doi: /anae.14345
|
|
|
- Owen Byrd
- 5 years ago
- Views:
Transcription
1 doi: /anae Original Article The effect of high-flow nasal oxygen on hospital length of stay in cardiac surgical patients at high risk for respiratory complications: a randomised controlled trial* V. Zochios, 1 T. Collier, 2 G. Blaudszun, 3 A. Butchart, 4 M. Earwaker, 5 N. Jones 6 and A. A. Klein 6 1 Specialty Registrar and National Institute for Health Research Academic Fellow, Department of Intensive Care Medicine, University Hospitals Birmingham National Health Service Foundation Trust, Queen Elizabeth Hospital Birmingham, University of Birmingham, UK 2 Associate Professor, Medical Statistics Department, London School of Hygiene and Tropical Medicine, London, UK 3 Senior Registrar, Department of Anaesthesia, Pharmacology and Intensive Care Medicine, Geneva University Hospitals, Geneve, Switzerland 4 Locum Consultant, 6 Consultant, Department of Cardiothoracic Anaesthesia and Intensive Care Medicine, 5 Clinical Trial Co-ordinator, Research and Development Department, 6 Consultant, Department of Anaesthesia and Intensive care, Royal Papworth Hospital National Health Service Foundation Trust, Cambridge, UK Summary There has been increased interest in the prophylactic and therapeutic use of high-flow nasal oxygen in patients with, or at risk of, non-hypercapnic respiratory failure. There are no randomised trials examining the efficacy of high-flow nasal oxygen in high-risk cardiac surgical patients. We sought to determine whether routine administration of high-flow nasal oxygen, compared with standard oxygen therapy, leads to reduced hospital length of stay after cardiac surgery in patients with pre-existing respiratory disease at high risk for postoperative pulmonary complications. Adult patients with pre-existing respiratory disease undergoing elective cardiac surgery were randomly allocated to receive high-flow nasal oxygen (n = 51) or standard oxygen therapy (n = 49). The primary outcome was hospital length of stay and all analyses were carried out on an intention-to-treat basis. Median (IQR [range]) hospital length of stay was 7 (6 9 [4 30]) days in the high-flow nasal oxygen group and 9 (7 16 [4 120]) days in the standard oxygen group (p=0.012). Geometric mean hospital length of stay was 29% lower in the high-flow nasal group (95%CI 11 44%, p = 0.004). High-flow nasal oxygen was also associated with fewer intensive care unit re-admissions (1/49 vs. 7/45; p = 0.026). When compared with standard care, prophylactic postoperative high-flow nasal oxygen reduced hospital length of stay and intensive care unit re-admission. This is the first randomised controlled trial examining the effect of prophylactic high-flow nasal oxygen use on patientcentred outcomes in cardiac surgical patients at high risk for postoperative respiratory complications.... Correspondence to: V. Zochios vasileioszochios@doctors.org.uk Accepted: 29 April 2018 Keywords: cardiothoracic surgery; length of stay; morbidity; oxygen therapy *Presented in part at the Association for Cardiothoracic Anaesthesia and Critical Care (ACTACC) meeting, Birmingham, UK, June 2017 and at the Association of Anaesthetists Annual Congress, Liverpool, UK, September The Authors. Anaesthesia published by John Wiley & Sons Ltd on behalf of Association of Anaesthetists. This is an open access article under the terms of the Creative Commons Attribution-NonCommercial License, which permits use, distribution and reproduction in any medium, provided the original work is properly cited and is not used for commercial purposes.
2 Zochios et al. High-flow nasal oxygen in high-risk cardiac surgical patients Introduction Patients undergoing cardiac surgery are at significant risk of postoperative pulmonary complications, and these complications may increase morbidity and mortality and lead to prolonged intensive care unit (ICU) and hospital length of stay (LOS) [1]. The reported incidence of postoperative pulmonary complications following cardiac surgery ranges from 8% to 79% [2]. Postoperative pulmonary complications manifest early as hypoxaemia, later pneumonia, and in rare cases also as acute respiratory distress syndrome [3]. The incidence of postoperative pulmonary complications is increased in patients with intrinsic respiratory disease, asthma, chronic obstructive pulmonary disease (COPD) and heavy smokers [4]. These patients often stay longer in the ICU after surgery due to lower respiratory tract infections, impaired ventilation and the need for prolonged ventilatory support. They are also more likely to require re-admission to ICU for unplanned continuous positive airways pressure (CPAP), non-invasive or invasive mechanical ventilation. Therefore, hospital stay is prolonged compared with low-risk patients after cardiac surgery [5 7]. A contributing mechanism of postoperative pulmonary complications is atelectasis, which has been shown to affect up to 90% of patients undergoing cardiac surgery. Atelectasis has been shown to be resistant to simple techniques such as patient positioning and incentive spirometry [8]. Lung recruitment manoeuvres and positive airways pressure may reduce atelectasis development, but this effect is lost after tracheal extubation [9]. Prophylactic nasal CPAP reduces postoperative pulmonary complications after cardiac surgery [10]. However, CPAP is costly and requires more intensive involvement by hospital staff. In many hospitals, its use requires admission to at least a high dependency area or even ICU, thus further increasing costs. Apart from the expense and extra healthcare provision costs, common potential side-effects from CPAP include mask discomfort, skin abrasions, inability to communicate effectively, inability to eat or drink while the device is in use, inability to mobilise and irritation from device noise [11, 12]. High-flow nasal oxygen therapy delivers warmed humidified oxygen and low level, flow-dependent positive airways pressure, and may be better tolerated than CPAP or non-invasive ventilation; moreover, high-flow nasal oxygen enhances washout of nasopharyngeal dead space, thus improving oxygenation [13 16]. It has been shown that high-flow nasal oxygen is both safe and noninferior to conventional CPAP in providing prophylactic support to very preterm neonates after extubation while the incidence of nasal trauma was significantly lower than in the CPAP group [17]. No study has assessed the effect of prophylactic use of high-flow nasal oxygen on hospital stay in adult cardiac surgical patients with significant risk factors for postoperative pulmonary complications. We therefore, decided to study high-risk patients with preexisting lung disease (COPD, asthma, recent lower respiratory tract infection), heavy smokers or morbidly obese patients (body mass index (BMI) 35 kg.m 2 ), who were expected to stay longer in ICU and hospital due to increased respiratory complications. We tested the hypothesis that routine administration of high-flow nasal oxygen leads to reduced hospital length of stay after cardiac surgery compared with standard oxygen therapy. Methods Following national research ethics service (East Midlands Research Ethics Committee UK) and local Research and Development approval, written informed consent was obtained from all patients. Patients scheduled for elective cardiac surgery (coronary artery bypass grafting (CABG), valve surgery or both) were screened for eligibility. Patients were included in the trial if they were aged > 18 years, had one or more patient-related risk factors for postoperative pulmonary complications (COPD, asthma, lower respiratory tract infection in preceding four weeks, BMI 35 kg.m 2, current (within last six weeks) heavy smokers (> 10 pack years)) and were capable of performing a 6-minute walk test (6MWT). Only patients with a formal COPD or asthma diagnosis (as defined by British Thoracic Society and National Institute for Health and Care Excellence) on inhaled therapy were enrolled [18, 19]. Lower respiratory tract infection was defined according to National Institute for Health and Care Excellence as an acute illness, usually with cough as the main symptom, and with at least one other lower respiratory tract symptom (such as fever, sputum production, breathlessness, wheeze or chest discomfort/pain) and no alternative explanation [20]. According to the trial protocol, patients in whom high-flow nasal oxygen was contraindicated (presence of a nasal septal defect), those who needed CPAP pre-operatively or those who did not meet tracheal extubation criteria by the day after surgery (as they did not follow the local protocolised peri-operative care pathway), were not studied. Randomisation was performed using a computer-generated assignment sequence and a centralised online system before the induction of anaesthesia while the patients were in the operating theatre. Participating patients were randomly allocated in a 1:1 ratio (block randomisation procedure 2018 The Authors. Anaesthesia published by John Wiley & Sons Ltd on behalf of Association of Anaesthetists. 1479
3 Zochios et al. High-flow nasal oxygen in high-risk cardiac surgical patients with randomly selected block sizes keeping the investigators blinded to the size of each block) to either the highflow nasal oxygen or standard oxygen therapy group. A research nurse or clinical investigator not involved in the clinical care of the patient obtained the treatment allocation and informed the ICU nursing staff in order that the allocated therapy was prepared. We were, therefore, unable to blind patients or nursing staff in the ICU. Surgical and nursing teams responsible for deciding when patients were discharged (and therefore hospital stay) and other aspects of their postoperative care on the surgical ward were blinded as to group allocation. Study participants underwent a 6MWT before the operation, conducted in a standard manner according to the guidelines of the American Thoracic Society [21]. Additionally, patients underwent pre-operative spirometry testing. This was repeated three times, and average values for forced expiratory volume in one second (FEV 1 ) and forced vital capacity (FVC), were calculated. The anaesthetic technique and surgical procedure were not affected by patients participation in this study. Anaesthesia was induced with midazolam, fentanyl and propofol, neuromuscular blockade achieved with pancuronium and anaesthesia maintained with a continuous infusion of propofol and/or inhalational anaesthetic agent at the discretion of the attending anaesthetist. All patients lungs were ventilated using volume control ventilation and the same intra-operative ventilatory settings, in accordance with local practice: tidal volume 6 8 ml.kg 1 predicted body weight; positive end-expiratory pressure (PEEP) level of 5 cmh 2 O; cessation of mechanical ventilation and zero PEEP during cardiopulmonary bypass. At the end of surgery, patients were transferred to the ICU where they received standard post-cardiac surgery monitoring and treatment. Patients tracheas were extubated once they were normothermic and not bleeding, had established a regular respiratory pattern, had no significant residual neuromuscular blockade and did not complain of anything other than mild pain. Postoperative pain relief was provided by regular paracetamol and opioid analgesia for all patients, unless they had a specific contraindication (e.g. known drug allergy). Following tracheal extubation, patients received either high-flow nasal oxygen or standard oxygen therapy, that is, low-flow oxygen via nasal prongs or a soft facemask, according to the randomisation performed before surgery. The high-flow nasal oxygen was set up and connected to the patients by the ICU nurses who had been trained before the start of the study. The fraction of inspired oxygen (F I O 2 ) delivered was titrated to that which resulted in a pulse oximeter saturation of at least 95% (93% for those at risk of hypercapnic respiratory failure, such as confirmed COPD patients and morbidly obese patients) according to the British Thoracic Society guidelines for oxygen use in adult patients [22]. The F I O 2 was actively reduced to the minimum level which achieved this goal. Gas flow for the high-flow nasal oxygen was calculated for each patient, based on their body characteristics and comfort level. The standard starting flow rate was 30 l.min 1, and this was adjusted up or down between a range of l.min 1 with the aim of achieving a respiratory rate of less than 16 breaths per minute and patient comfort. Patients randomised to receive standard oxygen therapy were fitted with nasal prongs or a soft facemask and the oxygen flow titrated to provide oximetry saturations of at least 95% (93% for those at risk of hypercapnic respiratory failure, such as confirmed COPD patients and morbidly obese patients). Both groups of patients had oxygen therapy prescribed for the first 24 h postoperatively and were transferred to surgical wards once they fulfilled pre-specified physiological criteria. Oxygen therapy was discontinued after 24 h unless there was evidence of respiratory deterioration (dyspnoea, oxygen saturation < 95% (or < 93% for COPD and morbidly obese patients), respiratory rate > 20 breaths per minute). Patients randomly allocated to receive high-flow nasal oxygen could have high-flow nasal oxygen continued for more than 24 h (in the ICU or surgical ward) if it was deemed necessary. Patients who continued to be in respiratory distress (respiratory rate > 20 breaths per minute, oxygen saturation < 95% (or < 93% for COPD and morbidly obese patients)) were treated initially by increasing the F I O 2. Failing these measures, CPAP, noninvasive ventilation or, if necessary, invasive mechanical ventilation were considered, as is standard practice at our institution. Participation in the study did not preclude any measures which the clinical team caring for the patient felt were necessary. As part of their standard care, all patients were instructed on appropriate respiratory exercises postoperatively. On postoperative day 5 or 6, patients had both the 6MWT and spirometry testing repeated. Removal of chest drains was decided upon by the surgical team, who also decided when patients would be discharged from the hospital. The surgical team and the physiotherapists were unaware of the study group allocations unless oxygen therapy was continued after discharge from ICU. The primary outcome of the study was hospital stay. Pre-specified secondary outcomes were: ICU stay; ICU readmission rate; in-hospital mortality rate; pulmonary The Authors. Anaesthesia published by John Wiley & Sons Ltd on behalf of Association of Anaesthetists.
4 Zochios et al. High-flow nasal oxygen in high-risk cardiac surgical patients function tests (postoperative FEV 1 and FVC); 6MWT (pre- and postoperatively) and postoperative quality of recovery assessed using the postoperative quality of recovery scale (PQRS) questionnaire [23]. The PQRS was completed on the day of admission (baseline) and before discharge (approximately 1 week after surgery), and again 1 month following surgery by telephone contact. The PQRS data were reported as the proportion of patients recovered at each time-point (baseline, first postoperative week, first postoperative month). We focused on non-physiological recovery domains (nociceptive, cognitive, activities of daily living (ADL), emotive) and overall patient satisfaction. The PQRS questionnaires were conducted face-to-face during hospital stay, and by telephone after hospital discharge. Detailed information around how to use the test and how different domains are being assessed is provided on the PQRS website ( topqrs. com/). When planning our study, we analysed our hospital database for more than 2000 cardiac surgical procedures carried out in the year 2014, and found that mean (SD) hospital stay was 10 (3) days in patients with the same risk factors. We expected high-flow nasal oxygen to reduce mean length of stay by 2 days (a 20% relative reduction) to 8 days; data from our trial in thoracic surgery patients showed a 35% reduction in length of stay, so we proposed that 20% was both feasible and clinically significant. Sample size calculation demonstrated that 92 patients (46 per group) would provide 90% power to detect a mean difference of 2 days in hospital length of stay. The required sample size was increased to 100 patients (50 per group) to allow for a 5% loss to follow-up and drop-outs. Baseline data were described using frequencies and percentages for categorical variables and either mean and SD or median, IQR and range for continuous variables. Total hospital stay was calculated for all patients who were discharged alive. As total hopsital length of stay was positively skewed, comparisons between groups were made using the Wilcoxon Rank Sum test and the ratio of geometric means. A risk ratio (RR) was used to compare prolonged stay (defined as total hospital stay > 10 days) in the two groups. Intensive care re-admission and death were compared using Fisher s exact test, and 6MWT and pulmonary function tests were compared using linear regression. Recovery profiles were compared using Chi-squared tests and multi-level mixed-effect logistic regression. All analyses were by intention-to-treat and were performed using Stata version 15.1 (StataCorp Stata Statistical Software: Release 15. College Station, TX: StataCorp LLC) software and a p value < 0.05 was considered statistically significant. Results One hundred patients were enrolled in the study, 51 patients were allocated to receive high-flow nasal oxygen and 49 to receive standard oxygen therapy. Of these, six patients were not included in the final analysis due to protocol violation (two patients in each group were not extubated by 10:00 on the morning after surgery), surgery being cancelled (one patient in the standard oxygen group) and withdrawal of consent (one patient in the standard oxygen group) (Fig. 1). All other randomly allocated patients were included in the intention-to-treat analysis. Baseline and clinical characteristics (including logistic EuroScore) are shown in Table 1. Study end-points are reported in Table 2. Median (IQR [range]) hospital length of stay was 7 (6 9 [4 30]) and 9 (7 16 [4 120]) days in the high-flow nasal oxygen group and the standard oxygen group, respectively, p = The geometric mean hospital length of stay was 29% lower in the high-flow nasal oxygen group (95%CI: 11 44%), p = A sensitivity analysis removing the single outlying value (120 days) from the standard oxygen group did not materially alter the conclusions (Figure 2). The risk of prolonged stay was 18.7% in the high-flow nasal oxygen group compared with 38.6% in the standard oxygen group (RR 0.49, 95%CI: ), p = There was no difference in ICU length of stay (p = 0.949) with the median (IQR [range]) being 1 (1 2 [1 15]) and 1 (1 2 [1 23]) in the high-flow nasal oxygen group and standard oxygen group, respectively. Patients in the high-flow nasal oxygen group had fewer ICU re-admissions (1/49 vs. 7/45; p = 0.026). There was one death in each group. Less than half of the patients enrolled performed a postoperative 6MWT. The mean (SD) distance was (98.9) m in the high-flow nasal oxygen group compared with (114.9) m in the standard oxygen group; mean difference was 21.3 m (95%CI: 44.0 to 86.6), p = Postoperative pulmonary function tests were performed in two-thirds of the patients. There was no significant difference between the two groups in terms of FEV 1 and FVC. The number of patients requiring escalation of respiratory support (unplanned CPAP, non-invasive or invasive ventilation) was three (6.1%) in the high-flow nasal oxygen group compared with six (13.3%) in the standard oxygen group (p = 0.190). One patient (in the standard oxygen group) required a 2018 The Authors. Anaesthesia published by John Wiley & Sons Ltd on behalf of Association of Anaesthetists. 1481
5 Zochios et al. High-flow nasal oxygen in high-risk cardiac surgical patients Enrolment Pa ents undergoing coronary artery bypass gra ing, valve surgery or both were assessed for eligibility (n = 1714) Excluded (n = 1614) Not mee ng inclusion criteria (n = 1187) Declined to par cipate (n = 69) Failed to consent (n = 8) Withdrew from study before randomisa on (n = 1) Study team not available (n = 349) Randomised (n = 100) Alloca on High-flow nasal oxygen group (n = 51) Standard oxygen group (n = 49) Procedure cancelled (n =1) Follow-Up Delayed extuba on (n = 2) Delayed extuba on (n = 2) Withdrew consent (n = 1) Included in analysis for primary outcome (n = 49) Analysis Included in analysis for primary outcome (n = 45) Figure 1 Study flow (CONSORT) chart showing patients allocated to either high-flow nasal oxygen or standard oxygen therapy. tracheostomy to aid weaning from mechanical ventilation. Four patients in the standard oxygen group crossed over and received high-flow nasal oxygen after 24 h (two patients required high-flow nasal oxygen for 48 h and the other two for 72 h). There were no significant between-group differences in extra-pulmonary postoperative complications (Table 3). The recovery profiles for each PQRS domain are summarised in Table 4. The differences in patient-reported outcomes between the two groups were not statistically significant. Discussion In this study, we randomly assigned patients undergoing cardiac surgery and at high risk for postoperative The Authors. Anaesthesia published by John Wiley & Sons Ltd on behalf of Association of Anaesthetists.
6 Zochios et al. High-flow nasal oxygen in high-risk cardiac surgical patients Table 1 Baseline characteristics of patients receiving high-flow nasal oxygen or standard oxygen therapy. Values are mean (SD), number (proportion) or median (IQR [range]). High-flow nasal oxygen group Standard oxygen group n = 49 n = 45 Age; y 67.3 (9.3) 69.1 (11.1) Sex; female 19 (38.8%) 17 (37.8%) Comorbidities a COPD b 14 (28.6%) 15 (33.3%) Asthma b 18 (36.7%) 19 (42.2%) Smoker 10 (20.4%) 10 (22.2%) BMI 35 kg.m 2 13 (26.5%) 12 (26.7%) Recent LRTI c 0 0 BMI; kg.m 2 32 (5.5) 30.2 (6.6) Pre-operative Hb; g.l ( [ ]) 131 ( [85 166]) Pre-operative creatinine; lmol.l 1 80 (71 90 [52 141]) 83 (74 96 [38 180]) Logistic EUROScore d 4(3 7 [1 30]) 4 (3 10 [1 26]) Six-minute walk test; m ( [ ]) ( [ ]) FEV 1 ; l 2.3 ( [ ]) 2.0 ( [ ]) FEV 1 ; % of predicted value 87 ( [41 127]) 81 (68 89 [42 147]) FVC; l 3.3 ( [ ]) 3.0 ( [ ]) FVC; % of predicted value 89 ( [49 138]) 92 ( [41 169]) Procedure CABG 17 (34.7%) 14 (31.1%) Valve(s) 24 (49.0%) 18 (40.0%) CABG + Valve(s) 8 (16.3%) 13 (28.9%) Surgery time; min 197 ( [ ]) 202 ( [55 470]) BMI, body mass index; CABG, coronary artery bypass graft; COPD, chronic obstructive pulmonary disease; EuroScore, European System for Cardiac Operative Risk Evaluation; Hb, haemoglobin; FEV 1, forced expiratory volume in one second; FVC, forced vital capacity. a More than one pathology may be present in each patient. b Only patients with a formal COPD or asthma diagnosis (as defined by British Thoracic Society and National Institute for Health and Care Excellence) on inhaled therapy were enrolled [18, 19]. c LRTI was defined according to National Institute for Health and Care Excellence as an acute illness, usually with cough as the main symptom, and with at least one other lower respiratory tract symptom (such as fever, sputum production, breathlessness, wheeze or chest discomfort or pain) and no alternative explanation [20]. d Logistic EUROSCORE is a risk model which allows prediction of mortality after cardiac surgery. It includes 17 factors (patient-, cardiac- and operation related) and uses logistic regression to calculate mortality risk. pulmonary complications to receive either high-flow nasal oxygen or standard oxygen therapy following tracheal extubation. This is the first randomised controlled trial examining the effect of prophylactic use of high-flow nasal oxygen on clinical outcomes in cardiac surgical patients with significant risk factors for peri-operative pulmonary complications. We demonstrated that highflow nasal oxygen use resulted in a statistically significant reduction in hospital length of stay and fewer re-admissions to ICU. There were no significant between-group differences in other secondary outcomes. Airflow limitation strongly predicts increased hospital stay and in-hospital mortality after cardiac surgery [24]. The beneficial effect of high-flow nasal oxygen after cardiac surgery and reduction in hospital stay in our study cohort could potentially be explained by the following mechanisms: washout of nasopharyngeal dead space; reduced work of breathing; improved respiratory mechanics; and generation of low-level PEEP [25 27]. The warmed and humidified oxygen facilitates optimum function of the airway mucosa and mucociliary clearance, and inhibits bronchomotor response, thus preventing bronchospasm and increases in airway resistance [28, 29]. It has been shown that high-flow nasal oxygen reduces dead space ventilation in a flow- and time-dependent manner, leading to a reduction in 2018 The Authors. Anaesthesia published by John Wiley & Sons Ltd on behalf of Association of Anaesthetists. 1483
7 Zochios et al. High-flow nasal oxygen in high-risk cardiac surgical patients Table 2 Study end-points for patients randomly allocated to either the high-flow nasal oxygen group or standard oxygen group. Values are median (IQR [range]) or number (proportion). High-flow nasal oxygen group Standard oxygen group n = 49 n = 45 Total length of stay; days 7 (6 9 [4 30]) 9 (7 16 [4 120]) ICU length of stay; days 1 (1 2 [1 15]) 1 (1 2 [1 23]) Re-admission to ICU 1 (2.0%) 7 (15.6%) Six-minute walk test; m 214 ( [40 380]) 165 ( [60 510]) Lung function FVC; l 1.9 ( [ ]) 1.9 ( [ ]) FVC; % of predicted value 57 (45 66 [31 102]) 57 (47 69 [34 123]) FEV 1 ; l 1.5 ( [ ]) 1.2 ( [ ]) FEV 1 ; % of predicted value 54 (42 64 [29 81]) 53 (39 65 [18 83]) ICU, intensive care unit; FEV 1, forced expiratory volume in one second; FVC, forced vital capacity. p value Length of stay (days) HFNO Standard oxygen Figure 2 Box plot showing hospital length of stay in cardiac surgical patients allocated to either high-flow nasal oxygen (HFNO) or standard oxygen therapy. The horizontal line is the median value, the box is the interquartile range and the whiskers extend out to the adjacent values. Outliers are plotted individually as open circles. rebreathing, more effective alveolar ventilation and decreased work of breathing [26]. Furthermore, high-flow nasal oxygen provides PEEP of 3 5 cmh 2 O at flows of l.min 1 which could potentially reduce postoperative atelectasis [15]. Prevention of postoperative hypoxaemia and hypercapnia, together with improved pulmonary mechanics, not only reduces pulmonary morbidity but may also improve cardiac function by reducing myocardial oxygen demand and the adverse effects of impaired gas exchange on pulmonary vasculature. These mechanisms could explain the beneficial effect of prophylactic high-flow nasal oxygen use in the immediate postoperative period. We would, therefore, expect an improvement in postoperative pulmonary function and Table 3 Extra-pulmonary complications in patients allocated to either high-flow nasal oxygen or standard oxygen therapy. High-flow nasal oxygen group Standard oxygen group n = 51 n = 49 p value Return to operating theatre Atrial fibrillation Pacemaker insertion Renal replacement therapy Sternal wound infection Delirium MWT which we were unable to demonstrate. A possible explanation for these results could be that the study was not powered to compare those secondary outcomes, or that patients had limited physiological reserve due to chronic lung disease (COPD, asthma), recent sternotomy and major surgery. In the non-cardiac surgery setting, high-flow nasal oxygen is increasingly being used as a first-line therapy in acute respiratory failure. This strategy is supported by data from well-designed and adequately powered trials showing that high-flow nasal oxygen application reduces tracheal re-intubation rate in low-risk patients [30] when compared with conventional oxygen therapy, confers survival benefit [31] and results in a lower tracheal re-intubation rate [32] in patients with, or at risk of, non-hypercapnic hypoxaemic respiratory failure. However, a recent systematic review of 11 randomised The Authors. Anaesthesia published by John Wiley & Sons Ltd on behalf of Association of Anaesthetists.
8 Zochios et al. High-flow nasal oxygen in high-risk cardiac surgical patients Table 4 Patient-reported outcomes from patients randomly allocated to high-flow nasal oxygen or standard oxygen therapy. Values are proportion recovery from baseline. Domain Time High-flow nasal oxygen (%) Standard oxygen (%) p value e p value f Nociceptive a 5 days month Emotional b 5 days month ADL c 5 days month Cognitive 5 days month Satisfaction d 5 days month a Nociception, pain and nausea. b Emotional, anxiety and depression. c ADL, activities of daily living (eat, walk, stand, dress). d Satisfaction, overall satisfaction with anaesthetic care, reported as satisfied or very satisfied. e p value for comparison at each visit. f p value for comparison over both follow-up visits. trials (n = 1972) examining the safety and efficacy of high-flow nasal oxygen in general ICU patients requiring respiratory support found insufficient evidence to determine superiority of high-flow nasal oxygen in the ICU setting [33]. In a pragmatic randomised controlled trial, Parke et al. demonstrated that high-flow nasal oxygen did not improve outcomes as assessed by oxygen saturation to fraction of inspired oxygen (S p O 2 /F I O 2 ) ratio after cardiac surgery, but did reduce the requirement for escalation of respiratory support [34]. In a recent randomised controlled trial, Corley et al. compared prophylactic tracheal extubation followed by high-flow nasal oxygen for 8 h with standard care post-cardiac surgery in obese patients (BMI 30 kg.m 2 ) [35]. Primary outcome was atelectasis on postoperative chest radiograph. Prophylactic tracheal extubation followed by high-flow nasal oxygen did not lead to improvements in respiratory function or a statistically significant difference in ICU stay. The limited high-flow nasal oxygen exposure time (8 h) in the Corley trial and use of surrogate (SpO 2 /F I O 2 ratio and atelectasis score) markers, rather than patient-oriented primary outcomes (which would have required a much larger sample size), were the main limitations of these studies. Furthermore, reporting non-validated surrogate primary outcomes is more likely to result in overestimation of treatment effect and uncertainty in predicting treatment benefit [36]. We selected hospital stay as the primary outcome because it is more relevant to patients and healthcare providers than physiological parameters such as oxygenation or haemodynamic data. Length of stay integrates postoperative pulmonary and extra-pulmonary complications, and speed of postoperative recovery. It is, therefore, a non-mortality patient-centred outcome which reflects quality and value-based healthcare delivery [37, 38]. A recent meta-analysis which included the aforementioned two randomised trials only, examined the efficacy and safety of high-flow nasal oxygen after cardiac surgery compared with conventional oxygen therapy and found that post-extubation application of high-flow nasal oxygen was associated with a significant reduction in escalation of respiratory support (RR, 0.61; 95%CI, ; z = 3.32, p < 0.001) [39]. However, due to the small number of studies analysed, the methods utilised to detect publication bias were underpowered. In addition, the definitions, strategies and criteria for escalation of respiratory support in the studies included in the meta-analysis were non-specific, making the validity of the results questionable. The differences in escalation of respiratory support (unplanned CPAP, non-invasive or invasive ventilation) between the high-flow nasal oxygen group and the standard oxygen group in our study cohort were non-significant. In a large (n = 830) non-inferiority multi-centre randomised trial, high-flow nasal oxygen was compared with BiPAP in patients with, or at risk of, respiratory failure after cardiothoracic surgery [40]. The primary outcome in this study was treatment failure, which was defined as a composite of tracheal re-intubation, switch 2018 The Authors. Anaesthesia published by John Wiley & Sons Ltd on behalf of Association of Anaesthetists. 1485
9 Zochios et al. High-flow nasal oxygen in high-risk cardiac surgical patients to the other study therapy or early discontinuation of the assigned therapy, and the authors concluded that highflow nasal oxygen was not inferior to BiPAP. The control group in this study does not necessarily represent the standard of care or best practice because there are no robust data indicating that BiPAP improves outcomes in the cardiac surgery setting. In addition, by using a composite primary outcome, the effect may be small for important individual components (e.g. tracheal re-intubation rate) and large for less important clinical components (e.g. crossover to another treatment group), limiting the generalisability of the results [41]. A recent post-hoc analysis in the subset of obese (BMI > 30 kg.m 2 ) patients from the same randomised controlled trial showed that continuous application of high-flow nasal oxygen compared with intermittent BiPAP in patients with or without respiratory failure did not lead to a higher rate of treatment failure [42]. The use of BiPAP was associated with improved oxygenation indices; however this did not translate into improved clinical outcomes. None of the high-flow nasal oxygen studies previously undertaken in the cardiac surgery setting were powered to detect differences in clinically important primary outcomes such as mortality or length of stay. No study exclusively investigated the effect of high-flow nasal oxygen on outcomes in patients at significantly higher risk of postoperative pulmonary dysfunction, such as patients with pre-existing pulmonary disease. Two studies focused on obese patients who are at higher risk of postoperative pulmonary complications, but methodological flaws relating to their non-inferiority design and post-hoc analysis diminish the validity of their results [40, 42]. Our trial has several limitations. Firstly, there is potential bias due to a lack of blinding of the patients and healthcare providers in the immediate postoperative period due to the obvious differences between the study interventions. Secondly, our study was underpowered for some of the secondary outcomes, for example, 6MWT and patient-reported outcomes, and the composite of postoperative complications. Although we did not discern significant between-group differences in patientreported outcomes, we highlight the importance of reporting recovery profiles as they reflect value-based care and provide potentially useful information in order to adequately power future studies. Thirdly, the single centre status of our study and potentially associated large intervention effect may not be directly transferable to other settings [43]. In conclusion, when compared with standard care, prophylactic postoperative use of high-flow nasal oxygen in cardiac surgical patients at high risk for postoperative respiratory complications reduced hospital length of stay and re-admissions to ICU. This has implications for reduced healthcare costs and potentially morbidity. We recommend routine use of high-flow nasal oxygen after tracheal extubation in this cohort of patients and further testing of our hypothesis in large multi-centre randomised trials. Acknowledgements The authors thank F.E. Botrill HNC (clinical trials co-ordinator) for her contribution in helping with study design, patient recruitment and site training, W. Lawson-Brown and T. Kriz (research fellow) who assisted with patient recruitment and data collection, and J. Hernandez-Sanchez (statistician) for his advice and guidance on sample size calculation. This trial was registered at clinicaltrials.gov (NCT ). The trial was funded by the Association of Anaesthetists of Great Britain and Ireland via a grant awarded by the National Institute of Academic Anaesthesia, and was approved by the UK National Institute of Health Research (NIHR) for portfolio status, and Royal Papworth Hospital acknowledges the support of the NIHR Clinical Research Network. Fisher and Paykel provided equipment and disposables, but were not involved with data collection or analysis, writing the manuscript or the decision to submit the manuscript for publication. AK has received educational grant funding, honoraria or assistance with travel from CSL Behring, Massimo, Pharmacosmos, Fisher and Paykel, Brightwake Ltd and Vifor Pharma. AK is the Editor-in-Chief of Anaesthesia. No other external funding or competing interests declared. References 1. Pasquina P, Merlani P, Granier JM, Ricou B. Continuous positive airway pressure versus noninvasive pressure support ventilation to treat atelectasis after cardiac surgery. Anesthesia and Analgesia 2004; 99: Wynne R, Botti M. Postoperative pulmonary dysfunction in adults after cardiac surgery with cardiopulmonary bypass: clinical significance and implications for practice. American Journal of Critical Care 2004; 13: Taggart DP, El-Fiky M, Carter R, Bowman A, Wheatley DJ. Respiratory dysfunction after uncomplicated cardio-pulmonary bypass. Annals of Thoracic Surgery 1993; 56: Weissman C. Pulmonary complications after cardiac surgery. Seminars in Cardiothoracic and Vascular Anesthesia 2004; 8: Adabag AS, Wassif HS, Rice K, et al. Preoperative pulmonary function and mortality after cardiac surgery. American Heart Journal 2010; 159: Leavitt BJ, Ross CS, Spence B, et al. Long-term survival of patients with chronic obstructive pulmonary disease The Authors. Anaesthesia published by John Wiley & Sons Ltd on behalf of Association of Anaesthetists.
10 Zochios et al. High-flow nasal oxygen in high-risk cardiac surgical patients undergoing coronary artery bypass surgery. Circulation 2006; 114: I Manganas H, Lacasse Y, Bourgeois S, Perron J, Dagenais F, Maltais F. Postoperative outcome after coronary artery bypass grafting in chronic obstructive pulmonary disease. Canadian Respiratory Journal 2007; 14: Duggan M, Kavanagh BP. Pulmonary atelectasis: a pathogenic perioperative entity. Anesthesiology 2005; 102: Lumb AB, Greenhill SJ, Simpson MP, Stewart J. Lung recruitment and positive airway pressure before extubation does not improve oxygenation in the post-anaesthesia care unit: a randomized clinical trial. British Journal of Anaesthesia 2010; 104: Zarbock A, Mueller E, Netzer S, Gabriel A, Feindt P, Kindgen-Milles D. Prophylactic nasal continuous positive airway pressure following cardiac surgery protects from postoperative pulmonary complications: a prospective, randomized, controlled trial in 500 patients. Chest 2009; 135: Kindgen-Milles D, M uller E, Buhl R, et al. Nasal-continuous positive airway pressure reduces pulmonary morbidity and length of hospital stay following thoracoabdominal aortic surgery. Chest 2005; 128: Westerlind A, Nilsson F, Ricksten SE. The use of continuous positive airway pressure by face mask and thoracic epidural analgesia after lung transplantation. Gothenburg Lung Transplant Group. Journal of Cardiothoracic and Vascular Anesthesia 1999; 13: Cuquemelle E, Lellouche F. Assessment of humidification performance: still no easy method!. Respiratory Care 2013; 58: Frizzola M, Miller TL, Rodriguez ME, et al. High-flow nasal cannula: impact on oxygenation and ventilation in an acute lung injury model. Pediatric Pulmonology 2011; 46: Parke R, McGuinness S, Eccleston M. Nasal high-flow therapy delivers low level positive airway pressure. British Journal of Anaesthesia 2009; 103: Parke RL, Eccleston ML, McGuinness SP. The effects of flow on airway pressure during nasal high-flow oxygen therapy. Respiratory Care 2011; 56: Manley BJ, Owen LS, Doyle LW, et al. High-flow nasal cannulae in very preterm infants after extubation. New England Journal of Medicine 2013; 369: National Institute for Health and Care Excellence. Chronic obstructive pulmonary disease in over 16s: diagnosis and management. NICE guideline [CG101] nice.org.uk/guidance/cg101/chapter/1-guidance#diagnos ingcopd (accessed 12/12/2017). 19. British Thoracic Society and Scottish Intercollegiate Guidelines Network. British guideline on the management of asthma. A national clinical guideline. London: British Thoracic Society, p22. document-library/clinical-information/asthma/btssignasthma-guideline-2014/ (accessed 25/07/2015). 20. National Institute for Health and Care Excellence. Pneumonia in adults: diagnosis and management. NICE guideline [CG191] (accessed 25/07/2015). 21. Copsfcpfl ATS. ATS statement: guidelines for the six-minute walk test. American Journal of Respiratory and Critical Care Medicine 2002; 166: O Driscoll BR, Howard LS, Davison AG. BTS guideline for emergency oxygen use in adult patients. Thorax 2008;63 Suppl 6: vi Royse CF, Newman S, Chung F, et al. Development and feasibility of a scale to assess postoperative recovery: the post-operative quality recovery scale. Anesthesiology 2010; 113: McAllister DA, Wild SH, MacLay JD, et al. Forced expiratory volume in one second predicts length of stay and in-hospital mortality in patients undergoing cardiac surgery: a retrospective cohort study. PLoS ONE 2013; 8: e Dysart K, Miller TL, Wolfson MR, Shaffer TH. Research in high flow therapy: mechanisms of action. Respiratory Medicine 2009; 103: M oller W, Feng S, Domanski U, et al. Nasal high flow reduces dead space. Journal of Applied Physiology 2017; 122: Delorme M, Bouchard PA, Simon M, Simard S, Lellouche F. Effects of high-flow nasal cannula on the work of breathing in patients recovering from acute respiratory failure. Critical Care Medicine 2017; 45: Williams R, Rankin N, Smith T, Galler D, Seakins P. Relationship between the humidity and temperature of inspired gas and the function of the airway mucosa. Critical Care Medicine 1996; 24: Fontanari P, Zattara-Hartmann MC, Burnet H, Jammes Y. Nasal eupnoeic inhalation of cold, dry air increases airway resistance in asthmatic patients. European Respiratory Journal 1997; 10: Hernandez G, Vaquero C, Gonzalez P, et al. Effect of postextubation high-flow nasal cannula vs conventional oxygen therapy on reintubation in low-risk patients: a randomized clinical trial. Journal of the American Medical Association 2016; 315: Frat JP, Thille AW, Mercat A, et al. High-flow oxygen through nasal cannula in acute hypoxemic respiratory failure. New England Journal of Medicine 2015; 372: Maggiore SM, Idone FA, Vaschetto R, et al. Nasal high-flow versus Venturi mask oxygen therapy after extubation. Effects on oxygenation, comfort, and clinical outcome. American Journal of Respiratory and Critical Care Medicine 2014; 190: Corley A, Rickard CM, Aitken LM, et al. High-flow nasal cannulae for respiratory support in adult intensive care patients. Cochrane Database of Systematic Reviews 2017; 5: CD Parke R, McGuinness S, Dixon R, Jull A. Open-label, phase II study of routine high-flow nasal oxygen therapy in cardiac surgical patients. British Journal of Anaesthesia 2013; 111: Corley A, Bull T, Spooner AJ, Barnett AG, Fraser JF. Direct extubation onto high-flow nasal cannulae post-cardiac surgery versus standard treatment in patients with a BMI 30: a randomised controlled trial. Intensive Care Medicine 2015; 41: Ciani O, Buyse M, Garside R, et al. Comparison of treatment effect sizes associated with surrogate and final patient relevant outcomes in randomised controlled trials: meta-epidemiological study. British Medical Journal 2013; 346: f Myles PS, Shulman MA, Heritier S, et al. Validation of days at home as an outcome measure after surgery: a prospective cohort study in Australia. British Medical Journal Open 2017; 7: e Hyder JA, Hirschberg RE, Nguyen LL. Home discharge as a performance metric for surgery. The Journal of the American Medical Association Surgery 2015; 150: Zhu Y, Yin H, Zhang R, Wei J. High-flow nasal cannula oxygen therapy vs conventional oxygen therapy in cardiac 2018 The Authors. Anaesthesia published by John Wiley & Sons Ltd on behalf of Association of Anaesthetists. 1487
11 Zochios et al. High-flow nasal oxygen in high-risk cardiac surgical patients surgical patients: a meta-analysis. Journal of Critical Care 2017; 38: Stephan F, Barrucand B, Petit P, et al. High-flow nasal oxygen vs noninvasive positive airway pressure in hypoxemic patients after cardiothoracic surgery: a randomized clinical trial. Journal of the American Medical Association 2015; 313: Del Sorbo L, Ferguson ND. High-flow nasal cannulae or noninvasive ventilation for management of postoperative respiratory failure. The Journal of the American Medical Association 2015; 313: Stephan F, Berard L, Rezaiguia-Delclaux S, Amaru P, BiPOP SG. High-flow nasal cannula therapy versus intermittent noninvasive ventilation in obese subjects after cardiothoracic surgery. Respiratory Care 2017; 62: Bafeta A, Dechartres A, Trinquart L, Yavchitz A, Boutron I, Ravaud P. Impact of single centre status on estimates of intervention effects in trials with continuous outcomes: metaepidemiological study. British Medical Journal 2012; 344: e The Authors. Anaesthesia published by John Wiley & Sons Ltd on behalf of Association of Anaesthetists.
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. This online publication has been corrected. The corrected
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. This online publication has been corrected. The corrected
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
FEV1 predicts length of stay and in-hospital mortality in patients undergoing cardiac surgery
 EUROPEAN SOCIETY OF CARDIOLOGY CONGRESS 2010 FEV1 predicts length of stay and in-hospital mortality in patients undergoing cardiac surgery Nicholas L Mills, David A McAllister, Sarah Wild, John D MacLay,
EUROPEAN SOCIETY OF CARDIOLOGY CONGRESS 2010 FEV1 predicts length of stay and in-hospital mortality in patients undergoing cardiac surgery Nicholas L Mills, David A McAllister, Sarah Wild, John D MacLay,
PRESSURES DELIVERED BY NASAL HIGH FLOW THERAPY DURING
 PRESSURES DELIVERED BY NASAL HIGH FLOW THERAPY DURING ALL PHASES OF THE RESPIRATORY CYCLE Rachael L. Parke, RN, MHSc (Hons) Cardiothoracic and Vascular Intensive Care Unit Auckland City Hospital Private
PRESSURES DELIVERED BY NASAL HIGH FLOW THERAPY DURING ALL PHASES OF THE RESPIRATORY CYCLE Rachael L. Parke, RN, MHSc (Hons) Cardiothoracic and Vascular Intensive Care Unit Auckland City Hospital Private
High Flow Humidification Therapy, Updates.
 High Flow Humidification Therapy, Updates. Bernardo Selim, M.D. I have no relevant financial relationships to disclose. Assistant Professor, Pulmonary, Critical Care and Sleep Medicine, Mayo Clinic What
High Flow Humidification Therapy, Updates. Bernardo Selim, M.D. I have no relevant financial relationships to disclose. Assistant Professor, Pulmonary, Critical Care and Sleep Medicine, Mayo Clinic What
NON-INVASIVE VENTILATION. Lijun Ding 23 Jan 2018
 NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
What you need to know about: High flow nasal oxygen therapy
 What you need to know about: High flow nasal oxygen therapy Main introduction Adequate oxygenation is essential in many disorders, and this article will discuss the physiology, practicalities and indications
What you need to know about: High flow nasal oxygen therapy Main introduction Adequate oxygenation is essential in many disorders, and this article will discuss the physiology, practicalities and indications
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
High Flow Oxygen Therapy in Acute Respiratory Failure. Laurent Brochard Toronto
 High Flow Oxygen Therapy in Acute Respiratory Failure Laurent Brochard Toronto Conflicts of interest Our clinical research laboratory has received research grants for clinical research projects from the
High Flow Oxygen Therapy in Acute Respiratory Failure Laurent Brochard Toronto Conflicts of interest Our clinical research laboratory has received research grants for clinical research projects from the
Nasal High Flow Humidification with or without Oxygen for COPD Management. Shereen Bailey, RCP, RRT, NPS
 Nasal High Flow Humidification with or without Oxygen for COPD Management Shereen Bailey, RCP, RRT, NPS Objectives How it works COPD Management today The role of NHFC Evidence Research/Case Studies Types
Nasal High Flow Humidification with or without Oxygen for COPD Management Shereen Bailey, RCP, RRT, NPS Objectives How it works COPD Management today The role of NHFC Evidence Research/Case Studies Types
Keeping Patients Off the Vent: Bilevel, HFNC, Neither?
 Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION
 SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
Emergency Medicine High Velocity Nasal Insufflation (Hi-VNI) VAPOTHERM POCKET GUIDE
 Emergency Medicine High Velocity Nasal Insufflation (Hi-VNI) VAPOTHERM POCKET GUIDE Indications for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) administration, the patient should be: Spontaneously
Emergency Medicine High Velocity Nasal Insufflation (Hi-VNI) VAPOTHERM POCKET GUIDE Indications for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) administration, the patient should be: Spontaneously
Fariba Rezaeetalab Associate Professor,Pulmonologist
 Fariba Rezaeetalab Associate Professor,Pulmonologist rezaitalabf@mums.ac.ir Patient related risk factors Procedure related risk factors Preoperative risk assessment Risk reduction strategies Age Obesity
Fariba Rezaeetalab Associate Professor,Pulmonologist rezaitalabf@mums.ac.ir Patient related risk factors Procedure related risk factors Preoperative risk assessment Risk reduction strategies Age Obesity
Perioperative Pulmonary Management. Objectives
 Citywide Resident Perioperative Medical Consult Conference Perioperative Pulmonary Management Frank Jacono, MD May 5, 2017 Objectives Definition of post-operative pulmonary complications (PPC) Risk factors
Citywide Resident Perioperative Medical Consult Conference Perioperative Pulmonary Management Frank Jacono, MD May 5, 2017 Objectives Definition of post-operative pulmonary complications (PPC) Risk factors
Commissioning for Better Outcomes in COPD
 Commissioning for Better Outcomes in COPD Dr Matt Kearney Primary Care & Public Health Advisor Respiratory Programme, Department of Health General Practitioner, Runcorn November 2011 What are the Commissioning
Commissioning for Better Outcomes in COPD Dr Matt Kearney Primary Care & Public Health Advisor Respiratory Programme, Department of Health General Practitioner, Runcorn November 2011 What are the Commissioning
Acute Paediatric Respiratory Pathway
 Guideline for the use of high Flow Nasal Cannula Oxygen Therapy (Optiflow or Airvo) in Children with Bronchiolitis or an acute respiratory illness Introduction: High flow nasal cannula (HFNC) oxygen enables
Guideline for the use of high Flow Nasal Cannula Oxygen Therapy (Optiflow or Airvo) in Children with Bronchiolitis or an acute respiratory illness Introduction: High flow nasal cannula (HFNC) oxygen enables
Chronic Obstructive Pulmonary Disease (COPD) Measures Document
 Chronic Obstructive Pulmonary Disease (COPD) Measures Document COPD Version: 3 - covering patients discharged between 01/10/2017 and present. Programme Lead: Jo Higgins Clinical Lead: Dr Paul Albert Number
Chronic Obstructive Pulmonary Disease (COPD) Measures Document COPD Version: 3 - covering patients discharged between 01/10/2017 and present. Programme Lead: Jo Higgins Clinical Lead: Dr Paul Albert Number
Sleep Apnea and ifficulty in Extubation. Jean Louis BOURGAIN May 15, 2016
 Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity
 NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Use of NIV 1998-2010 50 45 40 35 30 25 20 15 10 5 0 1998
NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Use of NIV 1998-2010 50 45 40 35 30 25 20 15 10 5 0 1998
BTS Guideline for Home Oxygen use in adults Appendix 9 (online only) Key Questions - PICO 10 December 2012
 BTS Guideline for Home Oxygen use in adults Appendix 9 (online only) Key Questions - PICO 10 December 2012 Evidence base for Home Oxygen therapy in COPD, non-copd respiratory disease and nonrespiratory
BTS Guideline for Home Oxygen use in adults Appendix 9 (online only) Key Questions - PICO 10 December 2012 Evidence base for Home Oxygen therapy in COPD, non-copd respiratory disease and nonrespiratory
High-flow nasal cannula use in a paediatric intensive care unit over 3 years
 High-flow nasal cannula use in a paediatric intensive care unit over 3 years Tracey I Wraight and Subodh S Ganu Respiratory illness and/or distress is the commonest reason for non-elective paediatric intensive
High-flow nasal cannula use in a paediatric intensive care unit over 3 years Tracey I Wraight and Subodh S Ganu Respiratory illness and/or distress is the commonest reason for non-elective paediatric intensive
Charisma High-flow CPAP solution
 Charisma High-flow CPAP solution Homecare PNEUMOLOGY Neonatology Anaesthesia INTENSIVE CARE VENTILATION Sleep Diagnostics Service Patient Support charisma High-flow CPAP solution Evidence CPAP therapy
Charisma High-flow CPAP solution Homecare PNEUMOLOGY Neonatology Anaesthesia INTENSIVE CARE VENTILATION Sleep Diagnostics Service Patient Support charisma High-flow CPAP solution Evidence CPAP therapy
Trial protocol - NIVAS Study
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
OXYGEN USE IN PHYSICAL THERAPY PRACTICE. Rebecca H. Crouch, PT,DPT,MS,CCS,FAACVPR
 OXYGEN USE IN PHYSICAL THERAPY PRACTICE Rebecca H. Crouch, PT,DPT,MS,CCS,FAACVPR Supplemental Oxygen Advantages British Medical Research Council Clinical Trial Improved survival using oxygen 15 hrs/day
OXYGEN USE IN PHYSICAL THERAPY PRACTICE Rebecca H. Crouch, PT,DPT,MS,CCS,FAACVPR Supplemental Oxygen Advantages British Medical Research Council Clinical Trial Improved survival using oxygen 15 hrs/day
Oxygen: Is there a problem? Tom Heaps Acute Physician
 Oxygen: Is there a problem? Tom Heaps Acute Physician Case 1 79-year-old female, diabetic, morbidly obese Admitted with LVF Overnight Reduced GCS?cause 15l NRB in situ ABG showed ph 6.9, pco 2 15.9kPa
Oxygen: Is there a problem? Tom Heaps Acute Physician Case 1 79-year-old female, diabetic, morbidly obese Admitted with LVF Overnight Reduced GCS?cause 15l NRB in situ ABG showed ph 6.9, pco 2 15.9kPa
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION
 SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date (DD/MMM/YYYY) (DD/MMM/YYYY) Gender Female Male Date of surgery (DD/MMM/YYYY)
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date (DD/MMM/YYYY) (DD/MMM/YYYY) Gender Female Male Date of surgery (DD/MMM/YYYY)
BTS/ICS Guidelines for the ventilatory management of acute hypercapnic respiratory failure in adults
 BTS/ICS Guidelines for the ventilatory management of acute hypercapnic respiratory failure in adults British Thoracic Society Intensive Care Society Introduction Acute Hypercapnic Respiratory Failure (AHRF)
BTS/ICS Guidelines for the ventilatory management of acute hypercapnic respiratory failure in adults British Thoracic Society Intensive Care Society Introduction Acute Hypercapnic Respiratory Failure (AHRF)
Oxygen & High flow nasal Oxygen therapy. Learning points. Why? 18/07/
 Oxygen & High flow nasal Oxygen therapy 13.07.2017 Learning points Update on BTS guidance May 2017 Help you understand the mechanism of action of high flow nasal oxygen therapy Help you think about the
Oxygen & High flow nasal Oxygen therapy 13.07.2017 Learning points Update on BTS guidance May 2017 Help you understand the mechanism of action of high flow nasal oxygen therapy Help you think about the
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Jain S, Kamimoto L, Bramley AM, et al. Hospitalized patients
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Jain S, Kamimoto L, Bramley AM, et al. Hospitalized patients
Web Appendix 1: Literature search strategy. BTS Acute Hypercapnic Respiratory Failure (AHRF) write-up. Sources to be searched for the guidelines;
 Web Appendix 1: Literature search strategy BTS Acute Hypercapnic Respiratory Failure (AHRF) write-up Sources to be searched for the guidelines; Cochrane Database of Systematic Reviews (CDSR) Database of
Web Appendix 1: Literature search strategy BTS Acute Hypercapnic Respiratory Failure (AHRF) write-up Sources to be searched for the guidelines; Cochrane Database of Systematic Reviews (CDSR) Database of
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Acute noninvasive ventilation what s the evidence? Respiratory Medicine Update: Royal College of Physicians & BTS Thu 28 th January 2016
 Acute noninvasive ventilation what s the evidence? Respiratory Medicine Update: Royal College of Physicians & BTS Thu 28 th January 2016 Annabel Nickol Consultant in Respiratory Medicine, Sleep & Ventilation
Acute noninvasive ventilation what s the evidence? Respiratory Medicine Update: Royal College of Physicians & BTS Thu 28 th January 2016 Annabel Nickol Consultant in Respiratory Medicine, Sleep & Ventilation
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Analgesia for chest trauma - RVI
 Analgesia for chest trauma - RVI Northern Network Initial Management Patients with blunt chest trauma will be managed in a standard fashion within the context of the well established trauma systems at
Analgesia for chest trauma - RVI Northern Network Initial Management Patients with blunt chest trauma will be managed in a standard fashion within the context of the well established trauma systems at
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
Acute NIV in COPD and what happens next. Dr Rachael Evans PhD Associate Professor, Respiratory Medicine, Glenfield Hospital
 Acute NIV in COPD and what happens next Dr Rachael Evans PhD Associate Professor, Respiratory Medicine, Glenfield Hospital Content Scenarios Evidence based medicine for the first 24 hrs Who should we refer
Acute NIV in COPD and what happens next Dr Rachael Evans PhD Associate Professor, Respiratory Medicine, Glenfield Hospital Content Scenarios Evidence based medicine for the first 24 hrs Who should we refer
Preoperative Pulmonary Evaluation. Michelle Zetoony, DO, FCCP, FACOI Board Certified Pulmonary, Critical Care, Sleep and Internal Medicine
 Preoperative Pulmonary Evaluation Michelle Zetoony, DO, FCCP, FACOI Board Certified Pulmonary, Critical Care, Sleep and Internal Medicine No disclosures related to this lecture. Objectives Identify pulmonary
Preoperative Pulmonary Evaluation Michelle Zetoony, DO, FCCP, FACOI Board Certified Pulmonary, Critical Care, Sleep and Internal Medicine No disclosures related to this lecture. Objectives Identify pulmonary
Postoperative Respiratory failure( PRF) Dr.Ahmad farooq
 Postoperative Respiratory failure( PRF) Dr.Ahmad farooq Is it really or/only a postoperative issue Multi hit theory first hits second hits Definition Pulmonary gas exchange impairment that presents after
Postoperative Respiratory failure( PRF) Dr.Ahmad farooq Is it really or/only a postoperative issue Multi hit theory first hits second hits Definition Pulmonary gas exchange impairment that presents after
APRV Ventilation Mode
 APRV Ventilation Mode Airway Pressure Release Ventilation A Type of CPAP Continuous Positive Airway Pressure (CPAP) with an intermittent release phase. Patient cycles between two levels of CPAP higher
APRV Ventilation Mode Airway Pressure Release Ventilation A Type of CPAP Continuous Positive Airway Pressure (CPAP) with an intermittent release phase. Patient cycles between two levels of CPAP higher
Assessing perioperative risk
 Assessing perioperative risk Chronic Obstructive Pulmonary Disease Dr. Michelle Caldecott Respiratory & Sleep Physician Epworth Healthcare Austin Health Impact of COPD on Postoperative Outcomes: Results
Assessing perioperative risk Chronic Obstructive Pulmonary Disease Dr. Michelle Caldecott Respiratory & Sleep Physician Epworth Healthcare Austin Health Impact of COPD on Postoperative Outcomes: Results
CPAP Reduces Hypoxemia After Cardiac Surgery (CRHACS Trial). A randomized controlled trial
 CPAP Reduces Hypoxemia After Cardiac Surgery (CRHACS Trial). A randomized controlled trial Backgrounds Postoperative pulmonary complications are most frequent after cardiac surgery and lead to increased
CPAP Reduces Hypoxemia After Cardiac Surgery (CRHACS Trial). A randomized controlled trial Backgrounds Postoperative pulmonary complications are most frequent after cardiac surgery and lead to increased
Effectiveness of nasal highflow in hypercapnic COPD patients is flow and leakage dependent
 Bräunlich et al. BMC Pulmonary Medicine (2018) 18:14 DOI 10.1186/s12890-018-0576-x RESEARCH ARTICLE Open Access Effectiveness of nasal highflow in hypercapnic COPD patients is flow and leakage dependent
Bräunlich et al. BMC Pulmonary Medicine (2018) 18:14 DOI 10.1186/s12890-018-0576-x RESEARCH ARTICLE Open Access Effectiveness of nasal highflow in hypercapnic COPD patients is flow and leakage dependent
Surgery Grand Rounds. Non-invasive Ventilation: A valuable tool. James Cromie, PGY 3 8/24/09
 Surgery Grand Rounds Non-invasive Ventilation: A valuable tool James Cromie, PGY 3 8/24/09 History of mechanical ventilation 1930 s: use of iron lung 1940 s: First NIV system (Bellevue Hospital) 1950 s:
Surgery Grand Rounds Non-invasive Ventilation: A valuable tool James Cromie, PGY 3 8/24/09 History of mechanical ventilation 1930 s: use of iron lung 1940 s: First NIV system (Bellevue Hospital) 1950 s:
Type of intervention Anaesthesia. Economic study type Cost-effectiveness analysis.
 Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
Day care adenotonsillectomy in sleep apnoea
 Day care adenotonsillectomy in sleep apnoea Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Day care adenotonsillectomy in presence of sleep apnoea 1a 2a 2b Contact
Day care adenotonsillectomy in sleep apnoea Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Day care adenotonsillectomy in presence of sleep apnoea 1a 2a 2b Contact
POLICY. Number: Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE. Authorization
 POLICY Number: 7311-60-024 Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE Authorization [ ] President and CEO [ x ] Vice President, Finance and Corporate Services Source:
POLICY Number: 7311-60-024 Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE Authorization [ ] President and CEO [ x ] Vice President, Finance and Corporate Services Source:
IICU Staff Meeting Minutes May 15 and 16, 2013 IICU Conference Room
 IICU Staff Meeting Minutes May 15 and 16, 2013 IICU Conference Room 1) Decreasing Telemetry Alarms Janice Marlett, BSN, RN, Nursing Staff Educator To decrease tele alarms: Properly prep the skin Shave
IICU Staff Meeting Minutes May 15 and 16, 2013 IICU Conference Room 1) Decreasing Telemetry Alarms Janice Marlett, BSN, RN, Nursing Staff Educator To decrease tele alarms: Properly prep the skin Shave
POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO
 POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO MD (ANAESTHESIOLOGY) FINAL EXAMINATION AUGUST 2013 Date : 2 nd August 2013 Time : 1.00 p.m. 4.00 p.m. Answer any three questions. Answer each question
POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO MD (ANAESTHESIOLOGY) FINAL EXAMINATION AUGUST 2013 Date : 2 nd August 2013 Time : 1.00 p.m. 4.00 p.m. Answer any three questions. Answer each question
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit
 Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1).
 PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
IPPB via the Servo I Guidelines for use in UCH Critical Care.
 IPPB via the Servo I Guidelines for use in UCH Critical Care. Version 1.3 Document Control Summary Approved by & date Date of publication Review Date Creator & telephone details Distribution/availability
IPPB via the Servo I Guidelines for use in UCH Critical Care. Version 1.3 Document Control Summary Approved by & date Date of publication Review Date Creator & telephone details Distribution/availability
1.1.2 CPAP therapy is used for patients who are suffering from an acute type 1 respiratory failure (Pa02 <8kPa with a normal or low Pac02).
 Guidelines for initiating and managing CPAP (Continuous Positive Airway Pressure) on a general ward. B25/2006 1.Introduction and Who Guideline applies to 1.1.1 This document provides guidance for Healthcare
Guidelines for initiating and managing CPAP (Continuous Positive Airway Pressure) on a general ward. B25/2006 1.Introduction and Who Guideline applies to 1.1.1 This document provides guidance for Healthcare
Non-invasive Ventilation protocol For COPD
 NHS LANARKSHIRE MONKLANDS HOSPITAL Non-invasive Ventilation protocol For COPD April 2017 S Baird Review Date: Oct 2019 Approved by Medical Directorate Indications for Non-Invasive Ventilation (NIV) NIV
NHS LANARKSHIRE MONKLANDS HOSPITAL Non-invasive Ventilation protocol For COPD April 2017 S Baird Review Date: Oct 2019 Approved by Medical Directorate Indications for Non-Invasive Ventilation (NIV) NIV
EUROANESTHESIA 2008 Copenhagen, Denmark, 31 May - 3 June 2008 THE EVIDENCE BASIS REGARDING POSTOPERATIVE PULMONARY COMPLICATIONS
 EUROANESTHESIA 2008 Copenhagen, Denmark, 31 May - 3 June 2008 THE EVIDENCE BASIS REGARDING POSTOPERATIVE PULMONARY COMPLICATIONS 05RC1 JAUME CANET, VALENTÍN MAZO, ZAHARA BRIONES Department of Anaesthesiology
EUROANESTHESIA 2008 Copenhagen, Denmark, 31 May - 3 June 2008 THE EVIDENCE BASIS REGARDING POSTOPERATIVE PULMONARY COMPLICATIONS 05RC1 JAUME CANET, VALENTÍN MAZO, ZAHARA BRIONES Department of Anaesthesiology
PAEDIATRIC RESPIRATORY FAILURE. Tang Swee Fong Department of Paediatrics University Kebangsaan Malaysia Medical Centre
 PAEDIATRIC RESPIRATORY FAILURE Tang Swee Fong Department of Paediatrics University Kebangsaan Malaysia Medical Centre Outline of lecture Bronchiolitis Bronchopulmonary dysplasia Asthma ARDS Bronchiolitis
PAEDIATRIC RESPIRATORY FAILURE Tang Swee Fong Department of Paediatrics University Kebangsaan Malaysia Medical Centre Outline of lecture Bronchiolitis Bronchopulmonary dysplasia Asthma ARDS Bronchiolitis
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
NI 60. Non-invasive ventilation without compromise. Homecare Pneumology Neonatology Anaesthesia. Sleep Diagnostics Service Patient Support
 NI 60 Non-invasive ventilation without compromise Homecare Pneumology Neonatology Anaesthesia INTENSIVE CARE VENTILATION Sleep Diagnostics Service Patient Support NI 60 Non-invasive ventilation without
NI 60 Non-invasive ventilation without compromise Homecare Pneumology Neonatology Anaesthesia INTENSIVE CARE VENTILATION Sleep Diagnostics Service Patient Support NI 60 Non-invasive ventilation without
BTS Guidelines for Home Oxygen in Children
 ISSN 2040-2023 August 2009 BTS Guidelines for Home Oxygen in Children A Quick Reference Guide British Thoracic Society www.brit-thoracic.org.uk HOME OXYGEN IN CHILDREN BTS GUIDELINES FOR HOME OXYGEN IN
ISSN 2040-2023 August 2009 BTS Guidelines for Home Oxygen in Children A Quick Reference Guide British Thoracic Society www.brit-thoracic.org.uk HOME OXYGEN IN CHILDREN BTS GUIDELINES FOR HOME OXYGEN IN
Introduction. Peripheral arterial disease. Hospital inpatient data - 5,498 FCE (2009/10), & 530 deaths in England alone
 1 Introduction 2 Introduction Peripheral arterial disease Affects 20% adults in Europe and North America In the UK 500-1000/million PAD, 1-2% require amputation LLA 8-15% in people with diabetes with up
1 Introduction 2 Introduction Peripheral arterial disease Affects 20% adults in Europe and North America In the UK 500-1000/million PAD, 1-2% require amputation LLA 8-15% in people with diabetes with up
11/20/2015. Beyond CPAP. No relevant financial conflicts of interest. Kristie R Ross, M.D. November 12, Describe advanced ventilation options
 Beyond CPAP Kristie R Ross, M.D. November 12, 2015 No relevant financial conflicts of interest Sponsored by The Warren Alpert Medical School of Brown University Describe advanced ventilation options Compare
Beyond CPAP Kristie R Ross, M.D. November 12, 2015 No relevant financial conflicts of interest Sponsored by The Warren Alpert Medical School of Brown University Describe advanced ventilation options Compare
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
High flow nasal Oxygen therapy. Learning points. Part 1: Oxygen 21/06/ Oxford Advanced Course: Newcastle
 High flow nasal Oxygen therapy 15.06.2017 Oxford Advanced Course: Newcastle Learning points Update on BTS guidance May 2017 Help you understand the mechanism of action of high flow nasal oxygen therapy
High flow nasal Oxygen therapy 15.06.2017 Oxford Advanced Course: Newcastle Learning points Update on BTS guidance May 2017 Help you understand the mechanism of action of high flow nasal oxygen therapy
This is the author s final accepted version.
 Smart, R., Carter, B., McGovern, J., Luckman, S., Connelly, A., Hewitt, J., Quasim, T. and Moug, S. (2017) Frailty exists in younger adults admitted as surgical emergency leading to adverse outcomes. Journal
Smart, R., Carter, B., McGovern, J., Luckman, S., Connelly, A., Hewitt, J., Quasim, T. and Moug, S. (2017) Frailty exists in younger adults admitted as surgical emergency leading to adverse outcomes. Journal
POLICY All patients will be assessed for risk factors associated with OSA prior to any surgical procedures.
 Revised Date: Page: 1 of 7 SCOPE All Pre-Admission Testing (PAT) and Same Day Surgery (SDS) nurses at HRMC. PURPOSE The purpose of this policy is to provide guidelines for identifying surgical patients
Revised Date: Page: 1 of 7 SCOPE All Pre-Admission Testing (PAT) and Same Day Surgery (SDS) nurses at HRMC. PURPOSE The purpose of this policy is to provide guidelines for identifying surgical patients
Systems differ in their ability to deliver optimal humidification
 Average Absolute Humidity (mg H 2 O/L) Systems differ in their ability to deliver optimal humidification 45 Flows Tested 40 35 30 Optiflow Airvo 2 Vapotherm Vapotherm 5 L/min 10L/min 20L/min 30L/min 40L/min
Average Absolute Humidity (mg H 2 O/L) Systems differ in their ability to deliver optimal humidification 45 Flows Tested 40 35 30 Optiflow Airvo 2 Vapotherm Vapotherm 5 L/min 10L/min 20L/min 30L/min 40L/min
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES
 JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
Written Guidelines for Laboratory Testing in Intensive Care - Still Effective After 3 Years
 Written Guidelines for Laboratory Testing in Intensive Care - Still Effective After 3 Years S. M. MEHARI, J. H. HAVILL Intensive Care Unit, Waikato Hospital, Hamilton, NEW ZEALAND ABSTRACT Objective: The
Written Guidelines for Laboratory Testing in Intensive Care - Still Effective After 3 Years S. M. MEHARI, J. H. HAVILL Intensive Care Unit, Waikato Hospital, Hamilton, NEW ZEALAND ABSTRACT Objective: The
Respiratory insufficiency in bariatric patients
 Respiratory insufficiency in bariatric patients Special considerations or just more of the same? Weaning and rehabilation conference 6th November 2015 Definition of obesity Underweight BMI< 18 Normal weight
Respiratory insufficiency in bariatric patients Special considerations or just more of the same? Weaning and rehabilation conference 6th November 2015 Definition of obesity Underweight BMI< 18 Normal weight
Dyspnea: Should we use BIPAP?
 Dyspnea: Should we use BIPAP? Thomas R. Gildea MD, MS FCCP Head Section of Bronchoscopy Respiratory Institute Transplant Center Disclosure SuperDimension Inc. PI for single center study Others: Aeris,
Dyspnea: Should we use BIPAP? Thomas R. Gildea MD, MS FCCP Head Section of Bronchoscopy Respiratory Institute Transplant Center Disclosure SuperDimension Inc. PI for single center study Others: Aeris,
Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600
 Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
SGRQ Questionnaire assessing respiratory disease-specific quality of life. Questionnaire assessing general quality of life
 SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
Mechanical Ventilation Principles and Practices
 Mechanical Ventilation Principles and Practices Dr LAU Chun Wing Arthur Department of Intensive Care Pamela Youde Nethersole Eastern Hospital 6 October 2009 In this lecture, you will learn Major concepts
Mechanical Ventilation Principles and Practices Dr LAU Chun Wing Arthur Department of Intensive Care Pamela Youde Nethersole Eastern Hospital 6 October 2009 In this lecture, you will learn Major concepts
Roflumilast (Daxas) for chronic obstructive pulmonary disease
 Roflumilast (Daxas) for chronic obstructive pulmonary disease August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
Roflumilast (Daxas) for chronic obstructive pulmonary disease August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
The Association Between High Flow Nasal Cannula Therapy and Intubation in Acute Respiratory Failure Patients, A Single Center Retrospective Analysis
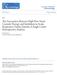 University of Kentucky UKnowledge DNP Projects College of Nursing 2017 The Association Between High Flow Nasal Cannula Therapy and Intubation in Acute Respiratory Failure Patients, A Single Center Retrospective
University of Kentucky UKnowledge DNP Projects College of Nursing 2017 The Association Between High Flow Nasal Cannula Therapy and Intubation in Acute Respiratory Failure Patients, A Single Center Retrospective
Transfusion & Mortality. Philippe Van der Linden MD, PhD
 Transfusion & Mortality Philippe Van der Linden MD, PhD Conflict of Interest Disclosure In the past 5 years, I have received honoraria or travel support for consulting or lecturing from the following companies:
Transfusion & Mortality Philippe Van der Linden MD, PhD Conflict of Interest Disclosure In the past 5 years, I have received honoraria or travel support for consulting or lecturing from the following companies:
Maria Tracey, Director-Perioperative and Elaine Warren, Directory-Surgery Level. III (Three)
 PAGE 1/6 MANAGEMENT OF ADULT SURGICAL CLIENTS WITH KNOWN OR SUSPECTED OBSTRUCTIVE SLEEP APNEA (OSA) Patient Care Issuing Authority Dr. James Flynn, Clinical Chief Surgical Services (Perioperative) Signed
PAGE 1/6 MANAGEMENT OF ADULT SURGICAL CLIENTS WITH KNOWN OR SUSPECTED OBSTRUCTIVE SLEEP APNEA (OSA) Patient Care Issuing Authority Dr. James Flynn, Clinical Chief Surgical Services (Perioperative) Signed
Bi-Level Therapy: Boosting Comfort & Compliance in Apnea Patients
 Bi-Level Therapy: Boosting Comfort & Compliance in Apnea Patients Objectives Describe nocturnal ventilation characteristics that may indicate underlying conditions and benefits of bilevel therapy for specific
Bi-Level Therapy: Boosting Comfort & Compliance in Apnea Patients Objectives Describe nocturnal ventilation characteristics that may indicate underlying conditions and benefits of bilevel therapy for specific
INDICATIONS FOR RESPIRATORY ASSISTANCE A C U T E M E D I C I N E U N I T P - Y E A R M B B S 4
 INDICATIONS FOR RESPIRATORY ASSISTANCE A C U T E M E D I C I N E U N I T P - Y E A R M B B S 4 RESPIRATORY FAILURE Acute respiratory failure is defined by hypoxemia with or without hypercapnia. It is one
INDICATIONS FOR RESPIRATORY ASSISTANCE A C U T E M E D I C I N E U N I T P - Y E A R M B B S 4 RESPIRATORY FAILURE Acute respiratory failure is defined by hypoxemia with or without hypercapnia. It is one
Managing peri-operative anaemiathe Papworth way. Dr Andrew A Klein Royal Papworth Hospital Cambridge UK
 Managing peri-operative anaemiathe Papworth way Dr Andrew A Klein Royal Papworth Hospital Cambridge UK Conflicts of interest: Unrestricted educational grants/honoraria from CSL Behring, Brightwake Ltd,
Managing peri-operative anaemiathe Papworth way Dr Andrew A Klein Royal Papworth Hospital Cambridge UK Conflicts of interest: Unrestricted educational grants/honoraria from CSL Behring, Brightwake Ltd,
pat hways Medtech innovation briefing Published: 1 October 2018 nice.org.uk/guidance/mib161
 pat hways myairvo2 for the treatment of chronic obstructive pulmonary disease Medtech innovation briefing Published: 1 October 2018 nice.org.uk/guidance/mib161 Summary The technology described in this
pat hways myairvo2 for the treatment of chronic obstructive pulmonary disease Medtech innovation briefing Published: 1 October 2018 nice.org.uk/guidance/mib161 Summary The technology described in this
Oxygen prescription and administration at the Emergency Department and medical wards in Mater Dei Hospital
 Original Article Oxygen prescription and administration at the Emergency Department and medical wards in Mater Dei Hospital Rachelle Asciak, Valerie Anne Fenech, Jurgen Gatt, Stephen Montefort Abstract
Original Article Oxygen prescription and administration at the Emergency Department and medical wards in Mater Dei Hospital Rachelle Asciak, Valerie Anne Fenech, Jurgen Gatt, Stephen Montefort Abstract
A comparison of fentanyl, sufentanil, and remifentanil for fast-track cardiac anesthesia Engoren M, Luther G, Fenn-Buderer N
 A comparison of fentanyl, sufentanil, and remifentanil for fast-track cardiac anesthesia Engoren M, Luther G, Fenn-Buderer N Record Status This is a critical abstract of an economic evaluation that meets
A comparison of fentanyl, sufentanil, and remifentanil for fast-track cardiac anesthesia Engoren M, Luther G, Fenn-Buderer N Record Status This is a critical abstract of an economic evaluation that meets
Effectiveness of high-flow nasal cannula oxygen therapy for acute respiratory failure with hypercapnia
 Original Article Effectiveness of high-flow nasal cannula oxygen therapy for acute respiratory failure with hypercapnia Eun Sun Kim, Hongyeul Lee, Se Joong Kim, Jisoo Park, Yeon Joo Lee, Jong Sun Park,
Original Article Effectiveness of high-flow nasal cannula oxygen therapy for acute respiratory failure with hypercapnia Eun Sun Kim, Hongyeul Lee, Se Joong Kim, Jisoo Park, Yeon Joo Lee, Jong Sun Park,
University of Bristol - Explore Bristol Research
 Rogers, C., Capoun, R., Scott, L., Taylor, J., Angelini, G., Narayan, P.,... Ascione, R. (2017). Shortening cardioplegic arrest time in patients undergoing combined coronary and valve surgery: results
Rogers, C., Capoun, R., Scott, L., Taylor, J., Angelini, G., Narayan, P.,... Ascione, R. (2017). Shortening cardioplegic arrest time in patients undergoing combined coronary and valve surgery: results
Setting The setting was tertiary care. The economic study appears to have been performed in Heidelberg, Germany.
 Comparative analysis of costs of total intravenous anaesthesia with propofol and remifentanil vs. balanced anaesthesia with isoflurane and fentanyl Epple J, Kubitz J, Schmidt H, Motsch J, Bottiger B W,
Comparative analysis of costs of total intravenous anaesthesia with propofol and remifentanil vs. balanced anaesthesia with isoflurane and fentanyl Epple J, Kubitz J, Schmidt H, Motsch J, Bottiger B W,
CORONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW
 CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW 2015 PQRS OPTIONS F MEASURES GROUPS: 2015 PQRS MEASURES IN CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP: #43 Coronary Artery Bypass Graft (CABG):
CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP OVERVIEW 2015 PQRS OPTIONS F MEASURES GROUPS: 2015 PQRS MEASURES IN CONARY ARTERY BYPASS GRAFT (CABG) MEASURES GROUP: #43 Coronary Artery Bypass Graft (CABG):
Weaning from Mechanical Ventilation. Dr Azmin Huda Abdul Rahim
 Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A.
 aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A. 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and
aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A. 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and
Recent Advances in Respiratory Medicine
 Recent Advances in Respiratory Medicine Dr. R KUMAR Pulmonologist Non Invasive Ventilation (NIV) NIV Noninvasive ventilation (NIV) refers to the administration of ventilatory support without using an invasive
Recent Advances in Respiratory Medicine Dr. R KUMAR Pulmonologist Non Invasive Ventilation (NIV) NIV Noninvasive ventilation (NIV) refers to the administration of ventilatory support without using an invasive
Ivax Pharmaceuticals UK Sponsor Submission to the National Institute for Health and Clinical Excellence
 Ivax Pharmaceuticals UK Sponsor Submission to the National Institute for Health and Clinical Excellence Clinical and cost-effectiveness of QVAR for the treatment of chronic asthma in adults and children
Ivax Pharmaceuticals UK Sponsor Submission to the National Institute for Health and Clinical Excellence Clinical and cost-effectiveness of QVAR for the treatment of chronic asthma in adults and children
Proposed presentation of data for ICU-ROX.
 Proposed presentation of data for ICU-ROX. Version 1 was posted online on 21 November 2017 (prior to the interim analysis which occurred when the 500 th participant reached day 28). This version (version
Proposed presentation of data for ICU-ROX. Version 1 was posted online on 21 November 2017 (prior to the interim analysis which occurred when the 500 th participant reached day 28). This version (version
Surveillance report Published: 6 April 2016 nice.org.uk. NICE All rights reserved.
 Surveillance report 2016 Chronic obstructive pulmonary disease in over 16s: diagnosis and management (2010) NICE guideline CG101 Surveillance report Published: 6 April 2016 nice.org.uk NICE 2016. All rights
Surveillance report 2016 Chronic obstructive pulmonary disease in over 16s: diagnosis and management (2010) NICE guideline CG101 Surveillance report Published: 6 April 2016 nice.org.uk NICE 2016. All rights
Protecting the Lungs
 Protecting the Lungs PGA New York 12/07 Disclosures: Peter Slinger MD, FRCPC University of Toronto 58 y.o. Male, Chronic Gallstone Pancreatitis, Open Cholecystectomy 100 pack/year smoker Dyspnea > 1 block
Protecting the Lungs PGA New York 12/07 Disclosures: Peter Slinger MD, FRCPC University of Toronto 58 y.o. Male, Chronic Gallstone Pancreatitis, Open Cholecystectomy 100 pack/year smoker Dyspnea > 1 block
THE NATIONAL QUALITY FORUM
 THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
Critical Appraisal Practicum. Fabio Di Bello Medical Implementation Manager
 Critical Appraisal Practicum Fabio Di Bello Medical Implementation Manager fdibello@ebsco.com What we ll talk about today: DynaMed process for appraising randomized trials and writing evidence summaries
Critical Appraisal Practicum Fabio Di Bello Medical Implementation Manager fdibello@ebsco.com What we ll talk about today: DynaMed process for appraising randomized trials and writing evidence summaries
