A novel CaSR mutation presenting as a severe case of neonatal familial hypocalciuric hypercalcemia
|
|
|
- Scott Hunt
- 5 years ago
- Views:
Transcription
1 Tonyushkina et al. International Journal of Pediatric Endocrinology 2012, 2012:13 CASE REPORT Open Access A novel CaSR mutation presenting as a severe case of neonatal familial hypocalciuric hypercalcemia Ksenia N Tonyushkina 1*, Stephen O Connor 2 and Nancy S Dunbar 1 Abstract Background: Familial Hypocalciuric Hypercalcemia (FHH) is a generally benign disorder caused by heterozygous inactivating mutations in the Calcium-Sensing Receptor (CaSR) gene resulting in altered calcium metabolism. Objective: We report a case of unusually severe neonatal FHH due to a novel CaSR gene mutation that presented with perinatal fractures and moderate hypercalcemia. Case overview: A female infant was admitted at 2 weeks of age for suspected non-accidental trauma (NAT). Laboratory testing revealed hypercalcemia (3.08 mmol/l), elevated ipth (20.4 pmol/l) and low urinary calcium clearance (0.0004). Radiographs demonstrated multiple healing metaphyseal and rib fractures and bilateral femoral bowing. The femoral deformity and stage of healing were consistent with prenatal injuries rather than nonaccidental trauma (NAT). Treatment was initiated with cholecalciferol, 400 IU/day, and by 6 weeks of age, ipth levels had decreased into the high-normal range. Follow up radiographs demonstrated marked improvement of bone lesions by 3 months. A CaSR gene mutation study showed heterozygosity for a T>C nucleotide substitution at c.1664 in exon 6, resulting in amino acid change I555T in the extracellular domain consistent with a missense mutation. Her mother does not carry the mutation and the father is unknown. At 18 months of age, the child continues to have relative hyperparathyroidism and moderate hypercalcemia but is otherwise normal. Conclusion: This neonate with intrauterine fractures and demineralization, moderate hypercalcemia and hyperparathyroidism was found to have a novel inactivating missense mutation of the CaSR not detected in her mother. Resolution of bone lesions and reduction of hyperparathyroidism was likely attributable to the natural evolution of the disorder in infancy as well as the mitigating effect of cholecalciferol treatment. Keywords: FHH, Neonatal hyperparathyroidism, Hypercalcemia, NHPT, CaSR, Vit D Introduction Familial hypocalciuric hypercalcemia (FHH) is an autosomal dominant disorder characterized by modestly elevated serum calcium (Ca), inappropriately high parathyroid hormone (PTH) levels and low urinary Ca excretion [1]. FHH is caused by inactivating mutations of the gene encoding the Calcium-Sensing Receptor (CaSR), a seven transmembrane G-protein-coupled receptor. The CaSR is expressed primarily in parathyroid chief cells and renal tubular cells and activates an * Correspondence: Ksenia.Tonyushkina@bhs.org 1 Baystate Children s Hospital, Tufts University School of Medicine, 759 Chestnut St. Dept of Pediatrics, Springfield, MA 01199, USA Full list of author information is available at the end of the article intracellular signaling cascade to maintain serum calcium levels within a narrow range. The gene for the CaSR is located on chromosome 3q and encodes for a 1078 amino acid sequence. Normally, elevated levels of serum calcium activate the CaSR which then inhibits both the secretion of PTH in the parathyroid glands and the reabsorption of Ca 2+ and Mg 2+ in the renal tubules. Therefore an inactivating mutation of the CaSR leads to an elevated set point for serum Ca with the consequence of having both inappropriate secretion of PTH and renal reabsorption of Ca 2+ [2]. The clinical impact of these mutations, at least 250 of which have been reported, is highly variable and ranges from totally asymptomatic to fatal. In the neonatal 2012 Tonyushkina et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
2 Tonyushkina et al. International Journal of Pediatric Endocrinology 2012, 2012:13 Page 2 of 7 period, homozygous inactivating mutations result in neonatal severe hyperparathyroidism (NSHPT) with severe symptomatic hypercalcemia, undermineralized bones, rib cage deformity, and long-bone and rib fractures [3]. This condition requires aggressive medical management often including emergent parathyroidectomy and can be fatal. Neonatal heterozygous inactivating mutations are usually associated with modest hypercalcemia and hyperparathyroidism with mild or absent bone disease which gradually evolves to a more benign FHH phenotype [4-7]. Lastly, heterozygous FHH can go wholly unrecognized for years until elevated serum calcium is noted [8]. Herein, we present the case of a newborn girl with a novel heterozygous inactivating mutation of the CaSR gene, severe hyperparathyroidism, overt skeletal demineralization, and perinatal fractures who was treated with cholecalciferol to moderate her clinical course. Case presentation A full term, healthy infant girl born via a normal spontaneous vaginal delivery presented at 2 weeks of age in a Massachusetts emergency room for evaluation of increased irritability and mild cough. Chest x-ray showed a healing left proximal humeral metaphyseal fracture and bilateral healing ribs fractures (Figure 1) prompting admission for suspicion of NAT. Physical exam She was an alert, well-nourished African-American infant girl whose length was at the 80 th percentile, weight was at the 75 th percentile and head circumference was at the 75 th percentile for age. Exam findings were significant for a prominent forehead and slightly bowed lower Figure 1 Chest radiograph at presentation. There is fragmentation, mixed sclerosis and lucency of the left upper humeral metaphysis and a small amount of subperiosteal new bone formation extending downward along the medial shaft (white arrows). There are expanded healing rib fractures above both CP angles (black arrows). extremities. There was full range of motion of extremities without pain. Labs A markedly elevated intact PTH with mild hypercalcemia and hypermagnesemia were noted on presentation (Table 1). A spot urinary calcium to creatinine clearance ratio was low[9]. After 2 days of hydration with normal saline and low-calcium infant formula (calcium content: <10 mg calcium/100 kcal, Vitamin D 0 IU/oz), serum Ca levels decreased to the high normal range for age (2.8 mmol/l ) (Figure 2). Skeletal survey Bone mineralization was subjectively diminished and there was coarsening of trabecular markings. Repeat CXR with oblique views confirmed multiple healing rib fractures (Figure 1). There was callus formation, flaring, medial beaking and fragmentation of both proximal humeri, the left proximal femur and both distal femurs (Figure 3). There was moderate antero-lateral bowing of both proximal femoral shafts and posterior bowing of the distal femoral shafts with thick confluent subperiosteal new bone formation suggesting advanced stages of healing/remodeling. The femoral bowing deformities and advanced stages of remodeling were consistent with prenatal changes, excluding NAT as a diagnostic consideration. The differential diagnosis included osteogenesis imperfecta and metabolic bone disease. Hospital course The elevated ipth of 20.4 pmol/l with serum calcium of mmol/l led to suspicion of a CaSR mutation. A Sestamibi Tc 99 scan was normal without evidence of adenoma. Lab evaluation of the maternal calcium metabolism was unrevealing (Table 1) and there was no known metabolic bone disease on the maternal side. The infant s father was unknown. Regular formula was restarted (calcium content 67 mg/100kcal, Vitamin D content 12 IU/oz) and cholecalciferol was given at a daily dose of 400 IU daily to suppress PTH [8]. In sum, her total daily vitamin D intake was approximately 600 IU. Follow up course Over the next 18 months, she continued on cholecalciferol and a regular age-appropriate diet. Her length and weight decreased from the 75 th percentile at birth to the th percentile by 6 months of age but then progressed consistently at the 50 th percentile for length and the 25 th percentile for weight. The ipth fell steadily from its peak of 20.4 pmol/l to 4.0 pmol/l by 2 months of age and then settled in the high normal range just under 6 pmol/l. At 12 months of age, the ipth
3 Tonyushkina et al. International Journal of Pediatric Endocrinology 2012, 2012:13 Page 3 of 7 Table 1 Initial biochemical parameters of the infant and mother Lab results Initial Lab Results Infant, 2 wks Infant s mother Ca { mmol/l}; ( mmol/l) Phos { mmol/l}; ( mmol/l) Mg ( mmol/l) 1.05 Cr { mol/l}; ( ) Alkaline Phosphatase { U/L}; ( U/L) 364 Calcium creatinine clearance ratio* ipth ( pmol/l) Vit D 25(OH) ( nmol/l) Vit D 1,25(OH)2 ( pmol/l) Normal adult ranges are given in parenthesis. Normal ranges for infants up to 24 months are given in curly brackets where applicable. *CCCR calcium creatinine clearance ratio = U-calcium/S-calcium/U-creatinine/S-creatinine; calculated with spot urine and serum indices. CCCR <0.02 considered hypocalciuric [9]. increased from 5.9 to 7.8 pmol/l so the cholecalciferol dose was increased to 800 IU/day. Calcium levels remained between 3.1 and 3.3 mmol/l with low calcium/creatinine clearance ratios (Figure 2). Follow-up films of the chest and femurs at age 3 months and again at 1 year showed resolution of metaphyseal deformities and periosteal reaction with improving femoral bowing deformities (Figure 3). Renal ultrasound performed at 1 year was normal without evidence of nephrocalcinosis. At her final appointment before being lost to follow-up at age 19 months, her ipth was 6.6 pmol/l. Genetic evaluation A CaSR gene mutation study (GeneDx DNA diagnostic experts, Gaithersburg, MD) demonstrated heterozygosity for a T>C nucleotide substitution at c.1664 in exon 6, resulting in an amino acid change I555T in the extracellular domain, which replaces an isoleucine with a threonine. This amino acid substitution was predicted by computer modeling performed by GeneDx to be a benign sequence variant although it occurs at a highly conserved region in the CaSR gene [5,10]. The mother s CaSR mutation testing was normal and the father is unknown. Discussion The severity of the clinical picture in this case including intrauterine fractures was unusual. Classical FHH due to a heterozygous loss of function (LOF) mutation of the CaSR can go unrecognized for years and only rarely is diagnosed in the neonatal period. However, heterozygous forms of FHH with overt neonatal bone disease are described in the literature and are typically defined as NHPT [5-7,10]. Possible causes of the more severe phenotype seen in these cases include the specific type of CaSR gene mutation, paternal versus maternal inheritance, prematurity and maternal vitamin D deficiency [4,8]. CaSR mutation type The exact mechanism of how CaSR activation directs intracellular signaling leading to inhibition of PTH secretion and increased reabsorption of calcium in kidneys remains unknown [1]. It is known that the CaSR functions on the cell surface as a homodimer [11]. Inactivation of the CaSR gene can be caused by missense, nonsense and splice site mutations [10]. The latter two types of mutations lead to truncated CaSR proteins lacking transmembrane or intracellular domains. These proteins cannot dimerize with the wild type CaSR proteins. As a result, in the heterozygous state, calcium sensing will be limited to the 50% structurally normal receptors. CaSR proteins affected by missense mutations can dimerize with the wild type CaSR protein but lead to a malfunctioning heterodimer. In rare instances, the missense mutations may exert a dominant negative effect leaving a minority of wild-type CaSR homodimers functional [4]. Thus, in our case, the presence of a missense mutation may have contributed to the more severe clinical picture but functional studies would be required to further substantiate this possibility. It is important to note that a point mutation in the same codon which also led to an I555T missense change was reported in a patient with FHH and was not present in 94 control patients [10]. Paternal vs. maternal inheritance Maternal serum calcium, which is actively transported through the placenta in the third trimester to maintain a maternal-fetal gradient, impacts fetal calcium metabolism. An infant with a maternally inherited mutated allele will have a more benign clinical picture than an infant with a paternally inherited mutated allele because the resulting mild maternal hypercalcemia helps to activate the mutated
4 Tonyushkina et al. International Journal of Pediatric Endocrinology 2012, 2012:13 Page 4 of 7 Calcium, mmol/ L ipth. pmol/ L Ca/Cr cl. ratio Alkaline phospatase, U/ L wks 1.5mos 2mos 3mos 4mos 9mos 12mos 15mos 19mos Figure 2 Serum Calcium, ipth, Calcium Creatinine Clearance Ratio (CCCR), alkaline phosphatase levels over the course of observation. Gray zones indicate the reference ranges for each parameter. CCCR reference range not included due to scale; however, values <0.02 consider hypocalciuric. fetal CaSR [8] and inhibit expression PTH secretion. Conversely, in an infant with a paternally inherited mutated allele, the normocalcemic maternal environment can lead to intrauterine fetal hyperparathyroidism as higher calcium levels would be required to satisfy the mutated fetal CaSR, suppress PTH gene expression, and prevent hyperplasia in thefetalparathyroidglands.inourcase,themissensemutation of the infant was not found in the mother. Therefore, presumed paternal inheritance or a de novo mutation may have contributed to the unusually severe presentation.
5 Tonyushkina et al. International Journal of Pediatric Endocrinology 2012, 2012:13 Page 5 of 7 A B Figure 3 Changes in radiographic findings of the left femur over the course of observation (age 2 weeks to 1 year). A. 2 weeks: antero-lateral bowing, widened and irregular metaphyses with flaring and medial beaking (black arrow), and thick, smooth periosteal reaction (white arrow). B. 3 months: improved bowing, resolved periosteal reaction and mild residual beaking of the medial upper femoral metaphysis. C. 1 year: Further improvement in lateral bowing, complete resolution of metaphyseal deformity. C Prematurity Prematurity can modify the expected phenotype of neonatal hyperparathyroidism (NHPT) to one more similar to NSHPT. Such a case has been reported previously of an infant born at 27 weeks gestation with moderate hypercalcemia and severe bone disease who was found to have an inactivating mutation (R220W) of CaSR. The infant received serial pamidronate infusions and two parathyroidectomies in an attempt to control the hypercalcemia, but ultimately succumbed to respiratory disease [12]. Because the fetal skeleton depends heavily on maternal calcium and phosphorus transfer during the third trimester, prematurity predisposes an infant to deficient bone mineral accrual. An inactivated CaSR in this setting could lead to further demineralization of an already weakened skeleton and potentially lead to more severe skeletal findings. In addition, the CaSR is expressed in the placenta. Mice studies of inactivating CaSR mutations have found decreased transfer of calcium to the fetus. Theoretically, this could lead to an additional stimulus for fetal PTH secretion. Maternal vitamin D deficiency Maternal vitamin D deficiency with a negative calcium balance has been suggested to cause stimulation of fetal parathyroid glands in utero [8]. The 25(OH) D 3 in the infant obtained soon after presentation was within the normal range. The mother s level at delivery is unknown but considering the prevalence of vitamin D deficiency in New England [13] and the fact that this child was born in March, it is plausible that some degree of maternal D insufficiency was involved in the pathogenesis of hyperparathyroidism in this patient, although likely to a small degree. After 2 3 months of cholecalciferol treatment, the skeletal findings resolved and the biochemical parameters more closely corresponded to the classical features seen in FHH. The infant had a combination of mild hypercalcemia, mildly elevated serum magnesium, inappropriately high-normal PTH and low urinary calcium creatinine clearance [1]. Postnatally, the CaSR is not widely expressed in renal tubular cells but its expression increases over the first several months leading to enhanced calcium reabsorption and declining urinary calcium excretion in the normal infant [14]. In our infant, the calcium/ creatinine clearance ratio (CCCR) was strikingly low throughout her course and consistently in the range seen in FHH which is <0.02 [9]. Despite resolution of the severe hyperparathyroidism over the infant s first 3 months, her PTH continued to be in the high normal range despite increasing cholecalciferol dosing. This might indicate a more severe than average course, since persistent elevation of PTH is reported only in 20% of cases of FHH [10]. In addition, CaSR mutations are associated with adenomatous primary hyperparathyroidism [15]. We elected to use cholecalciferol to try to hasten the resolution of the hyperparathyroidism because of the active bone disease. Within the parathyroid glands, local conversion of 25(OH)D 3 to 1,25(OH) 2 D 3 has been
6 Tonyushkina et al. International Journal of Pediatric Endocrinology 2012, 2012:13 Page 6 of 7 suggested as an independent factor modulating CaSR and PTH production [16]. 1,25(OH) 2 D 3 is known to regulate PTH and CaSR gene expression as well as parathyroid cell growth [17]. Vitamin D has been shown to help decrease PTH levels in primary and secondary hyperparathyroidism [18] and has been used in the treatment of clinically significant FHH [8]. Our experience showed that cholecalciferol treatment was safe. Potentially it may have supported the infant in achieving the elevated threshold for calcium-sensing of the mutated CaSR, but its role in moderating symptomatic FHH or altering the natural course of FHH has to be further investigated. Another medical treatment option for cases such as this would be calcimemetics like cinacalcet. This agent activates the CaSR through binding to the seven transmembrane domain of the CaSR and has been shown to improve the sensitivity of the parathyroid glands to calcium and to treat hyperparathyroidism [19]. Since there is significant genetic heterogeneity in FHH, calcimemetics might not render equivalent effects in different types of CaSR mutations. One might consider using a calcimemetic in the future if the persistent hyperparathyroidism and hypercalcemia leads to complications. Conclusion In summary, this report describes a case of neonatal FHH secondary to a heterozygous inactivating missense mutation within the CaSR gene that presented with severe hyperparathyroidism, overt neonatal skeletal demineralization and perinatal fractures. We reviewed the possible causes of the uncommonly severe clinical picture and its resolution. And finally, we discussed the theoretical role of cholecalciferol in supporting the infant with clinically significant neonatal FHH via PTH suppression. This child will require careful follow-up as her PTH level still remains elevated placing her at risk of clinical hyperparathyroidism in the future as well as monitoring for the development of primary HPT which has been reported in cases of FHH. Consent Informed consent was obtained from the patient s family for publication of this case and any accompanying images. Competing interests There are no potential conflicts of interest with respect to financial or personal relationships. Author details 1 Baystate Children s Hospital, Tufts University School of Medicine, 759 Chestnut St. Dept of Pediatrics, Springfield, MA 01199, USA. 2 Baystate Medical Center, Tufts University School of Medicine, 759 Chestnut St. Dept of Radiology, Springfield, MA 01199, USA. Authors contributions KT acquired the clinical information, drafted and revised the manuscript. ND conceived the case report, helped to draft and revised the manuscript. SO helped to revise the manuscript. All authors read and approved the final manuscript. Received: 21 February 2012 Accepted: 23 May 2012 Published: 23 May 2012 References 1. Brown EM: Clinical lessons from the calcium-sensing receptor. Nat Clin Pract Endocrinol Metab 2007, 3: Pidasheva S, D Souza-Li L, Canaff L, Cole DE, Hendy GN: CASRdb: calciumsensing receptor locus-specific database for mutations causing familial (benign) hypocalciuric hypercalcemia, neonatal severe hyperparathyroidism, and autosomal dominant hypocalcemia. Hum Mutat 2004, 24: Pollak MR, Brown EM, Chou YH, Hebert SC, Marx SJ, Steinmann B, Levi T, Seidman CE, Seidman JG: Mutations in the human Ca(2+)-sensing receptor gene cause familial hypocalciuric hypercalcemia and neonatal severe hyperparathyroidism. Cell 1993, 75: Brown EM: Editorial: mutant extracellular calcium-sensing receptors and severity of disease. J Clin Endocrinol Metab 2005, 90: Obermannova B, Banghova K, Sumnik Z, Dvorakova HM, Betka J, Fencl F, Kolouskova S, Cinek O, Lebl J: Unusually severe phenotype of neonatal primary hyperparathyroidism due to a heterozygous inactivating mutation in the CASR gene. Eur J Pediatr 2009, 168: Page LA, Haddow JE: Self-limited neonatal hyperparathyroidism in familial hypocalciuric hypercalcemia. J Pediatr 1987, 111: Wilkinson H, James J: Self limiting neonatal primary hyperparathyroidism associated with familial hypocalciuric hypercalcaemia. Arch Dis Child 1993, 69: Zajickova K, Vrbikova J, Canaff L, Pawelek PD, Goltzman D, Hendy GN: Identification and functional characterization of a novel mutation in the calcium-sensing receptor gene in familial hypocalciuric hypercalcemia: modulation of clinical severity by vitamin D status. J Clin Endocrinol Metab 2007, 92: Christensen SE, Nissen PH, Vestergaard P, Heickendorff L, Brixen K, Mosekilde L: Discriminative power of three indices of renal calcium excretion for the distinction between familial hypocalciuric hypercalcaemia and primary hyperparathyroidism: a follow-up study on methods. Clin Endocrinol 2008, 69: Nissen PH, Christensen SE, Heickendorff L, Brixen K, Mosekilde L: Molecular genetic analysis of the calcium sensing receptor gene in patients clinically suspected to have familial hypocalciuric hypercalcemia: phenotypic variation and mutation spectrum in a Danish population. J Clin Endocrinol Metab 2007, 92: Bai M, Trivedi S, Kifor O, Quinn SJ, Brown EM: Intermolecular interactions between dimeric calcium-sensing receptor monomers are important for its normal function. Proc Natl Acad Sci U S A 1999, 96: Fox L, Sadowksy J, Pringle KP, Kidd A, Murdoch J, Cole DEC, Wiltshire E: Neonatal hyperparathyroidism and pamidronate therapy in an extremely premature infant. Pediatrics 2007, 120:e Merewood A, Mehta SD, Grossman X, Chen TC, Mathieu JS, Holick MF, Bauchner H: Widespread vitamin D deficiency in urban Massachusetts newborns and their mothers. Pediatrics 2010, 125: Chattopadhyay N, Baum M, Bai M, Riccardi D, Hebert SC, Harris HW, Brown EM: Ontogeny of the extracellular calcium-sensing receptor in rat kidney. Am J Physiol 1996, 271:F Starker LF, Akerström T, Long WD, Delgado-Verdugo A, Donovan P, Udelsman R, Lifton RP, Carling T: Frequent germ-line mutations of the MEN1, CASR, and HRPT2/CDC73 genes in young patients with clinically non-familial primary hyperparathyroidism. Horm Cancer 2012, 3(1 2): Segersten U, Correa P, Hewison M, Hellman P, Dralle H, Carling T, Akerstrom G, Westin G: 25-hydroxyvitamin D(3)-1alpha-hydroxylase expression in normal and pathological parathyroid glands. J Clin Endocrinol Metab 2002, 87:
7 Tonyushkina et al. International Journal of Pediatric Endocrinology 2012, 2012:13 Page 7 of Ritter CS, Brown AJ: Direct suppression of Pth gene expression by the vitamin D prohormones doxercalciferol and calcidiol requires the vitamin D receptor. J Mol Endocrinol 2011, 46: Grey A, Lucas J, Horne A, Gamble G, Davidson JS, Reid IR: Vitamin D repletion in patients with primary hyperparathyroidism and coexistent vitamin D insufficiency. J Clin Endocrinol Metab 2005, 90: Festen-Spanjer B, Haring CM, Koster JB, Mudde AH: Correction of hypercalcaemia by cinacalcet in familial hypocalciuric hypercalcaemia. Clin Endocrinol (Oxf) 2008, 68: doi: / Cite this article as: Tonyushkina et al.: A novel CaSR mutation presenting as a severe case of neonatal familial hypocalciuric hypercalcemia. International Journal of Pediatric Endocrinology :13. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Hypercalcemia. Hypercalcemia: When to Worry, When to Treat! Mineral Metabolism : A Short Course
 Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Pediatric metabolic bone diseases
 Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
HYPERCALCEMIA (FHH) IN A YOUNG HISPANIC MAN. Running title: New mutation Calcium Sensing Receptor causing FHH.
 AACE Clinical Case Reports Rapid Electronic Articles in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited,
AACE Clinical Case Reports Rapid Electronic Articles in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited,
Approach to a patient with hypercalcemia
 Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
CALCIUM CREATININE CLEARANCE RATIO IS NOT HELPFUL IN DIFFERENTIATING PRIMARY
 ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
A novel mutation of the calcium-sensing receptor gene in a Greek family from Nisyros
 HORMONES 2015, 14(2):321-325 Letter to the Editor A novel mutation of the calcium-sensing receptor gene in a Greek family from Nisyros Evaggelia Zapanti, 1 Aikaterini Polonifi, 2 Michalis Kokkinos, 2 George
HORMONES 2015, 14(2):321-325 Letter to the Editor A novel mutation of the calcium-sensing receptor gene in a Greek family from Nisyros Evaggelia Zapanti, 1 Aikaterini Polonifi, 2 Michalis Kokkinos, 2 George
Hypophosphatasia. Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX
 Hypophosphatasia Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX Hypophosphatasia Case Teeth 57 y/o male with a hyperlipidemia and hypogonadism. Noted to have an alkaline phosphatase of
Hypophosphatasia Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX Hypophosphatasia Case Teeth 57 y/o male with a hyperlipidemia and hypogonadism. Noted to have an alkaline phosphatase of
Southern Derbyshire Shared Care Pathology Guidelines. Primary Hyperparathyroidism
 Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Calcium-sensing receptors
 Making sense of calcium Calcium-sensing receptors Prof Arthur D Conigrave School of Molecular Bioscience, University of Sydney Department of Endocrinology, Royal Prince Alfred Hospital The calcium-sensing
Making sense of calcium Calcium-sensing receptors Prof Arthur D Conigrave School of Molecular Bioscience, University of Sydney Department of Endocrinology, Royal Prince Alfred Hospital The calcium-sensing
PRIMARY HYPERPARATHYROIDISM PRIMARY HYPERPARATHYROIDISM. Hyperparathyroidism Etiology. Common Complex Insidious Chronic Global Only cure is surgery
 ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
4/20/2015. The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy. Learning Objectives
 The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning
The Neck xt Exploration: Intraoperative Parathyroid Hormone (IOPTH) Testing During Surgical Parathyroidectomy Nichole Korpi-Steiner, PhD, DABCC, FACB University of North Carolina Chapel Hill, NC Learning
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
Sachin Soni DNB Pediatrics
 Sachin Soni DNB Pediatrics Vitamin D physiology Introduction Etiology Clinical feature Radiology Diagnosis Lab Treatment Source: -Fish, liver and oil, - Human milk (30-40 IU/L) - Exposure to sun light
Sachin Soni DNB Pediatrics Vitamin D physiology Introduction Etiology Clinical feature Radiology Diagnosis Lab Treatment Source: -Fish, liver and oil, - Human milk (30-40 IU/L) - Exposure to sun light
King s Research Portal
 King s Research Portal DOI: 10.1002/ccr3.1074 Document Version Publisher's PDF, also known as Version of record Link to publication record in King's Research Portal Citation for published version (APA):
King s Research Portal DOI: 10.1002/ccr3.1074 Document Version Publisher's PDF, also known as Version of record Link to publication record in King's Research Portal Citation for published version (APA):
DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS
 DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS XLH IS CHARACTERIZED BY CHRONIC HYPOPHOSPHATEMIA XLH is a hereditary, progressive, lifelong disorder. In children and adults,
DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS XLH IS CHARACTERIZED BY CHRONIC HYPOPHOSPHATEMIA XLH is a hereditary, progressive, lifelong disorder. In children and adults,
Hyperparathyroidism. When to Suspect, How to Diagnose, When and How to Intervene. Johanna A. Pallotta, MD, FACP, FACE
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma
 ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 2 Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma P George, N Philip, B Pawar Citation P George,
ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 2 Radiographic Appearance Of Primary Hyperparathyroidism With Atypical Parathyroid Adenoma P George, N Philip, B Pawar Citation P George,
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyper and hypocalcaemia. Prof Tricia Tan
 Hyper and hypocalcaemia Prof Tricia Tan Learning Objectives Basic physiology of Ca regulation Case presentations Take home messages Calcium Total body calcium content ~1300g 99% in bone 1% intracellular
Hyper and hypocalcaemia Prof Tricia Tan Learning Objectives Basic physiology of Ca regulation Case presentations Take home messages Calcium Total body calcium content ~1300g 99% in bone 1% intracellular
Calcium & Calcium-sensing receptors
 Calcium & Calcium-sensing receptors Prof Arthur D Conigrave School of Life & Environmental Sciences, University of Sydney Department of Endocrinology, Royal Prince Alfred Hospital Collaborators Sydney
Calcium & Calcium-sensing receptors Prof Arthur D Conigrave School of Life & Environmental Sciences, University of Sydney Department of Endocrinology, Royal Prince Alfred Hospital Collaborators Sydney
Identification of AP2S1 Mutation and Effects of Low Calcium Formula in an Infant With Hypercalcemia and Hypercalciuria
 JCEM ONLINE Advances in Genetics Endocrine Research Identification of AP2S1 Mutation and Effects of Low Calcium Formula in an Infant With Hypercalcemia and Hypercalciuria Yasuko Fujisawa, Rie Yamaguchi,
JCEM ONLINE Advances in Genetics Endocrine Research Identification of AP2S1 Mutation and Effects of Low Calcium Formula in an Infant With Hypercalcemia and Hypercalciuria Yasuko Fujisawa, Rie Yamaguchi,
Primary Hyperparathyroidism
 Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment
 Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy: a case report
 Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Current Concepts in the Evaluation and Management of Abnormal Parathyroid Hormone (PTH) Levels Shireen Fatemi, M.D. April, 2012.
 Current Concepts in the Evaluation and Management of Abnormal Parathyroid Hormone (PTH) Levels Shireen Fatemi, M.D. April, 2012 Disclosures I have no financial relationships with commercial interests,
Current Concepts in the Evaluation and Management of Abnormal Parathyroid Hormone (PTH) Levels Shireen Fatemi, M.D. April, 2012 Disclosures I have no financial relationships with commercial interests,
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
HYPERCALCEMIA. Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
Hypercalcemia may be detected incidentally. Practice CMAJ. Primary hyperparathyroidism. Primer. Key points. The case. What causes hypercalcemia?
 CMAJ Practice Primer Primary hyperparathyroidism Hafsah Al-Azem HBSc, Aliya Khan MD The case A 17-year-old man presented at the clinic with thirst, lethargy and fatigue that had been ongoing for several
CMAJ Practice Primer Primary hyperparathyroidism Hafsah Al-Azem HBSc, Aliya Khan MD The case A 17-year-old man presented at the clinic with thirst, lethargy and fatigue that had been ongoing for several
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Newborn with Fractures. Payal Patel, M.D. Pediatric Endocrinology Fellow May 22, 2014
 Newborn with Fractures Payal Patel, M.D. Pediatric Endocrinology Fellow May 22, 2014 Chief Complaint 2-day-old F with prenatally dx ed osteogenesis imperfecta (OI). HPI Born via repeat C/S to a 30 yo G3P2
Newborn with Fractures Payal Patel, M.D. Pediatric Endocrinology Fellow May 22, 2014 Chief Complaint 2-day-old F with prenatally dx ed osteogenesis imperfecta (OI). HPI Born via repeat C/S to a 30 yo G3P2
PRIMARY HYPERPARATHYROIDISM
 PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones
 Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) 30 yr-old woman with 7 yr history
Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) 30 yr-old woman with 7 yr history
Pseudohypoparathyroidism: Case Presentation and Literature Review
 Pseudohypoparathyroidism: Case Presentation and Literature Review Aristides Maniatis, MD Rocky Mountain Pediatric Endocrinology PENS: 5/15/06 Disclosures Nothing to disclose Parental permission granted
Pseudohypoparathyroidism: Case Presentation and Literature Review Aristides Maniatis, MD Rocky Mountain Pediatric Endocrinology PENS: 5/15/06 Disclosures Nothing to disclose Parental permission granted
Sensipar. Sensipar (cinacalcet) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Case Report Clinical Phenotype in a Toddler with a Novel Heterozygous Mutation of the Vitamin D Receptor
 Hindawi Case Reports in Endocrinology Volume 2017, Article ID 3905905, 4 pages https://doi.org/10.1155/2017/3905905 Case Report Clinical Phenotype in a Toddler with a Novel Heterozygous Mutation of the
Hindawi Case Reports in Endocrinology Volume 2017, Article ID 3905905, 4 pages https://doi.org/10.1155/2017/3905905 Case Report Clinical Phenotype in a Toddler with a Novel Heterozygous Mutation of the
Esther Briganti. Fetal And Maternal Health Beyond the Womb: hot topics in endocrinology and pregnancy. Endocrinologist and Clinician Researcher
 Fetal And Maternal Health Beyond the Womb: hot topics in endocrinology and pregnancy Esther Briganti Endocrinologist and Clinician Researcher Director, Melbourne Endocrine Associates Associate Professor,
Fetal And Maternal Health Beyond the Womb: hot topics in endocrinology and pregnancy Esther Briganti Endocrinologist and Clinician Researcher Director, Melbourne Endocrine Associates Associate Professor,
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Journal of Clinical & Translational Endocrinology
 Journal of Clinical & Translational Endocrinology 2 (2015) 14e20 Contents lists available at ScienceDirect Journal of Clinical & Translational Endocrinology journal homepage: www.elsevier.com/locate/jcte
Journal of Clinical & Translational Endocrinology 2 (2015) 14e20 Contents lists available at ScienceDirect Journal of Clinical & Translational Endocrinology journal homepage: www.elsevier.com/locate/jcte
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Natpara (parathyroid hormone) Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Natpara (parathyroid hormone) Prime Therapeutics will review Prior Authorization
Natpara (parathyroid hormone) Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Natpara (parathyroid hormone) Prime Therapeutics will review Prior Authorization
Calcium Conundrums. California Chapter AACE. September 2015
 Calcium Conundrums California Chapter AACE September 2015 Michael W. Yeh, MD Chief, Section of Endocrine Surgery Associate Professor of Surgery and Medicine David Geffen School of Medicine at UCLA www.endocrinesurgery.ucla.edu
Calcium Conundrums California Chapter AACE September 2015 Michael W. Yeh, MD Chief, Section of Endocrine Surgery Associate Professor of Surgery and Medicine David Geffen School of Medicine at UCLA www.endocrinesurgery.ucla.edu
Genetic examination of diseases affecting bone development. and structure in newborns
 Genetic examination of diseases affecting bone development and structure in newborns Examination of molecular genetic markers in osteopenic preterm infants PhD Thesis Simone Funke, MD University of Pécs
Genetic examination of diseases affecting bone development and structure in newborns Examination of molecular genetic markers in osteopenic preterm infants PhD Thesis Simone Funke, MD University of Pécs
Hypophosphatemic rickets: new treatments
 Hypophosphatemic rickets: new treatments Gema Ariceta Pediatric Nephrology, University Hospital Vall d Hebron, Barcelona 1 11.06.18 Tubulopathies Disclosures Lectures and educational activities sponsored
Hypophosphatemic rickets: new treatments Gema Ariceta Pediatric Nephrology, University Hospital Vall d Hebron, Barcelona 1 11.06.18 Tubulopathies Disclosures Lectures and educational activities sponsored
Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B.
 Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B. Increased concentration of proteins in foods C. Decreasing
Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B. Increased concentration of proteins in foods C. Decreasing
Hypercalcemia. Brian Rose, M.D. Bozeman Health June 6, 2018
 Hypercalcemia Brian Rose, M.D. Bozeman Health June 6, 2018 Hypercalcemia Diagnosis PTH Mediated Primary Hyperparathyroidism Lithium Familial Hypocalciuric Hypercalcemia Non PTH mediated Malignancy Humoral
Hypercalcemia Brian Rose, M.D. Bozeman Health June 6, 2018 Hypercalcemia Diagnosis PTH Mediated Primary Hyperparathyroidism Lithium Familial Hypocalciuric Hypercalcemia Non PTH mediated Malignancy Humoral
Pituitary, Parathyroid Pheochromocytomas & Paragangliomas: The 4 Ps of NETs
 Pituitary, Parathyroid Pheochromocytomas & Paragangliomas: The 4 Ps of NETs Shereen Ezzat, MD, FRCP(C), FACP Professor Of Medicine & Oncology Head, Endocrine Oncology Princess Margaret Hospital/University
Pituitary, Parathyroid Pheochromocytomas & Paragangliomas: The 4 Ps of NETs Shereen Ezzat, MD, FRCP(C), FACP Professor Of Medicine & Oncology Head, Endocrine Oncology Princess Margaret Hospital/University
A case of hereditary hypophosphataemic rickets with hypercalciuria (HHRH)
 Case Reports A case of hereditary hypophosphataemic rickets with hypercalciuria (HHRH) M N Lucas 1, Savithri Dias 2 Sri Lanka Journal of Child Health, 2006; 35:141-3 (Key words: hereditary hypophosphataemic
Case Reports A case of hereditary hypophosphataemic rickets with hypercalciuria (HHRH) M N Lucas 1, Savithri Dias 2 Sri Lanka Journal of Child Health, 2006; 35:141-3 (Key words: hereditary hypophosphataemic
Plasma 25-hydroxyvitamin D, 1,25-dihydroxyvitamin D, and parathyroid hormone in familial hypocalciuric hypercalcemia and primary hyperparathyroidism
 European Journal of Endocrinology (2008) 159 719 727 ISSN 0804-4643 CLINICAL STUDY Plasma 25-hydroxyvitamin D, 1,25-dihydroxyvitamin D, and parathyroid hormone in familial hypocalciuric hypercalcemia and
European Journal of Endocrinology (2008) 159 719 727 ISSN 0804-4643 CLINICAL STUDY Plasma 25-hydroxyvitamin D, 1,25-dihydroxyvitamin D, and parathyroid hormone in familial hypocalciuric hypercalcemia and
What this study adds: - Sustained hypercalacemia affects 1 in 500 children in a general hospital setting
 FREQUENCY AND AETIOLOGY OF HYPERCALCAEMIA McNeilly JD 1, Boal R 2, Shaikh MG 2, Ahmed SF 2 1 Dept of Clinical Biochemistry, Queen Elizabeth University Hospital, Greater Glasgow & Clyde NHS Trust, Glasgow,
FREQUENCY AND AETIOLOGY OF HYPERCALCAEMIA McNeilly JD 1, Boal R 2, Shaikh MG 2, Ahmed SF 2 1 Dept of Clinical Biochemistry, Queen Elizabeth University Hospital, Greater Glasgow & Clyde NHS Trust, Glasgow,
Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP
 Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Intravenous use Treatment of hypercalcemia due to malignancy. Oral use Treatment of hypercalcemia
Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Intravenous use Treatment of hypercalcemia due to malignancy. Oral use Treatment of hypercalcemia
بسم هللا الرحمن الرحيم. Rickets
 بسم هللا الرحمن الرحيم Rickets 1 Rickets IS defined as failure of mineralization of growing bone or osteoid tissue due to vitamin D deficiency. Vitamin D appear as rickets in children and as oteomalacia
بسم هللا الرحمن الرحيم Rickets 1 Rickets IS defined as failure of mineralization of growing bone or osteoid tissue due to vitamin D deficiency. Vitamin D appear as rickets in children and as oteomalacia
SEX-LINKED INHERITANCE. Dr Rasime Kalkan
 SEX-LINKED INHERITANCE Dr Rasime Kalkan Human Karyotype Picture of Human Chromosomes 22 Autosomes and 2 Sex Chromosomes Autosomal vs. Sex-Linked Traits can be either: Autosomal: traits (genes) are located
SEX-LINKED INHERITANCE Dr Rasime Kalkan Human Karyotype Picture of Human Chromosomes 22 Autosomes and 2 Sex Chromosomes Autosomal vs. Sex-Linked Traits can be either: Autosomal: traits (genes) are located
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
Skeletal. Parathyroid hormone-related protein Analyte Information
 Skeletal Parathyroid hormone-related protein Analyte Information 1 2012-04-04 Parathyroid hormone related protein (PTHrP) Introduction Parathyroid hormone-related protein (PTHrP) is actually a family of
Skeletal Parathyroid hormone-related protein Analyte Information 1 2012-04-04 Parathyroid hormone related protein (PTHrP) Introduction Parathyroid hormone-related protein (PTHrP) is actually a family of
Ca, Mg metabolism, bone diseases. Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary
 Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Parathyroid hormone (serum, plasma)
 Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
OSTEOMALACIA UPDATE. Nothing to Disclose. Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco
 OSTEOMALACIA UPDATE Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco Nothing to Disclose 1 Case History 59 YO WM referred for evaluation of diffuse
OSTEOMALACIA UPDATE Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco Nothing to Disclose 1 Case History 59 YO WM referred for evaluation of diffuse
Magnesium Homeostasis
 ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Strensiq (asfotase alfa) Page 1 of 5 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Strensiq (asfotase alfa) Prime Therapeutics will review Prior Authorization
Strensiq (asfotase alfa) Page 1 of 5 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Strensiq (asfotase alfa) Prime Therapeutics will review Prior Authorization
OMICS Journals are welcoming Submissions
 OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
Disclosure. Topic Outline. Calcium, Vitamin D, PTH Disorders. PTH/Calcium-Normal Physiology. I have nothing to disclose
 Disclosure Calcium, Vitamin D, PTH Disorders I have nothing to disclose Chienying Liu MD Associate Clinical Professor Division of Endocrinology & Metabolism UCSF Topic Outline Calcium/Vitamin D/PTH physiology
Disclosure Calcium, Vitamin D, PTH Disorders I have nothing to disclose Chienying Liu MD Associate Clinical Professor Division of Endocrinology & Metabolism UCSF Topic Outline Calcium/Vitamin D/PTH physiology
The extracellular calcium-sensing receptor (CaSR) plays a
 ORIGINAL ARTICLE Endocrine Care Novel Inactivating Mutations of the Calcium-Sensing Receptor: The Calcimimetic NPS R-568 Improves Signal Transduction of Mutant Receptors Ramona Rus, Christine Haag, Christiane
ORIGINAL ARTICLE Endocrine Care Novel Inactivating Mutations of the Calcium-Sensing Receptor: The Calcimimetic NPS R-568 Improves Signal Transduction of Mutant Receptors Ramona Rus, Christine Haag, Christiane
International Journal of Biological & Medical Research. An Uncommon Case of Persistent Hypercalcaemia following Parathyroid Surgery
 Int J Biol Med Res.2015;6(4):5336-5340 Int J Biol Med Res www.biomedscidirect.com Volume 6, Issue 2, April 2015 Contents lists available at BioMedSciDirect Publications International Journal of Biological
Int J Biol Med Res.2015;6(4):5336-5340 Int J Biol Med Res www.biomedscidirect.com Volume 6, Issue 2, April 2015 Contents lists available at BioMedSciDirect Publications International Journal of Biological
Secondary and Familial Hyperparathyroidism
 Secondary and Familial Jeffrey F. Moley, M.D. Chief, Endocrine and Oncologic Surgery Section, Professor of Surgery Associate Director, The Alvin J. Siteman Cancer Center Occurs in setting of CRF Chronic
Secondary and Familial Jeffrey F. Moley, M.D. Chief, Endocrine and Oncologic Surgery Section, Professor of Surgery Associate Director, The Alvin J. Siteman Cancer Center Occurs in setting of CRF Chronic
Fibrous Dysplasia in Children. Professor Nick Shaw Birmingham Children s Hospital, UK
 Fibrous Dysplasia in Children Professor Nick Shaw Birmingham Children s Hospital, UK Overview What is Fibrous Dysplasia? Clinical Presentations Endocrine Problems Skeletal Problems Treatment Options Fibrous
Fibrous Dysplasia in Children Professor Nick Shaw Birmingham Children s Hospital, UK Overview What is Fibrous Dysplasia? Clinical Presentations Endocrine Problems Skeletal Problems Treatment Options Fibrous
Agent(s) FDA Labeled Indications Dosage and Administration. Perinatal/Infantile-onset hypophosphatasia. Juvenile-onset hypophosphatasia
 Strensiq (asfotase alfa) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE Agent(s) FDA Labeled Indications Dosage and Administration Strensiq (asfotase alfa) injection Perinatal/Infantile-onset
Strensiq (asfotase alfa) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE Agent(s) FDA Labeled Indications Dosage and Administration Strensiq (asfotase alfa) injection Perinatal/Infantile-onset
76 year-old female presents with muscle cramps. Jess Hwang 12/6/12
 76 year-old female presents with muscle cramps Jess Hwang 12/6/12 HPI Worked up for outpatient hypercalcemia Calcium had been 10.3-11.1, PTH ~120 No h/o osteoporosis, CKD, kidney stones Not taking calcium
76 year-old female presents with muscle cramps Jess Hwang 12/6/12 HPI Worked up for outpatient hypercalcemia Calcium had been 10.3-11.1, PTH ~120 No h/o osteoporosis, CKD, kidney stones Not taking calcium
PRIMARY HYPERPARATHYROIDISM WITH RICKETS. KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College
 PRIMARY HYPERPARATHYROIDISM WITH RICKETS KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College Presenting Complaints v 17 year old developmentally normal adolescent boy, first of a twin pregnancy,
PRIMARY HYPERPARATHYROIDISM WITH RICKETS KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College Presenting Complaints v 17 year old developmentally normal adolescent boy, first of a twin pregnancy,
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Clinical biochemistry of calcium and vitamin D
 Clinical biochemistry of calcium and vitamin D Dr Andrew Day Consultant in Clinical Biochemistry and Metabolic Medicine University Hospitals Bristol NHS Trust e-mail: andrew.day@uhbristol.nhs.uk A 48-year
Clinical biochemistry of calcium and vitamin D Dr Andrew Day Consultant in Clinical Biochemistry and Metabolic Medicine University Hospitals Bristol NHS Trust e-mail: andrew.day@uhbristol.nhs.uk A 48-year
Vitamin D The hidden deficiency. Dr Pamela von Hurst Senior Lecturer Human Nutrition Director of the Massey Vitamin D Research Centre
 Vitamin D The hidden deficiency Dr Pamela von Hurst Senior Lecturer Human Nutrition Director of the Massey Vitamin D Research Centre Overview Vitamin D what, where from, how much The New Zealand situation
Vitamin D The hidden deficiency Dr Pamela von Hurst Senior Lecturer Human Nutrition Director of the Massey Vitamin D Research Centre Overview Vitamin D what, where from, how much The New Zealand situation
Case study Group 2 presentation
 Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Parathyroidectomy. Surgery for Parathyroid Problems
 Parathyroidectomy Surgery for Parathyroid Problems Why You Need Parathyroid Surgery Has your doctor just recommended that you have parathyroid surgery? If so, you likely have many questions. What are the
Parathyroidectomy Surgery for Parathyroid Problems Why You Need Parathyroid Surgery Has your doctor just recommended that you have parathyroid surgery? If so, you likely have many questions. What are the
A Genetic Overview of Hypophosphatasia
 A Genetic Overview of Hypophosphatasia A Background in Genetics Cells are the basic building blocks of all living organisms. Our body is composed of trillions of cells. Each of these cells contains deoxyribonucleic
A Genetic Overview of Hypophosphatasia A Background in Genetics Cells are the basic building blocks of all living organisms. Our body is composed of trillions of cells. Each of these cells contains deoxyribonucleic
Potential conflicts of interest: None
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene November 6, 2013 Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene November 6, 2013 Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline
Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid Carcinoma: A Case Report
 CASE REPORT Hip Pelvis 28(3): 173-177, 2016 http://dx.doi.org/10.5371/hp.2016.28.3.173 Print ISSN 2287-3260 Online ISSN 2287-3279 Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid
CASE REPORT Hip Pelvis 28(3): 173-177, 2016 http://dx.doi.org/10.5371/hp.2016.28.3.173 Print ISSN 2287-3260 Online ISSN 2287-3279 Pathologic Fracture of the Femur in Brown Tumor Induced in Parathyroid
Bilateral rib fractures 2 on right and 1 on left In different stages of healing, with left fracture older than right fractures
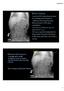 More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
ESPEN Congress Prague 2007
 ESPEN Congress Prague 2007 Key papers in the field of nutrition Dietitian Geila S Rozen Key Papers in the field of Nutrition ESPEN 2007 Prague Geila S Rozen Clinical Nutrition Dep. Rambam health campus
ESPEN Congress Prague 2007 Key papers in the field of nutrition Dietitian Geila S Rozen Key Papers in the field of Nutrition ESPEN 2007 Prague Geila S Rozen Clinical Nutrition Dep. Rambam health campus
Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients
 Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients A. WADGYMAR, MD Credit Valley Hospital, Mississauga, Ontario, Canada. June 1, 2007 1 Case: 22 y/o referred to Renal Clinic Case: A.M. 29 y/o Man
Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients A. WADGYMAR, MD Credit Valley Hospital, Mississauga, Ontario, Canada. June 1, 2007 1 Case: 22 y/o referred to Renal Clinic Case: A.M. 29 y/o Man
UPDATES ON PRIMARY HYPERPARATHYROIDISM. Natalie E. Cusano, MD, MS Director, Bone Metabolism Program Lenox Hill Hospital New York, NY
 UPDATES ON PRIMARY HYPERPARATHYROIDISM Natalie E. Cusano, MD, MS Director, Bone Metabolism Program Lenox Hill Hospital New York, NY Disclosures Speaker (Honorarium): Shire Off-label use of estrogen, raloxifene
UPDATES ON PRIMARY HYPERPARATHYROIDISM Natalie E. Cusano, MD, MS Director, Bone Metabolism Program Lenox Hill Hospital New York, NY Disclosures Speaker (Honorarium): Shire Off-label use of estrogen, raloxifene
Calcium Nephrolithiasis and Bone Health. Noah S. Schenkman, MD
 Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
The Parathyroid Glands
 The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast
 The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast September 27, 2018 Introduction: Hello everyone, my name is Dominique Piché
The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast September 27, 2018 Introduction: Hello everyone, my name is Dominique Piché
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE
 HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
THE NEW ZEALAND MEDICAL JOURNAL
 THE NEW ZEALAND MEDICAL JOURNAL Vol 116 No 1179 ISSN 1175 8716 Efficacy of an oral, 10-day course of high-dose calciferol in correcting vitamin D deficiency Fiona Wu, Toni Staykova, Anne Horne, Judy Clearwater,
THE NEW ZEALAND MEDICAL JOURNAL Vol 116 No 1179 ISSN 1175 8716 Efficacy of an oral, 10-day course of high-dose calciferol in correcting vitamin D deficiency Fiona Wu, Toni Staykova, Anne Horne, Judy Clearwater,
Cholecalciferol (D3) - sources Vitamin D. Endogenous - synthesis in the skin
 Department of Pediatrics and Developmental Disorders Medical University of Bialystok Vitamin D metabolism and clinical manifestation of its deficit Pawel Abramowicz M.D., Ph.D. Jerzy Konstantynowicz MD,
Department of Pediatrics and Developmental Disorders Medical University of Bialystok Vitamin D metabolism and clinical manifestation of its deficit Pawel Abramowicz M.D., Ph.D. Jerzy Konstantynowicz MD,
Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from the West?
 ecommons@aku Section of Urology Department of Surgery August 1999 Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from
ecommons@aku Section of Urology Department of Surgery August 1999 Bone and Renal Stone Disease in Patients Operated for Primary Hyperparathyroidism in Pakistan: Is the Pattern of Disease different from
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy
 "Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
ORIGINAL ARTICLE. Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism
 Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism Elizabeth A. Mittendorf, MD; Christopher R. McHenry, MD ORIGINAL ARTICLE Background: Persistent
Persistent Parathyroid Hormone Elevation Following Curative Parathyroidectomy for Primary Hyperparathyroidism Elizabeth A. Mittendorf, MD; Christopher R. McHenry, MD ORIGINAL ARTICLE Background: Persistent
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Summary Statement from a Workshop on Asymptomatic Primary Hyperparathyroidism: A Perspective for the 21st Century
 Summary Statement from a Workshop on Asymptomatic Primary Hyperparathyroidism: A Perspective for the 21st Century John P. Bilezikian, John T. Potts, Jr., Ghada El-Hajj Fuleihan, Michael Kleerekoper, Robert
Summary Statement from a Workshop on Asymptomatic Primary Hyperparathyroidism: A Perspective for the 21st Century John P. Bilezikian, John T. Potts, Jr., Ghada El-Hajj Fuleihan, Michael Kleerekoper, Robert
Osteopenia Of Prematurity Prevention And Treatment
 ISPUB.COM The Internet Journal of Advanced Nursing Practice Volume 4 Number 2 Osteopenia Of Prematurity Prevention And Treatment B Cross, E Vasquez Citation B Cross, E Vasquez. Osteopenia Of Prematurity
ISPUB.COM The Internet Journal of Advanced Nursing Practice Volume 4 Number 2 Osteopenia Of Prematurity Prevention And Treatment B Cross, E Vasquez Citation B Cross, E Vasquez. Osteopenia Of Prematurity
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names Osteogenesis Imperfecta
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names Osteogenesis Imperfecta
Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor
 Case Reports in Medicine Volume 2012, Article ID 432676, 4 pages doi:10.1155/2012/432676 Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor F. Mantar, 1 S. Gunduz,
Case Reports in Medicine Volume 2012, Article ID 432676, 4 pages doi:10.1155/2012/432676 Case Report A Reference Finding Rarely Seen in Primary Hyperparathyroidism: Brown Tumor F. Mantar, 1 S. Gunduz,
Calcium-Sensing Receptors
 Calcium-Sensing Receptors By William G. Goodman It is now known that variations in extracellular calcium concentration exert diverse physiologic effects in a variety of tissues that are mediated by a calcium-sensing
Calcium-Sensing Receptors By William G. Goodman It is now known that variations in extracellular calcium concentration exert diverse physiologic effects in a variety of tissues that are mediated by a calcium-sensing
