Management of Giant Aneurysm
|
|
|
- Rosaline Cameron
- 5 years ago
- Views:
Transcription
1 Management of Giant Aneurysm Paul P. Huang, M.D. and Jafar J. Jafar, M.D. Department of Neurosurgery New York University Medical Center New York, New York, USA Introduction Giant intracranial aneurysms account for about 5 percent of all aneurysms, and are arbitrarily defined as having a diameter greater than 25 mm. These lesions, if left untreated, have an extremely poor natural history, with higher rates of morbidity and mortality than smaller saccular aneurysms. A retrospective review of untreatable giant aneurysms revealed an 80% risk of death or severe disability within 5 years of presentation.(5) In prospective natural history studies, patients with unruptured, untreated giant aneurysms had a 5 year cumulative hemorrhage rate of 40-50%.(6) In contrast to patients with smaller aneurysms, 65 to 85% of patients with giant aneurysms present with symptoms related to mass effect. The presence of specific focal neurologic deficits, cranial neuropathies, and visual field defects are directly related to the size and location of the specific lesion.subarachnoid hemorrhages occur in 25 to 35 percent of patients on presentation.(1) Thrombus formation within these large aneurysms may result in ischemic events from parent vessel thrombosis, perforator vessel occlusion and embolic events. Evaluation Treatment of giant aneurysms can be particularly challenging. The size and complexity of these lesions, compared to smaller aneurysms, results in higher treatment morbidity and mortality. Successful outcomes require adequate proximal control, meticulous dissection, preservation of all perforating arteries, reduction of mass effect, and maintenance of distal outflow either directly or indirectly. Adequate pretreatment planning requires a detailed understanding of the local vascular anatomy, the configuration of the neck, and the involvement of perforators. Problems can be anticipated in the presence of thrombus, plaques or calcification. A thorough evaluation and understanding of the collateral circulation across both hemispheres and from the external circulation usually reveals several options for excluding the aneurysm from the cerebral circulation. This knowledge also proves invaluable should an unexpected event occur during treatment. Computed tomography (CT) scanning revolutionized neurosurgery when it first appeared several decades ago and remains an essential component of the diagnostic work-up. The CT scan can be obtained easily and rapidly at most centers, and so is often the first study obtained when one suspects a subarachnoid hemorrhage. The CT scan also provides excellent visualization of calcifications within the aneurysm
2 dome, neck and the surrounding vessels, since the presence of a highly calcified lesion can severely limit the possible treatment options. The quality of CT angiographic studies has improved immensely over the past few years and provides excellent visualization of the size and configuration of the aneurysm dome, aneurysm neck, and associated vessels. Current CT 3D reconstruction techniques produces high-resolution multi-planar views of the lesion in relation to the base of the skull, and in many centers are preferred over magnetic resonance imaging (MRI) studies in this regard. MRIs remain an excellent tool for evaluating the true size of the aneurysm dome. Other imaging modalities visualize only the intra-luminal dimensions of an aneurysm, and so may underestimate the true size of the lesion, especially when there is thrombus within the aneurysm dome. MRI also can also demonstrate the presence of edema or an ischemic event in the surrounding brain parenchyma. Despite the rapid advance of other imaging modalities, digital subtraction angiography remains the gold standard for evaluating aneurysms. This test provides detailed information about the aneurysm neck, associated perforators, and the surrounding vascular anatomy. It furnishes information regarding the presence or absence of collateral flow and the suitability of intracranial and extracranial vessels for bypass. In conjunction with a balloon test occlusion, angiography yields valuable information about the adequacy of collateral flow across the circle of Willis and thus allows us to evaluate the patient s tolerance for both temporary and permanent vessel occlusion. Treatment Direct Clipping Direct surgical clip application remains the treatment of choice for giant aneurysms. The large size of these aneurysms can make visualization of the neck challenging. Skull based approaches have been useful in widening the corridors of access to these aneurysm, thus providing better visualization of the aneurysm neck and important perforators. The wider angles allow more flexibility in clip application and decreases the amount of brain retraction needed for adequate exposure. Anterior Circulation Aneurysms The pterional craniotomy remains the standard approach for the vast majority of lesions located along the anterior circulation, providing access to the supraclinoid carotid, anterior communicating artery complex, and the middle cerebral arteries.
3 Patients are positioned in the supine position. The head is extended about 10 degrees and turned 30 degrees to the contralateral direction, and the bed is placed in about 30 degrees of reverse Trendelenberg to ensure that the head is above the level of the heart thus maximizing venous return. All giant aneurysms require intraoperative angiography, therefore, a radiolucent pin fixation device is preferred. The legs are kept straight, rather than slightly bent, to faciliate access to the groin for intraoperative femoral artery catheterization. A lumbar drain may be used to provide additional brain relaxation in when needed. The frontotemporal scalp is shaved about 1-2 cm behind the hairline from the tragus to the midline. The femoral artery is cannulated during the cranial exposure and then draped until needed later in the case. If we anticipate the need for proximal control of the carotid artery, the ipsilateral neck is also prepped and draped. A transverse incision through the neck from the midline to the medial edge of the sternocleidomastoid muscle is sufficient for exposure of the common, and internal carotid arteries for temporary occlusion. If a bypass is contemplated, a vertical incision is made along the medial border of the sternocleidomastoid muscle from the tip of the mastoid down to the base of the neck. The scalp incision is made from the midline to the zygomatic arch, taking care to stay behind the hairline for cosmetic reasons. The initial incision is kept above the level of the temporalis muscle fascia. It is useful to identify and preserve the superficial temporal artery whenever possible. Even if no bypass is planned, it can be used as a supplemental bypass if an unexpected situation occurs. The dissection is kept below the frontal fat pad as the skin is pulled forward to avoid injuring the frontalis muscle branch of the facial nerve. A second vertical incision is made through the temporalis muscle and fascia down to the base of the zygomatic arch. Superiorly, the incision is directed forward just under the insertion of the temporalis muscle at the superior temporal line, leaving a 1 cm cuff of tissue attached to the bone which aids in closure of the muscle at the end of the case. The incision is then reflected inferiorly along the
4 frontozygomatic process about 2 cm, which allows the temporal muscle to be reflected a little more inferiorly away from the pterion. A burr hole is placed at the superior temporal line, and additional burr holes are placed as needed. A frontotemporal craniotomy is performed. The lateral pterion is removed extradurally with a cutting high speed drill down to the superior orbital fissure. This provides a straight, flat trajectory down to the proximal carotid once the dura is opened. In most cases, the Sylvian fissure is opened to untether the frontal lobe from the temporal lobe. The arachnoid basal cisterns are opened. Release of CSF from these cisterns provides a substantial amount of brain relaxation, especially in unruptured cases. The addition of an intradural anterior clinoidectomy provides access to the proximal carotid and cavernous carotid segments. A crescent shaped dural incision is made from the anterior clinoid process to the medial part of the optic canal is performed. The dura is stripped free from the underlying bone. The bone overlying the optic canal, as well as the optic strut down to the body of the sphenoid ridge, are removed with a small, high speed irrigating diamond drill, allowing mobilization of the optic nerve and circumferential access to the clinoidal and cavenous segements of the carotid. The addition of an orbitozygomatic osteotomy enlarges the angle of access by removing the orbital rim and allowing the temporalis muscle to be deflected further inferiorly. For this procedure, the frontal and temporal dural are stripped away from the base of the frontal and temporal fossa. The periorbita needs to be separated from the superior and lateral wall of the orbit to a depth of about 3 cm from the orbital rim. A sagital cut is made using a reciprocating saw from the orbital rim posteriorly to a distance of about 3 cm. The periorbita and frontal dural are protected with retractors during this maneuver. A horizontal cut is then made across the roof and lateral wall of the orbit down to the inferior orbital fissure. Anteriorly, the zygoma is cut starting at the inferior orbital fissue and continuing posteroinferiorly to the zygomaticofacial foramen which is seen over the malar eminence. An addition cut starts at the anterior inferior edge of the zygomatic
5 arch forward to the zygomaticofacial foramen, connecting this to the previous cut. Finally, a cut is made at the root of the zygomatic arch. The entire block of bone can then be loosened and removed. Posterior Circulation Aneurysms When contemplating approaches to posterior circulations aneursms, it is useful to divide the posterior fossa into 3 zones: the upper basilar, mid basilar and vertebrobasilar segments. The pterional approach and its variations provide excellent access to the upper basilar region as previously described. The addition of an orbitozygomatic osteotomy provides a lower trajectory and is especially useful for high riding basilar tip lesions. The half and half procedure opens the lateral corridor by transecting the anterior temporal veins and retracting the temporal lobe posteriorly. However, we have found that a medial temporal uncusectomy with mild lateral retraction on the temporal lobe gives a similar view without the need to sacrifice any temporal veins.(3)
6 For low lying basilar apex lesions located about 1 cm below the posterior clinoid, and for posterior pointing basilar apex aneurysms, we favor the subtemporal approach, which gives an excellent visualization below the posterior clinoid and the top of the clivus. Important posterior perforators are well seen with this approach, although the contra-lateral posterior cerebral and superior cerebellar arteries are somewhat more difficult to visualize. The patients are positioned in the full lateral position. A lumbar drain is essential to decrease the amount of retraction on the temporal lobe. The head is tilted toward the floor. We use a horseshoe scalp incision, starting from the base of the zygomatic arch in front of the tragus. The incision extends upward, swings posteriorly over the ear, and then inferiorly down to the top of the mastoid bone. Two burr holes are placed at the inferior temporal fossa and the craniotomy is performed. Additional bone is drilled so that we are as flat as possible against the base of the temporal fossa. Retractors are usually required to lift the temporal lobe superiorly. The edge of the tentorium can also be cut or sutured back to provide additional exposure inferiorly. Mid basilar lesions require access deeper into the posterior fossa, and we prefer a combined subtemporal transpetrous approach. The patient is placed supine on a shoulder role with the head turned to the lateral position. The supratentorial portion of the exposure is the same as described for the subtemporal approach. The posterior inferior portion of the incision is extended down to the suboccipital bone. The suboccipital bone, mastoid and lateral petrous ridge are removed. This exposes the suboccipital dura, transverse and sigmoid sinuses, and the presigmoid dura. The dural opening extends along the base of the temporal fossa, crosses the superior petrosal sinus, and then extends down the presigmoid dura parallel to the sigmoid sinus. The tentorium can then be sectioned from
7 lateral to medial, thus exposing the entire lateral pons, thus communicating the supra and infratentorial compartments. Vertebrobasilar lesions are well exposed via a far lateral approach, which removes the suboccipital bone down to the foramen magnum and the lateral third of the occipital condyle.
8 The patient is again placed in the full lateral position as previously described. We prefer a hockey-stick incision starting over the mastroid, extending superiorly over the occiput, and then down the midline to the base of the neck. Sharp dissection is performed over the superior aspect of the C-1 lamina to indentify the vertebral artery. Bleeding from the perivertebral venous plexus can be controlled with bipolar coagulation or packing with Surgicel. A suboccipital craniotomy is performed including the foramen magnum. The lip of the foramen magnum sweeps forward to become the occipital condyle. A high speed drill is used to drill away the lateral rim of the foramen magnum and the medial third of the occipital condyle. A hemilaminectomy of C-1 is performed to the lateral mass. Additional Caveats The majority of patients with giant aneurysms require at least some period of temporary occlusion to aid in the dissection, and to soften the aneurysm during clip placement. Additional periods of ischemia are required if a bypass is needed. Prior to temporary occlusion, we will mildly elevate the blood pressure and deliver intravenous barbiturates. We prefer using thiopental sodium, a short acting barbiturate with a half life around 3-8 hours. Usually, a bolus dose of 3-5 mg/kg is sufficient for burst suppression. The complexity of these aneurysms can make clip application challenging. Temporary proximal vessel occlusion helps soften the aneurysm dome by reducing blood flow to the aneurysm. This allows for more vigorous manipulation of the dome, improves visualization of the neck, and aids in the dissection of important perforators. A large, pulsating dome can cause the clip to slide off the aneurysm neck, resulting in perforator or parent artery occlusion. Softening of the aneurysm can help adequately position the clip. For large paraclinoid lesions, a suction decompression technique performed via the internal carotid artery in the neck can be quite effective in deflating the aneurysm dome and improving the ease of clip placement. In some instances, particularly with posterior circulation aneurysms, the use of hypothermic circulatory arrest provides about 50 minutes of cerebral protection during the arrest phase. During arrest, the aneurysm becomes completely slack, allowing easier manipulation of the neck and dome, and improving the likelihood of a successful clipping. If there is a large thrombus within the aneurysm, or if the aneurysm had been previously coiled from a prior endovascular procedure, proximal vessel occlusion will be inadequate in softening the aneurysm. In these cases, the aneurysm must be opened, and the thrombus or coils removed, to allow adequate clip placement across the neck. Removal of the intra-aneurysmal coils should be avoided if 3 weeks pass after aneurysmal coiling. Most of these aneurysms have wide necks. The longer aneurysm clips may not have sufficient closing pressure to completely occlude the aneurysm neck. Sometimes, a booster clip can be used to supplement the main clip. More frequently, application of multiple smaller clips, either in tandem or parallel, is required for successful occlusion. Given the complex nature of these lesions and the need for innovative clipping techniques, intraoperative angiography is
9 important in confirming both successful occlusion of the aneurysm and patency of the surrounding vessels. Bypass Not infrequently, direct clip placement is not possible in giant aneurysms. In these situations, closure of the parent vessel may be a good alternative in excluding the aneurysm from the cerebral circulation. There must be adequate collateral circulation and no important functional perforators in the segment of vessel to be excluded. Aneurysms of the cavenernous carotid and paraclinoid region are often amenable to proximal ligation and simple trapping. If the collateral circulation is inadequate to perfuse the distal vasculature, then a bypass is necessary. The superficial temporal artery is readily available and easily accessible in most patients. This artery provides a relatively low flow rate, and cannot completely replace the carotid artery or even the main M1 trunk. However, it may be sufficient if there are additional, albeit less than adequeate, collaterals from the circle of Willis. It is also adequate for revascularizing a distal MCA branch vessel. A higher flow bypass is required to replace the flow demands of the carotid artery or M1 segment, and in this situation, a saphenous vein or radial artery grafts works very well. Unlike a low flow bypass, patients undergoing a high flow bypass are fully heparinzed during the actual contruction of the bypass. For the posterior circulation, the occipital artery can provide perfusion to proximal vessel segments. Distal supplementation usually requires a saphenous vein graft. Flow diversion When important perforators are incorporated within the walls of the aneurysm, or the aneurysm is fusiform with no discernable neck, it might not be possible to completely exclude the aneurysm from the cerebral circulation. Formation of these aneurysms is related to hemodynamic stress from proximal, or inflow, vessels. Theoretically, reversal of flow through the aneurysm should reduce the shear stress within the aneurysm and thus presumably alter the natural history. Flow reversal can be accomplished by occluding the proximal feeding vessel. The blood flow to the distal vessels is supplied by either natural collaterals or via a bypass. Reversal of flow through the aneurysm provides perfusion to important branches and perforators incorporated within the aneurysm itself. Although there appears to be a reduction in the hemorrhage rate from these aneurysms using this strategy, it is not completely protective with a long term rehemorrhage rate of approximately 11%. (2) Endovascular techniques Endovascular techniques continue to evolve, but its utility remains limited, especially in lesions with wide necks. Complete aneurysmal occlusion is difficult, although a larger number of lesions around the paraclinoid carotid have become amenable to successful treatment. Thrombus formation in giant aneurysms is quite dynamic, resulting in high rates of coil compaction and recanalization. The development of balloon remodeling techniques allow for tighter packing of wide necked aneurysms, reducing the incidence of coil migration into the intraluminal space. The development of stenting technology over the past several years has also allowed tighter, more complete packing of many wide necked aneurysms.
10 However, tight packing of large aneurysms, especially those compressing the brainstem and optic nerves, may result in increased mass effect, edema and progressive neurological deterioration.(4) Flow alteration techniques using multiple stents are currently being evaluated, but the long term results are unknown at this time. Conclusion The natural history of giant aneurysms is extremely poor with a high rate of hemorrhage, death and severe disability within 5 years of diagnosis. Despite the difficulty inherent in treating these lesions, good outcomes are still possible in the majority of cases. Successful treatment of these formidable lesions requires a detailed understanding of the vascular anatomy, as well as the sophisticated use of the entire range of neurosurgical and endovascular techniques. References 1. Atkinson JLD, Piepgras DG: Giant Aneurysms: Supratentorial, in Carter LP, Spetzler RF, Hamilton MG (eds): Neurovascular Surgery. New York, McGraw-Hill, 1995, p Hoh BL, Putman CM, Budzik RF, Carter BS, Ogilvy CS: Combined surgical and endovascular techniques of flow alteration to treat fusiform and complex widenecked intracranial aneurysms that are unsuitable for clipping or coil embolization. J Neurosurg 95:24-35, Post N, Russell SM, Jafar JJ: Role of uncal resection in optimizing transsylvian access to the basilar apex: cadaveric investigation and preliminary clinical experience in eight patients. Neurosurgery 56: ; discussion , Russell SM, Nelson PK, Jafar JJ: Neurological deterioration after coil embolization of a giant basilar apex aneurysm with resolution following parent artery clip ligation. Case report and review of the literature. J Neurosurg 97: , Steinberg GK, Drake CG, Peerless SJ: Deliberate basilar or vertebral artery occlusion in the treatment of intracranial aneurysms. Immediate results and long-term outcome in 201 patients. J Neurosurg 79: , Wiebers DO, Whisnant JP, Huston J, 3rd, Meissner I, Brown RD, Jr., Piepgras DG, Forbes GS, Thielen K, Nichols D, O'Fallon WM, Peacock J, Jaeger L, Kassell NF, Kongable-Beckman GL, Torner JC: Unruptured intracranial aneurysms: natural history, clinical outcome, and risks of surgical and endovascular treatment. Lancet 362: , 2003.
11 Case Studies High flow EC-IC bypass: A 52 year old female presented with acute right eye blindness. The radiologic studies revealed a calcified, partially thrombosed ophthalmic segment aneurysm, and poor collateral circulation necessitating a high flow external carotid to M-1 segment bypass. This was followed by occlusion of the ICA in the neck, and trapping of the aneurysm with a clip. A CTA showing a giant, partially thrombosed, and calcified paraclinoid aneurysm. Balloon test occlusion showing delayed venous drainage on the right, indicating inadequate collateral circulation bypass.wmv An intraoperative microsurgical video demonstrating the construction of the radial artery EC-IC bypass. The distal intracranial end is constructed first. An AP and lateral common carotid angiogram showing the high flow radial artery bypass. 6 months postoperatively the patient could count fingers with the right eye.
12 Direct clipping: A 45 year old nurse with subarachnoid hemorrhage. Neurologically she was intact. She underwent direct surgical clipping via a left pterional approach. Her postoperative course was uneventful. A brain CT revealing the subarachnoid hemorrhage. The blood within the aneurysm could also be seen. Left lateral and AP ICA angiography showing giant ICA bifurcation aneurysm. A postoperative lateral and AP left ICA angiogram showing successful clipping of the aneurysm, and good distal filling of the distal intracranial circulation.
13 Parent vessel Occlusion: A 33 year old female 2 weeks after a subarachnoid hemorrhage from a basilar aneurysm. The aneurysm was not amenable to endovascular treatment, because of the presence of basilar perforators proximal to the aneurysm. She had very good collateral blood flow to the posterior circulation via bilateral posterior communicating arteries. The patient underwent direct proximal basilar occlusion with a clip through a far lateral approach. She was discharged neurologically intact 2 days after her surgery. A CT scan of the brain revealing blood along the tentorium, and dilated ventricles. 3-D vertebral angiography showing a giant basilar aneurysm. The proximal small brainstem perforators are not appreciated in this film. Postoperative lateral ICA angiogram showing good basilar perfusion through the posterior communicating artery. The left lateral vertebral injection reveals that the left vertebral artery ends in PICA.
5. COMMON APPROACHES. Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2.
 5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
5.5. RETROSIGMOID APPROACH
 5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
As a group, basilar artery aneurysms are
 OPERATIVE NUANCES ORBITOZYGOMATIC APPROACH TO BASILAR APEX ANEURYSMS Frank P.K. Hsu, M.D., Ph.D. Division of Neurological Surgery, St. Joseph s Hospital and Medical Center, Phoenix, Arizona Richard E.
OPERATIVE NUANCES ORBITOZYGOMATIC APPROACH TO BASILAR APEX ANEURYSMS Frank P.K. Hsu, M.D., Ph.D. Division of Neurological Surgery, St. Joseph s Hospital and Medical Center, Phoenix, Arizona Richard E.
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note
 Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
History of revascularization
 History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Interpositional carotid artery bypass strategies in the surgical management of aneurysms and tumors of the skull base
 Neurosurg Focus 14 (3):Article 2, 2003, Click here to return to Table of Contents Interpositional carotid artery bypass strategies in the surgical management of aneurysms and tumors of the skull base JAMES
Neurosurg Focus 14 (3):Article 2, 2003, Click here to return to Table of Contents Interpositional carotid artery bypass strategies in the surgical management of aneurysms and tumors of the skull base JAMES
Unit 18: Cranial Cavity and Contents
 Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
Contralateral clipping of bilateral middle cerebral artery aneurysms. Case report
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Contralateral clipping of bilateral middle cerebral artery aneurysms. Case report Georgiana Ion, Alexandru Chiriac, Ziyad Faiyad,
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Contralateral clipping of bilateral middle cerebral artery aneurysms. Case report Georgiana Ion, Alexandru Chiriac, Ziyad Faiyad,
We describe some of the conceptual nuances and
 Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms
 J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
Microsurgery for ruptured cerebellar arteriovenous malformations
 European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
Surgical management of complex intracranial aneurysms
 Review Article Surgical management of complex intracranial aneurysms Daniel L. Barrow, C. Michael Cawley Department of Neurosurgery and Emory MBNA Stroke Center, Emory University School of Medicine, Atlanta,
Review Article Surgical management of complex intracranial aneurysms Daniel L. Barrow, C. Michael Cawley Department of Neurosurgery and Emory MBNA Stroke Center, Emory University School of Medicine, Atlanta,
25/06/2010. Scaricato da 1
 Approcci chirurgici al Clivus DIPARTIMENTO DI NEUROCHIRURGIA SECONDA UNIVERSITÀ DI NAPOLI Prof. Aldo Moraci Surgical Anatomy of the Clivus Scaricato da www.sunhope.it 1 Midsagittal Section of the Skull
Approcci chirurgici al Clivus DIPARTIMENTO DI NEUROCHIRURGIA SECONDA UNIVERSITÀ DI NAPOLI Prof. Aldo Moraci Surgical Anatomy of the Clivus Scaricato da www.sunhope.it 1 Midsagittal Section of the Skull
CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY
 Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
OBJECTIVES. At the end of the lecture, students should be able to: List the cerebral arteries.
 DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: List the cerebral arteries. Describe the cerebral arterial supply regarding the origin, distribution and branches.
DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: List the cerebral arteries. Describe the cerebral arterial supply regarding the origin, distribution and branches.
Surgical techniques and procedures for cerebrovascular surgery. Surgery for the AVF at the cranio-cervical junction and high cervical spine
 VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
Surgery of Middle Cerebral Artery (MCA) Aneurysm
 Surgery of Middle Cerebral Artery (MCA) Aneurysm 15 Fusao Ikawa 15.1 Sign and Symptoms Middle cerebral artery (MCA) aneurysm is one of the most popular cerebral aneurysm. The incidence of ruptured MCA
Surgery of Middle Cerebral Artery (MCA) Aneurysm 15 Fusao Ikawa 15.1 Sign and Symptoms Middle cerebral artery (MCA) aneurysm is one of the most popular cerebral aneurysm. The incidence of ruptured MCA
TREATMENT OF INTRACRANIAL ANEURYSMS
 TREATMENT OF INTRACRANIAL ANEURYSMS Presented by: Dr Nilesh S. Kurwale Introduction Incidence of aneurysm difficult to estimate Prevalence 0.2-7.9 % Half the aneurysms ruptures 2% present during childhood
TREATMENT OF INTRACRANIAL ANEURYSMS Presented by: Dr Nilesh S. Kurwale Introduction Incidence of aneurysm difficult to estimate Prevalence 0.2-7.9 % Half the aneurysms ruptures 2% present during childhood
Dr. Sami Zaqout, IUG Medical School
 The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE
 Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE 1 The two parietal bones articulate in the midline AT THE SAGITTAL
Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE 1 The two parietal bones articulate in the midline AT THE SAGITTAL
TABLES. Table 1 Terminal vessel aneurysms. Table. Aneurysm location. Bypass flow** Symptoms Strategy Bypass recipient. Age/ Sex.
 Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
External carotid blood supply to acoustic neurinomas
 External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
Skull-2. Norma Basalis Interna Norma Basalis Externa. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Skull-2. Norma Basalis Interna. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery
 Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Techniques in cerebral aneurysm surgery
 SYⅤ-1 Surgery for large and giant cerebral aneurysm Hidetoshi Murata, Ryohei Miyazaki, Mitsuru Sato, Nobuyuki Shimizu, Takahiro Tanaka, Taishi Nakamura, Shigeta Miyake, Jun Suenaga, Tetsuya Yamamoto Department
SYⅤ-1 Surgery for large and giant cerebral aneurysm Hidetoshi Murata, Ryohei Miyazaki, Mitsuru Sato, Nobuyuki Shimizu, Takahiro Tanaka, Taishi Nakamura, Shigeta Miyake, Jun Suenaga, Tetsuya Yamamoto Department
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Neuroanatomy Dr. Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018
 Neuroanatomy Dr. Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Blood Supply of Brain and Spinal Cord Arterial Supply of Brain The brain receives blood
Neuroanatomy Dr. Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Blood Supply of Brain and Spinal Cord Arterial Supply of Brain The brain receives blood
T HE direct surgical approach to an aneurysm on
 J Neurosurg 66:500-505, 1987 Aneurysms of the basilar artery trunk KENICHIRO SUGITA, M.D., SHIGEAKI KOBAYASHI, M.D., TOSHIKI TAKEMAE, M.D., TSUYOSHI TADA, M.D., AND YUICHIRO TANAKA, M.D. Department of
J Neurosurg 66:500-505, 1987 Aneurysms of the basilar artery trunk KENICHIRO SUGITA, M.D., SHIGEAKI KOBAYASHI, M.D., TOSHIKI TAKEMAE, M.D., TSUYOSHI TADA, M.D., AND YUICHIRO TANAKA, M.D. Department of
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Neurosurgical Techniques
 Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Brain ميهاربا لض اف دمح ا د The Meninges 1- Dura Mater of the Brain endosteal layer does not extend meningeal layer falx cerebri tentorium cerebelli
 .احمد د فاضل ابراهيم Lecture 15 Brain The Meninges Three protective membranes or meninges surround the brain in the skull: the dura mater, the arachnoid mater, and the pia mater 1- Dura Mater of the Brain
.احمد د فاضل ابراهيم Lecture 15 Brain The Meninges Three protective membranes or meninges surround the brain in the skull: the dura mater, the arachnoid mater, and the pia mater 1- Dura Mater of the Brain
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Cerebral revascularization: past, present and future
 Cerebral revascularization: past, present and future Tomás Funes 1 MD, Asis Lorente Muñoz 2 MD, Federico Fernández Molina 3 MD, Paula Ypa 3 MD, Francisco Mannara 4 MD, Luis González Martínez 2 MD, PhD
Cerebral revascularization: past, present and future Tomás Funes 1 MD, Asis Lorente Muñoz 2 MD, Federico Fernández Molina 3 MD, Paula Ypa 3 MD, Francisco Mannara 4 MD, Luis González Martínez 2 MD, PhD
Intrapetrous Internal Carotid Artery
 James C. Andrews, M.D., Neil A. Martin, M.D., Keith Black, M.D., Vincent F Honrubia, M.D., and Donald P Becker, M.D. Midd le Cranial Fossa Transtemporal Approach to the Intrapetrous Internal Carotid Artery
James C. Andrews, M.D., Neil A. Martin, M.D., Keith Black, M.D., Vincent F Honrubia, M.D., and Donald P Becker, M.D. Midd le Cranial Fossa Transtemporal Approach to the Intrapetrous Internal Carotid Artery
Tikrit University College of Dentistry Dr.Ban I.S. head & neck anatomy 2 nd y.
 Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Cranial cavity. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Cranial cavity Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology The Meninges The brain in the skull is surrounded by three membranes or meninges: 1-DURA MATER 2-ARACHNOID MATER 3-PIA MATER
Cranial cavity Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology The Meninges The brain in the skull is surrounded by three membranes or meninges: 1-DURA MATER 2-ARACHNOID MATER 3-PIA MATER
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al.
 ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
Cranial Cavity REFERENCES: OBJECTIVES OSTEOLOGY. Stephen A. Gudas, PT, PhD
 Stephen A. Gudas, PT, PhD Cranial Cavity REFERENCES: Moore and Agur, Essential Clinical Anatomy (ECA), 3rd ed., pp. 496 498; 500 507; 512 514 Grant s Atlas 12 th ed., Figs 7.6; 7.19 7.30. Grant s Dissector
Stephen A. Gudas, PT, PhD Cranial Cavity REFERENCES: Moore and Agur, Essential Clinical Anatomy (ECA), 3rd ed., pp. 496 498; 500 507; 512 514 Grant s Atlas 12 th ed., Figs 7.6; 7.19 7.30. Grant s Dissector
Cranial cavity. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 Cranial cavity Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Cerebrum Cerebral hemispheres The Meninges The brain in the skull is surrounded by three membranes or meninges: 1-THE DURA
Cranial cavity Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Cerebrum Cerebral hemispheres The Meninges The brain in the skull is surrounded by three membranes or meninges: 1-THE DURA
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Endovascular treatment of very large and giant intracranial
 REVIEW ARTICLE W.J. van Rooij M. Sluzewski Endovascular Treatment of Large and Giant Aneurysms SUMMARY: Very large and giant ( 15 mm) cerebral aneurysms have a poor natural history, with high risk of subarachnoid
REVIEW ARTICLE W.J. van Rooij M. Sluzewski Endovascular Treatment of Large and Giant Aneurysms SUMMARY: Very large and giant ( 15 mm) cerebral aneurysms have a poor natural history, with high risk of subarachnoid
Dr.Ban I.S. head & neck anatomy 2 nd y. جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull
جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Dural Arteriovenous Malformations and Fistulae (DAVM S DAVF S)
 Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine:
 Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Neurosurgical decision making in structural lesions causing stroke. Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery)
 Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
NIH Public Access Author Manuscript J Am Coll Radiol. Author manuscript; available in PMC 2013 June 24.
 NIH Public Access Author Manuscript Published in final edited form as: J Am Coll Radiol. 2010 January ; 7(1): 73 76. doi:10.1016/j.jacr.2009.06.015. Cerebral Aneurysms Janet C. Miller, DPhil, Joshua A.
NIH Public Access Author Manuscript Published in final edited form as: J Am Coll Radiol. 2010 January ; 7(1): 73 76. doi:10.1016/j.jacr.2009.06.015. Cerebral Aneurysms Janet C. Miller, DPhil, Joshua A.
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
HEAD/NECK VESSELS. Objectives
 Objectives Arterial Supply to Head and Neck Arteries to Head Surrounding Brain Common carotid arteries Arteries to Head Surrounding Brain External carotid arteries Arteries to Head Surrounding Brain External
Objectives Arterial Supply to Head and Neck Arteries to Head Surrounding Brain Common carotid arteries Arteries to Head Surrounding Brain External carotid arteries Arteries to Head Surrounding Brain External
be very thin and variable. Facial nerve branches that exit the parotid gland are deep to the SMAS.
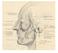 The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports-
 Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
TRANSVERSE SECTION PLANE Scalp 2. Cranium. 13. Superior sagittal sinus
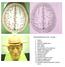 TRANSVERSE SECTION PLANE 1 1. Scalp 2. Cranium 3. Superior sagittal sinus 4. Dura mater 5. Falx cerebri 6. Frontal lobes of the cerebrum 7. Middle meningeal artery 8. Cortex, grey matter 9. Cerebral vessels
TRANSVERSE SECTION PLANE 1 1. Scalp 2. Cranium 3. Superior sagittal sinus 4. Dura mater 5. Falx cerebri 6. Frontal lobes of the cerebrum 7. Middle meningeal artery 8. Cortex, grey matter 9. Cerebral vessels
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Endosaccular aneurysm occlusion with Guglielmi detachable coils for obstructive hydrocephalus caused by a large basilar tip aneurysm Case report
 Neurosurg Focus 7 (4):Article 5, 1999 Endosaccular aneurysm occlusion with Guglielmi detachable coils for obstructive hydrocephalus caused by a large basilar tip aneurysm Case report Akira Watanabe, M.D.,
Neurosurg Focus 7 (4):Article 5, 1999 Endosaccular aneurysm occlusion with Guglielmi detachable coils for obstructive hydrocephalus caused by a large basilar tip aneurysm Case report Akira Watanabe, M.D.,
Surgical treatment of a dissecting aneurysm of the superior cerebellar artery: case report
 Romanian Neurosurgery (2014) XXI 3: 269-273 269 Surgical treatment of a dissecting aneurysm of the superior cerebellar artery: case report Florin Stefanescu 1, Stefanita Dima 2, Mugurel Petrinel Radoi
Romanian Neurosurgery (2014) XXI 3: 269-273 269 Surgical treatment of a dissecting aneurysm of the superior cerebellar artery: case report Florin Stefanescu 1, Stefanita Dima 2, Mugurel Petrinel Radoi
Blood Supply of the CNS
 Blood Supply of the CNS Lecture Objectives Describe the four arteries supplying the CNS. Follow up each artery to its destination. Describe the circle of Willis and its branches. Discuss the principle
Blood Supply of the CNS Lecture Objectives Describe the four arteries supplying the CNS. Follow up each artery to its destination. Describe the circle of Willis and its branches. Discuss the principle
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Quality Metrics. Stroke Related Procedure Outcomes
 Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Ruptured Cerebral Aneurysm of the Anterior Circulation
 Original Articles * Division of Neurosurgery Department of Surgery Ruptured Cerebral Aneurysm of the Anterior Circulation Management and Microsurgical Treatment Ossama Al-Mefty, MD* ABSTRACT Based on the
Original Articles * Division of Neurosurgery Department of Surgery Ruptured Cerebral Aneurysm of the Anterior Circulation Management and Microsurgical Treatment Ossama Al-Mefty, MD* ABSTRACT Based on the
Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach
 J Neurosurg 87:555 585, 1997 Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach HUNG T. WEN, M.D., ALBERT L. RHOTON, JR., M.D., TOSHIRO KATSUTA,
J Neurosurg 87:555 585, 1997 Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach HUNG T. WEN, M.D., ALBERT L. RHOTON, JR., M.D., TOSHIRO KATSUTA,
Veins of the Face and the Neck
 Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Pichayen Duangthongpon MD*, Chaiwit Thanapaisal MD*, Amnat Kitkhuandee MD*, Kowit Chaiciwamongkol MD**, Vilaiwan Morthong MD**
 The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
Anterior communicating artery aneurysm surgery: Determining the most appropriate. head position.
 Anterior communicating artery aneurysm surgery: Determining the most appropriate head position. Mevci Ozdemir, MD a, Ayhan Comert, MD b, Hasan Caglar Ugur, MD, PhD, c, Gokmen Kahilogullari, MD, PhD c,
Anterior communicating artery aneurysm surgery: Determining the most appropriate head position. Mevci Ozdemir, MD a, Ayhan Comert, MD b, Hasan Caglar Ugur, MD, PhD, c, Gokmen Kahilogullari, MD, PhD c,
Chapter XII: Temporal Expanding Processes, Including Those in the Sylvian Fissure and the Insula
 Acta Radiologica ISSN: 0001-6926 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iaro20 Chapter XII: Temporal Expanding Processes, Including Those in the Sylvian Fissure and the Insula
Acta Radiologica ISSN: 0001-6926 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iaro20 Chapter XII: Temporal Expanding Processes, Including Those in the Sylvian Fissure and the Insula
Cerebral aneurysms A case study
 August 2001 Cerebral aneurysms A case study Heather L. Hinds, Harvard Medical School Year III Our Patient 57yr old woman History of migraines Presents with persistent headache several months duration different
August 2001 Cerebral aneurysms A case study Heather L. Hinds, Harvard Medical School Year III Our Patient 57yr old woman History of migraines Presents with persistent headache several months duration different
Anterior Communicating Artery Aneurysms. Surgical approaches Review
 Anterior Communicating Artery Aneurysms. Surgical approaches Review Hirotoshi Sano Dept. of Neurosurgery Fujita Health University Introduction There are two main types of approaches for anterior communicating
Anterior Communicating Artery Aneurysms. Surgical approaches Review Hirotoshi Sano Dept. of Neurosurgery Fujita Health University Introduction There are two main types of approaches for anterior communicating
Skull Base Course. Dissection with fresh temporal bones and half heads
 Skull Base Course Dissection with fresh temporal bones and half heads 711 November 2016 Gruppo Otologico Via Emmanueli 42 Piacenza 29122 t +39 0523 754 362 fax +39 0523 453 708 www.gruppootologico.com
Skull Base Course Dissection with fresh temporal bones and half heads 711 November 2016 Gruppo Otologico Via Emmanueli 42 Piacenza 29122 t +39 0523 754 362 fax +39 0523 453 708 www.gruppootologico.com
Pterional-subolfactory Approach for Treatment of High Positioned Anterior Communicating Artery Aneurysms
 Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2013.15.3.177 Clinical Article Pterional-subolfactory Approach for Treatment of
Journal of Cerebrovascular and Endovascular Neurosurgery ISSN 2234-8565, EISSN 2287-3139, http://dx.doi.org/10.7461/jcen.2013.15.3.177 Clinical Article Pterional-subolfactory Approach for Treatment of
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Overview of imaging modalities for cerebral aneurysms
 Overview of imaging modalities for cerebral aneurysms Soroush Zaghi BIDMC PCE: Radiology August 2008 (Images from BIDMC, PACS.) Our Patient: Presentation Our patient is a 57 y/o woman who reports blowing
Overview of imaging modalities for cerebral aneurysms Soroush Zaghi BIDMC PCE: Radiology August 2008 (Images from BIDMC, PACS.) Our Patient: Presentation Our patient is a 57 y/o woman who reports blowing
Medical Neuroscience Tutorial Notes
 Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Unilateral extended suboccipital approach for a C1 dumbbell schwanoma
 38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Surgical anatomy of the juxtadural ring area
 Surgical anatomy of the juxtadural ring area Susumu Oikawa, M.D., Kazuhiko Kyoshima, M.D., and Shigeaki Kobayashi, M.D. Department of Neurosurgery, Shinshu University School of Medicine, Matsumoto, Japan
Surgical anatomy of the juxtadural ring area Susumu Oikawa, M.D., Kazuhiko Kyoshima, M.D., and Shigeaki Kobayashi, M.D. Department of Neurosurgery, Shinshu University School of Medicine, Matsumoto, Japan
For Emergency Doctors. Dr Suzanne Smallbane November 2011
 For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
Surgical anatomy of the juxta dural ring area
 J Neurosurg 89:250 254, 1998 Surgical anatomy of the juxta dural ring area SUSUMU OIKAWA, M.D., KAZUHIKO KYOSHIMA, M.D., AND SHIGEAKI KOBAYASHI, M.D. Department of Neurosurgery, Shinshu University School
J Neurosurg 89:250 254, 1998 Surgical anatomy of the juxta dural ring area SUSUMU OIKAWA, M.D., KAZUHIKO KYOSHIMA, M.D., AND SHIGEAKI KOBAYASHI, M.D. Department of Neurosurgery, Shinshu University School
Techniques in cerebral aneurysm surgery. Anatomical variation of middle meningeal artery origin ophthalmic artery
 SYⅤ-1 Anatomical variation of middle meningeal artery origin ophthalmic artery Yu Kinoshita, Rokuya Tanikawa, Kosumo Noda, Nakao Ota, Tomomasa Kondo, Takanori Miyazaki, Kiyotaka Toyoda, Syuichi Tanada,
SYⅤ-1 Anatomical variation of middle meningeal artery origin ophthalmic artery Yu Kinoshita, Rokuya Tanikawa, Kosumo Noda, Nakao Ota, Tomomasa Kondo, Takanori Miyazaki, Kiyotaka Toyoda, Syuichi Tanada,
Intraoperative angiography during aneurysm surgery: a prospective evaluation of efficacy
 See the Editorial and the Response in this issue, pp 979 980. J Neurosurg 96:993 999, 2002 Intraoperative angiography during aneurysm surgery: a prospective evaluation of efficacy GORDON TANG, M.D., C.
See the Editorial and the Response in this issue, pp 979 980. J Neurosurg 96:993 999, 2002 Intraoperative angiography during aneurysm surgery: a prospective evaluation of efficacy GORDON TANG, M.D., C.
THIEME. Scalp and Superficial Temporal Region
 CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
3. The Jaw and Related Structures
 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Presented by- Dr. Vivek Tandon
 Presented by- Dr. Vivek Tandon Basic principles of aneurysm surgery Hemostasisof the extradural portion should be meticulous. Hand rests, instrumentholders and self retaining retractors must be checked
Presented by- Dr. Vivek Tandon Basic principles of aneurysm surgery Hemostasisof the extradural portion should be meticulous. Hand rests, instrumentholders and self retaining retractors must be checked
Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique
 Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique Michael Horowitz M.D. Pittsburgh, Pennsylvania Background Iatrogenic intraprocedural rupture rates
Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique Michael Horowitz M.D. Pittsburgh, Pennsylvania Background Iatrogenic intraprocedural rupture rates
Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft
 J Neurosurg 58~25-429, 1983 Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft Case report RYOJI ISHII, M.D., TETSUO KOIKE, M.D.,
J Neurosurg 58~25-429, 1983 Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft Case report RYOJI ISHII, M.D., TETSUO KOIKE, M.D.,
Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge Procedure Using the Coil Mass as a Support
 Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
The orbitozygomatic approach achieves better
 OPERATIVE NUANCES THE ORBITOZYGOMATIC APPROACH Wouter Ralph van Furth, M.D., Ph.D. Department of Neurosurgery, Academic Medical Center, University of Amsterdam, Amsterdam, The Netherlands Anne Maria R.
OPERATIVE NUANCES THE ORBITOZYGOMATIC APPROACH Wouter Ralph van Furth, M.D., Ph.D. Department of Neurosurgery, Academic Medical Center, University of Amsterdam, Amsterdam, The Netherlands Anne Maria R.
Effect of early operation for ruptured aneurysms on prevention of delayed ischemic symptoms
 J Neurosurg 57:622-628, 1982 Effect of early operation for ruptured aneurysms on prevention of delayed ischemic symptoms MAMORU TANEDA, M.D. Department of Neurosurgery, Hanwa Memorial Hospital, Osaka,
J Neurosurg 57:622-628, 1982 Effect of early operation for ruptured aneurysms on prevention of delayed ischemic symptoms MAMORU TANEDA, M.D. Department of Neurosurgery, Hanwa Memorial Hospital, Osaka,
