Salvage of first metatarsophalangeal joint arthroplasty complications
|
|
|
- Austen Terry
- 6 years ago
- Views:
Transcription
1 Foot Ankle Clin N Am 8 (2003) Salvage of first metatarsophalangeal joint arthroplasty complications Judith F. Baumhauer, MD*, Benedict F. DiGiovanni, MD Orthopedic Department, University of Rochester Medical Center, 601 Elmwood Avenue, Box 665, Rochester, NY 14642, USA There are two broad categories of surgical techniques for first metatarsophalangeal joint arthroplasty. Resection arthroplasty is a resection of the base of the proximal phalanx with or without an interposition graft of capsule or adjacent tendon (Fig. 1). The second technique involves a partial or complete joint replacement (Fig. 2). The primary indication for these procedures is first metatarsophalangeal joint pain caused by arthritic change. The salvage surgical options for failed metatarsophalangeal joint arthroplasty are directed toward decreasing or eliminating the symptoms arising from the complications of these procedures. Resection arthroplasty Resection arthroplasty as a treatment for bunions was originally described by Keller in 1904 [1]. Indications for the procedure have expanded to include patients with arthritis of the first metatarsophalangeal (MTP) joint. Although pain centered around the first metatarsophalangeal joint was often improved after a Keller resection arthroplasty, a number of complications were described that have made this procedure less popular over the last 10 to 15 years. Postoperative metatarsalgia is the most frequently reported complication associated with a Keller resection arthroplasty [2 4]. Additionally, preoperative metatarsalgia often persists after the Keller procedure [3,5 9]. Other reported complications that resulted from joint resection arthroplasty include excessive shortening of the hallux [2,3], narrowing of the space of the first metatarsophalangeal joint over time [10], impaired weightbearing function of the hallux with weakening of the * Corresponding author. address: Judy_Baumhauer@URMC.rochester.edu (J.F. Baumhauer) /03/$ see front matter D 2003, Elsevier Science (USA). All rights reserved. PII: S (02)
2 38 J.F. Baumhauer, B.F. DiGiovanni / Foot Ankle Clin N Am 8 (2003) Fig. 1. A/P radiograph of a joint resection arthroplasty of the hallux. foot or toe [4,11], claw toe or cock up toe deformity of the hallux (Fig. 3) [12], and reduced motion of the interphalangeal joint [10]. The surgical technique may be one factor that influences the rate of these complications. The recommended fraction of proximal phalanx resection is broad and ranges from one third to two thirds of the bone length [7,8,13]. The more bone that is resected, the greater the risk of destabilizing the hallux; this leads to a loss of weightbearing function and the transfer of weight to the lateral rays, termed transfer metatarsalgia [2,12,14,15]. With excessive bone resection and the development of these complications, salvage can be challenging. Recommendations for an interposition iliac crest bone graft to restore hallux length, in addition to performing a first MTP arthrodesis, was described [6]. Two factors that were reported to influence the salvage arthrodesis rates include limited motion of the interphalangeal joint and an insufficient amount of bone remaining of the proximal phalanx [6]. Compared with a primary arthrodesis of the first MTP joint with a success rate of approximately 85% to 95% [16,17], the salvage MTP arthrodesis success rate ranges from 75% to 82% [5,6,9,18 20].
3 J.F. Baumhauer, B.F. DiGiovanni / Foot Ankle Clin N Am 8 (2003) Fig. 2. A/P radiograph of a single stem silicone replacement arthroplasty of the hallux. Literature review There are limited data about the success rate for arthrodesis of the first metatarsophalangeal joint as a salvage for a failed Keller resection arthroplasty [5,6,9,18 20]. Coughlin and Mann [6] reported on 11 patients (16 feet) who had an arthrodesis procedure for failed Keller resection arthroplasty. The major preoperative, subjective complaint was pain at the first MTP joint. Seventy-five percent of the patients also complained of lateral metatarsalgia and 88% had intractable plantar keratosis. Ninety-four percent had a cock up toe deformity of the hallux and 25% had marked shortening of the proximal phalanx. The surgical technique varied depending upon the amount of bone that was previously
4 40 J.F. Baumhauer, B.F. DiGiovanni / Foot Ankle Clin N Am 8 (2003) Fig. 3. Lateral radiograph illustrating a cock up deformity of the hallux. resected and the need for iliac crest interposition bone graft (four patients). Two longitudinal, double-ended, threaded Steinmann pins were used for fixation in the patients who did not require a bone graft. These pins remained for 12 to 16 weeks postoperatively. The patients who underwent interposition bone graft had three, threaded Steinmann pins which remained for 12 to 20 weeks postoperatively. All arthrodeses healed successfully. Twelve feet were rated as excellent and four had good results. Patients had decreased pain and improved ability to walk. Only one patient had mild transfer metatarsalgia complaints after the procedure. Motion at the interphalangeal joint was not significantly different after fusion. The authors concluded that an arthrodesis of the metatarsophalangeal joint is a useful and reliable technique for salvage of a failed Keller resection arthroplasty. An extensive literature review identified 11 additional patients in five articles in which a first MTP arthrodesis was performed for a failed Keller resection arthroplasty [5,9,18 20]. An average of an 82% success rate was achieved by using a variety of surgical techniques. Although a specific analysis of these patients was not performed, the data support the premise that a successful arthrodesis is more difficult to achieve with previous resection of bone. First metatarsophalangeal joint replacement arthroplasty Replacement arthroplasty of the first metatarsophalangeal joint has evolved over the past 30 to 40 years [21 34]. The advantages of the procedure include preservation or restoration of motion and excellent pain relief. The disadvantages include material failure of the implant which leads to silicone-induced synovitis and osteolysis [35 37]. The first metatarsophalangeal joint weightbearing function is altered as is the strength of the hallux because of the shortening and subluxation which occurs with joint replacement [25,35,38,39]. Patient complaints include transfer metatarsalgia, loss of motion at the first MTP joint
5 secondary to foreign body reaction and bone fragmentation, shortening of the toe, claw toe, or cock up toe deformity of the hallux. A wide spectrum of design factors affect the outcome of joint replacement arthroplasty (Box 1). These design factors influence the salvage of this procedure [40]. In the late 1970s, silicone implants were commonly used for metacarpophalangeal joint replacement surgery for the hand. The implants and techniques were extended to the feet for replacement of arthritic and malaligned metatarsophalangeal joints [30,31,41]. With significantly higher biomechanical demands, including the weightbearing function of the foot and differing joint kinematics of the MTP joints, the implants failed. The failure produced an inflammatory response with cyst formation, avascular cellular stroma, multinucleated giant cells, and wear debris with fragmentation of the prosthesis (Fig. 4) [35 37]. The destructive silicone synovitis process resulted in additional bone loss that was compounded by the amount of bone that was removed initially for placement of the prosthesis. The silicone implant design can be single- or double-hinged. The doublehinged components require that more bone is removed during initial placement. Alternative biomaterials that have been used for joint replacements include titanium with or without a polyethylene joint surface. These metal components were designed to replace the metatarsal head and proximal phalanx base or the phalanx base alone. The more bone that is resected with implant components, the greater the destabilization of the soft tissues and risk for subluxation and dislocation of the toe. Literature review J.F. Baumhauer, B.F. DiGiovanni / Foot Ankle Clin N Am 8 (2003) Two techniques were suggested for salvage of a failed first metatarsophalangeal joint replacement arthroplasty. Kitaoka [42] described a technique of implant Box 1. Design factors that affect the outcome of joint replacement arthroplasty Silicone stem Single Double Hinged Titanium stem Single Double With or without polyethylene With or without titanium grommets
6 42 J.F. Baumhauer, B.F. DiGiovanni / Foot Ankle Clin N Am 8 (2003) Fig. 4. A/P radiograph demonstrating first metatarsal head osteolysis, cyst formation, and proximal phalanx reactive bone spur formation secondary to silicone synovitis. removal and synovectomy for the treatment of 14 silicone-implant arthroplasties. Revision surgery was performed at an average of 3.1 years after the arthroplasty. The average follow-up was 4.9 years in 10 patients. Clinical results were judged as excellent in seven patients, good in one patient, fair in one patient, and poor in one patient. Clinical alignment did not change after removal of the implant although a trend toward toe extension (cock up deformity) was noted. Dynamic force plate studies were performed which demonstrated unweighting of the plantar aspect of the first metatarsal head and transfer of the loading to the lateral forefoot. The great toe had less contact time during gait in the involved feet than in the control feet. Hecht et al [43] reported on 15 feet that were treated with arthrodesis of the first metatarsophalangeal joint to salvage a failed silicone-implant arthroplasty. The average duration of follow-up was 55 months. The indication for surgery was first MTP joint pain that interfered with activities of daily living. Bone grafting was used in all cases. Eight cases had cancellous bone only and seven cases had tricortical interposition bone grafts. Two types of fixation were performed. Two intermedullary-threaded Steinmann pins were used in six cases; nine cases had an oblique compression screw technique with the application of a three- or four-hole,
7 J.F. Baumhauer, B.F. DiGiovanni / Foot Ankle Clin N Am 8 (2003) one third semitubular, dorsal neutralization plate. Of the 10 patients who underwent tricortical interposition bone graft, eight cases went on to solid union on both sides of the graft. Five of six cases that were fixed internally with Steinmann pins successfully fused at an average of approximately 14 weeks. Nine of 10 cases that were fixed with compression screws and dorsal plates successfully fused at approximately 8 weeks. Clinically, there was no evidence of transfer lesions, first MTP joint tenderness, or hallux subluxation. The hallux length was well-maintained after surgery with bone grafting. Sagittal and coronal plane alignment was difficult to achieve initially intraoperatively and to maintain after treatment. Walking ability was improved and patients had less pain after surgery. The overall level of satisfaction was high. The authors concluded that arthrodesis of the first metatarsophalangeal joint that uses bone graft to salvage a failed silicone-implant arthroplasty produced acceptable subjective and radiographic results. Although technically demanding, it produces long-term stability to the hallux, restores weightbearing, and allows for maintenance of propulsive gait. The authors recommended an arthrodesis procedure instead of an excisional arthroplasty of the implant to maintain a high level of function and overall patient satisfaction. The explanation for similar satisfactory results with both techniques may lie with the inflammatory reaction and scar formation that surround the silicone implants. This rind of tissue may impart some additional stability when removal of the implant is performed alone. Additional research is needed to support this theory. No studies are available to review the outcomes after implant removal versus arthrodesis following failed arthroplasty surgery with metal implants. The reactive scar is less impressive with metallic implants; an isolated implant removal may not impart the same level of stability to the hallux that results in less satisfactory results in this patient population. Preferred approach In patients with preoperative complaints of lateral ray metatarsalgia, a cock up toe deformity, or alignment issues that involve the hallux, a first MTP arthrodesis is the preferred surgical approach to stabilize the ray, while improving weightbearing function and alignment. In the elderly, more sedentary patient, an iliac crest interposition graft is not used. A medial malleolar bone graft may be obtained to fill in the metatarsal and proximal phalanx canal to facilitate fusion. Multiple, intermedullary, fully-threaded Steinmann pins are placed from the toe tip across the interphalangeal joint and metatarsophalangeal joint. They are cut short and buried beneath the skin by advancing the wire manually with a needle holder (Fig. 5). Because of the loss of length, less dorsiflexion and valgus positioning of the fusion is required. The toe is positioned in approximately 5 of dorsiflexion and 3 to 5 degrees of valgus. Careful preoperative assessment that specifically looks for osteoporosis is performed. A bone density evaluation is obtained if it is believed to be necessary. After bone graft harvesting, a stress fracture of the distal tibial metaphysis can occur in osteoporotic patients with
8 44 J.F. Baumhauer, B.F. DiGiovanni / Foot Ankle Clin N Am 8 (2003) Fig. 5. A/P radiograph of a first metatarsophalangeal arthrodesis using retrograde threaded Steinmann pins. Metatarsal head resections have been performed of the lesser toes stabilized with longitudinal smooth Kirshner wires. advancement to weightbearing, despite the use of a small, oval, cortical window. A common complication is prominent hardware. The Steinmann pins may become exposed at the toe tip in the future, which necessitates that pin s removal. The younger, more active patient with significant bone loss may be a candidate for an iliac crest interposition bone graft to re-establish length and weightbearing function. Preoperative education of the patient is important. A nonunion at one side of the bone graft occurs frequently and may require a second bone grafting procedure with cancellous bone to obtain a solid fusion (Figs. 6, 7). The hallux is positioned in 10 to 15 of dorsiflexion in relationship to the floor and 5 to 10 of valgus or adjacent to the second toe. A dorsal six- or seven-hole plate placed with compression-plating technique is used for stabilization. The postoperative protocol for either arthrodesis technique requires the patient to be nonweightbearing for 3 weeks. Elevation of the extremity is emphasized to
9 J.F. Baumhauer, B.F. DiGiovanni / Foot Ankle Clin N Am 8 (2003) Fig. 6. A/P and lateral foot radiographs depicting a first MTP arthrodesis with interposition iliac crest bone graft and stabilized with dorsal compressive plating technique. Fig. 7. A/P and lateral foot radiographs depicting a first MTP arthrodesis with interposition iliac crest bone graft and stabilized with dorsal compressive plating technique.
10 46 J.F. Baumhauer, B.F. DiGiovanni / Foot Ankle Clin N Am 8 (2003) aid in wound healing during this time. The patient is then placed in a short-leg walking cast for 5 additional weeks and radiographs are obtained at 8 weeks. If progressive bone healing is seen on radiographs and the patient is not tender at the MTP joint, the patient is placed in a stiff-soled, postoperative shoe and allowed to transition into a sneaker when swelling and comfort allow. This may take several weeks and the patient should be made aware of this preoperatively. Follow-up films are obtained 3 months after surgery. Isolated joint replacement removal is performed in the patient without lateral transfer lesions or in the patient with multiple medical problems that preclude arthrodesis. For the first 3 weeks after surgery, the patient is encouraged to keep the limb elevated and minimize the amount of walking in a postoperative shoe. After the wounds have healed, the patient may wear a regular shoe. A toe spacer between the great and second toes is used for 3 months to discourage molding of the great toe laterally or drifting into valgus. A multitude of shoe and orthotic modifications may aid in modifying weightbearing and can be used in the patient with transfer metatarsalgia, hallux instability, and joint pain. They include a custom metatarsal pad added just proximal to the painful metatarsal head to unweight the area. Shoe stretching or a high toe box shoe may be used to avoid rubbing of the hallux on the shoe. These alterations can be performed preoperatively or postoperatively to decrease the patient s symptoms. References [1] Keller WL. The surgical treatment of bunions and hallux valgus. NY Med J 1904;80: [2] Henry APJ, Waugh W. The use of footprints in assessing the results of operations for hallux valgus. A comparison of Keller s operation and arthrodesis. JBJS 1975;57-B(4): [3] Humbert JL, Bourbonniere C, Laurin CA. Metatarsophalangeal fusion for hallux valgus: indications and effect on the first metatarsal ray. Canadian Med Assn J 1979;120: [4] Rogers WA, Joplin RJ. Hallux valgus, weak foot and the Keller operation: an end-result study. Surg Clin North Am 1947;27: [5] Cleveland M, Winant EM. An end-result study of the Keller operation. JBJS 1950;32A: [6] Coughlin MJ, Mann RA. Arthrodesis of the first metatarsophalangeal joint as salvage for the failed Keller procedure. JBJS 1987;69A(1): [7] Jordan HH, Brodsky AE. Keller operation for hallux valgus and hallux rigidus. An end result study. Arch Surg 1951;62: [8] Moynihan FJ. Arthrodesis of the metatarsophalangeal joint of the great toe. JBJS 1967;49B(3): [9] Zadik FR. Arthrodesis of the great toe. BMJ 1960;2: [10] Thomas FB. Keller s arthroplasty modified. A technique to ensure post-operative distraction of the toe. JBJS 1962;44B(2): [11] Marin GA. Arthrodesis of the metatarsophalangeal joint of the big toe for hallux valgus and hallux rigidus. A new method. Internat Surg 1968;50: [12] Jahss MH. The sesamoids of the hallux. Clin Orthop 1981;157: [13] Bonney G, Macnab I. Hallux valgus and hallux rigidus. A critical survey of operative results. JBJS 1952;34B(3): [14] Bingold AC. Arthrodesis of the great toe. Proc R Soc Med 1958;51:435 7.
11 J.F. Baumhauer, B.F. DiGiovanni / Foot Ankle Clin N Am 8 (2003) [15] Hutton WC, Dhanendran M. The mechanics of normal and hallux valgus feet a quantitative study. Clin Orthop 1981;157:7 13. [16] Mann RA, Oates JC. Arthrodesis of the first metatarsophalangeal joint. Foot Ankle 1980;1: [17] Thompson FR, McElvenny RT. Arthrodesis of the first metatarsophalangeal joint. JBJS 1940; 22A: [18] VonSalis-Soglio GV, Thomas W. Arthrodesis of the metatarsophalangeal joint of the great toe. Arch Orthop Traumat Surg 1979;95:7 12. [19] Wilkinson J. Cone arthrodesis of the first metatarsophalangeal joint. Acta Orthop Scand 1978; 49: [20] Wilson JN. Cone arthrodesis of the first metatarso-phalangeal joint. JBJS 1967;49B(1): [21] Cracchiolo III A, Swanton A, Swanson GD. The arthritic great toe metatarsophalangeal joint: a review of flexible silicone implant arthroplasty from two medical centers. Clin Orthop 1981; 157:64 9. [22] Gordon M, Bullough PG. Synovial and osseous inflammation in failed silicone-rubber prostheses. A report of six cases. JBJS 1982;64A: [23] Gould N. Hallux rigidus: cheilotomy or implant? Foot Ankle 1981;1: [24] Granberry WM, Noble PC, Bishop JO, et al. Use of a hinged silicone prosthesis for replacement arthroplasty of the first metatarsophalangeal joint. JBJS 1991;73A: [25] Johnson KA, Buck PG. Total replacement arthroplasty of the first metatarsophalangeal joint. Foot Ankle 1981;1: [26] Molster AO, Lunde OD, Rait M. Hallux rigidus treated with the Swanson silastic hemi-joint prosthesis. Acta Scandinavica 1980;51: [27] Ris H-B, Mettler M, Engeloch F. Langzeitergebnisse mit der silastik-endoprothese nach Swanson am grosszehengrun diskrepanz zwischen klinik und radiologischem befund. (Long-term results using a Swanson silastic endoprosthesis of the metatarsophanlangeal joint of the great toe. Discrepancy between clinical and radiologic findings.) Zeitschr Orthop (Z Orthop Ihre Grenzgeb) 1988;126: [28] Sethu A, D Netto DC, Ramakrishna B. Swanson s silastic implants in great toes. JBJS 1980; 62B(1): [29] Shanker NS, Asaad SS, Craxford AD. Hinged silastic implants of the great toe. Clin Orthop 1991;272: [30] Swanson AB. Implant arthroplasty for the great toe. Clin Orthop 1972;85: [31] Swanson B, Lumsden RM, Swanson GD. Silicone implant arthroplasty of the great toe. A review of single stem and hinge implants. Clin Orthop 1979;142: [32] Vlatis G, Anderson EG. Swanson silastic spacer in hallux rigidus and valgus. JBJS 1987; 69B(4):678. [33] Wenger RJJ, Whalley RC. Total replacement of the first metatarsophalangeal joint. JBJS 1978; [34] Laird L. Silastic joint arthroplasty of the great toe. A review of 228 implants using the doublestemmed implant. Clin Orthop 1990;225: [35] Shereff MJ, Jahss MH. Complications of silastic implant arthroplasty in the hallux. Foot Ankle 1980;1(2): [36] Verhaar J, Bulstra S, Wallenkamp G. Silicone arthroplasty for hallux rigidus. Implant wear and osteolysis. Acta Orthop Scand 1989;60(1):30 3. [37] Verhaar J, Vermeulen A, Bulstra S, et al. Bone reaction to silicone metatarsophalangeal joint-1 hemiprosthesis. CORR 1989;245: [38] Duckworth T, Betts RP, Franks CI, et al. The measurement of pressures under the foot. Foot Ankle 1982;3: [39] Stokes IAF, Hutton WC, Stott JRR, et al. Forces under the hallux valgus foot before and after surgery. Clin Ortho 1979;142: [40] Shereff MJ, Baumhauer JF. Hallux rigidus and osteoarthrosis of the first metatarsophalangeal joint. JBJS 1998;80A(6):
12 48 J.F. Baumhauer, B.F. DiGiovanni / Foot Ankle Clin N Am 8 (2003) [41] Swanson AB. Implant arthroplasty in disabilities of the great toe. In: Instructional course lectures. The American Academy of Orthopaedic Surgeons, vol 21. St. Louis: CV Mosby; p [42] Kitaoka HB. Salvage of failed first metatarsophalangeal joint implant arthroplasty by implant removal and synovectomy: clinical and biomechanical evaluation. Foot Ankle 1992;13(5): [43] Hecht PJ, Gibbons MJ, Wapner KL, et al. Arthrodesis of the first metatarsophalangeal joint to salvage failed silicone implant arthroplasty. Foot Ankle Int 1997;18(7):
NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study
 Scandinavian Journal of Surgery 91: 202 207, 2002 NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study P. Ess, M.
Scandinavian Journal of Surgery 91: 202 207, 2002 NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study P. Ess, M.
HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT
 C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
Investigation performed at Orthopaedic Hospital Gersthof, Vienna, Austria
 1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
First metatarsophalangeal hemiarthroplasty for hallux rigidus
 DOI 10.1007/s00264-010-1012-x ORIGINAL PAPER First metatarsophalangeal hemiarthroplasty for hallux rigidus Eric Giza & Martin Sullivan & Dan Ocel & Gregory Lundeen & Matt Mitchell & Lauren Frizzell Received:
DOI 10.1007/s00264-010-1012-x ORIGINAL PAPER First metatarsophalangeal hemiarthroplasty for hallux rigidus Eric Giza & Martin Sullivan & Dan Ocel & Gregory Lundeen & Matt Mitchell & Lauren Frizzell Received:
Hallux Rigidus & Silastic Total Implants
 Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
19 Arthrodesis of the First Metatarsocuneiform Joint
 19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
Great Toe Joint Replacement Patient Guide
 Great Toe Joint Replacement Patient Guide The BioPro First MPJ Hemi Implant The proven long-term joint fusion alternative. Long-term use Clinically proven High implant survivorship Long-term implant survivorship
Great Toe Joint Replacement Patient Guide The BioPro First MPJ Hemi Implant The proven long-term joint fusion alternative. Long-term use Clinically proven High implant survivorship Long-term implant survivorship
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
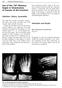 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Lesser MPJ Hemi Implant
 Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months.
 Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
18 Arthrodeses of the First Metatarsophalangeal Joint
 18 Arthrodeses of the First Metatarsophalangeal Joint DOMENICK A. CALISE PRAYA MAM VINCENT J. HETHERINGTON A versatile procedure in the armamentarium of the foot surgeon is arthrodesis of the first metatarsophalangeal
18 Arthrodeses of the First Metatarsophalangeal Joint DOMENICK A. CALISE PRAYA MAM VINCENT J. HETHERINGTON A versatile procedure in the armamentarium of the foot surgeon is arthrodesis of the first metatarsophalangeal
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint
 Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Investigation performed at the Department of Orthopaedic and Trauma Surgery, Glasgow Royal Infirmary, Glasgow, United Kingdom
 748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
Foot and ankle update
 Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
1. Orthoapedic Associates of Michigan, PC, Grand Rapids, MI 2. Michigan State University College of Human Medicine, Grand Rapids, MI
 Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
QUICK REFERENCE GUIDE. MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING
 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY
 C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital review
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito
 Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Merete BLP. Surgical Technique. - Bunion Locking Plate - Low Profile Locking Bone Plate System
 Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Distraction Osteogenesis and Fusion for Failed First Metatarsophalangeal Joint Replacement: Case Series
 737481FAIXXX10.1177/1071100717737481Foot & Ankle InternationalDa Cunha et al research-article2017 Case Report Distraction Osteogenesis and Fusion for Failed First Metatarsophalangeal Joint Replacement:
737481FAIXXX10.1177/1071100717737481Foot & Ankle InternationalDa Cunha et al research-article2017 Case Report Distraction Osteogenesis and Fusion for Failed First Metatarsophalangeal Joint Replacement:
ORIGINAL ARTICLE. Keywords Hallux Rigidus; Metatarsophalangeal Joint; Arthroplasty
 ORIGINAL ARTICLE Preliminary Results from the METIS-Newdeal total metatarsophalangeal prosthesis Luís Fernando Nunes Pires Silva 1, Cristina Varino Sousa 1, Ricardo Rodrigues Pinto 2, Claudia Santos 2,
ORIGINAL ARTICLE Preliminary Results from the METIS-Newdeal total metatarsophalangeal prosthesis Luís Fernando Nunes Pires Silva 1, Cristina Varino Sousa 1, Ricardo Rodrigues Pinto 2, Claudia Santos 2,
INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement
 016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
How to avoid complications of distraction osteogenesis for first brachymetatarsia
 220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
Joint Preserving Surgery in Severe Forefoot Disorders
 Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT. Miss Sue Kendall PhD FRCS (Orth&Trauma)
 THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy
 CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
SURGICAL TECHNIQUE CHI. Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY
 CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
Comparison of Hallux Rigidus Surgical Treatment Outcomes Between Active Duty and Non Active Duty Populations
 ORIGINAL ARTICLES Comparison of Hallux Rigidus Surgical Treatment Outcomes Between Active Duty and Non Active Duty Populations A Retrospective Review Marc D. Jones, DPM* Kerry J. Sweet, DPM Background:
ORIGINAL ARTICLES Comparison of Hallux Rigidus Surgical Treatment Outcomes Between Active Duty and Non Active Duty Populations A Retrospective Review Marc D. Jones, DPM* Kerry J. Sweet, DPM Background:
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant
 Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
PATIENT INFORMATION THE DIFFERENCE IS MOVING.
 PATIENT INFORMATION THE DIFFERENCE IS MOVING. THIS BROCHURE IS WRITTEN TO HELP YOU MAKE AN INFORMED DECISION ABOUT YOUR SURGERY. Please read this entire brochure carefully. Keep this brochure. You may
PATIENT INFORMATION THE DIFFERENCE IS MOVING. THIS BROCHURE IS WRITTEN TO HELP YOU MAKE AN INFORMED DECISION ABOUT YOUR SURGERY. Please read this entire brochure carefully. Keep this brochure. You may
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING.
 LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES
 PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus. Anand Vora, MD
 Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
First Metatarsophalangeal Arthrodesis: A Clinical, Pedobarographic and Gait Analysis Study
 FOOT & ANKLE INTERNATIONAL Copyright @ 2002 by the American Orthopaedic Foot & Ankle Society, Inc First Metatarsophalangeal Arthrodesis: A Clinical, Pedobarographic and Gait Analysis Study Paul Francis
FOOT & ANKLE INTERNATIONAL Copyright @ 2002 by the American Orthopaedic Foot & Ankle Society, Inc First Metatarsophalangeal Arthrodesis: A Clinical, Pedobarographic and Gait Analysis Study Paul Francis
A perspective on MPJ implant arthroplasty.
 A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE
 C H A P T E R 5 PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE Raymond G. Cavaliere, DPM INTRODUCTION Hammertoes can be classified as simple, moderate, and severe. The deformities
C H A P T E R 5 PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE Raymond G. Cavaliere, DPM INTRODUCTION Hammertoes can be classified as simple, moderate, and severe. The deformities
PEDUS-L. Locking Plantar Lapidus Plate
 PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
WHAT DO HALLUX VALGUS AND BUNION MEAN?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy
 Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
MULTIPLE APPLICATIONS OF THE MINIRAIL
 C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
1 st MP Arthrodesis. - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA
 1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
Are you living with toe pain?
 Are you living with toe pain? Unlike a toe fusion, the Arthrosurface Joint Restoration Systems can allow you to resume full activity and preserves the natural anatomy of your joint. Find out if the Arthrosurface
Are you living with toe pain? Unlike a toe fusion, the Arthrosurface Joint Restoration Systems can allow you to resume full activity and preserves the natural anatomy of your joint. Find out if the Arthrosurface
The Weil osteotomy. Lower limb A SEVEN-YEAR FOLLOW-UP. S. G. Hofstaetter, J. G. Hofstaetter, J. A. Petroutsas, F. Gruber, P. Ritschl, H.-J.
 Lower limb The Weil osteotomy A SEVEN-YEAR FOLLOW-UP S. G. Hofstaetter, J. G. Hofstaetter, J. A. Petroutsas, F. Gruber, P. Ritschl, H.-J. Trnka From Hospital Gersthof, Vienna, Austria We prospectively
Lower limb The Weil osteotomy A SEVEN-YEAR FOLLOW-UP S. G. Hofstaetter, J. G. Hofstaetter, J. A. Petroutsas, F. Gruber, P. Ritschl, H.-J. Trnka From Hospital Gersthof, Vienna, Austria We prospectively
Lesser toe deformities
 PATIENT INFORMATION Lesser toe deformities What are lesser toe deformities? Lesser toe deformities are caused by changes in normal anatomy that create an imbalance between the foot s muscle groups (intrinsic
PATIENT INFORMATION Lesser toe deformities What are lesser toe deformities? Lesser toe deformities are caused by changes in normal anatomy that create an imbalance between the foot s muscle groups (intrinsic
Bunions. A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus.
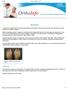 Bunions A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus. Bunions develop slowly. Pressure on the big toe joint
Bunions A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus. Bunions develop slowly. Pressure on the big toe joint
Fracture and Dislocation of Metacarpal Bones, Metacarpophalangeal Joints, Phalanges, and Interphalangeal Joints ( 1-Jan-1985 )
 In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES
 FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
First MPJ Hemi Implant
 First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
Moderate to severe hallux valgus deformity: correction with proximal crescentic osteotomy and distal soft-tissue release
 Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
The Ludloff Osteotomy
 Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Preservation of the First Ray in Patients with Diabetes
 Preservation of the First Ray in Patients with Diabetes Surgical approaches are often necessary to off-load excessive pressure. By Derek Ley, DPM, and Barry Rosenblum, DPM Introduction In approaching diabetic
Preservation of the First Ray in Patients with Diabetes Surgical approaches are often necessary to off-load excessive pressure. By Derek Ley, DPM, and Barry Rosenblum, DPM Introduction In approaching diabetic
NORTHERN OHIO FOUNDATION
 NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
Arthritis of the Foot and Ankle
 Arthritis of the Foot and Ankle Arthritis is inflammation of one or more of your joints. It can cause pain and stiffness in any joint in the body, and is common in the small joints of the foot and ankle.
Arthritis of the Foot and Ankle Arthritis is inflammation of one or more of your joints. It can cause pain and stiffness in any joint in the body, and is common in the small joints of the foot and ankle.
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
BUCKS MSK: FOOT AND ANKLE PATHWAY GP MANAGEMENT. Hallux Valgus. Assessment: Early Management. (must be attempted prior to any referral to imsk):
 Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Common Foot and Ankle Conditions: How Can You Find Relief?
 Common Foot and Ankle Conditions: How Can You Find Relief? Your Feet and Ankles are Workhorses They bear a lot of weight They perform various movements Common Conditions That Cause Foot/Ankle Pain Plantar
Common Foot and Ankle Conditions: How Can You Find Relief? Your Feet and Ankles are Workhorses They bear a lot of weight They perform various movements Common Conditions That Cause Foot/Ankle Pain Plantar
Osteotomy vs No Osteotomy Second Ray
 Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
pedcat Clinical Case Studies
 pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
Disclosures. 55 year old Male 2/23/2018. Recurrent Hallux Rigidus: Options Other than Arthrodesis
 Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
Modified Proximal Scarf Osteotomy for Hallux Valgus
 Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
SpeedTip CCS 2.2, 3.0
 PRODUCT INFORMATION SpeedTip CCS 2.2, 3.0 Cannulated Compression Screws APTUS 2 SpeedTip CCS 2.2, 3.0 Cannulated Compression Screws SpeedTip CCS * 2.2, 3.0 Cannulated Compression Screws A new generation
PRODUCT INFORMATION SpeedTip CCS 2.2, 3.0 Cannulated Compression Screws APTUS 2 SpeedTip CCS 2.2, 3.0 Cannulated Compression Screws SpeedTip CCS * 2.2, 3.0 Cannulated Compression Screws A new generation
A Patient s Guide to Claw Toes and Hammertoes
 A Patient s Guide to Claw Toes and Hammertoes 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
A Patient s Guide to Claw Toes and Hammertoes 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
Bunionectomy-Forefoot Surgery
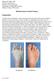 Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Bunionectomy-Forefoot Surgery A bunion (also called hallux
Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Bunionectomy-Forefoot Surgery A bunion (also called hallux
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Correction of Hallux Valgus Metatarsal Osteotomy Versus Excision Arthroplasty
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 376, pp. 183-194 0 2000 Lippincott Williams & Wilkins, Inc. Correction of Hallux Valgus Metatarsal Osteotomy Versus Excision Arthroplasty Alexander Zembsch,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 376, pp. 183-194 0 2000 Lippincott Williams & Wilkins, Inc. Correction of Hallux Valgus Metatarsal Osteotomy Versus Excision Arthroplasty Alexander Zembsch,
RECURRENT INTERMETATARSAL NEUROMA
 4 th Foot & Ankle Symposium RECURRENT INTERMETATARSAL NEUROMA Martin Berli, MD Department of Prosthetics and Orthotics Uniklinik Balgrist, Zurich martin.berli@balgrist.ch Recurrence: General Topics Pain
4 th Foot & Ankle Symposium RECURRENT INTERMETATARSAL NEUROMA Martin Berli, MD Department of Prosthetics and Orthotics Uniklinik Balgrist, Zurich martin.berli@balgrist.ch Recurrence: General Topics Pain
ToeMobile. Surgical Technique. Great Toe Endoprosthesis
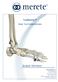 Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
A Patient s Guide to Bunions. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
Financial Disclosure. Turf Toe
 Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Seth O Brien, CP, LP Financial Disclosure Mr. Seth O'Brien has no relevant financial relationships with commercial interests to disclose. Turf Toe Common in athletes playing on firm, artificial turf Forceful
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot.
 Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Integra. Silicone Toe System SURGICAL TECHNIQUE
 Silicone Toe System SURGICAL TECHNIQUE Silicone Toe System Table of Contents Indications...2 Contraindications...2 Warnings...2 Precautions...2 Adverse Events...2 Flexible Great Toe (FGT)...3 Surgical
Silicone Toe System SURGICAL TECHNIQUE Silicone Toe System Table of Contents Indications...2 Contraindications...2 Warnings...2 Precautions...2 Adverse Events...2 Flexible Great Toe (FGT)...3 Surgical
Bunion Surgery. This article provides information on surgery for bunions. For more general information: Bunions (topic.cfm? topic=a00155).
 Bunion Surgery This article provides information on surgery for bunions. For more general information: Bunions (topic.cfm? topic=a00155). Most people with bunions find pain relief with simple treatments
Bunion Surgery This article provides information on surgery for bunions. For more general information: Bunions (topic.cfm? topic=a00155). Most people with bunions find pain relief with simple treatments
A Patient s Guide to Claw Toes and Hammertoes
 A Patient s Guide to Claw Toes and Hammertoes Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information
A Patient s Guide to Claw Toes and Hammertoes Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study
 Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Lesser Toe Correction
 Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Lesser Toe Correction Lesser toe deformities are classified
Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Lesser Toe Correction Lesser toe deformities are classified
Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis
 SPECIAL FOCUS Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis Alastair S.E. Younger a, Judith F. Baumhauer b and Mark Glazebrook c ABSTRACT End stage arthritis
SPECIAL FOCUS Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis Alastair S.E. Younger a, Judith F. Baumhauer b and Mark Glazebrook c ABSTRACT End stage arthritis
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair
 Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
ORTHOLOC 3Di. Foot Reconstruction System SURGIC AL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
Index. Clin Podiatr Med Surg 22 (2005) Note: Page numbers of article titles are in boldface type.
 Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
The Vilex Hemi-Implant: A Retrospective Analysis of 30 Patients in the Treatment of Hallux Rigidus
 Open Access Publication The Vilex Hemi-Implant: A Retrospective Analysis of 30 Patients in the Treatment of Hallux Rigidus by David M. Davidson, DPM 1, Kenneth T. Goldstein, DPM 2, James D. Yakel, DPM
Open Access Publication The Vilex Hemi-Implant: A Retrospective Analysis of 30 Patients in the Treatment of Hallux Rigidus by David M. Davidson, DPM 1, Kenneth T. Goldstein, DPM 2, James D. Yakel, DPM
CURRENT METHODS OF TREATMENT
 ~ CURRENT METHODS OF TREATMENT Rheumatoid Deformity of the Foot* By LEONARD MARMOR T HE PATIENT with rheumatoid arthritis often develops severe, crippling deformities of his upper and lower limbs. The
~ CURRENT METHODS OF TREATMENT Rheumatoid Deformity of the Foot* By LEONARD MARMOR T HE PATIENT with rheumatoid arthritis often develops severe, crippling deformities of his upper and lower limbs. The
Digital Surgery Complications
 Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
Surgical Care of the Lower Extremity in Rheumatoid Arthritis*
 Surgical Care of the Lower Extremity in Rheumatoid Arthritis* ROBY C. THOMPSON, JR., M. D. Professor of Orthopedic Surgery, University of Virginia School of Medicine, Charlottesville One of the most important
Surgical Care of the Lower Extremity in Rheumatoid Arthritis* ROBY C. THOMPSON, JR., M. D. Professor of Orthopedic Surgery, University of Virginia School of Medicine, Charlottesville One of the most important
