T HE use of balloon catheters in medicine is
|
|
|
- Avis Cunningham
- 5 years ago
- Views:
Transcription
1 J Neurosurg 52: , 1980 Some examples of balloon technology in neurosurgery SEAN MULLAN, M.D., EUGENE E. DUDA, M.D., AND NICHOLAS J. PATRONAS, M.D. Section of Neurological Surgery, University of Chicago Hospitals, Chicago, Illinois v' Examples are presented of the use of a compression balloon to treat trigeminal neuralgia, of a dilating balloon to release a web obstruction of the internal carotid artery, of detachable balloons to seal carotidcavernous and vertebral-venous fistulas, of a temporary occlusive balloon to aid in thrombogenic treatment of a giant aneurysm, and of a temporary occlusive balloon with double or triple-lumen capacity to assist in angiographic diagnosis and to provide reversible carotid occlusion. KEY WORDS 9 balloon 9 aneurysm 9 arteriovenous fistula 9 trigeminal neuralgia 9 carotid artery occlusion T HE use of balloon catheters in medicine is not new. In 1951, Carlens, et al.? used an occlusive balloon technique to obtain better angiographic detail. In 1963, Fogarty, et al., 7 introduced the operating catheter to remove arterial clot, and in 1964, Dotter and Judkins 6 described a dilating catheter. In 1970, Kessler and Wholey H occluded the internal carotid artery as treatment for intracranial aneurysm, and in 1971, Prolo and Hanbery 15 occluded it in the treatment of a carotidcavernous fistula. Others have utilized these occlusive balloons with success in carotid-cavernous, carotidjugular, and vertebral-jugular fistulas. 8'~~ Serbinenko ~8,1~ and later Debrun, et al., 8-5 described their detachable balloons, which offered the possibility of sealing a fistula or an aneurysm while sparing the arterial flow. Recently, we have described occlusion of a carotid-cavernous fistula by a transjugular balloon? ~ Our own experience also includes the occlusive radiography balloon, the permanent arterial occlusive balloon, and the detachable balloon. In addition, we have used a triple-lumen catheter with balloon for temporary occlusion of the carotid artery, a Fogartytype catheter to prevent surgically induced thrombus in a giant aneurysm from entering the parent artery, a balloon to dilate a web-stenosed carotid artery, and a compressive balloon which percutaneously compresses the trigeminal ganglion to relieve trigeminal neuralgia. Since our numbers in each category are limited, we will describe only a few significant cases in order to portray something of the scope of these new neurosurgical tools. Further experience will be nec- essary to delineate their clinical indications and limitations. Trigeminal Neuralgia This case illustrates the use of a No. 4 or 5 Fogarty catheter* compressive balloon with single lumen. Case 1. This 76-year-old woman had experienced trigeminal neuralgia for 14 years. Ten years previously, the right trigeminal ganglion was "compressed" at another institution, and she has had no further trigeminal neuralgia on the right. Two years later, left trigeminal neuralgia developed and it, too, was "compressed" at the same institution. Relief on this side lasted 3 years. She then had a radiofrequency lesion placed and relief lasted for 2 years. Since that time she has been taking Tegretol (carbamazepine) with decreasing relief. When she was first seen by us, it was impossible to test for sensation adequately because of the exquisitely sensitive "trigger" zones in the left second and third trigeminal divisions. With the patient under brief general anesthesia, a No. 4 Fogarty catheter balloon was inserted into the left trigeminal ganglion through a percutaneous No. 12 needle. It was inflated with 0.75 cc of Pantopaque for 10 minutes. It should be noted that the balloon tended to extrude into the neck of Meckel's cave, in- *Fogarty catheter manufactured by Downs Surgical, Ltd., Surrey, England. J. Neurosurg. / Volume 52 / March,
2 S. Mullan, E. E. Duda and N. J. Patronas dicating that the entering root sustained a substantial compression (Fig. 1). Postoperatively, she has been totally free from pain. There is a slight objective decrease in pin and touch sensation in the second division of her left fifth facial nerve. Because we were not able to test her adequately preoperatively, it is not possible to know how much of her sensory loss was due to her previous treatments and how much was due to the balloon compression. Giant Aneurysm This case illustrates the use of a No. 4 or 5 Fogarty catheter thrombogenic balloon with single lumen. Case 2. This 53-year-old woman was thought to have had a right "cavernous sinus thrombosis" for 10 years. At the onset, she had complete ophthalmoplegia, numbness in the first and second division of her right fifth facial nerve, and some right facial weakness. She improved with heparin and antibiotics, and recovered some good, but imperfect, eye movement. Numbness almost completely disappeared, and the facial strength returned to normal. Recent pain, right visual loss, and a subsequent computerized tomography (CT) scan led to angiography which disclosed a giant cavernous aneurysm (Fig. 2 upper left). She could not tolerate carotid artery compression, and therefore was ineligible for carotid ligation. These giant cavernous sinus aneurysms have, in our experience, a wide neck. In fact, it might be better to state that the proximal artery enters one point of the aneurysm and, a short distance away, the distal artery leaves the aneurysm wall. This was clearly demonstrated to us in one patient who died after FIG. I. Case 1. Angiographic view of a No. 4 Fogarty catheter balloon inserted into the left trigeminal ganglion through a percutaneous No. 12 needle. Note that the needle need not penetrate distal to the foramen ovale. The indentation in the left of the contrast-filled balloon represents unexpelled air. The protrusion to the right represents extension through the neck of Meckel's cave toward the posterior fossa. carotid occlusion subsequent to thrombosis of the aneurysm. Detailed angiography (Fig. 2 upper right) demonstrated an exactly similar situation in this patient. At craniotomy, therefore, we inserted two No. 5 Fogarty catheters into the aneurysm wall, inflated them with 1.0 cc contrast material each, and pushed one against the internal opening of the aneurysm (Fig. 2 lower left). The lumen of the aneurysm was then thrcmbosed by phosphor bronze wire after the lateral balloon was deflated; the clot was extruded from the carotid artery by the medial balloon. Probably only the medial balloon was necessary. When thrombosis was complete, as indicated by needling, this balloon was also decompressed and withdrawn. The postoperative radiograph demonstrated a subtotal occlusion of the aneurysm; the small portion adjacent to the neck was free from clot (Fig. 2 lower right). Subjectively, the patient has been quite well, with improved visual acuity and relief from her retroorbital pain. Web Obstruction of the Internal Carotid Artery This case illustrates the use of a Griintzig dilating balloon catheter.t Case 3. This 35-year-old woman presented with diplopia and pain behind her left eye. She also had tingling in the left side of her face. On examination, she had a partial left ophthalmoplegia. Her pain could be relieved by left carotid artery compression. Angiography demonstrated a giant aneurysm of the left cavernous sinus. Subsequent to this study, she had experienced a temporary left hemiparesis. After all methods and hazards were explained, the patient elected to undergo occlusion of the left internal carotid artery. This was safely carried out by an initial partial occlusion, after which all of the aneurysm except the neck area was seen to thrombose. It was completed under heparin, to prevent embolization of a spreading clot and to permit instant reopening should ischemia occur. Subsequently, her headache, ophthalmoplegia, and diplopia totally disappeared. Three months later, she complained of a pulsating noise in her right ear and of a thrill in the right side of her neck. Examination confirmed the thrill and a loud bruit over the right internal carotid artery. Angiography demonstrated a web-like constriction in the proximal right internal carotid artery, with some irregularities in the distal internal and in the external carotid arteries. After much deliberation, operative repair of the constriction was considered too dangerous, and the patient was discharged on a course of aspirin. Six months later, the symptoms and signs were unchanged tgrfintzig balloon catheter manufactured by Cook Catheter Co., Bloomington, Indiana. 322 J. Neurosurg. / Volume 52 / March, 1980
3 Balloon technology in neurosurgery but the arteriographic appearance (Fig. 3 left) was decidedly worse, suggesting that total occlusion was a distinct possibility. A Grtintzig dilating double-lumen catheter was chosen; this carries a firm balloon made of plastic rather than rubber, thus it cannot expand more than its chosen diameter which should not exceed that of the normal carotid artery. This ensures against rupture. The balloon is tapered proximally and distally. The waist lies several centimeters from the tip. FIo. 2. Case 2. Giant cavernous aneurysm demonstrated by angiography. Upper Left: The lateral view of the angiogram does not show the "neck" region of the giant aneurysm. Upper Right: After much radiographic effort, a selective view demonstrates the "neck" region. It is clearly seen that the entering and leaving arteries are separate. Lower Left." Two Fogarty catheters can be seen within the aneurysm. The more medial catheter guards the carotidartery against induced thrombosis; the other was probably unnecessary. Lower Right." The opaque area of the carotid artery superior to the coiled thrombogenic wire represents the distended area of the aneurysm "neck." In fact, it remains a small aneurysm. Y. Neurosurg. / Volume 52 / March,
4 S. Mullan, E. E. Duda and N. J. Patronas Ftc. 3. Case 3. Left: Angiography showing the web-like constriction in the proximal right internal carotid artery, with irregularities in the remaining internal and the external carotid arteries. Right: Appearance after dilation. Fluoroscopic imaging can be carried out by filling the balloon with a saline contrast mixture and by outlining the artery distally through the distal port. The catheter was inserted transfemorally and its tip guided up distal to the area of stenosis. The balloon was inflated for 5 seconds with 0.5 ml of fluid. When the force of the expanding balloon met the resistance of the stenosis, the balloon migrated inferiorly into the wider proximal lumen. Care was taken not to place the waist distal to the obstruction lest the expanding balloon should drive the rather firm catheter tip against a distal carotid bend. The balloon was inflated a total of eight times for 5 seconds each before the web was seen on fluoroscopy to disappear, although the continued proximal migration indicated that the base was still rigid (Fig. 3 right). The distal internal carotid irregularity was also smoothed out, but the external carotid, which had not been distended, remained unaltered. The catheter was then withdrawn, and the patient received heparin for 3 days to prevent any clots from forming on the dilated intima. The patient's symptoms have entirely disappeared. A faint bruit can still be heard, which may relate to the external carotid irregularity that persists. Carotid-Cavernous Fistula Cases 4 and 5 illustrate the use of a triple-lumen diagnostic occlusive balloon with a special catheter, and a detachable balloon with a Debrun catheter.~. Case 4. This 17-year-old girl sustained a fractured femur, a closed-head injury, and a right carotidcavernous fistula in an automobile accident. Two weeks later, her right eye had total ophthalmoplegia and proptosis. There was chemosis in both eyes. The leak was so large that the "neck" of the fistulous communication could not be accurately visualized angiographically (Fig. 4 upper left). Debrun's occlusive radiographic maneuver was used. This consists of vertebral injection to fill the fistula from above through the posterior communicating artery, while the carotid is proximally occluded (in this case by intracarotid triple-lumen balloon). In addition, we injected contrast material through the distal port while the balloon was distended. This located the site of the leak at the base of the skull but did not clearly delineate its exact size (Fig. 4 upper right). An initial craniotomy failed to close the fistula by cavernous sinus occlusion. Two weeks later, it was successfully occluded by a detachable balloon. The technique used was that described by Debrun, et al? The catheter floated freely through the fistulous opening (Fig. 4 lower left). Difficulty was experienced in filling the balloon to the exact volume necessary to effect the closure (Fig. 4 lower center); filling until it :l:special catheter manufactured by American Catheter Corp., Indian Mills, New Jersey; Debrun catheter manufactured by Ingenor, 70 Rue Orfila, Paris, France. 324 J. Neurosurg. / Volume 52 / March, 1980
5 Balloon technology in neurosurgery FIG. 4. Case 4. Angiographic demonstration of a right carotid-cavernous fistula. Upper Left: The fistula drains mainly inferiorly. There is little intracranial arterial filling and only moderate orbital venous filling. Upper Right." Slow filling distal to the occluded balloon shows the site of the fistula. Lower Left." The partly distended balloon passes easily into the fistula. Lower Center: Distention of the balloon within the venous compartment may occlude the carotid artery (radiographic-type contrast material was used). Lower Right: The special contrast material has partly settled out from the Silastic mixture and outlines the posterior aspect of the balloon. The negative anterior shadow indicates its anterior extension. The carotid artery is slightly indented. merely opposed the carotid was not enough, it had to be filled so that it impinged slightly upon the carotid from outside before the leak stopped. The required volume of contrast was then replaced by Silastic. One hour later, when a control sample of Silastic on the table had solidified, the catheter was withdrawn. Carotid flow was excellent (Fig. 4 lower right). The ophthalmoplegia totally disappeared, and the patient has since vigorously resumed all of her previous activities. Case 5. This 61-year-old man began to notice swell- ing of his right eye and right-sided headaches shortly after a minor brawl. Two months later when he was first seen, his right eye was completely ophthalmoplegic and he could not count fingers accurately with that eye. Since the visual loss was recent and rapidly progressive and since good arteriograms were available, it was believed that an emergency procedure might save his eyesight but that the delay inherent in a regularly scheduled procedure (as in a recent previous experience of ours) might lose it. Therefore, under local anesthesia, we prepared to insert a detachable balloon. This failed to enter the fistula, as we J. Neurosurg. / Volume 52 / March,
6 S. Mullan, E. E. Duda and N. J. Patronas suspected it might, because the fistulous connection was small (Fig. 5 upper). As we have previously commented, 14 visual loss may be severe if the drainage is exclusively anterior, whether the leak is, in fact, either small or large. This loss is related to the pressure the leak exerts upon the retina rather than to the volume of the leak, which in many instances is rapidly dispersed posteriorly. We therefore inserted a triplelumen No. 4 catheter up to the level of the fistula and occluded the lumen by distending the balloon with 0.2 ml contrast material. Proximal or distal thrombus formation was prevented by continuous irrigation of the proximal and distal ports with heparinized saline (1/1000 normal saline at 10 cc/hr) (Fig. 5 lower). Within 2 hours, the patient could clearly recognize faces; the next day he could read large print. Sixty hours later, the balloon spontaneously decompressed, and he could hear the murmur again. Within an hour his vision was reduced to his admission level. The balloon was again distended, resulting in a rapid FIG. 5. Case 5. Upper." The main drainage from this relatively small fistula is anteriorly into the orbit. Lower: The distended balloon blocks the fistula. Contrast material is injected through the proximal part (left) and the distal part (right). 326 J. Neurosurg. / Volume 52 / March, 1980
7 Balloon technology in neurosurgery return of vision. The patient was then taken to the operating room for craniotomy to occlude the fistula from its cavernous aspect. Before the skin incision was completed, the anesthesiologist noted that the heparin line to the distal catheter port had become disconnected. Blood could not be withdrawn. This raised the possibility of formation of a distal thrombus and its migration if we decompressed the balloon. It was therefore decided that we should seal the catheter in the distended position and bury the end in the neck tissues. The craniotomy attempt was stopped. In the ensuing year, the patient has been perfectly well with full restoration of visual acuity. It has not been possible to persuade him to have an arteriogram for review of the status of his distended balloon. Presumably it has again decompressed, but there has been no return of the fistula. Jugular- Venous Fistula This case illustrates the use of the double-lumen transfemoral diagnostic balloon with a Cook catheter, and the detachable balloon with a Debrun catheter. Case 6. Ten months previously, this 31-year-old man was hit on the back of the head with a baseball bat. Immediately, he was aware of a throbbing sound, which at first he thought was the sound of an external motor. Later he could decrease this sound by squeez- ing behind his mastoid on the left, and could convert it into a whistle by extending his neck. He had intense headaches initially, which improved over a few months and then got worse again. He had a left vertebral-venous fistula at the level of the posterior arch of the atlas, and a direct surgical attack failed to resolve it. Following this, the noise decreased for a few weeks and then returned more loudly than ever. The total left vertebral blood flow and some of the right vertebral flow discharged into the fistula. The fistulous site could not be viewed accurately because of the rapid and bulbous venous filling in the area. Occlusive left vertebral angiography by the transfemoral route delineated the fistula more easily on the posterior arch medial to the lateral mass (Fig. 6 left and center), Through a C-7 cutdown approach to the left vertebral artery, a Debrun balloon was floated up into the fistula. However, the middle catheter, which is necessary for detaching the balloon, stopped at the vertical and horizontal angle on the lateral arch of C-I, and did not accompany the balloon and inner catheter into the fistula. Distention of the balloon with 0.3 ml of contrast material stopped the murmur. Angiography showed complete closure of the fistula with good distal vertebral flow (Fig. 6 right). Distention to 0.5 ml did not alter the continuously recorded somatosensory evoked potentials. We were unwilling to distend the balloon (which had a capacity of 2.0 ml) FIG. 6. Case 6. Left vertebral-venous fistula demonstrated by angiography. Left: Lateral view of the subtraction occlusion angiography shows the flow and permits locating of the leak on the posterior aspect of the arch C-I. Note the balloon at C4-5. Center: Anteroposterior view of the subtraction occlusion angiography discloses the medial location of the fistula. Venous drainage is initially inside the spinal canal. Right: The Debrun balloon, which contains Silastic, is not visible. Arrows indicate the restored vertebral flow. Metallic discs are on the patient's ear lobes as part of the evoked potential measurement equipment. J. Neurosurg. / Volume 52 / March,
8 S. Mullan, E. E. Duda and N. J. Patronas any further, lest any pressure should be applied to the cord, or lest we should occlude the artery by compression from without. The catheter simply did not penetrate deeply into the venous system, and stopped only a few millimeters outside the presumed wall of the artery. The balloon was decompressed and the murmur returned. The balloon was then inflated with 0.3 ml of Silastic. Again the murmur ceased and angiography revealed a good distal flow. Renewed attempts to guide the middle catheter into the horizontal limb of the artery again failed, and we had to make a major decision on how to handle the detachment problem without the counter pressure that this catheter should provide. We were again reluctant to distend the balloon more than was necessary to secure occlusion. A good pull on the catheter of this small balloon might withdraw the distended balloon back into the artery, reopening the fistula and blocking the artery. A forceful pull might even tear the artery. We therefore decided reluctantly that the best solution was to leave the entering catheter in situ, cutting it off as it exited from the vertebral artery at C-7 in the neck. This was done, the sheath catheter was removed, and the puncture site wffs repaired by fine sutures. Angiography 1 week later showed that the left vertebral artery had occluded. The patient remains symptom-free. Discussion At the moment, the range of indications and the safety of these instruments are being explored. The simplest method, and that of potentially widest application, is the single-lumen compressive catheter, which revives the Taarnh~j-Sheldon-Pudenz procedure for trigeminal neuralgia? ~ This procedure began in an attempt to decompress the trigeminal nerve and developed into a deliberate operative compression, as in Case 1. This patient's experience indicated that the procedure was sometimes successful for as long as 10 years, although in other patients the duration was much shorter. The uncertain duration, together with some disturbing paresthesias, brought about its gradual decline as a therapeutic method. A percutaneous insertion of a compressing instrument under brief anesthesia should produce equally good results, freed from the inconveniences and dangers of a major operation. Our current experience with six patients over a period of 6 months bears this out. In fact, the procedure is technically more simple, safer, and more acceptable to the patient than either an alcohol or a radiofrequency needle insertion. The needle need not enter the foramen ovale; it must merely engage it. The blunt catheter then penetrates the foramen ovale, thus freeing the carotid artery and the cavernous sinus from the risk of needle injury. The degree and duration of distention remain to be determined by experience. Perhaps it might be arrived at more scientifically by a study of suppression of evoked potentials. Obviously, the degree of distention of a balloon located entirely within the cave is different from that of one that protrudes out through the cave entrance. Double- or triple-lumen balloons for occlusive diagnostic radiology offer a clear advantage in some fistulas and aneurysms, and appear to offer no added hazard to the patient (see Cases 4, 5 and 6). Transfemoral catheters are becoming available, and the procedure might now be regarded as established. In the treatment of fistulas, it appears that detachable balloons that enter the venous sac and totally spare the arterial flow are ideal. If they can be made to enter the cavernous sinus through the jugular vein, this would be ideal for carotid-cavernous fistulas with a posterior leak. In this we were successful in only one patient out of four. 1~ In one, the catheter always entered the lateral sinus. In a child, it entered the inferior petrosal sinus but would not ascend high enough to enter the cavernous sinus. In a third case, it entered the cavernous sinus successfully, but the fistula was then disclosed to lie anteriorly. Theoretically, a transarterial balloon is the next best device. We were successful in one of three attempts with this balloon. In the two failures, the lumen of the fistula was apparently too small or not in line with the catheter direction. However, for the larger, most difficult posttraumatic cases, as in Case 4, with a very large opening, a flow-directed entry into the fistulous sac was easy, and the method has much promise over cavernous occlusion by craniotomy. The latter remains the treatment of choice for the smaller fistulas, those in which the opening is not in the line of the ascending balloon, and for those patients who cannot tolerate carotid occlusion. The detaching mechanism is not yet without problems, as seen in Case 5. Such balloons can be detached in the straight ascending portion of the vertebral artery even when introduced transfemorally, 14 but the detaching collar may have difficulty in negotiating an angled bend. Since the applicability of these balloons is now probably established, it might be assumed that ingenuity will in time improve the detachment mechanism. The role of the thrombotic balloon in giant aneurysms is still quite undeveloped. It would appear that a coiled wire core in the catheter (as in the Fogarty catheter), which gives the operator the ability to control the direction of the catheter after insertion, is essential. In another patient, the triple-lumen catheter, without a wire core, was used. It floated in the center of the aneurysm without occluding the neck. The size of the balloon, the use of multiple balloons rather than a single balloon, the quantity, if any, of additional thrombogenic wire, and the sequence of wire before balloon or balloon before wire are all factors that must be worked out. The role of the triple-lumen, temporarily occluding catheter is another issue that will require experience. 328 J. Neurosurg. / Volume 52 / March, 1980
9 Balloon technology in neurosurgery The occluding balloon with proximal and distal ports, providing a continuous flow of heparinized saline proximally and distally, will keep an artery safely occluded, and may be opened safely at any time at election, such as for developing spasm. This offers the possibility of providing rapidly and percutaneously that protection offered by a Selverstone clamp. Whether this will prove useful or not remains to be seen. It might have been lifesaving in the case of transnasal exsanguination recently described by Moore, et al.13 The Griintzig dilating catheter is an efficient instrument for treating web constriction. One must be assured that the area is free from particles that might embolize. It would not appear to be applicable to the more common ulcerated stenosis. Gr~intzig and Kumpe a have recently reviewed the technique. Addendum Since submission of this paper, we have successfully controlled an exsanguinating carotid hemorrhage in a patient with neck cancer by means of an occluding balloon. References 1. Binkley FM, Wylie E J: A new technique for obliteration of cerebrovascular arteriovenous fistulae. Arch Surg 106: , Carlens E, Hanson HE, Nordenstr6m B: Temporary unilateral occlusion of the pulmonary artery. J Thorac Surg 22: , Debrun G, Lacour P, Caron JP, et al: Detachable balloon and calibrated-leak balloon techniques in the treatment of cerebral vascular lesions. J Neurosurg 49: , Debrun G, Lacour P, Caron JP, et al: Experimental approach to the treatment of carotid-cavernous fistulas with an inflatable and isolated balloon. Neuroradiolngy 9:9-12, Debrun G, Legre J, Kasbarian M, et al: Endovascular occlusion of vertebral fistulae by detachable balloons with conservation of the vertebral blood flow. Radiology 130: , Dotter CT, Judkins MP: Transluminal treatment of arteriosclerotic obstruction. Description of a new technic and a preliminary report of its application. Circulation 30: , Fogarty T J, Cranley J J, Krause R J, et al: A method for extraction of arterial emboli and thrombi. Surg Gynecol Obstet 116: , Goodman S J, Hasso A, Kirkpatrick D: Treatment of vertebrojugular fistula by balloon occlusion. Case report. J Neurosurg 43: , Grfintzig A, Kumpe DA: Technique of percutaneous transluminal angioplast3; with the Gr~intzig balloon catheter. AJR 132: , Herrmann H-D, Fischer D, Loew F: Experiences with intraluminal occlusion with the Fogarty catheter in the treatment of carotid-cavernous sinus fistulas and other lesions at the base of the skull. Acta Neurochir 32:35-54, I. Kessler LA, Wholey MH: Internal carotid occlusion for treatment of intracranial aneurysms. A new percutaneous technique. Radiology 95: , Lepoire J, Picard L, Montaut J, et al" Traitement des fistules carotido-caverneuses par occlusion endoart6rielle h l'aide d'une sonde ~ ballonnet. Neurochirurgie 20: , Moore D, Budde RB, Hunter CR, et al: Massive epistaxis from aneurysm of the carotid artery. Surg Neurol 11: , Mullan S: Treatment of carotid-cavernous fistulas by cavernous sinus occlusion. J Neurosurg 50: , Prolo DJ, Hanbery JW: Intraluminal occlusion of a carotid-cavernous sinus fistula with a balloon catheter. Technical note. J Neurosurg 35: , Rey A, Cophignon J, Djindjian R, et al: Traitement des fistules carotido-caverneuses. Neurochirurgie 19: , Rougerie J, Giulmet D, Bamberger-Bozo C: An6vrysme carotido-caverneux. Apropos d'une orientation th6rapeutique nouvelle. Neurochirurgie 19: , Serbinenko FA: [Balloon occlusion of a cavernous portion of the carotid artery as a method of treating carotid-cavernous fistulae.] Vopr Neirokhir 6:3-9, 1971 (Rus) 19. Serbinenko FA" Balloon catheterization and occlusion of major cerebral vessels. J Neurosurg 41: , Shelden CH, Pudenz RH, Freshwater DB, et al: Compression rather than decompression for trigeminal neuralgia. J Neurosurg 12: , Taarnh~tj P: Decompression of the trigeminal root and the posterior part of the ganglion as treatment in trigeminal neuralgia. Preliminary communication. J Neurosurg 9: , 1952 Address reprint requests to: Sean Mullan, M.D., Section of Neurological Surgery, University of Chicago Hospitals, 950 East 59th Street, Chicago, Illinois J. Neurosurg. / Volume 52 / March,
Treatment of carotid-cavernous fistula using a balloon-tipped intra-arterial catheter
 Journal of Neurology, Neurosurgery, and Psychiatry, 1978, 41, 996-1000 Treatment of carotid-cavernous fistula using a balloon-tipped intra-arterial catheter U. M. CHOWDHARY From the Department of Neurology,
Journal of Neurology, Neurosurgery, and Psychiatry, 1978, 41, 996-1000 Treatment of carotid-cavernous fistula using a balloon-tipped intra-arterial catheter U. M. CHOWDHARY From the Department of Neurology,
Deflation of metrizamide-filled balloon used to occlude a carotid-cavernous fistula
 J Neurosurg 59:524-528, 1983 Deflation of metrizamide-filled balloon used to occlude a carotid-cavernous fistula Case report THOMAS J. LEIPZIG, M.D., AND SEAN F. MULLAN, M.D. Section of Neurosurgery, University
J Neurosurg 59:524-528, 1983 Deflation of metrizamide-filled balloon used to occlude a carotid-cavernous fistula Case report THOMAS J. LEIPZIG, M.D., AND SEAN F. MULLAN, M.D. Section of Neurosurgery, University
High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils
 High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils Guido Guglielmi, Fernando Viñuela, Gary Duckwiler, Jacques Dion, and Alfredo Stocker Summary: We present one case of
High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils Guido Guglielmi, Fernando Viñuela, Gary Duckwiler, Jacques Dion, and Alfredo Stocker Summary: We present one case of
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Quality Metrics. Stroke Related Procedure Outcomes
 Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography
 Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography Case report ELISHA S. GURDJIAN, M.D., BLAISE AUDET, M.D., RENATO W. SIBAYAN, M.D., AND LLYWELLYN
Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography Case report ELISHA S. GURDJIAN, M.D., BLAISE AUDET, M.D., RENATO W. SIBAYAN, M.D., AND LLYWELLYN
External carotid blood supply to acoustic neurinomas
 External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
National Hospital for Neurology and Neurosurgery
 National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
Transarterial Occlusion of Solitary Intracerebral Arteriovenous Fistulas
 747 Transarterial Occlusion of Solitary Intracerebral Arteriovenous Fistulas Van V. Halbach 1 2 Randall T. Higashida 1 2 Grant B. Hieshima 1 2 Carl W. Hardin 1 Christopher F. Dowd 1 Stanley L. Barnwell
747 Transarterial Occlusion of Solitary Intracerebral Arteriovenous Fistulas Van V. Halbach 1 2 Randall T. Higashida 1 2 Grant B. Hieshima 1 2 Carl W. Hardin 1 Christopher F. Dowd 1 Stanley L. Barnwell
Percutaneous Embolization of Arteriovenous Fistulas of the External Carotid Artery
 937 Percutaneous Embolization of rteriovenous Fistulas of the External Carotid rtery lex erenstein 1 John Scote In Sup Choi 1 Mark Persky3 Nineteen arteriovenous fistulas of the external carotid branches
937 Percutaneous Embolization of rteriovenous Fistulas of the External Carotid rtery lex erenstein 1 John Scote In Sup Choi 1 Mark Persky3 Nineteen arteriovenous fistulas of the external carotid branches
Case Endovascular management of non maturing dyalisis vascular access
 Case 10238 Endovascular management of non maturing dyalisis vascular access Guedes Pinto 1, Erique; Madeira 2, Célia; Sousa 3, Marta; Penha 1, Diana; Rosa 1, Luís; Germano 1, Ana; Baptista 1, Manuela 1
Case 10238 Endovascular management of non maturing dyalisis vascular access Guedes Pinto 1, Erique; Madeira 2, Célia; Sousa 3, Marta; Penha 1, Diana; Rosa 1, Luís; Germano 1, Ana; Baptista 1, Manuela 1
Endovascular Embolization of Taumatic Intracavernous Pseudoaneurysm of Internal Carotid Artery
 Endovascular Embolization of Taumatic Intracavernous Pseudoaneurysm of Internal Carotid Artery Tanveer Ul Haq,Shahzad Ahmad Khan,Imtiaz Hussain Rizvi ( Department of Radiology, The Aga Khan University
Endovascular Embolization of Taumatic Intracavernous Pseudoaneurysm of Internal Carotid Artery Tanveer Ul Haq,Shahzad Ahmad Khan,Imtiaz Hussain Rizvi ( Department of Radiology, The Aga Khan University
Traumatic A-V A V Fistula
 Traumatic A-V A V Fistula PRESENT HISTORY PAST HISTORY 30 year-old, male ( XX); Denied other systemic disease before. PRESENT HISTORY A deep stabbing wound (3*1 cm) noted on 07/01/2002 over Right anterior
Traumatic A-V A V Fistula PRESENT HISTORY PAST HISTORY 30 year-old, male ( XX); Denied other systemic disease before. PRESENT HISTORY A deep stabbing wound (3*1 cm) noted on 07/01/2002 over Right anterior
Abdominal Aortic Aneurysms. A Surgeons Perspective Dr. Derek D. Muehrcke
 Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Treatment of 54 traumatic carotid-cavernous fistulas
 J Neurosurg 55:678-692, 1981 Treatment of 54 traumatic carotid-cavernous fistulas GI~RARD DEBRUN, M.D., PIERRE LACOUR, M.D., FERNANDO VINUELA, M.D., ALLAN FOX, M.D., CHARLES G. DRAKE, M.D., AND JEAN P.
J Neurosurg 55:678-692, 1981 Treatment of 54 traumatic carotid-cavernous fistulas GI~RARD DEBRUN, M.D., PIERRE LACOUR, M.D., FERNANDO VINUELA, M.D., ALLAN FOX, M.D., CHARLES G. DRAKE, M.D., AND JEAN P.
Irretrievable unraveled coil remaining in the vascular lumen between the cerebral aneurysm and puncture site
 Technical Note JNET 3:42-46, 2009 Irretrievable unraveled coil remaining in the vascular lumen between the cerebral aneurysm and puncture site Kouhei NII 1) Masanari ONIZUK 1) Yoshirou KNEKO 2) Hiroshi
Technical Note JNET 3:42-46, 2009 Irretrievable unraveled coil remaining in the vascular lumen between the cerebral aneurysm and puncture site Kouhei NII 1) Masanari ONIZUK 1) Yoshirou KNEKO 2) Hiroshi
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Technique-of catheterization and embolization of the lenticulostriate arteries
 J Neurosurg 54:783-789, 1981 Technique-of catheterization and embolization of the lenticulostriate arteries ALEX BERENSTEIN, M.D. New York University Medical Center and Bellevue Hospital, New York, New
J Neurosurg 54:783-789, 1981 Technique-of catheterization and embolization of the lenticulostriate arteries ALEX BERENSTEIN, M.D. New York University Medical Center and Bellevue Hospital, New York, New
Quick Reference Guide
 Quick Reference Guide Indications for Use The AFX Endovascular AAA System is indicated for endovascular treatment in patients with AAA. The devices are indicated for patients with suitable aneurysm morphology
Quick Reference Guide Indications for Use The AFX Endovascular AAA System is indicated for endovascular treatment in patients with AAA. The devices are indicated for patients with suitable aneurysm morphology
Introduction What Causes Peripheral Vascular Disease? How Do Doctors Treat Peripheral Vascular Disease?... 9
 Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Neurosurgery Sample Case
 120 Beulah Road, NE, Suite 200 Vienna, Virginia 22180 Toll Free: 800-336-0332 Fax: 703-255-6134 www.malpracticeexperts.com Neurosurgery Sample Case The patient had an intra-cerebral artery aneurysm operated
120 Beulah Road, NE, Suite 200 Vienna, Virginia 22180 Toll Free: 800-336-0332 Fax: 703-255-6134 www.malpracticeexperts.com Neurosurgery Sample Case The patient had an intra-cerebral artery aneurysm operated
Mechanisms of presentation of caroticocavernous
 Brit.. Ophthal. (1970) 54, I86 Mechanisms of presentation of caroticocavernous fistulae EDWIN R. BICKERSTAFF The Midland CentreJor Neurosurgery and Neurology, Smethwick The clinical features of carotico-cavernous
Brit.. Ophthal. (1970) 54, I86 Mechanisms of presentation of caroticocavernous fistulae EDWIN R. BICKERSTAFF The Midland CentreJor Neurosurgery and Neurology, Smethwick The clinical features of carotico-cavernous
Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully
 Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Thrombosis in Giant Basilar Tip Aneurysms during Coil Embolization
 Thrombosis in Giant Basilar Tip Aneurysms during Coil Embolization S. A. Renowden and A. J. Molyneux Summary: Two patients with giant basilar tip aneurysms underwent coil embolization, one with both platinum
Thrombosis in Giant Basilar Tip Aneurysms during Coil Embolization S. A. Renowden and A. J. Molyneux Summary: Two patients with giant basilar tip aneurysms underwent coil embolization, one with both platinum
Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases
 Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18
 INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18 www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular Stent Grafts: A treatment for Thoracic Aortic disease Table of
INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18 www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular Stent Grafts: A treatment for Thoracic Aortic disease Table of
Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge Procedure Using the Coil Mass as a Support
 Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
Originally Posted: November 15, 2014 BRUIT IN THE GROIN
 Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Ophthalmoplegia in carotid cavernous sinus fistula
 British Journal of Ophthalmology, 1984, 68, 128-134 Ophthalmoplegia in carotid cavernous sinus fistula T. J. K. LEONARD, I. F. MOSELEY, AND M. D. SANDERS From the Departments ofneuro-ophthalmology and
British Journal of Ophthalmology, 1984, 68, 128-134 Ophthalmoplegia in carotid cavernous sinus fistula T. J. K. LEONARD, I. F. MOSELEY, AND M. D. SANDERS From the Departments ofneuro-ophthalmology and
Ruptured aberrant internal carotid artery pseudoaneurysm presenting with spontaneous massive ear bleeding following a single sneeze: a case report
 Case eport JNET 7:312-316, 2013 uptured aberrant internal carotid artery pseudoaneurysm presenting with spontaneous massive ear bleeding following a single sneeze: a case report Seiichiro HIONO 1) Eiichi
Case eport JNET 7:312-316, 2013 uptured aberrant internal carotid artery pseudoaneurysm presenting with spontaneous massive ear bleeding following a single sneeze: a case report Seiichiro HIONO 1) Eiichi
1 Description. 2 Indications. 3 Warnings ASPIRATION CATHETER
 Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine:
 Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
SDAVFs are rare acquired vascular lesions predominantly
 CLINICAL REPORT W.J. van Rooij R.J. Nijenhuis J.P. Peluso M. Sluzewski G.N. Beute B. van der Pol Spinal Dural Fistulas without Swelling and Edema of the Cord as Incidental Findings SUMMARY: SDAVFs cause
CLINICAL REPORT W.J. van Rooij R.J. Nijenhuis J.P. Peluso M. Sluzewski G.N. Beute B. van der Pol Spinal Dural Fistulas without Swelling and Edema of the Cord as Incidental Findings SUMMARY: SDAVFs cause
Introducing a New Treatment Method for Brain Aneurysms
 Pipeline Embolization Device Introducing a New Treatment Method for Brain Aneurysms UNDERSTANDING ANEURYSMS What is a brain aneurysm? An aneurysm is an outpouching in an artery caused by weakness in the
Pipeline Embolization Device Introducing a New Treatment Method for Brain Aneurysms UNDERSTANDING ANEURYSMS What is a brain aneurysm? An aneurysm is an outpouching in an artery caused by weakness in the
Vertebral Artery Pseudoaneurysm
 Vertebral Artery Pseudoaneurysm T. W. Khanzada,K. R. Makhdoomi ( Department of Vascular Surgery, Liaquat National Postgraduate Medical Centre, Karachi. ) Vertebral artery (VA) pseudoaneurysms are exceedingly
Vertebral Artery Pseudoaneurysm T. W. Khanzada,K. R. Makhdoomi ( Department of Vascular Surgery, Liaquat National Postgraduate Medical Centre, Karachi. ) Vertebral artery (VA) pseudoaneurysms are exceedingly
NANOS Patient Brochure
 NANOS Patient Brochure Pseudotumor Cerebri Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for
NANOS Patient Brochure Pseudotumor Cerebri Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for
Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal
 AJNR Am J Neuroradiol 20:2016 2020, November/December 1999 Case Report Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal Robert Ernst, Robert Bulas,
AJNR Am J Neuroradiol 20:2016 2020, November/December 1999 Case Report Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal Robert Ernst, Robert Bulas,
The Surgical Treatment of Migraine Headaches
 The Surgical Treatment of Migraine Headaches Being migraine-free for 11 years has been a dream come true. I live my life now with a freedom that I hadn t known for more than 23 years. Kathy Where is the
The Surgical Treatment of Migraine Headaches Being migraine-free for 11 years has been a dream come true. I live my life now with a freedom that I hadn t known for more than 23 years. Kathy Where is the
AFRRI CHRONIC CAROTID AND JUGULAR CATHETERIZATION IN RHESUS MONKEYS TECHNICAL NOTE AFRRI TN73-2 FEBRUARY J. M. Fein
 AFRRI TECHNICAL NOTE AFRRI TN73-2 FEBRUARY 1973 CHRONIC CAROTID AND JUGULAR CATHETERIZATION IN RHESUS MONKEYS J. M. Fein ARMED FORCES RADIOBIOLOGY RESEARCH INSTITUTE Defense Nuclear Agency Bethesda, Maryland
AFRRI TECHNICAL NOTE AFRRI TN73-2 FEBRUARY 1973 CHRONIC CAROTID AND JUGULAR CATHETERIZATION IN RHESUS MONKEYS J. M. Fein ARMED FORCES RADIOBIOLOGY RESEARCH INSTITUTE Defense Nuclear Agency Bethesda, Maryland
ANGIOPLASTY AND STENTING
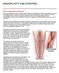 ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion
 Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Detection & Treatments
 Detection & Treatments Introduction 2 Other Procedures 12 Detection Methods 4 Familial Connection 15 Treatment Options for Brain Aneurysms 5 Clipping Treatment 7 Endovascular Therapy 9 Introduction Discovering
Detection & Treatments Introduction 2 Other Procedures 12 Detection Methods 4 Familial Connection 15 Treatment Options for Brain Aneurysms 5 Clipping Treatment 7 Endovascular Therapy 9 Introduction Discovering
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Intro: Slide 1. Slide 2. Slide 3. Basic understanding of interventional radiology. Gain knowledge of key terms and phrases
 Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
ER REBOA Catheter. Instructions for Use
 ER REBOA Catheter Instructions for Use Prytime Medical Devices, Inc. 229 N. Main Street Boerne, TX 78006, USA feedback@prytimemedical.com www.prytimemedical.com US 1 210 340 0116 U.S. and Foreign Patents
ER REBOA Catheter Instructions for Use Prytime Medical Devices, Inc. 229 N. Main Street Boerne, TX 78006, USA feedback@prytimemedical.com www.prytimemedical.com US 1 210 340 0116 U.S. and Foreign Patents
An endoleak is radiographic or ultrasonic evidence
 Complex Coil Embolization of Multiple Type II Endoleaks Liquid embolics, detachable coils, and plugs to repair an enlarging abdominal aortic aneurysm sac 5 years after EVAR. BY FRANK R. ARKO, MD; ABRAHAM
Complex Coil Embolization of Multiple Type II Endoleaks Liquid embolics, detachable coils, and plugs to repair an enlarging abdominal aortic aneurysm sac 5 years after EVAR. BY FRANK R. ARKO, MD; ABRAHAM
Introduction 3. What is Peripheral Vascular Disease? 5. What Are Some of the Symptoms of Peripheral Vascular Disease? 6
 Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
Patient guide: pfm Nit-Occlud PDA coil occlusion system. Catheter occlusion of. Patent Ductus Arteriosus. with the
 Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Carotid Cavernous Fistula
 Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Sample page. POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com.
 2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
Chapter IV: Percutaneous Puncture of Spinal Cord Cysts
 Acta Radiologica: Diagnosis ISSN: 0567-8056 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iard19 Chapter IV: Percutaneous Puncture of Spinal Cord Cysts To cite this article: (1966)
Acta Radiologica: Diagnosis ISSN: 0567-8056 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iard19 Chapter IV: Percutaneous Puncture of Spinal Cord Cysts To cite this article: (1966)
Periprosthetic leak and rupture after endovascular repair of abdominal aortic aneurysm: The significance of device design for long-term results
 CASE REPORTS Periprosthetic leak and rupture after endovascular repair of abdominal aortic aneurysm: The significance of device design for long-term results Kirsten Krohg-Sørensen, MD, PhD, Magne Brekke,
CASE REPORTS Periprosthetic leak and rupture after endovascular repair of abdominal aortic aneurysm: The significance of device design for long-term results Kirsten Krohg-Sørensen, MD, PhD, Magne Brekke,
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries. Goes to 6N
 Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Patient Information Booklet
 Patient Information Booklet Endovascular Stent Grafts: A Treatment for Thoracic Aortic Aneurysms Table of Contents Table of Contents Introduction 1 Anatomy of the Thoracic Aorta 2 What Is an Aneurysm?
Patient Information Booklet Endovascular Stent Grafts: A Treatment for Thoracic Aortic Aneurysms Table of Contents Table of Contents Introduction 1 Anatomy of the Thoracic Aorta 2 What Is an Aneurysm?
RECOMMENDED INSTRUCTIONS FOR USE
 Rapid Exchange PTCA Dilatation Catheter RECOMMENDED INSTRUCTIONS FOR USE Available in diameters 1.25mm to 4.5mm and in lengths 09mm to 40mm Caution: This device should be used only by physicians trained
Rapid Exchange PTCA Dilatation Catheter RECOMMENDED INSTRUCTIONS FOR USE Available in diameters 1.25mm to 4.5mm and in lengths 09mm to 40mm Caution: This device should be used only by physicians trained
CEREBRAL ANEURYSMS PRESENTING WITH VISUAL FIELD DEFECTS*
 Brit. J. Ophthal. (1966) 50, 251 CEREBRAL ANEURYSMS PRESENTING WITH VISUAL FIELD DEFECTS* BY University Department of Ophthalmology and Royal Infirmary, Edinburgh ANEURYSMS occur more frequently within
Brit. J. Ophthal. (1966) 50, 251 CEREBRAL ANEURYSMS PRESENTING WITH VISUAL FIELD DEFECTS* BY University Department of Ophthalmology and Royal Infirmary, Edinburgh ANEURYSMS occur more frequently within
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship
 Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Learning Objectives for Rotations in Vascular Surgery Year 3 Basic Clerkship CLINICAL PROBLEMS IN VASCULAR SURGERY 1. ABDOMINAL AORTIC ANEURYSM A 70 year old man presents in the emergency department with
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report
 Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports-
 Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al.
 ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
Occlusion of Arteriovenous Malformations of the Cavernous Sinus via the Superior Ophthalmic Vein
 539 Occlusion of Arteriovenous Malformations of the Cavernous Sinus via the Superior Ophthalmic Vein Michael Mu Huo Teng' 2 Wan-Yuo Guo' Chun-I Huang 3 Chih-Chiau Wu 4 Tsuen Chang' The treatment of five
539 Occlusion of Arteriovenous Malformations of the Cavernous Sinus via the Superior Ophthalmic Vein Michael Mu Huo Teng' 2 Wan-Yuo Guo' Chun-I Huang 3 Chih-Chiau Wu 4 Tsuen Chang' The treatment of five
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
Carotid Stenosis (carotid artery disease)
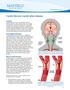 1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE
 MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE AAA FACTS 200,000 New Cases Each Year Ruptured AAA = 15,000 Deaths per Year in U.S. 13th Leading Cause of Death 80% Chance of
MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE AAA FACTS 200,000 New Cases Each Year Ruptured AAA = 15,000 Deaths per Year in U.S. 13th Leading Cause of Death 80% Chance of
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
A telescopic ventriculoatrial shunt that elongates with growth
 A telescopic ventriculoatrial shunt that elongates with growth Technical note BURTON L. WISE, M.D. Department of Surgery (Neurosurgery) and Neurological Institute, Mount Zion Hospital and Medical Center,
A telescopic ventriculoatrial shunt that elongates with growth Technical note BURTON L. WISE, M.D. Department of Surgery (Neurosurgery) and Neurological Institute, Mount Zion Hospital and Medical Center,
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Transvenous Embolization of Dural Fistulas Involving the Transverse and Sigmoid Sinuses
 385 Transvenous Embolization of Dural Fistulas Involving the Transverse and Sigmoid Sinuses Van V. Halbach 1 Randall T. Higashida 1 Grant B. Hieshima 1 C. Mark Mehringer 2 Carl W. Hardin 1 Received February
385 Transvenous Embolization of Dural Fistulas Involving the Transverse and Sigmoid Sinuses Van V. Halbach 1 Randall T. Higashida 1 Grant B. Hieshima 1 C. Mark Mehringer 2 Carl W. Hardin 1 Received February
Surgical Privileges Form: "Neurosurgery" Clinical Privileges Request. Requested (To be completed by the applicant) Not Recommended (For committee use)
 Surgical Form: Clinical Request "Neurosurgery" Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. the applicant) CATEGORY I: Core : 1. Interpretation of
Surgical Form: Clinical Request "Neurosurgery" Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. the applicant) CATEGORY I: Core : 1. Interpretation of
Dural Arteriovenous Malformations and Fistulae (DAVM S DAVF S)
 Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Complex dural arteriovenous fistulas. Results of combined endovascular and neurosurgical treatment in 16 patients
 J Neurosurg 71:352-358,1989 Complex dural arteriovenous fistulas Results of combined endovascular and neurosurgical treatment in 16 patients STANLEY L. BARNWELL, M.D., PH.D., VAN V. HALBACH, M.D., RANDALL
J Neurosurg 71:352-358,1989 Complex dural arteriovenous fistulas Results of combined endovascular and neurosurgical treatment in 16 patients STANLEY L. BARNWELL, M.D., PH.D., VAN V. HALBACH, M.D., RANDALL
Carotid Artery Dissection Causing an Isolated Hypoglossal. Nerve Palsy
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550035 Volume 2, Issue 5 Case Report Carotid Artery Dissection Causing an Isolated Hypoglossal Muzzammil Ali*, Yatin Sardana Nerve Palsy
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550035 Volume 2, Issue 5 Case Report Carotid Artery Dissection Causing an Isolated Hypoglossal Muzzammil Ali*, Yatin Sardana Nerve Palsy
Case #1. Case #1- Possible codes. Unraveling the -59 modifier. Principles of Interventional. CASE 1: Simple angioplasty
 Unraveling the -59 modifier Principles of Interventional Coding Donald Schon, MD, FACP Debra Lawson, CPC, PCS Distinct or independent from other services performed on the same day Normally not reported
Unraveling the -59 modifier Principles of Interventional Coding Donald Schon, MD, FACP Debra Lawson, CPC, PCS Distinct or independent from other services performed on the same day Normally not reported
The superior ophthalmic vein approach for the treatment of carotid-cavernous fistulas: our first experience
 230 Chiriac et al - Superior ophthalmic vein approach The superior ophthalmic vein approach for the treatment of carotid-cavernous fistulas: our first experience A. Chiriac, N. Dobrin 1, Georgiana Ion
230 Chiriac et al - Superior ophthalmic vein approach The superior ophthalmic vein approach for the treatment of carotid-cavernous fistulas: our first experience A. Chiriac, N. Dobrin 1, Georgiana Ion
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
CardioVascular Radiology
 Cardiovasc. Radiol. 2: 3-7, 1979 CardioVascular Radiology Percutaneous Transluminal Angioplasty (PTA) with the Griintzig Balloon Catheter: Technical Problems Encountered in the First Forty Patients B.T.
Cardiovasc. Radiol. 2: 3-7, 1979 CardioVascular Radiology Percutaneous Transluminal Angioplasty (PTA) with the Griintzig Balloon Catheter: Technical Problems Encountered in the First Forty Patients B.T.
Venous sampling. What is venous sampling? What are some common uses of the procedure?
 Scan for mobile link. Venous sampling Venous sampling is a diagnostic procedure that uses imaging guidance to insert a catheter into a specific vein and remove blood samples for laboratory analysis. Abnormal
Scan for mobile link. Venous sampling Venous sampling is a diagnostic procedure that uses imaging guidance to insert a catheter into a specific vein and remove blood samples for laboratory analysis. Abnormal
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Cerebrovascular. Disease
 Cerebrovascular Disease People take better care of their health when they know what s going on in their bodies. For those with cerebrovascular disease, this means understanding how the arteries work and
Cerebrovascular Disease People take better care of their health when they know what s going on in their bodies. For those with cerebrovascular disease, this means understanding how the arteries work and
Pericardiocentesis and Drainage by a Silicon Rubber Line. without Echocardiographic Guidance. Experience in 55 Consecutive Patients
 Pericardiocentesis and Drainage by a Silicon Rubber Line without Echocardiographic Guidance Experience in 55 Consecutive Patients Kunshen LIU, M.D., Wenling LIU, M.D., Xiaotao LI, M.D., Yue XIA, M.D.,
Pericardiocentesis and Drainage by a Silicon Rubber Line without Echocardiographic Guidance Experience in 55 Consecutive Patients Kunshen LIU, M.D., Wenling LIU, M.D., Xiaotao LI, M.D., Yue XIA, M.D.,
Artificial embolization of carotid-cavernous fistula with post-operative patency of internal carotid
 J. Neurol. Neurosurg. Psychiat., 1970, 33, 674-678 Artificial embolization of carotid-cavernous fistula with post-operative patency of internal carotid artery FABIAN ISAMAT, V. SALLERAS, AND A. M. MIRANDA
J. Neurol. Neurosurg. Psychiat., 1970, 33, 674-678 Artificial embolization of carotid-cavernous fistula with post-operative patency of internal carotid artery FABIAN ISAMAT, V. SALLERAS, AND A. M. MIRANDA
Transcatheter closure of patent foramen ovale using the internal jugular venous approach
 New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
Effectiveness of IVUS in Complex Cases
 Effectiveness of IVUS in Complex Cases Satoru Sumituji,M.D. Rinku General Medical Center IVUS is can provide images of the vessel wall and the tissue around the vessel which cannot be viewed by angiography.
Effectiveness of IVUS in Complex Cases Satoru Sumituji,M.D. Rinku General Medical Center IVUS is can provide images of the vessel wall and the tissue around the vessel which cannot be viewed by angiography.
Cordis EXOSEAL Vascular Closure Device
 to receive our latest news and key activities. Cordis EXOSEAL Vascular Closure Device A Guide to Good Access and Closure Transfemoral Access Closure Pocket Guide LinkedIn page Follow us on CORDIS EMEA
to receive our latest news and key activities. Cordis EXOSEAL Vascular Closure Device A Guide to Good Access and Closure Transfemoral Access Closure Pocket Guide LinkedIn page Follow us on CORDIS EMEA
2017 Cardiology Survival Guide
 2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
Talent Abdominal Stent Graft
 Talent Abdominal with THE Xcelerant Hydro Delivery System Expanding the Indications for EVAR Treat More Patients Short Necks The Talent Abdominal is the only FDA-approved device for proximal aortic neck
Talent Abdominal with THE Xcelerant Hydro Delivery System Expanding the Indications for EVAR Treat More Patients Short Necks The Talent Abdominal is the only FDA-approved device for proximal aortic neck
PRIVILEGE APPLICATION FORM - [Mercy Medical Center]
![PRIVILEGE APPLICATION FORM - [Mercy Medical Center] PRIVILEGE APPLICATION FORM - [Mercy Medical Center]](/thumbs/89/98821167.jpg) Current Privilege Status Key Practitioner's Current Privilege status is signified in ( ) preceding each privilege. G = W = Withdrawn T = Temporary P = With Proctor A = Assist with C = With Consult E =
Current Privilege Status Key Practitioner's Current Privilege status is signified in ( ) preceding each privilege. G = W = Withdrawn T = Temporary P = With Proctor A = Assist with C = With Consult E =
Peel-Apart Percutaneous Introducer Kits for
 Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Abdominal and thoracic aneurysm repair
 Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
