Supplementary Appendix
|
|
|
- Adela Fletcher
- 6 years ago
- Views:
Transcription
1 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Cooper DJ, Rosenfeld JV, Murray L, et al. Decompressive craniectomy in diffuse traumatic brain injury. N Engl J Med 2011;364: DOI: /NEJMoa (PDF updated April 5, 2011.)
2 Supplementary Appendix Table of Contents The DECRA Trial Committees and Members... 2 Surgical Technique: Bi-fronto-temporal Decompressive Craniectomy in Diffuse Traumatic Brain Injury... 3 Supplementary Figure 1. Assessment, randomization and follow-up of the trial Supplementary Table 1. Times Supplementary Table 2. Processes of care Supplementary Figure 2. Functional outcomes at 6 months after injury assessed by Extended Glasgow Outcomes Scale (GOSE) in decompressive craniectomy (DC) and standard care groups Supplementary Table 3. Surgical complications of craniectomy and subsequent cranioplasty for patients in the craniectomy group... 9 Supplementary Table 4. Causes of death Supplementary Figure 3. CT brain scans: Panels A and B Supplementary Figure 4. Operative photograph
3 The DECRA Trial Committees and Members The DECRA Trial Investigators were as follows: Co-Chief Investigators D.J. Cooper, J.V. Rosenfeld; Executive Committee D.J. Cooper (Chair), J.V. Rosenfeld, L. Murray, Y.M. Arabi, A.R. Davies, P. D Urso, T. Kossmann, J. Ponsford, I. Seppelt, P. Reilly, R. Wolfe; Data and Safety Monitoring Committee P. Myles (Chair), R. Bellomo, J. Santamaria, P. Komasarof, B. Byrne; Study Statistical Center Monash University, Melbourne, Australia R. Wolfe, P. Simpson; Study Coordinating Center The Alfred Hospital, Melbourne, Australia; Outcome Assessors S. Vallance, B. Howe, M. Kishi; Site Investigators (In order of patient numbers at each site recruited into the DECRA trial) Alfred Hospital, Melbourne, Australia D.J. Cooper, J.V. Rosenfeld, L. Murray, A.R. Davies, P. Hwang, V. Pellegrino; King Saud Bin Abdulaziz University for Health Sciences, Riyadh, Kingdom of Saudi Arabia Y.M. Arabi, S. Al-Qahtani, A. Al-Ferayan, N. Russell, A. Rishu; Royal Perth Hospital, Perth, Australia G. Dobb, S. Honeybul, J. Chamberlain, A. Gould, G. McEntaggart; Nepean Hospital, Sydney, Australia I. Seppelt, V. Casikar, S. Nair, K. Seex, L. Weisbrodt; John Hunter Hospital, Newcastle, Australia P. Harrigan, R. Ferch, B. McFadyen, E. Taylor, M. Hardie; Royal Melbourne Hospital, Melbourne, Australia J. Laidlaw, C. MacIsaac, M. Robertson, J. Presneill, T. Caf; Royal North Shore Hospital, Sydney, Australia S. Finfer, M. Briggs, R. Lee, N. Little, A. O Connor; Princess Alexandra Hospital, Brisbane, Australia C. Joyce, A. Nowitzke, B. Venkatesh, M. Harward, J. Helyar; Wellington Hospital, Wellington, New Zealand D. Dinsdale, M. Hunn, L. Andrew, D. Mackle, S. Mortimer; Auckland Hospital, Auckland New Zealand C. McArthur, A. Law, S. Streat, L. Newby; Gold Coast Hospital, Southport, Queensland B. Richards, T. Withers, M. Tallott; Sir Charles Gairdner Hospital, Perth, Australia P.V. van Heerden, S. Baker, M. Pinder, N. Knuckey, B. Roberts; Liverpool Hospital, Sydney, Australia M. Parr, R. Calcroft, J. Van Gelder, M. Sheridan, S. Micallef; Royal Adelaide Hospital, Adelaide, Australia N. Edwards, B. Brophy, M. Chapman, P. Reilly, S. O Connor; Christchurch Hospital, Christchurch, New Zealand S. Henderson, R. Boet, N. Finnis, M. Macfarlane, J. Mehrtens. The following hospitals commenced screening but did not enrol patients: Australia Westmead Hospital, Sydney, Royal Hobart Hospital, Hobart, Wollongong Hospital, Wollongong, Flinders Medical Centre, Adelaide; New Zealand Waikato Hospital, Hamilton; Canada Vancouver General Hospital, Vancouver, Royal Columbian Hospital, Vancouver, Sunnybrook Medical Centre, Toronto, Hamilton General Hospital, Hamilton; U.S.A. Baltimore Shock Trauma Center, Maryland, University of Pennsylvania, Pennsylvania. 2
4 Surgical Technique: Bi-fronto-temporal Decompressive Craniectomy in Diffuse Traumatic Brain Injury. The technique described by Polin et al 17 was used with minor modification. Senior neurosurgeons from all participating centres were given oral and written instruction by Dr J.V. Rosenfeld on our recommended craniectomy method and all their questions were answered. A diagram was supplied. In this way, the surgical procedure was standardized. The operation comprised a bicoronal incision raising the pericranium with the scalp flap. A bi-frontotemporo-parietal decompressive craniectomy was performed with the bone flap extending across the midline. The surgeon was permitted to divide the bone flap at or near the midline for ease of removal but no strip of bone was left over the sagittal sinus. The temporalis muscle was reflected inferiorly and posteriorly on each side down to or near to the level of the floor of the middle cranial fossa. Burr holes were located either side of the sagittal sinus at the posterior extent, bilaterally at the keyhole position just posterior to the zygomatic process of the frontal bone and if needed at the root of the zygoma inferiorly. The posterior limit extended at least back to the coronal suture posteriorly but many surgeons extended posteriorly 2 or 3 centimeters beyond this point at the midline. The bone cut was extended vertically and inferiorly on each side, thus passing posterior to the coronal suture and through the parietal bone and temporal bone. This cut was continued forwards low down on the squamous temporal bone and forwards across the greater wing of the sphenoid bone across to the burr hole at the keyhole position. The inferior bone cut was made just above the supra-orbital ridges. To avoid opening the frontal sinus, the inferior bone cut passed above the frontal bone overlying the sinus. The neurosurgeon judged this based on the size of the sinus on the preoperative CT scan. Following removal of the bone flap, an extension of the craniectomy was performed bilaterally by removing the squamous temporal bone and the greater wing of sphenoid with rongeurs close to the floor of the middle fossa on each side. Thus, bilateral sub-temporal decompressions were performed (Figure 3 in the Supplementary Appendix). The dura was opened over the frontal lobes in one of two ways: a large cruciate incision bilaterally (Figure 4 in the Supplementary Appendix), or a large L shaped incision with the lower corner of the L facing laterally and the horizontal limb pointing medially toward the sagittal sinus. The advantage to the latter method is that the cerebral veins are not disturbed medially by this incision although the co-ordinating center did not encounter any venous injury with the cruciate method. Kinking of large cortical veins at the cut dural edge was prevented by small radial cuts overlying the veins. Kinking of the sagittal sinus at the edge of the craniectomy was not an issue. Our procedure did not involve a fishmouth opening of the dura and dividing the sagittal sinus and falx as described by Polin et al 17. The durotomy was covered with a synthetic dural or fascial patch (temporalis or pericranium). The patch was placed to protect the surface of the brain from adhering to the scalp and to act as a further barrier to infection. The patches were tacked into position with sutures so that they did not migrate. Water-tight dural closure was not required (Figure 4 in the Supplementary Appendix). Attention was directed to haemostasis prior to closure of the scalp, but low pressure suction drains were placed beneath the scalp flap if oozing was a problem. These were usually removed after 24 hours and the exit wounds sutured to avoid CSF leak and infection. 3
5 In each patient, when possible, the initial ICP monitor was placed posterior to the line of a potential craniectomy incision so that it could be left undisturbed by the craniectomy procedure. The ICP monitor utilizing ventricular catheter and/or parenchymal transducer (± optional brain oxygen (PbrO 2 ) and temperature monitor) were replaced prior to closure and brought out through separate stab incisions posterior to the scalp flap. The bone flap was replaced once bone swelling resolved and the patient had improved and left the intensive care unit (6-12 weeks). The bone flap was stored in a clinical freezer at minus 70 C until reinsertion or it was implanted in the subcutaneous tissue of the abdominal wall as an alternative. 4
6 Supplementary Figure 1. Assessment, randomization and follow-up of the trial. Patients with severe traumatic brain injury assessed for eligibility (n=3478) Excluded (n=3302) Mass lesions (n=1222) Unsurvivable/poor prognosis (n=420) Age <15 & >60 years (n=211) ICP controlled (n=1105) Other (n=344) Declined Consent (n=21) Randomized (n=155) Allocated to craniectomy (n=73) Received craniectomy (n=70) Did not receive craniectomy (n=3) ICP stabilized prior to craniectomy (n=2) Incorrectly randomized (n=1) Allocated to standard care (n=82) Received standard care (n=78) Received craniectomy (n=4) Analyzed (n=73) Lost to follow up (n=0) Withdrew consent (n=0) Analyzed (n=82) Lost to follow up (n=0) Withdrew consent (n=0) 5
7 Supplementary Table 1. Times. Decompressive Craniectomy N=73 Median (IQR) Standard Care N=82 Median (IQR) Time from injury to hospital (hrs) 1.0 (0.8 to 1.8) 1.2 (0.7 to 1.9) Time from injury to randomization (hrs) 35.2 (23.3 to 52.8) 34.8 (25.8 to 45.4) Time from injury to surgery (hrs) 38.1 (27.1 to 55.0) 102 (73 to 174) Time from randomization to surgery (hrs) 2.3 (1.4 to 3.8) 75.8 (42.6 to 121.1) Time from craniectomy to cranioplasty (days) 76.6 (46.4 to 131.4) (95.4 to 162.7) Length of surgery for craniectomy (hrs) 2.8 (2.3 to 3.3) 2.8 (2.3 to 4.0) Length of surgery for cranioplasty (hrs) 2.4 (1.8 to 2.9) 2.6 (2.3 to 2.9) 6
8 Supplementary Table 2. Processes of care. Intracranial pressure (ICP) Parenchymal monitor inserted; n (%) Decompressive Craniectomy N=73 Standard Care N=82 P value 50 (68) 52 (64) 0.57 ICP Extra ventricular drain monitor inserted; n* (%) 49 (67) 59 (72) 0.51 Pre randomization Hypertonic saline 3% (mls); median (IQR) 650 (133 to 1333) 720 (200 to 1404) 0.40 Mannitol 20% (mls); n (%) (55) 51 (65) (32) 23 (29) (13) 5 (6) Thiopentone (gm); n (%) (71) 55 (67) (22) 19 (23) (7) 8 (10) Neuromuscular blockade; n (%) 57 (78) 63 (77) 0.85 Cerebrospinal fluid venting n (%) 46 (100^) 50 (100^) 1.0 Post randomization Hypertonic saline 3% (mls); median (IQR) 425 (0 to 1983) 1475 (200 to 3875) 0.01 Mannitol 20% (mls); n (%) (82) 55 (68) (18) 16 (20) (0) 10 (12) Thiopentone (gm); n (%) < (68) 19 (23) (32) 49 (60) (0) 14 (17) Paralysis; n (%) 42 (58) 70 (85) <0.001 Cerebrospinal fluid venting; n (%) 33 (77#) 57 (97#) Chi-square test to compare proportions, Wilcoxon rank sum test to compare distributions *Of these numbers, 3 in the decompressive craniectomy group and 9 in the standard care group had the extra ventricular drain monitor inserted post randomization ^ Percentage of those with extra ventricular drain monitor inserted pre randomization # Percentage of those with extra ventricular drain monitor inserted; 6 in decompressive craniectomy group had missing drain data and were excluded from calculation of percentage 7
9 Supplementary Figure 2. Functional outcomes at 6 months after injury assessed by the Extended Glasgow Outcomes Scale (GOSE) in decompressive craniectomy (DC) and standard care groups. GOSE 1 is dead; 2 is vegetative survival; 3/4 is severe disability; 5/6 is moderate disability (independent); 7/8 is good (independent). Grade 8 is pre-injury neurological function. Favorable outcome is GOSE
10 Supplementary Table 3. Surgical complications of craniectomy and subsequent cranioplasty for patients in the craniectomy group* Adverse events n (%) Craniectomy N=70 Cranioplasty N=56 Wound infection/breakdown 2 (3) 3 (6) Meningitis/Ventriculitis 2 (3) 0 (0) Subgaleal infection 0 (0) 2 (4) Cerebral abscess 1 (1) 1 (2) CSF leak 4 (6) 0 (0) Subgaleal hematoma 3 (4) 2 (4) Subdural/Extradural/Intracerebral hematoma 1 (1) 2 (4) Cerebral infarction 1 (1) 0 (0) Subgaleal infection 0 (0) 2 (4) *70 of 73 craniectomy group patients received the first operation per protocol (see supplementary Figure 1). Not all craniectomy patients survived to have the subsequent cranioplasty (56 of 70). Cranioplasty patients had their operation reversed by 6 months. 9
11 Supplementary Table 4. Causes of death. Decompressive Craniectomy N=73 Standard Care N=82 Treatment withdrawn due to TBI n (%) 11 (15) 8 (10) Brain death n (%) 2 (3) 4 (5) Pneumonia n (%) 0 (0) 1 (1) Septic shock n (%) 1 (1) 1 (1) Neurogenic pulmonary edema n (%) 0 (0) 1 (1) 10
12 Supplementary Figure 3. CT brain scans: Panels A and B. Examples to clarify extent of craniectomy: Panel A. Post-craniectomy lateral scout CT brain scan Panel B. Three days post-bi-fronto-temporo-parietal craniectomy 11
13 Supplementary Figure 4. Operative photograph. Operative photograph showing extent of craniectomy and magnitude of cruciate incisions in the dura. Surgicel is placed over the sagittal sinus. A ventricular drain is in situ. 12
Moron General Hospital Ciego de Avila Cuba. Department of Neurological Surgery
 Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Neurosurgical Techniques
 Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
A bs tr ac t. n engl j med 364;16 nejm.org april 21,
 The new england journal of medicine established in 1812 april 21, 2011 vol. 364 no. 16 Decompressive Craniectomy in Diffuse Traumatic Brain Injury D. James Cooper, M.D., Jeffrey V. Rosenfeld, M.D., Lynnette
The new england journal of medicine established in 1812 april 21, 2011 vol. 364 no. 16 Decompressive Craniectomy in Diffuse Traumatic Brain Injury D. James Cooper, M.D., Jeffrey V. Rosenfeld, M.D., Lynnette
Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience
 80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
Decompressive craniectomy following traumatic brain injury
 Decompressive craniectomy following traumatic brain injury Peter Hutchinson Division of Academic Neurosurgery University of Cambridge Escalating cycle of brain swelling Primary insult Brain swelling Secondary
Decompressive craniectomy following traumatic brain injury Peter Hutchinson Division of Academic Neurosurgery University of Cambridge Escalating cycle of brain swelling Primary insult Brain swelling Secondary
T HERE is an unusual and interesting variety of craniosynostosis in
 SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
5. COMMON APPROACHES. Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2.
 5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
Supplementary Online Content
 Supplementary Online Content Cooper DJ, Nichol A, Bailey M, et al. Effect of early sustained prophylactic hypothermia on neurologic outcomes among patients with severe traumatic brain injury: the POLAR
Supplementary Online Content Cooper DJ, Nichol A, Bailey M, et al. Effect of early sustained prophylactic hypothermia on neurologic outcomes among patients with severe traumatic brain injury: the POLAR
Accredited Sites for Advanced Training HAEMATOLOGY June 2018
 Accredited Sites for Advanced Training HAEMATOLOGY June 2018 Core Training in Haematology can only be undertaken in an accredited training setting. Applicants are advised that the position applied for
Accredited Sites for Advanced Training HAEMATOLOGY June 2018 Core Training in Haematology can only be undertaken in an accredited training setting. Applicants are advised that the position applied for
Accredited Sites for Advanced Training IMMUNOLOGY AND ALLERGY February 2017
 Sites for Advanced Training IMMUNOLOGY AND ALLERGY February 2017 Core Training in Immunology and Allergy can only be undertaken in an accredited training setting. Applicants are advised that the position
Sites for Advanced Training IMMUNOLOGY AND ALLERGY February 2017 Core Training in Immunology and Allergy can only be undertaken in an accredited training setting. Applicants are advised that the position
Brain under pressure Managing ICP. Giuseppe
 Brain under pressure Managing ICP Giuseppe Citerio giuseppe.citerio@unimib.it @Dr_Cit Intro Thresholds Treating HICP Conclusions NO COI for this presentation Produces pressure gradients: herniation HIGH
Brain under pressure Managing ICP Giuseppe Citerio giuseppe.citerio@unimib.it @Dr_Cit Intro Thresholds Treating HICP Conclusions NO COI for this presentation Produces pressure gradients: herniation HIGH
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth. Objectives 11/7/2017
 Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma
 Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Clinical Need. 3) At time of reconstruction there may be complications because the dura has adhered to the scalp
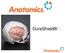 DuraShield DuraShield Contoured Silicone sheet that is implanted after decompressive craniectomy, to prevent epidural adhesions and improve cranial reconstruction Clinical Need 1) Traumatic brain injury
DuraShield DuraShield Contoured Silicone sheet that is implanted after decompressive craniectomy, to prevent epidural adhesions and improve cranial reconstruction Clinical Need 1) Traumatic brain injury
Is Neuromonitoring an expensive waste of time, in Severe Traumatic Brain Injury?
 Is Neuromonitoring an expensive waste of time, in Severe Traumatic Brain Injury? Edema Engorgement Contusion Hematoma Hypoxia Diffuse Axonal Injury Ross Bullock, MD, PhD. Director, Neurotrauma,- University
Is Neuromonitoring an expensive waste of time, in Severe Traumatic Brain Injury? Edema Engorgement Contusion Hematoma Hypoxia Diffuse Axonal Injury Ross Bullock, MD, PhD. Director, Neurotrauma,- University
5.5. RETROSIGMOID APPROACH
 5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
Decompressive Craniectomy: Surgical Indications, Clinical Considerations and Rationale
 23 Decompressive Craniectomy: Surgical Indications, Clinical Considerations and Rationale Dare Adewumi and Austin Colohan Loma Linda University Medical Center Department of Neurosurgery Loma Linda USA
23 Decompressive Craniectomy: Surgical Indications, Clinical Considerations and Rationale Dare Adewumi and Austin Colohan Loma Linda University Medical Center Department of Neurosurgery Loma Linda USA
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Neuropathology Of Head Trauma. Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center
 Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Traumatic Brain Injury:
 Traumatic Brain Injury: Changes in Management Across the Spectrum of Age and Time Omaha 2018 Trauma Symposium June 15, 2018 Gail T. Tominaga, M.D., F.A.C.S. Scripps Memorial Hospital La Jolla Outline Background
Traumatic Brain Injury: Changes in Management Across the Spectrum of Age and Time Omaha 2018 Trauma Symposium June 15, 2018 Gail T. Tominaga, M.D., F.A.C.S. Scripps Memorial Hospital La Jolla Outline Background
ORIGINAL ARTICLES ABSTRACT
 Venous thromboembolism prophylaxis in the critically ill: a point prevalence survey of current practice in Australian and New Zealand intensive care units Megan S Robertson, Alistair D Nichol, Alisa M
Venous thromboembolism prophylaxis in the critically ill: a point prevalence survey of current practice in Australian and New Zealand intensive care units Megan S Robertson, Alistair D Nichol, Alisa M
Craniosynostosis and Plagiocephaly
 Craniosynostosis and Plagiocephaly Andrew Jea MD MHA FAAP Professor and Chief Section of Pediatric Neurosurgery Riley Hospital for Children Department of Neurosurgery Indiana University School of Medicine
Craniosynostosis and Plagiocephaly Andrew Jea MD MHA FAAP Professor and Chief Section of Pediatric Neurosurgery Riley Hospital for Children Department of Neurosurgery Indiana University School of Medicine
Case 1. Case 5/30/2013. Traumatic Brain Injury : Review, Update, and Controversies
 Case 1 Traumatic Brain Injury : Review, Update, and Controversies Shirley I. Stiver MD, PhD 32 year old male s/p high speed MVA Difficult extrication Intubated at scene Case BP 75 systolic / palp GCS 3
Case 1 Traumatic Brain Injury : Review, Update, and Controversies Shirley I. Stiver MD, PhD 32 year old male s/p high speed MVA Difficult extrication Intubated at scene Case BP 75 systolic / palp GCS 3
Dr. Sami Zaqout, IUG Medical School
 The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE
 Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE 1 The two parietal bones articulate in the midline AT THE SAGITTAL
Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE 1 The two parietal bones articulate in the midline AT THE SAGITTAL
THIEME. Scalp and Superficial Temporal Region
 CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
Clinical Guideline. Thoracic Society of Australia and New Zealand. November Approved by Board: 22nd September 2016
 Thoracic Society of Australia and New Zealand Recognition of Competency in Thoracic Ultrasound Clinical Guideline November 2016 Approved by Board: 22nd September 2016 Document Review Date: November 2021
Thoracic Society of Australia and New Zealand Recognition of Competency in Thoracic Ultrasound Clinical Guideline November 2016 Approved by Board: 22nd September 2016 Document Review Date: November 2021
Comparison of Burr Holes and Decompressive Craniotomy in the Surgical Treatment of Traumatic Acute Subdural Hematoma
 Med. J. Cairo Univ., Vol. 83, No. 1, March: 259-266, 2015 www.medicaljournalofcairouniversity.net Comparison of Burr Holes and Decompressive Craniotomy in the Surgical Treatment of Traumatic Acute Subdural
Med. J. Cairo Univ., Vol. 83, No. 1, March: 259-266, 2015 www.medicaljournalofcairouniversity.net Comparison of Burr Holes and Decompressive Craniotomy in the Surgical Treatment of Traumatic Acute Subdural
Cranial Postoperative Site: MR Imaging Appearance
 27 Cranial Postoperative Site: MR Imaging Appearance Charles F. Lanzieri1 Mark Larkins2 Andrew Mancall 1 Ronald Lorig 1 Paul M. Duchesneau 1 Scott A. Rosenbloom 1 Meredith A. Weinstein 1 The ability to
27 Cranial Postoperative Site: MR Imaging Appearance Charles F. Lanzieri1 Mark Larkins2 Andrew Mancall 1 Ronald Lorig 1 Paul M. Duchesneau 1 Scott A. Rosenbloom 1 Meredith A. Weinstein 1 The ability to
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Surgical management of diastatic linear skull fractures in infants
 Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
OPERATIVE CORRECTION BY OSTEOTOMY OF RECESSED MALAR MAXILLARY COMPOUND IN A CASE OF OXYCEPHALY
 OPERATIVE CORRECTION BY OSTEOTOMY OF RECESSED MALAR MAXILLARY COMPOUND IN A CASE OF OXYCEPHALY By Sir HAROLD GILLIES, C.B.E., F.R.C.S., and STEWART H. HARRISON, F.R.C.S., L.D.S., R.C.S. From the Plastic
OPERATIVE CORRECTION BY OSTEOTOMY OF RECESSED MALAR MAXILLARY COMPOUND IN A CASE OF OXYCEPHALY By Sir HAROLD GILLIES, C.B.E., F.R.C.S., and STEWART H. HARRISON, F.R.C.S., L.D.S., R.C.S. From the Plastic
For Emergency Doctors. Dr Suzanne Smallbane November 2011
 For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D.
 J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
be very thin and variable. Facial nerve branches that exit the parotid gland are deep to the SMAS.
 The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
Update sulle lesioni emorragiche posttraumatiche
 Update sulle lesioni emorragiche posttraumatiche Corrado Iaccarino Neurochirurgia-Neurotraumatologia AOU Parma Neurochirurgia d'urgenza IRCCS ASMN Reggio Emilia LAW UPDATING This document provides recommendations
Update sulle lesioni emorragiche posttraumatiche Corrado Iaccarino Neurochirurgia-Neurotraumatologia AOU Parma Neurochirurgia d'urgenza IRCCS ASMN Reggio Emilia LAW UPDATING This document provides recommendations
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature
 Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
Saline or Albumin for Fluid Resuscitation in Patients with Traumatic Brain Injury
 T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Saline or Albumin for Fluid Resuscitation in Patients with Traumatic Brain Injury The SAFE Study Investigators* A bs tr ac t The
T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Saline or Albumin for Fluid Resuscitation in Patients with Traumatic Brain Injury The SAFE Study Investigators* A bs tr ac t The
Transcranial resection of tumors of the paranasal sinuses and nasal cavity
 J Neurosurg 71:10-15, 1989 Transcranial resection of tumors of the paranasal sinuses and nasal cavity J. BoB BLACKLOCK, M.D., RANDAL S. WEBER, M.D., YA-YEN LEE, M.D., AND HELMUTH GOEPFERT~ M.D. Section
J Neurosurg 71:10-15, 1989 Transcranial resection of tumors of the paranasal sinuses and nasal cavity J. BoB BLACKLOCK, M.D., RANDAL S. WEBER, M.D., YA-YEN LEE, M.D., AND HELMUTH GOEPFERT~ M.D. Section
Site Accreditation for Rehabilitation Medicine
 Site Accreditation for Rehabilitation Medicine Last updated September 2018 Hospital State Status No. of University of Canberra Hospital ACT Accredited 4 General, Neurological, Geriatric, Community Feb
Site Accreditation for Rehabilitation Medicine Last updated September 2018 Hospital State Status No. of University of Canberra Hospital ACT Accredited 4 General, Neurological, Geriatric, Community Feb
Bone flap preservation in abdominal wall after decompressive craniectomy in head injury: A single institute experience
 DOI: 10.2478/romneu-2018-0063 Article Bone flap preservation in abdominal wall after decompressive craniectomy in head injury: A single institute experience Pavan Kumar, Ashok Kumar, Gaurav Jaiswal, Tarun
DOI: 10.2478/romneu-2018-0063 Article Bone flap preservation in abdominal wall after decompressive craniectomy in head injury: A single institute experience Pavan Kumar, Ashok Kumar, Gaurav Jaiswal, Tarun
Anterior Communicating Artery Aneurysms. Surgical approaches Review
 Anterior Communicating Artery Aneurysms. Surgical approaches Review Hirotoshi Sano Dept. of Neurosurgery Fujita Health University Introduction There are two main types of approaches for anterior communicating
Anterior Communicating Artery Aneurysms. Surgical approaches Review Hirotoshi Sano Dept. of Neurosurgery Fujita Health University Introduction There are two main types of approaches for anterior communicating
Accredited Sites for Advanced Training Palliative Medicine Updated October 2018
 Accredited Sites for Advanced Training Palliative Medicine Updated October 2018 Training Terms 1 (Inpatient unit/hospice), 2 (Community) and 3 (Teaching Hospital/Consultation) should be completed at two
Accredited Sites for Advanced Training Palliative Medicine Updated October 2018 Training Terms 1 (Inpatient unit/hospice), 2 (Community) and 3 (Teaching Hospital/Consultation) should be completed at two
Integra B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE
 Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA
 SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA LEARNING OBJECTIVES At the end of this lecture, the student should be able to know: Parts of skeleton (axial and appendicular) Parts of skull Sutures of skull
SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA LEARNING OBJECTIVES At the end of this lecture, the student should be able to know: Parts of skeleton (axial and appendicular) Parts of skull Sutures of skull
Accredited Sites for Advanced Training Palliative Medicine Updated January 2019
 Accredited Sites for Advanced Training Palliative Medicine Updated January 2019 IMPORTANT NOTE: Training Terms 1 (Inpatient unit/hospice), 2 (Community) and 3 (Teaching Hospital/Consultation) should be
Accredited Sites for Advanced Training Palliative Medicine Updated January 2019 IMPORTANT NOTE: Training Terms 1 (Inpatient unit/hospice), 2 (Community) and 3 (Teaching Hospital/Consultation) should be
A PLEA FOR LATERAL ORBITOTOMY WITH CERTAIN MODIFICATIONS*
 Brit. J. Ophthal. (1960) 44, 718. A PLEA FOR LATERAL ORBITOTOMY WITH CERTAIN MODIFICATIONS* BY H. B. STALLARD London THE frontiers of human interest and work are often disputed and, there is no exception
Brit. J. Ophthal. (1960) 44, 718. A PLEA FOR LATERAL ORBITOTOMY WITH CERTAIN MODIFICATIONS* BY H. B. STALLARD London THE frontiers of human interest and work are often disputed and, there is no exception
North Oaks Trauma Symposium Friday, November 3, 2017
 + Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
+ Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
Keyhole craniectomy in the surgical management of spontaneous intracerebral hematoma
 Neurology Asia 2007; 12 : 21 27 Keyhole craniectomy in the surgical management of spontaneous intracerebral hematoma S Balaji Pai, RG Varma, JKBC Parthiban, KN Krishna, RM Varma, *R Srinivasa,*PT Acharya,*BP
Neurology Asia 2007; 12 : 21 27 Keyhole craniectomy in the surgical management of spontaneous intracerebral hematoma S Balaji Pai, RG Varma, JKBC Parthiban, KN Krishna, RM Varma, *R Srinivasa,*PT Acharya,*BP
Fracture frontal bone and its management
 From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
4.3 Surgical Management of anterior skull synostosis
 ISPN course 23 rd Nov, 2015 Cranial & Craniofacial disorders 4.3 Surgical Management of anterior skull synostosis Kazuaki Shimoji, Masakazu Miyajima and Hajime Arai Department of Neurosurgery, Juntendo
ISPN course 23 rd Nov, 2015 Cranial & Craniofacial disorders 4.3 Surgical Management of anterior skull synostosis Kazuaki Shimoji, Masakazu Miyajima and Hajime Arai Department of Neurosurgery, Juntendo
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
The University Hospital/ 90! Twenty-Third.Street, N.IV./ Washington, D.C Representatives Select Committee on Assassinations Staff Member
 222 ADDENDUM D REPORT OF DAVID O. DAVIS, M.D., CONCERNING THE EXAMINATION OF THE AUTOPSY X-RAYS OF PRESIDENT JOHN F. KENNEDY, DATED AUGUST 23, 1975 REPORT OF DAVID 0. DAVIS, M.D., CONCERNING THE EXAMINATION
222 ADDENDUM D REPORT OF DAVID O. DAVIS, M.D., CONCERNING THE EXAMINATION OF THE AUTOPSY X-RAYS OF PRESIDENT JOHN F. KENNEDY, DATED AUGUST 23, 1975 REPORT OF DAVID 0. DAVIS, M.D., CONCERNING THE EXAMINATION
Chapter 7: Head & Neck
 Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
Occipital flattening in the infant skull
 Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Microsurgery for ruptured cerebellar arteriovenous malformations
 European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
Cranial cavity. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Cranial cavity Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology The Meninges The brain in the skull is surrounded by three membranes or meninges: 1-DURA MATER 2-ARACHNOID MATER 3-PIA MATER
Cranial cavity Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology The Meninges The brain in the skull is surrounded by three membranes or meninges: 1-DURA MATER 2-ARACHNOID MATER 3-PIA MATER
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery
 Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
TBI are twice as common in males High potential for poor outcome Deaths occur at three points in time after injury
 Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
F OR several years we have used a linear. Limited exposure in cerebral surgery. Technical note. trephine aid drill. Technique
 Technical note DONALD H. WILSON, M.D. Section o/ Neurosurgery, Dartmouth-Hitchcock Medical Center, Hanover, New Hampshire ~' A limited exposure is possible, and perhaps preferable, for most cerebral surgery.
Technical note DONALD H. WILSON, M.D. Section o/ Neurosurgery, Dartmouth-Hitchcock Medical Center, Hanover, New Hampshire ~' A limited exposure is possible, and perhaps preferable, for most cerebral surgery.
Brain Meninges, Ventricles and CSF
 Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Traumatic Brain Injury TBI Presented by Bill Masten
 1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
SURGICAL PROCEDURES OPERATIONS ON THE NERVOUS SYSTEM
 98100 Hypothermia - when employed, basic fee for any procedure on nervous system... 25 25 BRAIN Astrocytoma, oligodendroglioma, glioblastoma or metastatic tumour Craniotomy plus excision 98130 - supratentorial...
98100 Hypothermia - when employed, basic fee for any procedure on nervous system... 25 25 BRAIN Astrocytoma, oligodendroglioma, glioblastoma or metastatic tumour Craniotomy plus excision 98130 - supratentorial...
cally, a distinct superior crease of the forehead marks this spot. The hairline and
 4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
Chapter XII: Temporal Expanding Processes, Including Those in the Sylvian Fissure and the Insula
 Acta Radiologica ISSN: 0001-6926 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iaro20 Chapter XII: Temporal Expanding Processes, Including Those in the Sylvian Fissure and the Insula
Acta Radiologica ISSN: 0001-6926 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iaro20 Chapter XII: Temporal Expanding Processes, Including Those in the Sylvian Fissure and the Insula
Long-term follow-up of motor function deterioration following microsurgical resection of middle third parasagittal and falx meningioma
 Elzarief and Ibrahim The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2018) 54:9 https://doi.org/10.1186/s41983-018-0013-3 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery
Elzarief and Ibrahim The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2018) 54:9 https://doi.org/10.1186/s41983-018-0013-3 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery
Cranial cavity. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 Cranial cavity Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Cerebrum Cerebral hemispheres The Meninges The brain in the skull is surrounded by three membranes or meninges: 1-THE DURA
Cranial cavity Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Cerebrum Cerebral hemispheres The Meninges The brain in the skull is surrounded by three membranes or meninges: 1-THE DURA
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
OBJECTIVES. At the end of the lecture, students should be able to: List the cerebral arteries.
 DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: List the cerebral arteries. Describe the cerebral arterial supply regarding the origin, distribution and branches.
DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: List the cerebral arteries. Describe the cerebral arterial supply regarding the origin, distribution and branches.
Open skull fractures with brain fungation: Simple principles for good outcome experience
 outcome Our experience. IAIM, 2015; 2(9): 65-69. Original Research Article Open skull fractures with brain fungation: Simple principles for good outcome Our experience M. V. Vijaya Sekhar 1, K.V. Ramprasad
outcome Our experience. IAIM, 2015; 2(9): 65-69. Original Research Article Open skull fractures with brain fungation: Simple principles for good outcome Our experience M. V. Vijaya Sekhar 1, K.V. Ramprasad
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Unit 18: Cranial Cavity and Contents
 Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
The SCALP. Prof. Dr. Muhammad Imran Qureshi
 The SCALP By Prof. Dr. Muhammad Imran Qureshi The SCALP includes FIVE layers external to the Calvaria. These are: S: Skin & Superficial Fascia C: Connective Tissue A: Aponeurosis (Epicranial) L: Loose
The SCALP By Prof. Dr. Muhammad Imran Qureshi The SCALP includes FIVE layers external to the Calvaria. These are: S: Skin & Superficial Fascia C: Connective Tissue A: Aponeurosis (Epicranial) L: Loose
External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS.
 External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS. External Ventricular Drain Indications: Therapeutic (To relieve raised
External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS. External Ventricular Drain Indications: Therapeutic (To relieve raised
The clinical scenario in this patient has been well reviewed by expert witnesses.
 September 29, 2014 Michael J. Cronkright, Esq. Kronzek & Cronkight, PLLC 420 S. Waverly Road, Suite 100 Lansing, MI 48917 Re: Preliminary Report on Naomi Burns Dear Mr. Cronkright, I have reviewed all
September 29, 2014 Michael J. Cronkright, Esq. Kronzek & Cronkight, PLLC 420 S. Waverly Road, Suite 100 Lansing, MI 48917 Re: Preliminary Report on Naomi Burns Dear Mr. Cronkright, I have reviewed all
Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
 Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Two-Stage Management of Mega Occipito Encephalocele
 Two-Stage Management of Mega Occipito Encephalocele CASE REPORT A I Mardzuki*, J Abdullah**, G Ghazaime*, A R Ariff!'*, M Ghazali* *Department of Neurosciences, **Department of Radiology, Hospital Universiti
Two-Stage Management of Mega Occipito Encephalocele CASE REPORT A I Mardzuki*, J Abdullah**, G Ghazaime*, A R Ariff!'*, M Ghazali* *Department of Neurosciences, **Department of Radiology, Hospital Universiti
Wicking Project Presentations
 Wicking Project Presentations VAADA Conference 2007 Health for all: Advocating for people who use alcohol and other drugs. 13-14 th February 2007. Melbourne. Averting incremental health decline among older
Wicking Project Presentations VAADA Conference 2007 Health for all: Advocating for people who use alcohol and other drugs. 13-14 th February 2007. Melbourne. Averting incremental health decline among older
A Comparison of Albumin and Saline for Fluid Resuscitation in the Intensive Care Unit
 The new england journal of medicine original article A Comparison of Albumin and Saline for Fluid Resuscitation in the Intensive Care Unit The SAFE Study Investigators* abstract background It remains uncertain
The new england journal of medicine original article A Comparison of Albumin and Saline for Fluid Resuscitation in the Intensive Care Unit The SAFE Study Investigators* abstract background It remains uncertain
We describe some of the conceptual nuances and
 Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
Index. Note: Page numbers of article titles are in bold face type.
 Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Quality Metrics. Stroke Related Procedure Outcomes
 Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
TITLE: CSF RHINORRHOEA SECONDARY TO MAYFIELD HEAD CLAMP
 TITLE: CSF RHINORRHOEA SECONDARY TO MAYFIELD HEAD CLAMP Authors Mr Ioannis Moumoulidis (MRCS), Miss Helen Fernandes (FRCS), Mr Ran De (FRCS) Institution Department of Neurosurgery / Otolaryngology University
TITLE: CSF RHINORRHOEA SECONDARY TO MAYFIELD HEAD CLAMP Authors Mr Ioannis Moumoulidis (MRCS), Miss Helen Fernandes (FRCS), Mr Ran De (FRCS) Institution Department of Neurosurgery / Otolaryngology University
Chapter 8: Cerebral protection Stephen Lo
 Chapter 8: Cerebral protection Stephen Lo Introduction There will be a variety of neurological pathologies that you will see within the intensive care. The purpose of this chapter is not to cover all neurological
Chapter 8: Cerebral protection Stephen Lo Introduction There will be a variety of neurological pathologies that you will see within the intensive care. The purpose of this chapter is not to cover all neurological
