIC PELVIC PAIN SYNDROME: RANDOMIZED, CONTROLLED TRIAL
 AL-AZHAR ASSIUT MEDCAIL JOURNAL TADALAFIL THERAPY IN PATIENTS WITH CHRONIC PROSTATITIS/CHRONIC PELVIC PAIN SYNDROME: RANDOMIZED, CONTROLLED TRIAL Department of Urology, Al-Azhar University, Cairo, Egypt.
AL-AZHAR ASSIUT MEDCAIL JOURNAL TADALAFIL THERAPY IN PATIENTS WITH CHRONIC PROSTATITIS/CHRONIC PELVIC PAIN SYNDROME: RANDOMIZED, CONTROLLED TRIAL Department of Urology, Al-Azhar University, Cairo, Egypt.
Non-Inflammatory Chronic Pelvic Pain Syndrome Can Be Caused by Bladder Neck Hypertrophy
 European Urology European Urology 44 (2003) 106 110 Non-Inflammatory Chronic Pelvic Pain Syndrome Can Be Caused by Bladder Neck Hypertrophy Petr Hruz, Hansjörg Danuser, Urs E. Studer, Werner W. Hochreiter
European Urology European Urology 44 (2003) 106 110 Non-Inflammatory Chronic Pelvic Pain Syndrome Can Be Caused by Bladder Neck Hypertrophy Petr Hruz, Hansjörg Danuser, Urs E. Studer, Werner W. Hochreiter
These authors contributed equally to this work. * (YZ); (CD)
 RESEARCH ARTICLE Erectile Dysfunction in Chronic Prostatitis/ Chronic Pelvic Pain Syndrome: Outcomes from a Multi-Center Study and Risk Factor Analysis in a Single Center Yadong Zhang 1 *, Tao Zheng 1,
RESEARCH ARTICLE Erectile Dysfunction in Chronic Prostatitis/ Chronic Pelvic Pain Syndrome: Outcomes from a Multi-Center Study and Risk Factor Analysis in a Single Center Yadong Zhang 1 *, Tao Zheng 1,
ESSIC 2008 Annual Meeting Rome
 Bladder Pain Syndrome Developing a History Protocol Normal Bladder Function Depends on Suzy, Arul, Andrei, Arvind Integrity of the macroscopic and microscopic anatomy of the bladder Central nervous system
Bladder Pain Syndrome Developing a History Protocol Normal Bladder Function Depends on Suzy, Arul, Andrei, Arvind Integrity of the macroscopic and microscopic anatomy of the bladder Central nervous system
Lower Urinary Tract Symptoms BPH vs OAB FLOW vs VOLUME. Matt T. Rosenberg, MD Family Practice Mid Michigan Health Centers Jackson, Michigan
 Lower Urinary Tract Symptoms BPH vs OAB FLOW vs VOLUME Matt T. Rosenberg, MD Family Practice Mid Michigan Health Centers Jackson, Michigan 1 Definition of OAB Syndrome or symptom complex defined as urgency,
Lower Urinary Tract Symptoms BPH vs OAB FLOW vs VOLUME Matt T. Rosenberg, MD Family Practice Mid Michigan Health Centers Jackson, Michigan 1 Definition of OAB Syndrome or symptom complex defined as urgency,
Male Chronic Pelvic Pain. Josef van Eyk Associate Specialist Jefferiss Wing
 Male Chronic Pelvic Pain Josef van Eyk Associate Specialist Jefferiss Wing Josef.vaneyk@nhs.net Learning Objectives Overview of Chronic Pelvic Pain Recognise the complexity of CPPS and importance of detailed
Male Chronic Pelvic Pain Josef van Eyk Associate Specialist Jefferiss Wing Josef.vaneyk@nhs.net Learning Objectives Overview of Chronic Pelvic Pain Recognise the complexity of CPPS and importance of detailed
Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy
 Review Article Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy Mauro Cervigni Interstitial Cystitis Referral Center, Catholic University, Rome, Italy Correspondence
Review Article Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy Mauro Cervigni Interstitial Cystitis Referral Center, Catholic University, Rome, Italy Correspondence
Interstitial cystitis (IC), also
 Interstitial cystitis: Algorithm to simplify diagnosis of chronic urinary symptoms By Anita L. Booth, DNP, FNP-BC and Jill Harpst Rodgers, DNP, FNP-BC This pre/post-test study was undertaken to determine
Interstitial cystitis: Algorithm to simplify diagnosis of chronic urinary symptoms By Anita L. Booth, DNP, FNP-BC and Jill Harpst Rodgers, DNP, FNP-BC This pre/post-test study was undertaken to determine
Cystoscopic and Histopathologic Patterns in Iraqi Patients with Chronic Cystitis /Painful Bladder Syndrome
 CHRONIC THE IRAQI POSTGRADUATE CYSTITIS /PAINFUL MEDICAL BLADDER JOURNAL SYNDROME VOL., NO., Cystoscopic and Histopathologic Patterns in Iraqi Patients with Chronic Cystitis /Painful Bladder Syndrome Issam
CHRONIC THE IRAQI POSTGRADUATE CYSTITIS /PAINFUL MEDICAL BLADDER JOURNAL SYNDROME VOL., NO., Cystoscopic and Histopathologic Patterns in Iraqi Patients with Chronic Cystitis /Painful Bladder Syndrome Issam
Bladder Pain Syndrome Current Concepts and Management Guidelines
 Review Article Bladder Pain Syndrome Current Concepts and Management Guidelines Amita Jain To cite: Jain A. Bladder Pain Syndrome Current Concepts and Management Guidelines. Pan Asian J Obs Gyn 2018;1(1):18-23.
Review Article Bladder Pain Syndrome Current Concepts and Management Guidelines Amita Jain To cite: Jain A. Bladder Pain Syndrome Current Concepts and Management Guidelines. Pan Asian J Obs Gyn 2018;1(1):18-23.
Prevalence of Prostatitis-Like Symptoms in Singapore: A Population-Based Study
 Singapore Med J 2002 Vol 43(4) : 189-193 O r i g i n a l A r t i c l e Prevalence of Prostatitis-Like Symptoms in Singapore: A Population-Based Study J K Tan, D J C Png, L C H Liew, M K Li, M L Wong ABSTRACT
Singapore Med J 2002 Vol 43(4) : 189-193 O r i g i n a l A r t i c l e Prevalence of Prostatitis-Like Symptoms in Singapore: A Population-Based Study J K Tan, D J C Png, L C H Liew, M K Li, M L Wong ABSTRACT
The Management of Urological Pelvic Pain Syndromes
 The Management of Urological Pelvic Pain Syndromes Professor of Urology North Shore-LIJ Hofstra School of Medicine The Arthur Smith Institute for Urology New Hyde Park, New York Chronic Pelvic Pain: The
The Management of Urological Pelvic Pain Syndromes Professor of Urology North Shore-LIJ Hofstra School of Medicine The Arthur Smith Institute for Urology New Hyde Park, New York Chronic Pelvic Pain: The
The Effect of Biofeedback Physical Therapy in Men with Chronic Pelvic Pain SyndromeType III
 European Urology European Urology 47 (2005) 607 611 The Effect of Biofeedback Physical Therapy in Men with Chronic Pelvic Pain SyndromeType III Erik B. Cornel a, *, Ernst P. van Haarst b, Ria W.M. Browning-Groote
European Urology European Urology 47 (2005) 607 611 The Effect of Biofeedback Physical Therapy in Men with Chronic Pelvic Pain SyndromeType III Erik B. Cornel a, *, Ernst P. van Haarst b, Ria W.M. Browning-Groote
Prevalence of the Overactive Bladder Syndrome byapplying the International Continence Society Definition
 European Urology European Urology 48 (2005) 622 627 Female Urology ^ Incontinence Prevalence of the Overactive Bladder Syndrome byapplying the International Continence Society Definition Christian Temml
European Urology European Urology 48 (2005) 622 627 Female Urology ^ Incontinence Prevalence of the Overactive Bladder Syndrome byapplying the International Continence Society Definition Christian Temml
NIH Public Access Author Manuscript J Urol. Author manuscript; available in PMC 2015 May 01.
 NIH Public Access Author Manuscript Published in final edited form as: J Urol. 2014 May ; 191(5): 1294 1299. doi:10.1016/j.juro.2013.11.099. Segmental Hyperalgesia to Mechanical Stimulus in Interstitial
NIH Public Access Author Manuscript Published in final edited form as: J Urol. 2014 May ; 191(5): 1294 1299. doi:10.1016/j.juro.2013.11.099. Segmental Hyperalgesia to Mechanical Stimulus in Interstitial
J.C. NICKEL, J. DOWNEY, M.A. PONTARI*, D.A. SHOSKES
 Original Article FINASTERIDE TREATMENT OF CHRONIC PELVIC PAIN SYNDROME J.C. NICKEL et al. A randomized placebo-controlled multicentre study to evaluate the safety and efficacy of finasteride for male chronic
Original Article FINASTERIDE TREATMENT OF CHRONIC PELVIC PAIN SYNDROME J.C. NICKEL et al. A randomized placebo-controlled multicentre study to evaluate the safety and efficacy of finasteride for male chronic
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Clinical comparison of intravesical hyaluronic acid and chondroitin sulfate therapies in the treatment of bladder pain syndrome/interstitial cystitis
 Received: 17 December 2016 Accepted: 26 February 2017 DOI: 10.1002/nau.23284 ORIGINAL CLINICAL ARTICLE Clinical comparison of intravesical hyaluronic acid and chondroitin sulfate therapies in the treatment
Received: 17 December 2016 Accepted: 26 February 2017 DOI: 10.1002/nau.23284 ORIGINAL CLINICAL ARTICLE Clinical comparison of intravesical hyaluronic acid and chondroitin sulfate therapies in the treatment
Overactive Bladder in Clinical Practice
 Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
5-8 July, 2008, Palais des Congrès, Paris, France
 A review of the 4 th INTERNATIONAL CONSULTATION ON INCONTINENCE 5-8 July, 2008, Palais des Congrès, Paris, France The 4 th International Consultation on Incontinence was held 5-8 July 2008 in Paris and
A review of the 4 th INTERNATIONAL CONSULTATION ON INCONTINENCE 5-8 July, 2008, Palais des Congrès, Paris, France The 4 th International Consultation on Incontinence was held 5-8 July 2008 in Paris and
The Role of Immunoglobulin E in the Pathogenesis of Ketamine Related Cystitis and Ulcerative Interstitial Cystitis: An Immunohistochemical Study
 Pain Physician 2016; 19:E581-E587 ISSN 2150-1149 Prospective Evaluation The Role of Immunoglobulin E in the Pathogenesis of Ketamine Related Cystitis and Ulcerative Interstitial Cystitis: An Immunohistochemical
Pain Physician 2016; 19:E581-E587 ISSN 2150-1149 Prospective Evaluation The Role of Immunoglobulin E in the Pathogenesis of Ketamine Related Cystitis and Ulcerative Interstitial Cystitis: An Immunohistochemical
Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder
 European Urology European Urology 48 (2005) 110 115 Female UrologyöIncontinence Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder Martin
European Urology European Urology 48 (2005) 110 115 Female UrologyöIncontinence Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder Martin
Role of Physiotherapy in the Management of Persistent Pelvic Pain. Brigitte Fung Physiotherapist Kwong Wah Hospital
 Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Department of Acupuncture and Neurology, Guang anmen Hospital, China Academy of Chinese Medical Sciences, Beijing , China;
 Review Article Page 1 of 8 Assessment of methodological quality of systematic reviews of acupuncture for chronic prostatitis/chronic pelvic pain symptom: an overview of systematic review Zongshi Qin 1,
Review Article Page 1 of 8 Assessment of methodological quality of systematic reviews of acupuncture for chronic prostatitis/chronic pelvic pain symptom: an overview of systematic review Zongshi Qin 1,
Treatment of chronic prostatitis/chronic pelvic pain syndrome
 International Journal of Antimicrobial Agents 31S (2008) S112 S116 Treatment of chronic prostatitis/chronic pelvic pain syndrome J. Curtis Nickel Department of Urology, Queen s University, Kingston General
International Journal of Antimicrobial Agents 31S (2008) S112 S116 Treatment of chronic prostatitis/chronic pelvic pain syndrome J. Curtis Nickel Department of Urology, Queen s University, Kingston General
Female&sexual& dysfunction&and& Interstitial&cystitis& Urology Grand Rounds November 14, 2012 Momoe Hyakutake, Urogynecology Fellow.
 Female&sexual& dysfunction&and& Interstitial&cystitis& Urology Grand Rounds November 14, 2012 Momoe Hyakutake, Urogynecology Fellow Objectives& 1) Overview of female sexual dysfunction 2) Explore the relationship
Female&sexual& dysfunction&and& Interstitial&cystitis& Urology Grand Rounds November 14, 2012 Momoe Hyakutake, Urogynecology Fellow Objectives& 1) Overview of female sexual dysfunction 2) Explore the relationship
Since the 19th century, searches for the pathogenesis
 Interstitial Cystitis/Bladder Pain Syndrome and Nonbladder Syndromes: Facts and Hypotheses John W. Warren, Joop P. van de Merwe, and J. Curtis Nickel Commentary Since the 19th century, searches for the
Interstitial Cystitis/Bladder Pain Syndrome and Nonbladder Syndromes: Facts and Hypotheses John W. Warren, Joop P. van de Merwe, and J. Curtis Nickel Commentary Since the 19th century, searches for the
REVIEW OF THE 27TH ANNUAL CONGRESS OF THE EUROPEAN ASSOCIATION OF UROLOGY (EAU), HELD IN PARIS, FRANCE, FEBRUARY 2012
 REVIEW OF THE 27TH ANNUAL CONGRESS OF THE EUROPEAN ASSOCIATION OF UROLOGY (EAU), HELD IN PARIS, FRANCE, 24-28 FEBRUARY 2012 Reviewed by Jane Meijlink The EAU Annual Congress 2012 in Paris began with a
REVIEW OF THE 27TH ANNUAL CONGRESS OF THE EUROPEAN ASSOCIATION OF UROLOGY (EAU), HELD IN PARIS, FRANCE, 24-28 FEBRUARY 2012 Reviewed by Jane Meijlink The EAU Annual Congress 2012 in Paris began with a
Targeted Therapeutics for Inflammatory Disease. June 2018
 Targeted Therapeutics for Inflammatory Disease June 2018 1 Forward Looking Statements/ Safe Harbor This presentation and the accompanying oral commentary contain forward-looking statements that involve
Targeted Therapeutics for Inflammatory Disease June 2018 1 Forward Looking Statements/ Safe Harbor This presentation and the accompanying oral commentary contain forward-looking statements that involve
Interstitial and chronic cystitis. Have you heard about the 2-component protection for the bladder wall?
 Interstitial and chronic cystitis Have you heard about the 2-component protection for the bladder wall? What is special about Instillamed? 2-component protection for the bladder wall Instillamed is an
Interstitial and chronic cystitis Have you heard about the 2-component protection for the bladder wall? What is special about Instillamed? 2-component protection for the bladder wall Instillamed is an
Treatment effectiveness in interstitial cystitis/bladder pain syndrome: Do patient perceptions align with efficacy-based guidelines?
 original research Treatment ness in interstitial cystitis/bladder pain syndrome: Do patient perceptions align with efficacy-based guidelines? Avril Lusty, MD; Elizabeth Kavaler, MD; Kay Zakariasen; Victoria
original research Treatment ness in interstitial cystitis/bladder pain syndrome: Do patient perceptions align with efficacy-based guidelines? Avril Lusty, MD; Elizabeth Kavaler, MD; Kay Zakariasen; Victoria
Interstitial Cystitis - Painful Bladder Syndrome
 Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
3/20/10. Prevalence of OAB Men: 16.0% Women: 16.9% Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Dry. Population (millions) Wet
 1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
Urinary nerve growth factor levels could be a biomarker for overactive bladder symptom: a meta-analysis
 Urinary nerve growth factor levels could be a biomarker for overactive bladder symptom: a meta-analysis H.C. Qu, S. Yan, X.L. Zhang, X.W. Zhu, Y.L. Liu and P. Wang Department of Urological Surgery, The
Urinary nerve growth factor levels could be a biomarker for overactive bladder symptom: a meta-analysis H.C. Qu, S. Yan, X.L. Zhang, X.W. Zhu, Y.L. Liu and P. Wang Department of Urological Surgery, The
Chronic Prostatitis: Approaches for Best Management
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.2.69 Review Article Chronic Prostatitis: Approaches for Best Management Kyung Seop Lee, Jae Duck Choi Department of Urology, Dongguk University School
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.2.69 Review Article Chronic Prostatitis: Approaches for Best Management Kyung Seop Lee, Jae Duck Choi Department of Urology, Dongguk University School
CYSTISTAT. Hyaluronan Training
 CYSTISTAT Hyaluronan Training HISTORICAL ASPECTS In 1934, Karl Meyer and his assistant, John Palmer, described for the first time the process to isolate a new Glucosa- Amino-Glycan (GAG) from the cows
CYSTISTAT Hyaluronan Training HISTORICAL ASPECTS In 1934, Karl Meyer and his assistant, John Palmer, described for the first time the process to isolate a new Glucosa- Amino-Glycan (GAG) from the cows
GUIDELINES ON URINARY INCONTINENCE
 12 GUIDELINES ON URINARY INCONTINENCE (Text updated March 2005) J. Thüroff, (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck Introduction The condition
12 GUIDELINES ON URINARY INCONTINENCE (Text updated March 2005) J. Thüroff, (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck Introduction The condition
Prostatitis refers to several clinical syndromes, including
 Prostatitis Michel A. Pontari,* Geoffrey F. Joyce, Matthew Wise, Mary McNaughton-Collins and the Urologic Diseases in America Project From the Department of Urology, Temple University School of Medicine,
Prostatitis Michel A. Pontari,* Geoffrey F. Joyce, Matthew Wise, Mary McNaughton-Collins and the Urologic Diseases in America Project From the Department of Urology, Temple University School of Medicine,
Urinary Incontinence for the Primary Care Provider
 Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Interstitial Cystitis/ Bladder Pain Syndrome
 page 1 Interstitial Cystitis/ Bladder Pain Syndrome Q: What is interstitial cystitis/bladder pain syndrome (IC/BPS)? A: Interstitial cystitis (int-uhr-stishuhl siss-tyt-uhss) (IC), is a chronic pain condition
page 1 Interstitial Cystitis/ Bladder Pain Syndrome Q: What is interstitial cystitis/bladder pain syndrome (IC/BPS)? A: Interstitial cystitis (int-uhr-stishuhl siss-tyt-uhss) (IC), is a chronic pain condition
Compassionate and effective management
 IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
General introduction
 General introduction http://hdl.handle.net/1765/103217 General introduction General introduction 1 2 Erasmus Medical Center Rotterdam General introduction 3 Functional pelvic floor disorders Symptoms related
General introduction http://hdl.handle.net/1765/103217 General introduction General introduction 1 2 Erasmus Medical Center Rotterdam General introduction 3 Functional pelvic floor disorders Symptoms related
PRE-OPERATIVE URODYNAMIC
 PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
PRE-OPERATIVE URODYNAMIC STUDIES: IS THERE VALUE IN PREDICTING POST-OPERATIVE STRESS URINARY INCONTINENCE IN WOMEN UNDERGOING PROLAPSE SURGERY? Dr K Janse van Rensburg Dr JA van Rensburg INTRODUCTION POP
Targeted Therapeutics for Inflammatory Disease. June 2017
 Targeted Therapeutics for Inflammatory Disease June 2017 1 Forward Looking Statements/ Safe Harbor This presentation and the accompanying oral commentary contain forward-looking statements that involve
Targeted Therapeutics for Inflammatory Disease June 2017 1 Forward Looking Statements/ Safe Harbor This presentation and the accompanying oral commentary contain forward-looking statements that involve
Factors influencing the diagnosis and treatment of chronic prostatitis among urologists in China
 DOI: 10.1111/j.1745-7262.2008.00416.x. Clinical Experience. Factors influencing the diagnosis and treatment of chronic prostatitis among urologists in China Long-Fei Liu 1, Jin-Rui Yang 1, David A.Ginsberg
DOI: 10.1111/j.1745-7262.2008.00416.x. Clinical Experience. Factors influencing the diagnosis and treatment of chronic prostatitis among urologists in China Long-Fei Liu 1, Jin-Rui Yang 1, David A.Ginsberg
Acupuncture versus Sham Acupuncture for Chronic Prostatitis/Chronic Pelvic Pain
 BRIEF OBSERVATION Acupuncture versus Sham Acupuncture for Chronic Prostatitis/Chronic Pelvic Pain Shaun Wen Huey Lee, MPharm, a Men Long Liong, MD, b Kah Hay Yuen, PhD, a Wing Seng Leong, MD, b Christopher
BRIEF OBSERVATION Acupuncture versus Sham Acupuncture for Chronic Prostatitis/Chronic Pelvic Pain Shaun Wen Huey Lee, MPharm, a Men Long Liong, MD, b Kah Hay Yuen, PhD, a Wing Seng Leong, MD, b Christopher
Urinary Nerve Growth Factor Could Be a Biomarker for Interstitial Cystitis/Painful Bladder Syndrome: A Meta-Analysis
 Urinary Nerve Growth Factor Could Be a Biomarker for Interstitial Cystitis/Painful Bladder Syndrome: A Meta-Analysis Hong-Chen Qu 1, Wei Zhang 2, Shi Yan 3, Yi-Li Liu 1, Ping Wang 1 * 1 Department of Urological
Urinary Nerve Growth Factor Could Be a Biomarker for Interstitial Cystitis/Painful Bladder Syndrome: A Meta-Analysis Hong-Chen Qu 1, Wei Zhang 2, Shi Yan 3, Yi-Li Liu 1, Ping Wang 1 * 1 Department of Urological
A Review on Interstitial Cystitis Syndrome (ICS)
 31 Review Article A Review on Interstitial Cystitis Syndrome (ICS) M Sushma*, TVV Vidyadhar, R Mohanraj, M Babu Department of Pharmacy Practice, Raghavendra Institute of Pharmaceutical Education & Research
31 Review Article A Review on Interstitial Cystitis Syndrome (ICS) M Sushma*, TVV Vidyadhar, R Mohanraj, M Babu Department of Pharmacy Practice, Raghavendra Institute of Pharmaceutical Education & Research
03/13/18. A. Symptoms lasting for greater than or equal to 12 months that have resulted to significant impairment in activities of daily living; and
 Reference #: MC/I008 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
Reference #: MC/I008 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
Interstitial Cystitis: Definitions and Confusable Diseases
 Interstitial Cystitis: Definitions and Confusable Diseases ESSIC Meeting 2005 Baden Joop P van de Merwe and Jørgen Nordling This report is the summary of the consensus obtained on definitions and confusable
Interstitial Cystitis: Definitions and Confusable Diseases ESSIC Meeting 2005 Baden Joop P van de Merwe and Jørgen Nordling This report is the summary of the consensus obtained on definitions and confusable
BJUI. Mini Reviews. Urological Oncology. Lower Urinary Tract. Sexual Medicine. Laparoscopic and Robotic Urology. Reconstructive and Paediatric Urology
 BJUI BJU INTERNATIONAL Mini Reviews Urological Oncology Sexual Medicine Lower Urinary Tract Laparoscopic and Robotic Urology Reconstructive and Paediatric Urology Investigative Urology 8 The Authors Original
BJUI BJU INTERNATIONAL Mini Reviews Urological Oncology Sexual Medicine Lower Urinary Tract Laparoscopic and Robotic Urology Reconstructive and Paediatric Urology Investigative Urology 8 The Authors Original
Daofang Zhu, Xianming Dou, Liang Tang, Dongdong Tang, Guiyi Liao, Weihua Fang, and Xiansheng Zhang
 Hindawi BioMed Research International Volume 2017, Article ID 3473796, 5 pages https://doi.org/10.1155/2017/3473796 Clinical Study Prevalence of Prostatitis-Like Symptoms and Outcomes of NIH-CPSI in Outpatients
Hindawi BioMed Research International Volume 2017, Article ID 3473796, 5 pages https://doi.org/10.1155/2017/3473796 Clinical Study Prevalence of Prostatitis-Like Symptoms and Outcomes of NIH-CPSI in Outpatients
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH
 TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH CONTENTS Overactive bladder (OAB) Treatment of OAB Beta-3 adrenoceptor agonist (Betmiga ) - Panacea? LASER treatment - a flash in the pan or the
TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH CONTENTS Overactive bladder (OAB) Treatment of OAB Beta-3 adrenoceptor agonist (Betmiga ) - Panacea? LASER treatment - a flash in the pan or the
Long-term efficacy and tolerability of pentosan polysulphate sodium in the treatment of bladder pain syndrome
 Original research Long-term efficacy and tolerability of pentosan polysulphate sodium in the treatment of bladder pain syndrome Ali A. Al-Zahrani, MD; Jerzy B. Gajewski, MD, FRCSC See related article on
Original research Long-term efficacy and tolerability of pentosan polysulphate sodium in the treatment of bladder pain syndrome Ali A. Al-Zahrani, MD; Jerzy B. Gajewski, MD, FRCSC See related article on
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging
 Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Program and Abstracts
 Program and Abstracts summary INTERNATIONAL SOCIETY FOR THE STUDY OF BPS ESSIC Annual Meeting Philadelphia (USA) 13-15 June 2014 Venue Geary Hall Hahnemann Hospital, Drexel University 230 North Broad Street
Program and Abstracts summary INTERNATIONAL SOCIETY FOR THE STUDY OF BPS ESSIC Annual Meeting Philadelphia (USA) 13-15 June 2014 Venue Geary Hall Hahnemann Hospital, Drexel University 230 North Broad Street
INJ. Tamsulosin Monotherapy versus Combination Therapy with Antibiotics or Anti-Inflammatory Agents in the Treatment of Chronic Pelvic Pain Syndrome
 Original Article Int Neurourol J 2011;15:92-96 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Tamsulosin Monotherapy versus Combination Therapy with Antibiotics or Anti-Inflammatory
Original Article Int Neurourol J 2011;15:92-96 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Tamsulosin Monotherapy versus Combination Therapy with Antibiotics or Anti-Inflammatory
The impact of overactive bladder on quality of life in south of China
 The impact of overactive bladder on quality of life in south of China Dong Chen, Yining Li * Department of Urology, Second Affiliated Hospital of Fujian Medical University, Quanzhou, 362000, China. * Corresponding
The impact of overactive bladder on quality of life in south of China Dong Chen, Yining Li * Department of Urology, Second Affiliated Hospital of Fujian Medical University, Quanzhou, 362000, China. * Corresponding
Interstitial Cystitis/ Bladder Pain Syndrome
 1 INTERNATIONAL PAINFUL BLADDER FOUNDATION Interstitial Cystitis/ Bladder Pain Syndrome Interstitial Cystitis, Bladder Pain Syndrome, Hypersensitive Bladder, Hunner Lesion Chronic Pelvic Pain, Associated
1 INTERNATIONAL PAINFUL BLADDER FOUNDATION Interstitial Cystitis/ Bladder Pain Syndrome Interstitial Cystitis, Bladder Pain Syndrome, Hypersensitive Bladder, Hunner Lesion Chronic Pelvic Pain, Associated
BJUI. Validity and reliability of the patient s perception of intensity of urgency scale in overactive bladder
 ; 2010 Lower Urinary Tract PATIENT S PERCEPTION OF INTENSITY OF URGENCY SCALE IN OAB CARTWRIGHT ET AL. BJUI Validity and reliability of the patient s perception of intensity of urgency scale in overactive
; 2010 Lower Urinary Tract PATIENT S PERCEPTION OF INTENSITY OF URGENCY SCALE IN OAB CARTWRIGHT ET AL. BJUI Validity and reliability of the patient s perception of intensity of urgency scale in overactive
