Inflammatory Bowel Disease
|
|
|
- Mabel Small
- 5 years ago
- Views:
Transcription
1 Inflammatory Bowel Disease Objectives: NOT FOUND. Team Members: Shrouq alsomali + Basel almeflh + Alaa alaqeel + Raneem alghamdi Team Leader: Haneen Alsubki Revised By: Maha AlGhamdi Resources: 435 team Slides Editing file Feedback Color index: IMPORTANT - NOTES - EXTRA - Books
2 Inflammatory Bowel Disease IBD : 8:58 minutes Definition : IBD is comprised of two major disorders: ulcerative colitis (UC) and crohn s disease(cd). These disorders have both distinct and overlapping pathologic and clinical characteristics. So it s clinically useful to distinguish between these two conditions because of differences in their management. Epidemiology: - More common in the west, but the incidence is increasing in the developing countries including saudi arabia. - IBD can present at any age: The peak: years. A second peak is 50 years old in our community we just see the peak of (15-30) cus people who are at age of 50 did not live in the environment that promotes the disease. Etiology: Both diseases has no clear cause, but there are multiple factors which hypothesized to Play Role: 1- Environmental factors: Smoking Appendectomy Persistent infection (triggered by organisms and the body exaggerates in response and unregulated inflammation happens) Defective mucosal integrity Dysbiosis Dysregulated immune response -increases the chance for crohn s disease. -has a protective role in Ulcerative colitis. have a protective role in Ulcerative colitis. -mycobacteria -helicobacter sp. -measles,mumps -listeria. -toxigenic -E.coli. - altered mucus. -increased permeability. -cellular starvation. -impaired restitution. ( change in microbiota of the gut): protective bacteria aggressive commensals -loss of tolerance -aggressive cellular activation. -defective apoptosis. 2- Diet: Western diet and Frozen food increase the chance of developing IBD, especially in children less 10 years-old.
3 Ulcerative Colitis Definition: UC is a chronic inflammatory disease characterized by recurrent episodes of inflammation limited to the mucosal layer of the rectum and colon. Starts at the rectum then extends proximally. General characteristics Involves the rectum in all cases and can involve the colon either partially or entirely: A. Ulcerative proctitis: rectum alone. B. Ulcerative proctosigmoiditis: rectum and sigmoid colon. C. Left-sided colitis: disease that extends beyond the rectum and as far proximally as the splenic flexure. D.Extensive colitis: beyond the splenic flexure. E.Pancolitis: whole colon. Ulcerative proctitis and Ulcerative proctosigmoiditis most common A+ B = 40-50% of patients Extending beyond the sigmoid C+ D = 30-40% of patients Pancolitis E = 20% of patients Ulcerations are not deep. from a clinical point of view we just divide them into (A+B+C), for example if someone gets extensive colitis, he will be treated as if he got pancolitis. The course is unpredictable and characterized by periodic exacerbation and periods of complete remission. Blood in the stool could be: A. Proctitis: fresh blood or blood-stained mucus that is either mixed with the stool or streaked on the surface. The stool could be normal or hard. B. If the disease extends beyond the rectum, blood is usually mixed with stool or grossly bloody diarrhea may be noted. C. If the disease is severe, patients pass liquid stool containing blood, pus, or fecal matter. Clinical features Diagnosis Diarrhea ( bloody diarrhea ). Also called large bowel diarrhea, (they will present with frequency and small amounts ) because ulcerations is usually in the rectum, so the rectum cant hold the stool that s why they have urgency ). Since it's almost always associated with bloody diarrhea its is more accompanied with anemia. Rectal bleeding ( Hematochezia ) Crampy abdominal pain. Start when the patient develop left sided colitis. Tenesmus recurrent need to evacuate the bowel. Passage of mucus. Extraintestinal symptoms: skin lesions, jaundice, arthritis. In moderate to severe disease: anorexia, nausea, vomiting, fever, weight loss. When its only limited to the rectum or sigmoid, the patient won t have severe symptoms NO SINGLE MODALITY IS ENOUGH FOR DIAGNOSIS! Combination of clinical picture, laboratory, endoscopy, pathology are required for the diagnosis of UC. Colonoscopy and mucosal biopsy are the gold standard investigation for the diagnosis of UC : 1- stool culture for C. difficile, ova and parasites - to rule out infectious diarrhea. 2- fecal leukocytes.
4 3- Colonoscopy: Vascular markings are lost. colon mucosa will disappear Petechiae, exudates, touch friability and frank hemorrhage rectal bleeding may be present. Colonic involvement is continuous in ulcerative colitis, in contrast to the patchy nature of Crohn's disease. Superficial ulcerations Pathology Inflammation is not transmural, it is limited to the mucosa. Chronic inflammation PMNs accumulate in the crypts of the colon (crypt abscesses) Chronic changes including branching of crypts, atrophy of glands, and loss of mucin in goblet cells. - They have pseudo-polyps (thats is the mucosa trying to re-generate) Complications Goals of therapy In both CD and UC : Hemorrhage. Perforation. Colon cancer: The risk correlates with extent and duration of colitis. However, in distal proctitis there is no increased risk for colorectal cancer. Toxic megacolon: is the leading cause of death in UC and affects <5% of patients. It is associated with a risk of colonic perforation. (It is a transverse colon with a diameter of more than 5-6 cm with loss of haustration) Iron deficiency anemia Electrolyte disturbances and dehydration secondary to diarrhea Sclerosing cholangitis (SC) Cholangiocarcinoma Half of all bile duct cancers are associated with UC. Growth retardation. Psychosocial issues (e.g., depression) often due to chronicity and the disabling nature of the disease. Induce and maintain remission. Ameliorate symptoms. Improve pts quality of life. Adequate nutrition. Prevent complication of both the disease and medications. Management 1- Medical: Rule out infections before start treatment (always First thing to do even if it's not the first visit) How? Stool culture. E.g. Salmonella gastroenteritis Even if the patient is a known case of UC, because you don't want to start with steroids and suppress their immune response while they have infection. a. 5-ASA Aminosalicylates : (oral, rectal) work very well with UC but no rule in Crohn s Sulfasalazine (topical application as a suppository) is the mainstay of treatment. Preferred over topical steroids because they are effective as maintenance therapy. Remission rates as high as 93% have been reported. 2- Surgical: often curative (unlike Crohn s disease) and involves total colectomy because there is great chance they will get the cancer in another area Indications for surgery include : a. Severe attacks that fail to respond to medical therapy. b. Complications of a severe attack (e.g., perforation, acute dilatation). c. Chronic continuous disease with an impaired quality of life.
5 It is effective in induction and maintaining remissions. 5-ASA (mesalamine) is the active component. 5-ASA enemas can be used for proctitis and distal colitis. give two forms (oral and rectal) if its beyond the rectum like rectosigmoiditis, more effective b. Systemic corticosteroids are used for acute exacerbations. Good for induction of remission ONLY. never for maintenance, because of the side effects. Systemic: Prednisolone Local acting: enema. c. Immunomodulators agents in patients with refractory disease may prevent relapses but are not effective for acute attacks. ( Azithyoprine - Methotrexate) just for maintanance. d. Dysplasia or carcinoma d. Anti TNF therapy ( infliximab ): if not responding. induction and maintaining remissions. Contraindicated in the presence of infections. Crohn's disease (CD) Definition: Location: I s a disorder of uncertain etiology that is characterized by chronic transmural inflammation of the gastrointestinal tract. It s also called (regional enteritis). CD may involve the entire gastrointestinal tract from mouth to the perianal area. 80% Small bowel. 50 % ileocolitis. Most common base of crohn s 20 % colon. 30% perianal disease. UGI < 5 % Upper GI (mouth, stomach, esophagus)
6 Clinical manifestation: KEY POINTS IN CD : Fever, Fatigue and malaise. Early manifestation Abdominal pain (usually RLQ pain), nausea and vomiting. early manifestation Non-bloody diarrhea. late manifestation Malabsorption and weight loss. Weight loss is a late manifestation. The pain is often associated with diarrhea, which is usually watery and does not contain blood or mucus. Extraintestinal manifestation :,Arthritis, Eye involvement: (uveitis - iritis - episcleritis), Skin disorders. Others: Primary sclerosing cholangitis more with UC, Venous and arterial thromboembolism,renal stones,bone loss and osteoporosis,vitamin B12 deficiency, aphthous oral ulcers, painless pyoderma gangrenosum and painful erythema nodosum (more details will be mentioned below). Crohn s colitis presents in an identical manner to ulcerative colitis, but rectal sparing and the presence of perianal disease are features which favour a diagnosis of Crohn s disease 1. Phlegmon/abscess: walled off inflammatory mass without bacterial infection Crohn s patients are more prone to have fistulas and abscesses than UC patients 2.Fistula: are tracts or communications that connect two epithelial-lined organs a. With other loop of the intestine ( enteroenteric ). b. With bladder ( enterovesical ). c. Vagina ( enterovgainal ). d. With skin ( enterocutaneous ) Perianal disease: Anorectal diseases ( in 30% ) Include fissures, abscesses, perianal fistulas (almost exclusively to Crohn s) e. Severe oral involvement: aphthous ulcers. Rarely f. Esophageal involvement: odynophagia and dysphagia. g. Gastroduodenal CD: upper abdominal pain and symptoms of gastric outlet obstruction. h. Gallstones. Usually the inflammation affects the ileum, and the reabsorption of bile salts happens there, normally bile salts bind to cholesterol and make it water soluble, so Without enough bile salts, cholesterol can form stones. i. Increased risk of renal stones (calcium oxalate calculi), inflammation of the small bowel result in accumulation of oxalate in the blood. The diagnosis of CD is usually established with endoscopic findings or imaging studies in a patient with a compatible clinical history. 1. Compatible clinical history. 2. Endoscopic findings: (the most accurate test) : A. Colonoscopy: B. Wireless capsule endoscopy. (helpful in pediatrics, and useful for identification of small bowel inflammation.. Diagnosis
7 Endoscopic features include focal ulcerations adjacent to areas of normal appearing mucosa along with polypoid mucosal changes that give a cobblestone. -You would also see non-caseating granulomas.. -Stricture or extreme narrowing are contraindications for this modality 3. I maging studies in a patient: a. small bowel follow through (SBFT) not done anymore b. computed tomography: CTS or CT enterography c. Magnetic resonance imaging (MRI) or MR enterography best imaging modality for CD. 4. Serologic markers: (used when the diagnosis still unclear) : Inflammatory marker: ESR, CRP Antineutrophil cytoplasmic antibodies ( panca) : positive in UC Anti-Saccharomyces cerevisiae antibodies (ASCA) : positive in CD Stool markers: fecal calprotectin. done very often, it detects any inflammation in the small bowel (it won t tell us if its crohn s or gastroenteritis) but at the very least it would tell us there is an inflammation ongoing, meaning it has good sensitivity and not specific. Inflammation would give a positive fecal calprotectin It CAN differentiate between IBS and (IBD or any inflammation) - Induce and maintain remission. - Ameliorate symptoms Goals of therapy - Improve patient quality of life - Adequate nutrition - Prevent complication of both the disease and medications 1- Medical: Rule out infections (again. First thing to do) How? Stool culture. a. corticosteroids (systemic = prednisone or long acting = budesonide): for acute exacerbations and if no response to metronidazole. Good for induction of remission ONLY not maintenance b. Immunomodulators (azathioprine, Methotrexate): in conjunction with steroids if the patient does not respond to above agents. Good for induction of remission AND maintenance c. Anti TNF therapy ( infliximab )
8 Management: d. Bile acid sequestrants (cholestyramine or colestipol): for patients with terminal ileal disease who cannot absorb bile acids e. Antidiarrheal agents generally not a good choice (may cause ileus) 5-ASA has NO role in treating Crohn s disease 2- Surgical: eventually required in most patients we don t want the patient to have short bowel syndrome Indications for surgery include: small bowel Obstruction, severe perianal disease unresponsive to medical therapy, difficult fistulas (especially between bowel and bladder, vagina), major bleeding, severe disability and perforation or abscess) Conservative surgery, just resect that one affected part, unlike ulcerative colitis you resect the whole bowel. Ileostomy is very helpful, it evacuates the stool if the condition is so severe. because the biggest problem which causes more pain and inflammation is that when the feces gets trapped inside the ulcers. 3- Nutritional supplementation and support: Parenteral nutrition is sometimes necessary.
9 Extraintestinal manifestations (BOTH CD AND UC) Davidsons Principles and Practice of Medicine 22ed CD and ulcerative colitis share a number of extraintestinal manifestations : Eye lesions: Epi-scleritis Anterior uveitis: independent course. iritis. Skin lesions: Erythema nodosum: especially in Crohn s disease; parallels bowel disease activity. Pyoderma gangrenosum: especially in UC; parallels bowel disease activity in 50% of cases. Arthritis: most common extraintestinal manifestation of IBD. Venous and arterial thromboembolism Bone loss and Osteoporosis. Renal stones Gallstones in Crohn s disease ( ileal involvement ). Primary Sclerosing cholangitis in UC. Vitamin B12 deficiency
10 Sum Up : Davidsons Principles and Practice of Medicine 22ed Feature CD UC Characteristics of CD and UC Location SB or colon colon Anatomic distribution Skip lesions Continuous Rectal involvement Rectal spare Involved in >90% Gross bleeding Only 25% Universal Peri-anal disease 1/3 Rare Fistulization Yes No Granulomas 30% No Endoscopic features of CD and UC
11 Mucosal involvement Discontinuous Continuous Aphthous ulcers Common Rare Surrounding mucosa Relatively normal Abnormal Longitudinal ulcer Common Rare Cobble stoning In severe cases No Mucosal friability Uncommon Common Vascular pattern Normal distorted Pathologic features of CD and UC Transmural inflammation Yes Uncommon Granulomas 30% No Fissures Common Rare Fibrosis Common No Submucosal inflammation Common Uncommon
12 SUMMARY Ulcerative colitis Crohn's disease Age of onset * The peak :15-30 years * A second peak 50 Etiology * Genetic factors: NOD2/CARD15 * aggressive commensals * Environmental factors Involvement Clinical features * limited to the mucosal layer of the colon * Start rectum then extend proximally * can be presented as: - proctitis - proctosigmoiditis / Left-sided colitis - Extensive colitis / Pancolitis * diarrhea * rectal bleeding * tenesmus * passage of mucus * crampy abdominal abdominal pain * blood stained mucus Streaked onto the surface of stool in case of proctitis * blood is usually mixed with stool or grossly bloody diarrhea disease extends beyond the rectum * anorexia, nausea, vomiting, fever, weight Loss in case of excessive and pancolitis * complications : ( Hemorrhage -Perforation Toxic megacolon - cancer ) * transmural inflammation may involve the entire gastrointestinal tract. * the most common presentation is ileocolitis * Fatigue * Diarrhea and Weight loss late symptoms because crohn s typically affect small area * Abdominal pain * Fever * Phlegmon/abscess (with no pus) * fistulas (due to transmural involvement) * Perianal disease * aphthous ulcers * Esophageal involvement odynophagia and dysphagia. * Gastroduodenal CD upper abdominal pain and gastric obstruction symptoms * gallstones * Extraintestinal mnifistatiom: ( Arthritis - Eye involvement - Skin disorders eg: erythema nodosum - Primary sclerosing cholangitis - thromboembolism - Renal stones - osteoporosis,vitamin B12 deficiency). Investigation : CD need different modalities and it difficult to be diagnosed * Colonoscopy * Colonoscopy * Wireless capsule endoscopy (before use it we have to insure that there is no stricture in small bowe) * SBFT (we used to use it in the past ) * CT * MRI * Serologic markers Findings * The vascular markings are lost * superficial ulceration * continuous involvement * pathology : - crypt abscesses - signs of chronic inflammation * skip lesions * cobblestone * Serologic markers: - ERS, CRP - antibodies : ( panka), (ASCA) - stool markers : fecal calprotectin (to investigate if there is inflammation or not so
13 Management : To induce and maintain remission, improve quality of life and prevent complications * Role out infection * 5 ASA therapy indicates and maintain remission * corticosteroid * Immunomodulators maintain remission - Azathioprine - Methotrexate * biological therapy: - Anti TNF therapy indicates and maintain remission can help in differentiation between IBD and IBS) * Role out infection * corticosteroid * Immunomodulators maintain remission - Azathioprine - Methotrexate * biological therapy: - Anti TNF therapy indicates and maintain remission Surgery indications last option, but do not wait until the patient is very sick and can not survive during surgery * Severe attacks that fail to respond to medical therapy * Complications * impaired quality of life * Dysplasia or carcinoma *Obstruction, *severe perianal disease unresponsive to medical therapy *major bleeding * severe disability QUESTIONS 1/ A 35-year-old white man presents with diarrhea, weight loss, and RLQ pain. On examination, a tender mass is noted in the RLQ; the stool is guaiac-positive. Colonoscopy shows segmental areas of inflammation. Barium small bowel series shows nodular thickening of the terminal ileum. a. Ulcerative colitis b. Crohn disease c. Ischemic colitis d. Diverticulosis 2/ A 75-year-old African American woman, previously healthy, presents with low-grade fever, diarrhea, and rectal bleeding. Colonoscopy shows continuous erythema from rectum to mid-transverse colon. The cecum is normal. a. Ulcerative colitis b. Crohn disease c. Ischemic colitis d. Diverticulosis 3/ 19-year-old woman presents with a 3-month history of crampy abdominal pain not related to eating. She also has bloody diarrhea, is fatigued, and has lost 5 pounds. She has both constipation and diarrhea. She has tender red sores on the anterior aspects of her lower extremities and decreased range of motion at the lumbar spine. She has anemia with a hemoglobin of g/dl. Which of the following is the most likely diagnosis? a. Inflammatory bowel disease b. Infectious colitis c. Irritable bowel disease d. Anal fissure
14 4/ A 32-year-old woman has a history of chronic diarrhea and gallstones and now has rectovaginal fistula. Which of the following is the most likely diagnosis? A. Crohn disease B. Ulcerative colitis C. Systemic lupus erythematosus D. Laxative abuse 5/ A 24-year-old male presents to your office having with worsening RLQ cramping abdominal pain for the past 2 months. He reports having diarrhea on and off for the past 1 to 2 years. He previously had colonoscopy with a terminal ileum biopsy showing ulceration, acute inflammation, and noncaseating granulomas. Two months ago he was placed on mesalamine. He has lost 20 lb since then despite attempting to increase his dietary intake. He denies any other medical problems and takes no other medications. His physical examination reveals mild tenderness in the RLQ with normal bowel sounds. There are no anal fissures or fistulae. His stool is negative for occult blood. Vital signs are as follows: Temperature = 98.7 F, RR = 15, BP = 122/78 mm Hg, pulse = 65. BMI 21. Laboratory test results show normal liver/renal function. CBC shows Hgb 9.9 g/dl, MCV 82 fl, WBC /mm3. X-ray abdomen reveals nonspecific gas pattern without free air or distended bowel loops. CT enterography reveals thickened mucosa in distal ileum with adjacent mesenteric stranding; there is no fistula, abscess, or free air present. What would be the single most effective intervention recommended to this patient? A. Loperamide B. Azathioprine C. Infliximab D. Surgical resection answers : 1/B 2/A 3/A 4/A 5/C
Treatment of Inflammatory Bowel Disease. Michael Weiss MD, FACG
 Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Surgical Management of IBD. Val Jefford Grand Rounds October 14, 2003
 Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
Inflammatory Bowel Disease When is diarrhea not just diarrhea?
 Inflammatory Bowel Disease When is diarrhea not just diarrhea? Jackie Kazik, MA, PA C CME Resources CAPA Annual Conference, 2011 Inflammatory Bowel Disease Objectives Discuss what is known about the pathophysiology
Inflammatory Bowel Disease When is diarrhea not just diarrhea? Jackie Kazik, MA, PA C CME Resources CAPA Annual Conference, 2011 Inflammatory Bowel Disease Objectives Discuss what is known about the pathophysiology
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
INFLAMMATORY BOWEL DISEASE. Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic
 INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
INFLAMMATORY BOWEL DISEASE
 National University Faculty of Medicine INFLAMMATORY BOWEL DISEASE Gehan M. Osman, MD. MBBS Pediatrician Jaffar Ibn Auf Specialized Hospital EDUCATIONAL OBJECTIVES Definitions and spectrum of (IBD) Epidemiology
National University Faculty of Medicine INFLAMMATORY BOWEL DISEASE Gehan M. Osman, MD. MBBS Pediatrician Jaffar Ibn Auf Specialized Hospital EDUCATIONAL OBJECTIVES Definitions and spectrum of (IBD) Epidemiology
SURGICAL MANAGEMENT OF ULCERATIVE COLITIS
 SURGICAL MANAGEMENT OF ULCERATIVE COLITIS Cary B. Aarons, MD Associate Professor of Surgery Division of Colon & Rectal Surgery University of Pennsylvania AGENDA Background Diagnosis/Work-up Medical Management
SURGICAL MANAGEMENT OF ULCERATIVE COLITIS Cary B. Aarons, MD Associate Professor of Surgery Division of Colon & Rectal Surgery University of Pennsylvania AGENDA Background Diagnosis/Work-up Medical Management
Crohn's disease CAUSES COURSE OF CROHN'S DISEASE TREATMENT. Sulfasalazine
 Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
What is Crohn's disease?
 What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
PEDIATRIC INFLAMMATORY BOWEL DISEASE
 PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
What do we need for diagnosis of IBD
 What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
Diseases of the Colon. Jack Bragg, D.O., F.A.C.O.I.
 Diseases of the Colon Jack Bragg, D.O., F.A.C.O.I. I have no disclosures I work for the Curators of the University of Missouri Inflammatory Bowel Disease ULCERATIVE COLITIS CROHN S DISEASE Transmural Inflammation
Diseases of the Colon Jack Bragg, D.O., F.A.C.O.I. I have no disclosures I work for the Curators of the University of Missouri Inflammatory Bowel Disease ULCERATIVE COLITIS CROHN S DISEASE Transmural Inflammation
Crohn's Disease. What causes Crohn s disease? What are the symptoms?
 Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
The Spectrum of IBD. Inflammatory Bowel Disease. Symptoms. Epidemiology. Tests for IBD. CD or UC? Inflamatory Bowel Disease. Fernando Vega, M.D.
 The Spectrum of IBD Inflammatory Bowel Disease Fernando Vega, M.D. Epidemiology CD and UC together 1:400 UC Prevalence 1:500 UC Incidence 6-12K/annum CD Prevalence 1:1000 CD Incidence 3-6K/annum Symptoms
The Spectrum of IBD Inflammatory Bowel Disease Fernando Vega, M.D. Epidemiology CD and UC together 1:400 UC Prevalence 1:500 UC Incidence 6-12K/annum CD Prevalence 1:1000 CD Incidence 3-6K/annum Symptoms
Crohn s Disease. Resident Lecture 1/17/19
 Crohn s Disease Resident Lecture 1/17/19 Objectives Features/Classification of Crohn s Disease Medical Treatment Surgical Indications Surgical Considerations 2 Case 25 yo F presents to your office with
Crohn s Disease Resident Lecture 1/17/19 Objectives Features/Classification of Crohn s Disease Medical Treatment Surgical Indications Surgical Considerations 2 Case 25 yo F presents to your office with
Patho Basic Chronic Inflammatory Bowel Diseases. Jürg Vosbeck Pathology
 Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
NEW CONCEPTS IN CROHN S DISEASE GLENDON BURRESS, MD PEDIATRIC GASTROENTEROLOGY ROCKFORD, IL
 NEW CONCEPTS IN CROHN S DISEASE GLENDON BURRESS, MD PEDIATRIC GASTROENTEROLOGY ROCKFORD, IL CROHN S DISEASE Chronic disease of uncertain etiology Etiology- genetic, environmental, and infectious Transmural
NEW CONCEPTS IN CROHN S DISEASE GLENDON BURRESS, MD PEDIATRIC GASTROENTEROLOGY ROCKFORD, IL CROHN S DISEASE Chronic disease of uncertain etiology Etiology- genetic, environmental, and infectious Transmural
Inflammatory Bowel Disease Ischemic bowel disease
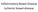 Inflammatory Bowel Disease Ischemic bowel disease Inflammatory Bowel Disease The two disorders that comprise IBD are: ulcerative colitis Crohn disease The distinction between ulcerative colitis and Crohn
Inflammatory Bowel Disease Ischemic bowel disease Inflammatory Bowel Disease The two disorders that comprise IBD are: ulcerative colitis Crohn disease The distinction between ulcerative colitis and Crohn
children Crohn s disease in MR enterography for GI Complications Microscopy Characterization Primary sclerosing cholangitis Anorectal fistulae
 MR enterography for Crohn s disease in children BOAZ KARMAZYN, MD PEDIATRIC RADIOLOGY ASSOCIATE PROFESSOR Characterization Crohn disease Idiopathic chronic transmural IBD Increasing incidence Age 7/100,000
MR enterography for Crohn s disease in children BOAZ KARMAZYN, MD PEDIATRIC RADIOLOGY ASSOCIATE PROFESSOR Characterization Crohn disease Idiopathic chronic transmural IBD Increasing incidence Age 7/100,000
Year 2002 Paper two: Questions supplied by Jo 1
 Year 2002 Paper two: Questions supplied by Jo 1 29) A 54 year old man with colonic Crohn s disease is in remission following an 8 week course of prednisolone. Which one of the following medications is
Year 2002 Paper two: Questions supplied by Jo 1 29) A 54 year old man with colonic Crohn s disease is in remission following an 8 week course of prednisolone. Which one of the following medications is
Certain genes passed on from parent to child increase the risk of developing Crohn's disease, if the right trigger occurs.
 Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
ULCERATIVE COLITIS. Sean Lynch, MD and Richard Bloomfeld, MD Wake Forest University School of Medicine Winston-Salem, NC
 ULCERATIVE COLITIS Sean Lynch, MD and Richard Bloomfeld, MD Wake Forest University School of Medicine Winston-Salem, NC What is Ulcerative Colitis? Ulcerative colitis (UC) is a disease marked by inflammation
ULCERATIVE COLITIS Sean Lynch, MD and Richard Bloomfeld, MD Wake Forest University School of Medicine Winston-Salem, NC What is Ulcerative Colitis? Ulcerative colitis (UC) is a disease marked by inflammation
Definitions. Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency)
 CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
Index. Surg Clin N Am 87 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Clin N Am 87 (2007) 787 796 Index Note: Page numbers of article titles are in boldface type. A Abscesses in anorectal Crohn s disease, 622 intra-abdominal, in Crohn s disease, 590 591 perirectal,
Surg Clin N Am 87 (2007) 787 796 Index Note: Page numbers of article titles are in boldface type. A Abscesses in anorectal Crohn s disease, 622 intra-abdominal, in Crohn s disease, 590 591 perirectal,
Chapter 34. Nursing Care of Patients with Lower Gastrointestinal Disorders
 Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
P a g e 1. Inflammatory Bowel Disease Guidelines
 P a g e 1 Inflammatory Bowel Disease Guidelines Introduction Inflammatory bowel disease (IBD) is a chronic inflammatory disease affecting the gastrointestinal (GI) system. It is comprised of two major
P a g e 1 Inflammatory Bowel Disease Guidelines Introduction Inflammatory bowel disease (IBD) is a chronic inflammatory disease affecting the gastrointestinal (GI) system. It is comprised of two major
Clinical Manifestations of Gastrointestinal Disorders. Awni Taleb Abu sneineh
 Clinical Manifestations of Gastrointestinal Disorders Awni Taleb Abu sneineh Major areas of Interest in GIT Esophageal disorders Peptic ulcer disease Inflamatory bowel disease Malignancy Liver disease
Clinical Manifestations of Gastrointestinal Disorders Awni Taleb Abu sneineh Major areas of Interest in GIT Esophageal disorders Peptic ulcer disease Inflamatory bowel disease Malignancy Liver disease
How do I choose amongst medicines for inflammatory bowel disease. Maria T. Abreu, MD
 How do I choose amongst medicines for inflammatory bowel disease Maria T. Abreu, MD Overview of IBD Pathogenesis Bacterial Products Moderately Acutely Inflamed Chronic Inflammation = IBD Normal Gut Mildly
How do I choose amongst medicines for inflammatory bowel disease Maria T. Abreu, MD Overview of IBD Pathogenesis Bacterial Products Moderately Acutely Inflamed Chronic Inflammation = IBD Normal Gut Mildly
An Unusual Complication of Crohn s Disease. Dr Gerald Busuttil Mr Debono s Firm Surgical Grand Round 25 th November 2008
 An Unusual Complication of Crohn s Disease Dr Gerald Busuttil Mr Debono s Firm Surgical Grand Round 25 th November 2008 Case Presentation 70 year old lady k/c of Crohns disease h/o of Hartmann s procedure
An Unusual Complication of Crohn s Disease Dr Gerald Busuttil Mr Debono s Firm Surgical Grand Round 25 th November 2008 Case Presentation 70 year old lady k/c of Crohns disease h/o of Hartmann s procedure
Mohamed EL-hemaly Gastro- intestinal surgical center, Mansoura University.
 Mohamed EL-hemaly Gastro- intestinal surgical center, Mansoura University. Chronic transmural inflammatory process of the bowel & affects any part of the gastro -intestinal tract from the mouth to the
Mohamed EL-hemaly Gastro- intestinal surgical center, Mansoura University. Chronic transmural inflammatory process of the bowel & affects any part of the gastro -intestinal tract from the mouth to the
ULCERATIVE COLITIS DEFINITION
 DR R DE LACY ULCERATIVE COLITIS DEFINITION Inflammation of the lining of the large bowel (colon and rectum) Aetiology is poorly understood Genetic factors - aggregation in families - identical twin concordance
DR R DE LACY ULCERATIVE COLITIS DEFINITION Inflammation of the lining of the large bowel (colon and rectum) Aetiology is poorly understood Genetic factors - aggregation in families - identical twin concordance
WHAT IS ULCERATIVE COLITIS?
 235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Ulcerative Colitis WHAT IS ULCERATIVE COLITIS? Ulcerative colitis is
235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Ulcerative Colitis WHAT IS ULCERATIVE COLITIS? Ulcerative colitis is
Understanding Learning is the first step to getting help.
 Understanding Inflammatory Bowel Disease (IBD) Learning is the first step to getting help. This booklet has been created through an educational grant provided by Fulford India Ltd., A subsidiary of Schering-Plough
Understanding Inflammatory Bowel Disease (IBD) Learning is the first step to getting help. This booklet has been created through an educational grant provided by Fulford India Ltd., A subsidiary of Schering-Plough
What is ulcerative colitis?
 What is ulcerative colitis? Ulcerative colitis is a disease that causes inflammation and sores, called ulcers, in the lining of the rectum and colon. Ulcers form where inflammation has killed the cells
What is ulcerative colitis? Ulcerative colitis is a disease that causes inflammation and sores, called ulcers, in the lining of the rectum and colon. Ulcers form where inflammation has killed the cells
Ulcerative Colitis. ulcerative colitis usually only affects the colon.
 Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
... Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment.
 Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
ExtraintestinalManifestations of IBD
 ExtraintestinalManifestations of IBD Hyun Kim, M.D. San Diego Digestive Disease Consultants Associate Professor, UCSD School of Medicine Why Other Organs Involved in IBD? Organ Involvement Bones, Joints
ExtraintestinalManifestations of IBD Hyun Kim, M.D. San Diego Digestive Disease Consultants Associate Professor, UCSD School of Medicine Why Other Organs Involved in IBD? Organ Involvement Bones, Joints
3/22/2011. Inflammatory Bowel Disease. Inflammatory Bowel Disease Objectives: Appendicitis. Lemone and Burke Chapter 26
 Inflammatory Bowel Disease Lemone and Burke Chapter 26 Inflammatory Bowel Disease Objectives: Discuss etiology, patho and clinical manifestations of Appendicitis Peritonitis Ulcerative Colitis Crohn s
Inflammatory Bowel Disease Lemone and Burke Chapter 26 Inflammatory Bowel Disease Objectives: Discuss etiology, patho and clinical manifestations of Appendicitis Peritonitis Ulcerative Colitis Crohn s
Managing. Inflammatory Bowel Disease. Slide 1. Slide 2. Slide 3. Disclosures. Vijay Yajnik, MD., PhD 01/25/14. None relevant to this talk
 Slide 1 Managing Inflammatory Bowel Disease Vijay Yajnik, MD., PhD 01/25/14 Slide 2 Disclosures None relevant to this talk 2 Slide 3 Inflammatory Bowel Disease Topics Covered My friend called me and she
Slide 1 Managing Inflammatory Bowel Disease Vijay Yajnik, MD., PhD 01/25/14 Slide 2 Disclosures None relevant to this talk 2 Slide 3 Inflammatory Bowel Disease Topics Covered My friend called me and she
Beyond Anti TNFs: positioning of other biologics for Crohn s disease. Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center
 Beyond Anti TNFs: positioning of other biologics for Crohn s disease Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center Objectives: To define high and low risk patient and disease features
Beyond Anti TNFs: positioning of other biologics for Crohn s disease Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center Objectives: To define high and low risk patient and disease features
Case Report Successful Long-Term Use of Infliximab in Refractory Pouchitis in an Adolescent
 Gastroenterology Research and Practice Volume 2010, Article ID 860394, 4 pages doi:10.1155/2010/860394 Case Report Successful Long-Term Use of Infliximab in Refractory Pouchitis in an Adolescent Jessica
Gastroenterology Research and Practice Volume 2010, Article ID 860394, 4 pages doi:10.1155/2010/860394 Case Report Successful Long-Term Use of Infliximab in Refractory Pouchitis in an Adolescent Jessica
My Child Has Inflammatory Bowel Disease : Why? What now? What s next?
 My Child Has Inflammatory Bowel Disease : Why? What now? What s next? George M. Zacur, M.D., M.S. Clinical Assistant Professor Department of Pediatrics and Communicable Diseases Division of Gastroenterology
My Child Has Inflammatory Bowel Disease : Why? What now? What s next? George M. Zacur, M.D., M.S. Clinical Assistant Professor Department of Pediatrics and Communicable Diseases Division of Gastroenterology
Pathology and Diagnosis of Inflammatory Bowel Disease (IBD)
 Inflammatory Bowel Disease Pathology and Diagnosis of Inflammatory Bowel Disease (IBD) JMAJ 45(2): 45 54, 2002 Takashi SHIMOYAMA Director, Department of Gastroenterology, Hyogo College of Medicine Abstract:
Inflammatory Bowel Disease Pathology and Diagnosis of Inflammatory Bowel Disease (IBD) JMAJ 45(2): 45 54, 2002 Takashi SHIMOYAMA Director, Department of Gastroenterology, Hyogo College of Medicine Abstract:
Understanding Inflammatory Bowel Diseases (IBD):
 Understanding Inflammatory Bowel Diseases (IBD): What Every Patient Needs to Know William H Holderman, MD Digestive Health Specialists Tacoma, WA Today s Objectives Define IBD, its potential causes and
Understanding Inflammatory Bowel Diseases (IBD): What Every Patient Needs to Know William H Holderman, MD Digestive Health Specialists Tacoma, WA Today s Objectives Define IBD, its potential causes and
Inflammatory Bowel Disease
 Inflammatory Bowel Disease William Sonnenberg, MD Titusville, PA Disclosure Dr. William Sonnenberg has no conflict of interest, financial agreement, or working affiliation with any group or organization.
Inflammatory Bowel Disease William Sonnenberg, MD Titusville, PA Disclosure Dr. William Sonnenberg has no conflict of interest, financial agreement, or working affiliation with any group or organization.
Inflammatory Bowel Disease IBD
 Inflammatory Bowel Disease IBD An Introduction Inflammatory bowel disease is a chronic inflammatory disorder characterized by a protracted relapsing and remitting course, usually extending over years.
Inflammatory Bowel Disease IBD An Introduction Inflammatory bowel disease is a chronic inflammatory disorder characterized by a protracted relapsing and remitting course, usually extending over years.
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN
 UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Soura
 Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Sourasky Medical Center Tel Aviv, Israel IBD- clinical features
Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Sourasky Medical Center Tel Aviv, Israel IBD- clinical features
The Role of Ultrasound in the Assessment of Inflammatory Bowel Disease
 The Role of Ultrasound in the Assessment of Inflammatory Bowel Disease Dr. Richard A. Beable Consultant Gastrointestinal Radiologist Queen Alexandra Hospital Portsmouth Hospitals NHS Trust Topics for Discussion
The Role of Ultrasound in the Assessment of Inflammatory Bowel Disease Dr. Richard A. Beable Consultant Gastrointestinal Radiologist Queen Alexandra Hospital Portsmouth Hospitals NHS Trust Topics for Discussion
The ABCs of Inflammatory Bowel Disease. Jennifer Choi, M.D. Associate Director March 31, 2012
 The ABCs of Inflammatory Bowel Disease Jennifer Choi, M.D. Associate Director March 31, 2012 What Will This Talk Cover? What is IBD? What causes it? What are complications of it? How do I find out if I
The ABCs of Inflammatory Bowel Disease Jennifer Choi, M.D. Associate Director March 31, 2012 What Will This Talk Cover? What is IBD? What causes it? What are complications of it? How do I find out if I
CHRONIC DIARRHEA DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE THAN 4 WEEKS
 DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND. Fabrizio Parente
 NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
The London Gastroenterology Partnership CROHN S DISEASE
 CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
IBD. Crohn s. Outline. Ulcerative colitis versus Crohn s disease: is biopsy useful? UC vs. Crohn s? Is it easy? Biopsy settings 21/07/2017 IBD
 Outline Ulcerative colitis versus Crohn s disease: is biopsy useful? Roger Feakins Colorectal biopsies Ileal and upper GI biopsies Special situations New techniques Summary Inflammatory bowel disease (IBD)
Outline Ulcerative colitis versus Crohn s disease: is biopsy useful? Roger Feakins Colorectal biopsies Ileal and upper GI biopsies Special situations New techniques Summary Inflammatory bowel disease (IBD)
Treating Crohn s and Colitis in the ASC
 Treating Crohn s and Colitis in the ASC Kimberly M Persley, MD Texas Digestive Disease consultants TASC Meeting Outline IBD 101 Diagnosis Treatment Burden of Disease Role of ASC Inflammatory Bowel Disease
Treating Crohn s and Colitis in the ASC Kimberly M Persley, MD Texas Digestive Disease consultants TASC Meeting Outline IBD 101 Diagnosis Treatment Burden of Disease Role of ASC Inflammatory Bowel Disease
Implementation of disease and safety predictors during disease management in UC
 Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Crohn s Disease. How does Crohn s disease affect the intestinal tract?
 Crohn s Disease Crohn s disease is one of the two main forms of inflammatory bowel disease (IBD). The second main form of inflammatory bowel disease is ulcerative colitis. Crohn s disease causes inflammation
Crohn s Disease Crohn s disease is one of the two main forms of inflammatory bowel disease (IBD). The second main form of inflammatory bowel disease is ulcerative colitis. Crohn s disease causes inflammation
INFLAMMATORY BOWEL DISEASE (IBD): CROHN S DISEASE
 INFLAMMATORY BOWEL DISEASE (IBD): CROHN S DISEASE Symptoms The symptoms of Crohn s disease can vary from person to person, based on where the disease is in the body and how bad the inflammation is. The
INFLAMMATORY BOWEL DISEASE (IBD): CROHN S DISEASE Symptoms The symptoms of Crohn s disease can vary from person to person, based on where the disease is in the body and how bad the inflammation is. The
Inflammatory Bowel Disease
 Inflammatory Bowel Disease Ali J. Olyaei, PharmD, BCPS Associate Professor of Medicine Director, Clinical Research Nephrology and Hypertension Associate Professor of Pharmacology School of Nursing Oregon
Inflammatory Bowel Disease Ali J. Olyaei, PharmD, BCPS Associate Professor of Medicine Director, Clinical Research Nephrology and Hypertension Associate Professor of Pharmacology School of Nursing Oregon
What is Inflammatory Bowel Disease (IBD)?
 INFLAMMATORY BOWEL DISEASE (IBD) What is Inflammatory Bowel Disease (IBD)? Inflammatory bowel disease, or IBD, is when there is inflammation, or swelling, in the gastrointestinal (GI) tract and a lifelong
INFLAMMATORY BOWEL DISEASE (IBD) What is Inflammatory Bowel Disease (IBD)? Inflammatory bowel disease, or IBD, is when there is inflammation, or swelling, in the gastrointestinal (GI) tract and a lifelong
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels.
 Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Management of the Hospitalized IBD Patient. Drew DuPont MD
 Management of the Hospitalized IBD Patient Drew DuPont MD Ulcerative Colitis: Indications for Admission Severe ulcerative colitis Frequent loose bloody stools ( 6 per day) Severe cramps Systemic toxicity:
Management of the Hospitalized IBD Patient Drew DuPont MD Ulcerative Colitis: Indications for Admission Severe ulcerative colitis Frequent loose bloody stools ( 6 per day) Severe cramps Systemic toxicity:
Garrick Brown, MD. Digestive Health Specialists Tacoma Gig Harbor
 Garrick Brown, MD Digestive Health Specialists Tacoma Gig Harbor Today s Objectives Define IBD, its potential causes and diagnosis Discuss management and treatment Discuss complementary and alternative
Garrick Brown, MD Digestive Health Specialists Tacoma Gig Harbor Today s Objectives Define IBD, its potential causes and diagnosis Discuss management and treatment Discuss complementary and alternative
8/29/2016 DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW. LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES
 DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES Define Diverticular Disease Discuss Epidemiology and Pathophysiology of Diverticular disease
DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES Define Diverticular Disease Discuss Epidemiology and Pathophysiology of Diverticular disease
12 Blueprints Q&A Step 2 Surgery
 12 Blueprints Q&A Step 2 Surgery 34. A 40-year-old female has been referred to you for a recent ER and hospital admission, from which she was given a diagnosis of acute diverticulitis. Treatment at that
12 Blueprints Q&A Step 2 Surgery 34. A 40-year-old female has been referred to you for a recent ER and hospital admission, from which she was given a diagnosis of acute diverticulitis. Treatment at that
The Road to Remission
 The Road to Remission Understanding, Treating and Living with Inflammatory Bowel Disease IBDCenterOrlando.com As many as 1.5 million Americans currently suffer from inflammatory bowel disease (IBD), and
The Road to Remission Understanding, Treating and Living with Inflammatory Bowel Disease IBDCenterOrlando.com As many as 1.5 million Americans currently suffer from inflammatory bowel disease (IBD), and
Inflammatory Bowel Disease RTC 10/30/09
 Inflammatory Bowel Disease RTC 10/30/09 October 30, 1735 2nd President of the United States, John Adams, was born. Prior to becoming president he served 2 terms as Vice President under George Washington.
Inflammatory Bowel Disease RTC 10/30/09 October 30, 1735 2nd President of the United States, John Adams, was born. Prior to becoming president he served 2 terms as Vice President under George Washington.
Crohn s Disease. Questions & Answers
 Crohn s Disease Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard - 0141 810 3151 Ph.
Crohn s Disease Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard - 0141 810 3151 Ph.
What is Crohn's disease?
 What is Crohn's disease? Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area
What is Crohn's disease? Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area
ABC of Colorectal Diseases
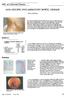 ABC of Colorectal Diseases NON-SPECIFIC INFLAMMATORY BOWEL DISEASE S Pettit, M H Irving Non-specific inflammatory bowel diseases are those for which there is no discernible aetiological agent. The two
ABC of Colorectal Diseases NON-SPECIFIC INFLAMMATORY BOWEL DISEASE S Pettit, M H Irving Non-specific inflammatory bowel diseases are those for which there is no discernible aetiological agent. The two
INFLAMMATORY BOWEL DISEASE
 1. Medical Condition INFLAMMATORY BOWEL DISEASE (IBD) specifically includes Crohn s disease (CD) and ulcerative colitis (UC) but also includes IBD unclassified (IBDu), seen in about 10% of cases. These
1. Medical Condition INFLAMMATORY BOWEL DISEASE (IBD) specifically includes Crohn s disease (CD) and ulcerative colitis (UC) but also includes IBD unclassified (IBDu), seen in about 10% of cases. These
Top 10 Things you need to know about IBD. Suresh Pola, MD Kaiser San Diego
 Top 10 Things you need to know about IBD Suresh Pola, MD Kaiser San Diego Top 10 Things to Know: IBD What you can eat How to treat the pain Not all diarrhea is a flare Ways to reduce your risk of getting
Top 10 Things you need to know about IBD Suresh Pola, MD Kaiser San Diego Top 10 Things to Know: IBD What you can eat How to treat the pain Not all diarrhea is a flare Ways to reduce your risk of getting
Surgery in Inflammatory Bowel Disease. Rajesh Gupta MS, MCh Surgical Gastroenterology Division Dept of General Surgery PGIMER, Chandigarh
 Surgery in Inflammatory Bowel Disease Rajesh Gupta MS, MCh Surgical Gastroenterology Division Dept of General Surgery PGIMER, Chandigarh 1 Ulcerative colitis (UC) Ulcerative colitis (UC) characterized
Surgery in Inflammatory Bowel Disease Rajesh Gupta MS, MCh Surgical Gastroenterology Division Dept of General Surgery PGIMER, Chandigarh 1 Ulcerative colitis (UC) Ulcerative colitis (UC) characterized
Title: Author: Journal:
 IMPORTANT COPYRIGHT NOTICE: This electronic article is provided to you by courtesy of Ferring Pharmaceuticals. The document is provided for personal usage only. Further reproduction and/or distribution
IMPORTANT COPYRIGHT NOTICE: This electronic article is provided to you by courtesy of Ferring Pharmaceuticals. The document is provided for personal usage only. Further reproduction and/or distribution
INVESTIGATIONS OF GASTROINTESTINAL DISEAS
 INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
Diarrhoea for the Acute Physician
 Diarrhoea for the Acute Physician STEPHEN INNS GASTROENTEROLOGIST AND PHYSICIAN HUTT VALLEY DHB August 2013 Outline Case History 1 Initial assessment of acute diarrhoea Management of fulminant UC Management
Diarrhoea for the Acute Physician STEPHEN INNS GASTROENTEROLOGIST AND PHYSICIAN HUTT VALLEY DHB August 2013 Outline Case History 1 Initial assessment of acute diarrhoea Management of fulminant UC Management
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK. Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center
 ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center 1 ST ADMISSION - 2015 38 y/o female Abdominal pain, diarrhea - intermittent
ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center 1 ST ADMISSION - 2015 38 y/o female Abdominal pain, diarrhea - intermittent
Perianal Fistula of Crohn s Disease
 Case 3 Perianal Fistula of Crohn s Disease A 16 year-old boy referred by surgeon due to perianal fistula since 6mo ago CC=perianal pain History of intermittent non-bloody diarrhea and mild abdominal pain
Case 3 Perianal Fistula of Crohn s Disease A 16 year-old boy referred by surgeon due to perianal fistula since 6mo ago CC=perianal pain History of intermittent non-bloody diarrhea and mild abdominal pain
Dr David Epstein Vincent Pallotti Hospital and University of Cape Town
 Inflammatory Bowel Disease Management in South Africa in 2016 Pharmaceutical Care Management Association Dr David Epstein Vincent Pallotti Hospital and University of Cape Town Inflammatory Bowel Disease
Inflammatory Bowel Disease Management in South Africa in 2016 Pharmaceutical Care Management Association Dr David Epstein Vincent Pallotti Hospital and University of Cape Town Inflammatory Bowel Disease
Predicting the natural history of IBD. Séverine Vermeire, MD, PhD Department of Gastroenterology University Hospital Leuven Belgium
 Predicting the natural history of IBD Séverine Vermeire, MD, PhD Department of Gastroenterology University Hospital Leuven Belgium Patient 1 Patient 2 Age 22 Frequent cramps and diarrhea for 6 months Weight
Predicting the natural history of IBD Séverine Vermeire, MD, PhD Department of Gastroenterology University Hospital Leuven Belgium Patient 1 Patient 2 Age 22 Frequent cramps and diarrhea for 6 months Weight
Mucosal Healing in Crohn s Disease. Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium
 Mucosal Healing in Crohn s Disease Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium Mucosal Lesions in CD: General Features CD can affect the entire GI tract
Mucosal Healing in Crohn s Disease Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium Mucosal Lesions in CD: General Features CD can affect the entire GI tract
Medical therapies and IBD
 Medical therapies and IBD Although there is no cure for IBD, there are many treatment options available. There is no standard treatment for IBD that is effective in all situations or for all patients,
Medical therapies and IBD Although there is no cure for IBD, there are many treatment options available. There is no standard treatment for IBD that is effective in all situations or for all patients,
study was undertaken to assess the epidemiology, course and outcome of UC patients attending a hospital in Jordan.
 Ulcerative colitis (UC) is a relatively uncommon, chronic, recurrent inflammatory disease of the colon or rectal mucosa [1]. Often a lifelong illness, the condition can have a profound emotional and social
Ulcerative colitis (UC) is a relatively uncommon, chronic, recurrent inflammatory disease of the colon or rectal mucosa [1]. Often a lifelong illness, the condition can have a profound emotional and social
How to manage your IBD patient: Tips for diagnosis and care
 How to manage your patient: Tips for diagnosis and care Oriana M. Damas, M.D. Assistant Prof Clinical Medicine Division of Gastroenterology No relevant disclosures Case Presentation: A.R. 32 yo woman with
How to manage your patient: Tips for diagnosis and care Oriana M. Damas, M.D. Assistant Prof Clinical Medicine Division of Gastroenterology No relevant disclosures Case Presentation: A.R. 32 yo woman with
VOLUME - X ISSUE - LX NOV / DEC 2013
 VOLUME - X ISSUE - LX NOV / DEC 2013 1 2 9 10 11 12 Editorial Disease Diagnosis Interpretation Bouquet Trouble Shooting Tulip News In medicine, inflammatory bowel disease (IBD) is a group of inflammatory
VOLUME - X ISSUE - LX NOV / DEC 2013 1 2 9 10 11 12 Editorial Disease Diagnosis Interpretation Bouquet Trouble Shooting Tulip News In medicine, inflammatory bowel disease (IBD) is a group of inflammatory
Diarrhea may be: Acute (short-term, usually lasting several days), which is usually related to bacterial or viral infections.
 Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
2015 복영증례 51/M C.C. Past Hx: DM, HTN (1998), Lab: WBC (11500/ μl ), CRP (0.71 mg/dl) 순천향서울병원황지영, 홍성숙 APCT (HAD #1) APCT (HAD#1) APCT (HAD #15)
 Case 1 2015 복영증례 순천향서울병원황지영, 홍성숙 51/M C.C Abdominal pain and chilling (1 week ago) Diarrhea (a month ago) Past Hx: DM, HTN (1998), Alcoholic liver disease (2008) Lab: WBC (11500/ μl ), CRP (0.71 mg/dl)
Case 1 2015 복영증례 순천향서울병원황지영, 홍성숙 51/M C.C Abdominal pain and chilling (1 week ago) Diarrhea (a month ago) Past Hx: DM, HTN (1998), Alcoholic liver disease (2008) Lab: WBC (11500/ μl ), CRP (0.71 mg/dl)
F A M N O P R S ! D !
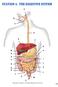 A B C D E F A M N O P Q G H I J R S T U V 595 W http://www.encognitive.com/images/digestive-system-2.jpg K L M A N B C O P D E F G D Q R H S I J K http://apbrwww5.apsu.edu/thompsonj/anatomy%20&%20physiology/2020/2020%20exam%20reviews/exam%203/colon%20diagram.jpgd
A B C D E F A M N O P Q G H I J R S T U V 595 W http://www.encognitive.com/images/digestive-system-2.jpg K L M A N B C O P D E F G D Q R H S I J K http://apbrwww5.apsu.edu/thompsonj/anatomy%20&%20physiology/2020/2020%20exam%20reviews/exam%203/colon%20diagram.jpgd
A Case of Inflammatory Bowel Disease
 A Case of Inflammatory Bowel Disease Dr Barrie Rathbone www.le.ac.uk 26 year old Polish woman Admitted as emergency under surgeons RUQ and RIF pain Abdominal pain had occurred intermittently for a few
A Case of Inflammatory Bowel Disease Dr Barrie Rathbone www.le.ac.uk 26 year old Polish woman Admitted as emergency under surgeons RUQ and RIF pain Abdominal pain had occurred intermittently for a few
Anne Griffiths MD, FRCPC. SickKids Hospital, University of Toronto. Buenos Aires, August 16, 2014
 Management and Medical Therapies for Crohn disease: strategies to enhance mucosal healing Anne Griffiths MD, FRCPC SickKids Hospital, University of Toronto Buenos Aires, August 16, 2014 New onset Crohn
Management and Medical Therapies for Crohn disease: strategies to enhance mucosal healing Anne Griffiths MD, FRCPC SickKids Hospital, University of Toronto Buenos Aires, August 16, 2014 New onset Crohn
Lower GI bleeding. Aliu Sanni, MD Long Island College Hospital 17 th June, 2010
 Lower GI bleeding Aliu Sanni, MD Long Island College Hospital 17 th June, 2010 Case Presentation CC: Hematochezia HPI: 28yr old male presents with 1 day episode of bloody stools. Denies any abdominal pain.
Lower GI bleeding Aliu Sanni, MD Long Island College Hospital 17 th June, 2010 Case Presentation CC: Hematochezia HPI: 28yr old male presents with 1 day episode of bloody stools. Denies any abdominal pain.
Pouchitis and Cuffitis A bloody mess. Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board
 Pouchitis and Cuffitis A bloody mess Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board Ileal-pouch anal anastomosis https://www.pennmedicine.org/for-health-care-professionals/for-physicians/physician-education-and-resources/clinicalbriefings/2018/february/total-proctocolectomy-with-jpouch-reconstruction-for-ulcerative-colitis
Pouchitis and Cuffitis A bloody mess Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board Ileal-pouch anal anastomosis https://www.pennmedicine.org/for-health-care-professionals/for-physicians/physician-education-and-resources/clinicalbriefings/2018/february/total-proctocolectomy-with-jpouch-reconstruction-for-ulcerative-colitis
FY 2016 MCRCEDP Approved ICD-10 Code List
 Approved List C18.0 Malignant neoplasm of cecum C18.1 Malignant neoplasm of appendix C18.2 Malignant neoplasm of ascending colon C18.3 Malignant neoplasm of hepatic flexure C18.4 Malignant neoplasm of
Approved List C18.0 Malignant neoplasm of cecum C18.1 Malignant neoplasm of appendix C18.2 Malignant neoplasm of ascending colon C18.3 Malignant neoplasm of hepatic flexure C18.4 Malignant neoplasm of
Inflammatory bowel disease. Kawa Obeid, PhD
 Inflammatory bowel disease Kawa Obeid, PhD 63 Introduction Inflammatory bowel disease (IBD) can be divided into two chronic inflammatory disorders of the gastro- intestinal tract, namely Crohn's disease
Inflammatory bowel disease Kawa Obeid, PhD 63 Introduction Inflammatory bowel disease (IBD) can be divided into two chronic inflammatory disorders of the gastro- intestinal tract, namely Crohn's disease
Deep Enteroscopy Methods to Diagnose Small Bowel IBD
 Deep Enteroscopy Methods to Diagnose Small Bowel IBD Name: Institution: Peter Draganov University of Florida, Gainesville, FL Overview Types of enteroscopy Enteroscopy equipment Enetoscopy do and don'ts
Deep Enteroscopy Methods to Diagnose Small Bowel IBD Name: Institution: Peter Draganov University of Florida, Gainesville, FL Overview Types of enteroscopy Enteroscopy equipment Enetoscopy do and don'ts
The National Association of Crohn s and Colitis of Trinidad and Tobago CROHN S DISEASE AND ULCERATIVE COLITIS GENERAL PATIENT INFORMATION
 The National Association of Crohn s and Colitis of Trinidad and Tobago CROHN S DISEASE AND ULCERATIVE COLITIS GENERAL PATIENT INFORMATION You are reading this pamphlet because you or someone you known
The National Association of Crohn s and Colitis of Trinidad and Tobago CROHN S DISEASE AND ULCERATIVE COLITIS GENERAL PATIENT INFORMATION You are reading this pamphlet because you or someone you known
