Diagnostic examination of the child with urolithiasis or nephrocalcinosis
|
|
|
- Darleen O’Neal’
- 6 years ago
- Views:
Transcription
1 Pediatr Nephrol (2010) 25: DOI /s x EDUCATIONAL REVIEW Diagnostic examination of the child with urolithiasis or nephrocalcinosis Bernd Hoppe & Markus J. Kemper Received: 28 August 2008 / Revised: 13 November 2008 / Accepted: 13 November 2008 / Published online: 23 December 2008 # IPNA 2008 Abstract Urolithiasis and nephrocalcinosis are more frequent in children then currently anticipated, but still remain under- or misdiagnosed in a significant proportion of patients, since symptoms and signs may be subtle or misleading. All children with colicky abdominal pain or macroscopic hematuria should be examined thoroughly for urolithiasis. Also, other, more general, abdominal manifestations can be the first symptoms of renal stones. The patients and their family histories, as well as physical examination, are important initial steps for diagnostic evaluation. Thereafter, diagnostic imaging should be aimed at the location of calculi but also at identification of urinary tract anomalies or acute obstruction due to stone disease. This can often be accomplished by ultrasound examination alone, but sometimes radiological methods such as plain abdominal films or more sensitive nonenhanced computed tomography are necessary. Since metabolic causes are frequent in children, diagnostic evaluation should be meticulous so that metabolic disorders that cause recurrent urolithiasis or even renal failure, such as the primary hyperoxalurias and others, can be ruled out. The stone is not the disease itself; it is only one serious sign! Therefore, thorough and early diagnostic examination is mandatory for every infant and child with the first stone event, or with nephrocalcinosis. B. Hoppe (*) Department of Pediatrics, Division of Pediatric Nephrology, University Children s Hospital Cologne, Kerpenerstr. 62, Cologne, Germany bernd.hoppe@uk-koeln.de M. J. Kemper Department of Pediatrics, Division of Pediatric Nephrology, University Hospital Medical Center Hamburg-Eppendorf, Hamburg, Germany Keywords Urolithiasis. Nephrocalcinosis. Children. Diagnostics Introduction Different incidence rates and aetiological factors are reported in children with urolithiasis or nephrocalcinosis, reflecting differences in geographic, genetic and socioeconomic background as well as the source of the series and the study design [1]. While the exact rates for nephrocalcinosis are unknown, the incidence of urolithiasis in childhood is believed to be approximately 10% of that in adults, which is around 5% in industrialized countries [2]. Since a significant proportion of patients remains undiagnosed or misdiagnosed (incidental discovery reported in 15 40%), numbers should be interpreted with caution [3]. In specific parts of the world prevalence rates are significantly higher and compare to those of adults [4]. Urolithiasis appears in all pediatric age groups, but a male predominance analogous to that in adult patients is observed. However, urolithiasis in childhood differs substantially from that in adults with regard to aetiology, symptoms and signs, imaging techniques and treatment [5, 6]. Approximately 40% of children with urolithiasis have a positive family history of kidney stones, and most of the children have a metabolic background of stone disease. Hence, specific and intensive diagnostic examination is necessary for every child experiencing even a single kidney stone event, to prevent recurrence of disease or even a disastrous outcome with kidney failure and end-stage renal disease [7]. Systematic diagnostic evaluation starts with a detailed medical history, followed by careful imaging studies (primarily avoiding plain X-ray) and specific urine analysis
2 404 Pediatr Nephrol (2010) 25: strategies. All diagnostic steps lead way to the determination of the pathophysiological background of stone disease [8], in order to initiate early and appropriate treatment to prevent recurrence. In this respect it always has to be kept in mind that kidney stone(s) or nephrocalcinosis are the sign (s) of the disease, but not the disease itself! The following teaching paper details the necessary steps of diagnostic examination of the child with stones or nephrocalcinosis. The stepwise procedure is also shown in Table 1. Medical history Obtaining a thorough medical history followed by a careful physical examination seems to have become a lost art, but it is indispensable for early and correct diagnosis. It is important to obtain information from the family on stones, hematuria and renal failure, and on metabolic diseases (draw a pedigree chart). Particular attention has to be paid to nutrition or specific diets, fluid intake (dehydration), medications (vitamins D/A, steroids, diuretics, etc.), immobilization, and any mineral supplementation. Children with chronic bowel disease (e.g. Crohn s disease, cystic fibrosis, post-bowel resection), neurologic disorders (anti-convulsant drugs, low fluid intake) or with anomalies of the urinary tract predisposing to urine stasis and urinary tract infection (neurogenic bladder, ileal loops, megaureter, megacalycosis, hydonephrosis) are at special risk for stone formation (Table 2). Clinical findings (physical examination) Symptoms of urinary tract stones are often non-specific, particularly in infants and young children [5, 9]. In addition, stones may remain asymptomatic for long periods of time. The most common symptom of urolithiasis is abdominal pain, in older children clearly identifiable as colicky pain, in infants and children, however, only recognized as non-specific abdominal pain and thus difficult to differentiate from acute appendicitis, etc. [10]. Unexplained sterile pyuria or recurrent urinary tract infections (UTIs) should raise the level of suspicion for urolithiasis, especially in the younger child. Gross or microscopic non-glomerular hematuria and, more rarely, flank tenderness or urinary retention are other symptoms encountered. Gross hematuria may be present for some time before urolithiasis or nephrocalcinosis become manifest. Sometimes there are secondary gastro-intestinal tract symptoms such as vomiting, flatulence or constipation. Symptoms differ according to the location of the stone. Stones of the lower urinary tract may manifest themselves by dysuria, voiding problems or complete urine retention, but enuresis, frequent voiding, hematuria and fever may also be diagnostic hints. Also, manipulation of genitals in younger children may be a first sign of urolithiasis of the urethra. In infants, especially, stones may become stuck and therefore palpable in the urethra, such that the first symptom of stones is inability to pass urine [5]. Stones may even be the first symptom in polycystic kidney disease, especially in the autosomal dominant form, and hence palpable kidneys may lead way to diagnosis. A missed diagnosis may have serious consequences. For example, diagnosis of primary hyperoxaluria is often only made after end-stage renal failure has occurred years or decades after the first symptom of nephrolithiasis had appeared [11]. In contrast to nephrolithiasis, nephrocalcinosis is mostly asymptomatic, especially during infancy and early child- Table 1 Diagnostic steps in urolithiasis (UTI urinary tract infection, CT computed tomography, MRI magnetic resonance imaging, PTH parathyroid hormone, pco 2 partial pressure of carbon dioxide) Step History, including family history Clinical findings Imaging Urine Blood/serum Stone analysis Diagnostic findings Diet, fluid intake, medication, vitamin supplementation Chronic diseases? Malabsorption syndromes? Immobilization? Pain, hematuria, vomiting, UTI Passage of stones, gravel Ultrasonography, (plain film) Non-contrast-enhanced CT, (MRI) (Intravenous urography) Density, specific gravity (osmolality), ph, glucose, protein, sediment, culture Spot urine: molar creatinine ratios of calcium, oxalate, uric acid, citrate, magnesium Cystine screening (nitroprusside test, amino acid screen) 24 hour urine: volume, ph; (lithogenic and stone-inhibitory parameters); calculation of urinary saturation Electrolytes, calcium, phosphorus, magnesium, creatinine, urea, uric acid, alkaline phosphatase, (PTH, vitamins D/A, plasma oxalate, serum vitamin B6 level) Acid-base status (ph, pco 2, base excess and/or standard bicarbonate) Infrared spectroscopy or X-ray diffraction
3 Pediatr Nephrol (2010) 25: Table 2 Disorders of special interest presenting with urolithiasis and/or nephrocalcinosis. For further information see other chapters of the teaching series on urolithiasis in childhood. MIM Mendelian inheritance in man (catalogue no.), HPRT hypoxanthine-guanine-phosphoribosyl transferase, APRT adenine phosphoribosyltransferase, drta distal renal tubular acidosis, AD autosomal dominant, AR autosomal recessive, XLR, X linked recessive, LMW low molecular weight, CRF chronic renal failure MIM Locus, gene Inheritance Gene product Phenotype Hypercalciuria-induced urolithiasis/nephrocalcinosis Autosomal dominant hypocalcemic hypercalciuria ; q13.3- q21, CASR AD CASR Hypercalciuria Hypocalcemia CRF Familial hypomagnesemia with hypercalciuria and nephrocalcinosis (FHHNC) ; q27, 1p34.2, CLDN16, CLDN 19 AR Paracellin 1, (Claudin 16, 19) Hypercalciuria, hypercalcemia, hypomagnesemia, drta, CRF, hypermagnesuria, polyuria, tetany seizures Dent s disease, (Dent 1) ; ; Xp11.22, CLCN5 XLR CLC-5 Hypercalciuria, renal phosphate leak (variable), LMW proteinuria, hypophosphatemia (variable) Lowe syndrome, (Dent 2) Xq.25-26, OCRL1 XLR OCRL1 protein Hypercalciuria, megalin deficiency, phosphate leak, Fanconi syndrome Bartter s syndrome type q15-q21.1, NKCC2 AR SLC12A1 Salt wasting, hypokalemic metabolic alkalosis, and hypercalciuria, nephrocalcinosis Bartter s syndrome type q24, ROMK AR KCNJ1 Salt wasting, hypokalemic metabolic alkalosis, and hypercalciuria, nephrocalcinosis Infantile Bartter s syndrome with sensorineural ; ; 1p31, 1p36, BSND AR Salt wasting, hypokalemic metabolic alkalosis, and deafness ; CLCNKB hypercalciuria, nephrocalcinosis Williams Beuren syndrome ; ; ; Nephrolithiasis and osteoporosis associated with hypophosphatemia due to mutation in the type 2 sodium phosphate co-transporter contiguous gene deletion syndrome 7q11.23, ELN, LIMK1, RFC2 AD Elastin, LIMkinase 1 Hypercalcemia, hypercalciuria, mental retardation happy party manner, aortic stenosis, Elfin-faces, nephrocalcinosis q.35 Unknown NPTZa Renal phosphate leak, hypercalciuria, osteoporosis, 1,25 dihydroxy-vitamin D Hyperoxaluria-induced urolithiasis/nephrocalcinosis Primary hyperoxaluria, type I ; q.37.3, AGXT AR AGT Hyperoxaluria, hyperglycolic aciduria, CRF, systemic oxalosis Primary hyperoxaluria, type II ; q.11, GRHPR AR GR/HPR Hyperoxaluria, L-gylceric aciduria, CRF Cystinuria and urolithiasis Cystinuria type A p q.16.3, SLC3A1 AR r BAT Elevated urinary excretion of cystine (and other dibasic amino acids) Urine microscopy: hexagonal cystine crystals, recurrent urolithiasis, (CRF) Cystinuria type B q.13.1/slc7a9 Inc AR B α + AT Elevated urinary excretion of cystine (and other dibasic amino acids) Urine microscopy: hexagonal cystine crystals, recurrent urolithiasis, (CRF) Cystinuria type A/B SLC3A1/SLC7A1
4 406 Pediatr Nephrol (2010) 25: Table 2 (continued) MIM Locus, gene Inheritance Gene product Phenotype Purine/pyrimidine-induced urolithiasis/nephrocalcinosis Lesch Nyhan syndrome Xq26, HPRT XLR HPRT Hyperuricosuria, gout, automutilation, recurrent urolithiasis Partial HPRT deficiency Xq , HPRT XLR HPRT Hyperuricosuria Glycogenosis type 1a q.21, G6PC AR Glucose-6- phosphatase Hyperuricosuria Glycogenosis type 1b q.23, SLC37A4 AR Transporter Hyperuricosuria Phosphoribosylphosphate synthetase 1 superactivity Xq21, PRPS1 XL Hyperuricosuria APRT deficiency q.24.3, APRT AR APRT 2,8 Dihydroxy-adeninuria, recurrent crystalluria (round + brown), urolithiasis (radiolucent), rarely renal failure from crystal nephropathy Xanthinuria (classical) p.22, XDH AR Xanthine oxydoreductase or dehydrogenase Xanthinuria, hypouricemia Distal renal tubular acidosis Renal tubular acidosis autosomal dominant ; q.21 q.22, SLC4A1, AE1 AD AE1 Hypocitric aciduria, hypercalciuria, hypokalemia, osteomalacia Autosomal recessive drta with hearing loss ; cen-q13, ATP6B1 AR B1 Hypercalciuria, hypocitric aciduria, hypokalemia, rickets, hearing loss Autosomal recessive drta ; q.33-34, SLC4A1 AR A4 Hypercalciuria, hypocitric aciduria, hypokalemia
5 Pediatr Nephrol (2010) 25: hood. Hence, diagnosis is often only made when nephrocalcinosis is incidentally noted on an imaging study performed for other reasons or when symptoms of reduced concentrating capacity of the renal tubules are obvious. However, the underlying pathological condition is not always evident and requires a detailed history and workup. Renal colic has been reported in some infants with nephrocalcinosis, but it is more likely due to passage of tiny calculi than to nephrocalcinosis per se. It is not unusual for nephrocalcinosis to be diagnosed during systematic renal ultrasound examination of high-risk infants or as part of the diagnostic evaluation of urinary tract infection. The first clinical symptoms, if any, are gross or microscopic hematuria and/or sterile leukocyturia that may be misdiagnosed as urinary tract infection [12]. Diagnostic imaging Initial diagnostic testing has to uncover, systematically, obstruction or stasis, infection, and metabolic abnormalities (Tables 1 and 2) and profoundly relies on imaging of the urinary tract. With the availability of minimally invasive imaging modalities, such as ultrasound and computed tomography (CT), the latter less used for pediatric patients, stones are increasingly being detected incidentally during evaluation of nonspecific symptoms or unrelated problems. At baseline, however, imaging of the urinary tract has to be sufficiently thorough to rule out, assertively, stasis or obstruction related either to a stone or to congenital or acquired abnormalities of the urinary tract. The appearance on imaging studies depends upon the stone s composition. Those composed of calcium oxalate or calcium phosphate have a very dense image on conventional radiographs and on CT scans. Struvite (magnesium ammonium phosphate) and cystine stones are of intermediate density, and small stones of all compositions can be difficult to appreciate by conventional radiography. Uric acid stones are radiolucent on radiographs, requiring the administration of contrast agents for adequate visualization, and have a low density image on CT scans. Stones composed of indinavir, ceftriaxone, sulfadiazine or matrix (all infrequent, the latter composed of protein structures as a matrix for, for example, calcium oxalate stones) are of variable density and may be difficult to differentiate from surrounding soft tissue by any modality, including ultrasound [13 15]. Stones of all composition, with the exception of drugs (e.g. indinavir) and matrix (protein), have distinguishing characteristics of echogenicity and shadowing on ultrasonography. Ultrasonography has the additional advantages of wide availability, avoidance of ionizing radiation, ready detection of hydronephrosis, and ability to define some aspects of the anatomy of the urinary tract. However, ultrasonography is not as sensitive as CT is for the detection of small stones or stones in the ureter. Indeed, small stones may not be detectable by routine ultrasound examination, even when strongly suspected. Measurement of stone size is less reproducible by ultrasound than by conventional radiographs or CT, thus maybe reducing its utility for the monitoring of metabolic stone forming activity over time. Nevertheless, and as stones as small as only mm in diameter can be visualized on ultrasonography (US), the success of this imaging method clearly depends on inter-observer and intra-observer variability and skills. Most stones can be imaged without the use of contrast agents. However, when obstruction is a concern, when radiolucent or low density stones require careful delineation, or when details of urinary tract anatomy are needed (such as confirmation of a duplicated collecting system), contrast agents (CT urography, intravenous pyelography, or retrograde ureteroscopy/pyelography, or orthograde pyelography) are usually required. Individual clinical characteristics, type of stone, and questions to be addressed should be considered in decisions regarding the best imaging modality. Ultrasonography is almost always a good initial choice and, in uncomplicated situations, may be all that is needed. The typical stone location is within the renal pelvis and/ or the renal calyces or the ureter and less often within the bladder. The most common ureteral calcification is a stone that has migrated down from the kidney. These stones typically become impacted at anatomic sites of narrowing and are especially difficult to detect when they overlie bony structures such as the sacrum. Detection of a ureteral stone via ultrasonography is difficult, but the stone may lead to obstruction (hydroureter or hydronephrosis) and may, thus, be suspected, even if not directly visualized. Next to that, the color Doppler twinkling artifact can be used in all sides negative for stones in B mode ultrasonography [16]. Studies of adult patients have shown that non-contrastenhanced CT is more effective than intravenous urography (IVU) in identifying and locating ureteral stones [10] and that almost all urinary calculi are now able to be seen with the appropriate selection of imaging techniques, no matter where they reside in the urinary tract [17]. However, in infants and young children, particularly, minimization of exposure to ionizing radiation, and the occasional need for sedation with CT, favors the use of ultrasonography or conventional radiography over CT, whenever they provide the necessary visualization. For the detecting and monitoring of nephrocalcinosis, high-resolution ultrasonography is the optimal imaging method (Fig. 1). Nephrocalcinosis is classified according to the anatomic area involved. Medullary nephrocalcinosis
6 408 Pediatr Nephrol (2010) 25: Fig. 1 a Normal, still hyperechoic kidney of a preterm infant; b Tamm Horsfall kidney; c medullary nephrocalcinosis (NC) grade I (mild increase of echogenicity around the pyramidal border); d medullary NC grade II (mild increase of echogenicity at whole pyramid); e medullary NC grade III (more severe hyperechogenicity of entire pyramid); f diffuse corticomedullary NC [6] a c d b e f is differentiated from either cortical nephrocalcinosis (e.g. in acute cortical necrosis, chronic glomerulonephritis and chronic graft rejection) or diffuse nephrocalcinosis and is divided into three subtypes according to the degree of echogenicity. Thanks to the routine use of ultrasonography in premature infants and in children at risk, a large number of conditions are now recognized to be associated with nephrocalcinosis (Table 2) [12]. Some pitfalls in the renal ultrasonography of neonates, and especially preterm infants, have to be noted: Tamm Horsfall protein (THP) deposits within the renal calyces may look like nephrocalcinosis (Fig. 1). THP deposition, however, disappears within 1 2 weeks, and follow-up will show completely normal kidneys. Furthermore, the echogenicity of the renal cortex in neonates is physiologically increased, hence detection of cortical nephrocalcinosis can be difficult and may become evident only some weeks later when a rim of cortical calcification becomes visible. However, diffuse cortical nephrocalcinosis may already be detectable shortly after birth in patients with suspected primary hyperoxaluria, and it is directly visible both by US and X-ray [18]. Medullary nephrocalcinosis can, sonographically, only be diagnosed when increased echogenicity appears in the area of the renal medulla. Normally, the renal pyramids are hypoechoic in relation to the cortex. A plain film of the abdomen is less helpful, as only the association of hyperechoic pyramids with a posterior acoustic shadow is a clear sign of nephrocalcinosis. Gross calcifications are thus required before nephrocalcinosis can be diagnosed from conventional radiographs. A comparison of US and CT in induced nephrocalcinosis in rabbits demonstrated a higher sensitivity for US (96% vs 64%), but a better specificity for CT (96% vs 85%) [19]. Still, renal ultrasonography is the first diagnostic imaging option in infants and children with suspected stones or nephrocalcinosis.
7 Pediatr Nephrol (2010) 25: Investigation: examination of urine and blood Complete urine analysis of a random voided specimen is a necessary diagnostic evaluation in every acute stone episode. Hematuria, white blood cell (WBC) count, pathogens and urinary protein excretion can easily be determined. Microscopic examination of the urine is important, not only for the differentiation between glomerular and non-glomerular hematuria, but also for WBC counts and detection of crystals such as hexagonal cystine crystals, 2,8 dihydroxy-adenine and certain drugs (e.g. indinavir urinary crystals [20]). Since the ph of the urine is a major factor in the formation of many stones, its measurement preferably by glass electrode, or, if a ph electrode is not available, by ph paper with the specific and adequately distinguishable range of ph 2 to 9 is of utmost importance. Sometimes, it is advisable to determine a daily profile of both the ph and the density (specific gravity or osmolality) of the urine. This may also be used for follow-up, e.g. to assess the effect of the administration of alkali or to check the patient s compliance regarding sufficient fluid intake. The presence or absence of infection can be addressed by a urine culture. Chemical analysis includes, apart from creatinine, calcium, uric acid, oxalic acid, phosphate [determine tubular reabsorption of phosphate (TRP) or tubular maximum for phosphate corrected for glomerular filtration rate (TmP/ GFR)], magnesium and citrate. Cystine is screened for by nitroprusside test or by chromatography for amino acids. For all patients, analyses for serum calcium, phosphorus, magnesium, uric acid, alkaline phosphatase, ph, bicarbonate, and creatinine should be performed. In specific cases further blood analyses for parathyroid hormone (PTH), vitamin D metabolites, vitamin A (for patients with hypercalciuria), serum vitamin B6 levels and plasma oxalate (for patients with primary hyperoxaluria) and, of course, molecular genetic testing (see Tables 1 and 2) will later be necessary. Predisposing causes for urolithiasis can be recognized in >75% of children and adolescents with urinary tract stones [7, 9]. Accordingly, every young patient with urolithiasis, and even with the first stone episode, deserves a comprehensive examination so that a delay in treatment, and hence early complication, e.g. acute renal failure in infantile oxalosis, can be avoided [6, 11]. Infection, obstruction, or stasis will be identified by the diagnostic evaluation outlined above. However, systematic detection of predisposing metabolic factors requires further testing. Metabolic factors, among which hypercalciuria, hyperoxaluria and hypocitraturia are the most common, are determined by measurement of relevant urinary solutes and naturally occurring inhibitors of crystal and stone forma- Table 3 Normal values for 24 h urine collection (there should be preservative in the container, either thymol 5% in isopropanol, or 2 N hydrochloric acid (HCl), before collection is started). Repeat collection after stone has been captured, as ongoing stone formation may diminish lithogenic excretion parameters. Check urine volume and creatinine excretion (2 mg/kg±0.8 mg) to ensure adequate collection [5, 6, 36 41]. FHHNC Familial hypomagnesemia and hypercalciuria with nephrocalcinosis syndrome, FE Mg fractional excretion of magnesium Parameter age Normal value per 24 h Remarks Calcium, all ages <0.1 mmol (<4 mg)/kg See Table 2 Oxalate <0.5 mmol (<45 mg)/1.73 m 2 Primary hyperoxaluria types I/II for constant excessive elevation, check also urinary glycolate, L-glycerate and plasma oxalate Secondary hyperoxaluria: determine intestinal oxalate absorption and stool. Oxalobacter formigenes colonization. Normal plasma oxalate different according to laboratory method, but clearly <8 μmol/l Citrate Male >1.9 mmol (365 mg)/1.73 m 2 Hypocitraturia: metabolic acidosis, hypokalemia, calcineurin Female >1.6 mmol (310 mg)/1.73 m 2 inhibitors Uric acid, all ages 0.56 mg/dl per GFR Hyperuricosuria: check diet, medication, tumor lysis, inborn errors of metabolism Magnesium >0.04 mmol (0.8 mg)/kg FHHNC with hypomagnesemia and elevated FE Mg,SeeTable2 Phosphate TmP/GFR Renal phosphate leakage with low serum phosphate, tumor <3 months <3.3 mmol/l lysis syndrome with high serum phosphate <6 months <2.6 mmol/l 2 15 years <2.44 mmol/l Cystine <10 years <55 μmol (13 mg)/1.73 m 2 Check morning urine for hexagonal crystals >10 years <200 (48 mg) Adults <250, (60 mg) Cystine solubility threshold mg cystine/l at ph 5 7
8 410 Pediatr Nephrol (2010) 25: Table 4 Normal values for spot urine samples: creatinine ratios (solute/creatinine). Ratios are more prone to error than are timed samples. Interpret with respect to daytime, relation to meals, diet, medication, age and regional differences [5, 6, 36 41] (Ca calcium, RTA renal tubular acidosis) Parameter age Ratio of solute to creatinine Remarks Calcium mol/mol mg/mg Highest Ca excretion with breast milk feeding, ratio increasing after meals (up to 40%), <12 months < by loop diuretics, immobilization and steroids 1 3 years < years < years < >7 years < Oxalate mmol/mol mg/g Primary hyperoxaluria types I/II for constant excessive elevation, check also urinary 0 6 months < glycolate, L-glycerate and plasma oxalate. Secondary hyperoxaluria: determine 7 24 months < intestinal oxalate absorption and stool Oxalobacter formigenes colonization 2 5 years < years < >16 years <40 32 Citrate mol/mol g/g Low with tubular dysfunction: RTA, prematurity, hypokalemia, renal transplantation 0 5 years > >5 years > Magnesium mol/mol g/g For <2 years, no reliable data >0.63 > 0.13 Uric acid >2 years <0.56 mg/dl (33 μmol/l) per GFR Higher than in adults throughout childhood; no reliable data for age <2 years (ratio plasma creatinine) tion, such as citrate. Blood levels of calcium and other analytes, as determinants of urine composition or as indicators of underlying disorders relevant to stone formation (such as metabolic acidosis), are also of importance. Since many urinary components are influenced by dietary intake, 24 h urine collections (to exclude diurnal fluctuations related to intake of food and beverages) provide the best information and also provide an objective assessment of the child s daily intake of fluid. Advise the patient or the parent to maintain the normal fluid intake and the normal dietary habits, and, meanwhile, 24 h urine should be collected. Next, avoid urine sampling under parenteral infusions. Also keep in mind that stones in situ may diminish the excretion of urinary lithogenic material, as these substances may concurrently be absorbed by the stone [21]. For urine collection, a preservative should ideally be placed directly into the sampling bottle; however, urine may be collected without initial preservation, so long as it is kept cool (at 4 C) and adequately preserved within 24 h [22]. In infants or young children, or in situations where a 24 h urine collection is difficult, random urine measurements, using the ratio of the concentration of each analyte to that of urine creatinine, provide valuable information. Again, the best results are obtained if urine is collected while patients are receiving their usual diets and fluid intake. Bladder catheterization only for 24 h urine collection should be avoided, especially for boys. Erroneous results might be obtained if obstruction or infection is present, or when stone fragments are being passed in the urine following a recent stone fragmentation procedure. Analysis should be deferred until infection has been treated and until at least 1 month after lithotripsy or resolution of the obstruction [23]. Normal values for the excretion rates of solutes that are most often implicated in stone formation are shown in Tables 3 and 4. However, it has to be kept in mind that such data clearly show regional and cultural variability, and, so far, no multi-institutional studies regarding normative data of pediatric excretion values exist. Specific abnormalities may dictate a more directed testing. Many children and adolescents with stones have more than one predisposing Table 5 Ten take-home messages Message 1. Kidney stones/nephrocalcinosis in children are the symptoms of a disease, not the disease itself 2. About 40% of children with urolithiasis have a positive family history 3. Predisposing causes for urolithiasis can be recognized in 75% of children and adolescents 4. Unexplained sterile pyuria or recurrent UTI should raise the suspicion for urolithiasis 5. Gross hematuria may precede manifest urolithiasis or nephrocalcinosis 6. Nephrocalcinosis is mostly asymptomatic 7. The diagnosis of primary hyperoxaluria is often delayed; early detection may prevent the development of renal failure 8. Calyceal depositions of Tamm Horsfall protein are harmless, but they may mimic nephrocalcinosis in (preterm) neonates 9. Metabolic urine analysis should be performed in 24 h urine collection 10. Passing stone fragments and UTI may hamper proper metabolic urine analysis
9 Pediatr Nephrol (2010) 25: factor [24]. With that in mind, it is important to complete a systematic evaluation, even when the etiology seems obvious. For example, patients with congenital ureteropelvic junction obstruction and stones may have hypercalciuria as a second predisposing cause. When an inherited metabolic disorder is suspected, urine samples from family members can be of help in the primary diagnosis, and they are also valuable for detection in affected family members. For patients with multiple stones at the onset, or those in whom there is active stone formation and no abnormalities have been identified, additional testing can be helpful. This testing should include a timed (preferably 24 h) urine collection for a full supersaturation profile [25, 26]. Owing to day-to-day variations in diet and fluid intake, three separate determinations on different days have been demonstrated to provide the best information [27]. However, the value of such computer-based calculation of urinary saturation is debatable, as are other determinants of stone risk factors, such the BONN risk index (BRI, [28, 29]). In patients with hyperoxaluria, intestinal absorption of oxalate may be increased, either due to an increased intake of dietary oxalate, or for enteric reasons such as chronic inflammatory bowel diseases or a lack of intestinal oxalatedegrading bacteria [30]. Next to that, the pathology of intestinal oxalate transporters, e.g. those of the solute carrier family (SLC26A6), may also play an important role, which is currently under specific evaluation [31]. To discriminate the primary from the secondary forms of hyperoxaluria better, a [ 13 C 2 ] oxalate absorption test can be performed, which is safe and reliable in children, as in adults. Intestinal oxalate absorption is normal in patients with primary hyperoxaluria and would be significantly increased in those with dietary or enteric hyperoxaluria [32]. Also, a stool analysis for the absence of oxalate-degrading bacteria, especially Oxalobacter formigenes, will give further evidence of the existence of a secondary reason for hyperoxaluria [33]. Stone analysis Qualitative analysis of the stone obtained after spontaneous stone passage or intervention is one of the most important diagnostic measures. Only one-third of all stones are composed of one single substance, and all components should, hence, be determined. The methods of choice are infrared spectroscopy or X-ray diffraction. Even amounts of less then 1 mg can be analyzed. Chemical stone analysis is inappropriate, as it is prone to errors and is obsolete. The analytic principle of X-ray diffraction is based on the crystal structure of the stone substances. With infrared spectroscopy the loss of energy in the infrared spectrum due to the circulation of the activated chemical molecules is determined. The diagrams of either method (the so-called fingerprints) provide an exact analysis [34]. Recurrent stones should be analyzed again, since the stone composition may change. After lithotripsy only stone fragments are available, and these can be recovered by straining the urine. All fragments should be sent for analysis to allow additional tests, if needed. With regard to treatment regimens, all stone components are of importance. Apart from the main stone components there are several other substances, such as salts of uric acid (urates), rare calcium phosphate compositions, protein matrix stones, stones comprised of medications or their metabolites (e.g. indinavir, ceftriaxone, sulfadiazine), and artifacts like gypsum or seeds. Conclusions Pediatric urolithiasis is not as rare as is generally believed. In addition, the prevalence of nephrocalcinosis may be high, especially in preterm infants [35]. Hence, thorough and early diagnostic examination is mandatory, for every infant or child with the first stone event or with nephrocalcinosis (see Table 5). Following this advice, recurrence of stone disease or progression of nephrocalcinosis can be prevented, or, taking the worst scenario into consideration, prevention of early end-stage renal failure (e.g. in patients with primary hyperoxaluria), can be achieved. Questions (Answers appear following the reference list) 1. Which of the following statements are true? Urolithiasis in children is a. more frequent than in adults b. has the same frequency as in adults c. is less frequent than in adults (approximately 10% the rate of adults) but is often under-diagnosed d. more frequent in boys than in girls e. all of the above are true 2. A metabolic cause of urolithiasis a. is more likely in children than in adults, since family history is often positive b. is unlikely, since the most frequent etiology is UTI c. can easily be ruled out by family history d. has the same frequency as in adults e. does not require consideration, since urolithiasis in children is so rare 3. Which of the following is not true? Symptoms of urinary tract stones may include a. gross hematuria b. pain
10 412 Pediatr Nephrol (2010) 25: c. vomiting d. fever e. isolated proteinuria 4. Risk factors for urolithiasis in children include a. dehydration b. gastro-intestinal disorders (e.g. Crohn s disease) c. urinary tract infections d. diet e. all of the above are true 5. Primary hyperoxaluria type 1 is a. a serious disorder that can cause urolithiasis but also end-stage renal disease b. the most frequent cause of urolithiasis in children c. always associated with hypercalciuria d. only likely if family history is positive e. a benign condition that does not require treatment 6. Imaging studies in urolithiasis a. are not important, since clinical details indicate localization b. should be thorough, since stones may be small and are difficult to detect c. should always include intravenous pyelography d. should only include abdominal CT, since conventional radiology is mostly insufficient e. all of the above are true 7. Which of the following are true? The investigation of metabolic causes in children should include a. hypercalciuria b. hypocitraturia c. hypertriglyceridemia d. phenylketonuria e. cystinuria References 1. López M, Hoppe B (2008) History, epidemiology and regional diversities of urolithiasis. Pediatr Nephrol doi: /s Hesse A (2005) Reliable data from diverse regions of the world exist to show that there has been a steady increase in the prevalence of urolithiasis (editorial). World J Urol 23: Sarica K (2006) Pediatric urolithiasis: etiology, specific pathogenesis and medical treatment. Urol Res 34: Edvardsson V, Elidottir H, Indridason OS, Palsson R (2005) High incidence of kidney stones in Icelandic children. Pediatr Nephrol 20: Leumann E, Hoppe B (1997) Urolithiasis in childhood. In: Proesmanns W (ed) Therapeutic strategies in children with renal disease, vol 5. Bailliere s Clinical Paediatrics, London, pp Hoppe B, Milliner D, Leumann E (2008) Urolithiasis and nephrocalcinosis in childhood. In: Geary D, Schaefer F (eds) Comprehensive pediatric nephrology, chapter 33. Mosby, Elsevier, Philadelphia, pp Van t Hoff WG (2004) Aetiological factors in paediatric urolithiasis. Nephron Clin Pract 98:c45 c48 8. Stapleton FB (1996) Clinical approach to children with urolithiasis. Semin Nephrol 3: Cameron MA, Sakkhae K, Moe OW (2005) Nephrolithiasis in children. Pediatr Nephrol 20: Smith RC, Rosenfield AT, Choe KA, Essenmacher KR, Verga M, Glickman MG, Lange RC (1995) Acute flank pain: comparison of non-contrast-enhanced CT and intravenous urography. Radiology 194: Van Woerden CS, Groothoff JW, Wanders RJ (2003) Primary hyperoxaluria type 1 in The Netherlands: prevalence and outcome. Nephrol Dial Transplant 18: Alon US (1997) Nephrocalcinosis. Pediatrics 9: Sandersius S, Rez P (2007) Morphology of crystals in calcium oxalate monohydrate kidney stones. Urol Res 35: Mohkam M, Karimi A, Gharib A, Daneshmand H, Khatami A, Ghojevand N, Sharifian M (2007) Ceftriaxone associated nephrolithiasis: a prospective study in 284 children. Pediatr Nephrol 22: Catalano-Pons C, Bargy S, Schlecht D, Tabone MD, Deschenes G, Bensman A Ulinski T (2004) Sulfadiazine induced nephrolithiasis in children. Pediatr Nephrol 19: Turrin A, Minola P, Costa F, Cerati L, Andrulli S, Trinchieri A (2007) Diagnostic value of colour Doppler twinkling artefact in sites negative for stones on B mode renal sonography. Urol Res 35: Mindell HJ, Cochran ST (1994) Current perspectives in the diagnosis and treatment of urinary stone disease. Am J Radiol 163: Benz-Bohm G, Hoppe B (2008) Urolithiasis and nephrocalcinosis. In: Fotter R (ed) Pediatric uroradiology. Springer, Heidelberg, pp Cramer B, Husa L, Pushpanathan C (1998) Nephrocalcinosis in rabbits correlation of ultrasound, computed tomography, pathology and renal function. Pediatr Radiol 28: Gagnon RF, Tsoukas CM, Watters AK (1998) Light microscopy of indinavir urinary crystals (letter). Ann Int Med 128: Laube N, Pullmann M, Hergarten S, Schmidt M, Hesse A (2003) The alteration of urine composition due to stone material present in the urinary tract. Eur Urol 44: van Woerden CS, Huidekoper HH, Groothoff JW, Wijburg FA, Duran M (2007) Postponing urine acidification for 24 h does not change the oxalate concentration. Clin Chim Acta 384: Beck B, Hoppe B (2005) Pediatric aspects of nephrolithiasis and nephrocalcinosis. In: Chaussy C, Haupt G, Jocham D, Köhrmann KU, Wilbert D (eds) Therapeutic energy applications in urology. Thieme, Heidelberg, pp Habbig S, Kratz J, Beck B, Feldkötter M, Taylan C, Körber F, Hoppe B (2008) Nephrocalcinosis and nephrolithiasis in children: is hypercalciuria the most important risk factor? J Am Soc Nephrol Abstr (in press) 25. Battino BS, DeFoor W, Coe F, Tackett L, Erhard M, Wacksman J, Sheldon CA, Minevich E (2002) Metabolic evaluation of children with urolithiasis: are adult references for supersaturation appropriate. J Urol 168: Defoor W, Asplin J, Jackson E, Jackson C, Reddy P, Sheldon C, Minevich E (2005) Results of a prospective trial to compare normal urine supersaturation in children and adults. J Urol 174: Parks JH, Goldfisher E, Asplin JR, Coe FL (2002) A single 24- hour urine collection is inadequate for the medical evaluation of nephrolithiasis. J Urol 167: Laube N, Hoppe B, Hesse A (2005) Problems in the investigation of urines from patients suffering from primary hyperoxaluria type I. Urol Res 33: Porowski T, Zoch-Zwierz W, Konstantynowicz J, Taranta-Janusz K (2008) A new approach to the diagnosis of children s urolithiasis based on the Bonn risk index. Pediatr Nephrol 23:
11 Pediatr Nephrol (2010) 25: Hoppe B, Leumann E, von Unruh G, Laube N, Hesse A (2003) Diagnostic and therapeutic approaches in patients with secondary hyperoxaluria. Front Biosci 8:e437 e Hatch M, Freel RW (2008) The roles and mechanisms of intestinal oxalate transport in oxalate homeostasis (review). Semin Nephrol 28: Sikora P, von Unruh GE, Beck B, Feldkötter M, Zajączkowska M, Hesse A, Hoppe B (2008) [(13)C(2)]oxalate absorption in children with idiopathic calcium oxalate urolithiasis or primary hyperoxaluria. Kidney Int 73: Kaufman DW, Kelly JP, Curhan GC, Anderson TE, Dretler SP, Preminger GM, Cave DR (2008) Oxalobacter formigenes may reduce the risk of calcium oxalate kidney stones. J Am Soc Nephrol 19: Hesse A (2002) Urinary calculi 1: epidemiology, laboratory diagnosis, genetics and infections. Urologe A 41: Sikora P, Roth B, Kribs A, Michalk DV, Hesse A, Hoppe B (2003) Hypocitraturia is one of the major risk factors for nephrocalcinosis in very low birth weight (VLBW) infants. Kidney Int 63: de Santo NG, Di Iorio B, Capasso G, Paduano C, Stamler R, Langman CB, Stamler J (1992) Population based data on urinary excretion of calcium, magnesium, oxalate, phosphate and uric acid in children from Cimitile (souther Italy). Pediatr Nephrol 6: Hoppe B, Jahnen A, Bach D, Hesse A (1997) Urinary calcium oxalate saturation in healthy infants and children. J Urol 158: Leumann EP, Dietl A, Matasovic A (1990) Urinary oxalate and glycolate excretion in healthy infants and children. Pediatr Nephrol 4: Brodehl J, Krause A, Hoyer P (1988) Assessment of maximal tubular phosphate reabsorption: comparison of direct measurement with the nomogram of Bijvoet. Pediatr Nephrol 2: Payne RB (1998) Renal tubular reabsorption of phosphate (TmP/ GFR): indications and interpretation. Ann Clin Biochem 35: Stapleton FB, Nash DA (1983) A screening test for hyperuricosuria. J Pediatr 102:88 90 Answers 1. Correct answers are c and d: The incidence of urolithiasis in childhood is believed to be approximately 10% of that in adults, which is around 5% in industrialized countries [2]. As a significant proportion of patients remains undiagnosed or misdiagnosed (incidental discovery is reported in 15 40%), numbers should be interpreted with caution. Urolithiasis appears in all age groups of children, but a male predominance analogous to that in adult patients is observed. 2. Correct answer is a: About 40% of children with urolithiasis have a positive family history of kidney stones, and most of the children have a metabolic background of stone disease. Hence, specific and intensive diagnostic examination is necessary for every child experiencing even a single kidney stone to prevent recurrence of disease or even a disastrous outcome, with kidney failure and end-stage renal disease. 3. Correct answer is e: The most common symptom of urolithiasis is abdominal pain, in older children clearly identifiable as colicky pain, in infants and children, however, only recognized as non-specific abdominal pain and thus difficult to differentiate from acute appendicitis, etc. Unexplained sterile pyuria or recurrent urinary tract infections should raise the level of suspicion for urolithiasis, especially in the younger child. Gross or microscopic (non-glomerular) hematuria and, more rarely, flank tenderness or urinary retention, are other symptoms encountered. Hematuria may be present for some time before urolithiasis or nephrocalcinosis becomes manifest. Sometimes, there are secondary gastro-intestinal tract symptoms, such as vomiting, flatulence or constipation. 4. Correct answer is e: Regarding the risk of nephrolithiasis or nephrocalcinosis, particular attention has to be paid to nutrition or specific diets, fluid intake (dehydration), medications (vitamins D/A, steroids, diuretics, etc.) and any mineral supplementation. Children with chronic bowel disease (e.g. Crohn s disease, cystic fibrosis, post-bowel resection), neurologic disorders (anticonvulsant drugs, low fluid intake) or with anomalies of the urinary tract predisposing to urine stasis and urinary tract infection (neurogenic bladder, ileal loops, megaureter, megacalycosis, hydronephrosis) are at special risk of stone formation. 5. Correct answer is a: Primary hyperoxaluria type I is an autosomal-recessive inherited disorder which leads to recurrent nephrolithiasis and/or progressive nephrocalcinosis and can lead to early end-stage renal failure in those patients with severe symptoms (infantile oxalosis). 6. Correct answer is b: Initial diagnostic testing has to uncover obstruction or stasis, infection, and metabolic abnormalities systematically (Table 1), and it relies profoundly on imaging of the urinary tract. With the availability of minimally invasive imaging modalities such as ultrasound and CT, the latter less used for pediatric patients, stones are being increasingly detected incidentally during evaluation of nonspecific symptoms or unrelated problems. At baseline, however, imaging of the urinary tract has to be sufficiently thorough to rule out, assertively, stasis or obstruction related either to a stone or to congenital or acquired abnormalities of the urinary tract. Intravenous urography is not a method of choice for the pediatric patient. 7. Correct answers are a, b and e: Chemical analysis includes, apart from creatinine, calcium, uric acid, oxalic acid, phosphate, magnesium and citrate. Cystine is screened for by nitroprusside test or by chromatography for amino acids. For all patients, analysis of serum calcium, phosphorus, magnesium, uric acid, alkaline phosphatase, ph, bicarbonate, and creatinine should be performed.
Martin Konrad has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve.
 Martin Konrad has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve. Nephrocalcinosis Clinical / Genetic Work-up and Outcome Martin Konrad University
Martin Konrad has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve. Nephrocalcinosis Clinical / Genetic Work-up and Outcome Martin Konrad University
CYSTIC DISEASES of THE KIDNEY. Dr. Nisreen Abu Shahin
 CYSTIC DISEASES of THE KIDNEY Dr. Nisreen Abu Shahin 1 Types of cysts 1-Simple Cysts 2-Dialysis-associated acquired cysts 3-Autosomal Dominant (Adult) Polycystic Kidney Disease 4-Autosomal Recessive (Childhood)
CYSTIC DISEASES of THE KIDNEY Dr. Nisreen Abu Shahin 1 Types of cysts 1-Simple Cysts 2-Dialysis-associated acquired cysts 3-Autosomal Dominant (Adult) Polycystic Kidney Disease 4-Autosomal Recessive (Childhood)
School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR
 1 School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR URINARY (RENAL) STONE FORMATION An Overview What are Urinary (Renal)
1 School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PLB SEMINAR URINARY (RENAL) STONE FORMATION An Overview What are Urinary (Renal)
Medical Approach to Nephrolithiasis. Seth Goldberg, MD September 15, 2017 ACP Meeting
 Medical Approach to Nephrolithiasis Seth Goldberg, MD September 15, 2017 ACP Meeting DISCLOSURES Seth Goldberg, MD Assistant Professor of Medicine Research support Abbott Kadmon Otsuka Pfizer Introduction
Medical Approach to Nephrolithiasis Seth Goldberg, MD September 15, 2017 ACP Meeting DISCLOSURES Seth Goldberg, MD Assistant Professor of Medicine Research support Abbott Kadmon Otsuka Pfizer Introduction
Urolithiasis. Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery
 Urolithiasis Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery Urolithiasis: Why should we care? Affects 5% of US men and women Men twice as
Urolithiasis Ali Kasraeian, MD, FACS Kasraeian Urology Advanced Laparoscopic, Robotic & Minimally Invasive Urologic Surgery Urolithiasis: Why should we care? Affects 5% of US men and women Men twice as
Identification and qualitative Analysis. of Renal Calculi
 Identification and qualitative Analysis of Renal Calculi 1 -Renal Calculi: Kidney stones, renal calculi or renal lithiasis (stone formation) are small, hard deposits that form inside your kidneys. The
Identification and qualitative Analysis of Renal Calculi 1 -Renal Calculi: Kidney stones, renal calculi or renal lithiasis (stone formation) are small, hard deposits that form inside your kidneys. The
2015 OPSC Annual Convention. syllabus. February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California
 2015 OPSC Annual Convention syllabus February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California FRIDAY, FEBRUARY 6, 2015: 4:00pm - 5:00pm Stone Disease^ Presented by John Grimaldi, DO ^ California
2015 OPSC Annual Convention syllabus February 4-8, 2015 Hyatt Regency Mission Bay San Diego, California FRIDAY, FEBRUARY 6, 2015: 4:00pm - 5:00pm Stone Disease^ Presented by John Grimaldi, DO ^ California
URINARY CRYSTALS. by Geoffrey K. Dube and Robert S. Brown
 URINARY CRYSTALS by Geoffrey K. Dube and Robert S. Brown A 26 year-old man presents with a fever and weakness. His WBC is 133,000, with 83% blasts. Creatinine is 2.0 mg/dl and serum uric acid is 15.4 mg/dl.
URINARY CRYSTALS by Geoffrey K. Dube and Robert S. Brown A 26 year-old man presents with a fever and weakness. His WBC is 133,000, with 83% blasts. Creatinine is 2.0 mg/dl and serum uric acid is 15.4 mg/dl.
The Nuts and Bolts of Kidney Stones. Soha Zouwail Consultant Chemical Pathology UHW Renal Training Day 2019
 The Nuts and Bolts of Kidney Stones Soha Zouwail Consultant Chemical Pathology UHW Renal Training Day 2019 Urinary Calculi Prevalence and incidence of kidney stones increasing across the world Environmental
The Nuts and Bolts of Kidney Stones Soha Zouwail Consultant Chemical Pathology UHW Renal Training Day 2019 Urinary Calculi Prevalence and incidence of kidney stones increasing across the world Environmental
NEPHROLITHIASIS Etiology, stone composition, medical management, and prevention
 NEPHROLITHIASIS Etiology, stone composition, medical management, and prevention Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Epidemiology Prevalence 2-3%, maybe in
NEPHROLITHIASIS Etiology, stone composition, medical management, and prevention Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Epidemiology Prevalence 2-3%, maybe in
Acute flank pain in children: Imaging considerations
 Acute flank pain in children: Imaging considerations Carlos J. Sivit MD Rainbow Babies and Children s Hospital Case Western Reserve School of Medicine Flank pain Results from distention of ureter or renal
Acute flank pain in children: Imaging considerations Carlos J. Sivit MD Rainbow Babies and Children s Hospital Case Western Reserve School of Medicine Flank pain Results from distention of ureter or renal
REVIEW: GENETICS OF UROLITHIASIS
 REVIEW: GENETICS OF UROLITHIASIS *Thomas Eggermann Institute of Human Genetics, University Hospital Aachen, Aachen, Germany *Correspondence to teggermann@ukaachen.de Disclosure: No potential conflict of
REVIEW: GENETICS OF UROLITHIASIS *Thomas Eggermann Institute of Human Genetics, University Hospital Aachen, Aachen, Germany *Correspondence to teggermann@ukaachen.de Disclosure: No potential conflict of
Alterations of Renal and Urinary Tract Function
 Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Inborn errors of metabolism presenting with kidney stones: clinical aspects. Francesco Emma
 Inborn errors of metabolism presenting with kidney stones: clinical aspects Francesco Emma Division of Nephrology and Dialysis Bambino Gesù Children s Hospital, IRCCS Rome, Italy September 6, 2016 Palazzo
Inborn errors of metabolism presenting with kidney stones: clinical aspects Francesco Emma Division of Nephrology and Dialysis Bambino Gesù Children s Hospital, IRCCS Rome, Italy September 6, 2016 Palazzo
The 82 nd UWI/BAMP CME Conference November 18, Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist
 The 82 nd UWI/BAMP CME Conference November 18, 2017 Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist Disclosures Outline Index case Introduction Etiology Risk factors Acute stone event Conservative
The 82 nd UWI/BAMP CME Conference November 18, 2017 Jeetu Nebhnani MBBS D.M. Urology Consultant Urologist Disclosures Outline Index case Introduction Etiology Risk factors Acute stone event Conservative
RISK FACTORS AND TREATMENT STRATEGIES FOR URINARY STONES Review of NASA s Evidence Reports on Human Health Risks
 Mayo Clinic O Brien Urology Research Center RISK FACTORS AND TREATMENT STRATEGIES FOR URINARY STONES 2017 Review of NASA s Evidence Reports on Human Health Risks John C Lieske, MD July 27, 2017 What types
Mayo Clinic O Brien Urology Research Center RISK FACTORS AND TREATMENT STRATEGIES FOR URINARY STONES 2017 Review of NASA s Evidence Reports on Human Health Risks John C Lieske, MD July 27, 2017 What types
Introduction to the primary hyperoxalurias Causes, Symptoms & Treatments. Prof. Dr. Bernd Hoppe
 Introduction to the primary hyperoxalurias Causes, Symptoms & Treatments Prof. Dr. Bernd Hoppe Hyperoxaluria Underestimated as risk factor for calcium containing stones Most frequent risk factor in our
Introduction to the primary hyperoxalurias Causes, Symptoms & Treatments Prof. Dr. Bernd Hoppe Hyperoxaluria Underestimated as risk factor for calcium containing stones Most frequent risk factor in our
Renal Tubular Acidosis
 1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics
 This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion
This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion
Functions of the kidney:
 Diseases of renal system : Normal anatomy of renal system : Each human adult kidney weighs about 150 gm, the ureter enters the kidney at the hilum, it dilates into a funnel-shaped cavity, the pelvis, from
Diseases of renal system : Normal anatomy of renal system : Each human adult kidney weighs about 150 gm, the ureter enters the kidney at the hilum, it dilates into a funnel-shaped cavity, the pelvis, from
Hydronephrosis. What is hydronephrosis?
 What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
What is hydronephrosis? Hydronephrosis Hydronephrosis describes the situation where the urine collecting system of the kidney is dilated. This may be a normal variant or it may be due to an underlying
Urine Stone Screen requirements
 Urine Stone Screen requirements Unique Identifying Index Number LP/PA/CB/CBSP030 Version number 4 Issue Date (this version) 03.08.15 Document Type Accreditation or Licensing Standard to which this applies
Urine Stone Screen requirements Unique Identifying Index Number LP/PA/CB/CBSP030 Version number 4 Issue Date (this version) 03.08.15 Document Type Accreditation or Licensing Standard to which this applies
A Rare Cause of Renal Stone Formation in Two Siblings. Chris Stockdale
 A Rare Cause of Renal Stone Formation in Two Siblings Chris Stockdale Index case-patient A Born 2000 Parents (first cousins) from Indian sub-continent Paternal Grandmother received dialysis for ESRF Possible
A Rare Cause of Renal Stone Formation in Two Siblings Chris Stockdale Index case-patient A Born 2000 Parents (first cousins) from Indian sub-continent Paternal Grandmother received dialysis for ESRF Possible
Shlomi Albert, M.D., Inc Warner Avenue, Suite 423 Fountain Valley, Ca Tel (714) Fax (714) Kidney Stone Disease in Adults
 Shlomi Albert, M.D., Inc. 11160 Warner Avenue, Suite 423 Fountain Valley, Ca 92708 Tel (714)549-3333 Fax (714)549-3334 Kidney Stone Disease in Adults Overview Kidney stones are one of the most painful
Shlomi Albert, M.D., Inc. 11160 Warner Avenue, Suite 423 Fountain Valley, Ca 92708 Tel (714)549-3333 Fax (714)549-3334 Kidney Stone Disease in Adults Overview Kidney stones are one of the most painful
Urologic Stone Disease. Urologic Stone Disease. Urologic Stone Disease. Urologic Stone Disease. Urologic Stone Disease 5/7/2010
 Diagnosis and Treatment Stephen E. Strup MD William Farish Professor and Chief of Urology Director of Minimally Invasive Urologic Surgery University of Kentucky I will not cut, even for the stone, but
Diagnosis and Treatment Stephen E. Strup MD William Farish Professor and Chief of Urology Director of Minimally Invasive Urologic Surgery University of Kentucky I will not cut, even for the stone, but
Excretory System. Biology 2201
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System. Excretory System
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Hereditary Kidney Stones
 In: Urolithiasis ISBN: 978-1-63463-500-4 Editor: Joseph Fletcher 2015 Nova Science Publishers, Inc. The exclusive license for this PDF is limited to personal website use only. No part of this digital document
In: Urolithiasis ISBN: 978-1-63463-500-4 Editor: Joseph Fletcher 2015 Nova Science Publishers, Inc. The exclusive license for this PDF is limited to personal website use only. No part of this digital document
Metabolic Stone Work-Up For Stone Prevention. Dr. Hazem Elmansy, MD, MSC, FRCSC Assistant Professor, NOSM, Urology Department
 Metabolic Stone Work-Up For Stone Prevention Dr. Hazem Elmansy, MD, MSC, FRCSC Assistant Professor, NOSM, Urology Department Faculty/Presenter Disclosure Slide Faculty: Hazem Elmansy Relationships with
Metabolic Stone Work-Up For Stone Prevention Dr. Hazem Elmansy, MD, MSC, FRCSC Assistant Professor, NOSM, Urology Department Faculty/Presenter Disclosure Slide Faculty: Hazem Elmansy Relationships with
Chapter 20 Diseases of the kidney:
 Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
Urinary System. Analyze the Anatomy and Physiology of the urinary system
 Urinary System Analyze the Anatomy and Physiology of the urinary system Kidney Bean-shaped Located between peritoneum and the back muscles (retroperitoneal) Renal pelvis funnelshaped structure at the beginning
Urinary System Analyze the Anatomy and Physiology of the urinary system Kidney Bean-shaped Located between peritoneum and the back muscles (retroperitoneal) Renal pelvis funnelshaped structure at the beginning
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Urinary Calculus Disease. Urinary Stones: Simplified Metabolic Evaluation. Urinary Calculus Disease. Urinary Calculus Disease 2/8/2008
 Urinary Stones: Simplified Metabolic Evaluation Marshall L. Stoller, M.D. Professor and Vice Chairman Department of Urology University of California San Francisco Incidence: 7-21/10,000 3 men: 1 woman
Urinary Stones: Simplified Metabolic Evaluation Marshall L. Stoller, M.D. Professor and Vice Chairman Department of Urology University of California San Francisco Incidence: 7-21/10,000 3 men: 1 woman
Inherited Calcium and Magnesium Disorders
 Inherited Calcium and Magnesium Disorders Martin Konrad University Children s Hospital Münster, Germany IPNA / ESPN Master Class, Leuven, Sep 2nd 2015 Outline Hypercalcemia Hypomagnesemia Outline Hypercalcemia
Inherited Calcium and Magnesium Disorders Martin Konrad University Children s Hospital Münster, Germany IPNA / ESPN Master Class, Leuven, Sep 2nd 2015 Outline Hypercalcemia Hypomagnesemia Outline Hypercalcemia
Acute renal colic Radiological investigation in patients with renal colic
 Acute renal colic Radiological investigation in patients with renal colic Mikael Hellström Professor Department of Radiology Sahlgrenska University Hospital Göteborg University 0.9-1.8/1.000 inhabitants
Acute renal colic Radiological investigation in patients with renal colic Mikael Hellström Professor Department of Radiology Sahlgrenska University Hospital Göteborg University 0.9-1.8/1.000 inhabitants
Pediatric metabolic bone diseases
 Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
US in non-traumatic acute abdomen. Lalita, M.D. Radiologist Department of radiology Faculty of Medicine ChiangMai university
 US in non-traumatic acute abdomen Lalita, M.D. Radiologist Department of radiology Faculty of Medicine ChiangMai university Sagittal Orientation Transverse (Axial) Orientation Coronal Orientation Intercostal
US in non-traumatic acute abdomen Lalita, M.D. Radiologist Department of radiology Faculty of Medicine ChiangMai university Sagittal Orientation Transverse (Axial) Orientation Coronal Orientation Intercostal
Excretory urography (EU) or IVP US CT & radionuclide imaging
 Excretory urography (EU) or IVP US CT & radionuclide imaging MRI arteriography studies requiring catherization or direct puncture of collecting system EU & to a lesser extent CT provide both functional
Excretory urography (EU) or IVP US CT & radionuclide imaging MRI arteriography studies requiring catherization or direct puncture of collecting system EU & to a lesser extent CT provide both functional
Lec-8 جراحة بولية د.نعمان
 4th stage Lec-8 جراحة بولية د.نعمان 11/10/2015 بسم هللا الرحمن الرحيم Ureteric, Vesical, & urethral stones Ureteric Calculus Epidemiology like renal stones Etiology like renal stones Risk factors like
4th stage Lec-8 جراحة بولية د.نعمان 11/10/2015 بسم هللا الرحمن الرحيم Ureteric, Vesical, & urethral stones Ureteric Calculus Epidemiology like renal stones Etiology like renal stones Risk factors like
Management of common uroliths through diet
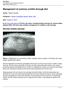 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Management of common uroliths through diet Author : Marge Chandler Categories : Canine, Companion animal, Feline, Vets Date
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Management of common uroliths through diet Author : Marge Chandler Categories : Canine, Companion animal, Feline, Vets Date
The Urinary System. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Distal renal tubular acidosis: genetic and clinical spectrum
 Distal renal tubular acidosis: genetic and clinical spectrum Sabrina Giglio Medical Genetics Unit, Meyer Children s University Hospital, University of Florence sabrina.giglio@meyer.it sabrinarita.giglio@unifi.it
Distal renal tubular acidosis: genetic and clinical spectrum Sabrina Giglio Medical Genetics Unit, Meyer Children s University Hospital, University of Florence sabrina.giglio@meyer.it sabrinarita.giglio@unifi.it
Outline. Introduction to imaging modalities of the urinary system. Case base learning of common diseases in urinary tract
 Outline Introduction to imaging modalities of the urinary system Case base learning of common diseases in urinary tract Outline Introduction to imaging modalities of the urinary system Case base learning
Outline Introduction to imaging modalities of the urinary system Case base learning of common diseases in urinary tract Outline Introduction to imaging modalities of the urinary system Case base learning
Outline. Introduction to imaging modalities of the urinary system. Case base learning of common diseases in urinary tract
 Outline Introduction to imaging modalities of the urinary system Case base learning of common diseases in urinary tract Diagnostic Investigations in Urinary System PLAIN KUB EXCRETORY UROGRAPHY RETROGRADE
Outline Introduction to imaging modalities of the urinary system Case base learning of common diseases in urinary tract Diagnostic Investigations in Urinary System PLAIN KUB EXCRETORY UROGRAPHY RETROGRADE
Kidney Stones EDITING FILE. Biochemistry Team 437 "الل ھ م لا س ھ ل إ لا ما ج ع ل ت ھ س ھ لا وأن ت ت ج ع ل الح ز ن إذ ا ش ي ت س ھ لا " Renal block
 "الل ھ م لا س ھ ل إ لا ما ج ع ل ت ھ س ھ لا وأن ت ت ج ع ل الح ز ن إذ ا ش ي ت س ھ لا " Kidney Stones Biochemistry Team 437 Color index: Doctors slides Doctor s notes Extra information Highlights Renal block
"الل ھ م لا س ھ ل إ لا ما ج ع ل ت ھ س ھ لا وأن ت ت ج ع ل الح ز ن إذ ا ش ي ت س ھ لا " Kidney Stones Biochemistry Team 437 Color index: Doctors slides Doctor s notes Extra information Highlights Renal block
EURACARE Multi-Specialist Hospital
 EURACARE Multi-Specialist Hospital PATIENT INFORMATION FORM MEDICAL MANAGEMENT OF URINARY STONE DISEASE Kidney & Urinary Stones Kidney stones, one of the most painful of the urologic disorders, have beset
EURACARE Multi-Specialist Hospital PATIENT INFORMATION FORM MEDICAL MANAGEMENT OF URINARY STONE DISEASE Kidney & Urinary Stones Kidney stones, one of the most painful of the urologic disorders, have beset
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Associated Terms: Bladder Stones, Ureteral Stones, Kidney Stones, Cystotomy, Urolithiasis, Cystic Calculi
 Associated Terms: Bladder Stones, Ureteral Stones, Kidney Stones, Cystotomy, Urolithiasis, Cystic Calculi The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery.
Associated Terms: Bladder Stones, Ureteral Stones, Kidney Stones, Cystotomy, Urolithiasis, Cystic Calculi The term "ACVS Diplomate" refers to a veterinarian who has been board certified in veterinary surgery.
Evaluation of different urinary constituent ratios in renal stone formers
 Available online at www.scholarsresearchlibrary.com Annals of Biological Research, 2010, 1 (3) : 50-55 (http://scholarsresearchlibrary.com/archive.html) ISSN 0976-1233 CODEN (USA): ABRNBW Evaluation of
Available online at www.scholarsresearchlibrary.com Annals of Biological Research, 2010, 1 (3) : 50-55 (http://scholarsresearchlibrary.com/archive.html) ISSN 0976-1233 CODEN (USA): ABRNBW Evaluation of
HYPERCALCEMIA. Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
Original Article. A Report of Infant Urolithiasis in a Tertiary Hospital S YEL, R DÜ ÜNSEL, DURSUN, F ELMALI, K YILMAZ
 HK J Paediatr (new series) 2019;24:3-8 Original Article A Report of Infant Urolithiasis in a Tertiary Hospital S YEL, R DÜ ÜNSEL, DURSUN, F ELMALI, K YILMAZ Abstract Key words Aim: The aim of the present
HK J Paediatr (new series) 2019;24:3-8 Original Article A Report of Infant Urolithiasis in a Tertiary Hospital S YEL, R DÜ ÜNSEL, DURSUN, F ELMALI, K YILMAZ Abstract Key words Aim: The aim of the present
The Excretory System
 The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
T H E K I D N E Y F O U N D A T I O N O F C A N A D A
 Kidney stones T H E K I D N E Y F O U N D A T I O N O F C A N A D A 1 Kidney stones What are the kidneys? The kidneys are the master chemists of the body. Normally, there are two of them, one on either
Kidney stones T H E K I D N E Y F O U N D A T I O N O F C A N A D A 1 Kidney stones What are the kidneys? The kidneys are the master chemists of the body. Normally, there are two of them, one on either
Educational review: role of the pediatric nephrologists in the work-up and management of kidney stones
 Pediatric Nephrology https://doi.org/10.1007/s00467-018-4179-9 EDUCATIONAL REVIEW Educational review: role of the pediatric nephrologists in the work-up and management of kidney stones Carmen Inés Rodriguez
Pediatric Nephrology https://doi.org/10.1007/s00467-018-4179-9 EDUCATIONAL REVIEW Educational review: role of the pediatric nephrologists in the work-up and management of kidney stones Carmen Inés Rodriguez
Assessment of risk factors of pediatric urolithiasis in Egypt
 Original Article Assessment of risk factors of pediatric urolithiasis in Egypt Mostafa Zakaria 1, Sherif Azab 2, Mona Rafaat 3 1 Department of Pediatrics, Faculty of medicine, Cairo University, Cairo,
Original Article Assessment of risk factors of pediatric urolithiasis in Egypt Mostafa Zakaria 1, Sherif Azab 2, Mona Rafaat 3 1 Department of Pediatrics, Faculty of medicine, Cairo University, Cairo,
Nursing Care for Children with Genitourinary Dysfunction I
 Nursing Care for Children with Genitourinary Dysfunction I 1 Assessment of renal function Clinical manifestations Laboratory tests Urinalysis Urine culture and sensitivity Renal/bladder ultrasound Testicular
Nursing Care for Children with Genitourinary Dysfunction I 1 Assessment of renal function Clinical manifestations Laboratory tests Urinalysis Urine culture and sensitivity Renal/bladder ultrasound Testicular
UTI are the most common genitourinary disease of childhood. The prevalence of UTI at all ages is girls and 1% of boys.
 UTI are the most common genitourinary disease of childhood. The prevalence of UTI at all ages is girls and 1% of boys. 1-3% of Below 1 yr. male: female ratio is 4:1 especially among uncircumcised males,
UTI are the most common genitourinary disease of childhood. The prevalence of UTI at all ages is girls and 1% of boys. 1-3% of Below 1 yr. male: female ratio is 4:1 especially among uncircumcised males,
Renal Stones in Children
 Renal Stones in Children Scottish Paediatric Renal & Urology Network Frank Willis Renal Unit RHSC-Yorkhill Glasgow May 2009 Aetiology Differs from adults Varies with geography & over time Most have primary
Renal Stones in Children Scottish Paediatric Renal & Urology Network Frank Willis Renal Unit RHSC-Yorkhill Glasgow May 2009 Aetiology Differs from adults Varies with geography & over time Most have primary
Historical Figures with Stone Disease. Egyptian mummies Pliny Sr. Walter Scott Sydenham Benjamin Franklin Napoleon Lyndon B.
 Historical Figures with Stone Disease Egyptian mummies Pliny Sr. Walter Scott Sydenham Benjamin Franklin Napoleon Lyndon B. Johnson goals Review epidemiology of stones and hypercalciuria Discuss risk factors
Historical Figures with Stone Disease Egyptian mummies Pliny Sr. Walter Scott Sydenham Benjamin Franklin Napoleon Lyndon B. Johnson goals Review epidemiology of stones and hypercalciuria Discuss risk factors
UROLITHIASIS ADULT & PEDIATRIC
 DEFINITION Calculi (stone) in the urinary tract (kidneys, bladder, urethra). Often causes renal colic, a pain produced by the presence and movement of a stone within the ureter or renal pelvis. Some clients
DEFINITION Calculi (stone) in the urinary tract (kidneys, bladder, urethra). Often causes renal colic, a pain produced by the presence and movement of a stone within the ureter or renal pelvis. Some clients
Calcium Oxalate Urolithiasis
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Calcium Oxalate Urolithiasis (Calcium Oxalate Stones in the Urinary Tract) Basics
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Calcium Oxalate Urolithiasis (Calcium Oxalate Stones in the Urinary Tract) Basics
Oxalate (urine, plasma)
 Oxalate (urine, plasma) 1 Name and description of analyte 1.1 Name of analyte Oxalate 1.2 Alternative names 1.3 NLMC code To follow 1.4. Function of analyte Oxalate is a metabolic end product primarily
Oxalate (urine, plasma) 1 Name and description of analyte 1.1 Name of analyte Oxalate 1.2 Alternative names 1.3 NLMC code To follow 1.4. Function of analyte Oxalate is a metabolic end product primarily
EXCRETION IN HUMANS 31 JULY 2013
 EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
EXCRETION IN HUMANS 31 JULY 2013 Lesson Description In this lesson we: Discuss organs of excretion Look at the structure of the urinary system Look at the structure and functioning of the kidney Discuss
Diet and fluid prescription in stone disease
 http://www.kidney-international.org & 2006 International Society of Nephrology mini review Diet and fluid prescription in stone disease EN Taylor 1 and GC Curhan 1,2 1 Renal Division, Department of Medicine,
http://www.kidney-international.org & 2006 International Society of Nephrology mini review Diet and fluid prescription in stone disease EN Taylor 1 and GC Curhan 1,2 1 Renal Division, Department of Medicine,
Pediatric GU Dysfunction
 Pediatric GU Dysfunction Assessment of pediatric renal function Signs and symptoms Laboratory tests Radiological tests Nursing considerations Psychosocial and developmental considerations GU Disorders
Pediatric GU Dysfunction Assessment of pediatric renal function Signs and symptoms Laboratory tests Radiological tests Nursing considerations Psychosocial and developmental considerations GU Disorders
Dietary Management of Nephrolithiasis. Sarah Yttri, NP Duke University Duke Comprehensive Kidney Stone Center
 Dietary Management of Nephrolithiasis Sarah Yttri, NP Duke University Duke Comprehensive Kidney Stone Center None Disclosures Prevalence 1 in 11 individuals in the US 10.6% of men, 7.1% of women 70% increase
Dietary Management of Nephrolithiasis Sarah Yttri, NP Duke University Duke Comprehensive Kidney Stone Center None Disclosures Prevalence 1 in 11 individuals in the US 10.6% of men, 7.1% of women 70% increase
Approach to the Patient with Nephrolithiasis; The Stone Quiz. Farahnak Assadi* 1, MD
 Education Article Iran J Ped Sep 2007; Vol 17 (No 3), Pp:283-292 Approach to the Patient with Nephrolithiasis; The Stone Quiz Farahnak Assadi* 1, MD 1. Pediatric Nephrologist, Rush University Medical Center,
Education Article Iran J Ped Sep 2007; Vol 17 (No 3), Pp:283-292 Approach to the Patient with Nephrolithiasis; The Stone Quiz Farahnak Assadi* 1, MD 1. Pediatric Nephrologist, Rush University Medical Center,
Kidneycentric. Follow this and additional works at:
 Washington University School of Medicine Digital Commons@Becker All Kidneycentric 2014 Gitelman syndrome David Steflik Washington University School of Medicine in St. Louis Follow this and additional works
Washington University School of Medicine Digital Commons@Becker All Kidneycentric 2014 Gitelman syndrome David Steflik Washington University School of Medicine in St. Louis Follow this and additional works
PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY. THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel
 PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel. 0925111552 Professional skills-2 THE URINARY SYSTEM The urinary system (review anatomy and physiology)
PROFESSIONAL SKILLS 1 3RD YEAR SEMESTER 6 RADIOGRAPHY THE URINARY SYSTEM Uz. Fatema shmus aldeen Tel. 0925111552 Professional skills-2 THE URINARY SYSTEM The urinary system (review anatomy and physiology)
GUIDELINES ON UROLITHIASIS
 GUIDELINES ON UROLITHIASIS (Text updated May 2005) H.G. Tiselius (chairman), D. Ackermann, P. Alken, C. Buck, P. Conort, M. Gallucci, T. Knoll Eur Urol 2001;40:362-371 Introduction Urinary stone disease
GUIDELINES ON UROLITHIASIS (Text updated May 2005) H.G. Tiselius (chairman), D. Ackermann, P. Alken, C. Buck, P. Conort, M. Gallucci, T. Knoll Eur Urol 2001;40:362-371 Introduction Urinary stone disease
A Phase 1/2 Trial of Lumasiran (ALN-GO1), an Investigational RNAi Therapeutic for Primary Hyperoxaluria Type 1
 A Phase 1/2 Trial of Lumasiran (ALN-GO1), an Investigational RNAi Therapeutic for Primary Hyperoxaluria Type 1 OxalEurope Meeting Naples, Italy 8 June 2018 2018 Alnylam Pharmaceuticals, Inc. Background
A Phase 1/2 Trial of Lumasiran (ALN-GO1), an Investigational RNAi Therapeutic for Primary Hyperoxaluria Type 1 OxalEurope Meeting Naples, Italy 8 June 2018 2018 Alnylam Pharmaceuticals, Inc. Background
Urinary tract infections, renal malformations and scarring
 Urinary tract infections, renal malformations and scarring Yaacov Frishberg, MD Division of Pediatric Nephrology Shaare Zedek Medical Center Jerusalem, ISRAEL UTI - definitions UTI = growth of bacteria
Urinary tract infections, renal malformations and scarring Yaacov Frishberg, MD Division of Pediatric Nephrology Shaare Zedek Medical Center Jerusalem, ISRAEL UTI - definitions UTI = growth of bacteria
MEDICAL STONE MANAGEMENT MADE EASY PRACTICAL ADVICE
 MEDICAL STONE MANAGEMENT MADE EASY PRACTICAL ADVICE Comprehensive Kidney Stone Center at Duke University Medical Center Durham, North Carolina Glenn M. Preminger, M.D. UCLA State-of-the Art Urology 02
MEDICAL STONE MANAGEMENT MADE EASY PRACTICAL ADVICE Comprehensive Kidney Stone Center at Duke University Medical Center Durham, North Carolina Glenn M. Preminger, M.D. UCLA State-of-the Art Urology 02
Summary and conclusions
 Summary and conclusions 7 Chapter 7 68 Summary and conclusions Chapter 1 provides a general introduction to this thesis focused on the use of ultrasound (US) in children with abdominal problems. The literature
Summary and conclusions 7 Chapter 7 68 Summary and conclusions Chapter 1 provides a general introduction to this thesis focused on the use of ultrasound (US) in children with abdominal problems. The literature
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
Urinary stone distribution in Samawah: current status and variation with age and sex a cohort study
 www.muthjm.com Muthanna Medical Journal 2015; 2(2):93-98 Urinary stone distribution in Samawah: current status and variation with age and sex a cohort study Saad Hallawee 1* The aim of the study was to
www.muthjm.com Muthanna Medical Journal 2015; 2(2):93-98 Urinary stone distribution in Samawah: current status and variation with age and sex a cohort study Saad Hallawee 1* The aim of the study was to
This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics
 This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion
This is the written version of our Hot Topic video presentation available at: MayoMedicalLaboratories.com/hot-topics Welcome to Mayo Medical Laboratories Hot Topics. These presentations provide short discussion
RENAL SCINTIGRAPHY IN THE 21 st CENTURY
 RENAL SCINTIGRAPHY IN THE 21 st CENTURY 99m Tc- MAG 3 with zero time injection of Furosemide (MAG 3 -F 0 ) : A Fast and Easy Protocol, One for All Indications Clinical Experience Congenital Disorders PROTOCOL
RENAL SCINTIGRAPHY IN THE 21 st CENTURY 99m Tc- MAG 3 with zero time injection of Furosemide (MAG 3 -F 0 ) : A Fast and Easy Protocol, One for All Indications Clinical Experience Congenital Disorders PROTOCOL
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University
 RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
RENAL FAILURE IN CHILDREN Dr. Mai Mohamed Elhassan Assistant Professor Jazan University OBJECTIVES By the end of this lecture each student should be able to: Define acute & chronic kidney disease(ckd)
Urinary System Part of the Excretory System
 Urinary System Part of the Excretory System Bellwork **only write the term and underlined definition INCONTINENCE involuntary urination, often seem in older persons, or due to illness and disease ENURESIS
Urinary System Part of the Excretory System Bellwork **only write the term and underlined definition INCONTINENCE involuntary urination, often seem in older persons, or due to illness and disease ENURESIS
Pediatric urinary tract infection. Dr. Nariman Fahmi Pediatrics/2013
 Pediatric urinary tract infection Dr. Nariman Fahmi Pediatrics/2013 objectives EPIDEMIOLOGY CAUSATIVE PATHOGENS PATHOGENESIS CATEGORIES OF URINARY TRACT INFECTIONS AND CLINICAL MANIFESTATIONS IN pediatrics
Pediatric urinary tract infection Dr. Nariman Fahmi Pediatrics/2013 objectives EPIDEMIOLOGY CAUSATIVE PATHOGENS PATHOGENESIS CATEGORIES OF URINARY TRACT INFECTIONS AND CLINICAL MANIFESTATIONS IN pediatrics
Urologic investigations
 Urologic investigations د. Laboratory studies EXAMINATION OF URINE Urinalysis: Urinalysis is one of the most important and useful urologic tests available. Reasons for inadequate urinalyses include: (1)
Urologic investigations د. Laboratory studies EXAMINATION OF URINE Urinalysis: Urinalysis is one of the most important and useful urologic tests available. Reasons for inadequate urinalyses include: (1)
Lecture 7. The Urinary System
 Lecture 7 The Urinary System Copyright 2006 Thomson Delmar Learning The Urinary System The urinary system removes wastes from the body The urinary system also maintains homeostasis or a constant internal
Lecture 7 The Urinary System Copyright 2006 Thomson Delmar Learning The Urinary System The urinary system removes wastes from the body The urinary system also maintains homeostasis or a constant internal
Case MDCT 3D reconstructed features of posterior urethral valve
 Case 12688 MDCT 3D reconstructed features of posterior urethral valve Hidayatullah Hamidi Third year Resident of Radiology French medical institute for children Radiology Department; Kabul, Afghanistan;
Case 12688 MDCT 3D reconstructed features of posterior urethral valve Hidayatullah Hamidi Third year Resident of Radiology French medical institute for children Radiology Department; Kabul, Afghanistan;
PHYSICAL CHARACTERISTICS, QUALITATIVE AND QUANTITATIVE ANALYSIS OF URINARY STONES (PATHARI)
 Int. J. Chem. Sci.: 11(1), 2013, 457463 ISSN 0972768X www.sadgurupublications.com PHYSICAL CHARACTERISTICS, QUALITATIVE AND QUANTITATIVE ANALYSIS OF URINARY STONES (PATHARI) SUMAN PARIHAR a, PRASOON HADA
Int. J. Chem. Sci.: 11(1), 2013, 457463 ISSN 0972768X www.sadgurupublications.com PHYSICAL CHARACTERISTICS, QUALITATIVE AND QUANTITATIVE ANALYSIS OF URINARY STONES (PATHARI) SUMAN PARIHAR a, PRASOON HADA
PRINCIPLE OF URINALYSIS
 PRINCIPLE OF URINALYSIS Vanngarm Gonggetyai Objective Can explain : the abnormalities detected in urine Can perform : routine urinalysis Can interprete : the results of urinalysis Examination of urine
PRINCIPLE OF URINALYSIS Vanngarm Gonggetyai Objective Can explain : the abnormalities detected in urine Can perform : routine urinalysis Can interprete : the results of urinalysis Examination of urine
HMM 4401 Genito-urinary tract diseases
 HMM 4401 Genito-urinary tract diseases Urine production Core elements: Glomerulus, proximal and distal convoluted tube, loop of Henle, collecting tubules, ureters, bladder, sphincter, uretra, and out
HMM 4401 Genito-urinary tract diseases Urine production Core elements: Glomerulus, proximal and distal convoluted tube, loop of Henle, collecting tubules, ureters, bladder, sphincter, uretra, and out
Evaluation of the Recurrent Stone Former
 Urol Clin N Am 34 (2007) 315 322 Evaluation of the Recurrent Stone Former Paramjit S. Chandhoke, MD, PhD* Department of Urology, Northwest Permanente, Portland, OR, USA At one time, metabolic kidney stone
Urol Clin N Am 34 (2007) 315 322 Evaluation of the Recurrent Stone Former Paramjit S. Chandhoke, MD, PhD* Department of Urology, Northwest Permanente, Portland, OR, USA At one time, metabolic kidney stone
GENERAL URINE EXAMINATION (URINE ANALYSIS)
 GENERAL URINE EXAMINATION (URINE ANALYSIS) Physiology Lab-8 December, 2018 Lect. Asst. Zakariya A. Mahdi MSc Pharmacology Background Urine (from Latin Urina,) is a typically sterile liquid by-product of
GENERAL URINE EXAMINATION (URINE ANALYSIS) Physiology Lab-8 December, 2018 Lect. Asst. Zakariya A. Mahdi MSc Pharmacology Background Urine (from Latin Urina,) is a typically sterile liquid by-product of
Urinary Stones. Urinary Stones. Published on: 1 Jul What are the parts of the urinary system?
 Published on: 1 Jul 2016 Urinary Stones Urinary Stones What are the parts of the urinary system? The urinary system consists of the kidneys, ureters, urinary bladder, and urethra. What are the functions
Published on: 1 Jul 2016 Urinary Stones Urinary Stones What are the parts of the urinary system? The urinary system consists of the kidneys, ureters, urinary bladder, and urethra. What are the functions
Struvite Urolithiasis in Cats
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Struvite Urolithiasis in Cats (Struvite Stones in the Urinary Tract of Cats) Basics
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Struvite Urolithiasis in Cats (Struvite Stones in the Urinary Tract of Cats) Basics
Nephrolithiasis Outline Epidemiology
 Nephrolithiasis Brian Duty, M.D. Assistant Professor Department of Urology Oregon Health & Sciences University Outline Epidemiology Pathophysiology Clinical Presentation Diagnosis Management Medical Surgical
Nephrolithiasis Brian Duty, M.D. Assistant Professor Department of Urology Oregon Health & Sciences University Outline Epidemiology Pathophysiology Clinical Presentation Diagnosis Management Medical Surgical
SCE Questions. Dr T
 SCE Questions Dr T Scale @drscale86 #RenalSCE http://www.welshkidney.org/ Question 1 A 33 year old man presented with a renal calculi, he eventually passes a stone which gets analysed and is mostly calcium
SCE Questions Dr T Scale @drscale86 #RenalSCE http://www.welshkidney.org/ Question 1 A 33 year old man presented with a renal calculi, he eventually passes a stone which gets analysed and is mostly calcium
PARTS OF THE URINARY SYSTEM
 EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
RENAL TUBULAR ACIDOSIS An Overview
 RENAL TUBULAR ACIDOSIS An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY CLINICAL BIOCHEMISTRY PBL MBBS IV VJ. Temple 1 What is Renal Tubular
RENAL TUBULAR ACIDOSIS An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY CLINICAL BIOCHEMISTRY PBL MBBS IV VJ. Temple 1 What is Renal Tubular
Instrumental determination of electrolytes in urine. Amal Alamri
 Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
R adio logical investigations of urinary system
 R adio logical investigations of urinary system There are 4 main radiological Ix: 1 IVU: Intravenous urography. 2- U/S 3-CT scan 4-Radioisotope scan. Others (not frequently used): MRI, arteriography, antegrade
R adio logical investigations of urinary system There are 4 main radiological Ix: 1 IVU: Intravenous urography. 2- U/S 3-CT scan 4-Radioisotope scan. Others (not frequently used): MRI, arteriography, antegrade
