18 Arthrodeses of the First Metatarsophalangeal Joint
|
|
|
- Bethanie Carpenter
- 6 years ago
- Views:
Transcription
1 18 Arthrodeses of the First Metatarsophalangeal Joint DOMENICK A. CALISE PRAYA MAM VINCENT J. HETHERINGTON A versatile procedure in the armamentarium of the foot surgeon is arthrodesis of the first metatarsophalangeal joint. Considering the large number of indications for metatarsophalangeal joint fusion, there are relatively few contraindications. Since Glutton 1 first described fusion of the first metatarsophalangeal joint, there have been numerous modifications and alterations to the procedure. Advances in fixation technique and in biomechanics have allowed for improved methods of fusion and greater ease of performance. This chapter discusses indications and contraindications for fusion of the first metatarsophalangeal joint. Technical considerations such as surgical approach, position of fusion fixation techniques, and postoperative care are also discussed. PREOPERATIVE CONSIDERATIONS The versatility of first metatarsophalangeal joint (MPJ) fusion is evident in the number of indications that exist for this procedure (Table 18-1). The most commonly cited indications for fusion are hallux valgus and hallux rigidus Other indications include rheumatoid arthritis, salvage of failed hallux valgus surgery (including failed Keller procedures), 5,8-10,18-21 posttraumatic arthrosis, 8-11 postosteomyelitis, and sep- Table Indications Severe hallux valgus Hallux rigidus Rheumatoid arthritis Salvage of failed surgery Failed Keller procedure Postinfection arthrosis Posttraumatic arthrosis Neuromuscular disease tic arthrosis 10 (Fig. 18-1). Stroh and Yee presented the use of first MPJ fusion in cases in which both hallucal sesamoids were fractured and there was a failure of conservative care. 22 First MPJ fusion is the procedure of choice in cerebral palsy patients and others with a hallux valgus deformity from neuromuscular disor- 8, ders. There are relatively few contraindications to MPJ fusion (Table 18-2). The most commonly cited contraindication is preexisting arthrosis of the interphalangeal joint of the hallux. 5-7,11 One must take special precautions preoperatively to inform the patient that there will be no motion present at the great toe and that changes in footwear will be necessary. Because osteoporotic bone may cause difficulty with placement of fixation devices, alternative procedures may be of more benefit to the patient. 267
2 268 HALLUX VALGUS AND FOREFOOT SURGERY A Fig Preoperative and postoperative radiographs demonstrating various indications for first MPJ fusion. (A & B) Severe hallux valgus. Fig. A: preoperative radiograph; Fig. B: radiograph taken years postoperatively. (Figure continues.} Preoperative evaluation should include a careful radiographic review including anteroposterior (AP), lateral, and oblique views to ensure competence of the hallucal interphalangeal joint. It may be of benefit to construct templates of the planned resection to obtain precise joint resections and optimal alignment. Ginsburg suggests obtaining a lateral radiograph of the foot with the patient wearing a shoe normally used so that the optimal sagittal plane position of the fusion could be determined. 8 The question of intermetatarsal angle relationships in first MPJ fusion has been raised by Mann and The need for ancillary first metatarsal osteotomy has been presented by relatively few authors It has been noted that the stability of the fusion in addition to the effect of the adductor complex will help to decrease the intermetatarsal angle by approximately 4 to 6. 4,10,26,27 Mann states that the others. 4,10,26-29 Table Contraindications Interphalangeal joint arthritis Osteoporotic bone Active infection Noncompliance with shoe wear (high heels)
3 ARTHRODESES OF THE FIRST METATARSOPHALANGEAL JOINT 269 Fig (Continued). (C-F) Salvage of failed implant. Fig. C: preoperative radiograph of a painful first metatarsophalangeal joint postimplant arthroplasty; Fig. D: postoperative radiograph showing K-wire fixation; Figs. E and F: other postoperative views. (Figure continues)
4 270 HALLUX VALGUS AND FOREFOOT SURGERY Fig (Continued). (G J) Hallux rigidus. Fig. G: preoperative view; Fig. H: preoperative lateral view (note dorsal flag sign); Figs. I and J: postoperative views. change in the intermetatarsal angle is directly proportional to the preoperative intermetatarsal angle and that concomitant first metatarsal osteotomy is not indicated. 26 Once the hallux is rigidly fused to the metatarsal, the adductor hallucis tendon and lateral soft tissue structures are no longer a deforming force. In fact, the adductor tendon gains mechanical advantage in this situation, and can now function to pull both the meta- tarsal and the proximal phalanx toward the midline of the foot, which decreases the intermetatarsal angle4 (Fig. 18-2). Interspace soft tissue dissection is discouraged in this procedure because release of the adductor tendon may lead to increased metatarsal splaying postoperatively. Postoperative splaying of the first metatarsal with a fused MPJ will lead to a hallux varus (Fig. 18-3).
5 ARTHRODESES OF THE FIRST METATARSOPHALANGEAL JOINT 271 FUSION POSITION Fig Decrease in intermetatarsal angle. (A & B) Schematic diagram of role of adductor hallucis in intermetatarsal angle reduction with first MPJ fusion. Fig Diagram of hallux varus as result of extensive dissection of first intermetatarsal space. Note loss of stabilization with transection of adductor tendon. The most critical aspect of MPJ fusion is the position of fusion. This key component of the procedure has been a point of great discussion since the inception of MPJ fusion. Although there is today a general consensus of opinion regarding toe position, there have been no randomized, controlled, prospective studies comparing one fusion position to another. Further, there is a paucity of research into the optimal length pattern of the first metatarsal in MPJ fusion. Although Duckworth has supplied research using pedobarographic measurements comparing gait in arthroplasty versus arthrodesis of the first MPJ, there is no statistical comparison of various fusion positions and no mention of metatarsal length patterns These pedobarographic comparisons of first MPJ arthroplasty versus fusion have shown that fusion is more stable than arthroplasty. Perhaps one of the greatest factors concerning disagreement over fusion position is the question of reference point. Many authors supply varying degrees of valgus and toe dorsiflexion; however, no proper reference point for the particular angle has been given. When discussing the dorsiflexion angle, it is necessary to state whether this measure is taken in relationship to the ground and the hallux or to the metatarsal and the hallux. Further clouding the picture are the questions of metatarsal angulation to the ground and of heel height differences worn by men and women. For MPJ fusion, we must consider rotation of the hallux in the frontal plane, valgus angulation of the hallux in the transverse plane (more appropriately termed abduction angle), and dorsiflexion of the hallux in the sagittal plane (Table 25-3). Most authors agree that there should be no frontal plane rotation of the hallux. 2-5,9,11,18,30 Rotation of the hallux will result in undue pressure along either nail border, keratosis along a prominent medial or lateral condyle, or increased weight-bearing stress through the interphalangeal joint. Intraoperatively, the surgeon should use the nail plate as a guide to the degree of rotation present at the hallux. Positioning of the hallux in the transverse plane (valgus angulation) should be such that the hallux appears to sit in natural alignment with the lesser toes. The patient should be made aware preoperatively that the great toe will not be "straight.'' An excessively rec-
6 272 HALLUX VALGUS AND FOREFOOT SURGERY Table Fusion Position Summary Sagittal 10º-15º Dorsiflexion Transverse 15º-25º Abduction Frontal 0º Rotation tus transverse plane alignment could cause problems with shoe fit and increased stress across the interphalangeal joint. Care should be taken when determining valgus position so as to not cause impingement between the first and second toe, which could lead to painful interdigital corn formation. General consensus regarding valgus angulation of the hallux has yet to be determined; from 5 to 30 of valgus have been proposed as a suitable transverse plane angulation. 2-7,9-11,16,18,20,30 Fitzgerald, in a long-term follow-up study, noted that in cases in which the MPJ was fused in less than 20 of valgus the incidence of postoperative degenerative changes at the interphalangeal joint of the hallux was three times greater than those fused in excess of 20 of valgus. 6 Smith noted that rheumatoid patients could tolerate a greater degree of valgus because of the laterally deviated position of the lesser toes with less possibility of the first and second toes impinging on each other. Smith went onto recommend that rheumatoid patients could be fused in 25 to 30 of valgus. 18 In general, the hallux should be placed in 15 to 25 of valgus and in line with the lesser toes. The final plane that needs to be addressed is the sagittal plane or dorsiflexion angle. Various authors have proposed values from 0 to 40 of hallux dorsiflexion. 2-5,9,11,18,30,35,37 These values can be somewhat misleading in that a plane of reference is not given. In determining dorsiflexion angles of the hallux in relationship to the horizontal surface of the ground, there may be difficulty in duplicating this angle in a nonweight-bearing foot on the operating room table. The first metatarsal forms a much better point of reference for measurement of the dorsiflexion angle. To properly position the hallux in the sagittal plane, preoperative measurements on weight-bearing radiographs are of the utmost importance. The relationship of the hallux to the first metatarsal and the first metatarsal to the ground can be determined on the lateral view. According to Ginsburg, an extra measure of accuracy can be achieved by obtaining a lateral weight-bearing radiograph while the patient is wearing a shoe with the preferred heel height 8 (Fig. 18-4). The first metatarsal is usually angulated 15 to the ground (first metatarsal declination angle), which would translate to the hallux being angled 15 to the first metatarsal on stance. Most authors agree that 10 of dorsiflexion of the hallux above the horizontal plane is sufficient for pain-free ambulation. 9,18,30 If the usual first metatarsal declination angle of 15 is added Fig Preoperative lateral radiograph with patient wearing a shoe. Note first metatarsal declination angle that will be the frame of reference for determining the sagittal plane position of fusion intraoperatively,
7 ARTHRODESES OF THE FIRST METATARSOPHALANGEAL JOINT 273 Fig Determination of hallux sagittal plane positioning; 10, hallux dorsiflexion angle; 15, preoperatively measured first metatarsal declination angle; 25, angle of fusion between hallux and metatarsal. The hallux dorsiflexion angle should not exceed 15. to the recommended 10 of dorsiflexion above the horizontal, a hallux to first metatarsal dorsiflexion angle of 25 results (Fig. 18-5). This angle can easily be measured intraoperatively with a sterile goniometer (Fig. 18-6). A great toe that is fused in less than 10 of dorsiflexion above the horizontal will subject the pa- tient to pain at the distal tip of the toe and increase stress at the interphalangeal joint of the hallux. Insufficient dorsiflexion will also lead to excess callus formation at the plantar aspect of the hallucal interphalangeal joint. Dorsiflexion angles greater than 15 above the horizontal will cause excessive retrograde pres- Fig Goniometer used intraoperatively to ensure precise position of first MPJ fusion.
8 274 HALLUX VALGUS AND FOREFOOT SURGERY sure on the metatarsal head, which will lead to excessive callus formation and pain beneath the first metatarsal 2,6,10 (Fig. 18-7). In summary, the hallux should be fused 10 to 15 above the horizontal; this value should be added to the preoperatively measured metatarsal declination angle to allow for accurate positioning of the hallux on the metatarsal in the sagittal plane. To ensure exact positioning of the fusion site, Sullivan 38 has proposed the use of the Reese osteotomy guide (Reese, Peoria, AZ). This instrument allows for the precise placement of a sagittally directed chevron fusion site, which will provide for simple placement of a cancellous screw. Another system allowing exact fusion positioning intraoperatively is the truncated cone reamer device (Biomet Inc., Warsaw, IN). This instrument prepares the fusion site into a perfectly matched peg and hole and allows for proper angular adjustments. Although the system facilitates placement, it is B Fig Complication of improper sagittal plane positioning of fusion site. (A) Sub-first metatarsal tyloma. Note preulcerative appearance of lesion. (B) Lateral radiograph of same foot shows excessive dorsiflexion of hallux on first metatarsal.
9 ARTHRODESES OF THE FIRST METATARSOPHALANGEAL JOINT 275 rather cumbersome in its use, and the instrumentation involved is somewhat complex. Improper use of the truncated cone reamer can lead to severe soft tissue damage. FIXATION METHODS Many different methods of fixation for first MPJ fusion have been proposed. 2,4,7-9,18,30,39-44 McKeever 2 presented the use of screw fixation via a plantarly placed screw running from distal to proximal. Harrison and Harvey 4 proposed the use of a Charnley clamp for fixation. The fixator was left in place for 3 weeks then replaced with a walking cast that completely incorporated the hallux. The cast was left in place for an additional 3 weeks. There have been no other reports to support or refute the use of external fixation devices for first MPJ fusions. Salis-Soglio has discussed the use of the dynamic compression plate applied to the dorsum of the first MPJ for fixation of the fusion site 7. They made no comment regarding the advantages of this form of fixation. The use of K-wires and Steinman pins for fixation of MPJ fusion has been supported by many authors. 8,9,18,20,40 The advantages to pin fixation include ease of the procedure, ability to provide stability in porotic bone, and ability to manipulate the fusion site if minor angular changes are necessary. Disadvantages include the possibility of pin tract infection and lack of compression. Wilson has presented the use of the Rush pin as a method of fixating MPJ fusions. 39 The intramedullary Rush nail supplies considerable compressive force across the fusion site, a factor that Wilson states "allows for rapid arthrodesis." Various other methods of fixation have been presented including the use of Herbert screws, wire loop, suture, and combinations of wire and pins The use of cannulated screws is an excellent method of first MPJ fusion which, to our knowledge, has yet to be presented in the literature. Sykes performed an elaborate biomechanical study using cadaveric specimens to determine the stability of various fixation devices used in first MPJ fusions. 43 He compared cancellous screws used with dome arthrodesis and planar arthrodesis with planar surfaces held by Charnley clamps and various wire constructs. The use of K-wires, Stienman pins, or plate fixation was not investigated. The study concluded that the best method of fixation was the use of planar surface fusion with a 4.0 cancellous screw; the method of fusion that was second in resistance to load was screw fixation with domed fusion surfaces. The study also noted that the critical component in screw fixation was an intact plantar flange on the proximal phalanx base. Screws were placed from plantar medial distal to dorsal lateral proximal. The head of the screw must impact against the intact plantar flange to obtain sufficient compression across the fusion site. SURGICAL PROCEDURE The surgical approach to the first MPJ is relatively straightforward, consisting of either a dorsomedial or a medial incision. The incision starts at about midshaft on the first metatarsal and extends out to the distal aspect of the proximal phalanx. Dissection is kept to a minimum because there is no need for interspace procedures or sesamoid rotation. The incision is carried down to the level of the first MPJ capsule where a linear capsulotomy is performed in line with the skin incision. The extensor hallucis longus tendon is reflected laterally, and the MPJ is disarticulated. Resection of the medial eminence is performed as needed, taking care to avoid excessive bone removal. At this point one must decide on what type of fusion is to be performed; options include end-to-end flat surface fusion, peg-in-hole fusion, or simple cartilage resection. 2,3,5,7,8,11,30,31,35,36 Each option has its advantages and disadvantages, but the final aim is the same; with any method used, there should be good bone-to-bone contact with no cartilaginous or soft tissue interposition. End-to-end fusion provides excellent bone apposition for increased stability and greater surface area for fusion. However, if the position of the hallux is not satisfactory, revisional bone cuts will be necessary. Repeated bone cuts may result in excessive shortening of the metatarsal, which may ultimately result in lesser metatarsalgia. Peg-in-hole and conical fusions provide remarkable stability and allow for angular adjustments but may cause excessive shortening. Peg-in-hole and conical fusions also require greater wound manipulation, are technically more demanding, and may require the use of specialized instrumentation such as power reamers.
10 276 HALLUX VALGUS AND FOREFOOT SURGERY Simple cartilage removal allows for minimal loss of bone and provides for a high degree of angular adjustment from the ball-and-socket architecture of the first MPJ. However, this ability to easily adjust position also renders simple cartilage resection highly unstable. Another shortcoming of simple cartilage resection is that the subchondral bone is relatively dense, a factor that may delay union. To overcome this problem, it is necessary to drill multiple holes in the subchondral surface of the metatarsal head and phalangeal base. These holes will increase the surface area for fusion and allow for vascular bridging and bone formation at the site. This is easily accomplished by using a 1.5-mm drill bit. Another method of increasing surface area for ingrowth is the "fish-scale" technique. Using a small sharp osteotome, multiple small cuts are made in the subchondral surface on both sides of the joint. These cuts should penetrate only through the subchondral bone, and care should be taken not to create fractures that propagate up the shaft of either the metatarsal or proximal phalanx. When the surfaces of the metatarsal head and base of the proximal phalanx are prepared, the next step in the procedure is the mating of the two surfaces and a check of angular relationships. This step is facilitated by the use of a goiniometer or intraoperative radiographs. Once the position of fusion is deemed accept- Fig (A-B) Radiographs demonstrating nonunion of first MPJ fusion.
11 ARTHRODESES OF THE FIRST METATARSOPHALANGEAL JOINT 277 able, a method of fixation is selected. Recommended fixation techniques include screws, plates, and K- wires. On completion of fixation, intraoperative radiographs are obtained as necessary and closure is performed in the usual fashion. One should keep in mind the words of Fitzgerald: "the precise operative technique is not important provided it maintains the position obtained at operation until the arthrodesis is sound." 6 The patient is then placed in a non-weightbearing cast for approximately 6 to 8 weeks. COMPLICATIONS Complications associated with first MPJ fusion are relatively few in number. Wound complications involving dehiscence, postoperative infections, and prolonged edema present at a rate similar to any other podiatric procedure and are not a major concern. Improper positioning of the fusion is a serious complication that can be avoided by proper preoperative planning and intraoperative decision making. Fusions that have been improperly positioned present with various signs and symptoms including inability to fit into shoes, interdigital heloma, incurvated or painful nails, lesser metatarsalgia, sub-first metatarsal pain, and tyloma formation. One of the more significant complications associated with malpositioning of the fusion is plantar ulceration at the first metatarsal head. This is particularly true in cases in which a fusion has been performed for a rheumatoid first MPJ. Thin plantar skin with the loss of the plantar fat pad in rheumatoid patients puts these patients at risk for developing plantar ulceration with an error in sagittal plane positioning of the fusion. Another possible complication of MPJ fusion is that of nonunion (Fig. 18-8). Nonunion rates have been noted to range from 2 to 23 percent with an average of 10 percent. 4,5,9-11,16,18,30,45 In most cases, the non-union develops into a painless pseudoarthrosis and no further intervention is needed. Possible causes for nonunion include hardware failure, improper or no fixation, and steroid or methotrexate use in rheumatoid patients. Patients occasionally will have problems with painful internal fixation devices, most often noted in plantarly placed screws. A final complication to consider is that of interphalangeal joint arthrosis. This complication can be avoided by ensuring proper transverse and sagittal plane positioning intraoperatively, thereby relieving abduction and dorsiflexion forces on the interphalangeal joint. REFERENCES 1. Glutton HH: The treatment of hallux valgus. St. Thomas Rep 22:1, McKeever D: Arthrodesis of the first metatarsophalangeal joint for hallux rigidus and metatarsus primus varus. J Bone Joint Surg 34:129, Marin G: Arthrodesis of the first metatarsophalangeal joint for hallux valgus and hallux rigidus. Guy's Hosp Rep 109:174, Harrison MHM, Harvey FJ: Arthrodesis of the first metatarsophalangeal joint for hallux valgus and rigidus. J Bone J Surg, 45A:471, Marin G: Arthrodesis of the first metatarsophalangeal joint for hallux valgus and hallux rigidus: a new method. Int Surg 50:175, Fitzgerald JAW: A review of long term results of arthrodesis of the first metatarsophalangeal joint. J Bone Joint Surg 51B:488, Salis-Soglio G, Thomas W: Arthrodesis of the metatarsophalangeal joint of the great toe. Arch Orthop Trauma Surg 95:7, Ginsburg AI: Arthrodesis of the first metatarsophalangeal joint. J Am Podiatry Assoc 69:367, Mann RA, Gates JC: Arthrodesis of the first metatarsophalangeal joint. Foot Ankle 1:159, Riggs SA, Johnson EW: McKeever arthrodesis for the painful hallux. Foot Ankle 3:248, Johansson JE, Barrington TW: Cone arthrodesis of the first metatarsophalangeal joint. Foot Ankle 4:244, Leavitt DC: Surgical treatment of arthritic feet. Northwest Med 55:1086, Du Vreis HL: Surgery of the foot. 2nd Ed. CV Mosby, St. Louis, Morrison P: Complications of forefoot operations in rheumatoid arthritis. Proc R Soc Med 67:110, Watson MS: A long term follow-up of forefoot arthroplasty. J Bone Joint Surg 56B:527, Mann RA, Thompson FM: Arthrodesis of the first metatarsophalangeal joint for hallux valgus in rheumatoid arthritis. J Bone Joint Surg 66A:687, Geppert MJ, Sobel M, Bohne WO: Foot fellows review: the rheumatoid foot; part I, forefoot. Foot Ankle 13:550, 1992
12 278 HALLUX VALGUS AND FOREFOOT SURGERY 18. Smith RW, Joanis TL, Maxwell PD: Great toe metatarsophalangeal joint arthrodesis: a user friendly technique. Foot Ankle 13:367, Henry APJ, Waugh W: The use of footprints in assessing the results of operations for hallux valgus. A comparison of Keller's operation and arthrodesis. J Bone J Surg 57(B):478, Coughlin MJ, Mann RA: Arthrodesis of the first metatarsophalangeal joint as a salvage for the failed Keller procedure. J Bone Joint Surg 69(A):68, Thompson FM: Complications of hallux valgus surgery and salvage. Orthopedics 13:1059, Stroh KI, Altman MI, Yee DY: First metatarsophalangeal joint arthrodesis: treatment for sesamoid fractures. J Am Podiatr Med Assoc 80:595, Thompson FR, McElvenny RT: Arthrodesis of the first metatarsophalangeal joint. J Bone Joint Surg 23:555, Renshaw T, Sirkin R, Drennan J: The management of hallux valgus in cerebral palsy. Dev Med Child Neurol 21:202, Richardson GE: The foot in adolescents and adults: hallux valgus in cerebral palsy, p In Crenshaw All (ed): Campbell's Operative Orthopedics, 7th Ed. CV Mosby, St. Louis, Mann RA, Katcherian DA: Relationship of metatarsophalangeal joint fusion on the intermetatarsal angle. Foot Ankle 10:8, Humbert JL, Bourbonniere C, Laurin CA: Metatarsophalangeal fusion for hallux valgus: indications and effects on the first metatarsal ray. Can Med Assoc J 120:937, Kampner SL. Total joint prosthetic arthroplasty of the great toe a 12-year experience. Foot Ankle 4: Raymakers R, Waugh W: The treatment of metatarsalgia with hallux valgus. J Bone Joint Surg 53(B):684, Coughlin MJ: Arthodesis of the first metatarsophalangeal joint with mini fragment plate fixation. Orthopedics 13:1037, Gould N: Surgery of the forepart of the foot in rheumatoid arthritis. Foot Ankle 3:173, Duckworth T, Betts RP, Franks CI: Foot pressure studies: normal and pathological gait analysis, p In Jahss MH (ed): Disorders of the Foot and Ankle. 2nd Ed. WB Saunders, Philadelphia, Duckworth T, Betts RP, Franks CI, Burke J: The measurement of pressures under the foot. Foot Ankle 3:130, Betts RP, Stockley I, Getty CJM: Foot pressure studies in the assessment of forefoot arthroplasty in the rheumatoid foot. Foot Ankle 8:315, Kelekian H: Hallux valgus, allied deformities of the forefoot and metatarsalgia. pp WB Saunders, Philadelphia, Zadik FR: Arthrodesis of the great toe. Br Med J 2:1573, Lipscomb PR: Arthrodesis of the first metatarsophalangeal joint for severe bunions and hallux rigidus. Clin Orthop Relat Res 142:48, Sullivan BT: Use of the Reese osteotomy guide system for fusion of the first metatarsophalangeal joint. J Bone Joint Surg 30:43, Wilson CL: A method of fusion of the metatarsophalangeal joint of the great toe. J Bone Joint Surg 40(A):384, Wilson JN: Cone arthrodesis of the first metatarsophalangeal joint. J Bone Joint Surg 49(B):98, l. Ghana GS, Andrew TA, Cotterill CP: A simple method of arthrodesis of the first metatarsophalangeal joint. J Bone Joint Surg 66(B):703, Phillips JE, Hooper G: A simple technique for arthrodesis of the first metatarsophalangeal joint. J Bone Joint Surg 62(B):774, Sykes A, Hughes AW: A biomechanical study using cadaveric toes to test the stability of fixation techniques employed in arthrodesis of the first metatarsophalangeal joint. Foot Ankle 7:18, Wu KK: Arthrodesis of the metatarsophalangeal joint of the great toe with Herbert screws: a clinical analysis of 27 cases. J Foot Ankle Surg 32:47, Moynihan FJ: Arthrodesis of the metatarsophalangeal joint of the great toe. J Bone Joint Surg 49B:544, 1967
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
19 Arthrodesis of the First Metatarsocuneiform Joint
 19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities
 Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS
 C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT
 C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
Lesser MPJ Hemi Implant
 Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
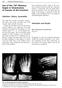 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
HemiEDGE. Patent No. 8,845,750. Surgical Technique
 HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy
 CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
Merete BLP. Surgical Technique. - Bunion Locking Plate - Low Profile Locking Bone Plate System
 Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy
 Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
CORRECTING HAMMERTOE DEFORMITIES UTILIZING AN INTRAMEDULLARY DEVICE: Case Reports
 C H A P T E R 1 1 CORRECTING HAMMERTOE DEFORMITIES UTILIZING AN INTRAMEDULLARY DEVICE: Case Reports B. Cory Brown, DPM Robert K. Cohen, DPM Jason R. Miller, DPM Scott R. Roman, DPM INTRODUCTION The most
C H A P T E R 1 1 CORRECTING HAMMERTOE DEFORMITIES UTILIZING AN INTRAMEDULLARY DEVICE: Case Reports B. Cory Brown, DPM Robert K. Cohen, DPM Jason R. Miller, DPM Scott R. Roman, DPM INTRODUCTION The most
Introduction Basics MIS Screw 2 System Characteristics 2 Indication 2
 Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
DARCO. Bow 2 Plate SURGIC AL TECHNIQUE
 DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
First MPJ Hemi Implant
 First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY
 C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
SURGICAL TECHNIQUE GUIDE
 DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
Index. Clin Podiatr Med Surg 22 (2005) Note: Page numbers of article titles are in boldface type.
 Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
The Ludloff Osteotomy
 Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Investigation performed at Orthopaedic Hospital Gersthof, Vienna, Austria
 1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES
 PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
1. Orthoapedic Associates of Michigan, PC, Grand Rapids, MI 2. Michigan State University College of Human Medicine, Grand Rapids, MI
 Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Modified Proximal Scarf Osteotomy for Hallux Valgus
 Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
CANNULINK. Intraossous Fixation System SURGICAL TECHNIQUE
 CANNULINK Intraossous Fixation System SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction The CANNULINK Advantage Indications for Use Preoperative Planning Chapter 2 5 Surgical Technique CANNULINK Standard
CANNULINK Intraossous Fixation System SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction The CANNULINK Advantage Indications for Use Preoperative Planning Chapter 2 5 Surgical Technique CANNULINK Standard
ToeMobile. Surgical Technique. Great Toe Endoprosthesis
 Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
QUICK REFERENCE GUIDE. MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING
 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital review
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
LAPIDUS What is Old is New
 LAPIDUS What is Old is New Alan Jay Block, DPM, MS, FASPS, FACFAS Fellowship trained in Advanced Ankle Techniques Adjunct Professor Dept Of Orthopeadics The Ohio State University Board Member The Ohio
LAPIDUS What is Old is New Alan Jay Block, DPM, MS, FASPS, FACFAS Fellowship trained in Advanced Ankle Techniques Adjunct Professor Dept Of Orthopeadics The Ohio State University Board Member The Ohio
Foot Reconstruction System SURGICAL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System SURGICAL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: Robert B. Anderson, MD OrthoCarolina Charlotte,
ORTHOLOC 3Di Foot Reconstruction System SURGICAL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: Robert B. Anderson, MD OrthoCarolina Charlotte,
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
1 st MP Arthrodesis. - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA
 1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY
 60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
JUVENILE AND ADOLESCENT HALLUX VALGUS. George E. Quill, Jr., M.D.
 JUVENILE AND ADOLESCENT HALLUX VALGUS George E. Quill, Jr., M.D. The development of a hallux valgus deformity in children and adolescents is actually an uncommon entity. Most of these occurrences can be
JUVENILE AND ADOLESCENT HALLUX VALGUS George E. Quill, Jr., M.D. The development of a hallux valgus deformity in children and adolescents is actually an uncommon entity. Most of these occurrences can be
Contents. Chapter 1 4 Chapter Chapter Chapter Chapter 5 15
 Contents Chapter 1 4 Chapter 2 5 5 Chapter 3 6 6 7 Chapter 4 8 8 8 8 9 10 10 11 12 13 14 14 Chapter 5 15 Introduction Intended Use Indications Device Description Implant Options and Sizing Instrumentation
Contents Chapter 1 4 Chapter 2 5 5 Chapter 3 6 6 7 Chapter 4 8 8 8 8 9 10 10 11 12 13 14 14 Chapter 5 15 Introduction Intended Use Indications Device Description Implant Options and Sizing Instrumentation
MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito
 Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Hallux Malleus develops after Flexible Hallux Varus correction with Tensioned Suture Device: A Case Report
 The Foot and nkle Online Journal Official publication of the International Foot & nkle Foundation Hallux Malleus develops after Flexible Hallux Varus correction with Tensioned Suture Device: Case Report
The Foot and nkle Online Journal Official publication of the International Foot & nkle Foundation Hallux Malleus develops after Flexible Hallux Varus correction with Tensioned Suture Device: Case Report
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot.
 Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Forefoot/Midfoot Plating System. Surgical Technique
 Forefoot/Midfoot Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Forefoot/Midfoot Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review
 Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
Chevron Osteotomy With Lateral Soft Tissue Release
 5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
ORTHOLOC 3Di. Foot Reconstruction System SURGIC AL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
Investigation performed at the Department of Orthopaedic and Trauma Surgery, Glasgow Royal Infirmary, Glasgow, United Kingdom
 748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
Locking Forefoot/Midfoot Plating System
 Locking Forefoot/Midfoot Plating System Locking Forefoot/Midfoot Plating System Acumed is an industry leader in innovative solutions for extremities and trauma. We are dedicated to pioneering solutions
Locking Forefoot/Midfoot Plating System Locking Forefoot/Midfoot Plating System Acumed is an industry leader in innovative solutions for extremities and trauma. We are dedicated to pioneering solutions
A pictorial review of reconstructive foot and ankle surgery: elective lesser forefoot procedures
 A pictorial review of reconstructive foot and ankle surgery: elective lesser forefoot procedures Andrew J Meyr 1*, Laura Sansosti 1, Sayed Ali 2 1. Department of Podiatric Surgery, Temple University School
A pictorial review of reconstructive foot and ankle surgery: elective lesser forefoot procedures Andrew J Meyr 1*, Laura Sansosti 1, Sayed Ali 2 1. Department of Podiatric Surgery, Temple University School
COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION
 C H A P T E R 3 0 COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION Scott R. Roman, DPM INTRODUCTION The most common fixation for proximal interphalangeal fusion
C H A P T E R 3 0 COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION Scott R. Roman, DPM INTRODUCTION The most common fixation for proximal interphalangeal fusion
MICA. Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE
 MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
PEDUS-L. Locking Plantar Lapidus Plate
 PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
DARCO. LPS Plate SURGICAL TECHNIQUE
 DARCO LPS Plate SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 5 5 6 7 9 Appendix 10 10 11 Design Rationale Preoperative Planning Surgical Technique Surgical Approach Joint Preparation Surgical
DARCO LPS Plate SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 5 5 6 7 9 Appendix 10 10 11 Design Rationale Preoperative Planning Surgical Technique Surgical Approach Joint Preparation Surgical
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
MULTIPLE APPLICATIONS OF THE MINIRAIL
 C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT
 C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
Foot & Ankle. Smart Toe II. Intramedullary Implant. Operative Technique. Foot & Ankle
 Foot & Ankle Smart Toe II Intramedullary Implant Operative Technique Foot & Ankle Smart Toe This publication sets forth detailed recommended procedures for using Stryker Osteosynthesis devices and instruments.
Foot & Ankle Smart Toe II Intramedullary Implant Operative Technique Foot & Ankle Smart Toe This publication sets forth detailed recommended procedures for using Stryker Osteosynthesis devices and instruments.
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD
 Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
Surgical technique. Angular Stable X-Plate and 2-Hole Plate. For osteotomies, arthrodeses and fractures of the foot.
 Surgical technique Angular Stable X-Plate and 2-Hole Plate. For osteotomies, arthrodeses and fractures of the foot. Table of Contents Indications 4 Implants 5 X-plate: Crescentic osteotomy 6 X-plate:
Surgical technique Angular Stable X-Plate and 2-Hole Plate. For osteotomies, arthrodeses and fractures of the foot. Table of Contents Indications 4 Implants 5 X-plate: Crescentic osteotomy 6 X-plate:
Hallux Valgus Deformity OPERATIVE TECHNIQUE
 Hallux Valgus Deformity OPERATIVE TECHNIQUE Table of Contents 1 ORDERING INFORMATION 3 OPERATIVE TECHNIQUE 9 INDICATIONS FOR USE The surgical technique shown is for illustrative purposes only. The technique(s)
Hallux Valgus Deformity OPERATIVE TECHNIQUE Table of Contents 1 ORDERING INFORMATION 3 OPERATIVE TECHNIQUE 9 INDICATIONS FOR USE The surgical technique shown is for illustrative purposes only. The technique(s)
InCoreTM Lapidus System
 InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
Salvage of first metatarsophalangeal joint arthroplasty complications
 Foot Ankle Clin N Am 8 (2003) 37 48 Salvage of first metatarsophalangeal joint arthroplasty complications Judith F. Baumhauer, MD*, Benedict F. DiGiovanni, MD Orthopedic Department, University of Rochester
Foot Ankle Clin N Am 8 (2003) 37 48 Salvage of first metatarsophalangeal joint arthroplasty complications Judith F. Baumhauer, MD*, Benedict F. DiGiovanni, MD Orthopedic Department, University of Rochester
THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery
 C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
Axi+LineTM Proximal Bunion CorrectionSystem. Surgical Technique
 Axi+LineTM Proximal Bunion CorrectionSystem Surgical Technique A i Line Proximal Bunion Correction System TM Desired angle correction is built into the plate, providing a self-reducing, 5-hole construct
Axi+LineTM Proximal Bunion CorrectionSystem Surgical Technique A i Line Proximal Bunion Correction System TM Desired angle correction is built into the plate, providing a self-reducing, 5-hole construct
Moderate to severe hallux valgus deformity: correction with proximal crescentic osteotomy and distal soft-tissue release
 Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
SURGICAL TECHNIQUE CHI. Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY
 CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
Index. Note: Page numbers of article titles are in bold face type.
 Index Note: Page numbers of article titles are in bold face type. A Achilles tendon, Zadek osteotomy effects on, 430 Adult acquired flatfoot disorder, 387 403 calcaneal Z osteotomy for, 397 399 historical
Index Note: Page numbers of article titles are in bold face type. A Achilles tendon, Zadek osteotomy effects on, 430 Adult acquired flatfoot disorder, 387 403 calcaneal Z osteotomy for, 397 399 historical
Forefoot/Midfoot Plating System
 Surgical Technique Forefoot/Midfoot Plating System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Surgical Technique Forefoot/Midfoot Plating System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
CHARLOTTE Lisfranc. Recontruction System SURGICAL TECHNIQUE
 CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
EFFECT OF EARLY WEIGHTBEARING AFTER MODIFIED LAPIDUS ARTHRODESIS: A Retrospective Study
 C H A P T E R 4 EFFECT OF EARLY WEIGHTBEARING AFTER MODIFIED LAPIDUS ARTHRODESIS: A Retrospective Study Irene O. Nwokolo, DPM Tony C. Nguyen, DPM Dan P. McDermott, DPM INTRODUCTION The modified Lapidus
C H A P T E R 4 EFFECT OF EARLY WEIGHTBEARING AFTER MODIFIED LAPIDUS ARTHRODESIS: A Retrospective Study Irene O. Nwokolo, DPM Tony C. Nguyen, DPM Dan P. McDermott, DPM INTRODUCTION The modified Lapidus
Astrid Modular Forefoot System. Surgical Technique
 Astrid Modular Forefoot System Surgical Technique Table of Contents Astrid a System for Surgery of the Forefoot... Scarf Osteotomies...6 Stabilization by Means of Two Parallel Double-Threaded Screws Introduced
Astrid Modular Forefoot System Surgical Technique Table of Contents Astrid a System for Surgery of the Forefoot... Scarf Osteotomies...6 Stabilization by Means of Two Parallel Double-Threaded Screws Introduced
Digital Surgery Complications
 Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
Angle-stable Foot plate system Pedus-O and Pedus-U
 www.marquardt-medizintechnik.de Angle-stable Foot plate system Pedus-O and Pedus-U Angle-stable Pedus-O and Pedus-U foot plate system > Angle-stable Pedus-O foot plate system 1. Product characteristics
www.marquardt-medizintechnik.de Angle-stable Foot plate system Pedus-O and Pedus-U Angle-stable Pedus-O and Pedus-U foot plate system > Angle-stable Pedus-O foot plate system 1. Product characteristics
PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE
 C H A P T E R 5 PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE Raymond G. Cavaliere, DPM INTRODUCTION Hammertoes can be classified as simple, moderate, and severe. The deformities
C H A P T E R 5 PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE Raymond G. Cavaliere, DPM INTRODUCTION Hammertoes can be classified as simple, moderate, and severe. The deformities
How to avoid complications of distraction osteogenesis for first brachymetatarsia
 220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING.
 LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
Technique Guide. 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot.
 Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair
 Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
AUTHOR(S): COUGHLIN, MICHAEL J., M.D., BOISE, IDAHO. An Instructional Course Lecture, The American Academy of Orthopaedic Surgeons
 JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
Diagnosing and treating hallux valgus: A conservative approach for a common problem
 REVIEW BRIAN G. DONLEY, MD Orthopaedic surgeon, Cleveland Clinic, specializing in foot and ankle disorders. CHRISTOPHER L. TISDEL, MD Orthopaedic surgeon. Cleveland Clinic. JAMES J. SFERRA, MD Orthopaedic
REVIEW BRIAN G. DONLEY, MD Orthopaedic surgeon, Cleveland Clinic, specializing in foot and ankle disorders. CHRISTOPHER L. TISDEL, MD Orthopaedic surgeon. Cleveland Clinic. JAMES J. SFERRA, MD Orthopaedic
A Patient s Guide to Bunions. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
Fracture and Dislocation of Metacarpal Bones, Metacarpophalangeal Joints, Phalanges, and Interphalangeal Joints ( 1-Jan-1985 )
 In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
Minimally Invasive Bunion Surgery: Methods and Outcomes
 Minimally Invasive Bunion Surgery: Methods and Outcomes Hummira H. Abawi, DPM Diplomate ABPM, AACFAS Instructor of Orthopedics, University of Maryland Medical Center Director of Education, Maryland VA
Minimally Invasive Bunion Surgery: Methods and Outcomes Hummira H. Abawi, DPM Diplomate ABPM, AACFAS Instructor of Orthopedics, University of Maryland Medical Center Director of Education, Maryland VA
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
PipTree. Arthrodesis of the PIP joint
 Arthrodesis of the PIP joint Table of Contents Introduction PipTree 2 System Characteristics 2 Indication 2 Surgical Technique Access 3 Osteotomy 3 Preparation of the proximal phalanx 3 Preparation of
Arthrodesis of the PIP joint Table of Contents Introduction PipTree 2 System Characteristics 2 Indication 2 Surgical Technique Access 3 Osteotomy 3 Preparation of the proximal phalanx 3 Preparation of
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant
 Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy
 Surgical Technique Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa Iowa
Surgical Technique Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa Iowa
The Flower Medial Column Fusion Plate
 The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
A New Incisional Approach to the Rheumatoid Foot
 A New Incisional Approach to the Rheumatoid Foot The authors introduce a new incisional approach to surgery of the rheumatoid foot. Advantages and disadvantages are presented. Historical comparisons are
A New Incisional Approach to the Rheumatoid Foot The authors introduce a new incisional approach to surgery of the rheumatoid foot. Advantages and disadvantages are presented. Historical comparisons are
Correction System. Surgical Technique
 Re+Line Bunion Correction System Surgical Technique Bunion Correction System Easy insertion and medial placement accuracy using Landmark Guide technology Greater and repeatable uniform compression across
Re+Line Bunion Correction System Surgical Technique Bunion Correction System Easy insertion and medial placement accuracy using Landmark Guide technology Greater and repeatable uniform compression across
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT. Miss Sue Kendall PhD FRCS (Orth&Trauma)
 THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
Essential Insights On Tendon Transfers For Digital Dysfunction
 Essential Insights On Tendon Transfers For Digital Dysfunction VOLUME: 23 PUBLICATION DATE: Apr 01 2010 Issue Number: 4 April 2010 Author(s): Lawrence DiDomenico, DPM, FACFAS While tendon transfers have
Essential Insights On Tendon Transfers For Digital Dysfunction VOLUME: 23 PUBLICATION DATE: Apr 01 2010 Issue Number: 4 April 2010 Author(s): Lawrence DiDomenico, DPM, FACFAS While tendon transfers have
CHARLOTTE. 3.0 and 4.3 Multi-Use Compression Screws SURGIC A L T ECHNIQUE
 CHARLOTTE 3.0 and 4.3 Multi-Use Compression Screws SURGIC A L T ECHNIQUE CHARLOTTE 3.0 and 4.3 Multi-Use Compression Screws SURGICAL TECHNIQUE Surgical Technique as described by: Robert Anderson, MD Bruce
CHARLOTTE 3.0 and 4.3 Multi-Use Compression Screws SURGIC A L T ECHNIQUE CHARLOTTE 3.0 and 4.3 Multi-Use Compression Screws SURGICAL TECHNIQUE Surgical Technique as described by: Robert Anderson, MD Bruce
Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2011.0704 Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis Kenneth J. Hunt, MD; J. Kent Ellington, MD, MS; Robert B. Anderson, MD; Bruce E. Cohen,
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2011.0704 Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis Kenneth J. Hunt, MD; J. Kent Ellington, MD, MS; Robert B. Anderson, MD; Bruce E. Cohen,
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint
 Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
