Kofi D. O. Boahene, MD
|
|
|
- Emma Hardy
- 5 years ago
- Views:
Transcription
1 The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. Contemporary Review Principles and Biomechanics of Muscle Tendon Unit Transfer: Application in Temporalis Muscle Tendon Transposition for Smile Improvement in Facial Paralysis Kofi D. O. Boahene, MD Muscle tendon unit (MTU) transfer is a common procedure performed to restore hand function after peripheral nerve or spinal cord injury. The principles of MTU transfer established for hand surgery can be adopted to optimize the dynamic excursion of the temporalis tendon transfer procedure for facial reanimation. Additionally, the force generating ability of a transferred MTU depends on the ideal length-tension relationship of the donor muscle. There are unclear guideline for selecting the ideal tension at which a transferred MTU will generate maximum force and excursion and current practice often leads to overstretch and suboptimal actin myosin interaction. The use of intraoperative electrical stimulation is an option for determining the ideal tension to optimize excursion of transferred temporalis tendon units in simile restoration. Understanding the biomechanics and principles of MTU and applying it to the temporalis tendon transfer procedure is necessary to improve its use in facial reanimation. Key Words: Temporalis tendon transfer, facial paralysis, Length-tension relationship, biomechanics of muscle tendon unit transfer, principles of muscle tendon transfer. Laryngoscope, 123: , 2013 INTRODUCTION The primary goal in reanimating the paralyzed face is to restore facial tone, symmetry, and dynamic movement that is synergistic and controlled. This is best achieved when the injured facial nerve is directly repaired, grafted, or substituted with other cranial nerves in a timely manner. When re-establishing neural input is not feasible, or when the facial muscles are irreversibly injured or congenitally absent, transfer of functional muscle tendon units (MTUs) offer the potential for restoring some facial tone, symmetry, and motion after a singlestage procedure. In MTU transfer, the tendon of a functioning muscle is detached, mobilized, and then reattached to another tendon or bone to substitute for the action of a nonfunctioning muscle. 1 MTU transfer differs from a free functional muscle transfer such as a gracillis From the Department of Otolaryngology Head and Neck Surgery, Johns Hopkins Institute of Medicine, Baltimore, Maryland, U.S.A. Editor s Note: This Manuscript was accepted for publication June 27, Additional Supporting Information may be found in the online version of this article. The authors have no funding, financial relationships, or conflicts of interest to disclose. Send correspondence to Kofi D. O. Boahene, Department of Otolaryngology Head and Neck Surgery, Johns Hopkins Institute of Medicine, 601 N. Caroline Street, Baltimore MD, dboahen1@jhmi. edu DOI: /lary or the pectoralis minor transfer in that the neurovascular pedicle in MTUs remains uninterrupted. MTU was first developed to restore ambulation in patients suffering from poliomyelitis and was later refined to treat traumatic injuries during the first and second world wars. MTU has been further developed for multiple peripheral nerve paralyses, including median, ulnar, and radial nerve palsies. For example, the flexor carpi ulnaris tendon transfer is a common procedure performed in patients with radial nerve palsy. 2 5 In 1952, McLaughlin introduced the concept and technique of mobilization and transposing the temporalis tendon for facial suspension. 6 The more traditional temporalis muscle transfer later replaced this technique until it was recently reintroduced by several authors. 7 9 Transfer of the digastric muscle tendon for correction of marginal facial nerve branch injury is another example of MTU transfer in the head and neck. 10 Even though newer techniques of functional microvascular transfer of muscles have added new dimensions to facial reanimation, tendon transfer remains a viable option in facial paralysis management. Through the vast experience gained in extremity surgery over the past century, the basic principles for MTU transfer procedures have been established and refined (Table I). 1 Adopting these principles may be helpful in advancing and refining the technique and outcome of MTU in the reanimation of the paralyzed face. The goal of this article was to explore the principles and biomechanics of MTU transfer established for extremity 350
2 TABLE I. The Principles of MTU Transfer. Fundamental principles of MTU transfer The muscle selected as an MTU donor must be expendable and functioning Adequate soft tissue bed for the transfer tendon Full passive range of motion of the involved joints (no fixed deformity) Adequate excursion and length of donor tendon Direct line of pull Suitable insertion technique and firm fixation Synergy of transfer Single function for each transferred tendon MTU ¼ muscle tendon unit. surgery and its application in the temporalis tendon transfer procedure for facial reanimation. PRINCIPLES OF MTU TRANSFER IN EXTREMITY SURGERY Table I outlines the fundamental principles of MTU transfer procedures. Although these principles were developed mainly as a result of experience with MTU in extremity surgery, the basic tenets may be applicable to all types of functional muscle transfer procedures including the temporalis muscle tendon transfer. Selected Donor Muscle Must Be Expendable and Functioning The success of muscle tendon transfer surgery depends on the proper selection of a donor muscle. First, the MTU selected as a potential donor must be expendable in that sacrificing its function should not cause significant morbidity. In the temporalis MTU procedure, the effect of the temporalis muscle on the mandible is completely lost onthesideofthetransfer.thetemporalismuscleworks in conjunction with the masseter muscle to raise the mandible during jaw closure. Clinically, one or both temporalis tendons can be transferred without significant functional deficits. The donor muscle selected for MTU transfer should also be functional. Muscles that have previously lost function and have recovered are not ideal donors for MTU transfer. The function of the temporalis muscle can be tested clinically by observing and palpating for contraction of the muscle in the temple area when the patient is asked to bite down. Intraoperatively, the temporalis muscle can also be stimulated with surface electrodes to detect jaw contractions. Preoperative testing of the temporalis muscle function is particularly important in patients with multiple cranial nerve injuries, M obius syndrome, or a history of previous cranial surgery where the temporalis muscle was divided. Patients who have previously undergone the traditional temporalis muscle transfer procedure may still be good candidates for the temporalis MTU procedure if strong contraction of the remnant muscle can be elicited. Selection of Muscle of Adequate Strength and Excursion When replacing the function of a deficient muscle with that of a donor MTU, the donor muscle should have adequate strength and excursion that is comparable to that of the paralyzed muscle. Choosing a donor muscle with a comparable contraction velocity is also desirable. The strength of a muscle depends on the maximal force it can generate. The maximal force a muscle is capable of producing is proportional to its physiological cross-sectional area and its excursion range to the length of the muscle fibers. 11 The length of the sarcomeres is a major determinant for both force and excursion range. The speed of muscle fiber contraction is largely determined by the heavy chain of the myosin molecule, which in turn determines the muscle type. Muscle fibers are traditionally classified into three groups depending on their physiological behavior. Type I fibers are slow contracting, fatigue resistant, and generate small forces, type IIA fibers are fast contracting, fatigue resistant, and generate larger forces, and type IIB fibers are fast contracting, fatigue resistant, and generate the largest forces. Freilinger et al. distinguished the function of the facial muscles based on the proportion of muscle fiber type. 12 The muscles that attach to the oral commissure for lip elevation (zygomaticus major, levator labii superioris) are intermediate phasic muscles with a mixture or type I and type II fibers suited for sustained tone and fast phasic movement seen in facial expression. The temporalis muscle is made predominantly of type I fibers with about 13% type II fibers. 13 This muscle fiber profile should allow sustained tone to support the paralyzed cheek and lip, and a moderate speed of contraction to elevate the oral commissure during smile. The temporalis muscle has a larger physiologic cross-sectional area than the lip elevators combined and generates significant contraction force during biting and chewing. Suitable Soft Tissue Bed for Transfer For unrestricted tendon movement, the transferred MTU should pass through a healthy soft tissue bed that is free from inflammation, edema, and scar. This is necessary to allow the tendon to glide freely untethered by adhesions and scar. In 1919, Steindler advocated achieving soft-tissue equilibrium, in which edema is resolved, joints are supple, and scars are soft, before proceeding with tendon transfer surgery. 14 In a 1988 article, Brand discussed the mechanical properties of the peritendinous scars that determine the final success of a tendon transfer. 15 When handled meticulously, the buccal space fat pad provides an ideal soft tissue bed for the transposed temporalis tendon. The buccal fat pad fills the masticator space and consists of a main body and four extensions: buccal, pterygoid, superficial, and deep temporal. 16 The deep temporal extension of the buccal fat pad lies directly over the temporalis muscle and its tendon separating it from the zygomatic arch. Disruption of the deep temporal fatpadrisksscaringofthemusclefibersandtendonto zygomatic arch and disruption of its smooth contraction. 351
3 Direct Line of Pull Tendon transfer procedures are most effective when the vector of force is along a straight line. Changing the line of pull will result in a significant loss of force. The anterior fibers of the temporalis muscle are strongly activated during biting and have a vector of pull that compares favorably with the vector of the zygomaticus major. The insertion site of the transposed temporalis tendon should be selected to match the line of contraction of the contralateral zygomaticus major muscle (Fig. 2). Fig. 1. The buccal fat provides a mobile bed through which the transposed temporalis tendon can glide. [Color figure can be viewed in the online issue, which is available at wileyonlinelibrary.com.] The buccal extension of the buccal fat pad passes anterior to the masseter and overlies the buccinator muscle as it courses to the lip musculature. The transposed temporalis tendon passes through the buccal extension to reach the melolabial crease and modiolus. To maintain a gliding path for optimal tendon movement, an adequate cushion of vascularized fat should be preserved on all sides of the tendon (Fig. 1). In addition, early mobilization of the transferred temporalis MTU is important to minimize tendinous adhesions and restrictive scar formation. Full Passive Range of Motion of the Involved Joint (No Fixed Deformity) A tendon transfer procedure will fail if the joint across which the transferred muscle is acting is stiff and immobile. Unlike extremity muscle, the facial muscles do not cross any joints so joint fixation in not applicable. However, for the purpose of smile restoration, oral commissure excursion may be compared to joint movement in extremity MTU. Scars and fibrosis around the lip, chin, and cheek, and additional forces that can oppose the free excursion on the oral commissure, can negatively affect the outcome of the temporalis tendon transfer. When present, these restrictive forces should be actively managed prior to the tendon transfer procedure. Suitable Insertion Technique and Firm Fixation Hand surgeons have recognized the importance of firm tendon fixation techniques in the success of MTU procedures. Factors that have influenced techniques in tendon repair can be summarized by the statement by Strickland, It now seems irrefutable that the most effective method of returning strength and excursion to repaired tendons involves the use of strong, gap resistant suture techniques followed by the frequent application of controlled motion stress. 17 Similar to tendon repair in hand surgery, a firm, stable, and gapresistant fixation of the transposed temporalis tendon to the modiolus is important. In clinical practice, leaving a small piece of the coronoid attached to the temporalis tendon provides a stable platform for anchoring sutures. Holes can also be drilled through the coronoid for firm suture placement. Controlled motion stress in the form of early mobilization has been shown to reduce range of motion loss, increase blood supply, and reduce the degree of muscle atrophy that typically occurs after tendon repair. 18 Early mobilization of the transposed temporalis tendon should be encouraged for the above reasons. Patients can be placed on soft diet for 2 weeks and quickly advanced to actively engage the temporalis muscle in oral commissure excursion. Synergy Synergism occurs when muscles contract simultaneously to augment the effectiveness of each muscle in a given function. The zygomaticus major and levator labii superioris perform synergistic movements to elevate the Fig. 2. A straight line vector of transfer maximizes the effectiveness of the transposed muscle tendon unit. The temporalis tendon should be inserted to match the vector of contraction of the contralateral zygomaticus major muscle. [Color figure can be viewed in the online issue, which is available at wileyonlinelibrary.com.] 352
4 Fig. 3. Length tension curve obtained using human filament lengths and assuming the sliding filament mechanism proposed by Gordon et al. 20 (Top) Schematic of filament lengths. Schematic myofibrillar filament overlaps at three different sarcomere lengths are illustrated along the length tension curve. upper lip and oral commissure during smile. On the contrary, the function of the zygomatic major and depressor anguli oris muscle are not synergistic. Thus, the temporalis MTU procedure should not be combined with a digastric tendon transfer to the oral commissure to mimic the function of the depressor anguli oris, as the new function of the transposed muscles will not be synergistic. Single Function for Each Transferred Tendon The final principle is that a single tendon should be used to restore a single function. Transfer of one muscletendon unit to restore multiple functions will result in compromised strength and movement. This principle is more relevant to hand surgery but applicable in MTU transfers for facial reanimation. As an example, the temporalis muscle has been used to provide dynamic support of the paralyzed eyelids, but combining this procedure with the tendon transfer to the modiolus will be contrary to the above principle and may result in reduced excursion and mass movement. BIOMECHANICS OF MTU TRANSFER Length Tension Relationship and Consequence of Overstretch One critical length tension relationship and consequence of overstretch factor that influences movement around a joint is the force generating ability of the muscle. 19 The biomechanical determinant of active muscle force after transfer is the classic Blix curve that depicts the relationship between active force, passive force, and muscle length. 20 The sarcomere length tension relationship illustrates that active muscle force increases as myofilament overlap increases, and passive muscle force increases as sarcomere length increases (Fig. 3). To achieve maximum force, the MTU must be set at the optimum sarcomere length tension relationship for actin myosin interaction. However, there are no clear intraoperative guidelines in determining the ideal sarcomere length and tension to insert a transferred muscle. Freehafer et al. suggested inserting the MTU as close as possible to its preoperative resting tension. 21 Overstretching of the MTU results in low-active force generation. Thus, although it is commonly believed that inserting a muscle in the stretched position may be beneficial because the repair site may slip or stress-relax, it would be unwise to rely on this unknown factor to optimize an overstretched transfer. 22 The routine practice of overcorrection to make up for anticipated slippage or stress relaxation may result in overstress and suboptimal excursion. 22 In hand MTU surgery, intraoperative sarcomere length measurements using laser diffraction have been shown to be a valuable tool for setting correct tension for tendon transfers. 23 To determine an optimal length tension of the transpose temporalis tendon, the temporalis muscle can be stimulated intraoperatively once the tendon has been released. Varying the tension exerted on the tendon while stimulating the muscle can help determine the ideal length for insertion (supporting video). The stimulator should provide a biphasic current of approximately 20 ma at 20 Hz with variable pulse width. Pulse widths of 100 to 200 ms applied to the neuromuscular junction generally maximize the contraction of the muscle. In the majority of cases, the temporalis tendon can be mobilized to reach the melolabial crease and oral commissure and inserted slightly over the passive length. In cases of inadequate tendon length, overstretch can be avoided by using a tendon extension. The effect of tendon extension on muscle force was studied by Brunner. 24 If functional length changes, a muscle adapts by altering the number of sarcomeres in a series. If the tendon is elongated without changing the functional range of motion at which the muscle is active on the joint, the passive tension is decreased. As a result, the number of sarcomeres in a series is reduced. The muscle produces less force and the range of active force production is narrowed. If by elongating the tendon, however, the functional range of motion of the muscle at the joint is moved and the tension remains unchanged, the muscle force can be preserved. Therefore, during an MTU procedure, judging the optimal tension for insertion to maintain functional range of motion becomes even more important in the temporalis tendon transfer procedure when a tendon extender is used. To gain tendon reach to the melolabial fold, Labbe described the temporalis tendon lengthening myoplasty procedure. 7 In his original description, the temporalis muscle is exposed through a scalp incision, and the posterior third of the muscle is released and elevated from its periosteal attachment. By sliding the released muscle inferiorly, the muscle fibers are redistributed and fixated inferiorly, thereby allowing the released coronoid with the attached temporalis tendon to reach the lip. When 353
5 Moment Arm The moment arm of a tendon transfer is an important biomechanical determinant of how much movement will occur. 15 The moment arm is a product of the force generated by the muscle and the perpendicular distance of its line of action from the axis of rotation (Fig. 4). The force generated by the muscle is dependent on the physiologic cross-sectional area of the donor muscle. The moment arm can be surgically varied depending on how far away the tendon is inserted from the axis of rotation. The closer the tendon line of action is to the axis of rotation, the smaller the moment arm but more muscle excursion and axis motion is achieved. Conversely, the larger the moment arm, the smaller the excursion. Because the facial mimetic muscles do not work across any joints, the relevance of moment arms in the temporalis MTU is not immediately apparent (Fig. 4). Nonetheless, this principle holds some value in the design of the temporalis MTU procedure. It is the author s clinical experience that the further away from the oral commissure along the melolabial crease the temporalis tendon is inserted (higher moment arm), the less effective excursion for smile restoration is realized. Fig. 4. The relationship between a muscle s moment arm and excursion is an important biomechanical factor to consider in the design of the muscle tendon unit. The length of a muscle s moment arm affects the excursion that results from a contraction. The further away the tendon is inserted (AC > AB) from the line of action (A), the higher the moment arm. Movement through an angle requires more contraction and shortening in a muscle with a long moment arm than in a muscle with a short moment arm. Tendons inserted closer to the oral commissure are more effective in commissure excursion. [Color figure can be viewed in the online issue, which is available at wileyonlinelibrary.com.] releasing the temporalis muscle, care should be taken to avoid injury to the neurovascular supply deep to the muscle. In addition, the released muscle should be refixated at the appropriate tension. 354 TIMING AND INDICATION FOR TEMPORALIS TENDON TRANSFER In 1974, Burkhalter reported the indications for MTU in extremity injury that are applicable to the temporalis tendon transfer. 25 These were: 1) the transfer can act as a substitute during regrowth of the nerve, which will thereby reduce the time of function loss; 2) the transfer can act as a helper and add power to normal reinnervated muscle function; and 3) the transfer can act as a substitute when, statistically, the recovery after neurorrhaphy or nerve repair is poor. When presented with facial paralysis, the clinician should make the determination if the paralysis is reversible. Reversible paralysis is that which may recover spontaneously (Seddon grade 1 or 2) or with intervention directed toward the nerve. Timely nerve grafting or nerve substitution to reinnervate a reversibly deinervated facial muscle yields superior results to muscle tendon procedures. Electromyography studies in combination with clinical history can help establish the reversibility of the paralyzed facial muscle. In cases were the repaired nerve is expected to recover partially or may take long to yield significant results, the temporalis MTU procedure can be performed as an adjunct while waiting for regrowth of the nerve, thereby reducing the time of function loss. A typical example is a patient who after a radical parotidectomy where the nerve was resected is also scheduled to undergo postoperative radiotherapy. Although the facial nerve is grafted, a temporalis MTU can be performed at the same time to provide lower facial support. In such situations, care should be taken to avoid disrupting the facial nerve branches during the MTU procedure. The temporalis MTU transfer procedure can also be considered as an option to upgrade partial facial paralysis that is either congenital or acquired. PHYSIOTHERAPY Muscle-retraining exercises are essential in optimizing the outcome of any muscle training procedure. In
6 the preoperative period, patients visit a physical therapist who plans out specific exercises to strengthen the temporalis muscle and to identify isolated jaw movements that will be essential in contracting the temporalis muscle. Patients should be motivated to direct their rehabilitation. After the first 2 postoperative weeks, active mobilization of the transposed temporalis MTU should be initiated. This should be followed by muscle strengthening exercises. The main goal of the therapy is to systematically rehabilitate smiling function by transferring labial and jugal functions to the transferred temporal muscle. Lambert-Prou describes several phases of therapy to acquire a temporal smile. 26 The first phase, termed the mandibular smile, involves mobilization of the mandible by contraction of the transferred temporalis muscle and inducing an elevation of the commissura labiorum. The second phase, the voluntary temporal smile, is attained by contracting of the temporal is muscle without mandibular movement, which remains under voluntary control. The smile produced should become as symmetrical as possible. Finally, the last phase focuses on achieving a spontaneous smile independent of mandibular movement, the spontaneous temporal smile. Temporal contraction should produce a real expressive smile and good-quality articulate speech, saliva evacuation, and labial junction. Biofeedback methods are helpful in this process. The role of electrical stimulation is unclear. As demonstrated by Coulson and colleagues, repeated exercises and practice with the aid of video feedback loops of the best symmetric smile can be powerful tools to achieve a spontaneous smile adapted for social settings. 27 CONCLUSION Several factors are essential for the success of tendon transfers procedures. Based on an understanding of muscle physiology and biomechanics of muscle contraction, many of principles of MTU transfer in extremity surgery can be applied to the temporalis tendon unit transfer for facial reanimation. Although adhering to these principles does not guarantee success, ignoring them invites failure. Intraoperative assessment with electrical stimulation or more sophisticated tools to determine the ideal tension length of the MTU is necessary to improve the outcome of the temporalis MTU transfer surgery in smile restoration. BIBLIOGRAPHY 1. Bell LD. Transplantation of tendon. In: Reconstructive and Plastic Surgery. Vol Green DP. Radial nerve palsy. In: Green DP, Hotchkiss RN, Pederson WC, eds. Green s Operative Hand Surgery. Vol. 2. 4th ed. New York, NY: Churchill Livingstone; 1999: Scuderi C. Tendon transfers for irreparable radial nerve paralysis. Surg Gynecol Obstet 1949;88: Richards RR. Tendon transfers for failed nerve reconstruction. In: Mackinnon SE, ed. Clinics in Plastic Surgery: Peripheral Nerve Surgery. Vol. 30. Philadelphia, PA: Saunders; 2003: Jones NF, Machado GR. Tendon transfers for radial, median, and ulnar nerve injuries: current surgical techniques. Clin Plast Surg 2011;38: McLaughlin CR. Surgical support in permanent facial paralysis. Plast Reconst Surg 1953;11: Labbe D, Huault M. Lengthening temporalis myoplasty and lip reanimation. Plast Reconstr Surg 2000;105: Croxson GR, Quinn MJ, Coulson SE. Temporalis muscle transfer for facial paralysis: a further refinement. Facial Plast Surg 2000;16: Boahene KD, Farrag TY, Ishii L, Byrne PJ. Minimally invasive temporalis tendon transposition. Arch Facial Plast Surg 2011;13: Tan ST. Anterior belly of digastric muscle transfer: a useful technique in head and neck surgery. Head Neck 2002;24: Lieber RL. Skeletal muscle architecture implications for muscle function and surgical tendon transfer. J Hand Ther 1993;6: Freilinger G, Happak W, Burggasser G, Gruber H. Histochemical mapping and fiber size analysis of mimic muscles. Plast Reconstr Surg 1990;86: Korfage JAM, Van Eijden TMGJ. Regional differences in fibre type composition in the human temporalis muscle. J Anat 1999;194(pt 3): Steindler A. Operative treatment of paralytic conditions of the upper extremities. J Orthop Surg 1919;1: Brand PW. Biomechanics of tendon transfers. Hand Clin 1988;4: Stuzin JM, Wagstrom L, Kawamoto HK, Baker TJ, Wolfe SA. The anatomy and clinical applications of the buccal fat pad. Plast Reconstr Surg 1990;85: Strickland JW, ed. The Hand: Master Techniques in Orthopaedic Surgery. Philadelphia, PA: Lippincott-Raven; Pneumaticos SG, Phd PCN, McGarvey WC, Mody DR, Trevino SG. The effects of early mobilization in the healing of achilles tendon repair. Foot Ankle Int 2000;21: Brand PW, Beach RB, Thompson DE. Relative tension and potential excursion of muscles in the forearm and hand. J Hand Surg 1981;3A: Gordon AM, Huxley AF, Julian FJ. The variation in isometric tension with sarcomere length in vertebrate muscle fibers. J Physiol (London) 1966; 184: Freehafer AA, Peckham HP, Keith MW. Determination of muscle tendon unit properties during tendon transfer. J Hand Surg Am 1979;4: Friden J, Lieber RL. Mechanical considerations in the design of surgical reconstructive procedures. J Biomech 2002;35: Friden J, Lieber RL. Evidence for muscle attachment at relatively long lengths in tendon transfer surgery. J Hand Surg 1998;23A: Brunner R. Changes in muscle power following tendon lengthening and tendon transfer [in German]. Orthopade 1995;24: Burkhalter WE. Early tendon transfer in upper extremity peripheral nerve injury. Clin Orthop Relat Res 1974;(104): Lambert-Prou MP. The temporal smile. Speech therapy for facial palsy patients after temporal lengthening myoplasty [in French]. Rev Stomatol Chir Maxillofac 2003;104: Coulson SE, Adams RD, O Dwyer NJ, Croxson GR. Physiotherapy rehabilitation of the smile after long-term facial nerve palsy using video selfmodeling and implementation intentions. Otolaryngol Head Neck Surg 2006;134:
This lab activity is aligned with Visible Body s Anatomy and Physiology app. Learn more at visiblebody.com/professors
 1 This lab activity is aligned with Visible Body s Anatomy and Physiology app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES A. Watch the video 13.1 Muscular System Overview and observe
1 This lab activity is aligned with Visible Body s Anatomy and Physiology app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES A. Watch the video 13.1 Muscular System Overview and observe
Lower Facial Reanimation Techniques Following Cancer Resection and Free Flap Reconstruction
 The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Lower Facial Reanimation Techniques Following Cancer Resection and Free Flap Reconstruction Alexandra E.
The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Lower Facial Reanimation Techniques Following Cancer Resection and Free Flap Reconstruction Alexandra E.
Dynamic Facial Reanimation With Orthodromic Temporalis Tendon Transfer in Children
 Research Case Report/Case Series Dynamic Facial Reanimation With Orthodromic Temporalis Tendon Transfer in Children Rajanya S. Petersson, MD; Daniel E. Sampson, MD; James D. Sidman, MD IMPORTNCE To our
Research Case Report/Case Series Dynamic Facial Reanimation With Orthodromic Temporalis Tendon Transfer in Children Rajanya S. Petersson, MD; Daniel E. Sampson, MD; James D. Sidman, MD IMPORTNCE To our
Endoscopic Approach for Lengthening the Temporalis Muscle
 Ideas and Innovations Endoscopic Approach for Lengthening the Temporalis Muscle Rubén Contreras-García, M.D., Pedro D. Martins, M.D., and Jefferson Braga-Silva, M.D., Ph.D. Porto Alegre, Brazil The temporalis
Ideas and Innovations Endoscopic Approach for Lengthening the Temporalis Muscle Rubén Contreras-García, M.D., Pedro D. Martins, M.D., and Jefferson Braga-Silva, M.D., Ph.D. Porto Alegre, Brazil The temporalis
Rehabilitation of the Paralyzed Face
 Rehabilitation of the Paralyzed Face Elizabeth J. Rosen, MD Faculty Advisor: Karen H. Calhoun, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation October 30,
Rehabilitation of the Paralyzed Face Elizabeth J. Rosen, MD Faculty Advisor: Karen H. Calhoun, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation October 30,
Muscle Weakness Or Paralysis With Compromise Of Peripheral Nerve
 Muscle Weakness Or Paralysis With Compromise Of Peripheral Nerve Muscle weakness or complete paralysis may be secondary to an interruption in the communication between the brain and nerve cells in the
Muscle Weakness Or Paralysis With Compromise Of Peripheral Nerve Muscle weakness or complete paralysis may be secondary to an interruption in the communication between the brain and nerve cells in the
Bone Practical. Labs Muscle Labs. Final Practical. Divisions of the Muscular System. Quiz format
 Bone Practical Labs 17 + 18 Muscles Wed 7/11 @ 8am 40 50 stations About half axial, half appendicular bones Disarticulated bones: Skulls, partial skulls, vertebrae, ribs, skeletons, arm bones, leg bones,
Bone Practical Labs 17 + 18 Muscles Wed 7/11 @ 8am 40 50 stations About half axial, half appendicular bones Disarticulated bones: Skulls, partial skulls, vertebrae, ribs, skeletons, arm bones, leg bones,
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY NASOLABIAL FLAP FOR ORAL CAVITY RECONSTRUCTION Harry Wright, Scott Stephan, James Netterville Designed as a true myocutaneous flap pedicled
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY NASOLABIAL FLAP FOR ORAL CAVITY RECONSTRUCTION Harry Wright, Scott Stephan, James Netterville Designed as a true myocutaneous flap pedicled
3. The Jaw and Related Structures
 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
The Role of Muscles in Movement
 The Role of Muscles in Movement Muscles can t push, they can only pull as they contract, so most often body movements are the result of the activity of pairs or teams of muscles acting together or against
The Role of Muscles in Movement Muscles can t push, they can only pull as they contract, so most often body movements are the result of the activity of pairs or teams of muscles acting together or against
Comparison of one-stage free gracilis muscle flap with two-stage method in chronic facial palsy*
 Original Research Medical Journal of the Islamic Republic of Iran.Vol. 21, No.2, August 2007. pp. 63-70 Comparison of one-stage free gracilis muscle flap with two-stage method in chronic facial palsy*
Original Research Medical Journal of the Islamic Republic of Iran.Vol. 21, No.2, August 2007. pp. 63-70 Comparison of one-stage free gracilis muscle flap with two-stage method in chronic facial palsy*
Assignment 4: Muscle Structure and Function
 Assignment 4: Muscle Structure and Function Unit 2: Chapter 5 Part A Multiple Choice Questions 1. Which of the following statements about skeletal muscle is true: A) Skeletal muscles are usually linked
Assignment 4: Muscle Structure and Function Unit 2: Chapter 5 Part A Multiple Choice Questions 1. Which of the following statements about skeletal muscle is true: A) Skeletal muscles are usually linked
Oral cavity landmarks
 By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
Head and Face Anatomy
 Head and Face Anatomy Epicranial region The Scalp The soft tissue that covers the vault of skull. Extends from supraorbital margin to superior nuchal line. Layers of the scalp S C A L P = skin = connective
Head and Face Anatomy Epicranial region The Scalp The soft tissue that covers the vault of skull. Extends from supraorbital margin to superior nuchal line. Layers of the scalp S C A L P = skin = connective
Musculoskeletal System. Terms. Origin (Proximal Attachment) Insertion (Distal Attachment)
 Musculoskeletal System Terms Origin (Proximal Attachment) Insertion (Distal Attachment) Agonist- prime mover Antagonist- provides a braking force Synergist- assists indirectly in the movement Musculoskeletal
Musculoskeletal System Terms Origin (Proximal Attachment) Insertion (Distal Attachment) Agonist- prime mover Antagonist- provides a braking force Synergist- assists indirectly in the movement Musculoskeletal
1) A motor neuron and all the muscle cells that it stimulates are referred to as a motor end plate. 1)
 Chapter 6: Muscular System Test Study Guide CP Anatomy Mrs. Puzon Name TRUE/FALSE. Write 'T' if the statement is true and 'F' if the statement is false. Please mark "A" for True and "B" for false on your
Chapter 6: Muscular System Test Study Guide CP Anatomy Mrs. Puzon Name TRUE/FALSE. Write 'T' if the statement is true and 'F' if the statement is false. Please mark "A" for True and "B" for false on your
THE pedicled flap, commonly used by the plastic surgeon in the reconstruction
 THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS. By B. GRUNDT, M.D. Oslo, Norway
 SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS By B. GRUNDT, M.D. Oslo, Norway WE are all familiar with the patient who has paralysis of the facial nerve. The oblique mouth and the corresponding oblique
SURGICAL TREATMENT OF SEVENTH NERVE PARALYSIS By B. GRUNDT, M.D. Oslo, Norway WE are all familiar with the patient who has paralysis of the facial nerve. The oblique mouth and the corresponding oblique
Lectures Muscular System 10-1
 Lectures 12-14 Muscular System 10-1 Properties of Muscle Ability of a muscle to shorten with force Capacity of muscle to respond to a stimulus Muscle can be stretched to its normal resting length and beyond
Lectures 12-14 Muscular System 10-1 Properties of Muscle Ability of a muscle to shorten with force Capacity of muscle to respond to a stimulus Muscle can be stretched to its normal resting length and beyond
Restoring Range of Motion and Improving Flexibility.
 Restoring Range of Motion and Improving Flexibility www.fisiokinesiterapia.biz Importance of Flexibility Important Goal: Restore or improve to normal pre-injury range of motion With injury there is generally
Restoring Range of Motion and Improving Flexibility www.fisiokinesiterapia.biz Importance of Flexibility Important Goal: Restore or improve to normal pre-injury range of motion With injury there is generally
EVALUATION AND MEASUREMENTS. I. Devreux
 EVALUATION AND MEASUREMENTS I. Devreux To determine the extent and degree of muscular weakness resulting from disease, injury or disuse. The records obtained from these tests provide a base for planning
EVALUATION AND MEASUREMENTS I. Devreux To determine the extent and degree of muscular weakness resulting from disease, injury or disuse. The records obtained from these tests provide a base for planning
Oral incompetence following composite reconstruction
 IDEAS AND INNOVATIONS Lower Lip Suspension Using Bilateral Temporalis Muscle Flaps and Fascia Lata Grafts Rodney K. Chan, M.D. Branko Bojovic, M.D. Simon G. Talbot, M.D. Denton Weiss, M.D. Julian J. Pribaz,
IDEAS AND INNOVATIONS Lower Lip Suspension Using Bilateral Temporalis Muscle Flaps and Fascia Lata Grafts Rodney K. Chan, M.D. Branko Bojovic, M.D. Simon G. Talbot, M.D. Denton Weiss, M.D. Julian J. Pribaz,
Reversing PIP Joint Contractures:
 Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System John M. Agee M.D. Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System
Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System John M. Agee M.D. Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System
Strattice Reconstructive Tissue Matrix used in the repair of rippling
 Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure
 Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
The Biomechanics of Human Skeletal Muscle
 AML2506 Biomechanics and Flow Simulation Day 03B The Biomechanics of Human Skeletal Muscle Session Speaker Dr. M. D. Deshpande 1 Session Objectives At the end of this session the delegate would have understood
AML2506 Biomechanics and Flow Simulation Day 03B The Biomechanics of Human Skeletal Muscle Session Speaker Dr. M. D. Deshpande 1 Session Objectives At the end of this session the delegate would have understood
Principles of Facial Reconstruction After Mohs Surgery
 Objectives Principles of Facial Reconstruction After Mohs Surgery Identify important functional anatomy and aesthetic units of the face. Describe techniques used in facial reconstruction. Discuss postoperative
Objectives Principles of Facial Reconstruction After Mohs Surgery Identify important functional anatomy and aesthetic units of the face. Describe techniques used in facial reconstruction. Discuss postoperative
The Human Muscular System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5th ed (2017) Chapters 10, 11, 12 INTRODUCTION
 Biology 322: Human Anatomy The Human Muscular System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapters 10, 11, 12 INTRODUCTION We will use a number of lab periods
Biology 322: Human Anatomy The Human Muscular System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapters 10, 11, 12 INTRODUCTION We will use a number of lab periods
The muscular system I Muscles of the head neck and trunk
 The muscular system I Muscles of the head neck and trunk Dr. Nabil Khouri Dr. Nabil Khouri MD MSc, PhD Interactions of Skeletal Muscles Skeletal muscles work together or in opposition Muscles only pull
The muscular system I Muscles of the head neck and trunk Dr. Nabil Khouri Dr. Nabil Khouri MD MSc, PhD Interactions of Skeletal Muscles Skeletal muscles work together or in opposition Muscles only pull
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Essentials of Human Anatomy & Physiology. The Muscular System
 Essentials of Human Anatomy & Physiology The Muscular System The Muscular System Muscles are responsible for all types of body movement they contract or shorten and are the machine of the body Three basic
Essentials of Human Anatomy & Physiology The Muscular System The Muscular System Muscles are responsible for all types of body movement they contract or shorten and are the machine of the body Three basic
CHAPTER 11 FACIAL PARALYSIS. Shailesh Agarwal, MD and Arash Momeni, MD
 CHAPTER 11 FACIAL PARALYSIS Shailesh Agarwal, MD and Arash Momeni, MD The facial nerve innervates a total of 23 paired muscles and the orbicularis oris muscle. The majority of muscles innervated by the
CHAPTER 11 FACIAL PARALYSIS Shailesh Agarwal, MD and Arash Momeni, MD The facial nerve innervates a total of 23 paired muscles and the orbicularis oris muscle. The majority of muscles innervated by the
3-Deep fascia: is absent (except over the parotid gland & buccopharngeal fascia covering the buccinator muscle)
 The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
Muscle Function: Understanding the Unique Characteristics of Muscle. Three types of muscle. Muscle Structure. Cardiac muscle.
 : Understanding the Unique Characteristics of Muscle Scott Riewald United States Olympic Committee Three types of muscle Cardiac muscle Involuntary Smooth muscle Involuntary Skeletal muscle Voluntary Involuntary
: Understanding the Unique Characteristics of Muscle Scott Riewald United States Olympic Committee Three types of muscle Cardiac muscle Involuntary Smooth muscle Involuntary Skeletal muscle Voluntary Involuntary
Chapter 20: Muscular Fitness and Assessment
 Chapter 20: Muscular Fitness and Assessment American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York: Lippincott, Williams
Chapter 20: Muscular Fitness and Assessment American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York: Lippincott, Williams
Skeletal Muscle. Cardiac Muscle. Smooth Muscle. II. Muscular System. The Muscular System
 Chapter CHAPTER 8 8 The Muscular System College Prep NOTES Smooth Muscle Found in body organs,vessels, respiratory passages Not striated, tapered, single cell nucleus involuntary, peristaltic contractions
Chapter CHAPTER 8 8 The Muscular System College Prep NOTES Smooth Muscle Found in body organs,vessels, respiratory passages Not striated, tapered, single cell nucleus involuntary, peristaltic contractions
Muscle Tissue- 3 Types
 AN INTRODUCTION TO MUSCLE TISSUE Muscle Tissue- 3 Types Skeletal muscle (focus on these) Cardiac muscle Smooth muscle FUNCTIONS OF SKELETAL MUSCLES Produce movement of the skeleton Maintain posture and
AN INTRODUCTION TO MUSCLE TISSUE Muscle Tissue- 3 Types Skeletal muscle (focus on these) Cardiac muscle Smooth muscle FUNCTIONS OF SKELETAL MUSCLES Produce movement of the skeleton Maintain posture and
Human Anatomy and Physiology - Problem Drill 09: The Muscular System
 Human Anatomy and Physiology - Problem Drill 09: The Muscular System Question No. 1 of 10 The muscular system of the human body fulfills many different roles. Which of the following statements about the
Human Anatomy and Physiology - Problem Drill 09: The Muscular System Question No. 1 of 10 The muscular system of the human body fulfills many different roles. Which of the following statements about the
Muscles Unit TEST and Final Exam Study Guide May 2017
 Muscles Unit TEST and Final Exam Study Guide May 2017 Part 1 of final exam is pictures, see bottom of the study guide Part 2 of the final exam is only going to cover muscles unit. If you do this study
Muscles Unit TEST and Final Exam Study Guide May 2017 Part 1 of final exam is pictures, see bottom of the study guide Part 2 of the final exam is only going to cover muscles unit. If you do this study
The International Journal of Periodontics & Restorative Dentistry
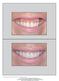 The International Journal of Periodontics & Restorative Dentistry 433 Lip Repositioning for Reduction of Excessive Gingival Display: A Clinical Report Ari Rosenblatt, DMD, DDS* Ziv Simon, DMD, MSc* Excessive
The International Journal of Periodontics & Restorative Dentistry 433 Lip Repositioning for Reduction of Excessive Gingival Display: A Clinical Report Ari Rosenblatt, DMD, DDS* Ziv Simon, DMD, MSc* Excessive
Module 6 - The Muscular System Introduction to the Muscular System and Muscles of the Head, Neck and Shoulder
 Module 6 - The Muscular System Introduction to the Muscular System and Muscles of the Head, Neck and Shoulder There will be three modules to cover the muscle anatomy of the body. The first module will
Module 6 - The Muscular System Introduction to the Muscular System and Muscles of the Head, Neck and Shoulder There will be three modules to cover the muscle anatomy of the body. The first module will
Skeletal Muscle. Smooth Muscle. Cardiac Muscle. I. 3 Types of Muscle Tissue. 1. Smooth 2. Cardiac 3. Skeletal
 I. 3 Types of Muscle Tissue 1. Smooth 2. Cardiac 3. Skeletal Smooth Muscle Found in body organs,vessels, respiratory passages Not striated, tapered, single cell nucleus involuntary, peristaltic contractions
I. 3 Types of Muscle Tissue 1. Smooth 2. Cardiac 3. Skeletal Smooth Muscle Found in body organs,vessels, respiratory passages Not striated, tapered, single cell nucleus involuntary, peristaltic contractions
RECONSTRUCTIVE.
 RECONSTRUCTIVE Intraoperative Muscle Electrical Stimulation for Accurate Positioning of the Temporalis Muscle Tendon during Dynamic, One-Stage Lengthening Temporalis Myoplasty for Facial and Lip Reanimation
RECONSTRUCTIVE Intraoperative Muscle Electrical Stimulation for Accurate Positioning of the Temporalis Muscle Tendon during Dynamic, One-Stage Lengthening Temporalis Myoplasty for Facial and Lip Reanimation
Improving Muscular Strength and Endurance
 Improving Muscular Strength and Endurance Introduction Outline Structure of Skeletal Muscle How Skeletal Muscle Contracts Motor Neurons Actin and Myosin Types of Contractions Muscle Fiber Types Determinants
Improving Muscular Strength and Endurance Introduction Outline Structure of Skeletal Muscle How Skeletal Muscle Contracts Motor Neurons Actin and Myosin Types of Contractions Muscle Fiber Types Determinants
Anatomy & Physiology B. Chapter 6: Muscles
 Anatomy & Physiology B Chapter 6: Muscles Warm-up What are the three types of muscle tissue? Where are each located? Which are voluntary and which are involuntary? Which are striated which are unstriated?
Anatomy & Physiology B Chapter 6: Muscles Warm-up What are the three types of muscle tissue? Where are each located? Which are voluntary and which are involuntary? Which are striated which are unstriated?
Module 15: Stretching Fitness
 Module 15: Stretching Fitness In this module you will learn: The importance of warming up and stretching before exercising What happens to your muscles while stretching How to stretch without causing injury
Module 15: Stretching Fitness In this module you will learn: The importance of warming up and stretching before exercising What happens to your muscles while stretching How to stretch without causing injury
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
cally, a distinct superior crease of the forehead marks this spot. The hairline and
 4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
Grading Facial Nerve Function Following Combined Static and Mimetic Surgical Techniques
 416 Original Article Grading Facial Nerve Function Following Combined Static and Mimetic Surgical Techniques John P. Leonetti 1 Sam J. Marzo 1 Douglas A. Anderson 2 Joshua M. Sappington 1 1 Department
416 Original Article Grading Facial Nerve Function Following Combined Static and Mimetic Surgical Techniques John P. Leonetti 1 Sam J. Marzo 1 Douglas A. Anderson 2 Joshua M. Sappington 1 1 Department
NOTES MUSCULAR SYSTEM
 NOTES for the MUSCULAR SYSTEM Anatomy & Physiology 2016 Johnson I. Muscular System A. Specialized tissue that does one thing: shorten. B. Functions: 1. Movement (of body, blood, food, etc.). 2. Stabilize
NOTES for the MUSCULAR SYSTEM Anatomy & Physiology 2016 Johnson I. Muscular System A. Specialized tissue that does one thing: shorten. B. Functions: 1. Movement (of body, blood, food, etc.). 2. Stabilize
Muscles of the Face, Head, and Neck
 Muscles of the Face, Head, and Neck 1 How Muscles Are Named Many muscles named using such features as Location Function Shape Direction of fibers Number of heads or divisions Points of attachment Size
Muscles of the Face, Head, and Neck 1 How Muscles Are Named Many muscles named using such features as Location Function Shape Direction of fibers Number of heads or divisions Points of attachment Size
SPASTICITY CAUSES A FUNDAMENTAL REARRANGEMENT OF MUSCLE JOINT INTERACTION
 ABSTRACT: Sarcomere length was measured in flexor carpi ulnaris (FCU) muscles from patients with severely spastic wrist flexion contractures (n = 6), as well as from patients with radial nerve injury and
ABSTRACT: Sarcomere length was measured in flexor carpi ulnaris (FCU) muscles from patients with severely spastic wrist flexion contractures (n = 6), as well as from patients with radial nerve injury and
10/4/18. Muscular System. 1 Copyright 2016 by Elsevier Inc. All rights reserved. Introduction. Anatomy. Physiology. Skeletal Muscle Anatomy
 Introduction Muscular System Chapter 20 Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
Introduction Muscular System Chapter 20 Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
The Subzygomatic Triangle: Rapid, minimally invasive identification of the masseteric nerve for facial ACCEPTED
 Plastic and Reconstructive Surgery Advance Online Article DOI: 10.1097/PRS.0b013e318290f6dc The Subzygomatic Triangle: Rapid, minimally invasive identification of the masseteric nerve for facial reanimation
Plastic and Reconstructive Surgery Advance Online Article DOI: 10.1097/PRS.0b013e318290f6dc The Subzygomatic Triangle: Rapid, minimally invasive identification of the masseteric nerve for facial reanimation
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
Test Bank for The Human Body in Health and Illness 4th Edition by Herlihy
 Test Bank for The Human Body in Health and Illness 4th Edition by Herlihy Chapter 9: Muscular System Test Bank MULTIPLE CHOICE 1. Which of the following muscles is described as striated and involuntary?
Test Bank for The Human Body in Health and Illness 4th Edition by Herlihy Chapter 9: Muscular System Test Bank MULTIPLE CHOICE 1. Which of the following muscles is described as striated and involuntary?
7/10/18. Introduction. Muscular System. Anatomy. Physiology. Skeletal Muscle Anatomy. Muscle Fiber
 Introduction Muscular System Chapter 20 Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
Introduction Muscular System Chapter 20 Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
SOFT TISSUE SUPPORT IS AN
 ORIGINAL ARTICLE Reconstructive Application of the Endotine Suspension Devices James H. Boehmler IV, MD; Benjamin L. Judson, MD; Steven P. Davison, MD, DDS Objective: To illustrate the potential reconstructive
ORIGINAL ARTICLE Reconstructive Application of the Endotine Suspension Devices James H. Boehmler IV, MD; Benjamin L. Judson, MD; Steven P. Davison, MD, DDS Objective: To illustrate the potential reconstructive
Unit 4: The Muscular System REVIEW GUIDE
 NPHS Anatomy & Physiology Questions to answer: 1) List the three functions of the muscular system. Unit 4: The Muscular System REVIEW GUIDE 2) What are the four characteristics of muscle tissue? Briefly
NPHS Anatomy & Physiology Questions to answer: 1) List the three functions of the muscular system. Unit 4: The Muscular System REVIEW GUIDE 2) What are the four characteristics of muscle tissue? Briefly
Autologous Fat Augmentation of the Vocal Folds
 Tokai J Exp Clin Med., Vol. 39, No. 3, pp. 146-150, 2014 Autologous Fat Augmentation of the Vocal Folds Shinya OKADA *1, Etsuyo TAMURA *2 and Masahiro IIDA *3 *1 Department of Otorhinolaryngology, Tokai
Tokai J Exp Clin Med., Vol. 39, No. 3, pp. 146-150, 2014 Autologous Fat Augmentation of the Vocal Folds Shinya OKADA *1, Etsuyo TAMURA *2 and Masahiro IIDA *3 *1 Department of Otorhinolaryngology, Tokai
Muscles of mastication [part 1]
![Muscles of mastication [part 1] Muscles of mastication [part 1]](/thumbs/76/73586850.jpg) Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Intraoperative Single-Site Sarcomere Length Measurement Accurately Reflects Whole-Muscle Sarcomere Length in the Rabbit
 Intraoperative Single-Site Sarcomere Length Measurement Accurately Reflects Whole-Muscle Sarcomere Length in the Rabbit Mitsuhiko Takahashi, MD, Samuel R. Ward, PhD, Richard L. Lieber, PhD From the Departments
Intraoperative Single-Site Sarcomere Length Measurement Accurately Reflects Whole-Muscle Sarcomere Length in the Rabbit Mitsuhiko Takahashi, MD, Samuel R. Ward, PhD, Richard L. Lieber, PhD From the Departments
The Muscular System PART C. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Muscular System 6 PART C Five Golden Rules of Skeletal Muscle Activity Table 6.2 Muscles and Body
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Muscular System 6 PART C Five Golden Rules of Skeletal Muscle Activity Table 6.2 Muscles and Body
Energy for Muscle Contractions: Direct phosphorylation. Creatine phosphate loses a phosphate to ADP to create ATP
 Energy for Muscle Contractions: Direct phosphorylation Aerobic respiration Anaerobic respiration (lactic acid fermentation) Creatine phosphate loses a phosphate to ADP to create ATP Requires oxygen to
Energy for Muscle Contractions: Direct phosphorylation Aerobic respiration Anaerobic respiration (lactic acid fermentation) Creatine phosphate loses a phosphate to ADP to create ATP Requires oxygen to
Interesting Case Series. Reconstruction of Dorsal Wrist Defects
 Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Chapter 9. The Muscular System
 1 Chapter 9 The Muscular System 2 Introduction Skeletal muscles: movement in environment Smooth muscles: intestines, ureters, veins and arteries Cardiac muscle: pumps blood through heart and blood vessels
1 Chapter 9 The Muscular System 2 Introduction Skeletal muscles: movement in environment Smooth muscles: intestines, ureters, veins and arteries Cardiac muscle: pumps blood through heart and blood vessels
The Scalp and Face Protocol. Julie Goodwin, BA, LMT
 The Scalp and Face Protocol Julie Goodwin, BA, LMT The Scalp and Face Protocol Julie Goodwin, BA, LMT Julie Goodwin 2014 2 Agenda Pertinent Anatomy and Physiology Treatment Planning Strokes, Techniques
The Scalp and Face Protocol Julie Goodwin, BA, LMT The Scalp and Face Protocol Julie Goodwin, BA, LMT Julie Goodwin 2014 2 Agenda Pertinent Anatomy and Physiology Treatment Planning Strokes, Techniques
Management of Brachial Plexus & Peripheral Nerves Blast Injuries. First Global Conflict Medicine Congress
 Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
X-Plain Muscles Reference Summary
 X-Plain Reference Summary Introduction are very important elements of the human body. They account for about half of a person s weight. Understanding how muscles work and how they can be injured is necessary
X-Plain Reference Summary Introduction are very important elements of the human body. They account for about half of a person s weight. Understanding how muscles work and how they can be injured is necessary
Monday, November 13, 2017 A & P 2401
 Monday, November 13, 2017 A & P 2401 Today you will complete the following handouts. Study the last part of the handout for this will be on your quiz, which will be on Wednesday. It is titled steps of
Monday, November 13, 2017 A & P 2401 Today you will complete the following handouts. Study the last part of the handout for this will be on your quiz, which will be on Wednesday. It is titled steps of
Introduction. Anatomy
 Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Rotator Cuff Tears Our approach
 Rotator Cuff Tears Our approach Terry R. Malone EdD., PT, ATC Professor of Physical Therapy University of Kentucky Nothing to disclose only wish Deep Musculature & Glenoid RC Insertion Data The RC insertion
Rotator Cuff Tears Our approach Terry R. Malone EdD., PT, ATC Professor of Physical Therapy University of Kentucky Nothing to disclose only wish Deep Musculature & Glenoid RC Insertion Data The RC insertion
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
MUSCULAR TISSUE. Dr. Gary Mumaugh
 MUSCULAR TISSUE Dr. Gary Mumaugh MUSCLE OVERVIEW The three types of muscle tissue are skeletal, cardiac, and smooth These types differ in structure, location, function, and means of activation FUNCTIONAL
MUSCULAR TISSUE Dr. Gary Mumaugh MUSCLE OVERVIEW The three types of muscle tissue are skeletal, cardiac, and smooth These types differ in structure, location, function, and means of activation FUNCTIONAL
Technique Guide. Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures.
 Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Peripheral Nerve Problems
 UW MEDICINE PATIENT EDUCATION Peripheral Nerve Problems How they develop and ways to treat them This handout explains how nerves work, what happens when they are injured, and how peripheral nerve problems
UW MEDICINE PATIENT EDUCATION Peripheral Nerve Problems How they develop and ways to treat them This handout explains how nerves work, what happens when they are injured, and how peripheral nerve problems
Sprains. Initially the ankle is swollen, painful, and may turn eccyhmotic (bruised). The bruising, and the initial swelling, is due to ruptured
 Sprains Introduction An ankle sprain is a common injury and usually results when the ankle is twisted, or inverted. The term sprain signifies injury to the soft tissues, usually the ligaments, of the ankle.
Sprains Introduction An ankle sprain is a common injury and usually results when the ankle is twisted, or inverted. The term sprain signifies injury to the soft tissues, usually the ligaments, of the ankle.
The Muscular System Part A
 10 The Muscular System Part A Lecture Presentation by Lori Garrett Section 1: Functional Organization of the Muscular System Learning Outcomes 10.1 Describe the general function of the body s axial and
10 The Muscular System Part A Lecture Presentation by Lori Garrett Section 1: Functional Organization of the Muscular System Learning Outcomes 10.1 Describe the general function of the body s axial and
Skeletal Muscles and Functions
 Skeletal Muscles and Functions Huei-Ming Chai, PT, Ph.D. School of Physical Therapy National Taiwan University Classification of Muscles striated muscles skeletal muscles: voluntary contraction cardiac
Skeletal Muscles and Functions Huei-Ming Chai, PT, Ph.D. School of Physical Therapy National Taiwan University Classification of Muscles striated muscles skeletal muscles: voluntary contraction cardiac
Sensitivity of a Method for the Analysis of Facial Mobility. II. Interlandmark Separation
 Sensitivity of a Method for the Analysis of Facial Mobility. II. Interlandmark Separation CARROLL-ANN TROTMAN, B.D.S., M.A., M.S. JULIAN J. FARAWAY, PH.D. Objective: This study demonstrates a method of
Sensitivity of a Method for the Analysis of Facial Mobility. II. Interlandmark Separation CARROLL-ANN TROTMAN, B.D.S., M.A., M.S. JULIAN J. FARAWAY, PH.D. Objective: This study demonstrates a method of
3A/3B FUNCTIONAL ANATOMY
 3A/3B FUNCTIONAL ANATOMY http://commons.wikimedia.org/wiki/file:complete_neuron_cell_diagram_en.svg 1 CONTENTS Structure of a skeletal muscle How do we produce movement? Structure of a sarcomere Sliding
3A/3B FUNCTIONAL ANATOMY http://commons.wikimedia.org/wiki/file:complete_neuron_cell_diagram_en.svg 1 CONTENTS Structure of a skeletal muscle How do we produce movement? Structure of a sarcomere Sliding
What is Kinesiology? Basic Biomechanics. Mechanics
 What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
A BIOMECHANICAL STUDY OF A SUTURE BETWEEN THE DELTOID MUSCLE AND A FREE TENDON GRAFT FOR RECONSTRUCTION OF THE ELBOW EXTENSION
 Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2011 Mar; 155(1):79 84. DOI 10.5507/bp.2011.011 I. Cizmar, Z. Florian, T. Navrat, D. Palousek 79 A BIOMECHANICAL STUDY OF A SUTURE BETWEEN THE DELTOID
Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2011 Mar; 155(1):79 84. DOI 10.5507/bp.2011.011 I. Cizmar, Z. Florian, T. Navrat, D. Palousek 79 A BIOMECHANICAL STUDY OF A SUTURE BETWEEN THE DELTOID
Rotator Cuff Tears. Christopher Jones, MD
 Rotator Cuff Tears Christopher Jones, MD Why this article? Most people find going to see the doctor an emotional experience which is made more stressful when surgery is a consideration. Hopefully this
Rotator Cuff Tears Christopher Jones, MD Why this article? Most people find going to see the doctor an emotional experience which is made more stressful when surgery is a consideration. Hopefully this
Bones Ethmoid bone Inferior nasal concha Lacrimal bone Maxilla Nasal bone Palatine bone Vomer Zygomatic bone Mandible
 splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
A Patient s Guide to Biceps Tendon Tears at the Elbow
 A Patient s Guide to Biceps Tendon Tears at the Elbow Introduction The muscles which flex the elbow are the bicep complex. Like all musculoskeletal units, the end connection is a tendon composed of strong,
A Patient s Guide to Biceps Tendon Tears at the Elbow Introduction The muscles which flex the elbow are the bicep complex. Like all musculoskeletal units, the end connection is a tendon composed of strong,
MUSCLE TISSUE (MUSCLE PHYSIOLOGY) PART I: MUSCLE STRUCTURE
 PART I: MUSCLE STRUCTURE Muscle Tissue A primary tissue type, divided into: skeletal muscle cardiac muscle smooth muscle Functions of Skeletal Muscles Produce skeletal movement Maintain body position Support
PART I: MUSCLE STRUCTURE Muscle Tissue A primary tissue type, divided into: skeletal muscle cardiac muscle smooth muscle Functions of Skeletal Muscles Produce skeletal movement Maintain body position Support
Circumferential skin defect - Ilizarov technique in plastic surgery
 Brief Communication Circumferential skin defect - Ilizarov technique in plastic surgery Vrisha Madhuri, Shankar R. Kurpad, Manasseh Nithyananth, Thilak S Jepegnanam, V. T. K. Titus, Prema Dhanraj Department
Brief Communication Circumferential skin defect - Ilizarov technique in plastic surgery Vrisha Madhuri, Shankar R. Kurpad, Manasseh Nithyananth, Thilak S Jepegnanam, V. T. K. Titus, Prema Dhanraj Department
Pronator Teres Is an Appropriate Donor Muscle for Restoration of Wrist and Thumb Extension
 Pronator Teres Is an Appropriate Donor Muscle for Restoration of Wrist and Thumb Extension Geoffrey D. Abrams, BA, Samuel R. Ward, PT, PhD, San Diego, CA Jan Fridén, MD, PhD, Göteborg, Sweden Richard L.
Pronator Teres Is an Appropriate Donor Muscle for Restoration of Wrist and Thumb Extension Geoffrey D. Abrams, BA, Samuel R. Ward, PT, PhD, San Diego, CA Jan Fridén, MD, PhD, Göteborg, Sweden Richard L.
Neuromuscular Mechanics
 Schematic Representation of Motor Units in Skeletal Muscle Neuromuscular Mechanics Hamill & Knutzen (Ch 4) Whatever text you read do not focus on motorneuron structure and sensory receptors Muscle Fibres
Schematic Representation of Motor Units in Skeletal Muscle Neuromuscular Mechanics Hamill & Knutzen (Ch 4) Whatever text you read do not focus on motorneuron structure and sensory receptors Muscle Fibres
Muscular Considerations for Movement. Kinesiology RHS 341 Lecture 4 Dr. Einas Al-Eisa
 Muscular Considerations for Movement Kinesiology RHS 341 Lecture 4 Dr. Einas Al-Eisa Role of muscles Prime mover Synergist Agonist Antagonist Stabilizers Neutralizers Role of muscles Agonist: Muscles producing
Muscular Considerations for Movement Kinesiology RHS 341 Lecture 4 Dr. Einas Al-Eisa Role of muscles Prime mover Synergist Agonist Antagonist Stabilizers Neutralizers Role of muscles Agonist: Muscles producing
Biceps Tendon Tear at the Elbow
 DISEASES & CONDITIONS Biceps Tendon Tear at the Elbow The biceps muscle is located in the front of your upper arm. It is attached to the bones of the shoulder and elbow by tendons strong cords of fibrous
DISEASES & CONDITIONS Biceps Tendon Tear at the Elbow The biceps muscle is located in the front of your upper arm. It is attached to the bones of the shoulder and elbow by tendons strong cords of fibrous
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures.
 Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Ch 10: Skeletal Muscle Tissue (Myology)
 Ch 10: Skeletal Muscle Tissue (Myology) main objectives: Describe the distinguishing characteristics of the different muscle tissues Discuss the organization of skeletal muscle Explain the micro-anatomy
Ch 10: Skeletal Muscle Tissue (Myology) main objectives: Describe the distinguishing characteristics of the different muscle tissues Discuss the organization of skeletal muscle Explain the micro-anatomy
Patellar Tendon Repair Rehabilitation Guideline
 Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
