Lengthening Temporalis Myoplasty for Single-Stage Smile Reconstruction in Children with Facial Paralysis
|
|
|
- Roger Underwood
- 5 years ago
- Views:
Transcription
1 RECONSTRUCTIVE Lengthening Temporalis Myoplasty for Single-Stage Smile Reconstruction in Children with Facial Paralysis Andre Panossian, M.D. Los Angeles, Calif. Background: Free muscle transfer for dynamic smile reanimation in facial paralysis is not always predictable with regard to cosmesis. Hospital stays range from 5 to 7 days. Prolonged operative times, longer hospital stays, and excessive cheek bulk are associated with free flap options. Lengthening temporalis myoplasty offers single-stage smile reanimation with theoretical advantages over free tissue transfer. Methods: From 2012 to 2014, 18 lengthening temporalis myoplasties were performed in 14 children for smile reconstruction. A retrospective chart review was completed for demographics, operative times, length of hospital stay, and perioperative complications. Results: Fourteen consecutive patients with complete facial paralysis were included. Four patients underwent single-stage bilateral reconstruction, and 10 underwent unilateral procedures. Diagnoses included Möbius syndrome (n = 5), posterior cranial fossa tumors (n = 4), posttraumatic (n = 2), hemifacial microsomia (n = 1), and idiopathic (n = 2). Average patient age was 10.1 years. Average operative time was 410 minutes (499 minutes for bilateral lengthening temporalis myoplasty and 373 for unilateral lengthening temporalis myoplasty). Average length of stay was 3.3 days (4.75 days for bilateral lengthening temporalis myoplasty and 2.8 for unilateral lengthening temporalis myoplasty). Nine patients required minor revisions. Conclusions: Lengthening temporalis myoplasty is a safe alternative to free tissue transfer for dynamic smile reconstruction in children with facial paralysis. Limited donor-site morbidity, shorter operative times, and shorter hospital stays are some benefits over free flap options. However, revisions are required frequently secondary to tendon avulsions and adhesions. (Plast. Reconstr. Surg. 137: 1251, 2016.) CLINICAL QUESTION/LEVEL OF EVIDENCE: Therapeutic, IV. Current techniques used for the correction of permanent and complete facial paralysis involve static or dynamic procedures. With the introduction of the innervated, vascularized free muscle transfer, a large jump was made in both aesthetics and function. 1 The procedure, designed to address lower facial nerve palsy, is highly successful in achieving excursion of the oral commissure and bilabial closure. The result has been an improvement in dynamic smile From the Division of Plastic and Maxillofacial Surgery, Children s Hospital Los Angeles. Received for publication May 6, 2015; accepted November 19, Copyright 2016 by the American Society of Plastic Surgeons DOI: /PRS reanimation. The muscle (e.g., gracilis, latissimus dorsi, biceps femoris, serratus anterior, pectoralis minor) may be staged with cross-face nerve grafting using the contralateral functioning Disclosure: The author has no financial interest to declare in relation to the content of this article. Supplemental digital content is available for this article. Direct URL citations appear in the text; simply type the URL address into any Web browser to access this content. Clickable links to the material are provided in the HTML text of this article on the Journal s Web site (www. PRSJournal.com)
2 Plastic and Reconstructive Surgery April 2016 facial nerve or connected directly to an ipsilateral donor nerve, such as the masseter nerve. 2 5 The advantage of two stages is spontaneous initiation of smiling by means of the unaffected contralateral facial nerve branches. Each option carries its own set of advantages and disadvantages, extensively outlined in previous studies. However, several persistent flaws exist when using functional free muscle transfer. First, the resulting increase in cheek bulk may be difficult to control, despite accommodation by means of lipectomy of the soft tissues. This problem may exist in either the resting state or with animation. Second, the placement of the nasolabial fold has proven challenging and can vary widely because of unpredictable changes that occur with animation. Its true placement cannot be known with certainty until reinnervation has occurred and excursion can be visualized. Third, the optimal vector of oral commissure excursion is also difficult to predict intraoperatively, making fine adjustments difficult to predict. Fourth, surgical times can be extensive and hospitalization may be as long as 5 to 7 days, often requiring admission to the intensive care unit for flap monitoring. Finally, the time to achieve excursion of the oral commissure can take between 2 and 6 months or longer for innervation to reach the transplanted muscle. In recent years, Labbé and Huault have repopularized the temporalis myoplasty for lip reanimation. 6 Several key refinements were made on the initial work by McLaughlin in 1949 to improve results. 7 The lengthening temporalis myoplasty, as described, involved mobilizing the ipsilateral temporalis muscle while keeping the neurovascular pedicle intact. The insertion of the muscle on the coronoid is mobilized and transmitted in an antegrade fashion, deep to the zygoma toward the upper lip where it is attached to the oral commissure and upper lip. Aside from a case series reported by Veyssière et al., there are no other case series on this technique in the pediatric population. 8 Recognizing the limitations of free muscle transfer for facial reanimation and the relative paucity of data of this technique in children, we describe our experience using the lengthening temporalis myoplasty in a largely pediatric population. PATIENTS AND METHODS Between 2012 and 2014, a total of 18 lengthening temporalis myoplasty procedures were performed in 14 consecutive patients. A retrospective chart review was performed to determine diagnosis, laterality, and ancillary procedures performed. Patient and operative variables collected included age, sex, operative times, length of hospital stay, perioperative complications, ancillary procedures, and revisions performed. Preoperative and postoperative frontal view photographs were used to assess excursion and vector symmetry. Excursion was measured on examination preoperatively and postoperatively at the oral commissure and the mid upper lip using the ruler technique described by Manktelow et al. 9 Surgical Technique The surgical technique has been described previously (Fig. 1). 6,10 Preoperative assessments of excursion of the oral commissure and vector of pull are made with the patient awake and in the upright position (Fig. 2). Markings are placed on the unaffected side, and contralateral markings are made for symmetry in the setting of unilateral facial nerve palsy. The temporalis muscle is accessed by means of a coronal incision. The zygomatic arch may be osteotomized to expose the contents of the infratemporal fossa. The temporalis tendon is identified in this space as it inserts on the coronoid process of the mandible. An oblique osteotomy releases the coronoid process with the attached temporalis tendon insertion. This can be accomplished from the coronal incision above or through the nasolabial fold incision from below. After mobilizing the temporalis muscle, the coronoid and temporalis tendon are passed as a unit through the buccal fat pad and into the cheek. A counterincision is placed carefully along the future nasolabial fold externally, if not already done for access to the coronoid process. Symmetry is determined preoperatively with the patient actively animating the lip. In the setting of bilateral facial paralysis (e.g., Möbius syndrome), an arbitrary nasolabial fold incision is placed at the expected location between the skin of the upper lip and cheek. The coronoid process is grasped through this incision and gently pulled through the buccal tunnel (Fig. 3). The tendon is carefully stripped, and the bone is discarded. The temporalis tendon is then opened into a broad, flat configuration from its conical shape. A large area of insertion is achieved from the oral commissure into the upper lip, just distal to the nasolabial fold. The temporalis muscle is rotated at the expense of the posterior half to allow the tendon to pass with enough length to avoid an interpositional graft. The muscle is reanchored in its new configuration within the temporalis fossa and tested for adequate excursion. A muscle stimulator is used 1252
3 Volume 137, Number 4 Lengthening Temporalis Myoplasty Fig. 1. Lengthening temporalis myoplasty. (Left) The coronoid process is osteotomized (dashed line) distal to the insertion of the temporalis tendon. (Center) The temporalis is mobilized posteriorly, and the tendon is freed. A tunnel is created in the buccal fat pad. The temporalis tendon is then passed through the tunnel and brought out through a nasolabial fold incision. (Right) The tendon is then stripped from the coronoid bone and unwound. It is anchored to the oral commissure and upper lip. Fig. 3. The temporalis tendon, attached to the coronoid process, is directed through the buccal fat pad and delivered through the nasolabial fold incision. Fig. 2. Preoperative markings of the planned nasolabial fold and vector of excursion of contralateral oral commissure. In this case, contralateral lower lip depressor myectomy was planned also (green hatch marks). to create a tetanic contraction to refine the vector of excursion at the oral commissure and reproduce movement as seen on the unaffected side. The tendon insertion is adjusted to replicate the patient s normal smile according to the Rubin classification. An indwelling anesthetic infusion catheter is placed along the neurovascular pedicle to avoid excessive spasm of the temporalis muscle and to provide pain relief. Ancillary procedures include contralateral zygomaticus major/minor and risorius chemodenervation with botulinum toxin type A (Botox; Allergan, Inc., Irvine, Calif.). 11,12 A total of 6 to 8 units of Botox (2 units per 0.1 ml of solution) is injected near the junction between these muscles and the orbicularis oris. Injection into the contralateral, active facial musculature causes relaxation of unopposed contraction and allows the temporalis muscle insertion and origin to anchor in their new position without excessive countertension. This small amount of Botox limited to the distal portions of the muscles only serves to weaken their pull on the upper lip and oral commissure without inducing lip lag on 1253
4 Plastic and Reconstructive Surgery April 2016 the unaffected side. In addition, some patients subjectively demonstrating excessive contralateral lower lip depressor muscle activity underwent transbuccal myectomy to reestablish lower lip symmetry. 13,14 Physical therapy is started 3 weeks after surgery. Goals are to achieve greater mobility and symmetry, develop spontaneity, and improve swallowing and speech. A physical therapist initiates a biofeedback program, scar and facial massage, tendon gliding, motor learning, and a home mirror (mime) exercise program. Anatomy The temporalis muscle originates broadly in the temporal fossa and the temporal crest. Deep and superficial layers have been described. 15 The muscle converges from its fan-like orientation to a unique three-dimensional tendon that inserts on the coronoid process of the mandible. 16 As it passes deep to the zygomatic arch, there is intimate association with the masseter muscle. Fibers from the masseter can intermingle and attach to the temporalis muscle and tendon, thereby potentially limiting excursion underneath the arch. These masseter fibers can insert as far as 2 cm above the zygomatic arch onto the deep temporalis fascia. 17 The temporalis is dually innervated by the anterior and posterior deep temporal nerves, arising from the anterior division of the mandibular nerve (V 3 ). Being a muscle of mastication, it is responsible for powerfully establishing occlusion. It is a single-vector muscle in this regard and an ideal candidate for smile reconstruction. Its arterial supply is from the anterior and posterior deep temporal arteries, divisions of the internal maxillary artery. The vessels emerge within the infratemporal fossa and travel with the anterior and posterior deep temporal nerves as they separate from the mandibular nerve (through the foramen ovale). Simply disinserting the temporalis tendon from the coronoid process and stretching it toward the perioral region is usually insufficient and overstretches the native resting length of the muscle. Tendon or fascial interposition grafts have been used to make up the difference in length. 18 However, this often results in inadequate excursion. Lengthening of the temporalis tendon in lengthening temporalis myoplasty occurs at the expense of the posterior half of the temporalis muscle. 19 RESULTS A total of 18 lengthening temporalis myoplasty procedures were performed in 14 consecutive patients with complete facial paralysis over a 2-year period (Table 1). Ten patients underwent unilateral procedures, and four patients had bilateral lengthening temporalis myoplasty performed. Average patient age was 10.1 years (range, 5.4 to 17.8 years). Follow-up ranged from 10 to 34 months, with an average of 28 months. All patients demonstrated mobility of the lip along the upper lip and oral commissure, with nasolabial fold creation. Average time to animation was 2.5 weeks. Range of oral commissure excursion was between 5 and 13 mm, with an average of 8.2 mm. Smiling was activated coincidently with biting in all patients. No interpositional fascia or tendon grafts were used. Average operative time was 410 minutes (499 minutes for bilateral lengthening temporalis myoplasty and 373 minutes for unilateral lengthening temporalis myoplasty). Average length of stay was 3.3 days (4.75 days for bilateral lengthening Table 1. Summary of Patient Data Patient Age (yr) Sex Diagnosis Laterality Follow-Up (mo) Operative Time (min) Length of Stay (days) Commissure Excursion (mm) Revision 1 5 F Möbius syndrome B No 2 14 F Möbius syndrome R Yes 3 12 M Medulloblastoma R No 4 5 F Idiopathic L Yes 5 7 M Möbius syndrome B Yes 6 9 M Möbius syndrome B Yes 7 10 F Medulloblastoma R Yes 8 6 M Astrocytoma L Yes 9 8 M Trauma L Yes F Trauma L Yes F Hemifacial microsomia R No 12 8 M Möbius syndrome B No F Medulloblastoma L No F Idiopathic R Yes M, male; F, female; L, left; R, right; B, bilateral. 1254
5 Volume 137, Number 4 Lengthening Temporalis Myoplasty temporalis myoplasty and 2.8 days for unilateral lengthening temporalis myoplasty). Five patients had simultaneous contralateral depressor angularis oris myectomy performed for lower lip symmetry. One patient underwent simultaneous lagophthalmos correction, and six patients had injection of Botox into the contralateral zygomaticus major and minor, risorius, and depressor angularis oris muscles. Three patients demonstrated moderate temporal hollowing. These patients did not undergo any further correction, although fat injection was offered. Nine patients required revision of the temporalis tendon insertion site or lysis of adhesions (64 percent), and two patients required blood transfusion during the perioperative period. One patient developed a postoperative infection requiring incision and drainage. CASE REPORTS Case 1 A 10-year-old girl (patient 7 in Table 1) developed complete right facial paralysis following resection of a medulloblastoma (Fig. 4). With no recovery of facial nerve function 18 months later, the patient underwent a lengthening temporalis myoplasty with simultaneous contralateral lower lip depressor angularis oris and labii inferioris myectomy for balance and symmetry. The patient developed moderate temporal hollowing. She subsequently underwent revision of the tendon insertion site 3 years later. At 3 months postoperatively, she demonstrated improved excursion and symmetry of her smile. (See Video, Supplemental Digital Content 1, which demonstrates the patient in case 1, a 10-year-old girl who underwent unilateral lengthening temporalis myoplasty and subsequent revision. Preoperative and postoperative perioral function is recorded, Case 2 An 8-year-old boy with Möbius syndrome (patient 12 in Table 1) and complete bilateral facial paralysis underwent smile Fig. 4. Case 1 (patient 7 in Table 1). (Above) Complete right facial paralysis over 2 years after resection of a medulloblastoma. Shown preoperatively at rest and with a full-tooth smile. (Below) Postoperative appearance at 2 months after revision of the tendon insertion site. She did demonstrate moderate right temporal hollowing after the initial operation. 1255
6 Plastic and Reconstructive Surgery April 2016 Video 1. Supplemental Digital Content 1 demonstrates the patient in case 1, a 10-year-old girl who underwent unilateral lengthening temporalis myoplasty and subsequent revision. Preoperative and postoperative perioral function is recorded, restoration with single-stage bilateral lengthening temporalis myoplasties (Fig. 5). The patient required a 4-day hospitalization and was discharged to home with an unremarkable postoperative course. Three weeks after surgery, the patient was started on facial therapy, including biofeedback and mirror exercises. He demonstrated excellent symmetry and mobility of the smile with 13 mm of oral commissure excursion and good nasolabial fold production. (See Video, Supplemental Digital Content 2, which demonstrates postoperative perioral function following a bilateral lengthening temporalis myoplasty procedure for the patient in case 2, Case 3 A 10-year-old girl (patient 13 in Table 1) presented with a 14-month history of complete left hemifacial paralysis following resection of a medulloblastoma (Fig. 6). Given the total lack of reinnervation of the facial nerve and persistent facial asymmetry, the patient was recommended for a lengthening temporalis myoplasty for lip reanimation. She also underwent contralateral depressor angularis oris and labii inferioris myectomy for lower lip balance. The patient was hospitalized for 4 days and had an unremarkable postoperative course. She demonstrated immediate mobility of the oral commissure (11-mm excursion) with improvement of facial symmetry. She developed effortless activation of the smile within 3 weeks and required no revisions. (See Video, Supplemental Digital Content 3, which demonstrates postoperative results following unilateral lengthening temporalis myoplasty for the patient in case 3, com/prs/b657.) DISCUSSION The lengthening temporalis myoplasty is an intriguing take on an infrequently used muscle transfer for facial paralysis. By advancing the temporalis in an antegrade fashion, the temporalis tendon achieves better elongation for upper lip and oral commissure attachment without the need for intervening grafts. The vector of excursion is optimal for smile restoration. There are numerous potential benefits to using lengthening temporalis myoplasty for smile reanimation over vascularized free muscle transfers such as the gracilis. First, by eliminating the microsurgical component, operative time is shortened substantially. There is no secondary donor site requiring healing, and postoperative vascular compromise is not a concern. Also, there is no requirement for postoperative intensive care unit stay or prolonged hospitalization. It is even conceivable that lengthening temporalis myoplasty can be performed on an outpatient basis in selected patients. Second, the actuating temporalis muscle is not denervated; therefore, the time to animation is negligible over free tissue transfer, which requires time for nerve regeneration. This has an impact on immediate results and on initiating facial therapy. Third, the problem of excessive cheek bulk common to free muscle transfers is avoided because of the trajectory of the temporalis tendon deep to the zygomatic arch and within the buccal fat pad. Fourth, smile reconstruction can be tested intraoperatively by direct muscle stimulation and adjusted as necessary. 6,20,21 This is an important advantage of lengthening temporalis myoplasty over free muscle transfer. By stimulating the muscle, the degree of expected postoperative movement is predicted along with vector of excursion and accurate placement of anchoring sutures. Fifth, placement of a nasolabial incision is helpful in defining the location of the nasolabial fold, exactly at the junction of the upper lip and cheek skin. 22 It also aids in the adjustment of anchoring sutures for the temporalis tendon insertion. In some instances, coronoidectomy can be performed through this incision without the need for zygomatic arch osteotomy. Lastly, by shortening the surgical time, ancillary procedures can be performed to help improve global facial symmetry. Contralateral lower lip depressor myectomy or Botox injection, ipsilateral lagophthalmos correction, ipsilateral brow elevation, and midface lift can all be performed in a single, comprehensive operative effort. There is one large disadvantage noted. Less than ideal excursion resulted from tendon avulsion from the insertion site and/or muscle adhesions within the cheek and subzygomatic region. In our study, 64 percent of patients required revision surgery, including tenolysis and readvancement of the temporalis tendon. This occurred 1256
7 Volume 137, Number 4 Lengthening Temporalis Myoplasty Fig. 5. Case 2. (Above, left) Bilateral facial paralysis in a Möbius syndrome patient (patient 12 in Table 1) during attempted smile. (Above, right) Reorientation and fixation of temporalis origin following bilateral lengthening temporalis myoplasty. (Below) Postoperative facial motion at 17 months. despite measures to reduce tension on the temporalis muscle, including use of Botox on contralateral facial musculature and placement of an indwelling local anesthetic infuser catheter near the neurovascular pedicle. This is admittedly a rather high rate. However, revisions were all performed on an outpatient basis through the nasolabial fold incision only. In older children and adults, it is conceivable that this type of revision can be performed under local anesthesia. Nonetheless, as experience with lengthening temporalis myoplasty evolves, refinements in technique may eliminate this problem or reduce it significantly. Another disadvantage is one that is common also to free gracilis muscle transfers that use the masseter nerve for stimulation. Given that the temporalis muscle is supplied by the trigeminal nerve, it lacks an element of spontaneity. Muscle retraining is a requirement and may not occur for months to years. However, other reports have indicated a return of spontaneous or effortless smile activation in the majority of patients. 23,24 These studies reiterate the existence of cortical plasticity and reorganization of the motor system to functionally relevant muscles. 25,26 Next, although placement of a nasolabial fold incision is helpful in defining the desired location on the paralyzed side and for insetting the temporalis tendon, the presence of an external incision is not ideal. Some studies have suggested that subdermal plication more accurately defines this structure by means of a facial skin flap The difficulty lies in reproducibility. Also, the presence of a nasolabial fold incision allows easy access for revision surgery when necessary, without the need to elevate large facial skin flaps. Although a buccal incision is an attractive option in accessing the temporalis tendon, it still proves challenging in the precise placement of tendon-anchoring 1257
8 Plastic and Reconstructive Surgery April 2016 Video 2. Supplemental Digital Content 2 demonstrates postoperative perioral function following a bilateral lengthening temporalis myoplasty procedure for the patient in case 2 (patient 12 in Table 1). sutures in the perioral region required for recreation of the nasolabial fold. Also, three patients demonstrated moderate temporal contour deficit several months postoperatively. There are three potential sources for this problem. As part of the learning curve, earlier cases were performed with complete mobilization of the temporalis within the temporal fossa as opposed to only the posterior half. The visual portion of the temporal fossa is the anterior portion. Despite resecuring the muscle to a cuff of strong fascia along the anterior temporal crest, thinning of the overlying tissues was observed. Alternatively, or synergistically, elevation of the coronal flap over the zygomatic arch must include a fat pad that resides on the deep temporalis fascia. This was inadvertently omitted in early efforts. The fat pad must then be excised if left on top of the temporalis, because it interferes with Fig. 6. Case 3 (patient 13 in table 1). (Above, left) Complete left facial paralysis nearly 3 years after resection of a medulloblastoma. Preoperative markings and asymmetric smile are shown. (Above, right) Postoperative appearance at 7 months after lengthening temporalis myoplasty. (Below) Oblique view of postoperative smile activation. 1258
9 Volume 137, Number 4 Lengthening Temporalis Myoplasty Video 3. Supplemental Digital Content 3 demonstrates postoperative results following unilateral lengthening temporalis myoplasty for the patient in case 3, elongation of the tendon in the subzygomatic region as it passes into the buccal space. Finally, zygomatic arch osteotomy itself may result in atrophy of the osteotomized segment. This final point is difficult to prove without further studies using postoperative computed tomography. Unlike cranial vault remodeling or fronto-orbital advancement where true temporal hollowing occurs as a result of a bony phenomenon, temporal contour deformities in lengthening temporalis myoplasty are related to soft-tissue changes. 30,31 Other variations of temporalis tendon transfer have been used with varying degrees of success The orthodromic temporalis tendon transfer uses a single incision to mobilize only the coronoid process and attached tendon. No additional lengthening is reported. Simple transfer of the tendon to the oral commissure from the coronoid process has proven to be difficult and frequently requires an interpositional tendon or fascial graft. 37,38 Results with interpositional grafting have been mediocre and difficult to reproduce. In lengthening temporalis myoplasty, by mobilizing the temporalis muscle and allowing it to advance or lengthen at the expense of its posterior segment, the tendon is able to achieve sufficient length to reach the upper lip and oral commissure without a tendon graft. We did observe this advantage. An intervening, nonvascularized graft has the disadvantage of succumbing to scarring and weakening over time, both of which can adversely affect outcomes. The more traditional temporalis turnover flap predates microvascular functional muscle transfers. 22,39 41 In this procedure, the entire muscle or a portion of it is turned over the zygomatic arch and stretched toward the perioral region. Many disadvantages make this a less desirable option. First, excessive bulk over the zygomatic arch can be unsightly. Second, the length of muscle from the top of the origin of the muscle to the pivot point above the arch is frequently too short to reach the corner of the mouth. This requires the use of a nonvascularized interpositional fascia or tendon graft, which frequently results in adhesions, weakening, and loss of movement. In addition, a secondary donor site is required. None of the patients in this study required an interpositional graft. Third, if the entire muscle is used, there is a significant degree of temporal hollowing requiring secondary procedures to fill. Other single-stage options for lip reanimation are available, including free latissimus dorsi, rectus abdominis, and serratus anterior flaps These flap options promise greater spontaneity by means of coaptation with the contralateral functioning facial nerve. Proposed initially by Harii, the segmental latissimus dorsi flap involves harvesting a long length of thoracodorsal nerve that will then need to regenerate into the implanted muscle. 48 Although some studies report favorable results, others highlight inconsistent results and a high failure rate as described by weak or no contraction. In addition, there are a wide range of reported latent periods until reinnervation occurred, from 3 to 16 months. In the pursuit of true spontaneity of smile, the two-stage cross-face nerve graft followed by free muscle graft is perhaps a better option. The length of time to reinnervation of the transplanted muscle is critical. By allowing the nerve impulse to regenerate along the cross-face nerve graft, the distance required for secondary innervation into the functional muscle is effectively shortened. As with gracilis muscle transfer for lip reanimation, lengthening temporalis myoplasty addresses only oral commissure and upper lip elevation as it occurs with smiling. The procedure by itself does not address other sequelae of facial paralysis, such as the lack of ipsilateral lower lip depression. However, the shortened operative time offered by lengthening temporalis myoplasty allows simultaneous correction of several facial asymmetries, including contralateral lower lip depressor myectomy, lagophthalmos correction, and contralateral frontalis myectomy. 49 In addition, 1259
10 Plastic and Reconstructive Surgery April 2016 chemodenervation of overactive contralateral facial musculature with Botox can be performed quickly and easily, without any discomfort. CONCLUSIONS The lengthening temporalis myoplasty is an excellent and reproducible alternative to free vascularized muscle transfer for smile reanimation in facial paralysis. Some of the advantages include reduced operative time and hospital stay, quicker time to activation, and improved cheek contour without excess bulk. The disadvantages include a steep learning curve and high revision rate secondary to problems at the temporalis tendon insertion site. We observed greater predictability of smile reanimation with increased experience with the technique. Modifications and refinements can conceivably improve results further. Andre Panossian, M.D Wilshire Boulevard, Suite 200 Beverly Hills, Calif drpanossian@drpanossian.com PATIENT CONSENT Parents or guardians provided written consent for the use of patients images. REFERENCES 1. Zuker RM. Microvascular management of facial palsy. In: Current Therapy in Plastic and Reconstructive Surgery. Boca Raton, Fla: CRC Press; 1989: Manktelow RT, Tomat LR, Zuker RM, Chang M. Smile reconstruction in adults with free muscle transfer innervated by the masseter motor nerve: Effectiveness and cerebral adaptation. Plast Reconstr Surg. 2006;118: Manktelow RT, Manktelow RT. Cross-facial nerve graft: The long and short graft. The first stage for microneurovascular muscle transfer. Oper Tech Plast Reconstr Surg. 1999;6: Fattah A, Borschel GH, Manktelow RT, Bezuhly M, Zuker RM. Facial palsy and reconstruction. Plast Reconstr Surg. 2012;129:340e 352e. 5. Bae YC, Zuker RM, Manktelow RT, Wade S. A comparison of commissure excursion following gracilis muscle transplantation for facial paralysis using a cross-face nerve graft versus the motor nerve to the masseter nerve. Plast Reconstr Surg. 2006;117: Labbé D, Huault M. Lengthening temporalis myoplasty and lip reanimation. Plast Reconstr Surg. 2000;105: ; discussion McLaughlin CR. Surgical support in permanent facial paralysis. Plast Reconstr Surg (1946) 1953;11: Veyssière A, Labbé D, Bénateau H. Lengthening temporalis myoplasty and facial paralysis from birth. J Plast Reconstr Aesthet Surg. 2015;68: Manktelow RT, Zuker RM, Tomat LR. Facial paralysis measurement with a handheld ruler. Plast Reconstr Surg. 2008;121: Labbé D. Lengthening temporalis myoplasty V.2. and lip reanimation (in French). Ann Chir Plast Esthet. 2009;54: Kim J. Contralateral botulinum toxin injection to improve facial asymmetry after acute facial paralysis. Otol Neurotol. 2013;34: Clark RP, Berris CE. Botulinum toxin: A treatment for facial asymmetry caused by facial nerve paralysis. Plast Reconstr Surg. 1989;84: Labbé D, Bénichou L, Iodice A, Giot JP. Depressor anguli oris sign (DAO) in facial paresis: How to search it and release the smile (technical note) (in French). Ann Chir Plast Esthet. 2012;57: Hussain G, Manktelow RT, Tomat LR. Depressor labii inferioris resection: An effective treatment for marginal mandibular nerve paralysis. Br J Plast Surg. 2004;57: Lee JY, Kim JN, Kim SH, et al. Anatomical verification and designation of the superficial layer of the temporalis muscle. Clin Anat. 2012;25: Bénateau H, Alix T, Labbé D, Elissalde JM, Salamé E. Anatomic study of the tendinous insertion lamina of the temporalis muscle. Surg Radiol Anat. 2004;26: Guerreschi P, Gahagnon T, Vacher C, Drizenko A, Francke JP, Labbe D. Masseter muscle termination over the deep surface of the temporal fascia: Look out the wrong path. Surg Radiol Anat. 2011;33: Brown JB. The utilization of the temporal muscle and fascia in facial paralysis. Ann Surg. 1939;109: Martín LP, Otero TG, Gallo JA, Pérez SM, García MB. Mioplastia de elongación de músculo temporal para rehabilitación de parálisis hemifacial. Rev Esp Cir Oral Maxilofacial 2011;33: Har-Shai Y, Gil T, Metanes I, Labbé D. Intraoperative muscle electrical stimulation for accurate positioning of the temporalis muscle tendon during dynamic, one-stage lengthening temporalis myoplasty for facial and lip reanimation. Plast Reconstr Surg. 2010;126: Har-Shai Y, Metanes I, Badarny S, et al. Lengthening temporalis myoplasty for facial palsy reanimation. Isr Med Assoc J. 2007;9: Baker DC, Conley J. Regional muscle transposition for rehabilitation of the paralyzed face. Clin Plast Surg. 1979;6: Garmi R, Labbé D, Coskun O, Compère JF, Bénateau H. Lengthening temporalis myoplasty and brain plasticity: A functional magnetic resonance imaging study. Ann Chir Plast Esthet. 2013;58: Blanchin T, Martin F, Labbe D. Lengthening temporalis myoplasty: A new approach to facial rehabilitation with the mirror-effect method (in French). Ann Chir Plast Esthet. 2013;58: Manduch M, Bezuhly M, Anastakis DJ, Crawley AP, Mikulis DJ. Serial fmri of adaptive changes in primary sensorimotor cortex following thumb reconstruction. Neurology 2002;59: Chen R, Anastakis DJ, Haywood CT, Mikulis DJ, Manktelow RT. Plasticity of the human motor system following muscle reconstruction: A magnetic stimulation and functional magnetic resonance imaging study. Clin Neurophysiol. 2003;114: Bhama PK, Park JG, Shanley K, Hadlock TA. Refinements in nasolabial fold reconstruction for facial paralysis. Laryngoscope 2014;124: Zhang L, Tang MY, Jin R, et al. Classification of nasolabial folds in Asians and the corresponding surgical approaches: By Shanghai 9 th People s Hospital. J Plast Reconstr Aesthet Surg. 2015;68: Rubin LR, Mishriki Y, Lee G. Anatomy of the nasolabial fold: The keystone of the smiling mechanism. Plast Reconstr Surg. 1989;83:
11 Volume 137, Number 4 Lengthening Temporalis Myoplasty 30. Steinbacher DM, Wink J, Bartlett SP. Temporal hollowing following surgical correction of unicoronal synostosis. Plast Reconstr Surg. 2011;128: Matic DB, Kim S. Temporal hollowing following coronal incision: A prospective, randomized, controlled trial. Plast Reconstr Surg. 2008;121:379e 385e. 32. Parker NP, Eisler LS, Dresner HS, Walsh WE. Orthodromic temporalis tendon transfer: Anatomical considerations. Arch Facial Plast Surg. 2012;14: Griffin GR, Kim JC. Orthodromic temporalis tendon transfer. Oper Tech Otolaryngol Head Neck Surg. 2012;23: Cannady SB, Rosenthal EL, Knott PD, Fritz M, Wax MK. Free tissue transfer for head and neck reconstruction: A contemporary review. JAMA Facial Plast Surg. 2014;16: Byrne PJ, Kim M, Boahene K, Millar J, Moe K. Temporalis tendon transfer as part of a comprehensive approach to facial reanimation. Arch Facial Plast Surg. 2007;9: Boahene KD, Farrag TY, Ishii L, Byrne PJ. Minimally invasive temporalis tendon transposition. Arch Facial Plast Surg. 2011;13: Aum JH, Kang DH, Oh SA, Gu JH. Orthodromic transfer of the temporalis muscle in incomplete facial nerve palsy. Arch Plast Surg. 2013;40: May M, Drucker C. Temporalis muscle for facial reanimation: A 13-year experience with 224 procedures. Arch Otolaryngol Head Neck Surg. 1993;119: ; discussion Mathog RH, Ragab MA. Temporalis muscle-galea flap in facial reanimation. Arch Otolaryngol. 1985;111: May M. Muscle transposition for facial reanimation: Indications and results. Arch Otolaryngol. 1984;110: Cheney ML, McKenna MJ, Megerian CA, Ojemann RG. Early temporalis muscle transposition for the management of facial paralysis. Laryngoscope 1995;105: Wei W, Zuoliang Q, Xiaoxi L, et al. Free split and segmental latissimus dorsi muscle transfer in one stage for facial reanimation. Plast Reconstr Surg. 1999;103: ; discussion Harii K, Asato H, Yoshimura K, Sugawara Y, Nakatsuka T, Ueda K. One-stage transfer of the latissimus dorsi muscle for reanimation of a paralyzed face: A new alternative. Plast Reconstr Surg. 1998;102: Asato H, Harii K, Takushima A. Smile reconstruction using one-stage transfer of the latissimus dorsi muscle. Oper Tech Plast Reconstr Surg. 2006;6: Sajjadian A, Song AY, Khorsandi CA, et al. One-stage reanimation of the paralyzed face using the rectus abdominis neurovascular free flap. Plast Reconstr Surg. 2006;117: Bartlett SP. Smile reconstruction using the serratus anterior muscle. Oper Tech Plast Reconstr Surg. 1999;6: Takushima A, Harii K, Asato H, Ueda K, Yamada A. Neurovascular free-muscle transfer for the treatment of established facial paralysis following ablative surgery in the parotid region. Plast Reconstr Surg. 2004;113: Harii K. Microneurovascular free muscle transplantation for reanimation of facial paralysis. Clin Plast Surg. 1979;6: Labbé D, Bussu F, Iodice A. A comprehensive approach to long-standing facial paralysis based on lengthening temporalis myoplasty. Acta Otorhinolaryngol Ital. 2012;32:
Rehabilitation of the Paralyzed Face
 Rehabilitation of the Paralyzed Face Elizabeth J. Rosen, MD Faculty Advisor: Karen H. Calhoun, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation October 30,
Rehabilitation of the Paralyzed Face Elizabeth J. Rosen, MD Faculty Advisor: Karen H. Calhoun, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation October 30,
Dynamic Facial Reanimation With Orthodromic Temporalis Tendon Transfer in Children
 Research Case Report/Case Series Dynamic Facial Reanimation With Orthodromic Temporalis Tendon Transfer in Children Rajanya S. Petersson, MD; Daniel E. Sampson, MD; James D. Sidman, MD IMPORTNCE To our
Research Case Report/Case Series Dynamic Facial Reanimation With Orthodromic Temporalis Tendon Transfer in Children Rajanya S. Petersson, MD; Daniel E. Sampson, MD; James D. Sidman, MD IMPORTNCE To our
Comparison of one-stage free gracilis muscle flap with two-stage method in chronic facial palsy*
 Original Research Medical Journal of the Islamic Republic of Iran.Vol. 21, No.2, August 2007. pp. 63-70 Comparison of one-stage free gracilis muscle flap with two-stage method in chronic facial palsy*
Original Research Medical Journal of the Islamic Republic of Iran.Vol. 21, No.2, August 2007. pp. 63-70 Comparison of one-stage free gracilis muscle flap with two-stage method in chronic facial palsy*
Endoscopic Approach for Lengthening the Temporalis Muscle
 Ideas and Innovations Endoscopic Approach for Lengthening the Temporalis Muscle Rubén Contreras-García, M.D., Pedro D. Martins, M.D., and Jefferson Braga-Silva, M.D., Ph.D. Porto Alegre, Brazil The temporalis
Ideas and Innovations Endoscopic Approach for Lengthening the Temporalis Muscle Rubén Contreras-García, M.D., Pedro D. Martins, M.D., and Jefferson Braga-Silva, M.D., Ph.D. Porto Alegre, Brazil The temporalis
RECONSTRUCTIVE.
 RECONSTRUCTIVE Intraoperative Muscle Electrical Stimulation for Accurate Positioning of the Temporalis Muscle Tendon during Dynamic, One-Stage Lengthening Temporalis Myoplasty for Facial and Lip Reanimation
RECONSTRUCTIVE Intraoperative Muscle Electrical Stimulation for Accurate Positioning of the Temporalis Muscle Tendon during Dynamic, One-Stage Lengthening Temporalis Myoplasty for Facial and Lip Reanimation
Smile Restoration for Permanent Facial Paralysis
 Continuing Medical Education Smile Restoration for Permanent Facial Paralysis Jonathan Leckenby, Adriaan Grobbelaar Department of Plastic Surgery, The Royal Free Hospital, University of London, London,
Continuing Medical Education Smile Restoration for Permanent Facial Paralysis Jonathan Leckenby, Adriaan Grobbelaar Department of Plastic Surgery, The Royal Free Hospital, University of London, London,
Head and Face Anatomy
 Head and Face Anatomy Epicranial region The Scalp The soft tissue that covers the vault of skull. Extends from supraorbital margin to superior nuchal line. Layers of the scalp S C A L P = skin = connective
Head and Face Anatomy Epicranial region The Scalp The soft tissue that covers the vault of skull. Extends from supraorbital margin to superior nuchal line. Layers of the scalp S C A L P = skin = connective
Lower Facial Reanimation Techniques Following Cancer Resection and Free Flap Reconstruction
 The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Lower Facial Reanimation Techniques Following Cancer Resection and Free Flap Reconstruction Alexandra E.
The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Lower Facial Reanimation Techniques Following Cancer Resection and Free Flap Reconstruction Alexandra E.
The Sublime Beauty of Normal
 Disclosures Basal Cell Carcinoma Surgical Advisory Board, Genentech Corp The Sublime Beauty of Normal P. Daniel Knott, MD FACS Director, Facial Plastic and Reconstructive Surgery UCSF Medical Center The
Disclosures Basal Cell Carcinoma Surgical Advisory Board, Genentech Corp The Sublime Beauty of Normal P. Daniel Knott, MD FACS Director, Facial Plastic and Reconstructive Surgery UCSF Medical Center The
jamafacialplasticsurgery.com JAMA Facial Plastic Surgery September/October 2014 Volume 16, Number 5 359
 Research Case Report/Case Series Salvage Procedures fter Failed Facial Reanimation Surgery Using the Masseteric Nerve as the Motor Nerve for Free Functional Gracilis Muscle Transfer Steffen U. Eisenhardt,
Research Case Report/Case Series Salvage Procedures fter Failed Facial Reanimation Surgery Using the Masseteric Nerve as the Motor Nerve for Free Functional Gracilis Muscle Transfer Steffen U. Eisenhardt,
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY NASOLABIAL FLAP FOR ORAL CAVITY RECONSTRUCTION Harry Wright, Scott Stephan, James Netterville Designed as a true myocutaneous flap pedicled
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY NASOLABIAL FLAP FOR ORAL CAVITY RECONSTRUCTION Harry Wright, Scott Stephan, James Netterville Designed as a true myocutaneous flap pedicled
Use of Gastrointestinal Anastomosis Stapler for Harvest of Gracilis Muscle and Securing It in the Face for Facial Reanimation: A Novel Technique
 Use of Gastrointestinal Anastomosis Stapler for Harvest of Gracilis Muscle and Securing It in the Face for Facial Reanimation: A Novel Technique Sachin M. Shridharani, MD, Sahael M. Stapleton, BS, Richard
Use of Gastrointestinal Anastomosis Stapler for Harvest of Gracilis Muscle and Securing It in the Face for Facial Reanimation: A Novel Technique Sachin M. Shridharani, MD, Sahael M. Stapleton, BS, Richard
Oral incompetence following composite reconstruction
 IDEAS AND INNOVATIONS Lower Lip Suspension Using Bilateral Temporalis Muscle Flaps and Fascia Lata Grafts Rodney K. Chan, M.D. Branko Bojovic, M.D. Simon G. Talbot, M.D. Denton Weiss, M.D. Julian J. Pribaz,
IDEAS AND INNOVATIONS Lower Lip Suspension Using Bilateral Temporalis Muscle Flaps and Fascia Lata Grafts Rodney K. Chan, M.D. Branko Bojovic, M.D. Simon G. Talbot, M.D. Denton Weiss, M.D. Julian J. Pribaz,
International Journal of Pharma and Bio Sciences DYNAMIC REANIMATION FOR FACIAL PARALYSIS A REVIEW ABSTRACT
 Review Article Allied Sciences International Journal of Pharma and Bio Sciences ISSN 0975-6299 DYNAMIC REANIMATION FOR FACIAL PARALYSIS A REVIEW RATHISHREE 1 AND DR. M.P.SANTHOSH KUMAR *2 1 Intern, saveetha
Review Article Allied Sciences International Journal of Pharma and Bio Sciences ISSN 0975-6299 DYNAMIC REANIMATION FOR FACIAL PARALYSIS A REVIEW RATHISHREE 1 AND DR. M.P.SANTHOSH KUMAR *2 1 Intern, saveetha
CHAPTER 11 FACIAL PARALYSIS. Shailesh Agarwal, MD and Arash Momeni, MD
 CHAPTER 11 FACIAL PARALYSIS Shailesh Agarwal, MD and Arash Momeni, MD The facial nerve innervates a total of 23 paired muscles and the orbicularis oris muscle. The majority of muscles innervated by the
CHAPTER 11 FACIAL PARALYSIS Shailesh Agarwal, MD and Arash Momeni, MD The facial nerve innervates a total of 23 paired muscles and the orbicularis oris muscle. The majority of muscles innervated by the
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL
 What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
Kofi D. O. Boahene, MD
 The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. Contemporary Review Principles and Biomechanics of Muscle Tendon Unit Transfer: Application in Temporalis
The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. Contemporary Review Principles and Biomechanics of Muscle Tendon Unit Transfer: Application in Temporalis
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
An Algorithm to Guide Recipient Vessel Selection in Cases of Free Functional Muscle Transfer for Facial Reanimation
 An Algorithm to Guide Recipient Vessel Selection in Cases of Free Functional Muscle Transfer for Facial Reanimation Original Article Francis P Henry, Jonathan I Leckenby, Daniel P Butler, Adriaan O Grobbelaar
An Algorithm to Guide Recipient Vessel Selection in Cases of Free Functional Muscle Transfer for Facial Reanimation Original Article Francis P Henry, Jonathan I Leckenby, Daniel P Butler, Adriaan O Grobbelaar
The muscular system I Muscles of the head neck and trunk
 The muscular system I Muscles of the head neck and trunk Dr. Nabil Khouri Dr. Nabil Khouri MD MSc, PhD Interactions of Skeletal Muscles Skeletal muscles work together or in opposition Muscles only pull
The muscular system I Muscles of the head neck and trunk Dr. Nabil Khouri Dr. Nabil Khouri MD MSc, PhD Interactions of Skeletal Muscles Skeletal muscles work together or in opposition Muscles only pull
It is now widely recognized that there is a critical. Dental Facial Aesthetics Aesthetic shaping of the neck/positive side effects on the gingiva
 Dental Facial Aesthetics Aesthetic shaping of the neck/positive side effects on the gingiva Warren Roberts, DMD This article discusses the relationship between Platysma, a large muscle of the face and
Dental Facial Aesthetics Aesthetic shaping of the neck/positive side effects on the gingiva Warren Roberts, DMD This article discusses the relationship between Platysma, a large muscle of the face and
be very thin and variable. Facial nerve branches that exit the parotid gland are deep to the SMAS.
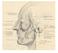 The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
The Role of Botulinum Toxin A in the Establishment of Symmetry in Pediatric Paralysis of the Lower Lip
 Research Original Investigation The Role of Botulinum Toxin A in the Establishment of Symmetry in Pediatric Paralysis of the Lower Lip Siba Haykal, MD, PhD; Ehud Arad, MD; Shaghayegh Bagher, MSc; Carolyn
Research Original Investigation The Role of Botulinum Toxin A in the Establishment of Symmetry in Pediatric Paralysis of the Lower Lip Siba Haykal, MD, PhD; Ehud Arad, MD; Shaghayegh Bagher, MSc; Carolyn
SOFT TISSUE SUPPORT IS AN
 ORIGINAL ARTICLE Reconstructive Application of the Endotine Suspension Devices James H. Boehmler IV, MD; Benjamin L. Judson, MD; Steven P. Davison, MD, DDS Objective: To illustrate the potential reconstructive
ORIGINAL ARTICLE Reconstructive Application of the Endotine Suspension Devices James H. Boehmler IV, MD; Benjamin L. Judson, MD; Steven P. Davison, MD, DDS Objective: To illustrate the potential reconstructive
The International Journal of Periodontics & Restorative Dentistry
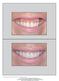 The International Journal of Periodontics & Restorative Dentistry 433 Lip Repositioning for Reduction of Excessive Gingival Display: A Clinical Report Ari Rosenblatt, DMD, DDS* Ziv Simon, DMD, MSc* Excessive
The International Journal of Periodontics & Restorative Dentistry 433 Lip Repositioning for Reduction of Excessive Gingival Display: A Clinical Report Ari Rosenblatt, DMD, DDS* Ziv Simon, DMD, MSc* Excessive
cally, a distinct superior crease of the forehead marks this spot. The hairline and
 4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
3-Deep fascia: is absent (except over the parotid gland & buccopharngeal fascia covering the buccinator muscle)
 The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
The question Which face lift technique is COSMETIC. A Comparison of Face Lift Techniques in Eight Consecutive Sets of Identical Twins
 COSMETIC A Comparison of Face Lift Techniques in Eight Consecutive Sets of Identical Twins Darrick E. Antell, M.D., D.D.S. Michael J. Orseck, M.D. New York, N.Y. Background: Selecting the correct face
COSMETIC A Comparison of Face Lift Techniques in Eight Consecutive Sets of Identical Twins Darrick E. Antell, M.D., D.D.S. Michael J. Orseck, M.D. New York, N.Y. Background: Selecting the correct face
The Subzygomatic Triangle: Rapid, minimally invasive identification of the masseteric nerve for facial ACCEPTED
 Plastic and Reconstructive Surgery Advance Online Article DOI: 10.1097/PRS.0b013e318290f6dc The Subzygomatic Triangle: Rapid, minimally invasive identification of the masseteric nerve for facial reanimation
Plastic and Reconstructive Surgery Advance Online Article DOI: 10.1097/PRS.0b013e318290f6dc The Subzygomatic Triangle: Rapid, minimally invasive identification of the masseteric nerve for facial reanimation
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS. By B. GRUNDT, M.D. Oslo, Norway
 SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS By B. GRUNDT, M.D. Oslo, Norway WE are all familiar with the patient who has paralysis of the facial nerve. The oblique mouth and the corresponding oblique
SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS By B. GRUNDT, M.D. Oslo, Norway WE are all familiar with the patient who has paralysis of the facial nerve. The oblique mouth and the corresponding oblique
Vertical mammaplasty has been developed
 BREAST Y-Scar Vertical Mammaplasty David A. Hidalgo, M.D. New York, N.Y. Background: Vertical mammaplasty is an effective alternative to inverted-t methods. Among other benefits, it results in a significantly
BREAST Y-Scar Vertical Mammaplasty David A. Hidalgo, M.D. New York, N.Y. Background: Vertical mammaplasty is an effective alternative to inverted-t methods. Among other benefits, it results in a significantly
Oral cavity landmarks
 By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
Rehabilitation of the Paralyzed Face October 2002
 TITLE: Rehabilitation of the Paralyzed Face SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: October 30, 2002 RESIDENT PHYSICIAN: Elizabeth J. Rosen, MD FACULTY PHYSICIAN: Karen H.
TITLE: Rehabilitation of the Paralyzed Face SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: October 30, 2002 RESIDENT PHYSICIAN: Elizabeth J. Rosen, MD FACULTY PHYSICIAN: Karen H.
Face. Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face
 Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
THE pedicled flap, commonly used by the plastic surgeon in the reconstruction
 THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
Upper arch. 1Prosthodontics. Dr.Bassam Ali Al-Turaihi. Basic anatomy & & landmark of denture & mouth
 1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
REHABILITATION AND REANIMATION. Facial Plastic Surgery. University of Missouri Columbia, Missouri
 FACIAL NERVE PARALYSIS: REHABILITATION AND REANIMATION Matthew A. Kienstra, MD, FACS Facial Plastic Surgery Mercy Health Care Springfield, Missouri University of Missouri Columbia, Missouri Incidence and
FACIAL NERVE PARALYSIS: REHABILITATION AND REANIMATION Matthew A. Kienstra, MD, FACS Facial Plastic Surgery Mercy Health Care Springfield, Missouri University of Missouri Columbia, Missouri Incidence and
Management of Facial Paralysis
 Section 3: Facial Surgery 6 Management of Facial Paralysis D Bray INTRODUCTION Significant functional, aesthetic and psychosocial sequelae accompany facial paralysis. Dysfunctional lacrimation, palpebral
Section 3: Facial Surgery 6 Management of Facial Paralysis D Bray INTRODUCTION Significant functional, aesthetic and psychosocial sequelae accompany facial paralysis. Dysfunctional lacrimation, palpebral
The Scalp and Face Protocol. Julie Goodwin, BA, LMT
 The Scalp and Face Protocol Julie Goodwin, BA, LMT The Scalp and Face Protocol Julie Goodwin, BA, LMT Julie Goodwin 2014 2 Agenda Pertinent Anatomy and Physiology Treatment Planning Strokes, Techniques
The Scalp and Face Protocol Julie Goodwin, BA, LMT The Scalp and Face Protocol Julie Goodwin, BA, LMT Julie Goodwin 2014 2 Agenda Pertinent Anatomy and Physiology Treatment Planning Strokes, Techniques
SELECTIVE NEURECTOMIES TO ACHIEVE SYMMETRY IN PARTIAL AND COMPLETE FACIAL PARALYSIS
 British Journal of Plastic Surgery (I976), 29, 43-52 SELECTIVE NEURECTOMIES TO ACHIEVE SYMMETRY IN PARTIAL AND COMPLETE FACIAL PARALYSIS By L. CLODIVS, M.D. Plastic Surgery Section, Second Surgical Department,
British Journal of Plastic Surgery (I976), 29, 43-52 SELECTIVE NEURECTOMIES TO ACHIEVE SYMMETRY IN PARTIAL AND COMPLETE FACIAL PARALYSIS By L. CLODIVS, M.D. Plastic Surgery Section, Second Surgical Department,
McGregor Flap Reconstruction of Extensive Lower Lip Defects Following Excision of Squamous Cell Carcinoma
 Kasr El Aini Journal of Surgery VOL., 12, NO 2 May 2011 27 McGregor Flap Reconstruction of Extensive Lower Lip Defects Following Excision of Squamous Cell Carcinoma Mohamed A. Albadawy, MD and Bassem M.
Kasr El Aini Journal of Surgery VOL., 12, NO 2 May 2011 27 McGregor Flap Reconstruction of Extensive Lower Lip Defects Following Excision of Squamous Cell Carcinoma Mohamed A. Albadawy, MD and Bassem M.
The Human Muscular System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5th ed (2017) Chapters 10, 11, 12 INTRODUCTION
 Biology 322: Human Anatomy The Human Muscular System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapters 10, 11, 12 INTRODUCTION We will use a number of lab periods
Biology 322: Human Anatomy The Human Muscular System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapters 10, 11, 12 INTRODUCTION We will use a number of lab periods
Occipital flattening in the infant skull
 Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Lateral Orbitotomy in the Management of Challenging Exotropia
 Lateral Orbitotomy in the Management of Challenging Exotropia Yahalom C (1, 2), Mc Nab A (3), Ben Simon G (3), Kowal L (1). 1- Centre for Eye Research Australia and Ocular Motility Clinic, Royal Victorian
Lateral Orbitotomy in the Management of Challenging Exotropia Yahalom C (1, 2), Mc Nab A (3), Ben Simon G (3), Kowal L (1). 1- Centre for Eye Research Australia and Ocular Motility Clinic, Royal Victorian
Intraoral mandibular distraction osteogenesis in facial asymmetry patients with unilateral temporomandibular joint bony ankylosis
 Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Facial Asymmetry Correction in Facial Palsy Patients with Silhouette Sutures
 International Journal of Clinical Medicine, 2012, 3, 55-59 http://dx.doi.org/10.4236/ijcm.2012.31012 Published Online January 2012 (http://www.scirp.org/journal/ijcm) Facial Asymmetry Correction in Facial
International Journal of Clinical Medicine, 2012, 3, 55-59 http://dx.doi.org/10.4236/ijcm.2012.31012 Published Online January 2012 (http://www.scirp.org/journal/ijcm) Facial Asymmetry Correction in Facial
Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System.
 Case Report Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System. Reconstruction of a Maxillary Oncologic Defect
Case Report Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System. Reconstruction of a Maxillary Oncologic Defect
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure
 Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
UCL Repair: Emphasis on Muscle Dissection and Reconstruction
 UCL Repair: Emphasis on Muscle Dissection and Reconstruction Unilateral cleft lip repair is performed using rotation-advancement technique. Markings are made on columella base, redlines, Cupid s bow on
UCL Repair: Emphasis on Muscle Dissection and Reconstruction Unilateral cleft lip repair is performed using rotation-advancement technique. Markings are made on columella base, redlines, Cupid s bow on
3. The Jaw and Related Structures
 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
An island flap based on the anterior branch of the superficial temporal artery for perioral defects
 Free full text on www.ijps.org Original Article An island flap based on the anterior branch of the superficial temporal artery for perioral defects V. Bhattacharya, Ganji Raveendra Reddy, Sheikh Adil Bashir,
Free full text on www.ijps.org Original Article An island flap based on the anterior branch of the superficial temporal artery for perioral defects V. Bhattacharya, Ganji Raveendra Reddy, Sheikh Adil Bashir,
Cleft lip is the most common craniofacial
 Ideas and Innovations Fat Grafting in Primary Cleft Lip Repair Elizabeth Gordon Zellner, M.D. Miles J. Pfaff, M.D. Derek M. Steinbacher, M.D., D.M.D. New Haven, Conn. Summary: The goal of primary cleft
Ideas and Innovations Fat Grafting in Primary Cleft Lip Repair Elizabeth Gordon Zellner, M.D. Miles J. Pfaff, M.D. Derek M. Steinbacher, M.D., D.M.D. New Haven, Conn. Summary: The goal of primary cleft
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Grading Facial Nerve Function Following Combined Static and Mimetic Surgical Techniques
 416 Original Article Grading Facial Nerve Function Following Combined Static and Mimetic Surgical Techniques John P. Leonetti 1 Sam J. Marzo 1 Douglas A. Anderson 2 Joshua M. Sappington 1 1 Department
416 Original Article Grading Facial Nerve Function Following Combined Static and Mimetic Surgical Techniques John P. Leonetti 1 Sam J. Marzo 1 Douglas A. Anderson 2 Joshua M. Sappington 1 1 Department
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
Our Experience with Endoscopic Brow Lifts
 Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
Figure (2-6): Labial frenum and labial notch.
 The anatomy of the edentulous ridge in the maxilla and mandible is very important for the design of a complete denture. The consistency of the mucosa and architecture of the underlying bone is different
The anatomy of the edentulous ridge in the maxilla and mandible is very important for the design of a complete denture. The consistency of the mucosa and architecture of the underlying bone is different
Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases
 J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
Adults with a capacious midface who desire refinement,
 Managing the uccal Fat Pad The author performs buccal fat pad excision to improve facial contour in some patients with buccal lipodystrophy and to treat buccal fat pad pseudoherniation. He recommends an
Managing the uccal Fat Pad The author performs buccal fat pad excision to improve facial contour in some patients with buccal lipodystrophy and to treat buccal fat pad pseudoherniation. He recommends an
The eyebrow is so aesthetically important that. Reconstructive
 Original Article Reconstructive Extended Hair-bearing Lateral Orbital Flap for Simultaneous Reconstruction of Eyebrow and Eyelid Shinji Matsuo, MD Ichiro Hashimoto, MD Takuya Seike, MD Yoshiro Abe, MD
Original Article Reconstructive Extended Hair-bearing Lateral Orbital Flap for Simultaneous Reconstruction of Eyebrow and Eyelid Shinji Matsuo, MD Ichiro Hashimoto, MD Takuya Seike, MD Yoshiro Abe, MD
The Role of Muscles in Movement
 The Role of Muscles in Movement Muscles can t push, they can only pull as they contract, so most often body movements are the result of the activity of pairs or teams of muscles acting together or against
The Role of Muscles in Movement Muscles can t push, they can only pull as they contract, so most often body movements are the result of the activity of pairs or teams of muscles acting together or against
CHAPTER 17 FACIAL AESTHETIC SURGERY. Christopher C. Surek, DO and Mohammed S. Alghoul, MD. I. BROW LIFT (Figures 1 and 2)
 CHAPTER 17 FACIAL AESTHETIC SURGERY Christopher C. Surek, DO and Mohammed S. Alghoul, MD I. BROW LIFT (Figures 1 and 2) A. Open Coronal Brow Lift Technique 1. Coronal incision is made in the hair-bearing
CHAPTER 17 FACIAL AESTHETIC SURGERY Christopher C. Surek, DO and Mohammed S. Alghoul, MD I. BROW LIFT (Figures 1 and 2) A. Open Coronal Brow Lift Technique 1. Coronal incision is made in the hair-bearing
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
Muscles of mastication [part 1]
![Muscles of mastication [part 1] Muscles of mastication [part 1]](/thumbs/76/73586850.jpg) Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Use of internal callus distraction in the treatment of congenital brachymetatarsia
 British Journal of Plastic Surgery (2005) 58, 1014 1019 CASE REPORT Use of internal callus distraction in the treatment of congenital brachymetatarsia Naoto Yamada*, Yoshihiro Yasuda, Nobuko Hashimoto,
British Journal of Plastic Surgery (2005) 58, 1014 1019 CASE REPORT Use of internal callus distraction in the treatment of congenital brachymetatarsia Naoto Yamada*, Yoshihiro Yasuda, Nobuko Hashimoto,
Facial Nerve Injury: Diagnosis and Repair
 Editor s Note: My thanks to the moderator, Julia K. Terzis, MD, PhD (board-certified plastic surgeon and ASAPS member, Norfolk, VA); and to panelists Ralph Manktelow, MD (board-certified plastic surgeon,
Editor s Note: My thanks to the moderator, Julia K. Terzis, MD, PhD (board-certified plastic surgeon and ASAPS member, Norfolk, VA); and to panelists Ralph Manktelow, MD (board-certified plastic surgeon,
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Effect of Depressor Septi Resection in Rhinoplasty on Upper Lip Length
 Research Original Investigation Effect of Depressor Septi Resection in Rhinoplasty on Upper Lip Length Yan Ho, MD; Robert Deeb, MD; Richard Westreich, MD; William Lawson, MD, DDS IMPORTANCE Resection of
Research Original Investigation Effect of Depressor Septi Resection in Rhinoplasty on Upper Lip Length Yan Ho, MD; Robert Deeb, MD; Richard Westreich, MD; William Lawson, MD, DDS IMPORTANCE Resection of
Module 6 - The Muscular System Introduction to the Muscular System and Muscles of the Head, Neck and Shoulder
 Module 6 - The Muscular System Introduction to the Muscular System and Muscles of the Head, Neck and Shoulder There will be three modules to cover the muscle anatomy of the body. The first module will
Module 6 - The Muscular System Introduction to the Muscular System and Muscles of the Head, Neck and Shoulder There will be three modules to cover the muscle anatomy of the body. The first module will
SCOPE OF PRACTICE PGY-6 PGY-7 PGY-8
 PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
THIEME. Scalp and Superficial Temporal Region
 CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
Quantitative Determination of
 The Application of 3D Images for Quantitative Determination of Zygoma in an Asian Population Shih-Hsuan Mao, Yu-Hsuan Hsieh, Chih-Hao Chen, Chien-Tzung Chen Department of Plastic and Reconstructive Surgery,
The Application of 3D Images for Quantitative Determination of Zygoma in an Asian Population Shih-Hsuan Mao, Yu-Hsuan Hsieh, Chih-Hao Chen, Chien-Tzung Chen Department of Plastic and Reconstructive Surgery,
This lab activity is aligned with Visible Body s Anatomy and Physiology app. Learn more at visiblebody.com/professors
 1 This lab activity is aligned with Visible Body s Anatomy and Physiology app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES A. Watch the video 13.1 Muscular System Overview and observe
1 This lab activity is aligned with Visible Body s Anatomy and Physiology app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES A. Watch the video 13.1 Muscular System Overview and observe
Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects
 Open Access Original Article DOI: 10.7759/cureus.2356 Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects Rhorie P. Kerr 1, Andrea Hanick 1, Michael A. Fritz 1 1. Head and Neck Institute,
Open Access Original Article DOI: 10.7759/cureus.2356 Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects Rhorie P. Kerr 1, Andrea Hanick 1, Michael A. Fritz 1 1. Head and Neck Institute,
Anatomy & Physiology B. Chapter 6: Muscles
 Anatomy & Physiology B Chapter 6: Muscles Warm-up What are the three types of muscle tissue? Where are each located? Which are voluntary and which are involuntary? Which are striated which are unstriated?
Anatomy & Physiology B Chapter 6: Muscles Warm-up What are the three types of muscle tissue? Where are each located? Which are voluntary and which are involuntary? Which are striated which are unstriated?
Bony hump reduction is an integral part of classic
 Rhinoplasty Nasal Hump Reduction With Powered Micro Saw Osteotomy INTERNATIONAL CONTRIBUTION Yakup Avşar, MD Background: Hump reduction with manual osteotomy is an invasive procedure in aesthetic rhinoplasty.
Rhinoplasty Nasal Hump Reduction With Powered Micro Saw Osteotomy INTERNATIONAL CONTRIBUTION Yakup Avşar, MD Background: Hump reduction with manual osteotomy is an invasive procedure in aesthetic rhinoplasty.
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
The history of face lift surgery encompasses a wide
 Richard Ellenbogen, MD; Anthony Youn, MD; Dan Yamini, MD; and Steven Svehlak, MD Dr. Ellenbogen, Dr. Yamini, and Dr. Svehlak are in private practice in Los Angeles, CA. Dr. Youn is in private practice
Richard Ellenbogen, MD; Anthony Youn, MD; Dan Yamini, MD; and Steven Svehlak, MD Dr. Ellenbogen, Dr. Yamini, and Dr. Svehlak are in private practice in Los Angeles, CA. Dr. Youn is in private practice
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Research report for MSc Dent. University of Witwatersrand. Faculty of health science. Dr J Beukes. Student number: h
 Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Techniques of local anesthesia in the mandible
 Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Interesting Case Series. Virtual Surgical Planning in Orthognathic Surgery
 Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
Disclosures. The Expanding Role of Microvascular Reconstruction. Overview. Things they are a Changing. Surgical Advisory Board, Genentech Corp
 Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Basic Anatomy and Physiology of the Lips and Oral Cavity. Dr. Faghih
 Basic Anatomy and Physiology of the Lips and Oral Cavity Dr. Faghih It is divided into seven specific subsites : 1. Lips 2. dentoalveolar ridges 3. oral tongue 4. retromolar trigone 5. floor of mouth 6.
Basic Anatomy and Physiology of the Lips and Oral Cavity Dr. Faghih It is divided into seven specific subsites : 1. Lips 2. dentoalveolar ridges 3. oral tongue 4. retromolar trigone 5. floor of mouth 6.
Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap.
 Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Features of Facial Asymmetry Following Incomplete Recovery from Facial Paralysis
 Original Article DOI.49/ymj..5.6.94 pissn: 5-5796, eissn: 976-47 Yonsei Med J 5(6):94-948, Features of Facial Asymmetry Following Incomplete Recovery from Facial Paralysis Jin Kim, Hyung Rok Lee, Jun Hui
Original Article DOI.49/ymj..5.6.94 pissn: 5-5796, eissn: 976-47 Yonsei Med J 5(6):94-948, Features of Facial Asymmetry Following Incomplete Recovery from Facial Paralysis Jin Kim, Hyung Rok Lee, Jun Hui
Surgical correction of unilateral and bilateral facial palsy
 562 REVIEW Surgical correction of unilateral and bilateral facial palsy D H Harrison... Unilateral and bilateral facial palsies are debilitating and depressing conditions for the patient. For the past
562 REVIEW Surgical correction of unilateral and bilateral facial palsy D H Harrison... Unilateral and bilateral facial palsies are debilitating and depressing conditions for the patient. For the past
Principles of Facial Reconstruction After Mohs Surgery
 Objectives Principles of Facial Reconstruction After Mohs Surgery Identify important functional anatomy and aesthetic units of the face. Describe techniques used in facial reconstruction. Discuss postoperative
Objectives Principles of Facial Reconstruction After Mohs Surgery Identify important functional anatomy and aesthetic units of the face. Describe techniques used in facial reconstruction. Discuss postoperative
