EMG CASE No. 61, April 2003
|
|
|
- Gwenda Cain
- 5 years ago
- Views:
Transcription
1 EMG CASE No. 61, April 2003 Presenting Symptom(s): Progressive left arm weakness, cramping, and muscle twitching. Case prepared by: Ann A. Little, M.D. James W. Teener, M.D. University of Michigan Department of Neurology Appropriate Audience: Residents and practicing physicians Learning Objectives: After completing this educational activity, participant will be able to: 1) evaluate patients presenting with limb weakness and muscular atrophy, 2) develop a differential diagnosis with regard to limb weakness and muscular atrophy, and 3) understand and differentiate between various lower motor neuron diseases. This case is no longer available for CME credit. History Chief Complaint: Left arm weakness and muscle wasting Presentation: A 20 year-old left-handed man has noticed insidious, painless, progressive weakness in his left arm over the last year associated with loss of muscle mass. He notices increasing muscle twitching in his forearm and hand, which in his hand results in coarse twitching movements of his fingers. He is finding it more difficult to use a computer keyboard and telephone at work secondary to compromised fine motor control. He has recently begun to have painful muscle cramps in his forearm, hand, and fingers. Initial Differential Diagnosis A lower motor neuron lesion is the most common cause of weakness and atrophy, although myopathies can also produce this combination. The presence of fasciculation in this case is strongly supportive of a lower motor neuron lesion. Considerations in this case include: Neuropathic causes with (only) lower motor neuron signs: cervical radiculopathy brachial plexopathy multiple mononeuropathies nerve entrapments mononeuritis multiplex polyneuropathies with asymmetric involvement inflammatory demyelinating neuropathy (AIDP, CIDP) multifocal motor neuropathy hereditary neuropathies (hereditary liability to pressure palsy, for example) motor neuron diseases spinal muscular atrophy progressive muscular atrophy spinobulbar muscular atrophy (Kennedy's disease) progressive post-polio muscular atrophy monomelic amyotrophy Copyright 2003 AAPM&R Page 1 of 9
2 motor neuron disease secondary to lymphoproliferative disorders Neuropathic causes which can present with lower motor neuron signs in combination with upper motor neuron signs, such as spasticity and hyperreflexia. amyotrophic lateral sclerosis cervical radiculopathy with cervical myelopathy syringomyelia Myopathic causes leading to weakness and atrophy: facioscapulohumeral muscular dystrophy inflammatory myopathies metabolic myopathies Musculoskeletal causes leading to disuse atrophy and weakness: local arthropathy inflammatory arthritis trauma Commentary I The onset of symptoms has been insidious in this patient. The history of progressive weakness and muscle atrophy with fasciculation points to a lower motor neuron process. The initial painless progression of symptoms is extremely helpful in formulating the differential diagnosis. Mononeuropathies and motor neuron diseases and perhaps a few myopathic disorders are now favored because of lack of pain. The painless progression of symptoms makes plexopathy, particularly brachial neuritis, and radiculopathy less likely. Among myopathic causes, facioscapulohumeral (FSH) dystrophy is still a viable thought. It often presents with asymmetric weakness and atrophy of the posterior shoulder muscles and biceps. However, the fasciculation described is not accounted for by myopathic disorders. Tremor, though, is often present in patients with FSH and perhaps the movements described could be due to tremor rather than fasciculation. His age would be consistent with onset of a dystrophy. Inflammatory and metabolic myopathies are less likely because of the profound asymmetry and the presence of the muscular twitching. Musculoskeletal causes are unlikely in this case because of the lack of pain. Additional history including further detail of symptoms, past medical history, and family history may help to pinpoint the cause of the progressive weakness in this patient. Ultimately, electrodiagnostic studies should allow definitive localization of the pathologic process. History, continued The patient denies any sensory changes or any deficits in the other three extremities. He occasionally has painful muscle cramping in his fingers, hand, and forearm. These symptoms began well after he first noticed weakness and atrophy. He reports no myalgia or Copyright 2003 AAPM&R Page 2 of 9
3 arthralgia. He denies cervical pain. Past medical history is unremarkable except for an incident in childhood in which the patient had trauma to his left shoulder, resulting in joint dislocation. He recovered from that incident without apparent sequelae. No other family members have had symptoms like those of the patient, and there is no family history of cancer. The patient does not smoke or drink alcohol. His health has otherwise been excellent. Prior imaging has included MRI of brain, cervical spine, and brachial plexus (with contrast), as well as plain films of the left shoulder. All studies were normal. Laboratory evaluation has included a normal sedimentation rate, routine chemistry battery, CBC, and CPK level. No antibody to GM-1 was detected Commentary II Lack of sensory complaints is extremely helpful in narrowing the differential diagnosis. We can discard processes that affect both sensory and motor function, including most neuropathies, radiculopathies, and plexopathies. We now must consider the disorders on our differential that typically produce only motor abnormalities. FSH muscular dystrophy and perhaps other unusual myopathies remain, but are distinctly unlikely given the fasciculation. Disorders of the motor neuron or motor nerve are now most likely. Brachial neuritis (i.e., neuralgic amyotrophy) can affect only motor function, but it is typically an extremely painful, acute condition, whereas the process here is painless and more chronically progressive. Revised Differential Diagnosis motor neuron diseases monomelic amyotrophy spinal muscular atrophy spino-bulbar muscular atrophy (Kennedy's disease) ALS progressive post-polio muscular atrophy motor neuron disease secondary to lymphoproliferative disorders motor neuropathies multifocal motor neuropathy hereditary motor neuropathy - not supported by family history and would be unlikely to have persistently asymmetric course Physical Examination Mental Status: Normal Cranial Nerves: 2-12 intact Muscular Examination: Left triceps, first dorsal interosseus, and thenar group have notable atrophy. Fasciculations are present. Strength is 5/5 throughout all muscle groups except in the left upper limb as noted in the following table: Copyright 2003 AAPM&R Page 3 of 9
4 Deltoid Biceps Triceps Wrist Extensors Median Hand Ulnar Hand Intrinsics Intrinsics Reflexes: 2+ throughout the upper and lower extremities with the exception of the left triceps reflex, which is absent. Babinski was negative. Sensation: intact to light touch, pinprick, vibration, and temperature in all four extremities, trunk, and neck. Gait: normal, narrow-based; patient is able to walk on his toes, heels, and in tandem fashion with no difficulty. Commentary III Physical examination supports lack of sensory changes and lack of upper motor neuron signs. Weakness and atrophy are restricted to the left arm. The presence of fasciculations is confirmed. The definite presence of fasciculations allows us to discard the myopathies from our differential. We are left with motor neuron diseases and motor neuropathies. A diagnosis of definite ALS cannot be made in the absence of upper motor neuron signs, but often patients will present with a purely lower motor neuron syndrome and later go on to develop upper motor neuron signs, then allowing a diagnosis of ALS to be made. Thus we cannot discard ALS from our differential at this time, although the development of ALS in a 20-year-old man would be distinctly unusual. Other motor neuron disorders are rarely this asymmetric with the exception of monomelic amyotrophy. Multifocal motor neuropathy also remains highly possible. Monomelic amyotrophy: Monomelic amyotrophy is a rare lower motor neuron disease that affects predominantly one upper limb with occasional minor involvement of the contralateral upper limb. It was described first in Japan (Hirayama et al., 1959) and perhaps is most common in Indian and Japanese populations, although cases are now being described worldwide. Average age of onset is between 15 and 25 years of age. Estimated male:female involvement ranges from 5:1 to 10:1. Onset is with insidious, painless wasting/weakness of muscles of one upper limb, often with sparing of the brachioradialis muscle. There is no sensory deficit; reflexes may be normal or may be reduced. With progression of the disease, tremor of fingers may be noted. Muscle stiffness/weakness may be exaggerated in cold environments. Hyperhidrosis is seen in some patients. The pathological process is related to focal loss of anterior horn cells often localized to one or two cervical levels with only minor involvement of anterior horn cells of neighboring cervical levels. Imaging of the cervical spine may be normal or may show asymmetric atrophy of one anterior horn region. Nerve conduction studies are often normal until later in the disease process when loss of axons may lead to low amplitude CMAP responses. Needle examination reveals denervative process in the distribution of the affected cervical segments. Often there is subclinical involvement in the contralateral arm detected on needle examination. There should be no abnormality in the legs or beyond the affected cervical segments. Disease progression generally halts after one to two years, though may continue longer in rare cases. There is no treatment currently. Absolutely positive differential from other motor neuron disorders may require prolonged observation. If there is no progression to other body segments over 1-2 years, then other motor neuron diseases have been excluded. Copyright 2003 AAPM&R Page 4 of 9
5 Multifocal Motor Neuropathy: Multifocal motor neuropathy is characterized by slowly progressive, asymmetric weakness with atrophy, although the weakness may often be more severe than expected for the degree of atrophy. Peak age of onset is from the 20s to the 40s; men are more affected than women. Upper limbs are often affected first and more severely. Progression may continue for years. Patients may or may not have muscle cramps and fasciculations. Nerve conduction studies are significant for complete or partial conduction blocks in motor nerves. Focal slowing of conduction may also be seen. Sensory nerve conduction studies are normal. The needle examination documents denervation in the territories of individual nerves, with multiple nerves often being affected. Laboratory studies reveal the presence of GM-1 antibodies in 40-80% of cases. There is effective treatment for mutifocal motor neuropathy and therefore it is important to differentiate from motor neuron diseases and other diseases for which there is no treatment. Treatment for multifocal motor neuropathy is with IVIG or cyclophosphamide; steroids may worsen the disease. Commentary IV Median nerves and ulnar nerves across the elbows should be examined to evaluate the clinical abnormalities. Electrodiagnostic evaluation should include motor and sensory nerve studies in three limbs to evaluate for peripheral polyneuropathy. F-waves should be performed to evaluate for a condition affecting proximal nerve function such as chronic idiopathic demyelinating polyradiculopathy. Electromyographic examination should include the hand muscles, which are the most involved clinically. A lower limb, including a foot muscle, should be studied to evaluate for a loss of motor innervation in a distal to proximal gradient. Electrophysiologic Data SENSORY NERVE CONDUCTION STUDIES NERVE SIDE STIM SITE RECORD cm AMPL (uv) LAT (ms) (m/sec) Median L Wrist Index Median R Wrist Index Radial L Forearm Wrist Radial R Forearm Wrist ulnar L Wrist 5th ulnar R Wrist 5th Sural L Calf Ankle MOTOR NERVE CONDUCTION STUDIES CV NERVE SIDE STIM SITE RECORD cm AMPL (mv) LAT (ms) CV(m/sec) Median L Wrist Thenar Median R Wrist Thenar Copyright 2003 AAPM&R Page 5 of 9
6 Median L Elbow Thenar 61.1 Median R Elbow Thenar 56.0 Ulnar L Wrist Hypothenar Ulnar R Wrist Hypothenar Ulnar L Below Hypothenar Elbow Ulnar R Below Hypothenar Elbow Ulnar L Above Elbow Hypothenar Peroneal L Ankle EDB Peroneal L Below EDB Knee Tibial L Ankle Abd. Hal Tibial f- response L 45.3 NEEDLE ELECTROMYOGRAPHY INSERtional activity: N, sust, unsust FIB: 0, 1+, 2+, 3+, 4+ OTHer: 0 or fascic, myotonia, myokymia EFFort: N, decr RECruitment: N, inc or dec 1+, 2+, 3+, 4+ AMPlitude: N, inc or dec 1+, 2+, 3+, 4+ DURation: N, inc or dec 1+, 2+, 3+, 4+ POLyphasia: N, inc or dec 1+, 2+, 3+, 4+ R/L MUSCLE INSER FIB OTH EFF REC AMP DUR POL L Biceps Brachii N 0 0 N +/- +/- +/- N L Triceps N 1+ fascic N /- L deltoid N 0 0 N N N N N L EI N 0 0 N L FDIH N 0 fascic N L APB N 0 0 N +/- +/ L Pronator N 1+ 0 N 4+ +/- 3+/- Teres 3+/- R Pronator Teres N 0 0 N +/- 1+ +/- +/- R FDIH N 0 0 N 1+ +/- +/- +/0 R Triceps N 0 0 N Copyright 2003 AAPM&R Page 6 of 9
7 R Deltoid N 0 0 N N N N N L Vastus N 0 0 N N N N N Medialis L Medial N 0 0 N N N N N Gastroc L Anterior Tibialis N 0 0 N N N N N Summary: The sensory nerve conduction studies are normal, even in the ulnar nerve where the CMAP amplitude is markedly reduced. No motor conduction block is detected, given the preservation of amplitudes with proximal stimulation. Needle examination reveals prominent denervation and reinnervation changes in the left arm with the C7 spinal level being most severely affected, but clearly involving muscles of the C6 - C8 myotomes. In addition, milder, chronic denervation changes are noted in similar spinal levels in the clinically asymptomatic right arm. Needle examination of select leg muscles is normal. Diagnostic Impression This study provides electrodiagnostic evidence of a denervating disorder affecting the left greater than right arms. Multilevel cervical radiculopathy or a disorder of the anterior horn cells best explain the electrodiagnostic findings. No conduction block was identified, making the diagnosis of multifocal motor neuropathy unlikely. This study, in combination with the clinical situation, is most suggestive of left monomelic amyotrophy. Commentary IV This case of slowly progressive weakness without pain or sensory abnormality in a young man represents a nearly classic presentation of monomelic amyotrophy. One question that has been raised in the past is whether monomelic amyotrophy might be an early presentation of ALS and whether or not the disease will eventually involve all limbs. Gourie- Devi et al. (2003) have recently addressed these issues in their long term follow up of 44 patients with monomelic amyotrophy. They included 44 patients in their study who had met criteria for monomelic amyotrophy for a minimum of five years, to a maximum of 23 years (mean 9.7 years, 68% for longer than 10 years). The mean age of onset of symptoms was 19.8 years with a range of years, however, 82% of patients had symptom onset between the ages of 16 and 25. Male:female ratio was 10:1. An equal distribution between sides (right:left) was noted. In 18.2% of patients, the contralateral upper limb was affected, but to a much milder degree. Regarding course of the disease, 70.3% of patients had no further progression of their symptoms after the first two years. 94.6% had no progression after 5 years. Of perhaps more importance to the patient is that the level of final disability was regarded to be mild in 68.2%, moderate in 22.7%, and severe in only 4.5%. No one in the study progressed to ALS or any other diagnosis. (It is not clear if that would be the case in persons who had not held the diagnosis for at least 5 years.) One case report (Rowin et al., 2001) suggests progression of monomelic amyotrophy after a period of 31 years of stability. One might hypothesize that progression in this case is due to aging and death of surviving anterior horn cells, much as has been proposed in post polio syndrome. Copyright 2003 AAPM&R Page 7 of 9
8 Monomelic amyotrophy, when first noted in the literature in 1959 (Hirayama et al., 1959), was called "juvenile muscular atrophy of the unilateral upper extremity," and the term, in its general use, refers to upper extremity involvement. There have been descriptions of a few cases of monomelic amyotrophy of the lower limb (Uncini et al., 1992); however, it is a less well-defined entity than monomelic amyotrophy affecting the upper limb(s). Only a few cases have been described overall. From the cases described, onset is more variable, having been noted to be from Anatomical abnormalities such as pes cavus may be associated. There is evidence of a diffuse, subclinical anterior horn cell involvement in all four limbs. Disease course has not been well-described. The majority of cases reported in the literature are sporadic. Gucuyener et al. (1991) report a case of affected siblings. No further diagnostic procedures are indicated at this time. Observation of this patient over the next 1-2 years will solidify the diagnosis. Additional studies that might have been done as a point of interest include needle examination of the brachioradialis and ECR, which are reported to be spared in a significant number of cases of monomelic amyotrophy (Orvema et al., 1990). Autonomic testing would also be of interest in this patient as there have been studies documenting involvement of the autonomic nervous system in monomelic amyotrophy. In a study of sympathetic skin responses of 9 patients and 25 controls (Gourie-Devi et al., 2001), sympathetic skin response (activation of sweat glands) was prolonged in the 9 patients relative to the controls, and the response was seen in both upper limbs. Treatment There is no treatment for monomelic amyotrophy. Observation over time is warranted. Progression generally stops in 1-2 years though may go on for up to 5 years in rare cases. Patients who have carried a diagnosis of monomelic amyotrophy for 5 years may be reassured that they will not progress to more serious diseases with poor prognosis such as ALS. Patients generally will stabilize with mild to moderate physical impairment in one upper limb with occasional minor impairment in the contralateral upper limb. Progression to lower limbs should not occur. Bibliography 1. Donofrio PD. AAEM case report #28: monomelic amyotrophy. Muscle Nerve 1994;17: Gourie-Devi M, Nalini A. Sympathetic skin response in monomelic amyotrophy. Acta Neurol Scand 2001;104: Gourie-Devi M, Nalini A. Long-term follow-up of 44 patients with brachial monomelic amyotrophy. Acta Neurol Scand 2003;107: Copyright 2003 AAPM&R Page 8 of 9
9 4. Gucuyener K, Aysun S, Topaloglu H, Inan L, Varli K. Monomelic amyotrophy in siblings. Pediatr Neurol 1991;7(3): Hirayama K, et al. Juvenile muscular atrophy of unilateral upper extremity. Pyschiat Neurol Jap 1959;61: Hirayama K, et al. Juvenile muscular atrophy of unilateral upper extremity. Neurology 1963;13: Hirayama K, Tomonaga M, Kitano K, Yamada T, Kojima S, Arai K. Focal cervical poliopathy causing juvenile muscular atrophy of the distal upper extremity: a pathological study. J of Neurol Neurosurg Psychiatry 1987;50: Oryema J, Ashby P, Spiegel S. Monomelic amyotrophy. Can J Neur Sci 1990;17: Rowin J, Meriggioli MN, Cochran EJ. Monomelic amyotrophy with late progression. Neuromuscul Disord 2001;11: Uncini A, Servidei S, Delli Pizzi C, Cutarella R, Di Muzio A, Gambi D, Tonali P. Benign monomelic amyotrophy of lower limb: report of three cases. Acta Neurol Scand 1992;85: Copyright 2003 AAPM&R Page 9 of 9
Differential Diagnosis of Neuropathies and Compression. Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre
 Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
A/Professor Arun Aggarwal Balmain Hospital
 A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
Making sense of Nerve conduction & EMG
 Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Two Cases of Benign Monomelic Amyotrophy of the Lower Extremities
 Journal of the K. S. C. N. Vol. 2, No. 2 Two Cases of Benign Monomelic Amyotrophy of the Lower Extremities Dong Kuck Lee, M.D. Department of Neurology, School of Medicine, Catholic University of Daegu
Journal of the K. S. C. N. Vol. 2, No. 2 Two Cases of Benign Monomelic Amyotrophy of the Lower Extremities Dong Kuck Lee, M.D. Department of Neurology, School of Medicine, Catholic University of Daegu
Nerve Conduction Studies and EMG
 Nerve Conduction Studies and EMG Limitations of other methods of investigations of the neuromuscular system - Dr Rob Henderson, Neurologist Assessment of Weakness Thanks Peter Silburn PERIPHERAL NEUROPATHY
Nerve Conduction Studies and EMG Limitations of other methods of investigations of the neuromuscular system - Dr Rob Henderson, Neurologist Assessment of Weakness Thanks Peter Silburn PERIPHERAL NEUROPATHY
Index. Note: Page numbers of article titles are in boldface type.
 Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
June 1996 EMG Case-of-the-Month
 June 1996 EMG Case-of-the-Month This case is no longer available for CME credit. Cases prepared by: Ian MacLean, MD; Daniel Dumitru, MD; Lawrence R. Robinson, MD HISTORY Six weeks ago a 28-year-old woman
June 1996 EMG Case-of-the-Month This case is no longer available for CME credit. Cases prepared by: Ian MacLean, MD; Daniel Dumitru, MD; Lawrence R. Robinson, MD HISTORY Six weeks ago a 28-year-old woman
Distal chronic spinal muscular atrophy involving the hands
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Electrodiagnostics for Back & Neck Pain. Steven Andersen, MD Providence Physiatry Clinic
 Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
AANEM Case Study: Hirayama s Disease. Children s National Health System George Washington University
 AANEM Case Study: Hirayama s Disease Author Information Full Name: Luca Bartolini, MD and Perry K. ichardson, MD Affiliation: Children s National Health System George Washington University No one involved
AANEM Case Study: Hirayama s Disease Author Information Full Name: Luca Bartolini, MD and Perry K. ichardson, MD Affiliation: Children s National Health System George Washington University No one involved
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment
 Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Abnormal EMG Patterns in Disease. Amanda C. Peltier, MD MS October 12, 2013
 Abnormal EMG Patterns in Disease Amanda C. Peltier, MD MS October 12, 2013 Disclosures I have no financial relationships to disclose that are relative to the content of my presentation. Basic Tenets of
Abnormal EMG Patterns in Disease Amanda C. Peltier, MD MS October 12, 2013 Disclosures I have no financial relationships to disclose that are relative to the content of my presentation. Basic Tenets of
A Tale of Five Demyelinating Neuropathies
 Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Lumbosacral plexus lesion Lumbosacral plexus disorders G54.1 Neuralgic amyotrophy Neuralgic amyotrophy G
 ICD-9-CM and ICD-10-CM NEUROMUSCULAR DIAGNOSIS CODES Focal Neuropathy ICD-9-CM ICD-10-CM Mononeuropathy G56.00 Carpal tunnel syndrome 354.00 Other median nerve lesion 354.10 Lesion of ulnar nerve 354.20
ICD-9-CM and ICD-10-CM NEUROMUSCULAR DIAGNOSIS CODES Focal Neuropathy ICD-9-CM ICD-10-CM Mononeuropathy G56.00 Carpal tunnel syndrome 354.00 Other median nerve lesion 354.10 Lesion of ulnar nerve 354.20
FOUR CASES OF CLASSICAL HIRAYAMA DISEASE WITH DIFFERENT STAGES OF EVOLUTION Venkatesan Nagarajan 1, Rajesh Venkat I 2, Mahesh I 3, Muthuraj k 4
 FOUR CASES OF CLASSICAL HIRAYAMA DISEASE WITH DIFFERENT STAGES OF EVOLUTION Venkatesan Nagarajan 1, Rajesh Venkat I 2, Mahesh I 3, Muthuraj k 4 HOW TO CITE THIS ARTICLE: Venkatesan Nagarajan, Rajesh Venkat
FOUR CASES OF CLASSICAL HIRAYAMA DISEASE WITH DIFFERENT STAGES OF EVOLUTION Venkatesan Nagarajan 1, Rajesh Venkat I 2, Mahesh I 3, Muthuraj k 4 HOW TO CITE THIS ARTICLE: Venkatesan Nagarajan, Rajesh Venkat
For convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables.
 Case tudy 8 or convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables. History: 60 year-ol man with a history of left hand weakness
Case tudy 8 or convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables. History: 60 year-ol man with a history of left hand weakness
CIDP + MMN - how to diagnose and treat. Dr Hadi Manji
 CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
JMSCR Vol 06 Issue 04 Page April 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i4.78 Electrophysiological Characteristics
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i4.78 Electrophysiological Characteristics
Case 3. Your Diagnosis?
 Case 3 45 year-old presenting with a history of injury to the right shoulder whilst working in the freezing work. He was loading a sheep over an incline with his arm around the sheep. He felt pain in the
Case 3 45 year-old presenting with a history of injury to the right shoulder whilst working in the freezing work. He was loading a sheep over an incline with his arm around the sheep. He felt pain in the
Assessment of the Brachial Plexus EMG Course CNSF Halifax Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University
 Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
Benign monomelic amyotrophy in a 7-year-old girl with proximal upper limb involvement: case report
 The Turkish Journal of Pediatrics 2011; 53: 471-476 Case Report Benign monomelic amyotrophy in a 7-year-old girl with proximal upper limb involvement: case report Öznur Yılmaz 1, İpek Alemdaroğlu 1, Ayşe
The Turkish Journal of Pediatrics 2011; 53: 471-476 Case Report Benign monomelic amyotrophy in a 7-year-old girl with proximal upper limb involvement: case report Öznur Yılmaz 1, İpek Alemdaroğlu 1, Ayşe
Tung Henry Tang, DO and Bryan Tsao, MD American Association of Neuromuscular and Electrodiagnostic Medicine 2621 Superior Dr NW Rochester, MN 55901
 Right Upper Extrem mity Pain and Weakness Tung Henry Tang, DO and Bryan Tsao, MD No one involved in the planning of this CME activity have anyy relevant financial relationships to disclose. Authors/faculty
Right Upper Extrem mity Pain and Weakness Tung Henry Tang, DO and Bryan Tsao, MD No one involved in the planning of this CME activity have anyy relevant financial relationships to disclose. Authors/faculty
Neurophysiological Diagnosis of Birth Brachial Plexus Palsy. Dr Grace Ng Department of Paed PMH
 Neurophysiological Diagnosis of Birth Brachial Plexus Palsy Dr Grace Ng Department of Paed PMH Brachial Plexus Anatomy Brachial Plexus Cords Medial cord: motor and sensory conduction for median and ulnar
Neurophysiological Diagnosis of Birth Brachial Plexus Palsy Dr Grace Ng Department of Paed PMH Brachial Plexus Anatomy Brachial Plexus Cords Medial cord: motor and sensory conduction for median and ulnar
Case Example. Nerve Entrapments in the Lower limb
 Nerve Entrapments in the Lower limb February, 2013 William S. Pease, M.D. Ernest W. Johnson Professor of PM&R Case Example CC: Right ankle dorsiflexion weakness with minimal paresthesias HPI: 87 year-old
Nerve Entrapments in the Lower limb February, 2013 William S. Pease, M.D. Ernest W. Johnson Professor of PM&R Case Example CC: Right ankle dorsiflexion weakness with minimal paresthesias HPI: 87 year-old
Central motor conduction in brachial monomelic amyotrophy
 Original Article Central motor conduction in brachial monomelic amyotrophy Pramod K. Pal, Nalini Atchayaram, Gaurav Goel 1, Ebenezer Beulah Departments of Neurology and 1 Neuroimaging and Interventional
Original Article Central motor conduction in brachial monomelic amyotrophy Pramod K. Pal, Nalini Atchayaram, Gaurav Goel 1, Ebenezer Beulah Departments of Neurology and 1 Neuroimaging and Interventional
Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype Five Years after Initial Diagnosis
 Case Reports in Neurological Medicine Volume 2013, Article ID 356157, 4 pages http://dx.doi.org/10.1155/2013/356157 Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype
Case Reports in Neurological Medicine Volume 2013, Article ID 356157, 4 pages http://dx.doi.org/10.1155/2013/356157 Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype
Electrophysiology of Brachial and Lumbosacral Plexopathies
 18 Electrophysiology of Brachial and Lumbosacral Plexopathies Juan A. Acosta and Elizabeth M. Raynor Summary Brachial and lumbosacral plexopathies represent a heterogeneous group of disorders including
18 Electrophysiology of Brachial and Lumbosacral Plexopathies Juan A. Acosta and Elizabeth M. Raynor Summary Brachial and lumbosacral plexopathies represent a heterogeneous group of disorders including
Disclosure. Entrapment Neuropathies - Overview. Common mononeuropathy sites. Definitions. Common mononeuropathy sites. Common mononeuropathy sites
 Disclosure Entrapment Neuropathies - Overview I receive compensation from Wiley- Blackwell publishers for my work as Editor-in-Chief of Muscle & Nerve Lawrence H. Phillips, II, MD Definitions Mononeuropathy:
Disclosure Entrapment Neuropathies - Overview I receive compensation from Wiley- Blackwell publishers for my work as Editor-in-Chief of Muscle & Nerve Lawrence H. Phillips, II, MD Definitions Mononeuropathy:
High Yield Neurological Examination
 High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
MOTOR NEURONE DISEASE
 MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
EDX in Myopathies Limitations. EDX in Myopathies Utility Causes of Myopathy. Myopathy: Issues for Electromyographers
 Electrodiagnostic Assessment of Myopathy Myopathy: Issues for Electromyographers Often perceived as challenging Ian Grant Division of Neurology QEII Health Sciences Centre Halifax NS CNSF EMG Course June
Electrodiagnostic Assessment of Myopathy Myopathy: Issues for Electromyographers Often perceived as challenging Ian Grant Division of Neurology QEII Health Sciences Centre Halifax NS CNSF EMG Course June
Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment
 Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment 11 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, LH Van den Berg
Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment 11 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, LH Van den Berg
Arm Pain, Numbness, and Tingling: Etiologies and Treatment
 Arm Pain, Numbness, and Tingling: Etiologies and Treatment Steve Fowler MD Confluence Health Department of Physiatry Education Medical School: University of Utah Residency: Mayo Clinic Work Confluence
Arm Pain, Numbness, and Tingling: Etiologies and Treatment Steve Fowler MD Confluence Health Department of Physiatry Education Medical School: University of Utah Residency: Mayo Clinic Work Confluence
Peripheral Nerve Injuries of the Upper Limb.
 Peripheral Nerve Injuries of the Upper Limb www.fisiokinesiterapia.biz Definitions Radiculopathy Process affecting the nerve root, most commonly by a herniated disc Weakness in muscles supplied by the
Peripheral Nerve Injuries of the Upper Limb www.fisiokinesiterapia.biz Definitions Radiculopathy Process affecting the nerve root, most commonly by a herniated disc Weakness in muscles supplied by the
The Internist s Approach to Neuropathy
 The Internist s Approach to Neuropathy VOLKAN GRANIT, MD, MSC ASSISTANT PROFESSOR OF NEUROLOGY NEUROMUSCU LAR DIVISION UNIVERSITY OF MIAMI, MILLER SCHOOL OF MEDICINE RELEVANT DECLARATIONS Financial disclosures:
The Internist s Approach to Neuropathy VOLKAN GRANIT, MD, MSC ASSISTANT PROFESSOR OF NEUROLOGY NEUROMUSCU LAR DIVISION UNIVERSITY OF MIAMI, MILLER SCHOOL OF MEDICINE RELEVANT DECLARATIONS Financial disclosures:
3/17/2015. Amyotrophic lateral sclerosis Nerve conduction studies/electromyography Differential diagnosis Other motor neuron syndromes
 B. Jane Distad, MD Associate Professor Department of Neurology 2015 Amyotrophic lateral sclerosis Nerve conduction studies/electromyography Differential diagnosis Other motor neuron syndromes Spinal muscular
B. Jane Distad, MD Associate Professor Department of Neurology 2015 Amyotrophic lateral sclerosis Nerve conduction studies/electromyography Differential diagnosis Other motor neuron syndromes Spinal muscular
Title. CitationInternal Medicine, 46(8): Issue Date Doc URL. Type. File Information
 Title Scapular Winging as a Symptom of Cervical Flexion My Author(s)Yaguchi, Hiroaki; Takahashi, Ikuko; Tashiro, Jun; Ts CitationInternal Medicine, 46(8): 511-514 Issue Date 2007-04-17 Doc URL http://hdl.handle.net/2115/20467
Title Scapular Winging as a Symptom of Cervical Flexion My Author(s)Yaguchi, Hiroaki; Takahashi, Ikuko; Tashiro, Jun; Ts CitationInternal Medicine, 46(8): 511-514 Issue Date 2007-04-17 Doc URL http://hdl.handle.net/2115/20467
Motor and sensory nerve conduction studies
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
Brachial Plexopathy in a Division I Football Player
 www.fisiokinesiterapia.biz Brachial Plexopathy in a Division I Football Player Brachial Plexus Injuries in Sport Typically a transient neurapraxia - 70% of injured players said they did not always report
www.fisiokinesiterapia.biz Brachial Plexopathy in a Division I Football Player Brachial Plexus Injuries in Sport Typically a transient neurapraxia - 70% of injured players said they did not always report
A Hypothesis Driven Approach to the Neurological Exam
 A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
Nerve Site Latency ms Amplitude mv Distance mm Conduction Velocity m/s
 Clinical Electrophysiology Instructions and Sample Reports NCS/EMG REPORT Date: August 2007 Reason for Electrophysiologic Referral: Bilateral upper extremity pain and numbness. History: 59 year-old female
Clinical Electrophysiology Instructions and Sample Reports NCS/EMG REPORT Date: August 2007 Reason for Electrophysiologic Referral: Bilateral upper extremity pain and numbness. History: 59 year-old female
Evaluation of Tingling and Numbness in the Upper Extremities
 Evaluation of Tingling and Numbness in the Upper Extremities DR. W. ANTHONY FRISELLA M.D. ADVANCED BONE & JOINT, ST CHARLES MO MONA 2018 Overview Polyneuropathy Compressive nerve lesions Carpal tunnel
Evaluation of Tingling and Numbness in the Upper Extremities DR. W. ANTHONY FRISELLA M.D. ADVANCED BONE & JOINT, ST CHARLES MO MONA 2018 Overview Polyneuropathy Compressive nerve lesions Carpal tunnel
Clinical and Neurophysiological Assessment of Cervical Radiculopathy
 Mohamed El-Khatib et al. Clinical and Neurophysiological Assessment of Cervical Radiculopathy Mohamed G. El-Khatib 1, Mohamed Saad 1, Seyam Saeed 2, Mohamed El-Sayed 1 Departments of Neurology, Mansoura
Mohamed El-Khatib et al. Clinical and Neurophysiological Assessment of Cervical Radiculopathy Mohamed G. El-Khatib 1, Mohamed Saad 1, Seyam Saeed 2, Mohamed El-Sayed 1 Departments of Neurology, Mansoura
Clinical Aspects of Peripheral Nerve and Muscle Disease. Roy Weller Clinical Neurosciences University of Southampton School of Medicine
 Clinical Aspects of Peripheral Nerve and Muscle Disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Nerves 1. Anterior Horn Cell 2. Dorsal root ganglion cell 3.
Clinical Aspects of Peripheral Nerve and Muscle Disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Nerves 1. Anterior Horn Cell 2. Dorsal root ganglion cell 3.
A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017
 A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017 Disclosures Research support from Cytokinetics, Inc Catalyst, Inc Editorial fees from UptoDate. Objectives Describe
A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017 Disclosures Research support from Cytokinetics, Inc Catalyst, Inc Editorial fees from UptoDate. Objectives Describe
Table 1: Nerve Conduction Studies (summarised)
 Table 1: Nerve Conduction Studies (summarised) Sensory nerve conduction 1 week* 3 months Superficial radial sensory Normal, symmetric SNAP and CV No change Median to digit II Normal, symmetric SNAP and
Table 1: Nerve Conduction Studies (summarised) Sensory nerve conduction 1 week* 3 months Superficial radial sensory Normal, symmetric SNAP and CV No change Median to digit II Normal, symmetric SNAP and
What can neuromuscular ultrasound do for you? 2017 Gloor Lecture
 What can neuromuscular ultrasound do for you? 2017 Gloor Lecture Dr. Nens van Alfen, neurologist/clinical neurophysiologist Radboud university medical center Nijmegen, The Netherlands Learning objectives
What can neuromuscular ultrasound do for you? 2017 Gloor Lecture Dr. Nens van Alfen, neurologist/clinical neurophysiologist Radboud university medical center Nijmegen, The Netherlands Learning objectives
CNS & PNS Entrapment. Disclosure - Nothing
 Peripheral Nerve Entrapments That Mimic Spinal Pathology: Evaluation And Treatment Both Medical And Surgical Michel Kliot MD Clinical Professor UCSF Department of NeuroSurgery Director Center For Evaluation
Peripheral Nerve Entrapments That Mimic Spinal Pathology: Evaluation And Treatment Both Medical And Surgical Michel Kliot MD Clinical Professor UCSF Department of NeuroSurgery Director Center For Evaluation
Brachial Neuritis: An Uncommon Cause of Shoulder Pain
 Brachial Neuritis: An Uncommon Cause of Shoulder Pain ROBERT G. HOSEY, MD; RICHARD E. RODENBERG, MD Brachial neuritis, an uncommon idiopathic syndrome, should be considered in the differential diagnosis
Brachial Neuritis: An Uncommon Cause of Shoulder Pain ROBERT G. HOSEY, MD; RICHARD E. RODENBERG, MD Brachial neuritis, an uncommon idiopathic syndrome, should be considered in the differential diagnosis
Peripheral Neuropathies
 Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
Spinal nerves. Aygul Shafigullina. Department of Morphology and General Pathology
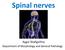 Spinal nerves Aygul Shafigullina Department of Morphology and General Pathology Spinal nerve a mixed nerve, formed in the vicinity of an intervertebral foramen, where fuse a dorsal root and a ventral root,
Spinal nerves Aygul Shafigullina Department of Morphology and General Pathology Spinal nerve a mixed nerve, formed in the vicinity of an intervertebral foramen, where fuse a dorsal root and a ventral root,
DIAGNOSIS OF DIABETIC NEUROPATHY
 DIAGNOSIS OF DIABETIC NEUROPATHY Dept of PM&R, College of Medicine, Korea University Dong Hwee Kim Electrodiagnosis ANS Clinical Measures QST DIAGRAM OF CASUAL PATHWAYS TO FOOT ULCERATION Rathur & Boulton.
DIAGNOSIS OF DIABETIC NEUROPATHY Dept of PM&R, College of Medicine, Korea University Dong Hwee Kim Electrodiagnosis ANS Clinical Measures QST DIAGRAM OF CASUAL PATHWAYS TO FOOT ULCERATION Rathur & Boulton.
Mononeuropathies of the Upper and Lower Extremity
 15 Mononeuropathies of the Upper and Lower Extremity Kevin R. Scott and Milind J. Kothari Summary Nerves of both the upper and lower extremities are frequently injured for a variety of reasons. In the
15 Mononeuropathies of the Upper and Lower Extremity Kevin R. Scott and Milind J. Kothari Summary Nerves of both the upper and lower extremities are frequently injured for a variety of reasons. In the
LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES
 Neurology DOI: 10.15386/cjmed-382 LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES ANA MARIA GALAMB, IOAN DAN MINEA Department of Medical and Surgical Specialities, Faculty of Medicine,
Neurology DOI: 10.15386/cjmed-382 LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES ANA MARIA GALAMB, IOAN DAN MINEA Department of Medical and Surgical Specialities, Faculty of Medicine,
Patogenesi e terapia della Neuropatia Motoria Multifocale
 26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi. E. mail:
 Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
Nerves of the upper limb Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Brachial plexus Median nerve After originating from the brachial plexus in the axilla,
sensory nerves, motor nerves, autonomic nerves
 damage or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health, depending on the type of nerve affected o chronic: long term, begins subtly
damage or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health, depending on the type of nerve affected o chronic: long term, begins subtly
The AANEM is accredited by the Accreditation Council for Continuing Medical Education (ACCME) to provide continuing medical education for physicians.
 The AANEM is accredited by the Accreditation Council for Continuing Medical Education (ACCME) to provide continuing medical education for physicians. The AANEM designates this live activity for a maximum
The AANEM is accredited by the Accreditation Council for Continuing Medical Education (ACCME) to provide continuing medical education for physicians. The AANEM designates this live activity for a maximum
Electrophysiological differences between Hirayama disease, amyotrophic lateral sclerosis and cervical spondylotic amyotrophy
 Jin et al. BMC Musculoskeletal Disorders 2014, 15:349 RESEARCH ARTICLE Open Access Electrophysiological differences between Hirayama disease, amyotrophic lateral sclerosis and cervical spondylotic amyotrophy
Jin et al. BMC Musculoskeletal Disorders 2014, 15:349 RESEARCH ARTICLE Open Access Electrophysiological differences between Hirayama disease, amyotrophic lateral sclerosis and cervical spondylotic amyotrophy
Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes
 Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes 1 This lab involves the second section of the exercise Spinal Cord, Spinal Nerves, and the Autonomic Nervous System,
Human Anatomy and Physiology I Laboratory Spinal and Peripheral Nerves and Reflexes 1 This lab involves the second section of the exercise Spinal Cord, Spinal Nerves, and the Autonomic Nervous System,
Management of Brachial Plexus & Peripheral Nerves Blast Injuries. First Global Conflict Medicine Congress
 Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD
 Numb Toes Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD No one involved in the planning of this CME activity have anyy relevant financial relationships to disclose. Authors/faculty have nothingg
Numb Toes Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD No one involved in the planning of this CME activity have anyy relevant financial relationships to disclose. Authors/faculty have nothingg
Introduction and aims of the study
 Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Nerve Injury. 1) Upper Lesions of the Brachial Plexus called Erb- Duchene Palsy or syndrome.
 Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
Nerve Injury - Every nerve goes to muscle or skin so if the nerve is injured this will cause paralysis in the muscle supplied from that nerve (paralysis means loss of function) then other muscles and other
 Nerve Compression Syndromes Median Nerve Carpal Tunnel Syndrome Pronator Syndrome Ulnar Nerve Cubital Tunnel Syndrome Ulnar Tunnel Syndrome TOS www.fisiokinesiterapia.biz Carpal Tunnel Syndrome (CTS) Definition
Nerve Compression Syndromes Median Nerve Carpal Tunnel Syndrome Pronator Syndrome Ulnar Nerve Cubital Tunnel Syndrome Ulnar Tunnel Syndrome TOS www.fisiokinesiterapia.biz Carpal Tunnel Syndrome (CTS) Definition
Lab Activity 13. Spinal Cord. Portland Community College BI 232
 Lab Activity 13 Spinal Cord Portland Community College BI 232 Definitions Tracts: collections of axons in CNS Nerves:collections of axons in PNS Ganglia: collections of neuron cell bodies in PNS Nucleus
Lab Activity 13 Spinal Cord Portland Community College BI 232 Definitions Tracts: collections of axons in CNS Nerves:collections of axons in PNS Ganglia: collections of neuron cell bodies in PNS Nucleus
Treatment of multifocal motor neuropathy with interferon-β1a
 Treatment of multifocal motor neuropathy with interferon-β1a 12 MMN RM Van den Berg-Vos, LH Van den Berg, H Franssen, PA Van Doorn, ISJ Martina, JHJ Wokke Adapted from Neurology 2000; 54: 1518-1521. Chapter
Treatment of multifocal motor neuropathy with interferon-β1a 12 MMN RM Van den Berg-Vos, LH Van den Berg, H Franssen, PA Van Doorn, ISJ Martina, JHJ Wokke Adapted from Neurology 2000; 54: 1518-1521. Chapter
Peripheral neuropathy (PN)
 Peripheral neuropathy (PN) damage or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health, depending on the type of nerve affected o chronic:
Peripheral neuropathy (PN) damage or disease affecting nerves, which may impair sensation, movement, gland or organ function, or other aspects of health, depending on the type of nerve affected o chronic:
Slide 1. Slide 2. Slide 3. Intro to Physical Therapy for Neuromuscular Conditions. PT Evaluation. PT Evaluation
 Slide 1 Intro to Physical Therapy for Neuromuscular Conditions PTA 103 Introduction to Clinical Practice 2 Slide 2 Mental status: consciousness, attention, orientation, cognition Communication: speech
Slide 1 Intro to Physical Therapy for Neuromuscular Conditions PTA 103 Introduction to Clinical Practice 2 Slide 2 Mental status: consciousness, attention, orientation, cognition Communication: speech
PREFACE INTRODUCTION TO THE EMG TRAINING PROGRAM MANUAL
 PREFACE Welcome to the Electromyography Laboratory (EMG) and the Neuromuscular Program. In the following months you will be exposed to the anatomic, physiologic, clinical, and technical information necessary
PREFACE Welcome to the Electromyography Laboratory (EMG) and the Neuromuscular Program. In the following months you will be exposed to the anatomic, physiologic, clinical, and technical information necessary
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2014;38(1):109-115 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.109 Annals of Rehabilitation Medicine Sonographic Evaluation of the Peripheral Nerves
Case Report Ann Rehabil Med 2014;38(1):109-115 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.109 Annals of Rehabilitation Medicine Sonographic Evaluation of the Peripheral Nerves
Acute Cervical Motor Radiculopathy Induced by Neck and Limb Immobilization in a Patient with Parkinson Disease
 CASE REPORT Acute Cervical Motor Radiculopathy Induced by Neck and Limb Immobilization in a Patient with Parkinson Disease Toshio Shimizu, Tetsuo Komori and Hideaki Hayashi Abstract A 68-year-old woman
CASE REPORT Acute Cervical Motor Radiculopathy Induced by Neck and Limb Immobilization in a Patient with Parkinson Disease Toshio Shimizu, Tetsuo Komori and Hideaki Hayashi Abstract A 68-year-old woman
Evaluation of Peripheral Neuropathy. Evaluation of Peripheral Neuropathy - Introduction
 Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
Nerve Conduction Studies NCS
 Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
UltraEMG Course Schedule 2015
 Ultra EMG February 20-25 Manchester Grand Hyatt San Diego, California Thursday February 19 Travel Date 5:00-6:00 Registration UltraEMG Course Schedule 2015 UltraEMG-MSK (Musculoskeletal Emphasis) Friday,
Ultra EMG February 20-25 Manchester Grand Hyatt San Diego, California Thursday February 19 Travel Date 5:00-6:00 Registration UltraEMG Course Schedule 2015 UltraEMG-MSK (Musculoskeletal Emphasis) Friday,
Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve Action Potential in Common Peroneal Neuropathy
 J Korean Med Sci 2008; 23: 117-21 ISSN 1011-8934 DOI: 10.3346/jkms.2008.23.1.117 Copyright The Korean Academy of Medical Sciences Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve
J Korean Med Sci 2008; 23: 117-21 ISSN 1011-8934 DOI: 10.3346/jkms.2008.23.1.117 Copyright The Korean Academy of Medical Sciences Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve
Cervical Radiculopathy: My 32 Year-Old Cyclist is Nervous What do I do on the initial visit?
 Cervical Radiculopathy: My 32 Year-Old Cyclist is Nervous What do I do on the initial visit? Scott D Boden, MD The Emory Spine Center Atlanta, Georgia History of Trauma? 2 History of Trauma? 3 Sometimes
Cervical Radiculopathy: My 32 Year-Old Cyclist is Nervous What do I do on the initial visit? Scott D Boden, MD The Emory Spine Center Atlanta, Georgia History of Trauma? 2 History of Trauma? 3 Sometimes
An Illustrated Guide For Peripheral Nerve Examination. Bedside Teaching for 2 nd year medical Students
 An Illustrated Guide For Peripheral Nerve Examination Bedside Teaching for 2 nd year medical Students Prepared by: Dr. Farid Ghalli Clinical Teacher (Hon) November 2016 Before Examination : Wash hands
An Illustrated Guide For Peripheral Nerve Examination Bedside Teaching for 2 nd year medical Students Prepared by: Dr. Farid Ghalli Clinical Teacher (Hon) November 2016 Before Examination : Wash hands
Mononeuropathies: A Practical Approach to Diagnosis and Treatment. Dr. Simran Singh Basi MD, FRCPC, CSCN Diplomate (EMG) February 28, 2018
 Mononeuropathies: A Practical Approach to Diagnosis and Treatment Dr. Simran Singh Basi MD, FRCPC, CSCN Diplomate (EMG) February 28, 2018 Faculty/Presenter Disclosure Faculty: Dr. Simran Singh Basi Relationships
Mononeuropathies: A Practical Approach to Diagnosis and Treatment Dr. Simran Singh Basi MD, FRCPC, CSCN Diplomate (EMG) February 28, 2018 Faculty/Presenter Disclosure Faculty: Dr. Simran Singh Basi Relationships
American Board of Physical Medicine & Rehabilitation. Part I Curriculum & Weights
 American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
UK practice for electrodiagnosis of MND Review of literature and background
 UK practice for electrodiagnosis of MND Review of literature and background UK practice for electrodiagnosis of MND Review of literature and background EMG Group Mark Baker Stephan Jaiser Stuart Viegas
UK practice for electrodiagnosis of MND Review of literature and background UK practice for electrodiagnosis of MND Review of literature and background EMG Group Mark Baker Stephan Jaiser Stuart Viegas
Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature Review
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 2 Number 1 Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature D Reichner, G Evans Citation D Reichner,
ISPUB.COM The Internet Journal of Plastic Surgery Volume 2 Number 1 Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature D Reichner, G Evans Citation D Reichner,
Ahmed Abbas, Mark Cook, Liong Hiew Fu, Alistair Lewthwaite, Colin Shirley, Yusuf A. Rajabally
 2016, Elsevier. Licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International http://creativecommons.org/licenses/by-nc-nd/4.0/ Accepted Manuscript A case of POEMS mimicking
2016, Elsevier. Licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International http://creativecommons.org/licenses/by-nc-nd/4.0/ Accepted Manuscript A case of POEMS mimicking
Year 2 MBChB Clinical Skills Session Examination of the Motor System
 Year 2 MBChB Clinical Skills Session Examination of the Motor System Reviewed & ratified by: o o o o Dr D Smith Consultant Neurologist Dr R Davies Consultant Neurologist Dr B Michael Neurology Clinical
Year 2 MBChB Clinical Skills Session Examination of the Motor System Reviewed & ratified by: o o o o Dr D Smith Consultant Neurologist Dr R Davies Consultant Neurologist Dr B Michael Neurology Clinical
Part 1: Communication between CNS & PNS
 Ch. 6: Peripheral Nervous System Objectives: 1. Communication between CNS & PNS: afferent (sensory) pathway versus efferent (motor) pathway of information. 2. Regulation of somatic (voluntary) motor system
Ch. 6: Peripheral Nervous System Objectives: 1. Communication between CNS & PNS: afferent (sensory) pathway versus efferent (motor) pathway of information. 2. Regulation of somatic (voluntary) motor system
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM. Andrzej Sladkowski
 Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases
 Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Median-ulnar nerve communications and carpal tunnel syndrome
 Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 982-986 Median-ulnar nerve communications and carpal tunnel syndrome LUDWIG GUTMANN From the Department of Neurology, West Virginia University,
Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 982-986 Median-ulnar nerve communications and carpal tunnel syndrome LUDWIG GUTMANN From the Department of Neurology, West Virginia University,
November 16-18, 2017 Hotel Monteleone New Orleans, LA. Provided by
 November 16-18, 2017 Hotel Monteleone New Orleans, LA Provided by Diabetic Neuropathy: A Global and Growing Problem John D. England, MD Louisiana State University Health Sciences Center School of Medicine
November 16-18, 2017 Hotel Monteleone New Orleans, LA Provided by Diabetic Neuropathy: A Global and Growing Problem John D. England, MD Louisiana State University Health Sciences Center School of Medicine
Conventional needle electromyography
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 5 Electromyography: Surface, needle conventional and single fiber - Level 1-2 Conventional
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 5 Electromyography: Surface, needle conventional and single fiber - Level 1-2 Conventional
International Journal of Ayurveda and Pharmaceutical Chemistry
 International Journal of Ayurveda and Pharmaceutical Chemistry Volume 7 Issue 2 2017 www.ijapc.com Managed by Green m RESEARCH ARTICLE www.ijapc.com e-issn 2350-0204 Role of an Advanced Diagnostic Technique
International Journal of Ayurveda and Pharmaceutical Chemistry Volume 7 Issue 2 2017 www.ijapc.com Managed by Green m RESEARCH ARTICLE www.ijapc.com e-issn 2350-0204 Role of an Advanced Diagnostic Technique
How to Think like a Neurologist Review of Exam Process and Assessment Findings
 Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
AII-type: Select the most appropriate answer
 AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
BEFORE THE ALASKA OFFICE OF ADMINISTRATIVE HEARINGS ON REFERRAL BY THE COMMISSIONER OF HEALTH AND SOCIAL SERVICES FAIR HEARING DECISION
 BEFORE THE ALASKA OFFICE OF ADMINISTRATIVE HEARINGS ON REFERRAL BY THE COMMISSIONER OF HEALTH AND SOCIAL SERVICES In the Matter of ) ) OAH No. 13-0689-APA T S ) Division No. ) I. Introduction FAIR HEARING
BEFORE THE ALASKA OFFICE OF ADMINISTRATIVE HEARINGS ON REFERRAL BY THE COMMISSIONER OF HEALTH AND SOCIAL SERVICES In the Matter of ) ) OAH No. 13-0689-APA T S ) Division No. ) I. Introduction FAIR HEARING
Nerve Conduction Studies NCS
 Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
Nerve Conduction Studies NCS Nerve conduction studies are an essential part of an EMG examination. The clinical usefulness of NCS in the diagnosis of diffuse and local neuropathies has been thoroughly
Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome
 Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(3): 138-143 Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome Received: 9 Mar 2014 Accepted:
Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(3): 138-143 Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome Received: 9 Mar 2014 Accepted:
Chronic focal polymyositis in the adult
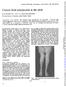 Journal of Neurology, Neurosurgery, and Psychiatry, 1981, 44, 419-425 Chronic focal polymyositis in the adult N E BHARUCHA AND J A MORGAN-HUGHES From the Institute of Neurology, Queen Square, London S
Journal of Neurology, Neurosurgery, and Psychiatry, 1981, 44, 419-425 Chronic focal polymyositis in the adult N E BHARUCHA AND J A MORGAN-HUGHES From the Institute of Neurology, Queen Square, London S
