Observing Renal Responses to Endurance Cycling in the Heat
|
|
|
- Nathaniel Melton
- 5 years ago
- Views:
Transcription
1 University of Arkansas, Fayetteville Theses and Dissertations Observing Renal Responses to Endurance Cycling in the Heat Cody Smith University of Arkansas, Fayetteville Follow this and additional works at: Part of the Exercise Science Commons Recommended Citation Smith, Cody, "Observing Renal Responses to Endurance Cycling in the Heat" (2016). Theses and Dissertations This Thesis is brought to you for free and open access by It has been accepted for inclusion in Theses and Dissertations by an authorized administrator of For more information, please contact
2 Observing Renal Responses to Endurance Cycling in the Heat A thesis submitted in partial fulfillment of the requirements for the degree of Master of Science in Kinesiology by Cody Reed Smith University of Arkansas Bachelor of Science in Education, 2010 August 2016 University of Arkansas This thesis is approved for recommendation to the Graduate Council Dr. Brendon McDermott Thesis Director Dr. Matthew Ganio Committee Member Dr. Stavros Kavouras Committee Member
3 Abstract AIM: To observe the effects of endurance cycling in the heat on renal function, and determine if the extent of impairment is related to hydration. METHODS: 40 cyclists (34 male, 6 female, 52 ± 9 y, 21.7 ± 6.5 % body fat) completed an endurance cycling event (5.7 ± 1.2 hours) in the heat (33.2 ± 5.0ºC, 38.4 ± 10.7% RH). Body mass was assessed to determine net fluid loss, muscle damage in the legs was assessed with a pain scale, a urine sample was collected to analyze hydration status, and a blood sample was drawn. All measurements were taken pre- and postevent. Serum creatinine was measured by colorimetric assay and analyzed via the Jaffe reaction, and creatinine clearance was estimated. An ELISA kit was used to measure serum neutrophil gelatinase-associated lipocalin. RESULTS: A net fluid loss of 1.3 ± 1.1 kg was observed. Urine specific gravity (P < 0.001) and leg muscle pain (P < 0.001) increased post-event. Serum creatinine increased from pre- (0.52 ± 0.14 mg/dl) to post-event (0.88 ± 0.21 mg/dl; P < 0.001). Creatinine clearance decreased from pre- (160.9 ± 48.9 ml/min) to post-event (95.2 ± 28.1 ml/min; P < 0.001). Serum neutrophil gelatinase-associated lipocalin increased from pre- (68.51 ± 17.54) to post-event ( ± 36.52; P < 0.001) CONCLUSION: Changes observed in renal measures suggest acute kidney injury and reduced kidney function after endurance cycling in the heat.
4 Table of Contents I. Introduction... 1 II. Review of Literature III. Methodology. 7 IV. Manuscript V. Discussion References. 22 Tables and Figures 24 Appendix 33
5 I. Introduction Strenuous running (1-3) and cycling (4) has been reported to compromise kidney function. A decrease in estimated creatinine clearance (CCr) from serum to urine as a result of reduced renal blood flow during exercise suggests this finding (4, 5). The kidneys play a vital role in maintaining fluid and electrolyte balance by filtering and excreting metabolic waste products from blood into urine, while also reabsorbing essential molecules such as water, glucose and amino acids. In a homeostatic state, the kidneys are supplied via the renal arteries with 20% of cardiac output. Each kidney has many nephrons that together produce 180 liters of filtrate each day, of which an estimated 2 liters are excreted in urine. Upon reaching the kidney, blood flows to the nephron through the afferent arteriole and subsequently into the glomerular capillaries. Molecules are then filtered from the blood through the capillaries into the renal corpuscle, and the filtrate is either reabsorbed into the peritubular capillaries or excreted in urine. The rate at which molecules are filtered through the kidneys is known as the glomerular filtration rate (GFR). Creatinine (Cr) is a muscle metabolic waste product that can be measured in serum and in urine to estimate GFR and subsequently manifest renal function. Cr is produced by the breakdown of creatine phosphate by creatine kinase, and is released into the blood stream where it is eventually filtered through the kidneys and excreted in urine. In a normal functioning kidney, the CCr in the blood is equal to the concentration of creatinine that is filtered and excreted in urine (6). Two determinants that contribute to an increase in serum creatinine (scr) are hydration status (7) and skeletal muscle damage (8). Hydration status is more important when exercising in the heat due to the loss of water via increased sweat rate and 1
6 respiration (9). Skeletal muscle damage is less common during exercise cycling versus running due to the lack of eccentric contractions of working skeletal muscle (4, 10). Other studies involving endurance events have examined the kidney biomarker neutrophil gelatinase-associated lipocalin (NGAL) as an early indicator of acute kidney injury (AKI) during exercise (7, 11, 12). AKI is a result of renal tissue damage that can occur during strenuous endurance exercise as a result of renal ischemia. NGAL is a glycoprotein that is synthesized as a result of inflamed epithelial cells in several human tissues such as uterus, prostate, lung, stomach, and kidney (13). Dramatic upregulation of NGAL is found in proximal tubules of mice within 3 hours of ischemic renal injury, leading to its suggested use of determining AKI in humans (14). Although NGAL has been thoroughly studied in clinical settings there is a need for further research to observe instances and determine causes of AKI in humans after strenuous exercise. II. Review of Literature During exercise, renal blood flow is reduced to as low as 25% of resting values as a result of renal blood vessel vasoconstriction (15). Reduction in blood flow to the kidneys is exacerbated by the effects of dehydration, particularly while exercising in the heat (9). A common assessment of dehydration involves participants to void their bladder before exercise, drink water to replenish fluid loss during exercise, and examine the difference in body weight post exercise. A greater loss of body weight during exercise suggests greater dehydration. Neviackas and Bauer reported 3.0 to 4.0kg were lost during warm weather marathon running versus just 2.0 to 2.5kg lost during cold weather marathon running (16). This finding suggests that exercising in the heat can lead to a greater reduction of renal blood flow than exercising in the cold. 2
7 Fluid replacement while running can be difficult to achieve due to the swinging motion of the arms to maintain balance and the unstable effect the movement of the legs have on the body. Therefore, replacing the amount of fluid necessary for maintaining hydration can be difficult during a marathon run in which great amounts of fluid are lost over a long period of exercise. Cycling, however, allows free use of the arm and a steady posture of the body, which can facilitate drinking during exercise. Neumayr et al. reported a moderate weight loss of 1.7kg, as well as no significant difference in urine osmolarity from pre to post event while marathon cycling in a cold environment (4). These findings, along with the findings from Neviackas et al., suggest a need to examine the effects of hydration status on the kidneys while endurance cycling in the heat. Dehydration decreases blood volume, reducing renal blood flow. Reductions in renal blood flow, and subsequent reductions in GFR, are increased when dehydration is associated with exercise in a hot environment (17). Otani et al. found that when full fluid loss is replaced during heavy exercise in a hot environment, dehydration is attenuated and GFR is unchanged (18). Conversely, when fluid is ingested voluntarily dehydration is augmented and GFR is reduced (18). Reduced GFR results in increased concentration of waste products in the blood, which leads to the method by which GFR can be estimated creatinine clearance. As a muscle metabolic waste product, creatinine is filtered from the blood and excreted in urine. Creatinine clearance is commonly assessed by observing the increase in SCr before and after insult. When renal function is impaired the filtration of waste products is reduced as evidenced by an increase in SCr. Therefore, decreases in creatinine clearance suggest detriments in renal function. The Acute Kidney Injury Network (AKIN) defines AKI as a 50% increase or an absolute increase of 0.3 mg/dl in SCr (19). Endurance running requires eccentric muscle 3
8 contractions resulting in muscle damage (10) leading to increases in creatinine in the blood immediately following exercise (1). Kao et al. found associations between increased plasma creatinine and reduced kidney function in ultramarathon runners (20). These findings present the question of whether muscle damage during endurance running overloads the kidney filtration system with creatinine or reductions in renal blood flow is the main contributor to increases in SCr. Using creatinine as a marker to assess kidney injury is questionable since increases in SCr could be only a reflection of the renal filtration system. Therefore, creatinine may be better described as a marker of kidney function instead of injury. Reductions in creatinine clearance are directly related to the intensity of exercise (15). Although many studies observing renal function have incorporated endurance running, endurance cycling has been examined as well (4, 21). Differences in mechanics while running and cycling reduce the likelihood to eccentrically contract leg muscles while cycling, resulting in reduced muscle damage (10). Neumayr et al. found that renal function is minimally altered during strenuous endurance cycling (4, 21). They hypothesized that exercise induced reduction of renal blood flow is likely the cause of decreases found in creatinine clearance since muscle damage was not identified (4). Further research of endurance cycling in a hot environment is necessary to verify this hypothesis as hypohydration could reduce renal blood flow even greater than their results. Cr has historically been used to diagnose AKI, but recent research has recognized NGAL as a more accurate and earlier marker of renal injury. Clinical research of NGAL has primarily investigated the biomarker s synthesis in rodents and human patients with induced or confirmed renal injury, respectively. Mishra et al. found NGAL to be a sensitive urinary biomarker for early detection of ischemic renal injury in mice (22). Interestingly, scr levels were normal in this study despite kidney injury, further suggesting Cr as a poor marker for AKI. In a study of 635 4
9 patients, single measurements of NGAL in urine helped distinguish AKI from CKD, azotemia and normal function (23). Makris et al. reported urinary NGAL as an early detector of AKI in severe trauma patients (24). While NGAL has been identified as a reliable marker of AKI in clinical settings, its application in exercise settings requires more research. In a study by McCullough et al., plasma NGAL (pngal) was measured in runners before and after a marathon in the cold, and then 24 hours after finishing the run. Results of this study showed a dramatic rise in pngal immediately after the race, but the levels returned to near baseline after 24 hours (12). Junglee et al. also found a significant increase in pngal after a heat stressed running protocol following exercise induced muscle damage (7). Furthermore, the increase in pngal was suggested to be a result of inflammation from the muscle damaging exercise (7). Lippi et al. observed NGAL variations in athletes after an ultramarathon run in cold weather and found an almost two fold increase in sngal (11). Based on these three studies involving running protocols strenuous running exercise could lead to AKI. However, to the best of our knowledge, there are no cycling protocols in which scr and sngal have been measured to observe renal function and assess potential injury. Electrolyte concentration has been reported to change post marathon running (1, 25). Fallon et al. found increased serum sodium (sna) and chloride (scl) levels post event, while Kratz et al. reported no change in sna or serum potassium (sk) but decreased scl levels post event (1, 25). Neumayr et al. reported increased sk and unchanged sna and scl post marathon cycling (4). Kratz et al. hypothesized that differences in fluid intake may be the cause of differences in post exercise serum electrolyte concentrations (25). Neumayr et al. found that urine was more dilute post-race, surmising that fluid replacement while cycling is more sufficient than that of runners who observe greater urine concentration post event (4). 5
10 Fluid replacement can become dangerous when fluid is replaced at a higher rate than necessary. Although insufficient replacement of fluid causes dehydration, over sufficient replacement of fluid could result in hyponatremia (26). Hyponatremia is characterized by an unsafe decrease in Na in the blood and could result in exhaustion, unconsciousness, and even death. The normal reference range of sna is mmol/l (25). Therefore, sna levels below 135 mmol/l are classified as hyponatremic. Urine sodium (una) levels are important to monitor as well. When filtered through healthy kidneys, Na is mostly reabsorbed before urine is excreted and a relatively low concentration of Na remains in urine. Irving et al. found that serum electrolytes were increased and una was decreased after ultramarathon running (3). Neumayr et al. also reported lower una post marathon cycling (4). Neither Irving et al. nor Neumayr et al. found differences in hydration, suggesting that proper fluid replacement during exercise may reduce sna imbalance. Fractional excretion of sodium (FENa) can be measured to determine how well the renal tubules are functioning to reabsorb molecules into the blood stream. Junglee et al. reported that a significant reduction in FENa after exercising in the heat suggests kidney stress due to higher energy demands from increased Na-K-ATPase activity in the renal tubules (7). The limited research available observing the effects of endurance cycling on renal function has been performed in environments lacking heat stress, and no research has measured preferred kidney injury markers. With knowledge of the effects of heat on fluid balance during exercise, an observational study of the effects of endurance cycling in a hot environment on the kidneys should be conducted. Based on previous research, we hypothesize: 1) that renal function will be minimally impaired due to normalized CCr as a result of attenuated muscle damage, 2) that hypohydration and alterations in electrolyte concentrations will be observed due to a lack of 6
11 sufficient fluid replacement, and 3) that sngal values will increase dramatically, possibly due to renal ischemia as a result of hypohydration and heat effects. III. Methodology Participants in either the 100 mile or 100 kilometer 2015 Hotter n Hell Hundred event (HHH) (33.2 ± 5.0ºC, 38.4 ± 10.7% RH) were recruited to participate in this study. During the two days leading up to the event a station was set up near the HHH expo with information about the study. Researchers actively sought and requested the participation of cyclists who were visiting the expo. Cyclists interested in participating were briefed of the details of the study, as described below, and what was required of them throughout the next couple of days. Upon being recruited and verbally consenting to participation, participants completed a medical history questionnaire. Participants were asked to comply with exclusion criteria including: medical condition or medication that alters body fluid balance, dietary manipulation that omits one nutrient or class of nutrients, present musculoskeletal injury, and use of tobacco products. An investigator then took 3-site skin fold measures to assess body composition using the Brozek equation (26). Those who were able and willing to participate in the study signed an informed consent document. The morning of the event, before starting HHH, participants arrived to our station where body mass was measured using a standard scale (Health-o-med 349 KLX, McCook, IL), a urine sample was collected, and a blood sample (50mL) was drawn via venipuncture of a cubital vein into a vacutainer serum separating tube where it remained in a vertical position until the blood clotted. After clotting, the sample was spun in a centrifuge at 1500 g for 10 minutes to separate serum from whole blood. Serum was then be aliquoted into a microcentrifuge tube and frozen 7
12 until analysis. Urine specific gravity (USG) and urine color (hydrationcheck.com) was assessed immediately to determine hydration status. Once analyzed for hydration, urine samples were aliquoted into microcentrifuge tubes and frozen. Serum and urine samples were stored in the tubes and frozen in coolers with dry ice until transported back to the laboratory. Immediately after HHH was completed participants returned to our station where body mass was assessed, a urine sample was collected, and a blood sample (50mL) was drawn. Urine was assessed immediately to determine hydration status. Serum and urine samples were stored in microcentrifuge tubes and frozen for transport as described before. Once transported to the laboratory, samples were frozen at -80 C until analysis. Samples were removed from the freezer at least one hour before analysis to ensure thawing. Preand post-urine and serum sodium, potassium and chloride concentrations were measured and recorded in duplicate via ion-sensitive electrodes. Pre- and post-event scr and ucr was measured in duplicate by colorimetric assay and analyzed via the Jaffe reaction. CCr was calculated via the Cockcroft and Gault formula (27). sngal was measured via commercially based ELISA kit as per instructions (R&D Systems, Minneapolis, MN). FENa was calculated using the equation [(una scr) (sna ucr) 100]. Pre- and post-event body mass difference was used to determine net fluid loss. Paired samples T- tests were used to determine whether sngal or scr concentrations were statistically different pre- and post-event, and whether any electrolyte measures were statistically different post-event compared to pre-event. Correlation tests were used to determine the cause of any differences in NGAL and Cr. An alpha level of 0.05 was set a priori. IV. Manucript 8
13 Introduction Strenuous running (1-3) and cycling (4) has been reported to compromise kidney function. A decrease in estimated creatinine clearance (CCr) from the blood to urine as a result of reduced renal blood flow during exercise suggests this finding (4, 5). The kidneys play a vital role in maintaining fluid and electrolyte balance by filtering and excreting metabolic waste products from the blood into urine, while also reabsorbing essential molecules such as water, glucose and amino acids. The rate at which molecules are filtered through the kidneys is known as the glomerular filtration rate (GFR). Creatinine (Cr) is a muscle metabolic waste product that is filtered from the blood to urine. Cr can be measured in serum and in urine to estimate GFR and subsequently manifest renal function. Therefore, an increase in scr and a subsequent decrease in CCr suggests detriments in renal function. In a normal functioning kidney, the concentration of Cr in the blood is equal to the concentration of Cr that is filtered and excreted in urine (6). Therefore, observing an increase in serum creatinine (scr) would reveal a decrease in CCr. Two determinants that contribute to an increase in scr are hydration status (7) and skeletal muscle damage (8). Hydration status is important when exercising in the heat due to the loss of water via increased sweat rate and respiration (9). Skeletal muscle damage is less common during exercise cycling versus running due to the lack of eccentric contractions of working skeletal muscle (4, 10). Reductions in CCr are directly related to the intensity of exercise (11). Although studies observing renal function during exercise have mostly incorporated endurance running, endurance cycling has been examined as well (4, 12). Differences in mechanics while running and cycling reduce the likelihood to eccentrically contract leg muscles while cycling, resulting in reduced muscle damage (10). Neumayr et al. found that renal function is minimally altered during 9
14 strenuous endurance cycling (4, 12). They hypothesized that exercise induced reduction of renal blood flow is likely the cause of decreases found in CCr since muscle damage was not identified (4). Further research of endurance cycling in a hot environment is necessary to verify this hypothesis as hypohydration could reduce renal blood flow even greater than their results. During exercise, renal blood flow is reduced to as low as 25% of resting values as a result of renal blood vessel vasoconstriction (11). A reduction in blood flow to the kidneys is exacerbated by the effects of dehydration, particularly while exercising in the heat (9). Dehydration decreases blood volume, reducing renal blood flow. Replenishing fluid losses during exercise can augment blood volume, increase the amount of blood available to flow to the kidneys, and subsequently diminish the effects of dehydration. A greater loss of body weight during exercise suggests a lack of fluid replacement and greater dehydration. Neviackas and Bauer reported 3.0 to 4.0 kg were lost during warm weather marathon running versus just 2.0 to 2.5 kg lost during cold weather marathon running (13). This finding suggests that exercising in the heat can lead to a greater reduction of renal blood flow than exercising in the cold. Reductions in renal blood flow, and subsequent reductions in GFR, are increased when dehydration is associated with exercise in a hot environment due to greater fluid loss through increased sweating (14). Otani et al. found that when full fluid loss is replaced during heavy exercise in a hot environment, dehydration is attenuated and GFR is unchanged (15). Conversely, when fluid is ingested voluntarily dehydration is augmented and GFR is reduced (15). Fluid replacement is simpler while cycling versus running due to the differences in stability and the use of the hands. Neumayr et al. reported a moderate weight loss of 1.7 kg, as well as no significant difference in urine osmolarity from pre- to post-event while marathon cycling in a cold environment (4). These findings, along with the findings from Neviackas et al., suggest a 10
15 need to examine the effects of hydration status on the kidneys while endurance cycling in the heat. Neumayr et al. found that urine was more dilute post-race, surmising that fluid replacement while cycling is more sufficient than that of runners who observe greater urine concentration post event (4). Fractional excretion of sodium (FENa) determines how well the renal tubules are functioning to reabsorb molecules into the blood stream. Junglee et al. reported that a significant reduction in FENa after exercising in the heat suggests kidney stress due to higher energy demands from increased Na-K-ATPase activity in the renal tubules (7). Studies involving endurance exercise have examined the biomarker neutrophil gelatinaseassociated lipocalin (NGAL) as an early indicator of acute kidney injury (AKI) during exercise (7, 16, 17). AKI is a result of renal tissue damage that can occur during strenuous endurance exercise as a result of renal ischemia. NGAL is a glycoprotein that is synthesized as a result of inflamed epithelial cells in several human tissues such as uterus, prostate, lung, stomach, and kidney (18). Dramatic upregulation of NGAL is found in the proximal tubules of mice within 3 hours of ischemic renal injury, leading to its suggested use of determining AKI in humans (19). Though NGAL has been thoroughly studied in clinical settings (19-21), there is a need for further research to observe instances of AKI in humans during endurance exercise. The Acute Kidney Injury Network (AKIN) defines AKI as a 50% increase or an absolute increase of 0.3 mg/dl in scr (22). Endurance running requires eccentric muscle contractions resulting in muscle damage (10) leading to increases in creatinine in the blood immediately following exercise (1). Kao et al. found associations between increased plasma creatinine and reduced kidney function in ultramarathon runners (23). These findings present the question of whether muscle-damaging exercise overloads the kidney filtration system with creatinine, or if a 11
16 reduction in renal blood flow is the main contributor to increases in scr. The use of creatinine as a marker to assess kidney injury is questionable as increases in scr could only be a reflection of the renal filtration system. Therefore, creatinine may be best utilized as a marker of kidney function instead of injury. In a study by McCullough et al., plasma NGAL (pngal) was measured in runners before and after a marathon in the cold, and then 24 hours after finishing the run. They found a dramatic rise in pngal immediately after the race, but the levels returned to near baseline after 24 hours (17). Junglee et al. found a two-fold increase in pngal, which exceeded their reported normal range ( ng/ml), after a heat stressed running protocol following exercise induced muscle damage (7). Furthermore, the increase in pngal was suggested to be a result of inflammation from the muscle damaging exercise (7). Lippi et al. observed NGAL variations in athletes after an ultramarathon run in cold weather and found an almost two fold increase in sngal (16). Based on these three studies involving running protocols, endurance running could lead to AKI. However, to the best of our knowledge, there are no cycling protocols in the heat that have measured scr and sngal to observe renal function and assess potential injury. The limited research available observing the effects of endurance cycling on renal function has been performed in environments lacking heat stress, and no research has measured preferred kidney injury markers. Therefore, the purpose of this study is to observe renal function and potential instances of AKI during endurance cycling in the heat. Methods The present study was designed to observe kidney function and instances of AKI in cyclists participating in an endurance event in the heat. The event was completed the same day it was 12
17 started and all measurements were taken the days leading up to and the day of the event. No variables were controlled, but this study was in collaboration with another study investigating NSAID use. Therefore, some of the participants took ibuprofen before the event. This study was approved by the University of Arkansas Institutional Review Board. Participants in either the 100 mi or 100 km 2015 Hotter n Hell Hundred event (HHH)(33.2 ± 5.0ºC, 38.4 ± 10.7% RH) were recruited to participate in this study. During the two days leading up to the event a station was set up near the HHH expo with information about the study. Researchers actively sought and requested the participation of cyclists who were visiting the expo. Cyclists interested in participating were briefed of the details of the study, as described below, and what was required of them throughout the next couple of days. Upon being recruited and consenting to participation, participants completed a medical history questionnaire. Exclusion criteria for this study included: medical condition or medication that alters body fluid balance, dietary manipulation that omits one nutrient or class of nutrients, present musculoskeletal injury, and use of tobacco products. Those who were able and willing to participate in the study signed an informed consent document. An investigator then measured body mass and took 3-site skin fold measures to assess body composition using the Brozek equation (24). The morning of the event, before starting HHH, participants arrived to our station where body mass was measured using a standard scale (Health-o-med 349 KLX, McCook, IL), a urine sample was collected, and a blood sample (50mL) was drawn via venipuncture of a cubital vein into a vacutainer serum separating tube where it remained in a vertical position until the blood clotted. After clotting, the sample was spun in a centrifuge at 1500 g for 10 minutes to separate serum from whole blood. Serum was then be aliquoted into a microcentrifuge tube and frozen 13
18 until analysis. Urine specific gravity (USG) and urine color (hydrationcheck.com) was assessed immediately to determine hydration status. Once analyzed for hydration, urine samples were aliquoted into microcentrifuge tubes and frozen. Serum and urine samples were stored in the tubes and frozen in coolers with dry ice until transported back to the laboratory. Participants were asked about their perceived pain in the legs and overall pain from a 0-10 muscle pain scale (25) pre- and post-event. Immediately after HHH was completed participants returned to our station where body mass was assessed, a urine sample was collected, and a blood sample (50mL) was drawn. Urine was assessed immediately to determine hydration status. Serum and urine samples were stored in microcentrifuge tubes and frozen for transport as described before. Once transported to the laboratory, samples were frozen at -80 C until analysis. Samples were removed from the freezer at least one hour before analysis to ensure thawing. Preand post-urine and serum sodium, potassium and chloride concentrations were measured and recorded in duplicate via ion-sensitive electrodes (Medica EasyElectrolyes, Bedford, MA). Preand post-event scr and ucr was measured in duplicate by colorimetric assay and analyzed via the Jaffe reaction. CCr was calculated via the Cockcroft and Gault formula (26). A commercially based ELISA kit was used to measure sngal as per instructions (R&D Systems, Minneapolis, MN). FENa was calculated using the equation [(una scr) (sna ucr) 100]. Pre- and post-event body mass difference was used to determine net fluid loss. Paired samples t- tests were used to determine any pre- versus post-event differences. Spearman s rho correlation tests were used to determine any relationships between select variables. An alpha level of 0.05 was set a priori. 14
19 Results Forty cyclists (34 male, 6 female) who completed the event (100 mi = 31, 100 km = 9) participated in this study. Average race time was 5.7 ± 1.2 hours and average body mass difference was -1.3 ± 1.1 kg (-1.6 ± 1.4 %, P < 0.001). Table 1 displays the demographic information of the participants included in our analysis. Pre- and post-event scr, sngal, CCr, muscle pain, and FENa results are displayed in Table 2 and hydration status results are displayed in Table 3. sngal increased ± ng/ml from pre- to post-event, approximately a two-fold increase (P < 0.001) as displayed in Figure 1. scr increased 0.32 ± 0.22 mg/dl from pre- to post-event, a 62% increase (P < 0.001), as displayed in Figure 2. Figure 3 shows a 60.9 ± 42.4 ml/min decrease (P < 0.001) in CCr from pre- to post-event. Table 4 is a correlation matrix displaying post-event relationships of sngal, scr and CCr with hydration status, muscle pain, FENa, and finish time. Another correlation matrix of the relationships between changes in preand post-event sngal, scr and CCr with hydration status, muscle pain, FENa, and finish time is shown in Table 5. Table 6 displays all electrolyte results. Discussion Our main findings were that endurance cycling in the heat resulted in renal function impairment and AKI based on decreases in CCr and increases in sngal (7, 17). The absolute increase in scr was consistent with the AKIN definition of AKI, but as mentioned earlier scr may not be the best variable to determine AKI (22). Interestingly, the identified rise in sngal was independent of hydration status and muscle pain, suggesting for the first time that AKI could result from heat exposure in an endurance exercise event. An increase in scr suggests that renal function was reduced. Although hydration status significantly decreased, which can contribute to increases in scr (7), there was no relationship 15
20 found between the two in the present study. There was a significant decrease in body mass, however it was moderate in comparison to the study by Neumayr et al. which was performed in a cool environment and it was also not related to scr (4). Therefore, our findings suggest that any potential renal blood flow impairment would be a result of the demands of blood elsewhere in the body during endurance exercise in the heat. Environmental conditions likely reduced renal blood flow and could have induced kidney stress. Endurance exercise combined with heat stress increases sweating which requires an increase in blood flow to the skin (14). As mentioned earlier, renal blood flow is reduced to as low at 25% during exercise and has even greater consequences when blood volume is reduced by dehydration (11). FENa was significantly reduced and in agreement with the results of Juglee et al. which further suggests heat stress contributes to kidney stress during exercise (7). CCr was reduced post-event which suggests renal function impairment during exercise in the heat. However, there were no correlations between CCr and any of the variables that would suggest that the reduction in CCr is related to hydration status, muscle damage, FENa, or heat exposure. Our findings are consistent with those of a cycling protocol by Neumayr et al. who suggested that exercise-induced renal blood flow reduction leads to a decrease in CCr (4). However, the difference between our study and that of Neumayr et al. is not only environmental conditions, but length of cycling as well. Cyclists in the present study rode for almost half the time of those in the study by Neumayr et al. Therefore, the duration of cycling exercise and the subsequent amount of time in which renal blood flow is reduced may play a role in the severity of kidney stress. Further research involving a shorter duration of cycling exercise should be conducted in order to determine the onset of renal function reduction. 16
21 Unlike the results of a similar cycling study by Neumayr and colleagues, we found an increase in muscle pain in the legs which would lead to the conclusion that there was muscle damage during the event (4). Furthermore, we found that muscle pain the legs post-event was related to the increase in scr. Our differing results could be due to the variances in terrain cycled between the two studies. Neumayr et al. performed their protocol in the mountains in Austria while the present study was conducted in a mostly flat area of Texas. With changes in elevation there are more opportunities to not need to pedal and thus not use the leg muscles, while on a flat course there would be a need for pedaling almost throughout the event. sngal more than doubled from pre- to post-event and reached a level consistent with previous studies involving a running protocol which observed AKI in exercise protocols (7, 17). Results from clinical studies suggests that an upregulation in serum is due to ischemic renal injury (19, 20). However, like the results of Cr, sngal results were not linked to hydration status or muscle pain. Therefore, it could be suggested that dehydration combined with endurance exercise, heat stress, or both may bring about AKI during endurance exercise. Unlike Junglee et al., who s protocol was designed to induce muscle damage, we did not find that the increase in sngal was related to muscle pain (7). Our results show sngal was increased to a level much greater than both McCullough et al. and Junglee et al. found, but was closest to the results of Junglee et al. (7, 17). Finish time was equated as the time from when the participants started the event until the time they finished, and tells how long they were exposed to the heat. Post-event sngal had a tendency to relate to finish time, suggesting for the first time that AKI could be due to heat exposure during exercise. This could be caused by several mechanistic physiological responses to the heat such as renal ischemia due to increased blood flow to the skin or decreased blood 17
22 volume. Participants were exposed to the heat for almost 6 hours during the present study compared to just 40 minutes in the study by Junglee et al., which may explain the greater level of sngal post-event in the present study (7). Because both studies induced increases in NGAL consistent with AKI, the differing suggested causes may not be mutually exclusive. Muscle damaging exercise as well as long periods of heat exposure while exercising may have a similar effect on the kidneys. In conclusion, endurance cycling in the heat stresses the kidneys and could result in AKI. While hydration and muscle pain do not have a direct relationship with these findings, the combination of them with the duration of heat exposure while exercising may increase the likelihood of renal stress and injury. Limitations We were unable to collect data the day following the event and therefore could not determine if the participants biomarkers recovered to baseline levels. It is also unknown if instances of AKI accumulated over time leads to CKD. Future research should investigate the role of AKI during exercise in CKD. 18
23 V. Discussion Our main findings were that endurance cycling in the heat resulted in renal function impairment and AKI based on decreases in CCr and increases in sngal (7, 17). The absolute increase in scr was consistent with the AKIN definition of AKI, but as mentioned earlier scr may not be the best variable to determine AKI (22). Interestingly, the identified rise in sngal was independent of hydration status and muscle pain, suggesting for the first time that AKI could result from heat exposure in an endurance exercise event. An increase in scr suggests that renal function was reduced. Although hydration status significantly decreased, which can contribute to increases in scr (7), there was no relationship found between the two in the present study. There was a significant decrease in body mass, however it was moderate in comparison to the study by Neumayr et al. which was performed in a cool environment and it was also not related to scr (4). Therefore, our findings suggest that any potential renal blood flow impairment would be a result of the demands of blood elsewhere in the body during endurance exercise in the heat. Environmental conditions likely reduced renal blood flow and could have induced kidney stress. Endurance exercise combined with heat stress increases sweating which requires an increase in blood flow to the skin (14). As mentioned earlier, renal blood flow is reduced to as low at 25% during exercise and has even greater consequences when blood volume is reduced by dehydration (11). FENa was significantly reduced and in agreement with the results of Juglee et al. which further suggests heat stress contributes to kidney stress during exercise (7). CCr was reduced post-event which suggests renal function impairment during exercise in the heat. However, there were no correlations between CCr and any of the variables that would suggest that the reduction in CCr is related to hydration status, muscle damage, FENa, or heat 19
24 exposure. Our findings are consistent with those of a cycling protocol by Neumayr et al. who suggested that exercise-induced renal blood flow reduction leads to a decrease in CCr (4). However, the difference between our study and that of Neumayr et al. is not only environmental conditions, but length of cycling as well. Cyclists in the present study rode for almost half the time of those in the study by Neumayr et al. Therefore, the duration of cycling exercise and the subsequent amount of time in which renal blood flow is reduced may play a role in the severity of kidney stress. Further research involving a shorter duration of cycling exercise should be conducted in order to determine the onset of renal function reduction. Unlike the results of a similar cycling study by Neumayr and colleagues, we found an increase in muscle pain in the legs which would lead to the conclusion that there was muscle damage during the event (4). Furthermore, we found that muscle pain the legs post-event was related to the increase in scr. Our differing results could be due to the variances in terrain cycled between the two studies. Neumayr et al. performed their protocol in the mountains in Austria while the present study was conducted in a mostly flat area of Texas. With changes in elevation there are more opportunities to not need to pedal and thus not use the leg muscles, while on a flat course there would be a need for pedaling almost throughout the event. sngal more than doubled from pre- to post-event and reached a level consistent with previous studies involving a running protocol which observed AKI in exercise protocols (7, 17). Results from clinical studies suggests that an upregulation in serum is due to ischemic renal injury (19, 20). However, like the results of Cr, sngal results were not linked to hydration status or muscle pain. Therefore, it could be suggested that dehydration combined with endurance exercise, heat stress, or both may bring about AKI during endurance exercise. Unlike Junglee et al., who s protocol was designed to induce muscle damage, we did not find that the increase in sngal was 20
25 related to muscle pain (7). Our results show sngal was increased to a level much greater than both McCullough et al. and Junglee et al. found, but was closest to the results of Junglee et al. (7, 17). Finish time was equated as the time from when the participants started the event until the time they finished, and tells how long they were exposed to the heat. Post-event sngal had a tendency to relate to finish time, suggesting for the first time that AKI could be due to heat exposure during exercise. This could be caused by several mechanistic physiological responses to the heat such as renal ischemia due to increased blood flow to the skin or decreased blood volume. Participants were exposed to the heat for almost 6 hours during the present study compared to just 40 minutes in the study by Junglee et al., which may explain the greater level of sngal post-event in the present study (7). Because both studies induced increases in NGAL consistent with AKI, the differing suggested causes may not be mutually exclusive. Muscle damaging exercise as well as long periods of heat exposure while exercising may have a similar effect on the kidneys. In conclusion, endurance cycling in the heat stresses the kidneys and could result in AKI. While hydration and muscle pain do not have a direct relationship with these findings, the combination of them with the duration of heat exposure while exercising may increase the likelihood of renal stress and injury. 21
26 References 1. Fallon KE, Sivyer G, Sivyer K, Dare A. The biochemistry of runners in a 1600 km ultramarathon. Br J Sports Med. 1999;33(4): Irving RA, Noakes TD, Buck R, van Zyl Smit R, Raine E, Godlonton J, et al. Evaluation of renal function and fluid homeostasis during recovery from exercise-induced hyponatremia. J Appl Physiol (1985). 1991;70(1): Irving RA, Noakes TD, Burger SC, Myburgh KH, Querido D, van Zyl Smit R. Plasma volume and renal function during and after ultramarathon running. Med Sci Sports Exerc. 1990;22(5): Neumayr G, Pfister R, Hoertnagl H, Mitterbauer G, Getzner W, Ulmer H, et al. The effect of marathon cycling on renal function. Int J Sports Med. 2003;24(2): Suzuki M, Sudoh M, Matsubara S, Kawakami K, Shiota M, Ikawa S. Changes in renal blood flow measured by radionuclide angiography following exhausting exercise in humans. Eur J Appl Physiol Occup Physiol. 1996;74(1-2): Perrone RD, Madias NE, Levey AS. Serum creatinine as an index of renal function: new insights into old concepts. Clin Chem. 1992;38(10): Junglee NA, Di Felice U, Dolci A, Fortes MB, Jibani MM, Lemmey AB, et al. Exercising in a hot environment with muscle damage: effects on acute kidney injury biomarkers and kidney function. Am J Physiol Renal Physiol. 2013;305(6):F Armstrong RB. Muscle damage and endurance events. Sports Med. 1986;3(5): Costill DL. Sweating: its composition and effects on body fluids. Ann N Y Acad Sci. 1977;301: Williams KR. The relationship between mechanical and physiological energy estimates. Med Sci Sports Exerc. 1985;17(3): Lippi G, Sanchis-Gomar F, Salvagno GL, Aloe R, Schena F, Guidi GC. Variation of serum and urinary neutrophil gelatinase associated lipocalin (NGAL) after strenuous physical exercise. Clin Chem Lab Med. 2012;50(9): McCullough PA, Chinnaiyan KM, Gallagher MJ, Colar JM, Geddes T, Gold JM, et al. Changes in renal markers and acute kidney injury after marathon running. Nephrology (Carlton). 2011;16(2): Cowland JB, Borregaard N. Molecular characterization and pattern of tissue expression of the gene for neutrophil gelatinase-associated lipocalin from humans. Genomics. 1997;45(1):
27 14. Devarajan P. Biomarkers for the early detection of acute kidney injury. Curr Opin Pediatr. 2011;23(2): Poortmans JR. Exercise and renal function. Sports Med. 1984;1(2): Neviackas JA, Bauer JH. Renal function abnormalities induced by marathon running. South Med J. 1981;74(12): SMITH JH, ROBINSON S, PEARCY M. Renal responses to exercise, heat and dehydration. J Appl Physiol. 1952;4(8): Otani H, Kaya M, Tsujita J. Effect of the volume of fluid ingested on urine concentrating ability during prolonged heavy exercise in a hot environment. J Sports Sci Med. 2013;12(1): Kao WF, Hou SK, Chiu YH, Chou SL, Kuo FC, Wang SH, et al. Effects of 100-km ultramarathon on acute kidney injury. Clin J Sport Med. 2015;25(1): Neumayr G, Pfister R, Hoertnagl H, Mitterbauer G, Prokop W, Joannidis M. Renal function and plasma volume following ultramarathon cycling. Int J Sports Med. 2005;26(1): Mishra J, Ma Q, Prada A, Mitsnefes M, Zahedi K, Yang J, et al. Identification of neutrophil gelatinase-associated lipocalin as a novel early urinary biomarker for ischemic renal injury. J Am Soc Nephrol. 2003;14(10): Nickolas TL, O'Rourke MJ, Yang J, Sise ME, Canetta PA, Barasch N, et al. Sensitivity and specificity of a single emergency department measurement of urinary neutrophil gelatinaseassociated lipocalin for diagnosing acute kidney injury. Ann Intern Med. 2008;148(11): Makris K, Markou N, Evodia E, Dimopoulou E, Drakopoulos I, Ntetsika K, et al. Urinary neutrophil gelatinase-associated lipocalin (NGAL) as an early marker of acute kidney injury in critically ill multiple trauma patients. Clin Chem Lab Med. 2009;47(1): Kratz A, Lewandrowski KB, Siegel AJ, Chun KY, Flood JG, Van Cott EM, et al. Effect of marathon running on hematologic and biochemical laboratory parameters, including cardiac markers. Am J Clin Pathol. 2002;118(6): von Duvillard SP, Arciero PJ, Tietjen-Smith T, Alford K. Sports drinks, exercise training, and competition. Curr Sports Med Rep. 2008;7(4): BROZEK J, GRANDE F, ANDERSON JT, KEYS A. DENSITOMETRIC ANALYSIS OF BODY COMPOSITION: REVISION OF SOME QUANTITATIVE ASSUMPTIONS. Ann N Y Acad Sci. 1963;110: Gault MH, Longerich LL, Harnett JD, Wesolowski C. Predicting glomerular function from adjusted serum creatinine. Nephron. 1992;62(3):
28 Tables and Figures Table 1. Demographic information (n = 40) expressed as mean ± standard deviation. Age (years) 52 ± 9 Height (cm) ± 18.2 Body Mass (kg) 84.5 ± 16.1 Body Fat (%) 21.7 ±
29 Table 2. Pre- and post-event measurements expressed as mean ± standard deviation when appropriate. Pre-event Post-event P-value sngal (ng/ml) ± ± <0.001 scr (mg/dl) 0.53 ± ± 0.19 <0.001 CCr (ml/min) ± ± 29.1 <0.001 Muscle Pain (legs) 0 ± 1 1 ± 2 <0.001 Muscle Pain (overall) 0 ± 1 1 ± Fractional Excretion Na (%) 0.52 ± ± 0.18 <
30 Table 3. Hydration status measurements pre- and post- event expressed as mean ± standard deviation. Pre-event Post-event P-value Urine Specific Gravity ± ± Color 2 ± 1 3 ± 1 <0.001 Body Mass (kg) 84.5 ± ± 15.9 <
31 Table 4. Correlation matrix of post-event measurements expressed as Spearman s rho and P- value. sngal scr CCr USG Correlation Coefficient Sig. (2-tailed) N Body Mass Loss Correlation Coefficient Sig. (2-tailed) N Leg Pain Overall Pain FENa Finish Time Correlation Coefficient Sig. (2-tailed) N Correlation Coefficient Sig. (2-tailed) N Correlation Coefficient Sig. (2-tailed) N Correlation Coefficient Sig. (2-tailed) N * Correlation is significant at the 0.01 level *
32 Table 5. Correlation matrix of the changes in pre- and post-event measurements expressed as Spearman s rho correlation coefficient and P-value. sngal scr CCr USG Correlation Coefficient Sig. (2-tailed) N Body Mass Loss Correlation Coefficient Sig. (2-tailed) N Leg Pain Correlation Coefficient Sig. (2-tailed) N Overall Pain Correlation Coefficient Sig. (2-tailed) N FENa Finish Time Correlation Coefficient Sig. (2-tailed) N Correlation Coefficient Sig. (2-tailed) N
33 Table 6. Electrolyte measurements pre- and post- event expressed as mean ± standard deviation. Pre-event Post-event P-value sna (mmol/l) ± ± sk (mmol/l) 4.4 ± ± scl (mmol/l) ± ± una (mmol/l) 95.8 ± ± 33.9 <0.001 uk (mmol/l) 34.6 ± ± 38.4 <0.001 ucl (mmol/l) ± ±
34 * sngal (ng/ml) Pre-Event Time point Post-Event Figure 1. sngal measurements pre- and post-event expressed as means (SD). * Indicates significantly different than pre-event (P < 0.001). 30
35 1.20 * 1.00 scr (ng/ml) Pre-Event Time point Post-Event Figure 2. scr measurements pre- and post-event expressed as means (SD). * Indicates significantly different than pre-event (P < 0.001). 31
36 * CCr (ml/min) Pre-Event Time point Post-Event Figure 3. CCr measurements pre- and post-event expressed as means (SD). * Indicates significantly different than pre-event (P < 0.001). 32
37 Appendix IRB Approval Letter 33
Daily Variability of Body Weight and Hydration Markers in Free Living Men and Women
 University of Arkansas, Fayetteville ScholarWorks@UARK Theses and Dissertations 12-2016 Daily Variability of Body Weight and Hydration Markers in Free Living Men and Women Lynndee Grace Summers University
University of Arkansas, Fayetteville ScholarWorks@UARK Theses and Dissertations 12-2016 Daily Variability of Body Weight and Hydration Markers in Free Living Men and Women Lynndee Grace Summers University
Biomarkers of renal diseases. By Dr. Gouse Mohiddin Shaik
 By Dr. Gouse Mohiddin Shaik Introduction Renal system performs several functions Excretory Waste products like urea, creatinine, drug, toxins clearance Regulatory Water, electrolyte and acid base balance
By Dr. Gouse Mohiddin Shaik Introduction Renal system performs several functions Excretory Waste products like urea, creatinine, drug, toxins clearance Regulatory Water, electrolyte and acid base balance
Introduction to Clinical Diagnosis Nephrology
 Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
Introduction to Clinical Diagnosis Nephrology I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of Florida College
Filtration and Reabsorption Amount Filter/d
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
1. remove: waste products: urea, creatinine, and uric acid foreign chemicals: drugs, water soluble vitamins, and food additives, etc.
 Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
BIOL 2402 Renal Function
 BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
Bio 322 Human Anatomy Objectives for the laboratory exercise Urinary System Filtration Reabsorption Secretion Concentration
 Bio 322 Human Anatomy Objectives for the laboratory exercise Urinary System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 25 For this lab you will use parts
Bio 322 Human Anatomy Objectives for the laboratory exercise Urinary System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 25 For this lab you will use parts
12/7/10. Excretory System. The basic function of the excretory system is to regulate the volume and composition of body fluids by:
 Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
The kidney. (Pseudo) Practical questions. The kidneys are all about keeping the body s homeostasis. for questions Ella
 The kidney (Pseudo) Practical questions for questions Ella (striemit@gmail.com) The kidneys are all about keeping the body s homeostasis Ingestion Product of metabolism H 2 O Ca ++ Cl - K + Na + H 2 O
The kidney (Pseudo) Practical questions for questions Ella (striemit@gmail.com) The kidneys are all about keeping the body s homeostasis Ingestion Product of metabolism H 2 O Ca ++ Cl - K + Na + H 2 O
HYDRATION & EXERCISE : IMPLICATIONS FOR KIDNEY HEALTH
 64 TH AMERICAN COLLEGE OF SPORTS MEDICINE ANNUAL MEETING HYDRATION & EXERCISE : IMPLICATIONS FOR KIDNEY HEALTH May 31 st 5.30pm-7.00pm Room 103 Colorado Convention Center Denver AGENDA Session chaired
64 TH AMERICAN COLLEGE OF SPORTS MEDICINE ANNUAL MEETING HYDRATION & EXERCISE : IMPLICATIONS FOR KIDNEY HEALTH May 31 st 5.30pm-7.00pm Room 103 Colorado Convention Center Denver AGENDA Session chaired
Dr.Nahid Osman Ahmed 1
 1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
CONTROLLING THE INTERNAL ENVIRONMENT
 AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
UNIT 3 Conditions supporting life
 Biology Form 4 Page 32 Ms. R. Buttigieg UNIT 3 Conditions supporting life In this unit we shall be seeing how an important condition that supports life is the ability of the organism to maintain a constant
Biology Form 4 Page 32 Ms. R. Buttigieg UNIT 3 Conditions supporting life In this unit we shall be seeing how an important condition that supports life is the ability of the organism to maintain a constant
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
** Accordingly GFR can be estimated by using one urine sample and do creatinine testing.
 This sheet includes the lecture and last year s exam. When a patient goes to a clinic, we order 2 tests: 1) kidney function test: in which we measure UREA and CREATININE levels, and electrolytes (Na+,
This sheet includes the lecture and last year s exam. When a patient goes to a clinic, we order 2 tests: 1) kidney function test: in which we measure UREA and CREATININE levels, and electrolytes (Na+,
MILK. Nutritious by nature. The science behind the health and nutritional impact of milk and dairy foods
 MILK Nutritious by nature The science behind the health and nutritional impact of milk and dairy foods Recovery after exercise Although this is a relatively new area of dairy research, milk shows promise
MILK Nutritious by nature The science behind the health and nutritional impact of milk and dairy foods Recovery after exercise Although this is a relatively new area of dairy research, milk shows promise
Fal Fal P h y s i o l o g y 6 1 1, S a n F r a n c i s c o S t a t e U n i v e r s i t y
 Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Urinary system. Lab-7
 Urinary system Lab-7 Excretion: processes that remove wastes and excess materials from the body Urinary system (kidneys): excretes nitrogenous wastes, excess solutes, and water The Kidneys Regulate Water
Urinary system Lab-7 Excretion: processes that remove wastes and excess materials from the body Urinary system (kidneys): excretes nitrogenous wastes, excess solutes, and water The Kidneys Regulate Water
28/04/2013 LEARNING OUTCOME C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS STUDENT ACHIEVEMENT INDICATORS URINARY SYSTEM & EXCRETION
 LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
Lab 19 The Urinary System
 Lab 19 The Urinary System Laboratory Objectives Identify and describe the micro- and macroscopic anatomy of the kidney. Track the blood flow in and out of the kidney. Compare blood, glomerular filtrate,
Lab 19 The Urinary System Laboratory Objectives Identify and describe the micro- and macroscopic anatomy of the kidney. Track the blood flow in and out of the kidney. Compare blood, glomerular filtrate,
Functions of the Urinary System
 The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Regulate aspects of homeostasis Water balance Electrolytes Acid-base balance in the blood
The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Regulate aspects of homeostasis Water balance Electrolytes Acid-base balance in the blood
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
EXCRETION IN HUMANS 31 JULY 2013
 EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
Assessing Renal Function: What you Didn t Know You Didn t Know
 Assessing Renal Function: What you Didn t Know You Didn t Know Presented By Tom Wadsworth PharmD, BCPS Associate Clinical Professor UAA/ISU Doctor of Pharmacy Program Idaho State University College of
Assessing Renal Function: What you Didn t Know You Didn t Know Presented By Tom Wadsworth PharmD, BCPS Associate Clinical Professor UAA/ISU Doctor of Pharmacy Program Idaho State University College of
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Research Article. NGAL as a biomarker to predict and diagnose Acute Kidney Injury (AKI)
 Available online wwwjocprcom Journal of Chemical and Pharmaceutical Research, 215, 7(5):224-232 Research Article ISSN : 975-7384 CODEN(USA) : JCPRC5 NGAL as a biomarker to predict and diagnose Acute Kidney
Available online wwwjocprcom Journal of Chemical and Pharmaceutical Research, 215, 7(5):224-232 Research Article ISSN : 975-7384 CODEN(USA) : JCPRC5 NGAL as a biomarker to predict and diagnose Acute Kidney
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
The Urinary System 15PART A. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART A Functions of the Urinary System Elimination of waste products Nitrogenous
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART A Functions of the Urinary System Elimination of waste products Nitrogenous
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Estimation of Serum Creatinine, Urine Creatinine and Creatinine Clearance. BCH472 [Practical] 1
![Estimation of Serum Creatinine, Urine Creatinine and Creatinine Clearance. BCH472 [Practical] 1 Estimation of Serum Creatinine, Urine Creatinine and Creatinine Clearance. BCH472 [Practical] 1](/thumbs/73/68933269.jpg) Estimation of Serum Creatinine, Urine Creatinine and Creatinine Clearance BCH472 [Practical] 1 -Kidney functions: - The kidneys serve three essential functions: 1. They function as filters, removing metabolic
Estimation of Serum Creatinine, Urine Creatinine and Creatinine Clearance BCH472 [Practical] 1 -Kidney functions: - The kidneys serve three essential functions: 1. They function as filters, removing metabolic
Excretion (IGCSE Biology Syllabus )
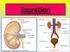
 Excretion (IGCSE Biology Syllabus 2016-2018) Structure of the Kidney Excretion is the removal from organisms of toxic materials, the waste products of metabolism and substances in excess of requirements
Excretion (IGCSE Biology Syllabus 2016-2018) Structure of the Kidney Excretion is the removal from organisms of toxic materials, the waste products of metabolism and substances in excess of requirements
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Citation for the original published paper (version of record):
 http://www.diva-portal.org Postprint This is the accepted version of a paper published in Clinical Biochemistry. This paper has been peerreviewed but does not include the final publisher proof-corrections
http://www.diva-portal.org Postprint This is the accepted version of a paper published in Clinical Biochemistry. This paper has been peerreviewed but does not include the final publisher proof-corrections
YR10. IGCSE Biology. Homeostasis
 YR10 IGCSE Biology Homeostasis Name: Prepared by William Green DBGS 2010 Homeostasis Body cells work best if they have the correct conditions e.g. 1. 2. 3. Write the definition of Homeostasis in the box
YR10 IGCSE Biology Homeostasis Name: Prepared by William Green DBGS 2010 Homeostasis Body cells work best if they have the correct conditions e.g. 1. 2. 3. Write the definition of Homeostasis in the box
Physical Characteristics of
 Physical Characteristics of Urine Bởi: OpenStaxCollege The urinary system s ability to filter the blood resides in about 2 to 3 million tufts of specialized capillaries the glomeruli distributed more or
Physical Characteristics of Urine Bởi: OpenStaxCollege The urinary system s ability to filter the blood resides in about 2 to 3 million tufts of specialized capillaries the glomeruli distributed more or
The Urinary System. Copyright 2003 Pearson Education, Inc. publishing as Benjamin Cummings
 The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Functions of the Urinary System Regulate aspects of homeostasis Water balance Electrolytes
The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Functions of the Urinary System Regulate aspects of homeostasis Water balance Electrolytes
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Glossary. Maintain keep up. Constant the same. Internal inside the body. Environment surroundings of the body.
 Homeostasis Glossary Maintain keep up. Constant the same. Internal inside the body. Environment surroundings of the body. What is Homeostasis? Body cells work best if they have the correct Temperature
Homeostasis Glossary Maintain keep up. Constant the same. Internal inside the body. Environment surroundings of the body. What is Homeostasis? Body cells work best if they have the correct Temperature
Neutrophil Gelatinase-Associated Lipocalin as a Biomarker of Acute Kidney Injury in Patients with Morbid Obesity Who Underwent Bariatric Surgery
 Published online: October 31, 213 1664 5529/13/31 11$38./ This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3. Unported license (CC BY-NC) (www.karger.com/oa-license),
Published online: October 31, 213 1664 5529/13/31 11$38./ This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3. Unported license (CC BY-NC) (www.karger.com/oa-license),
PARTS OF THE URINARY SYSTEM
 EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Lecture 16: The Nephron
 Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Seung Hyeok Han, MD, PhD Department of Internal Medicine Yonsei University College of Medicine
 Seung Hyeok Han, MD, PhD Department of Internal Medicine Yonsei University College of Medicine Age and Kidney Weight renal weight and thickening of the vascular intima Platt et al. Gerentology 1999;45:243-253
Seung Hyeok Han, MD, PhD Department of Internal Medicine Yonsei University College of Medicine Age and Kidney Weight renal weight and thickening of the vascular intima Platt et al. Gerentology 1999;45:243-253
What is excretion? Excretion is the removal of metabolic waste from the body.
 Excretion What is excretion? Excretion is the removal of metabolic waste from the body. Excretion in Plants Plants produce very little waste products. Plants lose oxygen and water vapour through the stomata.
Excretion What is excretion? Excretion is the removal of metabolic waste from the body. Excretion in Plants Plants produce very little waste products. Plants lose oxygen and water vapour through the stomata.
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Chapter 23. Composition and Properties of Urine
 Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
WEEK. MPharm Programme. Acute Kidney Injury. Alan M. Green MPHM13: Acute Kidney Injury. Slide 1 of 47
 MPharm Programme Acute Kidney Injury Alan M. Green 2017 Slide 1 of 47 Overview Renal Function What is it? Why does it matter? What causes it? Who is at risk? What can we (Pharmacists) do? How do you recognise
MPharm Programme Acute Kidney Injury Alan M. Green 2017 Slide 1 of 47 Overview Renal Function What is it? Why does it matter? What causes it? Who is at risk? What can we (Pharmacists) do? How do you recognise
Exercise increases water loss
 Exercise increases water loss During normal breathing, water is added to inspired air to protect delicate respiratory cells from drying out. Increased breathing during exercise increase this loss Heat
Exercise increases water loss During normal breathing, water is added to inspired air to protect delicate respiratory cells from drying out. Increased breathing during exercise increase this loss Heat
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Lecture-2 Review of the previous lecture:
 Lecture-2 Review of the previous lecture: -Kidney s function is to clean the blood by the removing of the waste plus adding some valuable substances -kidney failure will lead to death for many reasons,
Lecture-2 Review of the previous lecture: -Kidney s function is to clean the blood by the removing of the waste plus adding some valuable substances -kidney failure will lead to death for many reasons,
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure
 EXCRETORY SYSTEM WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure These wastes include: Carbon dioxide Mostly through breathing
EXCRETORY SYSTEM WHY DO WE NEED AN EXCRETORY SYSTEM? Function: To eliminate waste To maintain water and salt balance To maintain blood pressure These wastes include: Carbon dioxide Mostly through breathing
NGAL, a new markers for acute kidney injury
 NGAL, a new markers for acute kidney injury Prof. J. Delanghe, MD, PhD Dept. Clinical Chemistry Ghent University Lecture Feb 8, 2011 Serum creatinine is an inadequate marker for AKI. > 50% of renal
NGAL, a new markers for acute kidney injury Prof. J. Delanghe, MD, PhD Dept. Clinical Chemistry Ghent University Lecture Feb 8, 2011 Serum creatinine is an inadequate marker for AKI. > 50% of renal
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
A. Correct! Flushing acids from the system will assist in re-establishing the acid-base equilibrium in the blood.
 OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
Results Report. Welcome to Your ABT Report! Introduction to the ABT Report
 Results Report Athlete Name: SHEPPARD, JOSEPH Date of Blood Draw: Dec 08, 2017 Panel: ABT Gold Panel ABT Expert: Dr. Rock Welcome to Your ABT Report! Thank you for trusting AthleteBloodTest.com to be a
Results Report Athlete Name: SHEPPARD, JOSEPH Date of Blood Draw: Dec 08, 2017 Panel: ABT Gold Panel ABT Expert: Dr. Rock Welcome to Your ABT Report! Thank you for trusting AthleteBloodTest.com to be a
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Chapter 26 The Urinary System
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Excretion and Water Balance
 Excretion and Water Balance In the body, water is found in three areas, or compartments: Plasma, the liquid portion of the blood without the blood cells, makes up about 7 percent of body fluid. The intercellular
Excretion and Water Balance In the body, water is found in three areas, or compartments: Plasma, the liquid portion of the blood without the blood cells, makes up about 7 percent of body fluid. The intercellular
Unit 4 Homeostasis. The term homeostasis refers to the body s attempt. Your body systems must to maintain a stable internal environment -
 Unit 4 Homeostasis The term homeostasis refers to the body s attempt Your body systems must to maintain a stable internal environment - The body is trying to maintain, through a series of monitored adjustments.
Unit 4 Homeostasis The term homeostasis refers to the body s attempt Your body systems must to maintain a stable internal environment - The body is trying to maintain, through a series of monitored adjustments.
The Right Fluids and Foods
 The Right Fluids and Foods Handout 6-1 In addition to getting enough fluid, getting the right type of fluid is important. A rule of thumb is to try to drink 4 to 8 ounces (i.e., 1/2 to 1 cup) of cool water
The Right Fluids and Foods Handout 6-1 In addition to getting enough fluid, getting the right type of fluid is important. A rule of thumb is to try to drink 4 to 8 ounces (i.e., 1/2 to 1 cup) of cool water
Chapter: Interactions of Human Systems
 Table of Contents Chapter: Interactions of Human Systems Section 1: The Human Organism Section 2: How Your Body Works The Human Organism Organization in the Human Body Although your body is not made of
Table of Contents Chapter: Interactions of Human Systems Section 1: The Human Organism Section 2: How Your Body Works The Human Organism Organization in the Human Body Although your body is not made of
Chapter 32 Excretion
 Chapter 32 Excretion 3.4 Learning Objectives 3.4.6 The Excretory System in Humans 1. Role of the excretory system in homeostasis. 2. Importance of temperature regulation within the body. 3. Outline the
Chapter 32 Excretion 3.4 Learning Objectives 3.4.6 The Excretory System in Humans 1. Role of the excretory system in homeostasis. 2. Importance of temperature regulation within the body. 3. Outline the
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Biology Slide 1 of 36
 Biology 1 of 36 38 3 The Excretory System 2 of 36 Functions of the Excretory System 1.Function: process which eliminates metabolic wastes 3 of 36 Functions of the Excretory System (The skin excretes excess
Biology 1 of 36 38 3 The Excretory System 2 of 36 Functions of the Excretory System 1.Function: process which eliminates metabolic wastes 3 of 36 Functions of the Excretory System (The skin excretes excess
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Chapter 10: Urinary System & Excretion
 Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
Chapter 10: Urinary System & Excretion Organs of Urinary System Kidneys (2) form urine Ureters (2) Carry urine from kidneys to bladder Bladder Stores urine Urethra Carries urine from bladder to outside
Renal function parameters during early and late recovery periods following an all-out 21-km run in trained adolescent runners
 Clin Chem Lab Med 011;49(6):993 997 011 by Walter de Gruyter Berlin Boston. DOI 10.1515/CCLM.011.17 Renal function parameters during early and late recovery periods following an all-out 1-km run in trained
Clin Chem Lab Med 011;49(6):993 997 011 by Walter de Gruyter Berlin Boston. DOI 10.1515/CCLM.011.17 Renal function parameters during early and late recovery periods following an all-out 1-km run in trained
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE
 PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE - OBJECTIVES: 1- The simple examination of urine. 2- To detect some of the normal organic constituents of urine. 3- To detect some of the
PHYSICAL PROPERTIES AND DETECTION OF NORMAL CONSTITUENTS OF URINE - OBJECTIVES: 1- The simple examination of urine. 2- To detect some of the normal organic constituents of urine. 3- To detect some of the
AQA B3.3 Homeostasis LEVEL 1
 AQA B3.3 Homeostasis LEVEL 1 176 minutes 176 marks Page 1 of 48 ## (a) The table shows the compounds and ions dissolved in a student s urine. Compound or ion Percentage of total urea 60 negative ions 25
AQA B3.3 Homeostasis LEVEL 1 176 minutes 176 marks Page 1 of 48 ## (a) The table shows the compounds and ions dissolved in a student s urine. Compound or ion Percentage of total urea 60 negative ions 25
Lesson Overview. The Excretory System. Lesson Overview The Excretory System
 Lesson Overview 30.4 THINK ABOUT IT It s a hot day and you gulp down water. As you drink, you begin to wonder. Where s all that water going? Will it just dilute your blood, or is something in your body
Lesson Overview 30.4 THINK ABOUT IT It s a hot day and you gulp down water. As you drink, you begin to wonder. Where s all that water going? Will it just dilute your blood, or is something in your body
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Evaluation of the Cockroft Gault, Jelliffe and Wright formulae in estimating renal function in elderly cancer patients
 Original article Annals of Oncology 15: 291 295, 2004 DOI: 10.1093/annonc/mdh079 Evaluation of the Cockroft Gault, Jelliffe and Wright formulae in estimating renal function in elderly cancer patients G.
Original article Annals of Oncology 15: 291 295, 2004 DOI: 10.1093/annonc/mdh079 Evaluation of the Cockroft Gault, Jelliffe and Wright formulae in estimating renal function in elderly cancer patients G.
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
CHAPTER 10: Diet and nutrition & effect on physical activity and performance Practice questions - text book pages
 QUESTIONS AND ANSWERS CHAPTER 10: Diet and nutrition & effect on physical activity and performance Practice questions - text book pages 144-145 1) Complex carbohydrates do not include: a. lipids. b. triglycerides.
QUESTIONS AND ANSWERS CHAPTER 10: Diet and nutrition & effect on physical activity and performance Practice questions - text book pages 144-145 1) Complex carbohydrates do not include: a. lipids. b. triglycerides.
BCH472 [Practical] 1
![BCH472 [Practical] 1 BCH472 [Practical] 1](/thumbs/90/103504023.jpg) BCH472 [Practical] 1 1. They function as filters, removing metabolic products and toxins from the blood and excreting them through the urine. 2. They regulate the body s fluid status, electrolyte balance,
BCH472 [Practical] 1 1. They function as filters, removing metabolic products and toxins from the blood and excreting them through the urine. 2. They regulate the body s fluid status, electrolyte balance,
Renal Disease and PK/PD. Anjay Rastogi MD PhD Division of Nephrology
 Renal Disease and PK/PD Anjay Rastogi MD PhD Division of Nephrology Drugs and Kidneys Kidney is one of the major organ of drug elimination from the human body Renal disease and dialysis alters the pharmacokinetics
Renal Disease and PK/PD Anjay Rastogi MD PhD Division of Nephrology Drugs and Kidneys Kidney is one of the major organ of drug elimination from the human body Renal disease and dialysis alters the pharmacokinetics
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Heart Failure and Cardio-Renal Syndrome 1: Pathophysiology. Biomarkers of Renal Injury and Dysfunction
 CRRT 2011 San Diego, CA 22-25 February 2011 Heart Failure and Cardio-Renal Syndrome 1: Pathophysiology Biomarkers of Renal Injury and Dysfunction Dinna Cruz, M.D., M.P.H. Department of Nephrology San Bortolo
CRRT 2011 San Diego, CA 22-25 February 2011 Heart Failure and Cardio-Renal Syndrome 1: Pathophysiology Biomarkers of Renal Injury and Dysfunction Dinna Cruz, M.D., M.P.H. Department of Nephrology San Bortolo
Fluids and electrolytes
 Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
5. Maintaining the internal environment. Homeostasis
 5. Maintaining the internal environment Homeostasis Blood and tissue fluid derived from blood, flow around or close to all cells in the body. Blood and tissue fluid form the internal environment of the
5. Maintaining the internal environment Homeostasis Blood and tissue fluid derived from blood, flow around or close to all cells in the body. Blood and tissue fluid form the internal environment of the
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Excretion and Waste Management. Biology 30S - Miss Paslawski
 Excretion and Waste Management Biology 30S - Miss Paslawski Lesson 1 Waste Products and Organs 2 3 Excretion Excretion: Process by which dissolved metabolic wastes are separated from body fluids and removed
Excretion and Waste Management Biology 30S - Miss Paslawski Lesson 1 Waste Products and Organs 2 3 Excretion Excretion: Process by which dissolved metabolic wastes are separated from body fluids and removed
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Ch17-18 Urinary System
 Ch17-18 Urinary System Main Function: Filter the blood Other Functions: maintain purity and consistency of internal fluids eliminates nitrogenous wastes, toxins, and drugs from the body regulates blood
Ch17-18 Urinary System Main Function: Filter the blood Other Functions: maintain purity and consistency of internal fluids eliminates nitrogenous wastes, toxins, and drugs from the body regulates blood
