AJH 1998;11: by the American Journal of Hypertension, Ltd /98/$19.00
|
|
|
- Lambert McKinney
- 5 years ago
- Views:
Transcription
1 AJH 1998;11:8 13 Acute Effects of Intravenous Sodium Chloride Load on Calcium Metabolism and on Parathyroid Function in Patients With Primary Aldosteronism Compared With Subjects With Essential Hypertension Ermanno Rossi, Franco Perazzoli, Aurelio Negro, Carlo Sani, Simona Davoli, Claudio Dotti, Maria Cristina Casoli, and Giuseppe Regolisti To elucidate the mechanisms involved in increased parathyroid function in primary aldosteronism (PA), we evaluated the effects of an intravenous NaCl load on Ca metabolism and plasma level of intact parathyroid hormone (PTH) in patients with PA compared with that in patients with essential hypertension (EH). Sixteen PA patients and 16 EH patients who were well matched for age, gender, body mass index, renal function, and systolic (SBP) and diastolic blood pressure (DBP) were examined. In each subject, after 6 days of a controlled intake of Na, K, and Ca, isotonic saline was infused at a rate of 500 ml/h for 4 h. At baseline, in spite of similar BP values and urinary Na excretion (U Na V), urinary excretion of Ca (U Ca V) and PTH were higher in the PA group than in the EH group. In both groups, the NaCl load caused a decrease of serum ionized Ca (Ca 2 ) and an increase in PTH, U Na V, and U Ca V. However, these changes were significantly greater in the PA group. The increased baseline U Ca V in PA could be due to reduced reabsorption of sodium in aldosterone insensitive tubular sites, as a result of the escape phenomenon. The increased U Ca V may explain the higher basal PTH in PA patients, which is needed for maintaining a normal Ca 2. The greater changes in the Ca 2 /PTH profile elicited by the saline load in PA patients are apparently due to a higher calciuretic response following a more exaggerated natriuresis in PA. Am J Hypertens 1998;11: American Journal of Hypertension, Ltd. KEY WORDS: Intact parathyroid hormone, serum ionized calcium, urinary calcium excretion, primary aldosteronism, essential hypertension. Received July 22, Accepted July 15, From the Fourth Department of Internal Medicine, (ER, FP, AN, CS, SD, MCC, GR), and Laboratory of Endocrinology, S. Maria Nuova Hospital, Reggio Emilia, Italy. Address correspondence and reprint requests to Dr Ermanno Rossi, IV Divisione di Medicina Interna, Ospedale S. Maria Nuova, Padiglione L. Spallanzani, Viale Umberto I, N. 50, Reggio Emilia, Italy by the American Journal of Hypertension, Ltd /98/$19.00 Published by Elsevier Science, Inc. PII S (97)00366-X
2 AJH JANUARY 1998 VOL. 11, NO. 1, PART 1 NaCl, Ca, AND PTH IN PRIMARY ALDOSTERONISM 9 Alterations of calcium metabolism and parathyroid function, namely reduced concentration of serum ionized calcium (Ca 2 ), increased urinary calcium excretion, and elevated circulating level of parathyroid hormone, have been reported in both essential hypertension (EH) 1 3 and primary aldosteronism (PA). 4,5 In a previous study, we observed that in both patients with PA and subjects with EH, Ca 2 is lower than in normotensive controls. However, only in patients with PA intact serum PTH 1 84 (PTH) was higher than in normotensive subjects. Furthermore, in the former group, an increase in Ca 2 and a decrease in PTH were associated with both spironolactone administration and surgical treatment. 5 To elucidate better the mechanisms involved in the altered Ca 2 /PTH profile in PA, we evaluated the acute effects of an intravenous NaCl load on calcium metabolism and PTH in patients with PA compared to patients with EH, all subjects having being submitted to the same intake of Na, K, and Ca in the week preceding the NaCl load. SUBJECTS AND METHODS Sixteen patients with PA, 31 to 71 years of age, and 16 patients with EH, aged 33 to 69 years, were included in the study. The two groups were well matched for age, sex, body mass index (BMI), renal function, systolic (SBP) and diastolic blood pressure (DBP). PA was defined by the presence of each of the following findings: plasma aldosterone (ng/dl)/renin activity (ng/ ml/h) ratio 30 in the sitting position on three consecutive occasions; plasma renin activity (PRA) 1 ng/ml/h in the upright posture for 2 h, after 5 days of a sodium restricted diet; plasma aldosterone 7.5 ng/dl at the end of an intravenous load of 2Lof isotonic saline at an infusion rate of 500 ml/h; and upright plasma aldosterone (ALDO) 5 ng/dl after 5 days of fludrocortisone acetate administration (0.1 mg every 6 hours). Glucocorticoid-suppressible aldosteronism was excluded by a dexamethasone test. Adrenal lesions were assessed by high-resolution thin section computer tomography and dexamethasone suppressed scintigraphy with 131 I-6- -iodomethylnorcholesterol. Unilateral adrenal lesions were diagnosed in nine patients. Adrenocortical adenomas were found in the seven patients so far submitted to unilateral adrenalectomy. Idiopathic aldosteronism was presumed on the basis of the absence of a unilateral lesion in both computer tomographic and scintigraphic scanning in the other seven patients. EH was established after exclusion of secondary hypertension on the basis of appropriate clinical and laboratory evaluation. Antihypertensive drugs were discontinued 4 weeks before the beginning of the study. No subject had previously been treated with diuretics, spironolactone, or other potassium sparing drugs. For the purpose of the matching, the individual SBP and DBP were taken as the average of six office measurements in the seated position on three different visits in the 2 weeks before the beginning of the study. In the same period, endogenous creatinine clearance was determined in all subjects. All PA patients had DBP 90 mm Hg, and a DBP 90 mm Hg was used for the selection of patients with essential hypertension. All subjects were placed on a diet containing 110 mmol/day of sodium, 70 mmol/day of potassium, and 650 mg/day of calcium for 6 days. On the seventh day, following an overnight fast, isotonic saline was infused intravenously at a rate of 500 ml/h for 4 h from 8 am to noon. Four-hour urine samples were collected from 4 am to 8 am and from 8 am to noon. Venous blood samples were collected and blood pressures were measured immediately before and at the end of the saline load. Individual blood pressures were considered the mean of six recordings 2 minutes apart. The two urine samples were used to measure urinary output, creatinine, sodium, potassium, and calcium. The two blood samples were used to measure serum sodium, potassium, Ca 2, creatinine, plasma renin activity (PRA), plasma aldosterone (ALDO) and parathyroid hormone (PTH). For each of the two periods creatinine clearance and fractional excretion of sodium (Na clearance/creatinine clearance ratio 100) were calculated. All subjects gave their informed consent; the protocol was approved by the local ethical committee. Blood pressure was measured with a standard mercury sphygmomanometer, using Korotkoff phase V for diastolic blood pressure. Intact serum PTH (PTH 1 84 ) was measured using commercially available radiometric assay kits (Diagnostic Products Corporation, Los Angeles, CA). PRA was evaluated by radioimmunoassay (Sorin Biomedica, Saluggia, Italy) through quantitative determination of angiotensin I. Plasma ALDO was also measured by radioimmunoassay (Diagnostic System Laboratories, Webster, TX). Serum Ca 2 was measured with an ion selective electrode, with values adjusted to ph 7.4. Statistics Statistical analysis was primarily based on two-way analysis of variance (ANOVA) with repeated measures, with group (PA and EH) and time (before and after saline load) as main factors. If ANOVA yielded a significant result, post hoc comparisons were carried out with paired or unpaired Student s t test as appropriate. Percent changes in a given variable after saline load as compared with baseline were compared by unpaired t test. Data are shown as means SEM. A P.05 was considered statistically significant.
3 10 ROSSI ET AL AJH JANUARY 1998 VOL. 11, NO. 1, PART 1 TABLE 1. BLOOD PRESSURE AND LABORATORY VALUES BEFORE (BASELINE) AND AFTER SALINE LOAD Baseline After Saline Load ANOVA Table PA EH PA EH Group Time G T ALDO, ng/ml # F 1, P NS PRA, ng/ml/h # * *# F 1, P Ca 2, mmol/l # F 1, P PTH, pg/ml * F 1, P U Ca V, mg/h # F 1, P U Na V, mmol/h ** F 1, P U K V, mmol/h F 1, P NS.0001 NS FENa, % ** F 1, P V, ml/h F 1, P NS.0001 NS CrC1, ml/min/1.72 m * F 1, P NS.0001 NS SBP, mm Hg F 1, P NS NS NS DBP, mm Hg F 1, P NS NS NS PA, primary aldosteronism; EH, essential hypertension; ALDO, plasma aldosterone; PRA, plasma renin activity; Ca 2, serum ionized calcium; PTH, parathyroid hormone; U Ca V, U Na V, U K V, urinary calcium, sodium, and potassium excretion rate; FENa, fractional excretion of sodium; V, urinary flow rate; CrC1, creatinine clearance; SBP, systolic blood pressure; DBP, diastolic blood pressure. *P.05; P.01; P.001 v baseline by paired t test; ** P.05; #P.01; P.001 v PA by unpaired t test. RESULTS Patients with PA and EH were similar in age ( v years), gender distribution (M/F 8/8 v 8/8), BMI ( v kg/m 2 ), creatinine clearance, SBP, and DBP (Table 1). Serum potassium was lower in the PA group ( v mmol/l, P.05). Hemodynamic and laboratory data recorded before and after saline infusion are summarized in Table 1. In the 4 h baseline period, SBP, DBP, urinary output (V), urinary sodium (U Na V), and potassium (U K V) excretion rates, creatinine clearance (CrC1), fractional excretion of sodium (FENa), and serum Ca 2 did not differ between the two groups. However, at baseline, urinary excretion of calcium and PTH were higher in the PA than in the EH group. The saline load did not affect blood pressures. In both groups creatinine clearance was only slightly though significantly increased, whereas urine output markedly rose. The saline load elicited a significant increase in urinary calcium excretion rate in both groups as compared with baseline; however, this increase was proportionally greater in the patients with PA (Figure 1, panel A). Accordingly, serum Ca 2 decreased more and PTH secretion was more actively stimulated after the saline load in patients with PA as compared with those with EH (Figure 1, panels B and C). Urinary sodium excretion rate (Table 1) and FENa (Figure 1, panel D) were also more strongly enhanced in patients with PA, whereas a parallel increase in the urinary excretion of potassium was observed in the two groups. DISCUSSION Our study demonstrates firstly that both baseline urinary excretion of calcium and PTH are higher in primary aldosteronism than in essential hypertension, in the face of equal dietary intakes of calcium and sodium, and similar excretion rates of sodium (Table 1). The higher baseline U Ca V is consistent with the increase of U Ca V observed in both animals 6 and humans 7 after long-term mineralocorticoid administration, as well as with the higher U Ca V reported in patients with PA compared with that in normotensive control subjects. 8 However, this increase in urinary
4 AJH JANUARY 1998 VOL. 11, NO. 1, PART 1 NaCl, Ca, AND PTH IN PRIMARY ALDOSTERONISM 11 FIGURE 1. Percent changes in urinary calcium excretion rate (U Ca V, panel A), serum ionized calcium (Ca 2, panel B), parathyroid hormone (PTH, panel C), and fractional excretion of sodium (FENa, panel D) after the saline load as compared with baseline. EH, essential hypertension; PA, primary aldosteronism. *P.05; **P.01 by unpaired t test. calcium excretion associated with mineralocorticoid excess does not seem due to direct effects of aldosterone. Indeed, the increase of U Ca V requires volume expansion and the consequent escape phenomenon, as neither animals submitted to chronic mineralcorticoid administration 6 nor humans with PA 8 exhibit higher calcium excretion rates when sodium intake is substantially restricted. The increased U Ca V in PA
5 12 ROSSI ET AL AJH JANUARY 1998 VOL. 11, NO. 1, PART 1 could be due to reduced reabsorption of calcium following a reduced reabsorption of sodium in aldosterone-insensitive proximal tubular sites, where sodium handling is closely connected with that of calcium. In this case, the increased calcium excretion would be the result of the escape phenomenon elicited by plasma volume expansion. Some evidence suggests, however, that other possible mechanisms may be involved in mediating the increased calcium excretion. Micropuncture studies in escaped hypertensive saline expanded rats receiving DOCA, compared with hypertensive saline expanded control rats, have indicated a reduced calcium reabsorption in sites beyond the distal late tubule. 9 Moreover, clearance studies in the same animal model have demonstrated that either parathyroidectomy or parathyroid hormone administration following parathyroidectomy fail to alter calcium excretion, suggesting the absence of the anticalciuric effect of parathyroid hormone in the escape phase of mineralcorticoid excess. 9 The inhibition of calcium reabsorption in sites beyond the distal tubule could also follow the inhibition of sodium reabsorption on collecting ducts by atrial natriuretic peptide (ANP). 10 Indeed, the rise in plasma ANP associated with the escape phenomenon in patients with PA is accompanied by an increase in urinary calcium output. 11 Even the lower serum potassium level in PA patients compared to EH patients could contribute to the altered calcium metabolism in PA. In fact, hypokalemia following potassium deprivation in subjects with EH increases both urinary calcium excretion and plasma PTH levels. 12 On the other hand, these effects could be partly secondary to sodium retention and extracellular volume expansion following potassium depletion. Moreover, renal cysts in the collecting ducts and interstitial scarring, reported in PA patients and attributed to chronic hypokalemia, 13 could also adversely affect the tubular reabsorption of calcium. The increased calcium excretion, with the consequent trend towards a decrease of serum Ca 2, may explain the higher basal PTH level in PA patients, needed for restoring and maintaining normal or low normal serum Ca 2. In both PA and EH patients, intravenous saline load caused an increase in serum PTH levels and urinary calcium excretion rate, together with a reduction of serum Ca 2. However, the changes of U Ca V, serum Ca 2 and PTH were greater in PA patients (Figure 1). These changes were associated with a greater increase in sodium excretion in response to the saline load in PA patients, which is consistent with the more exaggerated natriuretic response to an acute volume expansion reported in PA compared with that in EH. 14 Considering the well known dependence of renal calcium reabsorption on sodium reabsorption, the calciuretic response to the intravenous saline load observed in both groups of patients may be the result of sodium reabsorption inhibition elicited by the acute intravascular volume expansion resulting from the saline load, whereas the greater calciuretic response in PA patients could follow a more exaggerated inhibition of sodium reabsorption in PA. In these patients, an amplification of the same factors responsible for the escape phenomenon and the higher calcium excretion in conditions of steady sodium balance is conceivable; in particular, patients with PA exhibit a greater increase in plasma ANP than patients with EH in response to acute saline load. 14 The combination of increased calcium excretion and hemodilution resulting from the saline infusion seems to explain the reduction of serum Ca 2 in both groups of patients. However, the greater decrease of serum Ca 2 in PA apparently depends exclusively on the higher calcium excretion. Indeed, in PA patients the extracellular volume increase following the saline load seems more attenuated than in EH patients, as indicated by the higher increase in sodium excretion. Finally, the reduction in serum Ca 2 explains the appropriate increase in PTH levels following the saline load in both groups of patients, the higher levels observed in PA being dependent on the lower serum Ca 2. Similar but less pronounced alterations of calcium metabolism have been reported in patients with lowrenin EH as compared with normotensive subjects and patients with normal and high renin EH. 2,3 Even the increase in calcium excretion following an intravenous salt load is greater in patients with NaCl sensitive and low renin EH than in subjects with NaCl resistant EH. 15 Our results in PA patients indirectly support the role of extracellular volume expansion in the altered calcium metabolism reported in low renin or NaCl sensitive EH, as PA represents a prototype of volume dependent hypertension. In conclusion, our results indicate an altered calcium metabolism and enhanced parathyroid function in patients with PA compared with that in patients with EH. These alterations seem to be strictly dependent on the alterations of sodium metabolism and extracellular volume, and could be mediated by the escape phenomenon and by the exaggerated natriuresis in response to an acute saline load. REFERENCES 1. McCarron DA, Pingree PA, Rubin RJ, et al: Enhanced parathyroid function in essential hypertension: a homeostatic response to a urinary calcium leak. Hypertension 1980;2: Resnick LM, Laragh JH, Sealey JE, et al: Divalent cations in essential hypertension: relations between serum ionized calcium, magnesium, and plasma renin activity. N Engl J Med 1983;309:
6 AJH JANUARY 1998 VOL. 11, NO. 1, PART 1 NaCl, Ca, AND PTH IN PRIMARY ALDOSTERONISM Resnick LM, Muller FB, Laragh JH: Calcium regulating hormones in essential hypertension: relation to plasma renin activity and sodium metabolism. Ann Intern Med 1986;105: Resnick LM, Laragh JH: Calcium metabolism and parathyroid function in primary aldosteronism. Am J Med 1985;78: Rossi E, Sani C, Perazzoli F, et al: Alterations of calcium metabolism and of parathyroid function in primary aldosteronism, and their reversal by spironolactone or by surgical removal of aldosterone-producing adenomas. Am J Hypertens 1995;8: Suki WN, Schwettmann RS, Rector FC, et al: Effect of chronic mineralcorticoid administration on calcium excretion in the rat. Am J Physiol 1968;215: Cappuccio FP, Markandu ND, Mac Gregor, GA: Renal handling of calcium and phosphate during mineralcorticoid administration in normal subjects. Nephron 1988;48: Rastegar A, Agus Z, Connor TB, et al: Renal handling of calcium and phosphate during mineralcorticoid escape in man. Kidney Int 1972;2: Gehr MK, Goldberg M: Hypercalciuria of mineralcorticoid escape: clearance and micropuncture studies in the rat. Am J Physiol 1986;251: Zeidel ML: Hormonal regulation of inner medullary collecting duct sodium transport. Am J Physiol 1993; 265:F159 F Nakamura T, Ichikawa S, Sakamaki T, et al: Role of atrial natriuretic peptide in mineralcorticoid escape phenomenon in patients with primary aldosteronism. Proc Exp Biol Med 1987;185: Krishna GC, Kapoor SC: Potassium depletion exacerbates essential hypertension. Ann Intern Med 1991;115: Torres VE, Young WFJ, Offord KP, et al: Association of hypokalemia, aldosteronism and renal cysts. New Engl J Med 1990;322: Kawabe H, Furukawa T, Saito I, et al: Importance of atrial natriuretic hormone in an exaggerated natriuresis during acute sodium load in primary aldosteronism. Acta Endocrinol 1992;126: Galletti F, Ferrara I, Stinga F, et al: Effect of intravenous sodium chloride on renal sodium and calcium handling in hypertensive patients with different sensitivities to sodium chloride. J Hypertens 1993;11(suppl 5):
Role of Minerals in Hypertension
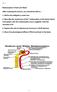
 Role of Minerals in Hypertension Lecture objectives By the end of the lecture students will be able to Define primary and secondary hypertention and their risk factors. Relate role of minerals with hypertention.
Role of Minerals in Hypertension Lecture objectives By the end of the lecture students will be able to Define primary and secondary hypertention and their risk factors. Relate role of minerals with hypertention.
Patterns of Sodium Excretion During Sympathetic Nervous System Arousal. Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S.
 1156 Patterns of Sodium Excretion During Sympathetic Nervous System Arousal Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S. Alpert The purpose of this study was to examine Na + handling and regulation
1156 Patterns of Sodium Excretion During Sympathetic Nervous System Arousal Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S. Alpert The purpose of this study was to examine Na + handling and regulation
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Hyperaldosteronism: Conn's Syndrome
 RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
H 2 O, Electrolytes and Acid-Base Balance
 H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
H 2 O, Electrolytes and Acid-Base Balance Body Fluids Intracellular Fluid Compartment All fluid inside the cells 40% of body weight Extracellular Fluid Compartment All fluid outside of cells 20% of body
Endocrine. Endocrine as it relates to the kidney. Sarah Elfering, MD University of Minnesota
 Endocrine Sarah Elfering, MD University of Minnesota Endocrine as it relates to the kidney Parathyroid gland Vitamin D Endocrine causes of HTN Adrenal adenoma PTH Bone Kidney Intestine 1, 25 OH Vitamin
Endocrine Sarah Elfering, MD University of Minnesota Endocrine as it relates to the kidney Parathyroid gland Vitamin D Endocrine causes of HTN Adrenal adenoma PTH Bone Kidney Intestine 1, 25 OH Vitamin
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance
 Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Updates in primary hyperaldosteronism and the rule
 Updates in primary hyperaldosteronism and the 20-50 rule I. David Weiner, M.D. Professor of Medicine and Physiology and Functional Genomics University of Florida College of Medicine and NF/SGVHS The 20-50
Updates in primary hyperaldosteronism and the 20-50 rule I. David Weiner, M.D. Professor of Medicine and Physiology and Functional Genomics University of Florida College of Medicine and NF/SGVHS The 20-50
Urinary Kallikrein Excretion in Hypertensive Man
 Urinary Kallikrein Excretion in Hypertensive Man RELATIONSHIPS TO SODIUM INTAKE AND SODIUM-RETAINING STEROIDS By Harry S. Margolius, David Horwttz, John J. Pisano, and Harry R. Kelser ABSTRACT Urinary
Urinary Kallikrein Excretion in Hypertensive Man RELATIONSHIPS TO SODIUM INTAKE AND SODIUM-RETAINING STEROIDS By Harry S. Margolius, David Horwttz, John J. Pisano, and Harry R. Kelser ABSTRACT Urinary
CHAPTER 27 LECTURE OUTLINE
 CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE
 Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
About 20% of the Canadian population
 Mineralocorticoid Hypertension: Common and Treatable Hypertension is the most common chronic disease treated by the primary-care physician. It is now evident that mineralocorticoid hypertension, which
Mineralocorticoid Hypertension: Common and Treatable Hypertension is the most common chronic disease treated by the primary-care physician. It is now evident that mineralocorticoid hypertension, which
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance
 Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Primary Aldosteronism: screening, diagnosis and therapy
 Primary Aldosteronism: screening, diagnosis and therapy Jacques W.M. Lenders, internist DEPT. OF INTERNAL MEDICINE, RADBOUD UNIVERSITY NIJMEGEN MEDICAL CENTER, NIJMEGEN,THE NETHERLANDS DEPT. OF INTERNAL
Primary Aldosteronism: screening, diagnosis and therapy Jacques W.M. Lenders, internist DEPT. OF INTERNAL MEDICINE, RADBOUD UNIVERSITY NIJMEGEN MEDICAL CENTER, NIJMEGEN,THE NETHERLANDS DEPT. OF INTERNAL
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Potassium, Aldosterone, and Hypertension: How Physiology Determines Treatment. Jamie Johnston, MD University of Pittsburgh School of Medicine
 Potassium, Aldosterone, and Hypertension: How Physiology Determines Treatment Jamie Johnston, MD University of Pittsburgh School of Medicine No Disclosures Acknowledgements: Evan Ray, MD, PhD Objectives
Potassium, Aldosterone, and Hypertension: How Physiology Determines Treatment Jamie Johnston, MD University of Pittsburgh School of Medicine No Disclosures Acknowledgements: Evan Ray, MD, PhD Objectives
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
BODY FLUID. Outline. Functions of body fluid Water distribution in the body Maintenance of body fluid. Regulation of fluid homeostasis
 BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
The endocrine system is made up of a complex group of glands that secrete hormones.
 1 10. Endocrinology I MEDCHEM 535 Diagnostic Medicinal Chemistry Endocrinology The endocrine system is made up of a complex group of glands that secrete hormones. These hormones control reproduction, metabolism,
1 10. Endocrinology I MEDCHEM 535 Diagnostic Medicinal Chemistry Endocrinology The endocrine system is made up of a complex group of glands that secrete hormones. These hormones control reproduction, metabolism,
Potassium regulation. -Kidney is a major regulator for potassium Homeostasis.
 Potassium regulation. -Kidney is a major regulator for potassium Homeostasis. Normal potassium intake, distribution, and output from the body. Effects of severe hyperkalemia Partial depolarization of cell
Potassium regulation. -Kidney is a major regulator for potassium Homeostasis. Normal potassium intake, distribution, and output from the body. Effects of severe hyperkalemia Partial depolarization of cell
WATER, SODIUM AND POTASSIUM
 WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
Counter-Current System Regulation of Renal Functions
 Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Year 2004 Paper two: Questions supplied by Megan 1
 Year 2004 Paper two: Questions supplied by Megan 1 QUESTION 96 A 32yo woman if found to have high blood pressure (180/105mmHg) at an insurance medical examination. She is asymptomatic. Clinical examination
Year 2004 Paper two: Questions supplied by Megan 1 QUESTION 96 A 32yo woman if found to have high blood pressure (180/105mmHg) at an insurance medical examination. She is asymptomatic. Clinical examination
Hormonal Control of Osmoregulatory Functions *
 OpenStax-CNX module: m44828 1 Hormonal Control of Osmoregulatory Functions * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
OpenStax-CNX module: m44828 1 Hormonal Control of Osmoregulatory Functions * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
CALCINEURIN INHIBITORS AND HYPERKALEMIA. Sheena Surindran, MD 3/22/2011
 CALCINEURIN INHIBITORS AND HYPERKALEMIA Sheena Surindran, MD 3/22/2011 DISTAL TUBULE K SECRETION EFFECTS OF CYCLOSPORINE ON RAS AND POTASSIUM EXCRETION 10 pts on CsA and prednisone / 10 on AZT and prednisone
CALCINEURIN INHIBITORS AND HYPERKALEMIA Sheena Surindran, MD 3/22/2011 DISTAL TUBULE K SECRETION EFFECTS OF CYCLOSPORINE ON RAS AND POTASSIUM EXCRETION 10 pts on CsA and prednisone / 10 on AZT and prednisone
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Primary Aldosteronism
 Primary Aldosteronism Odelia Cooper, MD Assistant Professor of Medicine Division of Endocrinology, Diabetes, and Metabolism Cedars-Sinai Medical Center HYPERTENSION CENTER Barriers to diagnosing primary
Primary Aldosteronism Odelia Cooper, MD Assistant Professor of Medicine Division of Endocrinology, Diabetes, and Metabolism Cedars-Sinai Medical Center HYPERTENSION CENTER Barriers to diagnosing primary
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are
 Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
بسم هللا الرحمن الرحيم ** Note: the curve discussed in this page [TF]/[P] curve is found in the slides, so please refer to them.**
![بسم هللا الرحمن الرحيم ** Note: the curve discussed in this page [TF]/[P] curve is found in the slides, so please refer to them.** بسم هللا الرحمن الرحيم ** Note: the curve discussed in this page [TF]/[P] curve is found in the slides, so please refer to them.**](/thumbs/87/96174275.jpg) بسم هللا الرحمن الرحيم ** Note: the curve discussed in this page [TF]/[P] curve is found in the slides, so please refer to them.** INULIN characteristics : 1 filtered 100 %. 2-Not secreted. 3-Not reabsorbed
بسم هللا الرحمن الرحيم ** Note: the curve discussed in this page [TF]/[P] curve is found in the slides, so please refer to them.** INULIN characteristics : 1 filtered 100 %. 2-Not secreted. 3-Not reabsorbed
After studying this lecture, you should be able to...
 Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
LONG-TERM EFFECTS OF SURGICAL MENAGEMENT OF PRIMARY ALDOSTERONISM ON THE CARDIOVASCULAR SISTEM
 LONG-TERM EFFECTS OF SURGICAL MENAGEMENT OF PRIMARY ALDOSTERONISM ON THE CARDIOVASCULAR SISTEM Riccardo Marsili, Pietro Iacconi, Massimo Chiarugi, Giampaolo Bernini*, Alessandra Bacca*, Paolo Miccoli Department
LONG-TERM EFFECTS OF SURGICAL MENAGEMENT OF PRIMARY ALDOSTERONISM ON THE CARDIOVASCULAR SISTEM Riccardo Marsili, Pietro Iacconi, Massimo Chiarugi, Giampaolo Bernini*, Alessandra Bacca*, Paolo Miccoli Department
Janni M Jensen 1,2*, Frank H Mose 1,2, Jesper N Bech 1,2, Soren Nielsen 3 and Erling B Pedersen 1,2
 Jensen et al. BMC Nephrology 2013, 14:202 RESEARCH ARTICLE Open Access Effect of volume expansion with hypertonic- and isotonic saline and isotonic glucose on sodium and water transport in the principal
Jensen et al. BMC Nephrology 2013, 14:202 RESEARCH ARTICLE Open Access Effect of volume expansion with hypertonic- and isotonic saline and isotonic glucose on sodium and water transport in the principal
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
UCLA Nutrition Bytes. Title. Permalink. Journal ISSN. Author. Publication Date. Calcium and Hypertension. https://escholarship.org/uc/item/68b658ss
 UCLA Nutrition Bytes Title Calcium and Hypertension Permalink https://escholarship.org/uc/item/68b658ss Journal Nutrition Bytes, 4(2) ISSN 1548-601X Author Martinez, Christina Publication Date 1998-01-01
UCLA Nutrition Bytes Title Calcium and Hypertension Permalink https://escholarship.org/uc/item/68b658ss Journal Nutrition Bytes, 4(2) ISSN 1548-601X Author Martinez, Christina Publication Date 1998-01-01
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
TUBULOPATHY Intensive Care Unit Sina Hospital
 TUBULOPATHY Intensive Care Unit Sina Hospital A 13 years old female who is known case of Scoliosis. She was operated 2 months ago for spinal curve repair. PMH:EMG-MCV In 2 years old =>No Motoneuron Disease
TUBULOPATHY Intensive Care Unit Sina Hospital A 13 years old female who is known case of Scoliosis. She was operated 2 months ago for spinal curve repair. PMH:EMG-MCV In 2 years old =>No Motoneuron Disease
Instrumental determination of electrolytes in urine. Amal Alamri
 Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
20 Barton et al. Fourteen female mongrel dogs, weighing between 10 to 20 kg, were studied. Light pentobarbital anesthesia
 20 Barton et al. critical determinant of the occurrence and magnitude of natriuresis. It is possible that volume expansion suppresses sodium reabsorption in the loop, and that in the absence of this inhibitory
20 Barton et al. critical determinant of the occurrence and magnitude of natriuresis. It is possible that volume expansion suppresses sodium reabsorption in the loop, and that in the absence of this inhibitory
NORMAL POTASSIUM DISTRIBUTION AND BALANCE
 NORMAL POTASSIUM DISTRIBUTION AND BALANCE 98% of body potassium is contained within cells, principally muscle cells, and is readily exchangeable. Only 2% is in ECF. Daily intake exceeds the amount in ECF.
NORMAL POTASSIUM DISTRIBUTION AND BALANCE 98% of body potassium is contained within cells, principally muscle cells, and is readily exchangeable. Only 2% is in ECF. Daily intake exceeds the amount in ECF.
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
Renal Reabsorption & Secretion
 Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
Several abnormalities of calcium metabolism
 AJH 1991; 4:404-409 Intestinal Absorption of Calcium and Calcium Metabolism in Patients With Essential Hypertension and Normal Renal Function Merit Gadallah, Shaul G. Massry, Roberto Bigazzi Ronald L Horst,
AJH 1991; 4:404-409 Intestinal Absorption of Calcium and Calcium Metabolism in Patients With Essential Hypertension and Normal Renal Function Merit Gadallah, Shaul G. Massry, Roberto Bigazzi Ronald L Horst,
The ability of the kidneys to regulate extracellular fluid volume by altering sodium
 REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
Acid-Base Balance 11/18/2011. Regulation of Potassium Balance. Regulation of Potassium Balance. Regulatory Site: Cortical Collecting Ducts.
 Influence of Other Hormones on Sodium Balance Acid-Base Balance Estrogens: Enhance NaCl reabsorption by renal tubules May cause water retention during menstrual cycles Are responsible for edema during
Influence of Other Hormones on Sodium Balance Acid-Base Balance Estrogens: Enhance NaCl reabsorption by renal tubules May cause water retention during menstrual cycles Are responsible for edema during
Cardiorenal and Renocardiac Syndrome
 And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
In nocturnal enuresis
 The role of the kidney In nocturnal enuresis Kostas Kamperis MD PhD Dept of Pediatrics, Section of Nephrology Aarhus University Hospital, Aarhus, Denmark Enuresis prototypes Nocturnal polyuria Bladder
The role of the kidney In nocturnal enuresis Kostas Kamperis MD PhD Dept of Pediatrics, Section of Nephrology Aarhus University Hospital, Aarhus, Denmark Enuresis prototypes Nocturnal polyuria Bladder
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
RENAL FUNCTION An Overview
 RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
Na concentration in the extracellular compartment is 140
 هللامسب Na regulation: Na concentration in the extracellular compartment is 140 meq\l. Na is important because: -It determines the volume of extracellular fluid : the more Na intake will expand extracellular
هللامسب Na regulation: Na concentration in the extracellular compartment is 140 meq\l. Na is important because: -It determines the volume of extracellular fluid : the more Na intake will expand extracellular
Fluid and electrolyte balance, imbalance
 Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
The Art and Science of Diuretic therapy
 The Art and Science of Diuretic therapy Dr. Fayez EL Shaer Associate Professour of cardiology Consultant cardiologist MD, MSc, PhD, CBNC, NBE FESC, ACCP, FASNC,HFA KKUH, KFCC Heart failure: fluid overload
The Art and Science of Diuretic therapy Dr. Fayez EL Shaer Associate Professour of cardiology Consultant cardiologist MD, MSc, PhD, CBNC, NBE FESC, ACCP, FASNC,HFA KKUH, KFCC Heart failure: fluid overload
Diuretic Use in Neonates
 Neonatal Nursing Education Brief: Diuretic Use in the Neonate http://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/ Diuretics
Neonatal Nursing Education Brief: Diuretic Use in the Neonate http://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/ Diuretics
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Paul M McKie, Alessandro Cataliotti, Guido Boerrigter, Horng C Chen, Fernando L Martin, and John C Burnett Jr
 Cardiorenal Enhancing and Aldosterone Suppressing Actions of a Novel Designer Natriuretic Peptide in Experimental Hypertension with Ventricular Pressure Overload Paul M McKie, Alessandro Cataliotti, Guido
Cardiorenal Enhancing and Aldosterone Suppressing Actions of a Novel Designer Natriuretic Peptide in Experimental Hypertension with Ventricular Pressure Overload Paul M McKie, Alessandro Cataliotti, Guido
Principles of Renal Physiology. 4th Edition
 Principles of Renal Physiology 4th Edition Principles of Renal Physiology 4th Edition Chris Lote Professor of Experimental Nephrology, University of Birmingham, UK SPRINGER SCIENCE+BUSINESS MEDIA, B.V.
Principles of Renal Physiology 4th Edition Principles of Renal Physiology 4th Edition Chris Lote Professor of Experimental Nephrology, University of Birmingham, UK SPRINGER SCIENCE+BUSINESS MEDIA, B.V.
DIURETICS. Assoc. Prof. Bilgen Başgut
 DIURETICS Assoc. Prof. Bilgen Başgut Classification of Diuretics The best way to classify diuretics is to look for their Site of action in the nephron A. Diuretics that inhibit transport in the Proximal
DIURETICS Assoc. Prof. Bilgen Başgut Classification of Diuretics The best way to classify diuretics is to look for their Site of action in the nephron A. Diuretics that inhibit transport in the Proximal
The Antihypertensive Effect of Verapamil at Extremes of Dietary Sodium Intake
 The Antihypertensive Effect of Verapamil at Extremes of Dietary Sodium Intake JOHN P. NICHOLSON, M.D.; LAWRENCE M. RESNICK, M.D.; and JOHN H. LARAGH, M.D.; New York, New York Restricting sodium intake
The Antihypertensive Effect of Verapamil at Extremes of Dietary Sodium Intake JOHN P. NICHOLSON, M.D.; LAWRENCE M. RESNICK, M.D.; and JOHN H. LARAGH, M.D.; New York, New York Restricting sodium intake
Upon completion, participants should be able to:
 Learning Objectives Upon completion, participants should be able to: Describe the causes of secondary hypertension and the prevalence of primary aldosteronism Discuss the diagnostic approach to primary
Learning Objectives Upon completion, participants should be able to: Describe the causes of secondary hypertension and the prevalence of primary aldosteronism Discuss the diagnostic approach to primary
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
mid ihsan (Physiology ) GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B **
 (Physiology ) mid ihsan GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B ** Colloid pressure in the efferent arteriole is: A- More than that leaving
(Physiology ) mid ihsan GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B ** Colloid pressure in the efferent arteriole is: A- More than that leaving
Primary aldosteronism clinical practice guidelines: a re-appraisal The Management of Primary Aldosteronism
 Primary aldosteronism clinical practice guidelines: a re-appraisal The Management of Primary Aldosteronism Prof. FRANCO MANTERO Division of Endocrinology University of Padua Italy Case Detection, Diagnosis
Primary aldosteronism clinical practice guidelines: a re-appraisal The Management of Primary Aldosteronism Prof. FRANCO MANTERO Division of Endocrinology University of Padua Italy Case Detection, Diagnosis
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
The Urinary S. (Chp. 10) & Excretion. What are the functions of the urinary system? Maintenance of water-salt and acidbase
 10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
Circadian rhythm of urinary potassium excretion during treatment with an angiotensin receptor blocker
 475909JRA15410.1177/1470320313475909Journal of the Renin-Angiotensin-Aldosterone SystemOgiyama et al. 2013 Original Article Circadian rhythm of urinary potassium excretion during treatment with an angiotensin
475909JRA15410.1177/1470320313475909Journal of the Renin-Angiotensin-Aldosterone SystemOgiyama et al. 2013 Original Article Circadian rhythm of urinary potassium excretion during treatment with an angiotensin
Physiology (4) 2/4/2018. Wael abu-anzeh
 Physiology (4) 2/4/2018 Wael abu-anzeh In the previous lectures we have discussed the filtration and the reabsorption processes but in this lecture we will talk about the factor that will regulate or control
Physiology (4) 2/4/2018 Wael abu-anzeh In the previous lectures we have discussed the filtration and the reabsorption processes but in this lecture we will talk about the factor that will regulate or control
The Urinary System. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Faculty version with model answers
 Faculty version with model answers Fluid & Electrolytes Bruce M. Koeppen, M.D., Ph.D. University of Connecticut Health Center 1. A 40 year old, obese man is seen by his physician, and found to be hypertensive.
Faculty version with model answers Fluid & Electrolytes Bruce M. Koeppen, M.D., Ph.D. University of Connecticut Health Center 1. A 40 year old, obese man is seen by his physician, and found to be hypertensive.
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Hypoparathyroid Patients *
 Journal of Clinical Investigation Vol. 44, No. 6, 1965 Effects of Serum Calcium Level and Parathyroid Extracts on Phosphate and Calcium Excretion in Hypoparathyroid Patients * EUGENE EISENBERG t (From
Journal of Clinical Investigation Vol. 44, No. 6, 1965 Effects of Serum Calcium Level and Parathyroid Extracts on Phosphate and Calcium Excretion in Hypoparathyroid Patients * EUGENE EISENBERG t (From
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
Renal Pharmacology. Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics BIMM118
 Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics Renal Pharmacology Kidneys: Represent 0.5% of total body weight, but receive ~25% of the total arterial blood
Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics Renal Pharmacology Kidneys: Represent 0.5% of total body weight, but receive ~25% of the total arterial blood
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Potassium Balance and the-control of Renin Secretion
 Potassium Balance and the-control of Renin Secretion JEAN E. SEALEY, IRWIN CLARK, MARCIA B. BULL, and JoHN H. LARAGH From the Departments of Medicine, Biochemistry, and Orthopedic Surgery, Columbia University,
Potassium Balance and the-control of Renin Secretion JEAN E. SEALEY, IRWIN CLARK, MARCIA B. BULL, and JoHN H. LARAGH From the Departments of Medicine, Biochemistry, and Orthopedic Surgery, Columbia University,
Water, Electrolytes, and Acid-Base Balance
 Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
Chapter 27 Water, Electrolytes, and Acid-Base Balance 1 Body Fluids Intracellular fluid compartment All fluids inside cells of body About 40% of total body weight Extracellular fluid compartment All fluids
For more information about how to cite these materials visit
 Author(s): Michael Heung, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Michael Heung, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
EFFECT OF ACUTE SALINE LOADING ON THE ERYTH ROCYTE SODIUM TRANSPORT IN CHILDREN
 Acta Medica et Biologica Vol. 36, No. 109-113, 1989 EFFECT OF ACUTE SALINE LOADING ON THE ERYTH ROCYTE SODIUM TRANSPORT IN CHILDREN M. UCHIYAMA I. SATOKATA T. AIKAWA K. SAKAI Department 0/ pediatrics,
Acta Medica et Biologica Vol. 36, No. 109-113, 1989 EFFECT OF ACUTE SALINE LOADING ON THE ERYTH ROCYTE SODIUM TRANSPORT IN CHILDREN M. UCHIYAMA I. SATOKATA T. AIKAWA K. SAKAI Department 0/ pediatrics,
Fluids and electrolytes
 Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Over- and underfill: not all nephrotic states are equal. Detlef Bockenhauer
 Over- and underfill: not all nephrotic states are equal Detlef Bockenhauer Objectives Review pathophysiology of oedema: undervs overfill Treatment options The clinical setting: case 1 A6-y old girl with
Over- and underfill: not all nephrotic states are equal Detlef Bockenhauer Objectives Review pathophysiology of oedema: undervs overfill Treatment options The clinical setting: case 1 A6-y old girl with
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Updates in primary hyperaldosteronism and the rule
 Updates in primary hyperaldosteronism and the 20-50 rule I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of
Updates in primary hyperaldosteronism and the 20-50 rule I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of
