HHS Public Access Author manuscript World Neurosurg. Author manuscript; available in PMC 2015 December 30.
|
|
|
- Maximilian Robinson
- 5 years ago
- Views:
Transcription
1 The Transconjunctival Transorbital Approach: A Keyhole Approach to the Midline Anterior Skull Base Shaan M. Raza 1, Alfredo Quinones-Hinojosa 1, Michael Lim 1, and Kofi D. Owusu Boahene 2 1 Department of Neurosurgery, The Johns Hopkins Neuro-Oncology Surgical Outcomes Research Laboratory, The Johns Hopkins University School of Medicine, Baltimore, Maryland, USA 2 Department of Otolaryngology, The Johns Hopkins Neuro-Oncology Surgical Outcomes Research Laboratory, The Johns Hopkins University School of Medicine, Baltimore, Maryland, USA Abstract OBJECTIVE To report an initial experience with a medial transorbital approach to the midline skull base performed via a transconjunctival incision. METHODS The authors retrospectively reviewed their clinical experience with this approach in the management of benign cranial base pathology. Preoperative imaging, intraoperative records, hospitalization charts, and postoperative records were reviewed for relevant data. RESULTS During the period , six patients underwent a transconjunctival craniotomy performed by a neurosurgeon and otolaryngologist head and neck surgeon working together. The indications for surgery were esthesioneuroblastoma in one patient, juvenile angiofibroma in one patient, Paget disease in one patient, and recalcitrant cerebrospinal fluid leaks in three patients. Three patients had prior cranial base surgery (either open craniotomy or an endonasal approach) done at another institution. The mean length of stay was 3.8 days; mean follow-up was 6 months. Surgery was considered successful in all cases (negative margins or no leak recurrence); diplopia was noted in one patient postoperatively. CONCLUSIONS The transconjunctival medial orbital craniectomy provides a minimally invasive keyhole approach to lesions located anteriorly along the anterior cranial fossa that are in the midline with lateral extension over the orbital roof. Based on our initial experience with this technique, the working space afforded limits complex surgical dissection; this approach is primarily well suited for less extensive pathology. Keywords HHS Public Access Author manuscript Published in final edited form as: World Neurosurg December ; 80(6): doi: /j.wneu Anterior cranial fossa; Keyhole craniotomy; Transconjunctival; Transorbital To whom correspondence should be addressed: Kofi D. Owusu Boahene, M.D., [dboahene1@jhmi.edu]. Conflict of interest statement: The authors declare that the article content was composed in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
2 Raza et al. Page 2 INTRODUCTION METHODS Numerous craniofacial approaches have been developed to address the anatomic challenges of approaching the anterior skull base (5, 19, 20, 24, 26). Anatomically, there are multiple osseous compartments (e.g., frontal sinus, the orbits) that can limit direct access to the anterior cranial fossa. These compartments must also be visualized to resect pathology extending into these regions from the anterior cranial fossa. These different approaches (i.e., frontotemporal sphenoidal craniotomy, extended bifrontal craniotomy, transfacial approaches) provide advantages and corridors appropriate for selected lesions (19, 20, 24, 26). Characteristics that influence the type of approach include the malignant potential of the lesion, lesion epicenter, goals of surgery (negative margins, en bloc resection, neural decompression), and involvement of the paranasal sinuses and surrounding compartments. These traditional craniofacial approaches are associated with risks, and although they are tolerated for the resection of malignant pathology, they may not be considered acceptable for benign pathology (i.e., CSF leaks, meningiomas) or malignant disease with less extensive anatomic involvement. In an effort to minimize these risks for such lesions, minimally invasive approaches, such as endonasal endoscopy and keyhole craniotomies, are now increasingly used (18, 20, 21). Although endonasal approaches have reduced the morbidity of accessing pathology in the nasal cavity, they have limitations in dealing with the anterior skull base, including the inability to perform microsurgical dissection with complex lesions, adequate dural closure, access to the anterior cranial fossa laterally over the orbits away from the midline, and limited working space when multiple surgeons are working (23). Supraorbital craniotomy with an orbital ridge osteotomy has been described through various incisions (supraciliary, transciliary, and transpalpebral) to the anterior cranial fossa, suprasellar region, and inter-peduncular cistern (3, 8, 9, 18, 20, 21, 22). However, these approaches are restricted by their anterolateral trajectory to the midline anterior skull base; the angulation of the orbital roof can be variable restricting access to the cribriform plate region. The transconjunctival incision, first described by Bourguet in 1924 (2) for cosmetic surgery, could provide an alternative, direct route to selected lesions in the anterior cranial fossa, while avoiding risks with traditional craniofacial approaches and circumventing obstacles with currently available keyhole craniotomies. Currently used for intraorbital lesions and orbital fractures (14, 15), an incision made in the conjunctiva could provide not only direct access to the orbital ridge but also a more medially based trajectory to the cribriform plate region and laterally over the orbits. In addition, the transconjunctival approach can be supplemented with endonasal endoscopy to permit improved access to lesions in the anterior cranial fossa also involving the paranasal sinuses. We present our initial experience with the transconjunctival approach in the management of anterior cranial base pathology. We describe our technique for transconjunctival medial orbital craniectomy for accessing the anterior cranial fossa. Depending on lesion location, an endonasal approach can be combined with the transconjunctival craniectomy. For the clinical portion of this study, all
3 Raza et al. Page 3 Surgical Technique patients treated via a transconjunctival craniectomy during the period at The Johns Hopkins Medical Institutions were included in the cohort study. Approval was obtained from The Johns Hopkins Institutional Review Board for this study. All patient charts, medical records, imaging, and clinical notes were reviewed retrospectively for pertinent surgical and study variables (target lesion location, reconstructive method, surgical outcome, complications, length of hospital stay, and follow-up). In addition to standard magnetic resonance imaging for navigation, all patients undergo preoperative computed tomography (CT) to delineate the bony structures of the paranasal sinuses in relation to the anterior cranial fossa in addition to the extent of the frontal sinus. After anesthesia induction, patients are positioned in a Mayfield head holder with the head slightly extended and rotated such that the surgeon is working directly perpendicular to the floor. A corneal shield is placed, and then the face and nose are prepared in a standard and sterile fashion. The conjunctiva, upper eyelid, and medial canthal region are infiltrated with anesthetic; the lacrimal glands are subsequently protected with small probes. An incision is made in the conjunctiva in front of the caruncle and extended superiorly and inferiorly into the upper and lower palpebral conjunctivae avoiding the lacrimal system (Figure 1A). Lacrimal probes placed in the lacrimal canaliculi aid in avoiding injury of the lacrimal canaliculi. After incision, the plane of dissection remains in the loose areolar tissue deep to the medial canthal tendon. The medial orbital wall and supraorbital roof are exposed in a subperiosteal plane back to the orbital apex. In the process of visualizing the lamina papyracea, the anterior and posterior ethmoidal arteries are identified and ligated to aid with further exposure by allowing the orbital contents to fall away laterally; identification of the ethmoidal arteries further serves as a landmark for the anterior cranial fossa floor and the subsequent craniectomy (Figure 1B). An additional osseous landmark that can be used is the frontoethmoidal suture, which lies in the same plane as the ethmoidal arteries and the optic canal (4). If necessary to expand lateral and posterior exposure along the orbital roof, the trochlea can be subperiosteally dissected and detached to increase bony exposure; however, as experienced in one patient, this can be associated with postoperative dysfunction of the superior oblique muscle. After this soft tissue dissection, a minicraniectomy along the superomedial aspect of the orbit is created to expose the polar and basal dura of the anterior cranial fossa (Figure 1C). The navigation probe is used to outline the location and size of the orbital window needed to create an adequate corridor to the target lesion or defect in addition to ensuring the craniotomy is located appropriately in relation to the floor of the anterior skull base. The frontoethmoidal suture and the associated ethmoidal arteries help determine the superior-inferior aspects of the opening. Placement of the craniotomy above these structures gains access to the anterior cranial fossa and intracranial space, whereas opening below these structures creates exposure into the nasal cavity and posteriorly toward the sphenoid sinus and sella. Figure 2 shows the overall relationship of the conjunctival incision and craniectomy in relation to the anterior skull base and ethmoid sinus. At this point, the remainder of the surgery is performed according to the pathology of interest; for the intracranial portion of the surgery, either microscopic or endoscopic illumination can be used for visualization (Figure 3). If necessary, concurrently, an endonasal endoscopic
4 Raza et al. Page 4 RESULTS Clinical Analysis approach can be performed to resect any portion of a lesion extending into the nasal cavity and paranasal sinuses. For closure and dural reconstruction, any dural incisions can be closed primarily with direct sutures. If necessary for reinforcement of smaller defects along the anterior skull base, a fascia lata graft can be placed through the minicraniectomy; concurrent endoscopic endonasal visualization is used to confirm if an entire defect is covered. For larger defects, a pericranial graft harvested endoscopically can be transposed through the orbital window and placed along the floor of the anterior cranial fossa (13). As previously described, this is done by separating the pericranium from the scalp and skull via two I-inch posttrichial incisions. Once the scalp is released posteriorly, an endoscopic brow elevator set where the endoscope is introduced via the transconjunctival incision to dissect the flap in a posterior-to-anterior fashion. A pericranial flap ultimately is created with a supraorbital neurovascular pedicle. After any such reconstruction, a lumbar drain is left in place postoperatively for hours depending on the underlying pathologic lesion or the size of the defect. After the dura is closed, the incision is closed with loosely approximated absorbable sutures. Six minicraniotomies via a transconjunctival approach were performed on three male and three female patients ranging in age from years (Table 1). Two patients underwent surgery for an oncologic process (juvenile angiofibroma, esthesioneuroblastoma); there was intracranial involvement in both patients and evidence of additional dural disease in the patient with esthesioneuroblastoma. The patient undergoing resection of a juvenile angiofibroma had disease involvement of the pterygomaxillary fossa in addition to the maxillary sinus, ethmoid sinus, orbits, and extension up to the epidural space of the anterior cranial fossa. Three patients underwent surgery for the repair of a CSF leak. All three patients who underwent repair for fistulas had prior surgery at other centers transsphenoidal and bifrontal craniotomy and the fistulas were a result of defects over the fovea ethmoidalis or planum sphenoidale. The remaining patient presented with diplopia and retroorbital pain and had a lesion along the medial orbital roof; surgery, done for biopsy and resection, led to the diagnosis of Paget disease. In all patients, surgery was considered successful (either gross total resection with negative margins or obliteration of the CSF fistula without recurrence) with no orbital, local soft tissue or wound healing, or neurologic complications noted. The mean length of hospital stay was 4 days. In patients requiring dural reconstruction along the floor of the anterior fossa, this was done with a fascia lata graft, followed by hours of postoperative lumbar drainage. The mean length of follow-up in the cohort was 6 months. Follow-up consisted of documented neurologic and ophthalmologic examinations (including extraocular movements) and cosmetic assessment (including ocular examination). One patient experienced postoperative diplopia lasting approximately 8 weeks; in this patient, the trochlea was intentionally detached during surgery to expand the lateral extent of the
5 Raza et al. Page 5 exposure. Otherwise, no other neurologic or wound healing complications were noted. Surgery was considered successful in all patients with either gross total resection and negative margins (for patients with tumors) or no CSF leak recurrence at last follow-up. Case Illustration: Esthesioneuroblastoma (Patient 2) A 55-year-old man presented with epistaxis to an outside institution, where work-up showed a midline intranasal mass with erosion of the cribriform plate and dural enhancement extending from the midline to approximately 5 mm laterally over the orbit from the intersection of cribriform plate and orbit (Figure 4A and B). The patient underwent a transnasal biopsy before presentation to our institution; the mass was determined to be an esthesioneuroblastoma (Kadish stage C). In light of negative lymph node involvement or distant metastases (based on positron emission tomography imaging), the patient was taken to surgery for resection. With regard to operative planning, most of the tumor was thought to be within the midline nasal cavity eroding the cribriform plate and involved the dura in the midline with extension laterally over the fovea ethmoidalis and left orbital roof. The endonasal approach was employed to access the midline and the lateral extent of the ethmoid sinus, and the transconjunctival approach was used to obtain negative margins from the dura along the lateral extent of the disease over the orbit (Figure 4C). After intraoperative exposure, it was thought that a pure endonasal approach would not provide adequate access to the disease dura laterally over the orbital roof. No intraoperative complications were encountered, and negative margins were obtained (Figure 4D). The patient was discharged to home on postoperative day 2. Case Illustration: CSF Fistula Repair (Patient 5) A 62-year-old woman presented to us with a history of sinus surgery approximately 5 years prior. Consequent to the surgery, the patient developed a CSF leak with recurrent episodes of meningitis for which she underwent an attempt at a transnasal repair at another institution. On presentation to our institution, she underwent CT cisternography, which showed a leak into her right ethmoid sinus; a maxillofacial CT scan (Figure 5A and B) showed a small defect in her fovea ethmoidalis. The surgical options for this patient included a pure endonasal endoscopic repair of the leak with a wide ethmoidectomy on the right side and placement of a graft or a right-sided transconjunctival approach with placement of a free graft (i.e., fascia lata). Although we thought that a pure endonasal approach would be successful, in light of the patient s prior nasal surgery, there was concern that a healthy nasoseptal flap could not be harvested. A transconjunctival approach was ultimately selected because it was thought that minimal bone work (i.e., ethmoidectomy) would be needed to repair the defect. The rationale was that an approach from above the defect would not involve removing the anterior cranial fossa floor a buttress necessary for graft placement; expansion of this defect would have been necessary to place a graft endonasally. The patient was taken to surgery for a right-sided transconjunctival craniectomy (Figure 5C) for placement of a fascia lata graft. Intraoperatively, she also underwent lumbar drain placement; visualization via endonasal endoscopy with fluorescein injection confirmed successful repair of the CSF leak. The lumbar drain remained in place for temporary CSF
6 Raza et al. Page 6 DISCUSSION diversion for 24 hours and was then removed. The patient was discharged home on postoperative day 3 with no issues. Recognizing that the approach should match the pathology of the lesion and the goals of surgery, minimally invasive approaches have been developed to minimize morbidity associated with the surgical approach. Interest has increased in minimally invasive approaches (open and endoscopic) to pathology in the anterior cranial fossa. Transorbital approaches as a means for emergency access to the ventricle have been described (25). The concept of the orbit as a natural corridor to the anterior cranial fossa has been described in the neurosurgical literature; the transpalpebral approach has been reported in the management of anterior circulation aneurysms and benign neoplasms in the anterior skull base and suprasellar regions (1, 3, 18). Such approaches provide adequate access for appropriately selected lesions and provide a direct trajectory to the superolateral orbital ridge. In an effort to provide a cosmetically hidden incision, the transconjunctival approach is a natural progression of the spectrum of transorbital approaches. The transconjunctival approach to the orbit was described more than a century ago by Bourguet for the aesthetic repair of eyelid defects (2). Over subsequent decades, numerous reports in the literature have described this incision in the treatment of intraorbital tumors, orbital malformations, and orbital fractures. Via the lower eyelid, this approach provides the soft tissue access necessary for a maxillectomy (6). Several studies have compared complications between subciliary incisions in the eyelid and the transconjunctival approach and found a significantly higher rate of eyelid-related complications with transcutaneous incisions. The differences are sometimes striking with one review detailing a 40% rate of eyelid retraction for subciliary incisions compared with only 3% for transconjunctival incisions (7, 10 12). Recognizing these relative advantages, the transconjunctival incision could logically be applied to neurosurgical approaches to the anterior cranial fossa. Moe et al. (14, 16) reported their initial experience with transorbital neuroendoscopic approaches for accessing laterally placed anterior skull base lesions; in their experience, they applied this technique to the management of CSF leaks, optic nerve decompression, cranial base fractures, and skull base tumors. In addition to extradural pathology, we have applied this technique to management of selected anterior cranial fossa pathology. In light of previously published articles that introduced the concept of this approach, we also explored its role in the treatment of various intradural and extradural pathology. Anatomic Considerations Compared with the transciliary incision and traditional unilateral approaches, such as the pterional craniotomy, the dissection plane of the transconjunctival incision eliminates the risk of injuring the facial nerve branches by eliminating the need for temporalis dissection and avoiding dissection of the brow elevators. In addition, when combined with appropriate osteotomies, this approach preserves sensation of the forehead, while still allowing removal of bone anteriorly along the orbital roof.
7 Raza et al. Page 7 Anatomically, this approach combines advantages of traditional midline techniques, anterolaterally based keyhole approaches, and transnasal endoscopic techniques in a minimally invasive manner. The more medial nature of the craniotomy as opposed to other keyhole approaches permits a more direct route to the cribriform plate region. Although traditional keyhole craniotomies provide a subfrontal trajectory, visualization of the midline skull base is hindered as a result of the anterolateral location of the craniotomy and the angulation of the orbital roof. In pathologic lesions that derive their vascular supply from the skull base, this access is crucial in safe resection of the pathologic lesion. This near-midline trajectory is provided without the risk of venous injury owing to exposure of the superior sagittal sinus needed with bifrontal craniotomies or retraction injury on the frontal lobe noted with unilateral approaches. All risks, although acceptable for malignant pathology or complicated benign pathology, should be avoided for benign processes such as encephaloceles and CSF leaks. The other advantage of this technique compared with midline approaches is the trajectory afforded in relation to the olfactory apparatus. Because the access to the cribriform plate is gained intraorbitally (as opposed to intranasally), the olfactory epithelium in the nasal mucosa is not disrupted; access to the posterior aspect of the cribriform plate and planum sphenoidale can be gained by working posteriorly to the olfactory bulbs. Another anatomic consideration of this approach deals with the issue of detaching the trochlear pulley. Detaching this structure primarily provides additional exposure posterior-lateral to this structure; for lesions anterior to this structure, detachment and the risk of postoperative (transient) diplopia is unnecessary. This approach also overcomes limitations seen with pure endoscopic approaches to the anterior skull base. Endonasal (including transethmoidal variants) approaches are limited in their access to parts of the anterior cranial fossa floor lateral to the cribriform plate overlying the orbits; accessing these regions endoscopically requires traversing neurovascular structures, which breaks a fundamental tenet of skull base surgery. In addition, for more anteriorly located lesions, transnasal endoscopy may become limited by difficult working angles. In contrast, a transconjunctival approach provides access to the lateral anterior skull base restricted in access by endonasal endoscopic approaches. Surgical Considerations and Indications The approach described combines the beneficial aspects of traditional open approaches and endonasal endoscopic approaches in a minimally invasive fashion. As with traditional craniotomies, microsurgical technique under the microscope for neoplastic processes is possible; however, the working space is limited compared with more conventional open approaches. This trajectory also allows for direct watertight dural repair by suturing and reinforcement with pedicled pericranial flaps or free fascia lata grafts. Although bimanual instrumentation working under the microscope is possible, the endoscope can also be used as an adjunct to improve visualization further in the lateral and superior directions. Based on our preliminary experience, when used alone, this technique is suited for anatomically straightforward lesions located along the paramedian skull base. Although this technique provides direct access to an elusive region of the anterior skull base (between the cribriform plate and the orbital roof up to the midpupillary line), it does not provide working
8 Raza et al. Page 8 space for the management of complex lesions (i.e., anterior cranial fossa meningiomas or malignancies with intraparenchymal extension). It is well suited for less complicated pathology (i.e., encephaloceles and CSF fistulas) where there is only a small cranial base defect that can be managed with a free or pedicled flap. When paired with endonasal endoscopy, the transconjunctival transorbital approach can also provide a combined approach to any anterior skull base pathology, while avoiding the use of visible facial incisions and large scalp flaps. This concept was also demonstrated by Ciporen et al. (4). For neoplastic processes, a combined transorbital-endonasal technique not only allows for two surgeons to work synchronously but also facilitates dissection of any tumor extending out of the anterior cranial fossa into the nasal cavity and paranasal sinuses (14). Although endoscopic approaches have been shown to be effective for low-grade and intermediate-grade malignancies restricted to the nasal cavity, they have been limited in their efficacy in the management of disease extending intracranially. This limitation is likely a consequence of the inability to perform extensive intracranial dissection with endoscopic approaches. This ability is critical when the goal of surgical resection is to obtain negative margins and achieve good dural coverage. A transconjunctival approach could be employed for malignancies eroding through the cribriform plate but not having extending dural or intraparenchymal involvement, as shown by the case illustration presented earlier. Although we have attempted to use this technique for malignant pathology, we recognize that this approach would be unsuitable for anatomically extensive malignancies. This approach ultimately does not provide the wide anatomic access that is often necessary to obtain negative margins and good reconstruction of larger skull base defects. The management of CSF leaks and similar pathologies such as meningoencephaloceles could also benefit from combined transorbital-endonasal techniques. Endonasal techniques face difficulties when managing extensive skull base defects of the anterior fossa floor. The primary challenges of repairing such leaks are due to the need for a large underlay graft that sits intracranially-extradurally or sometimes intradurally and the need for a vascularized flap to prevent recurrence after such large repairs, particularly after adjuvant radiation. The use of this approach combined with endonasal techniques further avoids the need to open prior scar tissue in situations involving repair of postoperative CSF leaks (whether from a craniotomy or an expanded endonasal approach). Via the transconjunctival transorbital approach, a pedicled pericranial graft can be harvested and placed along the floor of the anterior cranial fossa through the same incision (13, 17, 27). Endoscopy can be used concurrently to ensure that the graft adequately covers the entire defect and to mobilize a nasoseptal flap to buttress the graft from below. This technique not only could be employed for CSF leaks but also meningoencephaloceles. An additional consideration is the use of this techniques after a prior surgery (either open or endoscopic-endonasal) has been performed. The primary issue is that in these patients the standard dural closure techniques have already been used and exhausted the pericranial flap in prior open cases and the Haddad nasoseptal flap in prior endoscopic approaches. With reoperation in these areas, the goal is not to disrupt the vascular supply and the integrity for the prior flaps while attaining the goal of the surgery (repair of the CSF fistula was the most common indication in the reoperation cases). Avoiding vascular supply to the
9 Raza et al. Page 9 prior pedicled flap is primarily one of the reasons we employ the transconjunctival approach when possible. There is a theoretical risk of devascularizing any viable component of the prior flap when the same approach is employed as before for a delayed CSF fistula repair. Instead of removing the entire flap to repair a small defect, we believe that using a different approach (i.e., transconjunctival) provides another trajectory to the lesion without going through prior tissue planes. The other issue in these situations is with regard to the closure. Because the first-line pedicled flap options have already been employed, free grafts (e.g., fascia lata) are then used; this may be acceptable for smaller defects, but nonpedicled flaps pose the risk of failure for larger defects. Limitations and Orbital Complications A relative limitation of the use of the transconjunctival incision for minicraniotomies is entry into the frontal sinus in a fraction of patients with the associated consequences of mucocele formation. Although not encountered in our relatively early experience with this technique, the size and posterior extent of the frontal sinus should be considered preoperatively when selecting the operative approach. To minimize this risk, the use of neuronavigation is essential in positioning the orbitotomy posterior to the frontal sinus. Occasionally, violation of the ethmoid sinuses may occur resulting in communication of the sinuses with the orbital cavity and the intracranial cavity. Purposefully opening the ethmoid sinuses may be desirable with this approach to expose sinonasal pathology. Otherwise, undesired violation of the ethmoid sinuses can be addressed by placing a fascia barrier or a formal ethmoidectomy to minimize future ethmoid sinusitis. Several theoretical orbital complications are associated with the transconjunctival incision that must be highlighted. Injury to the lacrimal system is the major complication inherent to the location and placement of the pericaruncular conjunctival incision. Lacrimal canaliculi injury results in varying degrees of epiphora the may need subsequent intervention. Familiarity with the delicate anatomy around the lacrimal crest is essential in avoiding lacrimal injury. Placing lacrimal probes also aids in avoiding canaliculi injury. Precaruncular versus postcaruncular placement of the transconjunctival incision is a matter of familiarity and can be used to minimize further risk to the canaliculi. Traction on the orbital contents over a prolonged period increases intraorbital pressure and can be detrimental. We have used the Greenberg retractor in our experience alternating approximately 10 to 15 minutes of retraction with relaxation; this can be cumbersome and disrupt the flow of longer cases. Orbital traction should be minimized and the retractor released periodically. Working along the medial quadrant of the orbit theoretically puts the medial rectus at risk. Injury to the medial rectus is most likely to occur during the initial drilling and is best avoided by protecting the periorbita with a malleable retractor. The primary orbital complication noted in our series was superior oblique dysfunction as a result of intentional trochlea detachment to expand the lateral extent of the exposure. Trochlear detachment with craniofacial approaches has been reported and employed with more extensive transbasal approaches where extensive orbital osteotomies are included. When this technique is employed, the trochlea must be detached in a subperiosteal fashion to ensure that it reattaches properly in a delayed fashion. Although the diplopia experienced
10 Raza et al. Page 10 CONCLUSIONS postoperatively in one patient of our cohort eventually resolved, since then we have avoided performing this maneuver. The concept of minimally invasive neurosurgery does not simply refer to the incision or soft tissue dissection performed but ultimately the collateral damage created by neural manipulation and vascular sacrifice and whether or not the goals of surgery (i.e., negative margins for a sinonasal malignancy) have been effectively achieved. Ultimately, these considerations are important in deciding whether or not an open or endoscopic surgical approach should be performed and whether or not tailored craniotomies (as the one described in this article) are employed. The transconjunctival transorbital craniectomy provides a keyhole approach to the anterior cranial fossa and is well suited primarily for lesions located anteriorly along the cranial fossa floor that involve the midline and extend laterally over the orbits. The working space of this technique facilitates either endoscopic or microsurgical dissection but limits the complexity of dissection that can be performed. We believe this is most appropriately suited for benign pathologies (i.e., encephaloceles, CSF leaks) or less extensive oncologic processes. Although no major complications were encountered in our initial experience, theoretical risks primarily include orbital complications (i.e., orbital hematoma, extraocular muscle dysfunction). Lastly, this technique can be combined with endonasal approaches to provide multiple trajectories of access to the anterior cranial fossa floor, nasal cavity, and surrounding anatomic compartments. Ultimately, application of this technique to larger case series with careful scrutiny of oncologic, orbital, neurologic, and quality-of life-outcomes will provide a better understanding of the true utility of this approach. Abbreviations and Acronyms CSF CT References Cerebrospinal fluid Computed tomography 1. Boaehene K, Lim M, Chu E, Quinones-Hinojosa A. Transpalpebral orbitofrontal craniotomy: a minimally invasive approach to anterior cranial vault lesions. Skull Base. 2010; 20: [PubMed: ] 2. Bourguet J. Surgical treatment of orbital fat herniation [in French]. Bull Acad Med Paris. 1924; 92: Chu EA, Quinones-Hinojosa A, Boahene KD. Trans-blepharoplasty orbitofrontal craniotomy for repair of lateral and posterior frontal sinus cerebrospinal fluid leak. Otolaryngol Head Neck Surg. 2010; 142: [PubMed: ] 4. Ciporen JN, Moe KS, Ramanathan D, Lopez S, Ledesma E, Rostomily R, Sekhar LN. Multiportal endoscopic approaches to the central skull base: a cadaveric study. World Neurosurg. 2010; 73: [PubMed: ] 5. Feiz-Erfan I, Spetzler RF, Horn EM, Porter RW, Beals SP, Lettieri SC, Joganic EF, Demonte F. Proposed classification for the transbasal approach and its modifications. Skull Base. 2008; 18: [PubMed: ]
11 Raza et al. Page Goyal A, Tyagi I, Jain S, Syal R, Singh AP, Kapila R. Transconjunctival incision for total maxillectomy an alternative for subciliary incision. Br J Oral Maxillofac Surg. 2011; 49: [PubMed: ] 7. Habal MB. Transconjunctival approach to the orbit. J Craniofac Surg. 2009; 20:1416. [PubMed: ] 8. Jallo GI. Eyebrow surgery. J Neurosurg Pediatr. 2008; 1:144. [author reply 144]. [PubMed: ] 9. Jallo GI, Bognar L. Eyebrow surgery: the supraciliary craniotomy: technical note. Neurosurgery. 2006; 59(1 Suppl 1) ONSE157-ONSE158 [discussion ONSE ]. 10. Kung DS, Kaban LB. Supratarsal fold incision for approach to the superior lateral orbit. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1996; 81: [PubMed: ] 11. Lane CM. Cosmetic orbital surgery. Eye. 2006; 20: [PubMed: ] 12. Langsdon PR, Rohman GT, Hixson R, Stumpe MR, Metzinger SE. Upper lid transconjunctival versus transcutaneous approach for fracture repair of the lateral orbital rim. Ann Plast Surg. 2010; 65: [PubMed: ] 13. Melvin, T.; Quinones-Hinojosa, A.; Lim, M.; Stewart, C.; Boahene, K. Endoscopic harvest and transposition of vascularized pericranial flap for minimal access open and endoscopic skull base repair: technical notes and case illustration. Presented at North American Skull Base Society Annual Meeting; Scottsdale, AZ. February 18, 2010; 14. Moe KS, Bergeron CM, Ellenbogen RG. Transorbital neuroendoscopic surgery. Neurosurgery. 2010; 67(3 Suppl Operative):ons16 ons28. [PubMed: ] 15. Moe KS, Kim LJ, Bergeron CM. Transorbital endoscopic repair of cerebrospinal fluid leaks. Laryngoscope. 2011; 121: [PubMed: ] 16. Moe KS, Kim LJ, Bergeron CM. Transorbital endoscopic repair of cerebrospinal fluid leaks. The Laryngoscope. 2011; 121: [PubMed: ] 17. Patel MR, Shah RN, Snyderman CH, Carrau RL, Germanwala AV, Kassam AB, Zanation AM. Pericranial flap for endoscopic anterior skull-base reconstruction: clinical outcomes and radioanatomic analysis of preoperative planning. Neurosurgery. 2010; 66: [discussion 512]. [PubMed: ] 18. Raza SM, Boahene KD, Quinones-Hinojosa A. The transpalpebral incision: its use in keyhole approaches to cranial base brain tumors. Expert Rev Neurother. 2010; 10: [PubMed: ] 19. Raza SM, Conway JE, Li KW, Attenello F, Boahene K, Subramanian P, Quinones-Hinojosa A. A modified frontal-nasal-orbital approach to midline lesions of the anterior cranial fossa and skull base: technical note with case illustrations. Neurosurg Rev. 2010; 33: [PubMed: ] 20. Raza SM, Garzon-Muvdi T, Boaehene K, Olivi A, Gallia G, Lim M, Subramanian P, Quinones- Hinojosa A. The supraorbital craniotomy for access to the skull base and intraaxial lesions: a technique in evolution. Minim Invasive Neurosurg. 2010; 53:1 8. [PubMed: ] 21. Reisch R, Perneczky A. Ten-year experience with the supraorbital subfrontal approach through an eyebrow skin incision. Neurosurgery. 2005; 57(4 Suppl): [discussion ]. [PubMed: ] 22. Sanchez-Vazquez MA, Barrera-Calatayud P, Mejia-Villela M, Palma-Silva JF, Juan-Carachure I, Gomez-Aguilar JM, Sanchez-Herrera F. Transciliary subfrontal craniotomy for anterior skull base lesions: technical note. J Neurosurg. 1999; 91: [PubMed: ] 23. Snyderman CH, Carrau RL, Kassam AB, Zanation A, Prevedello D, Gardner P, Mintz A. Endoscopic skull base surgery: principles of endonasal oncological surgery. J Surg Oncol. 2008; 97: [PubMed: ] 24. Solero CL, DiMeco F, Sampath P, Mattavelli F, Pizzi N, Salvatori P, Cantu G. Combined anterior craniofacial resection for tumors involving the cribriform plate: early postoperative complications and technical considerations. Neurosurgery. 2000; 47(6): [discussion ]. [PubMed: ] 25. Tubbs RS, Loukas M, Shoja MM, Cohen-Gadol AA. Emergency transorbital ventricular puncture: refinement of external landmarks. J Neurosurg. 2009; 111: [PubMed: ]
12 Raza et al. Page Zabramski JM, Kiris T, Sankhla SK, Cabiol J, Spetzler RF. Orbitozygomatic craniotomy: technical note. J Neurosurg. 1998; 89: [PubMed: ] 27. Zanation AM, Snyderman CH, Carrau RL, Kassam AB, Gardner PA, Prevedello DM. Minimally invasive endoscopic pericranial flap: a new method for endonasal skull base reconstruction. Laryngoscope. 2009; 119: [PubMed: ]
13 Raza et al. Page 13 Figure 1. Demonstration of initial soft tissue dissection for transconjunctival craniectomy done in the left orbit. The red marking notes the location of the nose in all images. (The images are a combination of actual patient surgery and cadaver dissection.) (A) Initial conjunctival incision in the left orbit. (B) Subperiosteal dissection and exposure of the superior and medial orbital walls. (C) After verification of the anterior cranial fossa floor with neuronavigation and identification of the ethmoidal arteries, a craniectomy is performed with combined drilling and rongeur. (D) Exposure of basal frontal lobe dura after bony removal.
14 Raza et al. Page 14 Figure 2. Illustration showing the relationship of incision and craniectomy in relation to key anatomic landmarks.
15 Raza et al. Page 15 Figure 3. Demonstration of craniectomy in relation to the anterior skull and potential range of exposure. (A) Sagittal section shows how this approach can provide access to the anterior cranial fossa, orbital contents, and ethmoid sinus. In addition, the use of an endoscope expands intracranial visualization further. (B) Superiorly based view shows the extent of bony removal along the anterior cranial fossa floor in relation to the cribriform plate medially and optic nerve posteriorly.
16 Raza et al. Page 16 Figure 4. Case illustration. Kadish C esthesioneuroblastoma resected via a combined left-sided transconjunctival-endonasal approach. (A) Coronal computed tomography images show a primarily midline intranasal mass with erosion through the cribriform plate and slight lateral extension over the orbital roof. (B) Intraoperative image shows the setup for a combined approach; a left-sided transconjunctival craniectomy has already been performed, and a selfretaining retraction has been placed gently on the orbital contents. (C) Endoscopic image obtained endonasally shows a two-surgeon, four-handed technique where one surgeon is operating via s transconjunctival incision (upper right hand), and the primary surgeon is
17 Raza et al. Page 17 operating endonasally. The solid line marks the nasal septum; A is the anterior aspect of the skull base visualized, and P is the posterior extent of the skull base visualized. The dashed line indicates the interface between the diseased dura (anteriorly) and normal cribriform plate (posteriorly). (D) Postoperative axial computed tomography image shows the extent of the bony defect created via the transconjunctival approach to provide lateral access.
18 Raza et al. Page 18 Figure 5. Case illustration. Cerebrospinal fluid fistula resulting from a bony defect over the fovea ethmoidalis that is recalcitrant despite a prior attempt at endonasal repair. (A) Coronal computed tomography (CT) image shows the defect located slightly paramedian over the right ethmoid sinus. (B) Sagittal CT image shows the location of the defect in the anteroposterior axis. (C) Postoperative coronal CT scan shows the orbital window created via the transconjunctival approach to repair the defect with a fascia lata graft.
19 Raza et al. Page 19 Table 1 Overview of Patients Treated via the Transconjunctival Approach Length of Hospital Stay (days) Patient Age/Sex Adjunct Surgical Approach Lesion Lesion Location Lumbar Drain? Reconstruction Surgical Outcome 1 11/M Midfacial degloving Juvenile angiofibroma Anterior cranial fossa/orbit/maxilla No None GTR 3 Yes Fascia lata Negative margins /M Endoscopic endonasal Esthesioneuroblastoma Kadish C (nasal cavity, ethmoid sinus, frontal dura) /F Endoscopic endonasal CSF leak Planum sphenoidale Yes Fascia lata No CSF leak recurrence /M Endoscopic endonasal CSF leak Planum sphenoidale Yes Fascia lata No CSF leak recurrence /F Endonasal endoscopic CSF leak Cribriform plate/ethmoid sinus Yes Fascia lata No CSF leak recurrence 6 60/F None Paget disease Medial orbital roof No None GTR 3 CSF, cerebrospinal fluid; M, male; F, female; GTR, gross total resection.
Skullbase Lesions. Skullbase Surgery Open vs endoscopic. Choice Of Surgical Approaches 12/28/2015. Skullbase Surgery: Evolution
 Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K.
 05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
Skull Base Volume 12 Month. Patients. Anterior/Midline. Pituitary CSF Leak. Lateral. Craniocervical Junction
 UC SF 2 11/7/2009 Skull Base Surgery in 2009 Ivan El-Sayed MD, FACS Director- Otolaryngology Minimally Invasive Skull Base Surgery Program Department Otolaryngology-Head and Neck Surgery University of
UC SF 2 11/7/2009 Skull Base Surgery in 2009 Ivan El-Sayed MD, FACS Director- Otolaryngology Minimally Invasive Skull Base Surgery Program Department Otolaryngology-Head and Neck Surgery University of
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion
 THIEME Case Report e105 Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion Paolo Castelnuovo, MD 1,4 Giacomo Fiacchini, MD 2 Francesca Romana Fiorini, MD 3 Iacopo Dallan,
THIEME Case Report e105 Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion Paolo Castelnuovo, MD 1,4 Giacomo Fiacchini, MD 2 Francesca Romana Fiorini, MD 3 Iacopo Dallan,
The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery
 The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery Edsel Kim, M.D. Otolaryngology-Head and Neck Surgery The Oregon Clinic Providence Brain and Spine Institute Pituitary, Thyroid
The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery Edsel Kim, M.D. Otolaryngology-Head and Neck Surgery The Oregon Clinic Providence Brain and Spine Institute Pituitary, Thyroid
Protective Silastic sheet in combined transorbital and transnasal resection of sinonasal lesions*
 ORIGINAL CONTRIBUTION Protective Silastic sheet in combined transorbital and transnasal resection of sinonasal lesions* Nikul Amin 1, Thomas Jacques 2, Fiona Ting 1, Claire Hopkins 1, Pavol Šurda 1 Rhinology
ORIGINAL CONTRIBUTION Protective Silastic sheet in combined transorbital and transnasal resection of sinonasal lesions* Nikul Amin 1, Thomas Jacques 2, Fiona Ting 1, Claire Hopkins 1, Pavol Šurda 1 Rhinology
We describe some of the conceptual nuances and
 Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
Transcranial resection of tumors of the paranasal sinuses and nasal cavity
 J Neurosurg 71:10-15, 1989 Transcranial resection of tumors of the paranasal sinuses and nasal cavity J. BoB BLACKLOCK, M.D., RANDAL S. WEBER, M.D., YA-YEN LEE, M.D., AND HELMUTH GOEPFERT~ M.D. Section
J Neurosurg 71:10-15, 1989 Transcranial resection of tumors of the paranasal sinuses and nasal cavity J. BoB BLACKLOCK, M.D., RANDAL S. WEBER, M.D., YA-YEN LEE, M.D., AND HELMUTH GOEPFERT~ M.D. Section
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience
 80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
M. PIEMONTE SOC O.R.L. Az. Ospedaliero-Universitaria S.M.M., Udine
 M. PIEMONTE SOC O.R.L. Az. Ospedaliero-Universitaria S.M.M., Udine LIMITS OF ENDOSCOPIC RESECTIONS IN ANTERIOR SKULL BASE TUMORS Limiti delle resezioni endoscopiche nei tumori della rinobase anteriore
M. PIEMONTE SOC O.R.L. Az. Ospedaliero-Universitaria S.M.M., Udine LIMITS OF ENDOSCOPIC RESECTIONS IN ANTERIOR SKULL BASE TUMORS Limiti delle resezioni endoscopiche nei tumori della rinobase anteriore
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA
 ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY INFERIOR MAXILLECTOMY Tumours of the hard palate and superior alveolus may be resected by inferior maxillectomy (Figure 1). A Le Fort
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY INFERIOR MAXILLECTOMY Tumours of the hard palate and superior alveolus may be resected by inferior maxillectomy (Figure 1). A Le Fort
Eyebrow craniotomy for anterior skull base lesions: how I do it
 Acta Neurochir (2013) 155:99 106 DOI 10.1007/s00701-012-1552-5 HOW I DO IT - NEUROSURGICAL TECHNIQUES Eyebrow craniotomy for anterior skull base lesions: how I do it Zsolt Zador & Kanna Gnanalingham Received:
Acta Neurochir (2013) 155:99 106 DOI 10.1007/s00701-012-1552-5 HOW I DO IT - NEUROSURGICAL TECHNIQUES Eyebrow craniotomy for anterior skull base lesions: how I do it Zsolt Zador & Kanna Gnanalingham Received:
5. COMMON APPROACHES. Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2.
 5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
Radiological anatomy of frontal sinus By drtbalu
 2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
January th, 2012
 Basic Endoscopic Sinus Surgery for Residents & Novices and 1st International Advanced Course in Endoscopic Sinus Surgery & Skull Base Surgery January 17-20 th, 2012 January 17 th, 2012: Basic Endoscopic
Basic Endoscopic Sinus Surgery for Residents & Novices and 1st International Advanced Course in Endoscopic Sinus Surgery & Skull Base Surgery January 17-20 th, 2012 January 17 th, 2012: Basic Endoscopic
Chapter 7: Head & Neck
 Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
What Are the Limits of Endoscopic Sinus Surgery?: The Expanded Endonasal Approach to the Skull Base
 REVIEW What Are the Limits of Endoscopic Sinus Surgery?: The Expanded Endonasal Approach to the Skull Base Carl H. Snyderman, 1 Harshita Pant, 1 Ricardo L. Carrau, 1 Daniel Prevedello, 2 Paul Gardner 2
REVIEW What Are the Limits of Endoscopic Sinus Surgery?: The Expanded Endonasal Approach to the Skull Base Carl H. Snyderman, 1 Harshita Pant, 1 Ricardo L. Carrau, 1 Daniel Prevedello, 2 Paul Gardner 2
Case Presentation: Indications for orbital decompression in TED: Modern surgical techniques for orbital decompression in TED: Inferomedial
 Case Presentation: Jonathan W. Kim, MD Director, Oculoplastic Surgery Stanford Medical Center 61 year old man with active Graves orbitopathy Visual acuity 20/30 OD 20/50 OS Left RAPD Bilateral optic disc
Case Presentation: Jonathan W. Kim, MD Director, Oculoplastic Surgery Stanford Medical Center 61 year old man with active Graves orbitopathy Visual acuity 20/30 OD 20/50 OS Left RAPD Bilateral optic disc
10/23/2010. Excludes Single Surgeon Pituitary (N=~140) Skull Base Volume 12 Month UC SF. Patients. Anterior/Midline. Pituitary CSF Leak.
 Advances in Pituitary Surgery Ivan El-Sayed MD, FACS Director- Otolaryngology Minimally Invasive Skull Base Surgery Program Otolaryngology-Head and Neck Surgery University of California-San Francisco Minimally
Advances in Pituitary Surgery Ivan El-Sayed MD, FACS Director- Otolaryngology Minimally Invasive Skull Base Surgery Program Otolaryngology-Head and Neck Surgery University of California-San Francisco Minimally
Malignant growth Maxilla management an analysis
 ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
The sebaceous glands (glands of Zeis) open directly into the eyelash follicles, ciliary glands (glands of Moll) are modified sweat glands that open
 The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
How to Choose? Endoscopic Skull Base Reconstructive Options and Limitations
 ORIGINAL ARTICLE How to Choose? Endoscopic Skull Base Reconstructive Options and Limitations Mihir R. Patel, M.D., 1 Michael E. Stadler, M.D., 1 Carl H. Snyderman, M.D., 2,3 Ricardo L. Carrau, M.D., 4
ORIGINAL ARTICLE How to Choose? Endoscopic Skull Base Reconstructive Options and Limitations Mihir R. Patel, M.D., 1 Michael E. Stadler, M.D., 1 Carl H. Snyderman, M.D., 2,3 Ricardo L. Carrau, M.D., 4
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study
 Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
cally, a distinct superior crease of the forehead marks this spot. The hairline and
 4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Over the past 15 years, the endoscopic endonasal
 See the corresponding editorial in this issue (E5). Neurosurg Focus 37 (4):E4, 2014 AANS, 2014 Endoscopic skull base reconstruction: a review and clinical case series of 152 vascularized flaps used for
See the corresponding editorial in this issue (E5). Neurosurg Focus 37 (4):E4, 2014 AANS, 2014 Endoscopic skull base reconstruction: a review and clinical case series of 152 vascularized flaps used for
Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
 Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Incisionless Brain Surgery
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/incisionless-brainsurgery/3873/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/incisionless-brainsurgery/3873/
Research Article Expanded Endoscopic Endonasal Treatment of Primary Intracranial Tumors within the Paranasal Sinuses
 ISRN Minimally Invasive Surgery Volume 2013, Article ID 129780, 5 pages http://dx.doi.org/10.1155/2013/129780 Research Article Expanded Endoscopic Endonasal Treatment of Primary Intracranial Tumors within
ISRN Minimally Invasive Surgery Volume 2013, Article ID 129780, 5 pages http://dx.doi.org/10.1155/2013/129780 Research Article Expanded Endoscopic Endonasal Treatment of Primary Intracranial Tumors within
CT of Maxillofacial Fracture Patterns. CT of Maxillofacial Fracture Patterns
 CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
T HERE is an unusual and interesting variety of craniosynostosis in
 SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
PRINCIPLES OF ENDOSCOPIC MANAGEMENT OF NASAL AND. Frontier Steven D. Schaefer, MD, FACS
 PRINCIPLES OF ENDOSCOPIC MANAGEMENT OF NASAL AND SKULL : A New Frontier Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York keye and dear Infirmary New York Medical College
PRINCIPLES OF ENDOSCOPIC MANAGEMENT OF NASAL AND SKULL : A New Frontier Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York keye and dear Infirmary New York Medical College
SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA
 SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA LEARNING OBJECTIVES At the end of this lecture, the student should be able to know: Parts of skeleton (axial and appendicular) Parts of skull Sutures of skull
SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA LEARNING OBJECTIVES At the end of this lecture, the student should be able to know: Parts of skeleton (axial and appendicular) Parts of skull Sutures of skull
TOTAL MAXILLECTOMY, ORBITAL EXENTERATION
 TOTAL MAXILLECTOMY, ORBITAL EXENTERATION CC-BY-NC 3.0 Johan Fagan Total maxillectomy refers to surgical resection of the entire maxilla. Resection includes the floor and medial wall of the orbit and the
TOTAL MAXILLECTOMY, ORBITAL EXENTERATION CC-BY-NC 3.0 Johan Fagan Total maxillectomy refers to surgical resection of the entire maxilla. Resection includes the floor and medial wall of the orbit and the
ORIGINAL ARTICLE. The Precaruncular Approach to the Medial Orbit
 The Precaruncular Approach to the Medial Orbit Kris. S. Moe, MD ORIGINAL ARTICLE Background: Most approaches to the medial orbit and lower provide suboptimal access and leave visible scars. The transcaruncular
The Precaruncular Approach to the Medial Orbit Kris. S. Moe, MD ORIGINAL ARTICLE Background: Most approaches to the medial orbit and lower provide suboptimal access and leave visible scars. The transcaruncular
The surgical approach to the sphenoid sinus continues to
 A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
The authors discuss their surgical approaches
 GENERAL SCIENTIFIC SESSION 3 GENERAL SCIENTIFIC SESSION 3 Open vs Endoscopic: When To Use Which Laligam Sekhar, MD* Alessandra Mantovani, MD* Martin Mortazavi, MD* Theodore H. Schwartz, MD WIlliam T. Couldwell,
GENERAL SCIENTIFIC SESSION 3 GENERAL SCIENTIFIC SESSION 3 Open vs Endoscopic: When To Use Which Laligam Sekhar, MD* Alessandra Mantovani, MD* Martin Mortazavi, MD* Theodore H. Schwartz, MD WIlliam T. Couldwell,
DR. ASEEL DOUBI R5 ORL HNS SPONTANEOUS CSF LEAKS
 DR. ASEEL DOUBI R5 ORL HNS SPONTANEOUS CSF LEAKS OUTLINE: Physiology of CSF Types of CSF rhinorrhea Spontaneous CSF leak approach and diagnosis Operative options and postoperative care Lumbar drains current
DR. ASEEL DOUBI R5 ORL HNS SPONTANEOUS CSF LEAKS OUTLINE: Physiology of CSF Types of CSF rhinorrhea Spontaneous CSF leak approach and diagnosis Operative options and postoperative care Lumbar drains current
Communication issue - What should the radiologist report before functional endoscopic sinus surgery
 Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
Surgical Treatment of Olfactory Groove Meningioma
 Med. J. Cairo Univ., VoL 81, No. 1, March: 133-137, 2013 www.medicaljournalofcairouniversity.com Surgical Treatment of Olfactory Groove Meningioma AHMED ELSAWAF, M.D., Ph.D. The Department of Neurosurgery,
Med. J. Cairo Univ., VoL 81, No. 1, March: 133-137, 2013 www.medicaljournalofcairouniversity.com Surgical Treatment of Olfactory Groove Meningioma AHMED ELSAWAF, M.D., Ph.D. The Department of Neurosurgery,
ORIGINAL ARTICLE. Kris S. Moe, MD; Sumana Jothi, MD; Ryan Stern, MD; Holger G. Gassner, MD
 ORIGINAL ARTICLE Lateral Retrocanthal Orbitotomy A Minimally Invasive, Canthus-Sparing Approach Kris S. Moe, MD; Sumana Jothi, MD; Ryan Stern, MD; Holger G. Gassner, MD Objective: To develop and evaluate
ORIGINAL ARTICLE Lateral Retrocanthal Orbitotomy A Minimally Invasive, Canthus-Sparing Approach Kris S. Moe, MD; Sumana Jothi, MD; Ryan Stern, MD; Holger G. Gassner, MD Objective: To develop and evaluate
Salvage skull base reconstruction in the endoscopic era: Vastus lateralis free tissue transfer
 Received: 7 May 2017 Revised: 2 October 2017 Accepted: 10 January 2018 DOI: 10.1002/hed.25094 CASE REPORT Salvage skull base reconstruction in the endoscopic era: Vastus lateralis free tissue transfer
Received: 7 May 2017 Revised: 2 October 2017 Accepted: 10 January 2018 DOI: 10.1002/hed.25094 CASE REPORT Salvage skull base reconstruction in the endoscopic era: Vastus lateralis free tissue transfer
SKULL BASE 1 YEAR-FELLOWSHIP PROGRAM ACADEMIC YEAR 2018/2019
 SKULL BASE 1 YEAR-FELLOWSHIP PROGRAM ACADEMIC YEAR 2018/2019 The skull base Fellowship program program at the University of Insubria, Varese, Italy, is active from 2009 and involves both the Otorhinolaryngological
SKULL BASE 1 YEAR-FELLOWSHIP PROGRAM ACADEMIC YEAR 2018/2019 The skull base Fellowship program program at the University of Insubria, Varese, Italy, is active from 2009 and involves both the Otorhinolaryngological
Dr. Sami Zaqout, IUG Medical School
 The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
Exposure techniques in endoscopic skull base surgery: Posterior septectomy, medial maxillectomy, transmaxillary and transpterygoid approach
 European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 284 288 Available online at www.sciencedirect.com TECHNICAL NOTE Exposure techniques in endoscopic skull base surgery: Posterior
European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 284 288 Available online at www.sciencedirect.com TECHNICAL NOTE Exposure techniques in endoscopic skull base surgery: Posterior
PROBLEM RECOMMENDATION
 PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
Boundaries Septum Turbinates & Meati Lamellae Drainage Pathways Variants
 The Fastest 20 Minutes in Michelle A. Michel, MD Professor of Radiology and Otolaryngology Medical College of Wisconsin, Milwaukee Overview Nasal cavity Anterior skull base Ostiomeatal complex Frontal
The Fastest 20 Minutes in Michelle A. Michel, MD Professor of Radiology and Otolaryngology Medical College of Wisconsin, Milwaukee Overview Nasal cavity Anterior skull base Ostiomeatal complex Frontal
The orbitozygomatic approach achieves better
 OPERATIVE NUANCES THE ORBITOZYGOMATIC APPROACH Wouter Ralph van Furth, M.D., Ph.D. Department of Neurosurgery, Academic Medical Center, University of Amsterdam, Amsterdam, The Netherlands Anne Maria R.
OPERATIVE NUANCES THE ORBITOZYGOMATIC APPROACH Wouter Ralph van Furth, M.D., Ph.D. Department of Neurosurgery, Academic Medical Center, University of Amsterdam, Amsterdam, The Netherlands Anne Maria R.
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
1 Eyelids. Lacrimal Apparatus. Orbital Region. 3 The Orbit. The Eye
 1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
Fracture frontal bone and its management
 From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
CT of Maxillofacial Injuries
 CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
Ophthalmic complications after surgery for nasal and sinus polyposis
 European Journal of Ophthalmology / Vol. 11 no. 3, 2001 / pp. 218-222 Ophthalmic complications after surgery for nasal and sinus polyposis P. VASSALLO, F. TRANFA, R. FORTE, A. D APONTE, D. STRIANESE, G.
European Journal of Ophthalmology / Vol. 11 no. 3, 2001 / pp. 218-222 Ophthalmic complications after surgery for nasal and sinus polyposis P. VASSALLO, F. TRANFA, R. FORTE, A. D APONTE, D. STRIANESE, G.
Skull Base Danger Zones in FESS
 Skull Base Danger Zones in FESS Poster No.: C-2278 Congress: ECR 2014 Type: Educational Exhibit Authors: L. Renza Lozada, R. Carreño Gonzalez, G. Quintana Sanchez, 1 2 1 1 1 2 R. E. Figueroa ; Malaga/ES,
Skull Base Danger Zones in FESS Poster No.: C-2278 Congress: ECR 2014 Type: Educational Exhibit Authors: L. Renza Lozada, R. Carreño Gonzalez, G. Quintana Sanchez, 1 2 1 1 1 2 R. E. Figueroa ; Malaga/ES,
Omran Saeed. Luma Taweel. Mohammad Almohtaseb. 1 P a g e
 2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Imaging of the Paranasal Sinuses
 14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Olfactory groove meningiomas arise from the midline
 clinical article J Neurosurg 124:605 620, 2016 Endoscope-assisted endonasal versus supraorbital keyhole resection of olfactory groove meningiomas: comparison and combination of 2 minimally invasive approaches
clinical article J Neurosurg 124:605 620, 2016 Endoscope-assisted endonasal versus supraorbital keyhole resection of olfactory groove meningiomas: comparison and combination of 2 minimally invasive approaches
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit
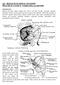 213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit OSTEOLOGY Identify the bones which comprise the walls of the orbit: maxilla, zygomatic, ethmoid, lachrymal, frontal, and
213: HUMAN FUNCTIONAL ANATOMY: PRACTICAL CLASS 12 Cranial cavity, eye and orbit OSTEOLOGY Identify the bones which comprise the walls of the orbit: maxilla, zygomatic, ethmoid, lachrymal, frontal, and
1. BRIEF DESCRIPTION OF TRAINING
 RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
Technique Guide. Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures.
 Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Frontal sinus disease continues to be one of the great
 Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Chapter 7 Part A The Skeleton
 Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY
 COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
ORIGINAL ARTICLE. Combined Subcranial Approaches for Excision of Complex Anterior Skull Base Tumors
 ORIGINAL ARTICLE Combined Subcranial Approaches for Excision of Complex Anterior Skull Base Tumors Dan M. Fliss, MD; Avraham Abergel, MD; Oren Cavel, MD; Nevo Margalit, MD; Ziv Gil, MD, PhD Objective:
ORIGINAL ARTICLE Combined Subcranial Approaches for Excision of Complex Anterior Skull Base Tumors Dan M. Fliss, MD; Avraham Abergel, MD; Oren Cavel, MD; Nevo Margalit, MD; Ziv Gil, MD, PhD Objective:
ORIGINAL ARTICLE TEMPORALIS MUSCLE FLAP FOR RECONSTRUCTION OF SKULL BASE DEFECTS
 ORIGINAL ARTICLE TEMPORALIS MUSCLE FLAP FOR RECONSTRUCTION OF SKULL BASE DEFECTS Jesse E. Smith, MD, 1,2 Yadranko Ducic, MD, FRCS(C), 1,2,3 Robert T. Adelson, MD 4 1 Department of Otolaryngology-Head and
ORIGINAL ARTICLE TEMPORALIS MUSCLE FLAP FOR RECONSTRUCTION OF SKULL BASE DEFECTS Jesse E. Smith, MD, 1,2 Yadranko Ducic, MD, FRCS(C), 1,2,3 Robert T. Adelson, MD 4 1 Department of Otolaryngology-Head and
MANAGEMENT OF CSF. Steven D. Schaefer, MD, FACS. Department of Otolaryngology New York Eye and Ear Infirmary
 MANAGEMENT OF CSF RHINORRHEA, MENIGIOCELES, Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College Anatomy and Physiology
MANAGEMENT OF CSF RHINORRHEA, MENIGIOCELES, Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College Anatomy and Physiology
Use of Pedicle Flaps for Skull Base Reconstruction after Expanded Endonasal Approaches
 Revision Article Use of Pedicle Flaps for Skull Base Reconstruction after Expanded Endonasal Approaches Carlos Diógenes Pinheiro Neto*, Sebastião Diógenes Pinheiro**. * ENT Physician ** Head of ENT Service
Revision Article Use of Pedicle Flaps for Skull Base Reconstruction after Expanded Endonasal Approaches Carlos Diógenes Pinheiro Neto*, Sebastião Diógenes Pinheiro**. * ENT Physician ** Head of ENT Service
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Maxilla, ORBIT and infratemporal fossa. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Endoscopic Assisted resection for congenital Midline Nasal Mass
 Endoscopic Assisted resection for congenital Midline Nasal Mass Ahmed Aly Ibrahim A.prof ORL Department Alexandria University Emad. A Magdy prof ORL Department Alexandria University Haytham Morsi,MD Mohammad
Endoscopic Assisted resection for congenital Midline Nasal Mass Ahmed Aly Ibrahim A.prof ORL Department Alexandria University Emad. A Magdy prof ORL Department Alexandria University Haytham Morsi,MD Mohammad
Surgical approaches to PITUITARY ADENOMAS
 Surgical approaches to PITUITARY ADENOMAS HISTORY OF PITUITARY SURGERY In 1893,Caton and Paul attempted to explore sella turcica via lateral sub temporal route along with orbital exenteration. The transfrontal
Surgical approaches to PITUITARY ADENOMAS HISTORY OF PITUITARY SURGERY In 1893,Caton and Paul attempted to explore sella turcica via lateral sub temporal route along with orbital exenteration. The transfrontal
Fronto-orbito-zygomatic (FOZ) Approach
 Fronto-orbito-zygomatic (FOZ) Approach 3 Imad N. Kanaan 3.1 Introduction Surgical management of skull base pathologies remains one of the most challenging tasks for neurosurgeons. Advances in neuroimaging
Fronto-orbito-zygomatic (FOZ) Approach 3 Imad N. Kanaan 3.1 Introduction Surgical management of skull base pathologies remains one of the most challenging tasks for neurosurgeons. Advances in neuroimaging
Benign Neoplasms of the Nose
 Department of Otolaryngology Head and Neck Surgery Pursuing Wellness Through Teaching, Learning and Healing Benign Neoplasms of the Nose Ivan El Sayed, MD Disclosure Principal Investigator: Grant Support
Department of Otolaryngology Head and Neck Surgery Pursuing Wellness Through Teaching, Learning and Healing Benign Neoplasms of the Nose Ivan El Sayed, MD Disclosure Principal Investigator: Grant Support
A Novel Reconstructive Technique After Endoscopic Expanded Endonasal Approaches: Vascular Pedicle Nasoseptal Flap
 The Laryngoscope Lippincott Williams & Wilkins, Inc. 2006 The American Laryngological, Rhinological and Otological Society, Inc. A Novel Reconstructive Technique After Endoscopic Expanded Endonasal Approaches:
The Laryngoscope Lippincott Williams & Wilkins, Inc. 2006 The American Laryngological, Rhinological and Otological Society, Inc. A Novel Reconstructive Technique After Endoscopic Expanded Endonasal Approaches:
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q
 The British Association of Plastic Surgeons (2004) 57, 37 44 Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q M. Kakibuchi*,
The British Association of Plastic Surgeons (2004) 57, 37 44 Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q M. Kakibuchi*,
Skull base defects that result in dural tears and CSF leaks can
 ORIGINAL RESEARCH V. La Fata N. McLean S.K. Wise J.M. DelGaudio P.A. Hudgins CSF Leaks: Correlation of High-Resolution CT and Multiplanar Reformations with Intraoperative Endoscopic Findings BACKGROUND
ORIGINAL RESEARCH V. La Fata N. McLean S.K. Wise J.M. DelGaudio P.A. Hudgins CSF Leaks: Correlation of High-Resolution CT and Multiplanar Reformations with Intraoperative Endoscopic Findings BACKGROUND
Case Report Gigant Transethmoidal Meningoencephalocele Operated by Full Endonasal Endoscopic Approach: Case Report
 Case Reports in Medicine Volume 2012, Article ID 763259, 4 pages doi:10.1155/2012/763259 Case Report Gigant Transethmoidal Meningoencephalocele Operated by Full Endonasal Endoscopic Approach: Case Report
Case Reports in Medicine Volume 2012, Article ID 763259, 4 pages doi:10.1155/2012/763259 Case Report Gigant Transethmoidal Meningoencephalocele Operated by Full Endonasal Endoscopic Approach: Case Report
Our Experience with Endoscopic Brow Lifts
 Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
Aesth. Plast. Surg. 24:90 96, 2000 DOI: 10.1007/s002660010017 2000 Springer-Verlag New York Inc. Our Experience with Endoscopic Brow Lifts Ozan Sozer, M.D., and Thomas M. Biggs, M.D. İstanbul, Turkey and
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures.
 Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
MAXILLA, ORBIT & PTERYGOPALATINE FOSSA. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 MAXILLA, ORBIT & PTERYGOPALATINE FOSSA Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine Maxilla MAXILLA Superior, middle, and inferior meatus Frontal
MAXILLA, ORBIT & PTERYGOPALATINE FOSSA Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine Maxilla MAXILLA Superior, middle, and inferior meatus Frontal
Neurosurgical Techniques
 Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
JOURNAL OF INTERNATIONAL ACADEMIC RESEARCH FOR MULTIDISCIPLINARY Impact Factor 3.114, ISSN: , Volume 4, Issue 11, December 2016
 SELLAR RECONSTRUCTION AFTER ENDOSCOPIC TRANSSPHENOID PITUITARY SURGERY: SYSTEMATIC REVIEW AND META-ANALYSIS ABDELRHMAN YOUNES BADAWY* AHMED ELFAROUK ABDELFATTAH** HESHAM NABIL LASHEEN*** *Lecturer of Otorhinolaryngology,
SELLAR RECONSTRUCTION AFTER ENDOSCOPIC TRANSSPHENOID PITUITARY SURGERY: SYSTEMATIC REVIEW AND META-ANALYSIS ABDELRHMAN YOUNES BADAWY* AHMED ELFAROUK ABDELFATTAH** HESHAM NABIL LASHEEN*** *Lecturer of Otorhinolaryngology,
Dr. Sami Zaqout Faculty of Medicine IUG
 The Nose External Nose Nasal Cavity External Nose Blood and Nerve Supplies of the External Nose Blood Supply of the External Nose The skin of the external nose Branches of the ophthalmic and the maxillary
The Nose External Nose Nasal Cavity External Nose Blood and Nerve Supplies of the External Nose Blood Supply of the External Nose The skin of the external nose Branches of the ophthalmic and the maxillary
Mucocele of paranasal sinuses
 From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
Nasal region. cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?
 Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
Anatomic Relations Summary. Done by: Sohayyla Yasin Dababseh
 Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
10/4/2013. Sinonasal and Skull Base Cancer Progress, Challenges, and Future Directions
 Ehab Hanna, M.D. Head and Neck Surgery MD Anderson Cancer Center Sinonasal and Skull Base Cancer Progress, Challenges, and Future Directions Context Advances in Diagnosis Office endoscopy High Resolution
Ehab Hanna, M.D. Head and Neck Surgery MD Anderson Cancer Center Sinonasal and Skull Base Cancer Progress, Challenges, and Future Directions Context Advances in Diagnosis Office endoscopy High Resolution
THIEME. Scalp and Superficial Temporal Region
 CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
