Can ketones compensate for deteriorating brain glucose uptake during aging? Implications for the risk and treatment of Alzheimer s disease
|
|
|
- Aron McCormick
- 5 years ago
- Views:
Transcription
1 Ann. N.Y. Acad. Sci. ISSN ANNALS OF THE NEW YORK ACADEMY OF SCIENCES Issue: Nutrition in Prevention and Management of Dementia Can ketones compensate for deteriorating brain glucose uptake during aging? Implications for the risk and treatment of Alzheimer s disease Stephen C. Cunnane, 1,2,3 Alexandre Courchesne-Loyer, 1,3 Valérie St-Pierre, 1,3 Camille Vandenberghe, 1,3 Tyler Pierotti, 1,4 Mélanie Fortier, 1 Etienne Croteau, 1 and Christian-Alexandre Castellano 1 1 Research Center on Aging, and 2 Departments of Medicine and 3 Pharmacology and Physiology, Université de Sherbrooke, Sherbrooke, Québec, Canada. 4 Department of Biology, Bishop s University, Sherbrooke, Québec, Canada Address for correspondence: Stephen C. Cunnane, Research Center on Aging, 1036 Belvedere St. South, Sherbrooke, Québec, Canada J1H 4C4. stephen.cunnane@usherbrooke.ca Brain glucose uptake is impaired in Alzheimer s disease (AD). A key question is whether cognitive decline can be delayed if this brain energy defect is at least partly corrected or bypassed early in the disease. The principal ketones (also called ketone bodies), -hydroxybutyrate and acetoacetate, are the brain s main physiological alternative fuel to glucose. Three studies in mild-to-moderate AD have shown that, unlike with glucose, brain ketone uptake is not different from that in healthy age-matched controls. Published clinical trials demonstrate that increasing ketone availability to the brain via moderate nutritional ketosis has a modest beneficial effect on cognitive outcomes in mildto-moderate AD and in mild cognitive impairment. Nutritional ketosis can be safely achieved by a high-fat ketogenic diet, by supplements providing g/day of medium-chain triglycerides containing the eight- and ten-carbon fatty acids octanoate and decanoate, or by ketone esters. Given the acute dependence of the brain on its energy supply, it seems reasonable that the development of therapeutic strategies aimed at AD mandates consideration of how the underlying problem of deteriorating brain fuel supply can be corrected or delayed. Keywords: Alzheimer s disease; glucose; ketones; beta-hydroxybutyrate ( -HB); acetoacetate (AcAc); medium-chain triglycerides (MCT) Introduction The adult brain requires a disproportionately large energy supply; while it represents about 2% of body weight, it consumes about 20 23% of whole-body energy requirements, mostly in the form of glucose. It is now well established that both uptake and metabolism of glucose by the brain deteriorate in Alzheimer s disease (AD). There is a particular pattern of regional brain glucose hypometabolism in AD affecting the parietal and temporal cortices, where the glucose deficit is on the order of 20 25% compared to age-matched, cognitively normal controls. 1 Because of a loss of synapses and neuronal dysfunction and death in AD, 2 the deficit in brain glucose utilization has generally been interpreted to be a consequence of AD (e.g., fewer functioning neurons decreases the need for glucose). This perspective is indeed logical but does not account for multiple examples of conditions in which regional brain glucose hypometabolism is present in presymptomatic individuals at risk of AD (i.e., before the clinical (cognitive) onset of the disease). There are several clear examples in which enhanced genetic or lifestyle-based risk of AD causes lower brain glucose uptake long before the onset of cognitive symptoms. Glucose is the brain s predominant fuel but, like other organs, the brain has a back-up fuel for occasions when glucose supply is insufficient, for example, during fasting, starvation, strenuous exercise, or malnutrition. Unlike other organs for which free fatty acids replace insufficient availability of glucose, the brain uses ketones doi: /nyas Ann. N.Y. Acad. Sci (2016) C 2016 New York Academy of Sciences.
2 Cunnane et al. Brain glucose and ketone uptake in Alzheimer s disease Table 1. Presymptomatic brain glucose hypometabolism in persons at risk of Alzheimer s disease (AD) Group at risk Age (years) Brain region with lower brain glucose uptake Magnitude of brain glucose deficit (% lower than control (100%)) Reference Carriers of presenilin 1 30 Posterior cingulate; parietal and temporal cortices Carriers of apolipoprotein 31 Prefrontal, parietal, temporal E4 cortices; posterior cingulate Maternal family history of AD Cognitively normal, prediabetic older persons Young women with polycystic ovary syndrome Cognitively normal older persons 43 Parietal cortex, temporal cortex, hippocampus, entorhinal cortex, posterior cingulate 74 Prefrontal, temporal, parietal cortices; posterior cingulate; precuneus 25 Frontal cortex, middle temporal cortex 20 Schöll et al Reiman et al Mosconi et al. 10 Lower (actual magnitude not provided) Baker et al Castellano et al Frontal cortex Nugent et al. 17 (also known as ketone bodies) as the only significant back-up fuel for glucose. The two ketones that replace glucose for the brain are -hydroxybutyrate ( -HB) and acetoacetate (AcAc). They are normally present in plasma in a ratio of 2:1 3:1 in favor of -HB, but it is only AcAc that is -oxidized in mitochondria; therefore, -HB must be converted to AcAc before being metabolized. The third ketone, acetone, is a volatile decarboxylation product of AcAc, the excretion of which on the breath correlates well with plasma ketone levels. 3 We discuss here how brain glucose hypometabolism could not only be a consequence of AD but could also be contributing to the risk of AD presymptomatically. We also compare findings on the problem of deteriorating brain glucose uptake to recent findings on brain ketone uptake in cognitively healthy older people and in AD, and make reference to the emerging literature on the therapeutic potential of ketogenic supplements or diets in AD. This review complements recently published reviews on changing brain energy metabolism. 4,5 Moreover, it extends the discussions in these reviews by providing more information about the differences between brain glucose and ketone uptake in AD, as well as proposing a therapeutic objective for the dose of ketogenic treatments that could be expected to have therapeutic benefit in AD. Presymptomatic brain glucose hypometabolism contributing to the onset of AD Carriers of the presenilin 1 mutation are at the highest risk of AD. 6 8 Carriers of the apolipoprotein E4 allele and persons with a family history of AD, especially on the maternal side, are also at increased risk of AD, 9 12 although their risk is still relatively low compared to presenilin 1 carriers. Type 2 diabetes and its associated insulin resistance rank among the most important of the nongenetic or predominantly lifestyle-based risk factors for AD. In these three situations, presymptomatic regional brain glucose hypometabolism on the order of 15% is clearly present despite results on cognitive batteries being normal (Table 1). Glucose hypometabolism in those atriskofdiabetesismostfrequently,butnotexclusively, observed in the frontal cortex and, in certain cases, can be observed at ages as young as 24 years. 13 We interpret these data (Table 1) to indicate that presymptomatic brain glucose hypometabolism can be present long before the threshold of cognitive symptoms of AD and could therefore potentially Ann. N.Y. Acad. Sci (2016) C 2016 New York Academy of Sciences. 13
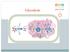
3 Brain glucose and ketone uptake in Alzheimer s disease Cunnane et al. be contributing to the development and/or progression of the cognitive decline associated with AD. A neuropathological link has not yet been convincingly demonstrated in humans, but it is clearly the case in amyloid precursor protein (APP) transgenic mouse models of AD, in which various experimental approaches to diminishing brain glucose supply all drive amyloid beta overproduction. 14 Nevertheless, the pattern of regional brain glucose hypometabolism varies across these different conditions; therefore, it remains speculative as to how they could contribute to AD. We also note that although mild cognitive impairment (MCI) is now widely recognized as a prodromal state to AD and displays regional brain glucose hypometabolism, objective evidence for cognitive deficits is already present in MCI; we have therefore excluded it from Table 1 as an example of a presymptomatic condition to AD. Aging is also a significant risk factor for AD. We and other researchers have used positron emission tomography (PET) with the glucose analogue and radiotracer 18 F-fluorodeoxyglucose (FDG) to study brain energy metabolism in cognitively normal older persons. Using quantitative PET-FDG, we have shown that in cognitively normal people averaging 72 years, the cerebral metabolic rate of glucose (CMRg) in the superior frontal cortex is approximately 35 ± 5 instead of the 40 ± 7 mmol/100 g/min as seen in young adults (i.e., the glucose uptake deficit in this brain region is on the order of 12 15%) CMRg did not differ significantly between young and older adults in either white or gray matter as a whole, nor did it differ in the temporal or parietal cortices where CMRg noticeably decreases in AD. Lower CMRg present mostly, if not exclusively, in the frontal cortex of cognitively normal older people has been previously reported. 1,18 Thus, lower CMRg in the temporal and parietal cortices in AD is a fundamentally different situation than lower CMRg in the frontal cortex during cognitively normal aging (but the former may arise from or be related to the latter). Widespread cortical thinning and regional brain atrophy are also present in older people with normal cognition; 17 therefore, although lower frontal CMRg can clearly be presymptomatic in relation to aging-associated cognitive decline, it is by no means the only or even the quantitatively most significant change occurring in the brain during aging. These observations suggest that the widespread perception that brain glucose hypometabolism is Figure 1. Latent brain glucose hypometabolism contributes to the development of a vicious cycle of accelerating metabolic deterioration and neuronal dysfunction, thereby increasing the risk of Alzheimer s disease (AD). Controlled clinical trials with ketogenic supplements are in progress and aim to bypass glucose hypometabolism and delay cognitive decline at (A) the very early stage of AD (i.e., mild cognitive impairment) or (B) later when the disease is more established. uniquely a consequence of synaptic dysfunction and neuronal failure or death associated with aging needs to be reevaluated. Indeed, this regional brain glucose hypometabolism can be present in young adults in their 20s. 13 We suggest that a vicious cycle can gradually develop in which latent presymptomatic brain glucose hypometabolism can lead to chronic brain energy deprivation, deteriorating neuronal function, further decline in demand for glucose, and further cognitive decline (Fig. 1). 1 The presence of presymptomatic brain glucose hypometabolism does not necessarily make it the primary cause of AD or indicate that neuronal function is necessarily still normal, nor even that glucose hypometabolism is the first abnormality detectable in those at risk of AD. Nevertheless, cognitive outcomes suggest that the brains of some older people can resist inadequate brain glucose supply for aconsiderabletime. 15,17 Knowing that brain glucose hypometabolism can be present in people at risk of AD but before the onset of measurable clinical (cognitive) deficits has implications for potential therapeutic strategies. 1,19 21 Ketones: the brain s physiological alternative fuel to glucose The now classic studies by Owen et al. 22 and Drenick et al. 23 demonstrated that ketones are the main 14 Ann. N.Y. Acad. Sci (2016) C 2016 New York Academy of Sciences.
4 Cunnane et al. Brain glucose and ketone uptake in Alzheimer s disease reserve fuel for the brain when glucose supply is severely compromised by medically supervised starvation lasting 40 or even 60 days, respectively. The liver can produce ketones at a rate of g/day, 24,25 which is sufficient to meet the brain s ketone utilization during starvation. The energy cost to the liver of producing ketones is supplied by gluconeogenesis (mostly in the kidney), the rate of which parallels and may eventually limit maximum achievable ketone production. 24,26 In adults, ketogenesis is principally from longchain fatty acids (mostly 16 and 18 carbons) stored in adipose tissue, the release of which is controlled by insulin. The branched-chain amino acids, valine, isoleucine, and leucine, are also ketogenic, with much of the amino acid catabolism occurring in skeletal muscle. During fasting, blood glucose and insulin decrease, which releases the inhibition on lipolysis in adipose tissue, permitting increased release of free fatty acids. The increase in plasma free fatty acids helps meet the need for an alternative fuel to glucose for most organs with the notable exception of the brain. The increased supply of free fatty acids entering the liver leads to fatty acid beta oxidation and ketogenesis due to condensation of pairs of acetyl CoA units as their availability exceeds their utilization by the tricarboxylic acid cycle. 27 Ketones produced by the liver cannot be catabolized by the liver and are released into the circulation. As far as is known, all organs can potentially use ketones as fuel but, in practice, as fasting or starvation becomes prolonged, skeletal muscle consumes progressively less ketones, and they are used principally by the brain. 18 Insulin sensitivity is an important parameter in ketogenesis because it controls the rise and fall of plasma glucose and free fatty acids. Indeed, conditions involving decreased insulin sensitivity (e.g., insulin resistance) impair tissue glucose uptake and become associated with a vicious cycle of hyperglycemia, hyperinsulinemia, and an eventual trend toward type 2 diabetes, which is a major risk factor for AD. 28,29 Postprandial hyperinsulinemia normally inhibits fatty acid release from adipose tissue and, hence, ketogenesis, but only as long as insulin sensitivity and tissue glucose uptake are normal (i.e., if insulin returns to baseline 2 3 h postprandially). Sedentary lifestyles and excessive intake of simple sugars commonly lead to slower insulin clearance and chronic hyperinsulinemia, which compromise not only tissue glucose metabolism but also ketogenesis and ketone catabolism. 30 Hyperinsulinemia therefore puts the aging brain in double jeopardy, in part because the brain is then acquiring/utilizing less glucose but also because less of the main alternative fuel, ketones, is being produced. 1,31,32 Regional brain ketone uptake in early AD We have compared brain glucose (FDG) and ketone ( 11 C AcAc) uptake using PET in early AD. 33 Our aim was threefold to verify earlier reports that AD patients had normal ketone but low brain glucose uptake, 34 to assess brain fuel metabolism in early AD rather than in the more advanced stages previously reported, 35 and to quantify the regional pattern of brain uptake of both fuels in AD under postprandial conditions. As expected, global brain FDG uptake was 14% lower in early AD patients compared to cognitively normal age-matched controls. This global glucose deficit was primarily confined to the parietal cortex, posterior cingulate, and thalamus. 33 However, neither net 11 C AcAc uptake nor the rate constant for AcAc uptake were significantly different in the brain as a whole or in any brainregioninadversuscontrols. 33 The kinetics of ketone PET tracer metabolism in the brain (whether 11 C AcAc or 11 C -HB 36 ) suggest a onecompartment model in which there is essentially no tissue ketone accumulation because utilization matches uptake. Hence, plasma AcAc or -HB are highly positively correlated to their respective utilization by the brain. Furthermore, the slope of this relationship does not appear to differ between controls and early AD, 33 at least when plasma ketones are relatively low and supplying less than 5% of brain energy requirements (Fig. 2). These results confirm the earlier studies of both Lying-Tunell et al. 35 and Ogawa et al C AcAc is chemically identical to AcAc produced by the body; therefore, unlike with FDG, which is taken up by the plasma membrane but not metabolized beyond hexokinase, it is possible to interpret our results as showing that both brain uptake and metabolism of ketones were normal in early AD. Ketone uptake into the brain occurs through monocarboxylate transporters, which are distinct from glucose transporters. Hence, brain cells in AD still have functional ketone uptake and metabolism and so the problem with glucose uptake/metabolism appears to be specific to glucose. Like glucose, ketones function as more than Ann. N.Y. Acad. Sci (2016) C 2016 New York Academy of Sciences. 15
5 Brain glucose and ketone uptake in Alzheimer s disease Cunnane et al. catabolism could not be maintained. These observations provide a rationale for the concept that the fuel hypometabolism in the AD brain is specific to glucose. Hence, providing the aging brain with more ketones may help it overcome the creeping deficit in glucose uptake and metabolism, thereby delaying brain energy exhaustion and decreasing the risk of AD (Fig. 1). Figure 2. Direct, linear relation between plasma ketone concentration and brain ketone uptake in adults. Two relationships are shown, one for plasma -hydroxybutyrate ( -HB) versus the rate of brain -HB uptake (solid line, R 2 = 0.97; Y = 1.57X 0.20; P < ), and the other for plasma acetoacetate (AcAc) versus the rate of brain AcAc uptake 33 (dotted line, R 2 = 0.83; Y = 3.46X 0.03; P < ): Alzheimer s disease (AD); healthy age-matched controls. Units are the same for both ketones and cerebral metabolic rate (CMR; mol/100 g/min). -HB data have been combined from several sources: postprandial state, 36 -HB infusion, 68 AD; and healthy older controls, day fast, day fast, 23 and AD and healthy older controls. 34 All the -HB data are from arteriovenous difference studies, except for one report that used -HB-PET. 36 The AcAc data were obtained using 11 C AcAc PET. 33 Each symbol represents a single individual except when not available in the original publication: Drenick et al. 23 in which represents a mean of n = 5 participants and Ogawa et al. 34 in which and both represent a mean of n = 7. The relationship between plasma -HB and the percentage of brain energy consumption supplied by -HBinadultsisasfollows: at plasma -HB values around 0.1 mm, ketones supply over 5% of brain energy; at 1 mm -HB, they supply about 10 15%; at 5 7 mm -HB, 50 65%; and at over 7 8 mm -HB, over 75% of brain energy consumption. For a given plasma AcAc concentration, AcAc is taken up by the brain more rapidly than -HB, which is why the dotted regression line lies above that of the solid line for -HB. just cellular fuels, so the latter may be beneficial for the AD brain because of effects other than replacing glucose as a fuel, including supporting glutamatergic function. 4,37 Like glucose, ketones generate ATP by oxidative phosphorylation in mitochondria. However, unlike glucose which can also be metabolized by aerobic glycolysis producing lactate, which, in turn, also generates some ATP in the cytosol ketones generate ATP uniquely via oxidative phosphorylation. Normal brain ketone metabolism in early AD indirectly supports the speculation that oxidative phosphorylation must still be normal in early AD, 38 becauseotherwisenormalketone Ketogenesis from medium-chain triglycerides: dose response relationship Fasting or very low carbohydrate intake induces ketosis because long-chain fatty acids are beta oxidized by the liver. In adults, most dietary and hence most adipose tissue long-chain fatty acids are of 16 or 18 carbons in length. However, breast milk contains medium-chain fatty acids (i.e., fatty acids of 6 12 carbons). Without resorting to fasting or starvation, breastfed infants achieve relatively sustained but mild ketosis by metabolizing medium-chain fatty acids as they are provided from breastmilk. 39 Medium-chain fatty acids are mostly absorbed through the portal vein, hence gaining direct access to the liver without first going through the peripheral circulation. They are also beta oxidized without needing to be activated by carnitine, the net result of which is more rapid ketogenesis from medium-chain than from long-chain fatty acids. With a couple of exceptions, there is normally no opportunity to consume medium-chain fatty acids from the diet once breastfeeding has been terminated. The exceptions are coconut oil and palm kernel oil, in which the most ketogenic mediumchain fatty acids, octanoic (caprylic) and decanoic (capric), make up approximately 9% and 10% of the fatty acids, respectively. The fraction of these oils that contain medium-chain fatty acids can be concentrated, resulting in the generic ketogenic product medium-chain triglyceride (MCT). 39,40 The ratio of these two ketogenic fatty acids and their proportion of the total can vary widely from one MCT product to another. Notwithstanding the generic nature of MCTs and different study designs to assess their metabolism, there is a remarkably strong positive correlation between the maximal plasma ketone ( -HB) level achieved and the oral dose of MCTs over a range of g (R 2 = 0.97; P < ). Hence, a 30-g oral dose of MCTs results in a maximal plasma -HB of approximately 16 Ann. N.Y. Acad. Sci (2016) C 2016 New York Academy of Sciences.
6 Cunnane et al. Brain glucose and ketone uptake in Alzheimer s disease Figure 3. Direct relationship between dose of medium-chain triglyceride and maximal observed plasma -hydroxybutyrate ( -HB) (Y = 0.01X ; R 2 = 0.97; P < ). Data were collated by dose from several human studies in which MCTs were given as single or multiple oral doses. 40,42,46,47,54,69,70 The exact composition or source of the MCTs used in these studies was not always stated in the original papers but is usually predominantly a mixture of octanoate and decanoate. However, the ratio of octanoate to decanoate can vary from 1:2 to 2: mm, and a 70-g dose raises plasma -HB to approximately 1.0 mm (Fig. 3). These dose response studies show similar results whether singleormultipledosesofmctsaregiven,probably because of rapid plasma ketone clearance. Healthy older people metabolize ketones to CO 2 at the same rate as younger adults. 40 Indeed, hyperketonemia after 18 h of fasting may actually be somewhat higher in the seventh to eighth decade of life compared to younger adults. 41 Hence, the capacity to produce and use ketones may actually be increasing somewhat during healthy aging. These studies did not distinguish between ketone utilization by the brain versus other organs, but our brain ketone PET studies confirm that the brain has similar ketone uptake and utilization in healthy older compared to younger persons 15 (Fig. 2). Experimental hyperketonemia in conditions of acute or chronic cognitive deficit Oral MCTs have been shown to improve cognitive outcomes during controlled experimental hypoglycemia caused by insulin infusion. 42 The very high-fat ketogenic diet has been reported to have a similar beneficial effect on cognitive and cardiovascular outcomes in MCI, the prodromal state to AD. 43 These reports complement the studies showing that autonomic and neurological symptoms of severe experimental hypoglycemia as low as 0.5 mm induced by insulin infusion can be avoided by ketone infusion 44,45 or prolonged medically supervised starvation. 18 They demonstrate that ketones can sustain normal brain function even when plasma glucose is severely reduced. Several products based on MCTs are now available on the market or by prescription in the United States and Europe. The arrival of these products was greatly facilitated by reports that MCTs had beneficial effects on cognitive outcomes in mild-to-moderate AD after a single dose 46 or with regular consumption over several months. 47 AcAc and -HB can also be administered orally or by infusion as salts or esters, with the esters being more practical for long-term use because they avoid the issues of cation overload. The safety of a -HB monoester 50 and its utility in improving some aspects of cognitive function in a single case history of early-onset AD have recently been reported. 51 The results of these clinical studies are still preliminary but they support the hypothesis that a brain glucose deficit could be contributing to impaired cognition associated with aging and that this brain fuel deficit can at least in part be bypassed by a source of ketones, whether it be a ketogenic supplement containing MCTs, a ketone ester, or a very high-fat ketogenic diet. Safety of medium-chain triglycerides MCTs in doses up to 1 g/kg/day have a robust safety record in all species studied, including humans. 52,53 Nevertheless, MCTs can have secondary side effects involving gastrointestinal distress, an issue that can be partially mitigated by gradual dose titration. MCTs are saturated fats and, as such, have long been assumed to increase cardiovascular risk factors and body weight. However, treatment for 30 days with 30 g/day of MCTs does not adversely affect body weight, body fat content, or body mass index, nor does it affect serum glucose, insulin, triglycerides, cholesterol, or free fatty acids. 54 Perspectives and challenges requiring further work We propose that AD is, in part, a product of chronic gradual brain energy starvation or exhaustion due specifically to an increasing deficit in brain glucose uptake and metabolism. In addition to the fuel deficit in the brain, neuroinflammation mediated by free radical damage may be exacerbated by impaired brain glucose uptake because glucose normally contributes to the synthesis of antioxidants via the pentose phosphate Ann. N.Y. Acad. Sci (2016) C 2016 New York Academy of Sciences. 17
7 Brain glucose and ketone uptake in Alzheimer s disease Cunnane et al. pathway. 55,56 Owing to mild insulin resistance associated with aging, 57,58 replacement of declining glucose transport into the brain by ketones produced endogenously from fatty acids in adipose tissue is also inefficient. Several clinical studies suggest that the early stages of AD may be amenable to nutritional treatments that raise plasma ketones. 46,47 Our PET results showing normal brain ketone uptake early in AD but low brain glucose uptake also support the plausibility of using a keto-neurotherapeutic strategy in early AD. The broadly similar neurological/cognitive benefit of a very high-fat ketogenic diet containing no MCTs, 43 or a typical diet containing over 50% carbohydrate to which MCTs or ketone esters are added, 51 suggests that the improvement in cognition is related to a common denominator of raised plasma ketones, which bypass chronically impaired glucose uptake and utilization by the AD brain. However, this is still speculative; to date, no study has provided a direct mechanism by which MCTs or ketones could improve cognitive outcomes. Moderate ketosis may stimulate mitochondrial biogenesis, 59 which may also help improve oxidative phosphorylation and ATP generation in the brain. It has not yet been established whether certain MCTs (e.g., octanoate, decanoate, or others) are more effective for ketogenesis than others. Octanoic acid can be taken up and consumed as a fuel by the brain; 60,61 therefore, it may have direct effects on brain function, including but not limited to conversion to ketones by astrocytes. 62 Ketones do not contribute to anaplerosis (replacement of tricarboxylic acid cycle intermediates), so whether the benefit of prolonged ketosis could be self-limiting remains to be seen. 63,64 Specific processes in the brain may need glycolysis-derived ATP but this remains quite controversial, and if confirmed, would be a function that glucose, but not ketones, could support. Several clinical trials registered on ClinicalTrials.gov are underway that combine either a ketogenic supplement or diet with cognitive evaluation and should produce results over the next 2 3 years. These studies should be able to shed further light on the potential utility of keto-therapeutics in neurodegenerative diseases such as AD. Acknowledgments Christine Brodeur-Dubreuil and Eric Lavallée provided excellent technical assistance. Financial support was provided by a Canada Research Chair and University Research Chair (S.C.C.), CFI, CIHR, NSERC, FRQS, Pfizer-FRQS, FQRNT, Sojecci II, INAF, The Alzheimer Association (USA), and the Université desherbrooke.somemctsusedinour studies were provided as gifts by Abitec and Nutricia. Conflicts of interest The authors declare no conflicts of interest. References 1. Cunnane, S. et al Brain fuel metabolism, aging, and Alzheimer s disease. Nutrition 27: Terry, R.D. et al Physical basis of cognitive alterations in Alzheimer s disease: synapse loss is the major correlate of cognitive impairment.ann. Neurol. 30: Musa-Veloso, K. et al Breath acetone predicts plasma ketone bodies in children with epilepsy on a ketogenic diet. Nutrition 22: Hertz, L., Y. Chen & H.S. Waagepetersen Effects of ketone bodies in Alzheimer s disease in relation to neural hypometabolism, beta-amyloid toxicity, and astrocyte function. J. Neurochem. 134: VanItallie, T.B Biomarkers, ketone bodies, and the prevention of Alzheimer s disease. Metabolism 64: S51 S Scholl, M. et al Time course of glucose metabolism in relation to cognitive performance and postmortem neuropathology in Met146Val PSEN1 mutation carriers. J. Alzheimers Dis. 24: Fox, N.C.et al Clinicopathological features of familial Alzheimer s disease associated with the M139V mutation in the presenilin 1 gene. Pedigree but not mutation specific age at onset provides evidence for a further genetic factor. Brain 120(Pt 3): Blennow, K., M.J. de Leon & H. Zetterberg Alzheimer s disease. Lancet 368: Kennedy, A.M. et al Deficits in cerebral glucose metabolism demonstrated by positron emission tomography in individuals at risk of familial Alzheimer s disease. Neurosci. Lett. 186: Mosconi, L. et al Reduced hippocampal metabolism in MCI and AD: automated FDG-PET image analysis. Neurology 64: Reiman, E.M. et al Functional brain abnormalities in young adults at genetic risk for late-onset Alzheimer s dementia. Proc.Natl.Acad.Sci.U.S.A.101: Bu, G Apolipoprotein E and its receptors in Alzheimer s disease: pathways, pathogenesis and therapy. Nat. Rev. Neurosci. 10: Castellano, C.A. et al Regional brain glucose hypometabolism in young women with polycystic ovary syndrome: possible link to mild insulin resistance. PLoS One 10: e Velliquette, R.A., T. O Connor & R. Vassar Energy inhibition elevates beta-secretase levels and activity and is potentially amyloidogenic in APP transgenic mice: possible early events in Alzheimer s disease pathogenesis. J. Neurosci. 25: Ann. N.Y. Acad. Sci (2016) C 2016 New York Academy of Sciences.
8 Cunnane et al. Brain glucose and ketone uptake in Alzheimer s disease 15. Nugent, S. et al Brain glucose and acetoacetate metabolism: a comparison of young and older adults. Neurobiol. Aging 35: Nugent, S. et al Glucose hypometabolism is highly localized but lower cortical thickness and brain atrophy are widespread in cognitively normal older adults. Am.J.Physiol. Endocrinol. Metab. 306: E1315 E Nugent, S. et al Relationship of metabolic and endocrine parameters to brain glucose metabolism in older adults: do cognitively-normal older adults have a particular metabolicphenotype?biogerontology. DOI /s Kalpouzos, G. et al Voxel-based mapping of brain gray matter volume and glucose metabolism profiles in normal aging. Neurobiol. Aging 30: Gibson, R.E. et al Non-invasive radiotracer imaging as a tool for drug development. Curr. Pharm. Des. 6: Veech, R.L. et al Ketone bodies, potential therapeutic uses. IUBMB Life 51: Blass, J.P A new approach to treating Alzheimer s disease. Ann. N.Y. Acad. Sci. 1147: Owen, O.E. et al Brain metabolism during fasting. J. Clin. Invest. 46: Drenick, E.J. et al Resistance to symptomatic insulin reactions after fasting. J. Clin. Invest. 51: Flatt, J.P On the maximal possible rate of ketogenesis. Diabetes 21: Reichard, G.A., Jr. et al Ketone-body production and oxidation in fasting obese humans. J. Clin. Invest. 53: Garber, A.J. et al Hepatic ketogenesis and gluconeogenesis in humans. J. Clin. Invest. 54: Hashim, S.A., A. Arteaga & T.B. Van Itallie Effect of a saturated medium-chain triglyceride on serum-lipids in man. Lancet 1: Craft, S The role of metabolic disorders in Alzheimer disease and vascular dementia: two roads converged. Arch. Neurol. 66: Baker, L.D. et al Insulin resistance and Alzheimerlike reductions in regional cerebral glucose metabolism for cognitively normal adults with prediabetes or early type 2 diabetes. Arch. Neurol. 68: Fukao, T., G.D. Lopaschuk & G.A. Mitchell Pathways and control of ketone body metabolism: on the fringe of lipid biochemistry. Prostaglandins Leukot. Essent. Fatty Acids 70: Henderson, S.T Ketone bodies as a therapeutic for Alzheimer s disease. Neurotherapeutics 5: Mamelak, M Sporadic Alzheimer s disease: the starving brain. J. Alzheimers Dis. 31: Castellano, C.A. et al Lower brain 18 F- fluorodeoxyglucose uptake but normal 11 C-acetoacetate metabolism in mild Alzheimer s disease dementia. J. Alzheimers Dis. 43: Ogawa, M. et al Altered energy metabolism in Alzheimer s disease. J. Neurol. Sci. 139: Lying-Tunell, U. et al Cerebral blood flow and metabolic rate of oxygen, glucose, lactate, pyruvate, ketone bodies and amino acids.acta Neurol. Scand. 63: Blomqvist, G. et al Use of R-beta-[1-11C] hydroxybutyrate in PET studies of regional cerebral uptake of ketone bodies in humans. Am. J. Physiol. 269: E948 E Roy, M. et al Rapid adaptation of rat brain and liver metabolism to a ketogenic diet: an integrated study using (1)H- and (13)C-NMR spectroscopy. J. Cereb. Blood Flow Metab. 35: Hoyer, S., K. Oesterreich & O. Wagner Glucose metabolism as the site of the primary abnormality in earlyonset dementia of Alzheimer type? J. Neurol. 235: Cunnane, S.C. & M.A. Crawford Energetic and nutritional constraints on infant brain development: implications for brain expansion during human evolution. J. Hum. Evol. 77: Freemantle, E. et al Metabolic response to a ketogenic breakfast in the healthy elderly. J. Nutr. Health Aging 13: London, E.D. et al Effects of fasting on ketone body concentrations in healthy men of different ages. J. Gerontol. 41: Page, K.A. et al Medium-chain fatty acids improve cognitive function in intensively treated type 1 diabetic patients and support in vitro synaptic transmission during acute hypoglycemia. Diabetes 58: Krikorian, R. et al Dietary ketosis enhances memory in mild cognitive impairment. Neurobiol. Aging 33: 425.e Amiel, S.A. et al Ketone infusion lowers hormonal responses to hypoglycaemia: evidence for acute cerebral utilization of a non-glucose fuel. Clin. Sci. (Lond.) 81: Veneman, T. et al Effect of hyperketonemia and hyperlacticacidemia on symptoms, cognitive dysfunction, and counterregulatory hormone responses during hypoglycemia in normal humans. Diabetes 43: Reger, M.A. et al Effects of beta-hydroxybutyrate on cognition in memory-impaired adults. Neurobiol. Aging 25: Henderson, S.T. et al Study of the ketogenic agent AC in mild to moderate Alzheimer s disease: a randomized, double-blind, placebo-controlled, multicenter trial. Nutr. Metab. (Lond.) 6: Plecko, B. et al Oral beta-hydroxybutyrate supplementation in two patients with hyperinsulinemic hypoglycemia: monitoring of beta-hydroxybutyrate levels in blood and cerebrospinal fluid, and in the brain by in vivo magnetic resonance spectroscopy. Pediatr. Res. 52: Hasselbalch, S.G.et al Changes in cerebral blood flow and carbohydrate metabolism during acute hyperketonemia. Am. J. Physiol. 270: E746 E Clarke, K. et al Kinetics, safety and tolerability of (R)-3-hydroxybutyl (R)-3-hydroxybutyrate in healthy adult subjects. Regul. Toxicol. Pharmacol. 63: Newport, M.T. et al A new way to produce hyperketonemia: use of ketone ester in a case of Alzheimer s disease. Alzheimers Dement. 11: Bach, A.C. & V.K. Babayan Medium-chain triglycerides: an update. Am. J. Clin. Nutr. 36: Traul, K.A. et al Review of the toxicologic properties of medium-chain triglycerides. Food Chem. Toxicol. 38: Ann. N.Y. Acad. Sci (2016) C 2016 New York Academy of Sciences. 19
9 Brain glucose and ketone uptake in Alzheimer s disease Cunnane et al. 54. Courchesne-Loyer, A. et al Stimulation of mild, sustained ketonemia by medium-chain triacylglycerols in healthy humans: estimated potential contribution to brain energy metabolism. Nutrition 29: Jiang, P., W. Du & M. Wu Regulation of the pentose phosphate pathway in cancer. Protein Cell 5: Bolanos, J.P. & A. Almeida The pentose-phosphate pathway in neuronal survival against nitrosative stress. IUBMB Life 62: Rowe, J.W. et al Characterization of the insulin resistance of aging.j. Clin. Invest. 71: Stout, R.W Glucose tolerance and ageing. J. R. Soc. Med. 87: Bough, K.J. et al Mitochondrial biogenesis in the anticonvulsant mechanism of the ketogenic diet. Ann. Neurol. 60: Ebert, D., R.G. Haller & M.E. Walton Energy contribution of octanoate to intact rat brain metabolism measured by 13 C nuclear magnetic resonance spectroscopy. J. Neurosci. 23: Kuge, Y. et al Brain uptake and metabolism of [1 11C]octanoate in rats: pharmacokinetic basis for its application as a radiopharmaceutical for studying brain fatty acid metabolism. Ann. Nucl. Med. 9: Auestad, N. et al Fatty acid oxidation and ketogenesis by astrocytes in primary culture. J. Neurochem. 56: Mochel,F. et al Pyruvate carboxylase deficiency: clinical and biochemical response to anaplerotic diet therapy. Mol. Genet. Metab. 84: Brunengraber, H. & C.R. Roe Anaplerotic molecules: current and future. J. Inherit. Metab. Dis. 29: Vaishnavi,S.N. et al Regional aerobic glycolysis in the human brain. Proc. Natl. Acad. Sci. U.S.A. 107: Dienel, G.A Brain lactate metabolism: the discoveries and the controversies. J. Cereb. Blood Flow Metab. 32: Hyder, F. et al Glutamatergic function in the resting awake human brain is supported by uniformly high oxidative energy. J. Cereb. Blood Flow Metab. 33: Blomqvist, G. et al Effect of acute hyperketonemia on thecerebraluptakeofketonebodiesinnondiabeticsubjects and IDDM patients. Am. J. Physiol. Endocrinol. Metab. 283: E20 E Seaton, T.B. et al Thermic effect of medium-chain and long-chain triglycerides in man. Am. J. Clin. Nutr. 44: Pi-Sunyer, F.X., S.A. Hashim & T.B. Van Itallie Insulin and ketone responses to ingestion of medium and long-chain triglycerides in man. Diabetes 18: Ann. N.Y. Acad. Sci (2016) C 2016 New York Academy of Sciences.
THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals
 Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Karin Borges, PhD. October The urgent need for new metabolic (dietary) treatments of epilepsy
 Karin Borges, PhD October 2016 The urgent need for new metabolic (dietary) treatments of epilepsy Epilepsy is a common neurological disease that is characterized by recurrent seizures due to the spontaneous
Karin Borges, PhD October 2016 The urgent need for new metabolic (dietary) treatments of epilepsy Epilepsy is a common neurological disease that is characterized by recurrent seizures due to the spontaneous
KETONES AS AN ALTERNATIVE FUEL FOR ALZHEIMER S DISEASE AND OTHER DISORDERS. Mary T. Newport MD Hippocrates Institute May 2014
 KETONES AS AN ALTERNATIVE FUEL FOR ALZHEIMER S DISEASE AND OTHER DISORDERS Mary T. Newport MD Hippocrates Institute May 2014 Plaques and Tangles 100 billion nerve cells. 100 trillion synapses. Dozens of
KETONES AS AN ALTERNATIVE FUEL FOR ALZHEIMER S DISEASE AND OTHER DISORDERS Mary T. Newport MD Hippocrates Institute May 2014 Plaques and Tangles 100 billion nerve cells. 100 trillion synapses. Dozens of
Integration Of Metabolism
 Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
CAPTEX FOOD FOR THOUGHT.
 CAPTEX FOOD FOR THOUGHT www.abiteccorp.com Are you getting better with age? Maybe! But what about your mind? The brain needs fuel in order to continue supplying us all the knowledge and memories we have
CAPTEX FOOD FOR THOUGHT www.abiteccorp.com Are you getting better with age? Maybe! But what about your mind? The brain needs fuel in order to continue supplying us all the knowledge and memories we have
Oxidation of Long Chain Fatty Acids
 Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
In glycolysis, glucose is converted to pyruvate. If the pyruvate is reduced to lactate, the pathway does not require O 2 and is called anaerobic
 Glycolysis 1 In glycolysis, glucose is converted to pyruvate. If the pyruvate is reduced to lactate, the pathway does not require O 2 and is called anaerobic glycolysis. If this pyruvate is converted instead
Glycolysis 1 In glycolysis, glucose is converted to pyruvate. If the pyruvate is reduced to lactate, the pathway does not require O 2 and is called anaerobic glycolysis. If this pyruvate is converted instead
Medical Biochemistry and Molecular Biology department
 Medical Biochemistry and Molecular Biology department Cardiac Fuels [Sources of energy for the Cardiac muscle] Intended learning outcomes of the lecture: By the end of this lecture you would be able to:-
Medical Biochemistry and Molecular Biology department Cardiac Fuels [Sources of energy for the Cardiac muscle] Intended learning outcomes of the lecture: By the end of this lecture you would be able to:-
Integration of Metabolism 1. made by: Noor M. ALnairat. Sheet No. 18
 Integration of Metabolism 1 made by: Noor M. ALnairat Sheet No. 18 Data :24/11/2016 SLIDE 2: Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP,
Integration of Metabolism 1 made by: Noor M. ALnairat Sheet No. 18 Data :24/11/2016 SLIDE 2: Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP,
CHY2026: General Biochemistry. Lipid Metabolism
 CHY2026: General Biochemistry Lipid Metabolism Lipid Digestion Lipid Metabolism Fats (triglycerides) are high metabolic energy molecules Fats yield 9.3 kcal of energy (carbohydrates and proteins 4.1 kcal)
CHY2026: General Biochemistry Lipid Metabolism Lipid Digestion Lipid Metabolism Fats (triglycerides) are high metabolic energy molecules Fats yield 9.3 kcal of energy (carbohydrates and proteins 4.1 kcal)
6. How Are Fatty Acids Produced? 7. How Are Acylglycerols and Compound Lipids Produced? 8. How Is Cholesterol Produced?
 Lipid Metabolism Learning bjectives 1 How Are Lipids Involved in the Generationand Storage of Energy? 2 How Are Lipids Catabolized? 3 What Is the Energy Yield from the xidation of Fatty Acids? 4 How Are
Lipid Metabolism Learning bjectives 1 How Are Lipids Involved in the Generationand Storage of Energy? 2 How Are Lipids Catabolized? 3 What Is the Energy Yield from the xidation of Fatty Acids? 4 How Are
Integrative Metabolism: Significance
 Integrative Metabolism: Significance Energy Containing Nutrients Carbohydrates Fats Proteins Catabolism Energy Depleted End Products H 2 O NH 3 ADP + Pi NAD + NADP + FAD + Pi NADH+H + NADPH+H + FADH2 Cell
Integrative Metabolism: Significance Energy Containing Nutrients Carbohydrates Fats Proteins Catabolism Energy Depleted End Products H 2 O NH 3 ADP + Pi NAD + NADP + FAD + Pi NADH+H + NADPH+H + FADH2 Cell
Lipid Metabolism. Remember fats?? Triacylglycerols - major form of energy storage in animals
 Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
Development of Alzheimer s Disease: Ketones to Help Rescue a Brain Running Out of Fuel?
 Development of Alzheimer s Disease: Ketones to Help Rescue a Brain Running Out of Fuel? Christian-Alexandre CASTELLANO, PhD Research Center on Aging, CIUSSS de l Estrie CHUS Université de Sherbrooke QC,
Development of Alzheimer s Disease: Ketones to Help Rescue a Brain Running Out of Fuel? Christian-Alexandre CASTELLANO, PhD Research Center on Aging, CIUSSS de l Estrie CHUS Université de Sherbrooke QC,
KETOGENIC DIET ISMAIL HALAHLEH, MSC. نقیب اخصاي یي التغذیة الفلسطینیین
 KETOGENIC DIET ISMAIL HALAHLEH, MSC. نقیب اخصاي یي التغذیة الفلسطینیین INTRODUCTION WHAT IS KETOGENIC DIET???? KETOGENIC DIET The ketogenic diet (KD) is a diet that is high in fat, low in carbohydrate,
KETOGENIC DIET ISMAIL HALAHLEH, MSC. نقیب اخصاي یي التغذیة الفلسطینیین INTRODUCTION WHAT IS KETOGENIC DIET???? KETOGENIC DIET The ketogenic diet (KD) is a diet that is high in fat, low in carbohydrate,
CHY2026: General Biochemistry UNIT 7& 8: CARBOHYDRATE METABOLISM
 CHY2026: General Biochemistry UNIT 7& 8: CARBOHYDRATE METABOLISM Metabolism Bioenergetics is the transfer and utilization of energy in biological systems The direction and extent to which a chemical reaction
CHY2026: General Biochemistry UNIT 7& 8: CARBOHYDRATE METABOLISM Metabolism Bioenergetics is the transfer and utilization of energy in biological systems The direction and extent to which a chemical reaction
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
Chapter 24 Lecture Outline
 Chapter 24 Lecture Outline Carbohydrate Lipid and Protein! Metabolism! In the catabolism of carbohydrates, glycolysis converts glucose into pyruvate, which is then metabolized into acetyl CoA. Prepared
Chapter 24 Lecture Outline Carbohydrate Lipid and Protein! Metabolism! In the catabolism of carbohydrates, glycolysis converts glucose into pyruvate, which is then metabolized into acetyl CoA. Prepared
Energy metabolism - the overview
 Energy metabolism - the overview Josef Fontana EC - 40 Overview of the lecture Important terms of the energy metabolism The overview of the energy metabolism The main pathways of the energy metabolism
Energy metabolism - the overview Josef Fontana EC - 40 Overview of the lecture Important terms of the energy metabolism The overview of the energy metabolism The main pathways of the energy metabolism
Integration Of Metabolism
 Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
Lipid Metabolism * OpenStax
 OpenStax-CNX module: m46462 1 Lipid Metabolism * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will be able
OpenStax-CNX module: m46462 1 Lipid Metabolism * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will be able
E. Haritov, E. Angeleska and N. Boyadjieva Department of pharmacology and toxicology, Medical Faculty, Medical University So a
 :.,..,, KETOGENIC DIET AND EPILEPSY: THE ROLE OF KETONE BODIES IN THE INFLUENCE N NEURONAL EXCITABILITY E. Haritov, E. Angeleska and N. Boyadjieva Department of pharmacology and toxicology, Medical Faculty,
:.,..,, KETOGENIC DIET AND EPILEPSY: THE ROLE OF KETONE BODIES IN THE INFLUENCE N NEURONAL EXCITABILITY E. Haritov, E. Angeleska and N. Boyadjieva Department of pharmacology and toxicology, Medical Faculty,
CEREBRAL BLOOD FLOW AND METABOLISM
 Supported by: HURO/0901/069/2.3.1 HU-RO-DOCS CEREBRAL BLOOD FLOW AND METABOLISM Part 11. Cerebral blood flow Supplies cerebral metabolism demanded by neuronal function Is required for the production and
Supported by: HURO/0901/069/2.3.1 HU-RO-DOCS CEREBRAL BLOOD FLOW AND METABOLISM Part 11. Cerebral blood flow Supplies cerebral metabolism demanded by neuronal function Is required for the production and
Chemistry 1120 Exam 4 Study Guide
 Chemistry 1120 Exam 4 Study Guide Chapter 12 12.1 Identify and differentiate between macronutrients (lipids, amino acids and saccharides) and micronutrients (vitamins and minerals). Master Tutor Section
Chemistry 1120 Exam 4 Study Guide Chapter 12 12.1 Identify and differentiate between macronutrients (lipids, amino acids and saccharides) and micronutrients (vitamins and minerals). Master Tutor Section
LIPID METABOLISM. Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI
 LIPID METABOLISM Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI Lipid metabolism is concerned mainly with fatty acids cholesterol Source of fatty acids from dietary fat de novo
LIPID METABOLISM Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI Lipid metabolism is concerned mainly with fatty acids cholesterol Source of fatty acids from dietary fat de novo
the fates of acetyl coa which produced by B oixidation :
 Ketone bodies the fates of acetyl coa which produced by B oixidation : 1) oxidized at the TCA cycle 2)synthesis of ketone bodies Ketone bodies : 1)acetoacetate 2) acetone 3) 3_hydroxybutyrate Naming acetonacetone:
Ketone bodies the fates of acetyl coa which produced by B oixidation : 1) oxidized at the TCA cycle 2)synthesis of ketone bodies Ketone bodies : 1)acetoacetate 2) acetone 3) 3_hydroxybutyrate Naming acetonacetone:
Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus
 Emerging Science Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus George Wolf Insulin resistance is defined as the reduced responsiveness to normal circulating
Emerging Science Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus George Wolf Insulin resistance is defined as the reduced responsiveness to normal circulating
number Done by Corrected by Doctor Nayef Karadsheh
 number 13 Done by Asma Karameh Corrected by Saad hayek Doctor Nayef Karadsheh Gluconeogenesis This lecture covers gluconeogenesis with aspects of: 1) Introduction to glucose distribution through tissues.
number 13 Done by Asma Karameh Corrected by Saad hayek Doctor Nayef Karadsheh Gluconeogenesis This lecture covers gluconeogenesis with aspects of: 1) Introduction to glucose distribution through tissues.
Intermediary metabolism. Eva Samcová
 Intermediary metabolism Eva Samcová Metabolic roles of tissues Four major tissues play a dominant role in fuel metabolism : liver, adipose, muscle, and brain. These tissues do not function in isolation.
Intermediary metabolism Eva Samcová Metabolic roles of tissues Four major tissues play a dominant role in fuel metabolism : liver, adipose, muscle, and brain. These tissues do not function in isolation.
Biol 219 Lec 7 Fall 2016
 Cellular Respiration: Harvesting Energy to form ATP Cellular Respiration and Metabolism Glucose ATP Pyruvate Lactate Acetyl CoA NAD + Introducing The Players primary substrate for cellular respiration
Cellular Respiration: Harvesting Energy to form ATP Cellular Respiration and Metabolism Glucose ATP Pyruvate Lactate Acetyl CoA NAD + Introducing The Players primary substrate for cellular respiration
Transfer of food energy to chemical energy. Includes anabolic and catabolic reactions. The cell is the metabolic processing center
 Metabolism There are a lot of diagrams here. DO NOT, I repeat, DO NOT get overly anxious or excited about them. We will go through them again slowly!! Read the slides, read the book, DO NOT TAKE NOTES.
Metabolism There are a lot of diagrams here. DO NOT, I repeat, DO NOT get overly anxious or excited about them. We will go through them again slowly!! Read the slides, read the book, DO NOT TAKE NOTES.
Physiology Unit 1 METABOLISM OF LIPIDS AND PROTEINS
 Physiology Unit 1 METABOLISM OF LIPIDS AND PROTEINS Alternate Fuel Sources When glucose levels are low Proteins and Triglycerides will be metabolized Tissues will use different fuel sources depending on:
Physiology Unit 1 METABOLISM OF LIPIDS AND PROTEINS Alternate Fuel Sources When glucose levels are low Proteins and Triglycerides will be metabolized Tissues will use different fuel sources depending on:
23.1 Lipid Metabolism in Animals. Chapter 23. Micelles Lipid Metabolism in. Animals. Overview of Digestion Lipid Metabolism in
 Denniston Topping Caret Copyright! The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Chapter 23 Fatty Acid Metabolism Triglycerides (Tgl) are emulsified into fat droplets
Denniston Topping Caret Copyright! The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Chapter 23 Fatty Acid Metabolism Triglycerides (Tgl) are emulsified into fat droplets
BASIC SCIENCES & BIOCHEMISTRY FOR BETZPAENIC BRIMBLERS
 BASIC SCIENCES & BIOCHEMISTRY FOR BETZPAENIC BRIMBLERS Lymphatic Vessels One main lymph vessel receives lymph from the right upper arm and the right side of the head and the thorax and empties into the
BASIC SCIENCES & BIOCHEMISTRY FOR BETZPAENIC BRIMBLERS Lymphatic Vessels One main lymph vessel receives lymph from the right upper arm and the right side of the head and the thorax and empties into the
Roles of Lipids. principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular
 Roles of Lipids principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular = Oxidation of fatty acids Central energy-yielding pathway in animals. O
Roles of Lipids principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular = Oxidation of fatty acids Central energy-yielding pathway in animals. O
Diagnostic exercise tests and treatment options in McArdle disease
 Diagnostic exercise tests and treatment options in McArdle disease John Vissing Neuromuscular Clinic and Research Unit, Department of Neurology, University of Copenhagen, Rigshospitalet, Copenhagen Exercise
Diagnostic exercise tests and treatment options in McArdle disease John Vissing Neuromuscular Clinic and Research Unit, Department of Neurology, University of Copenhagen, Rigshospitalet, Copenhagen Exercise
Introduction to Carbohydrate metabolism
 Introduction to Carbohydrate metabolism Some metabolic pathways of carbohydrates 1- Glycolysis 2- Krebs cycle 3- Glycogenesis 4- Glycogenolysis 5- Glyconeogenesis - Pentose Phosphate Pathway (PPP) - Curi
Introduction to Carbohydrate metabolism Some metabolic pathways of carbohydrates 1- Glycolysis 2- Krebs cycle 3- Glycogenesis 4- Glycogenolysis 5- Glyconeogenesis - Pentose Phosphate Pathway (PPP) - Curi
CHAPTER 24: Carbohydrate, Lipid, & Protein Metabolism. General, Organic, & Biological Chemistry Janice Gorzynski Smith
 CHAPTER 24: Carbohydrate, Lipid, & Protein Metabolism General, Organic, & Biological Chemistry Janice Gorzynski Smith CHAPTER 24: Carbohydrate, Lipid, & Protein Metabolism Learning Objectives: q Role in
CHAPTER 24: Carbohydrate, Lipid, & Protein Metabolism General, Organic, & Biological Chemistry Janice Gorzynski Smith CHAPTER 24: Carbohydrate, Lipid, & Protein Metabolism Learning Objectives: q Role in
What systems are involved in homeostatic regulation (give an example)?
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
Metabolism. Chapter 5. Catabolism Drives Anabolism 8/29/11. Complete Catabolism of Glucose
 8/29/11 Metabolism Chapter 5 All of the reactions in the body that require energy transfer. Can be divided into: Cell Respiration and Metabolism Anabolism: requires the input of energy to synthesize large
8/29/11 Metabolism Chapter 5 All of the reactions in the body that require energy transfer. Can be divided into: Cell Respiration and Metabolism Anabolism: requires the input of energy to synthesize large
BIOL212- Biochemistry of Disease. Metabolic Disorders: Diabetes
 BIOL212- Biochemistry of Disease Metabolic Disorders: Diabetes Diabetes mellitus is, after heart disease and cancer, the third leading cause of death in the west. Insulin is either not secreted in sufficient
BIOL212- Biochemistry of Disease Metabolic Disorders: Diabetes Diabetes mellitus is, after heart disease and cancer, the third leading cause of death in the west. Insulin is either not secreted in sufficient
Nutrients. Chapter 25 Nutrition, Metabolism, Temperature Regulation
 Chapter 25 Nutrition, Metabolism, Temperature Regulation 25-1 Nutrients Chemicals used by body to produce energy, provide building blocks or function in other chemical reactions Classes Carbohydrates,
Chapter 25 Nutrition, Metabolism, Temperature Regulation 25-1 Nutrients Chemicals used by body to produce energy, provide building blocks or function in other chemical reactions Classes Carbohydrates,
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 27 Fatty Acid Degradation Dietary Lipid (Triacylglycerol) Metabolism - In the small intestine, fat particles are coated with bile
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 27 Fatty Acid Degradation Dietary Lipid (Triacylglycerol) Metabolism - In the small intestine, fat particles are coated with bile
#16 made by Nour omar corrected by laith sorour date 17/11
 Lipid metabolism 2 #16 made by Nour omar corrected by laith sorour date 17/11 Keton Bodies Ketone bodies: acetone, -hydroxybutyrate, and acetoacetate formed principally in the liver mitochondria. can be
Lipid metabolism 2 #16 made by Nour omar corrected by laith sorour date 17/11 Keton Bodies Ketone bodies: acetone, -hydroxybutyrate, and acetoacetate formed principally in the liver mitochondria. can be
HISTORY OF THE KETOGENIC DIET
 Laura Roche RD Horizon Health Authority May 29, 2018 AGENDA History of the Ketogenic Diet Diet Pathophysiology Side Effects Pros and Cons How and Why the Diet works Ketogenic Diet for Type 2 Diabetes Ketogenic
Laura Roche RD Horizon Health Authority May 29, 2018 AGENDA History of the Ketogenic Diet Diet Pathophysiology Side Effects Pros and Cons How and Why the Diet works Ketogenic Diet for Type 2 Diabetes Ketogenic
radiotracer, 1 Research Center on Aging, Sherbrooke, Université de Sherbrooke,
 Original Article Inverse relationship between brain glucose and ketone metabolism in adults during short-term moderate dietary ketosis: A dual tracer quantitative positron emission tomography study Journal
Original Article Inverse relationship between brain glucose and ketone metabolism in adults during short-term moderate dietary ketosis: A dual tracer quantitative positron emission tomography study Journal
anabolic pathways- Catabolic Amphibolic
 METABOLISM Introduction The fate of dietary components after digestion and absorption constitute metabolism regulated by metabolic pathway 3 types: anabolic pathways- Synthesis of compound e.g. synthesis
METABOLISM Introduction The fate of dietary components after digestion and absorption constitute metabolism regulated by metabolic pathway 3 types: anabolic pathways- Synthesis of compound e.g. synthesis
MITOCW watch?v=qmqif0yj4lm
 MITOCW watch?v=qmqif0yj4lm The following content is provided under a Creative Commons license. Your support will help MIT OpenCourseWare continue to offer high quality educational resources for free. To
MITOCW watch?v=qmqif0yj4lm The following content is provided under a Creative Commons license. Your support will help MIT OpenCourseWare continue to offer high quality educational resources for free. To
Objectives By the end of lecture the student should:
 Objectives By the end of lecture the student should: Discuss β oxidation of fatty acids. Illustrate α oxidation of fatty acids. Understand ω oxidation of fatty acids. List sources and fates of active acetate.
Objectives By the end of lecture the student should: Discuss β oxidation of fatty acids. Illustrate α oxidation of fatty acids. Understand ω oxidation of fatty acids. List sources and fates of active acetate.
Using the Organic Acids Test Part 3 Dr. Jeff Moss
 Using organic acids to resolve chief complaints and improve quality of life in chronically ill patients Part III Jeffrey Moss, DDS, CNS, DACBN jeffmoss@mossnutrition.com 413-530-08580858 (cell) 1 Summer
Using organic acids to resolve chief complaints and improve quality of life in chronically ill patients Part III Jeffrey Moss, DDS, CNS, DACBN jeffmoss@mossnutrition.com 413-530-08580858 (cell) 1 Summer
Lecture 5: Cell Metabolism. Biology 219 Dr. Adam Ross
 Lecture 5: Cell Metabolism Biology 219 Dr. Adam Ross Cellular Respiration Set of reactions that take place during the conversion of nutrients into ATP Intricate regulatory relationship between several
Lecture 5: Cell Metabolism Biology 219 Dr. Adam Ross Cellular Respiration Set of reactions that take place during the conversion of nutrients into ATP Intricate regulatory relationship between several
Physiological Chemistry II Exam IV Dr. Melissa Kelley April 13, 2004
 Name Write your name on the back of the exam Physiological Chemistry II Exam IV Dr. Melissa Kelley April 13, 2004 This examination consists of forty-four questions, each having 2 points. The remaining
Name Write your name on the back of the exam Physiological Chemistry II Exam IV Dr. Melissa Kelley April 13, 2004 This examination consists of forty-four questions, each having 2 points. The remaining
Hompes Method Lesson 29 Organic Acids Part One
 Hompes Method Lesson 29 Organic Acids Part One Health for the People Ltd not for reuse without expressed permission Organic Acids - Introduction The ultimate tool for laboratory evaluations in nutritional
Hompes Method Lesson 29 Organic Acids Part One Health for the People Ltd not for reuse without expressed permission Organic Acids - Introduction The ultimate tool for laboratory evaluations in nutritional
ANSC/NUTR 618 LIPIDS & LIPID METABOLISM. Triacylglycerol and Fatty Acid Metabolism
 ANSC/NUTR 618 LIPIDS & LIPID METABOLISM II. Triacylglycerol synthesis A. Overall pathway Glycerol-3-phosphate + 3 Fatty acyl-coa à Triacylglycerol + 3 CoASH B. Enzymes 1. Acyl-CoA synthase 2. Glycerol-phosphate
ANSC/NUTR 618 LIPIDS & LIPID METABOLISM II. Triacylglycerol synthesis A. Overall pathway Glycerol-3-phosphate + 3 Fatty acyl-coa à Triacylglycerol + 3 CoASH B. Enzymes 1. Acyl-CoA synthase 2. Glycerol-phosphate
Biosynthesis of Fatty Acids. By Dr.QUTAIBA A. QASIM
 Biosynthesis of Fatty Acids By Dr.QUTAIBA A. QASIM Fatty Acids Definition Fatty acids are comprised of hydrocarbon chains terminating with carboxylic acid groups. Fatty acids and their associated derivatives
Biosynthesis of Fatty Acids By Dr.QUTAIBA A. QASIM Fatty Acids Definition Fatty acids are comprised of hydrocarbon chains terminating with carboxylic acid groups. Fatty acids and their associated derivatives
KetoActiv FAQs. Is a ketone supplement an energy source?
 KetoActiv FAQs Is a ketone supplement an energy source? B-hydroxbutyrate (BHB) is a ketone body that can be utilized as an ATP (cellular energy) substrate by our cells to generate ATP (energy). Research
KetoActiv FAQs Is a ketone supplement an energy source? B-hydroxbutyrate (BHB) is a ketone body that can be utilized as an ATP (cellular energy) substrate by our cells to generate ATP (energy). Research
Energy stores in different organs for a 155 lb male, in Calories
 Energy stores in different organs for a 155 lb male, in Calories Organ Glucose/ Glycogen Triacyl Glycerols* Liver 400 450 400 Brain 8 0 0 Mobile Proteins Muscle 1,200 450 24,000 Adipose Tissue 80 135,000
Energy stores in different organs for a 155 lb male, in Calories Organ Glucose/ Glycogen Triacyl Glycerols* Liver 400 450 400 Brain 8 0 0 Mobile Proteins Muscle 1,200 450 24,000 Adipose Tissue 80 135,000
Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine
 Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine Harvey Levy, MD Mark Korson, MD Piero Rinaldo, MD, PhD Larry Sweetman, PhD K. Michael Gibson, PhD Charlie Roe, MD Jerry
Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine Harvey Levy, MD Mark Korson, MD Piero Rinaldo, MD, PhD Larry Sweetman, PhD K. Michael Gibson, PhD Charlie Roe, MD Jerry
01/11/2012. Neurological disorders and nutrition. Nutritional and related assessments. Non-nutritional causes: nutritional implications
 Neurological disorders and nutrition General considerations, e.g., dysphagia Main topics and optional Canadian websites: STROKES www.heartandstroke.ca EPILEPSY www.epilepsy.ca PARKINSON S www.parkinson.ca
Neurological disorders and nutrition General considerations, e.g., dysphagia Main topics and optional Canadian websites: STROKES www.heartandstroke.ca EPILEPSY www.epilepsy.ca PARKINSON S www.parkinson.ca
Lecture 36. Key Concepts. Overview of lipid metabolism. Reactions of fatty acid oxidation. Energy yield from fatty acid oxidation
 Lecture 36 Lipid Metabolism 1 Fatty Acid Oxidation Ketone Bodies Key Concepts Overview of lipid metabolism Reactions of fatty acid oxidation Energy yield from fatty acid oxidation Formation of ketone bodies
Lecture 36 Lipid Metabolism 1 Fatty Acid Oxidation Ketone Bodies Key Concepts Overview of lipid metabolism Reactions of fatty acid oxidation Energy yield from fatty acid oxidation Formation of ketone bodies
BCM 221 LECTURES OJEMEKELE O.
 BCM 221 LECTURES BY OJEMEKELE O. OUTLINE INTRODUCTION TO LIPID CHEMISTRY STORAGE OF ENERGY IN ADIPOCYTES MOBILIZATION OF ENERGY STORES IN ADIPOCYTES KETONE BODIES AND KETOSIS PYRUVATE DEHYDROGENASE COMPLEX
BCM 221 LECTURES BY OJEMEKELE O. OUTLINE INTRODUCTION TO LIPID CHEMISTRY STORAGE OF ENERGY IN ADIPOCYTES MOBILIZATION OF ENERGY STORES IN ADIPOCYTES KETONE BODIES AND KETOSIS PYRUVATE DEHYDROGENASE COMPLEX
a tidal wave of chronic illness
 Using organic acids to resolve chief complaints and improve quality of life in chronically ill patients Part IV Jeffrey Moss, DDS, CNS, DACBN jeffmoss@mossnutrition.com 413-530-08580858 (cell) 1 Summer
Using organic acids to resolve chief complaints and improve quality of life in chronically ill patients Part IV Jeffrey Moss, DDS, CNS, DACBN jeffmoss@mossnutrition.com 413-530-08580858 (cell) 1 Summer
Major Pathways in Carbohydrate Metabolism
 Major Pathways in Carbohydrate Metabolism 70 Stage 1: Digestion of Carbohydrates In Stage 1, the digestion of carbohydrates Begins in the mouth where salivary amylase breaks down polysaccharides to smaller
Major Pathways in Carbohydrate Metabolism 70 Stage 1: Digestion of Carbohydrates In Stage 1, the digestion of carbohydrates Begins in the mouth where salivary amylase breaks down polysaccharides to smaller
nothing is perfect Problems with triheptanoin and clinical trials
 nothing is perfect Problems with triheptanoin and clinical trials MILAN, Italy, 7th 8th ctober 2016 Joerg Klepper The State-and-Region Agreement asks for a declaration by Moderators, Speakers, Teachers
nothing is perfect Problems with triheptanoin and clinical trials MILAN, Italy, 7th 8th ctober 2016 Joerg Klepper The State-and-Region Agreement asks for a declaration by Moderators, Speakers, Teachers
Providing the Right Fuels for FOD s. Elaina Jurecki, MS, RD Regional Metabolic Nutritionist Kaiser Permanente Medical Center Oakland, CA
 Providing the Right Fuels for FOD s Elaina Jurecki, MS, RD Regional Metabolic Nutritionist Kaiser Permanente Medical Center Oakland, CA Providing the Right Fuels for FOD s The Body s Use of Energy Fat
Providing the Right Fuels for FOD s Elaina Jurecki, MS, RD Regional Metabolic Nutritionist Kaiser Permanente Medical Center Oakland, CA Providing the Right Fuels for FOD s The Body s Use of Energy Fat
Week 3 The Pancreas: Pancreatic ph buffering:
 Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Overall Energy metabolism: Integration and Regulation
 Overall Energy metabolism: Integration and Regulation We have discussed various fuels which are oxidized via different catabolic pathways to generate ATP, or reducing equivalents required to carry out
Overall Energy metabolism: Integration and Regulation We have discussed various fuels which are oxidized via different catabolic pathways to generate ATP, or reducing equivalents required to carry out
Metabolic integration and Regulation
 Metabolic integration and Regulation 109700: Graduate Biochemistry Trimester 2/2016 Assistant Prof. Dr. Panida Khunkaewla kpanida@sut.ac.th School of Chemistry Suranaree University of Technology 1 Overview
Metabolic integration and Regulation 109700: Graduate Biochemistry Trimester 2/2016 Assistant Prof. Dr. Panida Khunkaewla kpanida@sut.ac.th School of Chemistry Suranaree University of Technology 1 Overview
LESSON 2.4 WORKBOOK. Part two: Glucose homeostasis in the blood Un-Storing energy
 DEFINITIONS OF TERMS Fasting A state of abstinence from all food or drinks that provide calories. For a complete list of defined terms, see the Glossary. LESSON 2.4 WORKBOOK Part two: Glucose homeostasis
DEFINITIONS OF TERMS Fasting A state of abstinence from all food or drinks that provide calories. For a complete list of defined terms, see the Glossary. LESSON 2.4 WORKBOOK Part two: Glucose homeostasis
Moh Tarek. Razi Kittaneh. Jaqen H ghar
 14 Moh Tarek Razi Kittaneh Jaqen H ghar Naif Karadsheh Gluconeogenesis is making glucose from non-carbohydrates precursors. Although Gluconeogenesis looks like Glycolysis in many steps, it is not the simple
14 Moh Tarek Razi Kittaneh Jaqen H ghar Naif Karadsheh Gluconeogenesis is making glucose from non-carbohydrates precursors. Although Gluconeogenesis looks like Glycolysis in many steps, it is not the simple
Connections of Carbohydrate, Protein, and Lipid Metabolic Pathways
 OpenStax-CNX module: m44441 1 Connections of Carbohydrate, Protein, and Lipid Metabolic Pathways OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution
OpenStax-CNX module: m44441 1 Connections of Carbohydrate, Protein, and Lipid Metabolic Pathways OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution
Regulation of Metabolism
 Regulation of Metabolism Pratt and Cornely Chapter 19 Regulation by Compartmentalization Form of reciprocal regulation Degradation vs biosynthesis Requires transporters 1 Specialization of organs Fuel
Regulation of Metabolism Pratt and Cornely Chapter 19 Regulation by Compartmentalization Form of reciprocal regulation Degradation vs biosynthesis Requires transporters 1 Specialization of organs Fuel
Fatty Acid and Triacylglycerol Metabolism 1
 Fatty Acid and Triacylglycerol Metabolism 1 Mobilization of stored fats and oxidation of fatty acids Lippincott s Chapter 16 What is the first lecture about What is triacylglycerol Fatty acids structure
Fatty Acid and Triacylglycerol Metabolism 1 Mobilization of stored fats and oxidation of fatty acids Lippincott s Chapter 16 What is the first lecture about What is triacylglycerol Fatty acids structure
The molecule that serves as the major source of readily available body fuel is: a. fat. b. glucose. c. acetyl CoA. d. cellulose.
 The molecule that serves as the major source of readily available body fuel is: a. fat. b. glucose. c. acetyl CoA. d. cellulose. Dietary fats are important because: a. they keep blood pressure normal.
The molecule that serves as the major source of readily available body fuel is: a. fat. b. glucose. c. acetyl CoA. d. cellulose. Dietary fats are important because: a. they keep blood pressure normal.
Lipid Metabolism. Catabolism Overview
 Lipid Metabolism Pratt & Cornely, Chapter 17 Catabolism Overview Lipids as a fuel source from diet Beta oxidation Mechanism ATP production Ketone bodies as fuel 1 High energy More reduced Little water
Lipid Metabolism Pratt & Cornely, Chapter 17 Catabolism Overview Lipids as a fuel source from diet Beta oxidation Mechanism ATP production Ketone bodies as fuel 1 High energy More reduced Little water
The Glucose Ketone Index Calculator: A Simple Tool to Monitor Therapeutic. Efficacy for Metabolic Management of Brain Cancer
 Nutrition & Metabolism (in press) The Glucose Ketone Index Calculator: A Simple Tool to Monitor Therapeutic Efficacy for Metabolic Management of Brain Cancer Joshua J. Meidenbauer, Purna Mukherjee and
Nutrition & Metabolism (in press) The Glucose Ketone Index Calculator: A Simple Tool to Monitor Therapeutic Efficacy for Metabolic Management of Brain Cancer Joshua J. Meidenbauer, Purna Mukherjee and
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 25 Metabolism and Nutrition Metabolic Reactions Metabolism refers to all of the chemical reactions taking place in the body. Reactions that break
Principles of Anatomy and Physiology 14 th Edition CHAPTER 25 Metabolism and Nutrition Metabolic Reactions Metabolism refers to all of the chemical reactions taking place in the body. Reactions that break
Energy Metabolism. Chapter Cengage Learning. All Rights Reserved.
 Energy Metabolism Chapter 7 Introduction Energy Heat, mechanical, electrical, and chemical Metabolism How the body uses foods to meet its needs Chemical Reactions in the Body Energy metabolism How body
Energy Metabolism Chapter 7 Introduction Energy Heat, mechanical, electrical, and chemical Metabolism How the body uses foods to meet its needs Chemical Reactions in the Body Energy metabolism How body
5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM
 5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM Introduction: Variety of hormones and other molecules regulate the carbohydrates metabolism. Some of these have already been cited in previous sections.
5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM Introduction: Variety of hormones and other molecules regulate the carbohydrates metabolism. Some of these have already been cited in previous sections.
Glucose is the only source of energy in red blood cells. Under starvation conditions ketone bodies become a source of energy for the brain
 Glycolysis 4 / The Text :- Some Points About Glucose Glucose is very soluble source of quick and ready energy. It is a relatively stable and easily transported. In mammals, the brain uses only glucose
Glycolysis 4 / The Text :- Some Points About Glucose Glucose is very soluble source of quick and ready energy. It is a relatively stable and easily transported. In mammals, the brain uses only glucose
Fatty Acid Degradation. Catabolism Overview. TAG and FA 11/11/2015. Chapter 27, Stryer Short Course. Lipids as a fuel source diet Beta oxidation
 Fatty Acid Degradation Chapter 27, Stryer Short Course Catabolism verview Lipids as a fuel source diet Beta oxidation saturated Unsaturated dd chain Ketone bodies as fuel Physiology High energy More reduced
Fatty Acid Degradation Chapter 27, Stryer Short Course Catabolism verview Lipids as a fuel source diet Beta oxidation saturated Unsaturated dd chain Ketone bodies as fuel Physiology High energy More reduced
Overview of Metabolism and provision of metabolic fuel. Dr. Uzma Nasib
 Overview of Metabolism and provision of metabolic fuel Dr. Uzma Nasib Metabolism The Transformation of Energy Cells Can t Eat Hamburgers How Does the Body Fuel Metabolism Metabolism (from Greek: metabolē,
Overview of Metabolism and provision of metabolic fuel Dr. Uzma Nasib Metabolism The Transformation of Energy Cells Can t Eat Hamburgers How Does the Body Fuel Metabolism Metabolism (from Greek: metabolē,
Name Class Date. 1. Cellular respiration is the process by which the of "food"
 Name Class Date Cell Respiration Introduction Cellular respiration is the process by which the chemical energy of "food" molecules is released and partially captured in the form of ATP. Carbohydrates,
Name Class Date Cell Respiration Introduction Cellular respiration is the process by which the chemical energy of "food" molecules is released and partially captured in the form of ATP. Carbohydrates,
Energy Production In A Cell (Chapter 25 Metabolism)
 Energy Production In A Cell (Chapter 25 Metabolism) Large food molecules contain a lot of potential energy in the form of chemical bonds but it requires a lot of work to liberate the energy. Cells need
Energy Production In A Cell (Chapter 25 Metabolism) Large food molecules contain a lot of potential energy in the form of chemical bonds but it requires a lot of work to liberate the energy. Cells need
MULTIPLE CHOICE QUESTIONS
 MULTIPLE CHOICE QUESTIONS 1. Which of the following statements concerning anabolic reactions is FALSE? A. They are generally endergonic. B. They usually require ATP. C. They are part of metabolism. D.
MULTIPLE CHOICE QUESTIONS 1. Which of the following statements concerning anabolic reactions is FALSE? A. They are generally endergonic. B. They usually require ATP. C. They are part of metabolism. D.
Metabolism: From Food to Life
 CHAPTER 7 Metabolism: From Food to Life Chapter Summary Metabolism is the sum total of all chemical and physical processes by which the body catabolizes and anabolizes molecules. Metabolic pathways are
CHAPTER 7 Metabolism: From Food to Life Chapter Summary Metabolism is the sum total of all chemical and physical processes by which the body catabolizes and anabolizes molecules. Metabolic pathways are
Unit 2: Metabolic Processes
 How is energy obtained biologically? Recall: Red Ox Reactions Unit 2: Metabolic Processes Oxidation Is the chief mechanism by which chemical potential energy is released This energy comes from reduced
How is energy obtained biologically? Recall: Red Ox Reactions Unit 2: Metabolic Processes Oxidation Is the chief mechanism by which chemical potential energy is released This energy comes from reduced
Metabolism Energy Pathways Biosynthesis. Catabolism Anabolism Enzymes
 Topics Microbial Metabolism Metabolism Energy Pathways Biosynthesis 2 Metabolism Catabolism Catabolism Anabolism Enzymes Breakdown of complex organic molecules in order to extract energy and dform simpler
Topics Microbial Metabolism Metabolism Energy Pathways Biosynthesis 2 Metabolism Catabolism Catabolism Anabolism Enzymes Breakdown of complex organic molecules in order to extract energy and dform simpler
Hompes Method Lesson 29 Organic Acids Part Three
 Hompes Method Lesson 29 Organic Acids Part Three Health for the People Ltd not for reuse without expressed permission Organic Acids - Review Fats, carbohydrates, and amino acids are converted into carboxylic
Hompes Method Lesson 29 Organic Acids Part Three Health for the People Ltd not for reuse without expressed permission Organic Acids - Review Fats, carbohydrates, and amino acids are converted into carboxylic
METABOLISM CATABOLIC Carbohydrates Lipids Proteins
 Index: - Overview: Catabolism and Anabolism. Few concepts:, NADPH. - Overview: Metabolism glucose, fatty acids and amino acids. - Table summary: Principal anabolic and catabolic pathways, and their main
Index: - Overview: Catabolism and Anabolism. Few concepts:, NADPH. - Overview: Metabolism glucose, fatty acids and amino acids. - Table summary: Principal anabolic and catabolic pathways, and their main
Manipulation of the Nutrient Sensors (AMPK/TOR) with Anaplerotic Diet Therapy (Triheptanoin) An Alternative to Diet Restriction
 Manipulation of the Nutrient Sensors (AMPK/TOR) with Anaplerotic Diet Therapy (Triheptanoin) An Alternative to Diet Restriction CharlesR.Roe,MD Institute of Metabolic Disease Baylor University Medical
Manipulation of the Nutrient Sensors (AMPK/TOR) with Anaplerotic Diet Therapy (Triheptanoin) An Alternative to Diet Restriction CharlesR.Roe,MD Institute of Metabolic Disease Baylor University Medical
(de novo synthesis of glucose)
 Gluconeogenesis (de novo synthesis of glucose) Gluconeogenesis Gluconeogenesis is the biosynthesis of new glucose. The main purpose of gluconeogenesis is to maintain the constant blood Glc concentration.
Gluconeogenesis (de novo synthesis of glucose) Gluconeogenesis Gluconeogenesis is the biosynthesis of new glucose. The main purpose of gluconeogenesis is to maintain the constant blood Glc concentration.
The Arctic Variant of CPT-1A
 The Arctic Variant of CPT-1A Matthew Hirschfeld, MD/PhD Department of Pediatric Hospital Medicine Alaska Native Medical Center Anchorage, AK Background CPT-1 = carnitine palmitoyltransferase type 1 Expressed
The Arctic Variant of CPT-1A Matthew Hirschfeld, MD/PhD Department of Pediatric Hospital Medicine Alaska Native Medical Center Anchorage, AK Background CPT-1 = carnitine palmitoyltransferase type 1 Expressed
BIOCHEMISTRY. Glycolysis. by Dr Jaya Vejayan Faculty of Industrial Sciences & Technology
 BIOCHEMISTRY Glycolysis by Dr Jaya Vejayan Faculty of Industrial Sciences & Technology email: jayavejayan@ump.edu.my Chapter Description Overview This chapter is related to carbohydrate catabolism. It
BIOCHEMISTRY Glycolysis by Dr Jaya Vejayan Faculty of Industrial Sciences & Technology email: jayavejayan@ump.edu.my Chapter Description Overview This chapter is related to carbohydrate catabolism. It
ENERGY FROM INGESTED NUTREINTS MAY BE USED IMMEDIATELY OR STORED
 QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
BCH Graduate Survey of Biochemistry
 BCH 5045 Graduate Survey of Biochemistry Instructor: Charles Guy Producer: Ron Thomas Director: Marsha Durosier Lecture 44 Slide sets available at: http://hort.ifas.ufl.edu/teach/guyweb/bch5045/index.html
BCH 5045 Graduate Survey of Biochemistry Instructor: Charles Guy Producer: Ron Thomas Director: Marsha Durosier Lecture 44 Slide sets available at: http://hort.ifas.ufl.edu/teach/guyweb/bch5045/index.html
Chapter 7- Metabolism: Transformations and Interactions Thomson - Wadsworth
 Chapter 7- Metabolism: Transformations and Interactions 2008 Thomson - Wadsworth Simple Overview of Energy Metabolism The sum of all chemical reactions that go on in living cells Introduction Energy Heat-
Chapter 7- Metabolism: Transformations and Interactions 2008 Thomson - Wadsworth Simple Overview of Energy Metabolism The sum of all chemical reactions that go on in living cells Introduction Energy Heat-
Anaerobic Pathways. Glycolysis
 Anaerobic Pathways Glycolysis Glucose + 2 ATP 4 ATP + 2 Pyruvate No oxygen required Fairly low energy yield Lactate byproduct Resting levels low Tolerances 40 mmole/kg in humans, 200 mmole/kg in sea turtles
Anaerobic Pathways Glycolysis Glucose + 2 ATP 4 ATP + 2 Pyruvate No oxygen required Fairly low energy yield Lactate byproduct Resting levels low Tolerances 40 mmole/kg in humans, 200 mmole/kg in sea turtles
DEPARTMENT OF SCIENCE COURSE OUTLINE Fall 2018 BC 2000 INTRODUCTORY BIOCHEMISTRY 3 (3-0-0) 45 HOURS FOR 15 WEEKS
 DEPARTMENT OF SCIENCE COURSE OUTLINE Fall 2018 BC 2000 INTRODUCTORY BIOCHEMISTRY 3 (3-0-0) 45 HOURS FOR 15 WEEKS INSTRUCTOR: Beatrice Amar Ph.D. PHONE: 780-539-2031 OFFICE: J208 E-MAIL: Bamar@gprc.ab.ca
DEPARTMENT OF SCIENCE COURSE OUTLINE Fall 2018 BC 2000 INTRODUCTORY BIOCHEMISTRY 3 (3-0-0) 45 HOURS FOR 15 WEEKS INSTRUCTOR: Beatrice Amar Ph.D. PHONE: 780-539-2031 OFFICE: J208 E-MAIL: Bamar@gprc.ab.ca
