بسن هلال الرحون الرحين
|
|
|
- Norman Goodwin
- 6 years ago
- Views:
Transcription
1 1 P a g e 3
2 بسن هلال الرحون الرحين Today we will continue talking about the histology of the kidney, but before we start we will go over a quick review of what we took yesterday which s about the different histological divisions of the structures within the kidney and we said that when we look under the microscope we can distinguish two embryologically different structures : 1) the nephron (which's a greek word that means kidney) 2) the collecting tubules *the nephron having the uriniferous tubule as a functional unit is the main part of the functional kidney. It ( the nephron) has two parts : 1) a small tiny body called the renal corpuscle which s located only in the cortex So if you see in (fig.1) the border between the medulla and the cortex the renal corpuscle is within the cortex The renal corpuscle is further subdivided into : A) the blood capillaries inside called the glomerulus ( the wool tuft الصوف (كرة it s actually condensed blood capillaries *down in (fig.1) the red part is the glomerulus and it s surrounded by a capsule (bowman s capsule) with a cavity inside it. B) the second part of the corpuscle is the bowman s capsule ( named after Sir William bowamn s a British physician who described this capsule) with a cavity inside this capsule And its further subdivided into: I) a visceral layer enclosing the blood capillaries and its made of special cells called podocytes ( podo:feet, cytes:cells, the cells with feet). II) an outer parietal layer made of simple squamous epithelium. Now, between the two layers there's the bowman s space which s very important, because it contains the filtrated blood which has ions and the plasma fluid. 2 P a g e
3 2) getting out of the corpuscle are the renal tubules and they're divided according to their location with respect to the corpuscle, the ones which are continues with the bowman s space are called the proximal tubules, the most proximal part is highly coiled thus called the convoluted part of the proximal tubules, then as they become closer to the medulla they straighten up so we call them the recta part of the proximal tubules Again>> pars convoluta which s the convoluted part and pars recta which s the straight part The proximal tubules are lined with simple cuboidal epithelium, But once they enter the medulla they become lined with simple squamous epithelium and they suddenly become very narrow their diameter decreases from 60 µm down to 20 µm and we will call them the loop of Henle because once they enter they re actually descending then they will loop back and ascend thus we called them a loop As they ascend they widen again and we will call them distal tubules starting with a straight part ( pars recta distalis) and continuing as the distal convoluted part, here s the end of the nephron, and it will be draining in the collecting tubules. Quick review: the nephron is made up of : 1) renal corpuscle with its parts the glomerulus and bowman s capsule 2) and renal tubules with its parts proximal, the loop of Henle and the distal tubules 3 P a g e
4 4 P a g e Figure 1 Now, the collecting tubules have three parts which are : a) cortical collecting ducts that are located in the cortex b) medullary collecting ducts c) papillary duct of bellini (named after Lorenzo Bellini an Italian anatomist who was a prof. of medicine at pisa university) which s a very large duct ( µm) made up of the union of all the medullary collecting ducts and its located in the inner part of the medulla close to the papilla. Notice that its called papillary duct since its close to the renal papilla. In the previous lecture we talked about the renal corpuscle and the mechanism of filtration and we said there s a specific kind of filter made up of three layers the fenestrae in the endothelium of the blood capillary,basal lamina which s made up of lamina densa and 2 lamina rara and the filtration slits (or clefts) between the pedicles of the podocytes. Today we will be talking about the renal tubules starting with the proximal tubules. Proximal tubules In a cross-section across them (figure 2) we can see a wide opening with empty lumen around 60 m in diameter that is surrounded by simple cuboidal epithelium.
5 They re 14 mm long. Figure 2 The histological distinguishing features of these tubules are : A)**the Eosinophilic cytoplasm which s due to their richness in mitochondria. They need the mitochondria to produce energy for the active transport of ions as the proximal tubules are responsible for 80% of the resorption of Na and Cl ions from the urine and returning them back into the blood circulation within the kidney interstitium. B)**Striated apical surface (apical microvilli or brush boarder) to increase the surface area (figures 3 and 4) in addition to them we can see a network of canaliculi in the Electron micrograph below (fig.4). Figure 3 5 P a g e
6 Figure 4 Notice in this figure the tubular mitochondria which are larger than the normal mitochondria, and the ion channels (Na channels) which are responsible for active transportation of Na from the lumen to the interstitium are located at the basal membrane of these cells. C) They have well defined basement membrane. D) **Few basally placed nuclei (fig 5), because the cells are wide so the nuclei appear to be few. 6 P a g e
7 Figure 5 E) Indistinct lateral membrane because they re interdigitated with each other. *the main distinguishing features are A, B and D which are again the eosinophillic cytoplasm, the brush boarder and the relatively fewer basal nuclei compared to the distal tubules. As we said the proximal tubules can be structurally divided into two parts: 1)Pars Convoluta (PCT) Near renal corpuscle in the cortex 2) Pars Recta (descending thick limb of Henle s loop) This part extends from the inner cortex until the junction between the outer stripe and the inner stripe of the outer zone of the medulla (fig.6) where it ends and the loop of Henle begins. 7 P a g e
8 8 P a g e Figure 6 The functions of cells in the proximal tubules : I) Resorption of 65-80% of Na +, Cl -, & water 1. Na+ is actively pumped out of the cells 2. Followed by Cl- to maintain electrical neutrality 3. Followed by water to maintain osmotic equilibrium II) Resorption of all glucose & AAs III) Elimination of organic solutes, drugs, & toxins Loop of Henle (Ansa Nephroni) (refer to the box) U-shaped thin (12 20 m) tube consisting of simple sq. epith. Divided into 3 regions - Descending thin limb highly permeable to water
9 - Henle s loop - Ascending thin limb low permeability to water * the length and extension of Henle s loop depends on the type of nephron. Remember we have two types of nephrons : a) cortical nephrons accounting for 80-85% located in the cortical zone of the cortex. named after Friedrich Gustav Henle whose an anatomist, histologist and pathologist in the university of Heidelberg in Germany,he s a very famous person because of his anatomical discoveries upon of which the loop of Henle being the most important,however he also discovered a common tendon between two muscles in the abdomen the transverses abdominus and the internal oblique that joins the pubic bone and he called it Henle s ligament but the name was changed later into conjoint tendon, and he also discovered a small spine in the external auditory meatus at the upper posterior boarder he called it Henle s spine. Henle was the supervisor for a famous student during his PHD his name is Robert Koch, Robert s PHD thesis was about the germ theory of disease, and since Henle was his supervisor he was considered as a co-founder of this theory. In these nephrons the length of the loop of Henle which will be in the outer zone of the medulla is no more than 1-2 mm and even sometimes they re totally absent. (Fig.7) 9 P a g e Figure 7 b) juxtamedullary nephrons accounting for 15-20%
10 The length of the loop of Henle in these nephrons is 9-10 mm it extends until the renal papilla deep in the medulla. This is very important in determining the volume and the concentration of urine because the descending part of the loop of Henle is highly permeable to water however the permeability decreases as you go forward to the ascending part until reaching the distal tubules which are impermeable to water. How to distinguish the loop of Henle in a histological section? As we said they re made up of simple squamous epithelium similar to the cells of the endothelium of the blood capillaries. We know squamous cells are flat so the nuclei will appear bulging into the lumen similar to what we see in capillaries (fig.8). The only distinguishing feature between the blood capillary and the loop of Henle is that the former has blood cells in their lumen (fig 9). Figure 8 10 P a g e
11 Figure 9 Distal tubules As the loop of Henle ascend up again it starts to widen however it will not be as wide as it was in the proximal tubules, it only widens to about µm and it will be called the distal tubule. The distal tubule starts at the border between the inner and outer zones of the medulla. They re narrower and much shorter than the PT. Their convoluted part is much less convoluted than that of the PT and that s why they re shorter. They re divided into 3 parts: -Pars recta (Ascending thick limb of Henle s loop) As this part ascends up to the cortex it ll go to become in close proximity to its own renal corpuscle specifically the vascular ball in the area between the efferent and afferent arterioles that enter and leave the corpuscle (fig.10) and this area is called the Macula Densa. -Macula Densa -Pars convoluta distalis (DCT) 11 P a g e
12 Figure 10 Pars Recta (Ascending Thick Limb of Henle s Loop) Its diameter is 40 µm It starts at the junction between the outer and inner zones of the medulla and ascends up into the cortex. Its impermeable to water and urea, but it has pumps for active transportation of Cl and Na follows passively. Remember in the proximal tubules the Na was actively transported. Now, at the end of the Pars Recta distalis the urine will be hypotonic (low concentration of Cl and Na) but it will have high concentration of urea and water. As it (distal tubules) ascends up in the area between afferent and efferent arteriole we will call this part the Macula Densa (macula= spot, densa= dense) why it is dense? Figure P a g e
13 Looking into a histological section (fig.11) we can see part of the distal tubule, they call it macula densa because the cells are becoming narrow and tall, as they are changing to become taller and narrower the nuclei will become closer to each other giving the dense appearance so when you look under a histological staining you will see that the nuclei are densly packed appearing as a densely stained spot called the macula densa. So the macula densa are the cells of the distal renal tubules located near their own renal corpuscle in the vascular ball trapped between the afferent and efferent arterioles. The cells are tall and narrow so the nuclei become closer to each other. It is part of a system called the juxtaglomerular apparatus (juxta= close to, glomerular= glomerulus).this apparatus is very important because it s involved in monitoring blood pressure through detecting sodium concentration. The last part of the distal tubule is the convoluted part, when they become convoluted they will widen a little bit more (from 40 µm in pars recta to 45 µm in diameter in the convoluted part) however they are much shorter than the proximal convoluted tubules, for every 7 turns of the proximal part there is a single turn of the distal part. 13 P a g e Figure 12 Therefore looking into a cross section (fig.12) you will see so many proximal tubules compared to distal tubules (pale in color and more nuclei). The ratio in a histological section between the proximal and distal tubules profiles is 7:1, so for every 7 proximal tubules there is 1 distal tubule, why is that? Because the distal
14 convoluted tubules are much shorter. Look at the asterisk in the histological section, what are these? this is simple squamous with bulging nuclei they can be either loop of Henle or blood capillaries but if they were blood capillaries they must contain blood cells but those are empty. So they are actually loop of Henle but why they are seen in the cortex? This is to tell you that what you study in medicine it's not always 1+1=2, what we study is the most common scenario so we can always find variations, remember when we spoke about the renal arteries we said that 30% of the population there is extra accessory renal artery therefore in some kidney sections you can see part of the loop of Henle in the cortex, in these cases instead of the pars recta, the loop of Henle will continue until the cortex. There are two main things ultra-structurally to distinguish cells of distal convoluted tubules from the proximal: 1- No brush border (microvilli) 2- Nuclei are located on the apical surface instead of being central or basal as in the proximal part and contain much less mitochondria Figure 13 In the ascending part there are chloride pumps pumping chloride outside and sodium will follow but it s impermeable to water, this is the case in the pars recta. After the macula densa, in the distal convoluted part it s a different story it is only 14 P a g e
15 functional in ion transportation when influenced by aldosterone hormone (a mineralocortcoid secreted by zona glomerulosa of adrenal cortex related to reabsorption of minerals) When aldosterone is secreted by the adrenal cortex it will influence the cuboidal epithelial cells in the distal convoluted tubules to do resorption of the remaining sodium through Na/K pumps in their basal membrane. Why does this happen? This is related to the juxtaglomerular apparatus. As the urine ascends in the pars recta and reaches the macula densa all the chloride and most of the sodium are gone with a little amount of sodium only remaining there, so the macula densa cells are specialized in detecting a specific threshold of sodium. If the concentration of sodium is above this threshold the macula densa cells will be stimulated through their receptors for the concentration of sodium, the cells will send signals through their basal part to the juxtaglomerular cells which are modified smooth muscle cells in the tunica media of afferent and efferent arteriole but mainly in the afferent arteriole. They are modified because they contain specific secretory granules that are rich in an enzyme called renin. When sodium concentration goes above the threshold it will be detected by the macula densa cells which are in a very close intimate contact with the juxtaglomerular cells as there is no basal lamina because we need direct communication between the cells. The basal membrane of macula densa cells are in close contact with the apical membrane of the juxtaglomerular cells, the stimulation in macula densa will stimulate juxtaglomerular cells which will then secrete renin into the circulation through their basal membrane. 15 P a g e
16 Figure 14 So the juxtaglomerular apparatus is made up of macula densa cells in the distal tubule, juxtaglomerular cells in the arterioles and in between them there are extraglomerular mesangial cells also called lacis cells (lacis from the word (رباط= lace because they tie the glomerular cells with the macula densa, they are forming like a lace as you can see in the figure above. They are also called polar cushion cells ( (هخدة because they are forming a cushion for the vascular ball of the glomerulus separating between the afferent and efferent arteriole. The exact function of these cells until now is unknown however some theories and some published articles revealed that they contain secretory granules for renin also and other secretory granules containing erythropoietin hormone which is involved in producing RBCs in the bone marrow. We have two types of mesangial cells 1- Extraglomerular mesangial cells : the ones at the vascular ball 2- Intraglomerular mesangial cells : the ones which are inside within the glomerulas between the blood capillaries Where does the word mesangial come from? Mes from the greek word mesos which means in the middle, angial from the greek word angio which means blood vessels because they are in the middle of blood vessels Intraglomerular are between the blood capillaries, the extraglomerular are between 16 P a g e
17 the afferent and efferent arterioles so both are mesangial cells but the difference is that the extraglomerular cells are part of the juxtaglomerular apparatus while the intraglomerular cells have two functions: 1- They are phagocytic cells involved in the regeneration of the basal lamina A student asked how do the structures pass through the collagen fibers in the basal lamina? The collagen fibers in the basal lamina are not closing the way totally there are spaces and if a large molecule sometimes pass between it can destroy these collagen fibers so we need to repair them and sometimes large proteins like the albumin (more than 69 kilodalton) gets stuck in the basal lamina so we need cells that can phagocytose the large proteins and the broken collagen fibers in addition to regenerating the basal lamina, and that is the function of the intraglomerular cells. 2- They are pericyte-like cells (peri= around, cyte=cells) located around the podocytes and the blood capillaries containing contractile proteins and once they contract they constrict the blood capillaries reducing the blood flow through the glomerulus The juxtaglomerular apparatus works through the RAAS signaling pathway which indicates the renin-angiotensin-aldosterone system. As we said when the urine reaches the macula densa with a higher concentration of sodium (above the threshold) and after being detected by their apical membrane, the basal membrane of the macula densa will stimulate the juxtaglomerular cells which will secrete renin, renin now goes to the blood where there is a protein called angiotensinogen, in blood the angiotensinogen will be broken down into angiotensin-i an inactive decapeptide (10 aminoacids) by the action of renin (that's why the old name of renin was angiotensinase).as angiotensin-i is circulating in the blood it will reach into the endothelial cells in the lungs which will secrete another enzyme called angiotensin-converting enzyme (ACE) that will break two aminoacids from the decapeptide forming an octapeptide called angiotensin-ii which is the active form of angiotensin. Angiotensin-II will go and do two things : 1- Goes to the zona glomerulosa of the adrenal cortex stimulating the cells to secrete aldosterone, aldosterone will go to the distal convoluted tubules and stimulate the cells to resorb sodium through Na/K pump and chloride will follow. 2- Goes to the smooth muscles in tunica media of blood vessels and stimulate them to contract causing constriction which will increase the speed of blood flow raising the blood pressure. 17 P a g e
18 Collecting tubules are of different embryological origin from the nephrons however they fuse together later on in the development. Collecting tubules are of 3 types : 1- Cortical collecting ducts (medullary rays) 2- Medullary collecting ducts 3- Papillary ducts of bellini (formed by the joining of the medullary collecting ducts) Collecting tubules are impermeable to water however under the influence of antidiuretic hormone (ADH) also called vasopressin (produced by hypothalamus and stored in the posterior pituitary gland) they will become permeable to water and will allow it to flow back instead of being excreted by the urine. Figure 15 Collecting tubules whether they are cortical (shown as rays in the figure) or medullary they are made up of simple cuboidal epithelium. Cortical collecting ducts: Have two types of cuboidal cells 1- Principal (main) cells with few mitochondria and short sparse microvilli, their function is unknown. 2- Intercalated cells containing many microvilli, numerous apical vesicles and abundant mitochondria because they are involved in active transportation of hydrogen ions against high concentration gradient. If the hydrogen concentration was more in the urine it will be transported from inside the cells into the urine and if it was more in the cells it will be resorbed from the urine. So they have contain 18 P a g e
19 two types of active channels out or in depending on the concentration of hydrogen ions that's why they are involved in the regulation of acid-base balance in the body. Medullary collecting ducts : 1- Larger caliber than cortical tubules 2- Located in the outer zone of medulla 3- Contain similar types of cells Figure 16 Figure 17 Papillary Ducts : 1- Formed by union of medullary tubules µm in diameter 3- Formed by tall columnar principal cells only 19 P a g e
20 Figure 18 As these collecting tubules become close to the renal papilla they will enlarge and join together to become the papillary ducts of bellini, moving to the papillary ducts the cells change from simple cuboidal to become simple columnar epithelium, the papillary ducts will open to the minor calyx and the epithelium will become transitional epithelium. In the minor calyx, major calyx, renal pelvis, ureter, and bladder the epithelium is transitional epithelium. Figure P a g e
21 A quick review of the different types of epithelium : *Visceral layer of bowman's capsule is made up of podocytes, parietal layer of simple squamous *Proximal tubules- simple cuboidal *Loop of Henle- simple squamous *Distal tubules- simple cuboidal except in the area of macula densa *Collecting ducts ( cortical and medullary)-simple cuboidal *Papillary ducts- simple columnar *Minor calyx until the bladder- transitional epithelium Remember as we go down the cells become paler,smaller and the nuclei become closer to each other. All slides are included. If you found any mistake don't think of tagging us و سالنتكم Made with love by: Sarat Al-shaba an and Lina Bshara 21 P a g e
22 22 P a g e
Kidney Structure. Renal Lobe = renal pyramid & overlying cortex. Renal Lobule = medullary ray & surrounding cortical labryinth.
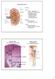 Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Urinary System kidneys, ureters, bladder & urethra
 Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra
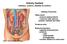 Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Lab Activity 31. Anatomy of the Urinary System. Portland Community College BI 233
 Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Urinary system. Urinary system
 INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph
 The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
Urinary System. Dr. Ahmed Maher Dr. Ahmed Manhal
 Urinary System Dr. Ahmed Maher Dr. Ahmed Manhal Presentation Map Kidney (cortex & medulla). Nephron. Duct system. Juxtaglomerular apparatus. Ureter, bladder & urethra. Definition & General Structure The
Urinary System Dr. Ahmed Maher Dr. Ahmed Manhal Presentation Map Kidney (cortex & medulla). Nephron. Duct system. Juxtaglomerular apparatus. Ureter, bladder & urethra. Definition & General Structure The
Histology Urinary system
 Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
THE RENAL / URINARY SYSTEM
 1 THE RENAL / URINARY SYSTEM Definition/Description: The Renal/Urinary system is the body system, which plays a vital role in the maintenance of homeostasis by the following processes: 1. Production of
1 THE RENAL / URINARY SYSTEM Definition/Description: The Renal/Urinary system is the body system, which plays a vital role in the maintenance of homeostasis by the following processes: 1. Production of
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Figure 26.1 An Introduction to the Urinary System
 Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
H I S T O L O G Y O F T H E U R I N A R Y S Y S T E M
 SCPA 602- Anatomical Basis For Pathological Study H I S T O L O G Y O F T H E U R I N A R Y S Y S T E M S O M P H O N G N A R K P I N I T, M. D. D E P A R T M E N T O F P A T H O B I O L O G Y F A C U
SCPA 602- Anatomical Basis For Pathological Study H I S T O L O G Y O F T H E U R I N A R Y S Y S T E M S O M P H O N G N A R K P I N I T, M. D. D E P A R T M E N T O F P A T H O B I O L O G Y F A C U
CHAPTER 25 URINARY. Urinary system. Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1. functions
 CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
Chapter 25: Urinary System
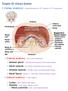 Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Chapter 23. The Nephron. (functional unit of the kidney
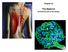 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Histology / First stage The Urinary System: Introduction. Kidneys
 The Urinary System: Introduction The urinary system consists of the paired kidneys and ureters, the bladder, and the urethra. This system helps maintain homeostasis by a complex combination of processes
The Urinary System: Introduction The urinary system consists of the paired kidneys and ureters, the bladder, and the urethra. This system helps maintain homeostasis by a complex combination of processes
Basic Urinary Tract Anatomy and Histology
 Basic Urinary Tract Anatomy and Histology The two kidneys are located in the retroperitoneum on either side of the vertebral bladder and the contraction of the detrusor muscle. Any mechanical barrier,
Basic Urinary Tract Anatomy and Histology The two kidneys are located in the retroperitoneum on either side of the vertebral bladder and the contraction of the detrusor muscle. Any mechanical barrier,
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Urinary System Laboratory
 Urinary System Laboratory 1 Adrenal gland Organs of The Urinary System Renal artery and vein Kidney Ureter Urinary bladder Figure 26.1 2 Urethra Functions of the urinary system organs: Urethra expels urine
Urinary System Laboratory 1 Adrenal gland Organs of The Urinary System Renal artery and vein Kidney Ureter Urinary bladder Figure 26.1 2 Urethra Functions of the urinary system organs: Urethra expels urine
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Histology Urinary system
 Histology Urinary system By the end of the topic the learner should be able to: Describe the histological structure of the kidney. Illustrate the ultrastructure of the blood renal barrier. Illustrate the
Histology Urinary system By the end of the topic the learner should be able to: Describe the histological structure of the kidney. Illustrate the ultrastructure of the blood renal barrier. Illustrate the
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Urinary system. Aleš Hampl
 Urinary system Aleš Hampl Functions of urinary system 1. Regulating blood volume and pressure 2. Regulating plasma concentrations of sodium, potassium, chloride and other ions 3. Stabilising blood ph 4.
Urinary system Aleš Hampl Functions of urinary system 1. Regulating blood volume and pressure 2. Regulating plasma concentrations of sodium, potassium, chloride and other ions 3. Stabilising blood ph 4.
Copyright 2003 Pearson Education, Inc. publishing as Benjamin Cummings. Dr. Nabil Khouri
 Dr. Nabil Khouri Objectives: General objectives: - to identify the kidney s structures, function and location - to analyze the relationship between microscopic structure and function Specific objectives:
Dr. Nabil Khouri Objectives: General objectives: - to identify the kidney s structures, function and location - to analyze the relationship between microscopic structure and function Specific objectives:
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
organs of the urinary system
 organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
HISTOLOGY OF THE URINARY SYSTEM
 HISTOLOGY OF THE URINARY SYSTEM The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the
HISTOLOGY OF THE URINARY SYSTEM The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary system. Urinary system
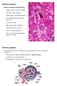 Distal convoluted tubule (DCT) Highly coiled, ~ 5 mm in length Last part of the nephron. Wall; simple cuboidal epithelium Less metabolically active than the PCT no brush border light eosinophilic cytoplasm
Distal convoluted tubule (DCT) Highly coiled, ~ 5 mm in length Last part of the nephron. Wall; simple cuboidal epithelium Less metabolically active than the PCT no brush border light eosinophilic cytoplasm
Urinary System (Anatomy & Physiology)
 Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 16 Urinary System 1 The Kidneys Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Functions of Urinary system o The Kidneys:
BIOH122 Human Biological Science 2 Session 16 Urinary System 1 The Kidneys Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Functions of Urinary system o The Kidneys:
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
28/04/2013 LEARNING OUTCOME C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS STUDENT ACHIEVEMENT INDICATORS URINARY SYSTEM & EXCRETION
 LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 17: Urinary System
 Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
19. RENAL PHYSIOLOGY ROLE OF THE URINARY SYSTEM THE URINARY SYSTEM. Components and function. V BS 122 Physiology II 151 Class of 2011
 19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
PHGY210 Renal Physiology
 PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden
 Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden The urinary system is important because it performs vital excretory functions Takes blood from renal arteries into the kidney to filtrate
Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden The urinary system is important because it performs vital excretory functions Takes blood from renal arteries into the kidney to filtrate
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
5.Which part of the nephron removes water, ions and nutrients from the blood?
 Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Unit #4 Waste and Excretion. The Kidneys
 Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
Frontal section of human kidney. (Scheme).
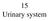 15 Urinary system 15-001 Kidney Cortex Medulla Papilla renalis Medial Lateral Medullary ray Labyrinth Columna renalis Pelvis renalis Calix renalis Ureter Capsula fibrosa Lobus renalis Columna renalis 15-01.
15 Urinary system 15-001 Kidney Cortex Medulla Papilla renalis Medial Lateral Medullary ray Labyrinth Columna renalis Pelvis renalis Calix renalis Ureter Capsula fibrosa Lobus renalis Columna renalis 15-01.
Chapter 26. The Urinary System. Lecture Presentation by Steven Bassett Southeast Community College Pearson Education, Inc.
 Chapter 26 The Urinary System Lecture Presentation by Steven Bassett Southeast Community College Introduction The urinary system does more than just get rid of liquid waste. It also: Regulates plasma ion
Chapter 26 The Urinary System Lecture Presentation by Steven Bassett Southeast Community College Introduction The urinary system does more than just get rid of liquid waste. It also: Regulates plasma ion
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY
 RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
General Anatomy of Urinary System
 General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note
![Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note](/thumbs/77/75431210.jpg) Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Collin College. BIOL Anatomy & Physiology WEEK 12. Urinary System INTRODUCTION. Main functions of the kidneys are
 Collin College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 INTRODUCTION Main functions of the kidneys are regulate blood volume, water content regulate blood composition e..g. Na, Cl, K, ph
Collin College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 INTRODUCTION Main functions of the kidneys are regulate blood volume, water content regulate blood composition e..g. Na, Cl, K, ph
Urinary System BIO 250. Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat. Routes of Waste Elimination
 Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
1. The Fibrous Capsule covers the outside of the kidney. It is made of fat and fibers.
 Slide 2 The kidney has a number of functions. First is the excretion of toxic metabolic waste through urine production. The kidneys filter blood plasma and as a result of filtering blood, the kidneys help
Slide 2 The kidney has a number of functions. First is the excretion of toxic metabolic waste through urine production. The kidneys filter blood plasma and as a result of filtering blood, the kidneys help
Urinary System. BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College
 Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
convoluted tubule. The proximal straight tubule is located in the medulla and dives down towards the pelvis.. [3] The Distal Straight Tubule receive
![convoluted tubule. The proximal straight tubule is located in the medulla and dives down towards the pelvis.. [3] The Distal Straight Tubule receive convoluted tubule. The proximal straight tubule is located in the medulla and dives down towards the pelvis.. [3] The Distal Straight Tubule receive](/thumbs/75/72965530.jpg) Chapter 16 Urinary System 16.1. Introduction The urinary system includes the: kidneys, ureters, urinary bladder, and urethra. The kidneys regulate the composition and volume of body fluids by constantly
Chapter 16 Urinary System 16.1. Introduction The urinary system includes the: kidneys, ureters, urinary bladder, and urethra. The kidneys regulate the composition and volume of body fluids by constantly
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
Urinary System Review Questions:
 Urinary System Review Questions: 1. This system would be lined with what type of membrane? 2. What type of epithelial tissue would line the opening of the urethra (the exit of the tract)? 3. What type
Urinary System Review Questions: 1. This system would be lined with what type of membrane? 2. What type of epithelial tissue would line the opening of the urethra (the exit of the tract)? 3. What type
URINARY SYSTEM. These organs lie posterior or inferior to the. (membrane).
 URINARY SYSTEM I. INTRODUCTION Each kidney is made up of about a million tiny tubules called nephrons. Each nephron individually filters the blood and makes urine and it does the job completely, from start
URINARY SYSTEM I. INTRODUCTION Each kidney is made up of about a million tiny tubules called nephrons. Each nephron individually filters the blood and makes urine and it does the job completely, from start
First is Urine Production. We ll discuss the specifics of this process momentarily.
 1 2 The kidney has a number of functions. First is Urine Production. We ll discuss the specifics of this process momentarily. Next, the kidneys filter blood. As a result of filtering blood, the kidneys
1 2 The kidney has a number of functions. First is Urine Production. We ll discuss the specifics of this process momentarily. Next, the kidneys filter blood. As a result of filtering blood, the kidneys
Waste Products & Kidney Function
 Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
The Urinary System Pearson Education, Inc.
 26 The Urinary System Introduction The urinary system does more than just get rid of liquid waste. It also: Regulates plasma ion concentrations Regulates blood volume and blood pressure Stabilizes blood
26 The Urinary System Introduction The urinary system does more than just get rid of liquid waste. It also: Regulates plasma ion concentrations Regulates blood volume and blood pressure Stabilizes blood
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
LABORATORY EXERCISES FOR THE URINARY SYSTEM
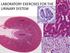 LABORATORY EXERCISES FOR THE URINARY SYSTEM cortex Medulla DEMO SLIDE BOX 172 (450-E001-H-76). Kidney, horse. the inner medulla medullary rays, Uriniferous tubules expand both the cortex and medulla corticomedullary
LABORATORY EXERCISES FOR THE URINARY SYSTEM cortex Medulla DEMO SLIDE BOX 172 (450-E001-H-76). Kidney, horse. the inner medulla medullary rays, Uriniferous tubules expand both the cortex and medulla corticomedullary
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
Waste. Urinary System Anatomy Urinary Section pages 5-8. Urinary System. Urinary System. Nitrogenous Wastes. Nitrogenous Wastes 4/22/2016
 Waste Urinary System Anatomy Urinary Section pages 5-8 Metabolism produces waste products What is the primary waste product of cellular respiration? How does the body dispose of it? Urinary System Urinary
Waste Urinary System Anatomy Urinary Section pages 5-8 Metabolism produces waste products What is the primary waste product of cellular respiration? How does the body dispose of it? Urinary System Urinary
Func%ons of the Urinary System
 Func%ons of the Urinary System Excre%on Regula%on of blood volume Regula%on of blood pressure Regula%on of blood- solute concentra%on Regula%on of ph of extracellular fluid Regula%on of erythropoiesis
Func%ons of the Urinary System Excre%on Regula%on of blood volume Regula%on of blood pressure Regula%on of blood- solute concentra%on Regula%on of ph of extracellular fluid Regula%on of erythropoiesis
Basic Functions of the Kidneys
 Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
1.&Glomerular/Pressure&Filtration&
 Urine&Formation& Overall&Process&! Urine gets rid of wastes (NH 3, urea, uric acid, creatinine) and other substances (vitamins, penicillin, histamines) found in excess in the blood!! blood is filtered
Urine&Formation& Overall&Process&! Urine gets rid of wastes (NH 3, urea, uric acid, creatinine) and other substances (vitamins, penicillin, histamines) found in excess in the blood!! blood is filtered
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Chapter 26 The Urinary System. Overview of Kidney Functions. External Anatomy of Kidney. External Anatomy of Kidney
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Chapter 24: The Urinary System
 Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a.
 I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a. Renal fascia b. Perinephric fat (Adipose) capsule c. Fibrous
I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a. Renal fascia b. Perinephric fat (Adipose) capsule c. Fibrous
Use the following diagram to answer the next question. 1. In the diagram above, pressure filtration occurs in a. W b. X c. Y d. Z
 Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
2. Ureters Composed of smooth muscle tissue ~25cm long Connects kidneys to bladder Undergoes peristaltic contraction to move urine to bladder
 Section 6: The Urinary System A) Organs of the Urinary system 1. Kidneys 2. Ureters 3. Bladder 4. Urethra 1. Kidneys Paired organs located on either side of vertebral column in upper part of abdominal
Section 6: The Urinary System A) Organs of the Urinary system 1. Kidneys 2. Ureters 3. Bladder 4. Urethra 1. Kidneys Paired organs located on either side of vertebral column in upper part of abdominal
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Human Anatomy Unit 3 URINARY SYSTEM
 Human Anatomy Unit 3 URINARY SYSTEM In Anatomy Today Components Kidneys Ureters Urinary bladder Urethra Functions Storage of urine Bladder stores up to 1 L of urine Excretion of urine Transport of urine
Human Anatomy Unit 3 URINARY SYSTEM In Anatomy Today Components Kidneys Ureters Urinary bladder Urethra Functions Storage of urine Bladder stores up to 1 L of urine Excretion of urine Transport of urine
