Extracorporeal membrane oxygenation as a rescue therapy for acute respiratory failure during chemotherapy in a patient with acute myeloid leukemia
|
|
|
- Garry Basil McKenzie
- 5 years ago
- Views:
Transcription
1 Case Report Extracorporeal membrane oxygenation as a rescue therapy for acute respiratory failure during chemotherapy in a patient with acute myeloid leukemia Sang Won Lee 1, Youn Seup Kim 2, Goohyeon Hong 2 1 Department of Internal Medicine, 2 Division of Pulmonary and Critical Care Medicine, Dankook University Hospital, Dankook University College of Medicine, Cheonan, Korea Correspondence to: Goohyeon Hong, MD. Division of Pulmonary and Critical Care Medicine, Department of Internal Medicine, Dankook University Hospital, Dankook University College of Medicine, 201 Manghyang-ro, Dongnam-gu, Cheonan 31116, Korea. hkh0519@hanmail.net. Abstract: Acute respiratory distress syndrome (ARDS) caused by pneumonia in patients with hematologic malignancies can be life-threatening. Extracorporeal membrane oxygenation (ECMO) is the only temporary treatment for patients with ARDS who are refractory to conventional treatment. However, the immunosuppression and coagulopathies in hematological malignancies such as lymphoma and acute leukemia are relative contraindications for ECMO, due to high risks of infection and bleeding. Here, we report a 22-year-old man with acute myeloid leukemia (AML) who developed pneumonia and ARDS during induction chemotherapy; he was treated with ECMO. Keywords: Extracorporeal membrane oxygenation (ECMO); acute myeloid leukemia (AML); chemotherapy Submitted Oct 20, Accepted for publication Dec 31, doi: /jtd View this article at: Introduction Acute respiratory distress syndrome (ARDS) caused by pneumonia is life-threatening, particularly in immunosuppressed patients with hematological malignancies such as acute myeloid leukemia (AML) or acute lymphoid leukemia (1-3). Extracorporeal membrane oxygenation (ECMO) is the only temporary method that can support or replace respiratory function in patients with severe refractory respiratory failure on conventional mechanical ventilator support. However, sepsis or cytopenia after chemotherapy are relative contraindications for ECMO (4,5). Compared to standard indications for ECMO, cytopenia further increases the risks of infection and bleeding. There are some data on the use of ECMO in patients with hematological malignancies (6-8), but few reports on its use in adults with AML through chemotherapy. Here, we report a patient with pneumonia and ARDS treated with ECMO during induction chemotherapy for AML. Case presentation A 22-year-old man was admitted with shortness of breath and fever that started 1 week earlier. He had no noteworthy history of medical problems or recent travel or unusual food consumption. On admission, his vital signs included a blood pressure of 140/100 mmhg, body temperature of 39.7 C, heart rate of 100 beats/min, and respiratory rate of 35 breaths/min. Chest auscultation revealed crackles in both lower lung fields. Arterial blood gas analysis (ABGA) showed ph 7.45, pco mmhg, PaO mmhg, HCO mmol/l, and SpO 2 92% on oxygen supplied via nasal prong at a flow rate of 4 L/min. A complete blood count results were as follows: leukocytes 6,870/mm 3 (segmented neutrophils 1.1%, lymphocytes 70.3%, monocytes 28.1%), hemoglobin 11.3 g/dl, hematocrit 32.4%, and platelets 37,000/mm 3. Blood chemistry was as follows: blood urea nitrogen (BUN) 7.7 mg/dl, creatinine 0.82 mg/dl, aspartate transaminase 16 U/L, alanine transaminase 25 U/L, total bilirubin
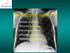
2 E134 Lee et al. ECMO rescue therapy during chemotherapy in AML A B Figure 1 Initial chest radiography and chest CT. (A) The chest radiography revealed an ill-defined patchy consolidation and GGO in both lower lung zones; (B) chest CT revealed a diffuse centrilobular GGO and consolidation in both lungs, particularly the lower lobes mg/dl, lactate dehydrogenase 331 U/L, C-reactive protein mg/dl, and procalcitonin 1.58 ng/ml. The prothrombin time (PT), international normalized ratio (INR), and activated partial thromboplastin time (aptt) were 18.1, 1.49, and 25.8 s, respectively. A chest radiography revealed ill-defined patchy consolidation in both lower lung field, particularly on the left side (Figure 1A). Chest computed tomography (CT) revealed bilateral ground glass opacities (GGO) with peribronchial consolidation in the both lower lobe, particularly on the left side (Figure 1B). Empirical intravenous antibiotic therapy was initiated with cefepime and levofloxacin. An initial sputum culture was negative, as was a sputum acid-fast bacilli (AFB) smear. On the second hospital day, his general condition and hypoxia deteriorated on a reserve mask with an oxygen flow rate of 15 L/min. He was transferred to intensive care unit and placed on mechanical ventilation. Flexible bronchoscopy for microbial evaluation showed no apparent endobronchial lesions, although bloody secretions were noted in the left upper and lower lobe bronchi. Bronchoalveolar lavage (BAL) performed in the lingular division of the left upper lobe revealed a white blood cell count of 2,480/mm 3 (segmented neutrophils 18%, lymphocytes 52%, other cells 30%); red blood cell count of 100,000/mm 3 ; no bacteria, viruses, or fungi; and negative AFB smear and culture results. All virus PCRs and microbial tests, including blood and urine cultures, were negative. On the third hospital day, the bone marrow was biopsied after finding abnormal immature blast cells in a peripheral blood smear. Despite maximal ventilator support with inhaled nitric oxide therapy with prone position, his hemodynamic and ventilator parameters were deteriorated further and chest radiography rapidly worsened (Figure 2A). The PaO 2 /FiO 2 ratio was 56, with a FiO 2 of 1.0 and a positive end-expiratory pressure (PEEP) of 10 cm H 2 O. The Murray score was 3 and the Respiratory Extracorporeal Membrane Oxygenation Survival Prediction score was 4. ECMO (Maquet Rotaflow Centrifugal Pumps with Quadrox-D oxygenators, Maquet, Rastatt, Germany) treatment was promptly established using the veno-venous method via the femorojugular route using biocoated circuits. The circuit had double access through a 17-Fr jugular catheter for oxygenated blood and a 19-Fr femoral catheter (Bio-medicus TM Medtronic, Minneapolis, MN) for deoxygenated blood to the pump. The gas exchange flow, initial oxygen fraction, pump speed, and cardiac index of VV ECMO were 6 L/min, 100%, 5,000 LPM and 2.8 L/min/m 2, respectively. Nafamostat mesylate was used as an alternative to heparin at a dosage of mg/kg/h to maintain an activated partial PT of seconds. During ECMO support, the patient was sedated and mechanically ventilated using lung protective settings of FiO 2 0.5, tidal volume ml, a respiratory rate 10 breaths/min, and PEEP 10 cm H 2 O. Acyclovir as a broad antiviral agent and Bactrim to cover Pneumocystis jiroveci were added intravenously. On the fifth hospital day, a bone marrow aspiration smear revealed that blasts made up to 64% of absolute neutrophil count (Figure 2B) and a leukemia marker study was positive for cmpo, CD34, CD117, CD13, CD33, CD38, CD123, HLA-DR. Consequently, AML (M1) was diagnosed and
3 Journal of Thoracic Disease, Vol 9, No 2 February 2017 E135 A B Figure 2 Chest radiography and bone marrow aspirate. (A) On hospital day 3, the chest radiography revealed a further increase in the extent of consolidation and GGO throughout both lungs and the ECMO catheter; (B) bone marrow aspirate shows blast cells (arrow), (optical microscope magnifications, 1,000). support was discontinued and he was maintained on a mechanical ventilator. His vital signs and PaO 2 remained stable and he had no dyspnea on the day of weaning from ECMO. Our patient had been isolated in a clean room with limited access, and laboratory tests were performed every day to check for new infections or organ failure. He was weaned from mechanical ventilator on the 19 th hospital day and transferred to general ward. Despite all of these efforts and weaning from ECMO and mechanical ventilator, he died during the consolidation chemotherapy as a result of septic shock with pancytopenia. Figure 3 On hospital day 13, the chest radiography showed an improvement in the consolidation and infiltration in both lungs. induction chemotherapy was started after consulting a hematologist, including 3 days with intravenous idarubicin 12 mg/m 2, 7 days of intravenous cytarabine 200 mg/m 2 and dexamethasone 40 mg/day. The antibiotic treatment was changed to intravenous vancomycin and meropenem to cover methicillin-resistant Streptococcus aureus and extended-spectrum beta-lactamase-positive bacteria and an intravenous antifungal agent was initiated. A bedside tracheostomy was performed on his 11 th hospital day because of prolonged intubation. There were no signs of significant bleeding such as intracranial hemorrhage or secondary infection. On the 13 th day, chest radiography showed improvements in his pneumonia and ARDS (Figure 3). As his vital signs were stable, the ECMO Discussion ARDS may develop in patients with hematological malignancies, resulting in high morbidity and mortality. Chemotherapy often induces prolonged periods of marrow aplasia, leading to neutropenia, thrombocytopenia and defective immunity. Consequently, patients are more susceptible to bacterial, viral and fungal infections. In patients with acute leukemia, pulmonary leukemic cell infiltration and subsequent pulmonary failure remain an unresolved problem and major cause of death (1). Immediately or shortly after induction chemotherapy, acute lysis pneumopathy can cause diffuse alveolar damage (9). Moreau et al. was reported that more than 80% of patients experienced acute respiratory events early days of the AML diagnosis and 61% of all respiratory events were related to leukemia-specific lung involvement (10). Therefore, there was probability of acute respiratory events related to AML such as pulmonary leukemic infiltration in our patient
4 E136 Lee et al. ECMO rescue therapy during chemotherapy in AML because we did not find any pathogen in our patient. One technique to improve the survival of patients with hematological malignancies with pulmonary failure is ECMO, which markedly benefits critically ill patients with severe respiratory failure refractory to conventional treatment including mechanical ventilation (11). However, compared with standard indications for ECMO, chemotherapy-induced cytopenia and respiratory failure pose additional medical challenges for the treatment of patients with acute leukemia when considering ECMO. Patients with hematological malignancies and a suppressed immune system on ECMO can develop severe complications, such as infections and bleeding. The risk of ECMO-induced septic episodes is increased in immunocompromised, severely neutropenic patients due to hematologic malignancies with chemotherapy. Even in immunocompetent patients, ECMO support is a high-risk procedure for nosocomial infection. Moreover, there is a high risk of bleeding and a markedly increased demand for transfusions during ECMO in acute leukemia and the need for anticoagulation can lead to hemorrhage with increased requirement for blood transfusions. These conditions remain a major cause of therapy-associated morbidity and death. With improvements in ECMO technology and expertise lowering morbidity and mortality, the criteria for the use of ECMO may be extended to ARDS patients with hematological malignancies such as acute leukemia and lymphoma (7,12). Wohlfarth et al. (7) reported a remarkable 50% survival rate, despite the presence of numerous factors known to be associated with an adverse outcome in patients with hematological malignancies undergoing ECMO. Consequently, we used veno-venous ECMO in this case. Our patient was a healthy young adult before this event, but he deteriorated rapidly at the initiation of chemotherapy. He was eligible candidate for ECMO as a rescue therapy because of very severe refractory hypoxemia with short high FiO 2 ventilation period. ECMO was instituted urgently to restore hemodynamic stability, improve end-organ function, and bridge the patient during consequences of additional chemotherapy administration until the tumor burden could be adequately reduced. After completing induction chemotherapy, the ECMO was discontinued and the patient decannulated at the bedside. There are some reports on weaning adult patients with hematological malignancies such as acute lymphoid leukemia, lymphoma, and multiple myeloma from ECMO (7,12). However, there are few reports of performing this during induction chemotherapy in an adult with AML (8). Our experience indicates that ARDS caused by pneumonia in patients with undergoing chemotherapy for acute leukemia should not be considered a contraindication to ECMO treatment. As successful treatment is associated with early initiation, we suggest that ECMO be started in the presence of severe hemodynamic instability or respiratory failure refractory to standard medical support. In conclusion, ECMO is a supportive tool that reduces the incidence of early treatment-related mortality and will ultimately improve the overall survival in patients with ARDS and pneumonia during induction chemotherapy for acute leukemia. Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. Informed Consent: Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images. References 1. Azoulay E, Mokart D, Pène F, et al. Outcomes of critically ill patients with hematologic malignancies: prospective multicenter data from France and Belgium-a groupe de recherche respiratoire en réanimation onco-hématologique study. J Clin Oncol 2013;31: Vadde R, Pastores SM. Management of Acute Respiratory Failure in Patients with Hematological Malignancy. J Intensive Care Med [Epub ahead of print]. 3. Azoulay E, Mokart D, Lambert J, et al. Diagnostic strategy for hematology and oncology patients with acute respiratory failure: randomized controlled trial. Am J Respir Crit Care Med 2010;182: Kasirajan V, Smedira NG, McCarthy JF, et al. Risk factors for intracranial hemorrhage in adults on extracorporeal membrane oxygenation. Eur J Cardiothorac Surg 1999;15: Maclaren G, Butt W. Extracorporeal membrane oxygenation and sepsis. Crit Care Resusc 2007;9: Worku B, DeBois W, Sobol I, et al. Extracorporeal
5 Journal of Thoracic Disease, Vol 9, No 2 February 2017 E137 Membrane Oxygenation as a Bridge through Chemotherapy in B-Cell Lymphoma. J Extra Corpor Technol 2015;47: Wohlfarth P, Ullrich R, Staudinger T, et al. Extracorporeal membrane oxygenation in adult patients with hematologic malignancies and severe acute respiratory failure. Crit Care 2014;18:R Kang HS, Rhee CK, Lee HY, et al. Clinical outcomes of extracorporeal membrane oxygenation support in patients with hematologic malignancies. Korean J Intern Med 2015;30: Tryka AF, Godleski JJ, Fanta CH. Leukemic cell lysis pneumonopathy. A complication of treated myeloblastic leukemia. Cancer 1982;50: Moreau AS, Lengline E, Seguin A, et al. Respiratory events at the earliest phase of acute myeloid leukemia. Leuk Lymphoma 2014;55: Ventetuolo CE, Muratore CS. Extracorporeal life support in critically ill adults. Am J Respir Crit Care Med 2014;190: Gorjup V, Fister M, Noc M, et al. Treatment of sepsis and ARDS with extracorporeal membrane oxygenation and interventional lung assist membrane ventilator in a patient with acute lymphoblastic leukemia. Respir Care 2012;57: Cite this article as: Lee SW, Kim YS, Hong G. Extracorporeal membrane oxygenation as a rescue therapy for acute respiratory failure during chemotherapy in a patient with acute myeloid leukemia.. doi: / jtd
ECMO: a breakthrough in care for respiratory failure. PD Dr. Thomas Müller Regensburg no conflict of interest
 ECMO: a breakthrough in care for respiratory failure? PD Dr. Thomas Müller Regensburg no conflict of interest 1 Overview Mortality of severe ARDS Indication for ECMO PaO 2 /FiO 2 Efficiency of ECMO: gas
ECMO: a breakthrough in care for respiratory failure? PD Dr. Thomas Müller Regensburg no conflict of interest 1 Overview Mortality of severe ARDS Indication for ECMO PaO 2 /FiO 2 Efficiency of ECMO: gas
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids
 Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
ECMO in oncology and immunosupressed patients. Peter Schellongowski Department of Medicine I Intensive Care Unit 13.i2 Medical University of Vienna
 ECMO in oncology and immunosupressed patients Peter Schellongowski Department of Medicine I Intensive Care Unit 13.i2 Medical University of Vienna ECMO in immunocompromised patients? Is it feasible? Is
ECMO in oncology and immunosupressed patients Peter Schellongowski Department of Medicine I Intensive Care Unit 13.i2 Medical University of Vienna ECMO in immunocompromised patients? Is it feasible? Is
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate. Carolyn Calfee, MD MAS Mark Eisner, MD MPH
 ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate Carolyn Calfee, MD MAS Mark Eisner, MD MPH June 3, 2010 Case Presentation Setting: Community hospital, November 2009 29 year old woman with
ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate Carolyn Calfee, MD MAS Mark Eisner, MD MPH June 3, 2010 Case Presentation Setting: Community hospital, November 2009 29 year old woman with
ARDS during Neutropenia. D Mokart DAR IPC GRRRRROH 2010
 ARDS during Neutropenia D Mokart DAR IPC GRRRRROH 2010 Definitions Neutropenia is a decrease in circulating neutrophil white cells in the peripheral blood. neutrophil count of 1,000 1,500 cells/ml = mild
ARDS during Neutropenia D Mokart DAR IPC GRRRRROH 2010 Definitions Neutropenia is a decrease in circulating neutrophil white cells in the peripheral blood. neutrophil count of 1,000 1,500 cells/ml = mild
Outcomes From Severe ARDS Managed Without ECMO. Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016
 Outcomes From Severe ARDS Managed Without ECMO Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016 Severe ARDS Berlin Definition 2012 P:F ratio 100 mm Hg Prevalence:
Outcomes From Severe ARDS Managed Without ECMO Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016 Severe ARDS Berlin Definition 2012 P:F ratio 100 mm Hg Prevalence:
Prolonged Extracorporeal Membrane Oxygenation Support for Acute Respiratory Distress Syndrome
 CASE REPORT Prolonged Extracorporeal Membrane Oxygenation Support for Acute Respiratory Distress Syndrome Wen-Je Ko,* Hsao-Hsun Hsu, Pi-Ru Tsai When all conventional treatments for respiratory failure
CASE REPORT Prolonged Extracorporeal Membrane Oxygenation Support for Acute Respiratory Distress Syndrome Wen-Je Ko,* Hsao-Hsun Hsu, Pi-Ru Tsai When all conventional treatments for respiratory failure
CASE PRESENTATION VV ECMO
 CASE PRESENTATION VV ECMO Joshua Huelster, MD Fellow in Critical Care Medicine Department of Pulmonary and Critical Care Medicine Hennepin County Medical Center Disclosure There are no conflicts of interest
CASE PRESENTATION VV ECMO Joshua Huelster, MD Fellow in Critical Care Medicine Department of Pulmonary and Critical Care Medicine Hennepin County Medical Center Disclosure There are no conflicts of interest
DAILY SCREENING FORM
 DAILY SCREENING FORM Patient s initials: Date of admission: Time of admission: Gender: M F Year of Birth: Type of admission: Medical/Surgical/Postoperative (elective) Days Date Mechanical ventilation Lung
DAILY SCREENING FORM Patient s initials: Date of admission: Time of admission: Gender: M F Year of Birth: Type of admission: Medical/Surgical/Postoperative (elective) Days Date Mechanical ventilation Lung
CRRT Fundamentals Pre- and Post- Test. AKI & CRRT Conference 2018
 CRRT Fundamentals Pre- and Post- Test AKI & CRRT Conference 2018 Question 1 Which ONE of the following statements regarding solute clearance in CRRT is MOST correct? A. Convective and diffusive solute
CRRT Fundamentals Pre- and Post- Test AKI & CRRT Conference 2018 Question 1 Which ONE of the following statements regarding solute clearance in CRRT is MOST correct? A. Convective and diffusive solute
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Outcome of patients with hematologic malignancy admitted to the ICU
 Outcome of patients with hematologic malignancy admitted to the ICU Geeta Mehta MD, FRCPC Mount Sinai Hospital Toronto, Canada CCCF November 2, 2016 Disclosures Hematologic Malignancy Advances in diagnostics,
Outcome of patients with hematologic malignancy admitted to the ICU Geeta Mehta MD, FRCPC Mount Sinai Hospital Toronto, Canada CCCF November 2, 2016 Disclosures Hematologic Malignancy Advances in diagnostics,
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
Systemic inflammatory response syndrome (SIRS) after extracorporeal membrane oxygenation (ECMO): Incidence, risks and survivals.
 Thomas Jefferson University Jefferson Digital Commons Department of Surgery Faculty Papers Department of Surgery 9-1-2016 Systemic inflammatory response syndrome (SIRS) after extracorporeal membrane oxygenation
Thomas Jefferson University Jefferson Digital Commons Department of Surgery Faculty Papers Department of Surgery 9-1-2016 Systemic inflammatory response syndrome (SIRS) after extracorporeal membrane oxygenation
ERJ Express. Published on August 9, 2012 as doi: /
 ERJ Express. Published on August 9, 2012 as doi: 10.1183/09031936.00076912 Extracorporeal membrane oxygenation in a non intubated patient with acute respiratory distress syndrome (ARDS) Olaf Wiesner, *
ERJ Express. Published on August 9, 2012 as doi: 10.1183/09031936.00076912 Extracorporeal membrane oxygenation in a non intubated patient with acute respiratory distress syndrome (ARDS) Olaf Wiesner, *
ARDS: an update 6 th March A. Hakeem Al Hashim, MD, FRCP SQUH
 ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
Adult Extracorporeal Life Support (ECLS)
 Adult Extracorporeal Life Support (ECLS) Steven Scott, M.D., F.A.C.S. Piedmont Heart Institute Cardiothoracic Surgery Disclosures None ECMO = ECLS A technique of life support that involves a continuous
Adult Extracorporeal Life Support (ECLS) Steven Scott, M.D., F.A.C.S. Piedmont Heart Institute Cardiothoracic Surgery Disclosures None ECMO = ECLS A technique of life support that involves a continuous
CRRT Fundamentals Pre-Test. AKI & CRRT 2017 Practice Based Learning in CRRT
 CRRT Fundamentals Pre-Test AKI & CRRT 2017 Practice Based Learning in CRRT Question 1 A 72-year-old man with HTN presents to the ED with slurred speech, headache and weakness after falling at home. He
CRRT Fundamentals Pre-Test AKI & CRRT 2017 Practice Based Learning in CRRT Question 1 A 72-year-old man with HTN presents to the ED with slurred speech, headache and weakness after falling at home. He
ECLS as Bridge to Transplant
 ECLS as Bridge to Transplant Marcelo Cypel MD, MSc Assistant Professor of Surgery Division of Thoracic Surgery Toronto General Hospital University of Toronto Application of ECLS Bridge to lung recovery
ECLS as Bridge to Transplant Marcelo Cypel MD, MSc Assistant Professor of Surgery Division of Thoracic Surgery Toronto General Hospital University of Toronto Application of ECLS Bridge to lung recovery
A Vietnamese woman with a 2-week history of cough
 Delphine Natali 1, Hai Tran Pham 1, Hung Nguyen The 2 delphinenatali@gmail.com Case report A Vietnamese woman with a 2-week history of cough A 52-year-old nonsmoker Vietnamese woman without any past medical
Delphine Natali 1, Hai Tran Pham 1, Hung Nguyen The 2 delphinenatali@gmail.com Case report A Vietnamese woman with a 2-week history of cough A 52-year-old nonsmoker Vietnamese woman without any past medical
ECCO 2 Removal The Perfusionists Perspective
 ECCO 2 Removal The Perfusionists Perspective BelSECT Education evening 2016-06-15 D. Hella, Th. Amand, J-N Koch Definition ECCO 2 Removal: Process by which an extracorporeal circuit is used for removing
ECCO 2 Removal The Perfusionists Perspective BelSECT Education evening 2016-06-15 D. Hella, Th. Amand, J-N Koch Definition ECCO 2 Removal: Process by which an extracorporeal circuit is used for removing
PULMONARY MEDICINE BOARD REVIEW. Financial Conflicts of Interest. Question #1: Question #1 (Cont.): None. Christopher H. Fanta, M.D.
 PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
Choc septique. Frédéric Pène
 Choc septique Frédéric Pène Réanimation Médicale, Hôpital Cochin, AP-HP Université Paris Descartes Institut Cochin, Inserm U1016, CNRS UMR-8104, Département 3i No conflict of interest A 54 y.o. male patient
Choc septique Frédéric Pène Réanimation Médicale, Hôpital Cochin, AP-HP Université Paris Descartes Institut Cochin, Inserm U1016, CNRS UMR-8104, Département 3i No conflict of interest A 54 y.o. male patient
Extracorporeal Membrane Oxygenation (ECMO)
 Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2017 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2017 Section: Other/Miscellaneous
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Septic shock. Babak Tamizi Far M.D Isfahan university of medical sciences
 Septic shock Babak Tamizi Far M.D Isfahan university of medical sciences Definitions Used to Describe the Condition of Septic Patients Approximately 750,000 cases of severe sepsis or septic shock occur
Septic shock Babak Tamizi Far M.D Isfahan university of medical sciences Definitions Used to Describe the Condition of Septic Patients Approximately 750,000 cases of severe sepsis or septic shock occur
Extracorporeal Membrane Oxygenation (ECMO)
 Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/01/2014 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/01/2014 Section: Other/Miscellaneous
Immunomodulation and Sepsis in Oncological Patients. Imad Haddad, M.D. Medical Director, PICU Banner Children s Hospital at BDMC
 Immunomodulation and Sepsis in Oncological Patients Imad Haddad, M.D. Medical Director, PICU Banner Children s Hospital at BDMC 1 Objectives Immune dys-regulation in oncological septic patients Implementation
Immunomodulation and Sepsis in Oncological Patients Imad Haddad, M.D. Medical Director, PICU Banner Children s Hospital at BDMC 1 Objectives Immune dys-regulation in oncological septic patients Implementation
Prone ventilation revisited in H1N1 patients
 International Journal of Advanced Multidisciplinary Research ISSN: 2393-8870 www.ijarm.com DOI: 10.22192/ijamr Volume 5, Issue 10-2018 Case Report DOI: http://dx.doi.org/10.22192/ijamr.2018.05.10.005 Prone
International Journal of Advanced Multidisciplinary Research ISSN: 2393-8870 www.ijarm.com DOI: 10.22192/ijamr Volume 5, Issue 10-2018 Case Report DOI: http://dx.doi.org/10.22192/ijamr.2018.05.10.005 Prone
ECMO for Refractory Septic Shock Prof. Alain Combes
 ECMO for Refractory Septic Shock Prof. Alain Combes Service de Réanimation ican, Institute of Cardiometabolism and Nutrition Hôpital Pitié-Salpêtrière, AP-HP, Paris Université Pierre et Marie Curie, Paris
ECMO for Refractory Septic Shock Prof. Alain Combes Service de Réanimation ican, Institute of Cardiometabolism and Nutrition Hôpital Pitié-Salpêtrière, AP-HP, Paris Université Pierre et Marie Curie, Paris
EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) REFERRAL FORM
 Patient Label This form is accessible on www.royalpapworth.nhs.uk Intensive Care Unit EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) REFERRAL FORM Please always phone Papworth ECMO Coordinator on 01480 830541,
Patient Label This form is accessible on www.royalpapworth.nhs.uk Intensive Care Unit EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) REFERRAL FORM Please always phone Papworth ECMO Coordinator on 01480 830541,
Septic Shock. Rontgene M. Solante, MD, FPCP,FPSMID
 Septic Shock Rontgene M. Solante, MD, FPCP,FPSMID Learning Objectives Identify situations wherein high or low BP are hemodynamically significant Recognize complications arising from BP emergencies Manage
Septic Shock Rontgene M. Solante, MD, FPCP,FPSMID Learning Objectives Identify situations wherein high or low BP are hemodynamically significant Recognize complications arising from BP emergencies Manage
Extracorporeal Membrane Oxygenation in Nivolumab Associated Pneumonitis
 The Journal of Critical Care Medicine 2017;3(2):84-88 CASE REPORT Extracorporeal Membrane Oxygenation in Nivolumab Associated Pneumonitis Thomas-Michael Schneider 1*, Friederike Klenner 2, Franz Brettner
The Journal of Critical Care Medicine 2017;3(2):84-88 CASE REPORT Extracorporeal Membrane Oxygenation in Nivolumab Associated Pneumonitis Thomas-Michael Schneider 1*, Friederike Klenner 2, Franz Brettner
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
7/4/2015. diffuse lung injury resulting in noncardiogenic pulmonary edema due to increase in capillary permeability
 Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
Veno-Venous ECMO Support. Chris Cropsey, MD Sept. 21, 2015
 Veno-Venous ECMO Support Chris Cropsey, MD Sept. 21, 2015 Objectives List indications and contraindications for ECMO Describe hemodynamics and oxygenation on ECMO Discuss evidence for ECMO outcomes Identify
Veno-Venous ECMO Support Chris Cropsey, MD Sept. 21, 2015 Objectives List indications and contraindications for ECMO Describe hemodynamics and oxygenation on ECMO Discuss evidence for ECMO outcomes Identify
Extracorporeal support in acute respiratory failure. Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London
 Extracorporeal support in acute respiratory failure Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London Objectives By the end of this session, you will be able to: Describe different
Extracorporeal support in acute respiratory failure Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London Objectives By the end of this session, you will be able to: Describe different
Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye
 Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye Steroids in ARDS: conclusion Give low-dose steroids if indicated for another problem
Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye Steroids in ARDS: conclusion Give low-dose steroids if indicated for another problem
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: The National Heart, Lung, and Blood Institute Acute Respiratory
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: The National Heart, Lung, and Blood Institute Acute Respiratory
Chapter 22. Pulmonary Infections
 Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Severe β-lactam allergy. Alternative (use for mild-moderate β-lactam allergy) therapy
 Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
The Pulmonary Pathology of Iatrogenic Immunosuppression. Kevin O. Leslie, M.D. Mayo Clinic Scottsdale
 The Pulmonary Pathology of Iatrogenic Immunosuppression Kevin O. Leslie, M.D. Mayo Clinic Scottsdale The indications for iatrogenic immunosuppression Autoimmune/inflammatory disease Chemotherapy for malignant
The Pulmonary Pathology of Iatrogenic Immunosuppression Kevin O. Leslie, M.D. Mayo Clinic Scottsdale The indications for iatrogenic immunosuppression Autoimmune/inflammatory disease Chemotherapy for malignant
Extracorporeal membrane oxygenators (ECMO) provide
 Case Report Interhospital Transport of the ECMO Patients in Bangkok Hospital Abstract An extracorporeal membrane oxygenator (ECMO) is used to support the heart and lungs in patients with severe cardiogenic
Case Report Interhospital Transport of the ECMO Patients in Bangkok Hospital Abstract An extracorporeal membrane oxygenator (ECMO) is used to support the heart and lungs in patients with severe cardiogenic
ESCMID Online Lecture Library. by author. CASE PRESENTATION ECCMID clinical grand round May Anat Stern, MD Rambam medical center Haifa, Israel
 CASE PRESENTATION ECCMID clinical grand round May 2014 Anat Stern, MD Rambam medical center Haifa, Israel An 18 years old Female, from Ukraine, diagnosed with acute lymphoblastic leukemia (ALL) in 2003.
CASE PRESENTATION ECCMID clinical grand round May 2014 Anat Stern, MD Rambam medical center Haifa, Israel An 18 years old Female, from Ukraine, diagnosed with acute lymphoblastic leukemia (ALL) in 2003.
Invasive Pulmonary Aspergillosis in
 Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Surviving Sepsis Campaign. Guidelines for Management of Severe Sepsis/Septic Shock. An Overview
 Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Pharmacokinetics of caspofungin in a critically ill patient with liver cirrhosis
 Pharmacokinetics of caspofungin in a critically ill patient with liver cirrhosis Isabel Spriet, Wouter Meersseman, Pieter Annaert, Jan Hoon, Ludo Willems To cite this version: Isabel Spriet, Wouter Meersseman,
Pharmacokinetics of caspofungin in a critically ill patient with liver cirrhosis Isabel Spriet, Wouter Meersseman, Pieter Annaert, Jan Hoon, Ludo Willems To cite this version: Isabel Spriet, Wouter Meersseman,
How hematologists perceive critical care- Acute myeloid leukemia
 How hematologists perceive critical care- Acute myeloid leukemia Groupe de Recherche Respiratoire en Réanimation Onco-Hématologique Research Meeting June 30 th 2011 Peter Schellongowski Intensive Care
How hematologists perceive critical care- Acute myeloid leukemia Groupe de Recherche Respiratoire en Réanimation Onco-Hématologique Research Meeting June 30 th 2011 Peter Schellongowski Intensive Care
Breathing life into new therapies: Updates on treatment for severe respiratory failure. Whitney Gannon, MSN ACNP-BC
 Breathing life into new therapies: Updates on treatment for severe respiratory failure Whitney Gannon, MSN ACNP-BC Overview Definition of ARDS Clinical signs and symptoms Causes Pathophysiology Management
Breathing life into new therapies: Updates on treatment for severe respiratory failure Whitney Gannon, MSN ACNP-BC Overview Definition of ARDS Clinical signs and symptoms Causes Pathophysiology Management
Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation
 Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation Gabriel Loor, MD Baylor St. Lukes Medical Center Surgical Director Lung Transplantation Co-chief Section of Adult Cardiac
Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation Gabriel Loor, MD Baylor St. Lukes Medical Center Surgical Director Lung Transplantation Co-chief Section of Adult Cardiac
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
EXTRA CORPOREAL MEMBRANE OXYGENATION
 EXTRA CORPOREAL MEMBRANE OXYGENATION Basic Overview and Case Study Bob Hayes, Chief Perfusionist Enloe Medical Center Jenny Humphries, RN, BSN, MBA, CFRN Chief Flight Nurse, Enloe FlightCare Normal Cardiopulmonary
EXTRA CORPOREAL MEMBRANE OXYGENATION Basic Overview and Case Study Bob Hayes, Chief Perfusionist Enloe Medical Center Jenny Humphries, RN, BSN, MBA, CFRN Chief Flight Nurse, Enloe FlightCare Normal Cardiopulmonary
Rounds in the ICU. Eran Segal, MD Director General ICU Sheba Medical Center
 Rounds in the ICU Eran Segal, MD Director General ICU Sheba Medical Center Real Clinical cases (including our mistakes) Emphasis on hemodynamic monitoring Usually no single correct answer We will conduct
Rounds in the ICU Eran Segal, MD Director General ICU Sheba Medical Center Real Clinical cases (including our mistakes) Emphasis on hemodynamic monitoring Usually no single correct answer We will conduct
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
BC Cancer Protocol Summary for Therapy of Acute Myeloid Leukemia Using azacitidine and SORAfenib
 BC Cancer Protocol Summary for Therapy of Acute Myeloid Leukemia Using azacitidine and SORAfenib Protocol Code Tumour Group Contact Physician ULKAMLAS Leukemia/BMT Dr. Donna Hogge ELIGIBILITY: Acute myeloid
BC Cancer Protocol Summary for Therapy of Acute Myeloid Leukemia Using azacitidine and SORAfenib Protocol Code Tumour Group Contact Physician ULKAMLAS Leukemia/BMT Dr. Donna Hogge ELIGIBILITY: Acute myeloid
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Sample Case Study. The patient was a 77-year-old female who arrived to the emergency room on
 Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Exam 1 Review. Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies
 Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Advance Pathology Services, P.C Professional Drive, Suite 3 Cadillac, MI Phone: Fax:
 Advance Pathology Services, P.C. 8865 Professional Drive, Suite 3 Cadillac, MI 49601 Phone: 231-468-2346 Fax: 231-468-2349 Pathology Analysis: Pneumonia and Pulmonary Hemorrhage Cause Death; Clinically
Advance Pathology Services, P.C. 8865 Professional Drive, Suite 3 Cadillac, MI 49601 Phone: 231-468-2346 Fax: 231-468-2349 Pathology Analysis: Pneumonia and Pulmonary Hemorrhage Cause Death; Clinically
Immunocompromised patients. Immunocompromised patients. Immunocompromised patients
 Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
Sepsis new definitions of sepsis and septic shock and Novelities in sepsis treatment
 Sepsis new definitions of sepsis and septic shock and Novelities in sepsis treatment What is sepsis? Life-threatening organ dysfunction caused by a dysregulated host response to infection A 1991 consensus
Sepsis new definitions of sepsis and septic shock and Novelities in sepsis treatment What is sepsis? Life-threatening organ dysfunction caused by a dysregulated host response to infection A 1991 consensus
Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill
 Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill Joe Palumbo PGY-2 Critical Care Pharmacy Resident Buffalo General Medical Center Disclosures
Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill Joe Palumbo PGY-2 Critical Care Pharmacy Resident Buffalo General Medical Center Disclosures
Management of refractory ARDS. Saurabh maji
 Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Pheochromocytoma Crisis Presenting as Fulminant Cardiopulmonary Failure: A Case Report
 170 Pheochromocytoma Crisis Presenting as Fulminant Cardiopulmonary Failure: A Case Report Chun-Wen Chiu 1, Cheng-Hsiung Chen 2 Fulminant cardiopulmonary failure in a patient with pheochromocytoma is a
170 Pheochromocytoma Crisis Presenting as Fulminant Cardiopulmonary Failure: A Case Report Chun-Wen Chiu 1, Cheng-Hsiung Chen 2 Fulminant cardiopulmonary failure in a patient with pheochromocytoma is a
clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS*
 clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS* Sanjay R. Patel, MD; Dimitri Karmpaliotis, MD; Najib T. Ayas, MD; Eugene J. Mark, MD; John Wain, MD, FCCP; B. Taylor Thompson,
clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS* Sanjay R. Patel, MD; Dimitri Karmpaliotis, MD; Najib T. Ayas, MD; Eugene J. Mark, MD; John Wain, MD, FCCP; B. Taylor Thompson,
Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data
 Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data David Ebler, MD David Skarupa, MD Andrew J. Kerwin, MD, FACS Jhun de Villa, MD Michael S. Nussbaum, MD, FACS J.J. Tepas III, MD, FACS
Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data David Ebler, MD David Skarupa, MD Andrew J. Kerwin, MD, FACS Jhun de Villa, MD Michael S. Nussbaum, MD, FACS J.J. Tepas III, MD, FACS
Staging Sepsis for the Emergency Department: Physician
 Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Does proning patients with refractory hypoxaemia improve mortality?
 Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
Acute Respiratory Distress Syndrome in Immunocompromised Patients
 Acute Respiratory Distress Syndrome in Immunocompromised Patients Laveena Munshi, MD, MSc Critical Care Canada Forum November 2018 Interdepartmental Division of Critical Care Medicine Mount Sinai Hospital/University
Acute Respiratory Distress Syndrome in Immunocompromised Patients Laveena Munshi, MD, MSc Critical Care Canada Forum November 2018 Interdepartmental Division of Critical Care Medicine Mount Sinai Hospital/University
ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013
 ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013 Pauline K. Park MD, FACS, FCCM University of Michigan School of Medicine Ann Arbor, MI OVERVIEW New Berlin definition of ARDS
ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013 Pauline K. Park MD, FACS, FCCM University of Michigan School of Medicine Ann Arbor, MI OVERVIEW New Berlin definition of ARDS
Sepsis is an important issue. Clinician s decision-making capability. Guideline recommendations
 Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012 Clinicians decision-making capability Guideline recommendations Sepsis is an important issue 8.7%
Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012 Clinicians decision-making capability Guideline recommendations Sepsis is an important issue 8.7%
Diagnostic Procedures for Pulmonary Infiltrates in the Compromised Host
 Diagnostic Procedures for Pulmonary Infiltrates in the Compromised Host Michael Douvas, MD Heme/Onc Gerald Donowitz, MD - ID Eric Davis, MD - Pulmonary Disclosure Drs. Davis, Donowitz, and Douvas do not
Diagnostic Procedures for Pulmonary Infiltrates in the Compromised Host Michael Douvas, MD Heme/Onc Gerald Donowitz, MD - ID Eric Davis, MD - Pulmonary Disclosure Drs. Davis, Donowitz, and Douvas do not
Radiological syndroms. Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome
 Radiological syndroms Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome Alveolar syndrome Pulmonary architecture : Morphological unit is the lobule 15-25mm
Radiological syndroms Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome Alveolar syndrome Pulmonary architecture : Morphological unit is the lobule 15-25mm
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Case scenario V AV ECMO. Dr Pranay Oza
 Case scenario V AV ECMO Dr Pranay Oza Case Summary 53 y/m, k/c/o MVP with myxomatous mitral valve with severe Mitral regurgitation underwent Mitral valve replacement with mini thoracotomy Pump time nearly
Case scenario V AV ECMO Dr Pranay Oza Case Summary 53 y/m, k/c/o MVP with myxomatous mitral valve with severe Mitral regurgitation underwent Mitral valve replacement with mini thoracotomy Pump time nearly
Keeping Patients Off the Vent: Bilevel, HFNC, Neither?
 Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
11/19/2012. The spectrum of pulmonary diseases in HIV-infected persons is broad.
 The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
Early Klebsiella pneumoniae Liver Abscesses associated with Pylephlebitis Mimic
 Early Klebsiella pneumoniae Liver Abscesses associated with Pylephlebitis Mimic Hepatocellular Carcinoma Chih-Hao Shen, MD 3, Jung-Chung Lin, MD, PhD 2, Hsuan-Hwai Lin, MD 1, You-Chen Chao, MD 1, and Tsai-Yuan
Early Klebsiella pneumoniae Liver Abscesses associated with Pylephlebitis Mimic Hepatocellular Carcinoma Chih-Hao Shen, MD 3, Jung-Chung Lin, MD, PhD 2, Hsuan-Hwai Lin, MD 1, You-Chen Chao, MD 1, and Tsai-Yuan
Antimicrobial Management of Febrile Neutropenic Sepsis
 Antimicrobial Management of Febrile Neutropenic Sepsis Written by: Dr J Joseph, Consultant Haematologist Dr K Gajee, Consultant Microbiologist Amended by: Larissa Claybourn, Antimicrobial Pharmacist Date:
Antimicrobial Management of Febrile Neutropenic Sepsis Written by: Dr J Joseph, Consultant Haematologist Dr K Gajee, Consultant Microbiologist Amended by: Larissa Claybourn, Antimicrobial Pharmacist Date:
Troubleshooting Adult ECMO
 The Journal of ExtraCorporeal Technology Troubleshooting Adult ECMO David Sidebotham, FANZCA Departments of Anaesthesia and Intensive Care, Auckland City Hospital, Auckland, New Zealand Presented at Perfusion
The Journal of ExtraCorporeal Technology Troubleshooting Adult ECMO David Sidebotham, FANZCA Departments of Anaesthesia and Intensive Care, Auckland City Hospital, Auckland, New Zealand Presented at Perfusion
Trial protocol - NIVAS Study
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
Panel Discussion: What s New with DRGs and ICD?
 Panel Discussion: What s New with DRGs and ICD? Moderator: Angie Comfort, RHIA, CDIP, CCS, CCS-P Thilo Koepfer, MD Wilbur Lo, MD, CDIP, CCA Objectives Get updated on the current status of ICD- 11 IR-DRG
Panel Discussion: What s New with DRGs and ICD? Moderator: Angie Comfort, RHIA, CDIP, CCS, CCS-P Thilo Koepfer, MD Wilbur Lo, MD, CDIP, CCA Objectives Get updated on the current status of ICD- 11 IR-DRG
This was a multicenter study conducted at 11 sites in the United States and 11 sites in Europe.
 Protocol CAM211: A Phase II Study of Campath-1H (CAMPATH ) in Patients with B- Cell Chronic Lymphocytic Leukemia who have Received an Alkylating Agent and Failed Fludarabine Therapy These results are supplied
Protocol CAM211: A Phase II Study of Campath-1H (CAMPATH ) in Patients with B- Cell Chronic Lymphocytic Leukemia who have Received an Alkylating Agent and Failed Fludarabine Therapy These results are supplied
NCCP Chemotherapy Regimen
 INDICATIONS FOR USE: Azacitidine i INDICATION ICD10 Regimen Code *Reimbursement Status Intermediate-1 and low risk myelodysplastic syndromes (MDS) according to the International Prognostic Scoring System
INDICATIONS FOR USE: Azacitidine i INDICATION ICD10 Regimen Code *Reimbursement Status Intermediate-1 and low risk myelodysplastic syndromes (MDS) according to the International Prognostic Scoring System
Community Acquired Pneumonia. Abdullah Alharbi, MD, FCCP
 Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Data Collection Tool. Standard Study Questions: Admission Date: Admission Time: Age: Gender:
 Data Collection Tool Standard Study Questions: Admission Date: Admission Time: Age: Gender: Specifics of Injury: Time of Injury: Mechanism of Injury Blunt vs Penetrating? Injury Severity Score? Injuries:
Data Collection Tool Standard Study Questions: Admission Date: Admission Time: Age: Gender: Specifics of Injury: Time of Injury: Mechanism of Injury Blunt vs Penetrating? Injury Severity Score? Injuries:
Supplementary Online Content
 Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
During the past two decades,
 Prospectively validated prediction of physiologic variables and organ failure in septic patients: The Systemic Mediator Associated Response Test (SMART) Gus J. Slotman, MD Objective: Conventional outcomes
Prospectively validated prediction of physiologic variables and organ failure in septic patients: The Systemic Mediator Associated Response Test (SMART) Gus J. Slotman, MD Objective: Conventional outcomes
MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSPLANTATION
 MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSP There are no translations available. MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSPLANTATION
MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSP There are no translations available. MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSPLANTATION
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS
 REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016
 Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016 Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care
Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016 Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care
2009 H1N1 influenza virus infection and necrotizing pneumonia treated with extracorporeal membrane oxygenation
 Case report http://dx.doi.org/10.3345/kjp.2011.54.8.345 Korean J Pediatr 2011;54(8):345-349 2009 H1N1 influenza virus infection and necrotizing pneumonia treated with extracorporeal membrane oxygenation
Case report http://dx.doi.org/10.3345/kjp.2011.54.8.345 Korean J Pediatr 2011;54(8):345-349 2009 H1N1 influenza virus infection and necrotizing pneumonia treated with extracorporeal membrane oxygenation
Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program
 PATIE NT I N FO R M ATI O N Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program A family s guide to understanding this specialized treatment for cardiac and pulmonary complications Saint Luke
PATIE NT I N FO R M ATI O N Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program A family s guide to understanding this specialized treatment for cardiac and pulmonary complications Saint Luke
Nitrofurantoin-Induced Lung Toxicity
 Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
UPDATE IN HOSPITAL MEDICINE
 UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
All I Need Is The Air That I Breathe: A Case Study of Immunotherapy and Severe Pneumonitis
 All I Need Is The Air That I Breathe: A Case Study of Immunotherapy and Severe Pneumonitis Presenter Disclosure Faculty/Speaker: Dr. Brett Finney BSc MD CCFP Relationships with financial sponsors: Grants/Research
All I Need Is The Air That I Breathe: A Case Study of Immunotherapy and Severe Pneumonitis Presenter Disclosure Faculty/Speaker: Dr. Brett Finney BSc MD CCFP Relationships with financial sponsors: Grants/Research
