Cystic and Cystic-Appearing Lesions of the Mandible: Review
|
|
|
- Rose Knight
- 6 years ago
- Views:
Transcription
1 AJR Integrative Imaging LIFELONG LEARNING FOR RADIOLOGY Cystic and Cystic-Appearing Lesions of the Mandible: Review Brooke Devenney-Cakir 1, Rathan M. Subramaniam 1,2, Susmitha M. Reddy 1, Heather Imsande 2, Anita Gohel 3, Osamu Sakai 1,2 Objective Cystic and cystic-appearing lesions of the mandible are commonly noted on head and neck imaging and present a diagnostic dilemma for the radiologist. This article aims to help outline the differential diagnosis for cystic mandibular lesions, outline the key imaging features, and suggest recommendations for further imaging and/or intervention when required. Conclusion After completing this article, the reader should have an improved ability to characterize cystic and cystic-appearing lesions of the mandible. By definition, a cyst is an epithelium-lined cavity that contains fluid or semisolid material. Pathologic analysis of the epithelial lining and contents and clinical and radiographic findings are generally required to achieve a definitive diagnosis [1]. Clinically, cysts in the mandible can present as functional disturbances caused by bone remodeling and weakening. Furthermore, cysts can present after a secondary infection. Cysts occurring in the mandible appear radiographically as either unilocular or multilocular lucencies that vary in size and definition. Displaced or resorbed tooth roots, displaced mandibular canal and expansion, and uneruption of the tooth are often seen. The cyst s spatial relationship to the tooth on imaging is an important diagnostic feature [1]. Accurate radiographic identification of cystic-appearing benign and malignant tumors is essential for appropriate clinical workup and management. Based on the cell of origin, cystic lesions in the mandible are subdivided into odontogenic (Appendix 1) and nonodontogenic (Appendix 2) lesions. Odontogenic cysts arise from tooth derivatives, and they are frequently divided into inflammatory and developmental types. Further subdivision can be achieved with histologic analysis of the epithelial lining and with imaging to determine whether calcifications are present and in correlation with clinical findings; occasionally the pathogenesis is unclear [1]. The World Health Organization classification published in 2005 is widely accepted [2]. This classification defines cysts (odontogenic and nonodontogenic cysts) and tumors (benign and malignant types) and further subdivides the lesions on the basis of odontogenic tissue type [2]. The majority of these lesions may initially be identified by the patient s dentist on either physical examination or routine dental radiographs. Further, cystic lesions are often identified as incidental lesions by the radiologist on imaging performed for different reasons. Collaborative interaction between the dentist, oral surgeon, and radiologist is essential for the appropriate evaluation, imaging, and treatment of cystic and cysticappearing lesions of the mandible (Tables 1 and 2). Odontogenic Lesions Humans have 20 primary and 32 permanent teeth. Each tooth develops from ectoderm and mesenchyme. The ectoderm develops into the enamel, whereas the mesenchymal cells form the dentin, cementum, periodontal ligament, and pulp contents [3, 4]. The dental lamina, a thickening of the oral epithelium, invaginates into the mesenchyme and the surrounding cells condense to form the tooth buds or tooth germs [3]. As the tooth bud grows, it develops into a cap shape with mesenchymal invagination, which forms the dental papilla [4]. The dental papilla forms both the dental pulp (the soft tissue in the root chamber of the tooth that contains nerves, vessels, and connective tissue) and odontoblasts, which form the dentin of the tooth. The ectoderm forms the enamel organ, which includes the outer enamel epithelium, the stellate reticulum, and the inner enamel epithelium. The inner enamel epithelium elongates into ameloblasts, which form the enamel of the tooth [4]. Odontogenic Cysts Cysts commonly occur in the mandible and appear as unilocular or multilocular radiolucencies on dental radiographs. Cystic lesions within the mandible can cause bony remodeling that can weaken the bone, leading to functional changes and predisposing the patient to infection and Keywords: cystic lesions, head and neck imaging, mandible DOI: /AJR Received November 25, 2009; accepted after revision August 4, Department of Radiology, Boston Medical Center, 820 Harrison Ave, FGH Bldg, Level 3, Boston, MA Address correspondence to R. Subramaniam (rathan.subramaniam@bmc.org). 2 Boston University School of Medicine, Boston, MA. 3 Boston University School of Dental Medicine, Boston, MA. AJR 2011; 196:WS66 WS X/11/1966 WS66 American Roentgen Ray Society WS66 AJR:196, June 2011
2 Lesions of the Mandible TABLE 1: Odontogenic Lesions Odontogenic Lesions Periapical cyst (radicular cyst) Dentigerous cyst (follicular cyst) Keratocystic odontogenic tumor Ameloblastoma Odontogenic myxoma TABLE 2: Nonodontogenic Lesions Nonodontogenic Lesions Simple bone cyst (traumatic bone cyst) Aneurysmal bone cyst Static bone cavity (Stafne cyst) Osteomyelitis Multiple myeloma and plasmacytoma Initial Radiographic Imaging Initial Radiographic Imaging a None typically required Fluid-fluid levels better visualized pathologic fracture [1]. The relationship of the cyst to adjacent structures is important, which includes features such as unerupted teeth, tooth displacement, root resorption, and canal displacement. Although many odontogenic cysts are developmental in origin, the most common type of odontogenic cyst, the periapical cyst, is acquired [5]. Periapical (radicular) cysts The periapical (radicular) cyst is the most common type of odontogenic cyst. These lesions have a slight male predominance and peak incidence between the ages of 30 and 50 years [5]. Periapical cysts generally originate after trauma or dental caries. Dental caries cause inflammation of the pulp cavity leading to pulp necrosis [6]. The infection then spreads to the tooth apex of the root causing periapical periodontitis, which leads to either an acute abscess or a chronic granuloma. Persistent chronic infection can lead to formation of a periapical cyst [1]. Treatment options include tooth extraction, endodontic therapy, and apical surgery. If the periapical cyst persists after surgical extraction of the associated tooth, it is referred to as a residual cyst [5]. A periapical cyst presents as a well-circumscribed corticated radiolucency at the apex of the nonvital tooth. Cortical expansion may be seen with large lesions (Figs. 1 and 2). Periapical cysts can cause root resorption of the affected tooth and can displace adjacent structures including adjacent teeth and the mandibular canal. MRI of periapical cysts shows high T2 (due to high fluid content) and variable T1 signal intensity (Fig. 3). Contrast-enhanced MR images show an enhancing cystic wall consistent with inflammation [1]. Dentigerous (follicular) cysts The dentigerous cyst is the second most common odontogenic cyst occurring in the mandible and is typically discovered in adults in the third and Additional Radiologic Evaluation CT MRI WBC or Gallium Scanning PET/CT If atypical features present, can aid in exclusion of other cystic lesions Contrast-enhanced for better characterization of soft tissues and bones Contrast-enhanced for solid lesions and extraosseous extension Note NR = not required in routine cases when other imaging is diagnostic. a May appear normal. Additional Radiologic Evaluation CT MRI PET/CT Extent of cyst, adjacent tooth involvement, preoperative planning Extent of cyst, adjacent tooth involvement, preoperative planning Extent of disease, presence of daughter cysts Extent of disease and osseous destruction, displacement of teeth Helps differentiate from hemangioma, central giant cell granuloma, ameloblastoma Note NR = not required in routine cases when other imaging is diagnostic, SCC = squamous cell carcinoma. Aids in differentiation among central giant cell granuloma, odontogenic myxoma, keratocystic odontogenic tumor, and ameloblastoma If atypical features present, can exclude simple bone cyst and ameloblastoma NR; enhance, showing a solid tumor NR; can differentiate from ameloblastoma if lesions have overlapping features Help differentiate from ameloblastoma; can suggest malignant transformation into SSC Presence of solid components aids in differentiation from dentigerous cyst; aggressive features suggest ameloblastic carcinoma Staging of disease especially if SSC transformation Staging of disease especially if SSC transformation Early diagnosis before changes noted on CT or For systemic staging and therapy response AJR:196, June 2011 WS67
3 Devenney-Cakir et al. fourth decades of life [7]. The cyst forms around the crown of an unerupted tooth as fluid collects between layers of epithelium or between the epithelium and enamel. The size of a typical follicle space is 2 3 mm; the presence of a dentigerous cyst should be suspected if the follicle space is greater than 5 mm [5]. Dentigerous cysts can vary in size but have the potential to grow large enough to cause significant expansion of the jaw and displacement of adjacent teeth; however, resorption of the root apex is uncommon [1, 8]. Superimposed infection and pathologic fractures can develop especially with larger lesions [1]. Small lesions are typically treated with enucleation, whereas larger lesions undergo surgical drainage and marsupialization to relieve the pressure inside the cyst and prevent damage to the involved permanent teeth. The presence of bilateral lesions is extremely rare in isolation and association with a syndrome, such as mucopolysaccharidosis (type 4) or cleidocranial dysplasia, should be suspected [9]. Radiographically, a dentigerous cyst appears as a wellcircumscribed unilocular radiolucent lesion adjacent to the crown of an unerupted tooth [9], most commonly the third molar tooth (Fig. 4). CT is useful to evaluate large lesions and can show the origin, size, and internal contents of the cyst and evaluate the integrity of the cortical plate and its relationship to the adjacent anatomic structures [9]. Significant cortical expansion or thinning of the buccal and lingual cortical plates may be seen with larger lesions [1]. The roots of the affected tooth are typically outside the lesion. Large lesions can develop undulating borders due to uneven expansion rates and may mimic ameloblastomas and keratocystic odontogenic tumors [5]. MRI is not required for diagnosis in most cases; however, it may aid in the characterization of large lesions. MRI will typically show high T2 and low to intermediate T1 signal within the cyst, whereas the tooth will appear as a signal void. Contrast-enhanced images may show enhancement of the thin cyst wall. The presence of a thick irregular wall or a solid component raises the possibility of ameloblastoma [10]. FDG PET/CT shows background Fig year-old woman with periapical cyst. Cropped panoramic radiograph shows radiolucent lesion (arrowhead) in posterior body of ramus of mandible with displacement of mandibular canal (arrow). Combination of findings suggests benign disease. FDG uptake; however, if inflammation is present, mild FDG hypermetabolism can be noted [11]. Other odontogenic cysts Other less common odontogenic cysts include entities such as lateral periapical cysts and buccal bifurcation cysts. Lateral periodontal cysts are developmental odontogenic cysts that are most common in adults. They most commonly occur in the mandibular premolar area and are typically discovered incidentally. Radiographically they appear as well-circumscribed lytic lesions associated with the tooth root in the premolar mandibular region. It is important to distinguish a lateral periodontal cyst from a keratocystic odontogenic tumor [12]. Buccal bifurcation cysts are extremely rare, likely secondary to inflammation, and arise from the buccal periodontium at the bifurcation of the roots of the mandibular molars [1]. The diagnosis of a buccal bifurcation cyst is made based solely on clinical and radiographic features. Buccal bifurcation cysts are typically unilateral; occur in the first or second molar; and are distinguished by the tipping of the involved molar, causing the root tips to be pushed into the lingual cortical plate of the mandible [5, 13]. Fig year-old man with periapical cyst. A C, Axial (A), sagittal (B), and volume-rendering 3D (C) CT images show well-circumscribed radiolucent lesions surrounding apex of first (white arrows, A and B) and second (black arrows, B and C) molars (teeth 18 and 19). Note large cavities in affected teeth with mild root resorption (arrowheads, B and C). WS68 AJR:196, June 2011
4 Lesions of the Mandible Fig year-old woman with periapical cyst. A, Coronal T2-weighted MR image shows high signal in anterior body of mandible (arrow). B, Axial gadolinium-enhanced fat-suppressed T1- weighted image shows enhancement of cyst wall (arrow); this finding is consistent with periapical cyst. Odontogenic Tumors Odontogenic tumors arise from abnormal proliferation of the tissues and cells involved in odontogenesis. These tumors represent a varied group of lesions and are classified by their stage in tooth development [1, 2]. Many odontogenic tumors can show a cystic appearance including keratocystic odontogenic tumor, ameloblastoma, ameloblastic fibroma, odontogenic myxoma, primordial cyst, and central odontogenic fibroma [14, 15]. One distinguishing feature between benign and malignant lesions is close evaluation of the character of tooth root absorption: Benign lesions show directional root resorption secondary to pressure effects, whereas malignant lesions show nondirectional root resorption [16]. Keratocystic odontogenic tumor Keratocystic odontogenic tumor was formally known as odontogenic keratocyst but recently was categorized as an odontogenic tumor rather than a cyst [2]. A keratocystic odontogenic tumor is a benign but locally aggressive developmental odontogenic tumor that is most commonly located in the mandibular ramus and body [17]. These lesions are typically found in adults in the second to fourth decades of life and represent 5 17% of all jaw cysts [15]. Keratocystic odontogenic tumors are lined with stratified keratinizing squamous epithelium [1] and arise from the dental lamina and overlying alveolar mucosa [18]. They can expand the cortical bone and erode the cortex. Keratocystic odontogenic tumors have a high postoperative recurrence rate [7]. The presence of multiple keratocystic odontogenic tumors should raise the possibility of basal cell nevus syndrome (i.e., Gorlin-Goltz syndrome) [17]. Findings associated with this autosomal-dominant disorder include midface hypoplasia, frontal bossing and prognathism, mental retardation, calcification of the falx cerebri and dura, bifid ribs, and multiple basal cell carcinomas of the skin [7]. Keratocystic odontogenic tumors may be unilocular or multiloculated and often contain daughter cysts that extend to the surrounding bone [7]. They typically extend into the marrow cavity with either a smooth border contributing to mild bulging of the cortex but without significant cortical expansion. Keratocystic odontogenic tumors can show a more aggressive growth pattern including multilocularity, cortical expansion, perforation of the cortical bone, tooth and mandibular canal displacement, root resorption, and extrusion of erupted teeth [15] (Fig. 5). Keratocystic odontogenic tumors show slight to no expansion within the body of the mandible; however, once they reach the mandibular ramus, they typically cause significant expansion [19]. Fig year-old man with dentigerous cyst. A C, Axial (A), coronal (B), and volume-rendering 3D (C) CT images show well-circumscribed unilocular radiolucent lesion (arrows) containing crown of unerupted second molar (tooth 31). AJR:196, June 2011 WS69
5 Devenney-Cakir et al. Fig year-old woman with keratocystic odontogenic tumor. A, Oblique sagittal reconstructed CT image obtained using bone algorithm shows large radiolucent lesion (arrows) in posterior body of mandibular ramus, with scalloping of cortex. B, Axial contrast-enhanced CT image obtained using soft-tissue algorithm shows cystic lesion with mild peripheral enhancement (arrow) breaking through cortex and extending into left masseter muscle. CT shows a unilocular or multilocular cyst with corticated margins. Keratocystic odontogenic tumors typically occur in the body and ramus of the mandible in association with an impacted tooth [15]. MRI shows a thin-walled, minimally peripherally enhancing cyst with heterogeneous intensity fluid contents (intermediate T1 signal and intermediate to high T2 signal) because of variable proteinaceous content [10]. MRI can help distinguish keratocystic odontogenic tumor from ameloblastoma, the latter of which has a mixed pattern of solid and cystic components, irregular thick walls, and avid enhancement of solid components [10, 20]. In rare cases, malignant transformation into squamous cell carcinoma occurs; PET/CT will typically show intense FDG hypermetabolism similar to other head and neck squamous cell carcinomas (Fig. 6). Ameloblastoma Ameloblastoma is a benign but locally aggressive epithelial odontogenic tumor thought to arise from the surface epithelium, remnants of the dental lamina, or pluripotential epithelial cells lining odontogenic cysts. Approximately 5% of ameloblastomas arise from the epithelial lining of dentigerous cysts [21]. They account for 10% of odontogenic tumors, and 80% are located within the mandible [21]. Ameloblastomas are most commonly found in adults in the third and fourth decades without sex predominance. Ameloblastomas are slow-growing painless masses and may present with local swelling [21]. Malignant ameloblastoma is a term given to tumors with metastasis, even those with a histologically benign appearance, and ameloblastic carcinoma is a term given to tumors that display histologically malignant features with or without metastasis [14]. Treatment is surgical resection; however, wide margin en bloc resection is required for tumors that infiltrate through the cyst wall into adjacent bone [22]. Radiographically, the appearance of ameloblastomas is variable and dependent on the histopathology of the lesion (Fig. 7). There are multiple classification systems for ameloblastoma. On the basis of its clinical behavior, anatomic location, radiographic appearance, and histologic characteristics, ameloblastoma can be grouped into four main forms: multicystic, unicystic, extraosseous or peripheral, and desmoplastic [21]. Fig year-old man with squamous cell carcinoma most likely derived from keratocystic odontogenic tumor. A and B, Axial (A) and volume-rendering 3D (B) CT images obtained using bone algorithm show large radiolucent lesion (arrows) within posterior body of left mandible with associated cortical break. Note periosteal reaction, which may suggest aggressiveness of lesion or superimposed infection. Lesion (arrowhead, B) contains crown of unerupted third molar. C, Fused PET/CT image shows intense FDG uptake (maximum standardized uptake value = 25.6) associated with left mandibular mass (arrow); this finding suggests malignancy. Bilateral hypermetabolic level II lymph nodes were also noted (not shown). WS70 AJR:196, June 2011
6 Lesions of the Mandible Fig year-old woman with ameloblastoma. A C, Axial bone algorithm (A) and coronal soft-tissue algorithm (B) contrast-enhanced CT images and volume-rendering 3D CT image (C) show well-circumscribed, slightly lobulated, expansile radiolucent lesion (arrows, A and C) in posterior body of mandibular ramus. Significant cortical thinning and remodeling are seen particularly in lingual cortex. There are cortical defects on both buccal and lingular aspects of mandible. Note that nodular solid components show mild enhancement. Solid or multicystic ameloblastoma is the most common variant, accounting for 85% of all ameloblastomas. This variant is also the most aggressive and has a high recurrence rate compared with the other variants [21]. Radiographically the multicystic (solid) ameloblastoma variant typically appears multiloculated with internal septations manifested by a honeycomb or soap-bubble appearance. This variant can be confused with large keratocystic odontogenic tumors [14]. The unicystic variant is characterized by a single cystic cavity lined by epithelium. Luminal proliferation of the epithelial cells or mural infiltration of the cyst wall can occur [21]. Common radiographic findings of the unicystic variant include a unilocular, well-circumscribed, and well-corticated lucent lesion often associated with the crown of an unerupted or impacted tooth. This variant can resemble a dentigerous cyst [19]. The presence of solid components, including internal bony septa, aids in the distinction between an ameloblastoma and a dentigerous cyst [19]. Many authors have concluded that the unicystic variant is generally less aggressive than the other ameloblastoma variants [21]. The peripheral ameloblastoma variant represents a softtissue tumor that is histologically identical to an intraosseous ameloblastoma but occurs over the tooth-bearing parts of the jaw. These lesions appear solid on imaging, have a benign clinical course, and can be treated with local excision [21]. The desmoplastic variant can be distinguished from other variants by the presence of multiple coarse internal calcifications with significant surrounding cortical destruction. The hallmark of ameloblastoma is extensive tooth root absorption. CT evaluation is useful to access the extent of the lesion, cortical perforation, and adjacent soft-tissue involvement [19, 21]. The presence of more aggressive imaging features such as large solid enhancing components, papillary projections, and extraosseous extension and invasion is suggestive of malignancy (e.g., ameloblastic carcinoma) [23] (Fig. 8), but Fig year-old boy with ameloblastic carcinoma. A and B, Axial (A) and volume-rendering 3D (B) CT images show large destructive radiolucent lesion (white arrowheads) centered in posterior body extending to manibular ramus, significant cortical destruction, and root erosion that significantly displaces second molar (black arrowhead). C, Axial gadolinium-enhanced fat-suppressed T1-weighted MR image shows heterogeneously enhancing lesion (white arrowheads) with regions of decreased signal that corresponded to cystic degeneration on pathologic specimen. AJR:196, June 2011 WS71
7 Devenney-Cakir et al. Fig year-old woman with odontogenic myxoma. A and B, Sagittal bone algorithm (A) and axial softtissue algorithm (B) CT images show slightly lobulated lesion in anterior body of mandible (arrows). Root resorption (black arrowhead, A) with cortical thinning and breakthrough (white arrowhead, B) indicates aggressive process. preoperative diagnosis is very difficult. MRI is useful for evaluation of intra- and extraosseous extension and involvement of adjacent structures. Contrast-enhanced images show strong enhancement of the solid components including papillary projections, lesion wall, and internal septa [10, 23]. Malignant ameloblastoma and ameloblastic carcinoma show strong FDG avidity on PET/CT, which can be used for initial staging, therapy assessment, and postsurgical surveillance [24]. Preoperative cross-sectional imaging is very important for surgical planning. The suspicion of ameloblastic carcinoma or the presence of distant metastasis requires a larger, more extensive surgery followed by radiation and chemotherapy. Odontogenic myxoma Accounting for % of odontogenic tumors [25], odontogenic myxoma is a true odontogenic tumor originating from the mesodermal portion of the odontogenic apparatus. These lesions are most common in adults in the second and third decades of life [1]. Odontogenic myxomas are benign, slow-growing painless lesions; however, they tend to be locally aggressive, exhibiting rapid growth leading to extensive osseous destruction and cortical expansion [26]. They present equally within the maxilla and mandible, with the ramus as the most common mandibular location [1]. Odontogenic myxomas are treated with wide margin surgical resection because they tend to infiltrate and recur [14]. Radiographically, odontogenic myxoma lesions appear as radiolucent regions separated by bony trabeculae that form geographic compartments. They typically contain multiple thin septations and internal osseous trabeculae and exhibit honeycomb-like structures [7,14,15,25] (Fig. 9). The tumor margins are typically poorly defined. An odontogenix myxoma may simulate entities such as hemangioma, central giant cell granuloma, and ameloblastoma. This aggressive tumor shows little encapsulation, often extending through bone into the adjacent soft tissues [25]. Occasionally odontogenic myxomas infiltrate between the adjacent tooth roots causing displacement and resorption [26]. CT typically shows an expansile osteolytic lesion within the mandible [15, 25]. Other odontogenic tumors Other less common odontogenic tumors that may show a cystic appearance include a primordial cyst, central odontogenic fibroma, and ameloblastic fibroma. A primordial cyst is an uncommon cystic lesion that develops instead of the tooth; however, most authors believe that all primordial cysts represent keratocystic odontogenic tumors [1]. Radiographically, a primordial cyst appears as a nonexpansile well-defined radiolucent lesion without an associated tooth [7]. A central odontogenic fibroma is a rare benign odontogenic neoplasm of the odontogenic apparatus (periodontal ligament and dental papilla). Radiographically a central odontogenic fibroma appears as a well-defined heterogeneous lesion causing cortical expansion [27]. An ameloblastic fibroma is composed of enamel and embryonic connective tissue. Radiographically, an ameloblastic fibroma typically appears as a well-defined, pericoronal radiolucent Fig year-old man with simple bone cyst. A and B, Axial (A) and coronal (B) CT images show wellcircumscribed radiolucent lesion (arrows) with cortical scalloping in anterior body of mandible without root resorption. Prominent expansile change is not typical of simple bone cyst. WS72 AJR:196, June 2011
8 Lesions of the Mandible Fig year-old man with static bone cavity. A and B, Axial (A) and volume-rendering 3D (B) CT images show well-circumscribed cortical defect (arrows) at lingual aspect of mandibular angle. lesion. Most are multiloculated and associated with impacted teeth, often in the posterior mandible. Although ameloblastic fibromas do not represent a variant of ameloblastomas, radiologically they can appear similar to a unilocular ameloblastoma [7]. Nonodontogenic Cysts and Pseudocysts Nonodontogenic cysts and cystlike lesions can mimic odontogenic cystic lesions and include entities such as traumatic bone cyst and aneurysmal bone cyst (ABC). Nonodontogenic cystic lesions are typically acquired with unclear causes. Nonodontogenic Cysts Simple bone cyst (traumatic bone cyst) The term simple bone cyst includes entities such as solitary bone cyst, hemorrhagic cyst, extravasation cyst, unicameral bone cyst, traumatic bone cyst, and idiopathic bone cavity. Despite its name, simple bone cyst lesions lack an epithelial lining and are not true cysts. Simple bone cysts are common lesions within the skeleton including the mandible [28]. Although the cause of a simple bone cyst is unknown, these lesions are thought to originate from intramedullary hemorrhage caused by trauma (including tooth extraction) [29]. Simple bone cysts are typically investigated surgically to exclude other processes [28]; after surgery, they heal by reossification. Simple bone cysts most commonly occur in the mandible and less commonly within the maxilla [29]. They are commonly located in the mandibular marrow space, which extends posterior from the premolar region. Radiologically simple bone cysts are typically unilocular with well-defined borders, causing a scalloped appearance of the cyst between the tooth roots [28] (Fig. 10). A simple bone cyst is a simple cavity and should not be associated with root resorption or tooth displacement [8]. Large cysts can extend into the interdental space. CT can characterize the high-density blood products commonly found within a simple bone cyst; however, the density can vary depending on the age of the blood products [1]. MRI can also show a thin rim of peripheral enhancement and the presence of blood products; however, signal characteristics vary on the basis of the stage of heme breakdown [1]. Aneurysmal bone cyst ABCs are very rare lesions that are most common within the mandible of children with a slight female predominance [30, 31]. Clinically these lesions present with rapid painless facial swelling that can be disfiguring [31]. The origin of ABCs is controversial: Some investigators believe ABCs are primary congenital lesions or vascular malformations, whereas others believe they are acquired and arise after local hemodynamic disturbances from trauma [31]. Typically these lesions are surgically removed; however, because ABCs Fig year-old woman with osteomyelitis. A, Axial CT image obtained using bone algorithm shows irregular radiolucent lesion with periosteal reaction (arrow) within body of mandible. B, Axial unenhanced CT image obtained using soft-tissue algorithm shows soft-tissue density within lesion with osseous fragments (sequestrum) (arrowhead). AJR:196, June 2011 WS73
9 Devenney-Cakir et al. contain multiloculations and bony septa, complete excision can be challenging. ABCs appear as uni- or multicystic radiolucencies causing expansion and destruction of the osseous cortex on radiographs [30]. They have a typical meshwork appearance on CT, which reflects the histopathologic appearance of a partially cystic, blood-filled meshwork divided by coarse septa [32]. Other CT features include the presence of an expansile hypoattenuating lesion with numerous fluid-fluid levels [30]. MRI characterization is critical to further characterize the soft-tissue features of these lesions and differentiate ABCs from other entities including giant cell granuloma, odontogenic myxoma, keratocystic odontogenic tumor, and ameloblastoma [31]. MRI shows multiple cystic lesions with fluid-fluid levels, enhancement of cyst wall, and enhancing septations [32]. Nonodontogenic Lesions Static bone cavity (Stafne cyst) A static bone cavity is a pseudocyst that appears as an inward bowing of the lingual mandibular cortex into the medullary space [33]. They are asymptomatic radiolucencies located at the angle of the mandible that represent a cortical defect with or without extension of submandibular salivary gland tissue [34]. A static bone cavity is a benign finding and no intervention is required [33]. The most common radiographic appearance is a unilateral, ovoid, radiolucent lingual cortical defect with a sclerotic margin near the angle of the mandible inferior to the mandibular canal [33]. The defect can extend deep to the buccal cortex [14]. Although no additional imaging is required, occasionally CT can be performed to exclude other cystic lesions [14] (Fig. 11). Static bone cavities are easily differentiated from odontogenic cysts by location [14]. CT shows a cortical defect in the lingual aspect of the mandibular angle filled with fat or, less commonly, continuity with the adjacent salivary gland [35]. Occasionally static bone cavities can have atypical features including multiple lobes, location superior to the inferior alveolar canal, or lack of a sclerotic border [36]. In these cases, MRI can aid in further characterization and can exclude other entities including traumatic bone cyst and ameloblastoma [35]. Osteomyelitis Osteomyelitis is an inflammatory condition, typically of dental origin, that occurs within the medullary cavity and adjacent cortex. Osteomyelitis can occur from direct extension of a pulpal infection [37] or from a secondary process, such as acute exacerbation of a periapical lesion, trauma, high-dose radiation therapy, or sepsis [1]. Healthy patients rarely develop osteomyelitis because of easy access to antimicrobial therapy [7]. Osteomyelitis is more commonly associated with a poorly controlled dental infection or overall debilitated medical state. Other considerations include diabetes; systemic immunosuppression; bisphosphonates; sickle cell anemia; and, in the correct demographic, tuberculosis [1]. It is essential to differentiate osteomyelitis from other conditions including neoplasms [37]. Treatment includes long-term IV antibiotic therapy and other supportive surgical measures such as débridement; sequestrectomy; and, if needed, resection of infected bone. The imaging appearance of osteomyelitis will differ on the basis of the type and stage of disease (lytic, sclerotic, mixed, or with a sequestrum pattern). Standard and panoramic radiographs and panoramic radiographs may appear normal or show periosteal reaction or osteolytic change [1]. Contrastenhanced CT allows better characterization of both osseous and soft-tissue findings; however, the appearance of osteomyelitis on CT is often nonspecific and differs depending on the stage of disease including lytic, sclerotic, mixed, or with a sequestrum pattern [37] (Fig. 12). Typically periosteal reaction and cortical plate disruption are seen, more commonly on the buccal surface [37]. Associated soft-tissue abscess and inflammatory change within the adjacent soft tissue are also common findings. Acute suppurative osteomyelitis is manifested by the sudden onset of severe constitutional symptoms; however, conventional radiographs may appear normal in the first 8 10 days [1]. Indium-labeled WBC or gallium scanning can be useful to diagnose acute osteomyelitis in the setting of negative radiographs. Low-grade infections can cause sclerosing osteomyelitis manifested by deposition of bone along the osseous cortex and trabeculae. These changes can be focal or diffuse [7]. The imaging appearances of osteomyelitis, radiation-induced osteonecrosis, bisphosphonate-associated osteonecrosis, and lytic metastatic lesions can overlap significantly. Close correlation with patient history and clinical findings is required for interpretation of the imaging findings. Other nonodontogenic pseudocysts Many other entities may present as lucent mandibular lesions including fibrous dysplasia, ossifying fibroma, cherubism, osteonecrosis, and Paget disease. Multiple other nonodontogenic lesions including osseous dysplasia can appear cystlike radiographi- Fig year-old man with plasmacytoma. A and B, Lateral (A) and panoramic (B) mandibular radiographs show poorly marginated radiolucent lesion (arrows) within body of mandible. Adjacent teeth are unaffected by lesion. WS74 AJR:196, June 2011
10 Lesions of the Mandible cally, especially on a panoramic radiograph. These entities include cementoosseous dysplasia. Cementoosseous dysplasia includes periapical, focal, and florid cemental dysplasia depending on the location and extent of disease. Cementoosseous dysplasia forms from a proliferation of connective tissue found within the periodontal membrane. These lesions are most common in African-American women in the fourth and fifth decades of life. Multiple lesions are often termed florid cementoosseous dysplasia. Radiographically these lesions initially appear as well-circumscribed radiolucent lesions at the apex of the tooth that evolve over time into a radiopaque mass with a radiolucent border [7]. Cementoblastoma, also termed true cementoma, is a rare odontogenic neoplasm of functional cementoblasts that forms a cementum-like mass connected to the tooth root (typically involving the permanent teeth) and can resemble cementoosseous dysplasia radiographically. These lesions are typically solitary and are found in men younger than 25 years old. Radiographically, cementoblastomas appear well defined with central dense radiopaque material attached to the tooth root surrounded by a radiolucent zone of uniform width [15]. Nonodontogenic Tumors Nonodontogenic tumors are typically disease processes that are not isolated to the mandible but can occur throughout the skeleton and will therefore have similar radiographic findings. Although most nonodontogenic tumors are solid, they may appear cystic, particularly on radiographs. These tumors include schwannoma, neurofibroma, central hemangioma, multiple myeloma (plasmacytoma), lymphoma, leukemia, and metastases [1]. Metastases to the mandible are four times more common that those to the maxilla. Because of the high marrow volume and vascularity, the angle and posterior body are the most common locations within the mandible [7]. The most common primary sites are lung, breast, thyroid, kidney, prostate, and gastrointestinal tract [1]. Recognition of malignant mandibular lesions is important because they may be asymptomatic and may be incidentally noted. Multiple myeloma (plasmacytoma) Multiple myeloma is a neoplasm of plasma cells at multiple locations, whereas plasmacytoma is limited to a single lesion. These lesions can be intramedullary or extramedullary and occur throughout the skeleton including the mandible. Because of the active hematopoietic activity within the mandible, the most common sites of involvement are the ramus, angle, and molar regions. After confirmation of a solitary lesion to exclude multiple myeloma is achieved, the lesion is treated with radiation [38]. However, systemic disease is treated with chemotherapy with or without bone marrow transplantation [16]. Multiple myeloma typically appears as multiple lytic lesions with poorly marginated, nonsclerotic borders on and CT [38] (Fig. 13). CT is useful to show solid lesions and extraosseous extension. These lesions typically show homogeneous soft-tissue density and enhancement. The MR signal intensity depends on the stage of disease [39]; however, lesions often show homogeneous intermediate signal intensity on both T1- and T2-weighted images and avid enhancement [38, 40]. MRI may have greater sensitivity for lesion detection but typically does not characterize the lesion better than CT [38]. PET/CT is increasingly used to diagnose multiple myeloma, assess multiple myeloma before and after transplantation, and determine the prognosis of patients with multiple myeloma. It is useful in identifying metabolically active disease and in staging [41]. Other nonodontogenic tumors Other nonodontogenic tumors include squamous cell carcinoma, osteoblastoma, chondrosarcoma, lymphoma, leukemia, mucoepidermoid carcinoma, metastatic disease, and Langerhans cell histiocytosis. Summary Cystic lesions of the mandible arise from both odontogenic and nonodontogenic sources. Given the wide range of pathologic features but similar imaging findings, familiarity with embryologic characteristics and with secondary imaging findings is crucial. The prevalence and location in the mandible of a particular lesion often help narrow the differential diagnosis and direct the workup and treatment of a lesion. Imaging may not provide a specific diagnosis but should help narrow the differential diagnosis, thereby helping to guide patient treatment. References 1. Weber AL, Kaneda T, Scrivani SJ, Aziz S. Jaw: cysts, tumors and nontumorous lesions. In: Som PM, Curtin HD, eds. Head and neck imaging, 4th ed. St. Louis, MO: Mosby, 2003: Barnes L, Reichart P, Eveson JW, Sidransky D. WHO classification of tumours: pathology and genetics of head and neck tumours. Lyon, France: IARC Press, Avery JK, Steele PF. Essentials of oral histology and embryology: a clinical approach. St. Louis, MO: Mosby, 2000: Abrahams JJ, Rock R, Hayt MW. Embryology and anatomy of the jaw and dentition. In: Som PM, Curtin HD, eds. Head and neck imaging, 4th ed. St. Louis, MO: Mosby, 2003: White SC, Pharoha MJ. Cysts and cystlike lesions of the jaws. In: White SC, Pharoha MJ, eds. Oral radiology: principles and interpretation, 6th ed. St. Louis, MO: Mosby Elsevier, 2009: Lin LM, Huang GT, Rosenberg PA. Proliferation of epithelial cell rests, formation of apical cysts, and regression of apical cysts after periapical wound healing. J Endod 2007; 33: Dunfee BL, Sakai O, Pistey R, Gohel A. Radiologic and pathologic characteristics of benign and malignant lesions of the mandible. RadioGraphics 2006; 26: Akman A, Sakai O. Periapical lucency: underappreciated lesions on CT. Contemporary Diag Radiol 2006; 29: Freitas DQ, Tempest LM, Sicoli E, Lopes-Neto FC. Bilateral dentigerous cysts: review of the literature and report of an unusual case. Dentomaxillofac Radiol 2006; 35: Konouchi H, Asaumi J, Yanagi Y, et al. Usefulness of contrast enhanced-mri in the diagnosis of unicystic ameloblastoma. Oral Oncol 2006; 42: Maeda T, Tateishi U, Terauchi T, et al. Unsuspected bone and soft tissue lesions identified at cancer screening using positron emission tomography. Jpn J Clin Oncol 2007; 37: Saygun I, Ozdemir A, Safali M. Lateral periodontal cyst. Turk J Med Sci 2001; 31: Thikkurissy S, Glazer KM, McNamara KK, Tatakis DN. Buccal bifurcation AJR:196, June 2011 WS75
11 Devenney-Cakir et al. cyst in a 7-year-old: surgical management and 14-month follow-up. J Periodontol 2010; 81: Scholl RJ, Kellett HM, Neumann DP, Lurie AG. Cysts and cystic lesions of the mandible: clinical and radiologic-histopathologic review. RadioGraphics 1999; 19: Theodorou SJ, Theodorou DJ, Sartoris DJ. Imaging characteristics of neoplasms and other lesions of the jawbones. Part 1. Odontogenic tumors and tumorlike lesions. Clin Imaging 2007; 31: Wood RE. Malignant diseases of the jaws. In: White SC, Pharoaha MJ, eds. Oral radiology: principles and interpretation, 6th ed. St. Louis, MO: Mosby Elsevier, 2009: González-Alva P, Tanaka A, Oku Y, et al. Keratocystic odontogenic tumor: a retrospective study of 183 cases. J Oral Sci 2008; 50: Minami M, Kaneda T, Ozawa K, et al. Cystic lesions of the maxillomandibular region: MR imaging distinction of odontogenic keratocysts and ameloblastomas from other cysts. AJR 1996; 166: White SC, Pharoaha MJ. Benign tumors of the jaws. In: White SC, Pharoha MJ, eds. Oral radiology: principles and interpretation, 6th ed. St. Louis, MO: Mosby Elsevier, 2009: Minami M, Kaneda T, Yamamoto H, et al. Ameloblastoma in the maxillomandibular region: MR imaging. Radiology 1992; 184: Sham E, Leong J, Maher R, Schenberg M, Leung M, Mansour AK. Mandibular ameloblastoma: clinical experience and literature review. ANZ J Surg 2009; 79: Carlson ER, Marx RE. The ameloblastoma: primary, curative surgical management. J Oral Maxillofac Surg 2006; 64: Suomalainen A, Hietanen J, Robinson S, Peltola JS. Ameloblastic carcinoma of the mandible resembling odontogenic cyst in a panoramic radiograph. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2006; 101: Nguyen BD. Malignant ameloblastoma with thoracic vertebral metastasis: PET/CT and MR imaging. Clin Nucl Med 2005; 30: Koseki T, Kobayashi K, Hashimoto K, et al. Computed tomography of odontogenic myxoma. Dentomaxillofac Radiol 2003; 32: Noffke CE, Raubenheimer EJ, Chabikuli NJ, Bouckaert MM. Odontogenic myxoma: review of the literature and report of 30 cases from South Africa. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007; 104: Lotay HS, Kalmar J, DeLeeuw K. Central odontogenic fibroma with features of central granular cell odontogenic tumor. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2010; 109:e63 e Suomalainen A, Apajalahti S, Kuhlefelt M, Hagstrom J. Simple bone cyst: a radiological dilemma. Dentomaxillofac Radiol 2009; 38: Cortell-Ballester I, Figueiredo R, Berini-Aytés L, Gay-Escoda C. Traumatic bone cyst: a retrospective study of 21 cases. Med Oral Patol Oral Cir Bucal 2009; 14:E239 E Theodorou SJ, Theodorou DJ, Sartoris DJ. Imaging characteristics of neoplasms and other lesions of the jawbones. Part 2. Odontogenic tumor-mimickers and tumor-like lesions. Clin Imaging 2007; 31: Capote-Moreno A, Acero J, García-Recuero I, Ruiz J, Serrano R, de Paz V. Giant aneurysmal bone cyst of the mandible with unusual presentation. Med Oral Patol Oral Cir Bucal 2009; 14:E137 E Asaumi J, Konouchi H, Hisatomi M, et al. MR features of aneurysmal bone cyst of the mandible and characteristics distinguishing it from other lesions. Eur J Radiol 2003; 45: Murdoch-Kinch CA. Developmental disturbances of the face and jaw. In: White SC, Pharoaha MJ, eds. Oral radiology: principles and interpretation, 6th ed. St. Louis, MO: Mosby Elsevier, 2009: Minowa K, Kobayashi I, Matsuda A, et al. Static bone cavity in the condylar neck and mandibular notch of the mandible. Aust Dent J 2009; 54: Shimizu M, Osa N, Okamura K, Yoshiura K. CT analysis of the Stafne s bone defects of the mandible. Dentomaxillofac Radiol 2006; 35: Branstetter BF, Weissman JL, Kaplan SB. Imaging of a Stafne bone cavity: what MR adds and why a new name is needed. AJNR 1999; 20: Taori KB, Solanke R, Mahajan SM, Rangankar V, Saini T. CT evaluation of mandibular osteomyelitis. Indian J Radiol Imaging 2005; 15: Vogl TJ, Steger W, Grevers G, Balzer J, Mack M, Felix R. MR characteristics of primary extramedullary plasmacytoma in the head and neck. AJNR 1996; 17: Baur-Melnyk A, Buhmann S, Durr HR, Reiser M. Role of MRI for the diagnosis and prognosis of multiple myeloma. Eur J Radiol 2005; 55: Pisano JJ, Coupland R, Chen SY, Miller AS. Plasmacytoma of the oral cavity and jaws: a clinicopathologic study of 13 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1997; 83: Hanrahan CJ, Christensen CR, Crim JR. Current concepts in the evaluation of multiple myeloma with MR imaging and FDG PET/CT. RadioGraphics 2010; 30: WS76 AJR:196, June 2011
12 Lesions of the Mandible APPENDIX 1: Odontogenic Lesions Cysts Periapical cyst (radicular cyst) Residual cyst (periapical cyst after the removal of periapical cyst) Dentigerous cyst (follicular cyst) Lateral periodontal buccal bifurcation cyst Paradental cyst Glandular odontogenic cyst Cystlike Benign cementoblastoma (cementoblastoma, true cementoma) Tumors Keratocystic odontogenic tumor (odontogenic keratocyst) Ameloblastoma Ameloblastic fibroma Odontogenic myxoma Central odontogenic fibroma Adenomatoid odontogenic tumor Calcifying epithelial odontogenic tumor (Pindborg tumor) Calcifying epithelial odontogenic tumor Malignant Ameloblastic carcinoma APPENDIX 2: Nonodontogenic Lesions Cysts Simple bone cyst (traumatic bone cyst) Aneurysmal bone cyst Cystlike Static bone cavity (Stafne cyst) Fibrous dysplasia Osteomyelitis Paget disease Central giant cell granuloma Ossifying fibroma Cherubism Radiation necrosis Cementoosseous dysplasia (periapical, focal, florid) Tumors Neurofibroma Neurilemmoma (schwannoma) Central hemangioma Arteriovenous fistula Malignant Multiple myeloma or plasmacytoma Squamous cell carcinoma Osteosarcoma Chondrosarcoma Chondroma Lymphoma Leukemia Mucoepidermoid carcinoma Metastatic lesions Langerhans cell histiocytosis AJR:196, June 2011 WS77
Keratocystic Odontogenic Tumor : What radiologist needs to know?
 Keratocystic Odontogenic Tumor : What radiologist needs to know? Poster No.: C-0444 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit K. El Karzazi, J. M. Villanueva Rincón, R. Corrales,
Keratocystic Odontogenic Tumor : What radiologist needs to know? Poster No.: C-0444 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit K. El Karzazi, J. M. Villanueva Rincón, R. Corrales,
Disclosure. Educational Objectives. Terminology. Odontogenic Cysts. Terminology
 Disclosure Lisa J. Koenig BChD, DDS, MS Professor & Program Director, Oral Medicine and Oral Radiology Marquette University School of Dentistry Consultant to Soredex for the Scanora 3D and 3Dx Author/Editor
Disclosure Lisa J. Koenig BChD, DDS, MS Professor & Program Director, Oral Medicine and Oral Radiology Marquette University School of Dentistry Consultant to Soredex for the Scanora 3D and 3Dx Author/Editor
Differential Diagnosis of Radiolucent Lesions of the Jaws
 Differential Diagnosis of Radiolucent Lesions of the Jaws Multilocular Multilocular Radiolucencies Odontogenic Keratocyst Botryoid Odontogenic Cyst Glandular odontogenic Cyst Invasive Ameloblastoma Central
Differential Diagnosis of Radiolucent Lesions of the Jaws Multilocular Multilocular Radiolucencies Odontogenic Keratocyst Botryoid Odontogenic Cyst Glandular odontogenic Cyst Invasive Ameloblastoma Central
RADIOGRAPHIC INTERPRETATION Differential Diagnosis
 RADIOGRAPHIC INTERPRETATION Differential Diagnosis MODULE 1: The Introduction. Chief complaint Demographics Age Sex Race Historical findings Physical findings Clinical Radiographic Location Maxilla/mandible
RADIOGRAPHIC INTERPRETATION Differential Diagnosis MODULE 1: The Introduction. Chief complaint Demographics Age Sex Race Historical findings Physical findings Clinical Radiographic Location Maxilla/mandible
Large Dentigerous Cyst
 Volume 16.2.1 Feb 2016 This Lecture Series qualifies for 0.5 Informal CPD Learning Hours Large Dentigerous Cyst By Dr Hassem Geha A 55 year-old male presented with a painless swelling in the right mandible.
Volume 16.2.1 Feb 2016 This Lecture Series qualifies for 0.5 Informal CPD Learning Hours Large Dentigerous Cyst By Dr Hassem Geha A 55 year-old male presented with a painless swelling in the right mandible.
Problem diagnoses. Current issues in Anatomic pathology. Problem Diagnoses in Tumors of the Oral Cavity 5/29/2009
 Current issues in Anatomic pathology Problem Diagnoses in Tumors of the Oral Cavity Richard Jordan DDS PhD FRCPath Professor of Oral Pathology & Pathology Director, UCSF Oral Pathology Diagnostic Laboratory
Current issues in Anatomic pathology Problem Diagnoses in Tumors of the Oral Cavity Richard Jordan DDS PhD FRCPath Professor of Oral Pathology & Pathology Director, UCSF Oral Pathology Diagnostic Laboratory
Origin of Odontogenic Cysts & Tumors
 Origin of Odontogenic Cysts & Tumors Odontogenic Apparatus Origin of Odontogenic Cysts & Tumors Odontogenic Apparatus Remnants of dental lamina Reduced enamel epithelium Odontogenic rests Basal cell layer
Origin of Odontogenic Cysts & Tumors Odontogenic Apparatus Origin of Odontogenic Cysts & Tumors Odontogenic Apparatus Remnants of dental lamina Reduced enamel epithelium Odontogenic rests Basal cell layer
Maxilla and mandible benign lesions: Radiologic Findings and Differential Diagnosis in CT
 Maxilla and mandible benign lesions: Radiologic Findings and Differential Diagnosis in CT Poster No.: C-0964 Congress: ECR 2012 Type: Scientific Exhibit Authors: N. Lopez 1, E. Marcos Naranjo 2, M. D.
Maxilla and mandible benign lesions: Radiologic Findings and Differential Diagnosis in CT Poster No.: C-0964 Congress: ECR 2012 Type: Scientific Exhibit Authors: N. Lopez 1, E. Marcos Naranjo 2, M. D.
高雄醫學大學 口腔醫學院 口腔病理影像科 牙科 X 光影像判讀 教學範例
 高雄醫學大學 口腔醫學院 口腔病理影像科 牙科 X 光影像判讀 教學範例 Content Image No. 001 Dentigerous cyst over left upper embedded canine--------------------- 頁 1 Image No. 002---------------------------------------------------------------
高雄醫學大學 口腔醫學院 口腔病理影像科 牙科 X 光影像判讀 教學範例 Content Image No. 001 Dentigerous cyst over left upper embedded canine--------------------- 頁 1 Image No. 002---------------------------------------------------------------
Odontomes and Odontogenic tumours
 Odontomes and Odontogenic tumours Odontomes Developmental hamartoma Hamartoma: normal tissue in abnormal location Any cells to be neoplastic it must be able to replicate, which is not seen in hamartoma
Odontomes and Odontogenic tumours Odontomes Developmental hamartoma Hamartoma: normal tissue in abnormal location Any cells to be neoplastic it must be able to replicate, which is not seen in hamartoma
IMAGING OF CYSTS OF THE JAWS July 2002 N. Serman
 IMAGING OF CYSTS OF THE JAWS July 2002 N. Serman This is an area where radiology plays an important role in assisting with the diagnosis, determining the size of the lesion and the relationship to adjacent
IMAGING OF CYSTS OF THE JAWS July 2002 N. Serman This is an area where radiology plays an important role in assisting with the diagnosis, determining the size of the lesion and the relationship to adjacent
Vascular. Extravasated blood. Melanocytic. Tattoo. Epidermolysis bullosa. Lichen planus. Pemphigoid Pemphigus Lupus. Candidosis. Surface Epithelial
 Oral Soft Tissue Pathology Epithelial Thickening (white) Combination Erythema migrans Epithelial atrophy (red) Surface Lesions Clinical Impression Enlargements Surface Debris Pigmented Vesicular Ulcerated
Oral Soft Tissue Pathology Epithelial Thickening (white) Combination Erythema migrans Epithelial atrophy (red) Surface Lesions Clinical Impression Enlargements Surface Debris Pigmented Vesicular Ulcerated
The clinical appearance and diagnosis of odontogenic cysts. SE Arc-Állcsont-Szájsebészeti és Fogászati Klinika BUDAPEST
 The clinical appearance and diagnosis of odontogenic cysts SE Arc-Állcsont-Szájsebészeti és Fogászati Klinika BUDAPEST DEFINITION A cyst is a sac with walls of connective tissue, lined by epithelium, containing
The clinical appearance and diagnosis of odontogenic cysts SE Arc-Állcsont-Szájsebészeti és Fogászati Klinika BUDAPEST DEFINITION A cyst is a sac with walls of connective tissue, lined by epithelium, containing
Common/Important Radiolucencies. B. Most Common Location Apex of permanent first molar, rare in primary teeth.
 Cincinnati Dental Association Breakfast at Tiffany s: The Jewels and Gems of Oral Pathology November 17, 2010 John A. Svirsky, DDS, MEd Virginia Commonwealth University 804-828-0547 FAX: 804-828-6234 EMAIL:
Cincinnati Dental Association Breakfast at Tiffany s: The Jewels and Gems of Oral Pathology November 17, 2010 John A. Svirsky, DDS, MEd Virginia Commonwealth University 804-828-0547 FAX: 804-828-6234 EMAIL:
Ameloblastomatous Gorlin s cyst
 319 Journal of Oral Science, Vol. 49, No. 4, 319-323, 2007 Case Report Ameloblastomatous Gorlin s cyst Mala Kamboj 1) and Manish Juneja 2) 1) Department of Oral Pathology and Microbiology, U.P. King George
319 Journal of Oral Science, Vol. 49, No. 4, 319-323, 2007 Case Report Ameloblastomatous Gorlin s cyst Mala Kamboj 1) and Manish Juneja 2) 1) Department of Oral Pathology and Microbiology, U.P. King George
Index. oralmaxsurgery.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Adenomatoid odontogenic tumor, pediatric, 50 51 Ameloblastic carcinoma, pediatric, 17, 49 Ameloblastic fibro-odontoma, pediatric, 54 Ameloblastic
Index Note: Page numbers of article titles are in boldface type. A Adenomatoid odontogenic tumor, pediatric, 50 51 Ameloblastic carcinoma, pediatric, 17, 49 Ameloblastic fibro-odontoma, pediatric, 54 Ameloblastic
Pre-reading - radiolucencies
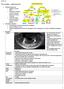 Pre-reading - radiolucencies Multiple radiolucencies o Suggests a systemic cause o Most likely: cherubism or KCOT s of nevoid basal cell carcinoma syndrome o Sometimes: florid osseous dysplasia (if limited
Pre-reading - radiolucencies Multiple radiolucencies o Suggests a systemic cause o Most likely: cherubism or KCOT s of nevoid basal cell carcinoma syndrome o Sometimes: florid osseous dysplasia (if limited
Inter-radicular Radiolucencies
 Inter-radicular Radiolucencies Differential Diagnosis Laterally Displaced Radicular Cyst Accessory canals Root fracture Lateral Periodontal Cyst Botryoid variant Odontogenic Keratocyst Incisive Canal Cyst
Inter-radicular Radiolucencies Differential Diagnosis Laterally Displaced Radicular Cyst Accessory canals Root fracture Lateral Periodontal Cyst Botryoid variant Odontogenic Keratocyst Incisive Canal Cyst
Pictorial Essay. CT of Calcifying Jaw Bone Diseases
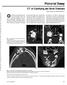 Pictorial Essay CT of Calcifying Jaw one Diseases Koichi Yonetsu 1 and Takashi Nakamura Downloaded from www.ajronline.org by 46.3.204.207 on 01/08/18 from IP address 46.3.204.207. Copyright RRS. For personal
Pictorial Essay CT of Calcifying Jaw one Diseases Koichi Yonetsu 1 and Takashi Nakamura Downloaded from www.ajronline.org by 46.3.204.207 on 01/08/18 from IP address 46.3.204.207. Copyright RRS. For personal
Development of teeth. 5.DM - Pedo
 Development of teeth 5.DM - Pedo Tooth development process of continuous changes in predetermined order starts from dental lamina A band of ectodermal cells growing from the epithelium of the embryonic
Development of teeth 5.DM - Pedo Tooth development process of continuous changes in predetermined order starts from dental lamina A band of ectodermal cells growing from the epithelium of the embryonic
Course Description 343 DDS- Clinical Oral and Maxillofacial Radiology II ( )
 King Saud University College of Dentistry Dept. of Oral Medicine & Diagnostic Sciences Division of Oral & Maxillofacial Radiology Course Description 343 DDS- Clinical Oral and Maxillofacial Radiology II
King Saud University College of Dentistry Dept. of Oral Medicine & Diagnostic Sciences Division of Oral & Maxillofacial Radiology Course Description 343 DDS- Clinical Oral and Maxillofacial Radiology II
Radiographic features of cysts and benign tumors of the jaws. Cyst. Effects on adjacent structures. Types. Odontogenic Cysts. Non-Odontogenic cysts
 Radiographic features of cysts and benign tumors of the jaws Cyst A Cyst is a benign pathologic cavity filled with fluid, lined by epithelium, and surrounded by a connective tissue wall Steven R. Singer,
Radiographic features of cysts and benign tumors of the jaws Cyst A Cyst is a benign pathologic cavity filled with fluid, lined by epithelium, and surrounded by a connective tissue wall Steven R. Singer,
Glandular Odontogenic Cyst Coexisting with a Dentigerous Cyst: Case Report
 SmyrnaMed Case 2018;2(1): 1-5 ISSN (Online): 2564-6869 www.smyrnamed.com Glandular Odontogenic Cyst Coexisting with a Dentigerous Cyst: Case Report Assist.Prof.Dr. Serap Keskin Tunç 1, Dt. Erkan Feslihan
SmyrnaMed Case 2018;2(1): 1-5 ISSN (Online): 2564-6869 www.smyrnamed.com Glandular Odontogenic Cyst Coexisting with a Dentigerous Cyst: Case Report Assist.Prof.Dr. Serap Keskin Tunç 1, Dt. Erkan Feslihan
TRAUMATIC BONE CYST OF IDIOPATHIC ORIGIN? A REPORT OF TWO CASES
 Traumatic Bone Cyst Kumar S. et al 183 CASE REPORT TRAUMATIC BONE CYST OF IDIOPATHIC ORIGIN? A REPORT OF TWO CASES Kumar Satish 1, S. Padmashree 1, Jayalekshmy Rema 1 ABSTRACT BACKGROUND: Traumatic bone
Traumatic Bone Cyst Kumar S. et al 183 CASE REPORT TRAUMATIC BONE CYST OF IDIOPATHIC ORIGIN? A REPORT OF TWO CASES Kumar Satish 1, S. Padmashree 1, Jayalekshmy Rema 1 ABSTRACT BACKGROUND: Traumatic bone
Epithelial Sources. Rests of Serres Rests of Malassez Reduced Enamel Epithelium Surface Mucosa
 ODONTOGENIC CYSTS Epithelial Sources Rests of Serres Rests of Malassez Reduced Enamel Epithelium Surface Mucosa Epithelial Sources Surface Epithelium Rests of Serres Reduced Enamel Epithelium Rests of
ODONTOGENIC CYSTS Epithelial Sources Rests of Serres Rests of Malassez Reduced Enamel Epithelium Surface Mucosa Epithelial Sources Surface Epithelium Rests of Serres Reduced Enamel Epithelium Rests of
IN THE NAME OF GOD. Dr.kheirandish DDS,MSC Oral and maxillofacial pathology
 IN THE NAME OF GOD Dr.kheirandish DDS,MSC Oral and maxillofacial pathology ODONTOGENIC CYSTS AND TUMORS Chapter 15 I. DENTIGEROUS CYST II. III. IV. ERUPTION CYST ODONTOGENIC KERATOCYST Orthokeratinized
IN THE NAME OF GOD Dr.kheirandish DDS,MSC Oral and maxillofacial pathology ODONTOGENIC CYSTS AND TUMORS Chapter 15 I. DENTIGEROUS CYST II. III. IV. ERUPTION CYST ODONTOGENIC KERATOCYST Orthokeratinized
Course Description 343 DDS- Clinical Oral and Maxillofacial Radiology II ( )
 King Saud University College of Dentistry Dept. of Oral Medicine & Diagnostic Sciences Division of Oral & Maxillofacial Radiology Course Description 343 DDS- Clinical Oral and Maxillofacial Radiology II
King Saud University College of Dentistry Dept. of Oral Medicine & Diagnostic Sciences Division of Oral & Maxillofacial Radiology Course Description 343 DDS- Clinical Oral and Maxillofacial Radiology II
Proceedings of the 36th World Small Animal Veterinary Congress WSAVA
 www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: http://www.ivis.org October 14(Fri) ~ 17(Mon) 2011 ICC Jeju, Korea 2011 WSAVA
www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: http://www.ivis.org October 14(Fri) ~ 17(Mon) 2011 ICC Jeju, Korea 2011 WSAVA
A Case Report of Odontogenic Keratocyst in Anterior Mandibule Position
 A Case Report of Odontogenic Keratocyst in Anterior Mandibule Position Malihe Moeini 1, Seyed Ehsan Anvar 2, Rasool Barzegari Bafghi 3* 1.Resident of Oral and Maxillofacial Radiology, Faculty of Dentistry,
A Case Report of Odontogenic Keratocyst in Anterior Mandibule Position Malihe Moeini 1, Seyed Ehsan Anvar 2, Rasool Barzegari Bafghi 3* 1.Resident of Oral and Maxillofacial Radiology, Faculty of Dentistry,
INFLAMMATORY DENTIGEROUS CYST OR INFLAMMATORY CYSTIC LESIONS OF MIXED DENTITION?: A REPORT OF THREE CASES
 Case Report International Journal of Dental and Health Sciences Volume 03, Issue 03 INFLAMMATORY DENTIGEROUS CYST OR INFLAMMATORY CYSTIC LESIONS OF MIXED DENTITION?: A REPORT OF THREE CASES Pritam K Mankapure
Case Report International Journal of Dental and Health Sciences Volume 03, Issue 03 INFLAMMATORY DENTIGEROUS CYST OR INFLAMMATORY CYSTIC LESIONS OF MIXED DENTITION?: A REPORT OF THREE CASES Pritam K Mankapure
Study of maxillary and mandibular cystic lesions
 Study of maxillary and mandibular cystic lesions Poster No.: C-1428 Congress: ECR 2013 Type: Educational Exhibit Authors: M. L. Rozas Rodríguez, M. E. Banegas Illescas, M. Y. Torres Sousa, R. M. Fernández
Study of maxillary and mandibular cystic lesions Poster No.: C-1428 Congress: ECR 2013 Type: Educational Exhibit Authors: M. L. Rozas Rodríguez, M. E. Banegas Illescas, M. Y. Torres Sousa, R. M. Fernández
Jaws: Cysts and Odontogenic Neoplasms
 Topic 10: Jaw Cysts General Features of Jaw Cysts Sources of Epithelium in Cysts Radiographic Features of Jaw Cysts Microscopic Features of Jaw Cysts Treatment and Prognosis of Jaw Cysts Classification
Topic 10: Jaw Cysts General Features of Jaw Cysts Sources of Epithelium in Cysts Radiographic Features of Jaw Cysts Microscopic Features of Jaw Cysts Treatment and Prognosis of Jaw Cysts Classification
Course Description 343 DDS- Clinical Oral and Maxillofacial Radiology II ( )
 King Saud University College of Dentistry Dept. of Oral Medicine & Diagnostic Sciences Division of Oral & Maxillofacial Radiology Course Description 343 DDS- Clinical Oral and Maxillofacial Radiology II
King Saud University College of Dentistry Dept. of Oral Medicine & Diagnostic Sciences Division of Oral & Maxillofacial Radiology Course Description 343 DDS- Clinical Oral and Maxillofacial Radiology II
Differential Diagnosis of Oral Masses. Gingival Lesions
 Differential Diagnosis of Oral Masses Gingival Lesions Gingival/Alveolar Ridge Masses Parulis Periodontal Abscess Tori and Exostoses Reactive Proliferations Peripheral Odontogenic Cysts Peripheral Odontogenic
Differential Diagnosis of Oral Masses Gingival Lesions Gingival/Alveolar Ridge Masses Parulis Periodontal Abscess Tori and Exostoses Reactive Proliferations Peripheral Odontogenic Cysts Peripheral Odontogenic
MULTILOCULAR AMELOBLASTOMA OF MANDIBLE-A CASE REPORT
 International Journal of Advancements in Research & Technology, Volume 2, Issue2, February-2013 1 MULTILOCULAR AMELOBLASTOMA OF MANDIBLE-A CASE REPORT DR SANTOSH KUMAR SUBUDHI*, DR SUMIT DASH**, DR.K..PREMANANDA***,
International Journal of Advancements in Research & Technology, Volume 2, Issue2, February-2013 1 MULTILOCULAR AMELOBLASTOMA OF MANDIBLE-A CASE REPORT DR SANTOSH KUMAR SUBUDHI*, DR SUMIT DASH**, DR.K..PREMANANDA***,
Role of MDCT and VR reconstructions in the diagnosis and characterization of maxillary cystic lesions.
 Role of MDCT and VR reconstructions in the diagnosis and characterization of maxillary cystic lesions. Poster No.: C-0704 Congress: ECR 2011 Type: Scientific Exhibit Authors: M. Coronella 1, P. V. Foti
Role of MDCT and VR reconstructions in the diagnosis and characterization of maxillary cystic lesions. Poster No.: C-0704 Congress: ECR 2011 Type: Scientific Exhibit Authors: M. Coronella 1, P. V. Foti
MARK D. MURPHEY MD, FACR. Physician-in-Chief, AIRP. Chief, Musculoskeletal Imaging
 ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE MARK D. MURPHEY MD, FACR Physician-in-Chief, AIRP Chief, Musculoskeletal Imaging ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE Giant cell tumor (GCT) Unicameral
ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE MARK D. MURPHEY MD, FACR Physician-in-Chief, AIRP Chief, Musculoskeletal Imaging ALPHABET SOUP AND CYSTIC LESIONS OF THE BONE Giant cell tumor (GCT) Unicameral
MALIGNANT TUMOURS OF THE JAWS
 MALIGNANT TUMOURS OF THE JAWS MALIGNANT TUMOURS OF THE JAWS Squamous cell carcinoma Osteogenic sarcoma Chondrosarcoma Fibrosarcoma Malignant lymphomas (incl. Burkitt s) Multiple myeloma Ameloblastoma Secondary
MALIGNANT TUMOURS OF THE JAWS MALIGNANT TUMOURS OF THE JAWS Squamous cell carcinoma Osteogenic sarcoma Chondrosarcoma Fibrosarcoma Malignant lymphomas (incl. Burkitt s) Multiple myeloma Ameloblastoma Secondary
The Radiology Assistant : Bone tumor - ill defined osteolytic tumors and tumor-like lesions
 Bone tumor - ill defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
Bone tumor - ill defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Central odontogenic fibroma of the mandible: a case report
 457 Journal of Oral Science, Vol. 51, No. 3, 457-461, 2009 Case Report Central odontogenic fibroma of the mandible: a case report Ioanna Daskala 1), Demos Kalyvas 2), Markos Kolokoudias 2), Dimitris Vlachodimitropoulos
457 Journal of Oral Science, Vol. 51, No. 3, 457-461, 2009 Case Report Central odontogenic fibroma of the mandible: a case report Ioanna Daskala 1), Demos Kalyvas 2), Markos Kolokoudias 2), Dimitris Vlachodimitropoulos
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 3/ Issue 18/May 05, 2014 Page 4859
 CYSTIC DEGENERATION IN FOLLICULAR AMELOBLASTOMA: A CASE REPORT Neeraj Kumar 1, Niharika Rathore 2, Hemant Shakya 3, Anshuman Jamdade 4, Puneet Chitlangia 5 HOW TO CITE THIS ARTICLE: Neeraj Kumar, Niharika
CYSTIC DEGENERATION IN FOLLICULAR AMELOBLASTOMA: A CASE REPORT Neeraj Kumar 1, Niharika Rathore 2, Hemant Shakya 3, Anshuman Jamdade 4, Puneet Chitlangia 5 HOW TO CITE THIS ARTICLE: Neeraj Kumar, Niharika
4/2/17. Panoramic Radiography: Normal Variants and Pathology. Composite of in-focused and blurred images. It s a type of Tomogram.
 Fundamentals Panoramic Radiography: Normal Variants and Pathology It s a type of Tomogram Jimmie L. Harper D.D.S., M.S. Cincinnati Oral and Maxillofacial Surgery, Inc. Volunteer Assistant Professor, Division
Fundamentals Panoramic Radiography: Normal Variants and Pathology It s a type of Tomogram Jimmie L. Harper D.D.S., M.S. Cincinnati Oral and Maxillofacial Surgery, Inc. Volunteer Assistant Professor, Division
Case Report Basal Cell Ameloblastoma of Mandible: A Rare Case Report with Review
 Case Reports in Dentistry Volume 2013, Article ID 187820, 4 pages http://dx.doi.org/10.1155/2013/187820 Case Report Basal Cell Ameloblastoma of Mandible: A Rare Case Report with Review Hemant Shakya, 1
Case Reports in Dentistry Volume 2013, Article ID 187820, 4 pages http://dx.doi.org/10.1155/2013/187820 Case Report Basal Cell Ameloblastoma of Mandible: A Rare Case Report with Review Hemant Shakya, 1
Radiology. & supporting structures. Lec. 14 Common diseases of teeth Dr. Areej
 Radiology Lec. 14 Common diseases of teeth Dr. Areej & supporting structures A radiograph is only one part of the diagnostic process. Usually one does NOT make a diagnosis solely from a radiograph. A diagnosis
Radiology Lec. 14 Common diseases of teeth Dr. Areej & supporting structures A radiograph is only one part of the diagnostic process. Usually one does NOT make a diagnosis solely from a radiograph. A diagnosis
Simple diagnostic approach for mandible and maxilla lesions.
 Simple diagnostic approach for mandible and maxilla lesions. Poster No.: C-1285 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Gargallo Vaamonde, A. Burguete, N. Baraibar Argota, M. M. 1 2 1
Simple diagnostic approach for mandible and maxilla lesions. Poster No.: C-1285 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Gargallo Vaamonde, A. Burguete, N. Baraibar Argota, M. M. 1 2 1
PACIFIC JOURNAL OF MEDICAL SCIENCES ISSN:
 PACIFIC JOURNAL OF MEDICAL SCIENCES {Formerly: Medical Sciences Bulletin} ISSN: 2072 1625 Pac. J. Med. Sci. (PJMS) www.pacjmedsci.com. Email: pacjmedsci@gmail.com. ADENOMATOID ODONTOGENIC TUMOR WITH RARE
PACIFIC JOURNAL OF MEDICAL SCIENCES {Formerly: Medical Sciences Bulletin} ISSN: 2072 1625 Pac. J. Med. Sci. (PJMS) www.pacjmedsci.com. Email: pacjmedsci@gmail.com. ADENOMATOID ODONTOGENIC TUMOR WITH RARE
Characteristics of bony changes and tooth displacement in the mandibular cystic lesion involving the impacted third molar
 ORIGINAL ARTICLE http://dx.doi.org/0.55/jkaoms.04.40.5.5 pissn 34-550 eissn 34-5930 Characteristics of bony changes and tooth displacement in the mandibular cystic lesion involving the impacted third molar
ORIGINAL ARTICLE http://dx.doi.org/0.55/jkaoms.04.40.5.5 pissn 34-550 eissn 34-5930 Characteristics of bony changes and tooth displacement in the mandibular cystic lesion involving the impacted third molar
Malignant Lesions Steven R. Singer, DDS
 Definitions Malignant Lesions Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Malignancies are uncontrolled growths of tissue Primary tumors represent de novo tumors in their initial site Metastatic
Definitions Malignant Lesions Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Malignancies are uncontrolled growths of tissue Primary tumors represent de novo tumors in their initial site Metastatic
Oral Embryology and Histology
 Oral Embryology and Histology Chapter 8 Copyright 2018, Elsevier Inc. All Rights Reserved. 1 Learning Objectives Lesson 8.1: Oral Embryology 1. Pronounce, define, and spell the key terms. 2. Define embryology
Oral Embryology and Histology Chapter 8 Copyright 2018, Elsevier Inc. All Rights Reserved. 1 Learning Objectives Lesson 8.1: Oral Embryology 1. Pronounce, define, and spell the key terms. 2. Define embryology
Radiological and Pathological Characteristics of Mandibular Cystic Lesion A Review
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 74-80 www.iosrjournals.org Radiological and Pathological Characteristics
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 74-80 www.iosrjournals.org Radiological and Pathological Characteristics
The Radiology Assistant : Bone tumor - well-defined osteolytic tumors and tumor-like lesions
 Bone tumor - well-defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
Bone tumor - well-defined osteolytic tumors and tumor-like lesions Henk Jan van der Woude and Robin Smithuis Radiology department of the Onze Lieve Vrouwe Gasthuis, Amsterdam and the Rijnland hospital,
Case Report Unicystic Ameloblastoma with Mural Proliferation Managed by Conservative Treatment
 Case Reports in Pathology Volume 2016, Article ID 3089540, 4 pages http://dx.doi.org/10.1155/2016/3089540 Case Report Unicystic Ameloblastoma with Mural Proliferation Managed by Conservative Treatment
Case Reports in Pathology Volume 2016, Article ID 3089540, 4 pages http://dx.doi.org/10.1155/2016/3089540 Case Report Unicystic Ameloblastoma with Mural Proliferation Managed by Conservative Treatment
Pericoronal radiolucency associated with incomplete crown
 Imaging Science in entistry 2013; 43: 295-301 http://dx.doi.org/10.5624/isd.2013.43.4.295 Pericoronal radiolucency associated with incomplete crown Kyung-Soo Nah 1, * 1 epartment of Oral and Maxillofacial
Imaging Science in entistry 2013; 43: 295-301 http://dx.doi.org/10.5624/isd.2013.43.4.295 Pericoronal radiolucency associated with incomplete crown Kyung-Soo Nah 1, * 1 epartment of Oral and Maxillofacial
10/23/2014. features to image interpretation what to look for and what it means. interpretation vs. diagnosis. science or art? image investigation
 features to image interpretation what to look for and what it means interpretation vs. diagnosis ERNEST LAM, DMD, MSc, PhD, FRCD(C) PROFESSOR AND THE DR. LLOYD & MRS. KAY CHAPMAN CHAIR IN CLINICAL SCIENCES
features to image interpretation what to look for and what it means interpretation vs. diagnosis ERNEST LAM, DMD, MSc, PhD, FRCD(C) PROFESSOR AND THE DR. LLOYD & MRS. KAY CHAPMAN CHAIR IN CLINICAL SCIENCES
Erupting Compound Odontome - A case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. V. (Mar. 2014), PP 26-30 Erupting Compound Odontome - A case report Dr. Sahana Srinath
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. V. (Mar. 2014), PP 26-30 Erupting Compound Odontome - A case report Dr. Sahana Srinath
JOURNAL TAOMFR Mandiblular Ameloblastic fibro-odontoma
 Ameloblastic Fibro-Odontoma of the Mandible with Emphasis on Evaluation Using Cone Beam Computed Tomography Jing-Yi Chen 1, Frank Lei 2, Yu-Fong Chen 3,4 * Divisions of 1 Oral Pathology, 2 Periodotology,
Ameloblastic Fibro-Odontoma of the Mandible with Emphasis on Evaluation Using Cone Beam Computed Tomography Jing-Yi Chen 1, Frank Lei 2, Yu-Fong Chen 3,4 * Divisions of 1 Oral Pathology, 2 Periodotology,
Successful Conservative Surgical Treatment of Ameloblastic Fibroma in the Posterior Maxilla : A Case Report
 http://dx.doi.org/10.5933/jkapd.2013.40.4.321 ISSN (print) 1226-8496 Successful Conservative Surgical Treatment of Ameloblastic Fibroma in the Posterior Maxilla : A Case Report Youngeun Lee 1, Hyojung
http://dx.doi.org/10.5933/jkapd.2013.40.4.321 ISSN (print) 1226-8496 Successful Conservative Surgical Treatment of Ameloblastic Fibroma in the Posterior Maxilla : A Case Report Youngeun Lee 1, Hyojung
A Case Report on Surgical Management of Odontogenic Keratocyst
 World Journal of Medical Sciences 10 (2): 212-216, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.2.82185 A Case Report on Surgical Management of Odontogenic Keratocyst 1
World Journal of Medical Sciences 10 (2): 212-216, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.2.82185 A Case Report on Surgical Management of Odontogenic Keratocyst 1
COMBINED PERIODONTAL-ENDODONTIC LESION. By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur
 COMBINED PERIODONTAL-ENDODONTIC LESION By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur Differential diagnosis For differential diagnostic purposed the endo-perio
COMBINED PERIODONTAL-ENDODONTIC LESION By Dr. P.K. Agrawal Sr. Prof and Head Dept. Of Periodontia Govt. Dental College, Jaipur Differential diagnosis For differential diagnostic purposed the endo-perio
Key words: Third molar, Impacted tooth, Tooth Eruption, Molar, Mandible, Unerupted Tooth.
 JOURNAL OF CASE REPORTS 2014;4(2):286-290 OPG and CBCT Finding s of an Ectopic Third Molar in the Sub-condylar Region Tatu Joy E 1, Farakath Khan 1, Shameel Mohammed 2 From the Department of Oral Medicine
JOURNAL OF CASE REPORTS 2014;4(2):286-290 OPG and CBCT Finding s of an Ectopic Third Molar in the Sub-condylar Region Tatu Joy E 1, Farakath Khan 1, Shameel Mohammed 2 From the Department of Oral Medicine
AMELOBLASTIC FIBROMA: A RARE CASE REPORT
 Case Report International Journal of Dental and Health Sciences Volume 04, Issue 03 AMELOBLASTIC FIBROMA: A RARE CASE REPORT Namratha Patil 1 1.Sr lecturer, dept of oral medicine and radiology, KAHES VK
Case Report International Journal of Dental and Health Sciences Volume 04, Issue 03 AMELOBLASTIC FIBROMA: A RARE CASE REPORT Namratha Patil 1 1.Sr lecturer, dept of oral medicine and radiology, KAHES VK
AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH
 AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH e-issn - 2348-2184 Print ISSN - 2348-2176 Journal homepage: www.mcmed.us/journal/ajbpr SOLID AND MULTICYSTIC FOLLICULAR AMELOBLASTOMA - A CASE
AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH e-issn - 2348-2184 Print ISSN - 2348-2176 Journal homepage: www.mcmed.us/journal/ajbpr SOLID AND MULTICYSTIC FOLLICULAR AMELOBLASTOMA - A CASE
Odontogenic Cysts - An Overview
 Namita V Nayyer Michaelina Macluskey and William Keys Odontogenic Cysts - An Overview Abstract: This article aims to discuss the clinical features, radiological assessment, histopathology and management
Namita V Nayyer Michaelina Macluskey and William Keys Odontogenic Cysts - An Overview Abstract: This article aims to discuss the clinical features, radiological assessment, histopathology and management
Arun V Subramaniam et al. / International Journal of Biopharmaceutics. 2014; 5(3): International Journal of Biopharmaceutics
 225 e- ISSN 0976-1047 Print ISSN 2229-7499 International Journal of Biopharmaceutics Journal homepage: www.ijbonline.com IJB ODONTOGENIC KERATOCYSTS: VARIOUS RADIOGRAPHIC APPEARANCES Arun Subramaniam*
225 e- ISSN 0976-1047 Print ISSN 2229-7499 International Journal of Biopharmaceutics Journal homepage: www.ijbonline.com IJB ODONTOGENIC KERATOCYSTS: VARIOUS RADIOGRAPHIC APPEARANCES Arun Subramaniam*
Educational Cases EQA November T.J. Palmer Raigmore Hospital Inverness
 Educational Cases EQA November 2013 T.J. Palmer Raigmore Hospital Inverness Case 2 Clinical Details Dob 11 February 1951 PMH: 1964 Extraction of 45 aet 13 yr 1966 Cyst between 44 and 46 enucleated 1973
Educational Cases EQA November 2013 T.J. Palmer Raigmore Hospital Inverness Case 2 Clinical Details Dob 11 February 1951 PMH: 1964 Extraction of 45 aet 13 yr 1966 Cyst between 44 and 46 enucleated 1973
Chapter 5. Developmental Disorders. Copyright 2014, 2009, 2004, 2000, 1996, 1992 by Saunders, an imprint of Elsevier Inc 1
 Chapter 5 Developmental Disorders Copyright 2014, 2009, 2004, 2000, 1996, 1992 by Saunders, an imprint of Elsevier Inc 1 Outline Ø Embryonic Development of the Face, Oral Cavity, and Teeth Ø Developmental
Chapter 5 Developmental Disorders Copyright 2014, 2009, 2004, 2000, 1996, 1992 by Saunders, an imprint of Elsevier Inc 1 Outline Ø Embryonic Development of the Face, Oral Cavity, and Teeth Ø Developmental
Peripheral Odontogenic Fibroma: A rare case report
 Annals of Dental Research (2013) Vol 3 (1): 10-14 HATAM Publishers: All Rights Reserved Annals of Dental Research www.hgpub.com www.adres.yolasite.com Case Report Peripheral Odontogenic Fibroma: A rare
Annals of Dental Research (2013) Vol 3 (1): 10-14 HATAM Publishers: All Rights Reserved Annals of Dental Research www.hgpub.com www.adres.yolasite.com Case Report Peripheral Odontogenic Fibroma: A rare
MRI XR, CT, NM. Principal Modality (2): Case Report # 2. Date accepted: 15 March 2013
 Radiological Category: Musculoskeletal Principal Modality (1): Principal Modality (2): MRI XR, CT, NM Case Report # 2 Submitted by: Hannah Safia Elamir, D.O. Faculty reviewer: Naga R. Chinapuvvula, M.D.
Radiological Category: Musculoskeletal Principal Modality (1): Principal Modality (2): MRI XR, CT, NM Case Report # 2 Submitted by: Hannah Safia Elamir, D.O. Faculty reviewer: Naga R. Chinapuvvula, M.D.
Unicystic Ameloblastoma of mandible. Aggresive treatment A myth or a need. Case report and Extensive review of literature
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 12, Issue 2 (Nov.- Dec. 2013), PP 26-31 Unicystic Ameloblastoma of mandible. Aggresive treatment A myth
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 12, Issue 2 (Nov.- Dec. 2013), PP 26-31 Unicystic Ameloblastoma of mandible. Aggresive treatment A myth
Orthokeratinized Odontogenic Cyst: A Rarity
 aijoc AIJOC Case Report 1 Heena Sonawane, 2 Freny R Karjodkar, 3 Kaustubh Sansare, 4 Nimish Prakash ABSTRACT Orthokeratinized odontogenic cyst (OOC) was first identified as the rare variant of keratocystic
aijoc AIJOC Case Report 1 Heena Sonawane, 2 Freny R Karjodkar, 3 Kaustubh Sansare, 4 Nimish Prakash ABSTRACT Orthokeratinized odontogenic cyst (OOC) was first identified as the rare variant of keratocystic
CENTRAL GIANT CELL GRANULOMA PRESENTING AS UNILOCULAR RADIOLUCENCY IN POSTERIOR MANDIBLE A CASE REPORT
 IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Case Report CENTRAL GIANT CELL GRANULOMA PRESENTING AS UNILOCULAR RADIOLUCENCY IN POSTERIOR MANDIBLE A CASE REPORT S. Aruleena Shaminey 1, G.
IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Case Report CENTRAL GIANT CELL GRANULOMA PRESENTING AS UNILOCULAR RADIOLUCENCY IN POSTERIOR MANDIBLE A CASE REPORT S. Aruleena Shaminey 1, G.
Diagnostic value of dynamic contrast-enhanced MRI for unilocular cystic-type
 Diagnostic value of dynamic contrast-enhanced MRI for unilocular cystic-type ameloblastomas with homogeneously bright high signal intensity on T2-weighted or STIR MR images Miki Hisatomi a, Yoshinobu Yanagi
Diagnostic value of dynamic contrast-enhanced MRI for unilocular cystic-type ameloblastomas with homogeneously bright high signal intensity on T2-weighted or STIR MR images Miki Hisatomi a, Yoshinobu Yanagi
INFECTED DENTIGEROUS CYST IN IMPACTED CANINE- A case report
 Case Report INFECTED DENTIGEROUS CYST IN IMPACTED CANINE- A case report Gazala Fatima Parveen, M.D. Akheel 1 Department of oral & maxillofacial surgery, MCDRC Lucknow, U.P.,India 1-Department of Oral &
Case Report INFECTED DENTIGEROUS CYST IN IMPACTED CANINE- A case report Gazala Fatima Parveen, M.D. Akheel 1 Department of oral & maxillofacial surgery, MCDRC Lucknow, U.P.,India 1-Department of Oral &
FOCAL CEMENTO-OSSEOUS DYSPLASIA OF LOWER JAW IN AN ELDERLY WOMAN: CLINICOPATHOLOGICAL FEATURES AND MANAGEMENT IN A CASE REPORT
 www.djas.co.in ISSN No-31-148 DJAS 4(III), 08-1, 016 All rights are reserved CASE REPORT Dental JOURNAL of Advance Studies FOCAL CEMENTO-OSSEOUS DYSPLASIA OF LOWER JAW IN AN ELDERLY WOMAN: CLINICOPATHOLOGICAL
www.djas.co.in ISSN No-31-148 DJAS 4(III), 08-1, 016 All rights are reserved CASE REPORT Dental JOURNAL of Advance Studies FOCAL CEMENTO-OSSEOUS DYSPLASIA OF LOWER JAW IN AN ELDERLY WOMAN: CLINICOPATHOLOGICAL
EXTENSIVE PERIAPICAL CYST IN THE MAXILLARY SINUS A CASE REPORT
 May, 2012 INTERNATIONAL DENTAL JOURNAL OF STUDENT S RESEARCH: CASE REPORT Article Code: IDJSR 0002 EXTENSIVE PERIAPICAL CYST IN THE MAXILLARY SINUS A CASE REPORT Authors Bouguezzi Adel, DDS, Resident 1
May, 2012 INTERNATIONAL DENTAL JOURNAL OF STUDENT S RESEARCH: CASE REPORT Article Code: IDJSR 0002 EXTENSIVE PERIAPICAL CYST IN THE MAXILLARY SINUS A CASE REPORT Authors Bouguezzi Adel, DDS, Resident 1
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Orthokeratinized Odontogenic Cyst: A Case Report- A Milder Variant of OKC or an Independent Entity Mariyam
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Orthokeratinized Odontogenic Cyst: A Case Report- A Milder Variant of OKC or an Independent Entity Mariyam
An Expansile Large Odontogenic Keratocyst Maxilla: A Case Report.
 RESEARCH AND REVIEWS: JOURNAL OF DENTAL SCIENCES An Expansile Large Odontogenic Keratocyst Maxilla: A Case Report. Nasib Chand Khabra 1, Ish Pandhi 1 *, Kiran DN 2, Sunil Alipuria 1, Bhawna Gulati 1, and
RESEARCH AND REVIEWS: JOURNAL OF DENTAL SCIENCES An Expansile Large Odontogenic Keratocyst Maxilla: A Case Report. Nasib Chand Khabra 1, Ish Pandhi 1 *, Kiran DN 2, Sunil Alipuria 1, Bhawna Gulati 1, and
Ossifying fibromas of the jaw bone: 20 cases
 (2010) 39, 57 63 2010 The British Institute of Radiology http://dmfr.birjournals.org CASE REPORT Ossifying fibromas of the jaw bone: 20 cases Y Liu 1, M You 1, H Wang*,1, Z Yang 1, J Miao 1, K Shimizutani
(2010) 39, 57 63 2010 The British Institute of Radiology http://dmfr.birjournals.org CASE REPORT Ossifying fibromas of the jaw bone: 20 cases Y Liu 1, M You 1, H Wang*,1, Z Yang 1, J Miao 1, K Shimizutani
[ 06-10] Dr. B. Siva Reddy, Dr. B. Ajay Reginald, Dr. D. Sireesha, Dr. Meda Samatha India Abstract: Keywords ARTICLE 20/07/ /09/2018
![[ 06-10] Dr. B. Siva Reddy, Dr. B. Ajay Reginald, Dr. D. Sireesha, Dr. Meda Samatha India Abstract: Keywords ARTICLE 20/07/ /09/2018 [ 06-10] Dr. B. Siva Reddy, Dr. B. Ajay Reginald, Dr. D. Sireesha, Dr. Meda Samatha India Abstract: Keywords ARTICLE 20/07/ /09/2018](/thumbs/87/95905171.jpg) Dentigerous Cyst Associated with an Impacted Mesiodens: A Rare Case Report with Review of Literature [PP: 06-10] Dr. B. Siva Reddy, Dr. B. Ajay Reginald, Dr. D. Sireesha, Dr. Meda Samatha, Department of
Dentigerous Cyst Associated with an Impacted Mesiodens: A Rare Case Report with Review of Literature [PP: 06-10] Dr. B. Siva Reddy, Dr. B. Ajay Reginald, Dr. D. Sireesha, Dr. Meda Samatha, Department of
A Radiographic technique for differentiating enamel and dentin in odontogenic tumors
 ISPUB.COM The Internet Journal of Radiology Volume 12 Number 1 A Radiographic technique for differentiating enamel and dentin in odontogenic tumors D Shetty, A Urs, R Kaur Citation D Shetty, A Urs, R Kaur.
ISPUB.COM The Internet Journal of Radiology Volume 12 Number 1 A Radiographic technique for differentiating enamel and dentin in odontogenic tumors D Shetty, A Urs, R Kaur Citation D Shetty, A Urs, R Kaur.
Periapical central giant cell granuloma misdiagnosed as odontogenic cyst
 doi: 10.1111/j.1365-2591.2006.01107.x CLINICAL ARTICLE Periapical central giant cell granuloma misdiagnosed as odontogenic cyst T. Lombardi 1, M. Bischof 1,2, R. Nedir 1,2, D. Vergain 1, C. Galgano 3,
doi: 10.1111/j.1365-2591.2006.01107.x CLINICAL ARTICLE Periapical central giant cell granuloma misdiagnosed as odontogenic cyst T. Lombardi 1, M. Bischof 1,2, R. Nedir 1,2, D. Vergain 1, C. Galgano 3,
The resident will be assigned to be on call with the Oral and Maxillofacial service. Call will be set according to PARO guidelines.
 Goals and Objectives for the Otolaryngology-Head & Neck Resident on the Oral and Maxillofacial Surgery (OMFS) Rotation St. Catharines General Hospital (1 four-week rotational block) During the second year
Goals and Objectives for the Otolaryngology-Head & Neck Resident on the Oral and Maxillofacial Surgery (OMFS) Rotation St. Catharines General Hospital (1 four-week rotational block) During the second year
Autologous Bone Augmentation in Combination with an Ameloblastoma in the Maxillary Region- A Case Report?
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550023 Volume 2, Issue 2 Case Report Autologous Bone Augmentation in Combination with an Ameloblastoma in the Maxillary Region- A Case
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550023 Volume 2, Issue 2 Case Report Autologous Bone Augmentation in Combination with an Ameloblastoma in the Maxillary Region- A Case
Aneurysmal Bone Cyst of Mandible: A Case Report and Review of Literature
 CASE REPORT Aneurysmal Bone Cyst of Mandible: A Case Report and Review of Literature ABSTRACT An aneurysmal bone cyst is a rare benign expanding osteolytic lesion of bone characterized by replacement with
CASE REPORT Aneurysmal Bone Cyst of Mandible: A Case Report and Review of Literature ABSTRACT An aneurysmal bone cyst is a rare benign expanding osteolytic lesion of bone characterized by replacement with
Benign Fibro-osseous Lesions
 Benign Fibro-osseous Lesions Plus Vision is the art of seeing things invisible. Jonathan Swift 1667-1745 Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Benign Fibro-osseous Lesions A group of lesions
Benign Fibro-osseous Lesions Plus Vision is the art of seeing things invisible. Jonathan Swift 1667-1745 Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Benign Fibro-osseous Lesions A group of lesions
IMAGING NONODONTOGENIC TUMORS OF THE JAWBONES
 IMAGING NONODONTOGENIC TUMORS OF THE JAWBONES N. Serman. Sept, 2002 W. & P Ch. 20 + 21. Stafne & Gibilisco Ch 15 Oral and Maxillofacial diagnostic Imaging Ch. 8 Non agenesis or non eruption of teeth often
IMAGING NONODONTOGENIC TUMORS OF THE JAWBONES N. Serman. Sept, 2002 W. & P Ch. 20 + 21. Stafne & Gibilisco Ch 15 Oral and Maxillofacial diagnostic Imaging Ch. 8 Non agenesis or non eruption of teeth often
Squamous Cell Carcinoma Arising in a Residual Cyst: A Case Report
 Squamous Cell Carcinoma Arising in a Residual Cyst: A Case Report Abstract Aim: The purpose of this report is to present a case of squamous cell carcinoma (SCC) arising from a mandibular residual cyst.
Squamous Cell Carcinoma Arising in a Residual Cyst: A Case Report Abstract Aim: The purpose of this report is to present a case of squamous cell carcinoma (SCC) arising from a mandibular residual cyst.
Cone Beam Computed Tomography Findings in Calcifying Cystic Odontogenic Tumor Associated with Odontome: A Case Report
 Phulambrikar T., et al. Dent Shiraz Univ Med Sci., December 2015; 16(4): 374-379. Case Report Cone Beam Computed Tomography Findings in Calcifying Cystic Odontogenic Tumor Associated with Odontome: A Case
Phulambrikar T., et al. Dent Shiraz Univ Med Sci., December 2015; 16(4): 374-379. Case Report Cone Beam Computed Tomography Findings in Calcifying Cystic Odontogenic Tumor Associated with Odontome: A Case
An unusual site of Adenomatoid Odontogenic Tumor: A rare case report
 J. Int Oral Health 2010 Case Report All right reserved An unusual site of Adenomatoid Odontogenic Tumor: A rare case report Sapna Panjwani*, Anjana Bagewadi**, Vaishali Keluskar*** *Post Graduate Student
J. Int Oral Health 2010 Case Report All right reserved An unusual site of Adenomatoid Odontogenic Tumor: A rare case report Sapna Panjwani*, Anjana Bagewadi**, Vaishali Keluskar*** *Post Graduate Student
Treatment Modalities of Odontogenic Keratocyst of Maxilla and Mandible: Our Experience
 wjd Parveen Akhter Lone et al Original Research 10.5005/jp-journals-10015-1344 Treatment Modalities of Odontogenic Keratocyst of Maxilla and Mandible: Our Experience 1 Parveen Akhter Lone, 2 Mohan Singh,
wjd Parveen Akhter Lone et al Original Research 10.5005/jp-journals-10015-1344 Treatment Modalities of Odontogenic Keratocyst of Maxilla and Mandible: Our Experience 1 Parveen Akhter Lone, 2 Mohan Singh,
ANEURYSMAL BONE CYST OF MANDIBLE - A CASE REPORT
 Case Report Received : 23-07-2013 Review completed : 29-08-2013 Accepted : 04-09-2013 ANEURYSMAL BONE CYST OF MANDIBLE - A CASE REPORT V. V. N Pavan Kumar,* Madhumati Singh,** Sandeep Kashyap,*** Madan
Case Report Received : 23-07-2013 Review completed : 29-08-2013 Accepted : 04-09-2013 ANEURYSMAL BONE CYST OF MANDIBLE - A CASE REPORT V. V. N Pavan Kumar,* Madhumati Singh,** Sandeep Kashyap,*** Madan
SURGICAL'MANAGEMENT'OF' PLEXIFORM'AMELOBLASTOMA:'A' CASE'REPORT'
 HARSH,Ashutosh* PUROHIT,Pragya* PUROHIT,NC** ADLAKHA,Twisha*** SURGICALMANAGEMENTOF PLEXIFORMAMELOBLASTOMA:A CASEREPORT ABSTRACT Ameloblastoma is a benign but locally invasive neoplasm of odontogenicepithelium.patientsusuallypresentlateafterthetumor
HARSH,Ashutosh* PUROHIT,Pragya* PUROHIT,NC** ADLAKHA,Twisha*** SURGICALMANAGEMENTOF PLEXIFORMAMELOBLASTOMA:A CASEREPORT ABSTRACT Ameloblastoma is a benign but locally invasive neoplasm of odontogenicepithelium.patientsusuallypresentlateafterthetumor
Erupted odontomas: a report of two unusual cases
 ISSN: Printed version: 1806-7727 Electronic version: 1984-5685 RSBO. 2012 Apr-Jun;9(2):199-203 Case Report Article Erupted odontomas: a report of two unusual cases Santosh Patil¹ Farzan Rahman² Shoaib
ISSN: Printed version: 1806-7727 Electronic version: 1984-5685 RSBO. 2012 Apr-Jun;9(2):199-203 Case Report Article Erupted odontomas: a report of two unusual cases Santosh Patil¹ Farzan Rahman² Shoaib
DISEASES OF THE JAWS I
 DISEASES OF THE JAWS I ODONTOGENIC AND PERIODONTAL INFECTIONS ODONTOGENIC INFECTIONS PERIAPICAL GRANULOMA PERIAPICAL ABSCESS APICAL PERIODONTAL CYST PHOENIX ABSCESS FISTULA, DRAINING SINUS SPACE INFECTIONS
DISEASES OF THE JAWS I ODONTOGENIC AND PERIODONTAL INFECTIONS ODONTOGENIC INFECTIONS PERIAPICAL GRANULOMA PERIAPICAL ABSCESS APICAL PERIODONTAL CYST PHOENIX ABSCESS FISTULA, DRAINING SINUS SPACE INFECTIONS
Lec. 11 & 12 Dr. Ali H. Murad Dental pulp 1- Coronal pulp
 Lec. 11 & 12 Dr. Ali H. Murad Dental pulp Is the soft connective tissue located in the central portion of each tooth. All pulps have similar morphologic characteristic, such as a soft, gelatinous consistency
Lec. 11 & 12 Dr. Ali H. Murad Dental pulp Is the soft connective tissue located in the central portion of each tooth. All pulps have similar morphologic characteristic, such as a soft, gelatinous consistency
Case Studies in the Skull Base
 Case Studies in the Skull Base Amy C Tsai, MD Neuroradiology Fellow Department of Radiology and Imaging Sciences University of Utah Health Sciences Center Salt Lake City, Utah, USA No disclosures related
Case Studies in the Skull Base Amy C Tsai, MD Neuroradiology Fellow Department of Radiology and Imaging Sciences University of Utah Health Sciences Center Salt Lake City, Utah, USA No disclosures related
Clinical details: Details of scan: CONE BEAM CT REPORT: Name: H. B. Gender: Reason for referral: Referred by:
 Name: H. B. Gender: Male DOB: 11/12/1950 Age: 64 Date taken: 16/11/2015 Date reported: 19/11/2015 Clinical details: Reason for referral: Referred by: Investigate symptoms related to left TMJ. Reconstructed
Name: H. B. Gender: Male DOB: 11/12/1950 Age: 64 Date taken: 16/11/2015 Date reported: 19/11/2015 Clinical details: Reason for referral: Referred by: Investigate symptoms related to left TMJ. Reconstructed
The future of health is digital
 Dated: XX/XX/XXXX Name: XXXXXXXX XXXXXXXXXXX Birth Date: XX/XX/XXXX Date of scan: XX/XX/XXXX Examination of the anatomical volume: The following structures are reviewed and evaluated for bilateral symmetry,
Dated: XX/XX/XXXX Name: XXXXXXXX XXXXXXXXXXX Birth Date: XX/XX/XXXX Date of scan: XX/XX/XXXX Examination of the anatomical volume: The following structures are reviewed and evaluated for bilateral symmetry,
