Fabry disease (FD) is a rare X-linked lysosomal storage
|
|
|
- Suzan Farmer
- 5 years ago
- Views:
Transcription
1 High-Sensitivity Troponin: A Clinical Blood Biomarker for Staging Cardiomyopathy in Fabry Disease Nora Seydelmann, MD; Dan Liu, MD; Johannes Kr amer, MD; Christiane Drechsler, MD; Kai Hu, MD; Peter Nordbeck, MD; Andreas Schneider, MD; Stefan St ork, MD, PhD; Bart Bijnens, PhD; Georg Ertl, MD; Christoph Wanner, MD; Frank Weidemann, MD Background- High-sensitivity troponin (hs-tnt), a biomarker of myocardial damage, might be useful for assessing fibrosis in Fabry cardiomyopathy. We performed a prospective analysis of hs-tnt as a biomarker for myocardial changes in Fabry patients and a retrospective longitudinal follow-up study to assess longitudinal hs-tnt changes relative to fibrosis and cardiomyopathy progression. Methods and Results- For the prospective analysis, hs-tnt from 75 consecutive patients with genetically confirmed Fabry disease was analyzed relative to typical Fabry-associated echocardiographic findings and total myocardial fibrosis as measured by late gadolinium enhancement (LE) on magnetic resonance imaging. Longitudinal data ( years), including hs-tnt, LE, and echocardiographic findings from 58 Fabry patients, were retrospectively collected. Hs-TNT level positively correlated with LE (linear correlation coefficient, 0.72; odds ratio, [95% CI, ]; P=0.002); patients with elevated baseline hs-tnt (>14 ng/ L) showed significantly increased LE (median: baseline, 1.9 [ ] %; follow-up, 3.2 [ ] %; P<0.001) and slightly elevated hs-tnt (baseline, 44.7 [ ] ng/l; follow-up, 49.1 [ ] ng/l; P=0.116) during follow-up. Left ventricular wall thickness and EF of patients with elevated hs-tnt were decreased during follow-up, indicating potential cardiomyopathy progression. Conclusions- hs-tnt is an accurate, easily accessible clinical blood biomarker for detecting replacement fibrosis in patients with Fabry disease and a qualified predictor of cardiomyopathy progression. Thus, hs-tnt could be helpful for staging and follow-up of Fabry patients. ( J Am Heart Assoc. 2016;5:e doi: /JAHA ) Key Words: biomarker cardiomyopathy fabry disease myocardial fibrosis troponin T Fabry disease (FD) is a rare X-linked lysosomal storage disorder caused by a mutation in the gene encoding hydrolase alpha-galactosidase A, leading to a deficiency of this enzyme. The consequence is a progressive intracellular accumulation of globotriaosylceramide (Gb3) in lysosomes of various tissues and organs. The most commonly affected organs are heart, vascular endothelium of the kidney, nervous system, eyes, and skin. 1 3 Typical clinical manifestations of FD include angiokeratoma, hypohydrosis, acroparesthesia, From the Medizinische Klinik I, University Hospital W urzburg, and Comprehensive Heart Failure Center, W urzburg, Germany (N.S., D.L., J.K., C.D., K.H., P.N., A.S., S.S., G.E., C.W., F.W.); ICREA Universitat Pompeu Fabra, Barcelona, Spain (B.B.); Innere Klinik II, Katharinen-Hospital, Unna, Germany (F.W.). Correspondence to: Frank Weidemann, MD, Innere Klinik II, Katharinen- Hospital Unna, Obere Husemannstr 2, D Unna, Germany. f.weidemann@katharinen-hospital.de Received January 18, 2016; accepted April 7, ª 2016 The Authors. Published on behalf of the American Heart Association, Inc., by Wiley Blackwell. This is an open access article under the terms of the Creative Commons Attribution-NonCommercial License, which permits use, distribution and reproduction in any medium, provided the original work is properly cited and is not used for commercial purposes. pain crises, and gastrointestinal symptoms such as diarrhea. Progressive Gb3 accumulation in the microvasculature causes ischemic damages, especially affecting the kidney, brain, and heart, which may cause symptoms related to renal failure, stroke, and cardiovascular diseases. 4 Cardiac manifestations, including arrhythmias, chronic heart failure, and small vessel disease, occur frequently. Storage of Gb3 in myocytes causes a regional concentric left ventricular (LV) hypertrophy (LVH) and results in intramural replacement fibrosis, first limited to the mid-myocardial layers of the posterolateral wall and then spreading to transmural fibrosis. 5 8 This myocardial fibrosis is a typical finding of more-advanced stages of Fabry cardiomyopathy 5,6 and seems to be a major factor in cardiac arrhythmias and heart failure, which increase morbidity and reduce life expectancy. 5,7,9 11 The most reliable noninvasive method of detecting myocardial fibrosis is by late gadoliniumenhanced (LE) magnetic resonance imaging (MRI). 6,12 Biomarkers such as cardiac troponin T (TNT) and brain natriuretic peptide (BNP) are established in the diagnosis of myocardial infarction (MI) and chronic heart failure, and high-sensitivity (hs) TNT has been used to detect myocardial tissue damage. To date, however, no detailed study has DOI: /JAHA Journal of the American Heart Association 1
2 assessed the use of biomarkers to detect myocyte turnover toward myocardial fibrosis in patients with FD. We hypothesized that level of hs-tnt correlates with myocardial fibrosis and investigated biomarkers, such as hs-tnt and N-terminal probnp (NT-proBNP), subsequently correlating the findings with myocardial fibrosis as measured by LE MRI. Methods Study Protocol The present study comprises 2 analyses: a prospective analysis to evaluate the relevance of biomarkers such as hs- TNT and NT-proBNP for detecting myocardial changes in Fabry patients and a retrospective longitudinal follow-up study to evaluate longitudinal changes in hs-tnt in relation to fibrosis, investigate the impact of hs-tnt on progression of cardiomyopathy, and evaluate the use of frozen blood for measuring hs- TNT. For the prospective part of the study, all patients with genetically confirmed FD who were observed between February 2013 and June 2014 at the Fabry center in Wuerzburg were screened. Criteria for inclusion were (1) genetically proven FD, (2) availability of blood samples for measurement of hs-tnt and NT-proBNP, (3) no contraindications to contrast agent-enhanced MRI, and (4) informed consent for examination and participation in the study. Exclusion criteria were contraindications to LE- MRI, such as claustrophobia, an implanted cardiac pacemaker, or end-stage renal dysfunction requiring chronic dialysis. Overall, 75 patients were included for the prospective analyses. In the context of a routine appointment as part of a clinical investigation program for Fabry patients, blood was taken and analyzed for hs-tnt and NT-proBNP. To evaluate the stage of Fabry cardiomyopathy, MRI with LE and echocardiography were performed within 24 hours. Typical Fabry-related parameters, symptoms, and comorbidities were determined by patient interviews and clinical record. A clinical examination was done by a doctor specialized in FD. In addition, 24- hour urine samples were collected. The retrospective cohort consisted of 58 Fabry patients for whom frozen blood samples were available for assessment of hs-tnt, as were patient records of MRI and echocardiography at baseline and after years. For the analyses, we separated the cohorts into 4 groups according to stage of cardiomyopathy, depending on myocardial fibrosis as measured by LE imaging and LVH and myocardial function as assessed by echocardiography, as follows: group 1, no cardiomyopathy, meaning no LE findings, no LVH (interventricular septal thickness at diastole [IVSd] <12 mm), and normal ejection fraction (EF; 55%); group 2, mild cardiomyopathy, consisting of LV hypertrophy (IVSd 12 mm) but no LE and normal EF ( 55%); group 3, intermediate cardiomyopathy, consisting of patients who were LE positive but had normal EF ( 55%); and group 4, end-stage cardiomyopathy, with reduced EF (<55%) and with fibrosis (LE positive). Written informed consent was obtained from all patients or their guardians. The study was approved by the Local Ethics Committee at the University of W urzburg and conducted in accord to the Declaration of Helsinki. Assessment of hs-tnt and NT-proBNP All serum concentrations of hs-tnt and NT-proBNP were measured in the laboratory of the Wuerzburg University Hospital using the Novel Electrochemiluminescence (ECL) technology on Roche Cobas e411 (Roche Diagnostics GmbH, Mannheim, Germany). Peripheral venous blood was taken from our cohort collected in serum tubes. In the prospective part of this study, fresh blood samples were immediately centrifuged at 50009U/min for 10 minutes; afterward, serum was analyzed within 1 hour. For the retrospective part, frozen serum was used to measure the level of the biomarkers. In this cohort, the blood samples were taken, at their first visit to our Fabry center (baseline) and at a follow-up visit at the latest time point possible. Serum tubes were also centrifuged at 50009U/min for 10 minutes, divided into aliquots, and stored at 80 C until analysis. After defrosting at room temperature to around 20 C degrees, samples were again centrifuged at 50009U/min for 10 minutes and analyzed. The reference ranges for hs-tnt were as follows: <5 ng/l, below the detection limit; 5 to 13.9 ng/l, detectable but normal; and 14 ng/l, elevated. 17,18 N-terminal of the prohormone brain natriuretic peptide (NTproBNP) was applied as a rule-out test for heart failure. Cutoff values were based on the recommendations by previous studies in acute and chronic health care settings (acute heart failure, 300 pg/ml; chronic heart failure: <60 years, 50 pg/ ml; years, 100 pg/ml; >75 years, 250 pg/ml). 19,20 Standard Echocardiographic Measurements All echocardiographic examinations were performed using standard ultrasound equipment (3.5 MHz; GE VingMed Vivid 7; GE VingMed, Horten, Norway). LV end-diastolic diameter (LVEDD), LV end-systolic diameter (LVESD), and end-diastolic wall thickness of the LV posterior wall (LVPWd) and the septum (IVSd) were manually measured from parasternal long-axis images using standard M-mode. Furthermore, left atrial diameter was measured, and the LV fraction shortening was calculated from LVEDD and LVESD. LV ejection fraction (LVEF) was measured with the biplane Simpson method in apical 4- and 2-chamber views. By placing a blood DOI: /JAHA Journal of the American Heart Association 2
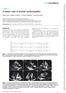
3 pool pulsed Doppler between the tips of the mitral valve leaflets, the peak in early (E) and late (A) diastolic flow velocity was measured, to yield the E/A ratio, and the deceleration time was extracted. Another parameter to evaluate diastolic function was the ratio of mitral peak velocity (E/E 0 ) calculated by measuring the ratio between early transmitral flow and peak early tissue Doppler velocity. LV mass, indexed to body surface area (LVMI), was estimated by LV cavity dimension and wall thickness at end diastole: LV mass (g)=0.89[1.049 (LVEDD+LVPWd+IVSd) 3 LVEDD 3 ]+0.6. Systolic pulmonary artery pressure (SPAP) was derived from peak tricuspid regurgitation (TR) jet velocity, using the simplified Bernoulli equation in combination with an estimated right atrial pressure (RAP): SPAP=4V 2 +RAP, where V is the peak TR jet velocity. RAP was estimated from inferior vena cava diameter and respiratory changes. Assessment of Fibrosis Cardiac MRI was performed in all patients using a 1.5 Tesla scanner (Magnetom Symphony Quantum; Siemens Medical Systems, Erlangen, Germany), after intravenous injection of gadopentetate dimeglumine 0.2 mmol/kg (Magnevist; Bayer HealthCare AG, Leverkusen, Germany). LE images were obtained with T1 inversion recovery sequences (8-mm slice thickness, breath hold, field of view mm 2, matrix size , repetition time 7.5 ms, echo time 3.4 ms, and flip angle 258). Areas with pathological mid- or transmural LE were measured manually in the basal, mid, and apical segments, covering the entire ventricle using continuous short-axis views. The sum of all enhanced areas was multiplied by the slice thickness and then set in relation to the LV myocardial volume. With this technique, every LV segment was scanned separately for occurrence of pathological LE. Attention was paid to a similar setting for the followup scan. Statistical Analysis Continuous data are presented as meansd or median (25th, 75th percentiles) and categorical variables as numbers (percentages). Differences in continuous data among 3 groups were compared using 1-way ANOVA after normalization, if indicated, followed by appropriate post-hoc tests for multiple comparisons (Tukey s if equal variances assumed; Games- Howell if equal variances not assumed). Pair-wise comparisons were only conducted if the global test was significant. Statistical significance was assumed at Bonferroni-adjusted P<0.025 (3 groups). Differences between baseline and follow up among 3 groups were compared using repeated-measures ANOVA followed by the appropriate post-hoc test for multiple comparisons. Non-normally distributed variables (hs-tnt and NT-proBNP) were normalized before analysis using natural logarithm values (Ln). Correlation between hs-tnt categories and other clinical and echocardiographic parameters were studied with the Spearman rank correlation (r s ). The difference between groups was compared using independentsamples t test. Categorical data were compared across groups using the chi-square test. Logistic regression was used to assess significant determinants of elevated hs-tnt. A P<0.05 (2 groups) was considered statistically significant, and all statistical analysis was performed using IBM SPSS software (version 22 for Windows; SPSS, Inc., Chicago, IL). Results Prospective Cohort Our prospective cohort of 75 patients with a mean age of 4314 years included 47 women and 28 men. Average body mass index (BMI) was normal (mean 255 kg/m 2 ). No patient had a history of MI, only 1 patient had undergone a coronary bypass operation, and 3 patients had coronary artery disease (CAD). Three patients had chronic heart failure corresponding with New York Heart Association (NYHA) class III or IV. Mean glomerular filtration rate (GFR) was in normal range (8323 ml/min), 29.3% (n=22) of patients had proteinuria, 84.2% had normal renal function, 7.9% (n=6) had a moderately reduced kidney function (stage III of chronic kidney disease [CKD], GFR between 30 and 59 ml/min), and 4.0% (n=3) had severely reduced kidney function (stage IV of CKD, GFR ml/min). Patients with end-stage renal disease (ESRD; 1.33%; n=1) were excluded. The median hs-tnt of the cohort was 7.7 ng/l, with a wide range of 4 to 278 ng/l. Of the 75 patients, 30 (40%) had an elevated hs-tnt (>14 ng/l). The general clinical data for all patients adjusted to the level of hs-tnt (<5, 5 14, and >14 ng/l) are presented in Table 1. Of note are some correlations between level of hs-tnt and other typical Fabry symptoms. Separation of the cohort into the stages of Fabry cardiomyopathy according to the above-mentioned criteria resulted in 38 patients with no cardiomyopathy, 3 with mild cardiomyopathy, 31 with intermediate cardiomyopathy, and 3 with end-stage cardiomyopathy (Figure 1). Patients with no or mild cardiomyopathy had low levels of hs-tnt, whereas those with intermediate and end-stage cardiomyopathy had elevated levels (Figure 1). Table 2 shows echocardiographic and MRI characteristics of the prospective cohort. LV wall thickness, LVMI on echocardiography, and MRI, E/E 0, and LE-positive myocardial volume gradually increased with increasing hs-tnt. All but 1 patient (97%) with an elevated hs-tnt >14 ng/l showed fibrosis as assessed by LE on MRI. DOI: /JAHA Journal of the American Heart Association 3
4 Table 1. Clinical Characteristics Among Subgroups According to hs-tnt Level in the Prospective Cohort (n=75) Total hs-tnt <5 ng/l hs-tnt 5 to 14 ng/l hs-tnt >14 ng/l n=75 n=29 n=16 n=30 Age, y Female, n (%) 47 (62.7) 19 (65.5) 12 (75) 16 (53.3) BMI, kg/m² hs-tnt*, ng/l 7.7 (4 20.8) ( ) 24.2 ( ) NT-proBNP*, pg/ml 99 (41 224) 49.5 ( ) 80.5 ( ) 221 ( ) Cardiovascular, n (%) NYHA class III/IV 3 (4.0) 1 (3.4) 0 (0) 2 (6.7) CAD 3 (4.0) (10.0) MI Bypass 1 (1.3) (3.3) ICD/pacemaker 7 (6.7) (16.7) Renal egfr, ml/min Creatinine, mg/dl Proteinuria, n (%) 22 (29.3) 6 (20.7) 2 (12.5) 14 (46.7) Renal insufficiency: 0/I/II/III/IV, % 64/0/2/6/3 (84.2/0/2.6/7.9/4.0) 28/0/1/0/0 (96.6/0/3.4/0/0) 14/0/0/2/0 (87.5/0/0/12.5/0) Renal transplantation, n (%) 3 (4.0) (10.0) Neurological, n (%) Vertigo 37 (49.3) 11 (37.9) 10 (62.5) 16 (53.3) Tinnitus 24 (32.0) 5 (17.2) 4 (25.0) 15 (50) Hearing loss 11 (14.7) 1 (3.4) 3 (18.8) 7 (23.3) Depression 7 (9.3) 2 (6.9) 2 (12.5) 3 (10.0) Dysarthria 6 (8.0) 2 (6.9) 1 (6.3) 3 (10.0) TIA 6 (8.0) 3 (10.3) 1 (6.3) 2 (6.7) Stroke 7 (9.3) 1 (3.4) 1 (6.3) 5 (16.7) Gastrointestinal, n (%) Nausea 7 (9.3) 3 (10.3) 1 (6.3) 3 (10.0) Diarrhea 24 (32.0) 5 (17.2) 5 (31.3) 14 (46.7) Abdominal pain 21 (28.0) 5 (17.2) 5 (31.3) 11 (36.7) Acroparesthesia, n (%) 43 (57.3) 16 (55.2) 8 (50) 19 (63.3) Chronic pain, n (%) 20 (26.7) 8 (27.6) 2 (12.5) 10 (33.3) Pain crisis, n (%) 24 (32.0) 10 (34.5) 3 (18.8) 11 (36.7) Medication, n (%) ACE/AT1 46 (61.3) 8 (27.6) 12 (75) 26 (86.7) ß-blockers 10 (13.3) 3 (10.3) 2 (12.5) 5 (16.7) Calcium antagonists 3 (4.0) 1 (3.4) 0 (0) 2 (6.7) Anticoagulant 4 (5.3) (13.3) Regular pain medication 13 (17.3) 6 (20.7) 1 (6.3) 6 (20.0) 22/0/1/4/3 (71/0/3.2/12.9/10.0) ACE indicates angiotensin-converting enzyme inhibitor; AT1, angiotensin II type 1 antagonists; BMI, body mass index; CAD, coronary arterial disease; egfr, estimated glomerular filtration rate; hs-tnt, high-sensitivity cardiac troponin T; ICD, implantable cardioverter-defibrillator; MI, myocardial infarction; NT-proBNP, N-terminal of the prohormone brain natriuretic peptide; NYHA, New York Heart Association; TIA, transient ischemic attack. *Natural logarithm (Ln) transformed. Bonferroni-adjusted P<0.025 vs hs-tnt <5 ng/l; P<0.025 vs hs-tnt 5 to 14 ng/l. DOI: /JAHA Journal of the American Heart Association 4
5 Figure 1. High-sensitivity cardiac troponin T (hs-tnt) levels in Fabry patients with different stages of cardiomyopathy (CM). Box plots represent median levels with 25th and 75th percentiles of observed data whereas whiskers indicate the 5th and 95th percentiles in each group. The y-axis ranges from 1 to 6 representing natural logarithm values of hs-tnt (Ln hs-tnt). EF indicates ejection fraction; IVSd, enddiastolic interventricular septal wall thicknes; LE, late enhancement; LV, left ventricle. Correlation analysis showed that hs-tnt categories positively correlated with NYHA functional class, NT-proBNP, creatinine, LE-positive myocardial volume, LV wall thickness, LVMI, LA diameter, and E/E 0 and negatively correlated with estimated GFR (egfr; Table 3). Multivariable logistic regression analysis suggested that only LE-positive myocardial volume was independently associated with hs-tnt elevation (Table 4; odds ratio [OR], 32.81; 95% CI, ; P=0.002). Comparison of hs-tnt with LVH (septal wall thickness, R 2 linear=0.58; r=0.76; P<0.001; Figure 2A) and amount of LV fibrosis (LE-positive myocardial volume, R 2 linear=0.66; r=0.72; P<0.001; Figure 2B) showed a strong positive correlation. A moderate positive correlation also was noted between NT-proBNP level and amount of LV fibrosis (R 2 linear=0.22; r=0.66; P<0.001; Figure 2C). A closer look at patients with renal insufficiency showed that CKD stage III to IV was more frequently present in patients with hs-tnt >14 ng/l compared to those with hs- TNT <5 and 5 to 14 ng/l. Advanced kidney dysfunction was significantly associated with an elevated hs-tnt level (median: DOI: /JAHA Journal of the American Heart Association 5
6 Table 2. Echocardiography and Cardiac Magnetic Resonance Imaging in the Prospective Cohort (n=75) CKD stage III IV, 32.7 [ ] ng/l vs stage 0 II, 6.7 [4 19.2] ng/l; P=0.003). There was a strong correlation between hs-tnt and LE-positive myocardial volume both in patients with CKD stage I to II (n=66; r=0.805; P<0.001) and in patients with stage III to IV (n=9; r=0.797; P=0.010). Longitudinal, Retrospective Data For follow-up, 58 patients were screened for hs-tnt, NTproBNP, and typical features of Fabry cardiomyopathy on MRI and echocardiography at baseline and at the latest possible time. As shown in Table 5, over a follow-up period of years, patients with an elevated hs-tnt (>14 ng/l) at baseline had significantly increasing replacement fibrosis (median: baseline, 1.9 [ ] %; follow-up, 3.2 [ ] %; P<0.001) and slightly increasing hs-tnt (baseline, 44.7 [30.1 Total hs-tnt <5 ng/l hs-tnt 5 to 14 ng/l hs-tnt >14 ng/l n=75 n=29 n=16 n=30 Echocardiography LV end-diastolic dimension, mm IVSd, mm * * LVPWd, mm * * LV fractional shortening, mm End-diastolic LV volume, ml End-systolic LV volume, ml Stroke volume, ml LV mass index, g/m² Left atrial diameter, mm * LVEF, % E/A E/E * * DT, ms SPAP, mm Hg Magnetic resonance imaging LE positive, n (%) 34 (45.3) 1 (3.4) 4 (25.0) 29 (96.7) LE-positive myocardial volume, % 0 (0 8.5) 0 (0 0.71) 0 (0 1.2)* 1.4 (0 8.5)* LVMI, g/m² * End-diastolic LV volume, ml End-systolic LV volume, ml Stroke volume, ml LVEF, % DT indicates deceleration time of early filling; E/A, early diastolic filling velocity (E) to late diastolic filling velocity (A) ratio; E/E 0, mitral inflow velocity (E) to tissue Doppler E 0 ratio; hs-tnt, high-sensitivity cardiac troponin T; IVSd, end-diastolic interventricular septal wall thickness; LE, late enhancement; LV, left ventricle; LVEF, LV ejection fraction; LVMI, LV mass indexed to body surface area; LVPWd, end-diastolic posterior wall thickness; SPAP, systolic pulmonary artery pressure. *P<0.05 vs hs-tnt <5 ng/l. P<0.05 vs hs-tnt 5 to 14 ng/l. 65.3] ng/l; follow-up, 49.1 [ ] ng/l; P=0.116). In addition, LV wall thickness of patients with elevated hs-tnt was significantly decreased (baseline, mm; followup, mm; P=0.043) and EF tended to be reduced (baseline, 666%; follow-up, 638%; P>0.05) during followup. LV wall thickness thinning might be associated with intramural replacement fibrosis and progression of heart failure and usually occurs in the late stage of disease. 21 Global systolic function (=EF) in patients with elevated hs-tnt was decreased during follow-up, indicating potential cardiomyopathy progression as well. Of the 58 patients with longitudinal data, 21 (36.2%) underwent enzyme replacement therapy (ERT). As shown in Table 6, patients in the ERT group had higher hs-tnt levels and thicker LV wall thickness compared to the no-ert group at baseline. LE-positive myocardial volume was similar DOI: /JAHA Journal of the American Heart Association 6
7 Table 3. Spearman s Rank Correlation Between hs-tnt Categories and Clinical and Echocardiographic Variables in the Prospective Cohort (n=75) Spearman s Rank Correlation Coefficient (r s ) P Value Age, y Sex 0.11 (v²=2.26) 0.33 BMI, kg/m² NYHA class 0.38 (v²=12.97) NT-proBNP*, mg/dl 0.55 <0.001 egfr, ml/min 0.51 <0.001 Creatinine, mg/dl LE-positive myocardial 0.82 <0.001 volume, % MRI-LVMI, g/m² 0.55 <0.001 Echo-LVMI, g/m² IVSd, mm 0.74 <0.001 LVPWd, mm 0.70 <0.001 LV end-diastolic dimension, mm EF, % Left atrial diameter, mm 0.44 <0.001 E/e <0.001 DT SPAP BMI indicates body mass index; DT, deceleration time of early filling; E/E 0, mitral inflow velocity (E) to tissue Doppler E 0 ratio; EF, ejection fraction; egfr, estimated glomerular filtration rate; hs-tnt, high-sensitivity cardiac troponin T; IVSd, end-diastolic interventricular septal wall thickness; LE, late enhancement; LV, left ventricle; LVMI, LV mass indexed to body surface area; LVPWd, end-diastolic posterior wall thickness; NTproBNP, N-terminal of the prohormone brain natriuretic peptide; NYHA, New York Heart Association; SPAP, systolic pulmonary artery pressure. *Ln-transformed. between groups at baseline. During follow-up, hs-tnt level and LE-positive myocardial volumes were significantly increased in both groups. Discussion The aim of this study was to investigate the clinical value of hs-tnt as a blood biomarker for evaluating myocardial replacement fibrosis in patients with FD. The main results are 4-fold: First, the well-known myocyte turnover resulting in myocardial replacement fibrosis was associated with plasma hs-tnt elevation. Second, hs-tnt level correlated with the total amount of replacement fibrosis. Third, elevated hs-tnt could predict an increase in the extent of fibrosis. Finally, hs- TNT was very stable and predictive even in frozen blood stored for more than 5 years. hs-tnt is a reliable, highly sensitive marker for myocyte necrosis and myocardial remodeling, both resulting in myocardial fibrosis. 22 Moreno et al. showed that patients with hypertrophic cardiomyopathy and LE on MRI have higher levels of hs-tnt than hypertrophic cardiomyopathy patients without LE. 23 In accord with these findings, Kawasaki et al. demonstrated that higher levels of hs-tnt are associated with LE on MRI in patients with cardiomyopathy and suggested that hs-tnt is therefore a direct marker for myocardial replacement fibrosis. 24 In an initial study, Feustel et al. showed that regular troponin I was continuously elevated in 3 patients with a Fabry cardiomyopathy. 25 However, this troponin I was, by far, not as sensitive for myocyte turnover as the hs-tnt used in the current study. To date, no well-performed study has investigated the association of hs-tnt and replacement fibrosis in patients with Fabry cardiomyopathy. In the current work, both the level of hs-tnt and LE-positive area were quantified, and absolute values were given for both parameters in all patients. In this way, we showed a clear correlation between the blood biomarkers and morphological finding of replacement fibrosis. However, whether or not the circulated hs-tnt is finally generated by myocyte turnover in the LE-positive region remains unclear. It can be speculated that hs-tnt is generated everywhere in the diseased myocardium of the LV. If so, then the correlation could Table 4. Determinants of Elevated hs-tnt (>14 ng/l) Assessed by Logistic Regression Analysis in the Prospective Cohort (n=75) Adjusted* Multivariate* OR (95% CI) P Value OR (95% CI) P Value egfr, ml/min 0.95 ( ) ( ) NT-proBNP, pg/ml 2.96 ( ) < ( ) LE-positive myocardial volume, % 97.2 ( ) < ( ) IVSd, mm 2.62 ( ) < ( ) Left atrial diameter, mm 1.27 ( ) ( ) egfr indicates estimated glomerular filtration rate; hs-tnt, high-sensitivity cardiac troponin T; IVSd, end-diastolic interventricular septal wall thickness; LE, late enhancement; NT-proBNP, N-terminal of the prohormone brain natriuretic peptide; OR, odds ratio. *Adjusted for age, sex, and body mass index. Ln-transformed. DOI: /JAHA Journal of the American Heart Association 7
8 Figure 2. Scatterplots demonstrating the correlation of (A) highsensitivity cardiac troponin T (hs-tnt) with septal wall thickness (IVSd, mm); (B) hs-tnt with late enhancement (LE) positive myocardial volume (%); and (C) NT-proBNP with LE-positive myocardial volume (%). Natural logarithm (Ln) values of hs-tnt (A and B) and NT-proBNP (C) are used as the Y-axis scale. NT-proBNP indicates N-terminal of the prohormone brain natriuretic peptide. result from the fact that the amount of replacement fibrosis mirrors the severity of the diseased myocardium. The current study also investigated NT-proBNP as a marker of cardiomyopathy. NT-proBNP is an established biomarker for heart failure and is mainly related to the wall stress acting on the heart. 24,26,27 In general, only truly end-stage Fabry cardiomyopathy patients suffer from heart failure; 7,28 in addition, blood pressure (one of the main components of wall stress) is not severely elevated in these patients. Thus, it was predictable that NT-proBNP was only a weak biomarker for cardiomyopathy and not clinically meaningful in terms of the amount of fibrosis. Evaluation of myocardial fibrosis by either imaging or biomarkers is clinically important because fibrosis defines the stage of cardiomyopathy, predicts the outcome during ERT, and indicates a poor prognosis. 5,11,29,30 The noninvasive gold standard for detecting intramural replacement fibrosis is LE MRI. 6 LE imaging is accurate for evaluating the LV and highly sensitive for detecting and quantifying a small amount of fibrosis However, this technique is expensive, timeconsuming, and often not available for routine diagnosis. Furthermore, many Fabry patients have contraindications for undergoing MRI, such as ESRD or an implanted cardiac defibrillator or pacemaker. 31 Another indirect way to screen for regional myocardial fibrosis is by functional deformation imaging. 27,28 This method is sensitive for detecting systolic functional abnormalities; however, it requires an experienced investigator. Additionally, this method is also time-consuming and not easy to postprocess. 30,31,33,35 Clinical Implication The current data suggest that hs-tnt could be measured in every Fabry patient at every visit because it is widely available and not expensive. If it is in normal range, that in combination with normal echocardiography and 12-lead electrocardiography means that a typical Fabry cardiomyopathy is very unlikely. If the level of hs-tnt is borderline, a sophisticated search, including cardiac MRI, for replacement fibrosis should be done. On the other hand, if the level is very high, an advanced cardiomyopathy is likely present, and imaging of the fibrosis is necessary only for confirmation. In addition, in patients with elevated hs-tnt, the progression of the cardiomyopathy can be anticipated even when these patients are treated with ERT; thus, a careful follow-up of these patients should be performed. Limitations ESRD patients treated with dialysis were excluded from these analyses because LE imaging is contraindicated. It is possible that hs-tnt could, in part, accumulate because of a decreased DOI: /JAHA Journal of the American Heart Association 8
9 Table 5. Changes in hs-tnt Level, LE-Positive Myocardium, Cardiac Morphology, and Function During Follow-up (n=58) hs-tnt <5 ng/l hs-tnt 5 to 14 ng/l hs-tnt >14 ng/l n=26 n=19 n=13 Duration of follow-up, y hs-tnt*, ng/l Baseline ( ) 44.7 ( ) Follow-up 4.0 ( ) 12.5 ( ) 49.1 ( ) LE-positive myocardial volume, % Baseline 0 (0 0.3) 0.4 (0 1.6) 1.9 ( ) Follow-up 0.3 (0 1.4) 1.5 ( ) 3.2 ( ) IVSd, mm Baseline Follow-up EF, % Baseline Follow-up Using repeated-measures ANOVA followed by Bonferroni post-hoc test for multiple comparisons. EF indicates ejection fraction; hs-tnt, high-sensitivity cardiac troponin T; IVSd, enddiastolic interventricular septal wall thickness; LE, late enhancement. *Ln-transformed. Bonferroni-adjusted P<0.025 vs hs-tnt <5 ng/l; P<0.025 vs hs-tnt 5 to 14 ng/l. P<0.05 vs baseline. renal filtration rate; thus, the suggested biomarker should not be used in hemodialysis patients. In addition, the patient sample was relatively small for the longitudinal cohort and all Table 6. Changes in hs-tnt Level, LE-Positive Myocardium, Cardiac Morphology, and Function During Follow-up (n=58) in Patients With and Without ERT No ERT ERT n=37 n=21 hs-tnt*, ng/l Baseline 4.0 ( ) 8.9 ( ) Follow-up 6.1 ( ) 14.6 ( ) LE-positive myocardial volume, % Baseline 0.2 (0 1.2) 0.6 (0 1.8) Follow-up 1.0 (0 2.3) 2.3 ( ) IVSd, mm Baseline Follow-up EF, % Baseline Follow-up Using repeated-measures ANOVA followed by Tukey s post-hoc test. EF indicates ejection fraction; ERT, enzyme replacement therapy; hs-tnt, high-sensitivity cardiac troponin T; IVSd, end-diastolic interventricular septal wall thickness; LE, late enhancement. *Ln-transformed. P<0.05 vs no ERT. P<0.05 vs baseline. data were retrospectively collected. The duration between baseline and follow-up examinations was unable to be standardized. These limitations could have introduced some bias. Prospective studies with larger sample size are certainly warranted to validate the current results. Conclusion The present study shows a clinically meaningful correlation between plasma hs-tnt level and the amount of replacement fibrosis as assessed by LE. These findings indicate that hs- TNT is a reliable tool for screening for myocardial fibrosis. It is convenient, cost-effective, easy to determine, and involves few contraindications. Moreover, hs-tnt can be used as an easy predictor of the progression of Fabry cardiomyopathy. Thus, we suggest that the biomarker hs-tnt could be helpful for staging and follow-up of Fabry patients. Sources of Funding This work was supported by grants from the Bundesministerium f ur Bildung und Forschung (BMBF project 01EO1004) and by Genzyme Corporation. Disclosures Weidemann and Wanner have received speaker honoraria from Genzyme and Shire corporations. Weidemann and DOI: /JAHA Journal of the American Heart Association 9
10 Wanner are members of the Fabry Registry European Board of Advisors and have received travel assistance and speaker honoraria. Research grants were given to the Institution by Genzyme and Shire corporations. References 1. Desnick RJ, Brady R, Barranger J, Collins AJ, Germain DP, Goldman M, Grabowski G, Packman S, Wilcox WR. Fabry disease, an under-recognized multisystemic disorder: expert recommendations for diagnosis, management, and enzyme replacement therapy. Ann Intern Med. 2003;138: Garman SC, Garboczi DN. The molecular defect leading to Fabry disease: structure of human alpha-galactosidase. J Mol Biol. 2004;337: De Francesco PN, Mucci JM, Ceci R, Fossati CA, Rozenfeld PA. Fabry disease peripheral blood immune cells release inflammatory cytokines: role of globotriaosylceramide. Mol Genet Metab. 2013;109: MacDermot KD, Holmes A, Miners AH. Anderson-Fabry disease: clinical manifestations and impact of disease in a cohort of 98 hemizygous males. J Med Genet. 2001;38: Weidemann F, Breunig F, Beer M, Sandstede J, Stork S, Voelker W, Ertl G, Knoll A, Wanner C, Strotmann JM. The variation of morphological and functional cardiac manifestation in Fabry disease: potential implications for the time course of the disease. Eur Heart J. 2005;26: Moon JC, Sachdev B, Elkington AG, McKenna WJ, Mehta A, Pennell DJ, Leed PJ, Elliott PM. Gadolinium enhanced cardiovascular magnetic resonance in Anderson-Fabry disease. Evidence for a disease specific abnormality of the myocardial interstitium. Eur Heart J. 2003;24: Linhart A, Kampmann C, Zamorano JL, Sunder-Plassmann G, Beck M, Mehta A, Elliott PM. Cardiac manifestations of Anderson-Fabry disease: results from the international Fabry outcome survey. Eur Heart J. 2007;28: Barbey F, Brakch N, Linhart A, Rosenblatt-Velin N, Jeanrenaud X, Qanadli S, Steinmann B, Burnier M, Palecek T, Bultas J, Hayoz D. Cardiac and vascular hypertrophy in Fabry disease: evidence for a new mechanism independent of blood pressure and glycosphingolipid deposition. Arterioscler Thromb Vasc Biol. 2006;26: Morrissey RP, Philip KJ, Schwarz ER. Cardiac abnormalities in Anderson-Fabry disease and Fabry s cardiomyopathy. Cardiovasc J Afr. 2011;22: Mehta A, Clarke JT, Giugliani R, Elliott P, Linhart A, Beck M, Sunder-Plassmann G. Natural course of Fabry disease: changing pattern of causes of death in FOS Fabry Outcome Survey. J Med Genet. 2009;46: Kramer J, Niemann M, Stork S, Frantz S, Beer M, Ertl G, Wanner C, Weidemann F. Relation of burden of myocardial fibrosis to malignant ventricular arrhythmias and outcomes in Fabry disease. Am J Cardiol. 2014;114: Moon JC, Reed E, Sheppard MN, Elkington AG, Ho SY, Burke M, Petrou M, Pennell DJ. The histologic basis of late gadolinium enhancement cardiovascular magnetic resonance in hypertrophic cardiomyopathy. J Am Coll Cardiol. 2004;43: Moe GW. B-type natriuretic peptide in heart failure. Curr Opin Cardiol. 2006;21: Armstrong EJ, Morrow DA, Sabatine MS. Inflammatory biomarkers in acute coronary syndromes: part III: biomarkers of oxidative stress and angiogenic growth factors. Circulation. 2006;113:e289 e Armstrong EJ, Morrow DA, Sabatine MS. Inflammatory biomarkers in acute coronary syndromes: part II: acute-phase reactants and biomarkers of endothelial cell activation. Circulation. 2006;113:e152 e Armstrong EJ, Morrow DA, Sabatine MS. Inflammatory biomarkers in acute coronary syndromes: part I: introduction and cytokines. Circulation. 2006;113: e72 e Saunders JT, Nambi V, de Lemos JA, Chambless LE, Virani SS, Boerwinkle E, Hoogeveen RC, Liu X, Astor BC, Mosley TH, Folsom AR, Heiss G, Coresh J, Ballantyne CM. Cardiac troponin T measured by a highly sensitive assay predicts coronary heart disease, heart failure, and mortality in the Atherosclerosis Risk in Communities Study. Circulation. 2011;123: de Lemos JA, Drazner MH, Omland T, Ayers CR, Khera A, Rohatgi A, Hashim I, Berry JD, Das SR, Morrow DA, McGuire DK. Association of troponin T detected with a highly sensitive assay and cardiac structure and mortality risk in the general population. JAMA. 2010;304: Januzzi JL, van Kimmenade R, Lainchbury J, Bayes-Genis A, Ordonez-Llanos J, Santalo-Bel M, Pinto YM, Richards M. NT-proBNP testing for diagnosis and short-term prognosis in acute destabilized heart failure: an international pooled analysis of 1256 patients: the International Collaborative of NT-proBNP Study. Eur Heart J. 2006;27: Hildebrandt P, Richards AM. Amino-terminal pro-b-type natriuretic peptide testing in patients with diabetes mellitus and with systemic hypertension. Am J Cardiol. 2008;101: Kawano M, Takenaka T, Otsuji Y, Teraguchi H, Yoshifuku S, Yuasa T, Yu B, Miyata M, Hamasaki S, Minagoe S, Kanmura Y, Tei C. Significance of asymmetric basal posterior wall thinning in patients with cardiac Fabry s disease. Am J Cardiol. 2007;99: Gomes AV, Barnes JA, Harada K, Potter JD. Role of troponin T in disease. Mol Cell Biochem. 2004;263: Moreno V, Hernandez-Romero D, Vilchez JA, Garcia-Honrubia A, Cambronero F, Casas T, Gonzalez J, Martinez P, Climent V, de la Morena G, Valdes M, Marin F. Serum levels of high-sensitivity troponin T: a novel marker for cardiac remodeling in hypertrophic cardiomyopathy. J Card Fail. 2010;16: Kawasaki T, Sakai C, Harimoto K, Yamano M, Miki S, Kamitani T. Usefulness of high-sensitivity cardiac troponin T and brain natriuretic peptide as biomarkers of myocardial fibrosis in patients with hypertrophic cardiomyopathy. Am J Cardiol. 2013;112: Feustel A, Hahn A, Schneider C, Sieweke N, Franzen W, Gunduz D, Rolfs A, Tanislav C. Continuous cardiac troponin I release in Fabry disease. PLoS One. 2014;9:e Ogino K, Ogura K, Kinugawa T, Osaki S, Kato M, Furuse Y, Kinugasa Y, Tomikura Y, Igawa O, Hisatome I, Shigemasa C. Neurohumoral profiles in patients with hypertrophic cardiomyopathy: differences to hypertensive left ventricular hypertrophy. Circ J. 2004;68: Arteaga E, Araujo AQ, Buck P, Ianni BM, Rabello R, Mady C. Plasma aminoterminal pro-b-type natriuretic peptide quantification in hypertrophic cardiomyopathy. Am Heart J. 2005;150: Weidemann F, Linhart A, Monserrat L, Strotmann J. Cardiac challenges in patients with Fabry disease. Int J Cardiol. 2010;141: Weidemann F, Niemann M, Breunig F, Herrmann S, Beer M, Stork S, Voelker W, Ertl G, Wanner C, Strotmann J. Long-term effects of enzyme replacement therapy on Fabry cardiomyopathy: evidence for a better outcome with early treatment. Circulation. 2009;119: Weidemann F, Niemann M, Herrmann S, Kung M, Stork S, Waller C, Beer M, Breunig F, Wanner C, Voelker W, Ertl G, Bijnens B, Strotmann JM. A new echocardiographic approach for the detection of non-ischaemic fibrosis in hypertrophic myocardium. Eur Heart J. 2007;28: Pieroni M, Chimenti C, Ricci R, Sale P, Russo MA, Frustaci A. Early detection of Fabry cardiomyopathy by tissue Doppler imaging. Circulation. 2003;107: Weidemann F, Breunig F, Beer M, Sandstede J, Turschner O, Voelker W, Ertl G, Knoll A, Wanner C, Strotmann JM. Improvement of cardiac function during enzyme replacement therapy in patients with Fabry disease: a prospective strain rate imaging study. Circulation. 2003;108: Rosen BD, Edvardsen T, Lai S, Castillo E, Pan L, Jerosch-Herold M, Sinha S, Kronmal R, Arnett D, Crouse JR III, Heckbert SR, Bluemke DA, Lima JA. Left ventricular concentric remodeling is associated with decreased global and regional systolic function: the Multi-Ethnic Study of Atherosclerosis. Circulation. 2005;112: Weidemann F, Strotmann JM. Use of tissue Doppler imaging to identify and manage systemic diseases. Clin Res Cardiol. 2008;97: Kramer J, Niemann M, Liu D, Hu K, Machann W, Beer M, Wanner C, Ertl G, Weidemann F. Two-dimensional speckle tracking as a non-invasive tool for identification of myocardial fibrosis in Fabry disease. Eur Heart J. 2013;34: DOI: /JAHA Journal of the American Heart Association 10
Long-Term Effects of Enzyme Replacement Therapy on Fabry Cardiomyopathy Evidence for a Better Outcome With Early Treatment
 Long-Term Effects of Enzyme Replacement Therapy on Fabry Cardiomyopathy Evidence for a Better Outcome With Early Treatment Frank Weidemann, MD*; Markus Niemann*; Frank Breunig, MD; Sebastian Herrmann;
Long-Term Effects of Enzyme Replacement Therapy on Fabry Cardiomyopathy Evidence for a Better Outcome With Early Treatment Frank Weidemann, MD*; Markus Niemann*; Frank Breunig, MD; Sebastian Herrmann;
Global left ventricular circumferential strain is a marker for both systolic and diastolic myocardial function
 Global left ventricular circumferential strain is a marker for both systolic and diastolic myocardial function Toshinari Onishi 1, Samir K. Saha 2, Daniel Ludwig 1, Erik B. Schelbert 1, David Schwartzman
Global left ventricular circumferential strain is a marker for both systolic and diastolic myocardial function Toshinari Onishi 1, Samir K. Saha 2, Daniel Ludwig 1, Erik B. Schelbert 1, David Schwartzman
Dr. Dermot Phelan MB BCh BAO PhD European Society of Cardiology 2012
 Relative Apical Sparing of Longitudinal Strain Using 2- Dimensional Speckle-Tracking Echocardiography is Both Sensitive and Specific for the Diagnosis of Cardiac Amyloidosis. Dr. Dermot Phelan MB BCh BAO
Relative Apical Sparing of Longitudinal Strain Using 2- Dimensional Speckle-Tracking Echocardiography is Both Sensitive and Specific for the Diagnosis of Cardiac Amyloidosis. Dr. Dermot Phelan MB BCh BAO
Mechanisms of False Positive Exercise Electrocardiography: Is False Positive Test Truly False?
 Mechanisms of False Positive Exercise Electrocardiography: Is False Positive Test Truly False? Masaki Izumo a, Kengo Suzuki b, Hidekazu Kikuchi b, Seisyo Kou b, Keisuke Kida b, Yu Eguchi b, Nobuyuki Azuma
Mechanisms of False Positive Exercise Electrocardiography: Is False Positive Test Truly False? Masaki Izumo a, Kengo Suzuki b, Hidekazu Kikuchi b, Seisyo Kou b, Keisuke Kida b, Yu Eguchi b, Nobuyuki Azuma
Velocity Vector Imaging as a new approach for cardiac magnetic resonance: Comparison with echocardiography
 Velocity Vector Imaging as a new approach for cardiac magnetic resonance: Comparison with echocardiography Toshinari Onishi 1, Samir K. Saha 2, Daniel Ludwig 1, Erik B. Schelbert 1, David Schwartzman 1,
Velocity Vector Imaging as a new approach for cardiac magnetic resonance: Comparison with echocardiography Toshinari Onishi 1, Samir K. Saha 2, Daniel Ludwig 1, Erik B. Schelbert 1, David Schwartzman 1,
Association and diagnostic utility of diastolic dysfunction and myocardial fibrosis in patients with Fabry disease
 Open access To cite: Liu D, Oder D, Salinger T, et al. Association and diagnostic utility of diastolic dysfunction and myocardial fibrosis in patients with Fabry disease. Open Heart 2018;5:e000803. doi:10.1136/
Open access To cite: Liu D, Oder D, Salinger T, et al. Association and diagnostic utility of diastolic dysfunction and myocardial fibrosis in patients with Fabry disease. Open Heart 2018;5:e000803. doi:10.1136/
Coronary artery disease (CAD) risk factors
 Background Coronary artery disease (CAD) risk factors CAD Risk factors Hypertension Insulin resistance /diabetes Dyslipidemia Smoking /Obesity Male gender/ Old age Atherosclerosis Arterial stiffness precedes
Background Coronary artery disease (CAD) risk factors CAD Risk factors Hypertension Insulin resistance /diabetes Dyslipidemia Smoking /Obesity Male gender/ Old age Atherosclerosis Arterial stiffness precedes
Evaluation of Left Ventricular Diastolic Dysfunction by Doppler and 2D Speckle-tracking Imaging in Patients with Primary Pulmonary Hypertension
 ESC Congress 2011.No 85975 Evaluation of Left Ventricular Diastolic Dysfunction by Doppler and 2D Speckle-tracking Imaging in Patients with Primary Pulmonary Hypertension Second Department of Internal
ESC Congress 2011.No 85975 Evaluation of Left Ventricular Diastolic Dysfunction by Doppler and 2D Speckle-tracking Imaging in Patients with Primary Pulmonary Hypertension Second Department of Internal
Individual Study Table Referring to Part of Dossier: Volume: Page:
 Synopsis Abbott Laboratories Name of Study Drug: Paricalcitol Capsules (ABT-358) (Zemplar ) Name of Active Ingredient: Paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For
Synopsis Abbott Laboratories Name of Study Drug: Paricalcitol Capsules (ABT-358) (Zemplar ) Name of Active Ingredient: Paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For
LV FUNCTION ASSESSMENT: WHAT IS BEYOND EJECTION FRACTION
 LV FUNCTION ASSESSMENT: WHAT IS BEYOND EJECTION FRACTION Jamilah S AlRahimi Assistant Professor, KSU-HS Consultant Noninvasive Cardiology KFCC, MNGHA-WR Introduction LV function assessment in Heart Failure:
LV FUNCTION ASSESSMENT: WHAT IS BEYOND EJECTION FRACTION Jamilah S AlRahimi Assistant Professor, KSU-HS Consultant Noninvasive Cardiology KFCC, MNGHA-WR Introduction LV function assessment in Heart Failure:
Highlights from EuroEcho 2009 Echo in cardiomyopathies
 Highlights from EuroEcho 2009 Echo in cardiomyopathies Bogdan A. Popescu University of Medicine and Pharmacy, Bucharest, Romania ESC Congress 2010 Hypertrophic cardiomyopathy To determine the differences
Highlights from EuroEcho 2009 Echo in cardiomyopathies Bogdan A. Popescu University of Medicine and Pharmacy, Bucharest, Romania ESC Congress 2010 Hypertrophic cardiomyopathy To determine the differences
Fabry Disease: A rare condition emerging from the darkness
 Fabry Disease: A rare condition emerging from the darkness Running Title: Fabry Disease: A rare condition emerging from the darkness Professor Perry Elliott MBBS; MD; FRCP; FESC; FACC Chair of Cardiovascular
Fabry Disease: A rare condition emerging from the darkness Running Title: Fabry Disease: A rare condition emerging from the darkness Professor Perry Elliott MBBS; MD; FRCP; FESC; FACC Chair of Cardiovascular
Supplementary Online Content
 Supplementary Online Content Inohara T, Manandhar P, Kosinski A, et al. Association of renin-angiotensin inhibitor treatment with mortality and heart failure readmission in patients with transcatheter
Supplementary Online Content Inohara T, Manandhar P, Kosinski A, et al. Association of renin-angiotensin inhibitor treatment with mortality and heart failure readmission in patients with transcatheter
Review of Cardiac Imaging Modalities in the Renal Patient. George Youssef
 Review of Cardiac Imaging Modalities in the Renal Patient George Youssef ECHO Left ventricular hypertrophy (LVH) assessment Diastolic dysfunction Stress ECHO Cardiac CT angiography Echocardiography - positives
Review of Cardiac Imaging Modalities in the Renal Patient George Youssef ECHO Left ventricular hypertrophy (LVH) assessment Diastolic dysfunction Stress ECHO Cardiac CT angiography Echocardiography - positives
Feasibility and limitations of 2D speckle tracking echocardiography
 ORIGINAL ARTICLE 204 A prospective study in daily clinical practice Feasibility and limitations of 2D speckle tracking echocardiography Lina Melzer, Anja Faeh-Gunz, Barbara Naegeli, Burkhardt Seifert*,
ORIGINAL ARTICLE 204 A prospective study in daily clinical practice Feasibility and limitations of 2D speckle tracking echocardiography Lina Melzer, Anja Faeh-Gunz, Barbara Naegeli, Burkhardt Seifert*,
Dialysis-Dependent Cardiomyopathy Patients Demonstrate Poor Survival Despite Reverse Remodeling With Cardiac Resynchronization Therapy
 Dialysis-Dependent Cardiomyopathy Patients Demonstrate Poor Survival Despite Reverse Remodeling With Cardiac Resynchronization Therapy Evan Adelstein, MD, FHRS John Gorcsan III, MD Samir Saba, MD, FHRS
Dialysis-Dependent Cardiomyopathy Patients Demonstrate Poor Survival Despite Reverse Remodeling With Cardiac Resynchronization Therapy Evan Adelstein, MD, FHRS John Gorcsan III, MD Samir Saba, MD, FHRS
Tissue Doppler and Strain Imaging. Steven J. Lester MD, FRCP(C), FACC, FASE
 Tissue Doppler and Strain Imaging Steven J. Lester MD, FRCP(C), FACC, FASE Relevant Financial Relationship(s) None Off Label Usage None a. Turn the wall filters on and turn down the receiver gain. b. Turn
Tissue Doppler and Strain Imaging Steven J. Lester MD, FRCP(C), FACC, FASE Relevant Financial Relationship(s) None Off Label Usage None a. Turn the wall filters on and turn down the receiver gain. b. Turn
Echocardiographic and Doppler Assessment of Cardiac Functions in Patients of Non-Insulin Dependent Diabetes Mellitus
 ORIGINAL ARTICLE JIACM 2002; 3(2): 164-8 Echocardiographic and Doppler Assessment of Cardiac Functions in Patients of Non-Insulin Dependent Diabetes Mellitus Rajesh Rajput*, Jagdish**, SB Siwach***, A
ORIGINAL ARTICLE JIACM 2002; 3(2): 164-8 Echocardiographic and Doppler Assessment of Cardiac Functions in Patients of Non-Insulin Dependent Diabetes Mellitus Rajesh Rajput*, Jagdish**, SB Siwach***, A
Tissue Doppler and Strain Imaging
 Tissue Doppler and Strain Imaging Steven J. Lester MD, FRCP(C), FACC, FASE Relevant Financial Relationship(s) None Off Label Usage None 1 Objective way with which to quantify the minor amplitude and temporal
Tissue Doppler and Strain Imaging Steven J. Lester MD, FRCP(C), FACC, FASE Relevant Financial Relationship(s) None Off Label Usage None 1 Objective way with which to quantify the minor amplitude and temporal
Heart disease. Other symptoms too? FABRY DISEASE IN PATIENTS WITH UNEXPLAINED HEART CONDITIONS
 Heart disease Other symptoms too? FABRY DISEASE IN PATIENTS WITH UNEXPLAINED HEART CONDITIONS You have been given this brochure because your heart condition may be linked to Fabry disease, which is a rare,
Heart disease Other symptoms too? FABRY DISEASE IN PATIENTS WITH UNEXPLAINED HEART CONDITIONS You have been given this brochure because your heart condition may be linked to Fabry disease, which is a rare,
Heart Failure in Women: Dr Goh Ping Ping Cardiologist Asian Heart & Vascular Centre
 Heart Failure in Women: More than EF? Dr Goh Ping Ping Cardiologist Asian Heart & Vascular Centre Overview Review pathophysiology as it relates to diagnosis and management Rational approach to workup:
Heart Failure in Women: More than EF? Dr Goh Ping Ping Cardiologist Asian Heart & Vascular Centre Overview Review pathophysiology as it relates to diagnosis and management Rational approach to workup:
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Clinical perspective It was recently discovered that small RNAs, called micrornas, circulate freely and stably in human plasma. This finding has sparked interest in the potential
SUPPLEMENTAL MATERIAL Clinical perspective It was recently discovered that small RNAs, called micrornas, circulate freely and stably in human plasma. This finding has sparked interest in the potential
Left atrial function. Aliakbar Arvandi MD
 In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
Μαρία Μπόνου Διευθύντρια ΕΣΥ, ΓΝΑ Λαϊκό
 Μαρία Μπόνου Διευθύντρια ΕΣΥ, ΓΝΑ Λαϊκό Diastolic HF DD: Diastolic Dysfunction DHF: Diastolic HF HFpEF: HF with preserved EF DD Pathophysiologic condition: impaired relaxation, LV compliance, LV filling
Μαρία Μπόνου Διευθύντρια ΕΣΥ, ΓΝΑ Λαϊκό Diastolic HF DD: Diastolic Dysfunction DHF: Diastolic HF HFpEF: HF with preserved EF DD Pathophysiologic condition: impaired relaxation, LV compliance, LV filling
HYPERTROPHY: Behind the curtain. V. Yotova St. Radboud Medical University Center, Nijmegen
 HYPERTROPHY: Behind the curtain V. Yotova St. Radboud Medical University Center, Nijmegen Disclosure of interest: none Relative wall thickness (cm) M 0.22 0.42 0.43 0.47 0.48 0.52 0.53 F 0.24 0.42 0.43
HYPERTROPHY: Behind the curtain V. Yotova St. Radboud Medical University Center, Nijmegen Disclosure of interest: none Relative wall thickness (cm) M 0.22 0.42 0.43 0.47 0.48 0.52 0.53 F 0.24 0.42 0.43
Evalua&on)of)Le-)Ventricular)Diastolic) Dysfunc&on)by)Echocardiography:) Role)of)Ejec&on)Frac&on)
 Evalua&on)of)Le-)Ventricular)Diastolic) Dysfunc&on)by)Echocardiography:) Role)of)Ejec&on)Frac&on) N.Koutsogiannis) Department)of)Cardiology) University)Hospital)of)Patras)! I have no conflicts of interest
Evalua&on)of)Le-)Ventricular)Diastolic) Dysfunc&on)by)Echocardiography:) Role)of)Ejec&on)Frac&on) N.Koutsogiannis) Department)of)Cardiology) University)Hospital)of)Patras)! I have no conflicts of interest
Supplementary Online Content
 Supplementary Online Content Nikolova AP, Hitzeman TC, Baum R, et al. Association of a novel diagnostic biomarker, the plasma cardiac bridging integrator 1 score, with heart failure with preserved ejection
Supplementary Online Content Nikolova AP, Hitzeman TC, Baum R, et al. Association of a novel diagnostic biomarker, the plasma cardiac bridging integrator 1 score, with heart failure with preserved ejection
Value of echocardiography in chronic dyspnea
 Value of echocardiography in chronic dyspnea Jahrestagung Schweizerische Gesellschaft für /Schweizerische Gesellschaft für Pneumologie B. Kaufmann 16.06.2016 Chronic dyspnea Shortness of breath lasting
Value of echocardiography in chronic dyspnea Jahrestagung Schweizerische Gesellschaft für /Schweizerische Gesellschaft für Pneumologie B. Kaufmann 16.06.2016 Chronic dyspnea Shortness of breath lasting
Tissue Doppler and Strain Imaging
 Tissue Doppler and Strain Imaging Steven J. Lester MD, FRCP(C), FACC, FASE Relevant Financial Relationship(s) None Off Label Usage None 1 Objective way with which to quantify the minor amplitude and temporal
Tissue Doppler and Strain Imaging Steven J. Lester MD, FRCP(C), FACC, FASE Relevant Financial Relationship(s) None Off Label Usage None 1 Objective way with which to quantify the minor amplitude and temporal
좌심실수축기능평가 Cardiac Function
 Basic Echo Review Course 좌심실수축기능평가 Cardiac Function Seonghoon Choi Cardiology Hallym university LV systolic function Systolic function 좌심실수축기능 - 심근의수축으로심실에서혈액을대동맥으로박출하는기능 실제임상에서 LV function 의의미 1Diagnosis
Basic Echo Review Course 좌심실수축기능평가 Cardiac Function Seonghoon Choi Cardiology Hallym university LV systolic function Systolic function 좌심실수축기능 - 심근의수축으로심실에서혈액을대동맥으로박출하는기능 실제임상에서 LV function 의의미 1Diagnosis
VECTORS OF CONTRACTION
 1/3/216 Strain, Strain Rate, and Torsion: Myocardial Mechanics Simplified and Applied VECTORS OF CONTRACTION John Gorcsan, MD University of Pittsburgh, Pittsburgh, PA Shortening Thickening Twisting No
1/3/216 Strain, Strain Rate, and Torsion: Myocardial Mechanics Simplified and Applied VECTORS OF CONTRACTION John Gorcsan, MD University of Pittsburgh, Pittsburgh, PA Shortening Thickening Twisting No
Fabry Disease and the Kidneys
 Department of Human Genetics Division of Medical Genetics Lysosomal Storage Disease Center www.genetics.emory.edu Fabry Disease and the Kidneys What is Fabry Disease? Fabry disease (FD) is an X-linked
Department of Human Genetics Division of Medical Genetics Lysosomal Storage Disease Center www.genetics.emory.edu Fabry Disease and the Kidneys What is Fabry Disease? Fabry disease (FD) is an X-linked
Appendix II: ECHOCARDIOGRAPHY ANALYSIS
 Appendix II: ECHOCARDIOGRAPHY ANALYSIS Two-Dimensional (2D) imaging was performed using the Vivid 7 Advantage cardiovascular ultrasound system (GE Medical Systems, Milwaukee) with a frame rate of 400 frames
Appendix II: ECHOCARDIOGRAPHY ANALYSIS Two-Dimensional (2D) imaging was performed using the Vivid 7 Advantage cardiovascular ultrasound system (GE Medical Systems, Milwaukee) with a frame rate of 400 frames
PRESENTER DISCLOSURE INFORMATION. There are no potential conflicts of interest regarding current presentation
 PRESENTER DISCLOSURE INFORMATION There are no potential conflicts of interest regarding current presentation Better synchrony and diastolic function for septal versus apical right ventricular permanent
PRESENTER DISCLOSURE INFORMATION There are no potential conflicts of interest regarding current presentation Better synchrony and diastolic function for septal versus apical right ventricular permanent
Influence of RAAS inhibition on outflow tract obstruction in hypertrophic cardiomyopathy
 ORIGINAL ARTICLE 5 RAAS inhibitors should be avoided if possible in patients with obstructive HCM Influence of RAAS inhibition on outflow tract obstruction in hypertrophic cardiomyopathy Katrin Witzel,
ORIGINAL ARTICLE 5 RAAS inhibitors should be avoided if possible in patients with obstructive HCM Influence of RAAS inhibition on outflow tract obstruction in hypertrophic cardiomyopathy Katrin Witzel,
Annalisa Sechi 1*, Gaetano Nucifora 2, Gianluca Piccoli 3, Andrea Dardis 1 and Bruno Bembi 1
 Sechi et al. BMC Cardiovascular Disorders 2014, 14:86 CASE REPORT Open Access Myocardial fibrosis as the first sign of cardiac involvement in a male patient with Fabry disease: report of a clinical case
Sechi et al. BMC Cardiovascular Disorders 2014, 14:86 CASE REPORT Open Access Myocardial fibrosis as the first sign of cardiac involvement in a male patient with Fabry disease: report of a clinical case
Strain and Strain Rate Imaging How, Why and When?
 Strain and Strain Rate Imaging How, Why and When? João L. Cavalcante, MD Advanced Cardiac Imaging Fellow Cleveland Clinic Foundation Disclosures: No conflicts of interest Movement vs Deformation Movement
Strain and Strain Rate Imaging How, Why and When? João L. Cavalcante, MD Advanced Cardiac Imaging Fellow Cleveland Clinic Foundation Disclosures: No conflicts of interest Movement vs Deformation Movement
THE RIGHT VENTRICLE IN PULMONARY HYPERTENSION R. DRAGU
 THE RIGHT VENTRICLE IN PULMONARY HYPERTENSION R. DRAGU Cardiology Dept. Rambam Health Care Campus Rappaport Faculty of Medicine Technion, Israel Why the Right Ventricle? Pulmonary hypertension (PH) Right
THE RIGHT VENTRICLE IN PULMONARY HYPERTENSION R. DRAGU Cardiology Dept. Rambam Health Care Campus Rappaport Faculty of Medicine Technion, Israel Why the Right Ventricle? Pulmonary hypertension (PH) Right
Hemodynamic Assessment. Assessment of Systolic Function Doppler Hemodynamics
 Hemodynamic Assessment Matt M. Umland, RDCS, FASE Aurora Medical Group Milwaukee, WI Assessment of Systolic Function Doppler Hemodynamics Stroke Volume Cardiac Output Cardiac Index Tei Index/Index of myocardial
Hemodynamic Assessment Matt M. Umland, RDCS, FASE Aurora Medical Group Milwaukee, WI Assessment of Systolic Function Doppler Hemodynamics Stroke Volume Cardiac Output Cardiac Index Tei Index/Index of myocardial
Troponin Assessment. Does it Carry Clinical Message? Stefan Blankenberg. University Heart Center Hamburg
 Biomarkers for Optimal Management of Heart Failure Troponin Assessment Does it Carry Clinical Message? Stefan Blankenberg University Heart Center Hamburg Congress of the European Society of Cardiology
Biomarkers for Optimal Management of Heart Failure Troponin Assessment Does it Carry Clinical Message? Stefan Blankenberg University Heart Center Hamburg Congress of the European Society of Cardiology
Diagnosis is it really Heart Failure?
 ESC Congress Munich - 25-29 August 2012 Heart Failure with Preserved Ejection Fraction From Bench to Bedside Diagnosis is it really Heart Failure? Prof. Burkert Pieske Department of Cardiology Med.University
ESC Congress Munich - 25-29 August 2012 Heart Failure with Preserved Ejection Fraction From Bench to Bedside Diagnosis is it really Heart Failure? Prof. Burkert Pieske Department of Cardiology Med.University
HFPEF Echo with Strain vs. MRI T1 Mapping
 HFPEF Echo with Strain vs. MRI T1 Mapping Erik Schelbert, MD MS Director, Cardiovascular Magnetic Resonance Assistant Professor of Medicine Heart & Vascular Institute University of Pittsburgh Disclosures
HFPEF Echo with Strain vs. MRI T1 Mapping Erik Schelbert, MD MS Director, Cardiovascular Magnetic Resonance Assistant Professor of Medicine Heart & Vascular Institute University of Pittsburgh Disclosures
BNP as a Predictor of Cardiovascular Disease and All Cause Mortality. Dr. Thierry Le Jemtel
 BNP as a Predictor of Cardiovascular Disease and All Cause Mortality Dr. Thierry Le Jemtel Outline Role of BNP and probnp as relevant biomarkers in cardiac conditions Role of BNP and probnp as relevant
BNP as a Predictor of Cardiovascular Disease and All Cause Mortality Dr. Thierry Le Jemtel Outline Role of BNP and probnp as relevant biomarkers in cardiac conditions Role of BNP and probnp as relevant
Little is known about the degree and time course of
 Differential Changes in Regional Right Ventricular Function Before and After a Bilateral Lung Transplantation: An Ultrasonic Strain and Strain Rate Study Virginija Dambrauskaite, MD, Lieven Herbots, MD,
Differential Changes in Regional Right Ventricular Function Before and After a Bilateral Lung Transplantation: An Ultrasonic Strain and Strain Rate Study Virginija Dambrauskaite, MD, Lieven Herbots, MD,
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Imaging in Heart Failure: A Multimodality Approach. Thomas Ryan, MD
 Imaging in Heart Failure: A Multimodality Approach Thomas Ryan, MD Heart Failure HFrEF HFpEF EF50% Lifetime risk 20% Prevalence 6M Americans Societal costs - $30B 50% 5-year survival 1 Systolic
Imaging in Heart Failure: A Multimodality Approach Thomas Ryan, MD Heart Failure HFrEF HFpEF EF50% Lifetime risk 20% Prevalence 6M Americans Societal costs - $30B 50% 5-year survival 1 Systolic
Heterozygous Fabry Disease Females Are Not Just Carriers, But Suffer From
 Heterozygous Fabry Disease Females Are Not Just Carriers, But Suffer From Significant Burden of Disease And Impaired Quality of Life Raymond Wang, M.D. Children s Hospital of Orange County Division of
Heterozygous Fabry Disease Females Are Not Just Carriers, But Suffer From Significant Burden of Disease And Impaired Quality of Life Raymond Wang, M.D. Children s Hospital of Orange County Division of
The new Guidelines: Focus on Chronic Heart Failure
 The new Guidelines: Focus on Chronic Heart Failure Petros Nihoyannopoulos MD, FRCP, FESC Professor of Cardiology Imperial College London and National & Kapodistrian University of Athens 2 3 4 The principal
The new Guidelines: Focus on Chronic Heart Failure Petros Nihoyannopoulos MD, FRCP, FESC Professor of Cardiology Imperial College London and National & Kapodistrian University of Athens 2 3 4 The principal
Quantitation of right ventricular dimensions and function
 SCCS Basics of cardiac assessment Quantitation of right ventricular dimensions and function Tomasz Kukulski, MD PhD Dept of Cardiology, Congenital Heart Disease and Electrotherapy Silesian Medical University
SCCS Basics of cardiac assessment Quantitation of right ventricular dimensions and function Tomasz Kukulski, MD PhD Dept of Cardiology, Congenital Heart Disease and Electrotherapy Silesian Medical University
Cardiomyopathy in Fabry s disease
 Cardiomyopathy in Fabry s disease Herzinsuffizienzlunch Basel, 11.09.2018 Christiane Gruner Kardiologie, UniversitätsSpital Zürich Content Background / epidemiology Differential diagnosis Clinical presentations
Cardiomyopathy in Fabry s disease Herzinsuffizienzlunch Basel, 11.09.2018 Christiane Gruner Kardiologie, UniversitätsSpital Zürich Content Background / epidemiology Differential diagnosis Clinical presentations
Abstract nr AHA, Chicago November European Heart Journal Cardiovascular Imaging, in press. Nr Peter Blomstrand
 Left Ventricular Diastolic Function Assessed by Echocardiography and Tissue Doppler Imaging is a strong Predictor of Cardiovascular Events in Patients with Diabetes Mellitus Type 2 Peter Blomstrand, Martin
Left Ventricular Diastolic Function Assessed by Echocardiography and Tissue Doppler Imaging is a strong Predictor of Cardiovascular Events in Patients with Diabetes Mellitus Type 2 Peter Blomstrand, Martin
Chamber Quantitation Guidelines: What is New?
 Chamber Quantitation Guidelines: What is New? Roberto M Lang, MD J AM Soc Echocardiogr 2005; 18:1440-1463 1 Approximately 10,000 citations iase in itune Cardiac Chamber Quantification: What is New? Database
Chamber Quantitation Guidelines: What is New? Roberto M Lang, MD J AM Soc Echocardiogr 2005; 18:1440-1463 1 Approximately 10,000 citations iase in itune Cardiac Chamber Quantification: What is New? Database
LEFT BUNDLE BRANCH BLOCK- BENIGN OR A HARBINGER OF HEART FAILURE? PROGNOSTIC INDICATOR?
 LEFT BUNDLE BRANCH BLOCK- BENIGN OR A HARBINGER OF HEART FAILURE? PROGNOSTIC INDICATOR? Juan Cinca Department and Chair of Cardiology Hospital de la Santa Creu i Sant Pau Universitat Autònoma de Barcelona
LEFT BUNDLE BRANCH BLOCK- BENIGN OR A HARBINGER OF HEART FAILURE? PROGNOSTIC INDICATOR? Juan Cinca Department and Chair of Cardiology Hospital de la Santa Creu i Sant Pau Universitat Autònoma de Barcelona
Myocardial Strain Imaging in Cardiac Diseases and Cardiomyopathies.
 Myocardial Strain Imaging in Cardiac Diseases and Cardiomyopathies. Session: Cardiomyopathy Tarun Pandey MD, FRCR. Associate Professor University of Arkansas for Medical Sciences Disclosures No relevant
Myocardial Strain Imaging in Cardiac Diseases and Cardiomyopathies. Session: Cardiomyopathy Tarun Pandey MD, FRCR. Associate Professor University of Arkansas for Medical Sciences Disclosures No relevant
Atrial dyssynchrony syndrome: An overlooked cause of heart failure with normal ejection fraction
 Atrial dyssynchrony syndrome: An overlooked cause of heart failure with normal ejection fraction JC Eicher, G Laurent, O Barthez, A Mathé, G Bertaux, JE Wolf Heart Failure Treatment Unit, Rhythmology and
Atrial dyssynchrony syndrome: An overlooked cause of heart failure with normal ejection fraction JC Eicher, G Laurent, O Barthez, A Mathé, G Bertaux, JE Wolf Heart Failure Treatment Unit, Rhythmology and
Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes
 Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes Seung-Jae Joo and other KAMIR-NIH investigators Department of Cardiology, Jeju National
Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes Seung-Jae Joo and other KAMIR-NIH investigators Department of Cardiology, Jeju National
Restrictive Cardiomyopathy
 ESC Congress 2011, Paris Imaging Unusual Causes of Cardiomyopathy Restrictive Cardiomyopathy Kazuaki Tanabe, MD, PhD Professor of Medicine Chair, Division of Cardiology Izumo, Japan I Have No Disclosures
ESC Congress 2011, Paris Imaging Unusual Causes of Cardiomyopathy Restrictive Cardiomyopathy Kazuaki Tanabe, MD, PhD Professor of Medicine Chair, Division of Cardiology Izumo, Japan I Have No Disclosures
Copeptin in heart failure: Associations with clinical characteristics and prognosis
 Copeptin in heart failure: Associations with clinical characteristics and prognosis D. Berliner, N. Deubner, W. Fenske, S. Brenner, G. Güder, B. Allolio, R. Jahns, G. Ertl, CE. Angermann, S. Störk for
Copeptin in heart failure: Associations with clinical characteristics and prognosis D. Berliner, N. Deubner, W. Fenske, S. Brenner, G. Güder, B. Allolio, R. Jahns, G. Ertl, CE. Angermann, S. Störk for
Right Ventricular Strain in Normal Healthy Adult Filipinos: A Retrospective, Cross- Sectional Pilot Study
 Right Ventricular Strain in Normal Healthy Adult Filipinos: A Retrospective, Cross- Sectional Pilot Study By Julius Caesar D. de Vera, MD Jonnah Fatima B. Pelat, MD Introduction Right ventricle contributes
Right Ventricular Strain in Normal Healthy Adult Filipinos: A Retrospective, Cross- Sectional Pilot Study By Julius Caesar D. de Vera, MD Jonnah Fatima B. Pelat, MD Introduction Right ventricle contributes
A classic case of amyloid cardiomyopathy
 Images in... A classic case of amyloid cardiomyopathy Hayan Jouni, 1 William G Morice, 2 S Vincent Rajkumar, 3 Joerg Herrmann 4 1 Department of Internal Medicine, Mayo Clinic, Rochester, Minnesota, USA
Images in... A classic case of amyloid cardiomyopathy Hayan Jouni, 1 William G Morice, 2 S Vincent Rajkumar, 3 Joerg Herrmann 4 1 Department of Internal Medicine, Mayo Clinic, Rochester, Minnesota, USA
Nancy Goldman Cutler, MD Beaumont Children s Hospital Royal Oak, Mi
 Nancy Goldman Cutler, MD Beaumont Children s Hospital Royal Oak, Mi Identify increased LV wall thickness (WT) Understand increased WT in athletes Understand hypertrophic cardiomyopathy (HCM) Enhance understanding
Nancy Goldman Cutler, MD Beaumont Children s Hospital Royal Oak, Mi Identify increased LV wall thickness (WT) Understand increased WT in athletes Understand hypertrophic cardiomyopathy (HCM) Enhance understanding
Title:Relation Between E/e' ratio and NT-proBNP Levels in Elderly Patients with Symptomatic Severe Aortic Stenosis
 Author's response to reviews Title:Relation Between E/e' ratio and NT-proBNP Levels in Elderly Patients with Symptomatic Severe Aortic Stenosis Authors: Mihai Strachinaru (m.strachinaru@erasmusmc.nl) Bas
Author's response to reviews Title:Relation Between E/e' ratio and NT-proBNP Levels in Elderly Patients with Symptomatic Severe Aortic Stenosis Authors: Mihai Strachinaru (m.strachinaru@erasmusmc.nl) Bas
Cardiac magnetic resonance imaging in patients with Fabry s disease
 Chorzy trudni nietypowi/case report Cardiac magnetic resonance imaging in patients with Fabry s disease Kardiologia Polska 2010; 68, 8: 929 934 Copyright Via Medica ISSN 0022 9032 Obrazowanie serca za
Chorzy trudni nietypowi/case report Cardiac magnetic resonance imaging in patients with Fabry s disease Kardiologia Polska 2010; 68, 8: 929 934 Copyright Via Medica ISSN 0022 9032 Obrazowanie serca za
Imaging in dilated cardiomyopathy : factors associated with a poor outcome
 Imaging in dilated cardiomyopathy : factors associated with a poor outcome Johan De Sutter, MD, PhD, FESC AZ Maria Middelares Gent and University Gent - Belgium Dilated cardiomyopathy Cardiomyopathy with
Imaging in dilated cardiomyopathy : factors associated with a poor outcome Johan De Sutter, MD, PhD, FESC AZ Maria Middelares Gent and University Gent - Belgium Dilated cardiomyopathy Cardiomyopathy with
An Integrated Approach to Study LV Diastolic Function
 An Integrated Approach to Study LV Diastolic Function Assoc. Prof. Adriana Ilieşiu, FESC University of Medicine Carol Davila Bucharest, Romania LV Diastolic Dysfunction impaired relaxation (early diastole)
An Integrated Approach to Study LV Diastolic Function Assoc. Prof. Adriana Ilieşiu, FESC University of Medicine Carol Davila Bucharest, Romania LV Diastolic Dysfunction impaired relaxation (early diastole)
Strain Imaging: Myocardial Mechanics Simplified and Applied
 9/28/217 Strain Imaging: Myocardial Mechanics Simplified and Applied John Gorcsan III, MD Professor of Medicine Director of Clinical Research Division of Cardiology VECTORS OF CONTRACTION Shortening Thickening
9/28/217 Strain Imaging: Myocardial Mechanics Simplified and Applied John Gorcsan III, MD Professor of Medicine Director of Clinical Research Division of Cardiology VECTORS OF CONTRACTION Shortening Thickening
Effect of Short-term Maximal Exercise on BNP Plasma Levels in. Healthy Individuals
 1 Effect of Short-term Maximal Exercise on BNP Plasma Levels in Healthy Individuals Jan Krupicka, MD, Tomas Janota, MD, Zdislava Kasalova, MD, Jaromir Hradec, MD 3rd Department of Internal Medicine, 1st
1 Effect of Short-term Maximal Exercise on BNP Plasma Levels in Healthy Individuals Jan Krupicka, MD, Tomas Janota, MD, Zdislava Kasalova, MD, Jaromir Hradec, MD 3rd Department of Internal Medicine, 1st
To estimate the serum level of N-terminal pro-brain natriuretic peptide levels in acute coronary syndrome
 Original Research Article To estimate the serum level of N-terminal pro-brain natriuretic peptide levels in acute coronary syndrome Mohamed Yasar Arafath 1, K. Babu Raj 2* 1 First Year Post Graduate, 2
Original Research Article To estimate the serum level of N-terminal pro-brain natriuretic peptide levels in acute coronary syndrome Mohamed Yasar Arafath 1, K. Babu Raj 2* 1 First Year Post Graduate, 2
Aortic stenosis (AS) is common with the aging population.
 New Insights Into the Progression of Aortic Stenosis Implications for Secondary Prevention Sanjeev Palta, MD; Anita M. Pai, MD; Kanwaljit S. Gill, MD; Ramdas G. Pai, MD Background The risk factors affecting
New Insights Into the Progression of Aortic Stenosis Implications for Secondary Prevention Sanjeev Palta, MD; Anita M. Pai, MD; Kanwaljit S. Gill, MD; Ramdas G. Pai, MD Background The risk factors affecting
LCZ696 A First-in-Class Angiotensin Receptor Neprilysin Inhibitor
 The Angiotensin Receptor Neprilysin Inhibitor LCZ696 in Heart Failure with Preserved Ejection Fraction The Prospective comparison of ARNI with ARB on Management Of heart failure with preserved ejection
The Angiotensin Receptor Neprilysin Inhibitor LCZ696 in Heart Failure with Preserved Ejection Fraction The Prospective comparison of ARNI with ARB on Management Of heart failure with preserved ejection
The ACC Heart Failure Guidelines
 The ACC Heart Failure Guidelines Fakhr Alayoubi, Msc,R Ph President of SCCP Cardiology Clinical Pharmacist Assistant Professor At King Saud University King Khalid University Hospital Riyadh-KSA 2017 ACC/AHA/HFSA
The ACC Heart Failure Guidelines Fakhr Alayoubi, Msc,R Ph President of SCCP Cardiology Clinical Pharmacist Assistant Professor At King Saud University King Khalid University Hospital Riyadh-KSA 2017 ACC/AHA/HFSA
10/7/2013. Systolic Function How to Measure, How Accurate is Echo, Role of Contrast. Thanks to our Course Director: Neil J.
 Systolic Function How to Measure, How Accurate is Echo, Role of Contrast Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University Washington, D.C. No Disclosures
Systolic Function How to Measure, How Accurate is Echo, Role of Contrast Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University Washington, D.C. No Disclosures
RIGHT VENTRICULAR SIZE AND FUNCTION
 RIGHT VENTRICULAR SIZE AND FUNCTION Edwin S. Tucay, MD, FPCC, FPCC, FPSE Philippine Society of Echocardiography Quezon City, Philippines Echo Mission, BRTTH, Legaspi City, July 1-2, 2016 NO DISCLOSURE
RIGHT VENTRICULAR SIZE AND FUNCTION Edwin S. Tucay, MD, FPCC, FPCC, FPSE Philippine Society of Echocardiography Quezon City, Philippines Echo Mission, BRTTH, Legaspi City, July 1-2, 2016 NO DISCLOSURE
PART II ECHOCARDIOGRAPHY LABORATORY OPERATIONS ADULT TRANSTHORACIC ECHOCARDIOGRAPHY TESTING
 PART II ECHOCARDIOGRAPHY LABORATORY OPERATIONS ADULT TRANSTHORACIC ECHOCARDIOGRAPHY TESTING STANDARD - Primary Instrumentation 1.1 Cardiac Ultrasound Systems SECTION 1 Instrumentation Ultrasound instruments
PART II ECHOCARDIOGRAPHY LABORATORY OPERATIONS ADULT TRANSTHORACIC ECHOCARDIOGRAPHY TESTING STANDARD - Primary Instrumentation 1.1 Cardiac Ultrasound Systems SECTION 1 Instrumentation Ultrasound instruments
E/Ea is NOT an essential estimator of LV filling pressures
 Euroecho Kopenhagen Echo in Resynchronization in 2010 E/Ea is NOT an essential estimator of LV filling pressures Wilfried Mullens, MD, PhD December 10, 2010 Ziekenhuis Oost Limburg Genk University Hasselt
Euroecho Kopenhagen Echo in Resynchronization in 2010 E/Ea is NOT an essential estimator of LV filling pressures Wilfried Mullens, MD, PhD December 10, 2010 Ziekenhuis Oost Limburg Genk University Hasselt
Impaired Regional Myocardial Function Detection Using the Standard Inter-Segmental Integration SINE Wave Curve On Magnetic Resonance Imaging
 Original Article Impaired Regional Myocardial Function Detection Using the Standard Inter-Segmental Integration Ngam-Maung B, RT email : chaothawee@yahoo.com Busakol Ngam-Maung, RT 1 Lertlak Chaothawee,
Original Article Impaired Regional Myocardial Function Detection Using the Standard Inter-Segmental Integration Ngam-Maung B, RT email : chaothawee@yahoo.com Busakol Ngam-Maung, RT 1 Lertlak Chaothawee,
Effectiveness of agalsidase alfa enzyme replacement in Fabry disease: cardiac outcomes after 10 years treatment
 Kampmann et al. Orphanet Journal of Rare Diseases (205) 0:25 DOI 0.86/s02-05-08-2 RESEARCH Open Access Effectiveness of agalsidase alfa enzyme replacement in Fabry disease: cardiac outcomes after 0 years
Kampmann et al. Orphanet Journal of Rare Diseases (205) 0:25 DOI 0.86/s02-05-08-2 RESEARCH Open Access Effectiveness of agalsidase alfa enzyme replacement in Fabry disease: cardiac outcomes after 0 years
Jong-Won Ha*, Jeong-Ah Ahn, Jae-Yun Moon, Hye-Sun Suh, Seok-Min Kang, Se-Joong Rim, Yangsoo Jang, Namsik Chung, Won-Heum Shim, Seung-Yun Cho
 Eur J Echocardiography (2006) 7, 16e21 CLINICAL/ORIGINAL PAPERS Triphasic mitral inflow velocity with mid-diastolic flow: The presence of mid-diastolic mitral annular velocity indicates advanced diastolic
Eur J Echocardiography (2006) 7, 16e21 CLINICAL/ORIGINAL PAPERS Triphasic mitral inflow velocity with mid-diastolic flow: The presence of mid-diastolic mitral annular velocity indicates advanced diastolic
Clinical material and methods. Departments of 1 Cardiology and 2 Anatomy, Gaziantep University, School of Medicine, Gaziantep, Turkey
 Interatrial Block and P-Terminal Force: A Reflection of Mitral Stenosis Severity on Electrocardiography Murat Yuce 1, Vedat Davutoglu 1, Cayan Akkoyun 1, Nese Kizilkan 2, Suleyman Ercan 1, Murat Akcay
Interatrial Block and P-Terminal Force: A Reflection of Mitral Stenosis Severity on Electrocardiography Murat Yuce 1, Vedat Davutoglu 1, Cayan Akkoyun 1, Nese Kizilkan 2, Suleyman Ercan 1, Murat Akcay
DISCLOSURE. Myocardial Mechanics. Relevant Financial Relationship(s) Off Label Usage
 7th Annual Team Echocardiography: The Heart of Cardiovascular Medicine Tissue Doppler, Strain, Speckle: What? How? Christopher J Kramer RDCS Aurora Medical Group Advanced Cardiovascular Services, Aurora
7th Annual Team Echocardiography: The Heart of Cardiovascular Medicine Tissue Doppler, Strain, Speckle: What? How? Christopher J Kramer RDCS Aurora Medical Group Advanced Cardiovascular Services, Aurora
ASCeXAM / ReASCE. Practice Board Exam Questions Monday Morning
 ASCeXAM / ReASCE Practice Board Exam Questions Monday Morning Ultrasound Physics Artifacts Doppler Physics Imaging, Knobology, and Artifacts Echocardiographic Evaluation of the RV Tricuspid and Pulmonary
ASCeXAM / ReASCE Practice Board Exam Questions Monday Morning Ultrasound Physics Artifacts Doppler Physics Imaging, Knobology, and Artifacts Echocardiographic Evaluation of the RV Tricuspid and Pulmonary
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM. General Instructions: ID NUMBER: FORM NAME: H F A DATE: 10/13/2017 VERSION: CONTACT YEAR NUMBER:
 ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
Cardiac Chamber Quantification by Echocardiography
 Cardiac Chamber Quantification by Echocardiography Maryam Bokhamseen, RCS, RCDS, EACVI Echotechnologist ǁ, Non invasive Cardiac Laboratory King Abdulaziz Cardiac Center. Outline: Introduction. Background
Cardiac Chamber Quantification by Echocardiography Maryam Bokhamseen, RCS, RCDS, EACVI Echotechnologist ǁ, Non invasive Cardiac Laboratory King Abdulaziz Cardiac Center. Outline: Introduction. Background
Left ventricular diastolic function and filling pressure in patients with dilated cardiomyopathy
 Left ventricular diastolic function and filling pressure in patients with dilated cardiomyopathy Bogdan A. Popescu University of Medicine and Pharmacy Bucharest, Romania My conflicts of interest: I have
Left ventricular diastolic function and filling pressure in patients with dilated cardiomyopathy Bogdan A. Popescu University of Medicine and Pharmacy Bucharest, Romania My conflicts of interest: I have
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Advanced Multi-Layer Speckle Strain Permits Transmural Myocardial Function Analysis in Health and Disease:
 Advanced Multi-Layer Speckle Strain Permits Transmural Myocardial Function Analysis in Health and Disease: Clinical Case Examples Jeffrey C. Hill, BS, RDCS Echocardiography Laboratory, University of Massachusetts
Advanced Multi-Layer Speckle Strain Permits Transmural Myocardial Function Analysis in Health and Disease: Clinical Case Examples Jeffrey C. Hill, BS, RDCS Echocardiography Laboratory, University of Massachusetts
Trial to Reduce. Aranesp* Therapy. Cardiovascular Events with
 Trial to Reduce Cardiovascular Events with Aranesp* Therapy John J.V. McMurray, Hajime Uno, Petr Jarolim, Akshay S. Desai, Dick de Zeeuw, Kai-Uwe Eckardt, Peter Ivanovich, Andrew S. Levey, Eldrin F. Lewis,
Trial to Reduce Cardiovascular Events with Aranesp* Therapy John J.V. McMurray, Hajime Uno, Petr Jarolim, Akshay S. Desai, Dick de Zeeuw, Kai-Uwe Eckardt, Peter Ivanovich, Andrew S. Levey, Eldrin F. Lewis,
Managing Hypertrophic Cardiomyopathy with Imaging. Gisela C. Mueller University of Michigan Department of Radiology
 Managing Hypertrophic Cardiomyopathy with Imaging Gisela C. Mueller University of Michigan Department of Radiology Disclosures Gadolinium contrast material for cardiac MRI Acronyms Afib CAD Atrial fibrillation
Managing Hypertrophic Cardiomyopathy with Imaging Gisela C. Mueller University of Michigan Department of Radiology Disclosures Gadolinium contrast material for cardiac MRI Acronyms Afib CAD Atrial fibrillation
Clinical benefit of enzyme replacement therapy in Fabry disease
 original article http://www.kidney-international.org & 2006 International Society of Nephrology Clinical benefit of enzyme replacement therapy in Fabry disease F Breunig 1, F Weidemann 2, J Strotmann 2,
original article http://www.kidney-international.org & 2006 International Society of Nephrology Clinical benefit of enzyme replacement therapy in Fabry disease F Breunig 1, F Weidemann 2, J Strotmann 2,
Cardiac Magnetic Resonance in pregnant women
 Cardiac Magnetic Resonance in pregnant women Chen SSM, Leeton L, Dennis AT Royal Women s Hospital and The University of Melbourne, Parkville, Australia alicia.dennis@thewomens.org.au Quantification of
Cardiac Magnetic Resonance in pregnant women Chen SSM, Leeton L, Dennis AT Royal Women s Hospital and The University of Melbourne, Parkville, Australia alicia.dennis@thewomens.org.au Quantification of
The right heart: the Cinderella of heart failure
 The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
Effects of Kidney Disease on Cardiovascular Morbidity and Mortality
 Effects of Kidney Disease on Cardiovascular Morbidity and Mortality Joachim H. Ix, MD, MAS Assistant Professor in Residence Division of Nephrology University of California San Diego, and Veterans Affairs
Effects of Kidney Disease on Cardiovascular Morbidity and Mortality Joachim H. Ix, MD, MAS Assistant Professor in Residence Division of Nephrology University of California San Diego, and Veterans Affairs
Congestive Heart Failure: Outpatient Management
 The Chattanooga Heart Institute Cardiovascular Symposium Congestive Heart Failure: Outpatient Management E. Philip Lehman MD, MPP Disclosure No financial disclosures. Objectives Evidence-based therapy
The Chattanooga Heart Institute Cardiovascular Symposium Congestive Heart Failure: Outpatient Management E. Philip Lehman MD, MPP Disclosure No financial disclosures. Objectives Evidence-based therapy
Echocardiography. Guidelines for Valve and Chamber Quantification. In partnership with
 Echocardiography Guidelines for Valve and Chamber Quantification In partnership with Explanatory note & references These guidelines have been developed by the Education Committee of the British Society
Echocardiography Guidelines for Valve and Chamber Quantification In partnership with Explanatory note & references These guidelines have been developed by the Education Committee of the British Society
ΒΙΟΔΕΙΚΤΕΣ ΣΤΗΝ ΚΑΡΔΙΑΚΗ ΑΝΕΠΑΡΚΕΙΑ. ΔΗΜΗΤΡΙΟΣ ΤΟΥΣΟΥΛΗΣ Καθηγητής Καρδιολογίας
 ΕΘΝΙΚΟ ΚΑΙ ΚΑΠΟΔΙΣΤΡΙΑΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΑΘΗΝΩΝ ΙΑΤΡΙΚΗ ΣΧΟΛΗ Ά ΚΑΡΔΙΟΛΟΓΙΚΗ ΚΛΙΝΙΚΗ Διευθυντής: Καθηγητής Δημήτριος Τούσουλης ΒΙΟΔΕΙΚΤΕΣ ΣΤΗΝ ΚΑΡΔΙΑΚΗ ΑΝΕΠΑΡΚΕΙΑ ΔΗΜΗΤΡΙΟΣ ΤΟΥΣΟΥΛΗΣ Καθηγητής Καρδιολογίας
ΕΘΝΙΚΟ ΚΑΙ ΚΑΠΟΔΙΣΤΡΙΑΚΟ ΠΑΝΕΠΙΣΤΗΜΙΟ ΑΘΗΝΩΝ ΙΑΤΡΙΚΗ ΣΧΟΛΗ Ά ΚΑΡΔΙΟΛΟΓΙΚΗ ΚΛΙΝΙΚΗ Διευθυντής: Καθηγητής Δημήτριος Τούσουλης ΒΙΟΔΕΙΚΤΕΣ ΣΤΗΝ ΚΑΡΔΙΑΚΗ ΑΝΕΠΑΡΚΕΙΑ ΔΗΜΗΤΡΙΟΣ ΤΟΥΣΟΥΛΗΣ Καθηγητής Καρδιολογίας
CT for Myocardial Characterization of Cardiomyopathy. Byoung Wook Choi, Yonsei University Severance Hospital, Seoul, Korea
 CT for Myocardial Characterization of Cardiomyopathy Byoung Wook Choi, Yonsei University Severance Hospital, Seoul, Korea Cardiomyopathy Elliott P et al. Eur Heart J 2008;29:270-276 The European Society
CT for Myocardial Characterization of Cardiomyopathy Byoung Wook Choi, Yonsei University Severance Hospital, Seoul, Korea Cardiomyopathy Elliott P et al. Eur Heart J 2008;29:270-276 The European Society
Effect of Ventricular Pacing on Myocardial Function. Inha University Hospital Sung-Hee Shin
 Effect of Ventricular Pacing on Myocardial Function Inha University Hospital Sung-Hee Shin Contents 1. The effect of right ventricular apical pacing 2. Strategies for physiologically optimal ventricular
Effect of Ventricular Pacing on Myocardial Function Inha University Hospital Sung-Hee Shin Contents 1. The effect of right ventricular apical pacing 2. Strategies for physiologically optimal ventricular
The Impact of Autonomic Neuropathy on Left Ventricular Function in Normotensive Type 1 Diabetic Patients: a Tissue Doppler Echocardiographic Study
 Diabetes Care Publish Ahead of Print, published online November 13, 2007 The Impact of Autonomic Neuropathy on Left Ventricular Function in Normotensive Type 1 Diabetic Patients: a Tissue Doppler Echocardiographic
Diabetes Care Publish Ahead of Print, published online November 13, 2007 The Impact of Autonomic Neuropathy on Left Ventricular Function in Normotensive Type 1 Diabetic Patients: a Tissue Doppler Echocardiographic
Doppler Basic & Hemodynamic Calculations
 Doppler Basic & Hemodynamic Calculations August 19, 2017 Smonporn Boonyaratavej MD Division of Cardiology, Department of Medicine Chulalongkorn University Cardiac Center, King Chulalongkorn Memorial Hospital
Doppler Basic & Hemodynamic Calculations August 19, 2017 Smonporn Boonyaratavej MD Division of Cardiology, Department of Medicine Chulalongkorn University Cardiac Center, King Chulalongkorn Memorial Hospital
ECHOCARDIOGRAPHY DATA REPORT FORM
 Patient ID Patient Study ID AVM - - Date of form completion / / 20 Initials of person completing the form mm dd yyyy Study period Preoperative Postoperative Operative 6-month f/u 1-year f/u 2-year f/u
Patient ID Patient Study ID AVM - - Date of form completion / / 20 Initials of person completing the form mm dd yyyy Study period Preoperative Postoperative Operative 6-month f/u 1-year f/u 2-year f/u
