Stephanie Banfield. 1. Frontal Lobe Controls: Behaviour Emotions Organisation Personality Planning Problem solving Arteries: ACA, MCA. 5.
|
|
|
- Milton Riley
- 5 years ago
- Views:
Transcription
1
2
3 1. Frontal Lobe Controls: Behaviour Emotions Organisation Personality Planning Problem solving Arteries: ACA, MCA 2. Parietal Lobe Controls: Judgement of shape,size,texture, and weight The sensation of pressure and touch Understanding of spoken/written language Arteries: ACA, MCA 3. Occipital Lobe Controls: Colour recognition Shape recognition Arteries: PCA Cerebellum Controls: Balance Muscle co-ordination Posture maintenance Arteries: Basilar PICA, AICA, SCA ACA = Anterior Cerebral Artery MCA = Middle Cerebral Artery PCA = Posterior Cerebral Artery PICA = Posterior Inferior Cerebellar Artery AICA = Anterior Inferior Cerebellar Artery SCA = Superior Cerebellar Artery Brainstem Controls: Alertness Blood pressure Digestion Breathing Heart rate Arteries: Vertebral Basilar 6. Hippocampus Controls: Object recognition Stores meaning of words or places Arteries: PCA 7. Temporal lobe Controls: Smell Identification Sound Identification Short-term Memory Hearing Arteries: MCA, PCA
4 Speech centres Broca; control the muscles of the larynx, pharynx and mouth that enable us to speak Wernicke s area, injury here may result in receptive dysphasia.
5 Contra-lateral Control
6 Blood Supply to the Brain
7 Stroke and Aetiology interruption of the blood supply to the brain, caused by a blocked or burst blood vessel cuts off the supply of oxygen and nutrients, causing damage to the brain tissue. (World Health Organisation 2010) Cerebral infarction/ischaemic 81% Intracerebral haemorrhage 13% Subarachnoid haemorrhage 6% Risk of recurrence within 5 years 30-40% (Stroke Association 2010)
8 Stroke What do you do if you think your patient is having a stroke?
9 Lacunar Stroke
10 Ischemic stroke (Thrombo/embolic stroke) hypercholesterolemia hypertension Atrial fibrillation Ischaemic heart disease/angina Peripheral vascular disease Diabetes
11 Previous stroke/tia Smoking Increased alcohol intake Poor diet/obesity Increased ageatherosclerosis Oral Contraceptive Pill Drug misuse
12 Haemorrhagic Stroke Chronic high blood pressure. Amphetamine. Amyloid angiopathy Arterial Venous malformation (AVM), inflammation of blood vessels (vasculitis), bleeding disorders, anticoagulants,
13 Intracerebral and subarachnoid haemorrhage
14 Subdural haemorrhage and small vessel disease
15 Subdural Haematoma A subdural hematoma (American spelling) or subdural haematoma (British spelling), also known as a subdural haemorrhage (SDH), is a type of haematoma, usually associated with traumatic brain injury. Blood gathers between the dura mater, and the brain. Usually resulting from tears in bridging veins which cross the subdural space, subdural hemorrhages may cause an increase in intracranial pressure (ICP), which can cause compression of and damage to delicate brain tissue. Subdural hematomas are often lifethreatening when acute. Chronic subdural hematomas, however, have a better prognosis if properly managed.
16 Raised Intracranial Pressure Early Signs Later Signs Agitation Vomiting Headache Dilated pupils Increased systolic blood pressure Bradicardia Abnormal respiratory pattern
17 Causes and Treatment Causes Treatment Oedema Steroids Haemorrhage Manitol Tumour Hyperventilation Encephalopathy Hemicraniectomy
18 Hemicraniectomy
19 Neurological Assessment AVPU what does this mean? Blood sugar Pupils Then move onto GCS and full neuro assessment
20 Neurological assessment Why perform a neurological assessment? The reasons to perform a neurological assessment include: 1. Identify the presence of nervous system dysfunction 2. Detect life-threatening situations 3. Establish a neurological baseline for the patient 4. Compare data to previous assessments to determine change, trends and necessary interventions 5. Determine the effects of nervous system dysfunction on activities of daily living and independent function 6. Provide a database upon which nursing interventions will be implemented.
21 The Glasgow Coma Scale The GCS evaluates three key categories of behaviour that most closely reflect activity in the higher centres of the brain: eye opening, verbal response and motor response (Waterhouse, 2005). These categories enable the MDT to determine whether the patient has cerebral dysfunction. Within each category, each level of response is attributed a numerical value. The lower the value, the greater the neurological deterioration and resulting brain insult. A Coma Score of 13 or higher correlates with a mild brain injury, 9 to 12 is a moderate injury and 8 or less a severe brain injury. The lowest possible score is 3 which indicates that the patient is completely unresponsive. The aim of the GCS, is to get a firm baseline for comparison. Without this, you will be unable to recognise deterioration in the patient s neurological condition and will not be able to react appropriately.
22 Illustration of GCS
23 Eye Opening The assessment of whether the patient is eye opening shows that the arousal mechanisms in the brain stem are functioning and also demonstrates that the reticular activating system (RAS) has been stimulated. Eye opening spontaneously = 4 This is recorded when the patient is seen to be awake, with their eyes open. The patient should not need to be roused with either speech or touch. Eye opening to verbal command = 3 This should be achieved without touching the patient. Speak to the patient in a normal voice at first, then, if necessary, gradually raise the volume of your voice. They may respond better to a familiar family voice. Eye opening to pain = 2 To avoid distressing the individual, initially simply touch or shake their shoulder. If this illicits no response, deeper stimulus is required. At this stage it is recommended to use peripheral stimulation, as central painful stimulus is likely to make the patient grimace and screw their eyes shut. Apply pressure, using a pen, to the lateral outer aspect of the second or third finger. Pain should be applied gradually and last no more than 10 seconds. Under no circumstances should sternal rubbing or nail-bed pressure be used.
24 Eye Opening No eye opening = 1 This should be recorded when there is no response to a painful stimulus the nurse should be satisfied that adequate stimulation has been applied. Points to note if the patients eyes are closed as a result of swelling, this is recorded as C on the chart. If the patient has been diagnosed as being in a persistent vegetative state, they may still open their eyes and track movement, but they will not be aware of themselves or their environment.
25 Eye Opening Spontaneous Observed before you approach the patient or speak to him To speech Call the patient s name To pain None Apply pressure to the side of the finger (central stimulus to supraorbital nerve will cause grimacing and eye closure) Ensure painful stimuli is adequate
26 Verbal Response This provides the nurse with information about the patient s speech, understanding and functioning areas of the higher, cognitive centres of the brain. It also reflects the patient s ability to express a reply and illustrates whether they are aware of themselves and their environment. Orientated = 5 The patient should be able to tell you who they are, where they are and the current year and month. If ALL three questions are answered correctly, they may be classed as orientated. Confused = 4 If one or more of the questions is answered incorrectly, he patient must be recorded as confused. Typically, a patient who is deteriorating will lose orientation to time, place and person, in that order. Words = 3 Understandable conversation is absent or limited. Patients will offer words, rather than sentences, which make little sense in the context of the question. Often these words will be obscenities.
27 Verbal Response Incomprehensible sounds = 2 Although the patient s response may follow questioning, sounds are more often made in response to a painful stimulus. The patient may only be able to produce moaning, groaning or crying sounds. If the patient has sustained damage to the speech centres in the brain and is alert and awake but unable to talk, it must still be recorded as sounds. No verbal response = 1 The patient is unable to produce any speech or sounds in response to speech or painful stimuli. Points to note: If the patient has a tracheostomy or endotracheal tube, this should be recorded as a T on the chart. If the patient is dysphasic, this should be recorded on the chart as D Cannot get 15 as a score!!
28 Verbal Response Orientated Confused Knows time, place, person should know who he is, where he is and why he is there and know the month, year, season. If patient answers one or more component incorrectly then he must be recorded as confused. Talking in sentences but disorientated to time and place. Inappropriate words Incomprehensible sounds Utters occasional words rather than sentences these are often abusive words elicited by noxious stimuli rather than spontaneous Groans or grunts None If the patient has and ET tube or tracheostomy T is recorded in this section
29 Motor Response This tests the area of the brain which identifies sensory input and translates this into a motor response. The best response is recorded as an indication of the functional state of the brain as a whole. The best possible result is the ability to obey simple commands convincingly. Upper limb response is recorded as these are more reliable than lower limb responses that could be reflexes. How to test arms Extend the index and middle fingers of both your hands and ask the patient to squeeze. The grasp should be firm and equal on both sides. Ask the patient to release their grip, let go some patients with brain injury can show an involuntary grip response when something is placed in the palm of their hand.
30 Motor Response Obeys commands = 6 The patient can respond to instructions accurately. It is worth asking the patient to perform several other movement, for example, stick out their tongue, show their teeth or raise their eyebrows. It is a good idea to make the patient obey at least two different commands or at least the same command twice. Localising to pain = 5 This is a response to a central painful stimulus. It involves the higher centres of the brain recognising that something is hurting and trying to remove the source of the pain. A painful stimulus should only be used if the patient is not responding to verbal instructions. To be classified as localisation, the patient must move their hands up to the point of stimulation, bringing their hands up towards the chin, across the midline, in an obvious co-ordinated effort to remove the source of pain. If the patient is already localising, for example, to a nasogastric tube or oxygen mask, then painful stimulus need not be applied.
31 Motor Response Painful stimulus can be: Supra-orbital pressure AVOID in patients who have suspected or known facial fractures and those who have a vagal nerve sensitivity Jaw margin pressure AVOID Sternal Rub AVOID Trapezius squeeze Other methods of painful stimulus are not recommended as they can elicit a peripheral reflex response only. Withdrawal from or flexing to pain = 4 In response to a central painful stimulus, the patient will flex or bend their arms at the elbow towards the source of pain, but will not attempt to remove it.
32 Motor Response Abnormal flexion to pain = 3 Also known as decorticate posturing and is a much slower response to painful stimuli. It can be recognised by the flexing of the upper arms and rotating the wrist. The thumb will often come through the fingers. This is an abnormal response and occurs when there is an interruption in the motor nerve pathway between the cortex of the brain and the brain stem. Extension to pain = 2 Also known as decerebrate posturing. This is a very serious sign, with a poor prognosis. It indicates that there is damage to the brainstem. It is characterised by straightening of the elbow and internal rotation of the shoulder and wrist. Often the legs will also extend, with the toes pointing downwards. No motor response = 1 The patient will not move at all in response to a painful stimulus. This indicates that the patient s brain is incapable of processing any sensory input or motor activity. Ensure that you have applied an adequate amount of stimulus Points to note: Always record the best arm response using a central painful stimulus. You are not testing the spinal response at this stage, you are testing the brain. Spinal reflexes can even occur in patients who have been certified as brainstem dead.
33 Motor Response Obeys commands Localises to pain Flexes to pain Hold up your arms, if asking patients to squeeze hands beware of grasp reflex in unconscious patients Apply painful stimulus to trapezius until a response is observed. If the patient responds by bringing up the hand to the chin or above this is localising Elbow bending is recorded as flexing to pain Abnormal flexion to pain Elbow flexion accompanied by a spastic flexion of the wrist Extension to pain Straightening of the elbow is recorded as extending to pain None Ensure stimulus is adequate
34 Limb assessment Evaluation of the limbs provides the nurse with detail of the geographical distribution of dysfunction and is important when performing a full neurological assessment of the patient. A difference in responsiveness in one limb compared to another indicates focal brain damage. Hemiparesis or hemiplegia usually occurs in the limbs on the opposite side to the lesion (due to the crossing over of nerve fibres in the medulla). However, it may also affect the limbs on the same side as the lesion due to the pressure on the contra lateral hemisphere
35 How to test limbs Each limb should be assessed separately. The patient should be awake, able to cooperate and understand what you are asking them to do. Have the patient flex and extend their arm against your hand, squeeze your fingers, lift their leg while you press down on their thigh, hold her leg straight and lift it against gravity, and flex and extend her foot against your hand. A peripheral stimulus needs to be applied to limbs that you have not seen move. As part of the motor assessment, also check for arm pronation or drift. Have the patient hold her arms out in front of her with her palms facing the ceiling, eyes closed. If you observe pronation a turning inward of the palm or the arm or the arm drifts downward, it means the limb is weak.
36 Grading of motor function Grade each extremity using a motor scale like the one below full ROM, full strength +4 - full ROM, less than normal strength +3 - can raise extremity but not against resistance +2 - can move extremity but not lift it +1 - slight movement 0 - no movement
37 Pupil assessment Pupil reaction is a very important observation and is often the only way to assess the neurological status of the sedated patient. Pupils should be round, equal in size and between 2 and 5mm in diameter. Abnormal shaped pupils may be a sign of brain damage, but they may also be due to a previous eye injury or because of cataracts. Any changes to pupil reaction, shape and size can be a late sign of raised ICP. Sluggish or suddenly dilated, unequal pupils are an indication that the oculomotor cranial nerve is being compressed through the foramen magnum. The patient will need urgent intervention at this stage. Any changes must be reported to the medical team, as this is a medical emergency.
38 How to test Pupils Explain to the patient what you are about to do. Wash your hands thoroughly. Note as a baseline the shape, size and equality of the pupils. Move a light from the outer aspect of the eye towards the pupil and withdraw it. This should cause the pupil to constrict quickly and redilate. Note the reaction of the untested pupil also the untested pupil will also have a reaction to the light, but less briskly, this is called consensual light reflex. Repeat on the other side. Record unusual eye movements, such as nystagmus or deviation to the side. Briskly reactive pupils are recorded as +, unreactive pupils as - and sluggishly reactive pupils as S. Points to note: If eyes are closed due to gross orbital swelling, this should be marked as C on the chart. A bright pen torch should be used. Minor inequalities in the size of the pupils is normal. The use of eye drops, such as Atropine, can dilate the pupils.
39 Size Appearance Causes Pinpoint Pupil so small it is barely visible Opiate overdose; pontine haemorrhage Small Smaller than average, larger than pinpoint Bright room; opiates; pontine haemorrhage; metabolic coma Midposition Pupil & iris observed, about half of their diameter is iris & half is pupil Seen normally; if unreactive, midbrain damage is indicated Large Pupils are larger than average Dark room; amphetamines; orbital injuries Dilated Pupil & iris observed, but pupil enlarged with iris barely visible Abnormal; terminal stage of sever anoxiaischaemia or death
40 Vital signs Temperature Regulation may be disrupted due to damage to the hypothalamus In the acute phase of brain injury hyperthermia should be treated as it will exacerbate cerebral ischaemia and adversely affect outcome Heart rate ECG changes may occur in the acute stage following cerebral insult as a result of catecholamine release These can include peaked P waves, prolonged QT interval, heightened T waves, ST segment elevation or depression Bradycardia is present in the later stages of raised ICP (compensatory phase Cushing s response) or when there is an associated cervical spine injury. Tachycardia is present in the terminal stage of raised ICP Arrhythmias are seen in posterior fossa lesions or when there is blood in the CSF
41 Vital signs Blood pressure In a normal brain a fall in blood pressure does not cause a drop in cerebral perfusion pressure since autoregulation results in cerebral vasodilation to protect brain tissue. However, following cerebral insult/injury, when autoregulation may be impaired, hypotension may lead to brain ischaemia. Hypotension (systolic BP <90mmHg) has been identified as a predominant factor in secondary brain injury and is related to morbidity and mortality. Hypotension is associated with a rising ICP and is part of the Cushing s response rising BP with a widening pulse pressure, bradycardia and decreasing respirations. This is a late response and may not appear in some patients and is invariably preceded by a drop in GCS.
42 Vital signs Respiration Changes in the respiratory pattern are common following cerebral insult and patients often require advanced respiratory support in the acute stage. Initially an acute rise in ICP will cause slowing of the respiratory rate indicating loss of all cerebral and cerebellar control of breathing, with respiratory function at only brain stem level As ICP continues to rise the rate becomes rapid indicating that the brain stem is affected too. A decreased level of consciousness may compromise respiratory function, therefore observe for potential airway problems Irregular pattern Noisy or snoring respirations Use of accessory muscles Tacypnoea/dyspnoea/apnoea
43 GCS...DONT FORGET Score the patient as you see them no guessing or backdating the results If they do not meet one criteria move down the score to the next one Always start the assessment with the patient as awake as possible (even at 2am)
44 GCS...DONT FORGET If patient looks different to the GCS scoring do a set of obs together at hand over Consistency with using the neuro. Obs is vital to detecting changes in the patients Don t forget to spot other changes like increasing confusion even if the GCS hasn t yet changed
45 GCS...DONT FORGET Patterns of change in GCS Dropping obviously! Fluctuating widely could it represent seizure (sub-clinically) Increasing difficulty in obtaining the same GCS Small changes within the category e.g. confused but worsening confusion, obeys some commands but not others
Neurological assessment
 Article 481. Shah S (1999) Neurological assessment. Nursing Standard. 13, 22, 49-56. This article relates to the UKCC Professional Development categories: Care enhancement and Reducing risk. Neurological
Article 481. Shah S (1999) Neurological assessment. Nursing Standard. 13, 22, 49-56. This article relates to the UKCC Professional Development categories: Care enhancement and Reducing risk. Neurological
Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology
 Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology Activity Everyone stand up, raise your right hand, tell your neighbors your name 1 What part of the brain
Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology Activity Everyone stand up, raise your right hand, tell your neighbors your name 1 What part of the brain
Neurocritical Care Basics. Tapan Kavi, MD Christina Fox, RN
 Neurocritical Care Basics Tapan Kavi, MD Christina Fox, RN GOAL 1: DON T LET THE PATIENT DIE Not unique ACLS, ATLS, ENLS, other strategies common to all emergency medical care ABCs MORE not less important
Neurocritical Care Basics Tapan Kavi, MD Christina Fox, RN GOAL 1: DON T LET THE PATIENT DIE Not unique ACLS, ATLS, ENLS, other strategies common to all emergency medical care ABCs MORE not less important
8th Annual NKY TBI Conference 3/28/2014
 Closed Head Injury: Headache to Herniation A N T H O N Y T. K R A M E R U N I V E R S I T Y O F C I N C I N N A T I B L U E A S H E M S T E C H N O L O G Y P R O G R A M Objectives Describe the pathological
Closed Head Injury: Headache to Herniation A N T H O N Y T. K R A M E R U N I V E R S I T Y O F C I N C I N N A T I B L U E A S H E M S T E C H N O L O G Y P R O G R A M Objectives Describe the pathological
10/6/2017. Notice. Traumatic Brain Injury & Head Trauma
 Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Head Trauma Inservice (October)
 John Tramell - Head Trauma Inservice, October 2005.doc Page 1 Head Trauma Inservice (October) Head trauma is the leading cause of death in trauma patients. Having a basic understanding of the anatomy and
John Tramell - Head Trauma Inservice, October 2005.doc Page 1 Head Trauma Inservice (October) Head trauma is the leading cause of death in trauma patients. Having a basic understanding of the anatomy and
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ٢ Level of consciousness is depressed Stuporous patients respond only to repeated
Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ٢ Level of consciousness is depressed Stuporous patients respond only to repeated
Pediatric Advanced Life Support
 Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Assessing the Stroke Patient. Arlene Boudreaux, MSN, RN, CCRN, CNRN
 Assessing the Stroke Patient Arlene Boudreaux, MSN, RN, CCRN, CNRN Cincinnati Pre-Hospital Stroke Scale May be done by EMS o One of many o F facial droop on one side o A arm drift (hold a pizza box, close
Assessing the Stroke Patient Arlene Boudreaux, MSN, RN, CCRN, CNRN Cincinnati Pre-Hospital Stroke Scale May be done by EMS o One of many o F facial droop on one side o A arm drift (hold a pizza box, close
It s All in Your Head: Neuro Assessment for Non- Neuro Folks
 It s All in Your Head: Neuro Assessment for Non- Neuro Folks Causes for Neuro Changes Stroke Head Injury Tumors Increased ICP Drugs Anoxia Altered Blood Glucose Toxins Alcohol Meningitis Poor Circulation
It s All in Your Head: Neuro Assessment for Non- Neuro Folks Causes for Neuro Changes Stroke Head Injury Tumors Increased ICP Drugs Anoxia Altered Blood Glucose Toxins Alcohol Meningitis Poor Circulation
what do the numbers really mean? NIHSS Timothy Hehr, RN MA Stroke Program Outreach Coordinator Allina Health
 what do the numbers really mean? NIHSS Timothy Hehr, RN MA Stroke Program Outreach Coordinator Allina Health NIHSS The National Institutes of Health Stroke Scale (NIHSS) is a tool used to objectively quantify
what do the numbers really mean? NIHSS Timothy Hehr, RN MA Stroke Program Outreach Coordinator Allina Health NIHSS The National Institutes of Health Stroke Scale (NIHSS) is a tool used to objectively quantify
Head & Brain Trauma. Presented By: Steven Jones, NREMT-P
 Head & Brain Trauma Presented By: Steven Jones, NREMT-P Head & Brain Trauma ~ 4 million head injuries in US per year ~ 450,000 require hospitalization Most are minor injuries Major head injury most common
Head & Brain Trauma Presented By: Steven Jones, NREMT-P Head & Brain Trauma ~ 4 million head injuries in US per year ~ 450,000 require hospitalization Most are minor injuries Major head injury most common
Mild Traumatic Brain Injury
 Mild Traumatic Brain Injury Concussions This presentation is for information purposes only, not for any commercial purpose, and may not be sold or redistributed. David Wesley, M.D. Outline Epidemiology
Mild Traumatic Brain Injury Concussions This presentation is for information purposes only, not for any commercial purpose, and may not be sold or redistributed. David Wesley, M.D. Outline Epidemiology
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
WHAT ARE the COMPONENTS OF THE NERVOUS SYSTEM?
 The Nervous System WHAT ARE the COMPONENTS OF THE NERVOUS SYSTEM? The nervous system is made of: the brain & the spinal cord the nerves the senses There are lots of proteins and chemicals in your body
The Nervous System WHAT ARE the COMPONENTS OF THE NERVOUS SYSTEM? The nervous system is made of: the brain & the spinal cord the nerves the senses There are lots of proteins and chemicals in your body
Stroke Transfer Checklist
 Stroke Transfer Checklist When preparing to transfer an acute stroke patient to the UF Health Shands Comprehensive Stroke Center, please make every attempt to include the following information: Results
Stroke Transfer Checklist When preparing to transfer an acute stroke patient to the UF Health Shands Comprehensive Stroke Center, please make every attempt to include the following information: Results
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
The Nervous System. Divisions of the Nervous System. Branches of the Autonomic Nervous System. Central versus Peripheral
 The Nervous System Divisions of the Nervous System Central versus Peripheral Central Brain and spinal cord Peripheral Everything else Somatic versus Autonomic Somatic Nerves serving conscious sensations
The Nervous System Divisions of the Nervous System Central versus Peripheral Central Brain and spinal cord Peripheral Everything else Somatic versus Autonomic Somatic Nerves serving conscious sensations
Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and
 1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
Stroke: Every Minute Counts! Primary Stroke Center, Ingalls Memorial Hospital
 Stroke: Every Minute Counts! Primary Stroke Center, Ingalls Memorial Hospital Objectives Describe the A & P of the nervous system Outline pathophysiological changes in the nervous system that may alter
Stroke: Every Minute Counts! Primary Stroke Center, Ingalls Memorial Hospital Objectives Describe the A & P of the nervous system Outline pathophysiological changes in the nervous system that may alter
BATLS Battlefield Advanced Trauma Life Support
 J R Army Med Corps 2002; 148: 151-158 BATLS Battlefield Advanced Trauma Life Support CHAPTER 8 HEAD INJURIES Aim 0801. On successfully completing this topic you will be able to: Discuss general management
J R Army Med Corps 2002; 148: 151-158 BATLS Battlefield Advanced Trauma Life Support CHAPTER 8 HEAD INJURIES Aim 0801. On successfully completing this topic you will be able to: Discuss general management
COMA. DIAH MUSTIKA HW,SpS,KIC INTENSIVE CARE UNIT of EMERGENCY DEPARTMENT
 COMA DIAH MUSTIKA HW,SpS,KIC INTENSIVE CARE UNIT of EMERGENCY DEPARTMENT NAVAL HOSPITAL dr RAMELAN, SURABAYA DEFINITIONS Coma State of unresponsiveness to external or internal stimuli in which a patient
COMA DIAH MUSTIKA HW,SpS,KIC INTENSIVE CARE UNIT of EMERGENCY DEPARTMENT NAVAL HOSPITAL dr RAMELAN, SURABAYA DEFINITIONS Coma State of unresponsiveness to external or internal stimuli in which a patient
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
A Healthy Brain. An Injured Brain
 A Healthy Brain Before we can understand what happens when a brain is injured, we must realize what a healthy brain is made of and what it does. The brain is enclosed inside the skull. The skull acts as
A Healthy Brain Before we can understand what happens when a brain is injured, we must realize what a healthy brain is made of and what it does. The brain is enclosed inside the skull. The skull acts as
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
CNS pathology Third year medical students,2019. Dr Heyam Awad Lecture 2: Disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students,2019 Dr Heyam Awad Lecture 2: Disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students,2019 Dr Heyam Awad Lecture 2: Disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Stroke & the Emergency Department. Dr. Barry Moynihan, March 2 nd, 2012
 Stroke & the Emergency Department Dr. Barry Moynihan, March 2 nd, 2012 Outline Primer Stroke anatomy & clinical syndromes Diagnosing stroke Anterior / Posterior Thrombolysis Haemorrhage The London model
Stroke & the Emergency Department Dr. Barry Moynihan, March 2 nd, 2012 Outline Primer Stroke anatomy & clinical syndromes Diagnosing stroke Anterior / Posterior Thrombolysis Haemorrhage The London model
Traumatic Brain Injury
 Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
TRAUMATIC BRAIN INJURY. Moderate and Severe Brain Injury
 TRAUMATIC BRAIN INJURY Moderate and Severe Brain Injury Disclosures Funded research: 1. NIH: RO1 Physiology of concussion 2016-2021, Co-PI, $2,000,000 2. American Medical Society of Sports Medicine: RCT
TRAUMATIC BRAIN INJURY Moderate and Severe Brain Injury Disclosures Funded research: 1. NIH: RO1 Physiology of concussion 2016-2021, Co-PI, $2,000,000 2. American Medical Society of Sports Medicine: RCT
Anesthetic Management of a Patient with Traumatic Brain Injury
 Anesthetic Management of a Patient with Traumatic Brain Injury Arne O. Budde, MD, DEAA Associate Professor of Anesthesiology Director, Division of Neuroanesthesia Department of Anesthesiology Milton S
Anesthetic Management of a Patient with Traumatic Brain Injury Arne O. Budde, MD, DEAA Associate Professor of Anesthesiology Director, Division of Neuroanesthesia Department of Anesthesiology Milton S
Head Trauma Protocol
 Injuries to the head may cause underlying brain tissue damage. Increased intracranial pressure from bleeding or swelling tissue is a common threat after head trauma. Common signs and symptoms of increased
Injuries to the head may cause underlying brain tissue damage. Increased intracranial pressure from bleeding or swelling tissue is a common threat after head trauma. Common signs and symptoms of increased
Patho-physiology of nervous System Talk 2 Syndromes in neurosciences. Petr Maršálek Dept pathological physiology 1.Med. F. CUNI
 Patho-physiology of nervous System Talk 2 Syndromes in neurosciences Petr Maršálek Dept pathological physiology 1.Med. F. CUNI Talks on NS Talk 1 - Pain and Motor disorders Talk 2 - This - Syndromes in
Patho-physiology of nervous System Talk 2 Syndromes in neurosciences Petr Maršálek Dept pathological physiology 1.Med. F. CUNI Talks on NS Talk 1 - Pain and Motor disorders Talk 2 - This - Syndromes in
Medical Neuroscience Tutorial Notes
 Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Traumatic Brain Injury TBI Presented by Bill Masten
 1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
The Neurological System. Neurological Exam 5 Components. Mental Status Examination
 The Neurological System 1 Neurological Exam 5 Components Mental status Cranial nerves Reflexes Motor- includes Cerebellar function Sensory 2 Mental Status Examination Examination - ABCT Appearance Behavior
The Neurological System 1 Neurological Exam 5 Components Mental status Cranial nerves Reflexes Motor- includes Cerebellar function Sensory 2 Mental Status Examination Examination - ABCT Appearance Behavior
North Oaks Trauma Symposium Friday, November 3, 2017
 Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
GLOSSARY. Active assisted movement: movement where the actions are assisted by an outside force.
 GLOSSARY The technical words used in this guide are listed here in alphabetic order. The first time one of these words is used in the guide, it is written in italics. Sometimes there is reference to a
GLOSSARY The technical words used in this guide are listed here in alphabetic order. The first time one of these words is used in the guide, it is written in italics. Sometimes there is reference to a
Cerebral Vascular Diseases. Nabila Hamdi MD, PhD
 Cerebral Vascular Diseases Nabila Hamdi MD, PhD Outline I. Stroke statistics II. Cerebral circulation III. Clinical symptoms of stroke IV. Pathogenesis of cerebral infarcts (Stroke) 1. Ischemic - Thrombotic
Cerebral Vascular Diseases Nabila Hamdi MD, PhD Outline I. Stroke statistics II. Cerebral circulation III. Clinical symptoms of stroke IV. Pathogenesis of cerebral infarcts (Stroke) 1. Ischemic - Thrombotic
INTRACRANIAL PRESSURE -!!
 INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
Cerebrovascular Disorders. Blood, Brain, and Energy. Blood Supply to the Brain 2/14/11
 Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
October 2009 CE Site code #107200E-1209
 October 2009 CE Site code #107200E-1209 The Patient with an Altered Mental Status Outline prepared by: Jeremy Lockwood FFPM Mundelein Fire Department Material reviewed and revised by Sharon Hopkins, RN,
October 2009 CE Site code #107200E-1209 The Patient with an Altered Mental Status Outline prepared by: Jeremy Lockwood FFPM Mundelein Fire Department Material reviewed and revised by Sharon Hopkins, RN,
PAEDIATRIC ACUTE CARE GUIDELINE. Resuscitation Coma
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Resuscitation Coma Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Resuscitation Coma Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be
CHILD IN NON - TRAUMATIC COMA
 May / 2018 PELC / SLCP 1 CHILD IN NON - TRAUMATIC COMA PELS May / 2018 PELC / SLCP 2 Objectives Recognize depressed mental status Know the causes of depressed mental status in children Assessment and workup
May / 2018 PELC / SLCP 1 CHILD IN NON - TRAUMATIC COMA PELS May / 2018 PELC / SLCP 2 Objectives Recognize depressed mental status Know the causes of depressed mental status in children Assessment and workup
D is for Disability Altered Mental Status in Children
 D is for Disability Altered Mental Status in Children Joshua Ross, MD, FAAP Pediatric Emergency Medicine Emergency Care and Trauma Symposium June 22, 2015 Objectives Describe a basic approach to evaluating
D is for Disability Altered Mental Status in Children Joshua Ross, MD, FAAP Pediatric Emergency Medicine Emergency Care and Trauma Symposium June 22, 2015 Objectives Describe a basic approach to evaluating
BRAIN PART I (A & B): VENTRICLES & MENINGES
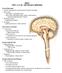 BRAIN PART I (A & B): VENTRICLES & MENINGES Cranial Meninges Cranial meninges are continuous with spinal meninges Dura mater: inner layer (meningeal layer) outer layer (endosteal layer) fused to periosteum
BRAIN PART I (A & B): VENTRICLES & MENINGES Cranial Meninges Cranial meninges are continuous with spinal meninges Dura mater: inner layer (meningeal layer) outer layer (endosteal layer) fused to periosteum
PEDIATRIC INITIAL ASSESSMENT - ALS
 PEDIATRIC INITIAL ASSESSMENT - ALS I. SCENE SIZE-UP A. Protect from body substance through isolation (glasses, gloves, gown and mask). B. Assess the scene for safety and take appropriate steps. C. Determine
PEDIATRIC INITIAL ASSESSMENT - ALS I. SCENE SIZE-UP A. Protect from body substance through isolation (glasses, gloves, gown and mask). B. Assess the scene for safety and take appropriate steps. C. Determine
Nervous system, integration: Overview, and peripheral nervous system:
 Nervous system, integration: Overview, and peripheral nervous system: Some review & misc. parts [Fig. 28.11B, p. 573]: - white matter --> looks white due to the myelinated sheaths, which are quite fatty.
Nervous system, integration: Overview, and peripheral nervous system: Some review & misc. parts [Fig. 28.11B, p. 573]: - white matter --> looks white due to the myelinated sheaths, which are quite fatty.
Stroke/TIA. Tom Bedwell
 Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Stroke: clinical presentations, symptoms and signs
 Stroke: clinical presentations, symptoms and signs Professor Peter Sandercock University of Edinburgh EAN teaching course Burkina Faso 8 th November 2017 Clinical diagnosis is important to Ensure stroke
Stroke: clinical presentations, symptoms and signs Professor Peter Sandercock University of Edinburgh EAN teaching course Burkina Faso 8 th November 2017 Clinical diagnosis is important to Ensure stroke
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
a) Central sulcus- shallow groove that runs across brain sagitally
 KEY BRAIN Brain Gross Anatomy Terms 1) Explain each of the following in terms of structure of the brain a) Central sulcus- shallow groove that runs across brain sagitally b) Lateral fissure- deep groove
KEY BRAIN Brain Gross Anatomy Terms 1) Explain each of the following in terms of structure of the brain a) Central sulcus- shallow groove that runs across brain sagitally b) Lateral fissure- deep groove
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
Acting in an emergency. Dr. Samer Sara
 Acting in an emergency Dr. Samer Sara 1 Acting in an emergency basic steps to follow: 1. Recognize the emergency. 2. Check the scene. 3. Call 110. 4. Check the victim. 5. Give first aid. 2 Dr. Samer Sara
Acting in an emergency Dr. Samer Sara 1 Acting in an emergency basic steps to follow: 1. Recognize the emergency. 2. Check the scene. 3. Call 110. 4. Check the victim. 5. Give first aid. 2 Dr. Samer Sara
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
A Hypothesis Driven Approach to the Neurological Exam
 A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
Nervous System C H A P T E R 2
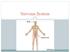 Nervous System C H A P T E R 2 Input Output Neuron 3 Nerve cell Allows information to travel throughout the body to various destinations Receptive Segment Cell Body Dendrites: receive message Myelin sheath
Nervous System C H A P T E R 2 Input Output Neuron 3 Nerve cell Allows information to travel throughout the body to various destinations Receptive Segment Cell Body Dendrites: receive message Myelin sheath
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Organic Mental Disorders. Organic Mental Disorders. Axes. Damrongsak Bulyalert Department of Internal Medicine
 Organic Mental Disorders Damrongsak Bulyalert Department of Internal Medicine www.metadon.net 1 Organic Mental Disorders In DSM (Diagnostic and Statistical Manual of Mental Disorders), OMD includes Delirium,
Organic Mental Disorders Damrongsak Bulyalert Department of Internal Medicine www.metadon.net 1 Organic Mental Disorders In DSM (Diagnostic and Statistical Manual of Mental Disorders), OMD includes Delirium,
HEAD AND NECK PART 2
 HEAD AND NECK PART 2 INTEGRATED CURRICULUM = Integrate Basic Science and Clinical Training 1- ENT PATIENT EXAM IN ICS COURSE - Today and next week - Review/Preview Anatomy underlying ENT exam 2- NEUROANATOMY/NEUROLOGY
HEAD AND NECK PART 2 INTEGRATED CURRICULUM = Integrate Basic Science and Clinical Training 1- ENT PATIENT EXAM IN ICS COURSE - Today and next week - Review/Preview Anatomy underlying ENT exam 2- NEUROANATOMY/NEUROLOGY
Injuries to the head and spine
 Injuries to the head and spine Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Nervous System Two sub-systems Central Nervous System ( CNS ) Brain and spinal cord Peripheral Nervous System 12 cranial
Injuries to the head and spine Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Nervous System Two sub-systems Central Nervous System ( CNS ) Brain and spinal cord Peripheral Nervous System 12 cranial
Cesarean section for breech presentation. Jonathan H. Waters, M.D.
 Cesarean section for breech presentation Jonathan H. Waters, M.D. 1 26 y.o. G1P0 presented to triage in labor at 38 weeks. Patient was a known breech with a failed version 5 days before presentation. PMH
Cesarean section for breech presentation Jonathan H. Waters, M.D. 1 26 y.o. G1P0 presented to triage in labor at 38 weeks. Patient was a known breech with a failed version 5 days before presentation. PMH
The Nervous System. Nerves, nerves everywhere!
 The Nervous System Nerves, nerves everywhere! Purpose of the Nervous System The information intake and response system of the body. Coordinates all body functions, voluntary and involuntary! Responds to
The Nervous System Nerves, nerves everywhere! Purpose of the Nervous System The information intake and response system of the body. Coordinates all body functions, voluntary and involuntary! Responds to
Three Ways to Apply Central Stimulus
 Three Ways to Apply Central Stimulus Objectives 1. State when to use central pressure to elicit response 2. Identify three consistent evidence-based practices for applying central noxious stimuli to elicit
Three Ways to Apply Central Stimulus Objectives 1. State when to use central pressure to elicit response 2. Identify three consistent evidence-based practices for applying central noxious stimuli to elicit
The NIHSS score is 4 (considering 2 pts for the ataxia involving upper and lower limbs.
 Neuroscience case 5 1. Speech comprehension, ability to speak, and word use were normal in Mr. Washburn, indicating that aphasia (cortical language problem) was not involved. However, he did have a problem
Neuroscience case 5 1. Speech comprehension, ability to speak, and word use were normal in Mr. Washburn, indicating that aphasia (cortical language problem) was not involved. However, he did have a problem
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth. Objectives 11/7/2017
 Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
IDPH EMS Region Five. Stroke Education
 IDPH EMS Region Five Stroke Education Time is Brain!!!!! Time is Brain!!!! Stroke refers to any spontaneous damage to the brain caused by an abnormality of the blood supply by means of a clot or bleed.
IDPH EMS Region Five Stroke Education Time is Brain!!!!! Time is Brain!!!! Stroke refers to any spontaneous damage to the brain caused by an abnormality of the blood supply by means of a clot or bleed.
May 2011 CE. Site code # E Head & Spinal Cord Trauma
 May 2011 CE Site code # 107200E-1211 Head & Spinal Cord Trauma Objectives by Mike Higgins, FF/PM Grayslake Fire Dept Program by Sharon Hopkins, RN, BSN, EMT-P To view on the Advocate Condell website visit:
May 2011 CE Site code # 107200E-1211 Head & Spinal Cord Trauma Objectives by Mike Higgins, FF/PM Grayslake Fire Dept Program by Sharon Hopkins, RN, BSN, EMT-P To view on the Advocate Condell website visit:
meninges Outermost layer of the meninge dura mater arachnoid mater pia mater membranes located between bone and soft tissue of the nervous system
 membranes located between bone and soft tissue of the nervous system meninges Outermost layer of the meninge dura mater middle layer of the meninges, contains no blood vessels arachnoid mater Innermost
membranes located between bone and soft tissue of the nervous system meninges Outermost layer of the meninge dura mater middle layer of the meninges, contains no blood vessels arachnoid mater Innermost
Stroke in the ED. Dr. William Whiteley. Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian
 Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
CVA. Alison Atwater PA-C
 CVA Alison Atwater PA-C Types of CVAs Ischemic strokes 80% of strokes 2/3 are thrombotic 1/3 are embolic emboli from the heart or arteries feeding the brain such as carotids, vertebral and basilar etc
CVA Alison Atwater PA-C Types of CVAs Ischemic strokes 80% of strokes 2/3 are thrombotic 1/3 are embolic emboli from the heart or arteries feeding the brain such as carotids, vertebral and basilar etc
M555 Medical Neuroscience Lab 1: Gross Anatomy of Brain, Crainal Nerves and Cerebral Blood Vessels
 M555 Medical Neuroscience Lab 1: Gross Anatomy of Brain, Crainal Nerves and Cerebral Blood Vessels Anatomical Directions Terms like dorsal, ventral, and posterior provide a means of locating structures
M555 Medical Neuroscience Lab 1: Gross Anatomy of Brain, Crainal Nerves and Cerebral Blood Vessels Anatomical Directions Terms like dorsal, ventral, and posterior provide a means of locating structures
CNS composed of: Grey matter Unmyelinated axons Dendrites and cell bodies White matter Myelinated axon tracts
 CNS composed of: Grey matter Unmyelinated axons Dendrites and cell bodies White matter Myelinated axon tracts The Brain: A Quick Tour Frontal Lobe Control of skeletal muscles Personality Concentration
CNS composed of: Grey matter Unmyelinated axons Dendrites and cell bodies White matter Myelinated axon tracts The Brain: A Quick Tour Frontal Lobe Control of skeletal muscles Personality Concentration
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
THE ESSENTIAL BRAIN INJURY GUIDE
 THE ESSENTIAL BRAIN INJURY GUIDE Neuroanatomy & Neuroplasticity Section 2 Contributors Erin D. Bigler, PhD Michael R. Hoane, PhD Stephanie Kolakowsky-Hayner, PhD, CBIST, FACRM Dorothy A. Kozlowski, PhD
THE ESSENTIAL BRAIN INJURY GUIDE Neuroanatomy & Neuroplasticity Section 2 Contributors Erin D. Bigler, PhD Michael R. Hoane, PhD Stephanie Kolakowsky-Hayner, PhD, CBIST, FACRM Dorothy A. Kozlowski, PhD
Functional Organization of the Central Nervous System
 Functional Organization of the Central Nervous System Hierarchical orgnization CNS consists of the brain and the spinal cord The brain analyzes and interprets the information Response messages are
Functional Organization of the Central Nervous System Hierarchical orgnization CNS consists of the brain and the spinal cord The brain analyzes and interprets the information Response messages are
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Blood Supply. Allen Chung, class of 2013
 Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
What Are We Going to Do? Fourth Year Meds Clinical Neuroanatomy. Hydrocephalus and Effects of Interruption of CSF Flow. Tube Blockage Doctrine
 Fourth Year Meds Clinical Neuroanatomy Ventricles, CSF, Brain Swelling etc. David A. Ramsay, Neuropathologist, LHSC What Are We Going to Do? Hydrocephalus and some effects of the interruption of CSF flow
Fourth Year Meds Clinical Neuroanatomy Ventricles, CSF, Brain Swelling etc. David A. Ramsay, Neuropathologist, LHSC What Are We Going to Do? Hydrocephalus and some effects of the interruption of CSF flow
NIHSS. Category Scale Definition Date/Time Date/Time Date/Time. Score Initial. Drip & Ship Protocol. Initials: Signature: Initials: Signature:
 NIHSS 1a. Level of Consciousness (Alert, drowsy, etc.) Category Scale Definition Date/Time Date/Time Date/Time 1b. LOC Question (Month, age) 1c. LOC Commands (Open, close eyes, make fist, let go) 2. Best
NIHSS 1a. Level of Consciousness (Alert, drowsy, etc.) Category Scale Definition Date/Time Date/Time Date/Time 1b. LOC Question (Month, age) 1c. LOC Commands (Open, close eyes, make fist, let go) 2. Best
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Pre-Hospital Stroke Care: Bringing It To The Street. by Bob Atkins, NREMT-Paramedic AEMD EMS Director Bedford Regional Medical Center
 Pre-Hospital Stroke Care: Bringing It To The Street by Bob Atkins, NREMT-Paramedic AEMD EMS Director Bedford Regional Medical Center Overview/Objectives Explain the reasons or rational behind the importance
Pre-Hospital Stroke Care: Bringing It To The Street by Bob Atkins, NREMT-Paramedic AEMD EMS Director Bedford Regional Medical Center Overview/Objectives Explain the reasons or rational behind the importance
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 14 The Brain and Cranial Nerves Introduction The purpose of the chapter is to: 1. Understand how the brain is organized, protected, and supplied
Principles of Anatomy and Physiology 14 th Edition CHAPTER 14 The Brain and Cranial Nerves Introduction The purpose of the chapter is to: 1. Understand how the brain is organized, protected, and supplied
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Chapter 18. Objectives. Objectives 01/09/2013. Altered Mental Status, Stroke, and Headache
 Chapter 18 Altered Mental Status, Stroke, and Headache Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives
Chapter 18 Altered Mental Status, Stroke, and Headache Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Stroke. Understanding. Professor Richard Iain Lindley
 Understanding Stroke Professor Richard Iain Lindley Published by Family Doctor Publications Limited in association with the British Medical Association IMPORTANT This book is intended not as a substitute
Understanding Stroke Professor Richard Iain Lindley Published by Family Doctor Publications Limited in association with the British Medical Association IMPORTANT This book is intended not as a substitute
THE CENTRAL NERVOUS SYSTEM. The Brain & Spinal Cord
 THE CENTRAL NERVOUS SYSTEM The Brain & Spinal Cord Review: Nervous System Parallel Distributed Processing Composition of the CNS Nuclei: Clusters of neurons in the CNS ( neighborhoods ) Fiber Tracts/Pathways:
THE CENTRAL NERVOUS SYSTEM The Brain & Spinal Cord Review: Nervous System Parallel Distributed Processing Composition of the CNS Nuclei: Clusters of neurons in the CNS ( neighborhoods ) Fiber Tracts/Pathways:
MCHENRY WESTERN LAKE COUNTY EMS SYSTEM Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #7 Strokes
 MCHENRY WESTERN LAKE COUNTY EMS SYSTEM Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #7 Strokes Stroke is the third leading cause of death and the leading cause of adult disability in the
MCHENRY WESTERN LAKE COUNTY EMS SYSTEM Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #7 Strokes Stroke is the third leading cause of death and the leading cause of adult disability in the
Clinical Learning Exercise #1
 Clinical Learning Exercise #1 Exercise: We are going to assume nothing is wrong with the peripheral nervous system and attempt to identify the central nervous system anatomical location for the following
Clinical Learning Exercise #1 Exercise: We are going to assume nothing is wrong with the peripheral nervous system and attempt to identify the central nervous system anatomical location for the following
Assessment and Scoring Tools
 Assessment and Scoring Tools 2013 APGAR Scale 0 points 1 point 2 points Heart Rate Absent 100 Respiratory Rate Absent Slow, irregular Good, drying Irritability Flaccid Some flexion Active motion
Assessment and Scoring Tools 2013 APGAR Scale 0 points 1 point 2 points Heart Rate Absent 100 Respiratory Rate Absent Slow, irregular Good, drying Irritability Flaccid Some flexion Active motion
10/15/2015. Structural Lesions Brain tumor (neoplasm) Degenerative disease Intracranial hemorrhage Parasites Trauma
 At the end of this seminar the participant shall be able to: Generally describe the pathophysiology of altered level of consciousness Describe some of the medical causes of altered level of consciousness
At the end of this seminar the participant shall be able to: Generally describe the pathophysiology of altered level of consciousness Describe some of the medical causes of altered level of consciousness
The Nervous System PART B
 7 The Nervous System PART B PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Central Nervous System
7 The Nervous System PART B PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Central Nervous System
