Addendum 1: International Consultation
|
|
|
- Philippa Stevens
- 5 years ago
- Views:
Transcription
1 Reprinted with Permission of the International Consultation on Urological Diseases and the International Continence Society Hanno PM, Cervigni M, Dinis P, Lin A, Nickel JC, Nordling J, van Ophoven A, Ueda T. Bladder pain syndrome. In: Abrams P, Cardozo L, Wagg A, Wein A, editors. Incontinence. 6th ed. London: ICS and ICUD; Chapter 19, ISBN: Definition Bladder Pain Syndrome (in the absence of a universally agreed definition, the International Society for the Study of Bladder Pain Syndrome ESSIC definition is given [1]. ESSIC: Chronic pelvic pain, pressure or discomfort of greater than 6 months duration perceived to be related to the urinary bladder accompanied by at least one other urinary symptom like persistent urge to void or urinary frequency. Confusable diseases as the cause of the symptoms must be excluded. There is no published data as to what duration of symptomatology indicates that early spontaneous resolution of symptoms is unlikely. While ESSIC arbitrarily uses a 6 month duration, the American Urological Association Guideline suggests 6 weeks is long enough to initiate diagnosis and treatment of BPS [2]. Without further data, the Consultation cannot make a recommendation and believes that it is up to the discretion of the physician and patient as to the proper interval between symptom onset and evaluation and diagnosis of a chronic condition Bladder Pain Syndrome (BPS) Nomenclature The scientific committee of the International Consultation voted to use the term bladder pain syndrome for the disorder that has been commonly referred to as interstitial cystitis (IC). The term painful bladder syndrome was dropped from the lexicon. The term IC implies an inflammation within the wall of the urinary bladder, involving gaps or spaces in the bladder tissue. This does not accurately describe the majority of patients with this syndrome. Painful Bladder Syndrome, as defined by the International Continence Society, is too restrictive for the clinical syndrome. Properly defined, the term Bladder Pain Syndrome appears to fit in well with the taxonomy of the International Association for the Study of Pain (IASP) (see below), and focuses on the actual symptom complex rather than what appears to be long-held misconception of the underlying pathology Bladder Pain Syndrome (XXIII-2) (per IASP) Bladder pain syndrome is the occurrence of persistent or recurrent pain perceived in the urinary bladder region, accompanied by at least one other symptom, such as pain worsening with bladder filling and day-time and/or night-time urinary frequency. There is no proven infection or other obvious local pathology. Bladder pain syndrome is often associated with negative cognitive, behavioral, sexual, or emotional consequences as Springer International Publishing AG 2018 P.M. Hanno et al. (eds.), Bladder Pain Syndrome An Evolution, 167
2 168 Chronic pelvic pain New concept Pelvic pain syndrome Bladder pain syndrome Interstital cystitis as a distinct disease; circa 1915 and Hunner description Hunner lesion diagnostic of interstitial cystitis Fig. A1 Conceptualization of bladder pain syndrome vis a vis interstitial cystitis well as with symptoms suggestive of lower urinary tract and sexual dysfunction. The Consultation believes that based on the pathology and endoscopic findings characteristic of the Hunner lesion, the epidemiologic pattern that distinguishes it from bladder pain syndrome, the clinical response to local treatment of the lesion by resection, fulguration, or steroid injection, the response to cyclosporine, and the absence of reports in the literature that non-hunner patients go on to develop Hunner lesions (i.e., the finding of Hunner lesion does not represent a continuum in the natural history of bladder pain syndrome), the presence of a Hunner lesion should be considered a distinct disease. It therefore should drop out of the bladder pain syndrome construct, much like we do not consider other painful conditions like radiation cystitis, ketamine cystitis, or urinary tract infection a part of bladder pain syndrome. The Consultation concludes that it would be reasonable to designate the Hunner lesion in symptomatic patients with the term interstitial cystitis, thus indicating a true interstitial inflammation. It would be defined much as Hunner defined it 100 years ago, and harmonize to a great extent the Asian, European, and North American concepts of interstitial cystitis. The Consultation will continue to refer to the symptom complex as bladder pain syndrome. Hunner lesion will be considered a distinct phenotype, but in the future may be classified as a separate disorder entirely, albeit with local symptoms that are difficult to differentiate from bladder pain syndrome in the absence of endoscopy. In other words, we may be coming full circle in the historical perspective (Fig. A1) History/Initial Assessment Males or females whose symptoms meet the requirements of the definition of bladder pain syndrome should be evaluated. The presence of commonly associated disorders including irritable bowel syndrome, chronic fatigue syndrome, and fibromyalgia in the presence of the cardinal symptoms of bladder pain syndrome also suggests the diagnosis. Abnormal gynecologic findings in women and well-characterized confusable diseases that may explain the symptoms must be ruled out. The initial assessment consists of a frequency/ volume chart, focused physical examination, urinalysis, and urine culture. In the absence of confusable disorders (uncomplicated disease), a
3 diagnosis can be made and treatment instituted. Urine cytology, cystoscopy, and urodynamic evaluation are recommended if clinically indicated and/or the diagnosis is in doubt (complicated disease). Patients with urinary infection should be treated and reassessed. Those with recurrent urinary infection, abnormal urinary cytology, and microscopic or gross hematuria are evaluated with appropriate imaging and endoscopic procedures, and only if findings are unable to explain the symptoms, are they diagnosed with BPS. Grade of recommendation: C Initial Treatment Patient education, dietary manipulation, nonprescription analgesics, stress reduction, pelvic floor relaxation techniques comprise the initial treatment of BPS. In the patient with findings suggesting pelvic floor dysfunction, pelvic floor physical therapy with myofascial trigger point release and intravaginal Thiele massage is often an effective therapeutic intervention. The treatment of pain needs to be addressed directly, and in some instances referral to an anesthesia/pain center can be an appropriate early step in conjunction with ongoing treatment of the syndrome. When conservative therapy fails or symptoms are severe and conservative management is unlikely to succeed, oral medication or intravesical treatment can be prescribed. It is recommended to initiate a single form of therapy and observe results, adding other modalities or substituting other modalities as indicated by degree of response or lack of response to treatment. Grade of recommendation: C Secondary Assessment If initial oral or intravesical therapy fails, or before beginning such therapy based on clinician judgment, it is reasonable to consider further evaluation which can include Urodynamics, pelvic imaging, and cystoscopy with bladder 169 distention and possible bladder biopsy under anesthesia. Findings of bladder overactivity suggest a trial of antimuscarinic therapy. The presence of a Hunner lesion suggests therapy with transurethral resection, fulguration of the lesion, or direct steroid injection into the lesion. Distention itself can have therapeutic benefit in 30 50% of patients, though benefits rarely persist for longer than a few months. Grade of recommendation: C Refractory BPS Those patients with persistent, unacceptable symptoms despite oral and/or intravesical therapy are candidates for more aggressive modalities. Many of these/ are best administered within the context of a clinical trial if possible. These may include neuromodulation, intradetrusor botulinum toxin, oral cyclosporine A, or clinical trials of newly described pharmacologic management techniques. At this point, most patients will benefit from the expertise of an anesthesia pain clinic. The last step in treatment is usually some type of surgical intervention aimed at increasing the functional capacity of the bladder or diverting the urinary stream. Urinary diversion with or without cystectomy has been used as a last resort with good results in selected patients. Cystectomy and urethrectomy do not appear to add any additional efficacy to diversion alone [3 5]. Augmentation or substitution cystoplasty seems less effective and more prone to recurrence of chronic pain in small reported series. Grade of recommendation: C Pain management is a primary consideration at every step of algorithm Patient enrollment in appropriate research trial is reasonable option at any point Evidence supporting neurostimulation, cyclosporine A, and botulinum toxin for BPS indication remains limited. These interventions are appropriate only for practitioners with experience treating BPS and willing to provide long-term care post-intervention.
4 170 SYMPTOMS Pain pressure or discomfort perceived to be related to the bladder with at least one other urinary symptom (e.g. frequency, nocturia) BLADDER PAIN SYNDROME Complicated BPS: Incontinence Urinary infection Haematuria Gynaecologic signs/symptoms BASIC ASSESSMENT History Bladder diary or frequency/volume chart Focused physical examination Urinalysis, culture URINARY INFECTION Consider: Urine cytology Further imaging Endoscopy Urodynamics Laparoscopy Test and reassess 1 ST LINE RX Uncomplicated BPS Conservative Therapy Stress reduction (B) Patient education (B) Dietary manipulation (B) Nonprescription analgesics Pelvic floor relaxation Pelvic floor physical therapy (A) Consult if associated disease Normal Abnormal TREAT AS INDICATED BPS REQUIRING MORE ACTIVE INTERVENTION 2 ND LINE (no hiearachy implied) Consider oral and or intravesical therapies; (B) Consider physical therapy; (A) Consider cystoscopy with hydrodistention under anaesthesia and treatment of any Hunner lesion (B) 3 RD LINE Consider, if not done previously: Cystoscopy under anaesthesia with bladder hydrodistension fulguration, resection or steroid injection of Hunner lesion (B) 4 TH LINE (no hiearachy implied) Sacral Nerve stimulation (B) Intra-detrusor botulinum toxin (B) Cyclosporine A (C) Consider new treatment trials 4 TH LINE Consider: Diversion with or without cystectomy (C) Substitution cystoplasty Improved with acceptable quality of life: Follow and support Note: The only FDA approved therapies are DMSO and pentosan polysulfate. Consider CONTINENCE PRODUCTS for temporary support during treatment. Pain management is a primary consideration at every step of the algorithm Patient enrollment in appropriate research trial is a reasonable option at any point Evidence supporting SNS, cyclosporine A, and botulinum toxin for BPS remains limited. These interventions are appropriate only for pracitioners with experience in treating BPS and who are willing to provide long-term care post-intervention Algorithm for diagnosis and treatment: 2016 International consultation on incontinence
5 171 Bibliography 1. van de Merwe JP, Nordling J, Bouchelouche P, Bouchelouche K, Cervigni M, Daha LK, et al. Diagnostic criteria, classification, and nomenclature for painful bladder syndrome/ interstitial cystitis: an ESSIC proposal. Eur Urol. 2008;53(1): Hanno PM, Erickson D, Moldwin R, Faraday MM. Diagnosis and treatment of interstitial cystitis/bladder pain syndrome: AUA guideline amendment. J Urol. 2015;193(5): Andersen AV, Granlund P, Schultz A, Talseth T, Hedlund H, Frich L. Long-term experience with surgical treatment of selected patients with bladder pain syndrome/interstitial cystitis. Scand J Urol Nephrol. 2012; 46(4): Norus T, Fode M, Nordling J. Ileal conduit without cystectomy may be an appropriate option in the treatment of intractable bladder pain syndrome/interstitial cystitis. Scand J Urol. 2014;48(2): Yang TX, Luo DY, Li H, Wang KJ, Shen H. Is urethrectomy necessary during cystectomy in patients with interstitial cystitis/bladder pain syndrome? Urology. 2016;97:73 9.
6 Addendum 2: AUA Guideline IC/BPS An unpleasant sensation (pain, pressure, discomfort) perceived to be related to the urinary bladder, associated with lower urinary tract symptoms of more than six weeks duration, in the absence of infection or other identifiable causes RESEARCH TRIALS BASIC ASSESSMENT History Frequency/Volume Chart Urinalysis, culture Cytology if smoking hx Confirmed/Uncomplicated IC/BPS FIRST-LINE S General Relaxation/ Stress Management Patient enrollment as appropriate at any point in treatment process Post-void residual Symptom questionnaire Patient Education Physical examination Pain evaluation Self-care/Behavioral Modification Signs/Symptoms of Complicated IC/BPS Incontinence/OAB GI signs/symptoms Microscopic/gross hematuria/sterile pyuria Gynecologic signs/symptoms CONSIDER: Urine cytology Imaging Cystoscopy Urodynamics Laparoscopy Specialist referral (urologic or non-urologic as appropriate) Dx Urinary Tract Infection TREAT & ASSESS CLINICAL MANAGEMENT PRINCIPLES Treatments are ordered from most to least conservative; surgical treatment is appropriate only after other treatment options have been found to be ineffective (except for treatment of Hunner s lesions if detected) Initial treatment level depends on symptom severity, clinician judgment, and patient preferences Multiple, simultaneous treatments may be considered if in best interests of patient Ineffective treatments should be stopped Pain management should be considered throughout course of therapy with goal of maximizing function and minimizing pain and side effects Diagnosis should be reconsidered if no improvement within clinically-meaningful time-frame SECOND-LINE S Appropriate manual physical therapy techniques Oral: amitriptyline, cimetidine, hydroxyzine, PPS Intravesical: DMSO, Heparin, Lidocaine THIRD-LINE S Cystoscopy under anesthesia w/ hydrodistention Tx of Hunner s lesions if found FOURTH-LINE S Intradetrusor botulinum toxin A Neuromodulation FIFTH-LINE S Cyclosporine A The evidence supporting the use of Neuromodulation, Cyclosporine A, and BTX for IC/BPS is limited by many factors including study quality, small sample sizes, and lack of durable follow up. None of these therapies have been approved by the U.S. Food and Drug Administration for this indication. The panel believes that none of these interventions can be recommended for generalized use for this disorder, but rather should be limited to practitioners with experience managing this syndrome and willingness to provide long term care of these patients post intervention. SIXTH-LINE S Diversion w/ or w/out cystectomy Substitution cystoplasty Note: For patients with end-stage structurally small bladders, diversion is indicated at any time clinician and patient believe appropriate. Guideline of the American Urological Association. Hanno PM, Erickson D, Moldwin R, Faraday MM: Diagnosis and treatment of interstitial cystitis/bladder pain syndrome: AUA guideline amendment. J. Urol. 193: , 2015 Springer International Publishing AG 2018 P.M. Hanno et al. (eds.), Bladder Pain Syndrome An Evolution, 173
7 Addendum 3: Asian Algorithm Asian conception of bladder pain syndrome from Homma. Homma Y, Ueda T, Tomoe H, Lin A, Kuo HC, Lee MH, Oh SJ, Kim JC, and Lee KS: Clinical guidelines for interstitial cystitis and hypersensitive bladder updated in International Journal of Urology. 23: , 2016 Springer International Publishing AG 2018 P.M. Hanno et al. (eds.), Bladder Pain Syndrome An Evolution, 175
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective?
 Original Article In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective? Hikaru Tomoe Department of Urology and Pelvic Reconstructive Surgery, Tokyo
Original Article In what type of interstitial cystitis/bladder pain syndrome is DMSO intravesical instillation therapy effective? Hikaru Tomoe Department of Urology and Pelvic Reconstructive Surgery, Tokyo
Bladder pain syndrome / Interstitial cystitis
 Bladder pain syndrome / Interstitial cystitis Terminology The term bladder pain syndrome/interstitial cystitis (BPS/IC) is defined as the presence of chronic pain, pressure, or pelvic discomfort lasting
Bladder pain syndrome / Interstitial cystitis Terminology The term bladder pain syndrome/interstitial cystitis (BPS/IC) is defined as the presence of chronic pain, pressure, or pelvic discomfort lasting
5-8 July, 2008, Palais des Congrès, Paris, France
 A review of the 4 th INTERNATIONAL CONSULTATION ON INCONTINENCE 5-8 July, 2008, Palais des Congrès, Paris, France The 4 th International Consultation on Incontinence was held 5-8 July 2008 in Paris and
A review of the 4 th INTERNATIONAL CONSULTATION ON INCONTINENCE 5-8 July, 2008, Palais des Congrès, Paris, France The 4 th International Consultation on Incontinence was held 5-8 July 2008 in Paris and
Interstitial Cystitis:
 Diagnosis and Definition ESSIC approach Jørgen Nordling, chairman ESSIC Professor of Urology University of Copenhagen Denmark Interstitial Cystitis: A painful, potentially disabling, inflammatory disease
Diagnosis and Definition ESSIC approach Jørgen Nordling, chairman ESSIC Professor of Urology University of Copenhagen Denmark Interstitial Cystitis: A painful, potentially disabling, inflammatory disease
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline.
 Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Treatment effectiveness in interstitial cystitis/bladder pain syndrome: Do patient perceptions align with efficacy-based guidelines?
 original research Treatment ness in interstitial cystitis/bladder pain syndrome: Do patient perceptions align with efficacy-based guidelines? Avril Lusty, MD; Elizabeth Kavaler, MD; Kay Zakariasen; Victoria
original research Treatment ness in interstitial cystitis/bladder pain syndrome: Do patient perceptions align with efficacy-based guidelines? Avril Lusty, MD; Elizabeth Kavaler, MD; Kay Zakariasen; Victoria
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
1 of 8 3/2/15 9:22 PM
 Close window Guideline Title Diagnosis and treatment of interstitial cystitis/bladder pain syndrome. Bibliographic Source(s) Hanno PM, Burks DA, Clemens JQ, Dmochowski RR, Erickson D, FitzGerald MP, Forrest
Close window Guideline Title Diagnosis and treatment of interstitial cystitis/bladder pain syndrome. Bibliographic Source(s) Hanno PM, Burks DA, Clemens JQ, Dmochowski RR, Erickson D, FitzGerald MP, Forrest
TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH
 TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH CONTENTS Overactive bladder (OAB) Treatment of OAB Beta-3 adrenoceptor agonist (Betmiga ) - Panacea? LASER treatment - a flash in the pan or the
TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH CONTENTS Overactive bladder (OAB) Treatment of OAB Beta-3 adrenoceptor agonist (Betmiga ) - Panacea? LASER treatment - a flash in the pan or the
Effect of Transurethral Resection With Hydrodistention for the Treatment of Ulcerative Interstitial Cystitis
 www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.10.682 Voiding Dysfunction/Female Urology Effect of Transurethral Resection With Hydrodistention for the Treatment of Ulcerative Interstitial Cystitis
www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.10.682 Voiding Dysfunction/Female Urology Effect of Transurethral Resection With Hydrodistention for the Treatment of Ulcerative Interstitial Cystitis
INTRODUCTION. Original Article - Lower Urinary Tract Dysfunction. Aram Kim 1, Kyeong-Ok Hoe 2, Jung Hyun Shin 2, Myung-Soo Choo 2 1
 Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:353-358. pissn 2466-0493 eissn 2466-054X Evaluation of the incidence and risk factors associated with persistent frequency
Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:353-358. pissn 2466-0493 eissn 2466-054X Evaluation of the incidence and risk factors associated with persistent frequency
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
BPS/IC: evolution of definition and prevalence
 BPS/IC: evolution of definition and prevalence ame in history Tic doloureux of the bladder 1836 Interstitial cystitis 1878 Cystitis parenchymatosa 197 unner s ulcer 1915 Panmural ulcerative cystitis 192
BPS/IC: evolution of definition and prevalence ame in history Tic doloureux of the bladder 1836 Interstitial cystitis 1878 Cystitis parenchymatosa 197 unner s ulcer 1915 Panmural ulcerative cystitis 192
DELAYED DIAGNOSIS. Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >60%
 DELAYED DIAGNOSIS Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >6% 1 PREVALENCE 1,, 9,, 8,, 7,, 6,, 5,, 4,, 3,, 2,, 1,, NHS "Prostatitis" "Endometriosis" The
DELAYED DIAGNOSIS Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >6% 1 PREVALENCE 1,, 9,, 8,, 7,, 6,, 5,, 4,, 3,, 2,, 1,, NHS "Prostatitis" "Endometriosis" The
Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive Bladder
 Advances in Urology Volume 2009, Article ID 328364, 4 pages doi:10.1155/2009/328364 Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive
Advances in Urology Volume 2009, Article ID 328364, 4 pages doi:10.1155/2009/328364 Clinical Study Predictors of Response to Intradetrusor Botulinum Toxin-A Injections in Patients with Idiopathic Overactive
Targeted Therapeutics for Inflammatory Disease. June 2017
 Targeted Therapeutics for Inflammatory Disease June 2017 1 Forward Looking Statements/ Safe Harbor This presentation and the accompanying oral commentary contain forward-looking statements that involve
Targeted Therapeutics for Inflammatory Disease June 2017 1 Forward Looking Statements/ Safe Harbor This presentation and the accompanying oral commentary contain forward-looking statements that involve
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Interstitial Cystitis - Painful Bladder Syndrome
 Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
ESSIC 2008 Annual Meeting Rome
 Bladder Pain Syndrome Developing a History Protocol Normal Bladder Function Depends on Suzy, Arul, Andrei, Arvind Integrity of the macroscopic and microscopic anatomy of the bladder Central nervous system
Bladder Pain Syndrome Developing a History Protocol Normal Bladder Function Depends on Suzy, Arul, Andrei, Arvind Integrity of the macroscopic and microscopic anatomy of the bladder Central nervous system
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Pelvic Floor Therapy for the Oncology Patient
 Therapy for the Oncology Patient CARINA SIRACUSA, PT, DPT, WCS OHIOHEALTH PELVIC FLOOR PHYSICAL THERAPIST ONCOLOGY REHABILITATION PROGRAM COORDINATOR What does a pelvic floor therapist treat? Muscles Muscles
Therapy for the Oncology Patient CARINA SIRACUSA, PT, DPT, WCS OHIOHEALTH PELVIC FLOOR PHYSICAL THERAPIST ONCOLOGY REHABILITATION PROGRAM COORDINATOR What does a pelvic floor therapist treat? Muscles Muscles
Interstitial cystitis
 Interstitial cystitis Ilse Truter, PharmITCom Consulting Bladder Normal protective bladder lining Thinning of the protective bladder lining Pinpoint bleeding (glomerulations) on the bladder wall Hunner
Interstitial cystitis Ilse Truter, PharmITCom Consulting Bladder Normal protective bladder lining Thinning of the protective bladder lining Pinpoint bleeding (glomerulations) on the bladder wall Hunner
Functional Bladder Problems
 european urology supplements 6 (2007) 710 716 available at www.sciencedirect.com journal homepage: www.europeanurology.com Functional Bladder Problems Emmanuel Chartier-Kastler * Department of Urology,
european urology supplements 6 (2007) 710 716 available at www.sciencedirect.com journal homepage: www.europeanurology.com Functional Bladder Problems Emmanuel Chartier-Kastler * Department of Urology,
Hypersensitive bladder: A solution to confused terminology and ignorance concerning interstitial cystitis
 bs_bs_banner International Journal of Urology (2014) 21 (Suppl 1), 43 47 doi: 10.1111/iju.12314 Review Article Hypersensitive bladder: A solution to confused terminology and ignorance concerning interstitial
bs_bs_banner International Journal of Urology (2014) 21 (Suppl 1), 43 47 doi: 10.1111/iju.12314 Review Article Hypersensitive bladder: A solution to confused terminology and ignorance concerning interstitial
Interstitial Cystitis
 Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Overactive Bladder in Clinical Practice
 Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
Chronic Prostatitis/Chronic Pelvic Pain Syndrome and Male Bladder Pain Syndrome/Interstitial Cystitis: How Are They Related?
 Review ISSN 2465-8243(Print) / ISSN: 2465-8510(Online) https://doi.org/10.14777/uti.2017.12.1.15 Urogenit Tract Infect 2017;12(1):15-21 http://crossmark.crossref.org/dialog/?doi=10.14777/uti.2017.12.1.&domain=pdf&date_stamp=2017-04-25
Review ISSN 2465-8243(Print) / ISSN: 2465-8510(Online) https://doi.org/10.14777/uti.2017.12.1.15 Urogenit Tract Infect 2017;12(1):15-21 http://crossmark.crossref.org/dialog/?doi=10.14777/uti.2017.12.1.&domain=pdf&date_stamp=2017-04-25
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Chronic pelvic pain-when surgery fails
 Chronic pelvic pain-when surgery fails Sherif Tawfeek FRANZCOG, FRCOG, FICS, MSc, Dip-Endoscopy Consultant in Obstetrics and Gynaecology Senior lecturer at University of Otago Objectives Identify the common
Chronic pelvic pain-when surgery fails Sherif Tawfeek FRANZCOG, FRCOG, FICS, MSc, Dip-Endoscopy Consultant in Obstetrics and Gynaecology Senior lecturer at University of Otago Objectives Identify the common
Role of cystoscopy and hydrodistention in the diagnosis of interstitial cystitis/bladder pain syndrome
 Review Article Role of cystoscopy and hydrodistention in the diagnosis of interstitial cystitis/bladder pain syndrome Gisela Ens, Gustavo L. Garrido Voiding Dysfunction and Urodynamic Section, Division
Review Article Role of cystoscopy and hydrodistention in the diagnosis of interstitial cystitis/bladder pain syndrome Gisela Ens, Gustavo L. Garrido Voiding Dysfunction and Urodynamic Section, Division
Painful Bladder Syndrome
 Painful Bladder Syndrome Department of Urology Patient Information What What is Painful is Painful Bladder Bladder Syndrome? Syndrome? Painful bladder syndrome also known as Interstitial Cystitis is a
Painful Bladder Syndrome Department of Urology Patient Information What What is Painful is Painful Bladder Bladder Syndrome? Syndrome? Painful bladder syndrome also known as Interstitial Cystitis is a
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Management of Bladder Pain Syndrome
 Management of ladder Pain Syndrome Green-top Guideline No. 70 RCOG/SUG Joint Guideline ecember 2016 Please cite this paper as: Tirlapur SA, irch JV, Carberry CL, Khan KS, Latthe PM, Jha S, Ward KL, Irving
Management of ladder Pain Syndrome Green-top Guideline No. 70 RCOG/SUG Joint Guideline ecember 2016 Please cite this paper as: Tirlapur SA, irch JV, Carberry CL, Khan KS, Latthe PM, Jha S, Ward KL, Irving
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Interstitial Cystitis. Dr. Gerard Testa
 Interstitial Cystitis Dr. Gerard Testa Auto Immune Disease Infection Glycosaminoglycan layer deficiency Reflex Sympathetic Dystrophy? Hereditary Classification of Interstitial Cystitis Ulcerative Non Ulcerative
Interstitial Cystitis Dr. Gerard Testa Auto Immune Disease Infection Glycosaminoglycan layer deficiency Reflex Sympathetic Dystrophy? Hereditary Classification of Interstitial Cystitis Ulcerative Non Ulcerative
Interstitial Cystitis/ Bladder Pain Syndrome
 page 1 Interstitial Cystitis/ Bladder Pain Syndrome Q: What is interstitial cystitis/bladder pain syndrome (IC/BPS)? A: Interstitial cystitis (int-uhr-stishuhl siss-tyt-uhss) (IC), is a chronic pain condition
page 1 Interstitial Cystitis/ Bladder Pain Syndrome Q: What is interstitial cystitis/bladder pain syndrome (IC/BPS)? A: Interstitial cystitis (int-uhr-stishuhl siss-tyt-uhss) (IC), is a chronic pain condition
INTERSTITIAL CYSTITIS (IC) MANAGEMENT
 INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Interstitial Cystitis (IC)/Painful Bladder Syndrome(PBS)
 Interstitial Cystitis (IC)/Painful Bladder Syndrome(PBS) Ene G. George M.D., FACOG, FPMRS Kaiser Permanente Baldwin Park Division of Urogynecology Department of Obstetrics and Gynecology PBS/IC I have
Interstitial Cystitis (IC)/Painful Bladder Syndrome(PBS) Ene G. George M.D., FACOG, FPMRS Kaiser Permanente Baldwin Park Division of Urogynecology Department of Obstetrics and Gynecology PBS/IC I have
Role of Physiotherapy in the Management of Persistent Pelvic Pain. Brigitte Fung Physiotherapist Kwong Wah Hospital
 Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Effect of Low-Dose Amitriptyline Treatment for Interstitial Cystitis/Bladder Pain Syndrome
 ORIGINAL ARTICLE Effect of Low-Dose Amitriptyline Treatment for Interstitial Cystitis/Bladder Pain Syndrome Weiguo Chen 1, Donghua Xie 2, Guolu Liu 1, Yifan Chen 1, Zongqiang Cai 1 1 Department of Urology,
ORIGINAL ARTICLE Effect of Low-Dose Amitriptyline Treatment for Interstitial Cystitis/Bladder Pain Syndrome Weiguo Chen 1, Donghua Xie 2, Guolu Liu 1, Yifan Chen 1, Zongqiang Cai 1 1 Department of Urology,
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
REVIEW OF THE 27TH ANNUAL CONGRESS OF THE EUROPEAN ASSOCIATION OF UROLOGY (EAU), HELD IN PARIS, FRANCE, FEBRUARY 2012
 REVIEW OF THE 27TH ANNUAL CONGRESS OF THE EUROPEAN ASSOCIATION OF UROLOGY (EAU), HELD IN PARIS, FRANCE, 24-28 FEBRUARY 2012 Reviewed by Jane Meijlink The EAU Annual Congress 2012 in Paris began with a
REVIEW OF THE 27TH ANNUAL CONGRESS OF THE EUROPEAN ASSOCIATION OF UROLOGY (EAU), HELD IN PARIS, FRANCE, 24-28 FEBRUARY 2012 Reviewed by Jane Meijlink The EAU Annual Congress 2012 in Paris began with a
Is Urethral Pain Syndrome Really Part of Bladder Pain Syndrome?
 Review ISSN 2465-8243(Print) / ISSN: 2465-8510(Online) https://doi.org/10.14777/uti.2017.12.1.22 Urogenit Tract Infect 2017;12(1):22-27 http://crossmark.crossref.org/dialog/?doi=10.14777/uti.2017.12.1.&domain=pdf&date_stamp=2017-04-25
Review ISSN 2465-8243(Print) / ISSN: 2465-8510(Online) https://doi.org/10.14777/uti.2017.12.1.22 Urogenit Tract Infect 2017;12(1):22-27 http://crossmark.crossref.org/dialog/?doi=10.14777/uti.2017.12.1.&domain=pdf&date_stamp=2017-04-25
Diagnosis and Mangement of Nocturia in Adults
 Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Botulinum Toxin: Applications in Urology
 Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
Botulinum Toxin: Applications in Urology Dr. Lee Jonat, PGY-4 Department of Urologic Sciences University of British Columbia Outline Mechanism of Action Technical Considerations Adverse Events Neurogenic
Botulinum Toxin Injection for OAB: Indications & Technique
 Classification of LUTS Botulinum Toxin Injection for OAB: Indications & Technique Sherif Mourad, MD Professor of Urology, Ain Shams University General Secretary of International Continence President of
Classification of LUTS Botulinum Toxin Injection for OAB: Indications & Technique Sherif Mourad, MD Professor of Urology, Ain Shams University General Secretary of International Continence President of
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website:
 Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website: www.female-gynecologist.com What is Painful Bladder (PBS) or Interstitial Cystitis
Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website: www.female-gynecologist.com What is Painful Bladder (PBS) or Interstitial Cystitis
LUTS after TURP: How come and how to manage? Matthias Oelke
 LUTS after TURP: How come and how to manage? Matthias Oelke Department of Urology Global Congress on LUTD, Rome, 26 th June 2015 Disclosures Consultant, speaker, trial participant and/or research grants
LUTS after TURP: How come and how to manage? Matthias Oelke Department of Urology Global Congress on LUTD, Rome, 26 th June 2015 Disclosures Consultant, speaker, trial participant and/or research grants
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
INTERSTITIAL CYSTITIS (IC)
 INTERSTITIAL CYSTITIS (IC) Painful Bladder Syndrome (PBS): THE BASIC FACTS ANDREW L. SIEGEL, M.D. Board-Certified Urologist and Urological Surgeon Specialty: Male and Female Incontinence, Voiding Dysfunction,
INTERSTITIAL CYSTITIS (IC) Painful Bladder Syndrome (PBS): THE BASIC FACTS ANDREW L. SIEGEL, M.D. Board-Certified Urologist and Urological Surgeon Specialty: Male and Female Incontinence, Voiding Dysfunction,
Clinical guidelines for interstitial cystitis and hypersensitive bladder updated in 2015
 International Journal of Urology (2016) 23, 542--549 doi: 10.1111/iju.13118 Guideline Clinical guidelines for interstitial cystitis and hypersensitive bladder updated in 2015 Yukio Homma, 1 Tomohiro Ueda,
International Journal of Urology (2016) 23, 542--549 doi: 10.1111/iju.13118 Guideline Clinical guidelines for interstitial cystitis and hypersensitive bladder updated in 2015 Yukio Homma, 1 Tomohiro Ueda,
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain
 Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
University College Hospital at Westmoreland Street. Percutaneous Tibial Nerve Stimulation (PTNS)
 University College Hospital at Westmoreland Street Percutaneous Tibial Nerve Stimulation (PTNS) Urology Directorate If you need a large print, audio or translated copy of this document, please contact
University College Hospital at Westmoreland Street Percutaneous Tibial Nerve Stimulation (PTNS) Urology Directorate If you need a large print, audio or translated copy of this document, please contact
BLADDER HEALTH. Painful Bladder AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION
 BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
Bladder Pain Syndrome Current Concepts and Management Guidelines
 Review Article Bladder Pain Syndrome Current Concepts and Management Guidelines Amita Jain To cite: Jain A. Bladder Pain Syndrome Current Concepts and Management Guidelines. Pan Asian J Obs Gyn 2018;1(1):18-23.
Review Article Bladder Pain Syndrome Current Concepts and Management Guidelines Amita Jain To cite: Jain A. Bladder Pain Syndrome Current Concepts and Management Guidelines. Pan Asian J Obs Gyn 2018;1(1):18-23.
Interstitial and chronic cystitis. Have you heard about the 2-component protection for the bladder wall?
 Interstitial and chronic cystitis Have you heard about the 2-component protection for the bladder wall? What is special about Instillamed? 2-component protection for the bladder wall Instillamed is an
Interstitial and chronic cystitis Have you heard about the 2-component protection for the bladder wall? What is special about Instillamed? 2-component protection for the bladder wall Instillamed is an
Posterior Tibial Nerve Stimulation
 Posterior Tibial Nerve Stimulation Policy Number: Original Effective Date: MM.02.025 01/01/2015 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2015 Section: Medicine Place(s)
Posterior Tibial Nerve Stimulation Policy Number: Original Effective Date: MM.02.025 01/01/2015 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2015 Section: Medicine Place(s)
Clinical comparison of intravesical hyaluronic acid and chondroitin sulfate therapies in the treatment of bladder pain syndrome/interstitial cystitis
 Received: 17 December 2016 Accepted: 26 February 2017 DOI: 10.1002/nau.23284 ORIGINAL CLINICAL ARTICLE Clinical comparison of intravesical hyaluronic acid and chondroitin sulfate therapies in the treatment
Received: 17 December 2016 Accepted: 26 February 2017 DOI: 10.1002/nau.23284 ORIGINAL CLINICAL ARTICLE Clinical comparison of intravesical hyaluronic acid and chondroitin sulfate therapies in the treatment
GUIDELINES ON URINARY INCONTINENCE
 12 GUIDELINES ON URINARY INCONTINENCE (Text updated March 2005) J. Thüroff, (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck Introduction The condition
12 GUIDELINES ON URINARY INCONTINENCE (Text updated March 2005) J. Thüroff, (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck Introduction The condition
Telford and Wrekin Clinical Commissioning Group
 Telford and Wrekin Clinical Commissioning Group Agenda Item 9.2 CLINICAL COMMISSIONING GROUP GOVERNANCE BOARD EXECUTIVE SUMMARY DATE: 9 th April 2013 TITLE OF PAPER: Continence pathway and Referral letter
Telford and Wrekin Clinical Commissioning Group Agenda Item 9.2 CLINICAL COMMISSIONING GROUP GOVERNANCE BOARD EXECUTIVE SUMMARY DATE: 9 th April 2013 TITLE OF PAPER: Continence pathway and Referral letter
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
Multimodal Therapy for Painful Bladder Syndrome / Interstitial Cystitis: Pilot Study Combining Behavioral, Pharmacologic, and Endoscopic Therapies
 Neurourology Multimodal Therapy for Interstitial Cystitis: A Pilot Study International Braz J Urol Vol. 35 (4): 467-474, July - August, 2009 Multimodal Therapy for Painful Bladder Syndrome / Interstitial
Neurourology Multimodal Therapy for Interstitial Cystitis: A Pilot Study International Braz J Urol Vol. 35 (4): 467-474, July - August, 2009 Multimodal Therapy for Painful Bladder Syndrome / Interstitial
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information
 Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information Round Rock Jollyville Westlake Central office: Phone 512-231-1444 Fax 512-231-1470 www.urologyteam.com Rev June 2017 What is Interstitial
Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information Round Rock Jollyville Westlake Central office: Phone 512-231-1444 Fax 512-231-1470 www.urologyteam.com Rev June 2017 What is Interstitial
Overactive Bladder (OAB) and Quality of Life
 Overactive Bladder (OAB) and Quality of Life Dr. Byron Wong MBBS (Sydney), FRCSEd, FRCSEd (Urol), FCSHK, FHKAM (Surgery) Specialist in Urology Central Urology Clinic Hong Kong Continence Society Annual
Overactive Bladder (OAB) and Quality of Life Dr. Byron Wong MBBS (Sydney), FRCSEd, FRCSEd (Urol), FCSHK, FHKAM (Surgery) Specialist in Urology Central Urology Clinic Hong Kong Continence Society Annual
CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF FEMALE LOWER URINARY TRACT SYMPTOMS
 CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF FEMALE LOWER URINARY TRACT SYMPTOMS The minimum standards required to initiate specialised conservative
CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF FEMALE LOWER URINARY TRACT SYMPTOMS The minimum standards required to initiate specialised conservative
Policy for Prostatism/Lower Urinary Tract Symptoms in men
 NHS Halton Clinical Commissioning Group NHS Liverpool Clinical Commissioning Group NHS St Helens Clinical Commissioning Group NHS South Sefton Clinical Commissioning Group NHS Southport and Formby Clinical
NHS Halton Clinical Commissioning Group NHS Liverpool Clinical Commissioning Group NHS St Helens Clinical Commissioning Group NHS South Sefton Clinical Commissioning Group NHS Southport and Formby Clinical
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy
 Review Article Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy Mauro Cervigni Interstitial Cystitis Referral Center, Catholic University, Rome, Italy Correspondence
Review Article Interstitial cystitis/bladder pain syndrome and glycosaminoglycans replacement therapy Mauro Cervigni Interstitial Cystitis Referral Center, Catholic University, Rome, Italy Correspondence
Program and Abstracts
 Program and Abstracts summary INTERNATIONAL SOCIETY FOR THE STUDY OF BPS ESSIC Annual Meeting Philadelphia (USA) 13-15 June 2014 Venue Geary Hall Hahnemann Hospital, Drexel University 230 North Broad Street
Program and Abstracts summary INTERNATIONAL SOCIETY FOR THE STUDY OF BPS ESSIC Annual Meeting Philadelphia (USA) 13-15 June 2014 Venue Geary Hall Hahnemann Hospital, Drexel University 230 North Broad Street
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
Managing urinary morbidity after brachytherapy. Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester
 Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
Managing urinary morbidity after brachytherapy Kieran O Flynn Department of Urology, Salford Royal Foundation Trust, Manchester Themes Can we predict urinary morbidity? Prevention of urinary morbidity
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
GREAT MEETING FOR CHRONIC PELVIC PAIN AND PAINFUL BLADDER!
 REVIEW OF THE 42 nd ANNUAL SCIENTIFIC MEETING OF THE INTERNATIONAL CONTINENCE SOCIETY (ICS) 15-19 OCTOBER 2012, BEIJING, CHINA GREAT MEETING FOR CHRONIC PELVIC PAIN AND PAINFUL BLADDER! Jane Meijlink This
REVIEW OF THE 42 nd ANNUAL SCIENTIFIC MEETING OF THE INTERNATIONAL CONTINENCE SOCIETY (ICS) 15-19 OCTOBER 2012, BEIJING, CHINA GREAT MEETING FOR CHRONIC PELVIC PAIN AND PAINFUL BLADDER! Jane Meijlink This
Interstitial cystitis (IC), also
 Interstitial cystitis: Algorithm to simplify diagnosis of chronic urinary symptoms By Anita L. Booth, DNP, FNP-BC and Jill Harpst Rodgers, DNP, FNP-BC This pre/post-test study was undertaken to determine
Interstitial cystitis: Algorithm to simplify diagnosis of chronic urinary symptoms By Anita L. Booth, DNP, FNP-BC and Jill Harpst Rodgers, DNP, FNP-BC This pre/post-test study was undertaken to determine
Recommandations de prise en charge des vessies neurogènes EAU 2006
 Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Targeted Therapeutics for Inflammatory Disease. June 2018
 Targeted Therapeutics for Inflammatory Disease June 2018 1 Forward Looking Statements/ Safe Harbor This presentation and the accompanying oral commentary contain forward-looking statements that involve
Targeted Therapeutics for Inflammatory Disease June 2018 1 Forward Looking Statements/ Safe Harbor This presentation and the accompanying oral commentary contain forward-looking statements that involve
Geriatric Urinary Incontinence
 Geriatric Urinary Incontinence Neil M. Resnick, MD Thomas Detre Professor of Medicine Chief, Division of Geriatric Medicine University of Pittsburgh/UPMC UI: The Problem Prevalence in elderly 33% Morbidity
Geriatric Urinary Incontinence Neil M. Resnick, MD Thomas Detre Professor of Medicine Chief, Division of Geriatric Medicine University of Pittsburgh/UPMC UI: The Problem Prevalence in elderly 33% Morbidity
GUIDELINES ON URINARY INCONTINENCE
 GUIDELINES ON URINARY INCONTINENCE 9 J. Thüroff, (chairman), P. Abrams, J-T. Andersen, W. Artibani, E. Chartier-Kastler, C. Hampel, M. Hohenfellner, T. Tammela, Ph. van Kerrebroeck Introduction The condition
GUIDELINES ON URINARY INCONTINENCE 9 J. Thüroff, (chairman), P. Abrams, J-T. Andersen, W. Artibani, E. Chartier-Kastler, C. Hampel, M. Hohenfellner, T. Tammela, Ph. van Kerrebroeck Introduction The condition
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
Interstitial Cystitis
 J Obstet Gynecol India Vol. 58, No. 1 : January/February 2008 pg 24-31 Review Article Interstitial Cystitis Satpathy Hemant K, Taylor Richert Department of Obstetrics and Gynecology, CUMC, Omaha, NE, USA,
J Obstet Gynecol India Vol. 58, No. 1 : January/February 2008 pg 24-31 Review Article Interstitial Cystitis Satpathy Hemant K, Taylor Richert Department of Obstetrics and Gynecology, CUMC, Omaha, NE, USA,
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
32 OBG Management July 2010 Vol. 22 No. 7 obgmanagement.com
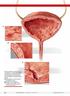 A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
Review of treatments for interstitial cystitis
 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Review of treatments for interstitial cystitis Lindsey Ann Miller The University of Toledo Follow this
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Review of treatments for interstitial cystitis Lindsey Ann Miller The University of Toledo Follow this
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
AUCKLAND REGIONAL UROLOGY GUIDELINES AND REFERRAL RECOMMENDATIONS
 AUCKLAND REGIONAL UROLOGY GUIDELINES AND REFERRAL RECOMMENDATIONS This document outlines the urological conditions currently funded at Auckland District Health Board (ADHB), Counties Manukau District Health
AUCKLAND REGIONAL UROLOGY GUIDELINES AND REFERRAL RECOMMENDATIONS This document outlines the urological conditions currently funded at Auckland District Health Board (ADHB), Counties Manukau District Health
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Investor & Analyst Event. February 9, 2018 David Main President & CEO
 Investor & Analyst Event February 9, 2018 David Main President & CEO Forward Looking Statements/ Safe Harbor This presentation and the accompanying oral commentary contain forward-looking statements that
Investor & Analyst Event February 9, 2018 David Main President & CEO Forward Looking Statements/ Safe Harbor This presentation and the accompanying oral commentary contain forward-looking statements that
Incontinence: The silent scourge of the young and old. The International Continence Society has. In this article:
 Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Interstitial Cystitis
 Clinical Communiqué Winter 2002 Interstitial Cystitis A Clinical Spectrum Jack Barkin, MD Chief of Urology, Humber River Regional Hospital, Toronto, Ontario Editorial Choosing the right treatment by J.
Clinical Communiqué Winter 2002 Interstitial Cystitis A Clinical Spectrum Jack Barkin, MD Chief of Urology, Humber River Regional Hospital, Toronto, Ontario Editorial Choosing the right treatment by J.
Interstitial Cystitis and Pelvic Pain: Looking Beyond the Bladder
 Interstitial Cystitis and Pelvic Pain: Looking Beyond the Bladder Kenneth M. Peters, MD Professor and Chairman of Urology Oakland University William Beaumont School of Medicine Royal Oak, Michigan Disclosures
Interstitial Cystitis and Pelvic Pain: Looking Beyond the Bladder Kenneth M. Peters, MD Professor and Chairman of Urology Oakland University William Beaumont School of Medicine Royal Oak, Michigan Disclosures
Multiple Sclerosis. Véronique Phé, MD, PhD Pitié-Salpêtrière Academic Hospital Department of Urology Paris 6 University Paris, FRANCE
 Queen Square Uro-neurology course, London, UK 20 th -21 st October 2016 Multiple Sclerosis Véronique Phé, MD, PhD Pitié-Salpêtrière Academic Hospital Department of Urology Paris 6 University Paris, FRANCE
Queen Square Uro-neurology course, London, UK 20 th -21 st October 2016 Multiple Sclerosis Véronique Phé, MD, PhD Pitié-Salpêtrière Academic Hospital Department of Urology Paris 6 University Paris, FRANCE
