Use of leadless pacemakers in Europe: results of the European Heart Rhythm Association survey
|
|
|
- Kristian Garrett
- 5 years ago
- Views:
Transcription
1 Europace (2018) 20, doi: /europace/eux381 EP WIRE Use of leadless pacemakers in Europe: results of the European Heart Rhythm Association survey Serge Boveda 1 *, Radoslaw Lenarczyk 2, Kristina H. Haugaa 3,4, Konstantinos Iliodromitis 5, Malcolm Finlay 6, Deirdre Lane 7,8, Frits W. Prinzen 9, and Nikolaos Dagres 10 1 Cardiology Cardiac Arrhythmias Management Department, Clinique Pasteur, 45 Avenue de Lombez, Toulouse Cedex, France; 2 Department of Cardiology, Congenital Heart Disease and Electrotherapy, Silesian Medical University, Silesian Centre for Heart Diseases, Curie-Sklodowska Street 9, Zabrze, Poland; 3 Center for Cardiological Innovation, Department of Cardiology and Institute for surgical Research, Oslo University Hospital, Rikshospitalet, Sognsvannsveien 20, 0372 Oslo, Norway; 4 Institute for clinical medicine, University of Oslo, Problemveien 7, 0315 Oslo, Norway; 5 Cardiovascular Center, Department of Cardiology, Electrophysiology section, Cardiovascular Center, OLV, Moorselbaan 164, 9300 Aalst, Belgium; 6 Barts Heart Centre and William Harvey Harvey Heart Centre, Queen Mary University of London, West Smithfield, London, EC1A 7BE, UK; 7 University of Birmingham Institute of Cardiovascular Sciences, Sandwell, B18 7QH, UK; 8 West Birmingham Hospitals NHS Trust, Dudley Road, Birmingham, West Midlands, B18 7QH, UK; 9 Department of Physiology, Cardiovascular Research Institute Maastricht (CARIM), Universiteitssingel 50, 6229 ER Maastricht PO Box 616, 6200 MD Maastricht, The Netherlands; and 10 Department of Electrophysiology, Heart Center Leipzig, Strümpellstr. 39, Leipzig, Germany Received 15 December 2017; editorial decision 17 December 2017; accepted 19 December 2017; online publish-ahead-of-print 17 January 2018 The purpose of this European Heart Rhythm Association (EHRA) survey is to provide an overview of the current use of leadless pacemakers (LLPM) across a broad range of European centres. An online questionnaire was sent to centres participating in the EHRA Electrophysiology Research Network. Questions dealt with standards of care and policies used for patient management, indications, and techniques of implantation of LLPM. In total, 52 centres participated in the survey. Most (86%) reported using LLPM, although 82% of these centres implanted <30 LLPM devices during the last 12 months. Non-availability (36%), lack of reimbursement (55%), and cost of the device (91%) were factors limiting the use of LLPM. The most commonly reported indications for LLPM were permanent atrial fibrillation (83%), a history of complicated conventional pacemaker (87%), or an anticipated difficult vascular access (91%). Implantation of LLPM is perceived as an easy-to-do and safe procedure by most implanters (64%), while difficult or risky in 28%, and comparable to conventional pacemakers by only a few (8%). Local vascular complications were the most frequently reported major problems (28%), but a significant number of respondents (36%) have never encountered any issue after LLPM implantation. Although cost and reimbursement issues strongly influence the use of LLPM, most respondents (72%) anticipate a significant increase in device utilization within next 2 years.... Keywords Leadless pacemakers Standards of care European Heart Rhythm Association survey EP Wire Introduction Cardiac pacing has been used for more than 50 years for the management of bradycardias. 1 3 Whereas the efficacy and overall safety of these devices are high, complications often related to the use of endovascular leads, including fracture, insulation breakdown, and infections may occur. 4,5 In the FOLLOWPACE study, the reported incidence of perforations, pericardial effusions, pocket complications, and pulse generator-related technical issues was 12.4% at 2 months and additional 9.2% at 5.9 years. 6 In addition, the extraction of the endovascular leads may be challenging and particularly risky. Furthermore, transvenous pacing may sometimes be very difficult or impossible because of venous thrombosis or occlusions. 4,5,7,8 For a long time, these considerations have motivated research into pacing systems free of endovascular leads. Currently, two devices are routinely used in many European centres: the Nanostim TM (St. Jude Medical, Inc., St. Paul, MN, USA) 9 and the Micra TM (Medtronic, Inc., Minneapolis, MN, USA) 10,11 which are both totally free-standing, intracardiac, single-chamber ventricular-only (VVIR) pacing devices, implanted in the right ventricular endocardium. All these leadless pacemakers (LLPM) are introduced via the femoral approach, using large (18 25 Fr) vascular sheaths, and they are screwed or anchored in the endocardium. The currently available pacemakers are only single-chamber devices, pacing in VVIR mode. 12 Several manufacturers are also working on the development of dual-chamber devices, with two modules implanted independently, which are able to *Corresponding author. Tel: þ ; fax: þ address: sboveda@clinique-pasteur.com Published on behalf of the European Society of Cardiology. All rights reserved. VC The Author(s) For Permissions, please journals.permissions@oup.com.
2 556 S. Boveda et al. communicate and interact with each other. These dual-chamber devices will include a right ventricular pacemaker, probably very similar to those already available, and a pacemaker implanted in the right atrium. Leadless pacing is just at the beginning, new systems are being developed, and the choice of devices will likely broaden in the near future. This technological breakthrough will most probably impact the future ofthepatientsandtheimplanters. 13 The aim of this European Heart Rhythm Association (EHRA) survey was to provide better insight into current LLPM utilization across a broad range of the European centres, and to anticipate what direction future trends may follow. Methods and results A questionnaire was sent via the internet to 151 centres that participate in the EHRA Electrophysiology (EP) Research Network. In this survey, 25 questions focused on standards and policies concerning patients management, indications, and techniques of implantation of LLPM in the participating EP centres. Participating centres Overall, 52 out of the 151 centres from 21 countries that were contacted (34% response rate), responded, with a wide geographical distribution of respondents: 15 centres from Poland, 8 centres from France and Spain, 6 centres from Germany, 3 centres from Sweden, 2 centres from Italy and from UK, and 1 centre each from Austria, Belgium, Georgia, Netherlands, Estonia, Lithuania, Czech Republic, and Switzerland. Among these 52 centres, 75% were university hospitals, 17% were non-university hospital, and 8% were private hospitals. Respondents were mostly high-volume centres: during the last 12 months 16% of them had implanted >500 dual or single chamber conventional pacemakers (CPM), 54% had implanted CPMs, 28% had implanted CPMs, 2% had implanted CPMs, and none reported <50 implantations. Use of leadless pacemakers At least once, LLPM has been implanted at 86% of the responding centres. Of all CPM implantations per centre, LLPMs represented <1 in 8 of the centres, 10 in 4% of the centres, 21 5 in 2% of the centres, and >5 in of the centres, while 14% of the responding centres reported to have never implanted LLPM. Regarding the number of patients implanted with LLPMs during the last 12 months, 4% of the responding centres implanted the device in patients, 4% in patients, 44% in patients, 39% reported <10 implantations, and 9% of did not implant LLPM (Figure 1). Implantation strategies and techniques In the majority of responding centres (79%), LLPM implantation procedures are performed during a short hospitalization (1 2 days), in 18% of centres peri-procedural hospitalization lasts 3 5 days, and never >5 days. Only in 3% of the centres are LLPM implantations being performed on an outpatient basis. In 72% of the centres, LLPM implantations are performed in an EP laboratory, and in 8% the procedure is done in a surgical theatre. In the remaining of the centres, a hybrid operating room is routinely used for these implantations % 39.1% 43.5% A B C D E F Figure 1 Proportion of respondents to the question: How many patients were equipped with a LLPM during the last 12 months in your centre? Each bar represents one possible answer. A, None; B, <10 patients; C, patients; D, patients; E, patients; and F, >100 patients. LLPM, leadless pacemaker. In the majority of centres, LLPM implantations are always performed by an electrophysiologist (9), by an interventional cardiologist or surgeon alone in 2% of the centres (each), and by both cardiologists and surgeons in the remaining 6% of the centres. Most of the responding centres routinely implant LLPM under local anaesthesia (56%), or deep sedation (36%), and only 8% of the centres perform the procedure under general anaesthesia. Among the two devices currently available in most countries, the Medtronic Micra was reportedly used in 87% of the respondents, the Abbott Nanostim in 5%, and both devices in 8%. Implantation of LLPM is perceived as an easy-to-do and safe procedure by 64% of the operators, an easy-to-do and risky procedure by 15%, a difficult and safe procedure by 5%, a difficult and risky procedure by 8% of the operators, and a procedure which is comparable with CPM implantation by further 8%. The mean implantation duration of LLPM from femoral vein puncture to sheath removal was reported as <30 min by 18% of the centres, min by 46%, 45 60minby23%,and>60minby13%. Repositioning of the device was required during the implant procedure in <1 of cases by 36% of the implanters, in 11 3 of cases by further 36%, in 31 5 of cases by 13%, in >5 of cases by 2% and was never required by 13% of the implanters. Finally, 72% of the responding centres declared having experience with LLPM retrieval. Reasons for not implanting leadless pacemakers As stated previously, 14% of the responding centres do not implant LLPM. The main reasons reported for not implanting these devices included the limited availability (36%), economic issues, such as lack of reimbursement (55% of not implanting centres), high cost of the device (91% of centres), issues associated with patient selection, such as the lack of dual-chamber or cardiac resynchronization therapy (CRT) pacing functions (27% of centres), or the absence of eligible patients (18% of centres). Lack of training was infrequently reported as the reason for not implanting LLPM (9%). Interestingly, physicians scepticism towards device efficacy, the complexity of the implantation procedure, the need of surgical back-up, or patients choice, were not reported as a potential obstacle for the use of this system (Figure 2).
3 Use of leadless pacemakers in Europe % % % 69.6% 54.5% 47.8% % 9.1% 27.3% 18.2% % 21.7% 32.6% A B C D E F G H I J A B C D E F G H I J Figure 2 Proportion of respondents to the question: If you don t implant leadless pacemakers in your centre, the reasons are (multiple answers)? A, Not available; B, not reimbursed; C, price too high; D, I don t believe in this system ; E, I ve not been trained to this procedure ; F, procedure too complex; G, need for a surgical back-up; H, lack of dual chamber or CRT pacing function; I, no patients who qualify; J patients rather opt for a conventional pacemaker. CRT, cardiac resynchronization therapy. Figure 4 Proportion of respondents to the question: Which features would make you more inclined to use leadless pacemaker, rather than conventional pacemaker implantation (multiple answers)? A, Young age; B, elderly; C, permanent atrial fibrillation; D, no pacing dependency; E, previous complicated endovascular conventional pacemaker; F, anticipated difficult vascular access; G, anticipated higher risk of infection; H, short anticipated survival; I, patient s preference; J, no particular feature % 23.9% 58.7% % 60.9% 19.6% A B C D E F G H I Figure 3 Proportion of respondents to the question: Which features in your opinion could represent an obstacle to leadless pacemaker use (multiple answers)? A, Overweight; B, underweight; C, age < 20 years old; D, age > 75 years old; E, pacing dependency; F, underlying sinus rhythm; G, tricuspid valvular prosthesis; H, patient s preference; I, no particular feature. Apart from device availability and reimbursement, the obstacles to LLPM use reported by most of the centres users and non-users were mainly linked to the presence of a tricuspid valvular prosthesis (61% of the respondents), age < 20 years (59%), underlying sinus rhythm (57%). More mitigating factors were being underweight (24%), patient s preference for CPM (), patient dependency (13%), followed by being overweight or age > 75 years (7% and 4%, respectively) (Figure 3). Features favouring leadless pacemaker over conventional pacemaker use Among responding centres routinely implanting LLPMs, the choice of LLPM system instead of CPM was mainly dictated by an anticipated difficult vascular access (91%), a history of complicated CPM (87%), a pacing indication in patients with permanent atrial fibrillation (83%), and an anticipated higher risk of infection (7). Less commonly reported factors favouring LLPM implantation were patient s advanced age (48% of the centres), or preference (33%), no pacing dependency (22%), and young age (17%) (Figure 4). 2.2% Current perception of indications for leadless pacemakers Among the responding centres, 77% undertake implantation of LLPMs only for very restricted indications, while in 1 discussion with the patient and shared decision-making (after both transvenous and leadless devices alternatives have been proposed) is the basis for device use. When no dual chamber pacing or CRT is needed, only few centres (5%) propose LLPMs as a first-choice therapy. Finally, 8% of the centres did not adopt any particular policy on the decision between transvenous CPM and LLPM devices. More interestingly, LLPM is also considered in patients with otherwise standard indications for dual-chamber pacemakers, when anticipated pacing burden is expected to be very low (74%), in patients with very advanced age (61%), in very active or non-cooperative patients, presenting with high risk of damage to the leads (39%), in patients with a normal left ventricular ejection fraction (28%), or in those with short anticipated survival, apart from age (26%). Only 11% of the respondents would never implant LLPM in a patient with indication for dual-chamber pacing (Figure 5). Outcomes after leadless pacemaker implantation Overall, 79% of survey participants reported very rare occurrence (<3%) of adverse events while managing patients with LLPM. More than one-third (36%) of the centres never encountered any issue after LLPM implantation. Among the major problems were local vascular complications (28%), high pacing thresholds at implant or during follow-up (23% and 8%, respectively), and pericardial effusion or tamponade requiring an intervention (). Less common problems included device dislodgment requiring recapturing and extraction (7%), and post-implant need for dual-chamber pacing or CRT requiring an up-grade (5%). Anticipated use of leadless pacemakers in the future The majority of respondents (63%) anticipated that the number of LLPM implantations will increase in their centre in the next 2 years,
4 558 S. Boveda et al % 60.9% 39.1% 28.3% 26.1% 10.9% % 28.3% 21.7% 8.7% 2.2% A B C D E F G A B C D E F Figure 5 Proportion of respondents to the question: In a patient with otherwise standard indications for dual chamber pacemaker implant, which one or more of the following would sway your opinion towards the use of a leadless pacemaker (multiple answers)? A, Low anticipated pacing burden; B, very advanced age; C, normal left ventricular ejection fraction; D, very active or not cooperating patient (high risk of damage to the leads); E, short anticipated survival, apart from age; F, I would never implant a leadless pacemaker in a patient with indications for dual-chamber pacing ; G, vascular or infectious issues. while 22% and 4% of centres estimate that the volume of LLPM patients in their centre will remain the same or will decrease, respectively. Many also expect that LLPM will be introduced in their centres (9%), while only 2% did not expect introduction of this technology within the next 2 years (Figure 6). Discussion This EP Wire provides an insight into contemporary European practice regarding LLPM implantation and management several years after its introduction in our countries. The main findings of this survey are: (i) the vast majority of the responding centres implant however, often sparingly LLPMs; (ii) the absence of reimbursement, limited availability, and device cost seem to be the main factors restricting the use of LLPM; (iii) the most commonly reported reasons for preferring LLPM over CPM are an anticipated difficult vascular access, previous complicated CPM, a pacing indication in a patient with permanent atrial fibrillation, or an anticipated high risk of infection; (iv) one-third of respondents have not encountered any problems following LLPM implantation; the most frequently reported major problems were local vascular complications; (v) most of the respondents to this surveyconsiderllpminpatientswithotherwisestandardindicationsfor dual-chamber pacemaker implant, and they anticipate that LLPM implantation rates will increase in their centre within the next 2 years. The LLPM system was developed to reduce the morbidity associated with endovascular leads (e.g. lead dislodgement or rupture, venous thrombosis, infection, etc.), while providing effective pacing function. 4,5 Although LLPM was introduced 3 5 years ago in most of the European countries, 9,14 its use is still not routine, even if it has already been implanted in most tertiary hospitals. In our survey, more than 8 of the respondents have already implanted LLPM. However, LLPM have been implanted in <10, or <30 patients during the last year in 48% and 91% of these high-volume centres, respectively. This emphasizes the very low proportion (<1 in 8 of the Figure 6 Proportion of respondents to the question: Do you think that the volume of patients equipped with leadless pacemakers in the next 2 years at your centre? A, Will increase by more than ; B, will increase by less than ; C, will decrease; D, will remain the same; E, leadless pacemakers will be introduced in your centre within the next 2 years; F, leadless pacemakers will not be used in your centre within the next 2 years. centres in this survey) of LLPMs among all pacemakers implanted in the majority of the European centres. There are many potential reasons for such discrepancy and slow penetration rate of LLPM across European countries. The LLPM is often considered as a niche for rare indications or difficult patients. On the other hand, LLPM is basically a substitute for a singlechamber CPM, providing same function by delivering endocardial VVIR pacing mode. 12,15 In this setting, one could theoretically expect that the LLPM would progressively replace the endovascular CPM in common indications, for example, in conduction disturbances. 15,16 Furthermore, most of respondents to this survey would consider LLPM in a patient with otherwise standard indications for dualchamber pacemaker under some circumstances 17 such as low expected pacing burden or advanced age. This highlights the gap existing between the wide theoretical LLPM indications and the far lower real implantation rate across European centres. Implantation of LLPM involves a completely new technique, 12,18 which requires specific training, posing a potential barrier to many operators who may have years of experience in implantation of CPMs In addition, the femoral sheath used for introducing LLPM is particularly large 12,18 (18 25 Fr), which engenders reluctance on the part of many implanters. Finally, this procedure needs to fit into the routine, everyday hospital regime, and at the moment most centres still appear to be in a learning phase. Increased organizational and logistic efforts are called for, in addition to, nursing training, requirements for a hybrid or a surgical theatre, anaesthetists, and surgical backup. 12 In this context, LLPM implantations lead to more complexity, which may ultimately discourage some teams. Last but not least, cost issues, largely reported by the responding centres in this survey, will indisputably negatively impact the availability of LLPM and its uptake across Europe. While one-third of the centres using LLPM in our survey reported no complications during or after implantation, local vascular complications were the most frequently reported adverse event. Importantly, pacemaker syndrome and/or infection were not reported as a major problem encountered with LLPM. These findings are consistent with the data from the literature, showing that LLPM short-term outcomes are mostly related to the implant procedure itself: cardiac perforation, device dislocation, and femoral vascular access site complications. It is
5 Use of leadless pacemakers in Europe 559 also clear, that the complication rate is significantly influenced by implanter experience with this new procedure. 10,15 It is surprising that the most reported obstacle to implant was considered to be the presence of a tricuspid valvular prosthesis. Paradoxically, some data suggest, that crossing a prosthetic tricuspid valve for LLPM placement is possible and can be facilitated by the valve visualization. 19 In addition, this option could offer the advantage of preventing tricuspid insufficiency and bioprosthesis chronic damages due to the implantation of a permanent endovascular ventricular pacing lead. 20 The risk of future infection is also expected to be lower in this setting. Other limitations for LLPM use are related to the risk of battery replacement after depletion in young patients and the need for atrial pacing in case of sinus node disease. 12,18 Leadless pacemaker is a major technological step forward in the world of cardiac pacing, and current first generation single-chamber devices represent the initial step of this new venture. Many further important enhancements are expected, such as multi chamber systems, and enhancements allowing for easier retrieval, for battery replacement for example. 12,15,18 It seems highly probable that LLPM implantations will significantly increase in the European countries, as anticipated by the participants of this survey. Limitations This survey has some limitations. First, because it is fully based on a voluntary participation, it is non-exhaustive. Second, because questions had a limited number of options to be chosen, some situations may have not been completely covered. Third, this questionnaire was launched before Abbott paused the distribution of the Nanostim LLPM. Finally, because purely declarative, it may not be entirely representative of the whole activity or decisions of the responding centres. However, the purpose of this survey was reached by providing an overview of the current use of LLPMs across a broad range of the European centres. Conclusion This survey provides an insight into LLPM implantation and management strategy in the European centres. The use of this device is influenced by cost issues and lack of reimbursement which currently limit its uptake in clinical practice. However, most respondents anticipate that LLPM implantation rates will increase significantly in the next 2 years. Acknowledgements This document is supported by Medtronic in the form of an educational grant. The content has not been influenced in any way by its sponsor. The production of this EP Wire document is under the responsibility of the Scientific Initiative Committee of the European Heart Rhythm Association: Nikolaos Dagres (Chair), Jan Steffel (Co- Chair), Serge Boveda, Georghe Andrei Dan, Malcolm Finlay, Stefano Fumagalli, Bulent Gorenek, Kristina Haugaa, Konstantinos E. Iliodromitis, Deirdre Lane, Radoslaw Lenarczyk, Francisco Marin, Frits Prinzen, Daniel Scherr, Katja Zeppenfeld. Document reviewer for EP- Europace: Irina Savelieva (St George s University of London, London, UK). The authors acknowledge the EHRA Research Network centres participating in this EP Wire. A list of the Research Network can be found on the EHRA website. Conflict of interest: S.B. reports consultant fees from Medtronic, Boston Scientific, and Livanova outside of the submitted work. N.D. reports grants from Biotronik, St. Jude Medical, and Boston Scientific outside of the submitted work and personal fees from Boston Scientific outside of the submitted work. All other authors declared no conflict of interest. References 1. Brignole M, Auricchio A, Baron-Esquivias G, Bordachar P, Boriani G, Breithardt OA et al ESC guidelines on cardiac pacing and cardiac resynchronization therapy: the task force on cardiac pacing and resynchronization therapy of the European Society of Cardiology (ESC). Developed in collaboration with the European Heart Rhythm Association (EHRA). Europace 2013;15: Epstein AE, DiMarco JP, Ellenbogen KA, Estes NAM, Freedman RA, Gettes LS et al ACCF/AHA/HRS focused update incorporated into the ACCF/AHA/ HRS 2008 guidelines for device-based therapy of cardiac rhythm abnormalities: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol 2013;61:e Raatikainen MJP, Arnar DO, Merkely B, Nielsen JC, Hindricks G, Heidbuchel H et al. A decade of information on the use of cardiac implantable electronic devices and interventional electrophysiological procedures in the European Society of Cardiology Countries: 2017 Report from the European Heart Rhythm Association. Europace 2017;19:ii1 ii Hauser RG, Hayes DL, Kallinen LM, Cannom DS, Epstein AE, Almquist AK et al. Clinical experience with pacemaker pulse generators and transvenous leads: an 8-year prospective multicenter study. Heart Rhythm 2007;4: Kirkfeldt RE, Johansen JB, Nohr EA, Jørgensen OD, Nielsen JC. Complications after cardiac implantable electronic device implantations: an analysis of a complete, nationwide cohort in Denmark. Eur Heart J 2014;35: Udo EO, Zuithoff NPA, Hemel NM. V, Cock CC. D, Hendriks T, Doevendans PA et al. Incidence and predictors of short- and long-term complications in pacemaker therapy: the FOLLOWPACE study. Heart Rhythm 2012;9: Haghjoo M, Nikoo MH, Fazelifar AF, Alizadeh A, Emkanjoo Z, Sadr-Ameli MA. Predictors of venous obstruction following pacemaker or implantable cardioverterdefibrillator implantation: a contrast venographic study on 100 patients admitted for generator change, lead revision, or device upgrade. Europace 2007;9: Grazia Bongiorni M, Dagres N, Estner H, Pison L, Todd D, Blomstrom-Lundqvist C. Scientific Initiative Committee, European Heart Rhythm Association. Management of malfunctioning and recalled pacemaker and defibrillator leads: results of the European Heart Rhythm Association survey. Europace 2014;16: Knops RE, Tjong FVY, Neuzil P, Sperzel J, Miller MA, Petru J et al. Chronic performance of a leadless cardiac pacemaker: 1-year follow-up of the LEADLESS trial. J Am Coll Cardiol 2015;65: Roberts PR, Clementy N, Al Samadi F, Garweg C, Martinez-Sande JL, Iacopino S et al. A leadless pacemaker in the real-world setting: the Micra transcatheter pacing system Post-Approval Registry. Heart Rhythm 2017;14: Ritter P, Duray GZ, Zhang S, Narasimhan C, Soejima K, Omar R, Micra Transcatheter Pacing Study Group et al. The rationale and design of the Micra Transcatheter Pacing Study: safety and efficacy of a novel miniaturized pacemaker. Europace 2015;17: Sperzel J, Burri H, Gras D, Tjong FVY, Knops RE, Hindricks G et al. State of the art of leadless pacing. Europace 2015;17: Grol R, Grimshaw J. From best evidence to best practice: effective implementation of change in patients care. Lancet Lond Engl 2003;362: Reddy VY, Exner DV, Cantillon DJ, Doshi R, Bunch TJ, Tomassoni GF et al. Percutaneous implantation of an entirely intracardiac leadless pacemaker. N Engl J Med 2015;373: Tjong FVY, Reddy VY. Permanent leadless cardiac pacemaker therapy: a comprehensive review. Circulation 2017;135: Ritter P, Duray GZ, Steinwender C, Soejima K, Omar R, Mont L et al. Early performance of a miniaturized leadless cardiac pacemaker: the Micra Transcatheter Pacing Study. Eur Heart J 2015;36: Healey JS, Toff WD, Lamas GA, Andersen HR, Thorpe KE, Ellenbogen KA et al. Cardiovascular outcomes with atrial-based pacing compared with ventricular pacing: meta-analysis of randomized trials, using individual patient data. Circulation 2006;114: Reynolds DW, Ritter P. A leadless intracardiac transcatheter pacing system. N Engl J Med 2016;374: Boveda S, Durand P, Combes S, Mariottini C-J. Leadless pacemaker surrounded by three valvular prostheses. Heart Rhythm 2017;14: Al-Mohaissen MA, Chan KL. Prevalence and mechanism of tricuspid regurgitation following implantation of endocardial leads for pacemaker or cardioverter-defibrillator. J Am Soc Echocardiogr 2012;25:
REVIEW ARTICLE. Leadless Cardiac Pacemaker Therapy. An Overview for the Hospitalist Richard Weachter 1
 Leadless Cardiac Pacemaker Therapy. An Overview for the Hospitalist Richard Weachter 1 1 Division of Cardiovascular Medicine, Department of Medicine, University of Missouri, Columbia, MO Correspondence:
Leadless Cardiac Pacemaker Therapy. An Overview for the Hospitalist Richard Weachter 1 1 Division of Cardiovascular Medicine, Department of Medicine, University of Missouri, Columbia, MO Correspondence:
MEET MICRA. Micra TM ACTUAL SIZE. Transcatheter Pacing System
 MEET MICRA ACTUAL SIZE Micra TM Transcatheter Pacing System MEET MICRA The world s smallest pacemaker 1 MINIATURIZED. 93% smaller than modern-day pacemakers 7 Completely self contained within the heart,
MEET MICRA ACTUAL SIZE Micra TM Transcatheter Pacing System MEET MICRA The world s smallest pacemaker 1 MINIATURIZED. 93% smaller than modern-day pacemakers 7 Completely self contained within the heart,
EHRA survey Ablation for atrial fibrillation
 Europace (2018) 20, 386 391 doi:10.1093/europace/eux365 EHRA survey Ablation for atrial fibrillation Patients knowledge and attitudes regarding living with implantable electronic devices: results of a
Europace (2018) 20, 386 391 doi:10.1093/europace/eux365 EHRA survey Ablation for atrial fibrillation Patients knowledge and attitudes regarding living with implantable electronic devices: results of a
MEET MICRA. Micra TM ACTUAL SIZE. Transcatheter Pacing System
 MEET MICRA ACTUAL SIZE Micra TM Transcatheter Pacing System MEET MICRA The world s smallest pacemaker 1 MINIATURIZED. 93% smaller than modern-day pacemakers 6 Completely self contained within the heart,
MEET MICRA ACTUAL SIZE Micra TM Transcatheter Pacing System MEET MICRA The world s smallest pacemaker 1 MINIATURIZED. 93% smaller than modern-day pacemakers 6 Completely self contained within the heart,
Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2018; 162:XX.
 Extraction of a dislocated leadless pacemaker in a patient with infective endocarditis and repeated endocardial and epicardial pacing system infections Milos Taborsky a, Tomas Skala a, Martin Kocher b,
Extraction of a dislocated leadless pacemaker in a patient with infective endocarditis and repeated endocardial and epicardial pacing system infections Milos Taborsky a, Tomas Skala a, Martin Kocher b,
Pacing Without Wires: Leadless Cardiac Pacing
 REVIEWS AND CONTEMPORARY UPDATES Ochsner Journal 16:238 242, 2016 Ó Academic Division of Ochsner Clinic Foundation Pacing Without Wires: Leadless Cardiac Pacing Michael L. Bernard, MD, PhD Department of
REVIEWS AND CONTEMPORARY UPDATES Ochsner Journal 16:238 242, 2016 Ó Academic Division of Ochsner Clinic Foundation Pacing Without Wires: Leadless Cardiac Pacing Michael L. Bernard, MD, PhD Department of
New generations pacemakers and ICDs: an update
 Advances in Cardiac Arrhythmias and Great Innovations in Cardiology XXVII Giornate Cardiologiche Torinesi New generations pacemakers and ICDs: an update Prof. Fiorenzo Gaita, MD Division of Cardiology
Advances in Cardiac Arrhythmias and Great Innovations in Cardiology XXVII Giornate Cardiologiche Torinesi New generations pacemakers and ICDs: an update Prof. Fiorenzo Gaita, MD Division of Cardiology
Leadless pacemakers a panacea for bradyarrhythmias?
 Leadless pacemakers a panacea for bradyarrhythmias? Peysh A Patel Take Home Messages Why may leadless systems be required? Where the cessation of vital action is very complete, and continues long, we ought
Leadless pacemakers a panacea for bradyarrhythmias? Peysh A Patel Take Home Messages Why may leadless systems be required? Where the cessation of vital action is very complete, and continues long, we ought
King s Research Portal
 King s Research Portal DOI: 10.1016/j.tcm.2016.03.003 Document Version Peer reviewed version Link to publication record in King's Research Portal Citation for published version (APA): Rinaldi, C. A. (2016).
King s Research Portal DOI: 10.1016/j.tcm.2016.03.003 Document Version Peer reviewed version Link to publication record in King's Research Portal Citation for published version (APA): Rinaldi, C. A. (2016).
EHRA Position Documents on new technology or standards of care
 EHRA Position Documents on new technology or standards of care Prof. Laurent Fauchier Cardiologie, Centre Hospitalier Universitaire Trousseau Tours, France Disclosures Laurent Fauchier: Lecture fees: Bayer,
EHRA Position Documents on new technology or standards of care Prof. Laurent Fauchier Cardiologie, Centre Hospitalier Universitaire Trousseau Tours, France Disclosures Laurent Fauchier: Lecture fees: Bayer,
Leadless Pacing. Osama Diab Assistant Prof. of Cardiology Ain Shams University Egypt
 Leadless Pacing Osama Diab Assistant Prof. of Cardiology Ain Shams University Egypt The weakest link in Pacemaker system the lead. The more the leads the more the complications Dislodgement Fracture Insulation
Leadless Pacing Osama Diab Assistant Prof. of Cardiology Ain Shams University Egypt The weakest link in Pacemaker system the lead. The more the leads the more the complications Dislodgement Fracture Insulation
Percutaneous Implantation of an Entirely Intracardiac Leadless Pacemaker
 Original Article Percutaneous Implantation of an Entirely Intracardiac Leadless Pacemaker Vivek Y. Reddy, M.D., Derek V. Exner, M.D., M.P.H., Daniel J. Cantillon, M.D., Rahul Doshi, M.D., T. Jared Bunch,
Original Article Percutaneous Implantation of an Entirely Intracardiac Leadless Pacemaker Vivek Y. Reddy, M.D., Derek V. Exner, M.D., M.P.H., Daniel J. Cantillon, M.D., Rahul Doshi, M.D., T. Jared Bunch,
FREQUENTLY ASKED QUESTIONS
 FREQUENTLY ASKED QUESTIONS Micra TPS U.S. Private Payer Prior Authorization Micra Transcatheter Pacing System Most commercial payers in the United States do not have a positive coverage policy for Micra
FREQUENTLY ASKED QUESTIONS Micra TPS U.S. Private Payer Prior Authorization Micra Transcatheter Pacing System Most commercial payers in the United States do not have a positive coverage policy for Micra
Recent Advances in Pacing and Defibrillation Harish Doppalapudi, MD
 Recent Advances in Pacing and Defibrillation Harish Doppalapudi, MD Harish Doppalapudi, MD Assistant Professor of Medicine Director, Clinical Cardiac Electrophysiology Training Program University of Alabama
Recent Advances in Pacing and Defibrillation Harish Doppalapudi, MD Harish Doppalapudi, MD Assistant Professor of Medicine Director, Clinical Cardiac Electrophysiology Training Program University of Alabama
Performance of a Miniaturized Transcatheter Pacing System: First-in-human experience
 Performance of a Miniaturized Transcatheter Pacing System: First-in-human experience Philippe Ritter, MD Gabor Z Duray, MD, PhD, FESC; Clemens Steinwender, MD, FESC; Kyoko Soejima, MD; Razali Omar, MD;
Performance of a Miniaturized Transcatheter Pacing System: First-in-human experience Philippe Ritter, MD Gabor Z Duray, MD, PhD, FESC; Clemens Steinwender, MD, FESC; Kyoko Soejima, MD; Razali Omar, MD;
Management of ventricular tachycardia in the ablation era: results of the European Heart Rhythm Association Survey
 Europace (2018) 20, 209 213 doi:10.1093/europace/eux332 EP WIRE in the ablation era: results of the European Heart Rhythm Association Survey Roland Richard Tilz 1 *, Radoslaw Lenarczyk 2, Daniel Scherr
Europace (2018) 20, 209 213 doi:10.1093/europace/eux332 EP WIRE in the ablation era: results of the European Heart Rhythm Association Survey Roland Richard Tilz 1 *, Radoslaw Lenarczyk 2, Daniel Scherr
MICRA TRANSCATHETER PACING SYSTEM (TPS) REIMBURSEMENT OVERVIEW
 MICRA TRANSCATHETER PACING SYSTEM (TPS) REIMBURSEMENT OVERVIEW MARCH 20, 2017 DISCLAIMER This presentation is intended only for educational use. Any duplication is prohibited without written consent of
MICRA TRANSCATHETER PACING SYSTEM (TPS) REIMBURSEMENT OVERVIEW MARCH 20, 2017 DISCLAIMER This presentation is intended only for educational use. Any duplication is prohibited without written consent of
Introduction EP WIRE. ... Keywords
 Europace (217), 1 6 doi:1.3/europace/eux254 EP WIRE Left atrial appendage occluder implantation in Europe: indications and anticoagulation post-implantation. Results of the European Heart Rhythm Association
Europace (217), 1 6 doi:1.3/europace/eux254 EP WIRE Left atrial appendage occluder implantation in Europe: indications and anticoagulation post-implantation. Results of the European Heart Rhythm Association
Long-term Performance of a Transcatheter Pacing System: 12 month results from the Micra Transcatheter Pacing Study
 Accepted Manuscript Long-term Performance of a Transcatheter Pacing System: 12 month results from the Micra Transcatheter Pacing Study Gabor Z. Duray, MD, PhD, Philippe Ritter, MD, Mikhael El-Chami, MD,
Accepted Manuscript Long-term Performance of a Transcatheter Pacing System: 12 month results from the Micra Transcatheter Pacing Study Gabor Z. Duray, MD, PhD, Philippe Ritter, MD, Mikhael El-Chami, MD,
Supplemental Material
 Supplemental Material 1 Table S1. Codes for Patient Selection Cohort Codes Primary PM CPT: 33206 or 33207 or 33208 (without 33225) ICD-9 proc: 37.81, 37.82, 37.83 Primary ICD Replacement PM Replacement
Supplemental Material 1 Table S1. Codes for Patient Selection Cohort Codes Primary PM CPT: 33206 or 33207 or 33208 (without 33225) ICD-9 proc: 37.81, 37.82, 37.83 Primary ICD Replacement PM Replacement
Essentials of Pacemakers and ICD s. Rajesh Banker, MD, MPH
 Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
Essentials of Pacemakers and ICD s Rajesh Banker, MD, MPH Pacemakers have 4 basic functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing
The learning curve associated with the implantation of the Nanostim leadless pacemaker
 Journal of Interventional Cardiac Electrophysiology (2018) 53:239 247 https://doi.org/10.1007/s10840-018-0438-8 MULTIMEDIA REPORT The learning curve associated with the implantation of the Nanostim leadless
Journal of Interventional Cardiac Electrophysiology (2018) 53:239 247 https://doi.org/10.1007/s10840-018-0438-8 MULTIMEDIA REPORT The learning curve associated with the implantation of the Nanostim leadless
Update on Device Innovation (S-ICD, Wearable, Leadless)
 Update on Device Innovation (S-ICD, Wearable, Leadless) C. W. Israel Dept. of Medicine - Cardiology Evangelical Hospital Bielefeld J. W. Goethe University Frankfurt Carsten.Israel@em.uni-frankfurt.de Conflicts
Update on Device Innovation (S-ICD, Wearable, Leadless) C. W. Israel Dept. of Medicine - Cardiology Evangelical Hospital Bielefeld J. W. Goethe University Frankfurt Carsten.Israel@em.uni-frankfurt.de Conflicts
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of leadless cardiac pacemaker implantation for bradyarrhythmias Bradyarrhythmias
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of leadless cardiac pacemaker implantation for bradyarrhythmias Bradyarrhythmias
Cardiac Rhythm Management Coder 2017
 Cardiac Rhythm Management Coder 2017 An easy-to-use tool for coding and reimbursement compliance Prepared and Published By: MedLearn Publishing, A Division of Panacea Healthcare Solutions, Inc. 287 East
Cardiac Rhythm Management Coder 2017 An easy-to-use tool for coding and reimbursement compliance Prepared and Published By: MedLearn Publishing, A Division of Panacea Healthcare Solutions, Inc. 287 East
Performance of Leadless Pacemaker in Japanese Patients vs. Rest of the World. Results From a Global Clinical Trial
 Circ J 2017; 81: 1589 1595 doi: 10.1253/circj.CJ-17-0259 ORIGINAL ARTICLE Arrhythmia/Electrophysiology Performance of Leadless Pacemaker in ese Patients vs. Rest of the World Results From a Global Clinical
Circ J 2017; 81: 1589 1595 doi: 10.1253/circj.CJ-17-0259 ORIGINAL ARTICLE Arrhythmia/Electrophysiology Performance of Leadless Pacemaker in ese Patients vs. Rest of the World Results From a Global Clinical
Transvenous Pacemaker Procedures
 Cardiology: Pacemaker and Defibrillator Coding Presented By: Moderate Sedation 2017 99151 : under age 5, initial 15 minutes by MD performing intervention 99152: age 5 or older, initial 15 minutes by MD
Cardiology: Pacemaker and Defibrillator Coding Presented By: Moderate Sedation 2017 99151 : under age 5, initial 15 minutes by MD performing intervention 99152: age 5 or older, initial 15 minutes by MD
INNOVATIONS IN DEVICE THERAPY:
 INNOVATIONS IN DEVICE THERAPY: Subcutaneous ICDs, Leadless Pacemakers, CRT Indications David J Wilber MD Loyola University Medical Center Disclosures: ACC Foundation: Consultant; Biosense / Webster: Consultant,
INNOVATIONS IN DEVICE THERAPY: Subcutaneous ICDs, Leadless Pacemakers, CRT Indications David J Wilber MD Loyola University Medical Center Disclosures: ACC Foundation: Consultant; Biosense / Webster: Consultant,
Introduction. CLINICAL RESEARCH Pacing and resynchronization therapy
 Europace (2015) 17, 787 793 doi:10.1093/europace/euv003 CLINICAL RESEARCH Pacing and resynchronization therapy Association between hospital procedure volume and early complications after pacemaker implantation:
Europace (2015) 17, 787 793 doi:10.1093/europace/euv003 CLINICAL RESEARCH Pacing and resynchronization therapy Association between hospital procedure volume and early complications after pacemaker implantation:
Introduction EHRA SURVEY
 Europace (2018) 0, 1 5 doi:10.1093/europace/euy112 EHRA SURVEY Management of patients with ventricular arrhythmias and prevention of sudden cardiac death translating guidelines into practice: results of
Europace (2018) 0, 1 5 doi:10.1093/europace/euy112 EHRA SURVEY Management of patients with ventricular arrhythmias and prevention of sudden cardiac death translating guidelines into practice: results of
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of a leadless cardiac pacemaker implantation for bradyarrhythmias Bradyarrhythmias
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of a leadless cardiac pacemaker implantation for bradyarrhythmias Bradyarrhythmias
The development of implantable. Original Research
 Original Research Hellenic J Cardiol 2016; 57: 33-38 Complications Related to Cardiac Rhythm Management Device Therapy and Their Financial Implication: A Prospective Single-Center Two- Year Survey John
Original Research Hellenic J Cardiol 2016; 57: 33-38 Complications Related to Cardiac Rhythm Management Device Therapy and Their Financial Implication: A Prospective Single-Center Two- Year Survey John
NOVEL DEVICE TECHNOLOGIES
 NOVEL DEVICE TECHNOLOGIES Leadless Pacemakers and Subcutaneous ICDs Do the Benefits Outweigh MRI Incompatibility? Disclosures None Background PPMs and ICDs are very effective therapy for treating bradyarrhythmias
NOVEL DEVICE TECHNOLOGIES Leadless Pacemakers and Subcutaneous ICDs Do the Benefits Outweigh MRI Incompatibility? Disclosures None Background PPMs and ICDs are very effective therapy for treating bradyarrhythmias
OHTAC Recommendation: Internet- Based Device-Assisted Remote Monitoring of Cardiovascular Implantable Electronic Devices
 OHTAC Recommendation: Internet- Based Device-Assisted Remote Monitoring of Cardiovascular Implantable Electronic Devices Ontario Health Technology Advisory Committee January 2012 Issue Background The Ontario
OHTAC Recommendation: Internet- Based Device-Assisted Remote Monitoring of Cardiovascular Implantable Electronic Devices Ontario Health Technology Advisory Committee January 2012 Issue Background The Ontario
EBR Systems, Inc. 686 W. Maude Ave., Suite 102 Sunnyvale, CA USA
 Over 200,000 patients worldwide are estimated to receive a CRT device each year. However, limitations prevent some patients from benefiting. CHALLENGING PROCEDURE 5% implanted patients fail to have coronary
Over 200,000 patients worldwide are estimated to receive a CRT device each year. However, limitations prevent some patients from benefiting. CHALLENGING PROCEDURE 5% implanted patients fail to have coronary
Leadless Pacemakers: practice and promise in congenital heart disease
 Clarke et al. Journal of Congenital Cardiology (2017) 1:4 DOI 10.1186/s40949-017-0007-5 Journal of Congenital Cardiology REVIEW Leadless Pacemakers: practice and promise in congenital heart disease T.S.O.
Clarke et al. Journal of Congenital Cardiology (2017) 1:4 DOI 10.1186/s40949-017-0007-5 Journal of Congenital Cardiology REVIEW Leadless Pacemakers: practice and promise in congenital heart disease T.S.O.
The EHRA White Book 2009 The Current Status of Cardiac Electrophysiology in ESC Member Countries J. Brugada, P. Vardas, C. Wolpert
 Albania. Algeria. Armenia. Austria. Belarus. Belgium. Bosnia & Herzegovina. Bulgaria. Croatia. Cyprus. Czech Republic Denmark. Egypt. Estonia. Finland. Former Yugoslav Republic of Macedonia. France. Georgia.
Albania. Algeria. Armenia. Austria. Belarus. Belgium. Bosnia & Herzegovina. Bulgaria. Croatia. Cyprus. Czech Republic Denmark. Egypt. Estonia. Finland. Former Yugoslav Republic of Macedonia. France. Georgia.
Cardiac implantable electronic devices (CIEDs) in children include pacemakers and implantable cardioverter defibrillators (ICDs).
 Management of Children with Cardiac Devices Guideline originally developed by Leann Miles, APRN; Lindsey Pumphrey, RN; Srikant Das, MD, and the ANGELS Team. Last reviewed by Lindsey Pumphrey, RN, Srikant
Management of Children with Cardiac Devices Guideline originally developed by Leann Miles, APRN; Lindsey Pumphrey, RN; Srikant Das, MD, and the ANGELS Team. Last reviewed by Lindsey Pumphrey, RN, Srikant
Leadless pacemakers and subcutaneous ICD s: will we use them for most of our patients? K.-H. Kuck Asklepios Klinik St. Georg Hamburg, Germany
 Leadless pacemakers and subcutaneous ICD s: will we use them for most of our patients? K.-H. Kuck Asklepios Klinik St. Georg Hamburg, Germany Disclosure Statement Research Grants Consultant / Advisory
Leadless pacemakers and subcutaneous ICD s: will we use them for most of our patients? K.-H. Kuck Asklepios Klinik St. Georg Hamburg, Germany Disclosure Statement Research Grants Consultant / Advisory
Comparator cohort In order to compare the Micra pacing thresholds with transvenous thresholds, we analyzed transvenous pacing thresholds
 Long-term outcomes in leadless Micra transcatheter pacemakers with elevated thresholds at implantation: Results from the Micra Transcatheter Pacing System Global Clinical Trial Jonathan P. Piccini, MD,
Long-term outcomes in leadless Micra transcatheter pacemakers with elevated thresholds at implantation: Results from the Micra Transcatheter Pacing System Global Clinical Trial Jonathan P. Piccini, MD,
Cardiac Rhythm Management Coder 2018
 Cardiac Rhythm Management Coder 2018 An easy-to-use tool for coding and reimbursement compliance Prepared and Published By: MedLearn Publishing, A Division of MedLearn Media, Inc. 445 Minnesota Street,
Cardiac Rhythm Management Coder 2018 An easy-to-use tool for coding and reimbursement compliance Prepared and Published By: MedLearn Publishing, A Division of MedLearn Media, Inc. 445 Minnesota Street,
Pediatric Pacemaker Implantation Endocardial or Epicardial
 Pediatric Pacemaker Implantation Endocardial or Epicardial HAITHAM BADRAN, MD, FEHRA CONSULTANT OF INTERVENTIONAL CARDIOLOGY CONSULTANT OF CARDIAC PACING AND ELECTROPHYSIOLOGY LECTURER OF CARDIOLOGY AIN
Pediatric Pacemaker Implantation Endocardial or Epicardial HAITHAM BADRAN, MD, FEHRA CONSULTANT OF INTERVENTIONAL CARDIOLOGY CONSULTANT OF CARDIAC PACING AND ELECTROPHYSIOLOGY LECTURER OF CARDIOLOGY AIN
How to treat Cardiac Resynchronization Therapy complications? C. Leclercq Departement of Cardiology Centre Cardio-Pneumologique Rennes, France
 How to treat Cardiac Resynchronization Therapy complications? C. Leclercq Departement of Cardiology Centre Cardio-Pneumologique Rennes, France Presenter Disclosure Information Christophe Leclercq, MD,
How to treat Cardiac Resynchronization Therapy complications? C. Leclercq Departement of Cardiology Centre Cardio-Pneumologique Rennes, France Presenter Disclosure Information Christophe Leclercq, MD,
The Current Status of Cardiac Electrophysiology in ESC Member Countries J. Brugada, P. Vardas, C. Wolpert
 Albania. Algeria. Armenia. Austria. Belarus. Belgium. Bosnia & Herzegovina. Bulgaria. Croatia. Cyprus. Czech Republic Denmark. Egypt. Estonia. Finland. Former Yugoslav Republic of Macedonia. France. Georgia.
Albania. Algeria. Armenia. Austria. Belarus. Belgium. Bosnia & Herzegovina. Bulgaria. Croatia. Cyprus. Czech Republic Denmark. Egypt. Estonia. Finland. Former Yugoslav Republic of Macedonia. France. Georgia.
Left Atrial Appendage Closure: The Good, The Bad and The Ugly
 Left Atrial Appendage Closure: The Good, The Bad and The Ugly John D. Hummel, MD Director of Electrophysiology Research Ross Heart Hospital, The Ohio State University Columbus, Ohio USA Disclosures Modest
Left Atrial Appendage Closure: The Good, The Bad and The Ugly John D. Hummel, MD Director of Electrophysiology Research Ross Heart Hospital, The Ohio State University Columbus, Ohio USA Disclosures Modest
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Table S1. Patient Selection Codes, CIED Generator Procedures Code Type Code Description ICD9 Proc 00.51 Implantation of cardiac resynchronization defibrillator, total system [CRT-D]
SUPPLEMENTAL MATERIAL Table S1. Patient Selection Codes, CIED Generator Procedures Code Type Code Description ICD9 Proc 00.51 Implantation of cardiac resynchronization defibrillator, total system [CRT-D]
Implantable Defibrillators Market by Product Type [Transvenous Implantable Cardioverter-Defibrillator (T-ICDs), Subcutaneous Implantable Cardioverter
 Implantable Defibrillators Market by Product Type [Transvenous Implantable Cardioverter-Defibrillator (T-ICDs), Subcutaneous Implantable Cardioverter Defibrillators (S-ICDS), and Cardiac Resynchronization
Implantable Defibrillators Market by Product Type [Transvenous Implantable Cardioverter-Defibrillator (T-ICDs), Subcutaneous Implantable Cardioverter Defibrillators (S-ICDS), and Cardiac Resynchronization
Quality Standards for the Implantation of Cardiac Rhythm Management Devices. Pan- London Arrhythmia Project Group. Version 3 (18 th July 2011)
 Quality Standards for the Implantation of Cardiac Rhythm Management Devices Pan- London Arrhythmia Project Group Version 3 (18 th July 2011) 1 Standards for Implantation of Permanent Pacemakers (including
Quality Standards for the Implantation of Cardiac Rhythm Management Devices Pan- London Arrhythmia Project Group Version 3 (18 th July 2011) 1 Standards for Implantation of Permanent Pacemakers (including
Interventional solutions for atrial fibrillation in patients with heart failure
 Interventional solutions for atrial fibrillation in patients with heart failure Advances in Cardiovascular Arrhythmias Great Innovations in Cardiology Matteo Anselmino, MD PhD Division of Cardiology Department
Interventional solutions for atrial fibrillation in patients with heart failure Advances in Cardiovascular Arrhythmias Great Innovations in Cardiology Matteo Anselmino, MD PhD Division of Cardiology Department
UnitedHealthcare Medicare Advantage Cardiology Prior Authorization Program
 Electrophysiology Implant Classification Table The table below contains the codes that apply to our UnitedHealthcare Medicare Advantage cardiology prior Description Includes Generator Placement Includes
Electrophysiology Implant Classification Table The table below contains the codes that apply to our UnitedHealthcare Medicare Advantage cardiology prior Description Includes Generator Placement Includes
Q1 In which country and city is your centre based?
 Q1 In which country and city is your centre based? Answered: 41 Skipped: 0 # Date 1 Poland, Warsaw 7/2/2017 11:55 PM 2 Poland, Polanica Zdrój 7/2/2017 10:08 PM 3 Poland 6/30/2017 11:34 PM 4 italy 6/30/2017
Q1 In which country and city is your centre based? Answered: 41 Skipped: 0 # Date 1 Poland, Warsaw 7/2/2017 11:55 PM 2 Poland, Polanica Zdrój 7/2/2017 10:08 PM 3 Poland 6/30/2017 11:34 PM 4 italy 6/30/2017
Outcomes of Defibrillator Lead Implants Performed by High Volume Operators vs. Low Volume Operators:
 Outcomes of Defibrillator Lead Implants Performed by High Volume Operators vs. Low Volume Operators: Results from the Pacemaker and Implantable Defibrillator Leads Survival Study ( PAIDLESS ) Partially
Outcomes of Defibrillator Lead Implants Performed by High Volume Operators vs. Low Volume Operators: Results from the Pacemaker and Implantable Defibrillator Leads Survival Study ( PAIDLESS ) Partially
How to Implant a Leadless Pacemaker With a Tine-Based Fixation
 Techniques, Technology, and Innovations Section Editor: Samuel J. Asirvatham, M.D. How to Implant a Leadless Pacemaker With a Tine-Based Fixation MIKHAEL F. EL-CHAMI, M.D., PAUL R. ROBERTS, M.D., ALEX
Techniques, Technology, and Innovations Section Editor: Samuel J. Asirvatham, M.D. How to Implant a Leadless Pacemaker With a Tine-Based Fixation MIKHAEL F. EL-CHAMI, M.D., PAUL R. ROBERTS, M.D., ALEX
The EHRA White Book 2010
 Albania. Algeria. Armenia. Austria. Belarus. Belgium. Bosnia & Herzegovina. Bulgaria. Croatia Cyprus. Czech Republic. Denmark. Egypt. Estonia. Finland. Former Yugoslav Republic of Macedonia France. Georgia.
Albania. Algeria. Armenia. Austria. Belarus. Belgium. Bosnia & Herzegovina. Bulgaria. Croatia Cyprus. Czech Republic. Denmark. Egypt. Estonia. Finland. Former Yugoslav Republic of Macedonia France. Georgia.
Automatic assessment of atrial pacing threshold in current medical practice
 Europace (212) 14, 1615 1619 doi:1.193/europace/eus76 CLINICAL RESEARCH Leads and lead extraction Automatic assessment of atrial pacing threshold in current medical practice Jean Luc Rey 1, Serge Quenum
Europace (212) 14, 1615 1619 doi:1.193/europace/eus76 CLINICAL RESEARCH Leads and lead extraction Automatic assessment of atrial pacing threshold in current medical practice Jean Luc Rey 1, Serge Quenum
file://c:\documents and Settings\admin\My Documents\CV\92.htm
 Page 1 of 5 Amir Farjam Fazelifar, M.D. Assistant Professor of Cardiac Electrophysiology Academic Address: Shaheed Rajaei Cardiovascular, Medical & Research Center, Vali- Asr Avenue Tehran- Iran Tel /
Page 1 of 5 Amir Farjam Fazelifar, M.D. Assistant Professor of Cardiac Electrophysiology Academic Address: Shaheed Rajaei Cardiovascular, Medical & Research Center, Vali- Asr Avenue Tehran- Iran Tel /
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc.
 Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
Primary prevention ICD recipients: the need for defibrillator back-up after an event-free first battery service-life
 Chapter 3 Primary prevention ICD recipients: the need for defibrillator back-up after an event-free first battery service-life Guido H. van Welsenes, MS, Johannes B. van Rees, MD, Joep Thijssen, MD, Serge
Chapter 3 Primary prevention ICD recipients: the need for defibrillator back-up after an event-free first battery service-life Guido H. van Welsenes, MS, Johannes B. van Rees, MD, Joep Thijssen, MD, Serge
A Leadless Intracardiac Transcatheter Pacing System
 Original Article A Leadless Intracardiac Transcatheter Pacing System Dwight Reynolds, M.D., Gabor Z. Duray, M.D., Ph.D., Razali Omar, M.D., Kyoko Soejima, M.D., Petr Neuzil, M.D., Shu Zhang, M.D., Calambur
Original Article A Leadless Intracardiac Transcatheter Pacing System Dwight Reynolds, M.D., Gabor Z. Duray, M.D., Ph.D., Razali Omar, M.D., Kyoko Soejima, M.D., Petr Neuzil, M.D., Shu Zhang, M.D., Calambur
Cardiac resynchronization therapy for mild-to-moderate heart failure
 For reprint orders, please contact reprints@expert-reviews.com Cardiac resynchronization therapy for mild-to-moderate heart failure Expert Rev. Med. Devices 8(3), 313 317 (2011) Haran Burri Electrophysiology
For reprint orders, please contact reprints@expert-reviews.com Cardiac resynchronization therapy for mild-to-moderate heart failure Expert Rev. Med. Devices 8(3), 313 317 (2011) Haran Burri Electrophysiology
Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm
 April 2000 107 Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm B. MERKELY Semmelweis University, Dept. of Cardiovascular Surgery,
April 2000 107 Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm B. MERKELY Semmelweis University, Dept. of Cardiovascular Surgery,
UnitedHealthcare, UnitedHealthcare of the River Valley and Neighborhood Health Partnership Cardiology Notification and Prior Authorization Program:
 Notification and Prior Authorization Program: Electrophysiology Implant Classification Table The following chart contains the codes that require notification or prior authorization as part of UnitedHealthcare
Notification and Prior Authorization Program: Electrophysiology Implant Classification Table The following chart contains the codes that require notification or prior authorization as part of UnitedHealthcare
Leadless Cardiac Pacemaker
 Leadless Cardiac Pacemaker Policy Number: Original Effective Date: MM.02.042 XXXMay 1, 2019 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration; FED87 XXXMay 1, 2019 Section: Medicine
Leadless Cardiac Pacemaker Policy Number: Original Effective Date: MM.02.042 XXXMay 1, 2019 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration; FED87 XXXMay 1, 2019 Section: Medicine
Lead Extraction: Challenges in our area
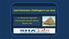 Lead Extraction: Challenges in our area More CRM Systems & Leads 600,000 new devices annually 1.2 million new leads annually Sources: 1) Medtronic CRDM Product Performance Report, Jan 2009. 2) Boston Scientific
Lead Extraction: Challenges in our area More CRM Systems & Leads 600,000 new devices annually 1.2 million new leads annually Sources: 1) Medtronic CRDM Product Performance Report, Jan 2009. 2) Boston Scientific
Factors influencing the use of subcutaneous. Rhythm Association prospective survey
 Europace (2018) 20, 887 892 doi:10.1093/europace/euy009 EHRA SURVEY Factors influencing the use of subcutaneous or transvenous implantable cardioverterdefibrillators: results of the European Heart Rhythm
Europace (2018) 20, 887 892 doi:10.1093/europace/euy009 EHRA SURVEY Factors influencing the use of subcutaneous or transvenous implantable cardioverterdefibrillators: results of the European Heart Rhythm
2010 Canadian Cardiovascular Society/ Canadian Heart Rhythm Society Training and Maintenance of Competency in Adult Clinical Cardiac
 2010 Canadian Cardiovascular Society/ Canadian Heart Rhythm Society Training and Maintenance of Competency in Adult Clinical Cardiac Electrophysiology Martin S. Green, Chair, CHRS Education Committee Peter
2010 Canadian Cardiovascular Society/ Canadian Heart Rhythm Society Training and Maintenance of Competency in Adult Clinical Cardiac Electrophysiology Martin S. Green, Chair, CHRS Education Committee Peter
Danish Pacemaker and ICD Register Annual Report 2016
 Danish Pacemaker and ICD Register Annual Report 2016 Preface The Danish Pacemaker Register was founded in 1982 by physicians from all Danish hospitals where pacemakers were implanted. When the first implantable
Danish Pacemaker and ICD Register Annual Report 2016 Preface The Danish Pacemaker Register was founded in 1982 by physicians from all Danish hospitals where pacemakers were implanted. When the first implantable
Introduction. Methods and results
 Europace (2015) 1, 468 42 doi:10.1093/europace/euv025 EP WIRE How are patients with atrial fibrillation approached and informed about their risk profile and available therapies in Europe? Results of the
Europace (2015) 1, 468 42 doi:10.1093/europace/euv025 EP WIRE How are patients with atrial fibrillation approached and informed about their risk profile and available therapies in Europe? Results of the
Comparison of clinical trials evaluating cardiac resynchronization therapy in mild to moderate heart failure
 HOT TOPIC Cardiology Journal 2010, Vol. 17, No. 6, pp. 543 548 Copyright 2010 Via Medica ISSN 1897 5593 Comparison of clinical trials evaluating cardiac resynchronization therapy in mild to moderate heart
HOT TOPIC Cardiology Journal 2010, Vol. 17, No. 6, pp. 543 548 Copyright 2010 Via Medica ISSN 1897 5593 Comparison of clinical trials evaluating cardiac resynchronization therapy in mild to moderate heart
UnitedHealthcare, UnitedHealthcare of the River Valley and Neighborhood Health Partnership Cardiology Notification and Prior Authorization Program:
 UnitedHealthcare, UnitedHealthcare of the River Valley and Neighborhood Health Partnership Cardiology Notification and Prior Authorization Program: Electrophysiology Implant Code Classification Table The
UnitedHealthcare, UnitedHealthcare of the River Valley and Neighborhood Health Partnership Cardiology Notification and Prior Authorization Program: Electrophysiology Implant Code Classification Table The
Results of transvenous lead extraction of coronary sinus leads in patients with cardiac 4,703 resynchronization therapy
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2013 Results of transvenous lead extraction of coronary sinus leads in patients
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2013 Results of transvenous lead extraction of coronary sinus leads in patients
Danish Pacemaker and ICD Register Annual report 2015
 Danish Pacemaker and ICD Register Annual report 2015 Preface The Danish Pacemaker Register was founded in 1982 by physicians from all Danish hospitals where pacemakers were implanted. When the first implantable
Danish Pacemaker and ICD Register Annual report 2015 Preface The Danish Pacemaker Register was founded in 1982 by physicians from all Danish hospitals where pacemakers were implanted. When the first implantable
Atrial fibrillation: why it's important to make opportunities diagnosis in single chamber ICD patients
 ADVANCES IN CARDIAC ARRHYTHMIAS and GREAT INNOVATIONS IN CARDIOLOGY Turin October 13-15, 2016 Atrial fibrillation: why it's important to make opportunities diagnosis in single chamber ICD patients Dott.
ADVANCES IN CARDIAC ARRHYTHMIAS and GREAT INNOVATIONS IN CARDIOLOGY Turin October 13-15, 2016 Atrial fibrillation: why it's important to make opportunities diagnosis in single chamber ICD patients Dott.
Model 5392 EPG Temporary Pacer
 Model 5392 EPG Temporary Pacer Compatible Components Reference Card 5392 Surgical Cables 5487 Disposable, short 5487L Disposable, long 5832S Reusable, small clip 5833S 5833SL Disposable, small clip, short
Model 5392 EPG Temporary Pacer Compatible Components Reference Card 5392 Surgical Cables 5487 Disposable, short 5487L Disposable, long 5832S Reusable, small clip 5833S 5833SL Disposable, small clip, short
MEDICAL POLICY Cardioverter Defibrillators
 POLICY........ PG-0224 EFFECTIVE......06/01/09 LAST REVIEW... 01/27/17 MEDICAL POLICY Cardioverter Defibrillators GUIDELINES This policy does not certify benefits or authorization of benefits, which is
POLICY........ PG-0224 EFFECTIVE......06/01/09 LAST REVIEW... 01/27/17 MEDICAL POLICY Cardioverter Defibrillators GUIDELINES This policy does not certify benefits or authorization of benefits, which is
Newer pacemakers also can monitor your blood temperature, breathing, and other factors and adjust your heart rate to changes in your activity.
 Pacemakers & Defibrillators A pacemaker system consists of a battery, a computerized generator and wires with sensors called electrodes on one end. The battery powers the generator, and both are surrounded
Pacemakers & Defibrillators A pacemaker system consists of a battery, a computerized generator and wires with sensors called electrodes on one end. The battery powers the generator, and both are surrounded
Introduction. Case Report ECG & EP CASES ABSTRACT
 Successful extraction of an implantable cardioverter-defibrillator lead in a patient with pocket infection via the femoral approach with a basket snare Jin-Bae Kim, MD, PhD. Cardiology Division, Department
Successful extraction of an implantable cardioverter-defibrillator lead in a patient with pocket infection via the femoral approach with a basket snare Jin-Bae Kim, MD, PhD. Cardiology Division, Department
CIEDs Infection: Lead Extraction, First or Last option?
 CIEDs Infection: Lead Extraction, First or Last option? More CRM Systems & Leads 600,000 new devices annually 1.2 million new leads annually Sources: 1) Medtronic CRDM Product Performance Report, Jan 2009.
CIEDs Infection: Lead Extraction, First or Last option? More CRM Systems & Leads 600,000 new devices annually 1.2 million new leads annually Sources: 1) Medtronic CRDM Product Performance Report, Jan 2009.
Top 5 Things to Know about Pacemakers and ICD s. Jeffrey S. Osborn, M.D., C.C.D.S. March 4, 2017.
 Top 5 Things to Know about Pacemakers and ICD s Jeffrey S. Osborn, M.D., C.C.D.S. March 4, 2017. Top 5 Things 1. Remote Monitoring leads to better care and outcomes. 2. MRI s CAN be done on device patients.
Top 5 Things to Know about Pacemakers and ICD s Jeffrey S. Osborn, M.D., C.C.D.S. March 4, 2017. Top 5 Things 1. Remote Monitoring leads to better care and outcomes. 2. MRI s CAN be done on device patients.
Upgrade to Resynchronization Therapy. Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic May 2016
 Upgrade to Resynchronization Therapy Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic May 2016 Event Free Survival (%) CRT Cardiac resynchronization therapy (CRT)
Upgrade to Resynchronization Therapy Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic May 2016 Event Free Survival (%) CRT Cardiac resynchronization therapy (CRT)
Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale
 Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale Jason Collinson & Stuart Tan Essex Cardiothoracic Centre, Basildon and Thurrock University Hospital. Contact: jason.collinson@nhs.net
Permanent Pacemaker Implantation Post Cardiac Surgery: A Cautionary Tale Jason Collinson & Stuart Tan Essex Cardiothoracic Centre, Basildon and Thurrock University Hospital. Contact: jason.collinson@nhs.net
Apparent Failure of Automated Threshold Evaluation: What is the Mechanism? Vikas Kalra, M.B.B.S. Lynne Foreman, R.N. Deepak Bhakta, M.D.
 Apparent Failure of Automated Threshold Evaluation: What is the Mechanism? Vikas Kalra, M.B.B.S. Lynne Foreman, R.N. Deepak Bhakta, M.D. Case Summary A 57-year-old man developed severe symptomatic tricuspid
Apparent Failure of Automated Threshold Evaluation: What is the Mechanism? Vikas Kalra, M.B.B.S. Lynne Foreman, R.N. Deepak Bhakta, M.D. Case Summary A 57-year-old man developed severe symptomatic tricuspid
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance FINAL SCOPE ENDURALIFE-powered CRT-D devices for the treatment of heart failure 1 Technology 1.1 Description of the technology
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance FINAL SCOPE ENDURALIFE-powered CRT-D devices for the treatment of heart failure 1 Technology 1.1 Description of the technology
Acute and 3-Month Performance of A Communicating Leadless Anti-Tachycardia Pacemaker and Subcutaneous Implantable Defibrillator
 Accepted Manuscript Acute and 3-Month Performance of A Communicating Leadless Anti-Tachycardia Pacemaker and Subcutaneous Implantable Defibrillator Fleur V.Y. Tjong, MD, Tom F. Brouwer, MD, Brendan Koop,
Accepted Manuscript Acute and 3-Month Performance of A Communicating Leadless Anti-Tachycardia Pacemaker and Subcutaneous Implantable Defibrillator Fleur V.Y. Tjong, MD, Tom F. Brouwer, MD, Brendan Koop,
Girish M Nair, Seeger Shen, Pablo B Nery, Calum J Redpath, David H Birnie
 268 Case Report Cardiac Resynchronization Therapy in a Patient with Persistent Left Superior Vena Cava Draining into the Coronary Sinus and Absent Innominate Vein: A Case Report and Review of Literature
268 Case Report Cardiac Resynchronization Therapy in a Patient with Persistent Left Superior Vena Cava Draining into the Coronary Sinus and Absent Innominate Vein: A Case Report and Review of Literature
COMMONLY BILLED CODES AND ASSOCIATED 2018 MEDICARE RATES
 CRHF REIMBURSEMENT & HEALTH POLICY Pacemaker Therapy COMMONLY BILLED CODES AND ASSOCIATED 2018 MEDICARE RATES This document reflects commonly billed codes for Pacemaker Therapy and their associated National
CRHF REIMBURSEMENT & HEALTH POLICY Pacemaker Therapy COMMONLY BILLED CODES AND ASSOCIATED 2018 MEDICARE RATES This document reflects commonly billed codes for Pacemaker Therapy and their associated National
Technical option of surgical approach for trouble-shooting
 JHRS Corner Device and lead trouble-shooting - standard strategy and technical option - Technical option of surgical approach for trouble-shooting Katsuhiko IMAI Department of Cardiovascular surgery, Hiroshima
JHRS Corner Device and lead trouble-shooting - standard strategy and technical option - Technical option of surgical approach for trouble-shooting Katsuhiko IMAI Department of Cardiovascular surgery, Hiroshima
Indication, Timing, Assessment and Update on TAVI
 Indication, Timing, Assessment and Update on TAVI Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Starr- Edwards Mechanical
Indication, Timing, Assessment and Update on TAVI Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Starr- Edwards Mechanical
Different indications for pacemaker implantation are the following:
 Patient Resources: ICD/Pacemaker Overview ICD/Pacemaker Overview What is a pacemaker? A pacemaker is a device that uses low energy electrical pulses to prompt the heart to beat whenever a pause in the
Patient Resources: ICD/Pacemaker Overview ICD/Pacemaker Overview What is a pacemaker? A pacemaker is a device that uses low energy electrical pulses to prompt the heart to beat whenever a pause in the
Biventricular Pacing - Hemodynamic Benefit for Patients with Congestive Heart Failure
 428 December 2000 Biventricular Pacing - Hemodynamic Benefit for Patients with Congestive Heart Failure K. MALINOWSKI Helios Clinics, Aue, Germany Summary Congestive heart failure afflicts a large and
428 December 2000 Biventricular Pacing - Hemodynamic Benefit for Patients with Congestive Heart Failure K. MALINOWSKI Helios Clinics, Aue, Germany Summary Congestive heart failure afflicts a large and
BSH Annual Autumn Meeting 2017
 BSH Annual Autumn Meeting 2017 Presentation title: The Development of CRT Speaker: John GF Cleland Conflicts of interest: I have received research support and honoraria from Biotronik, Boston Scientific,
BSH Annual Autumn Meeting 2017 Presentation title: The Development of CRT Speaker: John GF Cleland Conflicts of interest: I have received research support and honoraria from Biotronik, Boston Scientific,
PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS. HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate
 PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate Measure Title Description Measure Type Data Source Level of Analysis Numerator HRS-3:
PERFORMANCE MEASURE TECHNICAL SPECIFICATIONS HRS-3: Implantable Cardioverter-Defibrillator (ICD) Complications Rate Measure Title Description Measure Type Data Source Level of Analysis Numerator HRS-3:
Q & A: How to Safely Scan Patients with a SureScan MRI Pacemaker
 Q & A: How to Safely Scan Patients with a SureScan MRI Pacemaker Patient Scheduling and Screening Q: Is there any special (other than regular MRI consent) consent form that should be signed by the patient?
Q & A: How to Safely Scan Patients with a SureScan MRI Pacemaker Patient Scheduling and Screening Q: Is there any special (other than regular MRI consent) consent form that should be signed by the patient?
Make the Connection A clinical compendium on the relationship between AF, stroke, and early intervention
 Make the Connection A clinical compendium on the relationship between AF, stroke, and early intervention Data that date back to the 1970 s have illustrated the strong relationship between atrial fibrillation
Make the Connection A clinical compendium on the relationship between AF, stroke, and early intervention Data that date back to the 1970 s have illustrated the strong relationship between atrial fibrillation
2015 Procedural Payment Guide
 Contents Introduction Disclaimer (print page 2) Description of Payment Methods (print page 3) Procedural Payment Guide: Cardiac Rhythm Management and Electrophysiology Procedures (print page range: 4-17)
Contents Introduction Disclaimer (print page 2) Description of Payment Methods (print page 3) Procedural Payment Guide: Cardiac Rhythm Management and Electrophysiology Procedures (print page range: 4-17)
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29358 holds various files of this Leiden University dissertation. Author: Thijssen, Joep Title: Clinical aspects and socio-economic implications of implantable
Cover Page The handle http://hdl.handle.net/1887/29358 holds various files of this Leiden University dissertation. Author: Thijssen, Joep Title: Clinical aspects and socio-economic implications of implantable
Watchman. Left Atrial Appendage Closure Device. Uniquely engineered for the LAA 1-3 with proven safety and longterm efficacy. 4-8
 TM Watchman Left Atrial Appendage Closure Device PROOF OFLEADERSHIP Uniquely engineered for the LAA 1-3 with proven safety and longterm efficacy. 4-8 Patients with AF have a 5x increased risk of stroke.
TM Watchman Left Atrial Appendage Closure Device PROOF OFLEADERSHIP Uniquely engineered for the LAA 1-3 with proven safety and longterm efficacy. 4-8 Patients with AF have a 5x increased risk of stroke.
PACING AT THE BUNDLE OF HIS
 PACING AT THE BUNDLE OF HIS Cardiac Rhythm Heart Failure Coding Corner Disclaimer While Medtronic offers opinions about how to code when using our technology according to its FDA-approved labeling, these
PACING AT THE BUNDLE OF HIS Cardiac Rhythm Heart Failure Coding Corner Disclaimer While Medtronic offers opinions about how to code when using our technology according to its FDA-approved labeling, these
Dr Mark Earley MD FRCP Consultant Cardiologist
 Dr Mark Earley MD FRCP Consultant Cardiologist PERSONAL DETAILS ADDRESS (NHS) (Private practice) Dominion House, St Olaf House, St Bartholomew s London Bridge Hospital Hospital, 27 Tooley Street, London,
Dr Mark Earley MD FRCP Consultant Cardiologist PERSONAL DETAILS ADDRESS (NHS) (Private practice) Dominion House, St Olaf House, St Bartholomew s London Bridge Hospital Hospital, 27 Tooley Street, London,
