Department of Physical Medicine and Rehabilitation, Korea University Guro Hospital, Seoul, Korea
|
|
|
- Justin Arnold
- 6 years ago
- Views:
Transcription
1 Original Article Ann Rehabil Med 2016;40(2): pissn: eissn: Annals of Rehabilitation Medicine Sonoanatomical Change of Phrenic Nerve According to Posture During Ultrasound-Guided Stellate Ganglion Block Eui Soo Joeng, MD, Young Cheol Jeong, MD, Bum Jun Park, MD, Seok Kang, MD, Seung Nam Yang, MD, PhD, Joon Shik Yoon, MD, PhD Department of Physical Medicine and Rehabilitation, Korea University Guro Hospital, Seoul, Korea Objective To evaluate the risk of phrenic nerve injury during ultrasound-guided stellate ganglion block (US-SGB) according to sonoanatomy of the phrenic nerve, and determine a safer posture for needle insertion by assessing its relationship with surrounding structure according to positional change. Methods Twenty-nine healthy volunteers were recruited and underwent ultrasound in two postures, i.e., supine position with the neck extension and head rotation, and lateral decubitus position. The transducer was placed at the anterior tubercle of the C6 level to identify phrenic nerve. The cross-sectional area (CSA), depth from skin, distance between phrenic nerve and anterior tubercle of C6 transverse process, and the angle formed by anterior tubercle, posterior tubercle and phrenic nerve were measured. Results The phrenic nerve was clearly identified in the intermuscular fascia layer between the anterior scalene and sternocleidomastoid muscles. The distance between the phrenic nerve and anterior tubercle was 10.33±3.20 mm with the supine position and 9.20±3.31 mm with the lateral decubitus position, respectively. The mean CSA and skin depth of phrenic nerve were not statistically different between the two positions. The angle with the supine position was o ±27.43 o, and o ±30.02 o with the lateral decubitus position. The difference of angle between the two positions was statistically significant. Conclusion Ultrasound is a useful tool for assessing the phrenic nerve and its anatomical relation with other cervical structures. In addition, lateral decubitus position seems to be safer by providing wider angle for needle insertion than the supine position in US-SGB. Keywords Stellate ganglion, Phrenic nerve, Ultrasound, Posture Received May 6, 2015; Accepted August 12, 2015 Corresponding author: Joon Shik Yoon Department of Physical Medicine and Rehabilitation, Korea University Guro Hospital, 148 Gurodong-ro, Guro-gu, Seoul 08308, Korea Tel: , Fax: , rehab46@korea.ac.kr This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( licenses/by-nc/4.0) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Copyright 2016 by Korean Academy of Rehabilitation Medicine
2 Sonoanatomical Change of Phrenic Nerve According to Posture Introduction Stellate ganglion block (SGB) is a common intervention in the diagnosis and management of sympathetically mediated pain and vascular insufficiency of the upper extremities. In addition, this type of anesthetic block is commonly utilized for the treatment of pain conditions of the head and neck regions as well as the upper limbs, such as phantom pain, postherpetic neuralgia, cancer pain, cardiac arrhythmias, orofacial pain, and vascular headache [1]. The stellate ganglion lies medial to the scalene muscles, lateral to the longus colli muscle, anterior to the transverse processes and prevertebral fascia, and superior to the subclavian artery and the posterior aspect of the pleura. The SGB is typically performed at the C6 level. At C6 level, the cervical sympathetic chain is anterior to the longus colli muscle, embedded within the prevertebral fascia. There are many important soft-tissue structures that can be unintentionally injured at these levels during needle placement for SGB, including the trachea, thyroid gland, esophagus, arteries (carotid, vertebral, inferior thyroidal, deep and ascending cervical), cervical nerve roots, and external jugular vein. In addition, small nerves such as phrenic nerve or spinal accessory nerve should be identified to avoid inadvertent injury. The phrenic nerve arises from the ventral ramus of the fourth cervical nerve with contributions from the third and fifth cervical nerves [2]. The nerve lies on the anterior surface of the anterior scalene muscle behind its fascia at vertebral level C6, and runs distally following the upper portion of the anterior scalene muscle. It is mostly made up of motor fibers that regulate diaphragmatic contraction. In addition, it provides the pleura and many components of the mediastinum and upper abdomen with sensory innervation [3]. The phrenic nerve could be located on the needle pathway when performing SGB. Diaphragmatic paralysis due to concomitant phrenic nerve block could occur, hence, it should be prevented especially in patients with chronic respiratory disease, chronic obstructive pulmonary disease (COPD), bronchial asthma, or high body mass index (BMI) [2]. Thus, although the ultrasound provides excellent real-time visualization of the neurovascular structures, the identification of phrenic nerve and assessment of its location during SGB is important to avoid the needle-induced injury. Many detailed studies address the risk of injury to the esophagus, trachea, or major vessels when performing SGB, however, descriptions of the phrenic nerve are less common, and to our best knowledge, there are no prior reports on the sonoanatomy of phrenic nerve during SGB. The aim of this study was to evaluate the risk of phrenic nerve injury during ultrasound-guided SGB (US- SGB) by investigating the sonoanatomy of the phrenic nerve in the cervical region. In addition, we determined the safer position for SGB by examining the variations of the phrenic nerve and its relationship with surrounding structure according to the change of position. MATERIALS AND MEHTODS The protocol for this prospective study was approved by the Institutional Review Board of the Korea University Hospital. Informed consent was obtained from all patients prior to each US examination. A B Fig. 1. Sonographic evaluations were performed in two postures. (A) Supine position with the neck slightly extended, and the head rotated slightly to the opposite side to be blocked. (B) Lateral decubitus position with the side to be treated uppermost
3 Eui Soo Joeng, et al. Subjects A total of 29 healthy volunteers were recruited for this study. There were 18 males and 11 females, with an overall mean age 45.9±19.4 years (range, years). We excluded those who met the following exclusion criteria: 1) age <18 years, 2) history of cervical disorder, 3) history of cervical trauma or surgery, and 4) peripheral neuropathy. Sonographic technique and posture of patient All sonographic examinations were performed using a Philips HD15 equipped with a linear probe. US was performed with the volunteers in two postures, i.e., 1) supine position with the neck slightly extended, and the head rotated slightly to the opposite side to be blocked [2-5] [3,4], and 2) lateral decubitus position with the side to be treated uppermost [4-6] (Fig. 1). The transverse processes were initially examined in the axial plane for assessment of the level of the cervical vertebra. The transducer was initially placed at the level of the cricoid cartilage, and traced caudally to identify the typical appearance of the C6 transverse process, with a prominent anterior tubercle, a smaller posterior tubercle, and the C6 nerve root. The level was confirmed by scanning caudally to visualize the C7 transverse process. The anterior tubercle of the transverse process is selectively absent in the C7 vertebra and considered as the key landmark of C7 vertebra. The phrenic nerve was observed by first assessing the anterior scalene muscle, which was seen immediately behind the sternocleidomastoid muscle, lateral to the internal jugular vein and medial to the brachial plexus roots. The nerve appeared as an ovoid hypoechogenic structure, located on the anterior surface of the anterior scalene muscle behind its fascia at vertebral level C6. Sonographic landmarks, anterior scalene muscle, middle scalene muscle, sternocleidomastoid muscle, anterior tubercle, and phrenic nerve, were identified on the plane of vertebral C6 level (Fig. 2). Depth of phrenic nerve from skin and distance between phrenic nerve and anterior tubercle of C6 transverse process We measured the shortest distance between the epineurium of phrenic nerve and the surface of skin. We also measured the shortest distance between the epineurium of phrenic nerve and the anterior tubercle of the C6 transverse process (Fig. 3). The angle which is formed by anterior tubercle, posterior tubercle and phrenic nerve An imaginary line (AB) was drawn passing the upper Fig. 2. Sonographic landmarks, anterior scalene muscle (AS), middle scalene muscle (MS), sternocleidomastoid muscle (SCM), anterior tubercle (AT), and phrenic nerve (PN), were identified on the plane of vertebral C6 level. The margin of phrenic nerve was presented as dotted line. C6, C6 nerve root; PT, posterior tubercle. Fig. 3. Depth of phrenic nerve from skin was measured by the shortest distance between the epineurium of phrenic nerve and the surface of skin (presented as solid line). The shortest distance between the epineurium of phrenic nerve and the anterior tubercle (AT) of the C6 transverse process was also measured (presented as dotted line). SCM, sternocleidomastoid muscle; AS, anterior scalene muscle; MS, middle scalene muscle; C6, C6 nerve root
4 Sonoanatomical Change of Phrenic Nerve According to Posture margin of posterior tubercle ( A ) and anterior tubercle ( B ). In addition, another imaginary line (CD) was drawn passing the two points both the lower margin of epineurium of phrenic nerve ( C ) and the upper margin of anterior tubercle ( D ). The two imaginary lines were extended above and the point of intersection was designated as E. The angle formed by the lower margin of epineurium of phrenic nerve ( C ), point E, and the upper margin of posterior tubercle ( A ) ( CEA) was measured (Fig. 4). The cervical sympathetic chain, the target point of SGB (represented as shaded rectangle on Fig. 5), lies anterior to the longus colli muscle, and is embedded within the prevertebral fascia. When performing SGB, the anterior tubercle blocks the needle from reaching the target point, and the phrenic nerve is located in the needle pathway. Therefore, the angle formed by posterior tubercle, anterior tubercle and phrenic nerve, is a safe angle to perform successful SGB without phrenic nerve injury. Statistical analysis Statistical analyses were performed using the SPSS software package (ver. 20.0). A normal distribution was confirmed by Kolmogorov-Smirnov test. Paired t-test was used for comparing the depth of phrenic nerve from skin, A A PT C PN CEA E B AT D B Fig. 4. The angle formed by the lower margin of epineurium of PN (point C ), point E, and the upper margin of PT (point A ) ( CEA) was described on ultrasound image (A) and schematic image (B). A, upper margin of PT; B, point on the AT created by connecting PT and AT; C, lower margin of epineurium of PN; D, point on the AT created by connecting lower margin of PN and AT; E, crossed point of extended line AB and CD; PN, phrenic nerve; PT, posterior tubercle; AT, anterior tubercle. A B Fig. 5. Virtual needle pathways were described as dotted arrows. The target point was represented as shaded rectangle. (A) When the safe angle ( CEA) is small, if the needle aims at the target point directly, the needle would be blocked by AT and cannot reach the target point. (B) When the needle pathway is positioned within the range of safe angle ( CEA), the needle could reach the target point without contacting the AT and PN. Larger safe angle ( CEA) provides greater possibility to approach the target point safely. A, upper margin of PT; C, lower margin of epineurium of PN; E, crossed point of extended line AB and CD; AT, anterior tubercle; PN, phrenic nerve; PT, posterior tubercle; IJV, internal jugular vein; CA, carotid artery; PVF, prevertebral fascia; LCo, longus colli muscle
5 Eui Soo Joeng, et al. distance between the phrenic nerve and anterior tubercle of the transverse process, and the angle that is formed by anterior tubercle, posterior tubercle and phrenic nerve ( CEA) between supine and lateral decubitus positions. Wilcoxon signed-rank test was used for comparing the CSA of phrenic nerve between supine and lateral decubitus positions. Correlation analyses were performed for evaluation of correlation between the variants. Results Eighteen male and 11 female volunteers were enrolled. The characteristics of volunteers were summarized in Table 1. The mean age of 29 volunteers was 45.9±19.4 years (range, years). The mean BMI was 23.1±3.1 kg/m 2 (range, kg/m 2 ). The sonographic values of the phrenic nerve were shown in Table 2. The mean CSA of phrenic nerve was 0.68±0.35 mm 2 in supine position, and 0.66±0.35 mm 2 in lateral decubitus position. The depth of phrenic nerve from skin was 5.82±2.62 mm in supine position, and 6.04±2.15 mm in lateral decubitus position. The mean Table 1. Clinical characteristics of volunteers Parameter Value Sex (male:female) 18:11 Age (yr) 45.9±19.4 (18 81) Height (cm) 169.9±8.1 ( ) Weight (kg) 67.0±12.0 (48 99) BMI (kg/m 2 ) 23.1±3.1 ( ) Values are presented as mean±standard deviation (range) or number. CSA of phrenic nerve and depth of phrenic nerve from skin was not different between the two positions. The distance between the phrenic nerve and anterior tubercle in supine position was 10.33±3.20 mm and 9.20±3.31 mm in lateral decubitus position, respectively. Though the distance tended to decrease in the lateral decubitus position, it was not statistically significant. Twenty-two of 29 volunteers showed increment of the angle ( CEA) with the position change from supine to lateral decubitus position, but 7 showed decrement. The mean angle ( CEA) was o ±27.43 o with the supine position, and o ±30.02 o with the lateral decubitus position. The angle was significantly wider in lateral decubitus position. BMI was significantly correlated with the depth of phrenic nerve in both positions (p=0.022, r=0.455 in supine position; p<0.001, r=0.656 in lateral decubitus position). In addition, BMI was significantly correlated with the angle ( CEA) in supine position (p=0.001, r=0.625), while no significant correlation was found in lateral decubitus position (p=0.061, r=0.380). No significant correlations were found between the characteristics of subjects and the changed values of sonographic parameters. Discussion In performing cervical procedures, several anatomic structures have to be considered to avoid serious complications. The posterior cervical triangle includes a number of vascular structures, lymph nodes and components of the cervical and brachial plexus [7]. Severe complications are reported, including immediate seizures, hematoma formation with airway compromise, and death [8]. Spread of local anesthetic into the epidural space Table 2. Sonographic values of phrenic nerve Supine Lateral decubitus p-value CSA (mm 2 ) a) 0.68± ± (0.60, ) (0.60, ) Skin depth (mm) b) 5.82± ± Distance from anterior tubercle (mm) b) 10.33± ± CEA ( o ) b) 48.37± ± * Values are presented as mean±standard deviation (median, interquartile range). CSA, cross-sectional area; CEA, the angle formed by the lower margin of epineurium of phrenic nerve ( C ), point E, and the upper margin of posterior tubercle ( A ). a) CSA was analyzed by Wilcoxon signed-rank test. b) Paired t-test was used for comparing the values with two positions. *p<
6 Sonoanatomical Change of Phrenic Nerve According to Posture can result in hypotension and bradycardia. Unintentional esophageal puncture and pneumothorax are also reported as severe complications. Associated brachial plexus block is reported in up to 10% of patients. The recurrent laryngeal nerve may also be blocked, resulting in a hoarse voice and unilateral vocal cord paresis [9]. Some case reports of development of Horner syndrome cite bilateral occurrence, which may cause visual impairment [10]. The phrenic nerve could be placed in the needle-path and partial phrenic blocks could occur when performing various anesthetic procedures of cervical area. An accidental diaphragmatic paresis secondary to the cervical procedure is often asymptomatic but in cases of preexisting respiratory insufficiency, decompensation may occur rapidly post-procedure. It occurs in approximately 50% of cases, when performing supraclavicular brachial plexus block [11]. This side effect is possible even when diaphragmatic stimulation is not observed when performing the block. In addition to acute phrenic nerve block from local anesthesia, persistent phrenic nerve injury from interscalene block or internal jugular vein cannulation is reported [12]. Although US provides excellent direct and real-time visualization of the soft tissues of the neck [13], including neurovascular structures, the identification of phrenic nerve and assessment of its course before performing SGB is advisable to avoid intraprocedural needle-nerve contact. Several studies on sonoanatomy of phrenic nerve are reported. In an anatomical study in cadavers and volunteers, Canella et al. [3] reported the mean diameter of the phrenic nerves of 0.6 mm 1.0 mm with no significant differences between the values according to the gender, age or examined side. Kessler et al. [2] also identified the phrenic nerve with US in both cadavers and volunteers. They measured the distance between the phrenic nerve and the ventral ramus of C5, and the depth of phrenic nerve from skin. The distance between the phrenic nerve and the ventral ramus of C5 was 1.8 mm at the level of cricoid cartilage, and the depth of phrenic nerve from skin was 5.4 mm, respectively. In our study, we measured the anatomical parameters of phrenic nerve at C6 level to evaluate the risk of phrenic nerve injury in SGB. The phrenic nerve was well demarcated by US in cervical area. In supine position, the CSA of phrenic nerve was 0.68±0.35 mm 2 and the depth of phrenic nerve from the skin was 5.82±2.62 mm. The distance between phrenic nerve and the anterior tubercle of C6 transverse process was 10.33±3.20 mm in supine position. Two different needle approaches for US-SGB are reported. The first is the anterior paratracheal approach. The anterior paratracheal technique is performed as a standard technique to block stellate ganglion. However, this technique may result in a number of severe complications for e.g., subarachnoid or epidural injection, recurrent laryngeal nerve block, seizures, and blindness. The in-plane lateral approach is recently introduced [14]. The lateral approach seems to be an excellent alternative technique for avoiding the potential risks associated with the conventional approach. We performed sonographic examinations for lateral approach with two different positions, i.e., supine and lateral decubitus. The general anatomical parameters of phrenic nerve, such as the CSA, depth of location and distance from the anterior tubercle of C6, were not significantly different according to the position. We measured the angle formed by anterior tubercle, posterior tubercle and phrenic nerve, to determine whether the intraprocedural location of the phrenic nerve is on the needle pathway. During SGB with lateral approach, because the anterior tubercle blocks the needle pathway, the needle should be positioned between the phrenic nerve and the anterior tubercle to avoid phrenic nerve injury. Thus, we regarded the angle formed by posterior tubercle, anterior tubercle and phrenic nerve as clinically important. After passing beyond the anterior tubercle without phrenic nerve injury, the needle tip could be advanced to the target point by regulating the direction of needle pathway. Therefore, larger angle ( CEA) implies a greater possibility of approaching the target point safely. In supine position, the angle was o ±27.43 o, while lateral decubitus position provides wider maneuvering space (the angle was o ±30.02 o ) for the needle. The muscles and nerve are expected to move inferiorly due to the effect of gravity, because they are relatively softer and more movable than bony structures. Thus, lateral decubitus position may be safer to avoid injury of phrenic nerve and other related anatomical structures during SGB. However, although majority of subjects (22 of 29) showed increment of angle with lateral decubitus position, as compared to supine position, a small number of 249
7 Eui Soo Joeng, et al. individuals showed decrement of angle with lateral decubitus position. Thus, lateral decubitus position could result in decrement of angle in few cases. Therefore, we recommend performing SGB in lateral decubitus position; however, checking both positions is necessary when it is difficult to reach the target point due to small angle in lateral decubitus position. To our knowledge, this is the first study to evaluate the risk of phrenic nerve injury during US-SGB according to anatomical relation between phrenic nerve and C6 transverse process, and the changes of values according to positions. In addition, performing SGB with lateral approach in lateral decubitus position provides a more comfortable position for the physician, since the shoulder of the patient could disturb the injecting hand of the physician when performing SGB in supine position. Our study had several limitations. The major limitation was that this was an observational study of neck sonoanatomy. The results of this study suggest only the potential for the reduction of risk of phrenic nerve injury during SGB in lateral decubitus position. The enhanced safety of performing SGB with lateral decubitus position can be evaluated only in a clinical trial. A randomized controlled trial comparing the incidence of complications due to phrenic nerve injury using the two different positions for SGB (supine with neck rotation and lateral decubitus) may provide data on accuracy, efficacy, and complications, thus facilitating the choice between the two positions. Second, our study was performed on healthy volunteers. The clinical value of our findings needs to be confirmed in further studies on patients who require SGB. Third, intra- and inter-observer analysis of the sonographic assessment of the phrenic nerve was not conducted. Fourth, the values of the angle formed by anterior tubercle, posterior tubercle and phrenic nerve ( CEA) had large variation due to the small number of subjects. Thus, further larger group studies are needed. However, we aimed at not only measuring the angle but also evaluating the change of the value according to the posture. Our results indicated the amount of change and increasing tendency of the angle by changing to lateral decubitus position. US is a useful tool for localizing the phrenic nerve and assessing its anatomical relations with other structures in the cervical region during US-SGB. The angle formed by anterior tubercle, posterior tubercle and phrenic nerve was significantly wider in the lateral decubitus position than in the supine position, providing larger maneuvering space for the needle. In conclusion, the lateral decubitus position may be a safer technique because it is less likely to result in injury to the phrenic nerve and other related anatomical structures. CONFLICT OF INTEREST No potential conflict of interest relevant to this article was reported. REFERENCES 1. Elias M. Cervical sympathetic and stellate ganglion blocks. Pain Physician 2000;3: Kessler J, Schafhalter-Zoppoth I, Gray AT. An ultrasound study of the phrenic nerve in the posterior cervical triangle: implications for the interscalene brachial plexus block. Reg Anesth Pain Med 2008;33: Canella C, Demondion X, Delebarre A, Moraux A, Cotten H, Cotten A. Anatomical study of phrenic nerve using ultrasound. Eur Radiol 2010;20: Gofeld M, Bhatia A, Abbas S, Ganapathy S, Johnson M. Development and validation of a new technique for ultrasound-guided stellate ganglion block. Reg Anesth Pain Med 2009;34: Narouze SN. Ultrasound-guided cervical spine injections: ultrasound prevents whereas contrast fluoroscopy detects intravascular injections. Reg Anesth Pain Med 2012;37: Narouze SN, Vydyanathan A, Kapural L, Sessler DI, Mekhail N. Ultrasound-guided cervical selective nerve root block: a fluoroscopy-controlled feasibility study. Reg Anesth Pain Med 2009;34: Saranteas T, Paraskeuopoulos T, Anagnostopoulou S, Kanellopoulos I, Mastoris M, Kostopanagiotou G. Ultrasound anatomy of the cervical paravertebral space: a preliminary study. Surg Radiol Anat 2010;32: Siegenthaler A, Mlekusch S, Schliessbach J, Curatolo M, Eichenberger U. Ultrasound imaging to estimate risk of esophageal and vascular puncture after conventional stellate ganglion block. Reg Anesth Pain Med 2012;37: Abdi S, Zhou Y, Patel N, Saini B, Nelson J. A new and 250
8 Sonoanatomical Change of Phrenic Nerve According to Posture easy technique to block the stellate ganglion. Pain Physician 2004;7: Wallace MS, Milholland AV. Contralateral spread of local anesthetic withstellate ganglion block. Reg Anesth 1993;18: Mak PH, Irwin MG, Ooi CG, Chow BF. Incidence of diaphragmatic paralysis following supraclavicular brachial plexus block and its effect on pulmonary function. Anaesthesia 2001;56: Robaux S, Bouaziz H, Boisseau N, Raucoules-Aime M, Laxenaire MC; S.O.S. Regional Hot Line Service. Persistent phrenic nerve paralysis following interscalene brachial plexus block. Anesthesiology 2001;95: Boon AJ, Alsharif KI, Harper CM, Smith J. Ultrasoundguided needle EMG of the diaphragm: technique description and case report. Muscle Nerve 2008;38: Bhatia A, Flamer D, Peng PW. Evaluation of sonoanatomy relevant to performing stellate ganglion blocks using anterior and lateral simulated approaches: an observational study. Can J Anaesth 2012;59:
Estimation of Stellate Ganglion Block Injection Point Using the Cricoid Cartilage as Landmark Through X-ray Review
 Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Ultrasound-guided Stellate Ganglion Block Successfully Prevented Esophageal Puncture. Samer Narouze, MD, Amaresh Vydyanathan, MD, and Nilesh Patel, MD
 -Pain Physician 2007; 10:747-752 ISSN 1533-3159 Technical Report Ultrasound-guided Stellate Ganglion Block Successfully Prevented Esophageal Puncture Samer Narouze, MD, Amaresh Vydyanathan, MD, and Nilesh
-Pain Physician 2007; 10:747-752 ISSN 1533-3159 Technical Report Ultrasound-guided Stellate Ganglion Block Successfully Prevented Esophageal Puncture Samer Narouze, MD, Amaresh Vydyanathan, MD, and Nilesh
Comparative Study between Ultrasound Guided Lateral and Anterior Approach for Stellate Ganglion Block
 Med. J. Cairo Univ., Vol. 84,. 1, December: 1525-153, 16 www.medicaljournalofcairouniversity.net Comparative Study between Ultrasound Guided Lateral and Anterior Approach for Stellate Ganglion Block KHALED
Med. J. Cairo Univ., Vol. 84,. 1, December: 1525-153, 16 www.medicaljournalofcairouniversity.net Comparative Study between Ultrasound Guided Lateral and Anterior Approach for Stellate Ganglion Block KHALED
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
USRA OF THE UPPER EXTREMITY
 USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Stellate ganglion blockade-techniques and modalities
 (Acta Anaesth. Belg., 2016, 67, 1-5) Stellate ganglion blockade-techniques and modalities A. Ghai (*), T. Kaushik (*), R. Wadhera (**) and S. Wadhera Abstract : Stellate ganglion block (SGB) is utilized
(Acta Anaesth. Belg., 2016, 67, 1-5) Stellate ganglion blockade-techniques and modalities A. Ghai (*), T. Kaushik (*), R. Wadhera (**) and S. Wadhera Abstract : Stellate ganglion block (SGB) is utilized
Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear Transducer
 ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
Neck-2. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
Neck Ultrasound. Faculty Info: Amy Kule, MD
 Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Interscalene brachial plexus blockade - indications, anatomy, practical performance
 08RC2 Interscalene brachial plexus blockade - indications, anatomy, practical performance Urs Eichenberger Department of Anaesthesiology and Pain Therapy, University Hospital of Bern, Switzerland Saturday,
08RC2 Interscalene brachial plexus blockade - indications, anatomy, practical performance Urs Eichenberger Department of Anaesthesiology and Pain Therapy, University Hospital of Bern, Switzerland Saturday,
Ultrasound-guided Pulsed Radiofrequency of the Third Occipital Nerve
 Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Superficial (and Intermediate) Cervical Plexus Block
 Superficial (and Intermediate) Cervical Plexus Block Indications: -Tympanomastoid surgery. When combined with the auricular branch of the vagus ( nerve of arnold ) by infiltrating subcutaneously into the
Superficial (and Intermediate) Cervical Plexus Block Indications: -Tympanomastoid surgery. When combined with the auricular branch of the vagus ( nerve of arnold ) by infiltrating subcutaneously into the
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E
 Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi. E mail: a.al E. mail:
 Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
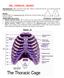 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Mediastinum It is a thick movable partition between the two pleural sacs & lungs. It contains all the structures which lie
 Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Mediastinum and pericardium
 Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
THE DESCENDING THORACIC AORTA
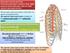 Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
thoracic cage inlet and outlet landmarks of the anterior chest wall muscles of the thoracic wall sternum joints ribs intercostal spaces diaphragm
 Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
cardiac plexus is continuous with the coronary and no named branches pain from the heart and lungs
 Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Human Anatomy Biology 351
 nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
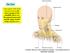 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Neck. BY: Lina Abdullah & Rahaf Jreisat
 The Neck BY: Lina Abdullah & Rahaf Jreisat Boundaries of the Neck: generally from base of the skull to root of the neck Superior margin :From superior nuchal line of occipital bone up to mastoid process
The Neck BY: Lina Abdullah & Rahaf Jreisat Boundaries of the Neck: generally from base of the skull to root of the neck Superior margin :From superior nuchal line of occipital bone up to mastoid process
Anatomy and Physiology II. Spine
 Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Ultrasound-Guided Cervical Nerve Root Block: Does Volume Affect the Spreading Pattern?
 Pain Medicine 2016; 17: 1978 1984 doi: 10.1093/pm/pnw027 SPINE SECTION Original Research Article Ultrasound-Guided Cervical Nerve Root Block: Does Volume Affect the Spreading Pattern? Seok Kang, MD, Seung
Pain Medicine 2016; 17: 1978 1984 doi: 10.1093/pm/pnw027 SPINE SECTION Original Research Article Ultrasound-Guided Cervical Nerve Root Block: Does Volume Affect the Spreading Pattern? Seok Kang, MD, Seung
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics
 Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Correspondence should be addressed to Stanley K. H. Lam;
 Hindawi BioMed Research International Volume 2017, Article ID 7920438, 17 pages https://doi.org/10.1155/2017/7920438 Research Article Transition from Deep Regional Blocks toward Deep Nerve Hydrodissection
Hindawi BioMed Research International Volume 2017, Article ID 7920438, 17 pages https://doi.org/10.1155/2017/7920438 Research Article Transition from Deep Regional Blocks toward Deep Nerve Hydrodissection
Ultrasound Guided Regional Nerve Blocks
 Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report
 SHORT REPORT Eur J Anat, 10 (3): 61-66 (2006) Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report K. Ramachandran, I. Kanakasabapathy and
SHORT REPORT Eur J Anat, 10 (3): 61-66 (2006) Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report K. Ramachandran, I. Kanakasabapathy and
Ultrasound guidance for interventional pain management
 Faculty Disclosure Ultrasound guidance for interventional pain management Dr. Roel Mestrum, MD, FIPP Anesthesiology, Intensive Care Medicine and Multidisciplinary Pain Centre Regionaal Ziekenhuis Heilig
Faculty Disclosure Ultrasound guidance for interventional pain management Dr. Roel Mestrum, MD, FIPP Anesthesiology, Intensive Care Medicine and Multidisciplinary Pain Centre Regionaal Ziekenhuis Heilig
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 )
 2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
Diaphragm and intercostal muscles. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
THE SURGEON S LIBRARY
 THE SURGEON S LIBRARY THE HISTORY AND SURGICAL ANATOMY OF THE VAGUS NERVE Lee J. Skandalakis, M.D., Chicago, Illinois, Stephen W. Gray, PH.D., and John E. Skandalakis, M.D., PH.D., F.A.C.S., Atlanta, Georgia
THE SURGEON S LIBRARY THE HISTORY AND SURGICAL ANATOMY OF THE VAGUS NERVE Lee J. Skandalakis, M.D., Chicago, Illinois, Stephen W. Gray, PH.D., and John E. Skandalakis, M.D., PH.D., F.A.C.S., Atlanta, Georgia
slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments
 Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
Diana Mathioudakis DEAA EDIC AFRCA. consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d)
 & Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
& Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2014;38(1):72-76 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.72 Annals of Rehabilitation Medicine Appropriate Depth of Needle Insertion During
Original Article Ann Rehabil Med 2014;38(1):72-76 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.72 Annals of Rehabilitation Medicine Appropriate Depth of Needle Insertion During
Chapter 5: Other mediastinal structures. The Large Arteries. The Aorta. Ascending aorta
 Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Thyroid and Parathyroid Glands
 Thyroid and Parathyroid Glands Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/ explanation Objectives: By the end of the lecture,
Thyroid and Parathyroid Glands Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/ explanation Objectives: By the end of the lecture,
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Prevertebral Region, Pharynx and Soft Palate
 Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Anatomy of thoracic wall
 Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
Tympanic Bulla Temporal Bone. Digastric Muscle. Masseter Muscle
 Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013
 Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli.
 Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli. Rectus Capitis Anterior. Rectus Capitis Lateralis. Rectus Capitis
Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli. Rectus Capitis Anterior. Rectus Capitis Lateralis. Rectus Capitis
Objectives. Thoracic Inlet. Thoracic Inlet Boundaries. Thoracic Inlet Sagittal View ANTERIOR SCALENE ANTERIOR SCALENE
 Objectives Thoracic Inlet Deborah L. Reede M.D. SUNY Downstate Medical Center Learn the anatomy of the thoracic inlet (TI) Review the clinical and radiographic findings of common lesions encountered in
Objectives Thoracic Inlet Deborah L. Reede M.D. SUNY Downstate Medical Center Learn the anatomy of the thoracic inlet (TI) Review the clinical and radiographic findings of common lesions encountered in
Infraclavicular brachial plexus blocks have been designed
 The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
Sectional Anatomy Quiz - III
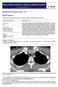 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
STERNUM. Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts:
 STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
Surgical anatomy of thyroid and parathyroid glands
 Head & Neck Surgery Course Surgical anatomy of thyroid and parathyroid glands Dr Pierfrancesco PELLICCIA Pr Benjamin LALLEMANT Service ORL et CMF CHU de Nîmes CH de Arles Thyroid glands Dr Pierfrancesco
Head & Neck Surgery Course Surgical anatomy of thyroid and parathyroid glands Dr Pierfrancesco PELLICCIA Pr Benjamin LALLEMANT Service ORL et CMF CHU de Nîmes CH de Arles Thyroid glands Dr Pierfrancesco
Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line
 L 14 A B O R A T O R Y Thorax THORACIC WALL Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line Identify the surface landmarks of
L 14 A B O R A T O R Y Thorax THORACIC WALL Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line Identify the surface landmarks of
Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th & 12 th Eds.)
 PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
THYROID & PARATHYROID. By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy
 THYROID & PARATHYROID By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy 1 OBJECTIVES By the end of the lecture, the student should be able to: Describe the shape, position, relations and structure of
THYROID & PARATHYROID By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy 1 OBJECTIVES By the end of the lecture, the student should be able to: Describe the shape, position, relations and structure of
Veins of the Face and the Neck
 Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
The mechanism responsible for dysphagia after anterior
 SPINE Volume 40, Number 1, pp E18 - E22 2014, Lippincott Williams & Wilkins Does a Medial Retraction Blade Transmit Direct Pressure to Pharyngeal/Esophageal Wall During Anterior Cervical Surgery? In Ho
SPINE Volume 40, Number 1, pp E18 - E22 2014, Lippincott Williams & Wilkins Does a Medial Retraction Blade Transmit Direct Pressure to Pharyngeal/Esophageal Wall During Anterior Cervical Surgery? In Ho
SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES
 SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES Overview Eugene Mitchell, MD Activity of the sympathetic efferents and their role in the pathology of chronic pain
SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES Overview Eugene Mitchell, MD Activity of the sympathetic efferents and their role in the pathology of chronic pain
Anatomy of the Thyroid Gland
 Anatomy of the Thyroid Gland Introduction Nomenclature G, thyreos= shield, eidos= like Location Root of the neck ventrally (C5-T1) Function endocrine gland that secretes: Thyroxine (T4) T3 Calcitonin LWW,
Anatomy of the Thyroid Gland Introduction Nomenclature G, thyreos= shield, eidos= like Location Root of the neck ventrally (C5-T1) Function endocrine gland that secretes: Thyroxine (T4) T3 Calcitonin LWW,
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
A novel suture-traction method for right internal jugular vein catheterization in left-lateral position in anesthetized patients.
 Biomedical Research 2017; 28 (12): 5628-5632 ISSN 0970-938X www.biomedres.info A novel suture-traction method for right internal jugular vein catheterization in left-lateral position in anesthetized patients.
Biomedical Research 2017; 28 (12): 5628-5632 ISSN 0970-938X www.biomedres.info A novel suture-traction method for right internal jugular vein catheterization in left-lateral position in anesthetized patients.
Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta.
 Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta. Fig-3: Showing high formation of Median nerve. Fig-1: Showing atypical formation of cords of Brachial plexus. 1 = Upper
Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta. Fig-3: Showing high formation of Median nerve. Fig-1: Showing atypical formation of cords of Brachial plexus. 1 = Upper
Gross Anatomy of Lower Spinal Cord
 Chapter 13 Spinal Cord, Spinal Nerves and Somatic Reflexes Spinal cord Spinal nerves Somatic reflexes Gross Anatomy of Lower Spinal Cord Meninges of Vertebra & Spinal Cord Spina Bifida Congenital defect
Chapter 13 Spinal Cord, Spinal Nerves and Somatic Reflexes Spinal cord Spinal nerves Somatic reflexes Gross Anatomy of Lower Spinal Cord Meninges of Vertebra & Spinal Cord Spina Bifida Congenital defect
Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D.
 Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D. Chest cavity - bony structures Chest cavity- bony structures Sternum Ribs True ribs: first seven pairs connect
Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D. Chest cavity - bony structures Chest cavity- bony structures Sternum Ribs True ribs: first seven pairs connect
Anterior triangle of neck
 Anterior triangle of neck Dept. of Anatomy Zhou Hong Ying Outline boundary and subdivisions of ant. triangle contents of the triangle Muscles: suprahyoid muscles, infrahyoid muscles Nerves: CNⅩ, CNⅪ, CNⅫ,
Anterior triangle of neck Dept. of Anatomy Zhou Hong Ying Outline boundary and subdivisions of ant. triangle contents of the triangle Muscles: suprahyoid muscles, infrahyoid muscles Nerves: CNⅩ, CNⅪ, CNⅫ,
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist
 Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Thyroid INTRODUCTION ANATOMY SUMMARY OF CHANGES
 AJC 7/14/06 1:19 PM Page 67 Thyroid C73.9 Thyroid gland SUMMARY OF CHANGES Tumor staging (T) has been revised and the categories redefined. T4 is now divided into T4a and T4b. Nodal staging (N) has been
AJC 7/14/06 1:19 PM Page 67 Thyroid C73.9 Thyroid gland SUMMARY OF CHANGES Tumor staging (T) has been revised and the categories redefined. T4 is now divided into T4a and T4b. Nodal staging (N) has been
The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care settings,
 American Journal of Emergency Medicine (2011) xx, xxx xxx www.elsevier.com/locate/ajem Clinical Notes The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care
American Journal of Emergency Medicine (2011) xx, xxx xxx www.elsevier.com/locate/ajem Clinical Notes The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care
Ultrasonography of Peripheral Nerve -upper extremity
 Ultrasonography of Peripheral Nerve -upper extremity Department of Physical Medicine and Rehabilitation Korea University Guro Hospital Korea University College of Medicine Yoon Joon Shik Normal median
Ultrasonography of Peripheral Nerve -upper extremity Department of Physical Medicine and Rehabilitation Korea University Guro Hospital Korea University College of Medicine Yoon Joon Shik Normal median
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
The Validation of Ultrasound-Guided Target Segment Identification in Thoracic Spine as Confirmed by Fluoroscopy
 Original Article Clinics in Orthopedic Surgery 2017;9:472-479 https://doi.org/10.4055/cios.2017.9.4.472 The Validation of Ultrasound-Guided Target Segment Identification in Thoracic Spine as Confirmed
Original Article Clinics in Orthopedic Surgery 2017;9:472-479 https://doi.org/10.4055/cios.2017.9.4.472 The Validation of Ultrasound-Guided Target Segment Identification in Thoracic Spine as Confirmed
Organisation of the nervous system
 Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Anatomy notes-thorax.
 Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Anatomy for anaesthetists
 VOL 17 NO 1 ANESTHESIA JANUARY 1962 Anatomy for anaesthetists (4) The thoracic inlet and the first rib HAROLD ELLIS, MCh, FRCS Senior Lecturer in Surgery, Westminster Hospital Illustrated by MISS MARGARET
VOL 17 NO 1 ANESTHESIA JANUARY 1962 Anatomy for anaesthetists (4) The thoracic inlet and the first rib HAROLD ELLIS, MCh, FRCS Senior Lecturer in Surgery, Westminster Hospital Illustrated by MISS MARGARET
Original Article Clinics in Orthopedic Surgery 2013;5:
 Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Vascular Access (venous (peripheral and central) and arterial)
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for
 Chapter 13 Outline Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for what you need to know from Exhibits 13.1 13.4 I. INTRODUCTION A. The spinal cord and spinal nerves
Chapter 13 Outline Note: Please refer to handout Spinal Plexuses and Representative Spinal Nerves for what you need to know from Exhibits 13.1 13.4 I. INTRODUCTION A. The spinal cord and spinal nerves
3 Mohammad Al-Mohtasib Areej Mosleh
 3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
A study of the anatomy of the caudal space using magnetic resonance imaging
 British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
THE GOOFY ANATOMIST QUIZZES
 THE GOOFY ANATOMIST QUIZZES 5. NERVES Q1. Which of the following classifications of the nervous systems is correct? A. The autonomic nervous system is composed of the brain, cranial nerves and spinal nerves.
THE GOOFY ANATOMIST QUIZZES 5. NERVES Q1. Which of the following classifications of the nervous systems is correct? A. The autonomic nervous system is composed of the brain, cranial nerves and spinal nerves.
HBA THE BODY Head & Neck Written Examination October 23, 2014
 HBA 531 - THE BODY Head & Neck Written Examination October 23, 2014 Name: NOTE 2: When asked to trace nerve, artery, or vein pathways, do so by using arrows, e.g., structure a structure b structure c...
HBA 531 - THE BODY Head & Neck Written Examination October 23, 2014 Name: NOTE 2: When asked to trace nerve, artery, or vein pathways, do so by using arrows, e.g., structure a structure b structure c...
Min Hur, Eun-Hee Kim, In-Kyung Song, Ji-Hyun Lee, Hee-Soo Kim, and Jin Tae Kim INTRODUCTION. Clinical Research
 Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Infraclavicular brachial plexus blocks aim at the
 REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
A Rare Case of Bilateral Jugular Venous Malformation
 JOURNAL OF CASE REPORTS 2013;3(2):326-330 A Rare Case of Bilateral Jugular Venous Malformation Prasanna LC, Alva R, D Souza AS, Bhat KMR Department of Anatomy, Kasturba Medical College, Manipal University,
JOURNAL OF CASE REPORTS 2013;3(2):326-330 A Rare Case of Bilateral Jugular Venous Malformation Prasanna LC, Alva R, D Souza AS, Bhat KMR Department of Anatomy, Kasturba Medical College, Manipal University,
