Dana Lecture 2 Chronic Kidney Disease
|
|
|
- Margaret Farmer
- 6 years ago
- Views:
Transcription
1 Medicine Dr. Dana Lecture 2 Chronic Kidney Disease Chronic Kidney Disease Assessment of renal function Classification of CKD Why Chronic renal failure tends to progress Risk factors for progression Management of CKD Complications of CKD the Kidney Each kidney has: a renal artery, a renal vein, a ureter which enter the kidney at the hilum. The kidney has: an outer cortex layer, an inner medullary pyramid layer, fine branches of the ureter which form the calyx The NEPHRON is the functional unit of the kidney. Each kidney has nearly a million of nephrons. Each nephron: is supplied with an afferent arteriole, and produces urine which drains into a collecting duct. The collecting ducts fuse together to make larger and larger tubes until they join together as the ureter Each nephron consists of: a glomerulus & Bowman s capsule, a proximal convoluted tubule, a loop of Henle, a distal convoluted tubule Chronic Kidney Disease Longstanding and irreversible decline in renal function Injured nephrons replaced by extensive fibrosis Normal nephrons gradually fail due to hyperfilteration Is mainly TUBULAR scarring, so urine output usually normal, though urine quality reduced Any cause of AKI can eventually lead to CKD Assessment of renal function 60 years old woman - Creatinine 1.1 ( mg/dl) - Wt 48 Kg 20 years old man - Creatinine 1.4 ( mg/dl) - Wt 98 Kg 1
2 How do we assess renal function? Serum urea and creatinine - Small molecules - Filtered by glomerulus measure of GFR - But creatinine also depends on: + Muscle mass + Body size + Sex and race Measurement of GFR - Direct measurement - Estimation of GFR (egfr) Serum Creatinine Familiar But confounding factors: - Muscle mass - Nutrition - Race - Sex Not a linear relationship with GFR Staging of chronic kidney disease - K/DOQI guideline Stage GFR (ml/min) Description 1* 90 Normal kidney function but other evidence of kidney damage 2* Mild reduction in kidney function with other evidence of kidney damage Moderate kidney damage Severe kidney damage 5 <15 Established renal failure or end stage renal failure *Only considered to be CKD stage 1 or 2 if proteinuria and/or haematuria or structural renal disease are present. 2
3 CKD prevalence Stage 1: 3.3% Stage 2: 3.0% Stage 3: 4.3% Stage 4: 0.2% Stage 5: 0.2% Why is it important to identify patients with CKD? CKD predispose to increased cardiovascular risk (modify risk factors such as Hypertension) Some patient may benefit from other investigations ( such as renal biopsy) It may be possible to slow down the progression Complications of CKD can be identified and treated early Preparation for dialysis or transplantation once they reach end-stage.?acute or Chronic kidney impairment History and duration of symptoms Previous urinalysis or measurement of renal function Rapid changes in renal function Normocytic, normochromic anaemia( but haemorrhage, haemolysis) Ultrasound: small kidneys and increased echogenicity Evidence of renal osteodystrophy ( ie digital subperiosteal erosions) Who is at risk? Known CKD Hypertension Diabetes Unexplained oedema Congestive cardiac failure Atherosclerotic disease ( coronary, cerebral, peripheral) Multi systemic disease ( myeloma, SLE) Bladder outflow obstruction, neurogenic bladder, renal stone disease, recurrent UTI Chronic nephrotoxic use ( NSAID, ACEI, ARBII, ciclosporin, lithium) Urologically unexplained haematuria Why chronic renal failure tends to progress? Once CKD established, inexorable progression is likely While only 10% of those with CKD stage 3 may progress, all are at risk Therefore life-long follow up is desirable Mechanism of progression Raised intraglomerular pressure Glomerular damage Proteinuria Tubulo-intestitial scarring 3
4 Importance of proteinuria Normal glomeruli do not leak protein Proteinuria is a sign of glomerular dysfunction Proteinuria is also risk factor for progression of CKD Importance of proteinuria Normal glomeruli do not leak protein Proteinuria is a sign of glomerular dysfunction Proteinuria is also risk factor for progression of CKD Measures which reduce proteinuria slow down the progression of CKD* Albuminuria is a marker of cardiovascualr risk** Causes of End Stage Renal Disease* Case 1 Diabetes Glomerulonephritis Reflux nephropathy Renovascular disease Hypertension Polycystic kidney disease 55 years old male History of diabetes for 15 years He has CKD with egfr 35ml/min( checked 6 months ago). His BP was 140/90 and his doctor started him on Ramipril 2.5 mg two weeks ago. Lab results: egfr of 25ml/min otherwise well, HbA1c 6.0%, urinary protein excretion of 0.5g/24hrs ( no changes from previous results). What is the most likely cause of his renal deterioration? 1- Progression of his diabetic nephropathy 2- Uncontrolled hypertension 3- Infection 4- Drug induced 4
5 Reversible causes of deteriorating renal function Blood pressure control Diabetes control Obstruction Drug, contrast agent Intercurrent illness Exacerbation of underlying kidney disease (sarcoidosis, lupus) Preventing progression Blood pressure and diabetes - Uncontrolled Hypertension and diabetes makes proteinuria worse - Controlling hypertension and diabetes is vital ACE inhibitors and ARBs have antiproteinuric effects over and above their effects via blood pressure - Agents of choice in proteinuric renal disease - Even if blood pressure normal Blood pressure targets* CKD with no proteinuria: <140/90 mmhg CKD with proteinuria: <130/80 mmhg Diabetic nephropathy: <130/80mmHg (aim for 125/75 mmhg). Managing CKD 1- General advice: Smoking cessation Weight reduction if obese Encourage aerobic exercise Aspirin 75mg od ( if 10 years cardiovascular risk>20%) Treat hyperlipidaemia Avoid NSAID and other nephrotoxic drugs Limit alcohol intake( <21units/wk in male, <14units/wk in female Vaccination against influenza and pneumococcus 2- CKD stages 1-3: Monitor egfr, urinalysis and protein creatinine ratio Meticulous BP and diabetes control If Hb < 11g/dl check ferritin, B12 and folate( if ferritin <100mg/dl start on oral or IV iron) Annual check of PTH, Calcium and phosphate 5
6 3- CKD stages 4-5: Refer to nephrologist Full dietary assessment Optimize PTH, Calcium and phosphate Correct acidosis Hepatitis B immunization Discuss future treatment (dialysis, transplant or conservative/palliative) Complications of CKD/ESKD Uraemia Anaemia Renal bone disease Salt and water retention Electrolyte imbalance Acidosis Cardiovascular disease and lipids Salt and water retention Dietary salt restriction ( aim <5g/day) Fluid intake restriction Diuretics such as furosemide, titrate up Add thiazide ( metolazone) Those with fluid overload and on diuretics monitor: - Weight ( loss of 1kg/day) - BP control - Monitor electrolyte - if Ur > 70mg/dl consider reducing diuretics - Refractory volume overload = dialysis Hyperkalaemia Common and potentially fatal Rapid rise of K+ is more dangerous than gradual ones, as cell membrane stability is more vulnerable to acute changes K+ depolarization of the membrane resting potential Na+ channel inactivation membrane excitability neuromuscular depression and cardiac dysrhythmias. When to treat: K+: mmol/l: recheck routinely. Review medications and arrange dietary advice. K+: mmol/l: recheck urgently, review med, stop ACEI/ARB2 and arrange dietary advice. K+: >6.5 mmol/l: admit for emergency management 6
7 Measures to prevent K+ Dietary restriction: dairy products, potatoes and some fruits (such as banana, grapes, pineapple), fresh fruit juice, tomatoes, sweet corn, mushrooms, chocolate and coffee. Loop diuretics: promote urinary K+ excretion. Drug withdrawal or dose reduction (ACEI, ARB2), review other contributory drugs (spironolactone, NSAID and B-blockers) Correct acidosis. Dialysis ( especially in refractory K+) Acidosis Leads to: Bone: increase bone resorption and impaired mineralization, contributing to renal osteodystrophy. Over ventilation (compensatory mechanism) Hyperkalaemia Increased ionized Calcium (acidosis lead to reduced albumin bound fraction) Malnutrition: acidosis promotes catabolism How to correct acidosis? Treat when venous HCO3- is <21 mmol/l Give NaHCO3 tablet g/tds Refractory acidosis: dialysis Uraemia Clinical syndrome caused by substantial fall in GFR Failure to eliminate potentially toxic small and middle size molecules. NOT a result of high blood urea concentration. Ur and Cr are not directly toxic. Leads to: - Chronic inflammation and oxida ve stress - Accumulation of metabolic end products - Accelerated atherogenesis - Disruption of immune system - phosphate is retained: leads to PTH, arteriosclerosis and vascular Calcifica on - Nausea/ vomiting - Anorexia and weight loss - Malaise, fatigue - Confusion, fits and coma - Pericarditis 7
8 Anaemia Erythropoietin (EPO) is essential for the terminal maturation of erythrocyte EPO produced by the peritubular interstitial fibroblasts in the outer renal medulla and deep cortex in the kidney EPO deficiency occur in most advanced CKD (egfr < 35ml/min) with exception: Adult polycystic kidney disease Benign renal cysts Renal cell carcinoma Differential diagnosis of anaemia in CKD Case 2 EPO deficiency Iron deficiency anaemia Blood loss (GI tract, Haemodialysis) Folate deficiency B12 deficiency Haemolysis Myelodyplasia Myeloma 54 years old male with CKD stage 4 History or recurrent chest infection for the last 3months On oral co-amoxiclav, Erythropoietin injection 6000 iu sc weekly (increased recently) Lab results: Hb 8.5g/dl (no changes), WBC: 14, egfr: 16, CRP: 75, ferritin: 600 What is the most likely cause of EPO non-responsiveness 1. Non-compliance 2. Inadequate dose of EPO 3. High CRP 4. Iron deficiency anaemia EPO non-response Iron deficiency Chronic blood loss Infection/inflammation Severe hyperparathyroidism (causes bone marrow fibrosis) B 12 and folate deficiency Haemolysis Malnutrition Inadequate dosing Poor compliance 8
9 Renal bone disease (Osteodystrophy) Heterogeneous disorder leading to diminished bone strength Is a function of bone turnover, density, mineralization and architecture Mostly occur beyond CKD stage 3 High turnover (PTH > 450ng/L*): caused by secondary hyperparathyroidism leads to increased bone resorption and formation. Haphazardly organized (osteitis fibrosa cystica) Low turnover (Adynamic bone disease) (PTH < 100ng/L): paucity of cells with decreased bone resorption and formation. Pathophysiology poorly understood Osteomalacia: defect in mineralization, deficiency of 1,25(OH)2D Osteoporosis: reduced bone density Clinical features 1. Secondary hyperparathyroidism: Usually asymptomatic Bone pain and arthralgia Muscle weakness Pruritis (cutaneous calcium phosphate deposition) Bone deformity Increased fracture risks (hip fracture x5 in Dialysis) Marrow fibrosis contribute to anaemia 2. Adynamic bone disorder: asymptomatic and may have twice increase in fracture risk than dynamic bone disease. 3. Increased cardiovascular risk Treatment Measures to reduce serum phosphate: o Dietary PO 4 restriction (meat, egg, milk, cereals) o Dialysis o Oral phosphate binders (prevent absorption) such as Ca +2 and non-ca +2 containing phosphate binder Measures to increase serum calcium and suppress PTH: o Ca +2 salts (also act as PO 4 binder) o Vit D analogues (calciterol, alfacalcidol) Measures to suppress PTH directly: o Calcimimetic agents (cinacalcet) o Parathyroidectomy (tertiary PTH = PTH, Ca 2, PO 4 and ALP) Malnutrition Causes: Anorexic uraemic toxins ( leptin) Chronic low grade inflammation and oxidative stress. Dietary restriction (low protein diet) Medications (iron, PO4 binders) Acidosis Dialysis itself (protein loss during dialysis) Biochemical indicators: s. albumin, transferrin and cholesterol 9
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012
 Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
Irish Practice Nurses Association Annual Conference Tullamore Court Hotel OCTOBER 6 th 2012 Susan McKenna Renal Clinical Nurse Specialist Cavan General Hospital Renal patient population ACUTE RENAL FAILURE
The Renal System. David Carroll
 The Renal System David Carroll dcarroll06@qub.ac.uk https://www.davidontheinter.net Learning Objectives What you need to pass your exam Anatomy Physiology Pharmacology Pathophysiology Renal Anatomy Renal
The Renal System David Carroll dcarroll06@qub.ac.uk https://www.davidontheinter.net Learning Objectives What you need to pass your exam Anatomy Physiology Pharmacology Pathophysiology Renal Anatomy Renal
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
The Renal System. Dr Noel Sharkey
 The Renal System Dr Noel Sharkey Learning Objectives Function Anatomy Physiology Pharmacology Pathophysiology The Function of the Kidney Excretion - Urea - Metabolites - Drugs Regulation - BP control (RAAS)
The Renal System Dr Noel Sharkey Learning Objectives Function Anatomy Physiology Pharmacology Pathophysiology The Function of the Kidney Excretion - Urea - Metabolites - Drugs Regulation - BP control (RAAS)
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Chronic Kidney Disease. Basics of CKD Terms Diagnosis Management
 Chronic Kidney Disease Basics of CKD Terms Diagnosis Management Review the prevalence of chronic kidney disease (CKD) Review how CKD develops Review populations at risk for CKD Review CKD diagnosis Objectives
Chronic Kidney Disease Basics of CKD Terms Diagnosis Management Review the prevalence of chronic kidney disease (CKD) Review how CKD develops Review populations at risk for CKD Review CKD diagnosis Objectives
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus
 Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
Swindon Diabetes Guidelines: Management of Chronic Kidney Disease Associated with Diabetes Mellitus 1 Contents Executive Summary... 3 How to Screen for Diabetic Nephropathy... 4 What to Measure... 4 Frequency
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009
 The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
The Diabetes Kidney Disease Connection Missouri Foundation for Health February 26, 2009 Teresa Northcutt, RN BSN Primaris Program Manager, Prevention - CKD MO-09-01-CKD This material was prepared by Primaris,
Chronic Kidney Disease
 Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
Chronic Kidney Disease Presence of kidney damage or decreased kidney function for three or more months, - necessary to distinguish CKD from acute kidney disease. Ascertained either by kidney biopsy or
QUICK REFERENCE FOR HEALTHCARE PROVIDERS
 KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
KEY MESSAGES 1 SCREENING CRITERIA Screen: Patients with DM and/or hypertension at least yearly. Consider screening patients with: Age >65 years old Family history of stage 5 CKD or hereditary kidney disease
Chronic Kidney Disease in Primary Care
 Clinical Stream Chronic Kidney Disease in Primary Care Dr Gerald Waters Dr Gerald Waters Renal Physician Chronic Kidney Disease Chronic Kidney Disease Normal functions of Kidneys Management of CKD Drugs
Clinical Stream Chronic Kidney Disease in Primary Care Dr Gerald Waters Dr Gerald Waters Renal Physician Chronic Kidney Disease Chronic Kidney Disease Normal functions of Kidneys Management of CKD Drugs
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
The hypertensive kidney and its Management
 The hypertensive kidney and its Management Dr H0 Chung Ping Hypertension Management Seminar 20061124 Hypertensive kidney Kidney damage asymptomatic till late stage Viscous cycle to augment renal damage
The hypertensive kidney and its Management Dr H0 Chung Ping Hypertension Management Seminar 20061124 Hypertensive kidney Kidney damage asymptomatic till late stage Viscous cycle to augment renal damage
CKD FOR INTERNISTS. Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College
 CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CKD FOR INTERNISTS Dr Ahmed Hossain Associate professor Medicine Sir Salimullah Medical College INTRODUCTION In 2002, the National Kidney Foundation s Kidney Disease Outcomes Quality Initiative(KDOQI)
CHRONIC KIDNEY DISEASE (CKD)
 CHRONIC KIDNEY DISEASE (CKD) CKD implies longstanding (more than 3 months), and usually progressive, impairment in renal function. In many instances, no effective means are available to reverse the primary
CHRONIC KIDNEY DISEASE (CKD) CKD implies longstanding (more than 3 months), and usually progressive, impairment in renal function. In many instances, no effective means are available to reverse the primary
Dr.Nahid Osman Ahmed 1
 1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
CHRONIC RENAL FAILURE: WHAT THE PRIMARY CARE CAN OFFER. The annual conference of the Lebanese Society of Family Medicine October 2017 Dr Hiba AZAR
 CHRONIC RENAL FAILURE: WHAT THE PRIMARY CARE CAN OFFER The annual conference of the Lebanese Society of Family Medicine October 2017 Dr Hiba AZAR OUTLINE: A journey through CKD Screening for CKD: The why,
CHRONIC RENAL FAILURE: WHAT THE PRIMARY CARE CAN OFFER The annual conference of the Lebanese Society of Family Medicine October 2017 Dr Hiba AZAR OUTLINE: A journey through CKD Screening for CKD: The why,
Office Management of Reduced GFR Practical advice for the management of CKD
 Office Management of Reduced GFR Practical advice for the management of CKD CKD Online Education CME for Primary Care April 27, 2016 Monica Beaulieu, MD FRCPC MHA CHAIR PROVINCIAL KIDNEY CARE COMMITTEE
Office Management of Reduced GFR Practical advice for the management of CKD CKD Online Education CME for Primary Care April 27, 2016 Monica Beaulieu, MD FRCPC MHA CHAIR PROVINCIAL KIDNEY CARE COMMITTEE
General Anatomy of Urinary System
 General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
CHRONIC KIDNEY FAILURE
 CHRONIC KIDNEY FAILURE Overview Chronic kidney disease, also called chronic kidney failure, describes the gradual loss of kidney function. Your kidneys filter wastes and excess fluids from your blood,
CHRONIC KIDNEY FAILURE Overview Chronic kidney disease, also called chronic kidney failure, describes the gradual loss of kidney function. Your kidneys filter wastes and excess fluids from your blood,
AP2, Lab 7 - THE URINARY SYSTEM
 AP2, Lab 7 - THE URINARY SYSTEM I. SYSTEM COMPONENTS (Figs. 25.1 25.4) KIDNEYS Each kidney contains approx. 1,000,000 tubular NEPHRONS which produce FILTRATE from the plasma and then add to or take from
AP2, Lab 7 - THE URINARY SYSTEM I. SYSTEM COMPONENTS (Figs. 25.1 25.4) KIDNEYS Each kidney contains approx. 1,000,000 tubular NEPHRONS which produce FILTRATE from the plasma and then add to or take from
The UK Renal Registry collects national data about the causes and treatment of kidney failure.
 1 Kidney failure is a serious condition. Many kidney patients receive some form of renal replacement therapy (RRT) such as dialysis. The UK Renal Registry collects national data about the causes and treatment
1 Kidney failure is a serious condition. Many kidney patients receive some form of renal replacement therapy (RRT) such as dialysis. The UK Renal Registry collects national data about the causes and treatment
CKD & HT. Anne-Marie Angus
 CKD & HT Anne-Marie Angus Hypertension definitions Persisting BP >140/90 and HBPM >135/85 Stage 1 >140/90 (HBPM >135/85) Stage 2 >160/100 (HBPM >150/90) Severe >180/100 White coat HT Why treat? A major
CKD & HT Anne-Marie Angus Hypertension definitions Persisting BP >140/90 and HBPM >135/85 Stage 1 >140/90 (HBPM >135/85) Stage 2 >160/100 (HBPM >150/90) Severe >180/100 White coat HT Why treat? A major
Professor Suetonia Palmer
 Professor Suetonia Palmer Department of Medicine Nephrologist Christchurch Hospital Christchurch 14:00-14:55 WS #108: The Kidney Test - When To Test and When to Refer ( and When Not To) 15:05-16:00 WS
Professor Suetonia Palmer Department of Medicine Nephrologist Christchurch Hospital Christchurch 14:00-14:55 WS #108: The Kidney Test - When To Test and When to Refer ( and When Not To) 15:05-16:00 WS
The Urinary System. Maintenance Systems Unit 5
 The Urinary System Maintenance Systems Unit 5 Basic Functions of the Urinary System Regulates the composition and volume of the blood by removing and restoring selected amounts of water and solutes. Eliminates
The Urinary System Maintenance Systems Unit 5 Basic Functions of the Urinary System Regulates the composition and volume of the blood by removing and restoring selected amounts of water and solutes. Eliminates
Chronic kidney disease in cats
 Chronic kidney disease in cats What is chronic kidney disease (CKD)? Chronic kidney disease (CKD) is the name now used to refer to cats with kidney failure (or chronic kidney failure). CKD is one of the
Chronic kidney disease in cats What is chronic kidney disease (CKD)? Chronic kidney disease (CKD) is the name now used to refer to cats with kidney failure (or chronic kidney failure). CKD is one of the
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
A. Correct! Flushing acids from the system will assist in re-establishing the acid-base equilibrium in the blood.
 OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
Identifying and Managing Chronic Kidney Disease: A Practical Approach
 Identifying and Managing Chronic Kidney Disease: A Practical Approach S. Neil Finkle, MD, FRCPC Associate Professor Division of Nephrology, Department of Medicine, Dalhousie University Program Director,
Identifying and Managing Chronic Kidney Disease: A Practical Approach S. Neil Finkle, MD, FRCPC Associate Professor Division of Nephrology, Department of Medicine, Dalhousie University Program Director,
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Mr PA. Clinical assessment of hydration. Poor urine output Sunken eyes Moistness of mucosa Cool peripheries Reduction in weight Postural hypotension
 X Anthony Warrens Mr PA 54 years old Previously well Went to Thailand Developed serious diarrhoea and vomiting two days before coming home 24 hours after return, still unwell GP found: urea 24 mmol/l creatinine
X Anthony Warrens Mr PA 54 years old Previously well Went to Thailand Developed serious diarrhoea and vomiting two days before coming home 24 hours after return, still unwell GP found: urea 24 mmol/l creatinine
Chronic Kidney Disease The 6 Pillars. Dr. Tiina Podymow Associate Professor Division of Nephrology McGill University Health Centre
 Chronic Kidney Disease The 6 Pillars Dr. Tiina Podymow Associate Professor Division of Nephrology McGill University Health Centre None Disclosures Objectives 1. Describe evidence-based measures to slow
Chronic Kidney Disease The 6 Pillars Dr. Tiina Podymow Associate Professor Division of Nephrology McGill University Health Centre None Disclosures Objectives 1. Describe evidence-based measures to slow
5/10/2014. Observation, control of blood pressure. Observation, control of blood pressure and risk factors.
 Overview The Kidneys Nicola Barlow Clinical Biochemistry Department City Hospital Renal physiology Renal pathophysiology Acute kidney injury Chronic kidney disease Assessing renal function GFR Proteinuria
Overview The Kidneys Nicola Barlow Clinical Biochemistry Department City Hospital Renal physiology Renal pathophysiology Acute kidney injury Chronic kidney disease Assessing renal function GFR Proteinuria
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University
 RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Acute Kidney Injury (AKI) Undergraduate nurse education
 Acute Kidney Injury (AKI) Undergraduate nurse education Year One Developed Summer 2017 Overview Basic A & P of: Urinary system Kidneys Followed by: Introduction to Acute Kidney Injury Urinary System The
Acute Kidney Injury (AKI) Undergraduate nurse education Year One Developed Summer 2017 Overview Basic A & P of: Urinary system Kidneys Followed by: Introduction to Acute Kidney Injury Urinary System The
Elevated Serum Creatinine, a simplified approach
 Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
* It is proportionate to body size and the reference value is usually expressed after correction for body surface area as 120 ± 25 ml/min/1.
 Ahmad Al-zoubi Glomerular filtration rate : is the sum of the ultrafiltration rates from plasma into the Bowman s space in each nephron and is a measure of renal excretory function *co : 6L *renal blood
Ahmad Al-zoubi Glomerular filtration rate : is the sum of the ultrafiltration rates from plasma into the Bowman s space in each nephron and is a measure of renal excretory function *co : 6L *renal blood
The Excretory System
 The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
A patient guide to membranous nephropathy
 A patient guide to membranous nephropathy Queen Elizabeth Hospital Kidney Care Department UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
A patient guide to membranous nephropathy Queen Elizabeth Hospital Kidney Care Department UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma. Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree
 Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree Topics CKD background egfr background Patient with egfr Referral Guidelines
Chronic Kidney Disease (CKD) and egfr: Decision and Dilemma Dr Bhavna K Pandya Consultant Nephrologist University Hospital Aintree Topics CKD background egfr background Patient with egfr Referral Guidelines
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERENCE CARDS Chronic Kidney Disease
 VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERECE CARDS Chronic Kidney Disease CKD VA/DoD Clinical Practice Guideline for the Management
VA/DoD Clinical Practice Guideline for the Management of Chronic Kidney Disease in Primary Care (2008) PROVIDER REFERECE CARDS Chronic Kidney Disease CKD VA/DoD Clinical Practice Guideline for the Management
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
The Urinary System. Medical Assisting Third Edition. Booth, Whicker, Wyman, Pugh, Thompson The McGraw-Hill Companies, Inc. All rights reserved
 The Urinary System PowerPoint presentation to accompany: Medical Assisting Third Edition Booth, Whicker, Wyman, Pugh, Thompson 30-2 Learning Outcomes 30.1 Describe the structure, location, and functions
The Urinary System PowerPoint presentation to accompany: Medical Assisting Third Edition Booth, Whicker, Wyman, Pugh, Thompson 30-2 Learning Outcomes 30.1 Describe the structure, location, and functions
Stages of Chronic Kidney Disease (CKD)
 Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Early Treatment is the Key Stages of Chronic Kidney Disease (CKD) Stage Description GFR (ml/min/1.73 m 2 ) >90 1 Kidney damage with normal or GFR 2 Mild decrease in GFR 60-89 3 Moderate decrease in GFR
Case study Group 2 presentation
 Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Acute renal failure ARF
 Acute renal failure ARF Definition ARF is a clinical syndrome characterized by an abrupt decline in GFR and the accumulation of nitrogenous waste (BUN & creatinine). The decrease in GFR occurs relatively
Acute renal failure ARF Definition ARF is a clinical syndrome characterized by an abrupt decline in GFR and the accumulation of nitrogenous waste (BUN & creatinine). The decrease in GFR occurs relatively
Diabetes in Renal Patients. Contents. Understanding Diabetic Nephropathy
 Diabetes in Renal Patients Contents Understanding Diabetic Nephropathy What effect does CKD have on a patient s diabetic control? Diabetic Drugs in CKD and Dialysis Patients Hyper and Hypoglycaemia in
Diabetes in Renal Patients Contents Understanding Diabetic Nephropathy What effect does CKD have on a patient s diabetic control? Diabetic Drugs in CKD and Dialysis Patients Hyper and Hypoglycaemia in
Applying clinical guidelines treating and managing CKD
 Applying clinical guidelines treating and managing CKD Develop patient treatment plan according to level of severity. Source: Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012
Applying clinical guidelines treating and managing CKD Develop patient treatment plan according to level of severity. Source: Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Make an appointment with your doctor if you have any signs or symptoms of acute kidney failure.
 Acute Kidney Failure Acute kidney failure occurs when your kidneys suddenly become unable to filter waste products from your blood. When your kidneys lose their filtering ability, dangerous levels of wastes
Acute Kidney Failure Acute kidney failure occurs when your kidneys suddenly become unable to filter waste products from your blood. When your kidneys lose their filtering ability, dangerous levels of wastes
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
HIHIM 409 7/26/2009. Kidney and Nephron. Fermamdo Vega, M.D. 1
 Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
12/7/10. Excretory System. The basic function of the excretory system is to regulate the volume and composition of body fluids by:
 Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Biology Slide 1 of 36
 Biology 1 of 36 38 3 The Excretory System 2 of 36 Functions of the Excretory System 1.Function: process which eliminates metabolic wastes 3 of 36 Functions of the Excretory System (The skin excretes excess
Biology 1 of 36 38 3 The Excretory System 2 of 36 Functions of the Excretory System 1.Function: process which eliminates metabolic wastes 3 of 36 Functions of the Excretory System (The skin excretes excess
6/10/2014. Chronic Kidney Disease - General management and standard of care. Management of CKD according to stage (KDOQI 2002)
 Chronic Kidney Disease - General management and standard of care Dr Nathalie Demoulin, Prof Michel Jadoul Cliniques universitaires Saint-Luc Université Catholique de Louvain What should and can be done
Chronic Kidney Disease - General management and standard of care Dr Nathalie Demoulin, Prof Michel Jadoul Cliniques universitaires Saint-Luc Université Catholique de Louvain What should and can be done
The future is here. It s just not widely distributed yet. William Gibson
 The future is here. It s just not widely distributed yet. William Gibson CHRONIC KIDNEY DISEASE MANAGEMENT A NEW PARADIGM Aaron Cass, MD, FRCPC Nephrologist, Fraser Health January 22, 2014 Where Are We
The future is here. It s just not widely distributed yet. William Gibson CHRONIC KIDNEY DISEASE MANAGEMENT A NEW PARADIGM Aaron Cass, MD, FRCPC Nephrologist, Fraser Health January 22, 2014 Where Are We
Unit #4 Waste and Excretion. The Kidneys
 Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
Chapter 12. Excretion and the Interaction of Systems
 Chapter 12 Excretion and the Interaction of Systems 1 2 Goals for This Chapter 1. Identify the main structures and functions of the human excretory system 2. Explain the function of the nephron 3. Describe
Chapter 12 Excretion and the Interaction of Systems 1 2 Goals for This Chapter 1. Identify the main structures and functions of the human excretory system 2. Explain the function of the nephron 3. Describe
network of thin-walled capillaries closely surrounded by a pear-shaped epithelial membrane called the Bowman s capsule
 Renal Terminology Renal-Root Words & Combining Forms calyx cortex glomerul/o medulla nephr/o pyel/o py/o ur/o ren/o cuplike division of the kidney outer layer of kidney glomerula inner or central portion
Renal Terminology Renal-Root Words & Combining Forms calyx cortex glomerul/o medulla nephr/o pyel/o py/o ur/o ren/o cuplike division of the kidney outer layer of kidney glomerula inner or central portion
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Outpatient Management of Chronic Kidney Disease for the Internist
 Outpatient Management of Chronic Kidney Disease for the Internist Annual Meeting of Maryland Chapter of the American College of Physicians February 3, 2018 MARY (TESSIE) BEHRENS, MD, FACP, FASN, FNKF MID-ATLANTIC
Outpatient Management of Chronic Kidney Disease for the Internist Annual Meeting of Maryland Chapter of the American College of Physicians February 3, 2018 MARY (TESSIE) BEHRENS, MD, FACP, FASN, FNKF MID-ATLANTIC
Management of early chronic kidney disease
 Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
Management of early chronic kidney disease GREENLANE SUMMER GP SYMPOSIUM 2018 Jonathan Hsiao Renal and General Physician Introduction A growing public health problem in NZ and throughout the world. Unknown
Nephrology. 3 rd Year Revision Session 06/05/17 Cathal Hannan
 Nephrology 3 rd Year Revision Session 06/05/17 Cathal Hannan Aims Acute Kidney Injury-recognition and management Sample OSCE Station Clinically relevant renal physiology Aetiology of Chronic Kidney Disease
Nephrology 3 rd Year Revision Session 06/05/17 Cathal Hannan Aims Acute Kidney Injury-recognition and management Sample OSCE Station Clinically relevant renal physiology Aetiology of Chronic Kidney Disease
Chapter 10: Urinary System & Excretion
 Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
Case Study: Chronic Kidney Disease
 Taylor Zwimpfer Joan Rupp Nutrition 409 23 September 2014 Case Study: Chronic Kidney Disease 1. Kidneys act to maintain the balance of fluids, electrolytes and organic solutes in the body through filtration
Taylor Zwimpfer Joan Rupp Nutrition 409 23 September 2014 Case Study: Chronic Kidney Disease 1. Kidneys act to maintain the balance of fluids, electrolytes and organic solutes in the body through filtration
HEALTHYSTART TRAINING MANUAL. Living well with Kidney Disease
 HEALTHYSTART TRAINING MANUAL Living well with Kidney Disease KIDNEY DISEASE CAN AFFECT ANYONE! 1 HEALTHYSTART PROGRAMME HEALTHYSTART is a lifestyle management programme to assist you to remain healthy
HEALTHYSTART TRAINING MANUAL Living well with Kidney Disease KIDNEY DISEASE CAN AFFECT ANYONE! 1 HEALTHYSTART PROGRAMME HEALTHYSTART is a lifestyle management programme to assist you to remain healthy
Urinary system. Urinary system
 INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
URINARY SYSTEM CHAPTER 28 I ANATOMY OF THE URINARY SYSTEM. Student Name
 Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Introduction to Clinical Diagnosis Nephrology
 Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
Doncaster & Bassetlaw. AKI guidelines for primary care
 Doncaster & Bassetlaw AKI guidelines for primary care Contents: FLOW DIAGRAM: MANAGEMENT OF PATIENTS WITH AKI DETECTED IN PRIMARY CARE... 2 FLOW DIAGRAM: MANAGEMENT OF HYPERKALAEMIA.... 3 FLOW DIAGRAM:
Doncaster & Bassetlaw AKI guidelines for primary care Contents: FLOW DIAGRAM: MANAGEMENT OF PATIENTS WITH AKI DETECTED IN PRIMARY CARE... 2 FLOW DIAGRAM: MANAGEMENT OF HYPERKALAEMIA.... 3 FLOW DIAGRAM:
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Outline the functional anatomy, and the physiological factors, that determine oxygen delivery to the renal medulla.
 2011-2-21 Outline the functional anatomy, and the physiological factors, that determine oxygen delivery to the renal medulla. Oxygen delivery = Blood flow CaO 2 Where Blood flow determined by (arterial
2011-2-21 Outline the functional anatomy, and the physiological factors, that determine oxygen delivery to the renal medulla. Oxygen delivery = Blood flow CaO 2 Where Blood flow determined by (arterial
Screen annually for patients with any of the following risk factors:
 CASE DEFINITION Chronic Kidney Disease (CKD) is either of the following, persisting for at least three months, repeated on at least two occasions: 1. Markers of kidney damage (e.g. proteinuria, haematuria
CASE DEFINITION Chronic Kidney Disease (CKD) is either of the following, persisting for at least three months, repeated on at least two occasions: 1. Markers of kidney damage (e.g. proteinuria, haematuria
Excretion: is the removal of waste products formed by metabolism, out of the body
 Excretion in Humans Excretion: is the removal of waste products formed by metabolism, out of the body Accumulation of wastes in the cells would affect the normal functioning of the cells By getting rid
Excretion in Humans Excretion: is the removal of waste products formed by metabolism, out of the body Accumulation of wastes in the cells would affect the normal functioning of the cells By getting rid
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Science of Veterinary Medicine. Urinary System Unit Handouts
 Science of Veterinary Medicine Urinary System Unit Handouts Urinary System Functions of the Urinary System Elimination of waste products Regulate aspects of homeostasis Organs of the Urinary system The
Science of Veterinary Medicine Urinary System Unit Handouts Urinary System Functions of the Urinary System Elimination of waste products Regulate aspects of homeostasis Organs of the Urinary system The
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
19. RENAL PHYSIOLOGY ROLE OF THE URINARY SYSTEM THE URINARY SYSTEM. Components and function. V BS 122 Physiology II 151 Class of 2011
 19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure
 EXCRETORY SYSTEM WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure These wastes include: Carbon dioxide Mostly through breathing
EXCRETORY SYSTEM WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure These wastes include: Carbon dioxide Mostly through breathing
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
EXCRETION IN HUMANS 31 JULY 2013
 EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
Acute Kidney Injury (AKI) Undergraduate nurse education
 Acute Kidney Injury (AKI) Undergraduate nurse education Year Three Developed Summer 2017 Objectives Understand Acute Kidney Injury and its relevance to patient care. Brief revision of the Anatomy and physiology
Acute Kidney Injury (AKI) Undergraduate nurse education Year Three Developed Summer 2017 Objectives Understand Acute Kidney Injury and its relevance to patient care. Brief revision of the Anatomy and physiology
Chronic kidney disease (CKD) (Southampton pathway)
 Background information Patient information Key messages for this pathway Definitions and abbreviations used in this pathway Classification of CKD Diagnosis of CKD Summary of referral criteria Screening
Background information Patient information Key messages for this pathway Definitions and abbreviations used in this pathway Classification of CKD Diagnosis of CKD Summary of referral criteria Screening
Hypertension diagnosis (see detail document) Diabetic. Target less than 130/80mmHg
 Hypertension diagnosis (see detail document) Non-diabetic Diabetic Very elderly (older than 80 years) Target less than 140/90mmHg Target less than 130/80mmHg Consider SBP target less than 150mmHg Non-diabetic
Hypertension diagnosis (see detail document) Non-diabetic Diabetic Very elderly (older than 80 years) Target less than 140/90mmHg Target less than 130/80mmHg Consider SBP target less than 150mmHg Non-diabetic
The Urinary S. (Chp. 10) & Excretion. What are the functions of the urinary system? Maintenance of water-salt and acidbase
 10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
** Accordingly GFR can be estimated by using one urine sample and do creatinine testing.
 This sheet includes the lecture and last year s exam. When a patient goes to a clinic, we order 2 tests: 1) kidney function test: in which we measure UREA and CREATININE levels, and electrolytes (Na+,
This sheet includes the lecture and last year s exam. When a patient goes to a clinic, we order 2 tests: 1) kidney function test: in which we measure UREA and CREATININE levels, and electrolytes (Na+,
The Urinary System 15PART A. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART A Functions of the Urinary System Elimination of waste products Nitrogenous
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART A Functions of the Urinary System Elimination of waste products Nitrogenous
What should you do next? Presenter Disclosure Information. Learning Objectives. Case: George
 2:45 3:45pm Optimizing the Management of Patients with Chronic Kidney Disease SPEAKER Jay B. Wish, MD, FACP Presenter Disclosure Information The following relationships exist related to this presentation:
2:45 3:45pm Optimizing the Management of Patients with Chronic Kidney Disease SPEAKER Jay B. Wish, MD, FACP Presenter Disclosure Information The following relationships exist related to this presentation:
Chapter 23. The Nephron. (functional unit of the kidney
 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
CHRONIC KIDNEY DISEASE DIAGNOSIS
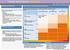 CHRONIC KIDNEY DISEASE DIAGSIS GFR categories, description and range WHO SHOULD BE TESTED FOR CKD CLASSIFICATION OF CKD USING egfr AND ACR CATEGORIES Offer testing for CKD using egfr, creatinine and ACR
CHRONIC KIDNEY DISEASE DIAGSIS GFR categories, description and range WHO SHOULD BE TESTED FOR CKD CLASSIFICATION OF CKD USING egfr AND ACR CATEGORIES Offer testing for CKD using egfr, creatinine and ACR
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
WEEK. MPharm Programme. Acute Kidney Injury. Alan M. Green MPHM13: Acute Kidney Injury. Slide 1 of 47
 MPharm Programme Acute Kidney Injury Alan M. Green 2017 Slide 1 of 47 Overview Renal Function What is it? Why does it matter? What causes it? Who is at risk? What can we (Pharmacists) do? How do you recognise
MPharm Programme Acute Kidney Injury Alan M. Green 2017 Slide 1 of 47 Overview Renal Function What is it? Why does it matter? What causes it? Who is at risk? What can we (Pharmacists) do? How do you recognise
Disclosures. Topics. Staging and GFR. K-DOQI Staging of Chronic Kidney Disease. Definition of Chronic Kidney Disease. Chronic Kidney Disease
 Disclosures Chronic Kidney Disease Consultant: Baxter Healthcare J. Kevin Tucker, M.D. Brigham and Women s Hospital Massachusetts General Hospital Topics Staging of chronic kidney disease (CKD) How to
Disclosures Chronic Kidney Disease Consultant: Baxter Healthcare J. Kevin Tucker, M.D. Brigham and Women s Hospital Massachusetts General Hospital Topics Staging of chronic kidney disease (CKD) How to
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
