Urinary Angiotensin Excretion During Sodium Restriction and Diuretics
|
|
|
- Edith Lester
- 5 years ago
- Views:
Transcription
1 Nephrol Dial Transplant (1989)4: European Dialysis and Transplant Association-European Renal Association Nephrology Dialysis Transplantation Original Article Urinary Angiotensin Excretion During Sodium Restriction and Diuretics P. Boer, H. A. Koomans, W. H. Boer and E. J. Dorhout Mees Department of Nephrology and Hypertension, University Hospital, Utrecht, The Netherlands Abstract. The urinary excretion rate and plasma concentration of angiotensin I (, PAI) and angiotensin II (I, ), and plasma renin activity () were measured in seven healthy volunteers in the supine and upright position both on free and restricted sodium intakes. The same variables were measured before and after intravenous injection of furosemide, as well as before and during intravenous infusion of chlorothiazide. Assumption of the upright posture as well as sodium restriction increased PAI,, and, but and I excretion were not altered by these manoeuvres. Furosemide injection resulted in increases of all variables, albeit that PAI and were elevated to a lesser extent then. Chlorothiazide infusion caused a reduction in PAI,, and, whereas and I excretion increased modestly. The discrepancies between changes in plasma and urinary AI and All may indicate that urinary angiotensin excretion provides information which is supplementary to that of plasma angiotensins. Key words: Angiotensin; Diuretics; Kidney; Renin; Sodium; Urine Abbreviations: PAI, plasma angiotensin I;, plasma angiotensin II;, urinary angiotensin I; I, urinary angiotensin II;, plasma renin activity; EDTA, ethylenediaminetetraacetate; PMSF, phenylmethylsulphonylfluoride Correspondence and offprint requests to: P. Boer, Department of Nephrology and Hypertension, University Hospital, P.O. Box 85500, 3508 G. A. Utrecht, The Netherlands. Tel: Introduction Intrarenally produced All plays an important role in the regulation of renal haemodynamics and salt handling [1]., PAI, and in peripheral or renal venous blood are generally employed as indicators of the intrarenal activity of the renin-angiotensin system. Some observations suggest that this is not invariably justified. For instance, and do not always change in the same direction as directly measured kidney concentrations [2,3]. Renal tissue and lymph concentrations of renin and All are much greater than might be expected on the basis of renal vein concentrations [4-6], indicating nonvascular renal release or generation. Renal perfusion studies with AH show that only a small fraction of the infused All appears in the renal vein blood [7], indicating renal uptake or degradation. In man, studies providing direct information on intrarenal angiotensin production cannot be done. To examine the value of the urinary angiotensin excretion rate as an indicator of the activity of the intrarenal renin-angiotensin system, and to investigate whether changes in urinary and plasma angiotensins are parallel, we performed studies involving sodium intake, change of posture, and the use of diuretics acting at different sites of the tubule in man. Methods Subjects Four studies as detailed below were performed in seven healthy normotensive subjects (4 male, 3 female, age 22 ±1 years, systolic and diastolic blood pressure and 74±3mmHg, respectively). The protocol was approved by the Hospital Committee for Research in
2 714 P. Boeretal Humans, and informed consent was obtained from all participants. The subjects were studied both on a free sodium intake and during sodium restriction, achieved by intravenous administration of 20 mg furosemide followed by four days on a lommol/day sodium diet. Sodium restriction resulted in a decrease in body weight from to kg. The mean sodium excretion on the days preceding the studies were and 11+2 mmol/day on the free and sodium restricted diet, respectively. Study Protocols All investigations were done after an overnight fast. was ensured by giving an oral water load of ml/kg body weight before the studies were started, and subsequent substitution of urinary water loss throughout the experiments. Under these conditions urinary flow rates of > 10 ml/min are obtained. Study 1: assumption of upright posture. The subjects consumed the free sodium diet. They remained recumbent for 90 min; during the last 30 min, a urine portion and a mid-point blood sample were collected. A similar study was done while the subjects remained in the upright position for 90 min. Study 2: sodium restriction. The protocol of study 1 was repeated while the subjects consumed the sodium restricted diet. Study 3: furosemide administration. The subjects were studied on the free sodium intake in the supine position before and after intravenous injection of 20 mg furosemide (which was administered to initiate the period of sodium restriction). One 30-min urine specimen before and four subsequent 20-min specimens after injection as well as corresponding mid-point blood samples were obtained. Study 4: chlorothiazide infusion. The subjects were investigated on the sodium-restricted diet in the recumbent position before and during intravenous infusion of chlorothiazide (5 mg/min, preceded by an intravenous bolus of 250 mg). Other parts of this study have been published elsewhere [8]. Three 20-min and five 15-min urine specimens were collected before and during the infusion, respectively. Mid-point blood specimens were obtained in the third control period and in the second and fifth infusion periods. Preliminary studies had shown that sodium losses due to chlorothiazide infusion amount to 9 mmol/collection period. To maintain sodium balance during the experiment, these losses were supplemented by slow intravenous infusion of a 0.9% NaCl solution at a rate of 4 ml/min during the last four infusion periods. The volume of saline infused was subtracted from the volume of water given orally. During the study, a sustained intravenous infusion of inulin was administered for assessment of the glomerular filtration rate (GFR). Urine specimens were analysed for AI, All, sodium, creatinine, and inulin (study 4 only); plasma samples for the same variables and. Analytical Methods Angiotensin Determination., I, PAI, and PAH were measured by a modification of a previously reported radioimmunoassay [9]. Blood was collected on ice with EDTA (15mmol/l), pepstatin (10 umol/1), captopril (100 umol/1), and PMSF (6 umol/1) to inhibit the activity of renin, converting enzyme, and angiotensinases (the final concentrations in plasma are given in parentheses). Urines were collected on ice with PMSF (final concentration 3 umol/1). Collected in this way, plasma and urinary angiotensins are stable for 3 and 20 h, respectively. The samples were stored at 20 C, at which temperature they were stable for at least 9 months. Concentrating and cleaning up of the samples was performed by reversed-phase chromatography using a Baker SPE-10 vacuum extraction device and butylsilane bonded silica gel columns (Baker Chemical Co., Deventer, Netherlands), prewashed with methanol and equilibrated with deionised water. Urine (20 ml), acidified with glacial acetic acid to ph 3, or plasma (2 ml), 1:5 diluted and acidified with 8 ml mol/1 HC1 to ph 3, were applied on the columns. The effluents were discarded, and the columns were washed with 0.01 mol/1 HC1 and eluted with methanol/trifluoro-acetic acid 99:1 v/v. The eluate was dried under nitrogen at 37 C and dissolved in assay buffer. Dilution curves of urine or plasma extracts, as well as standard curves containing aliquots of extract, were parallel to the standard curves used in the radioimmunoassay. Characteristics of the AI and All assays are, respectively: sensitivity, 2 and 4 fmol; recovery of added standard material, in urine 72% and 90%, in plasma 73% and 89%; within-assay variation coefficient, for urine ll%and 10%,forplasma9%and9%;betweenassay variation coefficient, for urine 19% and 17%, for plasma 17% and 16%. Corrections were made for procedural losses. Cross reactions of the All antibody with AI and the C-terminal hepta-, hexa-, and penta-peptide are 1.2, 100, 100, and 80%, respectively. All concentrations were corrected for cross reaction with AI, but not with peptide fragments. Cross reactions of the AI antibody with All or All-fragments are negligible (< 0.001%). Other Determinations. was measured by radioimmunoassay [10]. Sodium and creatinine in urine and plasma were measured by standard laboratory techniques. Inulin was determined by a colorimetric method [11].
3 Urinary Angiotensin Excretion Table 1. Studies 1 and 2: response of urinary angiotensins and other variables to assumption of upright posture and sodium restriction 715 Condition C-Cr 1 PAI Supine, free Na Upright, free Na Supine, low Na Upright, low Na 9±2 11± * 18±5f 21±2t ± * f *t 26±2 35 ±2* 48±4f *t ±3* 24±3t 38±5*t, urinary sodium excretion; C-Cr, creatinine clearance; and UAH, urinary excretion of angiotensin 1 and II;, plasma renin activity; PAI and, plasma concentration of angiotensin I and II; * = P<0.05 with respect to corresponding supine value; f = P<0.05 with respect to corresponding value on free Na intake Table 2. Study 3: response of urinary angiotensins and other variables to intravenous injection of furosemide Baseline Furosemide 1 Furosemide 2 Furosemide 3 Furosemide 4 9± * * * * ±300* 2461 ±210* 1536 ±120* 860 ±100* C-Cr 131 ± ± ±12 118±11 78 ±25 151±44* 148 ±22* 143 ±30* I 67± * I12±30* ±21 190± * 400±100* 310±60* * Furosemide 1-4, collection periods after intravenous injection of furosemide; * = / > <0.05 with respect to baseline value Statistics. Values of, I, PAI, PAH, and are given as geometric mean + standard error (SEM). According to Bartlett's chi-square test [12], the variances of these variables were homogeneous. The studies were evaluated by analysis of variance, using a two-way randomised block design for studies 1 and 2, and oneway randomised block designs for studies 3 and 4 [12]. If a variance ratio (F) reached statistical significance (P<0.05), the differences between the means were analysed at the 5% level by the least significant difference test [12], using the treatment mean square error or the interaction mean square error (when appropriate) to calculate the least significant difference. Results Studies 1 and 2 The results are shown in Table 1. Irrespective of the sodium intake, and I excretion did not change significantly with assumption of the upright posture, whereas PAI,, and increased (P<0.05). In the supine as well as in the upright position, and I excretion was not significantly altered by sodium restriction, whereas PAI,, and increased (P<0.05). The creatinine clearance did not change; the sodium excretion decreased with assumption of the upright posture and sodium restriction (P<0.05). Study 3 The results are presented in Table 2. Intravenous injection of furosemide gave a significant increase in and I PAI 29±4 34± ±3 11 ±3 I3± ±4 12±3 excretion, as well as in (P<0.05). The increases in PAI and were smaller and did not reach statistical significance (/ > <0.10), because the time between baseline and peak value differed from subject to subject. In every subject, however, the peak value was greater than the baseline value: AI increased from to 40 ± 4 pmol/1, All from to 16 ± 3 pmol/1 (P < 0.05). The creatinine clearance showed a non-significant transient increase during the first period. The sodium excretion increased 25-fold, and had not yet returned to the baseline value in the last collection period (P<0.05). Study 4 The results are given in Table 3. During chlorothiazide infusion, and I excretion tended to increase (P<0.05). In contrast, PAI,, and decreased (P<0.05). The inulin clearance diminished by 12% (/ > <0.05); the sodium excretion increased 25-fold Discussion A notablefindingin our study is the absence of parallelism between changes in plasma and urinary angiotensins. Plasma angiotensins are generated in the systemic circulation after stimulation of renin release, but they may also originate from the kidney. However, the major part of intrarenally formed All is degraded in the kidney before
4 716 Table 3. Study 4: response of urinary angiotensins and other variables to intravenous infusion of chlorothiazide P. Boer et al C-Inulin UAH PA1 Baseline 1 Baseline 2 Baseline 3 Chlorothiazide 1 Chlorothiazide 2 Chlorothiazide 3 Chlorothiazide 4 Chlorothiazide 5 10±l ±I* 15±1* 15±1* I4+I* 14+1* ± * 550 ±50* 540 ±30* 530 ±30* 520 ±30* * 93+9* 90±9* 91+8* 94 ±7* ±14 92±12* 92±I8* ±12 56 ±12 59± ±11* 64±12 60±10 59± ±190* 790 ±180* ±4 35±2* 20±7 18±6 15±6* C-Inulin. inulin clearance: Chlorothiazide 1-5, collection periods during intravenous infusion of chlorothiazide;' -P<0.05 with respect to baseline values reaching the renal vein, as demonstrated in the dog by in vivo kidney perfusion studies with physiological concentrations of All [7], or by injection of radiolabelled All into the renal artery [14]. Urinary angiotensins may arise from glomerular filtration, local production by a tubular reninangiotensin system, or transtubular diffusion or secretion from the renal interstitium. The behaviour of the urinary excretion of AI and All was similar in the four studies (Tables 1-3), implying that the information which can be obtained from the excretion of both peptides is equivalent for the protocols used in our studies. From the angiotensin data and glomerular filtration rates presented in the tables it can be calculated that the urinary agiotensin excretion rate amounts to 1 %-5% of the filtered load. Small peptides like angiotensins are freely filtered. Subsequently, the major part is rapidly hydrolysed and reabsorbed in the proximal tubule, as shown in in vivo microinfusion studies with radiolabelled All in the rat [15]. We found no parallelism in changes of plasma and urinary angiotensins, which suggests that filtration from plasma is not the major source of and I. However, we can not exclude that alterations in tubular degradation or reabsorption of filtered angiotensins also contribute to the observed changes in angiotensin excretion. Local production by a tubular renin-angiotensin system requires the presence of a complete reninangiotensin system within or at the surface of renal tubule cells. Although literature on this subject is scarce, renin and angiotensinogen m-rna were found to be present in mesangial, proximal, and collecting duct cells [16]. In addition, AI may be converted into All intraiuminally, since converting enzyme activity has been demonstrated in the brush border zone of the proximal tubular epithelial cells [17]. Renin is not only secreted from the juxtaglomerular granular cells into the blood, but also - and even predominantly - into the renal interstitium, in which all the components of a renin-angiotensin system are present [1,7,13]. It is conceivable that the urinary angiotensins originate partly from transtubular diffusion or transport in regions where the interstitial concentrations are great. In vivo microperfusion studies in the rat have shown that peptides introduced in the distal parts of the tubule are recovered largely intact in the urine [15,18]. Thus, peptides entering the tubule at this site may escape from hydrolysation by brush border peptidases and tubular reuptake, which mainly occurs in the proximal tubule [15,18]. During chlorothiazide infusion, plasma All and decreased, whereas I increased. Intrarenal All is probably involved in the adaptation of the GFR to an increase in sodium load at the macula densa by increasing the pre- and postglomerular resistance, the net effect being a decrease in GFR [19]. If I is a marker of intrarenal All production, our finding of an increase in I and a decrease in inulin clearance is compatible with a role of All in the tubuloglomerular feedback mediated decrease in GFR. The increase in urinary angiotensin excretion in studies 3 and 4 corresponds with an increase in urine flow and may thus be flow-related. To obtain flow-independent values we calculated the urinary angiotensin:creatinine ratio, which increased in the same way as and I (data not shown). This makes it unlikely that the increased excretion represents a wash-out phenomenon. On the other hand, tubular degradation, if present, may be less complete when the urineflowis greater. The modest increase in PAI and after furosemide despite a large increase in was unexpected, although not unprecedented [20]. In each subject, the peak was greater than the baseline value (/><0.05), but due to scatter in the time-to-peak values the mean increase did not reach statistical significance (0.05 < P< 0.10). Literature reporting on urinary All excretion is scanty. Fukuchi [21] found normal values in patients with essential hypertension or chronic glomerulonephritis, increased values in renovascular hypertension, and decreased values in primary aldosteronism. The reported excretion rates are about 50 times lower than ours. This
5 Urinary Angiotensin Excretion may be due to differences in extraction technique, to intravesical degradation caused by prolonged collection periods (2 h), or to incomplete voiding of the bladder due to low urinary flow rates (< 0.5 ml/min). We did not confirm by high performance liquid chromatography that the All-like immunoreactive material in urine actually was All. If All-like peptide fragments cross-reacting with the All antibody are present in urine, they most probably originate from All, and they will provide the same kind of information as All. In conclusion, during various manoeuvres in healthy humans we found a discrepant behaviour of plasma and urinary AI and All. Our study gave no definitive information on the exact origin of urinary AI and All. Local production by a tubular renin-angiotensin system and transtubular diffusion or secretion from the interstitium are among the possibilities. More studies, both in humans (e.g. during converting enzyme inhibition and angiotensin infusion) and animals (comparison of urine and lymph angiotensin excretion) are needed to define the source and possible meaning of urinary angiotensin excretion. References 1. Navar LG, Rosivall L. Contribution of the renin-angiotensin system to the control of intrarenal hemodynamics. Kidney lm 1984; 25: Mendelsohn FAO. Angiotensin II: evidence for its role as an intrarenal hormone. Kidney lm 1982; 22: suppl. 12, S78-S81 3. Thurau KWC, Dahlheim H, Griiner A, Mason J, Granger P. Activation of renin in the single juxtaglomerutar apparatus by sodium chloride in the tubular fluid at the macula densa. Circ Res 1972; suppl. 2: Bailey MD. Rector FC, Seldin DW. Angiotensin II in arterial and renal venous plasma and renal lymph in the dog. J Clin Invest 1971; 50: Mendelsohn FAO. Evidence for the local occurrence of angiotensin II in rat kidney and its modulation by dietary sodium intake and converting enzyme blockade. Clin Sci 1979; 57: OMorchoe CC, O'Morchoe PJ, Albertine K.H, Jarosz HM. Concentration of renin in the renal interstitium, as reflected in lymph. Renal Physiot 1981; 4: Rosivall L, Narkates AJ, Oparil S, Navar LG. De novo intrarenal formation of angiotensin II during control and enhanced renin secretion. Am J Physiot 1987; 252: Fl 118-F Boer WH. Koomans HA, Dorhout Mees EJ. Acute effect of thiazides, with or without carbonic anhydrase activity, on lithium and free water clearance in man. Clin Sci 1989; 76: Boer P, Geyskes GG. Apparently high angiotensin II levels in patients with essential hypertension treated by converting enzyme inhibition. ScandJ Clin Lab Invest 1985; 45: Boer P, Sleumer JH, Spriensma M. Confirmation of the optimal ph for measuring renin activityin plasma. Clin Chem 1985; 31: Heyrowski A. A new method for the determination of inulin in plasma and urine. Clin Chim Ada 1956; 1: Snedecor GW, Cochran WG. Statistical Methods. Iowa State University Press, Ames, 1979; Ch. 10, Hackenthal E, Metz R, Buhrle CP, Taugner R. Intrarenal and intracellular distribution of renin and angiotensin. Kidney lm 1987; 31, suppl.20:s4-s Bailey MD, Oparil S. Relation of renal hemodynamics to metabolism of angiotensin II by the canine kidney. Circ Res 1977; 41: Carone F, Peterson DR, Oparil S, Pullman TN. Renal tubular transport and catabolism of proteins and peptides. Kidney Int 1979; 16: Rajamaran S, Graves K, Kunapuli P. Intrarenal renin-angiotensin system: in situ hybridization study. FedAbs Soc Exp BiolJ 1988; 2: A Taugner R, Hackenthal E, Helmchen U et al. The intrarenal reninangiotensin system. An immunocytological study on the localization of renin, angiotensin, converting enzyme and the angiotensins in the kidney of mouse and rat. Klin Wochenschr 1982; 60: Ganapathy V, Leibach FH. Carrier-mediated reabsorption of small peptides in renal proximal tubule. Am J Physiol 1986; 251: F945-F Navar LG, Rosivall L, Carmines PK, Oparil S. Effects of locally formed angiotensin II on renal hemodynamics. Fed Proc 1986; 45: Walker WG, Moore MA. Horvath JS, Whelton PK. Arterial and venous angiotensin II in normal subjects. Relation to plasma renin activity and plasma aldosterone concentration, and response to posture and volume changes. Circ Res 1976; 38: Fukuchi S. Estimation of urinary angiotensin II by radioimmunoassay. TohokuJ Exp Med 1974; 114: Receivedfor publication Accepted in revised form
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Introduction to the kidney: regulation of sodium & glucose. Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health
 Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Introduction. Acids, Bases and ph; a review
 0 P a g e Introduction In this sheet, we discuss acidbase balance in our body and the role of kidneys in its establishment. Arrangement of topics is different from that of the lecture, to assure consistency
0 P a g e Introduction In this sheet, we discuss acidbase balance in our body and the role of kidneys in its establishment. Arrangement of topics is different from that of the lecture, to assure consistency
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
RENAL FUNCTION An Overview
 RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
Physiology (4) 2/4/2018. Wael abu-anzeh
 Physiology (4) 2/4/2018 Wael abu-anzeh In the previous lectures we have discussed the filtration and the reabsorption processes but in this lecture we will talk about the factor that will regulate or control
Physiology (4) 2/4/2018 Wael abu-anzeh In the previous lectures we have discussed the filtration and the reabsorption processes but in this lecture we will talk about the factor that will regulate or control
Renal Blood flow; Renal Clearance. Dr Sitelbanat
 Renal Blood flow; Renal Clearance Dr Sitelbanat Objectives At the end of this lecture student should be able to describe: Renal blood flow Autoregulation of GFR and RBF Regulation of GFR The Calcuation
Renal Blood flow; Renal Clearance Dr Sitelbanat Objectives At the end of this lecture student should be able to describe: Renal blood flow Autoregulation of GFR and RBF Regulation of GFR The Calcuation
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The kidney. (Pseudo) Practical questions. The kidneys are all about keeping the body s homeostasis. for questions Ella
 The kidney (Pseudo) Practical questions for questions Ella (striemit@gmail.com) The kidneys are all about keeping the body s homeostasis Ingestion Product of metabolism H 2 O Ca ++ Cl - K + Na + H 2 O
The kidney (Pseudo) Practical questions for questions Ella (striemit@gmail.com) The kidneys are all about keeping the body s homeostasis Ingestion Product of metabolism H 2 O Ca ++ Cl - K + Na + H 2 O
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
BIOL 2402 Renal Function
 BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Renal Reabsorption & Secretion
 Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Principles of Renal Physiology. 4th Edition
 Principles of Renal Physiology 4th Edition Principles of Renal Physiology 4th Edition Chris Lote Professor of Experimental Nephrology, University of Birmingham, UK SPRINGER SCIENCE+BUSINESS MEDIA, B.V.
Principles of Renal Physiology 4th Edition Principles of Renal Physiology 4th Edition Chris Lote Professor of Experimental Nephrology, University of Birmingham, UK SPRINGER SCIENCE+BUSINESS MEDIA, B.V.
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION
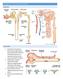 LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
Functional morphology of kidneys Clearance
 Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM
 RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Answers and Explanations
 Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Hyperaldosteronism: Conn's Syndrome
 RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
Renal Physiology - Lectures
 Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
MAJOR FUNCTIONS OF THE KIDNEY
 MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
renoprotection therapy goals 208, 209
 Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
RENAL. 6. Renal acid secretion is affected by all of the following except a. pco 2 b. K c. Carbonic anhydrase d. Aldosterone e. Ca
 RENAL 1. The reabsorption of Na in the proximal tubules a. Reabsorbs 80% of the filtered sodium load b. Causes increased hypertonicity c. Is powered by N/H ATPase d. Shares a common carrier with glucose
RENAL 1. The reabsorption of Na in the proximal tubules a. Reabsorbs 80% of the filtered sodium load b. Causes increased hypertonicity c. Is powered by N/H ATPase d. Shares a common carrier with glucose
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
Filtration and Reabsorption Amount Filter/d
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
Interrelationship between Angiotensin Catecholamines. Tatsuo SATO, M.D., Masaru MAEBASHI, M.D., Koji GOTO, M.D., and Kaoru YOSHINAGA, M.D.
 Interrelationship between Angiotensin and Catecholamines Tatsuo SATO, M.D., Masaru MAEBASHI, M.D., Koji GOTO, M.D., and Kaoru YOSHINAGA, M.D. SUMMARY Urinary catecholamines were measured with an attempt
Interrelationship between Angiotensin and Catecholamines Tatsuo SATO, M.D., Masaru MAEBASHI, M.D., Koji GOTO, M.D., and Kaoru YOSHINAGA, M.D. SUMMARY Urinary catecholamines were measured with an attempt
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Patterns of Sodium Excretion During Sympathetic Nervous System Arousal. Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S.
 1156 Patterns of Sodium Excretion During Sympathetic Nervous System Arousal Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S. Alpert The purpose of this study was to examine Na + handling and regulation
1156 Patterns of Sodium Excretion During Sympathetic Nervous System Arousal Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S. Alpert The purpose of this study was to examine Na + handling and regulation
Renal Physiology. April, J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine.
 Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
JINNAH SINDH MEDICAL UNIVERSITY
 MODULE TITLE INTRODUCTION TARGET STUDENTS DURATION MODULE OUTCOMES Spiral -1 Renal and Excretory-1 Module The Renal and Excretory-1 Module is designed to help the learners understand how the urinary system
MODULE TITLE INTRODUCTION TARGET STUDENTS DURATION MODULE OUTCOMES Spiral -1 Renal and Excretory-1 Module The Renal and Excretory-1 Module is designed to help the learners understand how the urinary system
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Chapter 15 Fluid and Acid-Base Balance
 Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
modulating the tubuloglomerular feed-back mechanism in the canine kidney; Sciences Center, 4200 East Ninth Avenue, Denver, CO 80262, U.S.A.
 J. Physiol. (1986), 380, pp. 35-43 35 With 3 text-figures Printed in Great Britain RENAL VASOCONSTRICTOR RESPONSE TO HYPERTONIC SALINE IN THE DOG: EFFECTS OF PROSTAGLANDINS, INDOMETHACIN AND THEOPHYLLINE
J. Physiol. (1986), 380, pp. 35-43 35 With 3 text-figures Printed in Great Britain RENAL VASOCONSTRICTOR RESPONSE TO HYPERTONIC SALINE IN THE DOG: EFFECTS OF PROSTAGLANDINS, INDOMETHACIN AND THEOPHYLLINE
11/05/1431. Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate
 Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Plasma Renin Activity and Renin-Substrate Concentration in Patients with Liver Disease
 Plasma Renin Activity and Renin-Substrate Concentration in Patients with Liver Disease By Carlos R. Ayers, M.D. ABSTRACT Peripheral venous renin activity was determined by the method of Boucher in 15 patients
Plasma Renin Activity and Renin-Substrate Concentration in Patients with Liver Disease By Carlos R. Ayers, M.D. ABSTRACT Peripheral venous renin activity was determined by the method of Boucher in 15 patients
Potassium secretion. E k = -61 log ([k] inside / [k] outside).
![Potassium secretion. E k = -61 log ([k] inside / [k] outside). Potassium secretion. E k = -61 log ([k] inside / [k] outside).](/thumbs/80/80478709.jpg) 1 Potassium secretion In this sheet, we will continue talking about ultrafiltration in kidney but with different substance which is K+. Here are some informations that you should know about potassium;
1 Potassium secretion In this sheet, we will continue talking about ultrafiltration in kidney but with different substance which is K+. Here are some informations that you should know about potassium;
Na + Transport 1 and 2 Linda Costanzo, Ph.D.
 Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
hold for the human kidney.2 Shannon and Smith (4) have rightfully stressed
 THE RENAL EXCRETION OF INULIN AT LOW PLASMA CONCEN- TRATIONS OF THIS COMPOUND, AND ITS RELATIONSHIP TO THE GLOMERULAR FILTRATION RATE IN NORMAL, NEPHRITIC AND HYPERTENSIVE INDIVIDUALS' By BENJAMIN F. MILLER,
THE RENAL EXCRETION OF INULIN AT LOW PLASMA CONCEN- TRATIONS OF THIS COMPOUND, AND ITS RELATIONSHIP TO THE GLOMERULAR FILTRATION RATE IN NORMAL, NEPHRITIC AND HYPERTENSIVE INDIVIDUALS' By BENJAMIN F. MILLER,
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Lecture 16: The Nephron
 Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
You should know the T max for any substance that you use and for PAH ; T max = mg / min
 Tubular function - What is clearance? o clearance referred to the theoretical volume of plasma from which a substance is cleared ( cleaned ) over a period of time and so its unit would be ((ml/min)) -
Tubular function - What is clearance? o clearance referred to the theoretical volume of plasma from which a substance is cleared ( cleaned ) over a period of time and so its unit would be ((ml/min)) -
The Urinary S. (Chp. 10) & Excretion. What are the functions of the urinary system? Maintenance of water-salt and acidbase
 10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
The Urinary System. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BLOCK REVIEW Renal Physiology. May 9, 2011 Koeppen & Stanton. EXAM May 12, Tubular Epithelium
 BLOCK REVIEW Renal Physiology Lisa M. HarrisonBernard, Ph.D. May 9, 2011 Koeppen & Stanton EXAM May 12, 2011 Tubular Epithelium Reabsorption Secretion 1 1. 20, 40, 60 rule for body fluid volumes 2. ECF
BLOCK REVIEW Renal Physiology Lisa M. HarrisonBernard, Ph.D. May 9, 2011 Koeppen & Stanton EXAM May 12, 2011 Tubular Epithelium Reabsorption Secretion 1 1. 20, 40, 60 rule for body fluid volumes 2. ECF
clamped. At 30- or 60-minute intervals urine specimens were collected and the bladder washed out with saline
 Downloaded from http://www.jci.org on January 11, 218. https://doi.org/1.1172/jci11171 THE MECHANISM OF THE EXCRETION OF VITAMIN C BY THE HUMAN KIDNEY AT LOW AND NORMAL PLASMA LEVELS OF ASCORBIC ACID 1
Downloaded from http://www.jci.org on January 11, 218. https://doi.org/1.1172/jci11171 THE MECHANISM OF THE EXCRETION OF VITAMIN C BY THE HUMAN KIDNEY AT LOW AND NORMAL PLASMA LEVELS OF ASCORBIC ACID 1
PARTS OF THE URINARY SYSTEM
 EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
Urinary System. BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College
 Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Fluid and electrolyte balance, imbalance
 Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Excretory System-Training Handout
 Excretory System-Training Handout Karen L. Lancour National Rules Committee Chairman Life Science Excretion - Excretion is the removal of the metabolic wastes of an organism. Wastes that are removed include
Excretory System-Training Handout Karen L. Lancour National Rules Committee Chairman Life Science Excretion - Excretion is the removal of the metabolic wastes of an organism. Wastes that are removed include
Use the following diagram to answer the next question. 1. In the diagram above, pressure filtration occurs in a. W b. X c. Y d. Z
 Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Renal physiology II. Basic renal processes. Dr Alida Koorts BMS
 Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Chapter 26 The Urinary System
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Class XI Chapter 19 Excretory Products and their Elimination Biology
 Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
Urinary System BIO 250. Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat. Routes of Waste Elimination
 Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance
 Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Renal Clearance. Dr. Eman El Eter
 Renal Clearance Dr. Eman El Eter Concept of clearance Clearance is the volume of plasma that is completely cleared of a substance each minute. Example: Renal clearance of Substance X is defined as the
Renal Clearance Dr. Eman El Eter Concept of clearance Clearance is the volume of plasma that is completely cleared of a substance each minute. Example: Renal clearance of Substance X is defined as the
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
Renal Physiology II Tubular functions
 Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
A. Correct! Flushing acids from the system will assist in re-establishing the acid-base equilibrium in the blood.
 OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection
 SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection Hiddo Lambers Heerspink Department of Clinical Pharmacy and Pharmacology University Medical Center
SGLT2 inhibition in diabetes: extending from glycaemic control to renal and cardiovascular protection Hiddo Lambers Heerspink Department of Clinical Pharmacy and Pharmacology University Medical Center
Chapter 44. Regulating the Internal Environment. AP Biology
 Chapter 44. Regulating the Internal Environment Homeostasis Living in the world organisms had a choice: regulate their internal environment maintain relatively constant internal conditions conform to the
Chapter 44. Regulating the Internal Environment Homeostasis Living in the world organisms had a choice: regulate their internal environment maintain relatively constant internal conditions conform to the
