Paediatric Inherited Metabolic Medicine
|
|
|
- Cornelius O’Neal’
- 6 years ago
- Views:
Transcription
1 RCPCH Progress Paediatric curriculum for excellence Paediatric Inherited Metabolic Medicine Level 3 Paediatrics Sub-specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College of Paediatrics and Child Health is a registered charity in England and Wales (105774) and in Scotland (SCO38299)
2 This document outlines the syllabus to be used by doctors completing completing Level 3 Paediatric Inherited Metabolic Medicine training in the United Kingdom training in the United Kingdom (UK). It accompanies the RCPCH Progress curriculum and assessment strategy. Introduction This is Version 1.0. As the document is updated, version numbers will be changed, and content changes noted in the table below. Version number Date issued Summary of changes This syllabus supports the completion of the RCPCH Progress curriculum, and should be used in conjunction with the curriculum document. The purpose of the curriculum is to train doctors to acquire a detailed knowledge and understanding of health and illness in babies, children and young people. The curriculum provides a framework for training, articulating the standard required to work at Consultant level, and at key progression points during their training, as well as encouraging the pursuit of excellence in all aspects of clinical and wider practice. The curriculum comprises of Learning Outcomes which specify the standard that trainees must demonstrate as they progress through training and ultimately attain a Certificate of Completion of Training (CCT). The syllabi support the curriculum by providing further instructions and guidance as to how the Learning Outcomes can be achieved and demonstrated. Using the Syllabus Paediatric trainees are required to demonstrate achievement of generic and sub-specialty or General Paediatric Learning Outcomes throughout their training period. For all level 1 and level 2 trainees, there are 11 generic paediatric Learning Outcomes for each level. At level 3, there are a further 11 generic paediatric Learning Outcomes for all trainees, and several additional Learning Outcomes in either General Paediatrics or the GRID sub-specialty the trainee has been appointed into. This syllabus contains 5 interlinked elements, as outlined in figure 1 which illustrates how each element elaborates on the previous one. This information is correct and up to date at time of Publication. RCPCH
3 Elements of the Syllabus The Introductory Statement sets the scene for what makes a Metabolic Paediatrician. The Learning Outcomes are stated at the beginning of each section. These are the outcomes which the trainee must demonstrate they have met to be awarded their Certificate of Completion of Training (CCT) in Paediatrics. Progress towards achievement of the Learning Outcomes is reviewed annually at the Annual Review of Competence Progression (ARCP). Each Learning Outcome is mapped to the GMC (General Medical Council) Generic Professional Capabilities framework. Each trainee must achieve all the Generic Professional Capabilities to meet the minimum regulatory standards for satisfactory completion of training. Using the Syllabus with eportfolio Recording evidence in the eportfolio to demonstrate progression against the learning outcomes and key capabilities can be done from any assessment or event in the eportfolio. At the end of any event or assessment, there is an opportunity to add tags, documents and comments. Expanding this by clicking show more will enable you to link your assessment to the curriculum items, where you will find the learning outcomes for each domain, key capabilities and example illustrations. Trainees will therefore be able to track their progress in fulfilling the mandatory learning outcomes and key capabilities. The Key Capabilities are mandatory capabilities which must be evidenced by the trainee, in their eportfolio, to meet the Learning Outcome. Key Capabilities are therefore also mapped to the GMC Generic Professional Capabilities framework. The Illustrations are examples of evidence and give the range of clinical contexts that the trainee may use to support their achievement of the Key Capabilities. These are intended to provide a prompt to the trainee and trainer as to how the overall outcomes might be achieved. They are not intended to be exhaustive, and excellent trainees may produce a broader portfolio or include evidence that demonstrates deeper learning. It is not expected that trainees provide eportfolio evidence against every individual illustration (or a set quota); the aim of assessment is to provide evidence against every Key Capability. The Assessment Grid indicates suggested assessment methods, which may be used to demonstrate the Key Capabilities. Trainees may use differing assessment methods to demonstrate each capability (as indicated in each Assessment Grid), but there must be evidence of the trainee having achieved all Key Capabilities. Introductory Statement Learning Outcomes Key Capabilities Illustrations Assessment Grid Figure 1: The 5 elements of the syllabus 4 5
4 Paediatric Inherited Metabolic Medicine Introductory Statement Sub-specialty Learning Outcomes Introductory Statement A Metabolic Paediatrician is a doctor who cares for children and families who have inherited disorders that affect the body s normal biochemical reactions. There are many rare metabolic disorders that can affect the function of any organ system and can present at any age. They have detailed knowledge of normal human biochemistry and the impact of metabolic diseases, and use this knowledge in the diagnostic process (including identifying novel disorders) and in planning management strategies. They strive to improve the early recognition and diagnosis of metabolic diseases, including through newborn screening. Metabolic Paediatricians work closely with laboratory scientists, metabolic dietitians, pharmacist specialists and nursing teams. They are research-active and keep up to date with the rapid and innovative developments in therapeutics for metabolic disorders. They are advocates for their patients, actively engaging in developing and commissioning high-quality services and evolving therapies. Sub-specialty Learning Outcomes 1. Recognises, assesses and manages the full range of acute paediatric inherited metabolic emergencies. 2. Demonstrates sound understanding of the full range of metabolic conditions and applies this knowledge to newly referred patients. 3. Counsels families of a patient with the diagnosis of an inherited metabolic disorder (IMD) detected through the newborn screening programme. 4. Explains the inheritance of IMD to families and applies this within a cultural context. 5. Liaises effectively with hospital and community specialist teams for managing paediatric inherited metabolic conditions, particularly with specialists such as dietitians, pharmacists, nurses and laboratory scientists. 6. Effectively works with paediatricians in district general hospitals and specialist centres to coordinate patient care, and maintains consistent quality in the context of a paediatric inherited metabolic medicine service. GMC Generic Professional Capabilities GPC 2, 3, 5 GPC 2, 3, 5 GPC 1, 2, 3, 4, 5 GPC 1, 2, 3, 4, 5 GPC 1, 2, 3, 4, 5 GPC 1, 2, 3, 4, 5, 6 7. Contributes to international collaborations and research. GPC 5, 6, 9 6 7
5 Key Capabilities Illustrations Takes responsibility for the holistic management of a child with the following conditions: Phenylketonuria (see Illustration A1 for details) Branched-chain organic aciduria (see Illustration B1 for details) Urea cycle disorder (see Illustration C2 for details) Glycogen storage disorder (see Illustration D1 for details) Galactosaemia, including dietary management and the early identification of need for educational support (see Illustration D2 for details) Medium-chain acyl-coa dehydrogenase (MCAD) deficiency, including the counselling of a new family from newborn screening and the management of intercurrent illnesses (see Illustration E1 for details) Long-chain fatty acid oxidation disorder, including dietary management and the management of intercurrent illnesses (see Illustration E2 for details) Lysosomal storage disorder (for which there is an approved treatment, see Illustration F1 for details) Advises senior colleagues on the investigation and management of a child with the following conditions: Hyperammonaemia in an acutely unwell child (see Illustration C1 for details) Hypoglycaemia Cholestasis, liver failure or hepatomegaly/hepatosplenomegaly Cardiomyopathy Dysmorphic features, corneal clouding/cataracts and/or skeletal dysplasia Neurological regression and/or myopathy Counsels families initially regarding the inheritance of metabolic disorders in conjunction with a clinical genetics service (see Illustration J1 for details). Contributes to effective and up-to-date local and regional multidisciplinary team (MDT) management of children with inherited disorders of metabolism (see Illustration J2 for details). Prescribes a range of specialised drugs for the treatment of inherited disorders of metabolism (e.g. enzyme replacement therapies, ammoniascavenging medications and other examples given in this syllabus). Utilises specialised metabolic investigations, where indicated, with appropriate interpretation and application to the diagnosis of a child with a suspected inherited metabolic disorder (see Illustration K for details). Undertakes the following procedures: skin biopsy lumbar puncture for neurotransmitter analysis GPC 2, 3, 5, 7 GPC 2, 3, 5, 7 GPC 1, 2, 3 GPC 1, 2, 3, 5 GPC 6 GPC 3 GPC 3 A Disorders of amino acid metabolism 1. Phenylketonuria examples of aspects of management to consider: a. Newborn screening for phenylketonuria technique, role and counselling for a new diagnosis b. Effect of hyperphenylalaninaemia on children and foetuses, including management of phenylketonuria in pregnancy c. Dietary treatment of phenylketonuria, including monitoring and prevention of nutritional deficiencies d. Drug treatment sapropterin dihydrochloride (roles and limitations) e. Testing for and treating the related defects of biopterin metabolism 2. Tyrosinaemia examples of aspects of management to consider: a. Drug treatment nitisinone (NTBC) b. Clinical presentations and the long-term complications of tyrosinaemia types 1, 2 and 3 c. Dietary treatment of tyrosinaemia types 1 and 2, including monitoring of a child on dietary treatment/ntbc d. Indications for liver transplantation in tyrosinaemia type 1 3. Homocystinuria examples of aspects of management to consider: a. Clinical presentation and long-term complications of classical homocystinuria b. Clinical presentation of remethylation defects c. Causes of combined homocystinuria and methylmalonic aciduria d. Drug treatment betaine and pyridoxine e. Dietary treatment of homocystinuria, including monitoring of a child on dietary or medical treatment f. Management and prevention of thromboembolic disease, including pregnancy g. Pyridoxine responsiveness test h. Newborn screening for homocystinuria technique, role and counselling for a new diagnosis 4. Maple syrup urine disease (MSUD) examples of aspects of management to consider: a. Clinical presentations b. Newborn screening technique, role and counselling for a new diagnosis c. Dietary treatment, including monitoring of a child on dietary treatment d. Management of acute MSUD, including extracorporeal therapy e. Management of acute illness in a child with MSUD, including the emergency protocol f. Indications for liver transplantation 5. Other aminoacidopathies to consider: a. Hyperornithinaemia with gyrate atrophy, including dietary treatment and complications b. Alkaptonuria, including the role of NTBC 8 9
6 B Disorders of organic acid metabolism 1. Branched-chain organic acidurias examples of aspects of management to consider: a. Propionic acidaemia clinical presentation b. Methylmalonic acidaemia clinical presentation c. Isovaleric acidaemia clinical presentation and newborn screening d. Dietary management of branched-chain organic acidurias, including monitoring e. Management of intercurrent illness, emergency regimen, and decompensation f. Ensuring adequate nutrition for children with organic acidaemias, including indications for enteral feeding g. Rarer organic acidurias (e.g. malonic aciduria) h. Drug treatment (KC5) L-carnitine, glycine and vitamin B12 preparations i. Indications for and arguments for and against organ transplantation in organic acidurias j. Different managements of biotin/vitamin-responsive organic acidurias, including the vitamin B12 responsiveness test 2. Glutaric aciduria examples of aspects of management to consider: a. Clinical presentation of glutaric aciduria type 1 b. Newborn screening for glutaric aciduria type 1 c. Dietary treatment and monitoring of a child with glutaric aciduria type 1 d. Treatment of dystonia in glutaric aciduria type 1 (including the role of deep brain stimulation) e. Management of acute illness in a child with glutaric aciduria type 1, including the emergency regimen f. Different presentations of L- and D-2-hydroxyglutaric aciduria C Hyperammonaemia and urea cycle disorders 1. Acute hyperammonaemia examples of aspects of management to consider: a. Clinical presentation and recognition of hyperammonaemia b. Methods of measuring blood ammonia and the effects of sampling and processing c. Causes of hyperammonaemia, including secondary causes d. Management of acute hyperammonaemia, including extracorporeal treatment 2. Urea cycle disorders examples of aspects of management to consider: a. The different presentations of N-Acetyl glutamate synthase (NAGS), Carbamoyl phosphate synthetase (CPS), Ornithine transcarbamylase (OTC), argininosuccinate synthetase (ASS), Argininosuccinate lyase (ASL) and arginase deficiencies b. The different managements and presentations of transport defects, including citrin deficiency, lysinuric protein intolerance and Hyperornithinemiahyperammonemia-homocitrullinuria (HHH) c. Dietary management of urea cycle disorders, including monitoring d. Emergency regimens for and management of intercurrent illness/ decompensations e. Ensuring adequate nutrition for children with urea cycle disorders, including indications for enteral feeding f. Drug treatment (KC5) N-carbamylglutamate, sodium benzoate, sodium phenylbutyrate, citrulline and L-arginine g. Indications for organ transplantation in urea cycle disorders D Disorders of carbohydrate metabolism 1. Glycogen storage diseases (GSDs) examples of aspects of management to consider: a. Different presentations of GSD 1a and 1b, including the management of neutropenia and inflammatory bowel disease b. Different presentations of GSD III, IV, VI and IX c. Different presentations of muscle GSDs, including GSD V, VII and IX d. Monitoring of a child on dietary treatment for GSD, including the use of glucose lactate profiles and continuous glucose monitoring e. Dietary treatment of GSDs associated with fasting intolerance, including the use of corn starch and enteral feedings f. Management of intercurrent illness and emergency regimens g. Indications for liver transplantation in GSD 2. Galactosaemia examples of aspects of management to consider: a. Clinical presentation of classical galactosaemia and the differential diagnosis of neonatal liver failure b. Long-term complications, including learning difficulties, and referral for educational support c. Recognition and management of ovarian failure in females d. Dietary treatment of galactosaemia and monitoring e. Molecular and enzymatic investigations of galactosaemia, including Duarte variants 3. Other rare carbohydrate metabolism disorders examples of conditions to consider: a. Fructosaemia b. Fructose 1,6-bisphosphatase deficiency c. Glucose transporter deficiency (GLUT1), including the use of the ketogenic diet d. Fanconi Bickel syndrome 10 11
7 E Disorders of fatty acid oxidation and ketone body metabolism 1. MCAD deficiency (MCADD): a. Newborn screening for MCADD technique, role and counselling for a new diagnosis b. Dietary treatment of MCADD, including emergency regimens and appropriate fasting tolerances in infancy 2. Long-chain fatty acid oxidation disorders: a. The different presentations of Very long-chain acyl-coa dehydrogenase deficiency (VLCAD deficiency), Long-chain 3-hydroxyacyl-CoA dehydrogenase (LCHAD) deficiency and mitochondrial Trifunctional protein deficiency (TFP) deficiency b. The different presentations of disorders of carnitine transport Carnitine palmitoyltransferase I (CPT1), Carnitine palmitoyltransferase 2 (CPT2), Carnitineacylcarnitine translocase (CACT) and carnitine transporter deficiencies c. Dietary treatment for a child with a long-chain fatty acid oxidation disorder, including monitoring d. Management and investigation of metabolic causes of rhabdomyolysis e. Management of intercurrent illness and emergency regimens in fatty acid oxidation disorders 3. Other disorders of fatty acid oxidation and ketone body metabolism: a. The different presentations and management of glutaric aciduria type 2 and Multiple Acyl-CoA-Dehydrogenase Deficiency (MADD) b. Drug treatment (KC5) riboflavin for some cases of MADD c. The different presentations and management of Short-chain acyl-coa dehydrogenase (SCAD) and Short chain 3-hydroxyacyl-CoA dehydrogenase (SCHAD) deficiencies d. The different presentations and management of ketolytic defects e.g. Methionine adenosyl transferase (MAT) and Succinyl-CoA:3-oxoacid CoA transferase (SCOT) deficiencies e. The different presentations and management of ketogenic defects (e.g. HMG CoA synthase and lyase deficiencies) F Lysosomal storage disorders 1. Lysosomal storage disorders (LSDs) for which there is an approved therapy examples of aspects of management to consider: a. The different clinical presentations and treatments for the mucopolysaccharidoses (I, II, IV and VI) b. The different clinical presentations and treatments for Fabry disease, Gaucher disease (I and III), Pompe disease, Danon disease and lysosomal acid lipase deficiency c. The different clinical presentations and treatments for Niemann Pick disease type C d. Drug treatments (KC5) laronidase, idursulfase, elosulfase alfa, galsulfase, agalsidase alfa/beta, imiglucerase, velaglucerase, alglucosidase alfa, sebelipase alfa, miglustat and migalastat e. Monitoring of children on enzyme replacement or substrate reduction, including awareness of agreed protocols for treatment monitoring and continuation f. Management of drug-associated reactions and side effects of approved treatments for LSDs g. Understanding of the indications for, choice and complications of central venous catheters for enzyme replacement h. Understanding of anaesthetic and surgical considerations for children with MPS disorders i. Indications for stem-cell transplantation for some LSDs 2. LSDs for which there is no approved therapy examples of aspects of management to consider: a. The different clinical presentations of Krabbe disease, metachromatic leukodystrophy and multiple sulfatase deficiency b. The different clinical presentations of Niemann Pick diseases (types A and B) and the mucopolysaccharidoses (III, VII and IX) c. The different clinical presentations of GM1 and GM2 gangliosidoses, mannosidosis and other oligosaccharidoses d. Familiarity with the current state of clinical trials of novel therapies for currently untreatable LSDs e. Indications for stem-cell transplantation for some otherwise untreatable LSDs f. Understanding of effective palliative care for degenerative diseases 12 13
8 G Disorders of lipid metabolism 1. Familial hypercholesterolaemia (FH) examples of aspects of management to consider: a. Diagnostic criteria and clinical signs of FH b. Drug treatment (KC5) indications, side effects and monitoring of cholesterollowering medications c. Dietary recommendations for FH d. Assessment of cardiovascular risk in patients with hypercholesterolaemia e. Treatments available for homozygous FH, including referral for liver transplantation 2. Rare disorders of lipid metabolism examples of aspects of management to consider: a. Clinical presentation and dietary treatment of lipoprotein lipase deficiency b. Disorders of cholesterol synthesis, including Smith Lemli Opitz syndrome and the use of cholesterol supplementation c. Clinical presentation and treatments of abetalipoproteinaemia and hypobetalipoproteinaemia H Mitochondrial disorders (may include a period of training in neurology) 1. Mitochondrial disease aspects of management to consider: a. The differing clinical presentations and long-term complications of Leigh syndrome, Mitochondrial encephalomyopathy, lactic acidosis, and strokelike episodes (MELAS), Myoclonic epilepsy with ragged red fibres (MERRF), Neuropathy, ataxia, and retinitis pigmentosa (NARP), Leber s hereditary optic neuropathy (LHON), Pearson syndrome, Kearns Sayre syndrome, Mitochondrial neurogastrointestinal encephalopathy syndrome (MNGIE) syndrome, Barth syndrome, ethylmalonic encephalopathy b. The different clinical presentations of disorders associated with mitochondrial DNA depletion, including Alpers syndrome c. The different clinical presentations and long-term complications of pyruvate dehydrogenase deficiency and pyruvate carboxylase deficiency d. Drug treatment (KC5) indications for and limitations of ubiquinone, biotin, riboflavin, thiamine and sodium dichloroacetate e. Advising appropriate investigations for an undiagnosed child with primary lactic acidosis, including diagnostic tissue biopsies f. Understanding of effective palliative care for degenerative diseases I Neurometabolic and other disorders (may include a period of training in neurology) 1. Neonatal seizures examples of conditions and aspects of management to consider: a. Nonketotic hyperglycinaemia b. Pyridoxine- and pyridoxal phosphate-dependent epilepsies c. Disorders of serine metabolism d. Disorders of purine metabolism, including sulphite oxidase deficiency and molybdenum cofactor deficiency e. Disorders of metal metabolism, including Menkes disease and Wilson s disease f. Drug treatments (KC5) indications and limitations of pyridoxine, pyridoxal phosphate, copper histidine injections, dextromethorphan, serine and cyclic PMP 2. Other neurometabolic disorders examples of conditions and aspects of management to consider: a. Disorders of peroxisomal biogenesis b. Single enzyme disorders of peroxisomal metabolism, including X-linked adrenoleukodystrophy c. Disorders of purine metabolism, including Lesch Nyhan syndrome d. Disorders of pyrimidine metabolism e. Disorders of neurotransmission f. Cerebral folate and creatine deficiency syndromes g. The different clinical presentations of, investigations for and management of the porphyrias, including the treatment of acute intermittent porphyria with haem arginate h. Drug treatments (KC5) indications for and limitations of drugs for Wilson s disease (e.g. L-dopa, folinic acid, 5-hydroxytryptophan, dextromethorphan and haem arginate) i. Management of X-linked adrenoleukodystrophy, including an awareness of Lorenzo s Oil and the indications for stem-cell transplantation 3. Other disorders examples of conditions and aspects of management to consider: a. The different clinical presentations of and diagnostic protocols for the congenital disorders of glycosylation b. The presentation, investigation and management of trimethylaminuria 14 15
9 J Genetics and generic skills (may include a period of training within clinical genetics) 1. Genetic testing and counselling examples of aspects to consider: a. Understanding and ability to explain simply the principles of autosomal recessive, dominant, X-linked and mitochondrial DNA inheritance patterns b. Understanding and ability to explain simply the principles of DNA mutation analysis and sequencing c. Understanding and ability to explain simply the different ways of performing antenatal or presymptomatic genetic diagnosis (and understanding of the cultural differences in attitudes towards these) d. Familiarity with clinical situations in which molecular testing may be an appropriate first-line investigation and the selection of appropriate samples for testing (e.g. genomic DNA vs cdna) e. Understanding issues regarding informed consent for DNA testing and whole exome or genome testing 2. Maintaining standards in inherited metabolic disorders examples of aspects to consider: a. Knowledge of external quality assurance schemes for laboratories b. Critical appraisal of published literature, including a working knowledge of medical statistics c. How to use online resources such as Online Mendelian Inheritance in Man (OMIM) to obtain up-to-date information on inherited metabolic disorders d. Participation in and keeping up to date with multicentre research studies of inherited metabolic disorders K Technical skills Is able to conduct: 1. Metabolic investigations examples to be familiar with: a. Acylcarnitines b. Urine organic acids, including Gas chromatography/mass spectrometry (GC/MS) data c. Quantitative amino acid profiles d. Enzyme assays e. Urinary glycosaminoglycan and oligosaccharide analysis f. Urine purine and pyrimidine data g. Lipid profiles/lipoprotein electrophoresis h. Plasma very long-chain fatty acids (and other investigations for peroxisomal disease) i. Molecular genetic analyses 2. Dynamic tests examples to be familiar with: a. Allopurinol loading test b. Penicillamine challenge c. Responsiveness tests to pyridoxine/pyridoxal phosphate and vitamin B12 3. Invasive investigations examples to be able to perform/recommend and/or interpret include: a. Muscle biopsy for respiratory chain analysis (recommend) b. Liver biopsy for enzymology (recommend) c. Skin biopsy for fibroblast culture and enzymology (perform; KC7a) d. Lumbar puncture for CSF neurotransmitters, glucose, catecholamines and amino acids e. Awareness of specific counselling for peri- and post-mortem sampling 16 17
10 Assessment Grid Key Capabilities Assessment / Supervised Learning Event suggestions This table suggests assessment tools which may be used to assess the Key Capabilities for these Learning Outcomes. This is not an exhaustive list, and trainees are permitted to use other methods within the RCPCH Assessment Strategy to demonstrate achievement of the Learning Outcome, where they can demonstrate these are suitable. (epaed Mini-CEX) Paediatric Mini Clinical Evaluation Paediatric Case-based Discussion(ePaed CbD) (DOP/AoP) Assessment of Performance Directly Observed Procedure / Acute Care Assessment Tool (ACAT) Discussion of Correspondence (DOC) Clinical Leadership Assessment Skills (LEADER) Handover Assessment Tool (HAT) Paediatric Multi Source Feedback (epaed MSF) Paediatric Carers for Children Feedback (Paed CCF) Other Key Capabilities Takes responsibility for the holistic management of a child with the following conditions: Phenylketonuria (see Illustration A1 for details) Branched-chain organic aciduria (see Illustration B1 for details) Urea cycle disorder (see Illustration C2 for details) Glycogen storage disorder (see Illustration D1 for details) Takes responsibility for the holistic management of a child with the following conditions: Galactosaemia, including dietary management and the early identification of need for educational support (see Illustration D2 for details) Medium-chain acyl-coa dehydrogenase (MCAD) deficiency, including the counselling of a new family from newborn screening and the management of intercurrent illnesses (see Illustration E1 for details) Long-chain fatty acid oxidation disorder, including dietary management and the management of intercurrent illnesses (see Illustration E2 for details) Lysosomal storage disorder (for which there is an approved treatment, see illustration F1 for details) Paediatric Mini Clinical Evaluation (epaed Mini-CEX) Paediatric Case-based Discussion(ePaed CbD) Assessment / Supervised Learning Event suggestions (DOP/AoP) Assessment of Performance Directly Observed Procedure / Discussion of Correspondence (DOC) Acute Care Assessment Tool (ACAT) Handover Assessment Tool (HAT) Clinical Leadership Assessment Skills (LEADER) Paediatric Multi Source Feedback (epaed MSF) Paediatric Carers for Children Feedback (Paed CCF) Other Advises senior colleagues on the investigation and management of a child with the following conditions: Hyperammonaemia in an acutely unwell child (see Illustration C1 for details). Hypoglycaemia. Cholestasis, liver failure or hepatomegaly/ hepatosplenomegaly. Cardiomyopathy. Dysmorphic features, corneal clouding/ cataracts and/or skeletal dysplasia. Neurological regression and/or myopathy Counsels families initially regarding the inheritance of metabolic disorders in conjunction with a clinical genetics service (see Illustration J1 for details). Contributes to effective and up-to-date local and regional multidisciplinary team (MDT) management of children with inherited disorders of metabolism (see Illustration J2 for details). Prescribes a range of specialised drugs for the treatment of inherited disorders of metabolism (e.g. enzyme replacement therapies, ammoniascavenging medications and other examples given in this syllabus). Utilises specialised metabolic investigations, where indicated, with appropriate interpretation and application to the diagnosis of a child with a suspected inherited metabolic disorder (see Illustration K for details). Undertakes the following procedures: skin biopsy. lumbar puncture for neurotransmitter analysis 18 19
11 RCPCH Progress: Paediatric Inherited Metabolic Medicine Level 3 Syllabus This information is correct and up to date at time of Publication. RCPCH 2017
Training Syllabus CLINICAL SYLLABUS
 Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE
 SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
General Paediatrics Syllabus
 RCPCH Progress Paediatric curriculum for excellence General Paediatrics Syllabus Level 3 Paediatrics Specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College
RCPCH Progress Paediatric curriculum for excellence General Paediatrics Syllabus Level 3 Paediatrics Specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College
Paediatric Respiratory Medicine
 RCPCH Progress Paediatric curriculum for excellence Paediatric Respiratory Medicine Level 3 Paediatrics Sub-specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The
RCPCH Progress Paediatric curriculum for excellence Paediatric Respiratory Medicine Level 3 Paediatrics Sub-specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The
Current Management and Future Developments in Metabolic Disease
 Current Management and Future Developments in Metabolic Disease APAGBI Annual Scientific Meeting Friday 15 th May 2015 Dr Saikat Santra Birmingham Children s Hospital, UK Outline Metabolic disorders in
Current Management and Future Developments in Metabolic Disease APAGBI Annual Scientific Meeting Friday 15 th May 2015 Dr Saikat Santra Birmingham Children s Hospital, UK Outline Metabolic disorders in
Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff
 Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Diagnose a broad range of metabolic disorders with a single test, Global MAPS
 PEDIATRIC Assessing or diagnosing a metabolic disorder commonly requires several tests. Global Metabolomic Assisted Pathway Screen, commonly known as Global MAPS, is a unifying test for analyzing hundreds
PEDIATRIC Assessing or diagnosing a metabolic disorder commonly requires several tests. Global Metabolomic Assisted Pathway Screen, commonly known as Global MAPS, is a unifying test for analyzing hundreds
Presentation and investigation of mitochondrial disease in children
 Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
INBORN ERRORS OF METABOLISM (IEM) IAP UG Teaching slides
 INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up
 HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
Paediatric Nephrology
 RCPCH Progress Paediatric curriculum for excellence Paediatric Nephrology Level 3 Paediatrics Sub-specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College
RCPCH Progress Paediatric curriculum for excellence Paediatric Nephrology Level 3 Paediatrics Sub-specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College
Paediatric Neurology RCPCH. Level 3 Paediatrics Sub-Specialty Syllabus. Paediatric curriculum for excellence
 RCPCH Progress Paediatric curriculum for excellence Paediatric Neurology Level 3 Paediatrics Sub-Specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College
RCPCH Progress Paediatric curriculum for excellence Paediatric Neurology Level 3 Paediatrics Sub-Specialty Syllabus Version 1 Approved by the GMC for implementation from 1st August 2018 The Royal College
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Metabolic Changes in ASD. Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius
 Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
COMMON INHERITED METABOLIC CONDITIONS IN SOUTH AFRICA DIAGNOSING RARE DISEASE IN GENETICALLY UNIQUE AND UNDERSTUDIED POPULATION GROUPS
 COMMON INHERITED METABOLIC CONDITIONS IN SOUTH AFRICA DIAGNOSING RARE DISEASE IN GENETICALLY UNIQUE AND UNDERSTUDIED POPULATION GROUPS S MELDAU, G VAN DER WATT INHERITED METABOLIC DISEASES GROUP UCT /
COMMON INHERITED METABOLIC CONDITIONS IN SOUTH AFRICA DIAGNOSING RARE DISEASE IN GENETICALLY UNIQUE AND UNDERSTUDIED POPULATION GROUPS S MELDAU, G VAN DER WATT INHERITED METABOLIC DISEASES GROUP UCT /
Inborn Errors of Metabolism (IEM)
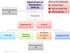 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
7 Medical Genetics. Hemoglobinopathies. Hemoglobinopathies. Protein and Gene Structure. and Biochemical Genetics
 SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015
 Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Childhood epilepsy: the biochemical epilepsies. Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary
 Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
The laboratory investigation of lactic acidaemia. J Bonham/T Laing
 The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA
 UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
Understanding metabolic disease
 Understanding metabolic disease Let s build a restaurant Chris Hendriksz Birmingham Children s Hospital 2006 The Task Let s build a restaurant! 2 Partners join to draw the plan. How can we change the
Understanding metabolic disease Let s build a restaurant Chris Hendriksz Birmingham Children s Hospital 2006 The Task Let s build a restaurant! 2 Partners join to draw the plan. How can we change the
Inborn Errors of Metabolism Clinical Approach to Diagnosis and Treatment
 Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Nutritional Interventions in Primary Mitochondrial Disorders
 Nutritional Interventions in Primary Mitochondrial Disorders Carolyn J Ellaway MBBS PhD FRACP CGHGSA Genetic Metabolic Disorders Service Sydney Children s Hospital Network Disciplines of Child and Adolescent
Nutritional Interventions in Primary Mitochondrial Disorders Carolyn J Ellaway MBBS PhD FRACP CGHGSA Genetic Metabolic Disorders Service Sydney Children s Hospital Network Disciplines of Child and Adolescent
National Metabolic Biochemistry Network Best Practice Guidelines. The Biochemical Investigation of Fits and Seizures for Inherited Metabolic Disorders
 Introduction National Metabolic Biochemistry Network Best Practice Guidelines The Biochemical Investigation of Fits and Seizures for Inherited Metabolic Disorders These guidelines describe the differential
Introduction National Metabolic Biochemistry Network Best Practice Guidelines The Biochemical Investigation of Fits and Seizures for Inherited Metabolic Disorders These guidelines describe the differential
Mitochondrial Diseases
 Mitochondrial Diseases Simon Heales SWIM Conference Taunton, November 29 th 2018 Respiratory Failure Cardiomyopathy Optic Atrophy / Retinitis Pigmentosa Seizures / Developmental delay Liver Failure Deafness
Mitochondrial Diseases Simon Heales SWIM Conference Taunton, November 29 th 2018 Respiratory Failure Cardiomyopathy Optic Atrophy / Retinitis Pigmentosa Seizures / Developmental delay Liver Failure Deafness
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD
 Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Title: Assessing Recommendations Related To Timeliness of Newborn Screening
 Title: Assessing Recommendations Related To Timeliness of Newborn Screening Purpose: In January 2014, the Secretary s Discretionary Advisory Committee on Heritable Diseases on Newborns and Children (Committee)
Title: Assessing Recommendations Related To Timeliness of Newborn Screening Purpose: In January 2014, the Secretary s Discretionary Advisory Committee on Heritable Diseases on Newborns and Children (Committee)
Fatty acid oxidation. Naomi Rankin
 Fatty acid oxidation Naomi Rankin Fatty acid oxidation Provides energy to muscles from lipid stores, spares glucose for the brain Lipolysis of triglycerides results in FFA, mainly C16 and C18 FA oxidation
Fatty acid oxidation Naomi Rankin Fatty acid oxidation Provides energy to muscles from lipid stores, spares glucose for the brain Lipolysis of triglycerides results in FFA, mainly C16 and C18 FA oxidation
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital
 e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
Fatty Acid Oxidation Disorders- an update. Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London
 Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Post mortem investigation of Inherited Metabolic Disease - the last opportunity for a diagnosis -
 Post mortem investigation of Inherited Metabolic Disease - the last opportunity for a diagnosis - Dr Simon Olpin Lead Clinical Scientist in Inherited Metabolic Disease Sheffield Children s Hospital SIDS/SUDI
Post mortem investigation of Inherited Metabolic Disease - the last opportunity for a diagnosis - Dr Simon Olpin Lead Clinical Scientist in Inherited Metabolic Disease Sheffield Children s Hospital SIDS/SUDI
For Your Baby s Health Department of Health
 Newborn Screening For Your Baby s Health Department of Health Why is my baby tested? To help make sure your baby will be as healthy as possible. The blood test provides important information about your
Newborn Screening For Your Baby s Health Department of Health Why is my baby tested? To help make sure your baby will be as healthy as possible. The blood test provides important information about your
Metabolic Disorders Screened Overseas but not Screened in Australia Condition Features Inherited Diagnosis Treatment Newborn Screen
 Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
Further expansion of the neonatal screening panel in the Netherlands
 Further expansion of the neonatal screening panel in the Netherlands J.Gerard Loeber APHL-NBSGT, St.Louis (MO), USA 290216 Population Area Newborns 6.01 million 0.35:1 16.8 million 180,693 sq km 4.3:1
Further expansion of the neonatal screening panel in the Netherlands J.Gerard Loeber APHL-NBSGT, St.Louis (MO), USA 290216 Population Area Newborns 6.01 million 0.35:1 16.8 million 180,693 sq km 4.3:1
NEUROMETABOLIC DISORDERS IN ADULT NEUROLOGY: AN OVERVIEW
 NEUROMETABOLIC DISORDERS IN ADULT NEUROLOGY: AN OVERVIEW Dr. Alessandro Burlina, MD, PhD Director of the Neurological Unit, St. Bassiano Hospital, Bassano del Grappa, Consultant in Adult Neurometabolic
NEUROMETABOLIC DISORDERS IN ADULT NEUROLOGY: AN OVERVIEW Dr. Alessandro Burlina, MD, PhD Director of the Neurological Unit, St. Bassiano Hospital, Bassano del Grappa, Consultant in Adult Neurometabolic
When users open the application interface, the starting page presents a disclaimer. Upon agreeing to the
 Walkthrough of IEMbase When users open the application interface, the starting page presents a disclaimer. Upon agreeing to the disclaimer, users are directed to the main page, which presents a search
Walkthrough of IEMbase When users open the application interface, the starting page presents a disclaimer. Upon agreeing to the disclaimer, users are directed to the main page, which presents a search
Neonatal Guidelines. Chapter 10: Metabolic V Date Revised : January 2017 Ratified 6 th February Date for Review: 1 st of March 2021
 Neonatal Guidelines Chapter 10: Metabolic V2017.1 Specialty: Neonatal Medicine Revised by: Jean Matthes Date Revised : January 2017 Ratified 6 th February 2017 Approved by: ABMU Joint Perinatal Forum Date
Neonatal Guidelines Chapter 10: Metabolic V2017.1 Specialty: Neonatal Medicine Revised by: Jean Matthes Date Revised : January 2017 Ratified 6 th February 2017 Approved by: ABMU Joint Perinatal Forum Date
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM
 LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
Robert Barski. Biochemical Genetics St James s University Hospital, Leeds. MetBioNet IEM Introductory Training
 Robert Barski Biochemical Genetics St James s University Hospital, Leeds Lactate is produced as the fate of anaerobic metabolism of pyruvate. It is an important intermediary metabolite especially with
Robert Barski Biochemical Genetics St James s University Hospital, Leeds Lactate is produced as the fate of anaerobic metabolism of pyruvate. It is an important intermediary metabolite especially with
Inborn Errors of Metabolism. Metabolic Pathway. Digestion and Fasting. How is Expanded Newborn Screening Different? MS/MS. The body is a factory.
 Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
BROADENING YOUR PATIENT S OPTIONS FOR GENETIC CARRIER SCREENING.
 BROADENING YOUR PATIENT S OPTIONS FOR GENETIC CARRIER SCREENING. The Inheritest SM Carrier Screen provides relevant genetic screening for many inherited diseases found throughout the pan-ethnic US population.
BROADENING YOUR PATIENT S OPTIONS FOR GENETIC CARRIER SCREENING. The Inheritest SM Carrier Screen provides relevant genetic screening for many inherited diseases found throughout the pan-ethnic US population.
Neurodegenerative disorders: an approach to investigation. Robert Robinson Practical Paediatric Neurology Study Days April 2018
 Neurodegenerative disorders: an approach to investigation Robert Robinson Practical Paediatric Neurology Study Days April 2018 Aims An approach to investigating and diagnosing young children with progressive
Neurodegenerative disorders: an approach to investigation Robert Robinson Practical Paediatric Neurology Study Days April 2018 Aims An approach to investigating and diagnosing young children with progressive
Medical Foods for Inborn Errors of Metabolism
 Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
A. disorders of amino acid metabolism classical phenylketonuria and hyperphenylalaninemia
 OMIM # FULL NAME A. disorders of amino acid metabolism 1 261600 classical phenylketonuria and hyperphenylalaninemia 2 261640 phenylketonuria due to PTPS deficiency 3 261630 phenylketonuria due to DHPR
OMIM # FULL NAME A. disorders of amino acid metabolism 1 261600 classical phenylketonuria and hyperphenylalaninemia 2 261640 phenylketonuria due to PTPS deficiency 3 261630 phenylketonuria due to DHPR
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition
 Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Introduction to Organic Acidemias. Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.
 Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE. Bwee Tien Poll-The Amsterdam UMC The Netherlands
 CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
Doenças Hereditárias do Metabolismo: de Garrod às Ciências Ómicas
 Doenças Hereditárias do Metabolismo: de Garrod às Ciências Ómicas Isabel Tavares de Almeida Lab. Met & Gen. FFULisboa XIII Curso Básico de Doenças Hereditárias do Metabolismo Coimbra, 5 a 7 Dezembro 2016
Doenças Hereditárias do Metabolismo: de Garrod às Ciências Ómicas Isabel Tavares de Almeida Lab. Met & Gen. FFULisboa XIII Curso Básico de Doenças Hereditárias do Metabolismo Coimbra, 5 a 7 Dezembro 2016
Information for health professionals
 Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Inborn Error Of Metabolism :
 Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Inherited Metabolic Disease
 IMD and Newborn Screening Specialist Portfolio Tutorial Jenna Waldron 17th March 2014 Inherited Metabolic Disease What is IMD? Gene mutations prevent synthesis of protein or cause synthesis of abnormal
IMD and Newborn Screening Specialist Portfolio Tutorial Jenna Waldron 17th March 2014 Inherited Metabolic Disease What is IMD? Gene mutations prevent synthesis of protein or cause synthesis of abnormal
An Introduction to mitochondrial disease.
 9 th September 2017 An Introduction to mitochondrial disease. Dr Andy Schaefer Consultant Neurologist and Clinical Lead NHS Highly Specialised Rare Mitochondrial Disease Service and Wellcome Trust Centre
9 th September 2017 An Introduction to mitochondrial disease. Dr Andy Schaefer Consultant Neurologist and Clinical Lead NHS Highly Specialised Rare Mitochondrial Disease Service and Wellcome Trust Centre
MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES
 NEWBORN SCREENING Protecting your newborn MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES [ 1 ] NEWBORN SCREENING [ 2 ] FREQUENTLY ASKED QUESTIONS [ 4 ] DISORDERS INCLUDED IN NEWBORN SCREENING [ 12 ]
NEWBORN SCREENING Protecting your newborn MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES [ 1 ] NEWBORN SCREENING [ 2 ] FREQUENTLY ASKED QUESTIONS [ 4 ] DISORDERS INCLUDED IN NEWBORN SCREENING [ 12 ]
CHRONIC MYELOGENOUS LEUKEMIA
 CHRONIC MYELOGENOUS LEUKEMIA SHUFFLING THE GENETIC DECK IN CML 9 9 (q+) 22 Ph (22q-) bcr bcr-abl abl Fusion protein causes cancer GLEEVEC AND BCR-ABL FUSION PROTEIN GENETIC MEDICINE A. Genetic diseases
CHRONIC MYELOGENOUS LEUKEMIA SHUFFLING THE GENETIC DECK IN CML 9 9 (q+) 22 Ph (22q-) bcr bcr-abl abl Fusion protein causes cancer GLEEVEC AND BCR-ABL FUSION PROTEIN GENETIC MEDICINE A. Genetic diseases
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism
 Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet
 Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Newborn Metabolic Screening Programme. Annual Report
 Newborn Metabolic Screening Programme Annual Report January to December 2016 1 Disclaimer This publication reports on information provided to the Ministry of Health by the Auckland District Health Board.
Newborn Metabolic Screening Programme Annual Report January to December 2016 1 Disclaimer This publication reports on information provided to the Ministry of Health by the Auckland District Health Board.
Newborn Bloodspot Screening (NBS) Training for Health Visitors. December 2017
 Newborn Bloodspot Screening (NBS) Training for Health Visitors www.newbornbloodspotscreening.wales.nhs.uk December 2017 Aims To enable you to gain a clear understanding of the following: Aim and rationale
Newborn Bloodspot Screening (NBS) Training for Health Visitors www.newbornbloodspotscreening.wales.nhs.uk December 2017 Aims To enable you to gain a clear understanding of the following: Aim and rationale
Inborn errors of metabolism
 ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
Slide 1: Newborn Bloodspot Screening for Medium-chain Acyl-CoA Dehydrogenase Deficiency (MCADD)
 Slide 1: Newborn Bloodspot Screening for Medium-chain Acyl-CoA Dehydrogenase Deficiency (MCADD) The information has been produced with thanks to the NHS Newborn Blood Spot Screening Programme. 1 Slide
Slide 1: Newborn Bloodspot Screening for Medium-chain Acyl-CoA Dehydrogenase Deficiency (MCADD) The information has been produced with thanks to the NHS Newborn Blood Spot Screening Programme. 1 Slide
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
ESPEN Congress Madrid 2018
 ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
LILY FOUNDATION. An Introduction to Ketogenic Diets. Susan Wood. Matthew s Friends. Registered Dietitian Adults & Paediatrics
 LILY FOUNDATION An Introduction to Ketogenic Diets Susan Wood Registered Dietitian Adults & Paediatrics Matthew s Friends What is a ketogenic diet? A MEDICAL treatment. Mimics fasting metabolism Alters
LILY FOUNDATION An Introduction to Ketogenic Diets Susan Wood Registered Dietitian Adults & Paediatrics Matthew s Friends What is a ketogenic diet? A MEDICAL treatment. Mimics fasting metabolism Alters
Newborn Metabolic Screening Programme Annual Report
 Newborn Metabolic Screening Programme Annual Report January to December 2015 Disclaimer This publication reports on information provided to the Ministry of Health by the Auckland District Health Board.
Newborn Metabolic Screening Programme Annual Report January to December 2015 Disclaimer This publication reports on information provided to the Ministry of Health by the Auckland District Health Board.
All diseases on Foresight
 All diseases on Foresight Disease 11-Beta-Hydroxylase- Deficient Congenital Adrenal Hyperplasia 21-Hydroxylase-Deficient Congenital Adrenal Hyperplasia 3-Hydroxy-3-Methylglutaryl- CoA Lyase Deficiency
All diseases on Foresight Disease 11-Beta-Hydroxylase- Deficient Congenital Adrenal Hyperplasia 21-Hydroxylase-Deficient Congenital Adrenal Hyperplasia 3-Hydroxy-3-Methylglutaryl- CoA Lyase Deficiency
Detection of inborn errors of metabolism in the newborn
 Arch Dis Child Fetal Neonatal Ed 2001;84:F205 F210 F205 REVIEW Willink Biochemical Genetics Unit, Manchester M27 4HA, UK A Chakrapani M A Cleary J E Wraith Correspondence to: Dr Cleary maureen@willink.demon.co.uk
Arch Dis Child Fetal Neonatal Ed 2001;84:F205 F210 F205 REVIEW Willink Biochemical Genetics Unit, Manchester M27 4HA, UK A Chakrapani M A Cleary J E Wraith Correspondence to: Dr Cleary maureen@willink.demon.co.uk
NEWBORN SCREENING. health.mo.gov/newbornscreening MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES
 NEWBORN SCREENING health.mo.gov/newbornscreening MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES Table of Contents NEWBORN SCREENING...1 FREQUENTLY ASKED QUESTIONS...2 DISORDERS INCLUDED IN NEWBORN SCREENING...4
NEWBORN SCREENING health.mo.gov/newbornscreening MISSOURI DEPARTMENT OF HEALTH AND SENIOR SERVICES Table of Contents NEWBORN SCREENING...1 FREQUENTLY ASKED QUESTIONS...2 DISORDERS INCLUDED IN NEWBORN SCREENING...4
Acylcarnitine measurement in blood spots: methodological aspects, problems and pitfalls with reference to the ERNDIM QA scheme
 Acylcarnitine measurement in blood spots: methodological aspects, problems and pitfalls with reference to the ERNDIM QA scheme Charles Turner Laboratory Guy s Hospital (Evelina Childrens Hospital, St Thomas
Acylcarnitine measurement in blood spots: methodological aspects, problems and pitfalls with reference to the ERNDIM QA scheme Charles Turner Laboratory Guy s Hospital (Evelina Childrens Hospital, St Thomas
MetBioNet Best Practice Guidelines. Investigation of an inherited metabolic cause of cardiomyopathy
 Introduction MetBioNet Best Practice Guidelines Investigation of an inherited metabolic cause of Inborn errors of metabolism (IEM) account for at least 5% of cases of. In some disorders, is the major cause
Introduction MetBioNet Best Practice Guidelines Investigation of an inherited metabolic cause of Inborn errors of metabolism (IEM) account for at least 5% of cases of. In some disorders, is the major cause
BCM 225 LECTURE ON INBORN ERRORS OF METABOLISM OJEMEKELE O.
 BCM 225 LECTURE ON INBORN ERRORS OF METABOLISM BY OJEMEKELE O. OUTLINE (week 11 and 12) Inborn errors of carbohydrate metabolism Inborn errors of amino acid metabolism Inborn errors of fatty acid metabolism
BCM 225 LECTURE ON INBORN ERRORS OF METABOLISM BY OJEMEKELE O. OUTLINE (week 11 and 12) Inborn errors of carbohydrate metabolism Inborn errors of amino acid metabolism Inborn errors of fatty acid metabolism
inborn errors of metabolism biochemical basis
 inborn errors of metabolism biochemical basis What is an inborn error of metabolism (IEM)? Genetically determined biochemical disorders, that affect an individual s ability to convert nutrients or to use
inborn errors of metabolism biochemical basis What is an inborn error of metabolism (IEM)? Genetically determined biochemical disorders, that affect an individual s ability to convert nutrients or to use
MEDICAL COVERAGE GUIDELINES ORIGINAL EFFECTIVE DATE: 12/19/17 SECTION: MEDICINE LAST REVIEW DATE: LAST CRITERIA REVISION DATE: ARCHIVE DATE:
 MEDICAL FOODS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are
MEDICAL FOODS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are
When to think about metabolic disorders in adulthood? Wouter Meersseman
 When to think about metabolic disorders in adulthood? Wouter Meersseman General Internal Medicine Adult Metabolic Clinic Wouter Meersseman, Leuven, Belgium Man, 25 year-old Normal development From 15 months
When to think about metabolic disorders in adulthood? Wouter Meersseman General Internal Medicine Adult Metabolic Clinic Wouter Meersseman, Leuven, Belgium Man, 25 year-old Normal development From 15 months
Most common is the congenital adrenogenital syndrome (AGS) or congenital adrenal hyperplasia (CAH) due to 21-hydroxylase deficiency.
 Newborn Screening Examination parameters: TSH-neonatal (hypothyreosis), 17-OH progesterone (AGS), galactose (galactosemia), galactose-uridyl transferase (galacto semia), biotinidase (biotinidase ), phenylalanine
Newborn Screening Examination parameters: TSH-neonatal (hypothyreosis), 17-OH progesterone (AGS), galactose (galactosemia), galactose-uridyl transferase (galacto semia), biotinidase (biotinidase ), phenylalanine
REQUISITION FORM NOTE: ALL FORMS MUST BE FILLED OUT COMPLETELY FOR SAMPLE TO BE PROCESSED. Last First Last First
 #: DEPARTMENT OF NEUROLOGY COLUMBIA COLLEGE OF PHYSICIANS & SURGEONS Room 4-420 630 West 168th Street, New York, NY 10032 Telephone #: 212-305-3947 Fax#: 212-305-3986 REQUISITION FORM NOTE: ALL FORMS MUST
#: DEPARTMENT OF NEUROLOGY COLUMBIA COLLEGE OF PHYSICIANS & SURGEONS Room 4-420 630 West 168th Street, New York, NY 10032 Telephone #: 212-305-3947 Fax#: 212-305-3986 REQUISITION FORM NOTE: ALL FORMS MUST
Metabolic diseases of the liver
 Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company Chapter 30 Outline Amino acids are obtained from the
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company Chapter 30 Outline Amino acids are obtained from the
Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when
 CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
Urea Cycle Disorders Prior Authorization Program Summary
 Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
Beyond the case for NBS in South Africa. Chris Vorster 28/05/2016
 Beyond the case for NBS in South Africa Chris Vorster 28/05/2016 The case for NBS in SA Economic justification Cost Utility analysis = Cost/QALY GDP/Capita Immediate implementation (WHO) Political justification
Beyond the case for NBS in South Africa Chris Vorster 28/05/2016 The case for NBS in SA Economic justification Cost Utility analysis = Cost/QALY GDP/Capita Immediate implementation (WHO) Political justification
TRANSAMINATION AND UREA CYCLE
 TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
Newborn Metabolic Screening Programme
 Newborn Metabolic Screening Programme Annual Report January to December 2017 Released 2018 health.govt.nz Disclaimer This publication reports on information provided to the Ministry of Health by the Auckland
Newborn Metabolic Screening Programme Annual Report January to December 2017 Released 2018 health.govt.nz Disclaimer This publication reports on information provided to the Ministry of Health by the Auckland
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable
 Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
VLCAD At a Glance. Before VLCAD was included on the newborn screening test, three types of VLCAD were recognized by the severity of the condition:
 VLCAD At a Glance VLCAD is one of several *Fatty Acid Oxidation Disorders (FAOD) in which there is an inability to break down certain fats, caused by an enzyme deficiency. This results in a decreased ability
VLCAD At a Glance VLCAD is one of several *Fatty Acid Oxidation Disorders (FAOD) in which there is an inability to break down certain fats, caused by an enzyme deficiency. This results in a decreased ability
UREA CYCLE DISORDERS - The What, Why, How and When
 UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
MSUD HCU Tyrosinaemia MMA/PA IVA (for PKU cooler see pages 11-13)
 (for PKU see pages 11-13) + Description A food for special medical purposes. Cooler is a ready-to-drink protein substitute containing essential and non-essential amino acids (but excluding the offending
(for PKU see pages 11-13) + Description A food for special medical purposes. Cooler is a ready-to-drink protein substitute containing essential and non-essential amino acids (but excluding the offending
Newborn Screening in Manitoba. Information for Health Care Providers
 Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
NEWBORN SCREENING. in Massachusetts: Answers for You and Your Baby. University of Massachusetts Medical School
 University of Massachusetts Medical School NEWBORN SCREENING in Massachusetts: Answers for You and Your Baby New England Newborn Screening Program Biotech 4, 2nd Floor UMass Medical School 377 Plantation
University of Massachusetts Medical School NEWBORN SCREENING in Massachusetts: Answers for You and Your Baby New England Newborn Screening Program Biotech 4, 2nd Floor UMass Medical School 377 Plantation
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
Newborn Screening: Focus on Treatment
 Newborn Screening: Focus on Treatment Alan R. Fleischman, M.D. Senior Vice President and Medical Director March of Dimes National Conference of State Legislatures July 21, 2008 Newborn Screening: A Public
Newborn Screening: Focus on Treatment Alan R. Fleischman, M.D. Senior Vice President and Medical Director March of Dimes National Conference of State Legislatures July 21, 2008 Newborn Screening: A Public
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese. DOI: /neo.
 Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
Inborn Errors of Metabolism
 30 Inborn Errors of Metabolism Inborn errors of metabolism (IEM) are disorders in which there is a block in the normal metabolic pathway that is caused by a genetic defect of a specific enzyme. The number
30 Inborn Errors of Metabolism Inborn errors of metabolism (IEM) are disorders in which there is a block in the normal metabolic pathway that is caused by a genetic defect of a specific enzyme. The number
Metabolic Muscle Diseases
 Metabolic Muscle Diseases Dr Tim Hutchin, Birmingham Children s Hospital Jan 13, 2012 Metabolic myopathies are heterogeneous conditions with defects of muscle energy metabolism that result in predominantly
Metabolic Muscle Diseases Dr Tim Hutchin, Birmingham Children s Hospital Jan 13, 2012 Metabolic myopathies are heterogeneous conditions with defects of muscle energy metabolism that result in predominantly
Investigation of metabolic encephalopathy
 Investigation of metabolic encephalopathy Encephalopathy may be a presenting sign in a wide range of medical conditions. G F van der Watt, FCPath (SA) Chem, MMed, MB ChB, DA (SA) Principal Pathologist
Investigation of metabolic encephalopathy Encephalopathy may be a presenting sign in a wide range of medical conditions. G F van der Watt, FCPath (SA) Chem, MMed, MB ChB, DA (SA) Principal Pathologist
