Stellate ganglion blockade-techniques and modalities
|
|
|
- Suzanna Pope
- 6 years ago
- Views:
Transcription
1 (Acta Anaesth. Belg., 2016, 67, 1-5) Stellate ganglion blockade-techniques and modalities A. Ghai (*), T. Kaushik (*), R. Wadhera (**) and S. Wadhera Abstract : Stellate ganglion block (SGB) is utilized in the diagnosis and management of various vascular disorders and sympathetically mediated pain in upper extremity, head and neck. The stellate ganglion lies medial to the scalene muscles, lateral to longus coli muscle, esophagus, trachea and recurrent laryngeal nerve, anterior to C 7 transverse process and prevertebral fascia, superior to the subclavian artery and posterior to vertebral vessels. Consequently, inadvertent placement of the needle tip into these soft tissues and vessels occur with blind technique. Henceforth, various interventional modalities are being used for SGB, these have been reviewed in this paper. Various techniques of SGB have been described, and vary from the use of standard blind technique to the use of fluoroscopy, computerized tomography, magnetic resonance imaging, and radio nucleotide tracers. However, these techniques may not be practical in a clinical setting, insofar as they are time consuming, costly, and may involve radiation exposure. The use of fluoroscopy does not visualize the blood vessels close to the stellate ganglion. Ultrasounds are the alternative. They help in visualization of soft tissues to prevent complications and help in deposition of drug subfascially, under direct visual control. Key words : Stellate ganglion ; Stellate ganglion block ; blind technique ; fluoroscopy ; sonographic guidance. magnetic resonance imaging (MRI) and ultrasound guided techniques (2-4). The stellate ganglion is located immediately below the prevertebral fascia covering the longus coli muscle, separated by loose areolar tissue from posterior osseous structures. The vertebral artery is located anterior to the stellate ganglion, usually runs ventrally to the seventh cervical transverse process, and usually enters the foramen transversum of the C 6 vertebra (Fig. 1). In 10% of individuals, it enters the foramen transversum at the C 5 level or higher, and is more tortuous on the left side. This can lead to vertebral artery injury during SGB. The inferior thyroid artery runs ventrally to C 6 and C 7, lying anterior to the vertebral artery. The close proximity of stellate ganglion may lead to retropharyngeal hematoma, and accidental intravascular injections, eventually leading to cardiac arrest (5). The preganglionic fibers of the head and neck continue to travel cephalic to the superior and middle cervical ganglion through the cervical sympathetic trunk, which is located anterior to the prevertebral fascia (6). Hence, all sympathetic fibers to the head and neck either synapse at the level of the sympathetic ganglion, or pass through it to the more cephalic ganglion. SGB provides complete blockade of head and neck sympathetic structures (7-10). Introduction The stellate ganglion block (SGB) has been used to treat vascular insufficiency, va sospasm, hyper hidrosis, and a variety of pain syndromes, including complex re gional pain syndrome, type I and II, phan tom limb pain, postherpetic neuralgia, herpes zoster, pain from cen tral nervous system lesions, atypical facial pain, and intractable angina pectoris. First implemented by Leriche and further refined by Findley and Patzer (1), the most common technique is blind paratracheal approach. However, various complications like subarachnoid or epidural injection, recurrent laryngeal nerve palsy, seizures, and blindness have led to the emergence of interventional radiology, including fluoroscopy, computerized tomography (CT scan), Approaches and imaging modalities Classic blind approach The patient is placed in the supine position, with head extended. The landmark is the anterior Anju Ghai ; Teshi Kaushik ; Raman Wadhera ; Sarthak Wadhera. (*) Departments of Anesthesia and Critical Care, (**) Dept. of ENT Pt. BD Sharma, PGIMS, Rohtak, Haryana, India. Correspondence address : R. Wadhera, House no. 6/8 FM, Medical campus, PGIMS, Rohtak, Haryana, India. Tel. : , dr.wadhera@yahoo.com
2 2 a. ghai et al. recurrent laryngeal nerve is also possible (2), as well as esophageal injury (12). Fluoroscopy-guided stellate ganglion block This technique aims at guiding the needle towards the Chassaignac s tubercle. However, there is a large variability in size and location of it (13). Epidural and intrathecal injections can be ruled out using the spread of contrast in fluoroscopy. The needle can be accurately directed to the landmark, using oblique approach (14). tubercle of C 6, which lies against the cricoid cartilage. The sternocleidomastoid muscle is retracted laterally, pulling the internal carotid artery away. The needle is then inserted perpendicularly between the cricoid cartilage and the operator fingers, and passed until contact is made with the C 6 tubercle. The needle is withdrawn a few millimeters away from the periosteum of C 6 transverse process and, after a negative aspiration test for blood and cerebrospinal fluid (CSF) detection, 1 ml of the local anesthetic solution is injected. Fig. 1. Anatomy of stellate ganglion The C 6 landmark is in close proximity to the middle cervical ganglion instead of the stellate ganglion, and the cervical sympathetic ganglion is primarily blocked when the injected solution spreads to the T 1 level (2). The width of the C 6 tubercle can be as small as 6 mm, and can be missed during blind needle advancement. A small deviation of the needle may puncture the vertebral artery. If the needle is directed to the posterior tubercle, the drug can spread around the spinal nerve roots. The final position of the needle and the spread of local anesthetic (LA) agents is unpredictable (10, 11). There is also a risk of thyroid gland hematoma. Intravascular injections and vascular injury have been reported despite a negative aspiration test, leading to life threatening complications like retropharyngeal hematoma, cardiac arrest, and convulsions (5). A paralysis of the The patient is positioned in a similar way as for the blind technique. The fluoroscopy beam is directed in anteroposterior direction, with caudocranial angulations of the C arm. The needle is directed towards the C 6 anterior tubercle, and advanced under real time imaging to contact the bony target. The stylet is then removed, and the needle is connected to a three-way extension set to allow a 1-2 ml radio opaque contrast injection. After a negative aspiration test, a test dose of local anesthetic agent is given, followed by the injection of the therapeutic dose. Flow of contrast to the head of first rib can be observed by increasing the amount of contrast injection, which pushes the contrast up and down. A modified fluoroscopy-guided technique is performed with the patient in the supine position, with the neck slight ly extended and the head rotated slightly to the opposite side. The skin temperatures are recorded at the distal portion of both upper extremities, in mirror-image locations. The fluoroscopy beam is directed in an anteroposterior direction, until the C5-C6 disc is well visualized. This usually requires caudocra nial angulations of the C-arm. The C-arm is then rotated obliquely, on the side of the block. The rota tion must occur to allow adequate visu alization of the neural foramina. A skin wheal is raised at the surface point of the junction of the uncinate process and the vertebral body, as seen on the fluoroscope. Under real-time imaging, a single pass is made with a 25-gauge spinal needle to contact bone at this point. The stylet is removed, and 2 ml of radioopaque contrast is injected to vi sualize the longus coli muscle. A 0.5 ml test dose is injected.. This approach provides better upper extremity blockade and less chances of vertebral artery puncture due to oblique rather than perpendicular view (13).
3 stellate ganglion blockade 3 With this technique, the intravascular injection is prevented by the prior administration of dye, identification of bony anatomy is possible, and the spread of drug is visualized. The anterior tubercle is only a surrogate marker of the location of the stellate ganglion. This location is defined by the fascia plane of the pre- vertebral fascia, which can t be visualized using fluoroscopy. Soft tissue structures surrounding the stellate ganglion are poorly visualized, including the longus coli muscle, the thyroid gland, and the esophagus, leading to increased risk of injury (15). The precise needle placement into the subfascial plane of the longus coli is not possible (16). The contrast agent may show aberrant and inconsistent spread (16). The fluoroscopic technique helps to avoid inadvertent intravascular injection of local anesthetic agent, but the injection can be identified only after artery is punctured. Therefore, vascular injury is possible (15). CT/ MRI guided block The spread of local anesthetic agent after C6 stellate ganglion block has been defined using computerized axial tomography (CAT) in 10 patients. Radiocontrast and local anesthetic mixture were given in 5 ml increments up to a 20 ml total volume for C6 stellate ganglion nerve blocks in eight patients and C7 in two patients. CAT scanning was performed at baseline and after 5, 10, 15, and 20 ml administration. Cervical level and pattern of spread was recorded after each increment. One half of the injections were beneath the pre-vertebral fascia. Injections on top of the fascia spread more diffusely around C6. All injections of high volume reached the medial aspect of T1 around the head, not neck, of the first rib (16). Although fluoroscopic guidance has helped reducing the complication rate of stellate ganglion blocks, some complications such as lesions to the lung or pleura may occur, particularly when a C7 approach is performed. Moreover, the accuracy of needle placement allowed by the use of CT guidance, which is highly superior to that of fluoro scopic guidance, explains the low complication rate (1.7%) with that technique (17). The use of MRI and CT can be expensive, time-con suming, and impractical for most pain physicians. Another point to consider is that different blocks in the same patient can produce variable spread and may consequently explain the inconsistent outcomes seen with a blind technique (18). Studies using MRI (8) or CT (16) have failed demonstrating any evi dence of spread to the stellate ganglion itself, although in the CT study, the stellate ganglion could not actually be visualized. However, an ultrasound imaging study showed spread from C4 to C7 while us ing 5 ml of local anesthetic mixture. In that study, the authors considered to be an effective clinical stellate ganglion block in 23 out of 24 cases (19). Ultrasound guided stellate ganglion block The success or failure of either blind or fluoroscopic-guided injection depends on the thickness of the longus coli muscle, and on the anatomic location of the cervical sympathetic trunk. The endpoint for injection in the ultrasound-guided technique is the pre-vertebral fascia, and not a contact with bone as with the fluoroscopy and blind techniques. The patient is positioned in the supine or lateral position. A high frequency linear transducer (6-13 MHz) is placed at the level of C 6 or C 7 to enable cross sectional visualization of anatomic structures the transverse process and anterior tubercle of C 6, the longus coli muscle, the pre-vertebral fascia covering the muscle, the carotid artery, and the thyroid gland. The transducer is gently pressed between the carotid artery and the trachea, in a para-tracheal approach, to retract the carotid artery laterally and to position the transducer close to the longus coli. A 1.0 inch, 25 G needle is inserted para-tracheally, with the needle staying out-of -plane to the ultrasound beam towards the middle of the longus coli. A pre-scan is important to determine the path of needle insertion, as the esophagus, the inferior thyroid artery, and, in some cases, the vertebral artery may obviate the needle insertion path between the carotid artery and the trachea. In this situation, the needle is inserted lateral to the carotid artery (Fig. 2). When advancing the needle from the lateral
4 4 a. ghai et al. Fig. 2. Colour doppler mode used before needling to identify major vessels. [A] Thyroid gland. [B] Carotid artery [C] Internal Jugular vein. [D] Vertebral artery [E] Transverse process of C 7. aspect, the best interval is between the carotid artery and the tip of the anterior tubercle, with needle staying in plane of the ultrasound beam. This needle path avoids hitting the cervical nerve root. This pathway is intramuscular, with needle passing through the sternocleidomastoid and anterior scalene muscle. With this approach, the internal jugular vein can be visualized by decreasing the probe pressure. Avoiding jugular vein puncture is obtained by pushing it away with the needle (Fig. 3). The tip of the needle is directed to the prevertebral fascia, superficial to the longus coli. A total of 5 ml of local anesthetic mixture is injected. The visualization of the spread under real time scanning is important, insofar as the absence of spread indicates intravascular injection (20). This technique improves the safety of the procedure through the direct visualization of the related soft tissue structures that are not visualized with fluoroscopy. It minimizes the risk of thyroid gland, vessels, including vertebral artery, or esophageal injury (21). A minimal amount of drug is also needed (22). It provides real time needle advancement so that the clinician may visualize the needle entry to the soft tissue target? and its final placement in the subfascial plane. Ultrasound guidance allows a direct monitoring of the spread of the local anesthetic solution. It results in more caudal spread due to subfascial injection than cephalic spread due to suprafascial injection with fluoroscopy. Level of sympathetic blockade Studies have shown that blockade at the C 6 level have resulted in more successful sympathetic Fig. 3. Needle path in real time imaging [A] carotid artery [B] Internal jugular vein [C] Needle piercing the fascia covering longus colli. [D] Transverse process of C 7 [E] longus colli. blockade to the head and neck as compared to sympathetic blockade at the C 7 level (2, 14). This is because of the presence of Kuntz s nerves. The caudal spread of the solution to the T 2 to T 3 level is required to block the sympathetic outflow to the upper extremity. Methylene blue dye has been visualized at the stellate ganglion level in only 46% of cases when the C 6 level is targeted, while at C 7 the dye was seen in 63% of cases (22). Therefore, the C 7 level may be more appropriate for upper limb sympathetic blockade. Conclusion Studies using MRI or CT have failed to demonstrate any evi dence of spread to the stellate ganglion itself, However, the use of ultrasound imaging has shown spread from C4 to C7. The bedside availability of ultrasound, the visualization of soft tissues, and the subfascial drug deposition with realtime imaging place the ultrasound above other imaging modalities. References 1. Buckley F. P., Morricca G., Murphy T. M., Neurolytic blockade and hypophysectomy. In : Bonica J. J., The management of pain. 2 nd ed. Philadelphia : Lea and Febiger, 1990, p Elias M., Cervical Sympathetic and stellate ganglion bocks, Pain Physician, 3, , Hogan Q. H., Erickson S. J., Abram S. E., Computerized tomography (CT) guided Stellate ganglion blockade, Anesthesiology, 83, 424-6, Slappendel F., Thijssen H., Crul B. J., Merx J. L., The stellate ganglion in magnetic resonance imaging, a
5 stellate ganglion blockade 5 quantification of anatomic varability, Anesthesiology, 83, 424-6, Higa K., Hirata K., Hirota K., Nithara K., Shono S., Retropharyngeal haematoma after stellate ganglion block, Anesthesiology, 105, , Drake L. D., Vogl W., Michel A. W., Head and Neck. In : Gray s anatomy for students. New York : Churchill Livingstone, 2005, Raj P. P., Stellate ganglion block. In : Waldman and Wenner, eds. Interventional pain management. Philadelphia : WB Saunders publication, 1996, Hogan Q. H., Erickson S. J., Magnetic resonance imaging of stellate ganglion : Normal appearance, Am. J. Roentgen., 158, 655-9, Mamquivst E. L., Bengtsson M., Soren J., Efficacy of stellate ganglion block : A clinical study with bupivacaine, Reg. Anesth., 17, 340-7, Ellis H., Feldman S., Anatomy of Anaesthetists. 3 rd ed. Oxford, Blackwell Scientific Publications, 1979, p Feigl G. C., Rosmarin W., Stelzl A., Weninger B., Likar R., Comparison of different injectate volume for stellate ganglion block : an anatomic and radiologic study, Reg. Anesth. Pain Med., 32, 203-8, Narouze S., Vydyanathan A., Patel N., Ultrasound- guided stellate ganglion block successfully prevented esophageal puncture, Pain Physician, 10, , Abdi S., A new and easy way to block stellate ganglion, Pain Physician, 7, , Jadon A., Revalidation of a modified and safe approach of stellate ganglion block, Indian J. Anaesthesia, 55, 52-6, Sibhata Y., Fujiwara Y., Komatsu T., A new approach of ultrasound guided stellate ganglion block, Anesth. Analg., 105, 550-1, Christie J. M., Martinez C. R., Computerized axial tomography to define the distribution of solution after stellate ganglion nerve block, J. Clin. Anesth., 7 (4), , Kastler D., Aubry S., Sailley N., Michalakis D., Siliman G., Gory G., Lajoie J. L., Kastler B., CT-guided stellate ganglion blockade vs. radiofrequency neurolysis in the management of refractory type I complex regional pain syndrome of the upper limb, Eur. Radiol., 23, , Davies R. M., Stellate ganglion block a new approach, Anaesthesia, 7, , Kapral S., Krafft P., Gosch M., et al., Ultrasound imaging for stellate ganglion block : Direct visualization of puncture site and local anesthetic spread, Reg. Anesth., 20, , Gofeld M., Bhatia A., Abbas S., Ganapathy S., Johnson M., Development and validation of a new technique for ultrasound guided stellate ganglion block, Reg. Anesth. Pain Med., 34, 475-9, Lee M. H., Kim K. Y., Song J. H., Jung H. J., Lim H. K., Lee D. I, et al., Minimal volume of anaesthetic required for an ultrasound guided stellate ganglion block, Pain Medicine, 13, , Harano K., Difference of spread of injectate solutions after stellate ganglion block to sixth and seventh vertebral levels, Anesthesiolgy, 15, 871-7, 1998.
Ultrasound-guided Stellate Ganglion Block Successfully Prevented Esophageal Puncture. Samer Narouze, MD, Amaresh Vydyanathan, MD, and Nilesh Patel, MD
 -Pain Physician 2007; 10:747-752 ISSN 1533-3159 Technical Report Ultrasound-guided Stellate Ganglion Block Successfully Prevented Esophageal Puncture Samer Narouze, MD, Amaresh Vydyanathan, MD, and Nilesh
-Pain Physician 2007; 10:747-752 ISSN 1533-3159 Technical Report Ultrasound-guided Stellate Ganglion Block Successfully Prevented Esophageal Puncture Samer Narouze, MD, Amaresh Vydyanathan, MD, and Nilesh
Comparative Study between Ultrasound Guided Lateral and Anterior Approach for Stellate Ganglion Block
 Med. J. Cairo Univ., Vol. 84,. 1, December: 1525-153, 16 www.medicaljournalofcairouniversity.net Comparative Study between Ultrasound Guided Lateral and Anterior Approach for Stellate Ganglion Block KHALED
Med. J. Cairo Univ., Vol. 84,. 1, December: 1525-153, 16 www.medicaljournalofcairouniversity.net Comparative Study between Ultrasound Guided Lateral and Anterior Approach for Stellate Ganglion Block KHALED
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E
 Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Department of Physical Medicine and Rehabilitation, Korea University Guro Hospital, Seoul, Korea
 Original Article Ann Rehabil Med 2016;40(2):244-251 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2016.40.2.244 Annals of Rehabilitation Medicine Sonoanatomical Change of Phrenic Nerve
Original Article Ann Rehabil Med 2016;40(2):244-251 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2016.40.2.244 Annals of Rehabilitation Medicine Sonoanatomical Change of Phrenic Nerve
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Estimation of Stellate Ganglion Block Injection Point Using the Cricoid Cartilage as Landmark Through X-ray Review
 Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
USRA OF THE UPPER EXTREMITY
 USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Interscalene brachial plexus blockade - indications, anatomy, practical performance
 08RC2 Interscalene brachial plexus blockade - indications, anatomy, practical performance Urs Eichenberger Department of Anaesthesiology and Pain Therapy, University Hospital of Bern, Switzerland Saturday,
08RC2 Interscalene brachial plexus blockade - indications, anatomy, practical performance Urs Eichenberger Department of Anaesthesiology and Pain Therapy, University Hospital of Bern, Switzerland Saturday,
SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES
 SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES Overview Eugene Mitchell, MD Activity of the sympathetic efferents and their role in the pathology of chronic pain
SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES Overview Eugene Mitchell, MD Activity of the sympathetic efferents and their role in the pathology of chronic pain
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Neck Ultrasound. Faculty Info: Amy Kule, MD
 Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Types of blocks. Clinical considerations 8/11/2009. Let s Discuss Sympathetic Blocks. Stellate Celiac plexis Lumbar sympathetic Hypogastric
 Let s Discuss Sympathetic Blocks Janette Elliott, RN-BC, MSN, AOCN ASPMN 19 th Annual Conference September 2009 Types of blocks Stellate Celiac plexis Lumbar sympathetic Hypogastric Clinical considerations
Let s Discuss Sympathetic Blocks Janette Elliott, RN-BC, MSN, AOCN ASPMN 19 th Annual Conference September 2009 Types of blocks Stellate Celiac plexis Lumbar sympathetic Hypogastric Clinical considerations
Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear Transducer
 ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
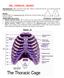 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Vascular Access (venous (peripheral and central) and arterial)
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
ISPUB.COM. Lumbar Sympathectomy by Laser Technique. S Kantha, B Kantha METHODS AND MATERIALS
 ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
A study of the anatomy of the caudal space using magnetic resonance imaging
 British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
Interscalene brachial plexus blocks in the management of shoulder dislocations
 Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Prevertebral Region, Pharynx and Soft Palate
 Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Welcome to ANAT 10A! What is Anatomy? Different levels of Anatomy The Language of Anatomy Pearson Education, Inc.
 Welcome to ANAT 10A! What is Anatomy? Different levels of Anatomy The Language of Anatomy Introduction Anatomy means to dissect: (ANAT 10A) The study of internal & external body structures The study of
Welcome to ANAT 10A! What is Anatomy? Different levels of Anatomy The Language of Anatomy Introduction Anatomy means to dissect: (ANAT 10A) The study of internal & external body structures The study of
Correspondence should be addressed to Stanley K. H. Lam;
 Hindawi BioMed Research International Volume 2017, Article ID 7920438, 17 pages https://doi.org/10.1155/2017/7920438 Research Article Transition from Deep Regional Blocks toward Deep Nerve Hydrodissection
Hindawi BioMed Research International Volume 2017, Article ID 7920438, 17 pages https://doi.org/10.1155/2017/7920438 Research Article Transition from Deep Regional Blocks toward Deep Nerve Hydrodissection
Neck-2. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
Anatomy for anaesthetists
 VOL 17 NO 1 ANESTHESIA JANUARY 1962 Anatomy for anaesthetists (4) The thoracic inlet and the first rib HAROLD ELLIS, MCh, FRCS Senior Lecturer in Surgery, Westminster Hospital Illustrated by MISS MARGARET
VOL 17 NO 1 ANESTHESIA JANUARY 1962 Anatomy for anaesthetists (4) The thoracic inlet and the first rib HAROLD ELLIS, MCh, FRCS Senior Lecturer in Surgery, Westminster Hospital Illustrated by MISS MARGARET
Anatomy and Physiology II. Spine
 Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
nerve blocks in the diagnosis and therapy of visceral disease
 Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Diana Mathioudakis DEAA EDIC AFRCA. consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d)
 & Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
& Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
Superficial (and Intermediate) Cervical Plexus Block
 Superficial (and Intermediate) Cervical Plexus Block Indications: -Tympanomastoid surgery. When combined with the auricular branch of the vagus ( nerve of arnold ) by infiltrating subcutaneously into the
Superficial (and Intermediate) Cervical Plexus Block Indications: -Tympanomastoid surgery. When combined with the auricular branch of the vagus ( nerve of arnold ) by infiltrating subcutaneously into the
REGIONAL/LOCAL ANESTHESIA and OBESITY
 REGIONAL/LOCAL ANESTHESIA and OBESITY Jay B. Brodsky, MD Stanford University School of Medicine Jbrodsky@stanford.edu Potential Advantages Regional compared to General Anesthesia Minimal intra-operative
REGIONAL/LOCAL ANESTHESIA and OBESITY Jay B. Brodsky, MD Stanford University School of Medicine Jbrodsky@stanford.edu Potential Advantages Regional compared to General Anesthesia Minimal intra-operative
Brachial Plexus Nerve Block with CT Guidance for Regional Pain Management: Initial Results 1
 Technical Developments Suresh K. Mukherji, MD Archana Wagle, MD Diane M. Armao, MD Sunil Dogra, MD Index terms: Brachial plexus, 276.126 Computed tomography (CT), guidance, 276.1211 Interventional procedures,
Technical Developments Suresh K. Mukherji, MD Archana Wagle, MD Diane M. Armao, MD Sunil Dogra, MD Index terms: Brachial plexus, 276.126 Computed tomography (CT), guidance, 276.1211 Interventional procedures,
Lies in front and sides of the neck. Consists of two lobe connected anterior to the trachea by an isthmus.
 THYROID GLAND 1 Lies in front and sides of the neck. Consists of two lobe connected anterior to the trachea by an isthmus. A small pyramidal lobe projects upwards from the left lobe in 40% of cases. The
THYROID GLAND 1 Lies in front and sides of the neck. Consists of two lobe connected anterior to the trachea by an isthmus. A small pyramidal lobe projects upwards from the left lobe in 40% of cases. The
Veins of the Face and the Neck
 Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
JlntSocPlastination, Vol4:16-22,
 JlntSocPlastination, Vol4:16-22, 1990 16 SECTIONAL ANATOMY: STANDARDIZED METHODOLOGY Alexander Lane, Coordinator of Anatomy and Physiology, Triton College, Visiting Associate Professor, University of Illinois
JlntSocPlastination, Vol4:16-22, 1990 16 SECTIONAL ANATOMY: STANDARDIZED METHODOLOGY Alexander Lane, Coordinator of Anatomy and Physiology, Triton College, Visiting Associate Professor, University of Illinois
Human Anatomy Biology 351
 nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Ultrasound-Guided Superior Hypogastric Plexus Block: A Cadaveric Feasibility Study with Fluoroscopic Confirmation
 ORIGINAL ARTICLE Ultrasound-Guided Superior Hypogastric Plexus Block: A Cadaveric Feasibility Study with Fluoroscopic Confirmation Michael Gofeld, MD; Chuan-Whei Lee, MBChB Department of Anesthesia, St
ORIGINAL ARTICLE Ultrasound-Guided Superior Hypogastric Plexus Block: A Cadaveric Feasibility Study with Fluoroscopic Confirmation Michael Gofeld, MD; Chuan-Whei Lee, MBChB Department of Anesthesia, St
THE ANATOMICAL APPROACH IN STELLATE GANGLION INJECTION
 Brit. J. Anaesth. (1955), 27, 616 THE ANATOMICAL APPROACH IN STELLATE GANGLION INJECTION BY W. K. J. WALLS Department of Anatomy, University of Leeds THE sympathetic outflow to the head and neck and the
Brit. J. Anaesth. (1955), 27, 616 THE ANATOMICAL APPROACH IN STELLATE GANGLION INJECTION BY W. K. J. WALLS Department of Anatomy, University of Leeds THE sympathetic outflow to the head and neck and the
Anatomical Terminology
 Anatomical Terminology Dr. A. Ebneshahidi Anatomy Anatomy : is the study of structures or body parts and their relationships to on another. Anatomy : Gross anatomy - macroscopic. Histology - microscopic.
Anatomical Terminology Dr. A. Ebneshahidi Anatomy Anatomy : is the study of structures or body parts and their relationships to on another. Anatomy : Gross anatomy - macroscopic. Histology - microscopic.
The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care settings,
 American Journal of Emergency Medicine (2011) xx, xxx xxx www.elsevier.com/locate/ajem Clinical Notes The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care
American Journal of Emergency Medicine (2011) xx, xxx xxx www.elsevier.com/locate/ajem Clinical Notes The ultrasound-guided superficial cervical plexus block for anesthesia and analgesia in emergency care
The Language of Anatomy. (Anatomical Terminology)
 The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
Infraclavicular brachial plexus blocks have been designed
 The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Technical Note NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE FLUOROSCOPIC VIEWS DURING CERVICAL RADIOFREQUENCY NEUROTOMY.
 Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
Thyroid and Parathyroid Glands
 Thyroid and Parathyroid Glands Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/ explanation Objectives: By the end of the lecture,
Thyroid and Parathyroid Glands Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/ explanation Objectives: By the end of the lecture,
A Rare Case of Bilateral Jugular Venous Malformation
 JOURNAL OF CASE REPORTS 2013;3(2):326-330 A Rare Case of Bilateral Jugular Venous Malformation Prasanna LC, Alva R, D Souza AS, Bhat KMR Department of Anatomy, Kasturba Medical College, Manipal University,
JOURNAL OF CASE REPORTS 2013;3(2):326-330 A Rare Case of Bilateral Jugular Venous Malformation Prasanna LC, Alva R, D Souza AS, Bhat KMR Department of Anatomy, Kasturba Medical College, Manipal University,
Ultrasound-guided Pulsed Radiofrequency of the Third Occipital Nerve
 Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Mediastinum and pericardium
 Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Ultrasound-guided supraclavicular block
 THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
CHAPTER 5 Femoral Nerve Block. Arun Nagdev, MD Mike Mallin, MD, RDCS, RDMS
 CHAPTER 5 Femoral Nerve Block Arun Nagdev, MD Mike Mallin, MD, RDCS, RDMS SECTION 1 Introduction An ultrasound-guided femoral nerve block (USFNB) can be a rapid and definitive tool for pain control for
CHAPTER 5 Femoral Nerve Block Arun Nagdev, MD Mike Mallin, MD, RDCS, RDMS SECTION 1 Introduction An ultrasound-guided femoral nerve block (USFNB) can be a rapid and definitive tool for pain control for
Ultrasound Guided Regional Nerve Blocks
 Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Organisation of the nervous system
 Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
The goal of this article is to describe the. Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation.
 Pain Physician 2011; 14:45-53 ISSN 1533-3159 Technique Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation Jie Zhu, MD 1, Frank Falco, MD 1,2, C. Obi Onyewu, MD 1, Youssef
Pain Physician 2011; 14:45-53 ISSN 1533-3159 Technique Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation Jie Zhu, MD 1, Frank Falco, MD 1,2, C. Obi Onyewu, MD 1, Youssef
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Original Article Clinics in Orthopedic Surgery 2013;5:
 Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
A New Anterior Approach for Fluoroscopy-guided Suprascapular Nerve Block
 Original Article Korean J Pain 2012 July; Vol. 25, No. 3: 168-172 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.3.168 A New Anterior Approach for Fluoroscopy-guided Suprascapular
Original Article Korean J Pain 2012 July; Vol. 25, No. 3: 168-172 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.3.168 A New Anterior Approach for Fluoroscopy-guided Suprascapular
A Comparison between the Anterior and Posterior Approach to US-guided Shoulder Articular Injections for MR Arthrography 1
 A Comparison between the Anterior and Posterior Approach to US-guided Shoulder Articular Injections for MR Arthrography 1 Joo Yeon Ji, M.D. Purpose: To assess the feasibility of ultrasound-guided shoulder
A Comparison between the Anterior and Posterior Approach to US-guided Shoulder Articular Injections for MR Arthrography 1 Joo Yeon Ji, M.D. Purpose: To assess the feasibility of ultrasound-guided shoulder
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
The Neck. BY: Lina Abdullah & Rahaf Jreisat
 The Neck BY: Lina Abdullah & Rahaf Jreisat Boundaries of the Neck: generally from base of the skull to root of the neck Superior margin :From superior nuchal line of occipital bone up to mastoid process
The Neck BY: Lina Abdullah & Rahaf Jreisat Boundaries of the Neck: generally from base of the skull to root of the neck Superior margin :From superior nuchal line of occipital bone up to mastoid process
Thyroidectomy. Siu Kwan Ng. Modified Radical Neck Dissection Type II 47
 06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
First stage Lec.1 : Introduction. Asst.Lec.Dr.ABDULRIDHA ALASADY
 First stage 2018-2019 Lec.1 : Introduction Asst.Lec.Dr.ABDULRIDHA ALASADY Anatomy the study of the structure and shape of the body and body parts & their relationships to one another aided by dissection
First stage 2018-2019 Lec.1 : Introduction Asst.Lec.Dr.ABDULRIDHA ALASADY Anatomy the study of the structure and shape of the body and body parts & their relationships to one another aided by dissection
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
Lecture 01. The Thyroid & Parathyroid Glands. By: Dr Farooq Khan PMC Date: 12 th March. 2018
 Lecture 01 The Thyroid & Parathyroid Glands By: Dr Farooq Khan PMC Date: 12 th March. 2018 INTRODUCTION LAYERS OF THE NECK The neck has four major compartments or layer which are enclosed by an outer musculofascial
Lecture 01 The Thyroid & Parathyroid Glands By: Dr Farooq Khan PMC Date: 12 th March. 2018 INTRODUCTION LAYERS OF THE NECK The neck has four major compartments or layer which are enclosed by an outer musculofascial
Introduction to The Human Body
 1 Introduction to The Human Body FOCUS: The human organism is often examined at seven structural levels: chemical, organelle, cell, tissue, organ, organ system, and the organism. Anatomy examines the structure
1 Introduction to The Human Body FOCUS: The human organism is often examined at seven structural levels: chemical, organelle, cell, tissue, organ, organ system, and the organism. Anatomy examines the structure
Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli.
 Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli. Rectus Capitis Anterior. Rectus Capitis Lateralis. Rectus Capitis
Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli. Rectus Capitis Anterior. Rectus Capitis Lateralis. Rectus Capitis
THYROID & PARATHYROID. By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy
 THYROID & PARATHYROID By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy 1 OBJECTIVES By the end of the lecture, the student should be able to: Describe the shape, position, relations and structure of
THYROID & PARATHYROID By Prof. Saeed Abuel Makarem & Dr. Sanaa Al-Sharawy 1 OBJECTIVES By the end of the lecture, the student should be able to: Describe the shape, position, relations and structure of
Cervical Spine: Pearls and Pitfalls
 Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
INTRODUCTION. Getting the best scan. Choosing a probe. Choosing the frequency
 Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
Drawing Blood From the Llama (Venipuncture)
 Drawing Blood From the Llama (Venipuncture) Drawing blood (venipuncture) in the llama is more difficult than in common domestic animals. Their wooly fleece impairs visibility when you try to locate the
Drawing Blood From the Llama (Venipuncture) Drawing blood (venipuncture) in the llama is more difficult than in common domestic animals. Their wooly fleece impairs visibility when you try to locate the
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Magnetic Resonance Imaging Demonstrates Lack of Precision in Needle Placement by the Infraclavicular Brachial Plexus Block Described by Raj Et Al.
 Magnetic Resonance Imaging Demonstrates Lack of Precision in Needle Placement by the Infraclavicular Brachial Plexus Block Described by Raj Et Al. Øivind Klaastad, MD*, Finn G. Lilleås, MD, Jan S. Røtnes,
Magnetic Resonance Imaging Demonstrates Lack of Precision in Needle Placement by the Infraclavicular Brachial Plexus Block Described by Raj Et Al. Øivind Klaastad, MD*, Finn G. Lilleås, MD, Jan S. Røtnes,
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
Ultrasound guidance for interventional pain management
 Faculty Disclosure Ultrasound guidance for interventional pain management Dr. Roel Mestrum, MD, FIPP Anesthesiology, Intensive Care Medicine and Multidisciplinary Pain Centre Regionaal Ziekenhuis Heilig
Faculty Disclosure Ultrasound guidance for interventional pain management Dr. Roel Mestrum, MD, FIPP Anesthesiology, Intensive Care Medicine and Multidisciplinary Pain Centre Regionaal Ziekenhuis Heilig
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
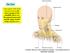 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
Head & Neck Contouring
 Head & Neck Contouring Presented by James Wheeler, MD Center for Cancer Care Goshen, IN 46526 September 12, 2014 Special Thanks to: Spencer Boulter, Director of Operations (AAMD) Adam Moore, RT(T), CMD
Head & Neck Contouring Presented by James Wheeler, MD Center for Cancer Care Goshen, IN 46526 September 12, 2014 Special Thanks to: Spencer Boulter, Director of Operations (AAMD) Adam Moore, RT(T), CMD
Review Article. Cervical Sympathetic and Stellate Ganglion Blocks. Elias Cervical Sympathetic Blocks. Mazin Elias, MD
 294 Pain Physician, Volume 3, Number 3, pp 294-304 2000, Association of Pain Management Anesthesiologists Review Article Cervical Sympathetic and Stellate Ganglion Blocks Mazin Elias, MD Sympathetic blocks
294 Pain Physician, Volume 3, Number 3, pp 294-304 2000, Association of Pain Management Anesthesiologists Review Article Cervical Sympathetic and Stellate Ganglion Blocks Mazin Elias, MD Sympathetic blocks
Diaphragm and intercostal muscles. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Cervical Cooled RF Training Presentation
 Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Anuj Bhatia, MD David Flamer, MD Philip W. H. Peng, MD
 Can J Anesth/J Can Anesth (2012) 59:1040 1047 DOI 10.1007/s12630-012-9779-4 REPORTS OF ORIGINAL INVESTIGATIONS Evaluation of sonoanatomy relevant to performing stellate ganglion blocks using anterior and
Can J Anesth/J Can Anesth (2012) 59:1040 1047 DOI 10.1007/s12630-012-9779-4 REPORTS OF ORIGINAL INVESTIGATIONS Evaluation of sonoanatomy relevant to performing stellate ganglion blocks using anterior and
The role of ultrasound duplex in endovenous procedures
 The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
Transsacrococcygeal Approach to Ganglion Impar Block for Management Of Chronic Perineal Pain: A Prospective Observational Study
 Pain Physician 2007; 10:661-666 ISSN 1533-3159 Prospective Evaluation Transsacrococcygeal Approach to Ganglion Impar Block for Management Of Chronic Perineal Pain: A Prospective Observational Study Gokul
Pain Physician 2007; 10:661-666 ISSN 1533-3159 Prospective Evaluation Transsacrococcygeal Approach to Ganglion Impar Block for Management Of Chronic Perineal Pain: A Prospective Observational Study Gokul
thoracic cage inlet and outlet landmarks of the anterior chest wall muscles of the thoracic wall sternum joints ribs intercostal spaces diaphragm
 Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Surgical anatomy of thyroid and parathyroid glands
 Head & Neck Surgery Course Surgical anatomy of thyroid and parathyroid glands Dr Pierfrancesco PELLICCIA Pr Benjamin LALLEMANT Service ORL et CMF CHU de Nîmes CH de Arles Thyroid glands Dr Pierfrancesco
Head & Neck Surgery Course Surgical anatomy of thyroid and parathyroid glands Dr Pierfrancesco PELLICCIA Pr Benjamin LALLEMANT Service ORL et CMF CHU de Nîmes CH de Arles Thyroid glands Dr Pierfrancesco
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Anatomy notes-thorax.
 Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Ultrasound Guidance Needle Techniques
 Ultrasound Guidance Needle Techniques Dr TANG Ho-ming AED/UCH USG Guidance Needle Techniques Commonly used in EM 1. Vessel cannulation-peripheral & central 2. Foreign body removal 3. Peripheral nerve/plexus
Ultrasound Guidance Needle Techniques Dr TANG Ho-ming AED/UCH USG Guidance Needle Techniques Commonly used in EM 1. Vessel cannulation-peripheral & central 2. Foreign body removal 3. Peripheral nerve/plexus
SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE CORNISH TECHNIQUE
 THE JOURNAL OF NEW YORK SCHOOL OF REGIONAL ANESTHESIA SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE BY CORHISH PB Author Affiliation: Nelson, New Zealand This essay is based on a project which has
THE JOURNAL OF NEW YORK SCHOOL OF REGIONAL ANESTHESIA SUPRACLAVICULAR REGIONAL ANAESTHESIA REANALYSED: THE BY CORHISH PB Author Affiliation: Nelson, New Zealand This essay is based on a project which has
Classification of the nervous system. Prof. Dr. Nikolai Lazarov 2
 1 1. Formation and general organization 2. Spinal ganglia 3. Zonal and segmental innervation 4. Dorsal rami of the spinal nerves 5. Ventral rami of the spinal nerves 6. Cervical plexus Classification of
1 1. Formation and general organization 2. Spinal ganglia 3. Zonal and segmental innervation 4. Dorsal rami of the spinal nerves 5. Ventral rami of the spinal nerves 6. Cervical plexus Classification of
Infraclavicular brachial plexus blocks aim at the
 REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
Body Planes & Positions
 Learning Objectives Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how it is used to reference the body. Distinguish
Learning Objectives Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how it is used to reference the body. Distinguish
Tympanic Bulla Temporal Bone. Digastric Muscle. Masseter Muscle
 Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
