ORIGINAL STUDY INTRODUCTION
|
|
|
- Rodger Carroll
- 5 years ago
- Views:
Transcription
1 Acta Orthop. Belg., 2006, 72, ORIGINAL STUDY Clinical results of isolated reconstruction of the medial patellofemoral ligament for recurrent dislocation and subluxation of the patella Yoshinori MIKASHIMA, Masashi KIMURA, Yasukazu KOBAYASHI, Motoko MIYAWAKI, Taisuke TOMATSU From Gunma Sports Medicine Research Center, Gunma, and Institute of Rheumatology, Tokyo Women s University, Tokyo, Japan Complications and results of medial patellofemoral ligament (MPFL) reconstruction, performed between 2000 and 2003, were studied retrospectively in 24 randomised patients (24 knees). All procedures were performed for recurrent dislocation or subluxation of the patella, using an autogenous semitendinosus tendon. Two different methods of anchoring of the transplant were compared. After a 2-year followup, patellar stability was found to be similar, when the transplant was sutured to the fibrous tissue and periosteum overlying the patella or when it was fixed in a bone tunnel through the patella. The majority of the patients who had undergone MPFL reconstruction have returned to their previous level of sports activities. We had two cases of patella fracture and one case of persisting patella apprehension after surgery. Further studies must determine which measures are necessary to prevent these complications. Keywords : patella ; recurrent dislocation ; subluxation ; medial patellofemoral ligament reconstruction. INTRODUCTION Although more than 100 different surgical techniques for the treatment of patellar instability have been described over the past 100 years, various questions continue to be raised (1, 2, 10, 12). Based on recent biomechanical studies, the medial patellofemoral ligament (MPFL) is considered as the primary restraint against lateral dislocation among the medial patellar stabilisers (3, 5, 9). Conlan et al. (3) reported that the MPFL provided 53% of the total medial restraining force. Hautamaa et al (9) and Desio et al (5) respectively reported 55% and 60%. The MPFL extends from the superior two-thirds of the medial patellar margin to a point distal to the adductor tubercle and proximal to the posterior aspect of the femoral attachment of the medial collateral ligament (MCL). The superficial fibers blend with the posterior capsule of the knee (16). Several recent studies have documented the value of MPFL reconstruction for recurrent patellar dislocation and subluxation, and have investigated especially the association between clinical symptoms and patellofemoral congruency following different surgical techniques (4, 6-8, 13, 15, 17, 20, 21). Yoshinori Mimashima, MD, Registrar Masashi Kimura, MD, Head of Department Yasukazu Kobayashi, MD, Consultant Orthopaedic Surgeon Motoko Miyawaki, MD, Registrar Department of Orthopaedic Surgery, Gunma Sports Medicine Research Center, Gunma, Japan. Taisuke Tomatsu, MD, Professor, Department of Orthopaedic Surgery, Institute of Rheumatology, Tokyo Women s Medical University, Kawata chou, Shinjuku, Tokyo, Japan. Correspondence : Yoshinori Mikashima,? Takagi Hospital, , Imadera, Oume city, Tokyo, Japan. mikashima@mwb.biglobe.ne.jp 2006, Acta Orthopædica Belgica. No benefits or funds were received in support of this study
2 66 Y. MIKASHIMA, M. KIMURA, Y. KOBAYASHI, M. MIYAWAKI, T. TOMATSU We compared clinical symptoms, return to sports activities, complications, and results after MPFL reconstruction for recurrent patellar dislocation and subluxation with two different tendon anchorage methods. MATERIALS AND METHODS We retrospectively reviewed 24 randomised patients (24 knees) with recurrent patellar dislocation or subluxation, who had undergone MPFL reconstruction using an autogenous tendon as an isolated procedure between 2000 and There were 10 males and 14 females. Patients presenting with generalised joint laxity were excluded from this analysis. The mean age at the time of operation was 21.8 ± 4.9 years (range : 13 to 24). The average follow-up was 41.0 ± 8.7 months (range : 28 to 52). All patients were Japanese. The indication for MPFL reconstruction was made when, after three months of conservative treatment and quadriceps muscle exercises, symptoms such as giving way, painful clicking and instability in activities of daily living or sports activities were not satisfactorily ameliorated. On a skyline x-ray view, the sulcus angle was 138 to 162 (mean : ± 4.6 ). On computed tomography, the tibial external rotation angle was 0 to 10 (mean : 6.9 ± 5.5 ). Patients with recurrent patellar dislocation and subluxation with a tibial external rotation angle of 8 or less Fig. 1. The tibial external rotation angle, i.e. the angle between the posterior femoral condylar line and the posterior tibial condylar line on computed tomography. (fig 1), were treated with isolated MPFL reconstruction. When the tibial external rotation angle exceeded 8, MPFL reconstruction was combined with a distal realignment according to Elmslie-Trillat. The semitendinosus was used as an autogenous tendon to reconstruct the MPFL. The autogenous tendon was fixed over a button on the femur. On the patella it was either routed through a bone tunnel and then sutured to itself (fig 2 a, b), or directly sutured to the periosteal and fibrous tissue overlying the patella (fig 3). The bone tunnel was drilled through the patella from the proximal half of its medial margin to the center of its anterior surface using a 4.5 mm drill. The autogenous tendon was fixed temporarily using stitches, while the knee was held in 45 flexion and the patella was correctly positioned manually. The anatomical position of the patella was controlled intra-operatively with an axial X-ray view, with the knee in 45 knee flexion. Permanent fixation was done when the joint congruence was satisfactory and MPFL tension remained satisfactory throughout the whole range of knee flexion. Immediately after surgery, patients were placed in a knee immobiliser. Quadriceps exercises with the knee extended were started as soon as tolerated by the patient. Continuous passive motion began on the second postoperative day. At three weeks post-surgery a patellar brace was applied. Five weeks post-surgery, full weight bearing was allowed. Jogging and mild sports activities were permitted at 4 months and full sports activities at 6 months post-surgery. The patients were evaluated two years after surgery. Postoperative assessment included postoperative clinical symptoms, return to sports activities, and complications. The results of the two methods of fixation of the reconstructed ligament to the patella were compared. Postoperative clinical symptoms were evaluated comparing the pre- and post-operative Kujala score (11), which includes a variety of symptoms and signs of patellar instability with a maximal score of 100 points. To evaluate the results, we compared the level of preoperative and post-operative sports activity (previous level, reduced level, or sports activities abandoned). The delay in sports resumption was noted and the muscular condition was followed. Muscle strength of the flexors and extensors of the knee was measured at 6 months, 12 months, and 24 months after surgery using a Cybex II device, and the unaffected/affected side ratio was calculated. The results were compared between the two methods used to anchor the reconstructed ligament to the patella : the 24 patients were classified into two groups. Group A
3 CLINICAL RESULTS OF ISOLATED RECONSTRUCTION OF THE MEDIAL PATELLOFEMORAL LIGAMENT 67 b Fig. 2a-b. Bone tunnel fixation of the autogenous tendon through the patella with endo-button and end to end sutures. a included 12 patients whose reconstructed MPFL was anchored to the surface of the patella ; group B included 12 patients whose reconstructed MPFL was fixed into a patellar bone tunnel. Both groups consisted of 5 males and 7 females. In Group A, ages ranged from 16 to 25 years, with a mean of 24.0 ± 6.7 years. In Group B ages ranged from 13 to 24 years, with a mean of 22.3 ± 4.9 years. Stress radiographs were obtained. Radiological assessment included the lateral stress shift ratio following Ochi et al (18), obtained from a skyline view in 30 flexion with a stress of 2 kg (figs 4, 5). The findings were compared to those made on stress radiographs in 60 normal knees (Group N : 30 normal male knees and 30 normal female knees). For statistical analysis, Mann-Whitney s test was used, and p < 0.05 was regarded as significant. Fig. 3. Fixation of the autogenous tendon to fibrous tissues and periosteum overlying the patella.
4 68 Y. MIKASHIMA, M. KIMURA, Y. KOBAYASHI, M. MIYAWAKI, T. TOMATSU Fig. 4. Lateral stress shift ratio according to Ochi et al (18). lateral shift ratio = (BC/AB) 100 Fig. 5. Skyline view in 30 flexion with 2 kg stress. We also recorded all postoperative complications in the 24 patients. RESULTS The mean Kujala score was 95.2 ± 12.9 points (range : 82 to 100), compared to 30.5 ± 6.7 points (range : 28 to 38) before surgery. Four knees scored 100 points. Seventeen (70.8%) of the 24 patients were involved in recreational sports activities prior to injury (the appearance of knee pain). After surgery, 13 of the 17 patients (76.5%) resumed sport activities at the previous level, and 4 (23.5%) at a reduced level. None complained of patella apprehension or knee joint pain postoperatively. The mean interval until return to sport activities was 6.1 ± 0.85 months. The mean values for the ratio of extensor strength of the affected to the unaffected knee at 6 months, 12 months, 24 months after the surgery were 82.6 ± 10.6%, 90.6 ± 13.2%, and 95.8 ± 19.9%. The mean values for the ratio of the flexor strength of the affected to the unaffected knee at 6 months, 12 months, 24 months after the surgery were 75.6 ± 12.4%, 79.9 ± 11.5%, and 83.9 ± 12.8%. In those who had returned to previous sports activities, 24 months after surgery, the mean ratio of the extensor strength of the affected to the unaffected knee was 98.6 ± 7.6%, and 78.9 ± 6.8% in those who had reduced sports levels. The mean ratio of the flexor strength of the affected to the unaffected knee 24 months after the surgery was 88.6 ± 9.2% in those who had returned to the previous sports level, and 75.9 ± 7.8% in those who had reduced the sports level. The mean stress lateral shift ratios was 15.0 ± 5.5% (males : 14.4 ± 4.5%, females : 15.7 ± 6.7%) in the normal group, 20.0 ± 9.4% in Group A, and 19.2 ± 6.3% in Group B, against 32.3 ± 10.3% in group A and 35.6 ± 8.9% in group B before surgery. The postoperative values between Group A and B (p = 0.19), and between Group A/B and the normal group (p = 0.17) were not significantly different. Fracture of the patella occurred in two patients, both in Group B. One of them fractured her patella by hyperflexing the knee during a fall in her bathroom 4 weeks post-surgery (fig. 6a,b). She underwent surgery to remove a fragment of the patella and made a satisfactory recovery. In the other patient, a patella fracture was disclosed on a follow-up radiograph 5 weeks post-surgery, without a history of trauma. Rehabilitation was delayed, and the patient made a satisfactory recovery. Whereas the apprehension test was positive in all the knees pre-operatively, it was found positive at follow-up in only one patient (4.2%) belonging to Group B. The stress lateral shift ratio of this patient was 25.0%, against 35.3% before surgery.
5 CLINICAL RESULTS OF ISOLATED RECONSTRUCTION OF THE MEDIAL PATELLOFEMORAL LIGAMENT 69 a b Fig. 6. Patella fracture after drill hole fixation. DISCUSSION In our institution, the surgical procedure for patellofemoral tracking disorders was selected according to the type of patellofemoral joint incongruence. We use a Tanaka classification based on the sulcus angle and the tibial external rotation angle (fig 7). Type I (recurrent patellar dislocation) includes knees with a large sulcus angle and a large tibial external rotation angle of the tibia. Type II (patellar subluxation) includes knees with a large sulcus angle and a small tibial external rotation angle. Type III (excessive lateral pressure syndrome) includes knees with a small sulcus angle and a large tibial external rotation angle. Type IV (normal) includes knees with a small sulcus angle and a small tibial external rotation angle. We performed distal realignment mainly for type I, proximal realignment mainly for type II (19). Initially, the Elmslie-Trillat procedure alone was employed for distal realignment. However, many patients showed residual apprehension signs. Therefore, recently, MPFL reconstruction has been performed alone or combined with the Elmslie- Trillat procedure (13). Nomura et al (15) reported that, at an average follow-up of 5.9 years, MPFL reconstruction should be considered a safe and effective procedure, because 26 of 27 MPFL reconstructions using a mesh type artificial ligament were classified as excellent and good using the Crosby and Insall grading system. Deie et al (4) reported that at an average follow-up of 7.4 years, MPFL reconstruction should be considered an effective procedure, as the postoperative average Kujala score in 6 patients with MPFL reconstruction was 96.3 points. In our survey, there was no patient with recurrent dislocation, and good results were obtained with respect to activities of daily living. Few studies have reported on return to sports activities after MPFL reconstruction. Nomura (15) reported that jogging and mild sports activities Fig. 7. The Tanaka classification based on sulcus angle and tibial external rotation angle.
6 70 Y. MIKASHIMA, M. KIMURA, Y. KOBAYASHI, M. MIYAWAKI, T. TOMATSU were permitted after 8 weeks and full sport activities 12 weeks post-surgery using an artificial ligament for recurrent patellar dislocation. In our survey, the return to sports activities took longer after surgery, possibly because in our patients the semitendinosus tendon had been sacrificed. However, return to previous sports activities was achieved in many of our patients, possibly because MPFL reconstruction improved lateral patellar instability and eliminated anxiety to participate in sport activities. The reason why some patients returned to sports activities at a reduced level was thought to be muscular weakness around the knee, rather than persistence of patella apprehension or knee joint pain. As postoperative complications of MPFL reconstruction, Nomura (15) reported local pain about the femoral staples used for fixation of the artificial ligament, Yamada (21) reported restriction of flexion, and Watanabe (20) persisting patellar apprehension. We had two patella fractures in our 24 patients. Both of the patients with patella fracture were in Group B (patients whose reconstructed MPFL was fixed into a bone tunnel in the patella). We also had one patient complaining of persisting patellar apprehension postoperatively. Because in this study no significant difference after a 2-year follow-up was observed in the quality of fixation between suturing to the periosteum and the fibrous tissue overlying the patella and fixation in a bone tunnel, we recommend suturing to fibrous tissue and the patellar periosteum as the first choice, especially in patients with a small patella or open physes. The reconstructed ligament should be sutured as close as possible to the lateral retinaculum to ensure firm fixation. Fixation in a bone tunnel is recommended in patients with a thin fibrous and periosteal covering of the patella. Gomes et al (7) warned against damaging the cartilage surface of the patella by creating a bone tunnel. Utmost caution not to damage the cartilage surface or to cause fracture is necessary in creating a bone tunnel. The direction of the bone tunnel varied from parallel (Yamada et al. (21)) to oblique, as in our technique (fig 1 b) in relation to the patellar surface, needs further evaluation. In our survey, one knee was judged to have mild hypermobility. The influence of the knee angle during final fixation and the tension of fixation of the reconstructed ligament, on the persistence of patellar apprehension need further consideration. Gomes et al (7) fixed at 90 flexion, Nomura et al (15, 17) at 60, Yamada et al (21) at 45, Deie et al (4) at 30. Nomura et al (15, 17) placed a temporary 6-mm high tension spacer with traction at 0.5 kg while the artificial ligament was temporarily fixed, and fixed permanently after confirming the tension of the ligament to be adequate in the entire range of motion. Yamada et al (21) manually pushed the patella to the lateral side, while the transplant tension was adjusted so that the patella could not be dislocated. Since the tension of fixation is considered to change when autogenous tendons are used, such as a semitendinous tendon and a gracilis tendon, a quantitative measurement as with the artificial ligament of Nomura et al (15, 17) is less reliable. Further evaluation is necessary to find the limb position and tension of fixation appropriate for the prevention of slackness. Opinions also differ concerning the material to be used for ligament reconstruction. Nomura et al (15, 17) used an artificial ligament, and Deie et al (4) Yamada et al (21), Drez et al (6), and Watanabe et al (20) used autogenous tendons such as a semitendinosus or a gracilis tendon for the reconstruction. Gomes et al (7, 8) performed reconstruction initially using artificial ligaments (polyester, 8 mm wide) but have recently used a semitendinosus tendon. In summary, autogenous tendons are used in a majority of reports at present. We think that autogenous tendons are best, because we have achieved good results using autogenous tendons and there is nothing that surpasses an autologous histocompatibility. Further evaluation is also necessary concerning the reconstruction material. CONCLUSION 1. In this study, we investigated clinical symptoms, return to sports activities, complications, and outcome with two different methods of anchoring the reconstructed MPFL to the patella for recurrent patellar dislocation and subluxation.
7 CLINICAL RESULTS OF ISOLATED RECONSTRUCTION OF THE MEDIAL PATELLOFEMORAL LIGAMENT The majority of patients have returned to sports activities after MPFL reconstruction surgery. 3. The two methods used to anchor the reconstructed MPFL to the patella resulted in a similar postoperative outcome. REFERENCES 1. Aichroth PM, Al-Duri Z. Dislocation and subluxation of the patella : an overview. In : Aichroth PM, Al-Duri Z, eds. Knee Surgery. Martin Dunitz, London ; pp Barney L. Freeman III. Recurrent dislocation. In : Campbell s Operative Orthopaedics. Seventh edition, Mosby, Philadelphia 1987 ; 52 : pp Conlan T, Gaeth WPJr, Lemons JE. Evaluation of the medial soft-tissue restraints of the extensor mechanism of the knee. J Bone Joint Surg 1993 ; 75-A : Deie M, Ochi M, Yasumoto M et al. Reconstruction of the medial patellofemoral ligament for the treatment of habitual or recurrent dislocation of the patella in children. J Bone Joint Surg 2003 ; 85-B : Desio DS, Burk RT, Bachus KN. Soft tissue restraint to lateral patellar translation in human knee. Am J Sports Med 1998 ; 26 : Drez D, Edwards TB, Williams CS. Results of medial patellofemoral ligament reconstruction in the treatment of patellar dislocation. Arthroscopy 2001 ; 17 : Gomes JLE. Medial patellofemoral ligament reconstruction for recurrent dislocation of the patella ; a preliminary report. Arthroscopy 1992 ; 8 : Gomes JLE, Marczyk LRS, Cesar PC et al. Medial patellofemoral ligament reconstruction with semitendinosus autograft for chronic patellar instability : a follow up study. Arthroscopy 2004 ; 20 : Hautamaa PV, Fithian DC, Kaufmann KR et al. Medial soft tissue restraints in lateral patellar instability and repair. Clin Orthop 1998 ; 349 : Hughston JC, Deese M. Medial subluxation of the patella as a complication of lateral retinacular release. Am J Sports Med 1998 ; 16 : Kujala UM, Jaakkola LH, Koshinen SK et al. Scoring of patellofemoral disorders. : Arthroscopy 1993 ; 9 : Madigan R, Wissinger HA., Donaldson WF. Preliminary experience with a method of quadricepsplasty in recurrent subluxation of the patella. J Bone Joint Surg 1975 ; 57-A : Mikashima Y, Kimura M, Kobayashi Y et al. Medial patellofemoral ligament reconstruction for recurrent patellar instability. Acta Orthop Belg 2004 ; 70 : Morikawa T, Moriya H, Katsuro T et al. The study of operative treatment for recurrent patellar dislocation and subluxation. Rinshou Suports Igaku 1985 ; 2 : Nomura E, Horiuchi Y, Kihara M. A mid-term followup of medial patellofemoral ligament reconstruction using an artificial ligament for recurrent patellar dislocation. Knee 2000 ; 7 : Nomura E, Donald CF, Elizabeth EA. The significance of the medial patellofemoral ligament in patellar dislocation. Seikeigeka 2002 ; 53 : 1 : Nomura E, Inoue M. Surgical Technique and rationale for medial patellofemoral ligament reconstruction for recurrent patellar dislocation. Arthroscopy 2003 ; 19 : Ochi M, Murakami Y, Deie M et al. Roentgenographic examination of subluxation and instability of the patella. J Joint Surg 1996 ; 15 : Tanaka K, Kimura M, Hasegawa J. Study for patellofemoral malalignment. Tokyo hiza kansetugakkai kaishi 1990 ; 11 : Watanabe S, Omori G, Sofue T et al. Short term result of medial patellofemoral ligament reconstruction for recurrent dislocation of patella. J Japan Knee Society 2004 ; 29 : Yamada Y, Toritsuka Y, Shino K et al. The bi-socket medial patellofemoral ligament reconstruction for recurrent dislocation of the patella. J Japan Knee society 2004 ; 28 : Yoshimatsu T, Saito A, Fukushima K et al. Clinical follow-up study of the recurrent patella dislocation and patella subluxation syndrome ; relation between muscle recovery and sports activity. Seikeisaigaigeka (in Japanese) 2001 ; 44 :
Jia Li 1, Yongqian Li 1, Jingchao Wei 2, Jianzhao Wang 1, Shijun Gao 1 and Yong Shen 1*
 Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Li et al. Journal of Orthopaedic Surgery and Research 2014, 9:66 RESEARCH ARTICLE Open Access A simple technique for reconstruction of medial patellofemoral ligament with bone-fascia tunnel fixation at
Reconstruction of the medial patellofemoral ligament for treatment of patellar instability
 354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
354 Acta Orthopaedica 2008; 79 (3): 354 360 Review Reconstruction of the medial patellofemoral ligament for treatment of patellar instability Martin Lind, Bent W Jakobsen, Bent Lund, and Svend Erik Christiansen
Surgical treatments of patellar instability have been
 Reconstruction of the Medial Patellofemoral Ligament With Gracilis Tendon Autograft in Transverse Patellar Drill Holes Svend Erik Christiansen, M.D., Bent W. Jacobsen, M.D., Bent Lund, M.D., and Martin
Reconstruction of the Medial Patellofemoral Ligament With Gracilis Tendon Autograft in Transverse Patellar Drill Holes Svend Erik Christiansen, M.D., Bent W. Jacobsen, M.D., Bent Lund, M.D., and Martin
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Medial Patellofemoral Ligament (MPFL) Surgical Technique
 Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis Autograft without Bone Tunnel
 Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
Original Article Clinics in Orthopedic Surgery 2015;7:457-464 http://dx.doi.org/10.4055/cios.2015.7.4.457 Medial Patellofemoral Ligament Reconstruction for Recurrent Patellar Instability Using a Gracilis
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES
 HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES Written by Philippe Landreau, Qatar The treatment of anterior cruciate ligament injuries remains challenging in young athletic populations. A residual
HISTORY AND INDICATIONS OF LATERAL TENODESIS IN ATHLETES Written by Philippe Landreau, Qatar The treatment of anterior cruciate ligament injuries remains challenging in young athletic populations. A residual
Jacques Menetrey, MD, PD. Uniklinik Balgrist. Unité d Orthopédie et Traumatologie du Sport (UOTS)
 Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Abstract. Introduction. Michele Vasso 1 Katia Corona 2 Giuseppe Toro 1 Marco Rossini 1 Alfredo Schiavone Panni 1
 256 Technical Note THIEME Anatomic Double-Bundle Medial Patellofemoral Ligament Reconstruction with Autologous Semitendinosus: Aperture Fixation Both at the Femur and the Patella Michele Vasso 1 Katia
256 Technical Note THIEME Anatomic Double-Bundle Medial Patellofemoral Ligament Reconstruction with Autologous Semitendinosus: Aperture Fixation Both at the Femur and the Patella Michele Vasso 1 Katia
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact)
 STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
A Systematic Review Of Complications And Failures Associated With Medial Patellofemoral Ligament Reconstruction For Recurrent Patellar Dislocation
 Archived version from NCDOCKS Institutional Repository http://libres.uncg.edu/ir/asu/ A Systematic Review Of Complications And Failures Associated With Medial Patellofemoral Ligament Reconstruction For
Archived version from NCDOCKS Institutional Repository http://libres.uncg.edu/ir/asu/ A Systematic Review Of Complications And Failures Associated With Medial Patellofemoral Ligament Reconstruction For
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco
 Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Peggers Super Summaries: PFJ
 Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Anatomical Medial Patellofemoral Ligament Reconstruction in Management of Cases of Patellar Instability
 Med. J. Cairo Univ., Vol. 84, No. 2, September: 145-151, 2016 www.medicaljournalofcairouniversity.net Anatomical Medial Patellofemoral Ligament Reconstruction in Management of Cases of Patellar Instability
Med. J. Cairo Univ., Vol. 84, No. 2, September: 145-151, 2016 www.medicaljournalofcairouniversity.net Anatomical Medial Patellofemoral Ligament Reconstruction in Management of Cases of Patellar Instability
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Extensor Mechanism Rupture
 Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
Extensor Mechanism Rupture Repair or Augmentation Michael J. Stuart MD Mayo Clinic Rochester, MN Michael J. Stuart MD February 25, 2018 Financial Relationships Consultant & Royalties- Arthrex Research
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
MCL Injuries: When and How to Repair Scott D. Mair, MD
 MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
Medial patellofemoral ligament reconstruction using dual patella docking technique
 2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN. Guy BELLIER PARIS France
 BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN Guy BELLIER PARIS France TREATMENT OF ACL TEARS IN CHILDREN CONTROVERSIAL DIAGNOSIS clinical exam X-rays (stress) M.R.I. arthroscopy ACL TEARS
BAD RESULTS OF CONSERVATIVE TREATMENT OF ACL TEARS IN CHILDREN Guy BELLIER PARIS France TREATMENT OF ACL TEARS IN CHILDREN CONTROVERSIAL DIAGNOSIS clinical exam X-rays (stress) M.R.I. arthroscopy ACL TEARS
Acute patellar dislocation in adults
 CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. MPFL RECONSTRUCTION
 ! SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. LATERAL PATELLOFEMORAL INSTABILITY AND THE MEDIAL PATELLOFEMORAL COMPLEX Lateral patellofemoral instability is characterized
! SURGICAL TECHNIQUE PREPARED BY MEDSHAPE, INC. IN CONJUNCTION WITH JACK FARR, M.D. LATERAL PATELLOFEMORAL INSTABILITY AND THE MEDIAL PATELLOFEMORAL COMPLEX Lateral patellofemoral instability is characterized
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella Treated with a Different Method in Each Knee
 Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Complications of Total Knee Arthroplasty
 Progress in Clinical Medicine Complications of Total Knee Arthroplasty JMAJ 44(5): 235 240, 2001 Shinichi YOSHIYA*, Masahiro KUROSAKA** and Ryosuke KURODA*** *Director, Department of Orthopaedic Surgery,
Progress in Clinical Medicine Complications of Total Knee Arthroplasty JMAJ 44(5): 235 240, 2001 Shinichi YOSHIYA*, Masahiro KUROSAKA** and Ryosuke KURODA*** *Director, Department of Orthopaedic Surgery,
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management
 SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
Anterolateral Ligament. Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine
 Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions T Smith, S Donell Citation T Smith, S Donell. The Rehabilitation
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 8 Number 1 The Rehabilitation Following Medial Patellofemoral Ligament Reconstructions T Smith, S Donell Citation T Smith, S Donell. The Rehabilitation
Minimally Invasive ACL Surgery
 Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
OPERATIVE TREATMENT OF THE INTERCONDYLAR FRACTURE OF THE FEMUR
 OPERATIVE TREATMENT OF THE INTERCONDYLAR FRACTURE OF THE FEMUR S G Chee, K S Lam, B K Tay, N Balachandran SYNOPSIS Operative treatment of 28 intercondylar fractures of femur were done from 98 to 985. The
OPERATIVE TREATMENT OF THE INTERCONDYLAR FRACTURE OF THE FEMUR S G Chee, K S Lam, B K Tay, N Balachandran SYNOPSIS Operative treatment of 28 intercondylar fractures of femur were done from 98 to 985. The
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY
 SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
Medial Patellofemoral Ligament Reconstruction
 Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
Medial Patellofemoral Ligament Reconstruction 1. Defined a. Reconstruction of the medial patellofemoral ligament in an effort to restore medial patellar stability and reduce chances of lateral dislocation.
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction
 In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia
 Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
The AperFix II System
 The AperFix II System A Complete Anatomic Solution Transtibial Surgical Technique 2 AperFix II System Transtibial Surgical Technique Figure 1 A Complete Anatomic Solution The Cayenne Medical AperFix and
The AperFix II System A Complete Anatomic Solution Transtibial Surgical Technique 2 AperFix II System Transtibial Surgical Technique Figure 1 A Complete Anatomic Solution The Cayenne Medical AperFix and
Anterior Tibial Subluxation with ACL Deficient Knees influences the Knee Stability after ACL Reconstruction.
 Anterior Tibial Subluxation with ACL Deficient Knees influences the Knee Stability after ACL Reconstruction. RYOTA TAKASE 1), KAZUHISA HATAYAMA 1), MASANORI TERAUCHI 1) KENICHI SAITO 2), HIROTAKA CHIKUDA
Anterior Tibial Subluxation with ACL Deficient Knees influences the Knee Stability after ACL Reconstruction. RYOTA TAKASE 1), KAZUHISA HATAYAMA 1), MASANORI TERAUCHI 1) KENICHI SAITO 2), HIROTAKA CHIKUDA
Why anteromedial portal is the best
 Controversies in ACL Reconstruction Why anteromedial portal is the best Robert A. Gallo, MD Associate Professor Nothing to disclose Case presentation 20-year-old Division III track athlete sustained ACL
Controversies in ACL Reconstruction Why anteromedial portal is the best Robert A. Gallo, MD Associate Professor Nothing to disclose Case presentation 20-year-old Division III track athlete sustained ACL
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Anatomy and Sports Injuries of the Knee
 Anatomy and Sports Injuries of the Knee I. Anatomy II. Assessment III. Treatment IV. Case Study V. Dissection Anatomy Not a hinge joint 6 degrees of freedom Flexion/Extension Rotation Translation Anatomy
Anatomy and Sports Injuries of the Knee I. Anatomy II. Assessment III. Treatment IV. Case Study V. Dissection Anatomy Not a hinge joint 6 degrees of freedom Flexion/Extension Rotation Translation Anatomy
Human ACL reconstruction
 Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Computational Evaluation of Predisposing Factors to Patellar Dislocation
 Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System
 Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
OMICS - 3rd Int. Conference & 2
 KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
KNEE OBJECTIVE STABILITY AND ISOKINETIC THIGH MUSCLE STRENGTH AFTER ANTERIOR CRUCIATE LIGAMENT (ACL) RECONSTRUCTION: A Randomized Six-Month Follow-Up Study M. Sajovic Department of Orthopedics and Sports
SLARD Symposium: MCL s Injuries
 SLARD Symposium: MCL s Injuries ISAKOS 11 th Biennial Congress Tue June 6 th 2017 13:30 14:15 Shanghai, China Gustavo A. Rincón, MD Chairman Department Orthopedic Surgery Hospital de San José Bogotá -
SLARD Symposium: MCL s Injuries ISAKOS 11 th Biennial Congress Tue June 6 th 2017 13:30 14:15 Shanghai, China Gustavo A. Rincón, MD Chairman Department Orthopedic Surgery Hospital de San José Bogotá -
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Please differentiate an internal derangement from an external knee injury.
 Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
Knee Orthopaedic Tests Sports and Knee Injuries James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Knee Injury Strain, Sprain, Internal Derangement Anatomy of the Knee Please
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents
 Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Patellar instability
 Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Surgical treatment of patellar instability can be
 Medial Patellofemoral Ligament Reconstruction Using a Modified Reverse-Loop Technique Nels E. Sampatacos, M.D., and Mark H. Getelman, M.D. Abstract: Medial patellofemoral ligament reconstruction is a commonly
Medial Patellofemoral Ligament Reconstruction Using a Modified Reverse-Loop Technique Nels E. Sampatacos, M.D., and Mark H. Getelman, M.D. Abstract: Medial patellofemoral ligament reconstruction is a commonly
Retinacular tear knee
 P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
P ford residence southampton, ny Retinacular tear knee The medial patellofemoral ligament (MPFL) helps to keep the kneecap centered along the front of the knee, so that it tracks well during knee movements.
Patellofemoral instability is a common cause of knee
 280 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4):280-93 Patella Instability Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H. Sherman, M.D. Patellofemoral instability is a common
280 Bulletin of the NYU Hospital for Joint Diseases 2007;65(4):280-93 Patella Instability Reuven Minkowitz, M.D., Chris Inzerillo, M.D., and Orrin H. Sherman, M.D. Patellofemoral instability is a common
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System
 Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
Functional outcome following modified Elmslie Trillat procedure
 The Knee 13 (2006) 464 468 www.elsevier.com/locate/knee Functional outcome following modified Elmslie Trillat procedure D. Karataglis, M.A. Green, D.J.A. Learmonth Royal Orthopaedic Hospital, Bristol Road
The Knee 13 (2006) 464 468 www.elsevier.com/locate/knee Functional outcome following modified Elmslie Trillat procedure D. Karataglis, M.A. Green, D.J.A. Learmonth Royal Orthopaedic Hospital, Bristol Road
Ligamentous and Meniscal Injuries: Diagnosis and Management
 Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft
 384 Clinicale Evaluation Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft Swaroop Patel, Resident, Vijendra D. Chauhan, Professor, Anil Juyal, Professor, Rajesh
384 Clinicale Evaluation Evaluation of Arthroscopic Anterior Cruciate Ligament Reconstruction using Hamstring Graft Swaroop Patel, Resident, Vijendra D. Chauhan, Professor, Anil Juyal, Professor, Rajesh
International Journal of Orthopaedics Sciences 2017; 3(3): Dr. Anas M and Dr. Ansari N. DOI:
 2017; 3(3): 588-592 ISSN: 2395-1958 IJOS 2017; 3(3): 588-592 2017 IJOS www.orthopaper.com Received: 23-05-2017 Accepted: 24-06-2017 Dr. Anas M MS(Orthopaedics) Senior Resident Department of Dr. Ansari
2017; 3(3): 588-592 ISSN: 2395-1958 IJOS 2017; 3(3): 588-592 2017 IJOS www.orthopaper.com Received: 23-05-2017 Accepted: 24-06-2017 Dr. Anas M MS(Orthopaedics) Senior Resident Department of Dr. Ansari
ARTICLE IN PRESS. Technical Note
 Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients
 Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player
 UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
UNUSUAL ACL CASE: Tibial Eminence Fracture in a Female Collegiate Basketball Player Cheri Drysdale, MEd,, ATC Margot Putukian,, MD Jeffery Bechler,, MD Princeton University How many of you have done an
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability
 Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
Medial Patellofemoral Ligament Repair Versus Reconstruction for Recurrent Patellar Instability Two-Year Results of an Algorithm-Based Approach Jason L. Dragoo,* MD, Michael Nguyen, MD, Corey T. Gatewood,
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
Personal use only. MRI of the extensor mechanism of the knee. 5 th Musculoskeletal MRI meeting. Falkowski, MD, MHBA
 MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
QuadsTape System TM. For Quadriceps Tendon Reconstruction. Surgical Technique Manual
 QuadsTape System TM For Quadriceps Tendon Reconstruction Surgical Technique Manual 0086 Introduction QuadsTape System TM The QuadsTape System comprises a wide open weave Poly-Tape prosthesis with associated
QuadsTape System TM For Quadriceps Tendon Reconstruction Surgical Technique Manual 0086 Introduction QuadsTape System TM The QuadsTape System comprises a wide open weave Poly-Tape prosthesis with associated
Investigation of the factors to affect the duration to return sports after the surgery of anterior talofibular ligament repair with arthroscopy
 Investigation of the factors to affect the duration to return sports after the surgery of anterior talofibular ligament repair with arthroscopy Hamamatsu University School of Medicine Mitsuru Hanada, Shoichi
Investigation of the factors to affect the duration to return sports after the surgery of anterior talofibular ligament repair with arthroscopy Hamamatsu University School of Medicine Mitsuru Hanada, Shoichi
Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery. Restore patella stability.
 Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
The medial side of the knee has been relatively overlooked
 REVIEW ARTICLE Medial and Posteromedial Instability of the Knee: Evaluation, Treatment, and Results James P. Stannard, MD Abstract: Medial-sided knee ligament injuries are complex and require a thorough
REVIEW ARTICLE Medial and Posteromedial Instability of the Knee: Evaluation, Treatment, and Results James P. Stannard, MD Abstract: Medial-sided knee ligament injuries are complex and require a thorough
Morbidity Following Anterior Cruciate Ligament Reconstruction Using Hamstring Autograft
 214 ACL Morbidities with Hamstring Grafts M Soon et al Original Article Morbidity Following Anterior Cruciate Ligament Reconstruction Using Hamstring Autograft M Soon, 1 MBBS, MRCS, P Chang, 2 MBBS, FRCS,
214 ACL Morbidities with Hamstring Grafts M Soon et al Original Article Morbidity Following Anterior Cruciate Ligament Reconstruction Using Hamstring Autograft M Soon, 1 MBBS, MRCS, P Chang, 2 MBBS, FRCS,
Minimally invasive medial patellofemoral ligament reconstruction for patellar instability using an artificial ligament: A two year follow-up
 The University of Notre Dame Australia ResearchOnline@ND Medical Papers and Journal Articles School of Medicine 2016 Minimally invasive medial patellofemoral ligament reconstruction for patellar instability
The University of Notre Dame Australia ResearchOnline@ND Medical Papers and Journal Articles School of Medicine 2016 Minimally invasive medial patellofemoral ligament reconstruction for patellar instability
Knee Joint Assessment and General View
 Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes
 Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
Knee Dislocation: Spectrum of Injury, Evolution of Treatment & Modern Outcomes William M Weiss, MD MSc FRCSC Orthopedic Surgery & Rehabilitation Sports Medicine, Arthroscopy & Extremity Reconstruction
PROSPECTIVE AND COMPAR TMENT (MEDIAL PETELLOFEMOR
 ORIGINAL ARTICLE PROSPECTIVE AND COMPAR ARATIVE STUDY BETWEEN CONSERVATIVE AND SURGICAL TREATMENT TMENT (MEDIAL PETELLOFEMOR OFEMORAL LIGAMENT REPAIR) IN PATELL TELLAR ACUTE DISLOCA OCATIONS GILBERTO LUIS
ORIGINAL ARTICLE PROSPECTIVE AND COMPAR ARATIVE STUDY BETWEEN CONSERVATIVE AND SURGICAL TREATMENT TMENT (MEDIAL PETELLOFEMOR OFEMORAL LIGAMENT REPAIR) IN PATELL TELLAR ACUTE DISLOCA OCATIONS GILBERTO LUIS
AFX. Femoral Implant. System. The AperFix. AM Portal Surgical Technique Guide. with the. The AperFix System with the AFX Femoral Implant
 The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
Knee Joint Anatomy 101
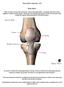 Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Financial Disclosure. Medial Collateral Ligament
 Matthew Murray, M.D. UTHSCSA Sports Medicine Financial Disclosure Dr. Matthew Murray has no relevant financial relationships with commercial interests to disclose. Medial Collateral Ligament Most commonly
Matthew Murray, M.D. UTHSCSA Sports Medicine Financial Disclosure Dr. Matthew Murray has no relevant financial relationships with commercial interests to disclose. Medial Collateral Ligament Most commonly
Isolated reconstruction of the medial patellofemoral ligament with autologous quadriceps tendon
 J Orthopaed Traumatol (2016) 17:155 162 DOI 10.1007/s10195-015-0375-6 ORIGINAL ARTICLE Isolated reconstruction of the medial patellofemoral ligament with autologous quadriceps tendon Giovanni Vavalle 1,2
J Orthopaed Traumatol (2016) 17:155 162 DOI 10.1007/s10195-015-0375-6 ORIGINAL ARTICLE Isolated reconstruction of the medial patellofemoral ligament with autologous quadriceps tendon Giovanni Vavalle 1,2
Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea
 Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Assessment of Patellar Laxity in the in vitro Native Knee
 Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
