C H A P T E R 8 T H E R M A L I N J U R I E S
|
|
|
- Arnold Harris
- 5 years ago
- Views:
Transcription
1 CHAPTER 8 THERMAL INJURIES Thermal destruction of the skin results in severe local and systemic alterations. This destruction can occur from thermal energy, chemical reactions, electricity, or the response to cold. The management of the patient with a major thermal injury requires understanding of the pathophysiology, diagnosis, and treatment not only of the local skin injury but also of the derangements that occur in hemodynamic, metabolic, nutritional, immunologic, and psychologic homeostatic mechanisms. I. BURNS A. Pathophysiology:Amount of tissue destruction is based on temperature (>40 C) and time of exposure (Fig. 8-1) B. Diagnosis and prognosis 1. Burn size: % of total body surface area (TBSA) burned a. Rough estimate is based on rule of 9s (Fig. 8-2) b. Different charts are required for adults and children because of head-chest size discrepancy and limb differentials for ages birth to seven years (Fig. 8-3 and 8-4) Fig
2 Fig. 8-2 Fig
3 2. Age: burns at the extremes of age carry a greater morbidity and mortality 3. Depth: difficult to assess initially a. History of etiologic agent and time of exposure helpful b. Classification (Fig. 8-5) i. First degree: erythema but no skin breaks ii. Second degree: blisters, red and painful (a) Superficial partial-thickness, involves epidermis and upper dermis (b) Deep partial-thickness, involves deeper dermis iii. Third degree: full-thickness-insensate, charred or leathery iv. Fourth degree: muscle, bone 4. Location: face and neck, hands, feet, and perineum may cause special problems and warrant careful attention; often necessitate hospitalization/burn center 5. Inhalation injury: beware of closed quarters burn, burned nasal hair, carbon particles in pharynx, hoarseness, conjunctivitis 6. Associated injuries, e.g. fractures Fig Fig
4 7. Co-morbid factors, e.g. pre-existing cardiovascular, respiratory, renal and metabolic diseases; seizure disorders, alcoholism, drug abuse 8. Prognosis: best determined by burn size (TBSA) and age of patient, inhalation injury 9. Circumferential burns: can restrict blood flow to extremity, respiratory excursion of chest and may require escharotomy C. Categorization of burns is used to make treatment decisions and to decide if treatment in a burn center is necessary (Table 8-1,Table 8-2) D. Treatment plan 1. History and physical exam 2. Relieve respiratory distress escharotomy and/or intubation 3. Prevent and/or treat burn shock IV large bore needle 4. Monitor resuscitation Foley catheter and hourly urine output 5. Treat ileus and nausea N.G. tube if > 20% burn 6. Tetanus prophylaxis 7. Baseline laboratory studies i.e. Hct., UA, glucose, BUN, chest x-ray, electrolytes, EKG, cross-match, arterial blood gases, and carboxyhemoglobin 8. Cleanse, debride, and treat the burn wound E. Respiratory distress 1. Three major causes of respiratory distress in the burned patient: a. Unyielding burn eschar encircling chest i. Distress may be apparent immediately ii. Requires escharotomy (cutting into the eschar to relieve constriction) b. Carbon monoxide poisoning i. May be present immediately or later ii. Diagnosed by carboxyhemoglobin levels measured in arterial blood gas iii. Initial Rx is displacement of CO by 100% O 2 by facemask iv. Hyperbaric oxygen treatment may be of value Categorization of burns (American Burn Association): Major Burn Moderate Burn Minor Burn Size-Partial > 25% adults 15-25% adults < 15% adults thickness > 20% children 10-20% children < 10% children Size-Full >10% 2-10% < 2% thickness Primary major burn not involved not involved areas if involved Inhalation major burn if injury present or not suspected not suspected suspected Associated major burn if not present not present injury present Co-morbid poor risk patients patient relatively not present factors make burn major good risk Miscellaneous electrical injuries Treatment usually general hospital often managed environment specialized with designated as out-patient burn care facility team Table 8-1 Burns That Dictate Patient Admission to a Hospital or Burn Center 2 and 3 burns greater than 10% of BSA in patients under 10 or over 50 years of age 2 and 3 burns greater than 20% BSA in any age group 2 and 3 burns posing a serious threat of functional or cosmetic impairment, e.g. the face, hands, feet, genitalia, perineum, and about major joints) 3 burns greater than 5% BSA in any age Electrical burns including lightning Chemical burns posing a serious threat of functional or cosmetic impairment Inhalation injury Burns associated with major trauma 80 Table
5 82 c. Smoke inhalation leading to pulmonary injury i. Insidious in onset (18-36) hours ii. Due to incomplete products of combustion, not heat iii. Causes chemical injury to alveolar basement membrane and pulmonary edema iv. Initial Rx is humidified O 2 but intubation and respiratory support may be required v. Secondary bacterial infection of the initial chemical injury leads to progressive pulmonary insufficiency vi. Severe inhalation injury alone or in combination with thermal injury carries a grave prognosis vii. Three stages of presentation have been described: (a) Acute pulmonary insufficiency (immediately post burn to 48 hours) (b) Pulmonary edema (48-72 hours) (c) Bronchopneumonia (25 days) F. Burn shock 1. Massive amounts of fluid, electrolytes, and protein are lost from circulation almost immediately after burning (Table 8-3) Burn or Associated Condition Dictating Extra Fluid Administration Underestimation of the % TBSA burn Burn greater than 80% TBSA Associated traumatic injury Electrical burn Associated inhalation injury Delayed start of resuscitation 4º burn Administration of osmotic diuretics Pediatric burns Table Resuscitation requires replacement of sodium ions and water to restore plasma volume and cardiac output a. Many formulas have been reported to achieve resuscitation i. This can be given by prescribing 4cc Ringer s lactate/kg/%tbsa burn over the first 24 hours (Baxter or Parkland Hospital formula) ii. 1/2 of the first 24 hour fluid requirement should be given in the first eight hours postburn and the remaining 1/2 over the next 16 hours b. A plasma volume gap may remain Restored between hours postburn by administering cc plasma/kg/% TBSA burn c. After 30 hours D5W can be given at a rate to maintain a normal serum sodium G. Monitoring resuscitation 1. Urine output 30-55cc/hr in adults and 1.2cc/Kg/hr in children < age A clear sensorium, pulse <120/min, HCO 3 > 18 meq/l, cardiac output >3.1 L/M 2 3. CVP in acute major burns is unreliable H. Treatment of the burn wound (Table 8-4) 1. Wound closure by the patient s own skin is the ultimate goal of treatment a. By spontaneous healing b. Autograft c. Allograft d. Xenograft e. Artificial skin f. Cultured epithelial cells 2. Specific treatment of the burn wound differs from one burn center to another a. The most commonly employed topical antibacterials are silver sulfadiazine (Silvadene ) and mafenide acetate (Sulfamylon ) b. Status of burn wound bacterial colonization and effectiveness of topical antibacterial treatment can be monitored by biopsies of wound for quantitative and qualitative bacteriology 83
6 Sample Orders For a 70 Kg 40 year old patient with a 40% flame burn: 1. Admit to ICU portion of burn center 2. Strict bedrest with head elevated Maintain elevation of burned extremities 4. Vital signs: pulse, BP respiration q 15 min, temperature q 2 h 5. Check circulation of extremities (capillary refill or Doppler) q 30 min % O 2 face mask 7. Infuse Ringer s lactate at 700cc for first hour, then reassess 8. Measure urinary output by Foley catheter to closed drainage 9. Notify physician of first hour s urine output (must be 30-50cc: cc in pediatric patient) 10. N.P.O. 11. N.G. tube to intermittent low suction 12. Measure ph of gastric content q 2 h stress ulcer prophylaxis (e.g. Zantac) 13. Morphine sulfate 4 mg intravenously q 2-3 hr prn pain - no intramuscular narcotics (unreliable absorption) 14. Tetanus toxoid 0.5cc IM (if patient previously immunized) 15. Send blood for Hct., glucose, BUN, cross match 2 units, electrolytes 16. Urine for U.A. and culture 17. Chest x-ray 18. EKG 19. Arterial blood gases q 6 h and prn 20. Cleanse wounds with Betadine solution, debride all blisters, map injury on Lund-Browder chart, and photograph wounds 21. Apply silver sulfadiazine to all wounds with sterile gloved hand (use reverse isolation technique when burn wounds are exposed) 22. Dress wounds with burn gauze and surgifix 23. Splint extremities as per physical therapist 24. Change all dressings, cleanse wounds, and reapply topical antibacterial q 8 h or q 12 h 25. Bronchoscopy If inhalation injury suspected 3. Necrotic tissues may be removed by any of several techniques: a. Formal excision b. Tangential (layered) debridement c. Enzymatic debridement d. Hydrotherapy a useful adjunct 4. Autografts should be applied to priority areas first, such as the hands, face and important joints 5. Once healed, pressure is usually necessary with elastic supports to minimize hypertrophic scarring 6. Physical therapy important adjunct in burn care I. Complications: can occur in every physiologic system secondary to burn injury (Table 8-5) 1. Renal failure a. From hypovolemia b. Beware of nephrotoxic antibiotics in the burn patient Risk Factors in Burn Wound Infection I. PATIENT FACTORS A. Extent of burn > 30% of body surface B. Depth of burn: full-thickness vs. partial-thickness C. Age of patient (very young or very old at higher risk) D. Pre-existing disease E. Wound dryness F. Wound temperature G. Secondary impairment of blood flow to wound H. Acidosis II. MICROBIAL FACTORS A. Density >10 5 organisms per gram of tissue B. Motility C. Metabolic products 1. Endotoxin 2. Exotoxins 3. Permeability factors 4. Other factors D. Antimicrobial resistance 84 Table 8-4 Table
7 2. Gastrointestinal bleeding a. More likely in burns over 40% b. Usually remains subclinical c. Antacids and H 2 blockers d. Increased risk with burn wound sepsis 3. Burn wound sepsis a. Monitored by tissue biopsy qualitative and quantitative b. Must keep bacterial count < 10 5 bacteria/gm of tissue c. Clinically suspect sepsis with i. Sudden onset of hyper or hypothermia ii. Unexpected congestive heart failure or pulmonary edema iii. Development of the acute respiratory distress syndrome iv. Ileus occurring after 48 hours postburn v. Mental status change vi. Azotemia vii. Thrombocytopenia viii. Hypofibrinogenemia ix. Hyper or hypoglycemia is especially suspect if burn > 40% TBSA x. Blood cultures may be positive but in many cases are not 4. Progressive pulmonary insufficiency a. Can occur after: i. Smoke inhalation ii. Pneumonia iii. Cardiac decompensation iv. Sepsis from any cause b. Produces: i. Hypoxemia ii. Hypocarbia iii. Pulmonary shunting iv. Acidosis II. 5. Wound contracture and hypertrophic scarring a. Largely preventable b. Since a burn wound will contract until it meets an opposing force, splinting is necessary from the outset i. Splints are used to prevent joint contractures, e.g. elbow and knee are kept in extension, and MCP joints of fingers in flexion c. Timely wound closure with adequate amounts of skin should largely eliminate these problems d. Continued postoperative splinting and elastic pressure supports are of value in the remolding of collagen with prevention of hypertrophic scars CHEMICAL BURNS A. Pathophysiology 1. Tissue damage secondary to a chemical depends on: a. Nature of agent b. Concentration of the agent c. Quantity of the agent d. Length of time the agent is in contact with tissue e. Degree of tissue penetration f. Mechanism of action B. Diagnosis 1. Chemical burns are deeper than initially appear and may progress with time a. Fluid resuscitation needs often underestimated b. Watch for renal/liver/pulmonary damage C. Treatment 1. Initial treatment is dilution of the chemical with water 2. Special attention to eyes after copious irrigation with saline, consult ophthalmologist 3. After 12 hours initial dilution, local care of the wound with debridement, topical antibacterials, and eventual wound closure is same as for thermal burn 86 87
8 88 III. D. Of particular note are: 1. Gasoline a. Excretion by lung b. May cause large skin burn, if immersed c. Watch for atelectasis, pulmonary infiltrates; surfactant is inhibited 2. Phenol a. Dull, gray color to skin, may turn black b. Urine may appear smoky in color c. Spray water on burn surface d. Wipe with polyethylene glycol e. Direct renal toxicity 3. Hydrofluoric acid a. Irrigate copiously with water b. Subcutaneous injections of 10% of calcium gluconate c. Monitor EKG patients may become hypocalcemic d. Pulmonary edema may occur if subjected to fumes 4. White phosphorous a. Do not allow to desiccate may ignite b. Each particle must be removed mechanically c. Copper sulfate (2%) may counteract to make phosphorous more visible (turns black in color) d. Watch for EKG changes (Q T interval and S T and T wave changes) e. May cause hemoglobinuria and renal failure ELECTRICAL INJURIES A. Pathophysiology 1. Effects of passage of electric current through the body depend on: a. Type of circuit b. Voltage of circuit c. Resistance offered by body d. Amperage of current flowing through tissue e. Pathway of current through the body f. Duration of contact 2. Tissue resistance to electrical current increases from nerve (least resistant) to vessel to muscle to skin to tendon to fat to bone B. Diagnosis 1. Types of injury a. Arc injury: localized injury caused by intense heat b. Injury due to current i. Due to heat generated as current flows through tissue (a) Injury more severe in tissue with high resistance (i.e. bone) (b) Vessels thrombose as current passes ii. rapidly along them Effects of current may not be immediately seen C. Special effects of electrical injury 1. Cardiopulmonary a. Anoxia and ventricular fibrillation may cause immediate death b. Early and delayed rhythm abnormalities can occur c. EKG changes may occur some time after the burn 2. Renal a. High risk of renal failure due to hemoglobin and myoglobin deposits in renal tubules i. Requires higher urine flow (75cc/hr in adults) ii. iii. Must alkalinize urine to keep hemoglobin and myoglobin in more soluble state Mannitol may be useful to clear heavy protein load 3. Fractures: a. Tetanic muscle contractions may be strong enough to fracture bones, especially spine 4. Spinal cord damage a. Can occur secondary to fracture or demyelinating effect of current 5. Abdominal effects a. Intraperitoneal damage can occur to G.I. tract secondary to current 89
9 90 IV. 6. Vascular effects a. Vessel thrombosis progresses with time b. Delayed rupture of major vessels can occur 7. Cataract formation late complication 8. Seizures D. Treatment 1. CPR if necessary 2. Fluids usually large amounts a. No formula is accurate because injury is more extensive than can be predicted by skin damage b. Alkalinize with NaHCO 3, if myoglobinuria or hemoglobinuria present 3. Monitoring a. CVP or pulmonary wedge pressure helpful since total capillary leak does not occur as it does in a thermal burn b. Maintain urine output at cc/hr until all myoglobin and/or hemoglobin disappears from urine 4. Wound Management a. Topical agent with good penetrating ability is needed [i.e. silver sulfadiazine (Silvadene ) or mafenide acetate (Sulfamylon )] b. Debride non-viable tissue early and repeat as necessary (every 48 hrs) to prevent sepsis c. Major amputations frequently required d. Technicium-99 stannous pyrophosphate scintigraphy may be useful to evaluate muscle damage 5. Treat associated injuries (e.g. fractures) COLD INJURIES The two conditions of thermal injury due to cold are local injury (frostbite) and systemic injury (hypothermia) A. Frostbite 1. Pathophysiology a. Formation of ice crystals in tissue fluid i. Usually in areas which lose heat rapidly (e.g. extremities) b. Anything which increases heat loss from the body such as wind velocity, or decreases tissue perfusion, such as tight clothing, predisposes patient to frostbite c. Ability of various tissue to withstand cold injury is inversely proportional to their water content 2. Treatment a. The key to successful treatment is rapid rewarming in a 40 C waterbath i. Admission to hospital usually required (a) Tetanus prophylaxis (b) Wound management (c) Physical therapy (i) Maintenance of range of motion important (ii) Daily whirlpool and exercise (d) Sympathectomy, anti-coagulants, and early amputation of questionable value in controlled studies ii. Usually wait until complete demarcation before proceeding with amputations. Nonviable portions of extremities will often autoamputate with good cosmetic and functional results. B. Hypothermia 1. Diagnosis a. Core temperature < 34 C b. Symptoms and signs mimic many other diseases c. High level of suspicion necessary during cold injury season 2. Treatment a. Must be rapid to prevent death b. Monitor EKG, CVP, and arterial blood gases and ph during warming and resuscitation, maintain urine output of 50cc/hr c. Begin Ringer s Lactate with 1 ampule NaHCO 3 d. Oral airway or endotracheal tube if necessary e. Rapidly rewarm in 40 hydrotherapy tank (requires 1-2 hours to maintain body temperature at 37 C) f. Treat arrhythmias with IV Lidocaine drip if necessary g. Evaluate and treat any accompanying disease states 91
10 V. LIGHTNING INJURIES A. Cutaneous effects lightning strikes may cause cutaneous burn wounds 1. Contact burns from clothing on fire or contact with hot metal (i.e. zippers) 2. Entry and exit burns are usually small, may be partial or full thickness 3. Lightning burns are not the same as electrical burns don t get deep tissue injury B. May have temporary ischemic effects on extremity pallor or neurologic deficits. Spontaneous recovery after a few hours is the rule probably due to local vasoconstriction C. Systemic effects can occur such as arrhythmias, cataracts, CNS symptoms CHAPTER 8 BIBLIOGRAPHY THERMAL INJURIES 1. Gibran, N.S. and Heimbach, D.M. Current status of burn wound pathophysiology. Clin Plast Surg. 2000; 27: Matthews, M.S. and Fahey,A.L. Plastic surgical considerations in lightning injuries. Ann Plast Surg. 1997; 39: van Zuijlen, P.P. et al. Dermal substitution in acute burns and reconstructive surgery: a subjective and objective long-term follow-up. Plast Reconstr Surg. 2001; 108:
A. Pathophysiology: Amount of tissue destruction is based on temperature (> 40 C) and time of exposure (Figure 1).
 CHAPTER 24 THERMAL, ELECTRICAL AND CHEMICAL INJURIES Maureen Beederman, MD and Eamon O Reilly, MD, LCDR, USN Thermal injuries can result from exposure to heat, chemicals, electricity, or cold, and can
CHAPTER 24 THERMAL, ELECTRICAL AND CHEMICAL INJURIES Maureen Beederman, MD and Eamon O Reilly, MD, LCDR, USN Thermal injuries can result from exposure to heat, chemicals, electricity, or cold, and can
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
BURNS MODULE. In the paediatric population consider non-accidental injury as a mechanism for burn injuries.
 BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
Burn Injuries & Its Management M JARI.MD
 Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test
 Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
At the conclusion of this course the learner will be able to
 Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department
 Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Burns. A Comprehensive Review Assessment & Management
 Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
EmergencyKT: Management of Thermal Injury in Adult Patients
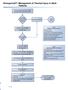 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
The immediate management of burns patients should be similar to management of trauma.
 CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
Objectives. Initial Burn Care and Fluid Resuscitation 6/5/2015 INITIAL MANAGEMENT
 Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Chapter 23 Caring for Clients with Burns
 Chapter 23 Caring for Clients with Burns Burn Injuries 4500 people die from burns each year High risk group ~ children and the elderly The most common cause of burns Smoking material Scalding Lighting
Chapter 23 Caring for Clients with Burns Burn Injuries 4500 people die from burns each year High risk group ~ children and the elderly The most common cause of burns Smoking material Scalding Lighting
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Applicable to. Team Members Performing MD House Staff APRN/PA RN LPN
 Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Burn injury. A : patent airway with smoking inhalation, stridor. D: E4V5M6,pupil 2mm RTLBE
 Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Wisecracks 1. What are the indications for an escharotomy 2. What are the primary considerations in mechanical ventilation of burn patients
 Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Advanced Paediatric Nursing. Burn Trauma. 26 April Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH
 Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
BLS, ILS, ALS OTEP BURNS BURN INTRODUCTION TYPES OF BURNS
 BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
ELECTRICAL INJURY 9/21/2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
 ELECTRICAL INJURY SAMUEL P. MANDELL, MD, MPH ASSISTANT PROFESSOR OF SURGERY UNIVERSITY OF WASHINGTON SEPTEMBER 28, 2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
ELECTRICAL INJURY SAMUEL P. MANDELL, MD, MPH ASSISTANT PROFESSOR OF SURGERY UNIVERSITY OF WASHINGTON SEPTEMBER 28, 2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
Management of Acute Burn Injuries: The First 24 Hours
 Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Epidemiology. Burn Rehabilitation. Epidemiology. Epidemiology. United States. United States Cause of injury. Incidence has declined
 Burn Rehabilitation Peter Esselman, MD Professor and Chair Department of Rehabilitation Medicine University of Washington Epidemiology United States 450,000 burn injuries/year in USA that receive medical
Burn Rehabilitation Peter Esselman, MD Professor and Chair Department of Rehabilitation Medicine University of Washington Epidemiology United States 450,000 burn injuries/year in USA that receive medical
FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
 Manual: Section: Protocol #: Approval Date: Effective Date: Revision Due Date: 10/2019 LifeLine Patient Care Protocols Adult/Pediatrics AP1-011 10/2018 10/2018 FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
Manual: Section: Protocol #: Approval Date: Effective Date: Revision Due Date: 10/2019 LifeLine Patient Care Protocols Adult/Pediatrics AP1-011 10/2018 10/2018 FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
Responsibility This guideline applies to teams of health professions caring for burn patients.
 Page 1 of 9 Guideline: Initial Assessment & Management of Burn Injuries Purpose This document provides a guideline for the initial assessment and management of burn patients. It is not intended as a full
Page 1 of 9 Guideline: Initial Assessment & Management of Burn Injuries Purpose This document provides a guideline for the initial assessment and management of burn patients. It is not intended as a full
INTRODUCTION OBJECTIVES. When the student has finished this module, he/she will be able to:
 Burn Care and Management WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017 RN.ORG, S.A., RN.ORG,
Burn Care and Management WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017 RN.ORG, S.A., RN.ORG,
Burns. Chapter 9. Burns
 Burns Chapter 9 Burns Introduction Natural childhood curiosity and lack of supervision frequently combine to make thermal injuries a major cause of morbidity and mortality in the pediatric patient. Whether
Burns Chapter 9 Burns Introduction Natural childhood curiosity and lack of supervision frequently combine to make thermal injuries a major cause of morbidity and mortality in the pediatric patient. Whether
Current Trends in Burn Care
 Objectives Current Trends in Burn Care Jordan Murphy, BSN, CFRN Clinical Educator-KY/FL PHI Air Medical Describes normal skin anatomy. Differentiates pathophysiology related to etiology of injury. Identify
Objectives Current Trends in Burn Care Jordan Murphy, BSN, CFRN Clinical Educator-KY/FL PHI Air Medical Describes normal skin anatomy. Differentiates pathophysiology related to etiology of injury. Identify
Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital. Mr Adam Bialostocki Plastic Surgeon, Tauranga
 Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital Mr Adam Bialostocki Plastic Surgeon, Tauranga Mr. Adam Bialostocki Plastic Surgeon Minor Burns First Aid Remove the burning agent / wet clothes
Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital Mr Adam Bialostocki Plastic Surgeon, Tauranga Mr. Adam Bialostocki Plastic Surgeon Minor Burns First Aid Remove the burning agent / wet clothes
Medical APMLE. Podiatry and Medical.
 Medical APMLE Podiatry and Medical http://killexams.com/exam-detail/apmle Question: 290 Signs and symptoms of hemolytic transfusion reactions include: A. Hypothermia B. Hypertension C. Polyuria D. Abnormal
Medical APMLE Podiatry and Medical http://killexams.com/exam-detail/apmle Question: 290 Signs and symptoms of hemolytic transfusion reactions include: A. Hypothermia B. Hypertension C. Polyuria D. Abnormal
Pediatrics Grand Rounds 1 June University of Texas Health Science Center at San Antonio. Management of Burn Wounds. Management of Burn Wounds
 Management of Burn Wounds Management of Burn Wounds History of Burn Care Pathophysiology of Burn Lillian F. Liao, MD, MPH Division of Trauma and Emergency Surgery Department of Surgery UTHSCSA Acute burn
Management of Burn Wounds Management of Burn Wounds History of Burn Care Pathophysiology of Burn Lillian F. Liao, MD, MPH Division of Trauma and Emergency Surgery Department of Surgery UTHSCSA Acute burn
Burn & Soft Tissue Service Orientation Slides
 Burn & Soft Tissue Service Orientation Slides Damien Wilson Carter, MD Director, Burn/Soft Tissue Service Sue Reeder, BSN, CWOCN Burn Resource Nurse Specialist Scope ALL Burn injuries (> Age 12) Cold injury/
Burn & Soft Tissue Service Orientation Slides Damien Wilson Carter, MD Director, Burn/Soft Tissue Service Sue Reeder, BSN, CWOCN Burn Resource Nurse Specialist Scope ALL Burn injuries (> Age 12) Cold injury/
Initial assessment. ATLS/ABLS protocol and assess for other injuries/fractures based on mechanism. Inhalational injury. Vascular compromise:
 Complex Hand Burns Brent Egeland, MD Assistant Professor Dell Medical School Department of Surgery and Perioperative Care Institute of Reconstructive Plastic Surgery Plastic, Hand, and Reconstructive Microsurgery
Complex Hand Burns Brent Egeland, MD Assistant Professor Dell Medical School Department of Surgery and Perioperative Care Institute of Reconstructive Plastic Surgery Plastic, Hand, and Reconstructive Microsurgery
EMERGENCYROOM BURN MANAGEMENT
 EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
Burns Management in the Emergency Department
 Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose.
 Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
Burn wounds - Determining the size and type degree
 1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
Cellular and Tissue Effects. Pathophysiology of the Burn Wound. Special Topics: Thermal Burns & Smoke Inhalation
 Special Topics: Thermal Burns & Smoke Inhalation MEDICAL RESPONDER AND RECEIVER SEMINAR; EXPLOSION AND BLAST INJURIES Pathophysiology of the Burn Wound The burn wound is the source of virtually all ill
Special Topics: Thermal Burns & Smoke Inhalation MEDICAL RESPONDER AND RECEIVER SEMINAR; EXPLOSION AND BLAST INJURIES Pathophysiology of the Burn Wound The burn wound is the source of virtually all ill
Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie
 Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie History 3 yo boy, presents to pediatric ED with mother Child can be heard crying inside waiting/patient room, has both hands bandaged
Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie History 3 yo boy, presents to pediatric ED with mother Child can be heard crying inside waiting/patient room, has both hands bandaged
Appendix. Sedatives and Pain Medications. Gabapentin ( mg po q8h) or Pregabalin ( mg po q8h)
 Appendix Sedatives and Pain Medications Non-intubated patients Non-opioid analgesics Acetaminophen (500 1,000 mg po q6h) NSAID (Ibuprofen, Naprosyn, Celebrex) Gabapentin (100 300 mg po q8h) or Pregabalin
Appendix Sedatives and Pain Medications Non-intubated patients Non-opioid analgesics Acetaminophen (500 1,000 mg po q6h) NSAID (Ibuprofen, Naprosyn, Celebrex) Gabapentin (100 300 mg po q8h) or Pregabalin
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center
 Management of the Burn Patient Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center American Burn Association Transfer Criteria Burn > 10%
Management of the Burn Patient Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center American Burn Association Transfer Criteria Burn > 10%
Review. A. abrasion B. contusion C. hematoma D. avulsion
 Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Cold Injuries: An Update on Hypothermia and Frostbite
 Cold Injuries: An Update on Hypothermia and Frostbite HYPOTHERMIA Definitions Shell = skin, subcutaneous tissues and extremities; temperature of the shell varies according to environment Core = brain,
Cold Injuries: An Update on Hypothermia and Frostbite HYPOTHERMIA Definitions Shell = skin, subcutaneous tissues and extremities; temperature of the shell varies according to environment Core = brain,
Thermal Burns PFN: SOMEML07. Terminal Learning Objective. References. Hours: 3.0 Instructor: Action: Communicate knowledge of thermal burns
 Thermal Burns PFN: SOMEML07 Hours: 3.0 Instructor: Slide 1 Terminal Learning Objective Action: Communicate knowledge of thermal burns Condition: Given a lecture in a classroom environment Standard: Received
Thermal Burns PFN: SOMEML07 Hours: 3.0 Instructor: Slide 1 Terminal Learning Objective Action: Communicate knowledge of thermal burns Condition: Given a lecture in a classroom environment Standard: Received
Titrating Critical Care Medications
 Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Chapter 29. Objectives. Objectives 01/09/2013. Burns
 Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
CARE OF PATIENTS WITH BURNS. NUR 240 Donna Ricketts, MSN, RN, OCN
 CARE OF PATIENTS WITH BURNS NUR 240 Donna Ricketts, MSN, RN, OCN INCIDENCE/PREVALENCE OF BURN INJURY 5 th most common unintentional injury deaths 3 rd leading cause of fatal home injuries 4,000 burn deaths
CARE OF PATIENTS WITH BURNS NUR 240 Donna Ricketts, MSN, RN, OCN INCIDENCE/PREVALENCE OF BURN INJURY 5 th most common unintentional injury deaths 3 rd leading cause of fatal home injuries 4,000 burn deaths
Dr. Muhammad Shamim. FCPS (Pak), FACS (USA), FICS (USA), MHPE (Nl & Eg)
 Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA), MHPE (Nl & Eg) Assistant Professor, Dept. of Surgery College of Medicine, Salman bin Abdulaziz University Email: surgeon.shamim@gmail.com Web: surgeonshamim.com
Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA), MHPE (Nl & Eg) Assistant Professor, Dept. of Surgery College of Medicine, Salman bin Abdulaziz University Email: surgeon.shamim@gmail.com Web: surgeonshamim.com
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
Fire Deaths. Dr Julie McAdam Consultant Forensic Pathologist Glasgow University
 Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
Thermal Injuries. Manika Bhandari, Malika Bhola, Rucha Desai, Dhruvika Joshi, Abir Shamim Life Science 4M03
 Thermal Injuries Manika Bhandari, Malika Bhola, Rucha Desai, Dhruvika Joshi, Abir Shamim Life Science 4M03 INTRODUCTION Anatomy of the skin The skin has three anatomical layers Epidermis Dermis Subcutaneous
Thermal Injuries Manika Bhandari, Malika Bhola, Rucha Desai, Dhruvika Joshi, Abir Shamim Life Science 4M03 INTRODUCTION Anatomy of the skin The skin has three anatomical layers Epidermis Dermis Subcutaneous
Burn Management. Praz Patcha, MD 13 March 2014
 Burn Management Praz Patcha, MD 13 March 2014 Epidemiology 500,000 / yr 40,000 to 60,000 requiring admission < 1% total injuries in US but $10.4 billion Risk Factors Age Location Demographics Socioeconomics
Burn Management Praz Patcha, MD 13 March 2014 Epidemiology 500,000 / yr 40,000 to 60,000 requiring admission < 1% total injuries in US but $10.4 billion Risk Factors Age Location Demographics Socioeconomics
Current Concepts in Burn Rehabilitation
 Current Concepts in Burn Rehabilitation 7 th Congress of the Baltic Association of Rehabilitation Tallinn, Estonia September 2010 R. Scott Ward, PT, PhD Professor and Chair Department of Physical Therapy
Current Concepts in Burn Rehabilitation 7 th Congress of the Baltic Association of Rehabilitation Tallinn, Estonia September 2010 R. Scott Ward, PT, PhD Professor and Chair Department of Physical Therapy
Burns and electrical injuries. Shelley Westwood, RN, BSN
 Burns and electrical injuries Shelley Westwood, RN, BSN Burns A burn is an injury caused by fire, heat, chemicals, radiation, or electricity. Burns are traumatic in that they can cause extreme pain, permanent
Burns and electrical injuries Shelley Westwood, RN, BSN Burns A burn is an injury caused by fire, heat, chemicals, radiation, or electricity. Burns are traumatic in that they can cause extreme pain, permanent
Frostbite. Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department
 Frostbite Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department Question 1 An 8 year old male is brought in by EMS from an icy mountain. He was with his family skiing but was separated from
Frostbite Jessica Cardona PGY1 Jackson Memorial Hospital Pediatrics Department Question 1 An 8 year old male is brought in by EMS from an icy mountain. He was with his family skiing but was separated from
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline
 TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
INITIAL CARE AND TREATMENT OF BURN INJURIES. November 10,
 INITIAL CARE AND TREATMENT OF BURN INJURIES 2 11/10/2012 November 10, 2012 2 Oregon Burn Center Only burn center in Oregon and SW Washington New unit 16 beds, 20,000 square feet Opened in February 2002
INITIAL CARE AND TREATMENT OF BURN INJURIES 2 11/10/2012 November 10, 2012 2 Oregon Burn Center Only burn center in Oregon and SW Washington New unit 16 beds, 20,000 square feet Opened in February 2002
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Not All That Blisters Is a Burn! Jamie Hoffman-Rosenfeld, MD CHAMP Webinar December 6, 2012
 Not All That Blisters Is a Burn! Jamie Hoffman-Rosenfeld, MD CHAMP Webinar December 6, 2012 Objectives To review the epidemiology of burns in children including burns caused by abuse To review the steps
Not All That Blisters Is a Burn! Jamie Hoffman-Rosenfeld, MD CHAMP Webinar December 6, 2012 Objectives To review the epidemiology of burns in children including burns caused by abuse To review the steps
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Wound Care in the Community. Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts
 Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
MY STRATEGY FOR TREATING BURN INJURIES. Warren Garner MD FACS Keck School of Medicine at USC Los Angeles, CA
 MY STRATEGY FOR TREATING BURN INJURIES Warren Garner MD FACS Keck School of Medicine at USC Los Angeles, CA ASSUMPTIONS: Burns which heal to normal have best outcome. Medical risk, functional recovery,
MY STRATEGY FOR TREATING BURN INJURIES Warren Garner MD FACS Keck School of Medicine at USC Los Angeles, CA ASSUMPTIONS: Burns which heal to normal have best outcome. Medical risk, functional recovery,
Shock. Perfusion. The cardiovascular system s circulation of blood and oxygen to all the cells in different tissues and organs of the body
 Shock Chapter 10 Shock State of collapse and failure of the cardiovascular system Leads to inadequate circulation Without adequate blood flow, cells cannot get rid of metabolic wastes The result- hypoperfusion
Shock Chapter 10 Shock State of collapse and failure of the cardiovascular system Leads to inadequate circulation Without adequate blood flow, cells cannot get rid of metabolic wastes The result- hypoperfusion
INTRODUCTION. Objectives. When the student has finished this module, he/she will be able to:
 Hydrofluoric Acid Burns WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017 RN.ORG, S.A., RN.ORG,
Hydrofluoric Acid Burns WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017 RN.ORG, S.A., RN.ORG,
BASICS OF BURN MANAGEMENT
 BASICS OF BURN MANAGEMENT Dr S M Keswani Cosmetic Surgeon National Burns Centre, Airoli,Navi-Mumbai Breach Candy Hospital Wockhardt Hospital National Burns Centre, Airoli, Navi-Mumbai. CLASSIFICATION 1.
BASICS OF BURN MANAGEMENT Dr S M Keswani Cosmetic Surgeon National Burns Centre, Airoli,Navi-Mumbai Breach Candy Hospital Wockhardt Hospital National Burns Centre, Airoli, Navi-Mumbai. CLASSIFICATION 1.
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER
 DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
The Surgical Patient. Objectives:
 The Surgical Patient Objectives: 1. Discuss the effect of surgery on the body systems. 2. Explain the etiological factors, nursing assessment, and management of potential problems during the postoperative
The Surgical Patient Objectives: 1. Discuss the effect of surgery on the body systems. 2. Explain the etiological factors, nursing assessment, and management of potential problems during the postoperative
Outpatient Burn Care for Primary Care: Who needs a referral?
 Outpatient Burn Care for Primary Care: Who needs a referral? J. Kevin Bailey, MD Associate Professor Department of Surgery Division of Trauma, Critical Care and Burn The Ohio State University Wexner Medical
Outpatient Burn Care for Primary Care: Who needs a referral? J. Kevin Bailey, MD Associate Professor Department of Surgery Division of Trauma, Critical Care and Burn The Ohio State University Wexner Medical
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Burn Resuscitation Formulas. John P. Sabra, MD Seton Surgical Group Department of Surgery Dell Medical School Austin, TX
 Burn Resuscitation Formulas John P. Sabra, MD Seton Surgical Group Department of Surgery Dell Medical School Austin, TX BURN INJURY % Physiologic Change % TBSA burn Stasis BURN VASCULAR PERMEABILITY
Burn Resuscitation Formulas John P. Sabra, MD Seton Surgical Group Department of Surgery Dell Medical School Austin, TX BURN INJURY % Physiologic Change % TBSA burn Stasis BURN VASCULAR PERMEABILITY
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
UNIT VI: ACID BASE IMBALANCE
 UNIT VI: ACID BASE IMBALANCE 1 Objectives: Review the physiological mechanism responsible to regulate acid base balance in the body i.e.: Buffers (phosphate, hemoglobin, carbonate) Renal mechanism Respiratory
UNIT VI: ACID BASE IMBALANCE 1 Objectives: Review the physiological mechanism responsible to regulate acid base balance in the body i.e.: Buffers (phosphate, hemoglobin, carbonate) Renal mechanism Respiratory
Bill Hall, MD Mesa County EMS System
 Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Proceedings of the 36th World Small Animal Veterinary Congress WSAVA
 www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
IV Fluids. I.V. Fluid Osmolarity Composition 0.9% NaCL (Normal Saline Solution, NSS) Uses/Clinical Considerations
 IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
Clinical Connections April 16, 2014
 Management of Burns Eric McCoy PA-C Kathy Johnston RN, BSN Trauma/Burn Service UPMC Mercy A Long Tradition of Caring Comprehensive burn care from initial treatment through rehabilitation Region s only
Management of Burns Eric McCoy PA-C Kathy Johnston RN, BSN Trauma/Burn Service UPMC Mercy A Long Tradition of Caring Comprehensive burn care from initial treatment through rehabilitation Region s only
Modern management of paediatric burns
 Modern management of paediatric burns Burn injuries pose a major threat to children in South Africa and remain a devastating injury, because of the resulting severe emotional and physical scarring and
Modern management of paediatric burns Burn injuries pose a major threat to children in South Africa and remain a devastating injury, because of the resulting severe emotional and physical scarring and
Management of Burns under Prolonged Field Care
 This Role 1, prolonged field care (PFC) guideline is intended to be used after TCCC Guidelines when evacuation to higher level of care is not immediately possible. A provider of PFC must first and foremost
This Role 1, prolonged field care (PFC) guideline is intended to be used after TCCC Guidelines when evacuation to higher level of care is not immediately possible. A provider of PFC must first and foremost
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Cold-Related Illness. Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic
 Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Chapter 21: Burns Introduction to Burn Injuries (1 of 2) Introduction to Burn Injuries (2 of 2) Reduction in Burn Injuries Pathophysiology of Burns
 1 2 3 4 5 6 7 8 Chapter 21: Burns Introduction to Burn Injuries (1 of 2) 1.25-2 million Americans treated for burns annually 50,000 require 3-5% considered life threatening leading cause of death for children
1 2 3 4 5 6 7 8 Chapter 21: Burns Introduction to Burn Injuries (1 of 2) 1.25-2 million Americans treated for burns annually 50,000 require 3-5% considered life threatening leading cause of death for children
7/4/2015. diffuse lung injury resulting in noncardiogenic pulmonary edema due to increase in capillary permeability
 Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
Sachiko YAMADA, Yasukazu SHIINO, Keiko MIYAJI, Jun SUGIURA, Nobuharu TAKEHARA, Jiro TAKAHASHI, Toshihiro HOTTA, Takahiro INOUE, Ryukoh OGINO
 Kawasaki Medical Journal 42(1):9-13,2016 doi:10.11482/kmj-e42(1)9 9 Case Report A Case of Non-Operative Management for Sulfuric Acid Burns Sachiko YAMADA, Yasukazu SHIINO, Keiko MIYAJI, Jun SUGIURA, Nobuharu
Kawasaki Medical Journal 42(1):9-13,2016 doi:10.11482/kmj-e42(1)9 9 Case Report A Case of Non-Operative Management for Sulfuric Acid Burns Sachiko YAMADA, Yasukazu SHIINO, Keiko MIYAJI, Jun SUGIURA, Nobuharu
EVALUATION OF SELF LEARNING BASED ON WHO MANUAL SURGICAL CARE AT THE DISTRICT HOSPITAL (SCDH)
 EVALUATION OF SELF LEARNING BASED ON WHO MANUAL SURGICAL CARE AT THE DISTRICT HOSPITAL (SCDH) Note: For the answers, refer to the SCDH Manual. The pages listed below each question will contain the answers,
EVALUATION OF SELF LEARNING BASED ON WHO MANUAL SURGICAL CARE AT THE DISTRICT HOSPITAL (SCDH) Note: For the answers, refer to the SCDH Manual. The pages listed below each question will contain the answers,
Update on Burn Care and Resuscitation
 Niknam Eshraghi, M.D., F.A.C.S General and Burn Surgery; The Oregon Clinic Director; Oregon Burn Center, Legacy Emanuel Medical Center Affiliate Professor of Surgery, Oregon Health Sciences University
Niknam Eshraghi, M.D., F.A.C.S General and Burn Surgery; The Oregon Clinic Director; Oregon Burn Center, Legacy Emanuel Medical Center Affiliate Professor of Surgery, Oregon Health Sciences University
Contents. Preface v Reviewers vii
 Contents Preface v Reviewers vii 1 Administrative Procedures 1 1-1 Incoming Telephone Calls 1 Patient Appointments 1-2 New Patient Appointments 2 1-3 Established Patient Appointments 3 1-4 Referrals to
Contents Preface v Reviewers vii 1 Administrative Procedures 1 1-1 Incoming Telephone Calls 1 Patient Appointments 1-2 New Patient Appointments 2 1-3 Established Patient Appointments 3 1-4 Referrals to
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02
 PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT
 PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
CEDR 2018 QCDR Measures for CMS 2018 MIPS Performance Year Reporting
 ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
Critical Care Treatment Guidelines
 Critical Care Treatment Guidelines West Virginia Office of Emergency Medical Services CCT Guidelines CCT Guidelines TABLE OF CONTENTS Preface Acknowledgments Using the Guidelines INITIAL TREATMENT / UNIVERSAL
Critical Care Treatment Guidelines West Virginia Office of Emergency Medical Services CCT Guidelines CCT Guidelines TABLE OF CONTENTS Preface Acknowledgments Using the Guidelines INITIAL TREATMENT / UNIVERSAL
Cardiovascular System L-5 Special Circulations, hemorrhage and shock. Dr Than Kyaw March 2012
 Cardiovascular System L-5 Special Circulations, hemorrhage and shock Dr Than Kyaw March 2012 Special circulation (Coronary, Pulmonary, and Cerebral circulations) Introduction Special attention to circulation
Cardiovascular System L-5 Special Circulations, hemorrhage and shock Dr Than Kyaw March 2012 Special circulation (Coronary, Pulmonary, and Cerebral circulations) Introduction Special attention to circulation
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
