Ophthalmoplegia in carotid cavernous sinus fistula
|
|
|
- Hector Horton
- 5 years ago
- Views:
Transcription
1 British Journal of Ophthalmology, 1984, 68, Ophthalmoplegia in carotid cavernous sinus fistula T. J. K. LEONARD, I. F. MOSELEY, AND M. D. SANDERS From the Departments ofneuro-ophthalmology and Neuro-Radiology, National Hospitalfor Nervous Diseases, Queen Square, London WC] SUMMARY The aetiology of ophthalmoplegia in 15 patients with carotid-cavernous sinus fistula is discussed, and the clinical findings are correlated with angiographic and orbital CT appearances. After closure of the fistula the majority of patients with generalised ophthalmoplegia recovered full ocular movements rapidly, while patients with an isolated abduction weakness required much longer to return to normal. Orbital CT studies showed enlarged extraocular muscles in the patients with generalised ophthalmoplegia but muscles of normal size in those with abduction failure alone. After closure of the fistula repeat CT studies of patients with enlarged extraocular muscles showed a diminution in muscle size. We suggest that generalised ophthalmoplegia in carotid cavernous sinus fistula is due to hypoxic, congested extraocular muscles. Isolated abduction weakness is due to a sixth nerve palsy, which probably occurs either in the cavernous sinus or more posteriorly near the inferior petrosal sinus. A combination of these 2 mechanisms may be found in some patients. A caroticocavernous fistula (CCF) results from abnormal communications between the carotid arterial system and the cavernous sinus. The combination of reduced arterial perfusion and raised venous pressure creates a unique example of orbital and ocular hypoxia, with accompanying venous congestion. ' CCF are of 2 types, direct and dural. Direct fistulae are caused by tears in the intracavernous portion of the internal carotid artery arising either from trauma (often severe) or possibly from rupture of a preexisting aneurysm; they usually lie anteriorly in the cavernous sinus2 and drain forwards into the orbit. They are high-flow fistulae; the onset of symptoms may be dramatic with severe pulsatile proptosis, bruit, and poor vision due to ocular hypoxia. Dural fistulae occur when meningeal branches of the internal or external carotid arteries rupture within the cavernous sinus. These vessels are thin walled2 and may rupture spontaneously-especially in the hypertensive patient-after minor trauma or on straining. Dural fistulae often lie in the posterior cavernous sinus3 and drain backwards into the inferior petrosal sinus. Since they are low-flow fistulae4 the clinical presentation may be subtle, with mild proptosis, redness, and ocular hypertension. Horizontal diplopia due to an ipsilateral weakness of Correspondence to Mr M. D. Sanders, Department of Neuro- Ophthalmology, National Hospital for Nervous Diseases, Queen Square, London WC1N 3BG. abduction is common and may herald the other symptoms and signs.3 Diplopia is a common symptom in patients with CCF. Approximately one-half of patients with CCF have VI nerve palsies, but the incidence of III and IV nerve palsies varies considerably. Moseley and Sanders5 illustrated a case of ophthalmoplegia due to a CCF and emphasised the associated swelling of extraocular muscles, shown by CT. After spontaneous closure of the fistula the ophthalmoplegia improved rapidly, accompanied by diminution of the extraocular muscle swelling. It was therefore suggested that the swollen muscles contributed to the ophthalmoplegia. The aim of this paper is to evaluate the aetiology of the ophthalmoplegia in CCF. The clinical findings have been correlated with the angiographic and orbital CT appearances. Patients Fifteen patients with CCF were studied. Seven patients (ofwhom 3 had suffered a severe head injury) had direct CCF, and 8 had dural fistulae of spontaneous onset. Results Incidence ofimportant clinicalfindings atpresentation. (1) Chemosis and redness 100%, (2) Proptosis 100%, 128
2 Ophthalmoplegia in carotid cavernous sinusfistula (3) Ophthalmoplegia 95%, (4) Subjective bruit 70%, (5) Reduced visual acuity 50%, (6) Posterior segment changes 50%, (7) Raised intraocular pressure 21%, (8) Anterior segment ischaemia 20%. Ophthalmoplegia and CT scan appearances. Fourteen patients had ophthalmoplegia. In 10 of them ocular movements improved after closure of the fistula. The clinical findings when correlated with the orbital CT appearances and pattern of recovery allowed a division of these 10 patients into 3 groups. The 4 patients who did not recover normal eye movements were placed in a separate category. Group L. Four patients showed an isolated abduction weakness with muscles of normal size on CT and a delayed recovery of the ophthalmoplegia following closure of the fistula (Table 1). Group I. In contrast, these 4 patients had a generalised ophthalmoplegia with enlarged extraocular muscles on CT and a rapid recovery of ocular movements after closure of the fistula (Table 2). Group III. Two patients had a generalised ophthalmoplegia with enlarged muscles on CT but differed from those in group II by showing a biphasic recovery of ocular movements after closure of the fistula. Vertical movements and adduction recovered quickly accompanied by a diminution in extraocular muscle size on CT scan. However, the abduction weakness persisted for 3 months (Table 3). Table 1 Isolated abduction failure Group IV. Four patients showed no improvement in the ophthalmoplegia after closure of the fistula, although several of the other symptoms and signs regressed (Table 4). One patient had no evidence of ophthalmoplegia associated with her direct fistula. Her symptoms of a bruit and a dull ache in the eye accompanied by signs of chemosis, redness, and proptosis all resolved rapidly following embolisation of the fistula. The presentation and natural history of groups I, II, and III is illustrated by a typical patient from each group. Each patient in group IV is briefly described, since there were different factors leading to their failure of treatment. GROUP I (4 PATIENTS) Isolated abduction failure. Normal size extraocular muscles on CT. Delayed recovery ofabduction following closure of the fistula (Table 1) Case 1. A 67-year-old woman presented with horizontal diplopia, redness of the right eye, and blurring of the right eye vision. There was no bruit; visual acuity was 6/9 N5 right and 6/6 N5 left. The right eye showed 3 mm of proptosis with chemosis and redness but was otherwise normal; ocular movements were full except for complete failure of abduction on the right. Orbital CT showed extra- Patient Angiography- Ophthalmoplegia Orbital CT Ophthalmoplegia Follow-up Type and site post closure offistula Dural 100 SOV* 100 All symptoms and signs female Both EC to EOM normal save right abduction right posterior 0-o-100 Full 0-O-100 Full failure improved by 1/52. CS Abduction recovered by / Dural 100 SOV* 100 All symptoms and signs female EC to EOM normal save right abduction posterior CS 0o-100 Full 0-o-100 Full failure improved by 1/52. Abduction recovered by / Dural 100 SOV* 100 All symptoms and signs female IC to left SOV* save left abduction failure posterior CS Full 100o-{- EOM normal Full 100o{-0 improved by 1/52. abduction full at 3/ Dural 100 SOV* 100 Complete resolution of all male EC to EOM normal signs by 1/12 anterior 50-u-100 Full 50-( -100 Cs IC=Internal carotid. EC=External carotid. EOM=Extraocular muscles. SOV=Superior ophthalmic vein. CS=Cavernous sinus. **Very swollen. *Swollen. 129
3 130 Table 2 T. J. K. Leonard, I. F. Moseley, and M. D. Sanders Ophthalmoplegia with swollen extraocular muscles. Complete and rapid recovery following closure ofthefistula Patient Angiography Ophthalmoplegia Orbital CT Follow-up Post closure CT Direct fistula EOM** Balloon embolisation. Normal at 1/52 male IC to right Nil Full SOV** All signs resolved by 1/52 anterior CS Dural 10 EOM** Spontaneous resolution. Normal at 1/52 male IC to right SOV** All signs regressed by 1/52 anterior CS 20-O-20 Full Dural 5 SOV** Spontaneous resolution Not done female IC to right EOM** after angiography. anterior CS 5-o-5 Full All signs regressed 1/52 after angiogram Direct 5 SOV* Failcd cmbolisation. Not done male IC to right EOM* Spontaneous resolution CS 90o--20 Full 2/12 later. All signs including ophthalmoplegia 60 resolved by 1/52 Abbreviations and symbols as in Table 1. ocular muscles of normal size and enlargement of the right superior ophthalmic vein. Carotid angiography demonstrated a right dural fistula supplied by both external carotid arteries via the middle meningeal and ascending pharyngeal branches. Drainage was from the posterior aspect of the right cavernous sinus. Embolisation by balloon was effective in causing regression of all ocular signs except the right abduction weakness, which required 3 months to recover. GROUP 11 (4 PATIENTS) Generalised ophthalmoplegia. Enlarged extraocular muscles on CT. Rapid, complete recovery ofeye movements following closure of thefistula. (Table 2) Case 5. A 73-year-old man developed right-sided bruit and poor visual acuity, three days after severe head trauma. The left eye was normal on examination, but the right eye was red with chemosis and 3 mm of proptosis. He had a complete right ophthalmoplegia without ptosis. Intraocular pressure in the right eye was normal in the primary position but rose by 8 mm on attempted upgraze, indicating tethering. Carotid angiography demonstrated a direct CCF from the right internal carotid artery to the anterior cavemous sinus, while orbital CT showed gross swelling of the extraocular muscles with an enlarged superior ophthalmic vein. Balloon embolisation effected complete cure within one week, including a Table 3 Ophthalmoplegia with swollen muscles and biphasic recovery. (1) Rapid recovery ofall movements save abduction. (2) Delayed recovery of abduction Patient Angiography Ophthalmoplegia Orbital CT Follow-up Direct 5 EOM** Balloon embolisation via left IC. All female IC to left anterior Ptosis SOVW * signs including ptosis and EOM CS and right CS 5-0--A Nil EOM** recovered in 1/52 except bilateral SOV** abduction failure left>right. 5 recovered 1/12, left recovered 3/ No angiogram 70 SOV* Spontaneous closure after 3/52. All female EOM** symptoms and signs regressed save 70-o--80 Full diplopia and recovery of right abduction. Post closure scan showed 80 muscle shrinkage Abbreviations and symbols as in Table 1.
4 Ophthalmoplegia in carotid cavernous sinusfistula return of vision to 6/9 and recovery of full ocular movements. The right intraocular pressure no longer showed a rise on elevation of the eye. GROUP III (2 PATIENTS) Mixed. Generalised ophthalmoplegia. Enlarged extraocular muscles on CT. Rapid recovery of all eye movements except abduction following closure of the fistula. (Table 3) Case 9. A 56-year-old female with no history of trauma presented with a short history of diplopia, bruit, and redness of both eyes; there was bilateral symmetrical proptosis. Vision on admission was 6/5 N5 in each eye. Ocular movements were grossly restricted bilaterally and she had a left ptosis (Figs. 1A, 1C); the pupillary reactions were entirely normal. CT showed swelling of extraocular muscles in both orbits and enlargement of both superior ophthalmic veins. Carotid angiography demonstrated a direct fistula feeding from the left internal Figs. IA, B, C, D Case 9. Bilateral signsfrom left unilateral CCF. To show rapid regression ofsigns save left abduction failure after embolisation offistula by balloon. Fig. la: Pre-embolisation. Note left ptosis. One week post embolisation left ptosis resolved. Fig. 1C Pre-embolisation. Attempted left gaze. Note incomplete right adduction and absent left abduction. Bilateral conjunctival injection is also shown. Fig. ID: Oneweekpostembolisation.Attemptedleftgaze. Note full right adduction but absent left abduction persists. The bilateral conjunctival injection has improved. 131 carotid artery to the left cavernous sinus and, via the intercavernous plexus, to the right anterior cavernous sinus. Embolisation was carried out by detachable balloon catheter via the left internal carotid artery. Within 5 days the bruit, chemosis, and proptosis had disappeared, and considerable recovery of ocular movement was evident with regression of the ptosis (Figs. 1B, 1D). Although vertical eye movements and adduction were generally much improved after 3 days, and had returned to normal in 2 weeks, the failure of left abduction persisted and did not recover for 3 months. GROUP IV (4 PATIENTS) No recovery ofophthalmoplegia Table 4 illustrates the patients whose eye movements failed to recover. Patient II had an aberrant trigeminal artery which continued to supply the fistula despite embolisation of the internal carotid. The bruit disappeared, but the other signs remained. Patient 12 could not be embolised owing to her haemophilia. Her bruit eventually ceased, but the proptosis and ophthalmoplegia remained. The fistula in case 13 was unusually anterior, draining almost directly via small vessels into the superior ophthalmic vein, and was considered inaccessible to embolisation. CT showed marked proptosis, enlarged superior ophthalmic vein, and enormous extraocular muscles. This unfortunate patient rapidly developed ocular ischaemia with poor vision. Case 14 was unusual in that a direct fistula resulted from the rupture of an intracavernous aneurysm. Gradual compression of the cranial nerves in the cavernous sinus had resulted in a complete ophthalmoplegia with a diminished corneal reflex. Embolisation eliminated the bruit but the ophthalmoplegia did not improve. Discussion Previous reviews of CCF' have drawn attention to the incidence of ocular motor nerve palsies with VI nerve involvement occurring in approximately onehalf of all patients. There is less agreement on the frequency with which III and IV nerve palsies are found. The diagnosis of III and IV nerve palsies in congested orbits may be very difficult. Although III nerve involvement may be associated with ptosis or an afferent pupillary defect, a mechanical ptosis is often found in inflamed eyes, and in many cases of CCF the iris becomes ischaemic, making interpretation of the pupillary signs unreliable. Our findings suggest that many patients do have VI nerve palsies, but that the other ocular motor problems are due to swollen extraocular muscles. The
5 132 Table 4 No recovery ofophthalmoplegia T. J. K. Leonard, L. F. Moseley, and M. D. Sanders Patient Angiogram Ophthalmoplegia CT Follow-up Direct Full Nil SOV** Embolisation removed bruit but all male IC to left CS. Also EOM* * other signs remained. CCF continued to supplied from aberrent be fed from trigeminal artery trigeminal artery Direct Nil Full SOV** Patient had haemophilia. Bruit female IC to right anterior EOM** gradually regressed. Other signs CS and left CS SOV* unchanged at 1 year Dural from left IC to Full Nil EOM** Dural vessels not possible to embolise. female left anterior CS and SOV** All signs unchanged at 6/12 left SOV Direct Nil Full EOM** Symptoms signs for 1 year. Embolised. female? rupture of right SOV** Bruit eliminated. All other signs intracavernous IC unchanged at 6/12 aneurysm into right CS Abbreviations and symbols as in Table 1. different mechanisms can be determined by correlation of the physical signs, angiography, and orbital CT İsolated abduction weakness was the only ocular motor problem in cases 1-4, in whom CT demonstrated extraocular muscles of normal size. There was no evidence of orbital or ocular ischaemia, and the III, IV, and V nerves were uninvolved. Carotid angiography demonstrated the site of the fistula to be posterior in cases 1, 2, and 3 but anterior in case 4. Abduction completely recovered in each patient but required from one month (case 4) to 3 months (cases 1-3). This slow recovery, in the absence of swollen muscles, involvement of other cranial nerves, or orbital ischaemia, suggests that these patients had suffered a VI nerve palsy posterior to the superior orbital fissure. The probable site of damage was either posteriorly where the VI nerve passes beneath the petroclinoid ligament near the inferior petrosal sinus or in the cavernous sinus. Newton and Hoyt3 commented on the frequent posterior location of the dural fistulae within the cavernous sinus. Posterior fistulae may drain into the inferior petrosal sinus, causing distension of the sinus and intermittent compression of the VI nerve.3 This would explain the characteristic transient horizontal diplopia which may herald the other symptoms and signs in dural fistulae. Compression of the nerve against the petroclinoid ligament or interruption of the fragile arterial blood supply would cause a VI nerve palsy. The IV nerve enters the cavernous sinus posteriorly either in or contiguous to the inferior petrosal sinus.23 Usually it lies immediately lateral to the internal carotid artery, surrounded by a separate sheath, but it may be adherent to the lateral wall of the artery. In the posterior part of the cavernous sinus the blood supply to the VI nerve is from the dorsomeningeal branch of the internal carotid artery. There are therefore 2 potential sites for damage to the VI nerve within the cavernous sinus. A direct fistula could involve the closely related internal carotid artery or a dural fistula feeding from the dorsomeningeal branch might jeopardise the blood supply of the nerve. In this series the 4 patients thought to have VI nerve palsies had dural fistulae confirmed by carotid angiography. Three months was required in each patient for recovery of abduction. In contrast, case 4 had an anteriorly placed fistula, and abduction improved within a month of closure. The 4 patients with a generalised ophthalmoplegia and swollen extraocular muscles on orbital CT had a different mechanism for their reduced eye movements from the cases in group I. Each patient showed a rapid recovery of normal eye movements after closure of the fistula accompanied by a diminution of extraocular muscle swelling on the orbital CT Ėach patient in group II had a bruit. The sudden elimination of the bruit, either following embolisation or spontaneous cure, was used as a guide to determine the time of closure of the fistula. On closure of the fistula the bruit in case 5 ceased immediately and the ophthalmoplegia resolved within one week. In case 6 the fistula appeared to close spontaneously, as shown by cessation of the bruit and
6 Ophthalmoplegia in carotid cavernous sinusfistula loss of the persistent ache within the eye. The eye movements improved within a week, and the improvement was accompanied by a diminution in ocular muscle swelling on orbital CT scan. In cases 7 and 8 the fistula closed after invasive procedures, angiography in case 7 and attempted embolisation in case 8. Again the ophthalmoplegia improved rapidly in each patient after a sudden cessation of the bruit. Anteriorly placed fistulae tend to drain into the orbit.2 This applies to both direct fistulae (case 5) and dural fistulae (cases 6 and 7). A narrowing of arteriovenous pressure gradient occurs within the orbit' leading to orbital hypoxia and venous congestion. The extraocular muscles may become extremely swollen, often trebling their usual size, with consequent mechanical interference with normal function like that seen in dysthyroid eye disease. Tamponade of the globe may raise the intraocular pressure, especially on attempted upgaze, emphasising the restrictive component of the ophthalmoplegia as shown in case 5. The rapid recovery of extraocular muscle function following closure of the fistula was associated with a diminution in extraocular muscle size. This recovery occurred despite the ophthalmoplegia having been present for several months in some cases. If the mechanism of the ophthalmoplegia were purely ischaemic, then such a rapid and complete recovery would be unlikely. There was little evidence of III and IV nerve dysfunction, though ischaemia to the ocular motor nerves within the orbit might be implicated as a possible cause of the ophthalmoplegia. However, the corneal reflex, usually a sensitive indicator of compression or ischaemic insult at the orbital apex, remained intact in all the patients shown in Table 2. None had evidence of anterior segment ischaemia, and pupil reactions were normal in each case. The 2 patients in group III showed a combination of the mechanisms so far identified as causing ophthalmoplegia in CCF. Case 9 as detailed above illustrated a severe bilateral ophthalmoplegia due to a unilateral direct fistula. Grossly swollen extraocular muscles could be demonstrated on CT scan, and angiography confirmed the site of the fistula in the left anterior cavernous sinus. Balloon embolisation effected complete cure of the symptoms and signs of the fistula, except the ophthalmoplegia, within one week. Although the ptosis, vertical eye movement, and adduction recovered quickly, a return of full abduction was delayed. The patient reported as case 10 similarly showed resolution of the generalised ophthalmoplegia except for abduction following spontaneous closure of the Fig. LA Case l. Preclosure orbital scan to show swollen extraocular muscles in right orbit. 133 fistula. The orbital scans (Figs. 2A, 2B) illustrate the diminution in extraocular muscle swelling and also the failure of abduction (Fig. 2B). In conclusion, we suggest different aetiologies for the ophthalmoplegia in a series of patients with CCF. Analysis of the clinical signs, the results of investigations, and recovery after cure indicate that isolated abduction failure without CT evidence of ocular muscle swelling is due to a VI nerve palsy, while a generalised ophthalmoplegia is caused by mechanical restriction from swollen ocular muscles. Fig. 2 OJne week post closure orbital scan taken with eyes in attempted dextroversion (see position ofthe lens in each eye). While the left eye performs normal adduction, the right eye cannot abduct despite reduction in extraocular muscle size.
7 134 References 1 Sanders MD, Hoyt WF. Hypoxic sequelae of carotid cavernous fistulae. Br J Ophthalmol 1969; 53: Parkinson D. A surgical approach to the cavernous portion of the carotid artery. Can J Surg 1964; 7: Newton T, Hoyt W. Dural arteriovenous shunts in the region of the cavernous sinus. Neuroradiology 1970; 1: Hayes GJ. External carotid-cavernous fistulae. J Neurosurg 1963; 20: T. J. K. Leonard, l. F. Moseley, and M. D. Sanders 5 Moseley IF, Sanders MD. Computerised tomography in neuroophthalmology. London: Chapman and Hall, 1982: Henderson JW, Schreider RC. Ocular findings in carotid cavernous fistula. Am J Ophthalmol 1959; 48: Madsen PH. Carotid cavernous fistula. Acta Ophthalmol (Kbh) 1970; 48: Odom GL. Ophthalmic involvement in neurological vascular lesions. In: Smith JL, ed. Neuro-ophthalmology. Springfield: Thomas, 1964:1: Palestine AG, Younge B, Diepgmas D. Visual prognosis in carotid cavernous fistula. Arch Ophthalmol 1981; 99: Br J Ophthalmol: first published as /bjo on 1 February Downloaded from on 28 January 2019 by guest. Protected by copyright.
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Carotid Cavernous Fistula
 Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
Mechanisms of presentation of caroticocavernous
 Brit.. Ophthal. (1970) 54, I86 Mechanisms of presentation of caroticocavernous fistulae EDWIN R. BICKERSTAFF The Midland CentreJor Neurosurgery and Neurology, Smethwick The clinical features of carotico-cavernous
Brit.. Ophthal. (1970) 54, I86 Mechanisms of presentation of caroticocavernous fistulae EDWIN R. BICKERSTAFF The Midland CentreJor Neurosurgery and Neurology, Smethwick The clinical features of carotico-cavernous
Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case
 Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case Soo-Bin Yim, M.D., Jong-Sung Kim, M.D., Yang Kwon,M.D.*, Choong-Gon
Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case Soo-Bin Yim, M.D., Jong-Sung Kim, M.D., Yang Kwon,M.D.*, Choong-Gon
Transient third nerve palsy after electrometallicthrombosis of carotid cavernous fistulae
 Journal of Neurology, Neurosurgery, and Psychiatry, 1976, 39, 854-860 Transient third nerve palsy after electrometallicthrombosis of carotid cavernous fistulae W. BRUCE WILSON,1 P. R. BRINGEWALD, Y. HOSOBUCHI,
Journal of Neurology, Neurosurgery, and Psychiatry, 1976, 39, 854-860 Transient third nerve palsy after electrometallicthrombosis of carotid cavernous fistulae W. BRUCE WILSON,1 P. R. BRINGEWALD, Y. HOSOBUCHI,
Vertical Muscles Transposition with Medical Rectus Botulinum Toxin Injection for Abducens Nerve Palsy
 JKAU: Med. Sci., Vol. 16 No. 2, pp: 43-49 (2009 A.D. / 1430 A.H.) DOI: 10.4197/Med. 16-2.4 Vertical Muscles Transposition with Medical Rectus Botulinum Toxin Injection for Abducens Nerve Palsy Nizar M.
JKAU: Med. Sci., Vol. 16 No. 2, pp: 43-49 (2009 A.D. / 1430 A.H.) DOI: 10.4197/Med. 16-2.4 Vertical Muscles Transposition with Medical Rectus Botulinum Toxin Injection for Abducens Nerve Palsy Nizar M.
Dural arteriovenous fistulas of the cavernous sinus - clinical case and treatment
 166 Chiriac et al Dural arteriovenous fistulas of the cavernous sinus Dural arteriovenous fistulas of the cavernous sinus - clinical case and treatment A. Chiriac, N. Dobrin*, St.M. Iencean, I. Poeata
166 Chiriac et al Dural arteriovenous fistulas of the cavernous sinus Dural arteriovenous fistulas of the cavernous sinus - clinical case and treatment A. Chiriac, N. Dobrin*, St.M. Iencean, I. Poeata
Investigations. The blood count was normal with an erythrocyte. sedimentation rate of 5 mm. ist hr, and negative Waaler-
 Brit. J. Ophthal. (I975) 59, 149 Tolosa-Hunt syndrome The dangers of an eponym T. J. FOWLER, C. J. EARL, V. L. McALLISTER, AND W. I. McDONALD From the Institute of Neurology, National Hospitalfor Nervous
Brit. J. Ophthal. (I975) 59, 149 Tolosa-Hunt syndrome The dangers of an eponym T. J. FOWLER, C. J. EARL, V. L. McALLISTER, AND W. I. McDONALD From the Institute of Neurology, National Hospitalfor Nervous
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Direct carotid-cavernous fistula and glaucoma: case reports
 D. Petraru et al Direct carotid-cavernous fistula and glaucoma Direct carotid-cavernous fistula and glaucoma: case reports D. Petraru 1, D. Costin 2, G. Mihalache 3 1 2 nd Ophthalmological Clinic, Clinical
D. Petraru et al Direct carotid-cavernous fistula and glaucoma Direct carotid-cavernous fistula and glaucoma: case reports D. Petraru 1, D. Costin 2, G. Mihalache 3 1 2 nd Ophthalmological Clinic, Clinical
The superior ophthalmic vein approach for the treatment of carotid-cavernous fistulas: our first experience
 230 Chiriac et al - Superior ophthalmic vein approach The superior ophthalmic vein approach for the treatment of carotid-cavernous fistulas: our first experience A. Chiriac, N. Dobrin 1, Georgiana Ion
230 Chiriac et al - Superior ophthalmic vein approach The superior ophthalmic vein approach for the treatment of carotid-cavernous fistulas: our first experience A. Chiriac, N. Dobrin 1, Georgiana Ion
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
GNK485 The eye and related structures. Prof MC Bosman 2012
 GNK485 The eye and related structures Prof MC Bosman 2012 Surface anatomy Bony orbit Eyeball and Lacrimal apparatus Extra-ocular muscles Movements of the eye Innervation Arterial supply and venous drainage
GNK485 The eye and related structures Prof MC Bosman 2012 Surface anatomy Bony orbit Eyeball and Lacrimal apparatus Extra-ocular muscles Movements of the eye Innervation Arterial supply and venous drainage
A Patient Presenting with Ptosis, Ophthalmoplegia, and Decreased Periorbital Sensations and Facial Droop in Tolosa-Hunt Syndrome
 A Patient Presenting with Ptosis, Ophthalmoplegia, and Decreased Periorbital Sensations and Facial Droop in Tolosa-Hunt Syndrome medicine2.missouri.edu/jahm/patient-presenting-ptosis-ophthalmoplegia-decreased-periorbital-sensations-facial-drooptolosa-hunt-syndrome/
A Patient Presenting with Ptosis, Ophthalmoplegia, and Decreased Periorbital Sensations and Facial Droop in Tolosa-Hunt Syndrome medicine2.missouri.edu/jahm/patient-presenting-ptosis-ophthalmoplegia-decreased-periorbital-sensations-facial-drooptolosa-hunt-syndrome/
Differences between CS-DAVF and TCCF to reveal and redefine CS-DAVF
 Pan et al. Chinese Neurosurgical Journal (2018) 4:26 https://doi.org/10.1186/s41016-018-0121-z CHINESE MEDICAL ASSOCIATION COMMENTARY Differences between CS-DAVF and TCCF to reveal and redefine CS-DAVF
Pan et al. Chinese Neurosurgical Journal (2018) 4:26 https://doi.org/10.1186/s41016-018-0121-z CHINESE MEDICAL ASSOCIATION COMMENTARY Differences between CS-DAVF and TCCF to reveal and redefine CS-DAVF
Cavernous sinus thrombosis: Departmental guidelines
 Michele Long Division of Otorhinolaryngology Faculty of Health Sciences Tygerberg Campus, University of Stellenbosch Cavernous sinus thrombosis: Departmental guidelines Anatomy- cavernous sinus 2cm in
Michele Long Division of Otorhinolaryngology Faculty of Health Sciences Tygerberg Campus, University of Stellenbosch Cavernous sinus thrombosis: Departmental guidelines Anatomy- cavernous sinus 2cm in
Treatment of carotid-cavernous fistula using a balloon-tipped intra-arterial catheter
 Journal of Neurology, Neurosurgery, and Psychiatry, 1978, 41, 996-1000 Treatment of carotid-cavernous fistula using a balloon-tipped intra-arterial catheter U. M. CHOWDHARY From the Department of Neurology,
Journal of Neurology, Neurosurgery, and Psychiatry, 1978, 41, 996-1000 Treatment of carotid-cavernous fistula using a balloon-tipped intra-arterial catheter U. M. CHOWDHARY From the Department of Neurology,
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Occlusion of Arteriovenous Malformations of the Cavernous Sinus via the Superior Ophthalmic Vein
 539 Occlusion of Arteriovenous Malformations of the Cavernous Sinus via the Superior Ophthalmic Vein Michael Mu Huo Teng' 2 Wan-Yuo Guo' Chun-I Huang 3 Chih-Chiau Wu 4 Tsuen Chang' The treatment of five
539 Occlusion of Arteriovenous Malformations of the Cavernous Sinus via the Superior Ophthalmic Vein Michael Mu Huo Teng' 2 Wan-Yuo Guo' Chun-I Huang 3 Chih-Chiau Wu 4 Tsuen Chang' The treatment of five
Occipital lobe infarction: a rare presentation of bilateral giant cavernous carotid aneurysms: a case report
 Vanikieti et al. BMC Ophthalmology (2018) 18:25 DOI 10.1186/s12886-018-0687-4 CASE REPORT Open Access Occipital lobe infarction: a rare presentation of bilateral giant cavernous carotid aneurysms: a case
Vanikieti et al. BMC Ophthalmology (2018) 18:25 DOI 10.1186/s12886-018-0687-4 CASE REPORT Open Access Occipital lobe infarction: a rare presentation of bilateral giant cavernous carotid aneurysms: a case
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit
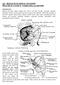 213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit OSTEOLOGY Identify the bones which comprise the walls of the orbit: maxilla, zygomatic, ethmoid, lachrymal, frontal, and
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit OSTEOLOGY Identify the bones which comprise the walls of the orbit: maxilla, zygomatic, ethmoid, lachrymal, frontal, and
The Ishikawa Classification of Cavernous Sinus Lesions by Clinico-anatomical Findings
 The Ishikawa Classification of Cavernous Sinus Lesions by Clinico-anatomical Findings Mutsumi Yoshihara, Noriko Saito, Yoji Kashima and Hiroshi Ishikawa Department of Ophthalmology, Nihon University School
The Ishikawa Classification of Cavernous Sinus Lesions by Clinico-anatomical Findings Mutsumi Yoshihara, Noriko Saito, Yoji Kashima and Hiroshi Ishikawa Department of Ophthalmology, Nihon University School
C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital
 C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital Disclosures Neither I nor any family members have any pertinent financial relations
C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital Disclosures Neither I nor any family members have any pertinent financial relations
Endovascular treatment with transvenous approach for embolization of carotid cavernous fistula
 169 Case Report Endovascular treatment with transvenous approach for embolization of carotid cavernous fistula Benny Young, Agusmanan Bojeng Department of Radiology, University Malaysia Sarawak, Faculty
169 Case Report Endovascular treatment with transvenous approach for embolization of carotid cavernous fistula Benny Young, Agusmanan Bojeng Department of Radiology, University Malaysia Sarawak, Faculty
A.J. Hauer Intracranial dural arteriovenous fistulae
 A.J. Hauer 27-06-2018 Intracranial dural arteriovenous fistulae Dural arteriovenous fistulae (davfs) epidemiology Pathological anastomoses (within the dural leaflets) between meningeal arteries and dural
A.J. Hauer 27-06-2018 Intracranial dural arteriovenous fistulae Dural arteriovenous fistulae (davfs) epidemiology Pathological anastomoses (within the dural leaflets) between meningeal arteries and dural
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
Primary optic nerve meningioma
 Primary optic nerve meningioma British Journal of Ophthalmology, 1980, 64, 553-558 J. E. WRIGHT, N. B. CALL,* AND S. LIARICOSt From the Orbital Clinic, Moorfields Eye Hospital, City Road, London ECJ V
Primary optic nerve meningioma British Journal of Ophthalmology, 1980, 64, 553-558 J. E. WRIGHT, N. B. CALL,* AND S. LIARICOSt From the Orbital Clinic, Moorfields Eye Hospital, City Road, London ECJ V
Emergency Ocular Motility Disorders Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital
 Emergency Ocular Motility Disorders Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Emergency Ocular Motility Disorders Cranial nerves palsies (oculomotor, Trochlear & abducent) Orbital
Emergency Ocular Motility Disorders Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Emergency Ocular Motility Disorders Cranial nerves palsies (oculomotor, Trochlear & abducent) Orbital
Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving the Laterocavernous Sinus
 Journal of Neuroendovascular Therapy 2017; 11: 1 7 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0062 Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving
Journal of Neuroendovascular Therapy 2017; 11: 1 7 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0062 Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving
Orbital facia. Periororbital facia Orbital septum Bulbar facia Muscular facia
 Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
External carotid blood supply to acoustic neurinomas
 External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
Acute onset diplopia. Methods. Introduction. Una O Colmain, Claire Gilmour and Caroline J. MacEwen. Acta Ophthalmologica 2014
 Acute onset diplopia Una O Colmain, Claire Gilmour and Caroline J. MacEwen Ninewells Hospital and Medical School, Dundee, UK ABSTRACT. Purpose: To investigate the clinical features of all patients with
Acute onset diplopia Una O Colmain, Claire Gilmour and Caroline J. MacEwen Ninewells Hospital and Medical School, Dundee, UK ABSTRACT. Purpose: To investigate the clinical features of all patients with
Literature Review: Neurosurgery
 NANOS 2018 Kona, Hawaii Literature Review: Neurosurgery Neil R. Miller, MD FACS Frank B. Walsh Professor of Neuro-Ophthalmology Professor of Ophthalmology, Neurology & Neurosurgery Johns Hopkins University
NANOS 2018 Kona, Hawaii Literature Review: Neurosurgery Neil R. Miller, MD FACS Frank B. Walsh Professor of Neuro-Ophthalmology Professor of Ophthalmology, Neurology & Neurosurgery Johns Hopkins University
Three-dimensional FISP Imaging in the Evaluation of Carotid Cavernous Fistula: Comparison with Contrast-Enhanced CT and Spin-Echo MR
 AJNR Am J Neuroradiol 19:253 259, February 1998 Three-dimensional Imaging in the Evaluation of Carotid Cavernous Fistula: Comparison with and Toshinori Hirai, Yukunori Korogi, Satoshi Hamatake, Ichiro
AJNR Am J Neuroradiol 19:253 259, February 1998 Three-dimensional Imaging in the Evaluation of Carotid Cavernous Fistula: Comparison with and Toshinori Hirai, Yukunori Korogi, Satoshi Hamatake, Ichiro
Professor Helen Danesh-Meyer. Eye Institute Auckland
 Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Jacqueline Theis, O.D., F.A.A.O.
 Neuro-Ophthalmological Emergencies Presenting in Primary Care Optometry Describes the symptoms, signs, and management of neuro-ophthalmological emergencies. Signs/Symptoms to be Concerned about (especially
Neuro-Ophthalmological Emergencies Presenting in Primary Care Optometry Describes the symptoms, signs, and management of neuro-ophthalmological emergencies. Signs/Symptoms to be Concerned about (especially
No Financial Interest
 Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Embryology of the Ophthalmic Artery: a Revived Concept
 www.centauro.it Interventional Neuroradiology 15: 363-368, 2009 Letter to the Editor Embryology of the Ophthalmic Artery: a Revived Concept M. KOMIYAMA Department of Neurosurgery, Osaka City General Hospital;
www.centauro.it Interventional Neuroradiology 15: 363-368, 2009 Letter to the Editor Embryology of the Ophthalmic Artery: a Revived Concept M. KOMIYAMA Department of Neurosurgery, Osaka City General Hospital;
13/02/1440 بسم ا هلل ا لرحمن ا لر حيم
 بسم ا هلل ا لرحمن ا لر حيم 1 Slowly progressive versus rapidly progressive proptosis by Ali M ISMAIL professor of ophthalmology @SOHAG U H Occuloplastic fellow @NNUH Occuloplastic fellow @Cambridge UH
بسم ا هلل ا لرحمن ا لر حيم 1 Slowly progressive versus rapidly progressive proptosis by Ali M ISMAIL professor of ophthalmology @SOHAG U H Occuloplastic fellow @NNUH Occuloplastic fellow @Cambridge UH
Supplementary Online Content
 Supplementary Online Content Park KH, Kim YK, Woo SJ, et al. Iatrogenic occlusion of the ophthalmic artery after cosmetic facial filler injections: a national survey by the Korean Retina Society. JAMA
Supplementary Online Content Park KH, Kim YK, Woo SJ, et al. Iatrogenic occlusion of the ophthalmic artery after cosmetic facial filler injections: a national survey by the Korean Retina Society. JAMA
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
A Shunt of the Diploic Vein of the Orbital Roof Accompanying a Cavernous Sinus Dural Arteriovenous Fistula: A Case Report
 Journal of Neuroendovascular Therapy 2018; 12: 38 42 Online September 11, 2017 DOI: 10.5797/jnet.cr.2017-0056 A Shunt of the Diploic Vein of the Orbital Roof Accompanying a Cavernous Sinus Dural Arteriovenous
Journal of Neuroendovascular Therapy 2018; 12: 38 42 Online September 11, 2017 DOI: 10.5797/jnet.cr.2017-0056 A Shunt of the Diploic Vein of the Orbital Roof Accompanying a Cavernous Sinus Dural Arteriovenous
! Women greater than men (4:1)» Typical of other autoimmune diseases
 1 2 3 4 : Overview and Diagnosis Suzanne K. Freitag, M.D. Director, Ophthalmic Plastic Surgery Massachusetts Eye and Ear Infirmary Harvard Medical School! I have no financial disclosures. Learning Objectives!
1 2 3 4 : Overview and Diagnosis Suzanne K. Freitag, M.D. Director, Ophthalmic Plastic Surgery Massachusetts Eye and Ear Infirmary Harvard Medical School! I have no financial disclosures. Learning Objectives!
Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal
 AJNR Am J Neuroradiol 20:2016 2020, November/December 1999 Case Report Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal Robert Ernst, Robert Bulas,
AJNR Am J Neuroradiol 20:2016 2020, November/December 1999 Case Report Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal Robert Ernst, Robert Bulas,
Cerebellar Hemorrhage due to a Direct Carotid Cavernous Fistula after Surgery for Maxillary Cancer
 Case Report J Korean Neurosurg Soc 60 (1) : 89-93, 2017 https://doi.org/10.3340/jkns.2015.1206.001 pissn 2005-3711 eissn 1598-7876 Cerebellar Hemorrhage due to a Direct Carotid Cavernous Fistula after
Case Report J Korean Neurosurg Soc 60 (1) : 89-93, 2017 https://doi.org/10.3340/jkns.2015.1206.001 pissn 2005-3711 eissn 1598-7876 Cerebellar Hemorrhage due to a Direct Carotid Cavernous Fistula after
Cilioretinal collateral circulation after occlusion of the central retinal artery
 British Journal of Ophthalmology, 1985, 69, 805-809 Cilioretinal collateral circulation after occlusion of the central retinal artery MICHAEL F MARMOR,' LEE M JAMPOL,2 AND LISA WOHL2 From the 'Division
British Journal of Ophthalmology, 1985, 69, 805-809 Cilioretinal collateral circulation after occlusion of the central retinal artery MICHAEL F MARMOR,' LEE M JAMPOL,2 AND LISA WOHL2 From the 'Division
Ocular Manifestations and Prognosis of Secondary Glaucoma in Patients with Carotid-Cavernous Fistula
 Ocular Manifestations and Prognosis of Secondary Glaucoma in Patients with Carotid-Cavernous Fistula Kiyotaka Ishijima*, Kenji Kashiwagi*, Kenichi Nakano*, Takashi Shibuya, Toyoaki Tsumura and Shigeo Tsukahara*
Ocular Manifestations and Prognosis of Secondary Glaucoma in Patients with Carotid-Cavernous Fistula Kiyotaka Ishijima*, Kenji Kashiwagi*, Kenichi Nakano*, Takashi Shibuya, Toyoaki Tsumura and Shigeo Tsukahara*
Carotid Artery Dissection Causing an Isolated Hypoglossal. Nerve Palsy
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550035 Volume 2, Issue 5 Case Report Carotid Artery Dissection Causing an Isolated Hypoglossal Muzzammil Ali*, Yatin Sardana Nerve Palsy
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550035 Volume 2, Issue 5 Case Report Carotid Artery Dissection Causing an Isolated Hypoglossal Muzzammil Ali*, Yatin Sardana Nerve Palsy
Unruptured Aneurysms with Cranial Nerve Symptoms: Efficacy of Endosaccular Guglielmi Detachable Coil Treatment
 nruptured Aneurysms with Cranial Nerve Symptoms: Efficacy of Endosaccular Guglielmi Detachable Coil Treatment Dong Joon Kim, MD Dong Ik Kim, MD Seung-Koo Lee, MD Si Yeon Kim, MD Objective: To evaluate
nruptured Aneurysms with Cranial Nerve Symptoms: Efficacy of Endosaccular Guglielmi Detachable Coil Treatment Dong Joon Kim, MD Dong Ik Kim, MD Seung-Koo Lee, MD Si Yeon Kim, MD Objective: To evaluate
Neuro-Ocular Grand Rounds
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Post-traumatic right carotid-cavernous fistula resulting in symptoms in the contralateral eye: a case report and literature review
 Zhu et al. BMC Ophthalmology (2018) 18:183 https://doi.org/10.1186/s12886-018-0863-6 CASE REPORT Open Access Post-traumatic right carotid-cavernous fistula resulting in symptoms in the contralateral eye:
Zhu et al. BMC Ophthalmology (2018) 18:183 https://doi.org/10.1186/s12886-018-0863-6 CASE REPORT Open Access Post-traumatic right carotid-cavernous fistula resulting in symptoms in the contralateral eye:
IMAGE OF THE MOMENT PRACTICAL NEUROLOGY
 178 PRACTICAL NEUROLOGY IMAGE OF THE MOMENT Gawn G. McIlwaine*, James H. Vallance* and Christian J. Lueck *Princess Alexandra Eye Pavilion, Chalmers Street, Edinburgh UK; The Canberra Hospital, P.O. Box
178 PRACTICAL NEUROLOGY IMAGE OF THE MOMENT Gawn G. McIlwaine*, James H. Vallance* and Christian J. Lueck *Princess Alexandra Eye Pavilion, Chalmers Street, Edinburgh UK; The Canberra Hospital, P.O. Box
Colour Doppler Imaging of Superior Ophthalmic Vein in Thyroid-Associated Eye Disease
 Colour Doppler Imaging of Superior Ophthalmic Vein in Thyroid-Associated Eye Disease Deniz Somer*, Seyhan Bahar Özkan*, Hakan Özdemir, Serhan Atilla, Meltem Fatma Söylev* and Sunay Duman* *Department of
Colour Doppler Imaging of Superior Ophthalmic Vein in Thyroid-Associated Eye Disease Deniz Somer*, Seyhan Bahar Özkan*, Hakan Özdemir, Serhan Atilla, Meltem Fatma Söylev* and Sunay Duman* *Department of
Orbital and Ocular Adnexal Disorders with Red Eyes
 Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Management of ipsilateral ptosis with hypotropia
 British Journal of Ophthalmology, 1986, 70, 732-736 Management of ipsilateral ptosis with hypotropia L A FICKER, J R 0 COLLIN, AND J P LEE From Moorfields Eye Hospital, London SUMMARY Thirty-one patients
British Journal of Ophthalmology, 1986, 70, 732-736 Management of ipsilateral ptosis with hypotropia L A FICKER, J R 0 COLLIN, AND J P LEE From Moorfields Eye Hospital, London SUMMARY Thirty-one patients
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
CT of Maxillofacial Fracture Patterns. CT of Maxillofacial Fracture Patterns
 CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
ANGIOGRAPHY OF THE NORMAL OPHTHALMIC
 Brit. J. Ophthal., 35, 473. ANGIOGRAPHY OF THE NORMAL OPHTHALMIC ARTERY AND CHOROIDAL PLEXUS OF THE EYE* BY P. H. SCHURR From the Department of Neurosurgery, Radcliffe Infirmary, Oxford THE ophthalmic
Brit. J. Ophthal., 35, 473. ANGIOGRAPHY OF THE NORMAL OPHTHALMIC ARTERY AND CHOROIDAL PLEXUS OF THE EYE* BY P. H. SCHURR From the Department of Neurosurgery, Radcliffe Infirmary, Oxford THE ophthalmic
The Orbit. The Orbit OCULAR ANATOMY AND DISSECTION 9/25/2014. The eye is a 23 mm organ...how difficult can this be? Openings in the orbit
 The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
A neurysms arising from the cavernous portion of the
 863 PAPER Long term visual and neurological prognosis in patients with treated and untreated cavernous sinus aneurysms N Goldenberg-Cohen, C Curry, N R Miller, R J Tamargo, K P J Murphy... See end of article
863 PAPER Long term visual and neurological prognosis in patients with treated and untreated cavernous sinus aneurysms N Goldenberg-Cohen, C Curry, N R Miller, R J Tamargo, K P J Murphy... See end of article
Passive ocular proptosis
 Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 1198-1202 Passive ocular proptosis BRIAN P. O'NEILL From the Department of Neurology, University of Michigan Medical Center, and the Neurology
Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 1198-1202 Passive ocular proptosis BRIAN P. O'NEILL From the Department of Neurology, University of Michigan Medical Center, and the Neurology
The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3-
 1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils
 High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils Guido Guglielmi, Fernando Viñuela, Gary Duckwiler, Jacques Dion, and Alfredo Stocker Summary: We present one case of
High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils Guido Guglielmi, Fernando Viñuela, Gary Duckwiler, Jacques Dion, and Alfredo Stocker Summary: We present one case of
Percutaneous Embolization of Arteriovenous Fistulas of the External Carotid Artery
 937 Percutaneous Embolization of rteriovenous Fistulas of the External Carotid rtery lex erenstein 1 John Scote In Sup Choi 1 Mark Persky3 Nineteen arteriovenous fistulas of the external carotid branches
937 Percutaneous Embolization of rteriovenous Fistulas of the External Carotid rtery lex erenstein 1 John Scote In Sup Choi 1 Mark Persky3 Nineteen arteriovenous fistulas of the external carotid branches
In a recent retrospective study we analyzed the technical success
 ORIGINAL RESEARCH A. Bink K. Goller M. Lüchtenberg T. Neumann-Haefelin S. Dützmann F. Zanella J. Berkefeld R. du Mesnil de Rochemont Long-Term Outcome after Coil Embolization of Cavernous Sinus Arteriovenous
ORIGINAL RESEARCH A. Bink K. Goller M. Lüchtenberg T. Neumann-Haefelin S. Dützmann F. Zanella J. Berkefeld R. du Mesnil de Rochemont Long-Term Outcome after Coil Embolization of Cavernous Sinus Arteriovenous
Brain Injuries. Presented By Dr. Said Said Elshama
 Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
EYE INJURIES OBJECTIVES COMMON EYE EMERGENCIES 7/19/2017 IMPROVE ASSESSMENT OF EYE INJURIES
 EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
Papilledema. Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D.
 Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Bilateral common carotid occlusion with hypoxic ocular sequelae
 Brit. J. Ophthal. (1971) 55, 383 Bilateral common carotid occlusion with hypoxic ocular sequelae C. T. HART AND S. HAWORTH Cheltenham A patient is described who was referred with anterior uveitis; following
Brit. J. Ophthal. (1971) 55, 383 Bilateral common carotid occlusion with hypoxic ocular sequelae C. T. HART AND S. HAWORTH Cheltenham A patient is described who was referred with anterior uveitis; following
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Herpes Zoster Ophthalmicus and Lateral Rectus Palsy in an Elderly Patient
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Methods. Yahya Paksoy, Bülent Oğuz Genç, and Emine Genç. AJNR Am J Neuroradiol 24: , August 2003
 AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
Amaurosis fugax: some aspects of management
 Journal of Neurology, Neurosurgery, and Psvchiatry 1982;45:1-6 Amaurosis fugax: some aspects of management PJ PARKIN, BE KENDALL, J MARSHALL, WI McDONALD From the National Hospital for Nervous Diseases,
Journal of Neurology, Neurosurgery, and Psvchiatry 1982;45:1-6 Amaurosis fugax: some aspects of management PJ PARKIN, BE KENDALL, J MARSHALL, WI McDONALD From the National Hospital for Nervous Diseases,
Clinical Manifestation of Ocular Motor Nerve Palsies in a Tertiary Eye Hospital of Kathmandu, Nepal
 72 Original article Clinical Manifestation of Ocular Motor Nerve Palsies in a Tertiary Eye Hospital of Kathmandu, Nepal Sitaula S 1, Sharma AK 1, Shrestha GB 1, Gajurel BP 2, Shrestha GS 1 1 Department
72 Original article Clinical Manifestation of Ocular Motor Nerve Palsies in a Tertiary Eye Hospital of Kathmandu, Nepal Sitaula S 1, Sharma AK 1, Shrestha GB 1, Gajurel BP 2, Shrestha GS 1 1 Department
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Haemorrhagic glaucoma
 Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Post-traumatic persistent trigeminal artery-cavernous fistula: a case report and review of literature
 . 252. Post-traumatic persistent trigeminal artery-cavernous fistula: a case report and review of literature HU Wei-peng 胡伟鹏 *, HUANG Tian-zao 黄天造, GAO Hong-zhi 高宏志, YU Mao-qing 余茂清 and XU Chao-yang 徐朝阳
. 252. Post-traumatic persistent trigeminal artery-cavernous fistula: a case report and review of literature HU Wei-peng 胡伟鹏 *, HUANG Tian-zao 黄天造, GAO Hong-zhi 高宏志, YU Mao-qing 余茂清 and XU Chao-yang 徐朝阳
Congenital ocular palsy
 Brit. j. Ophthal. (1972) 56, 356 Congenital ocular palsy C. G. KEITH Queen Elizabeth Hospitalfor Children, Hackney Road, London Three patients with severe restriction of the ocular movements in one eye
Brit. j. Ophthal. (1972) 56, 356 Congenital ocular palsy C. G. KEITH Queen Elizabeth Hospitalfor Children, Hackney Road, London Three patients with severe restriction of the ocular movements in one eye
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
LECTURE # 7 EYECARE REVIEW: PART III
 LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
Anterior Segment Ischemia After Strabismus Surgery for IIIrd Nerve Palsy. Tenley Bower, MD, ARCT Michael Flanders, MD
 Anterior Segment Ischemia After Strabismus Surgery for IIIrd Nerve Palsy Tenley Bower, MD, ARCT Michael Flanders, MD Outline 1. Bilateral nuclear 3rd nerve palsy + vertical gaze palsy 2. Strabismus Surgery
Anterior Segment Ischemia After Strabismus Surgery for IIIrd Nerve Palsy Tenley Bower, MD, ARCT Michael Flanders, MD Outline 1. Bilateral nuclear 3rd nerve palsy + vertical gaze palsy 2. Strabismus Surgery
Endovascular Embolization of Taumatic Intracavernous Pseudoaneurysm of Internal Carotid Artery
 Endovascular Embolization of Taumatic Intracavernous Pseudoaneurysm of Internal Carotid Artery Tanveer Ul Haq,Shahzad Ahmad Khan,Imtiaz Hussain Rizvi ( Department of Radiology, The Aga Khan University
Endovascular Embolization of Taumatic Intracavernous Pseudoaneurysm of Internal Carotid Artery Tanveer Ul Haq,Shahzad Ahmad Khan,Imtiaz Hussain Rizvi ( Department of Radiology, The Aga Khan University
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Isolated Cranial Nerve-III Palsy Secondary to Perimesencephalic Subarachnoid Hemorrhage
 Lehigh Valley Health Network LVHN Scholarly Works Department of Medicine Isolated Cranial Nerve-III Palsy Secondary to Perimesencephalic Subarachnoid Hemorrhage Hussam A. Yacoub MD Lehigh Valley Health
Lehigh Valley Health Network LVHN Scholarly Works Department of Medicine Isolated Cranial Nerve-III Palsy Secondary to Perimesencephalic Subarachnoid Hemorrhage Hussam A. Yacoub MD Lehigh Valley Health
Dural Arteriovenous Malformations and Fistulae (DAVM S DAVF S)
 Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Ocular and periocular trauma
 Ocular and periocular trauma No financial disclosures. Tina Rutar M.D. Assistant Professor of Clinical Ophthalmology and Pediatrics Director, Visual Center for the Child University of California San Francisco
Ocular and periocular trauma No financial disclosures. Tina Rutar M.D. Assistant Professor of Clinical Ophthalmology and Pediatrics Director, Visual Center for the Child University of California San Francisco
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy
 Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Case Conference: Neuroradiology. Case 1: Tumor Case 1: 22yo F w/ HA and prior Seizures
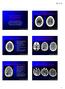 Case Conference: Neuroradiology Case 1: 22yo F w/ HA and prior Seizures David E. Rex, MD, PhD Stanford University Hospital Department of Radiology Case 1: Tumor Most likely gangiloglioma, oligodendroglioma,
Case Conference: Neuroradiology Case 1: 22yo F w/ HA and prior Seizures David E. Rex, MD, PhD Stanford University Hospital Department of Radiology Case 1: Tumor Most likely gangiloglioma, oligodendroglioma,
Ischaemic ocular necrosis from carotid-cavernous fistula
 Brit. J. Ophthal. (I973) 57, I45 Communications Ischaemic ocular necrosis from carotid-cavernous fistula Pathology of stagnant anoxic "inflammation" in orbital and ocular tissues W. H. SPENCER, H. S. THOMPSON,*
Brit. J. Ophthal. (I973) 57, I45 Communications Ischaemic ocular necrosis from carotid-cavernous fistula Pathology of stagnant anoxic "inflammation" in orbital and ocular tissues W. H. SPENCER, H. S. THOMPSON,*
Brain ميهاربا لض اف دمح ا د The Meninges 1- Dura Mater of the Brain endosteal layer does not extend meningeal layer falx cerebri tentorium cerebelli
 .احمد د فاضل ابراهيم Lecture 15 Brain The Meninges Three protective membranes or meninges surround the brain in the skull: the dura mater, the arachnoid mater, and the pia mater 1- Dura Mater of the Brain
.احمد د فاضل ابراهيم Lecture 15 Brain The Meninges Three protective membranes or meninges surround the brain in the skull: the dura mater, the arachnoid mater, and the pia mater 1- Dura Mater of the Brain
mistake ;slides in bold but you still have to go back to our slides to see the figure, tables and some scheme
 Khozama jehad : I am doing my best and I am sorry for any unintended mistake ;slides in bold but you still have to go back to our slides to see the figure, tables and some scheme The Orbit, Orbital Contents
Khozama jehad : I am doing my best and I am sorry for any unintended mistake ;slides in bold but you still have to go back to our slides to see the figure, tables and some scheme The Orbit, Orbital Contents
Traumatic Partial Optic Nerve Avulsion with Globe luxation. Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine
 Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
Endovascular Treatment of Cavernous Sinus Dural Arteriovenous Fistulas by Direct Puncture of Facial Vein
 J Radiol Sci 2011; 36: 129-134 Endovascular Treatment of Cavernous Sinus Dural Arteriovenous Fistulas by Direct Puncture of Facial Vein Shih-Wei Hsu 1 Yeh-Lin Kuo 1 Min-Hsiung Cheng 2 Department of Diagnostic
J Radiol Sci 2011; 36: 129-134 Endovascular Treatment of Cavernous Sinus Dural Arteriovenous Fistulas by Direct Puncture of Facial Vein Shih-Wei Hsu 1 Yeh-Lin Kuo 1 Min-Hsiung Cheng 2 Department of Diagnostic
1 Eyelids. Lacrimal Apparatus. Orbital Region. 3 The Orbit. The Eye
 1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
