Musculoskeletal Imaging Original Research
|
|
|
- Sylvia Joseph
- 5 years ago
- Views:
Transcription
1 Musculoskeletal Imaging Original Research Isotropic Resolution 3D FSE MRI of Articular Cartilage of Knee Joint Musculoskeletal Imaging Original Research Cristy N. Gustas 1 Donna G. Blankenbaker 2 Alejandro Munoz Del Rio 2,3 Carl S. Winalski 4 Richard Kijowski 2 Gustas CN, Blankenbaker DG, Munoz Del Rio A, Winalski CS, Kijowski R Keywords: 3 T, cartilage, diagnostic performance, morphology, MRI DOI: /AJR Received December 9, 2014; accepted after revision February 6, Based on a presentation at the Society of Skeletal Radiology 2014 annual meeting, San Diego, CA. 1 Department of Radiology, Penn State Milton S. Hershey Medical Center, 500 University Dr, Hershey, PA Address correspondence to C. N. Gustas (cgustas@hmc.psu.edu). 2 Department of Radiology, University of Wisconsin School of Medicine and Public Health, Madison, WI. 3 Department of Biostatistics, University of Wisconsin School of Medicine and Public Health, Madison, WI. 4 Department of Biomedical Engineering, Lerner Research Institute, Cleveland Clinic, Cleveland, OH. AJR 2015; 205: X/15/ American Roentgen Ray Society Evaluation of the Articular Cartilage of the Knee Joint Using an Isotropic Resolution 3D Fast Spin-Echo Sequence With Conventional and Radial OBJECTIVE. The purpose of this study was to determine whether the use of radial reformatted images could improve the diagnostic performance of a 3D fast spin-echo (FSE) sequence for detecting surgically confirmed cartilage lesions within the knee joint. MATERIALS AND METHODS. An MRI examination consisting of five 2D FSE sequences and a sagittal 3D FSE sequence was performed at 3 T on the knee joint of 150 patients who underwent subsequent knee arthroscopy, which included grading of the articular cartilage. Conventional axial, sagittal, and coronal reformatted images and radial reformatted images were created from the 3D FSE source data. Two musculoskeletal radiologists independently used the 2D FSE sequences, the 3D FSE sequence with conventional reformatted images only, and the 3D FSE sequence with both radial and conventional reformatted images at three separate sessions to grade each articular surface of the knee joint. McNemar tests were used to compare diagnostic performance for detecting cartilage lesions using arthroscopy as the reference standard. RESULTS. The 3D FSE sequence with radial and conventional reformatted images had higher sensitivity (p < 0.001) and similar specificity (p = 0.73) to the 2D FSE sequences for detecting cartilage lesions and higher sensitivity (p < 0.001) and specificity (p = 0.002) than the 3D FSE sequence with conventional reformatted images for detecting cartilage lesions. The 3D FSE sequence with conventional reformatted images had similar sensitivity (p = 0.93) and lower specificity (p = 0.005) than did the 2D FSE sequences for detecting cartilage lesions. CONCLUSION. A 3D FSE sequence had improved diagnostic performance compared with 2D FSE sequences for detecting cartilage lesions within the knee joint but only when using both radial and conventional reformatted images for cartilage evaluation. O steoarthritis is a widely prevalent chronic disease and a leading cause of disability in the United States and worldwide [1, 2]. Accurate detection of cartilage lesions within the knee joint is essential to identify patients who may benefit from early interventions because there are currently few treatment options available for individuals with advanced stages of the disease. Lifestyle modifications, including weight loss and physical activity, can alleviate symptoms in patients with early osteoarthritis and may potentially slow the progression of joint degeneration [3]. In addition, there has also been much recent effort in developing improved cartilage repair procedures [4 7] and new disease-modifying therapies [8 11] to treat patients with early posttraumatic and degenerative cartilage lesions. Noninvasive methods to assess longitudinal changes in morphologic cartilage degenera- tion can play an important role in investigating the ability of these new treatment options to slow or stop disease progression [12, 13]. MRI is well suited to evaluate articular cartilage because of its ability to acquire images with high spatial resolution and excellent tissue contrast in any plane [12, 13]. The increasing interest in the treatment of articular cartilage disease has resulted in quadratic growth in cartilage imaging publications over the previous 2 decades [14]. Several of the more recent studies have focused on the potential advantages of 3D sequences for evaluating the articular cartilage of the knee joint [15 23]. When acquired at similar spatial resolutions, 3D sequences have higher signal-to-noise ratio and greater tissue contrast than do the 2D fast spin-echo (FSE) sequences typically used for clinical cartilage imaging [24 28]. Three-dimensional sequences can also reduce the effects AJR:205, August
2 TABLE 1: Imaging Parameters for MRI Examination Sequences Imaging Parameter Axial Fat-Suppressed T2-Weighted 2D FSE of through-plane partial volume averaging by acquiring thin continuous slices through joints. In addition, when isotropic or nearisotropic voxel dimensions are used, multiplanar reformatted images can be created from the 3D volumetric source data, which allows articular cartilage to be evaluated in any orientation [29]. Despite the clear theoretic advantages, the use of 3D sequences has not translated into a substantial improvement in diagnostic performance for detecting cartilage lesions within the knee joint in multiple clinical studies [15 21]. In most of these studies, the sensitivity for identifying cartilage lesions using both 2D FSE and 3D sequences is highest on the thick articular surface of the patella and lowest on the lateral tibial plateau, where the curved articular surface is prone to partial volume averaging and imaging artifacts. One of the unique benefits of 3D sequences is that they can yield reformatted images, which allow articular cartilage to be evaluated in orientations other than the conventional axial, sagittal, and coronal planes [29]. In particular, radial imaging has been used in the hip for years with mixed results in terms of improvement in the detection of joint abnormalities [30 33]. Theoretically, radial sections offer improved characterization of curved articular surfaces by providing an orthogonal view at each surface point, which minimizes the effects of partial volume averaging [34]. The purpose of this study was to determine whether the use of radial reformatted images could improve the diagnostic performance of a 3D FSE sequence for detecting surgically confirmed cartilage lesions within the knee joint. Coronal Intermediate-Weighted 2D FSE Sequence Coronal Fat-Suppressed Intermediate-Weighted 2D FSE Materials and Methods Study Group This retrospective study was performed at the University of Wisconsin in compliance with HIPAA regulations, with approval of our institutional review board and with a waiver of informed consent. The study group consisted of 150 symptomatic patients (90 male and 60 female patients; mean age, 41 years; age range, years) who underwent MRI examination and subsequent arthroscopic surgery performed on the same knee within 6 months. The study group was selected by reviewing a PACS workstation (Horizon Medical Imaging, McKesson) to identify all patients who underwent a knee MRI examination on a single 3-T MRI scanner at our institution between October 8, 2008, and December 27, 2009, and then by reviewing the medical records of these individuals to determine whether they had undergone subsequent arthroscopic knee surgery. No patient was excluded from the study on the basis of any factor, including age, sex, weight, severity of knee pain, history of knee surgery, or quality of the MR images. MRI Examination All 150 patients in the study group underwent an MRI examination of the knee on the same 3-T scanner (Signa Excite HDx, GE Healthcare) using an eight-channel phased-array extremity coil (Precision Eight TX/TR High Resolution Knee Array, Invivo). All MRI examinations consisted of the following six sequences, with the imaging parameters summarized in Table 1: axial frequency-selective fat-suppressed T2-weighted 2D FSE sequence, coronal intermediate-weighted 2D FSE sequence, coronal frequency-selective fat-suppressed intermediate-weighted 2D FSE sequence, sagittal intermediate-weighted 2D FSE sequence, sagittal Sagittal Intermediate-Weighted 2D FSE Sagittal Fat-Suppressed T2-Weighted 2D FSE TR/TE 4300/ / / / / /24 Matrix size (mm) FOV (cm) Slice thickness (mm) Bandwidth (khz) Echo-train length No. of signal averages Scanning time (min:s) 3:30 3:25 3:26 3:26 3:16 5:00 Note FSE = fast spin-echo. 3D FSE frequency-selective fat-suppressed T2-weighted 2D FSE sequence, and sagittal frequency-selective fat-suppressed isotropic resolution intermediateweighted 3D FSE sequence. The 3D FSE sequence used a 2D parallel imaging reconstruction technique (ARC, GE Healthcare) with an acceleration factor of 3 to reduce scanning time. The 3D FSE volumetric source data were used to create conventional axial, sagittal, and coronal reformatted images of the knee joint with 1.0-mm slice thickness. The conventional reformatted images were used along with the 2D FSE images and sagittal 3D FSE source images to make the official interpretation of the MRI examination. For the purposes of the research study, radial reformatted images were retrospectively created from the 3D FSE volumetric source data using a commercially available MRI workstation (Advantage Workstation 4.2, GE Healthcare). Three sets of 1.0-mm-thick radial reformatted images were created with centers of rotation for the trochlea, medial femoral condyle, and lateral femoral condyle chosen from the sagittal 3D FSE source images to produce reformatted images orthogonal to the respective articular surfaces. Each radial reformation set was acquired with 180 of coverage at 1 intervals. The time required to create all radial reformatted images on the MRI workstation was less than 3 minutes. Image Analysis All MRI examinations were independently reviewed on the PACS workstation at three separate sessions by two fellowship-trained musculoskeletal radiologists who had 12 and 14 years of clinical experience and were blinded to the clinical and surgical findings of all patients. To minimize recall bias, the radiologists reviewed the MRI examinations at three separate sessions approximately 6 months apart, with the order of review of the MRI 372 AJR:205, August 2015
3 Isotropic Resolution 3D FSE MRI of Articular Cartilage of Knee Joint examinations randomized at each session. During the first review of the MRI examinations, the radiologists used all five 2D FSE sequences together to evaluate the articular cartilage of the knee joint. During the second review, the radiologists used the sagittal 3D FSE source images with conventional axial, sagittal, and coronal reformatted images only. During the third review, the radiologists used the sagittal 3D FSE source images with conventional axial, sagittal, and coronal reformatted images along with the three sets of radial reformatted images to evaluate the articular cartilage. During the three reviews of the MRI examinations, the radiologists graded all six articular surfaces (patella, trochlea, medial femoral condyle, lateral femoral condyle, medial tibial plateau, and lateral tibial plateau) of the knee joint using a modified Noyes classification system (grade 0 = normal cartilage, grade 1 = increased T2 signal intensity within morphologically normal cartilage, grade 2A = superficial partial-thickness cartilage lesion < 50% of the thickness of the articular surface, grade 2B = deep partial-thickness cartilage lesion > 50% of the thickness of the articular surface, and grade 3 = full-thickness cartilage lesion) [35, 36]. If more than one cartilage lesion was identified on an articular surface, the lesion with the highest grade was recorded. During the third review of the MRI examinations, the radiologists also determined whether the use of the 3D FSE radial reformatted images provided a subjective improvement in the ability to visualize a cartilage lesion when compared with the use of the sagittal 3D FSE source images and conventional reformatted images only. Arthroscopic Knee Surgery All 150 patients in the study group underwent arthroscopic knee surgery within 6 months of their MRI examination (mean interval, 59 days; range, days). All arthroscopic knee surgeries were performed by one of three orthopedic surgeons at our institution who specialized in sports medicine and who had years of clinical experience. At the time of arthroscopy, the surgeons were aware of the official interpretations of the MRI examinations, which were made without the use of the 3D FSE radial reformatted images. The surgeons at our institution routinely inspect all articular surfaces of the knee joint at arthroscopy, both visually and with a surgical probe, and record the grade of any cartilage lesions detected on each articular surface in their surgical report using the Noyes classification system (grade 1 = cartilage softening, grade 2A = superficial partialthickness cartilage defect < 50% of the thickness of the articular surface, grade 2B = deep partialthickness cartilage defect > 50% of the thickness of the articular surface, and grade 3 = full-thickness cartilage defect) [37]. The surgical reports of all patients in the study group were retrospectively reviewed to determine the grade of cartilage lesion on each articular surface of the knee joint. A C D Fig year-old woman with surgically confirmed grade 2B cartilage lesion on lateral femoral condyle. A and B, Coronal intermediate-weighted 2D fast spin-echo (FSE) image (A) and coronal fat-suppressed intermediate-weighted 2D FSE image (B) show normal-appearing cartilage (arrows) on lateral femoral condyle. C, Coronal 3D FSE reformatted image shows deep partial-thickness cartilage lesion (arrow) on lateral femoral condyle. D, Radial 3D FSE reformatted image provides better visualization of exact depth of cartilage lesion (arrow) on lateral femoral condyle. Statistical Analysis Statistical analysis was performed using the R programming environment (version 2.3.1, R Foundation). Statistical significance for all statistical tests was defined as p < To assess the diagnostic performance for detecting cartilage lesions within the knee joint, the data from the independent reviews of both readers at each of the three sessions were combined to increase statistical power. Using the cartilage grades assigned to each articular surface at arthroscopy as the reference standard, the sensitivity and specificity of the 2D FSE sequences; the 3D FSE sequence with conventional axial, sagittal, and coronal reformatted images; and the 3D FSE sequence with radial and conventional reformatted images were calculated. The calculations were made to determine the detection ability for each individual arthroscopic grade of cartilage lesion and all arthroscopic grades combined as well as for each individual articular surface and all articular surfaces combined. For the calculation of sensitivity and specificity, the cartilage grades assigned at MRI were classified as either the absence (MRI grade 0) or presence (MRI grades 1, 2A, 2B, and 3) of a cartilage lesion on each articular surface. Standard errors of the mean were calculated by bootstrapping patients to account for dependence within patients between the two readers and among the six articular surfaces [38]. The McNemar test was used to compare differences in the diagnostic performance between the 2D FSE sequences, the 3D B AJR:205, August
4 TABLE 2: Sensitivity and Specificity of 2D Fast Spin-Echo (FSE) Sequences, 3D FSE Sequence With Conventional, and 3D FSE Sequence With Radial and Conventional for Detecting Each Grade and All Grades of Surgically Confirmed Cartilage Lesions on All Articular Surfaces of the Knee Joint for Both Readers Combined Arthroscopic Grade Coronal 2D FSE Grade 1 (n = 40) 16.3 (13/80) [ ] Grade 2A (n = 106) 49.5 a (105/212) [ ] Grade 2B (n = 137) 82.8 a (227/274) [ ] Grade 3 (n = 45) 97.8 (88/90) [ ] All grades (n = 328) 66.0 a (433/656) [ ] FSE sequence with conventional reformatted images, and the 3D FSE sequence with radial and conventional reformatted images. The proportions of cartilage lesions graded identically at MRI and arthroscopy were calculated for the 2D FSE sequences, 3D FSE sequence with conventional reformatted images, and the 3D FSE sequence with radial and conventional reformatted images. Kappa statistics were used to assess interobserver agreement between the two radiologists for determining the presence and absence of cartilage lesions on each articular surface of the knee joint using the 2D FSE sequences, 3D FSE sequence with conventional reformatted images, and 3D FSE sequence with radial and conventional reformatted images. Standard errors of the mean were calculated by bootstrapping patients [38]. McNemar test was used to compare differences in the proportion of correctly graded cartilage lesions and kappa values among the three groups. Results There were 328 surgically confirmed cartilage lesions within the knee joints of the 150 patients in the study group. The sensitivity and specificity for detecting all grades of cartilage lesions on all articular surfaces of the knee joint were 66.0% and 90.7%, respectively, for the 2D FSE sequences; 66.2% and 88.0%, respectively, for the 3D FSE sequence with conventional reformatted images; and 74.2% and 91.0%, respectively, for the 3D FSE sequence with radial and conventional reformatted images. The 3D FSE Sensitivity Coronal 3D FSE 21.3 (17/80) [ ] 51.9 b (110/212) [ ] 79.9 b (219/274) [ ] 97.8 (88/90) [ ] 66.2 b (434/656) [ ] 3D FSE With Radial and Conventional 23.8 (19/80) [ ] 64.2 a,b (136/212) [ ] 88.7 a,b (243/274) [ ] 98.9 (89/90) [ ] 74.2 a,b (487/656) [ ] Coronal 2D FSE sequence with radial and conventional reformatted images had statistically significantly higher sensitivity (p < 0.001) and similar specificity (p = 0.73), when compared with the 2D FSE sequences for detecting cartilage lesions, and statistically significantly higher sensitivity (p < 0.001) and specificity (p = 0.002) than the 3D FSE sequence with conventional reformatted images for detecting cartilage lesions. The 3D FSE sequence with conventional reformatted images had similar sensitivity (p = 0.93) and statistically significantly lower specificity (p = 0.005) than the 2D FSE sequences for detecting cartilage lesions (Table 2). The 3D FSE sequence with radial and conventional reformatted images had statistically significantly higher sensitivity for detecting 106 superficial partial-thickness cartilage lesions and 137 deep partial-thickness cartilage lesions when compared with the 2D FSE sequences (p < for superficial partial-thickness cartilage lesions and p = for deep partial-thickness cartilage lesions) and the 3D FSE sequence with conventional reformatted images (p < for both superficial and deep partial thickness cartilage lesions). The 3D FSE sequence with radial and conventional reformatted images had similar sensitivity for detecting 40 areas of cartilage softening and 45 full-thickness cartilage lesions when compared with the 2D FSE sequences (p = for cartilage softening and p = 1.00 for Specificity Coronal 3D FSE 3D FSE With Radial and Conventional NA NA NA NA NA NA NA NA NA NA NA NA 90.7 c (1038/1144) [ ] 88.0 b,c (1007/1144) [ ] 91.0 b (1041/1144) [ ] Note Data are percentage (numerator/denominator) [95% CI]. NA = not applicable (i.e., specificity cannot be calculated for individual grades of cartilage lesions). a Statistically significant difference at p < 0.05 between 3D FSE sequence with radial and conventional reformatted images and 2D FSE sequences. b Statistically significant difference at p < 0.05 between 3D FSE sequence with radial and conventional reformatted images and 3D FSE sequence with conventional reformatted images. c Statistically significant difference at p < 0.05 between 2D FSE sequences and 3D FSE sequence with conventional reformatted images. full-thickness cartilage lesions) and the 3D FSE sequence with conventional reformatted images (p = for cartilage softening and p = 1.00 for full-thickness cartilage lesions) (Table 2). The use of the radial reformatted images subjectively improved the ability to visualize 54 surgically confirmed partial-thickness cartilage lesions for reader 1 and 74 surgically confirmed partialthickness cartilage lesions for reader 2 when compared with the use of the sagittal 3D FSE source images and conventional reformatted images only (Figs. 1 4). The 3D FSE sequence with radial and conventional reformatted images had statistically significantly higher sensitivity for detecting cartilage lesions on the patella (p = 0.022), trochlea (p = 0.036), medial tibial plateau (p = 0.018), and lateral tibial plateau (p < 0.001) and similar sensitivity for detecting cartilage lesions on the medial femoral condyle (p = 0.061) and lateral femoral condyle (p = 0.743) when compared with the 2D FSE sequences. The 3D FSE sequence with radial and conventional reformatted images had statistically significantly higher sensitivity for detecting cartilage lesions on the trochlea (p = 0.048), medial femoral condyle (p = 0.006), and medial tibial plateau (p = 0.024) and similar sensitivity for detecting cartilage lesions on the patella (p = 0.219), lateral femoral condyle (p = 0.187), and lateral tibial plateau (p = 0.134) when compared with the 3D FSE sequence with conventional reformatted 374 AJR:205, August 2015
5 Isotropic Resolution 3D FSE MRI of Articular Cartilage of Knee Joint A D B E Fig year-old man with surgically confirmed grade 2B cartilage lesion on medial femoral condyle. A, Sagittal intermediate-weighted 2D fast spin-echo (FSE) image shows normal-appearing cartilage (arrow) on medial femoral condyle. B, Sagittal fat-suppressed T2-weighted 2D FSE image shows linear area of high signal intensity (arrow) within cartilage on medial femoral condyle. C, Sagittal 3D FSE reformatted image shows decreased conspicuity of linear area of high signal intensity (arrow) within cartilage on medial femoral condyle due to image blurring. D and E, Radial 3D FSE reformatted images display well-defined deep partial-thickness cartilage flap tear (arrows) on medial femoral condyle. TABLE 3: Sensitivity and Specificity of 2D Fast-Spin Echo (FSE) Sequences, 3D FSE Sequence With Conventional Reformatted Images, and 3D FSE Sequence With Radial and Conventional for Detecting All Grades of Surgically Confirmed Cartilage Lesions on Each Articular Surface of the Knee Joint for Both Readers Combined Articular Surface Coronal 2D FSE Patella (n = 83) 83.1 a (138/166) [ ] Trochlea (n = 51) 72.5 a (74/102) Medial femoral condyle (n = 67) Lateral femoral condyle (n = 30) Medial tibial plateau (n = 38) Lateral tibial plateau (n = 55) 64.2 (86/134) [ ] 66.7 (40/60) [ ] 44.7 a (34/76) [ ] 51.7 a,c (61/118) [ ] Sensitivity 3D FSE With Conventional 84.9 b (141/166) 70.6 (72/102) 60.4 b (81/134) [ ] 58.3 (35/60) 44.7 b (34/76) 60.2 c (71/118) 3D FSE With Radial and Conventional 88.0 a,b (146/166) [ ] 78.4 a (80/102) [ ] 71.6 b (96/134) [ ] 68.3 (41/60) [ ] 59.2 a,b (45/76) [ ] 66.9 a (79/118) [ ] Coronal 2D FSE 76.9 a (103/134) [ ] 89.9 c (178/198) [ ] 95.2 (158/166) [ ] 94.6 (227/240) [ ] 90.6 (203/224) [ ] 92.9 (169/182) [ ] Specificity 3D FSE With Conventional 75.4 b (101/134) [ ] 84.3 c (167/198) [ ] 94.6 (157/166) [ ] 92.1 (221/240) [ ] 88.4 b (198/224) [ ] 89.6 (163/182) [ ] C 3D FSE With Radial and Conventional 84.3 a,b (113/134) [ ] 87.4 (173/198) [ ] 94.0 (156/166) [ ] 92.1 (221/240) [ ] 94.2 b (211/224) [ ] 91.8 (167/182) [ ] Note Data are percentage (numerator/denominator) [95% CI]. a Statistically significant difference at p < 0.05 between 3D FSE sequence with radial and conventional reformatted images and 2D FSE sequences. b Statistically significant difference at p < 0.05 between 3D FSE sequence with radial and conventional reformatted images and 3D FSE sequence with conventional reformatted images. c Statistically significant difference at p < 0.05 between 2D FSE sequences and 3D FSE sequence with conventional reformatted images. AJR:205, August
6 images. The 3D FSE sequence with radial and conventional reformatted images had statistically significantly higher specificity for detecting cartilage lesions on the patella (p = 0.008) when compared with the 2D FSE sequences and on the patella (p = 0.005) and medial tibial plateau (p = 0.010) when compared with the 3D FSE sequence with conventional reformatted images (Table 3). The proportion of cartage lesions graded identically on MRI and arthroscopy was 33.8% (95% CI, %) for the 2D FSE sequences, 29.4% (95% CI, %) for the 3D FSE sequence with conventional reformatted images, and 40.5% (95% CI, %) for the 3D FSE sequence with radial and conventional reformatted images. The 3D FSE sequence with radial and conventional reformatted images had a statistically significantly higher proportion of correctly graded cartilage lesions than did the 2D FSE sequences (p = 0.001) and the 3D FSE sequence with conventional reformatted images (p < 0.001). There was no statistically significant difference (p = 0.15) in the proportion of correctly graded cartilage lesions between the 2D FSE sequences and the 3D FSE sequence with conventional reformatted images. The kappa value for interobserver agreement between the two radiologists for determining the presence or absence of cartilage lesions on each articular surface of the knee joint was 0.70 (95% CI, ) for the 2D FSE sequence, 0.67 (95% CI, ) for the 3D FSE sequence with conventional reformatted images, and 0.71 (95% CI, ) for the 3D FSE sequence with radial and conventional reformatted images. There was no statistically significant difference (p = ) in kappa values between the 2D FSE sequences, the 3D FSE sequence with conventional reformatted images, and the 3D FSE sequence with radial and conventional reformatted images. Discussion Our study has shown that a 3D FSE sequence can significantly improve the diagnostic performance of MRI for evaluating the articular cartilage of the knee joint at 3 T when compared with commonly used 2D FSE sequences. However, the improved ability of the 3D FSE sequence to detect and accurately grade cartilage lesions was evident only when the full advantage of the isotropic voxel acquisition was exploited by using radial reformatted images along with the sagittal source images and conventional axial, sagittal, and coronal reformatted images to evaluate articular cartilage. Radial imaging has been used for years to detect labral tears and cartilage lesions within the hip joint [30 33], labral tears within the shoulder joint [39], and meniscus tears within the knee joint [40]. However, to our knowledge, no previous study has evaluated the use of alternative imaging planes, neither those obtained using dedicated acquisitions nor reformations created from volumetric source data, for evaluating the articular cartilage of the knee joint. Three-dimensional FSE sequences offer many potential advantages over 2D FSE sequences for evaluating articular cartilage, including higher cartilage signal-to-noise ratio, improved tissue contrast, and the ability to acquire thin continuous slices, which reduce the effects of through-plane partial volume averaging [27, 28]. However, our study A C D Fig year-old woman with surgically confirmed grade 2A cartilage lesion on femoral trochlea. A C, Sagittal intermediate-weighted 2D fast spin-echo (FSE) image (A), sagittal fat-suppressed T2-weighted 2D FSE image (B), and sagittal 3D FSE reformatted image (C) show normal-appearing cartilage (arrows) on femoral trochlea. D, Radial 3D FSE reformatted image shows small superficial partial-thickness cartilage fissure (arrow) on femoral trochlea. found that a 3D FSE sequence with conventional axial, sagittal, and coronal reformatted images had similar sensitivity and statistically significantly lower specificity for detecting surgically confirmed cartilage lesions within the knee joint when compared with 2D FSE sequences. The lower specificity of the 3D FSE sequence may be due to its lower in-plane spatial resolution and greater image blurring from the acquisition of high spatial frequencies late in the echo train [27]. In addition, the longer imaging time may have resulted in increased patient motion artifact. The combination of factors may have caused the smooth surface of normal articular cartilage to appear irregular and ill-defined, simulating the appearance of cartilage fibrillation or fissuring. Our results have confirmed the findings of previous studies that have also failed to B 376 AJR:205, August 2015
7 Isotropic Resolution 3D FSE MRI of Articular Cartilage of Knee Joint A C D Fig year-old man with surgically confirmed grade 2A cartilage lesion on lateral tibial plateau. A C, Coronal intermediate-weighted 2D fast spin-echo (FSE) image (A), coronal fat-suppressed intermediateweighted 2D FSE image (B), and coronal 3D FSE reformatted image (C) show normal-appearing cartilage (arrows) on lateral tibial plateau. D, Radial 3D FSE reformatted image shows small superficial partial-thickness cartilage fissure (arrow) on lateral tibial plateau. B document a diagnostic superiority of 3D sequences with reformatted images in conventional planes over 2D FSE sequences for evaluating the articular cartilage of the knee joint. Kijowski et al. [18] found that a 3D FSE sequence had significantly higher sensitivity but significantly lower specificity for detecting 189 surgically confirmed cartilage lesions within the knee joint. In addition, studies performed by Kudo et al. [21] and Milewski et al. [16] showed similar diagnostic performance of 2D FSE and 3D FSE sequences for detecting smaller numbers of cartilage lesions in patients with arthroscopic correlation. Studies comparing 3D steadystate free-precession [15, 19, 22] and gradient recall-echo acquired in the steady-state [20] sequences with 2D FSE sequences have also shown similar sensitivities and specificities for detecting surgically confirmed cartilage within the knee joint, indicating that performance issues are not unique to 3D FSE sequences. Thus, it is possible that the theoretic advantages of 3D sequences simply do not translate into improved diagnostic performance over 2D FSE sequences when only using reformatted images in the conventional axial, sagittal, and coronal planes. Our study found that the use of a 3D FSE sequence with radial and conventional reformatted images improved the sensitivity for detecting cartilage lesions on all articular surfaces of the knee joint when compared with 2D FSE sequences, although differences were statistically significant only for the patella, trochlea, medial tibial plateau, and lateral tibial plateau. The lack of significant improvement in the detection of cartilage lesions on the curved surfaces of the medial and lateral femoral condyles is somewhat unexpected. However, there was a trend toward significance (p = 0.061) for the difference in the sensitivities of the 2D FSE and 3D FSE sequences for detecting cartilage lesions on the medial femoral condyle, whereas the small number of cartilage lesions on the lateral femoral condyle may have reduced the statistical power. The improvement in the detection of cartilage lesions on the medial tibial plateau and lateral tibial plateau with use of the radial reformatted images is substantial in that multiple prior studies using both 2D FSE sequences and various 3D sequences have documented poor sensitivity for detecting cartilage lesions on these articular surfaces [15 22]. The ability to visualize cartilage at multiple different orientations may provide readers with more diagnostic confidence for detecting cartilage lesions in areas of the tibia plateau, such as the peripheral margins and adjacent to the intercondylar notch, which are often difficult to characterize using conventional imaging planes. Previously published studies investigating the usefulness of 3D sequences for evaluating articular cartilage and other joint structures have limited evaluation to the conventional axial, sagittal, and coronal planes; thus, the full potential of the volumetric source data has not been used [15 22]. The benefit of 3D isotropic resolution acquisitions is an unlimited number of possibilities for image reformation. Creating radial and other unconventional reformatted images can be quickly and easily performed on commercially available MRI workstations. Furthermore, most commercially available PACS workstations have the ability to reformat 3D sequences in any orientation. Radial reformatted images were used in our study as a standardized easily reproducible method to determine whether the addition of images in unconventional orientations could improve the diagnostic performance of a 3D FSE sequence for evaluating the articular cartilage of the knee joint. The improvement in diagnostic performance was significant but not as dramatic as expected. However, the results are encouraging and advocate for better utilization of the volumetric source data when using 3D sequences for musculoskeletal imaging. Our study has several limitations. One limitation was the presence of selection bias because our study group consisted of only a subset of all patients at our institution who underwent MRI of the knee during the time the study was being performed. An additional limitation was that image evaluation was AJR:205, August
8 performed in a retrospective manner. As a result, the readers were aware that all patients had undergone subsequent arthroscopic knee surgery, which could have potentially biased their interpretations when evaluating the articular cartilage. Furthermore, information regarding the presence or absence of cartilage lesions on each articular surface of the knee joint at arthroscopy was obtained by retrospective review of the surgical reports. Thus, it is possible that cartilage lesions could have been missed at arthroscopy and errors could have been made when describing the arthroscopic findings in the surgical report. The retrospective nature of the study also prevented a detailed analysis of the clinical significance of the improved detection of cartilage lesions using the radial reformatted images and whether the identification of additional cartilage lesions actually influenced treatment decisions, ultimately affecting patient outcome. Another limitation was that our study did not investigate the diagnostic performance of the radial reformatted images alone for evaluating articular cartilage. However, the objective of the study was to create a typical clinical scenario in which the radial reformatted images would be used along with the conventional reformatted images and 3D FSE source images to grade each articular surface of the knee joint. Furthermore, the readers were not blinded to the MRI sequences they were using for cartilage evaluation and the surgeons were not blinded to the official interpretations of the MRI examinations, which were made without the use of the 3D FSE radial reformatted images. Both factors may have contributed to bias when determining the presence or absence of cartilage lesions on MRI and at arthroscopy. An additional limitation of our study was the lag time between MRI and arthroscopy of up to 6 months, which may have allowed the development or progression of cartilage lesions in some individuals. A final limitation was the assumption that grading of articular cartilage at arthroscopy was unequivocally accurate and reproducible. Arthroscopy is an imperfect reference standard for evaluating articular cartilage, and it is especially difficult for orthopedic surgeons to reliably identify cartilage softening and to distinguish between deep and superficial partial-thickness cartilage lesions at arthroscopy [41]. In conclusion, our study has shown the benefit of using radial reformatted images created from volumetric source data for evaluating the articular cartilage of the knee joint. Although radial reformatted images can be quickly and easily created on commercially available MRI workstations, additional time is required to review the images. Thus, the use of radial imaging may not be feasible when evaluating every patient with joint pain undergoing routine MRI. For this reason, the use of radial or other unconventional imaging planes may be best suited for certain patient populations for whom accurate cartilage assessment is clinically important, such as individuals with knee pain and no evidence of internal derangement, individuals being imaged before cartilage repair procedures, and individuals with persistent knee pain after surgical interventions. Additional studies are needed to further investigate the use of unconventional imaging planes for evaluating articular cartilage and other joint structures in clinical practice. Further research should also focus on determining the best combination of 2D FSE and 3D sequences with both conventional and unconventional reformatted images that would minimize acquisition time and expedite workflow, while maintaining high diagnostic performance for providing comprehensive joint assessment. References 1. Centers for Disease Control and Prevention (CDC). Arthritis: meeting the challenge of living well at a glance CDC website. chronicdisease/resources/publications/aag/arthritis. htm. Published Accessed April 20, Felson DT. An update on the pathogenesis and epidemiology of osteoarthritis. Radiol Clin North Am 2004; 42: Altman RD. Early management of osteoarthritis. Am J Manag Care 2010; 16(suppl management):s41 S47 4. Jakob RP, Franz T, Gautier E, Mainil-Varlet P. Autologous osteochondral grafting in the knee: indication, results, and reflections. Clin Orthop Relat Res 2002; Brittberg M, Lindahl A, Nilsson A, Ohlsson C, Isaksson O, Peterson L. Treatment of deep cartilage defects in the knee with autologous chondrocyte transplantation. N Engl J Med 1994; 331: Mazor M, Lespessailles E, Coursier R, Daniellou R, Best TM, Toumi H. Mesenchymal stem-cell potential in cartilage repair: an update. J Cell Mol Med 2014; 18: Bhardwaj N, Devi D, Mandal BB. Tissue-engineered cartilage: the crossroads of biomaterials, cells and stimulating factors. Macromol Biosci 2015; 15: Pelletier JP, Martel-Pelletier J. DMOAD developments: present and future. Bull NYU Hosp Jt Dis 2007; 65: Qvist P, Bay-Jensen AC, Christiansen C, Dam EB, Pastoureau P, Karsdal MA. The disease modifying osteoarthritis drug (DMOAD): is it in the horizon? Pharmacol Res 2008; 58: Hellio Le Graverand-Gastineau MP. OA clinical trials: current targets and trials for OA choosing molecular targets. What have we learned and where we are headed? Osteoarthritis Cartilage 2009; 17: Hunter DJ, Hellio Le Graverand-Gastineau MP. How close are we to having structure-modifying drugs available? Med Clin North Am 2009; 93: [xiii] 12. Link TM, Stahl R, Woertler K. Cartilage imaging: motivation, techniques, current and future significance. Eur Radiol 2007; 17: Roemer FW, Crema MD, Trattnig S, Guermazi A. Advances in imaging of osteoarthritis and cartilage. Radiology 2011; 260: Winalski CS, Rajiah P. The evolution of articular cartilage imaging and its impact on clinical practice. Skeletal Radiol 2011; 40: Duc SR, Pfirrmann CW, Schmid MR, et al. Articular cartilage defects detected with 3D waterexcitation true FISP: prospective comparison with sequences commonly used for knee imaging. Radiology 2007; 245: Milewski MD, Smitaman E, Moukaddam H, et al. Comparison of 3D vs. 2D fast spin echo imaging for evaluation of articular cartilage in the knee on a 3T system scientific research. Eur J Radiol 2012; 81: Ristow O, Steinbach L, Sabo G, et al. Isotropic 3D fast spin-echo imaging versus standard 2D imaging at 3.0 T of the knee: image quality and diagnostic performance. Eur Radiol 2009; 19: Kijowski R, Davis KW, Woods MA, et al. Knee joint: comprehensive assessment with 3D isotropic resolution fast spin-echo MR imaging diagnostic performance compared with that of conventional MR imaging at 3.0 T. Radiology 2009; 252: Kijowski R, Blankenbaker DG, Klaers JL, Shinki K, De Smet AA, Block WF. Vastly undersampled isotropic projection steady-state free precession imaging of the knee: diagnostic performance compared with conventional MR. Radiology 2009; 251: Kijowski R, Blankenbaker DG, Woods MA, Shinki K, De Smet AA, Reeder SB. 3.0-T evaluation of knee cartilage by using three-dimensional IDEAL GRASS imaging: comparison with fast spin-echo imaging. Radiology 2010; 255: Kudo H, Inaoka T, Kitamura N, et al. Clinical value of routine use of thin-section 3D MRI using 3D FSE sequences with a variable flip angle technique for internal derangements of the knee joint 378 AJR:205, August 2015
9 Isotropic Resolution 3D FSE MRI of Articular Cartilage of Knee Joint at 3T. Magn Reson Imaging 2013; 31: MRI of the knee with 3D fast spin-echo extended diographics 2013; 33:E97 E Duc SR, Koch P, Schmid MR, Horger W, Hodler echo-train acquisition (XETA): initial experience. 35. Potter HG, Linklater JM, Allen AA, Hannafin JA, J, Pfirrmann CW. Diagnosis of articular cartilage abnormalities of the knee: prospective clinical evaluation of a 3D water-excitation true FISP sequence. Radiology 2007; 243: Kijowski R, Blankenbaker DG, Woods M, Del Rio AM, De Smet AA, Reeder SB. Clinical usefulness of adding 3D cartilage imaging sequences to a routine knee MR protocol. AJR 2011; 196: Kijowski R, Lu A, Block W, Grist T. Evaluation of the articular cartilage of the knee joint with vastly undersampled isotropic projection reconstruction steady-state free precession imaging. J Magn Reson Imaging 2006; 24: Gold GE, Hargreaves BA, Vasanawala SS, et al. Articular cartilage of the knee: evaluation with fluctuating equilibrium MR imaging initial experience in healthy volunteers. Radiology 2006; 238: Gold GE, Reeder SB, Yu H, et al. Articular cartilage of the knee: rapid three-dimensional MR imaging at 3.0 T with IDEAL balanced steady-state free precession initial experience. Radiology 2006; 240: Gold GE, Busse RF, Beehler C, et al. Isotropic AJR 2007; 188: Chen CA, Lu W, John CT, et al. Multiecho IDEAL gradient-echo water-fat separation for rapid assessment of cartilage volume at 1.5 T: initial experience. Radiology 2009; 252: Kijowski R. Three-dimensional magnetic resonance imaging of joints. Top Magn Reson Imaging 2010; 21: Yoon LS, Palmer WE, Kassarjian A. Evaluation of radial-sequence imaging in detecting acetabular labral tears at hip MR arthrography. Skeletal Radiol 2007; 36: Horii M, Kubo T, Hirasawa Y. Radial MRI of the hip with moderate osteoarthritis. J Bone Joint Surg Br 2000; 82: Kubo T, Horii M, Harada Y, et al. Radial-sequence magnetic resonance imaging in evaluation of acetabular labrum. J Orthop Sci 1999; 4: Lattanzi R, Petchprapa C, Ascani D, et al. Detection of cartilage damage in femoroacetabular impingement with standardized dgemric at 3 T. Osteoarthritis Cartilage 2014; 22: Petchprapa CN, Dunham KS, Lattanzi R, Recht MP. Demystifying radial imaging of the hip. Ra- Haas SB. Magnetic resonance imaging of articular cartilage in the knee: an evaluation with use of fast-spin-echo imaging. J Bone Joint Surg Am 1998; 80: Sonin AH, Pensy RA, Mulligan ME, Hatem S. Grading articular cartilage of the knee using fast spin-echo proton density-weighted MR imaging without fat suppression. AJR 2002; 179: Noyes FR, Stabler CL. A system for grading articular cartilage lesions at arthroscopy. Am J Sports Med 1989; 17: De Angelis D, Young G. Bootstrap method. In: Armitage P, Colton T, eds. Encyclopedia of biostatistics, 2nd ed. Hoboken, NJ: Wiley, Munk PL, Holt RG, Helms CA, Genant HK. Glenoid labrum: preliminary work with use of radial-sequence MR imaging. Radiology 1989; 173: Quinn SF, Brown TR, Szumowski J. Menisci of the knee: radial MR imaging correlated with arthroscopy in 259 patients. Radiology 1992; 185: Cameron ML, Briggs KK, Steadman JR. Reproducibility and reliability of the Outerbridge classification for grading chondral lesions of the knee arthroscopically. Am J Sports Med 2003; 31:83 86 AJR:205, August
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
Sensitivity and Specificity in Detection of Labral Tears with 3.0-T MRI of the Shoulder
 Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Comparative study of imaging at 3.0 T versus 1.5 T of the knee
 Skeletal Radiol (2009) 38:761 769 DOI 10.1007/s00256-009-0683-0 SCIENTIFIC ARTICLE Comparative study of imaging at 3.0 T versus 1.5 T of the knee Scott Wong & Lynne Steinbach & Jian Zhao & Christoph Stehling
Skeletal Radiol (2009) 38:761 769 DOI 10.1007/s00256-009-0683-0 SCIENTIFIC ARTICLE Comparative study of imaging at 3.0 T versus 1.5 T of the knee Scott Wong & Lynne Steinbach & Jian Zhao & Christoph Stehling
dgemric Effectively Predicts Cartilage Damage Associated with Femoroacetabular Impingement
 Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
Imaging of Articular Cartilage
 Clinical Imaging of Articular Cartilage Imaging of Articular Cartilage Prof. Dr. K. Verstraete Ghent University Introduction : Articular Cartilage Histology and biochemical composition Review of Imaging
Clinical Imaging of Articular Cartilage Imaging of Articular Cartilage Prof. Dr. K. Verstraete Ghent University Introduction : Articular Cartilage Histology and biochemical composition Review of Imaging
Quantitative Comparison of 2D and 3D MRI Techniques for the Evaluation of Chondromalacia Patellae in 3.0T MR Imaging of the Knee
 doi: 10.5505/actamedica.2016.81905 Acta Medica Anatolia Volume 4 Issue 3 2016 Quantitative Comparison of 2D and 3D MRI Techniques for the Evaluation of Chondromalacia Patellae in 3.0T MR Imaging of the
doi: 10.5505/actamedica.2016.81905 Acta Medica Anatolia Volume 4 Issue 3 2016 Quantitative Comparison of 2D and 3D MRI Techniques for the Evaluation of Chondromalacia Patellae in 3.0T MR Imaging of the
Articular cartilage and labral lesions of the glenohumeral joint: diagnostic performance of 3D water-excitation true FISP MR arthrography
 Skeletal Radiol (2010) 39:473 480 DOI 10.1007/s00256-009-0844-1 SCIENTIFIC ARTICLE Articular cartilage and labral lesions of the glenohumeral joint: diagnostic performance of 3D water-excitation true FISP
Skeletal Radiol (2010) 39:473 480 DOI 10.1007/s00256-009-0844-1 SCIENTIFIC ARTICLE Articular cartilage and labral lesions of the glenohumeral joint: diagnostic performance of 3D water-excitation true FISP
Usefulness of Unenhanced MRI and MR Arthrography of the Shoulder in Detection of Unstable Labral Tears
 Musculoskeletal Imaging Original Research Unenhanced MRI and MR rthrography for Unstable Labral Tears Musculoskeletal Imaging Original Research Thomas 1,2 T Keywords: labral tear, MRI, shoulder DOI:10.2214/JR.14.14262
Musculoskeletal Imaging Original Research Unenhanced MRI and MR rthrography for Unstable Labral Tears Musculoskeletal Imaging Original Research Thomas 1,2 T Keywords: labral tear, MRI, shoulder DOI:10.2214/JR.14.14262
Modified Oblique Sagittal Magnetic Resonance Imaging of Rotator Cuff Tears: Comparison with Standard Oblique Sagittal Images
 Journal of Magnetics 22(3), 519-524 (2017) ISSN (Print) 1226-1750 ISSN (Online) 2233-6656 https://doi.org/10.4283/jmag.2017.22.3.519 Modified Oblique Sagittal Magnetic Resonance Imaging of Rotator Cuff
Journal of Magnetics 22(3), 519-524 (2017) ISSN (Print) 1226-1750 ISSN (Online) 2233-6656 https://doi.org/10.4283/jmag.2017.22.3.519 Modified Oblique Sagittal Magnetic Resonance Imaging of Rotator Cuff
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Prevalence of Meniscal Radial Tears of the Knee Revealed by MRI After Surgery
 Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Meniscal Tears: Role of Axial MRI Alone and in Combination with Other Imaging Planes
 Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
Intramuscular Rotator Cuff Cysts: Association with Tendon Tears on MRI and Arthroscopy
 Kassarjian et al. MRI of Rotator Cuff Cysts and Tendon Tears Musculoskeletal Imaging Clinical Observations Ara Kassarjian 1 Martin Torriani Hugue Ouellette William E. Palmer Kassarjian A, Torriani M, Ouellette
Kassarjian et al. MRI of Rotator Cuff Cysts and Tendon Tears Musculoskeletal Imaging Clinical Observations Ara Kassarjian 1 Martin Torriani Hugue Ouellette William E. Palmer Kassarjian A, Torriani M, Ouellette
Added value of MR myelography using 3D COSMIC sequence in the diagnosis of lumbar canal stenosis: comparison with routine MR imaging
 Added value of MR myelography using 3D COSMIC sequence in the diagnosis of lumbar canal stenosis: comparison with routine MR imaging Poster No.: C-1099 Congress: ECR 2012 Type: Authors: Scientific Exhibit
Added value of MR myelography using 3D COSMIC sequence in the diagnosis of lumbar canal stenosis: comparison with routine MR imaging Poster No.: C-1099 Congress: ECR 2012 Type: Authors: Scientific Exhibit
MR Imaging of a Posterior Root Tear of the Medial Meniscus: Diagnostic Accuracy of Various Tear Configurations and
 MR Imaging of a Posterior Root Tear of the Medial Meniscus: Diagnostic Accuracy of Various Tear Configurations and Associated Knee Abnormalities 1 Hyang Mi Lee, M.D., Jae Chan Shim, M.D., Jin Goo Kim,
MR Imaging of a Posterior Root Tear of the Medial Meniscus: Diagnostic Accuracy of Various Tear Configurations and Associated Knee Abnormalities 1 Hyang Mi Lee, M.D., Jae Chan Shim, M.D., Jin Goo Kim,
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
Clinical Cartilage Imaging of the Knee and Hip Joints
 Musculoskeletal Imaging Review Kijowski Imaging of the Knee and Hip Joints Musculoskeletal Imaging Review Richard Kijowski 1 Kijowski R FOCUS ON: Keywords: articular cartilage, hip, knee, MRI DOI:10.2214/JR.10.4661
Musculoskeletal Imaging Review Kijowski Imaging of the Knee and Hip Joints Musculoskeletal Imaging Review Richard Kijowski 1 Kijowski R FOCUS ON: Keywords: articular cartilage, hip, knee, MRI DOI:10.2214/JR.10.4661
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
Echelon Oval provides a robust suite of leading musculoskeletal imaging capabilities for detailed assessment of all anatomy for your most challenging
 Echelon Oval provides a robust suite of leading musculoskeletal imaging capabilities for detailed assessment of all anatomy for your most challenging cases. Hitachi Medical Systems America, Inc. 1959 Summit
Echelon Oval provides a robust suite of leading musculoskeletal imaging capabilities for detailed assessment of all anatomy for your most challenging cases. Hitachi Medical Systems America, Inc. 1959 Summit
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration
 Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings
 Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Post-injury painful and locked knee
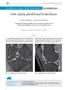 H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
Acute Injury of the Articular Cartilage and Subchondral Bone: A Common but Unrecognized Lesion in the Immature Knee
 Rachel S. Oeppen 1,2 Susan. Connolly 3 Jenny T. encardino 4 Diego Jaramillo 1 Received May 19, 2003; accepted after revision July 28, 2003. 1 Department of Pediatric Radiology, Massachusetts General Hospital,
Rachel S. Oeppen 1,2 Susan. Connolly 3 Jenny T. encardino 4 Diego Jaramillo 1 Received May 19, 2003; accepted after revision July 28, 2003. 1 Department of Pediatric Radiology, Massachusetts General Hospital,
Why Talk About Technique? MRI of the Knee:
 Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
CT ARTHROGRAPHY It s not Always About the
 CT ARTHROGRAPHY It s not Always About the Magnet Kirkland W. Davis, M.D. University of Wisconsin Department of Radiology Disclosures Financial FDA IA Gd! What Is CT Arthrography? (CTR) Arthrogram: imaging
CT ARTHROGRAPHY It s not Always About the Magnet Kirkland W. Davis, M.D. University of Wisconsin Department of Radiology Disclosures Financial FDA IA Gd! What Is CT Arthrography? (CTR) Arthrogram: imaging
FieldStrength. Achieva 3.0T enables cutting-edge applications, best-in-class MSK images
 FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
MRI of Osteochondral Defects of the Lateral Femoral Condyle: Incidence and Pattern of Injury After Transient Lateral Dislocation of the Patella
 Sanders et al. MRI of Osteochond ral Defects of the Lateral Femoral Condyle Musculoskeletal Imaging Clinical Observations A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:1332 1337 0361 803X/06/1875
Sanders et al. MRI of Osteochond ral Defects of the Lateral Femoral Condyle Musculoskeletal Imaging Clinical Observations A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:1332 1337 0361 803X/06/1875
Comparison of Three-dimensional Isotropic T1-weighted Fast Spin-Echo MR Arthrography with Two-dimensional MR Arthrography of the Shoulder 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Hye Jung Choo, MD
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Hye Jung Choo, MD
imri 2018;22:
 pissn 2384-1095 eissn 2384-1109 imri 2018;22:229-239 Diagnosis of Rotator Cuff Tears with Non-Arthrographic MR Imaging: 3D Fat-Suppressed Isotropic Intermediate-Weighted Turbo Spin-Echo Sequence versus
pissn 2384-1095 eissn 2384-1109 imri 2018;22:229-239 Diagnosis of Rotator Cuff Tears with Non-Arthrographic MR Imaging: 3D Fat-Suppressed Isotropic Intermediate-Weighted Turbo Spin-Echo Sequence versus
21 year-old collegiate rower: R/O labral tear
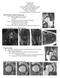 Hip MRI Primer AOSSM 2014 Hollis G. Potter, MD Chair, Department of Radiology & Imaging The Coleman Chair, MRI Research Hospital for Special Surgery Professor of Radiology Weill Medical College of Cornell
Hip MRI Primer AOSSM 2014 Hollis G. Potter, MD Chair, Department of Radiology & Imaging The Coleman Chair, MRI Research Hospital for Special Surgery Professor of Radiology Weill Medical College of Cornell
Viviane Khoury, MD. Assistant Professor Department of Radiology University of Pennsylvania
 U Penn Diagnostic Imaging: On the Cape Chatham, MA July 11-15, 2016 Viviane Khoury, MD Assistant Professor Department of Radiology University of Pennsylvania Hip imaging has changed in recent years: new
U Penn Diagnostic Imaging: On the Cape Chatham, MA July 11-15, 2016 Viviane Khoury, MD Assistant Professor Department of Radiology University of Pennsylvania Hip imaging has changed in recent years: new
Meniscal Tears with Fragments Displaced: What you need to know.
 Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
Tissue-engineered medical products Evaluation of anisotropic structure of articular cartilage using DT (Diffusion Tensor)-MR Imaging
 Provläsningsexemplar / Preview TECHNICAL REPORT ISO/TR 16379 First edition 2014-03-01 Tissue-engineered medical products Evaluation of anisotropic structure of articular cartilage using DT (Diffusion Tensor)-MR
Provläsningsexemplar / Preview TECHNICAL REPORT ISO/TR 16379 First edition 2014-03-01 Tissue-engineered medical products Evaluation of anisotropic structure of articular cartilage using DT (Diffusion Tensor)-MR
Original Article. Hyun Su Kim, MD 1, Young Cheol Yoon, MD 1, Jong Won Kwon, MD 1, Bong-Keun Choe, MD, PhD 2 INTRODUCTION
 Original Article http://dx.doi.org/10.3348/kjr.2012.13.4.443 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(4):443-449 Qualitative and Quantitative Assessment of Isotropic Ankle Magnetic Resonance
Original Article http://dx.doi.org/10.3348/kjr.2012.13.4.443 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(4):443-449 Qualitative and Quantitative Assessment of Isotropic Ankle Magnetic Resonance
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
When (How) MRI Became the Gold Standard Hollis G. Potter, MD
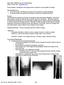 When (How) MRI Became the Gold Standard Hollis G. Potter, MD potterh@hss.edu Target audience: Radiologists and imaging scientists interested in assessing MRI of cartilage Outcome/Objectives: 1. To become
When (How) MRI Became the Gold Standard Hollis G. Potter, MD potterh@hss.edu Target audience: Radiologists and imaging scientists interested in assessing MRI of cartilage Outcome/Objectives: 1. To become
Lesions of the Menisci of the Knee: Value of MR Imaging Criteria for Recognition of Unstable Lesions
 B. C. Vande Berg 1 P. Poilvache 2 F. Duchateau 1 F. E. Lecouvet 1 J. E. Dubuc 2 B. Maldague 1 J. Malghem 1 Received June 12, 2000; accepted after revision August 24, 2000. 1 Department of Radiology, Cliniques
B. C. Vande Berg 1 P. Poilvache 2 F. Duchateau 1 F. E. Lecouvet 1 J. E. Dubuc 2 B. Maldague 1 J. Malghem 1 Received June 12, 2000; accepted after revision August 24, 2000. 1 Department of Radiology, Cliniques
Personalized Solutions. MRI Protocol for PSI and Signature Guides
 Personalized Solutions MRI Protocol for PSI and Signature Guides 2 Personalized Solutions MRI Protocol for PSI and Signature Guides Purpose and Summary This protocol is applicable for the Zimmer Biomet
Personalized Solutions MRI Protocol for PSI and Signature Guides 2 Personalized Solutions MRI Protocol for PSI and Signature Guides Purpose and Summary This protocol is applicable for the Zimmer Biomet
MR imaging of the knee in marathon runners before and after competition
 Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Arthroscopy / MRI Correlation Conference. Department of Radiology, Section of MSK Imaging Department of Orthopedic Surgery 7/19/16
 Arthroscopy / MRI Correlation Conference Department of Radiology, Section of MSK Imaging Department of Orthopedic Surgery 7/19/16 Case 1: 29 YOM with recurrent shoulder dislocations Glenoid Axial T1FS
Arthroscopy / MRI Correlation Conference Department of Radiology, Section of MSK Imaging Department of Orthopedic Surgery 7/19/16 Case 1: 29 YOM with recurrent shoulder dislocations Glenoid Axial T1FS
In vivo diffusion tensor imaging (DTI) of articular cartilage as a biomarker for osteoarthritis
 In vivo diffusion tensor imaging (DTI) of articular cartilage as a biomarker for osteoarthritis Jose G. Raya 1, Annie Horng 2, Olaf Dietrich 2, Svetlana Krasnokutsky 3, Luis S. Beltran 1, Maximilian F.
In vivo diffusion tensor imaging (DTI) of articular cartilage as a biomarker for osteoarthritis Jose G. Raya 1, Annie Horng 2, Olaf Dietrich 2, Svetlana Krasnokutsky 3, Luis S. Beltran 1, Maximilian F.
MRI of Cartilage. D. BENDAHAN (PhD)
 MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
KNEE ALIGNMENT SYSTEM (KAS) MRI Protocol
 KNEE ALIGNMENT SYSTEM (KAS) MRI Protocol Sample referral sticker Referral Sticker Insert here Corin 17 Bridge Street Pymble NSW Australia 2073 P: +61 (0)2 9497 7400 F: +61 (0)2 9497 7498 E: KAS.customerservice@coringroup.com
KNEE ALIGNMENT SYSTEM (KAS) MRI Protocol Sample referral sticker Referral Sticker Insert here Corin 17 Bridge Street Pymble NSW Australia 2073 P: +61 (0)2 9497 7400 F: +61 (0)2 9497 7498 E: KAS.customerservice@coringroup.com
JMSCR Vol 05 Issue 01 Page January
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
New Directions in Osteoarthritis Research
 New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
Musculoskeletal Imaging Clinical Observations
 MRI of Internal Impingement of the Shoulder Musculoskeletal Imaging Clinical Observations Eddie L. Giaroli 1 Nancy M. Major Laurence D. Higgins Giaroli EL, Major NM, Higgins LD DOI:10.2214/AJR.04.0971
MRI of Internal Impingement of the Shoulder Musculoskeletal Imaging Clinical Observations Eddie L. Giaroli 1 Nancy M. Major Laurence D. Higgins Giaroli EL, Major NM, Higgins LD DOI:10.2214/AJR.04.0971
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Three-Dimensional MRI of the Musculoskeletal System
 Musculoskeletal Imaging Review Naraghi and White 3D MRI of the Musculoskeletal System Musculoskeletal Imaging Review FOCUS ON: li Naraghi 1 Lawrence M. White Naraghi, White LM Keywords: 3D MRI, articular
Musculoskeletal Imaging Review Naraghi and White 3D MRI of the Musculoskeletal System Musculoskeletal Imaging Review FOCUS ON: li Naraghi 1 Lawrence M. White Naraghi, White LM Keywords: 3D MRI, articular
The clinical utility of a 3D-isotrophic-voxel MRI compared to a
 Chiba Medical J. 94E:1 ~ 8,2018 doi:10.20776/s03035476-94e-1-p1 Original Article The clinical utility of a 3D-isotrophic-voxel MRI compared to a 2D-radial sequence in diagnosis of hip labral tears Shigeo
Chiba Medical J. 94E:1 ~ 8,2018 doi:10.20776/s03035476-94e-1-p1 Original Article The clinical utility of a 3D-isotrophic-voxel MRI compared to a 2D-radial sequence in diagnosis of hip labral tears Shigeo
MRI of Bucket-Handle Te a rs of the Meniscus of the Knee 1
 MRI of ucket-handle Te a rs of the Meniscus of the Knee 1 Joon Yong Park, M.D., Young-uk Lee M.D., Eun-Chul Chung M.D., Hae-Won Park M.D., E u n - Kyung Youn M.D., Shin Ho Kook, M.D., Young Rae Lee, M.D.
MRI of ucket-handle Te a rs of the Meniscus of the Knee 1 Joon Yong Park, M.D., Young-uk Lee M.D., Eun-Chul Chung M.D., Hae-Won Park M.D., E u n - Kyung Youn M.D., Shin Ho Kook, M.D., Young Rae Lee, M.D.
Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of the Tibia
 Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Department of Orthopaedic Surgery, Tampere University Hospital, Tampere, Finland 3
 Scandinavian Journal of Surgery 101: 56 61, 2012 Sensitivity of MRI for articular cartilage lesions of the patellae V. M. Mattila 1, 2, M. Weckström 1, V. Leppänen 1, M. Kiuru 1, H. Pihlajamäki 1, 3 1
Scandinavian Journal of Surgery 101: 56 61, 2012 Sensitivity of MRI for articular cartilage lesions of the patellae V. M. Mattila 1, 2, M. Weckström 1, V. Leppänen 1, M. Kiuru 1, H. Pihlajamäki 1, 3 1
Classification of Acetabular Cartilage Lesions. Claudio Mella, MD
 Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Classification of Acetabular Cartilage Lesions Claudio Mella, MD Acetabular cartilage lesions are frequently found during hip arthroscopy. The arthroscopic view offers an exceptional perspective to assess
Conservative surgical treatments for osteoarthritis: A Finite Element Study
 Conservative surgical treatments for osteoarthritis: A Finite Element Study Diagarajen Carpanen, BEng (Hons), Franziska Reisse, BEng(Hons), Howard Hillstrom, PhD, Kevin Cheah, FRCS, Rob Walker, PhD, Rajshree
Conservative surgical treatments for osteoarthritis: A Finite Element Study Diagarajen Carpanen, BEng (Hons), Franziska Reisse, BEng(Hons), Howard Hillstrom, PhD, Kevin Cheah, FRCS, Rob Walker, PhD, Rajshree
MRI Characteristics of Healed and Unhealed Peripheral Vertical Meniscal Tears
 Musculoskeletal Imaging Original Research Kijowski et al. MRI of Peripheral Meniscal Tears Musculoskeletal Imaging Original Research Richard Kijowski 1 Humberto G. Rosas 1 Kenneth S. Lee 1 rnold Cheung
Musculoskeletal Imaging Original Research Kijowski et al. MRI of Peripheral Meniscal Tears Musculoskeletal Imaging Original Research Richard Kijowski 1 Humberto G. Rosas 1 Kenneth S. Lee 1 rnold Cheung
ACR MRI Accreditation: Medical Physicist Role in the Application Process
 ACR MRI Accreditation: Medical Physicist Role in the Application Process Donna M. Reeve, MS, DABR, DABMP Department of Imaging Physics University of Texas M.D. Anderson Cancer Center Educational Objectives
ACR MRI Accreditation: Medical Physicist Role in the Application Process Donna M. Reeve, MS, DABR, DABMP Department of Imaging Physics University of Texas M.D. Anderson Cancer Center Educational Objectives
Accuracy of SPECT bone scintigraphy in diagnosis of meniscal tears ABSTRACT
 1 Iran J Nucl Med 2005; 23 Accuracy of SPECT bone scintigraphy in diagnosis of meniscal tears M. Saghari 1, M. Moslehi 1, J. Esmaeili 2, M.N. Tahmasebi 3, A. Radmehr 4, M. Eftekhari 1,2, A. Fard-Esfahani
1 Iran J Nucl Med 2005; 23 Accuracy of SPECT bone scintigraphy in diagnosis of meniscal tears M. Saghari 1, M. Moslehi 1, J. Esmaeili 2, M.N. Tahmasebi 3, A. Radmehr 4, M. Eftekhari 1,2, A. Fard-Esfahani
Relaxometric Maps: Sequence Development and Clinical Impact. Initial Observations.
 Relaxometric Maps: Sequence Development and Clinical Impact. Initial Observations. Poster No.: C-0998 Congress: ECR 2011 Type: Scientific Exhibit Authors: E. Soscia, G. Palma, C. Sirignano, D. Iodice,
Relaxometric Maps: Sequence Development and Clinical Impact. Initial Observations. Poster No.: C-0998 Congress: ECR 2011 Type: Scientific Exhibit Authors: E. Soscia, G. Palma, C. Sirignano, D. Iodice,
Repeatability of 2D FISP MR Fingerprinting in the Brain at 1.5T and 3.0T
 Repeatability of 2D FISP MR Fingerprinting in the Brain at 1.5T and 3.0T Guido Buonincontri 1,2, Laura Biagi 1,3, Alessandra Retico 2, Michela Tosetti 1,3, Paolo Cecchi 4, Mirco Cosottini 1,4,5, Pedro
Repeatability of 2D FISP MR Fingerprinting in the Brain at 1.5T and 3.0T Guido Buonincontri 1,2, Laura Biagi 1,3, Alessandra Retico 2, Michela Tosetti 1,3, Paolo Cecchi 4, Mirco Cosottini 1,4,5, Pedro
Key words: arthroscopy, orthopaedic examination, magnetic resonance imaging, knee injury.
 Original paper Videosurgery Arthroscopic verification of objectivity of the orthopaedic examination and magnetic resonance imaging in intra-articular knee injury. Retrospective study Julian Dutka, Michał
Original paper Videosurgery Arthroscopic verification of objectivity of the orthopaedic examination and magnetic resonance imaging in intra-articular knee injury. Retrospective study Julian Dutka, Michał
Original Research Article
 Original Research Article Intermediate Weighted Fast Spin Echo (IW FSE) MR Imaging of Hyaline Cartilage Defects of the Knee: Comparison with the Fat Suppressed Three Dimensional Gradient Echo (3D SPGR)
Original Research Article Intermediate Weighted Fast Spin Echo (IW FSE) MR Imaging of Hyaline Cartilage Defects of the Knee: Comparison with the Fat Suppressed Three Dimensional Gradient Echo (3D SPGR)
Original Research Article
 Original Research Article Intermediate Weighted Fast Spin Echo (IW FSE) MR Imaging of Hyaline Cartilage Defects of the Knee: Comparison with the Fat Suppressed Three Dimensional Gradient Echo (3D SPGR)
Original Research Article Intermediate Weighted Fast Spin Echo (IW FSE) MR Imaging of Hyaline Cartilage Defects of the Knee: Comparison with the Fat Suppressed Three Dimensional Gradient Echo (3D SPGR)
Musculoskeletal Imaging Original Research
 Musculoskeletal Imaging Original Research Subhas et al. Comparison of Fast and Standard Shoulder MRI Protocols Musculoskeletal Imaging Original Research Naveen Subhas 1 Alex Benedick 2 Nancy A. Obuchowski
Musculoskeletal Imaging Original Research Subhas et al. Comparison of Fast and Standard Shoulder MRI Protocols Musculoskeletal Imaging Original Research Naveen Subhas 1 Alex Benedick 2 Nancy A. Obuchowski
D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1.
 Responsiveness of qualitative and quantitative MRI measures over 2.7 years D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1. 1 Menzies Research Institute Tasmania,
Responsiveness of qualitative and quantitative MRI measures over 2.7 years D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1. 1 Menzies Research Institute Tasmania,
Orthopedic Hardware Imaging Part II: MRI v. Metal
 Orthopedic Hardware Imaging Trent Roth, MD And Lauren Ladd, MD Indiana University School of Medicine IU Health Physicians-Radiology Recap: Imaging Techniques Radiography Standard for initial and surveillance
Orthopedic Hardware Imaging Trent Roth, MD And Lauren Ladd, MD Indiana University School of Medicine IU Health Physicians-Radiology Recap: Imaging Techniques Radiography Standard for initial and surveillance
The magic angle phenomenon in tendons: effect of varying the MR echo time
 T he British Journal of Radiology, 7 (998), 3 36 998 The British Institute of Radiology The magic angle phenomenon in tendons: effect of varying the MR echo time W C G PEH, FRCR and J H M CHAN, MSc Department
T he British Journal of Radiology, 7 (998), 3 36 998 The British Institute of Radiology The magic angle phenomenon in tendons: effect of varying the MR echo time W C G PEH, FRCR and J H M CHAN, MSc Department
Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A
 Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy
 The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
MR Advance Techniques. Vascular Imaging. Class II
 MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
ORIGINAL ARTICLE. ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel
 ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
High Field MR of the Spine
 Department of Radiology University of California San Diego 3T for MR Applications Advantages High Field MR of the Spine Increased signal-to-noise Better fat suppression Increased enhancement with gadolinium
Department of Radiology University of California San Diego 3T for MR Applications Advantages High Field MR of the Spine Increased signal-to-noise Better fat suppression Increased enhancement with gadolinium
Department of Orthopaedic Surgery University of California, Davis
 Department of Orthopaedic Surgery University of California, Davis Lloyd W. Taylor Resident Award: Diagnostic Accuracy of MRI in SLAP Tears: A Retrospective Review of 444 Patients Utilizing Musculoskeletal
Department of Orthopaedic Surgery University of California, Davis Lloyd W. Taylor Resident Award: Diagnostic Accuracy of MRI in SLAP Tears: A Retrospective Review of 444 Patients Utilizing Musculoskeletal
Delaminated Tears of the Rotator Cuff: Prevalence, Characteristics, and Diagnostic Accuracy Using Indirect MR Arthrography
 Musculoskeletal Imaging Original Research Choo et al. MR Arthrography of Delaminated Tears of the Rotator Cuff Musculoskeletal Imaging Original Research Hye Jung Choo 1 Sun Joo Lee 1 Jung-Han Kim 2 Dong
Musculoskeletal Imaging Original Research Choo et al. MR Arthrography of Delaminated Tears of the Rotator Cuff Musculoskeletal Imaging Original Research Hye Jung Choo 1 Sun Joo Lee 1 Jung-Han Kim 2 Dong
CAN SOFT TISSUES STRUCTURES DIFFERENTIATE BETWEEN DYSPLASIA AND CAM-FAI OF THE HIP?
 CAN SOFT TISSUES STRUCTURES DIFFERENTIATE BETWEEN DYSPLASIA AND CAM-FAI OF THE HIP? A Le Bouthillier, KS Rakhra 1, PE Beaulé 2, RCB Foster 1 1 Department of Medical Imaging 2 Division of Orthopaedic Surgery
CAN SOFT TISSUES STRUCTURES DIFFERENTIATE BETWEEN DYSPLASIA AND CAM-FAI OF THE HIP? A Le Bouthillier, KS Rakhra 1, PE Beaulé 2, RCB Foster 1 1 Department of Medical Imaging 2 Division of Orthopaedic Surgery
The topic that tends to get most attention in musculoskeletal radiology
 Introducing Radiology Select: Imaging of Joints Thomas M., MD, PhD The topic that tends to get most attention in musculoskeletal radiology during continuing medical education courses is imaging of joints,
Introducing Radiology Select: Imaging of Joints Thomas M., MD, PhD The topic that tends to get most attention in musculoskeletal radiology during continuing medical education courses is imaging of joints,
Rakesh Patel, MD 4/9/09
 Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Sonography of the Acetabular Labrum
 Case Series Visualization of Labral Injuries During Intra-Articular Injections Carolyn M. Sofka, MD, Ronald S. Adler, PhD, MD, Martha A. Danon, MD Objective. The purpose of this series was to describe
Case Series Visualization of Labral Injuries During Intra-Articular Injections Carolyn M. Sofka, MD, Ronald S. Adler, PhD, MD, Martha A. Danon, MD Objective. The purpose of this series was to describe
Sensitivity of MR Arthrography in the Evaluation of Acetabular Labral Tears
 MR Arthrography of Acetabular Labral Tears Musculoskeletal Imaging Original Research A C D E M N E U T R Y L I A M C A I G O F I N G Glen A. Toomayan 1 W. Russell Holman 1 Nancy M. Major 1 Shannon M. Kozlowicz
MR Arthrography of Acetabular Labral Tears Musculoskeletal Imaging Original Research A C D E M N E U T R Y L I A M C A I G O F I N G Glen A. Toomayan 1 W. Russell Holman 1 Nancy M. Major 1 Shannon M. Kozlowicz
Disclosures. Background. Background
 Kinematic and Quantitative MR Imaging Evaluation of ACL Reconstructions Using the Mini-Two Incision Method Compared to the Anteromedial Portal Technique Drew A. Lansdown, MD Christina Allen, MD Samuel
Kinematic and Quantitative MR Imaging Evaluation of ACL Reconstructions Using the Mini-Two Incision Method Compared to the Anteromedial Portal Technique Drew A. Lansdown, MD Christina Allen, MD Samuel
1Pulse sequences for non CE MRA
 MRI: Principles and Applications, Friday, 8.30 9.20 am Pulse sequences for non CE MRA S. I. Gonçalves, PhD Radiology Department University Hospital Coimbra Autumn Semester, 2011 1 Magnetic resonance angiography
MRI: Principles and Applications, Friday, 8.30 9.20 am Pulse sequences for non CE MRA S. I. Gonçalves, PhD Radiology Department University Hospital Coimbra Autumn Semester, 2011 1 Magnetic resonance angiography
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord
 The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
Magnetic Resonance Angiography
 Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
Effects of body mass index, infrapatellar fat pad volume and age on patellar cartilage defect
 Acta Orthop. Belg., 2015, 81, 41-46 ORIGINAL STUDY Effects of body mass index, infrapatellar fat pad volume and age on patellar cartilage defect Semra Duran, Ertugrul Aksahin, Onur Kocadal, Cem Nuri Aktekin,
Acta Orthop. Belg., 2015, 81, 41-46 ORIGINAL STUDY Effects of body mass index, infrapatellar fat pad volume and age on patellar cartilage defect Semra Duran, Ertugrul Aksahin, Onur Kocadal, Cem Nuri Aktekin,
Cartilage Repair Center Brigham and Women s Hospital Harvard Medical School
 Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
doi: /j.knee
 doi: 10.1016/j.knee.2013.04.016 Title page (a) title: Oblique coronal and oblique sagittal MRI for diagnosis of anterior cruciate ligament tears and evaluation of anterior cruciate ligament remnant tissue
doi: 10.1016/j.knee.2013.04.016 Title page (a) title: Oblique coronal and oblique sagittal MRI for diagnosis of anterior cruciate ligament tears and evaluation of anterior cruciate ligament remnant tissue
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION
 LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION R. ŚMIGIELSKI, B. DOMINIK, U, ZDANOWICZ, Z. GAJEWSKI, K. SKIERBISZEWSKA, K. SIEWRUK,
LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION R. ŚMIGIELSKI, B. DOMINIK, U, ZDANOWICZ, Z. GAJEWSKI, K. SKIERBISZEWSKA, K. SIEWRUK,
High-Resolution 3D Cartilage Imaging with IDEAL SPGR at 3 T
 Siepmann et al. Knee MRI with IDEL SPGR Musculoskeletal Imaging Technical Innovation David. Siepmann 1 Jeff McGovern 2 Jean H. rittain 3 Scott. Reeder 1,4 Siepmann D, McGovern J, rittain JH, Reeder S Keywords:
Siepmann et al. Knee MRI with IDEL SPGR Musculoskeletal Imaging Technical Innovation David. Siepmann 1 Jeff McGovern 2 Jean H. rittain 3 Scott. Reeder 1,4 Siepmann D, McGovern J, rittain JH, Reeder S Keywords:
3D high-resolution MR imaging can provide reliable information
 Published April 11, 2013 as 10.3174/ajnr.A3472 ORIGINAL RESEARCH HEAD & NECK High-Resolution MRI of the Intraparotid Facial Nerve Based on a Microsurface Coil and a 3D Reversed Fast Imaging with Steady-State
Published April 11, 2013 as 10.3174/ajnr.A3472 ORIGINAL RESEARCH HEAD & NECK High-Resolution MRI of the Intraparotid Facial Nerve Based on a Microsurface Coil and a 3D Reversed Fast Imaging with Steady-State
Musculoskeletal MR Protocols
 Musculoskeletal MR Protocols Joint-based protocols MSK 1: Shoulder MRI MSK 1A: Shoulder MR arthrogram MSK 1AB: Shoulder MR arthrogram (instability protocol) MSK 2: Elbow MRI MSK 2A: Elbow MR arthrogram
Musculoskeletal MR Protocols Joint-based protocols MSK 1: Shoulder MRI MSK 1A: Shoulder MR arthrogram MSK 1AB: Shoulder MR arthrogram (instability protocol) MSK 2: Elbow MRI MSK 2A: Elbow MR arthrogram
Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping
 TR_002 Technical Reports Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping Min A Yoon 1,*, Suk-Joo Hong 1, Chang Ho Kang 2, Baek Hyun Kim 3 1 Korea University
TR_002 Technical Reports Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping Min A Yoon 1,*, Suk-Joo Hong 1, Chang Ho Kang 2, Baek Hyun Kim 3 1 Korea University
MRI of the Knee: Part 2 - menisci. Mark Anderson, M.D. University of Virginia Health System
 MRI of the Knee: Part 2 - menisci Mark Anderson, M.D. University of Virginia Health System Learning Objectives At the end of the presentation, each participant should be able to: describe the normal anatomy
MRI of the Knee: Part 2 - menisci Mark Anderson, M.D. University of Virginia Health System Learning Objectives At the end of the presentation, each participant should be able to: describe the normal anatomy
Meniscal tears on 3T MR: Patterns, pearls and pitfalls
 Meniscal tears on 3T MR: Patterns, pearls and pitfalls Poster No.: C-2221 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: J. C. Kandathil; Singapore/SG Keywords: Knee injuries,
Meniscal tears on 3T MR: Patterns, pearls and pitfalls Poster No.: C-2221 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: J. C. Kandathil; Singapore/SG Keywords: Knee injuries,
MENISCAL INJURY. Meniscus. Anterior Roots. Medial Meniscus. Lateral Meniscus. Posterior Roots. MRI and Arthroscopic Findings
 Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries
 Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
T2 & T2# maps: Sequence Development and Clinical Impact on Joint Study
 T2 & T2# maps: Sequence Development and Clinical Impact on Joint Study Poster No.: C-2444 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Sirignano, E. Soscia, D. Iodice, S. Innocenti, G. Palma,
T2 & T2# maps: Sequence Development and Clinical Impact on Joint Study Poster No.: C-2444 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Sirignano, E. Soscia, D. Iodice, S. Innocenti, G. Palma,
