Predicting cardiac output responses to passive leg raising by a PEEP-induced increase in central venous pressure, in cardiac surgery patients
|
|
|
- Hector Harris
- 6 years ago
- Views:
Transcription
1 British Journal of Anaesthesia 17 (2): 1 6 (211) Advance Access publication 27 May 211. doi:1.193/bja/aer12 Predicting cardiac output responses to passive leg raising by a PEEP-induced increase in central venous pressure, in cardiac surgery patients B. F. Geerts 1,2 *, L. P. H. J. Aarts 1, A. B. Groeneveld 3 and J. R. C. Jansen 2 1 Department of Anaesthesiology and 2 Department of Intensive Care, Leiden University Medical Centre, Albinusdreef 2, PO Box 96, 23 RC Leiden, The Netherlands 3 Department of Intensive Care and Institute for Cardiovascular Research, VU University Medical Center, Amsterdam, The Netherlands * Corresponding author. b.f.geerts@lumc.nl Editor s key points Dynamic measures of circulatory filling such as stroke volume variation (SVV) with mechanical ventilation are generally considered more reliable than static measures such as central venous filling pressure (CVP). Drawbacks of SVV include dependence of the changes on tidal volume and ventilatory frequency. Change in CVP upon the application of increased PEEP is not subject to these limitations. In this small study in cardiac surgery patients, the change in CVP with PEEP performed similar to SVV as an indicator of fluid responsiveness. Background. Changes in central venous pressure (CVP) rather than absolute values may be used to guide fluid therapy in critically ill patients undergoing mechanical ventilation. We conducted a study comparing the changes in the CVP produced by an increase in PEEP and stroke volume variation (SVV) as indicators of fluid responsiveness. Fluid responsiveness was assessed by the changes in cardiac output (CO) produced by passive leg raising (PLR). Methods. In 2 fully mechanically ventilated patients after cardiac surgery, PEEP was increased +1 cm H 2 O for min followed by PLR. CVP, SVV, and thermodilution CO were measured before, during, and directly after the PEEP challenge and 3 PLR. The CO increase.7% upon PLR was used to define responders. Results. Twenty patients were included; of whom, 1 responded to PLR. The increase in CO by PLR directly related (r¼.77, P,.1) to the increase in CVP by PEEP. PLR responsiveness was predicted by the PEEP-induced increase in CVP [area under receiver-operating characteristic (AUROC) curve.99, P,.1] and by baseline SVV (AUROC.9, P¼.3). The AUROC s for dcvp and SVV did not differ significantly (P¼.299). Conclusions. Our data in mechanically ventilated, cardiac surgery patients suggest that the newly defined parameter, PEEP-induced CVP changes, like SVV, appears to be a good parameter to predict fluid responsiveness. Keywords: cardiac output, monitoring; cardiac surgery; central venous pressure; fluid loading responsiveness; passive leg raising Accepted for publication: 2 February 211 Changes in central venous pressure (CVP) are probably more useful in guiding fluid treatment of mechanically ventilated hypovolaemic patients than absolute pressure values which are confounded by concomitant PEEP. 1 3 Furthermore, assessment of a reliable predictor before fluid loading would allow the physician to prevent harmful overloading. Ventilator-induced stroke volume variations (SVVs) are commonly used to predict fluid responsiveness, that is, an increase in cardiac output (CO) by fluid loading or passive leg raising (PLR). However, SVV is only applicable in mechanically ventilated patients without spontaneous breathing efforts and with a regular heart rhythm. Furthermore, SVV depends on ventilatory frequencies and tidal volumes. PLR can be used as a reversible, endogenous fluid challenge of about 2 3 ml and, if correctly performed, the CO response correlates well to that upon exogenous fluid administration in predicting fluid responsiveness. 9 2 However, repeated PLR is not practicable in all patients and all settings. Another manoeuvre to predict fluid responsiveness is an end-expiratory hold which produces an increase in pulse pressure and CO. The magnitude of the change may be assessed by comparatively noninvasive pulse contour methods. 19 However, it is likely that the change depends on inspiratory pressure and thus on tidal volume and the resultant impediment in venous return. Taken together, current dynamic methods to predict fluid responsiveness have limitations and may not prevent harmful fluid overloading in mechanically ventilated, critically ill patients. We hypothesized that the change in CVP produced by a change in PEEP of short duration can be used to predict the response of CO to fluid loading, since an increase in PEEP is associated with an increase in CVP and a decrease in CO, dependent on volume status To test this hypothesis, we measured the changes in CVP due to an increase in PEEP of 1 cm H 2 O and defined fluid & The Author [211]. Published by Oxford University Press on behalf of the British Journal of Anaesthesia. All rights reserved. For Permissions, please journals.permissions@oup.com
2 A PEEP challenge BJA responsiveness by the response in CO to subsequent PLR. We compared the predictive value of the change in CVP with those of absolute CVP and SVV. Methods The study was approved by the Medical Ethics Committee of the Leiden University Medical Centre and written informed consent was obtained before surgery. Twenty consecutive patients undergoing elective cardiac surgery were enrolled into the study. During surgery, before admission to the intensive care unit (ICU), each patient underwent pulmonary artery catheter insertion (Intellicath; Edwards Lifesciences, Irvine, CA, USA) to measure thermodilution CO and CVP. A radial artery catheter was used to measure radial arterial pressure in all patients. In the ICU, anaesthesia was continued with propofol target control infusion (1. mg ml 21 ) and sufentanil according to institutional standards. The lungs were mechanically ventilated in a volume-control mode with standard settings to achieve normocapnia with a tidal volume of 1 ml kg 21 and a respiratory frequency of 12 1 bpm. The FIO 2 was. and baseline PEEP cm H 2 O. None of the patients suffered significant blood loss (. ml h 21 ) during the data collection period. Protocol and measurements Blood pressure transducers were referenced to the level of the intersection of the anterior axillary line and the fifth intercostal space. CVP, mean arterial pressure (MAP), and heart rate (HR) were averaged over 3 s intervals. Bolus thermodilution CO was obtained, within 3 min with an automated system under computer control, by the mean of triplicate measurements equally spread over the ventilatory cycle. 2 SVV was determined from beat-to-beat CO values measured over 2 s intervals using the LiDCO (LiDCO Ltd, Cambridge, UK) radial artery pulse contour system. The system was calibrated by entering the mean value of the first series of three thermodilution measurements at the start of our protocol. All measurements were carried out following stabilization and within 2 h of arrival on the ICU. During the observation period, the patients remained supine and doses of sedative and vasoactive agents were unaltered. Measurements of CVP, SVV, CO, MAP, and HR were made under five experimental conditions: (i) baseline 1; (ii) PEEP increased with 1 cm H 2 O (to a level of 1 cm H 2 O); (iii) baseline 2; (iv) PLR; and (v) baseline 3. Each condition was maintained for a min period and measurements were performed in the final 3 min of each period. PLR was performed by maintaining the patient in the supine position and raising the legs 3 by using the facility to raise the lower end of the bed. The thorax and head (i.e. the heart and baroreceptors) were maintained at the same position through all of the study periods and the pressure transducers did not have to be re-referenced. Statistical analysis Usually, fluid responsiveness is characterized by an increase of 1 1% in CO after rapid fluid loading with ml. 2 Recently, Jabot and colleagues 17 showed that PLR from the supine position induces smaller increases in CO than PLR from the semi-recumbent position. On the basis of their results and those of Lafanechere and colleagues, 1 we reasoned that in responders, PLR from the supine position should result in an increase of CO.7%. Our thermodilution technique with automated triplicate measurements equally spread over the respiratory cycle has a precision of 3.%. 2 Therefore, this technique should detect changes in CO induced by PLR.7% accurately, thereby allowing identification of responders. All data were normally distributed (Kolmogorov Smirnov test P..). The effects of PEEP and PLR were evaluated by subtracting the mean of the baseline value before and after the challenge from the value found during the challenge. Comparisons of different experimental conditions were performed using the paired t-test. The Pearson correlation coefficient was used to relate baseline variables to increases in CO upon PLR. Receiver operating characteristic (ROC) curves and 9% confidence intervals (9% CIs) for the area under the curve (AUC) were computed. A P-value for the difference between the AUC and the reference value of. (i.e. prediction of responders and non-responders by chance) is calculated. From the ROC curves, the optimum cut-off value with the greatest combined sensitivity and specificity was computed, using baseline SVV, absolute values, and changes in CVP. 2 Areas under the curve of the ROC curves (AUROC) of baseline SVV and PEEP-induced change in CVP were compared. Data are summarized by mean and standard deviation (SD). A P-value of,. was considered statistically significant. Statistical calculations were performed using SPSS for Windows (V12; SPSS Institute, Chicago, IL, USA), and MedCalc (V9, Mariakerke, Belgium). Results Twenty patients were included in the study; patient characteristics are tabulated in Table 1. Twelve patients underwent coronary artery bypass surgery (CABG), and eight received either a single-valve replacement or a combination of CABG and valvular repair surgery. Table 2 shows that, compared with baseline, an increase of 1 cm H 2 O in PEEP decreased CO, increased CVP and SVV, but had little effect on MAP and HR. PLR increased CO, CVP, and MAP but decreased SVV. All variables returned to baseline after the PEEP and PLR challenges. Whereas baseline CVP and baseline SVV related to the percentage change in CO due to PLR (Fig. 1), the change in CVP due to PEEP correlated best to the change in CO due to PLR (Fig. 1). Changes in CO upon PEEP moderately correlated to changes in CO by PLR (r¼2.7, P¼.36). There were 1 PLR responders and 1 non-responders. CO values before and after the PEEP challenge were.1 (1.2) and.3 (1.) litre min 21, in responders and non-responders (ns), 11
3 BJA Geerts et al. respectively. CO values around PLR were. (1.6) and. (1.) litre min 21 in responders and non-responders (ns), respectively. Baseline CVP values before and after the PEEP challenge were 7.1 (2.) and 11.3 (3.1) mm Hg in responders and non-responders, respectively (P¼.3). Baseline SVV values around the PEEP challenge were.7 (3.2)% and 3. (2.1)% in PLR responders and non-responders, respectively (P¼.1), but the PEEP-induced change in SVV did not differ. The PEEP-induced increase in CVP was less in nonresponders to PLR than in responders: 1.1 (.) and 3.6 (1.) mm Hg or 9 (7)% and 62 (2)% (P¼.1). Baseline values of CVP for responders and non-responders were 11.3 (3.1) and 7.1 (2.) mm Hg (P¼.6), respectively. Also, the decrease in CO upon the application of PEEP was less in PLR non-responders than responders [6 (7)% vs 16 (1)%, P¼.1]. The results of ROC curves analyses are shown in Figure 2. For baseline CVP, the AUC was. (9% CI.6 and 1., P¼.) and the optimum cut-off value of 9. mm Hg had a sensitivity of % and a specificity of % to predict PLR responsiveness. The AUC for baseline SVV was.9 (9% CI.76 1., P¼.3), and a baseline SVV cut-off of 7.3% had a sensitivity of 7% and a specificity of 1% to Table 1 Patient characteristics (n¼2). Data collected postoperative immediately before the study were performed. Data, except in the case of age, are shown as mean (SD) Age 61 (range 3 ) yr Sex, M/F 16 (%)/ (2%) Body surface area 2. (.21) m 2 Type of surgery Coronary artery bypass grafting 11 (%) Valvular repair 9 (%) Dobutamine or dopamine 3 (1%) Norepinephrine 2 (1%) Tidal volume 72 (127) ml Mean airway pressure 9 (1) cm H 2 O PEEP () cm H 2 O. FIO2 Pa O2 Pa O2 /FIO (.13) kpa ratio 31. (1.1) predict PLR responsiveness. For the predictive value of the CVP response (change) to PEEP, the AUC was.99 (9% CI.9 1., P,.1) and a cut-off value of an increase of 1. mm Hg had a sensitivity of 1% and a specificity of 9% for PLR responsiveness. The AUC of baseline SVV was not significantly different from the AUC for CVP response to PEEP (P¼.299), suggesting that baseline SVV and the CVP response to PEEP can be used equally to predict responders and non-responders to fluid loading. Discussion Our study shows that with higher baseline SVV values, lower baseline CVP values, and greater increases in CVP upon a PEEP challenge, the response of CO on an endogenous fluid loading by PLR can be predicted. Of these predictors, the increase in CVP with PEEP seems most robust for predicting fluid responsiveness with least risk for confounding by ventilatory conditions. We based our study on the simplified Guytonian model of the circulation (Fig. 3). We consider the effects of PEEP and of PLR in the hypo- and normovolaemic state. Many authors demonstrated that the venous return curve, that is, the relationship between CO and CVP, moves up in parallel with increased blood volumes (Fig. 3, lines hypo- and normovolaemia). We have previously constructed venous return curves using prolonged inspiratory hold manoeuvres in cardiac surgical patients and showed that the slopes were equal in hypo-, normo-, and hypervolaemic conditions. 29 Magder and colleagues 1 have shown that application of PEEP shifts the cardiac function curve to the right, altering the intersection with the venous return curve to a lower CO and a higher CVP (Fig. 3A, change from point A to point B). In patients with hypovolaemia, the increase in CVP and decrease in CO (dcvp1 and dco1) are larger than in patients with normovolaemia (dcvp2 and dco2), in line with experimental data. 21 Thus, the PEEP-induced change in CVP and the change in CO describe in which part of its function curve, the heart operates. Fluid loading by PLR will move up the venous return curve (Fig. 3B, dashed lines). In patients with hypovolaemia and in those with normovolemia, the intersection with the cardiac function curve will move towards its plateau. 3 Fluid loading in these two volaemic conditions results in an increasing change in CVP (Fig. 3B, Table 2 Haemodynamics at baseline and after an increase in PEEP of 1 cm H 2 O and after PLR. PLR, passive leg raising; CVP, central venous pressure; SVV, stroke volume variation; CO, cardiac output by thermodilution; MAP, mean arterial pressure; HR, heart rate. Baseline PEEP is the group average of the values before and after the PEEP challenge; baseline PLR, the group averaged value before and after PLR. The results are shown as mean (SD) Baseline PEEP 11 cm H 2 O PEEP Change P-value Baseline PLR PLR Change P-value CVP (mm Hg) 9.2 (3.6) 11. (3.2) 2. (1.), (3.6) 11.6 (3.6) 2.3 (1.3),.1 SVV (%) 6.2 (3.) 1.6 (6.).7 (3.7),.1. (3.) 3.9 (2.7) 21.9 (1.),.1 CO (litre min 21 ).2 (1.3).6 (1.2) 2.6 (.),.1. (1.).9 (1.7). (.3),.1 MAP (mm Hg) 3 (13) (1) 23 (1). (16) 92 (1) (1).3 HR (beats min 21 ) 79 (13) 7 (12) 21 (1). 79 (12) 77 (12) 22 (3).29 12
4 A PEEP challenge BJA 1 A Responders 1 dco, PLR (%) - 12 Baseline CVP (mm Hg) B dco, PLR (%) dco, PLR (%) Baseline SVV (%) C - 2 dcvp, PEEP (mm Hg) 6 Fig 1 In the first graph (A), the relationship between Baseline CVP and change in thermodilution CO by PLR (dco, PLR) is shown (r¼2.63, P¼.3); in the second graph (B), the relationship between baseline SVV and dco, PLR (r¼.67, P¼.2). In the third graph (C), the relationship between the PEEP-induced change in CVP (dcvp, PEEP) and dco, PLR is depicted (r¼.77, P,.1). Baseline values of CVP and SVV were the averaged results of baseline measurements before and after the PEEP challenge. dcvp is the change in CVP due to PEEP compared with the averaged baseline value. The horizontal dashed line in the graphs indicates the cut-off between responders and non-responders. from dcvp1 to dcvp2) and a decreasing effect on CO (Fig. 3B, from dco1 to dco2). Thus, with PEEP, dcvp and dco should change inversely but proportionally, depending on the volume status, whereas with fluid loading, reverse effects of dcvp and dco are predicted. We used PLR as a surrogate for fluid infusion since it correlates well with responsiveness to exogenous fluids. 9 2 Moreover, the use of PLR obviates unnecessary and potentially harmful fluid loading in non-responders. We found, as predicted by the model, that the increase in CVP by PEEP directly relates to the increase in CO by PLR and thus may be of value to predict fluid responsiveness (Fig. 1); secondly, that PEEP increases CVP and decreases CO, but that the increase in CVP and the decrease in CO are less in non- 13
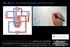
5 BJA Geerts et al. responders than in responders (normo- vs hypovolaemia). Our results imply that the predominant mechanism of the decrease in CO with PEEP is diminished venous return and a decrease in right ventricular preload, which in turn may Sensitivity Specificity Fig 2 ROC curve of baseline CVP (dotted line), baseline SVV (dashed line), and change in CVP (straight line) upon a PEEP challenge to predict responsiveness to PLR. The AUC is. (with a 9% CI of.6 1.) for baseline CVP,.99 (with a 9% CI of.9 1.) for changes in CVP, and.9 (with a 9% CI of.76 and 1.) for baseline SVV. A CO (litre min 1 ) dco1 dco2 A B normo limit the increase in CVP We cannot judge from our data the effect of abnormal lungs and altered airway pressure transmission on the circulatory response to PEEP Another limitation of the model is that it does not take circulatory control mechanisms into account. Therefore, we measured the effects of PEEP between 2 and min after its application. Changes in myocardial contractility may change the position and shape of the heart function curve. Therefore, a deterioration of cardiac function may lead to a decrease in SVV and a decrease in the change in CVP produced by PEEP and also a less fluid-responsive patient. This was not examined in this study. The fact that baseline CVP was also associated with changes in CO can be explained by the relatively low PEEP we used in our patients, but changes in filling pressures to guide fluid treatment are less confounded by PEEP than absolute levels. 322 The observation that the CO response to PEEP was of less predictive value than the CVP response for the CO increase upon PLR can be explained by a lesser decrease in CO for a given PEEP-induced increase in CVP in hypo- than in normovolaemic conditions, as shown in animal experiments. 21 We should also keep in mind that the PEEP challenge moves the work-point of the cardiac function and venous return curves downwards to the steep part of the curve (larger change in CO), whereas PLR moves the work-point upwards into the flat part of the curve (smaller change in CO, Fig. 3). This may help explain why the PLR response of CO was of less predictive value for the PEEP-induced decrease in CO B CO (litre min 1 ) dco1 dco2 normo 1 dcvp1 dcvp2 PEEP 1 12 CVP (mm Hg) hypo 1 dcvp1 dcvp2 hypo 1 12 CVP (mm Hg) Fig 3 A simplified model of the interaction of the heart function curve and venous return curve. The effects of (A) PEEP and (B) fluid loading by PLR on CVP and CO are indicated. From hypovolaemia (hypo) to normovolaemia (normo), the venous return curve (straight line) moves up and the intersection with the cardiac function curve (curved line) increases to a higher CO and CVP level. (A) Addition of PEEP shifts the heart function curve to the right (dashed line) altering the intersection with the venous return curve to a lower CO and a higher CVP. With the application of PEEP, the change in CVP (dcvp) and the change in CO (dco) are larger during hypovolaemia (dcvp1 and dco1) than during normovolaemia (dcvp2 and dco2). This suggests that the value of dcvp is an indicator for fluid loading responsiveness. (B) Addition of PLR (dashed lines) results in an increase in CVP and CO. With fluid loading by PLR during normovolaemia, a greater dcvp (dcvp2) and a smaller dco (dco2) are observable than during hypovolaemia (dcvp1 and dco1). dco with PLR have been shown to be an indicator of fluid loading responsiveness. For further explanation, see text. 1
6 A PEEP challenge BJA than vice versa (data not shown). The decrease in CO with PEEP may lead to an unacceptably too low CO for several minutes. Thus, when there are clear signs of hypovolaemia, the use of the PEEP challenge may not be appropriate. Our proposed challenge resembles the end-expiratory occlusion test 19 to predict fluid responsiveness but carries the relative advantage, of being independent of ventilatory conditions provided that PEEP can be increased by 1 cm H 2 O. Since the PEEP challenge is easy to apply and CVP is measured routinely in the ICU, the PEEP-induced change in CVP may provide the physician with a robust and easy-to-use tool to assess fluid responsiveness. The drawback of the PEEP challenge is its dependence on maintenance of a steady state during the challenge and potential worsening of hypotension. An SVV of about 1% or above, derived from noninvasive arterial pulse contour algorithms, has been used to predict an increase of 1 1% in CO in response to ml fluid loading. Our patients were subjected to a smaller preload challenge and the optimal cut-off to define responsiveness was somewhat lower. The SVV requires a regular HR and full mechanical ventilatory support, with predictive values dependent on ventilatory frequencies and tidal volumes. 7 Again, we may speculate that our PEEP challenge is less dependent on these prerequisites. Even though SVV had a similar predictive value to the PEEP challenge, the latter may thus be preferable, particularly in the case of arrhythmias. One might also argue that performing a PLR and looking at the CO response would render our PEEP challenge redundant. However, PLR is not always feasible and necessitates some CO measurement, while our PEEP challenge does not. (In contrast, the PLR challenge does not require mechanical ventilation.) 1 1 Finally, the relatively small changes in CVP evoked by PEEP can only be discerned at the bedside when accurately measured. In conclusion, our data suggest that brief PEEP-induced increases in CVP predict fluid responsiveness at least and also absolute values of CVP and SVV, after cardiac surgery, and are less likely to be confounded by ventilatory conditions. Conflict of interest None declared. Funding Solely by institutional funding. References 1 Magder S, Lagonidis D, Erice F. The use of respiratory variations in right atrial pressure to predict the cardiac output response to PEEP. J Crit Care 21; 16: Marik PE, Baram M, Vahid B. Does central venous pressure predict fluid responsiveness? A systematic review of the literature and the tale of seven mares. Chest 2; 13: Verheij J, van Lingen A, Beishuizen A, et al. Cardiac response is greater for colloid than saline fluid loading after cardiac or vascular surgery. Intensive Care Med 26; 32: 13 Rex S, Brose S, Metzelder S, et al. Prediction of fluid responsiveness in patients during cardiac surgery. Br J Anaesth 2; 93: 72 Hofer CK, Senn A, Weibel L, Zollinger A. Assessment of stroke volume variation for prediction of fluid responsiveness using the modified FloTrac and PiCCOplus system. Crit Care 2; 12: R2 6 Preisman S, Kogan S, Berkenstadt H, Perel A. Predicting fluid responsiveness in patients undergoing cardiac surgery: functional haemodynamic parameters including the Respiratory Systolic Variation Test and static preload indicators. Br J Anaesth 2; 9: 76 7 De Backer D, Taccone FS, Holsten R, Ibrahimi F, Vincent JL. Influence of respiratory rate on stroke volume variation in mechanically ventilated patients. Anesthesiology 29; 11: Reuter DA, Bayerlein J, Goepfert MS, et al. Influence of tidal volume on left ventricular stroke volume variation measured by pulse contour analysis in mechanically ventilated patients. Intensive Care Med 23; 29: 76 9 Thomas M, Shillingford J. The circulatory response to a standard postural change in ischaemic heart disease. Br Heart J 196; 27: Rutlen DL, Wackers FJ, Zaret BL. Radionuclide assessment of peripheral intravascular capacity: a technique to measure intravascular volume changes in the capacitance circulation in man. Circulation 191; 6: Wong DH, Tremper KK, Zaccari J, Hajduczek J, Konchigeri HN, Hufstedler SM. Acute cardiovascular response to passive leg raising. Crit Care Med 19; 16: Wong DH, O Connor D, Tremper KK, Zaccari J, Thompson P, Hill D. Changes in cardiac output after acute blood loss and position change in man. Crit Care Med 199; 17: Lamia B, Ochagavia A, Monnet X, Chemla D, Richard C, Teboul JL. Echocardiographic prediction of volume responsiveness in critically ill patients with spontaneously breathing activity. Intensive Care Med 27; 33: Maizel J, Airapetian N, Lorne E, Tribouilloy C, Massy Z, Slama M. Diagnosis of central hypovolemia by using passive leg raising. Intensive Care Med 27; 33: Lafanechere A, Pene F, Goulenok C, et al. Changes in aortic blood flow induced by passive leg raising predict fluid responsiveness in critically ill patients. Crit Care 26; 1: R Monnet X, Rienzo M, Osman D, et al. Passive leg raising predicts fluid responsiveness in the critically ill. Crit Care Med 26; 3: Jabot J, Teboul JL, Richard C, Monnet X. Passive leg raising for predicting fluid responsiveness: importance of the postural change. Intensive Care Med 29; 3: 9 1 Boulain T, Achard JM, Teboul JL, Richard C, Perrotin D, Ginies G. Changes in BP induced by passive leg raising predict response to fluid loading in critically ill patients. Chest 22; 121: Monnet X, Osman D, Ridel C, Lamia B, Richard C, Teboul JL. Predicting volume responsiveness by using the end-expiratory occlusion in mechanically ventilated intensive care unit patients. Crit Care Med 29; 37: Cavallaro F, Sandroni C, Marano C, et al. Diagnostic accuracy of passive leg raising for prediction of fluid responsiveness in adults: systematic review and meta-analysis of clinical studies. Intensive Care Med 21; 36:
7 BJA Geerts et al. 21 Schreuder JJ, Jansen JR, Versprille A. Hemodynamic effects of PEEP applied as a ramp in normo-, hyper-, and hypovolemia. J Appl Physiol 19; 9: Luecke T, Pelosi P. Clinical review: positive end-expiratory pressure and cardiac output. Crit Care 2; 9: Fougeres E, Teboul JL, Richard C, Osman D, Chemla D, Monnet X. Hemodynamic impact of a positive end-expiratory pressure setting in acute respiratory distress syndrome: importance of the volume status. Crit Care Med 21; 3: Jansen JR, Schreuder JJ, Settels JJ, Kloek JJ, Versprille A. An adequate strategy for the thermodilution technique in patients during mechanical ventilation. Intensive Care Med 199; 16: 22 2 Hanley JA, McNeil BJ. The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology 192; 13: Guyton AC, Lindsey AW, Abernathy B, Richardson T. Venous return at various right atrial pressures and the normal venous return curve. Am J Physiol 197; 19: Pinsky MR. Instantaneous venous return curves in an intact canine preparation. J Appl Physiol 19; 6: Versprille A, Jansen JR. Mean systemic filling pressure as a characteristic pressure for venous return. Pflugers Arch 19; : Maas JJ, Geerts BF, de Wilde RB, van den Berg PC, Pinsky MR, Jansen JR. Assessment of venous return curve and mean systemic filling pressure in post-operative cardiac surgery patients. Crit Care Med 29; 37: Versprille A, Jansen JR. Tidal variation of pulmonary blood flow and blood volume in piglets during mechanical ventilation during hyper-, normo- and hypovolaemia. Pflugers Arch 1993; 2:
Predicting cardiac output responses to passive leg raising by a PEEP-induced increase in central venous pressure, in cardiac surgery patients
 Chapter 10 Predicting cardiac output responses to passive leg raising by a PEEP-induced increase in central venous pressure, in cardiac surgery patients Bart Geerts, Leon Aarts, Johan Groeneveld and Jos
Chapter 10 Predicting cardiac output responses to passive leg raising by a PEEP-induced increase in central venous pressure, in cardiac surgery patients Bart Geerts, Leon Aarts, Johan Groeneveld and Jos
Assessing Preload Responsiveness Using Arterial Pressure Based Technologies. Patricia A. Meehan, RN, MS Education Consultant Edwards Lifesciences, LLC
 Assessing Preload Responsiveness Using Arterial Pressure Based Technologies Patricia A. Meehan, RN, MS Education Consultant Edwards Lifesciences, LLC Content Description : Fluid administration is a first
Assessing Preload Responsiveness Using Arterial Pressure Based Technologies Patricia A. Meehan, RN, MS Education Consultant Edwards Lifesciences, LLC Content Description : Fluid administration is a first
Assessment of venous return curve and mean systemic filling pressure in postoperative cardiac surgery patients
 Chapter 8 Assessment of venous return curve and mean systemic filling pressure in postoperative cardiac surgery patients Jacinta Maas, Bart Geerts, Paul van den Berg, Micheal Pinsky and Jos Jansen Critical
Chapter 8 Assessment of venous return curve and mean systemic filling pressure in postoperative cardiac surgery patients Jacinta Maas, Bart Geerts, Paul van den Berg, Micheal Pinsky and Jos Jansen Critical
Jan M. Headley, R.N. BS
 Fluid First: Using PLR & SVV to Optimize Volume Jan M. Headley, R.N. BS Disclosure Director, Clinical Marketing & Professional Education Edwards Lifesciences Does this Patient NEED Fluid?? WE Have a Problem
Fluid First: Using PLR & SVV to Optimize Volume Jan M. Headley, R.N. BS Disclosure Director, Clinical Marketing & Professional Education Edwards Lifesciences Does this Patient NEED Fluid?? WE Have a Problem
Chapter 2. Performance of three minimally invasive cardiac output monitoring systems
 Chapter 2 Performance of three minimally invasive cardiac output monitoring systems Rob de Wilde, Bart Geerts, Jisheng Cui, Paul van den Berg and Jos Jansen Anaesthesia 2009; 64: 762 769 (45 46) Ideally
Chapter 2 Performance of three minimally invasive cardiac output monitoring systems Rob de Wilde, Bart Geerts, Jisheng Cui, Paul van den Berg and Jos Jansen Anaesthesia 2009; 64: 762 769 (45 46) Ideally
Cardiac filling pressures are not appropriate to predict hemodynamic response to volume challenge*
 Cardiac filling pressures are not appropriate to predict hemodynamic response to volume challenge* David Osman, MD; Christophe Ridel, MD; Patrick Ray, MD; Xavier Monnet, MD, PhD; Nadia Anguel, MD; Christian
Cardiac filling pressures are not appropriate to predict hemodynamic response to volume challenge* David Osman, MD; Christophe Ridel, MD; Patrick Ray, MD; Xavier Monnet, MD, PhD; Nadia Anguel, MD; Christian
Hemodynamic monitoring beyond cardiac output
 Hemodynamic monitoring beyond cardiac output Prof Xavier MONNET Medical Intensive Care Unit Bicêtre Hospital Assistance publique Hôpitaux de Paris FRANCE Conflicts of interest Lilly GlaxoSmithKline Pulsion
Hemodynamic monitoring beyond cardiac output Prof Xavier MONNET Medical Intensive Care Unit Bicêtre Hospital Assistance publique Hôpitaux de Paris FRANCE Conflicts of interest Lilly GlaxoSmithKline Pulsion
Respiratory systolic variation test in acutely impaired cardiac function for predicting volume responsiveness in pigs
 British Journal of Anaesthesia 106 (5): 659 64 (2011) Advance Access publication 25 March 2011. doi:10.1093/bja/aer064 Respiratory systolic variation test in acutely impaired cardiac function for predicting
British Journal of Anaesthesia 106 (5): 659 64 (2011) Advance Access publication 25 March 2011. doi:10.1093/bja/aer064 Respiratory systolic variation test in acutely impaired cardiac function for predicting
Fluid responsiveness and extravascular lung water
 Fluid responsiveness and extravascular lung water Prof. Jean-Louis TEBOUL Medical ICU Bicetre hospital University Paris-South France Conflicts of interest Member of the Medical Advisory Board of Maquet/Pulsion
Fluid responsiveness and extravascular lung water Prof. Jean-Louis TEBOUL Medical ICU Bicetre hospital University Paris-South France Conflicts of interest Member of the Medical Advisory Board of Maquet/Pulsion
Fluid bolus of 20% Albumin in post-cardiac surgical patient: a prospective observational study of effect duration
 Fluid bolus of 20% Albumin in post-cardiac surgical patient: a prospective observational study of effect duration Investigators: Salvatore Cutuli, Eduardo Osawa, Rinaldo Bellomo Affiliations: 1. Department
Fluid bolus of 20% Albumin in post-cardiac surgical patient: a prospective observational study of effect duration Investigators: Salvatore Cutuli, Eduardo Osawa, Rinaldo Bellomo Affiliations: 1. Department
The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter
 1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter for continuous central venous oximetry (ScvO2) 3
1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the Edwards PreSep oximetry catheter for continuous central venous oximetry (ScvO2) 3
The effects of vasoactive drugs on pulse pressure and stroke volume variation in postoperative ventilated patients,
 Journal of Critical Care (211) 26, 328.e1 328.e8 The effects of vasoactive drugs on pulse pressure and stroke volume variation in postoperative ventilated patients, Mehrnaz Hadian MD a, Donald A. Severyn
Journal of Critical Care (211) 26, 328.e1 328.e8 The effects of vasoactive drugs on pulse pressure and stroke volume variation in postoperative ventilated patients, Mehrnaz Hadian MD a, Donald A. Severyn
Predicting fluid responsiveness in the intensive care unit: a clinical guide
 review Netherlands Journal of Critical Care Copyright 2008, Nederlandse Vereniging voor Intensive Care. All Rights Reserved. Received June 2008; accepted January 2009 Predicting fluid responsiveness in
review Netherlands Journal of Critical Care Copyright 2008, Nederlandse Vereniging voor Intensive Care. All Rights Reserved. Received June 2008; accepted January 2009 Predicting fluid responsiveness in
Using Functional Hemodynamic Indicators to Guide Fluid Therapy
 CE 2.6 HOURS Continuing Education Using Functional Hemodynamic Indicators to Guide Fluid Therapy A more accurate and less invasive way to gauge responsiveness to iv volume replacement. OVERVIEW: Hemodynamic
CE 2.6 HOURS Continuing Education Using Functional Hemodynamic Indicators to Guide Fluid Therapy A more accurate and less invasive way to gauge responsiveness to iv volume replacement. OVERVIEW: Hemodynamic
The cornerstone of treating patients with hypotension,
 Does the Central Venous Pressure Predict Fluid Responsiveness? An Updated Meta-Analysis and a Plea for Some Common Sense* Paul E. Marik, MD, FCCM 1 ; Rodrigo Cavallazzi, MD 2 Background: Aim: Data Sources:
Does the Central Venous Pressure Predict Fluid Responsiveness? An Updated Meta-Analysis and a Plea for Some Common Sense* Paul E. Marik, MD, FCCM 1 ; Rodrigo Cavallazzi, MD 2 Background: Aim: Data Sources:
ICU Volume 12 - Issue 4 - Winter 2012/ Matrix Features
 ICU Volume 12 - Issue 4 - Winter 2012/2013 - Matrix Features Fluid Management in Critically Ill Patients: A Guided Approach Prof. Antonio Artigas, MD, PhD ICU Management & Practice Editorial Board Member
ICU Volume 12 - Issue 4 - Winter 2012/2013 - Matrix Features Fluid Management in Critically Ill Patients: A Guided Approach Prof. Antonio Artigas, MD, PhD ICU Management & Practice Editorial Board Member
Sepsis Update: Focus on Early Recognition and Intervention. Disclosures
 Sepsis Update: Focus on Early Recognition and Intervention Jessie Roske, MD October 2017 Disclosures I have no actual or potential conflict of interest in relation to this program/presentation. I will
Sepsis Update: Focus on Early Recognition and Intervention Jessie Roske, MD October 2017 Disclosures I have no actual or potential conflict of interest in relation to this program/presentation. I will
Bioreactance-based passive leg raising test can predict fluid responsiveness in elderly patients with septic shock
 Original Article Page 1 of 6 Bioreactance-based passive leg raising test can predict fluid responsiveness in elderly patients with septic shock Caibao Hu 1 *, Guolong Cai 1 *, Jing Yan 1, Hongjie Tong
Original Article Page 1 of 6 Bioreactance-based passive leg raising test can predict fluid responsiveness in elderly patients with septic shock Caibao Hu 1 *, Guolong Cai 1 *, Jing Yan 1, Hongjie Tong
Tailored Volume Resuscitation in the Critically Ill is Achievable. Objectives. Clinical Case 2/16/2018
 Tailored Volume Resuscitation in the Critically Ill is Achievable Heath E Latham, MD Associate Professor Fellowship Program Director Pulmonary and Critical Care Objectives Describe the goal of resuscitation
Tailored Volume Resuscitation in the Critically Ill is Achievable Heath E Latham, MD Associate Professor Fellowship Program Director Pulmonary and Critical Care Objectives Describe the goal of resuscitation
Dynamic indices do not predict volume responsiveness in routine clinical practice
 British Journal of Anaesthesia 18 (3): 395 41 (212) Advance Access publication 2 December 211. doi:1.193/bja/aer411 CARDIOVASCULAR in routine clinical practice B. Lansdorp 1,2 *, J. Lemson 2, M. J. A.
British Journal of Anaesthesia 18 (3): 395 41 (212) Advance Access publication 2 December 211. doi:1.193/bja/aer411 CARDIOVASCULAR in routine clinical practice B. Lansdorp 1,2 *, J. Lemson 2, M. J. A.
Effects of passive leg raising and volume expansion on mean systemic pressure and venous return in shock in humans
 Guérin et al. Critical Care (2015) 19:411 DOI 10.1186/s13054-015-1115-2 RESEARCH Effects of passive leg raising and volume expansion on mean systemic pressure and venous return in shock in humans Laurent
Guérin et al. Critical Care (2015) 19:411 DOI 10.1186/s13054-015-1115-2 RESEARCH Effects of passive leg raising and volume expansion on mean systemic pressure and venous return in shock in humans Laurent
Sepsis Wave II Webinar Series. Sepsis Reassessment
 Sepsis Wave II Webinar Series Sepsis Reassessment Presenters Nova Panebianco, MD Todd Slesinger, MD Fluid Reassessment in Sepsis Todd L. Slesinger, MD, FACEP, FCCM, FCCP, FAAEM Residency Program Director
Sepsis Wave II Webinar Series Sepsis Reassessment Presenters Nova Panebianco, MD Todd Slesinger, MD Fluid Reassessment in Sepsis Todd L. Slesinger, MD, FACEP, FCCM, FCCP, FAAEM Residency Program Director
Chapter 6. Performance of three minimal invasive cardiac output monitoring systems
 Chapter 6 Performance of three minimal invasive cardiac output monitoring systems R.B.P. de Wilde 1, B.F. Geerts 2, J. Cui 3, P.C.M. van den Berg 4 and J.R.C. Jansen 5 1 Research Assistant, 2 Registrar,
Chapter 6 Performance of three minimal invasive cardiac output monitoring systems R.B.P. de Wilde 1, B.F. Geerts 2, J. Cui 3, P.C.M. van den Berg 4 and J.R.C. Jansen 5 1 Research Assistant, 2 Registrar,
Hemodynamic Monitoring Pressure or Volumes? Antonio Pesenti University of Milan Italy
 Hemodynamic Monitoring Pressure or Volumes? Antonio Pesenti University of Milan Italy antonio.pesenti@unimi.it CCCF 2017 Is it useful? YES: CVP It is an important diagnostic element! Your best guess CVP
Hemodynamic Monitoring Pressure or Volumes? Antonio Pesenti University of Milan Italy antonio.pesenti@unimi.it CCCF 2017 Is it useful? YES: CVP It is an important diagnostic element! Your best guess CVP
The effect of propofol on haemodynamics: cardiac output, venous return, mean systemic filling pressure, and vascular resistances
 British Journal of Anaesthesia, 116 (6): 784 9 (216) doi:.93/bja/aew126 Cardiovascular CARDIOVASCULAR The effect of propofol on haemodynamics: cardiac output, venous return, mean systemic filling pressure,
British Journal of Anaesthesia, 116 (6): 784 9 (216) doi:.93/bja/aew126 Cardiovascular CARDIOVASCULAR The effect of propofol on haemodynamics: cardiac output, venous return, mean systemic filling pressure,
Making the Case For Less Invasive Flow Based Parameters: APCO + SVV. Patricia A. Meehan, RN, MS, CCRN (a) Education Consultant Edwards Lifesciences
 Making the Case For Less Invasive Flow Based Parameters: APCO + SVV Patricia A. Meehan, RN, MS, CCRN (a) Education Consultant Edwards Lifesciences A New Gold Standard? How does the system work? Sensor
Making the Case For Less Invasive Flow Based Parameters: APCO + SVV Patricia A. Meehan, RN, MS, CCRN (a) Education Consultant Edwards Lifesciences A New Gold Standard? How does the system work? Sensor
Preload optimisation in severe sepsis and septic shock
 Preload optimisation in severe sepsis and septic shock Prof. Jean-Louis TEBOUL Medical ICU Bicetre hospital University Paris South France Conflicts of interest Member of themedical Advisory Board ofpulsion
Preload optimisation in severe sepsis and septic shock Prof. Jean-Louis TEBOUL Medical ICU Bicetre hospital University Paris South France Conflicts of interest Member of themedical Advisory Board ofpulsion
Invasive Cardiac Output Monitoring and Pulse Contour Analysis. Harshad B. Ranchod Paediatric Intensivist Chris Hani Baragwanath Hospital COPICON 2011
 Invasive Cardiac Output Monitoring and Pulse Contour Analysis Harshad B. Ranchod Paediatric Intensivist Chris Hani Baragwanath Hospital COPICON 2011 Introduction The primary goal of haemodynamic monitoring
Invasive Cardiac Output Monitoring and Pulse Contour Analysis Harshad B. Ranchod Paediatric Intensivist Chris Hani Baragwanath Hospital COPICON 2011 Introduction The primary goal of haemodynamic monitoring
Evaluation of Stroke Volume Variation Obtained by the FloTrac /Vigileo System to Guide Preoperative Fluid Therapy in Patients Undergoing Brain Surgery
 The Journal of International Medical Research 2012; 40: 1175 1181 [first published online as 40(3) 11] Evaluation of Stroke Volume Variation Obtained by the FloTrac /Vigileo System to Guide Preoperative
The Journal of International Medical Research 2012; 40: 1175 1181 [first published online as 40(3) 11] Evaluation of Stroke Volume Variation Obtained by the FloTrac /Vigileo System to Guide Preoperative
Original Article. Qiang Fu*, Feng Zhao*, Weidong Mi**, Hong Zhang. BioScience Trends. 2014; 8(1):
 BioScience Trends. 2014; 8(1):59-63. 59 Original Article DOI: 10.5582/bst.8.59 Stroke volume variation fail to predict fluid responsiveness in patients undergoing pulmonary lobectomy with one-lung ventilation
BioScience Trends. 2014; 8(1):59-63. 59 Original Article DOI: 10.5582/bst.8.59 Stroke volume variation fail to predict fluid responsiveness in patients undergoing pulmonary lobectomy with one-lung ventilation
Prediction of fluid responsiveness in patients during cardiac surgery
 British Journal of Anaesthesia 93 (6): 782 8 (24) doi:1.193/bja/aeh28 Advance Access publication October 1, 24 Prediction of fluid responsiveness in patients during cardiac surgery S. Rex 1 *, S. Brose
British Journal of Anaesthesia 93 (6): 782 8 (24) doi:1.193/bja/aeh28 Advance Access publication October 1, 24 Prediction of fluid responsiveness in patients during cardiac surgery S. Rex 1 *, S. Brose
British Journal of Anaesthesia 101 (6): (2008) doi: /bja/aen277 Advance Access publication October 12, 2008
 British Journal of Anaesthesia 11 (6): 761 8 (28) doi:1.193/bja/aen277 Advance Access publication October 12, 28 CARDIOVASCULAR Uncalibrated pulse contour-derived stroke volume variation predicts fluid
British Journal of Anaesthesia 11 (6): 761 8 (28) doi:1.193/bja/aen277 Advance Access publication October 12, 28 CARDIOVASCULAR Uncalibrated pulse contour-derived stroke volume variation predicts fluid
Goal-directed resuscitation in sepsis; a case-based approach
 Goal-directed resuscitation in sepsis; a case-based approach Jorge A Guzman, MD, FCCM Head, Section Critical Care Medicine Respiratory Institute Cleveland Clinic Foundation The challenges to managing septic
Goal-directed resuscitation in sepsis; a case-based approach Jorge A Guzman, MD, FCCM Head, Section Critical Care Medicine Respiratory Institute Cleveland Clinic Foundation The challenges to managing septic
The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the PreSep oximetry catheter for
 1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the PreSep oximetry catheter for continuous central venous oximetry (ScvO2) 3 The Vigileo
1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the PreSep oximetry catheter for continuous central venous oximetry (ScvO2) 3 The Vigileo
Predictive value of pulse pressure variation for fluid responsiveness in septic patients using lung-protective ventilation strategies
 British Journal of Anaesthesia 110 (3): 402 8 (2013) Advance Access publication 15 November 2012. doi:10.1093/bja/aes398 CRITICAL CARE Predictive value of pulse pressure variation for fluid responsiveness
British Journal of Anaesthesia 110 (3): 402 8 (2013) Advance Access publication 15 November 2012. doi:10.1093/bja/aes398 CRITICAL CARE Predictive value of pulse pressure variation for fluid responsiveness
Comparison of automated and static pulse respiratory mechanics during supported ventilation
 Comparison of automated and static pulse respiratory mechanics during supported ventilation Alpesh R Patel, Susan Taylor and Andrew D Bersten Respiratory system compliance ( ) and inspiratory resistance
Comparison of automated and static pulse respiratory mechanics during supported ventilation Alpesh R Patel, Susan Taylor and Andrew D Bersten Respiratory system compliance ( ) and inspiratory resistance
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency
 Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
Disclaimer. Improving MET-based patient care using treatment algorithms. Michael R. Pinsky, MD, Dr hc. Different Environments Demand Different Rules
 Michael R. Pinsky, MD - June 29, 26 Improving MET-based patient care using Michael R. Pinsky, MD, Dr hc Department of Critical Care Medicine University of Pittsburgh Disclaimer Michael R. Pinsky, MD is
Michael R. Pinsky, MD - June 29, 26 Improving MET-based patient care using Michael R. Pinsky, MD, Dr hc Department of Critical Care Medicine University of Pittsburgh Disclaimer Michael R. Pinsky, MD is
Editor s key points. Y. Song 1,2, Y. L. Kwak 1,2,3, J. W. Song 1,2, Y. J. Kim 1 and J. K. Shim 1,2 *
 British Journal of Anaesthesia 113 (1): 61 6 (2014) Advance Access publication 9 April 2014. doi:10.1093/bja/aeu057 Respirophasic carotid artery peak velocity variation as a predictor of fluid responsiveness
British Journal of Anaesthesia 113 (1): 61 6 (2014) Advance Access publication 9 April 2014. doi:10.1093/bja/aeu057 Respirophasic carotid artery peak velocity variation as a predictor of fluid responsiveness
Comparison of an automated respiratory systolic variation test with dynamic preload indicators to predict fluid responsiveness after major surgery
 British Journal of Anaesthesia 111 (5): 736 42 (213) Advance Access publication 27 June 213. doi:1.193/bja/aet24 CARDIOVASCULAR Comparison of an automated respiratory systolic variation test with dynamic
British Journal of Anaesthesia 111 (5): 736 42 (213) Advance Access publication 27 June 213. doi:1.193/bja/aet24 CARDIOVASCULAR Comparison of an automated respiratory systolic variation test with dynamic
Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy
 Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy A 44 year old female undergoing 10 hour Cytoreductive (CRS) procedure followed by Hyperthermic Intraperitoneal Chemotherapy (HIPEC).
Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy A 44 year old female undergoing 10 hour Cytoreductive (CRS) procedure followed by Hyperthermic Intraperitoneal Chemotherapy (HIPEC).
P. Grassi 1, L. Lo Nigro 2, K. Battaglia 1, M. Barone 2, F. Testa 2, G. Berlot 1,2 INTRODUCTION
 ORIGINAL ARTICLE HSR Proc Intensive Care Cardiovasc Anesth. 2013; 5(2): 98-109 98 Pulse pressure variation as a predictor of fluid responsiveness in mechanically ventilated patients with spontaneous breathing
ORIGINAL ARTICLE HSR Proc Intensive Care Cardiovasc Anesth. 2013; 5(2): 98-109 98 Pulse pressure variation as a predictor of fluid responsiveness in mechanically ventilated patients with spontaneous breathing
Prof. Dr. Iman Riad Mohamed Abdel Aal
 The Use of New Ultrasound Indices to Evaluate Volume Status and Fluid Responsiveness in Septic Shock Patients Thesis Submitted for partial fulfillment of MD degree in Anesthesiology, Surgical Intensive
The Use of New Ultrasound Indices to Evaluate Volume Status and Fluid Responsiveness in Septic Shock Patients Thesis Submitted for partial fulfillment of MD degree in Anesthesiology, Surgical Intensive
Purist? or Pragmatist? Assessment & Management of ICU Volume Status
 Assessment & Management of ICU Volume Status 9 th Annual Rocky Mountain Hospital Medicine Symposium Denver, Colorado Paula Dennen, MD Assistant Professor of Medicine Nephrology and Critical Care Medicine
Assessment & Management of ICU Volume Status 9 th Annual Rocky Mountain Hospital Medicine Symposium Denver, Colorado Paula Dennen, MD Assistant Professor of Medicine Nephrology and Critical Care Medicine
End-tidal carbon dioxide is better than arterial pressure for predicting volume responsiveness by the passive leg raising test
 Intensive Care Med DOI 10.1007/s00134-012-2693-y ORIGINAL Xavier Monnet Aurélien Bataille Eric Magalhaes Jérôme Barrois Marine Le Corre Clément Gosset Laurent Guerin Christian Richard Jean-Louis Teboul
Intensive Care Med DOI 10.1007/s00134-012-2693-y ORIGINAL Xavier Monnet Aurélien Bataille Eric Magalhaes Jérôme Barrois Marine Le Corre Clément Gosset Laurent Guerin Christian Richard Jean-Louis Teboul
Clinical implications of heart-lung interactions during mechanical ventilation: an update
 R e v i e w Clinical implications of heart-lung interactions during mechanical ventilation: an update L. Smeding 1, E. Lust 2, F.B. Plötz 1, A.B.J. Groeneveld 2* Departments of 1 Paediatric Intensive Care
R e v i e w Clinical implications of heart-lung interactions during mechanical ventilation: an update L. Smeding 1, E. Lust 2, F.B. Plötz 1, A.B.J. Groeneveld 2* Departments of 1 Paediatric Intensive Care
Volume Responsiveness in Critically Ill Patients
 SOUND JUDGMENT SERIES Volume Responsiveness in Critically Ill Patients Use of Sonography to Guide Management David Evans, MD, Giovanna Ferraioli, MD, John Snellings, MD, Alexander Levitov, MD Invited paper
SOUND JUDGMENT SERIES Volume Responsiveness in Critically Ill Patients Use of Sonography to Guide Management David Evans, MD, Giovanna Ferraioli, MD, John Snellings, MD, Alexander Levitov, MD Invited paper
Decrease in pulse pressure and stroke volume variations after mini-fluid challenge accurately predicts fluid responsiveness
 British Journal of Anaesthesia, 2015, 449 56 doi: 10.1093/bja/aev222 Advance Access Publication Date: 6 July 2015 Critical Care CRITICAL CARE Decrease in pulse pressure and stroke volume variations after
British Journal of Anaesthesia, 2015, 449 56 doi: 10.1093/bja/aev222 Advance Access Publication Date: 6 July 2015 Critical Care CRITICAL CARE Decrease in pulse pressure and stroke volume variations after
The Comparison of Stroke Volume Variation and Arterial Pressure Based Cardiac Output with Standard Hemodynamic Measurements during Cardiac Surgery
 ISPUB.COM The Internet Journal of Anesthesiology Volume 22 Number 2 The Comparison of Stroke Volume Variation and Arterial Pressure Based Cardiac Output with Standard H Liu, M Konia, Z Li, N Fleming Citation
ISPUB.COM The Internet Journal of Anesthesiology Volume 22 Number 2 The Comparison of Stroke Volume Variation and Arterial Pressure Based Cardiac Output with Standard H Liu, M Konia, Z Li, N Fleming Citation
Fluid responsiveness Monitoring in Surgical and Critically Ill Patients
 Fluid responsiveness Monitoring in Surgical and Critically Ill Patients Impact clinique de la Goal-directed-therapy Patrice FORGET, M.D Cliniques universitaires Saint Luc Université catholique de Louvain,
Fluid responsiveness Monitoring in Surgical and Critically Ill Patients Impact clinique de la Goal-directed-therapy Patrice FORGET, M.D Cliniques universitaires Saint Luc Université catholique de Louvain,
Arterial Pulse Pressure Variation During Positive Pressure Ventilation and Passive Leg Raising
 Arterial Pulse Pressure Variation During Positive Pressure Ventilation and Passive Leg Raising J.-L. Teboul, X. Monnet, and C. Richard Introduction Inadequate cardiac preload can play a major role in the
Arterial Pulse Pressure Variation During Positive Pressure Ventilation and Passive Leg Raising J.-L. Teboul, X. Monnet, and C. Richard Introduction Inadequate cardiac preload can play a major role in the
Edwards FloTrac Sensor & Performance Assessments of the FloTrac Sensor and Vigileo Monitor
 Edwards FloTrac Sensor & Edwards Vigileo Monitor Performance Assessments of the FloTrac Sensor and Vigileo Monitor 1 Topics System Configuration Performance and Validation Dr. William T. McGee, Validation
Edwards FloTrac Sensor & Edwards Vigileo Monitor Performance Assessments of the FloTrac Sensor and Vigileo Monitor 1 Topics System Configuration Performance and Validation Dr. William T. McGee, Validation
福島県立医科大学学術成果リポジトリ. Title laparoscopic adrenalectomy in patie pheochromocytoma. Midori; Iida, Hiroshi; Murakawa, Ma
 福島県立医科大学学術成果リポジトリ Examination of the usefulness of no Title variation monitoring for adjusting laparoscopic adrenalectomy in patie pheochromocytoma Isosu, Tsuyoshi; Obara, Shinju; Oha Author(s) Atsuyuki;
福島県立医科大学学術成果リポジトリ Examination of the usefulness of no Title variation monitoring for adjusting laparoscopic adrenalectomy in patie pheochromocytoma Isosu, Tsuyoshi; Obara, Shinju; Oha Author(s) Atsuyuki;
Nurse Driven Fluid Optimization Using Dynamic Assessments
 Nurse Driven Fluid Optimization Using Dynamic Assessments 2016 1 WHAT WE BELIEVE We believe that clinicians make vital fluid and drug decisions every day with limited and inconclusive information Cheetah
Nurse Driven Fluid Optimization Using Dynamic Assessments 2016 1 WHAT WE BELIEVE We believe that clinicians make vital fluid and drug decisions every day with limited and inconclusive information Cheetah
Dr. F Javier Belda Dept. Anesthesiology and Critical Care Hospital Clinico Universitario Valencia (Spain) Pulsion MAB
 State of the Art Hemodynamic Monitoring III CO, preload, lung water and ScvO2 The winning combination! Dr. F Javier Belda Dept. Anesthesiology and Critical Care Hospital Clinico Universitario Valencia
State of the Art Hemodynamic Monitoring III CO, preload, lung water and ScvO2 The winning combination! Dr. F Javier Belda Dept. Anesthesiology and Critical Care Hospital Clinico Universitario Valencia
escco, estimated Continuous Cardiac Output device DESEBBE OLIVIER SAUVEGARDE CLINIC, LYON, FRANCE
 escco, estimated Continuous Cardiac Output device DESEBBE OLIVIER SAUVEGARDE CLINIC, LYON, FRANCE No conflict of interest u Technology, based on Pulse Wave Transit Time u Limits of the technology u Precision
escco, estimated Continuous Cardiac Output device DESEBBE OLIVIER SAUVEGARDE CLINIC, LYON, FRANCE No conflict of interest u Technology, based on Pulse Wave Transit Time u Limits of the technology u Precision
Radboud University Nijmegen Medical Centre Why measure cardiac output in critically ill children?
 Radboud University Nijmegen Medical Centre Why measure cardiac output in critically ill children? J. Lemson Anesthesiologist/(pediatric)intensivist Case; Girl 2 years, 12 kg, severe meningococcal septic
Radboud University Nijmegen Medical Centre Why measure cardiac output in critically ill children? J. Lemson Anesthesiologist/(pediatric)intensivist Case; Girl 2 years, 12 kg, severe meningococcal septic
Goal-directed vs Flow-guidedresponsive
 Goal-directed vs Flow-guidedresponsive therapy S Magder Department of Critical Care, McGill University Health Centre Flow-directed vs goal directed strategy for management of hemodynamics S Magder Curr
Goal-directed vs Flow-guidedresponsive therapy S Magder Department of Critical Care, McGill University Health Centre Flow-directed vs goal directed strategy for management of hemodynamics S Magder Curr
FLUIDS AND SOLUTIONS IN THE CRITICALLY ILL. Daniel De Backer Department of Intensive Care Erasme University Hospital Brussels, Belgium
 FLUIDS AND SOLUTIONS IN THE CRITICALLY ILL Daniel De Backer Department of Intensive Care Erasme University Hospital Brussels, Belgium Why do we want to administer fluids? To correct hypovolemia? To increase
FLUIDS AND SOLUTIONS IN THE CRITICALLY ILL Daniel De Backer Department of Intensive Care Erasme University Hospital Brussels, Belgium Why do we want to administer fluids? To correct hypovolemia? To increase
Review Article. Interactive Physiology in Critical Illness : Pulmonary and Cardiovascular Systems. Introduction
 310 Indian Deepak J Physiol Shrivastava Pharmacol 2016; 60(4) : 310 314 Indian J Physiol Pharmacol 2016; 60(4) Review Article Interactive Physiology in Critical Illness : Pulmonary and Cardiovascular Systems
310 Indian Deepak J Physiol Shrivastava Pharmacol 2016; 60(4) : 310 314 Indian J Physiol Pharmacol 2016; 60(4) Review Article Interactive Physiology in Critical Illness : Pulmonary and Cardiovascular Systems
EVOLUCIÓN DE LA MONITORIZACIÓN CARDIOVASCULAR EN LA UCI
 EVOLUCIÓN DE LA MONITORIZACIÓN CARDIOVASCULAR EN LA UCI Antonio Artigas Critical Care Center Sabadell Hospital CIBER Enfermedades Respiratorias Autonomos University of Barcelona Spain aartigas@tauli.cat
EVOLUCIÓN DE LA MONITORIZACIÓN CARDIOVASCULAR EN LA UCI Antonio Artigas Critical Care Center Sabadell Hospital CIBER Enfermedades Respiratorias Autonomos University of Barcelona Spain aartigas@tauli.cat
Cardiac Output Monitoring - 6
 Cardiac Output Monitoring - 6 How to use Wrexham s Cardiac Output Monitors. Wrexham Maelor Critical Care Version 02.05.16 Introduction Types of Devices: NICOM - Cheetah Oesophageal Doppler +/- Pulse Contour
Cardiac Output Monitoring - 6 How to use Wrexham s Cardiac Output Monitors. Wrexham Maelor Critical Care Version 02.05.16 Introduction Types of Devices: NICOM - Cheetah Oesophageal Doppler +/- Pulse Contour
Shock, Monitoring Invasive Vs. Non Invasive
 Shock, Monitoring Invasive Vs. Non Invasive Paula Ferrada MD Assistant Professor Trauma, Critical Care and Emergency Surgery Virginia Commonwealth University Shock Fluid Pressors Ionotrope Intervention
Shock, Monitoring Invasive Vs. Non Invasive Paula Ferrada MD Assistant Professor Trauma, Critical Care and Emergency Surgery Virginia Commonwealth University Shock Fluid Pressors Ionotrope Intervention
Functional Hemodynamic Monitoring and Management A practical Approach
 Functional Hemodynamic Monitoring and Management A practical Approach Daniel A. Reuter Center of Anesthesiology and Intensive Care Medicine Hamburg-Eppendorf University Hospital Hamburg, Germany Euronaesthesia
Functional Hemodynamic Monitoring and Management A practical Approach Daniel A. Reuter Center of Anesthesiology and Intensive Care Medicine Hamburg-Eppendorf University Hospital Hamburg, Germany Euronaesthesia
Mechanical Ventilation & Cardiopulmonary Interactions: Clinical Application in Non- Conventional Circulations. Eric M. Graham, MD
 Mechanical Ventilation & Cardiopulmonary Interactions: Clinical Application in Non- Conventional Circulations Eric M. Graham, MD Background Heart & lungs work to meet oxygen demands Imbalance between supply
Mechanical Ventilation & Cardiopulmonary Interactions: Clinical Application in Non- Conventional Circulations Eric M. Graham, MD Background Heart & lungs work to meet oxygen demands Imbalance between supply
Hemodynamic Monitoring in Critically ill Patients in Arthur Simonnet, interne Tuteur : Pr. Raphaël Favory
 Hemodynamic Monitoring in Critically ill Patients in 2017 Arthur Simonnet, interne Tuteur : Pr. Raphaël Favory Rationale for Hemodynamic Monitoring Identify the presence of hemodynamic instability Identify
Hemodynamic Monitoring in Critically ill Patients in 2017 Arthur Simonnet, interne Tuteur : Pr. Raphaël Favory Rationale for Hemodynamic Monitoring Identify the presence of hemodynamic instability Identify
Division of Perioperative and Emergency Medicine, University Medical Center Utrecht, the Netherlands
 04RC1 Advances in cardiovascular monitoring Wolfgang Buhre Division of Perioperative and Emergency Medicine, University Medical Center Utrecht, the Netherlands Saturday, 11 June 2011 13:00-13:45 Room:
04RC1 Advances in cardiovascular monitoring Wolfgang Buhre Division of Perioperative and Emergency Medicine, University Medical Center Utrecht, the Netherlands Saturday, 11 June 2011 13:00-13:45 Room:
The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the PreSep oximetry catheter for
 1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the PreSep oximetry catheter for continuous central venous oximetry (ScvO 2 ) 3 The Vigileo
1 2 The Vigileo monitor by Edwards Lifesciences supports both the FloTrac Sensor for continuous cardiac output and the PreSep oximetry catheter for continuous central venous oximetry (ScvO 2 ) 3 The Vigileo
Assessing fluid responses after coronary surgery: role of mathematical coupling of global end-diastolic volume to
 954 Original article Assessing fluid responses after coronary surgery: role of mathematical coupling of global end-diastolic volume to cardiac output measured by transpulmonary thermodilution Rose-Marieke
954 Original article Assessing fluid responses after coronary surgery: role of mathematical coupling of global end-diastolic volume to cardiac output measured by transpulmonary thermodilution Rose-Marieke
Utility of transthoracic echocardiography (TTE) in assessing fluid responsiveness in critically ill patients a challenge for the bedside sonographer
 Continuing education Med Ultrason 2016, Vol. 18, no. 4, -514 DOI: 10.11152/mu-880 Utility of transthoracic echocardiography (TTE) in assessing fluid responsiveness in critically ill patients a challenge
Continuing education Med Ultrason 2016, Vol. 18, no. 4, -514 DOI: 10.11152/mu-880 Utility of transthoracic echocardiography (TTE) in assessing fluid responsiveness in critically ill patients a challenge
Clinical Applications of The Pleth. Variability Index (PVI):
 Clinical Applications of The Pleth. Variability Index (PVI): A non invasive and continuous monitoring of fluid responsiveness J.PIRSON, MD 26 nov. 2011 Preoperative hypovolemia after an overnight fasting
Clinical Applications of The Pleth. Variability Index (PVI): A non invasive and continuous monitoring of fluid responsiveness J.PIRSON, MD 26 nov. 2011 Preoperative hypovolemia after an overnight fasting
How can the PiCCO improve protocolized care?
 How can the PiCCO improve protocolized care? Azriel Perel Professor and Chairman Department of Anesthesiology and Intensive Care Sheba Medical Center, Tel Aviv University, Israel ESICM, Vienna 2009 Disclosure
How can the PiCCO improve protocolized care? Azriel Perel Professor and Chairman Department of Anesthesiology and Intensive Care Sheba Medical Center, Tel Aviv University, Israel ESICM, Vienna 2009 Disclosure
Department of Intensive Care Medicine UNDERSTANDING CIRCULATORY FAILURE IN SEPSIS
 Department of Intensive Care Medicine UNDERSTANDING CIRCULATORY FAILURE IN SEPSIS UNDERSTANDING CIRCULATORY FAILURE IN SEPSIS a mismatch between tissue perfusion and metabolic demands the heart, the vasculature
Department of Intensive Care Medicine UNDERSTANDING CIRCULATORY FAILURE IN SEPSIS UNDERSTANDING CIRCULATORY FAILURE IN SEPSIS a mismatch between tissue perfusion and metabolic demands the heart, the vasculature
FLUID RESUSCITATION AND MONITORING IN SEPSIS PROTOCOLIZED VS USUAL CARE DEEPA BANGALORE GOTUR MD, FCCP ASSISTANT PROFESSOR, WEILL CORNELL MEDICAL
 FLUID RESUSCITATION AND MONITORING IN SEPSIS PROTOCOLIZED VS USUAL CARE DEEPA BANGALORE GOTUR MD, FCCP ASSISTANT PROFESSOR, WEILL CORNELL MEDICAL COLLEGE NOVEMBER 10 TH 2017 TEXAS SCCM SYMPOSIUM Disclosures
FLUID RESUSCITATION AND MONITORING IN SEPSIS PROTOCOLIZED VS USUAL CARE DEEPA BANGALORE GOTUR MD, FCCP ASSISTANT PROFESSOR, WEILL CORNELL MEDICAL COLLEGE NOVEMBER 10 TH 2017 TEXAS SCCM SYMPOSIUM Disclosures
PCV and PAOP Old habits die hard!
 PCV and PAOP Old habits die hard! F Javier Belda MD, PhD Head of Department Associate Professor Anaesthesia and Critical Care Hospital Clínico Universitario Valencia (SPAIN) An old example TOBACO SMOKING
PCV and PAOP Old habits die hard! F Javier Belda MD, PhD Head of Department Associate Professor Anaesthesia and Critical Care Hospital Clínico Universitario Valencia (SPAIN) An old example TOBACO SMOKING
Review Article Echocardiographic Assessment of Preload Responsiveness in Critically Ill Patients
 Cardiology Research and Practice Volume 2012, Article ID 819696, 7 pages doi:10.1155/2012/819696 Review Article Echocardiographic Assessment of Preload Responsiveness in Critically Ill Patients Alexander
Cardiology Research and Practice Volume 2012, Article ID 819696, 7 pages doi:10.1155/2012/819696 Review Article Echocardiographic Assessment of Preload Responsiveness in Critically Ill Patients Alexander
Cardiac Output (C.O.) Regulation of Cardiac Output
 Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Cardiac output by Portapres
 Clinical Science (2004) 106, 407 412 (Printed in Great Britain) 407 Cardiac output by Portapres Marjorie S. PITT, Paul MARSHALL, Jonathan P. DIESCH and Roger HAINSWORTH Institute for Cardiovascular Research,
Clinical Science (2004) 106, 407 412 (Printed in Great Britain) 407 Cardiac output by Portapres Marjorie S. PITT, Paul MARSHALL, Jonathan P. DIESCH and Roger HAINSWORTH Institute for Cardiovascular Research,
Impedance Cardiography (ICG) Method, Technology and Validity
 Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
WE NEED TO REDISCOVER PHYSIOLOGY!
 WE NEED TO REDISCOVER PHYSIOLOGY! MERVYN SINGER BLOOMSBURY INSTITUTE OF INTENSIVE CARE MEDICINE UNIVERSITY COLLEGE LONDON, UK DECLARATIONS OF INTEREST GE Healthcare (manufacturer of Venue ultrasound/echo)
WE NEED TO REDISCOVER PHYSIOLOGY! MERVYN SINGER BLOOMSBURY INSTITUTE OF INTENSIVE CARE MEDICINE UNIVERSITY COLLEGE LONDON, UK DECLARATIONS OF INTEREST GE Healthcare (manufacturer of Venue ultrasound/echo)
Useful Ectopics: Case Study. Effects of vasodilation and the diagnostic value of ectopic heartbeats
 Effects of vasodilation and the diagnostic value of ectopic heartbeats 83 year old man, weight 66 kg, height 177 cm, BSA 1.82m 2. Closure of colostomy. No cardiac history. Screenshot 1 Baseline at start
Effects of vasodilation and the diagnostic value of ectopic heartbeats 83 year old man, weight 66 kg, height 177 cm, BSA 1.82m 2. Closure of colostomy. No cardiac history. Screenshot 1 Baseline at start
The Hemodynamic Puzzle
 The Hemodynamic Puzzle SVV NIRS O 2 ER Lactate Energy Metabolism (Oxygen Consumption) (Ml/min/m 2 ) Oxygen Debt: To Pay or Not to Pay? Full Recovery Possible Delayed Repayment of O 2 Debt Oxygen Deficit
The Hemodynamic Puzzle SVV NIRS O 2 ER Lactate Energy Metabolism (Oxygen Consumption) (Ml/min/m 2 ) Oxygen Debt: To Pay or Not to Pay? Full Recovery Possible Delayed Repayment of O 2 Debt Oxygen Deficit
Echocardiography Volume assessment. Justin Mandeville 2014
 Echocardiography Volume assessment Justin Mandeville 2014 Volume assessment and the intensivist Hypovolaemic shock Fluid tolerance Optimising cardiac output Avoiding overloading Guided fluid removal Add
Echocardiography Volume assessment Justin Mandeville 2014 Volume assessment and the intensivist Hypovolaemic shock Fluid tolerance Optimising cardiac output Avoiding overloading Guided fluid removal Add
Michael T. Ganter 1, Martin Geisen 2, Sonja Hartnack 3, Omer Dzemali 4 and Christoph K. Hofer 2*
 Ganter et al. BMC Anesthesiology (2018) 18:55 https://doi.org/10.1186/s12871-018-0520-x RESEARCH ARTICLE Open Access Prediction of fluid responsiveness in mechanically ventilated cardiac surgical patients:
Ganter et al. BMC Anesthesiology (2018) 18:55 https://doi.org/10.1186/s12871-018-0520-x RESEARCH ARTICLE Open Access Prediction of fluid responsiveness in mechanically ventilated cardiac surgical patients:
Admission of patient CVICU and hemodynamic monitoring
 Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
Admission of patient CVICU and hemodynamic monitoring Prepared by: Rami AL-Khatib King Fahad Medical City Pi Prince Salman Heart tcentre CVICU-RN Admission patient to CVICU Introduction All the patients
The Use of Dynamic Parameters in Perioperative Fluid Management
 The Use of Dynamic Parameters in Perioperative Fluid Management Gerard R. Manecke Jr., M.D. Chief, Cardiac Anesthesia UCSD Medical Center San Diego, CA, USA Thanks to Tom Higgins, M.D. 1 Goals of today
The Use of Dynamic Parameters in Perioperative Fluid Management Gerard R. Manecke Jr., M.D. Chief, Cardiac Anesthesia UCSD Medical Center San Diego, CA, USA Thanks to Tom Higgins, M.D. 1 Goals of today
Chapter 3. An evaluation of cardiac output by five arterial pulse contour techniques during cardiac surgery
 Chapter 3 An evaluation of cardiac output by five arterial pulse contour techniques during cardiac surgery R.B.P. de Wilde 1, J.J. Schreuder 2, P.C.M. van den Berg 1 and J.R.C. Jansen 1 1 Department of
Chapter 3 An evaluation of cardiac output by five arterial pulse contour techniques during cardiac surgery R.B.P. de Wilde 1, J.J. Schreuder 2, P.C.M. van den Berg 1 and J.R.C. Jansen 1 1 Department of
Echocardiography to guide fluid therapy in critically ill patients: check the heart and take a quick look at the lungs
 Editorial Echocardiography to guide fluid therapy in critically ill patients: check the heart and take a quick look at the lungs Federico Franchi 1 *, Luigi Vetrugno 2 *, Sabino Scolletta 1 1 Department
Editorial Echocardiography to guide fluid therapy in critically ill patients: check the heart and take a quick look at the lungs Federico Franchi 1 *, Luigi Vetrugno 2 *, Sabino Scolletta 1 1 Department
Actualités sur le remplissage peropératoire. Philippe Van der Linden MD, PhD
 Actualités sur le remplissage peropératoire Philippe Van der Linden MD, PhD Fees for lectures, advisory board and consultancy: Fresenius Kabi GmbH B Braun Medical SA Perioperative Fluid Volume Administration
Actualités sur le remplissage peropératoire Philippe Van der Linden MD, PhD Fees for lectures, advisory board and consultancy: Fresenius Kabi GmbH B Braun Medical SA Perioperative Fluid Volume Administration
3/14/2017. Disclosures. None. Outline. Fluid Management and Hemodynamic Assessment Paul Marik, MD, FCCP, FCCM
 Fluid Management and Hemodynamic Assessment Paul Marik, MD, FCCP, FCCM Disclosures Stocks Advisory boards Grants Speakers Bureau None Outline Hemodynamic Goals Fluid Resuscitation Historical Perspective
Fluid Management and Hemodynamic Assessment Paul Marik, MD, FCCP, FCCM Disclosures Stocks Advisory boards Grants Speakers Bureau None Outline Hemodynamic Goals Fluid Resuscitation Historical Perspective
Anesthesiology, V 110, No 5, May
 Anesthesiology 2009; 110:1092 7 Copyright 2009, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Influence of Respiratory Rate on Stroke Volume Variation in Mechanically
Anesthesiology 2009; 110:1092 7 Copyright 2009, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Influence of Respiratory Rate on Stroke Volume Variation in Mechanically
DESIGNER RESUSCITATION: TITRATING TO TISSUE NEEDS
 DESIGNER RESUSCITATION: TITRATING TO TISSUE NEEDS R. Phillip Dellinger MD, MSc, MCCM Professor and Chair of Medicine Cooper Medical School of Rowan University Chief of Medicine Cooper University Hospital
DESIGNER RESUSCITATION: TITRATING TO TISSUE NEEDS R. Phillip Dellinger MD, MSc, MCCM Professor and Chair of Medicine Cooper Medical School of Rowan University Chief of Medicine Cooper University Hospital
Hemodynamic Monitoring To Guide Volume Resuscitation
 Hemodynamic Monitoring To Guide Volume Resuscitation Nick Johnson, MD Acting Assistant Professor Division of Emergency Medicine Attending Physician, Medical & Neuro-Intensive Care Units Harborview Medical
Hemodynamic Monitoring To Guide Volume Resuscitation Nick Johnson, MD Acting Assistant Professor Division of Emergency Medicine Attending Physician, Medical & Neuro-Intensive Care Units Harborview Medical
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Relax and Learn At the Farm 2012
 Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Standard Operating Procedure (SOP) Management of intervention group patients SOP 001
 ` Standard Operating Procedure (SOP) Management of intervention group patients SOP 001 Authors: Mark Edwards & Rupert Pearse Authorisation: Rupert Pearse (Chief Investigator) Scope To provide guidance
` Standard Operating Procedure (SOP) Management of intervention group patients SOP 001 Authors: Mark Edwards & Rupert Pearse Authorisation: Rupert Pearse (Chief Investigator) Scope To provide guidance
Handling Common Problems & Pitfalls During. Oxygen desaturation in patients receiving mechanical ventilation ACUTE SEVERE RESPIRATORY FAILURE
 Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Sepsis overview. Dr. Tsang Hin Hung MBBS FHKCP FRCP
 Sepsis overview Dr. Tsang Hin Hung MBBS FHKCP FRCP Epidemiology Sepsis, severe sepsis, septic shock Pathophysiology of sepsis Recent researches and advances From bench to bedside Sepsis bundle Severe sepsis
Sepsis overview Dr. Tsang Hin Hung MBBS FHKCP FRCP Epidemiology Sepsis, severe sepsis, septic shock Pathophysiology of sepsis Recent researches and advances From bench to bedside Sepsis bundle Severe sepsis
FloTrac Sensor and Edwards PreSep Central Venous Oximetry Catheter Case Presentations
 Edwards FloTrac Sensor & Edwards Vigileo Monitor FloTrac Sensor and Edwards PreSep Central Venous Oximetry Catheter Case Presentations 1 Topics System Configuration FloTrac Sensor and PreSep Catheter Thoracotomy
Edwards FloTrac Sensor & Edwards Vigileo Monitor FloTrac Sensor and Edwards PreSep Central Venous Oximetry Catheter Case Presentations 1 Topics System Configuration FloTrac Sensor and PreSep Catheter Thoracotomy
Rounds in the ICU. Eran Segal, MD Director General ICU Sheba Medical Center
 Rounds in the ICU Eran Segal, MD Director General ICU Sheba Medical Center Real Clinical cases (including our mistakes) Emphasis on hemodynamic monitoring Usually no single correct answer We will conduct
Rounds in the ICU Eran Segal, MD Director General ICU Sheba Medical Center Real Clinical cases (including our mistakes) Emphasis on hemodynamic monitoring Usually no single correct answer We will conduct
