Decreased Perihematomal Edema in Thrombolysis-Related Intracerebral Hemorrhage Compared With Spontaneous Intracerebral Hemorrhage
|
|
|
- Gloria Stewart
- 5 years ago
- Views:
Transcription
1 Decreased Perihematomal Edema in Thrombolysis-Related Intracerebral Hemorrhage Compared With Spontaneous Intracerebral Hemorrhage James M. Gebel, MD; Thomas G. Brott, MD; Cathy A. Sila, MD; Thomas A. Tomsick, MD; Edward Jauch, MD; Shelia Salisbury, MS; Jane Khoury, MS; Rosemary Miller, RN; Arthur Pancioli, MD; John E. Duldner, MD; Eric J. Topol, MD; Joseph P. Broderick, MD Background and Purpose Intracerebral hemorrhage (ICH) is a highly morbid disease process. Perihematomal edema is reported to contribute to clinical deterioration and death. Recent experimental observations indicate that clotting of the intrahematomal blood is the essential prerequisite for hyperacute perihematomal edema formation rather than blood-brain barrier disruption. Methods We compared a series of patients with spontaneous ICH (SICH) to a series of patients with thrombolysis-related ICH (TICH). All patients were imaged within 3 hours of clinical onset. We reviewed relevant neuroimaging features, emphasizing and quantifying perihematomal edema. We then analyzed clinical and radiological differences between the 2 ICH types and determined whether these factors were associated with perihematomal edema. Results TICHs contained visible perihematomal edema less than half as often as SICHs (31% versus 69%, P 0.001) and had both lower absolute edema volumes (0 cc [25th, 75th percentiles: 0, 6] versus 6 cc [0, 13], P ) and relative edema volumes (0.16 [0.10, 0.33] versus 0.55 [0.40, 0.83], P ). Compared with SICHs, TICHs were 3 times larger in volume (median [25th, 75th percentiles] volume 69 cc [30, 106] versus 21 cc [8, 45], P ), 4 times more frequently lobar in location (62% versus 15%, P 0.001), 80 times more frequently contained blood-fluid level(s) (86% versus 1%, P 0.001), and were more frequently multifocal (22% versus 0%, P 0.001). Conclusions The striking qualitative and quantitative lack of perihematomal edema observed in the thrombolysis-related ICHs compared with the SICHs provides the first substantial, although indirect, human evidence that intrahematomal blood clotting is a plausible pathogenetic factor in hyperacute perihematomal edema formation. (Stroke. 2000;31: ) Key Words: brain edema cerebral hemorrhage hematoma thrombolysis Intracerebral hemorrhage (ICH) kills approximately Americans annually. 1 Although significant ICH-related morbidity arises from hematoma mass effect and intraventricular extension, further clinical deterioration related to rebleeding and/or perihematomal edema development often occurs. 2 Recent experimental evidence 3 6 suggests that hyperacute perihematomal edema results from the clotting of intrahematomal blood with liberation of remaining serum proteins into the surrounding brain tissue rather than by blood-brain barrier disruption, as traditionally thought. Anticoagulants, such as heparin, prolong the time necessary for blood to clot. Thrombolytic drugs, such as streptokinase and tissue plasminogen activator (tpa), lead to enzymatic lysing of fibrin. Our previously reported clinicoradiological analysis of all intracranial hemorrhages complicating the GUSTO-1 trial of systemic thrombolysis for acute myocardial infarction demonstrated large volumes of ICH and high frequencies of lobar hematomas, intrahematomal blood-fluid level(s), and multifocal hemorrhage compared with values typical for SICH. Furthermore, perihematomal edema was less frequent and severe than that typically seen in SICH. This largely descriptive analysis, however, did not address time from ICH symptom onset to brain CT and lacked a comparison group of SICHs. For this report, we performed a comparative clinicoradiological analysis of a large series of acutely imaged TICHs and a large series of acutely imaged SICHs. We qualitatively and quantitatively described differences between these 2 ICH types, emphasizing perihematomal edema. By including only Received August 4, 1999; final revision received November 12, 1999; accepted November 12, From the Department of Neurology, University of Pittsburgh Medical Center (J.M.G.),, Pittsburgh, Pa; Department of Neurology, Mayo Clinic Educational Foundation (T.G.B.),, Jacksonville, Fla; Departments of Neurology and Cardiology, Cleveland Clinic Foundation (C.A.S., E.J.T.), Cleveland, Ohio; and Departments of Neurology and Emergency Medicine, University of Cincinnati Medical Center (T.A.T., E.J., S.S., J.K., R.M., A.P., J.E.D., J.P.B.), Cincinnati, Ohio. J.M.G. and J.P.B. are members of the Genentech Speaker s Bureau. Correspondence and reprint requests to James M. Gebel, MD, University of Pittsburgh Medical Center Stroke Institute, 200 Lothrop Street, C-420 PUH, Pittsburgh, PA jgebel@stroke.upmc.edu 2000 American Heart Association, Inc. Stroke is available at 596
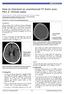
2 Gebel et al Decreased Edema in Thrombolysis-Related ICH 597 TICH compared with SICH. A typical SICH of 20-cc volume with significant perihematomal edema (left). This contrasts with the much larger (70-cc) typical TICH with a blood-fluid level and minimal visible perihematomal edema (right). patients who underwent brain CT within 3 hours of ICH symptom onset, we controlled for the important confounding factor: time. Finally, we hypothesized what these observations suggest about the pathogenesis of hyperacute perihematomal edema in humans. Subjects and Methods We studied 2 separate study populations. The first group was derived from patients randomized into the GUSTO-1 coronary artery thrombolysis trial for acute myocardial infarction. 7 In this trial, 268 patients suffered intracranial (parenchymal and/or subdural) hemorrhage with no identifiable underlying structural cause such as neoplasm, aneurysm, or vascular malformation. We excluded those whose CT scans of the brain were not available for review (19), those with subdural hematoma (44), those with missing CT times (13), those in whom the time difference between ICH symptom onset time and CT scan time was a negative value (which indicated inaccurate data transcription) (19), those with missing times of ICH symptom onset (6), and those with no radiological evidence of ICH (4). Finally, in the remaining group of 173 patients, those imaged 3 hours after ICH symptom onset (99 patients) were excluded, leaving 74 patients with 1 or more parenchymal hematomas imaged within 3 hours of clinical onset. The second group was derived from a large, prospective series of 142 patients living in Greater Cincinnati and Northern Kentucky during 1988 to 1993 with spontaneous ICH imaged within 3 hours of clinical symptom onset. Details of this study s design and patient recruitment have been published elsewhere. 2 Only the initial (baseline) CT scans in this study were used for our analysis. We excluded patients with underlying structural lesions, such as neoplasm, aneurysm, or vascular malformation (12); those unable to complete the original study (10); those whose CT scans could not be located (10); those with anticoagulant-, thrombolysis-, or coagulopathy-related ICH (7); those with missing clinical symptom onset times (4); and those unable or unwilling to give informed consent (2). This left a group of 97 patients with 1 or more spontaneous parenchymal hematomas imaged within 3 hours of clinical symptom onset. In both patient populations, ICH symptom onset was defined by witnessed onset of acute headache, decreased level of consciousness, or appearance of focal neurological deficits secondary to ICH identified on the subsequent noncontrast brain CT. All noncontrast CT scans of the brain were reviewed by at least 1 principal investigator (J.M.G., T.G.B., C.A.S., or T.A.T.). Parenchymal hematoma, intraventricular hemorrhage, and edema volumes in the TICH patients were measured with computer-assisted 3D volumetric analysis (proprietary software, Center for Computer Assisted Neurosurgery, Cleveland Clinic Foundation, run on Sun Microsystems SparcStation I). Volumes in the SICH patient group were determined by another similar technique, the details of which have been published elsewhere. 8 In both groups, relative edema volume was defined as the ratio of absolute perihematomal edema volume to parenchymal hematoma volume. The number of hemorrhage foci was determined. Hematoma location was classified as follows: lobar, defined as hematoma predominately confined to 1 or more lobes of the brain and adjacent subcortical white matter; deep, defined as hematoma predominantly confined to the caudate nucleus, putamen, globus pallidus, internal capsule, and/or thalamus; brain stem, defined as hematoma confined to the midbrain, pons, and/or medulla; or cerebellar, defined as hematoma confined to the cerebellar vermis and/or hemispheres. The presence or absence of hydrocephalus, mass effect, herniation (transtentorial or subfalcial), and intrahematomal blood-fluid level was noted for each scan. Detailed definitions and criteria for each of these features have been published elsewhere. 9,10 It should be reiterated that blood-fluid level is defined as the presence of uniform low attenuation above and high attenuation below a discrete line of horizontal separation within a hematoma. (Figure, bottom.) Clinical and demographic data were obtained from the preexisting databases for each of the 2 studies. In the GUSTO-1 trial, from which the thrombolysis-related ICH patient group in the present study was derived, all patients received 160 to 325 mg aspirin on study enrollment and daily thereafter and were randomized to 1 of the following 4 thrombolytic agent and anticoagulant treatment strategies: (1) streptokinase 1.5 million U over 1 hour with subcutaneous heparin U twice daily; (2) streptokinase 1.5 million U over 1 hour with intravenous (IV) heparin; (3) tpa 15-mg IV bolus, then 0.75 mg/kg (maximum 50 mg) over 30 minutes and 0.5 mg/kg (maximum 35 mg) over 1 hour with IV heparin; or (4) combination therapy with tpa 1.0 mg/kg (maximum 90 mg) over 1 hour with 10% given as a bolus and streptokinase 1.0 million U over 1 hour with IV heparin. The IV heparin regimen consisted of a 5000-U bolus, then 1000 U/h for 48 hours, subsequently adjusted to maintain an activated partial thromboplastin time (aptt) of 60 to 85 seconds. Baseline demographic and clinical risk factor variables for each patient group, and hematoma, edema, and intraventricular hemorrhage volumes were summarized as means with SDs for normally distributed continuous variables. Non-normally distributed continuous variables were summarized by median (25th, 75th percentile) values. Categorical variables were summarized as frequencies or percentages. The Student t test was used to compare differences in normally distributed continuous variable, and the Wilcoxon rank sum test was used to compare differences in non-normally distributed continuous variables. The 2 test was used to compare differences between patient groups for categorical variables. Values of P 0.05 were considered statistically significant. The correlation coefficient was used to measure the degree of linear association between 2 continuous variables. Regression analysis was also used to evaluate relationships between continuous variables.
3 598 Stroke March 2000 TABLE 1. Baseline Demographic Information for TICH and SICH Patient Groups TABLE 3. Radiographic Features of Acutely Imaged TICHs Versus SICHs Variable TICHs SICHs (n 97) P Age* 68.5 (8.3) 63.0 (14.0) Male sex 58% 63% History of diabetes 18% 13% Nonwhite race 12% 30% History of hypertension 62% 65% Current smoker 29% 28% *Mean (SD); by Student t test; by 2 test. Results The distribution of baseline demographic variables and ICH risk factors were similar in both patient groups, except that the TICH patients were on average 6 years older than the SICH patients (P 0.002), and the proportion of nonwhite patients was greater in the SICH group (30%) than the TICH group (12%, P 0.006). (Table 1). Mean (SD) time from ICH symptom onset to CT scanning was 1.48 (0.61) hours for the SICH group compared with 1.52 (0.78) hours for the TICH group. Striking differences in the frequency and amount of perihematomal edema were observed between the 2 groups. Specifically, visible perihematomal edema was present less than half as often in the TICHs (31%) as in the SICHs (69%, P 0.001). Furthermore, the quantity of perihematomal edema was much lower in TICHs compared with SICHs, whether measured by absolute volume (0 cc [0, 6] versus 6 cc [0, 13], P ) or by relative volume (0.43 [0, 0.66] versus 0 [0, 0.10]; Table 2). Factors not associated with the presence or amount of perihematomal edema included patient age, gender, time from symptom onset to CT, hypertension, smoking, and diabetes. A statistically significant difference was observed, however, in the median absolute amount of perihematomal edema between nonwhite (1.9 cc) and white (7.6 cc, P 0.02) patients in the SICH group but not in relative edema values. Despite the lower frequency and amount of perihematomal edema observed in TICHs, their median total volumes were 3 times those of the spontaneous ICHs (P ) and were more frequently associated with mass effect (P 0.010) and herniation (P 0.023; Table TABLE 2. ICH and Edema Volumes in TICH and SICH TICH Variable TICHs 3) None of the 10 hematomas with no blood-fluid level in the thrombolysis-related ICH group had visible perihematomal edema (P 0.027). However, there was a significant difference in the median time from symptom onset to imaging of these 10 hematomas (1.15 hours) versus the 64 hematomas with a blood-fluid level (1.72 hours, P 0.043). Other important radiological differences between the 2 ICH types were that TICHs were of lobar anatomic location (61%) 4 times more often than SICHs (15%, P 0.001), and TICHs also more often contained blood-fluid level(s) (86%) than SICHs (1%, P 0.001; Table 3). Those TICHs with a blood-fluid level (n 64, median [25th, 75th percentiles] volume 74.0 [43, 116]) were almost 4 times larger than those without a blood-fluid level (n 10, median [25th, 75th percentiles] volume 30 cc [7, 85], P 0.040) Finally, TICHs were much more often multifocal than SICHs (22% versus 0%, P 0.001). Table 3 describes other noteworthy radiological differences between the 2 hemorrhage types. Discussion In this study, we observed a significant qualitative and quantitative lack of perihematomal edema surrounding TICHs compared with the SICHs, controlling for time from symptom onset to CT scanning. Specifically, visible perihematomal edema was present less than half as often in TICH as in with SICH, and amounts of edema in TICHs were small SICH (n 97) P * Total hemorrhage volume, cc 69 (30, 106) 21 (8, 45) Percent of ICHs with any edema 31% 69% Total absolute edema volume, cc 0 (0, 6) 6 (0, 13) Total relative edema volume 0 (0, 0.10) 0.43 (0, 0.66) Total relative edema volume (0.10, 0.33) [n 23] 0.55 (0.40, 0.83) [n 67] Results are reported as percentage frequencies for categorical variables and median (25th, 75th percentiles) values for continuous variables. *P values determined by 2 test for categorical variables and Wilcoxon rank sum test for continuous variables. Relative edema volume is defined as the ratio of absolute edema volume to hematoma volume. Relative edema volume in only those hematomas surrounded by visible perihematomal edema in each group (n 23/74 for TICH group and n 67/97 in SICH group). SICHs (n 97) Multifocal 22% 0% Blood-fluid level(s) 86% 1% Any mass effect 93% 78% Herniation 33% 18% Intraventricular hemorrhage present 46% 44% Hydrocephalus 49% 26% Lobarich location 61% 15% Deep ICH location 20% 69% Other ICH location 19% 16% *All P values determined by 2 test. P
4 Gebel et al Decreased Edema in Thrombolysis-Related ICH 599 even when present less than one third the amount of that seen in SICH, in relative terms (Table 3). We limited the time from ICH symptom onset to neuroimaging to 3 hours in both patient groups for several reasons. First, we wished to control as much as possible for the important confounding effects of time. Second, limiting this time window allowed us to observe these 2 very different ICH types as close to their clinical origins as realistically possible. Finally, we sought to identify important factors in the pathogenesis of perihematomal edema formation in hyperacute human ICH. It should be emphasized up front, however, that both restricting our analysis to those patients imaged within 3 hours of clinical onset and not having follow-up scans available for any of the TICH patients prevent us from drawing direct conclusions about delayed perihematomal edema formation and its pathogenic factors. All edema measurements had been completed in both patient groups by experienced technicians before our study was conceived or implemented; thus, the possibility of bias related to knowledge of its anticipated results by the investigators is minimal. As noted above, in attempting to understand the observed differences in perihematomal edema formation between the 2 patient groups, our first goal was to eliminate time from symptom onset to CT scanning as a confounding variable. In this regard, the first and foremost relevant observation is that no significant difference existed between times from clinical symptom onset to imaging between the TICH and SICH groups. Thus, as intended, a difference in timing of imaging between the 2 patient groups does not explain the observed differences. Regarding whether a longer time or some minimum absolute amount of time might be required for perihematomal edema formation within the TICH patient group itself, we note the following observations. The frequency and amounts of perihematomal edema reported in the acutely imaged TICH patient group in this study do not appreciably differ from the overall results previously reported for the entire GUSTO-1 intracranial hemorrhage population, 9 which included patients whose times from ICH symptom onset to neuroimaging were delayed up to 96 hours. This observation argues strongly against an obligatory minimum time requirement for hyperacute perihematomal edema formation as a likely explanation for the greatly diminished amount of perihematomal edema observed in the TICH patient group in our study. Other supportive observations for this conclusion are that neither time from thrombolytic treatment to symptom onset nor time from symptom onset to neuroimaging correlated with perihematomal edema volume within the overall GUSTO-1 intracranial hemorrhage population. 9 Given that there is no evidence to support either the hypotheses that more prompt imaging of the TICH group explains the greatly diminished perihematomal edema formation in this group, and no evidence to support the hypothesis that some minimum amount of time ( 3 hours) is necessary for perihematomal formation in this group, we next considered whether or not any associations between ICH clinical risk factors or demographic variables and amount of perihematomal edema might explain the observations. In reviewing available data for important demographic or clinical pathogenetic factors, none approached statistical significance when related to perihematomal edema in a univariate analysis, except for race within the SICH group only. Although nonwhite patients had a significantly greater median absolute perihematomal edema volume than white patients in this group, this association was not sustained when relative perihematomal edema amounts were compared. This in essence means that total ICH volumes were smaller in the nonwhite subgroup of this population. Thus, no apparent clinical risk factor or demographic variable adequately explains the differences in perihematomal edema volume observed between the TICH and SICH patients. Because neither time nor clinical risk factor or demographic variables were associated with the observed differences in perihematomal edema formation between the 2 patient groups, the remaining logical possibility is that the thrombolytic agents and/or heparin themselves were responsible for the observed decreased amount of perihematomal edema formation in the TICH patient group. Regarding this possibility, we should first reiterate that all patients in the TICH group had received aspirin, heparin, and 1 or more thrombolytic agents prior to their ICH onset. However, each of the 4 thrombolytic/anticoagulant treatment regimens used within the TICH group was different. No significant differences in edema frequency and volume were observed between the 268 patients in each of the 4 treatment groups in the overall GUSTO-1 trial, 9 indicating that a unique biological action specific to tpa, streptokinase, or subcutaneous versus IV heparin to explain the lack of edema is unlikely. All of the drugs used within each of the 4 thrombolytic treatment regimens, however, share the common feature of preventing (heparin and aspirin) or actively degrading (streptokinase and tpa via fibrinolysis) blood clotting. The very high frequency of blood-fluid levels observed in the hematomas of the TICH patients strongly supports the notion that blood within these hematomas is indeed largely unclotted. A number of recent experimental animal model observations closely parallel those seen in our study. Lee et al, 4 in a murine model, confirmed that clotting cascade activation is a necessary prerequisite for hyperacute perihematomal edema formation. Wagner et al, 3 in a porcine lobar ICH model, demonstrated significant hyperacute perihematomal edema development despite an intact blood-brain barrier. Furthermore, the separation of unclotted plasma and red cells, manifest radiologically by blood-fluid level(s) in our TICH patients, was reproduced experimentally by Xi 11 and colleagues when heparinized blood injected into porcine brain white matter produced an unclotted, RBC-serum layered clot with no perihematomal edema at 4 hours. Such a blood-serum separation has not, to the best of our knowledge, ever been observed and reported in this or any other animal ICH model when normal whole blood was injected. These experimental observations collectively suggest that in animal models, hyperacute perihematomal edema formation within the time frame observed in our human study results from clotting of intrahematomal blood, which allows remaining serum proteins to diffuse from the clotted RBCfibrin central hematoma mass into brain parenchyma. This
5 600 Stroke March 2000 event may represent the first in a cascade of hematological and biochemical reactions that ultimately mediate significant tissue injury in ICH. Lee and colleagues 5,6,12,13 have furthermore observed that in murine models, thrombin itself may be directly neurotoxic and is uniquely linked to hyperacute perihematomal edema formation. These observations provide a more specific plausible explanation for the biochemical mechanisms through which heparin and/or fibrinolytic agents such as streptokinase and tpa might plausibly inhibit such edema formation. We hypothesize, therefore, based on both these collective experimental observations and the clinicoradiological observations reported in this study, that clotting of intrahematomal blood is a plausible pathogenetic factor in the formation of hyperacute perihematomal edema in humans. We acknowledge that our evidence to support this hypothesis is indirect. However, ethical considerations in humans preclude the type of systematic, sequential, direct measurement techniques of specific intrahematomal substances or blood-brain barrier permeability in perihematomal brain tissue employed in animal models. Thus, we do not have specific evidence in this or other human studies to differentiate whether prevention of blood clotting in a general sense, or some more specific known or unknown biochemical interaction (such as active degradation of fibrin and/or other serum proteins by the thrombolytic agents) between the thrombolytic agents and/or heparin and adjacent perihematomal brain tissue (or blood vessels) explains the inhibition of hyperacute perihematomal edema formation observed in the TICH patient group in our study. Therapeutic implications of such hypotheses are significant, and deserve to be investigated both experimentally and, to whatever extent is ethically feasible, clinically. The durable absence of perihematomal edema observed beyond 3 hours in the overall GUSTO-1 intracranial hemorrhage population, 9 in particular, suggests the possibility of therapeutic intrahematomal instillation of tpa or other thrombolytic agent to reduce perihematomal edema. In this regard, Wagner et al recently reported that perihematomal edema at 24 hours can be reduced by 70% by early (3.5 hours) tpa-induced clot lysis and aspiration and that tpa also likely lyses interstitial fibrin and removes edemagenic plasma proteins. 14 In summary, we observe a greatly diminished frequency and amount of hyperacute perihematomal edema formation in thrombolysis-related ICHs as compared with spontaneous ICH. We hypothesize, based on available experimental and clinical evidence, that clotting of intrahematomal blood is a plausible and probable pathogenetic factor associated with hyperacute perihematomal edema formation in humans. More research is needed to elucidate the precise mechanisms of hyperacute edema formation in human ICH and subsequent associated brain injury events. Understanding these events could engender development of novel therapeutic strategies aimed at antagonizing or preventing such events in an illness which, to date, has little proven effective therapy. Acknowledgments This study was partially funded by NINDS grant RO1-NS We wish to gratefully acknowledge the manuscript preparation assistance of Amy Hess and Kerri Jackson, and the contributions of Kenneth R. Wagner, PhD, in reviewing the scientific content of the manuscript s discussion. References 1. Broderick JP, Brott TG, Tomsick T, Miller R, Huster G. Intracerebral hemorrhage is more than twice as common as subarachnoid hemorrhage. J Neurosurg. 1993;78: Brott TG, Broderick JP, Kothari RU, Barsan W, Tomsick T, Sauerbeck L, Spilker J, Duldner J, Khoury J. Early hemorrhage growth in patients with intracerebral hemorrhage. Stroke. 1997;28: Wagner KR, Guohua X, Hua Y, Kleinholz M, de Courten-Meyers GM, Myers RE, Broderick JP, Brott TG. Lobar intracerebral hemorrhage model in pigs: rapid edema development in perihematomal white matter. Stroke. 1996;27: Lee KR, Betz AL, Kim S, Keep RF, Hoff JT. The role of the coagulation cascade in brain edema formation after intracerebral hemorrhage. Acta Neurochir. 1996;138: Lee KR, Colon GP, Betz AL, Keep RF, Kim S, Hoff JT. Edema from intracerebral hemorrhage: the role of thrombin. J Neurosurg. 1996;84: Lee KR, Kawai N, Kim S, Sagher O, Hoff JT. Mechanisms of edema formation after intracerebral hemorrhage: effects of thrombin on cerebral blood flow, blood-brain barrier permeability, and cell survival in a rat model. J Neurosurg. 1997;86: The Global Utilization of Streptokinase and Tissue Plasminogen Activator for Occluded Coronary Arteries (GUSTO) Investigators. An international randomized trial comparing four thrombolytic for acute myocardial infarction. N Engl J Med. 1993;329: Loncaric S, Dhawan AP, Broderick JP, Brott TG. 3-D image analysis of intra-cerebral brain hemorrhage from digitized CT films. Comput. Methods Programs Biomed. 1995;46: Gebel JM, Sila CA, Sloan MA, Granger CB, Mahaffey KW, Weisenberger J, Green CL, White HD, Gore JM, Weaver WD, Califf RM, Topol EJ. Thrombolysis-related intracranial hemorrhage: a radiographic analysis of 244 cases from the GUSTO-1 trial with clinical correlation. Stroke. 1998;29: Lisk DR, Pasteur W, Rhoades H, Putnam RD, Grotta JC. Early presentation of hemispheric intracerebral hemorrhage: prediction of outcome and guidelines for treatment allocation. Neurology. 1994;44: Xi G, Wagner KR, Keep RF, Hua Y, de Courten-Myers GM, Broderick JP, Brott TG, Hoff JT. Role of blood clot formation on early edema development after experimental intracerebral hemorrhage. Stroke. 1998; 29: Lee KR, Betz AL, Keep RF, Chenevert TL, Kim S, Hoff JT. Intracerebral infusion of thrombin as a cause of brain edema. J Neurosurg. 1995;83: Lee KR, Drury I, Vitarbo E, Hoff JT. Seizures induced by intracerebral injection of thrombin: a model of intracerebral hemorrhage. J Neurosurg. 1997;87: Wagner KR, Xi G, Hua Y, Zuccarello M, de Courten-Myers GM, Broderick JP, Brott TG. Ultra-early clot aspiration after lysis with tissue plasminogen activator in a porcine model of intracerebral hemorrhage: Edema reduction and blood brain barrier protection. J Neurosurg. 1999; 90:
7 TI - Epidemiology of intracerebral hemorrhage.
 1 TI - Multiple postoperative intracerebral haematomas remote from the site of craniotomy. AU - Rapana A, et al. SO - Br J Neurosurg. 1998 Aug;1():-8. Review. IDS - PMID: 1000 UI: 991958 TI - Cerebral
1 TI - Multiple postoperative intracerebral haematomas remote from the site of craniotomy. AU - Rapana A, et al. SO - Br J Neurosurg. 1998 Aug;1():-8. Review. IDS - PMID: 1000 UI: 991958 TI - Cerebral
Intracranial hemorrhage is an uncommon but serious complication
 Original Contributions Thrombolysis-Related Intracranial Hemorrhage A Radiographic Analysis of 244 Cases From the GUSTO-1 Trial With Clinical Correlation James M. Gebel, MD; Cathy A. Sila, MD; Michael
Original Contributions Thrombolysis-Related Intracranial Hemorrhage A Radiographic Analysis of 244 Cases From the GUSTO-1 Trial With Clinical Correlation James M. Gebel, MD; Cathy A. Sila, MD; Michael
GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE
 2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
Intracerebral Hemorrhage
 Review of Primary Intracerebral Hemorrhage Réza Behrouz, DO Assistant Professor of Neurology University of South Florida College of Medicine STROKE 85% ISCHEMIC 15% HEMORRHAGIC HEMORRHAGIC STROKE 1/3 Subarachnoid
Review of Primary Intracerebral Hemorrhage Réza Behrouz, DO Assistant Professor of Neurology University of South Florida College of Medicine STROKE 85% ISCHEMIC 15% HEMORRHAGIC HEMORRHAGIC STROKE 1/3 Subarachnoid
Recombinant Factor VIIa for Intracerebral Hemorrhage
 Recombinant Factor VIIa for Intracerebral Hemorrhage January 24, 2006 Justin Lee Pharmacy Resident University Health Network Outline 1. Introduction to patient case 2. Overview of intracerebral hemorrhage
Recombinant Factor VIIa for Intracerebral Hemorrhage January 24, 2006 Justin Lee Pharmacy Resident University Health Network Outline 1. Introduction to patient case 2. Overview of intracerebral hemorrhage
Index. C Capillary telangiectasia, intracerebral hemorrhage in, 295 Carbon monoxide, formation of, in intracerebral hemorrhage, edema due to,
 Neurosurg Clin N Am 13 (2002) 395 399 Index Note: Page numbers of article titles are in boldface type. A Age factors, in intracerebral hemorrhage outcome, 344 Albumin, for intracerebral hemorrhage, 336
Neurosurg Clin N Am 13 (2002) 395 399 Index Note: Page numbers of article titles are in boldface type. A Age factors, in intracerebral hemorrhage outcome, 344 Albumin, for intracerebral hemorrhage, 336
Early Surgical Treatment for Supratentorial Intracerebral Hemorrhage. A Randomized Feasibility Study
 Early Surgical Treatment for Supratentorial Intracerebral Hemorrhage A Randomized Feasibility Study Mario Zuccarello, MD; Thomas Brott, MD; Laurent Derex, MD; Rashmi Kothari, MD; Laura Sauerbeck, RN, BSN;
Early Surgical Treatment for Supratentorial Intracerebral Hemorrhage A Randomized Feasibility Study Mario Zuccarello, MD; Thomas Brott, MD; Laurent Derex, MD; Rashmi Kothari, MD; Laura Sauerbeck, RN, BSN;
Comparison of ABC/2 Estimation Technique to Computer-Assisted Planimetric Analysis in Warfarin-Related Intracerebral Parenchymal Hemorrhage
 Comparison of ABC/2 Estimation Technique to Computer-Assisted Planimetric Analysis in Warfarin-Related Intracerebral Parenchymal Hemorrhage Hagen B. Huttner, MD; Thorsten Steiner, MD; Marius Hartmann,
Comparison of ABC/2 Estimation Technique to Computer-Assisted Planimetric Analysis in Warfarin-Related Intracerebral Parenchymal Hemorrhage Hagen B. Huttner, MD; Thorsten Steiner, MD; Marius Hartmann,
Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective
 Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective Cathy Sila MD George M Humphrey II Professor and Vice Chair of Neurology Director, Comprehensive Stroke Center
Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective Cathy Sila MD George M Humphrey II Professor and Vice Chair of Neurology Director, Comprehensive Stroke Center
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Updated Ischemic Stroke Guidelines นพ.ส ชาต หาญไชยพ บ ลย ก ล นายแพทย ทรงค ณว ฒ สาขาประสาทว ทยา สถาบ นประสาทว ทยา กรมการแพทย กระทรวงสาธารณส ข
 Updated Ischemic Stroke Guidelines นพ.ส ชาต หาญไชยพ บ ลย ก ล นายแพทย ทรงค ณว ฒ สาขาประสาทว ทยา สถาบ นประสาทว ทยา กรมการแพทย กระทรวงสาธารณส ข Emergency start at community level: Prehospital care Acute stroke
Updated Ischemic Stroke Guidelines นพ.ส ชาต หาญไชยพ บ ลย ก ล นายแพทย ทรงค ณว ฒ สาขาประสาทว ทยา สถาบ นประสาทว ทยา กรมการแพทย กระทรวงสาธารณส ข Emergency start at community level: Prehospital care Acute stroke
9/24/2013. Thrombolytics in 2013: Never Say Never. September 19 th, 2013 Scott M Lilly, MD PhD. Clinical Case
 September 19 th, 2013 Scott M Lilly, MD PhD Thrombolytics in 2013: Never Say Never Clinical Case 2 1 Evolution of STEMI Therapy The importance of absolute rest in bed for several days is clear James B
September 19 th, 2013 Scott M Lilly, MD PhD Thrombolytics in 2013: Never Say Never Clinical Case 2 1 Evolution of STEMI Therapy The importance of absolute rest in bed for several days is clear James B
Decompressive Hemicraniectomy in Hypertensive Basal Ganglia Hemorrhages
 Decompressive Hemicraniectomy in Hypertensive Basal Ganglia Hemorrhages Joarder MA 1, Karim AKMB 2, Sujon SI 3, Akhter N 4, Waheeduzzaman M 5, Shankar DR 6, Jahangir SM 7, Chandy MJ 8 Abstract Objectives:
Decompressive Hemicraniectomy in Hypertensive Basal Ganglia Hemorrhages Joarder MA 1, Karim AKMB 2, Sujon SI 3, Akhter N 4, Waheeduzzaman M 5, Shankar DR 6, Jahangir SM 7, Chandy MJ 8 Abstract Objectives:
Journal Club. 1. Develop a PICO (Population, Intervention, Comparison, Outcome) question for this study
 Journal Club Articles for Discussion Tissue plasminogen activator for acute ischemic stroke. The National Institute of Neurological Disorders and Stroke rt-pa Stroke Study Group. N Engl J Med. 1995 Dec
Journal Club Articles for Discussion Tissue plasminogen activator for acute ischemic stroke. The National Institute of Neurological Disorders and Stroke rt-pa Stroke Study Group. N Engl J Med. 1995 Dec
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
Sinus Venous Thrombosis
 Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
Thrombolysis administration
 Thrombolysis administration Liz Mackey Stroke Nurse Practitioner Western Health Sunshine & Footscray Hospital, Melbourne Thanks ASNEN committee members Skye Coote, Acute Stroke Nurse, Eastern Health (slide
Thrombolysis administration Liz Mackey Stroke Nurse Practitioner Western Health Sunshine & Footscray Hospital, Melbourne Thanks ASNEN committee members Skye Coote, Acute Stroke Nurse, Eastern Health (slide
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS. ACUTE CEREBROVASCULAR ACCIDENT TPA (ACTIVASE /alteplase) FOR THROMBOLYSIS
 NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS ACUTE CEREBROVASCULAR ACCIDENT TPA (ACTIVASE /alteplase) FOR THROMBOLYSIS I. Purpose : A. To reduce morbidity and mortality associated
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS ACUTE CEREBROVASCULAR ACCIDENT TPA (ACTIVASE /alteplase) FOR THROMBOLYSIS I. Purpose : A. To reduce morbidity and mortality associated
Primary intracerebral hemorrhage (ICH) is one of the most
 ORIGINAL RESEARCH J. Kim A. Smith J.C. Hemphill III W.S. Smith Y. Lu W.P. Dillon M. Wintermark Contrast Extravasation on CT Predicts Mortality in Primary Intracerebral Hemorrhage BACKGROUND AND PURPOSE:
ORIGINAL RESEARCH J. Kim A. Smith J.C. Hemphill III W.S. Smith Y. Lu W.P. Dillon M. Wintermark Contrast Extravasation on CT Predicts Mortality in Primary Intracerebral Hemorrhage BACKGROUND AND PURPOSE:
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Short Communications. Alcoholic Intracerebral Hemorrhage
 Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
Hypertensive Haemorrhagic Stroke. Dr Philip Lam Thuon Mine
 Hypertensive Haemorrhagic Stroke Dr Philip Lam Thuon Mine Intracerebral Haemorrhage Primary ICH Spontaneous rupture of small vessels damaged by HBP Basal ganglia, thalamus, pons and cerebellum Amyloid
Hypertensive Haemorrhagic Stroke Dr Philip Lam Thuon Mine Intracerebral Haemorrhage Primary ICH Spontaneous rupture of small vessels damaged by HBP Basal ganglia, thalamus, pons and cerebellum Amyloid
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
FVIIa for Acute Hemorrhagic Stroke Administered at Earliest Time (FASTEST) Trial. Joseph P. Broderick, MD James Grotta, MD Jordan Elm, PhD
 FVIIa for Acute Hemorrhagic Stroke Administered at Earliest Time (FASTEST) Trial Joseph P. Broderick, MD James Grotta, MD Jordan Elm, PhD Background Intracerebral hemorrhage (ICH) accounts for more than
FVIIa for Acute Hemorrhagic Stroke Administered at Earliest Time (FASTEST) Trial Joseph P. Broderick, MD James Grotta, MD Jordan Elm, PhD Background Intracerebral hemorrhage (ICH) accounts for more than
Prognostic Value of the Hyperdense Middle Cerebral Artery Sign and Stroke Scale Score before Ultraearly Thrombolytic Therapy
 Prognostic Value of the Hyperdense Middle Cerebral Artery Sign and Stroke Scale Score before Ultraearly Thrombolytic Therapy Thomas Tomsick, Thomas Brott, William Barsan, Joseph Broderick, E. Clarke Haley,
Prognostic Value of the Hyperdense Middle Cerebral Artery Sign and Stroke Scale Score before Ultraearly Thrombolytic Therapy Thomas Tomsick, Thomas Brott, William Barsan, Joseph Broderick, E. Clarke Haley,
The management of ICH when to operate when not to?
 The management of ICH when to operate when not to? Intracranial Hemorrhage High Incidence o Accounts for 10-15% of all strokes 1,2,5 o 80,000 cases in US; 2 million WW 2,5 o Incidence doubles for African-
The management of ICH when to operate when not to? Intracranial Hemorrhage High Incidence o Accounts for 10-15% of all strokes 1,2,5 o 80,000 cases in US; 2 million WW 2,5 o Incidence doubles for African-
Stroke 101. Maine Cardiovascular Health Summit. Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013
 Stroke 101 Maine Cardiovascular Health Summit Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013 Stroke Statistics Definition of stroke Risk factors Warning signs Treatment
Stroke 101 Maine Cardiovascular Health Summit Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013 Stroke Statistics Definition of stroke Risk factors Warning signs Treatment
Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients
 AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
ACCESS CENTER:
 ACCESS CENTER: 1-877-367-8855 Emergency Specialty Services: BRAIN ATTACK Criteria: Stroke symptom onset time less than 6 hours Referring Emergency Department Patient Information Data: Time last known normal:
ACCESS CENTER: 1-877-367-8855 Emergency Specialty Services: BRAIN ATTACK Criteria: Stroke symptom onset time less than 6 hours Referring Emergency Department Patient Information Data: Time last known normal:
When the learner has completed this module, she/he will be able to:
 Thrombolytics and Myocardial Infarction WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017
Thrombolytics and Myocardial Infarction WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD.
 Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
Thrombolytic therapy should be the first line treatment in acute ishchemic stroke. We are against it!!
 Thrombolytic therapy should be the first line treatment in acute ishchemic stroke We are against it!! 85% of strokes are ischaemic, and related to blockage of an artery by a blood clot, so potential treatments
Thrombolytic therapy should be the first line treatment in acute ishchemic stroke We are against it!! 85% of strokes are ischaemic, and related to blockage of an artery by a blood clot, so potential treatments
Protocol for IV rtpa Treatment of Acute Ischemic Stroke
 Protocol for IV rtpa Treatment of Acute Ischemic Stroke Acute stroke management is progressing very rapidly. Our team offers several options for acute stroke therapy, including endovascular therapy and
Protocol for IV rtpa Treatment of Acute Ischemic Stroke Acute stroke management is progressing very rapidly. Our team offers several options for acute stroke therapy, including endovascular therapy and
Prognostic Factors of Motor Recovery after Stereotactic Evacuation of Intracerebral Hematoma
 Tohoku J. Exp. Med., 2012, 227, 63-67Motor Recovery after Stereotactic ICH Evacuation 63 Prognostic Factors of Motor Recovery after Stereotactic Evacuation of Intracerebral Hematoma Rei Enatsu, 1 Minoru
Tohoku J. Exp. Med., 2012, 227, 63-67Motor Recovery after Stereotactic ICH Evacuation 63 Prognostic Factors of Motor Recovery after Stereotactic Evacuation of Intracerebral Hematoma Rei Enatsu, 1 Minoru
The Multi arm Optimization of Stroke Thrombolysis (MOST) Trial
 The Multi arm Optimization of Stroke Thrombolysis (MOST) Trial Study Team Principal Investigators: Opeolu Adeoye, University of Cincinnati (Lead) Andrew Barreto, University of Texas Houston Jim Grotta,
The Multi arm Optimization of Stroke Thrombolysis (MOST) Trial Study Team Principal Investigators: Opeolu Adeoye, University of Cincinnati (Lead) Andrew Barreto, University of Texas Houston Jim Grotta,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
Cerebrovascular diseases-2
 Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS. ACTIVASE (t-pa) INFUSION PROTOCOL FOR ACUTE MYOCARDIAL INFARCTION
 NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS ACTIVASE (t-pa) FOR ACUTE MYOCARDIAL INFARCTION I. PURPOSE: A. To reduce the extent of myocardial infarction by lysing the clot in
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS ACTIVASE (t-pa) FOR ACUTE MYOCARDIAL INFARCTION I. PURPOSE: A. To reduce the extent of myocardial infarction by lysing the clot in
A Report From the Second National Registry of Myocardial Infarction (NRMI-2)
 1240 JACC Vol. 31, No. 6 Clinical Experience With Primary Percutaneous Transluminal Coronary Angioplasty Compared With Alteplase (Recombinant Tissue-Type Plasminogen Activator) in Patients With Acute Myocardial
1240 JACC Vol. 31, No. 6 Clinical Experience With Primary Percutaneous Transluminal Coronary Angioplasty Compared With Alteplase (Recombinant Tissue-Type Plasminogen Activator) in Patients With Acute Myocardial
 www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
Shawke A. Soueidan, MD. Riverside Neurology & Sleep Specialists
 Shawke A. Soueidan, MD Riverside Neurology & Sleep Specialists 757-221-0110 Epidemiology of stroke 2018 Affects nearly 800,000 people in the US annually Approximately 600000 first-ever strokes and 185000
Shawke A. Soueidan, MD Riverside Neurology & Sleep Specialists 757-221-0110 Epidemiology of stroke 2018 Affects nearly 800,000 people in the US annually Approximately 600000 first-ever strokes and 185000
Acute Stroke Protocols Modified- What s New in 2013
 Acute Stroke Protocols Modified- What s New in 2013 KUMAR RAJAMANI, MD, DM. Vascular Neurologist-MSN Associate Professor of Neurology WSU School of Medicine. Saturday, September 21, 2013 Crystal Mountain
Acute Stroke Protocols Modified- What s New in 2013 KUMAR RAJAMANI, MD, DM. Vascular Neurologist-MSN Associate Professor of Neurology WSU School of Medicine. Saturday, September 21, 2013 Crystal Mountain
Acute Stroke Care: the Nuts and Bolts of it. ECASS I and II ATLANTIS. Chris V. Fanale, MD Colorado Neurological Institute Swedish Medical Center
 Acute Stroke Care: the Nuts and Bolts of it Chris V. Fanale, MD Colorado Neurological Institute Swedish Medical Center ECASS I and II tpa for patients presenting
Acute Stroke Care: the Nuts and Bolts of it Chris V. Fanale, MD Colorado Neurological Institute Swedish Medical Center ECASS I and II tpa for patients presenting
Review of the TICH-2 Trial
 Review of the TICH-2 Trial Mikaela Hofer, PharmD PGY-1 Pharmacy Resident Pharmacy Grand Rounds September 18, 2018 2018 MFMER slide-1 Objectives Review the pharmacologic options to limit hematoma expansion
Review of the TICH-2 Trial Mikaela Hofer, PharmD PGY-1 Pharmacy Resident Pharmacy Grand Rounds September 18, 2018 2018 MFMER slide-1 Objectives Review the pharmacologic options to limit hematoma expansion
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
William Barr, M.D. January 28, 2017
 William Barr, M.D. January 28, 2017 Types of Stroke Ischemic Stroke Small vessel (20%) Large vessel (31%) Embolic (32%) Hemorrhagic Intracerebral Hemorrhage (10%) Subarachnoid Hemorrhage (7%) The Majority
William Barr, M.D. January 28, 2017 Types of Stroke Ischemic Stroke Small vessel (20%) Large vessel (31%) Embolic (32%) Hemorrhagic Intracerebral Hemorrhage (10%) Subarachnoid Hemorrhage (7%) The Majority
The Effect of Diagnostic Catheter Angiography on Outcomes of Acute Ischemic Stroke Patients Being Considered for Endovascular Treatment
 The Effect of Diagnostic Catheter Angiography on Outcomes of Acute Ischemic Stroke Patients Being Considered for Endovascular Treatment Adnan I. Qureshi, MD 1, Muhammad A. Saleem, MD 1, Emrah Aytaç, MD
The Effect of Diagnostic Catheter Angiography on Outcomes of Acute Ischemic Stroke Patients Being Considered for Endovascular Treatment Adnan I. Qureshi, MD 1, Muhammad A. Saleem, MD 1, Emrah Aytaç, MD
Effects of Stroke on Medical Resource Use and Costs in Acute Myocardial Infarction
 Effects of Stroke on Medical Resource Use and Costs in Acute Myocardial Infarction Chen Y. Tung, MD; Christopher B. Granger, MD; Michael A. Sloan, MD; Eric J. Topol, MD; J. David Knight, MS; W. Douglas
Effects of Stroke on Medical Resource Use and Costs in Acute Myocardial Infarction Chen Y. Tung, MD; Christopher B. Granger, MD; Michael A. Sloan, MD; Eric J. Topol, MD; J. David Knight, MS; W. Douglas
11/27/2017. Stroke Management in the Neurocritical Care Unit. Conflict of interest. Karel Fuentes MD Medical Director of Neurocritical Care
 Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Conflict of interest None Introduction Reperfusion therapy remains the mainstay in the treatment
Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Conflict of interest None Introduction Reperfusion therapy remains the mainstay in the treatment
Intracranial Hemorrhage. Objectives. What Do Need to Know?
 Intracranial Hemorrhage What Do Need to Know? Kerry Brega, MD Associate Professor of Neurosurgery University of Colorado Objectives Know the common types of ICH. Know how they can be differentiated. Know
Intracranial Hemorrhage What Do Need to Know? Kerry Brega, MD Associate Professor of Neurosurgery University of Colorado Objectives Know the common types of ICH. Know how they can be differentiated. Know
11/23/2015. Disclosures. Stroke Management in the Neurocritical Care Unit. Karel Fuentes MD Medical Director of Neurocritical Care.
 Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Disclosures I have no relevant commercial relationships to disclose, and my presentations will not
Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Disclosures I have no relevant commercial relationships to disclose, and my presentations will not
Dating Neurological Injury
 Dating Neurological Injury wwwwwwwww Jeff L. Creasy Dating Neurological Injury A Forensic Guide for Radiologists, Other Expert Medical Witnesses, and Attorneys Jeff L. Creasy Associate Professor of Neuroradiology
Dating Neurological Injury wwwwwwwww Jeff L. Creasy Dating Neurological Injury A Forensic Guide for Radiologists, Other Expert Medical Witnesses, and Attorneys Jeff L. Creasy Associate Professor of Neuroradiology
Managing the Measures: A Serious Look at Key Abstraction Concepts for the Comprehensive Stroke (CSTK) Measure Set Session 2
 Managing the Measures: A Serious Look at Key Abstraction Concepts for the Comprehensive Stroke (CSTK) Measure Set Session 2 January 28, 2015 1 to 3 PM Central Time Continuing Education Credit This course
Managing the Measures: A Serious Look at Key Abstraction Concepts for the Comprehensive Stroke (CSTK) Measure Set Session 2 January 28, 2015 1 to 3 PM Central Time Continuing Education Credit This course
Intracerebral hemorrhage (ICH) is associated with poor outcome,
 Low Serum Calcium Levels Contribute to Larger Hematoma Volume in Acute Intracerebral Hemorrhage Yasuteru Inoue, MD; Fumio Miyashita, MD; Kazunori Toyoda, MD; Kazuo Minematsu, MD Downloaded from http://stroke.ahajournals.org/
Low Serum Calcium Levels Contribute to Larger Hematoma Volume in Acute Intracerebral Hemorrhage Yasuteru Inoue, MD; Fumio Miyashita, MD; Kazunori Toyoda, MD; Kazuo Minematsu, MD Downloaded from http://stroke.ahajournals.org/
The restoration of coronary flow after an
 Pharmacological Reperfusion in Acute Myicardial Infarction after ASSENT 3 and GUSTO V [81] DANIEL FERREIRA, MD, FESC Serviço de Cardiologia, Hospital Fernando Fonseca, Amadora, Portugal Rev Port Cardiol
Pharmacological Reperfusion in Acute Myicardial Infarction after ASSENT 3 and GUSTO V [81] DANIEL FERREIRA, MD, FESC Serviço de Cardiologia, Hospital Fernando Fonseca, Amadora, Portugal Rev Port Cardiol
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases
 How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Clinical Analysis of Risk Factors Affecting Rebleeding in Patients with an Aneurysm. Gab Teug Kim, M.D.
 / 119 = Abstract = Clinical Analysis of Risk Factors Affecting Rebleeding in Patients with an Aneurysm Gab Teug Kim, M.D. Department of Emergency Medicine, College of Medicine, Dankook University, Choenan,
/ 119 = Abstract = Clinical Analysis of Risk Factors Affecting Rebleeding in Patients with an Aneurysm Gab Teug Kim, M.D. Department of Emergency Medicine, College of Medicine, Dankook University, Choenan,
Perihematomal Edema and Functional Outcomes in Intracerebral Hemorrhage Influence of Hematoma Volume and Location
 Perihematomal Edema and Functional Outcomes in Intracerebral Hemorrhage Influence of Hematoma Volume and Location Santosh B. Murthy, MD, MPH; Yogesh Moradiya, MD; Jesse Dawson, MD; Kennedy R. Lees, MD;
Perihematomal Edema and Functional Outcomes in Intracerebral Hemorrhage Influence of Hematoma Volume and Location Santosh B. Murthy, MD, MPH; Yogesh Moradiya, MD; Jesse Dawson, MD; Kennedy R. Lees, MD;
Complications of Thrombolysis
 Complications of Thrombolysis David H. Jang, M.D. Lewis S. Nelson, M.D. Case Summary: An 88 year-old man with a past medical history of hypertension and paroxysmal atrial fibrillation presented to the
Complications of Thrombolysis David H. Jang, M.D. Lewis S. Nelson, M.D. Case Summary: An 88 year-old man with a past medical history of hypertension and paroxysmal atrial fibrillation presented to the
Use of the Original, Modified, or New Intracerebral Hemorrhage Score to Predict Mortality and Morbidity After Intracerebral Hemorrhage
 Use of the Original, Modified, or New Intracerebral Hemorrhage Score to Predict Mortality and Morbidity After Intracerebral Hemorrhage Raymond Tak Fai Cheung, MBBS, PhD; Liang-Yu Zou, MBBS, MPhil Background
Use of the Original, Modified, or New Intracerebral Hemorrhage Score to Predict Mortality and Morbidity After Intracerebral Hemorrhage Raymond Tak Fai Cheung, MBBS, PhD; Liang-Yu Zou, MBBS, MPhil Background
Update in Management of Acute Spontaneous Intracerebral Haemorrhage
 Update in Management of Acute Spontaneous Intracerebral Haemorrhage Aldy S. Rambe Neurology Department, School of Medicine EPIDEMIOLOGY Although ICH represents only about 9% of all stroke, it accounts
Update in Management of Acute Spontaneous Intracerebral Haemorrhage Aldy S. Rambe Neurology Department, School of Medicine EPIDEMIOLOGY Although ICH represents only about 9% of all stroke, it accounts
Correlation between Intracerebral Hemorrhage Score and surgical outcome of spontaneous intracerebral hemorrhage
 Bangladesh Med Res Counc Bull 23; 39: -5 Correlation between Intracerebral Hemorrhage Score and surgical outcome of spontaneous intracerebral hemorrhage Rashid HU, Amin R, Rahman A, Islam MR, Hossain M,
Bangladesh Med Res Counc Bull 23; 39: -5 Correlation between Intracerebral Hemorrhage Score and surgical outcome of spontaneous intracerebral hemorrhage Rashid HU, Amin R, Rahman A, Islam MR, Hossain M,
Modern Management of ICH
 Modern Management of ICH Bradley A. Gross, MD Assistant Professor, Dept of Neurosurgery, University of Pittsburgh October 2018 ICH Background Assessment & Diagnosis Medical Management Surgical Management
Modern Management of ICH Bradley A. Gross, MD Assistant Professor, Dept of Neurosurgery, University of Pittsburgh October 2018 ICH Background Assessment & Diagnosis Medical Management Surgical Management
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
Lothian Audit of the Treatment of Cerebral Haemorrhage (LATCH)
 1. INTRODUCTION Stroke physicians, emergency department doctors, and neurologists are often unsure about which patients they should refer for neurosurgical intervention. Early neurosurgical evacuation
1. INTRODUCTION Stroke physicians, emergency department doctors, and neurologists are often unsure about which patients they should refer for neurosurgical intervention. Early neurosurgical evacuation
framework for flow Objectives Acute Stroke Treatment Collaterals in Acute Ischemic Stroke framework & basis for flow
 Acute Stroke Treatment Collaterals in Acute Ischemic Stroke Objectives role of collaterals in acute ischemic stroke collateral therapeutic strategies David S Liebeskind, MD Professor of Neurology & Director
Acute Stroke Treatment Collaterals in Acute Ischemic Stroke Objectives role of collaterals in acute ischemic stroke collateral therapeutic strategies David S Liebeskind, MD Professor of Neurology & Director
Insertion of an external ventricular drain (EVD) is a
 Short Communication Intracerebral Hemorrhage With Severe Ventricular Involvement Lumbar Drainage for Communicating Hydrocephalus Hagen B. Huttner, MD; Simon Nagel, MD; Elena Tognoni; Martin Köhrmann, MD;
Short Communication Intracerebral Hemorrhage With Severe Ventricular Involvement Lumbar Drainage for Communicating Hydrocephalus Hagen B. Huttner, MD; Simon Nagel, MD; Elena Tognoni; Martin Köhrmann, MD;
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery
 Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Primary Stroke Center Acute Stroke Transfer Guidelines When to Consider a Transfer:
 When to Consider a Transfer: Hemorrhagic Stroke Large volume intracerebral hematoma greater than 5cm on CT Concern for expanding hematoma Rapidly declining mental status, especially requiring intubation
When to Consider a Transfer: Hemorrhagic Stroke Large volume intracerebral hematoma greater than 5cm on CT Concern for expanding hematoma Rapidly declining mental status, especially requiring intubation
Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital
 ISPUB.COM The Internet Journal of Neurosurgery Volume 9 Number 2 Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital A Granger, R Laherty Citation A Granger, R Laherty.
ISPUB.COM The Internet Journal of Neurosurgery Volume 9 Number 2 Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital A Granger, R Laherty Citation A Granger, R Laherty.
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Intracerebral hemorrhage (ICH) is the most fatal form of
 Hematoma Growth and Outcome in Treated Neurocritical Care Patients With Intracerebral Hemorrhage Related to Oral Anticoagulant Therapy Comparison of Acute Treatment Strategies Using Vitamin K, Fresh Frozen
Hematoma Growth and Outcome in Treated Neurocritical Care Patients With Intracerebral Hemorrhage Related to Oral Anticoagulant Therapy Comparison of Acute Treatment Strategies Using Vitamin K, Fresh Frozen
Advances in Neuro-Endovascular Care for Acute Stroke
 Advances in Neuro-Endovascular Care for Acute Stroke Ciarán J. Powers, MD, PhD, FAANS Associate Professor Program Director Department of Neurological Surgery Surgical Director Comprehensive Stroke Center
Advances in Neuro-Endovascular Care for Acute Stroke Ciarán J. Powers, MD, PhD, FAANS Associate Professor Program Director Department of Neurological Surgery Surgical Director Comprehensive Stroke Center
Intracranial spontaneous hemorrhage mechanisms, imaging and management
 Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
New Clinical Trials For ICH: MISTIE III Minimally invasive techniques for hemorrhagic stroke
 New Clinical Trials For ICH: MISTIE III Minimally invasive techniques for hemorrhagic stroke 1 Wendy Ziai, MD, MPH Daniel F. Hanley, MD Johns Hopkins Medical Institutions Dept. of Neurology Division of
New Clinical Trials For ICH: MISTIE III Minimally invasive techniques for hemorrhagic stroke 1 Wendy Ziai, MD, MPH Daniel F. Hanley, MD Johns Hopkins Medical Institutions Dept. of Neurology Division of
Keyhole craniectomy in the surgical management of spontaneous intracerebral hematoma
 Neurology Asia 2007; 12 : 21 27 Keyhole craniectomy in the surgical management of spontaneous intracerebral hematoma S Balaji Pai, RG Varma, JKBC Parthiban, KN Krishna, RM Varma, *R Srinivasa,*PT Acharya,*BP
Neurology Asia 2007; 12 : 21 27 Keyhole craniectomy in the surgical management of spontaneous intracerebral hematoma S Balaji Pai, RG Varma, JKBC Parthiban, KN Krishna, RM Varma, *R Srinivasa,*PT Acharya,*BP
Neurosurgical Management of Stroke
 Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Building a Stroke Portfolio. June 28, 2018
 Building a Stroke Portfolio June 28, 2018 1 Forward-Looking Statements This presentation contains forward-looking statements, including statements relating to: the potential benefits, safety and efficacy
Building a Stroke Portfolio June 28, 2018 1 Forward-Looking Statements This presentation contains forward-looking statements, including statements relating to: the potential benefits, safety and efficacy
Canadian Best Practice Recommendations for Stroke Care. (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management
 Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS. Justin Nolte, MD Assistant Profession Marshall University School of Medicine
 ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS Justin Nolte, MD Assistant Profession Marshall University School of Medicine History of Presenting Illness 64 yo wf with PMHx of COPD, HTN, HLP who was in
ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS Justin Nolte, MD Assistant Profession Marshall University School of Medicine History of Presenting Illness 64 yo wf with PMHx of COPD, HTN, HLP who was in
Neurocritical Care. Inaugural Issue. Eelco F.M. Wijdicks, MD. HumanaJournals.com. Editor-in-Chief: Search, Read, and Download
 Inaugural Issue Neurocritical Care Volume 1 Number 1 2004 ISSN 1541 6933 A Journal of Acute and Emergency Care Editor-in-Chief: Eelco F.M. Wijdicks, MD The Official Journal of the www.neurocriticalcare.org
Inaugural Issue Neurocritical Care Volume 1 Number 1 2004 ISSN 1541 6933 A Journal of Acute and Emergency Care Editor-in-Chief: Eelco F.M. Wijdicks, MD The Official Journal of the www.neurocriticalcare.org
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
ACUTE ISCHEMIC STROKE. Current Treatment Approaches for Acute Ischemic Stroke
 ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
COMPREHENSIVE SUMMARY OF INSTOR REPORTS
 COMPREHENSIVE SUMMARY OF INSTOR REPORTS Please note that the following chart provides a sampling of INSTOR reports to differentiate this registry s capabilities as a process improvement system. This list
COMPREHENSIVE SUMMARY OF INSTOR REPORTS Please note that the following chart provides a sampling of INSTOR reports to differentiate this registry s capabilities as a process improvement system. This list
ENCHANTED Era: Is it time to rethink treatment of acute ischemic stroke? Kristin J. Scherber, PharmD, BCPS Emergency Medicine Clinical Pharmacist
 ENCHANTED Era: Is it time to rethink treatment of acute ischemic stroke? Kristin J. Scherber, PharmD, BCPS Emergency Medicine Clinical Pharmacist Pharmacy Grand Rounds 26 July 2016 2015 MFMER slide-1 Learning
ENCHANTED Era: Is it time to rethink treatment of acute ischemic stroke? Kristin J. Scherber, PharmD, BCPS Emergency Medicine Clinical Pharmacist Pharmacy Grand Rounds 26 July 2016 2015 MFMER slide-1 Learning
Updated tpa Guidelines: Expanding the opportunity for good outcomes. Benjamin Morrow, MSN RN UPMC Stroke Institute
 Updated tpa Guidelines: Expanding the opportunity for good outcomes Benjamin Morrow, MSN RN UPMC Stroke Institute 1 Outline History Current State Review Exclusions: Minor stroke symptoms Severe strokes
Updated tpa Guidelines: Expanding the opportunity for good outcomes Benjamin Morrow, MSN RN UPMC Stroke Institute 1 Outline History Current State Review Exclusions: Minor stroke symptoms Severe strokes
Use of CT in minor traumatic brain injury. Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD
 Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Hypertensive Caudate Hemorrhage Prognostic Predictor, Outcome, and Role of External Ventricular Drainage
 Hypertensive Caudate Hemorrhage Prognostic Predictor, Outcome, and Role of External Ventricular Drainage Po-Chou Liliang, MD; Cheng-Loong Liang, MD; Cheng-Hsien Lu, MD; Hsueh-Wen Chang, PhD; Ching-Hsiao
Hypertensive Caudate Hemorrhage Prognostic Predictor, Outcome, and Role of External Ventricular Drainage Po-Chou Liliang, MD; Cheng-Loong Liang, MD; Cheng-Hsien Lu, MD; Hsueh-Wen Chang, PhD; Ching-Hsiao
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Mechanical thrombectomy in Plymouth. Will Adams. Will Adams
 Mechanical thrombectomy in Plymouth Will Adams Will Adams History Intra-arterial intervention 1995 (NINDS) iv tpa improved clinical outcome in patients treated within 3 hours of ictus but limited recanalisation
Mechanical thrombectomy in Plymouth Will Adams Will Adams History Intra-arterial intervention 1995 (NINDS) iv tpa improved clinical outcome in patients treated within 3 hours of ictus but limited recanalisation
The epidemiology of intracerebral hemorrhage
 Section 1 Chapter 1 Epidemiology The epidemiology of intracerebral hemorrhage Matthew L. Flaherty, Daniel Woo, and Joseph P. Broderick Introduction Advances in brain imaging have dramatically changed our
Section 1 Chapter 1 Epidemiology The epidemiology of intracerebral hemorrhage Matthew L. Flaherty, Daniel Woo, and Joseph P. Broderick Introduction Advances in brain imaging have dramatically changed our
Advances in critical care/emergency medicine 2013
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Advances in critical care/emergency medicine 2013 Keller, Emanuela; Becker,
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Advances in critical care/emergency medicine 2013 Keller, Emanuela; Becker,
Sensitivity and Specificity of Fluid-Blood Levels for Coagulopathy in Acute Intracerebral Hematomas
 Sensitivity and Specificity of Fluid-Blood Levels for Coagulopathy in Acute Intracerebral Hematomas Mark J. Pfleger, Eric P. Hardee, Charles F. Contant, Jr., and L. Anne Hayman PURPOSE: To characterize
Sensitivity and Specificity of Fluid-Blood Levels for Coagulopathy in Acute Intracerebral Hematomas Mark J. Pfleger, Eric P. Hardee, Charles F. Contant, Jr., and L. Anne Hayman PURPOSE: To characterize
Hypothermia Reduces Perihemorrhagic Edema After Intracerebral Hemorrhage
 Hypothermia Reduces Perihemorrhagic Edema After Intracerebral Hemorrhage Rainer Kollmar, MD*; Dimitre Staykov, MD*; Arnd Dörfler, MD; Peter D. Schellinger, MD; Stefan Schwab, MD; Jürgen Bardutzky, MD Background
Hypothermia Reduces Perihemorrhagic Edema After Intracerebral Hemorrhage Rainer Kollmar, MD*; Dimitre Staykov, MD*; Arnd Dörfler, MD; Peter D. Schellinger, MD; Stefan Schwab, MD; Jürgen Bardutzky, MD Background
