New prediction model for diagnosis of bacterial infection in febrile infants younger than 90 days
|
|
|
- Christopher McCormick
- 5 years ago
- Views:
Transcription
1 The Turkish Journal of Pediatrics 2017; 59: DOI: /turkjped Original New prediction model for diagnosis of bacterial infection in febrile infants younger than 90 days Matea Vujevic 1, Benjamin Benzon 1, Josko Markic 1,2 1 University of Split School of Medicine, Soltanska 2, 2 University Hospital Centre Split, Department of Pediatrics, Spinciceva 1, Split, Croatia. josko.markic@gmail.com Received: 6th February 2017, Accepted: 20th February 2017 SUMMARY: Vujevic M, Benzon B, Markic J. New prediction model for diagnosis of bacterial infection in febrile infants younger than 90 days. Turk J Pediatr 2017; 59: Due to non-specific clinical presentation in febrile infants, extensive laboratory testing is often carried out to distinguish simple viral disease from serious bacterial infection (SBI). Objective of this study was to compare efficacy of different biomarkers in early diagnosis of SBI in infants <90 days old. Also, we developed prediction models with whom it will be possible to diagnose SBI with more accuracy than with any biomarkers independently. Febrile <90-day-old infants hospitalized in 2-year-period at Department of Pediatrics, University Hospital Centre Split with suspicion of having SBI were included in this study. Retrospective cohort analysis of data acquired from medical records was performed. Out of 181 enrolled patients, SBI was confirmed in 70. Most common diagnosis was urinary tract infection (68.6%), followed by pneumonia (12.9%), sepsis (11.4%), gastroenterocolitis (5.7%) and meningitis (1.4%). Male gender was shown to be a risk factor for SBI in this population (p=0.008). White blood cell count (WBC), absolute neutrophil count (ANC) and C-reactive protein (CRP) were confirmed as the independent predictors of SBI, with CRP as the best one. Two prediction models built by combining biomarkers and clinical variables were selected as optimal with sensitivities of 74.3% and 75.7%, and specificities of 88.3% and 86%. Evidently, CRP is a more superior biomarker in diagnostics of SBI comparing to WBC and ANC. Prediction models were shown to be better in predicting SBI than independent biomarkers. Although both showed high sensitivity and specificity, their true strength should be determined using validation cohort. Key words: C-reactive protein, biomarkers, fever, infant, bacterial infection. Fever is among the most frequent reasons for bringing children to the Emergency Department, especially infants during the first three months of life 1. It is also the main reason for, often unrealistic and exaggerated, parental concern 2. Despite ingrained parental fear, fever in infants mostly occurs due to the self-limiting viral infection which resolves without need for any specific therapy other than relieving the symptoms 3. However, in significant percentage of cases underlying cause is bacterial and requires adequate antibiotic treatment to avoid possible complications. Infants under three months of age, especially newborns, are more susceptible to infections because their immune system is still relatively immature and has not fully developed yet 4. Also, setting a correct diagnosis is especially challenging because symptoms and signs of infection in children this age are most often non-specific, with elevated body temperature often as the only symptom, especially on examination at the initial stages of disease 5,6. Because of that, extensive laboratory testing is often carried out, along with initiation of empirical intravenous antibiotic therapy consequently requiring hospitalization 5. That practice, in addition to the increased risk of side-effects and allergic reactions, also raises the medical costs and increases bacterial resistance to most commonly used antibiotics 7. Also, hospitalization should be avoided due to
2 262 Vujevic M, et al The Turkish Journal of Pediatrics May-June 2017 the fact that infants are prone to the hospitalacquired infections during their stay. Therefore, it is necessary, during diagnostic workup, to successfully single out those febrile infants suffering from bacterial infections, especially serious bacterial infections (SBI), and start treating them with antibiotics on time. Primary objective of this study was to compare efficacy and diagnostic value of white blood cell count (WBC), absolute neutrophil count (ANC), and C-reactive protein (CRP) in the early diagnosis of SBI in febrile infants younger than 90 days. Also, secondary objective was to develop a prediction model with whom it will be possible to diagnose SBI with more accuracy than using any of the biomarkers independently. Material and Methods This retrospective cohort study was performed at the Department of Pediatrics of the University Hospital Centre, Split. The Ethics Committee of the University Hospital Centre, Split approved the study (No /06/J.B.-16-2) and the parents of the enrolled infants were contacted and signed informed consent. The study included febrile infants aged 0-90 days, who were hospitalized between January 1 st, 2014 and December 31 st, 2015 with suspicion of having SBI. Other inclusion criteria were gestational age 37 weeks and rectally measured body temperature 38ºC during the last 24 h. Exclusion criteria were antibiotic treatment during the previous 48 h, previously known immunodeficiency, vaccination during the 5 days before admission, chronic diseases and conditions in medical history and transfer from other medical institutions. Based upon medical charts review, patients were divided into two groups: a group of patients with serious bacterial infection (SBI) and a group of patients without a serious bacterial infection (nonsbi). The SBI group included patients who met the same criteria for SBI already described in previous studies. Those criteria were: (a) sepsis/bacteremia microbiologically confirmed by positive blood culture or bacterial meningitis diagnosed by positive cerebrospinal fluid culture; (b) urinary tract infection (UTI) confirmed by positive urine culture (>105 colony forming units/ml of a single microorganism in a sample collected by sterile method); (c) chest radiographic features consistent with pneumonia (lobar consolidation or an infiltrate) confirmed by pediatric radiologist; (d) bacterial gastroenteritis confirmed by positive stool culture; (e) cellulitis with an appropriate physical examination 8,9. Patients with other discharge diagnoses were included in the nonsbi group. None of the patients received pneumococcal or meningococcal vaccine. By using available medical records, for each enrolled patient a series of data were collected: gender, birth weight and birth length, age at the time of admission, body weight and length, maximum measured body temperature and the results of tests performed at the time of admission, including complete blood count (CBC) with differential, CRP, blood cultures, urine cultures, coprocultures, cerebrospinal fluid cultures and the results of viral antigen isolation from blood samples, stool or nasopharyngeal lavage (RSV, rotavirus and adenovirus). Using WBC and the number of segmented and nonsegmented neutrophils, absolute neutrophil count (ANC) was calculated for each patient with the following formula: ANC=0.01xWBC x (non-segmented neutrophils (%) + segmented neutrophils (%) Statistical analysis Differences between continuous variables were tested for statistical significance using Mann Whitney test. The values of categorical variables were compared between groups using Chi-square test. For all statistical calculations, the value of p<0.05 was considered statistically significant. Optimal sensitivity and specificity of biomarkers were determined from the ROC curves using Youden indicator. Positive (LR+) and negative (LR-) likelihood ratios were also used as a measure of diagnostic usefulness. ROC analysis and Mann Whitney test were carried out using GraphPad Prism 7.6 (GraphPad Software, La Jolla, California, USA). Logit function was used for logistic regression and the best model was chosen by information theoretic approach using Akaike information criterion (AIC). Logistic regression was performed using XLSTAT application (Addinsoft, New York, NY, USA).
3 Volume 59 Number 3 Serious Bacterial Infection Prediction Model 263 Results During the observed period of time, 5141 children aged 0-18 years were hospitalized and 790 of them (15.4%) were infants up to 90 days old. Of them, 187 (23.7%) were hospitalized for febrile illness with suspicion of having SBI. Having met the inclusion criteria and none of exclusion criteria, 181 of them were included in the study. Based upon the discharge diagnoses, subjects were allocated to SBI group (n=70) or nonsbi group (n=111). No subjects remained unallocated. Table I shows demographic characteristics of study groups and they were comparable for age, body weight and body length. Significant predominance of male gender was found in SBI group. Statistically significant difference between the groups was also found for birth weight and birth length. The most common diagnosis in SBI group was urinary tract infection (68.6%), followed by sepsis (11.4%), meningitis (1.4%), pneumonia (12.9%) and gastroenterocolitis (5.7%). The most common isolated causative pathogen was Escherichia coli, which was found in 81.3% of patients with urinary tract infection and in 60% of all patients in SBI group. Other isolated pathogens were: beta-hemolytic group B Streptococcus (GBS, Streptococcus agalactiae), Enterobacter cloacae, Klebsiella pneumoniae (ESBL+), Pseudomonas aeruginosa, methicillin-resistant Staphylococcus epidermidis (MRSE), unfermentable gram-negative bacilli and coagulase-negative Staphylococcus sp. In the SBI group, WBC, ANC, CRP and maximum measured body temperature were found statistically significantly elevated (Fig. 1). Sensitivity, specificity and the calculated optimal cut-off value of biomarkers and maximum measured body temperature are shown in Table II. CRP proved to be the most useful biomarker for differentiation between SBI and nonsbi groups, with both sensitivity and specificity of 80% at the cut-off value of 13.3 mg/l. The diagnostic values of biomarkers and maximum measured body temperature are shown using ROC curves (Fig. 2). The secondary objective of this study was, using a combination of studied biomarkers and demographic indicators, to develop a prediction model in which we followed the principle of Fig. 1. Display of biomarker findings and maximum measured body temperature by subject groups using box and whiskers plot (a) White blood cell count is higher in SBI group (median 15.2 x10 9 /L, IQR in SBI group as opposed to median 10.2 x10 9 /L, IQR in nonsbi group; p<0.0001) (b) Absolute neutrophil count is higher in SBI group (median 6.97 x10 9 /L, IQR in SBI group as opposed to median 3.66 x10 9 /L, IQR in nonsbi group; p<0.0001) (c) C-reactive protein (CRP) level is higher in SBI group (median 35.7 mg/l, IQR in SBI group as opposed to median 4.2 mg/l, IQR in nonsbi group; p<0.0001) (d) Maximum measured body temperature is statistically significantly higher in SBI group (median 38.9 C, IQR in SBI group as opposed to median 38.5 C, IQR in nonsbi group; p=0.0257) SBI serious bacterial infection group; nonsbi patients without serious bacterial infection group; IQR interquartile range Fig. 2. Diagnostic value of biomarkers and maximum measured body temperature in predicting serious bacterial infection shown using receiver operating characteristic (ROC) curves (a) AUC for white blood cell count is 0.74 (95%CI ), (b) AUC for absolute neutrophil count is 0.76 (95%CI ), (c) AUC for C-reactive protein (CRP) level is 0.83 (95%CI ), (d) AUC for maximum measured body temperature is 0.6 (95%CI ) AUC- area under the curve, CI- confidence interval
4 264 Vujevic M, et al The Turkish Journal of Pediatrics May-June 2017 parsimony, i.e. Ockham s razor, keeping in mind the future validation of this model. The model using a combination of CRP, WBC, gender and maximum measured body temperature was the one with the greatest Akaike weight. However, model with same variables, just without maximum measured body temperature, is equally good. Given sample size, we were not able to decisively show whether maximum measured body temperature adds more accuracy to the simpler model or it is just a superfluous variable (Table III and Table IV). Both models yielded similar diagnostic characteristics when applied to the patient cohort on which they were developed. More complex model (model No. 10) yielded LR+ of 6.35 (95% CI ) and LR (95% CI ) at the cut-off value of 0.4 (40%) probability for SBI. Simpler model (model No. 8) showed LR+ of 5.4 (95% CI ) and LR- of 0.28 (95% CI ) at the cut off value of 0.36 (36%) probability for SBI. Discussion The aim of this study was to determine the diagnostic value and effectiveness of the most common biomarkers in clinical practice. We have shown that WBC, ANC and CRP are significantly higher in the group of infants who suffer from SBI, compared to those without SBI. The CRP seems to have higher diagnostic value than ANC and WBC. Various studies confirm our results that CRP poses greater diagnostic value versus WBC 8,10-12 and ANC 10,13. Only one study has shown better performance of ANC than CRP. 14 The optimal WBC cut-off value of 13.4x10 9 /L determined in this study is somewhat lower than the value 15x10 9 /L commonly used in other studies 8,10,11,13, However, with its sensitivity of 60% and specificity 83%, the WBC in this study proved to be more sensitive and equally specific, comparing to results from those studies. Still, our results also confirm that it does not have sufficient diagnostic value to be used independently as a predictor of SBI and it is recommended to be used in combination with other biomarkers. With standalone use, 40% of children would be a falsely classified as negative for SBI. Similar conclusion goes for ANC, as well. ANC has shown the diagnostic value similar to that of WBC, but slightly more sensitive, with a sensitivity of 65.7% and specificity of 81% for the cut-off value 5.7x10 9 /L. Diagnostic value coincides with the results of studies conducted by other researchers, but using the cut-off values of 10000/ mm 3 and 10600/ mm 3. 13,14 Given that there is no consensus on the specific cut-off value for CRP that should be used to distinguish high and low risk of SBI in infants with fever, each author chooses the value to be used. Typically, in studies it varies in the range from 20 to 70 mg/l 19, provided that for the population up to 90 days old most frequently used value is 20 mg/l 8,11,12,20. Our cut-off value of 13.3 mg/l is somewhat lower than theirs, but close to the one used in a research by Zarkesh et al. 10, whose diagnostic value of CRP (sensitivity 81.6% and specificity 89.8%) shows results comparable to ours. Table I. Demographic Characteristics of Study Subjects (n=181). SBI Non-SBI (n=70) (n=111) P value Gender (male, female) (%) 71.14%, 27.14% 53.15%, 46.84% Age (days)* (20.00 to 72.00) (29.00 to 70.00) 0.41 Body weight (g)* 4950 (4088 to 5985) 4780 (4250 to 5600) 0.53 Body length (cm)* (54.00 to 60.00) (54.00 to 60.00) 0.51 Birth weight (g)* 3800 (3325 to 4103) 3470 (3120 to 3800) Birth length (cm)* (50.00 to 53.00) (50.00 to 52.00) SBI: serious bacterial infection group; Non-SBI: patients without serious bacterial infection group; IQR: interquartile range.data is presented as median (IQR)
5 Volume 59 Number 3 Serious Bacterial Infection Prediction Model 265 Table II. Diagnostic Properties of Biomarkers and Maximum Measured Body Temperature. Likelihood ratios Biomarker Cut-off value Sensitivity (95% CI) Specificity (95% CI) Positive Negative White blood cell count 13.4 x 10 9 /L 60% ( %) 82.88% ( %) 3.5 ( ) 0.48 ( ) Absolute neutrophil count 5.7 x 10 9 /L 65.71% ( %) 81.08% ( %) 3.4 ( ) 0.42 ( ) C-reactive protein 13.3 mg/l 80% ( %) 80.81% ( %) 4.02 ( ) 0.25 ( ) Maximum body temperature C 51.43% ( %) 72.07% ( %) 1.84 ( ) 0.67 ( ) CI: confidence interval Similar applies to the maximum measured body temperature. Different cut-off values which are considered a fever in various studies also represent a problem 21. Although this study demonstrates that fever is statistically significantly higher in infants with SBI, maximum measured body temperature as an independent indicator has poor diagnostic predictive value. Similar results are shown in a French study 22. However, in conjunction with other biomarkers, it still contributes to improving the accuracy of detection of SBI. In the studied population of hospitalized children, the most frequent SBI was urinary tract infection, with the most common isolated causative pathogen being Escherichia coli. This is consistent with results of previously published studies 9,10,21,23,24. Our results have showed significant predominance of male gender in SBI group, with male to female ratio 2.6:1, as opposed to nonsbi group where gender is equally distributed. These findings imply that male gender is a risk factor for the development of SBI in infants up to 90 days old. Other authors suggest a similar conclusion 1,22,25-27, so it is important to take gender into consideration during the evaluation of febrile infants. Although most studies found no link between gender and SBI 10,12,20,28-31, that discrepancy should be considered from the epidemiological and population point of view. These studies were generally carried out in countries with widespread circumcision of young boys. Various previous studies have shown that this process significantly, up to 10 times, reduces the incidence of urinary tract infections in infants younger than three months As our research, as well as others 9,10,21,23,24, showed that urinary tract infection is the most common SBI in this population of children, we believe that is the cause of discrepancy in the results. Therefore, uncircumcised boys aged up to three months, such as our patients, are at increased risk for the development of SBI. Also, the reason may be a relatively small sample size in this study. The differences in birth weight and length between the groups, although statistically significant, might reflect that males are overrepresented in SBI group so we do not think that they play a role in risk stratification. This conclusion is in accordance with the
6 266 Vujevic M, et al The Turkish Journal of Pediatrics May-June 2017 Table III. Optimal Model Selection Using Akaike Information Criterion (AIC). Model no. Model variables Deviance AIC Number of variables ΔAIC waici Evidence ratio 1 WBC ANC CRP CRP, gender CRP, WBC CRP, ANC CRP, ANC, WBC * CRP, WBC, gender CRP, ANC, WBC, gender 10 * CRP, WBC, gender, Tmax 11 CRP, ANC, WBC, gender, Tmax WBC: white blood cell count, ANC: absolute neutrophil count, Tmax: maximum measured body temperature, ΔAIC: difference in AIC between considered model and model with minimum AIC, waici: Akaike weight. *: models chosen as optimal results of other studies 9,27. Given the non-specific clinical presentation, invasiveness of the current diagnostic gold standards and the need for an early start of antibiotic treatment in infants where it is required, the role of biomarkers in the diagnosis of febrile infants up to three months of age is extremely important, primarily to distinguish between bacterial and viral infections. Although there are numerous biomarkers, some of the most commonly used being: WBC, ANC, CRP and procalcitonin (PCT), there is still no biomarker sufficiently sensitive and specific to determine with certainty whether the infant is suffering from SBI or not. Therefore, the secondary objective of this study was, using a combination of evaluated biomarkers and demographic characteristics, to develop a prediction model which will be more efficient in diagnosing SBI. Keeping in mind the future validation of the model, we applied the principle of parsimony, i.e. Ockham s razor, and selected the models with the minimum number of parameters and maximum specificity and sensitivity. Two selected models were shown to be superior both in terms of model selection and LR+ when compared to CRP alone, thus suggesting their potential use as tools to confirm candidate diagnosis. On the other hand, LR- values are very similar between any of the models and CRP. However, in order to determine true diagnostic values of selected models and biomarkers (with their proposed cut-offs) a study on validation cohort should be conducted. CRP is a more superior biomarker in diagnostics of SBI comparing to WBC and ANC. Prediction models were shown to be better in predicting SBI than independent biomarkers. Although both showed high sensitivity and specificity, their true strength should be determined using validation cohort. REFERENCES 1. Shin SH, Choi CW, Lee J-A, et al. Risk factors for serious bacterial infection in febrile young infants in a community referral hospital. J Korean Med Sci 2009; 24: Schmitt BD. Fever phobia: misconceptions of parents about fevers. Arch Pediatr Adolesc Med 1980; 134: Vorwerk C, Manias K, Davies F, Coats TJ. Prediction of severe bacterial infection in children with an emergency department diagnosis of infection. Emerg Med J 2011; 28: Arora R, Mahajan P. Evaluation of child with fever without source: review of literature and update. Pediatr Clin North Am 2013; 60:
7 Volume 59 Number 3 Serious Bacterial Infection Prediction Model 267 Table IV. Parameters and Diagnostic Characteristics of the Best Models. Sensitivity (%) Specificity (%) Likelihood ratio (95% CI) (95% CI) Positive (95% CI) Negative (95% CI) 74.3 ( ) 88.3 ( ) 6.35 ( ) 0.29 ( ) Cut-off value Odds ratio for parameter (95% CI) Model Parameter No. 10 CRP ( ) 40% WBC ( ) probability ( ) Gender (male) Tmax ( ) 75.7 ( ) 86 ( ) 5.4 ( ) 0.28 ( ) No. 8 CRP ( ) 36% WBC ( ) probability ( ) Gender (male) WBC: white blood cell count, ANC: absolute neutrophil count, Tmax: maximum measured body temperature, CI: confidence interval 5. Biondi EA, Byington CL. Evaluation and Management of Febrile, Well-appearing Young Infants. Infect Dis Clin North Am 2015; 29: Bachur RG, Harper MB. Predictive model for serious bacterial infections among infants younger than 3 months of age. Pediatrics 2001; 108: DeAngelis C, Joffe A, Wilson M, Willis E. Iatrogenic risks and financial costs of hospitalizing febrile infants. Am J Dis Child 1983; 137: Olaciregui I, Hernández U, Munoz J, et al. Markers that predict serious bacterial infection in infants under 3 months of age presenting with fever of unknown origin. Arch Dis Child 2009; 94: Markic J, Jeroncic A, Polancec D, et al. CD15s is a potential biomarker of serious bacterial infection in infants admitted to hospital. Eur J Ped 2013; 172: Zarkesh M, Sedaghat F, Heidarzadeh A, et al. Diagnostic Value of IL-6, CRP, WBC, and Absolute Neutrophil Count to Predict Serious Bacterial Infection in Febrile Infants. Acta Med Iran 2015; 53: Bressan S, Andreola B, Cattelan F, et al. Predicting severe bacterial infections in well-appearing febrile neonates: laboratory markers accuracy and duration of fever. Pediatr Infect Dis J 2010; 29: Hsiao AL, Chen L, Baker MD. Incidence and predictors of serious bacterial infections among 57-to 180-day-old infants. Pediatrics 2006; 117: Pratt A, Attia MW. Duration of fever and markers of serious bacterial infection in young febrile children. Pediatr Int 2007; 49: Isaacman DJ, Burke BL. Utility of the serum C-reactive protein for detection of occult bacterial infection in children. Arch Pediatr Adolesc Med 2002; 156: Andreola B, Bressan S, Callegaro S, et al. Procalcitonin and C-reactive protein as diagnostic markers of severe bacterial infections in febrile infants and children in the emergency department. Pediatr Infect Dis J 2007; 26: Schwartz S, Raveh D, Toker O, et al. A week-by-week analysis of the low-risk criteria for serious bacterial infection in febrile neonates. Arch Dis Child 2009; 94: Galetto-Lacour A, Zamora S, Gervaix A. Bedside procalcitonin and C-reactive protein tests in children with fever without localizing signs of infection seen in a referral center. Pediatrics 2003; 112: Lacour A, Gervaix A, Zamora S, et al. Procalcitonin, IL-6, IL-8, IL-1 receptor antagonist and C-reactive protein as identificators of serious bacterial infections in children with fever without localising signs. Eur J Ped 2001; 160: Galetto-Lacour A, Gervaix A. Identifying severe bacterial infection in children with fever without source. Expert Rev Anti Infect Ther 2010; 8: Nosrati A, Ben Tov A, Reif S. Diagnostic markers of serious bacterial infections in febrile infants younger than 90 days old. Pediatr Int 2014; 56:
8 268 Vujevic M, et al The Turkish Journal of Pediatrics May-June Hui C, Neto G, Tsertsvadze A, et al. Diagnosis and management of febrile infants (0-3 months). Evid Rep Technol Assess 2012; 205: Gajdos V, Foix L, Mollet-Boudjemline A, et al. Factors predicting serious bacterial infections in febrile infants less than three months old: multivariate analysis. Arch Pediatr 2005; 12: Baker MD, Bell LM, Avner JR. Outpatient management without antibiotics of fever in selected infants. New Engl J Med 1993; 329: Byington CL, Reynolds CC, Korgenski K, et al. Costs and infant outcomes after implementation of a care process model for febrile infants. Pediatrics 2012; 130: e16-e Kumar V, Singhi S. Predictors of serious bacterial infection in infants up to 8 weeks of age. Indian Pediatr 1994; 31: Chen C-J, Lo Y-F, Huang M-C, et al. A model for predicting risk of serious bacterial infection in febrile infants younger than 3 months of age. J Chin Med Assoc 2009; 72: Méndez Espinola BM, Herrera Labarca P. Children less than 3 months hospitalised due to acute febrile syndrome. 5 years clinical experience. Rev Chil Pediatr 2014; 86: Bilavsky E, Yarden Bilavsky H, Ashkenazi S, Amir J. C reactive protein as a marker of serious bacterial infections in hospitalized febrile infants. Acta Paediatr 2009; 98: Ashkenazi-Hoffnung L, Livni G, Amir J, Bilavsky E. Serious bacterial infections in hospitalized febrile infants aged 90 days or younger: The traditional combination of ampicillin and gentamicin is still appropriate. Scand J Infect Dis 2011; 43: Dagan R, Powell KR, Hall CB, Menegus MA. Identification of infants unlikely to have serious bacterial infection although hospitalized for suspected sepsis. J Pediatr 1985; 107: Pantell RH, Newman TB, Bernzweig J, et al. Management and outcomes of care of fever in early infancy. JAMA 2004; 291: Shaikh N, Morone NE, Bost JE, Farrell MH. Prevalence of urinary tract infection in childhood: a meta-analysis. Pediatr Infect Dis J 2008; 27: Zorc JJ, Levine DA, Platt SL, et al. Clinical and Demographic Factors Associated With Urinary Tract Infection in Young Febrile Infants. Pediatrics 2005; 116: Ishimine P. Risk stratification and management of the febrile young child. Emerg Med Clin North Am 2013; 31: Baraff LJ. Management of fever without source in infants and children. Ann Emerg Med 2000; 36:
Faculty Disclosure. Stephen I. Pelton, MD. Dr. Pelton has listed no financial interest/arrangement that would be considered a conflict of interest.
 Faculty Disclosure Stephen I. Pelton, MD Dr. Pelton has listed no financial interest/arrangement that would be considered a conflict of interest. Advances in the management of fever in infants 0 to 3 and
Faculty Disclosure Stephen I. Pelton, MD Dr. Pelton has listed no financial interest/arrangement that would be considered a conflict of interest. Advances in the management of fever in infants 0 to 3 and
Hsiu-Lin Chen, Chih-Hsing Hung, Hsing-I Tseng and Rei-Cheng Yang*
 Jpn. J. Infect. Dis., 61, 31-35, 2008 Original Article Soluble Form of Triggering Receptor Expressed on Myeloid Cells-1 (strem-1) as a Diagnostic Marker of Serious Bacterial Infection in Febrile Infants
Jpn. J. Infect. Dis., 61, 31-35, 2008 Original Article Soluble Form of Triggering Receptor Expressed on Myeloid Cells-1 (strem-1) as a Diagnostic Marker of Serious Bacterial Infection in Febrile Infants
Reactive Thrombocytosis in Febrile Young Infants with Serious Bacterial Infection
 R E S E A R C H P A P E R Reactive Thrombocytosis in Febrile Young Infants with Serious Bacterial Infection S FOUZAS, L MANTAGOU, E SKYLOGIANNI AND A VARVARIGOU From the Department of Pediatrics, University
R E S E A R C H P A P E R Reactive Thrombocytosis in Febrile Young Infants with Serious Bacterial Infection S FOUZAS, L MANTAGOU, E SKYLOGIANNI AND A VARVARIGOU From the Department of Pediatrics, University
REACTIVE THROMBOCYTOSIS IN FEBRILE CHILDREN WITH SERIOUS BACTERIAL INFECTION Amita Jane D Souza 1, Anil Shetty 2, Divya Krishnan K 3
 REACTIVE THROMBOCYTOSIS IN FEBRILE CHILDREN WITH SERIOUS BACTERIAL INFECTION Amita Jane D Souza 1, Anil Shetty 2, Divya Krishnan K 3 HOW TO CITE THIS ARTICLE: Amita Jane D Souza, Anil Shetty, Divya Krishnan
REACTIVE THROMBOCYTOSIS IN FEBRILE CHILDREN WITH SERIOUS BACTERIAL INFECTION Amita Jane D Souza 1, Anil Shetty 2, Divya Krishnan K 3 HOW TO CITE THIS ARTICLE: Amita Jane D Souza, Anil Shetty, Divya Krishnan
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 66/ Aug 17, 2015 Page 11432
 BLOOD CULTURE AND BACTEREMIA PREDICTORS IN INFANTS LESS THAN ONE YEAR OF AGE WITH FEVER WITHOUT SOURCE (FWS) Y. G. Sathish Kumar 1, A. Udayamaliny 2, S. Ankitha 3 HOW TO CITE THIS ARTICLE: Y. G. Sathish
BLOOD CULTURE AND BACTEREMIA PREDICTORS IN INFANTS LESS THAN ONE YEAR OF AGE WITH FEVER WITHOUT SOURCE (FWS) Y. G. Sathish Kumar 1, A. Udayamaliny 2, S. Ankitha 3 HOW TO CITE THIS ARTICLE: Y. G. Sathish
Fever in neonates (age 0 to 28 days)
 Fever in neonates (age 0 to 28 days) INCLUSION CRITERIA Infant 28 days of life Temperature 38 C (100.4 F) by any route/parental report EXCLUSION CRITERIA Infants with RSV Febrile Infant 28 days old Ill
Fever in neonates (age 0 to 28 days) INCLUSION CRITERIA Infant 28 days of life Temperature 38 C (100.4 F) by any route/parental report EXCLUSION CRITERIA Infants with RSV Febrile Infant 28 days old Ill
Fevers and Seizures in Infants and Young Children
 Fevers and Seizures in Infants and Young Children Kellie Holtmeier, PharmD Pediatric Clinical Pharmacist University of New Mexico Hospital Disclosure I have no conflicts of interest 1 Pharmacist Objectives
Fevers and Seizures in Infants and Young Children Kellie Holtmeier, PharmD Pediatric Clinical Pharmacist University of New Mexico Hospital Disclosure I have no conflicts of interest 1 Pharmacist Objectives
The Journal of Critical Care Medicine 2015;1(1):11-17
 The Journal of Critical Care Medicine 2015;1(1):11-17 RESEARCH ARTICLE DOI: 10.1515/jccm-2015-0003 The Value of the Lab-Score Method in Identifying Febrile Infants at Risk for Serious Bacterial Infections
The Journal of Critical Care Medicine 2015;1(1):11-17 RESEARCH ARTICLE DOI: 10.1515/jccm-2015-0003 The Value of the Lab-Score Method in Identifying Febrile Infants at Risk for Serious Bacterial Infections
Beyond the Reflex Arc: An Evidence-Based Discussion of the Management of Febrile Infants
 Beyond the Reflex Arc: An Evidence-Based Discussion of the Management of Febrile Infants Cole Condra, MD MSc Division of Emergency Medical Services Children s Mercy Hospital October 1, 2011 Disclosure
Beyond the Reflex Arc: An Evidence-Based Discussion of the Management of Febrile Infants Cole Condra, MD MSc Division of Emergency Medical Services Children s Mercy Hospital October 1, 2011 Disclosure
Fever in the Newborn Period
 Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Fever in Infants: Pediatric Dilemmas in Antibiotherapy
 Fever in Infants: Pediatric Dilemmas in Antibiotherapy Jahzel M. Gonzalez Pagan, MD, FAAP Pediatric Emergency Medicine Associate Professor, UPH Medical Advisor, SJCH June 9 th, 2017 S Objectives S Review
Fever in Infants: Pediatric Dilemmas in Antibiotherapy Jahzel M. Gonzalez Pagan, MD, FAAP Pediatric Emergency Medicine Associate Professor, UPH Medical Advisor, SJCH June 9 th, 2017 S Objectives S Review
Time to Detection of Bacterial Cultures in Infants Aged 0 to 90 Days
 RESEARCH ARTICLE Time to Detection of Bacterial Cultures in Infants Aged 0 to 90 Days AUTHORS Rianna C. Evans, MD, Bryan R. Fine, MD, MPH Division of Pediatric Hospital Medicine, Department of Pediatrics,
RESEARCH ARTICLE Time to Detection of Bacterial Cultures in Infants Aged 0 to 90 Days AUTHORS Rianna C. Evans, MD, Bryan R. Fine, MD, MPH Division of Pediatric Hospital Medicine, Department of Pediatrics,
Critical Review Form Clinical Prediction or Decision Rule
 Critical Review Form Clinical Prediction or Decision Rule Development and Validation of a Multivariable Predictive Model to Distinguish Bacterial from Aseptic Meningitis in Children, Pediatrics 2002; 110:
Critical Review Form Clinical Prediction or Decision Rule Development and Validation of a Multivariable Predictive Model to Distinguish Bacterial from Aseptic Meningitis in Children, Pediatrics 2002; 110:
Evidence-based Management of Fever in Infants and Young Children
 Evidence-based Management of Fever in Infants and Young Children Shabnam Jain, MD, MPH Associate Professor of Pediatrics Emory University Medical Director for Clinical Effectiveness Objectives Understand
Evidence-based Management of Fever in Infants and Young Children Shabnam Jain, MD, MPH Associate Professor of Pediatrics Emory University Medical Director for Clinical Effectiveness Objectives Understand
Serum procacitonin as a diagnostic marker of bacterial infection in febrile children
 International Journal of Contemporary Pediatrics Brindha K et al. Int J Contemp Pediatr. 2017 Jul;4(4):1381-1388 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
International Journal of Contemporary Pediatrics Brindha K et al. Int J Contemp Pediatr. 2017 Jul;4(4):1381-1388 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Original Research Article DOI:
PDFlib PLOP: PDF Linearization, Optimization, Protection. Page inserted by evaluation version
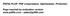 PDFlib PLOP: PDF Linearization, Optimization, Protection Page inserted by evaluation version www.pdflib.com sales@pdflib.com ACAD EMERG MED d December 2004, Vol. 11, No. 12 d www.aemj.org 1297 A Low Peripheral
PDFlib PLOP: PDF Linearization, Optimization, Protection Page inserted by evaluation version www.pdflib.com sales@pdflib.com ACAD EMERG MED d December 2004, Vol. 11, No. 12 d www.aemj.org 1297 A Low Peripheral
The Febrile Infant. SJRH ED Rounds Dec By: Robin Clouston
 1 The Febrile Infant SJRH ED Rounds Dec 11 2018 By: Robin Clouston 2 Objectives Discuss the risk of serious bacterial infection (SBI) in the neonate or young infant (
1 The Febrile Infant SJRH ED Rounds Dec 11 2018 By: Robin Clouston 2 Objectives Discuss the risk of serious bacterial infection (SBI) in the neonate or young infant (
Fever Without a Source Age: 0-28 Day Pathway - Emergency Department Evidence Based Outcome Center
 Age: 0-28 Day Pathway - Emergency Department EXCLUSION CRITERIA Toxic appearing No fever Born < 37 weeks gestational age INCLUSION CRITERIA Non-toxic with temperature > 38 C (100.4 F) < 36 C (96.5 F) measured
Age: 0-28 Day Pathway - Emergency Department EXCLUSION CRITERIA Toxic appearing No fever Born < 37 weeks gestational age INCLUSION CRITERIA Non-toxic with temperature > 38 C (100.4 F) < 36 C (96.5 F) measured
abstract ARTICLE BACKGROUND: There is considerable variation in the approach to infants presenting to the
 Management and Outcomes of Previously Healthy, Full-Term, Febrile Infants Ages 7 to 90 Days Tara L. Greenhow, MD, a Yun-Yi Hung, PhD, b Robert H. Pantell, MD c BACKGROUND: There is considerable variation
Management and Outcomes of Previously Healthy, Full-Term, Febrile Infants Ages 7 to 90 Days Tara L. Greenhow, MD, a Yun-Yi Hung, PhD, b Robert H. Pantell, MD c BACKGROUND: There is considerable variation
Ancillary Testing in Children with Rotavirus Gastroenteritis
 ORIGINAL RESEARCH Ancillary Testing in Children with Rotavirus Gastroenteritis Peter A. Rowinsky, MD 1,2 Andrew P. Steenhoff, MBBCh, DCH (UK), FCP (SA) Paed 3,4,5,6,7 Shiang-Ju Kung, MBBCh, DCH (SA) 8
ORIGINAL RESEARCH Ancillary Testing in Children with Rotavirus Gastroenteritis Peter A. Rowinsky, MD 1,2 Andrew P. Steenhoff, MBBCh, DCH (UK), FCP (SA) Paed 3,4,5,6,7 Shiang-Ju Kung, MBBCh, DCH (SA) 8
Disclosures. Background. Definitions. Why Worry about these Infants? Goals. Bacterial infection in the neonate and young infant: a review
 Disclosures Bacterial infection in the neonate and young infant: a review Russell J. McCulloh, MD Med-Peds Infectious Diseases August 8, 2017 I have no financial interests to disclose Funding: Eva and
Disclosures Bacterial infection in the neonate and young infant: a review Russell J. McCulloh, MD Med-Peds Infectious Diseases August 8, 2017 I have no financial interests to disclose Funding: Eva and
The value of acute phase reactants and LightCycler SeptiFast test in the diagnosis of bacterial and viral infections in pediatric patients
 Original article Arch Argent Pediatr 2018;116(1):35-41 / 35 The value of acute phase reactants and LightCycler SeptiFast test in the diagnosis of bacterial and viral infections in pediatric patients Gulcin
Original article Arch Argent Pediatr 2018;116(1):35-41 / 35 The value of acute phase reactants and LightCycler SeptiFast test in the diagnosis of bacterial and viral infections in pediatric patients Gulcin
Fever accounts for 10% to 20% of all pediatric emergency department
 CME REVIEW ARTICLE Update for the 21st Century Christopher Woll, MD,* Mark I. Neuman, MD, MPH, and Paul L. Aronson, MD* Abstract: Infants aged 90 days or younger with fever are frequently evaluated in
CME REVIEW ARTICLE Update for the 21st Century Christopher Woll, MD,* Mark I. Neuman, MD, MPH, and Paul L. Aronson, MD* Abstract: Infants aged 90 days or younger with fever are frequently evaluated in
Judith Klein, MD 2011 FEVER IN THE FIRST 36 MONTHS OF LIFE
 Judith Klein, MD 2011 FEVER IN THE FIRST 36 MONTHS OF LIFE Objectives A short history of the kiddie fever business Vaccinations Rapid viral testing Biomarkers Month-by-month approach to fevers in these
Judith Klein, MD 2011 FEVER IN THE FIRST 36 MONTHS OF LIFE Objectives A short history of the kiddie fever business Vaccinations Rapid viral testing Biomarkers Month-by-month approach to fevers in these
4/14/2010. Theoretical purpose of fever? Andrea Marmor, MD, MSEd Assistant Clinical Professor, Pediatrics UCSF April 13, 2010
 Andrea Marmor, MD, MSEd Assistant Clinical Professor, Pediatrics UCSF April 13, 2010 Parental touch? Absence of fever more reliable than presence. Axillary and tympanic Vulnerable to environmental and
Andrea Marmor, MD, MSEd Assistant Clinical Professor, Pediatrics UCSF April 13, 2010 Parental touch? Absence of fever more reliable than presence. Axillary and tympanic Vulnerable to environmental and
Top Ten Articles in Pediatric Hospital Medicine: Breaking Traditions
 Top Ten Articles in Pediatric Hospital Medicine: Breaking Traditions by Jimmy Beck MD, MEd, Assistant Professor of Pediatrics University of Washington, Seattle Children's Hospital; Anupama Subramony MD,
Top Ten Articles in Pediatric Hospital Medicine: Breaking Traditions by Jimmy Beck MD, MEd, Assistant Professor of Pediatrics University of Washington, Seattle Children's Hospital; Anupama Subramony MD,
ISF criteria (International sepsis forum consensus conference of infection in the ICU) Secondary peritonitis
 Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
PREDICTORS OF SERIOUS BACTERIAL INFECTION IN INFANTS UPTO 8 WEEKS OF AGE
 PREDICTORS OF SERIOUS BACTERIAL INFECTION IN INFANTS UPTO 8 WEEKS OF AGE Virendra Kumar Sunit Singhi ABSTRACT During a period of 2 years we prospectively studied 116 infants upto 8 weeks of age with suspected
PREDICTORS OF SERIOUS BACTERIAL INFECTION IN INFANTS UPTO 8 WEEKS OF AGE Virendra Kumar Sunit Singhi ABSTRACT During a period of 2 years we prospectively studied 116 infants upto 8 weeks of age with suspected
abstract ARTICLE BACKGROUND: A sequential approach to young febrile infants on the basis of clinical and
 Validation of the Step-by-Step Approach in the Management of Young Febrile Infants Borja Gomez, MD, a, b Santiago Mintegi, MD, PhD, a, b Silvia Bressan, MD, PhD, c Liviana Da Dalt, MD, d Alain Gervaix,
Validation of the Step-by-Step Approach in the Management of Young Febrile Infants Borja Gomez, MD, a, b Santiago Mintegi, MD, PhD, a, b Silvia Bressan, MD, PhD, c Liviana Da Dalt, MD, d Alain Gervaix,
MICROBIOLOGICAL TESTING IN PICU
 MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
REVIEW ARTICLE. Occult Serious Bacterial Infection in Infants Younger Than 60 to 90 Days With Bronchiolitis
 REVIEW ARTICLE Occult Serious Bacterial Infection in Infants Younger Than 60 to 90 Days With A Systematic Review Shawn Ralston, MD; Vanessa Hill, MD; Ami Waters, MD Objective: To summarize the risk of
REVIEW ARTICLE Occult Serious Bacterial Infection in Infants Younger Than 60 to 90 Days With A Systematic Review Shawn Ralston, MD; Vanessa Hill, MD; Ami Waters, MD Objective: To summarize the risk of
Clinical and laboratory indices of severe renal lesions in children with febrile urinary tract infection
 Clinical and laboratory indices of severe renal lesions in children with febrile urinary tract infection Constantinos J. Stefanidis Head of Pediatric Nephrology P. & A. Kyriakou Children s Hospital, Athens,
Clinical and laboratory indices of severe renal lesions in children with febrile urinary tract infection Constantinos J. Stefanidis Head of Pediatric Nephrology P. & A. Kyriakou Children s Hospital, Athens,
more than 90% of the bacterial isolates identified as Streptococcus pneumoniae
 Research Highlights Highlights from the latest papers in pediatric emergency medicine NEWS & VIEWS Wendy L Woolley & John H Burton Author for correspondence Department of Emergency Medicine Albany Medical
Research Highlights Highlights from the latest papers in pediatric emergency medicine NEWS & VIEWS Wendy L Woolley & John H Burton Author for correspondence Department of Emergency Medicine Albany Medical
greater than 10 will be considered ill appearing; a score of 10 or less will be considered well appearing.
 1 Use the Yale Observation Scale to assess whether the patient is ill or well appearing. A score greater than 10 will be considered ill appearing; a score of 10 or less will be considered well appearing.
1 Use the Yale Observation Scale to assess whether the patient is ill or well appearing. A score greater than 10 will be considered ill appearing; a score of 10 or less will be considered well appearing.
Management of Pediatric Urinary Tract Infections in Kuwait: Current Practices and Practicality of New Guidelines
 June 215 KUWAIT MEDICAL JOURNAL 139 Original Article Management of Pediatric Urinary Tract Infections in Kuwait: Current Practices and Practicality of New Guidelines Entesar H Husain 1,2, Talal Al-Saleem
June 215 KUWAIT MEDICAL JOURNAL 139 Original Article Management of Pediatric Urinary Tract Infections in Kuwait: Current Practices and Practicality of New Guidelines Entesar H Husain 1,2, Talal Al-Saleem
Low prevalence of invasive bacterial infection in febrile infants under 3 months of age with enterovirus infection
 ORIGINAL ARTICLE INFECTIOUS DISEASES Low prevalence of invasive bacterial infection in febrile infants under 3 months of age with enterovirus infection A. Martínez Planas 1, C. Muñoz Almagro 2, C. Luaces
ORIGINAL ARTICLE INFECTIOUS DISEASES Low prevalence of invasive bacterial infection in febrile infants under 3 months of age with enterovirus infection A. Martínez Planas 1, C. Muñoz Almagro 2, C. Luaces
Medline Abstracts for References 15,30-37
 Page 1 of 5 Official reprint from UpToDate www.uptodate.com 2013 UpToDate Medline Abstracts for References 15,30-37 of 'Fever without a source in children 3 to 36 months of age' 15 Check for full text
Page 1 of 5 Official reprint from UpToDate www.uptodate.com 2013 UpToDate Medline Abstracts for References 15,30-37 of 'Fever without a source in children 3 to 36 months of age' 15 Check for full text
Fever in Children. Dr Shane George Staff Specialist - Emergency Medicine & Children s Critical Care Gold Coast University Hospital
 Fever in Children Dr Shane George Staff Specialist - Emergency Medicine & Children s Critical Care Gold Coast University Hospital Update on Children s services @ GCUH Dedicated Children s Pod in the Emergency
Fever in Children Dr Shane George Staff Specialist - Emergency Medicine & Children s Critical Care Gold Coast University Hospital Update on Children s services @ GCUH Dedicated Children s Pod in the Emergency
1. Introduction Algorithm: Infant with Fever 0-28 Days Algorithm: Infant with Fever Days...3
 These guidelines are designed to assist clinicians and are not intended to supplant good clinical judgement or to establish a protocol for all patients with this condition. MANAGEMENT OF FEVER 38 C (100.4F)
These guidelines are designed to assist clinicians and are not intended to supplant good clinical judgement or to establish a protocol for all patients with this condition. MANAGEMENT OF FEVER 38 C (100.4F)
NIH Public Access Author Manuscript Pediatrics. Author manuscript; available in PMC 2007 November 14.
 NIH Public Access Author Manuscript Published in final edited form as: Pediatrics. 2006 July ; 118(1): 34 40. Prospective Evaluation of the Risk of Serious Bacterial Infection in Children Who Present to
NIH Public Access Author Manuscript Published in final edited form as: Pediatrics. 2006 July ; 118(1): 34 40. Prospective Evaluation of the Risk of Serious Bacterial Infection in Children Who Present to
How to Predict the Development of Severe Renal Lesions in Children with febrile UTI?
 How to Predict the Development of Severe Renal Lesions in Children with febrile UTI? Constantinos J. Stefanidis Head of Pediatric Nephrology P. & A. Kyriakou Children s Hospital, Athens, Greece Long term
How to Predict the Development of Severe Renal Lesions in Children with febrile UTI? Constantinos J. Stefanidis Head of Pediatric Nephrology P. & A. Kyriakou Children s Hospital, Athens, Greece Long term
Early infection diagnosis
 Procalcitonin in the EMERGENCY DEPARTMENT Early infection diagnosis and risk assessment with Procalcitonin (PCT) Early differential diagnosis and therapy decision in the emergency department Antibiotic
Procalcitonin in the EMERGENCY DEPARTMENT Early infection diagnosis and risk assessment with Procalcitonin (PCT) Early differential diagnosis and therapy decision in the emergency department Antibiotic
Good Morning! Welcome Applicants! FRIDAY, N OVEMBER, 7 TH 2014
 Good Morning! Welcome Applicants! FRIDAY, N OVEMBER, 7 TH 2014 Prep Question You are camping with a group of boys at a rural campground in the southeastern Unites States when one of the campers is bitten
Good Morning! Welcome Applicants! FRIDAY, N OVEMBER, 7 TH 2014 Prep Question You are camping with a group of boys at a rural campground in the southeastern Unites States when one of the campers is bitten
 Fever Phobia and the ED Doc Ran Goldman, MD (rgoldman@cw.bc.ca) BC Children s Hospital, Professor, University of British Columbia SLIDES ON : www.clinicalpeds.com/whistler Define Fever 38.0 o Doesn t
Fever Phobia and the ED Doc Ran Goldman, MD (rgoldman@cw.bc.ca) BC Children s Hospital, Professor, University of British Columbia SLIDES ON : www.clinicalpeds.com/whistler Define Fever 38.0 o Doesn t
Fever Interval before Diagnosis, Prior Antibiotic Treatment, and Clinical Outcome for Young Children with Bacterial Meningitis
 MAJOR ARTICLE Fever Interval before Diagnosis, Prior Antibiotic Treatment, and Clinical Outcome for Young Children with Bacterial Meningitis Bema K. Bonsu 1 and Marvin B. Harper 2 1 Department of Medicine,
MAJOR ARTICLE Fever Interval before Diagnosis, Prior Antibiotic Treatment, and Clinical Outcome for Young Children with Bacterial Meningitis Bema K. Bonsu 1 and Marvin B. Harper 2 1 Department of Medicine,
NEONATAL SEPSIS. Dalima Ari Wahono Astrawinata Departemen Patologi Klinik, FKUI-RSCM
 NEONATAL SEPSIS Dalima Ari Wahono Astrawinata Departemen Patologi Klinik, FKUI- Background Neonatal sepsis : Early-onset Late-onset Early-onset : mostly premature neonates Within 24 hours 85% 24-48 hours
NEONATAL SEPSIS Dalima Ari Wahono Astrawinata Departemen Patologi Klinik, FKUI- Background Neonatal sepsis : Early-onset Late-onset Early-onset : mostly premature neonates Within 24 hours 85% 24-48 hours
Hot Hot Tot:! The Hot Tot. Fever in KIds <90 Days 5/26/10
 Hot Hot Tot:! Fever in KIds
Hot Hot Tot:! Fever in KIds
Fever in Young Infants 7 90 days of age
 Fever in Young Infants 7 90 days of age Derek Zhorne, MD Clinical Assistant Professor of Pediatrics Pediatric Hospitalist Disclosures I have no actual or potential conflicts in relation to this presentation.
Fever in Young Infants 7 90 days of age Derek Zhorne, MD Clinical Assistant Professor of Pediatrics Pediatric Hospitalist Disclosures I have no actual or potential conflicts in relation to this presentation.
Urinary tract infection. Mohamed Ahmed Fouad Lecturer of pediatrics Jazan faculty of medicine
 Urinary tract infection Mohamed Ahmed Fouad Lecturer of pediatrics Jazan faculty of medicine Objectives To differentiate between types of urinary tract infections To recognize the epidemiology of UTI in
Urinary tract infection Mohamed Ahmed Fouad Lecturer of pediatrics Jazan faculty of medicine Objectives To differentiate between types of urinary tract infections To recognize the epidemiology of UTI in
FACTORS ASSOCIATED WITH DIAGNOSIS OF BACTERIAL PNEUMONIA IN CHILDREN OF NORTHERN THAILAND
 FACTORS ASSOCIATED WITH DIAGNOSIS OF BACTERIAL PNEUMONIA IN CHILDREN OF NORTHERN THAILAND Charung Muangchana National Vaccine Committee Office, Department of Disease Control, Ministry of Public Health,
FACTORS ASSOCIATED WITH DIAGNOSIS OF BACTERIAL PNEUMONIA IN CHILDREN OF NORTHERN THAILAND Charung Muangchana National Vaccine Committee Office, Department of Disease Control, Ministry of Public Health,
Management of Febrile Neonates in US Pediatric Emergency Departments
 ARTICLE Management of Febrile Neonates in US Pediatric Emergency Departments AUTHORS: Shabnam Jain, MD, MPH, a John Cheng, MD, a Elizabeth R. Alpern, MD, MSCE, b Cary Thurm, PhD, c Lisa Schroeder, MD,
ARTICLE Management of Febrile Neonates in US Pediatric Emergency Departments AUTHORS: Shabnam Jain, MD, MPH, a John Cheng, MD, a Elizabeth R. Alpern, MD, MSCE, b Cary Thurm, PhD, c Lisa Schroeder, MD,
11/9/2012. Group B Streptococcal Infections: Consensus and Controversies. Prevention of Early-Onset GBS Disease in the USA.
 Group B Streptococcal Infections: Consensus and Controversies Carol J. Baker, M.D. Professor of Pediatrics, Molecular Virology and Microbiology Executive Director, Center for Vaccine Awareness and Research
Group B Streptococcal Infections: Consensus and Controversies Carol J. Baker, M.D. Professor of Pediatrics, Molecular Virology and Microbiology Executive Director, Center for Vaccine Awareness and Research
Supplementary Online Content
 Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Fever is one of the most important reasons for childhood
 Fever in the Toddler-Aged Child: Old Concerns Replaced With New Ones Prashant Mahajan, MD, MPH, MBA, Rachel Stanley, MD, MHSA The widespread use of highly effective and safe vaccines against Haemophilus
Fever in the Toddler-Aged Child: Old Concerns Replaced With New Ones Prashant Mahajan, MD, MPH, MBA, Rachel Stanley, MD, MHSA The widespread use of highly effective and safe vaccines against Haemophilus
Paediatrica Indonesiana. Urine dipstick test for diagnosing urinary tract infection
 Paediatrica Indonesiana VOLUME 53 November NUMBER 6 Original Article Urine dipstick test for diagnosing urinary tract infection Syarifah Julinawati, Oke Rina, Rosmayanti, Rafita Ramayati, Rusdidjas Abstract
Paediatrica Indonesiana VOLUME 53 November NUMBER 6 Original Article Urine dipstick test for diagnosing urinary tract infection Syarifah Julinawati, Oke Rina, Rosmayanti, Rafita Ramayati, Rusdidjas Abstract
Clinical and Molecular Characteristics of Community- Acquired Methicillin-Resistant Staphylococcus Aureus Infections In Chinese Neonates
 Clinical and Molecular Characteristics of Community- Acquired Methicillin-Resistant Staphylococcus Aureus Infections In Chinese Neonates Xuzhuang Shen Beijing Children's Hospital, Capital Medical University,
Clinical and Molecular Characteristics of Community- Acquired Methicillin-Resistant Staphylococcus Aureus Infections In Chinese Neonates Xuzhuang Shen Beijing Children's Hospital, Capital Medical University,
Should blood cultures be obtained in all infants 3 to 36 months presenting with significant fever? abstract CLINICAL QUESTION REVIEW
 CLINICAL QUESTION REVIEW CQR is a recurring section in Hospital Pediatrics where authors start with a relevant clinical question, find and synthesize the recent literature and provide their best answer
CLINICAL QUESTION REVIEW CQR is a recurring section in Hospital Pediatrics where authors start with a relevant clinical question, find and synthesize the recent literature and provide their best answer
JMSCR Vol 05 Issue 04 Page April 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-76x ISSN (p) 2455-0450 DOI: https://dx.doi.org/0.8535/jmscr/v5i4.66 Research Paper Usefulness of routine haematological
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-76x ISSN (p) 2455-0450 DOI: https://dx.doi.org/0.8535/jmscr/v5i4.66 Research Paper Usefulness of routine haematological
Yield of Suprapubic Aspirate versus Bag Collection in Diagnosis of UTI in Children 0 to 6 Months of Age
 Proceeding S.Z.P.G.M.I. Vol: 25(2): pp. 61-65, 2011. Yield of Suprapubic Aspirate versus Bag Collection in Diagnosis of UTI in Children 0 to 6 Months of Age Lubna Riaz, Muhammad Aslam, Waqar Hussain, Anita
Proceeding S.Z.P.G.M.I. Vol: 25(2): pp. 61-65, 2011. Yield of Suprapubic Aspirate versus Bag Collection in Diagnosis of UTI in Children 0 to 6 Months of Age Lubna Riaz, Muhammad Aslam, Waqar Hussain, Anita
National Survey on the Impact of Viral Testing for the ED and Inpatient Management of Febrile Young Infants
 RESEARCH ARTICLE National Survey on the Impact of Viral Testing for the ED and Inpatient Management of Febrile Young Infants Brett Burstein, MD CM, PhD, a Alexander Sasha Dubrovsky, MD CM, MSc, a Andrew
RESEARCH ARTICLE National Survey on the Impact of Viral Testing for the ED and Inpatient Management of Febrile Young Infants Brett Burstein, MD CM, PhD, a Alexander Sasha Dubrovsky, MD CM, MSc, a Andrew
Scott Williams, MD Pediatric Nephrology OLOL Children s Hospital September 29, Controversies in Urinary Tract Infections
 Scott Williams, MD Pediatric Nephrology OLOL Children s Hospital September 29, 2013 Controversies in Urinary Tract Infections Disclaimer I have no affiliations with any pharmaceutical or equipment company
Scott Williams, MD Pediatric Nephrology OLOL Children s Hospital September 29, 2013 Controversies in Urinary Tract Infections Disclaimer I have no affiliations with any pharmaceutical or equipment company
Management of the Non Toxic-Appearing Acutely Febrile Child: A 21st Century Approach
 Management of the Non Toxic-Appearing Acutely Febrile Child: A 21st Century Approach Ravi Jhaveri, MD, Carrie L. Byington, MD, Jerome O. Klein, MD, and Eugene D. Shapiro, MD Although most febrile children
Management of the Non Toxic-Appearing Acutely Febrile Child: A 21st Century Approach Ravi Jhaveri, MD, Carrie L. Byington, MD, Jerome O. Klein, MD, and Eugene D. Shapiro, MD Although most febrile children
Fever in Babies. Too much testing or not enough testing? Martin E. Weisse, M.D. Pediatric Infectious Diseases
 Fever in Babies Too much testing or not enough testing? Martin E. Weisse, M.D. Pediatric Infectious Diseases Disclosures I have nothing to disclose Learning Objectives At the end of the talk, participants
Fever in Babies Too much testing or not enough testing? Martin E. Weisse, M.D. Pediatric Infectious Diseases Disclosures I have nothing to disclose Learning Objectives At the end of the talk, participants
Epidemiology of Infectious Complications of H1N1 Influenza Virus Infection
 Epidemiology of Infectious Complications of H1N1 Influenza Virus Infection Lyn Finelli, DrPH, MS Lead, Influenza Surveillance and Outbreak Response Epidemiology and Prevention Branch Influenza Division
Epidemiology of Infectious Complications of H1N1 Influenza Virus Infection Lyn Finelli, DrPH, MS Lead, Influenza Surveillance and Outbreak Response Epidemiology and Prevention Branch Influenza Division
Urinary tract infection and hyperbilirubinemia
 The Turkish Journal of Pediatrics 2006; 48: 51-55 Original Urinary tract infection and hyperbilirubinemia Hülya Bilgen 1, Eren Özek 1, Tamer Ünver 1, Neşe Bıyıklı 2 Harika Alpay 2, Dilşat Cebeci 3 Divisions
The Turkish Journal of Pediatrics 2006; 48: 51-55 Original Urinary tract infection and hyperbilirubinemia Hülya Bilgen 1, Eren Özek 1, Tamer Ünver 1, Neşe Bıyıklı 2 Harika Alpay 2, Dilşat Cebeci 3 Divisions
5/1/2015 SEPSIS SURVIVING SEPSIS CAMPAIGN HOW TO APPROACH THE POSSIBLE SEPTIC CHILD 2015 INFECTION CAN BE CONFIRMED BY:
 SURVIVING SEPSIS CAMPAIGN HOW TO APPROACH THE POSSIBLE SEPTIC CHILD 2015 Omer Nasiroglu MD Baptist Children s Hospital Pediatric Emergency Department SEPSIS IS A SYSTEMIC INFLAMMATORY RESPONSE SYNDROME
SURVIVING SEPSIS CAMPAIGN HOW TO APPROACH THE POSSIBLE SEPTIC CHILD 2015 Omer Nasiroglu MD Baptist Children s Hospital Pediatric Emergency Department SEPSIS IS A SYSTEMIC INFLAMMATORY RESPONSE SYNDROME
+ Objectives. n Define who is at risk for SBI. n Clarify risk stratification. n Provide treatment guidelines. n Bust some myths
 Objectives n Define wo is at risk for SBI n Clarify risk stratification n Provide treatment guidelines Neonatal Fever Benjamin B. Constance, MD, FAWM n Bust some myts Based on Case wat do you want to know?
Objectives n Define wo is at risk for SBI n Clarify risk stratification n Provide treatment guidelines Neonatal Fever Benjamin B. Constance, MD, FAWM n Bust some myts Based on Case wat do you want to know?
Outpatient treatment in women with acute pyelonephritis after visiting emergency department
 LETTER TO THE EDITOR Korean J Intern Med 2017;32:369-373 Outpatient treatment in women with acute pyelonephritis after visiting emergency department Hee Kyoung Choi 1,*, Jin-Won Chung 2, Won Sup Oh 3,
LETTER TO THE EDITOR Korean J Intern Med 2017;32:369-373 Outpatient treatment in women with acute pyelonephritis after visiting emergency department Hee Kyoung Choi 1,*, Jin-Won Chung 2, Won Sup Oh 3,
Clinical characteristics of febrile seizures and risk factors of its recurrence in Chiang Mai University Hospital
 Neurology Asia 2017; 22(3) : 203 208 Clinical characteristics of febrile seizures and risk factors of its recurrence in Chiang Mai University Hospital Worawit Kantamalee MD, Kamornwan Katanyuwong MD, Orawan
Neurology Asia 2017; 22(3) : 203 208 Clinical characteristics of febrile seizures and risk factors of its recurrence in Chiang Mai University Hospital Worawit Kantamalee MD, Kamornwan Katanyuwong MD, Orawan
Supplementary Online Content
 Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
Recommendations for Hospital Quality Measures in 2011:
 Pediatric Measures: Recommendations for Hospital Quality Measures in 2011: Based on the input of a group of healthcare stakeholders, the following new hospital measures are recommended: 1) Home Management
Pediatric Measures: Recommendations for Hospital Quality Measures in 2011: Based on the input of a group of healthcare stakeholders, the following new hospital measures are recommended: 1) Home Management
pneumonia 2015;6:48 56
 pneumonia 2015 Aug 21;6:48 56 pneumonia Brief Report Anne B Chang a,b, Heidi Smith-Vaughan a,c, Theo P Sloots f, Patricia C Valery a, David Whiley f, Jemima Beissbarth a, Paul J Torzillo d,e a Menzies
pneumonia 2015 Aug 21;6:48 56 pneumonia Brief Report Anne B Chang a,b, Heidi Smith-Vaughan a,c, Theo P Sloots f, Patricia C Valery a, David Whiley f, Jemima Beissbarth a, Paul J Torzillo d,e a Menzies
Blood cultures in ED. Dr Sebastian Chang MBBS FACEM
 Blood cultures in ED Dr Sebastian Chang MBBS FACEM Why do we care about blood cultures? blood cultures are the most direct method for detecting bacteraemia in patients a positive blood culture: 1. can
Blood cultures in ED Dr Sebastian Chang MBBS FACEM Why do we care about blood cultures? blood cultures are the most direct method for detecting bacteraemia in patients a positive blood culture: 1. can
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine
 Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine Discuss advances in predicting prognosis Understand dwhat we know (and don t know) about the Microbiology Recognize important
Brice Taylor Assistant Professor Division of Pulmonary and Critical Care Medicine Discuss advances in predicting prognosis Understand dwhat we know (and don t know) about the Microbiology Recognize important
Fever is one of the most frequent reasons for consultation in
 ORIGINAL STUDIES Impact of Rapid Viral Testing for Influenza A and B Viruses on Management of Febrile Infants Without Signs of Focal Infection Javier Benito-Fernández, MD, Miguel A. Vázquez-Ronco, MD,
ORIGINAL STUDIES Impact of Rapid Viral Testing for Influenza A and B Viruses on Management of Febrile Infants Without Signs of Focal Infection Javier Benito-Fernández, MD, Miguel A. Vázquez-Ronco, MD,
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
SURVEILLANCE BLOODSTREAM INFECTIONS IN BELGIAN HOPITALS ( SEP ) RESULTS ANNUAL REPORT data
 SURVEILLANCE BLOODSTREAM INFECTIONS IN BELGIAN HOPITALS ( SEP ) RESULTS ANNUAL REPORT data 2000-2014 SEP Workgroup Meeting 24 June 2015 Dr. Naïma Hammami Dr. Marie-Laurence Lambert naima.hammami@wiv-isp.be
SURVEILLANCE BLOODSTREAM INFECTIONS IN BELGIAN HOPITALS ( SEP ) RESULTS ANNUAL REPORT data 2000-2014 SEP Workgroup Meeting 24 June 2015 Dr. Naïma Hammami Dr. Marie-Laurence Lambert naima.hammami@wiv-isp.be
3.5. Background - CAP. Disclosure. Goal. Why Guidelines
 Disclosure The New PIDS-IDSA Community Acquired Pneumonia Guidelines Ricardo Quiñonez, MD, FAAP, FHM Section of Pediatric Hospital Medicine Baylor College of Medicine Texas Children s Hospital I have no
Disclosure The New PIDS-IDSA Community Acquired Pneumonia Guidelines Ricardo Quiñonez, MD, FAAP, FHM Section of Pediatric Hospital Medicine Baylor College of Medicine Texas Children s Hospital I have no
EPG Clinical Guidelines
 Guidelines for the Management of Febrile Young Children Neonate age 7 days Temperature > 38 C, documented at home or in the ED Complete blood count with manual differential (CBCD), urinalysis (UA), urine
Guidelines for the Management of Febrile Young Children Neonate age 7 days Temperature > 38 C, documented at home or in the ED Complete blood count with manual differential (CBCD), urinalysis (UA), urine
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Robinson, J, et al. and the Canadian Pediatric Society. Urinary tract infection in infants and children: Diagnosis and management. Pediatr Child Health 2014;
The McMaster at night Pediatric Curriculum Robinson, J, et al. and the Canadian Pediatric Society. Urinary tract infection in infants and children: Diagnosis and management. Pediatr Child Health 2014;
Routine endotracheal cultures for the prediction of sepsis in ventilated babies
 Archives of Disease in Childhood, 1989, 64, 34-38 Routine endotracheal cultures for the prediction of sepsis in ventilated babies T A SLAGLE, E M BIFANO, J W WOLF, AND S J GROSS Department of Pediatrics,
Archives of Disease in Childhood, 1989, 64, 34-38 Routine endotracheal cultures for the prediction of sepsis in ventilated babies T A SLAGLE, E M BIFANO, J W WOLF, AND S J GROSS Department of Pediatrics,
FEVER. What is fever?
 FEVER What is fever? Fever is defined as a rectal temperature 38 C (100.4 F), and a value >40 C (104 F) is called hyperpyrexia. Body temperature fluctuates in a defined normal range (36.6-37.9 C [97.9-100.2
FEVER What is fever? Fever is defined as a rectal temperature 38 C (100.4 F), and a value >40 C (104 F) is called hyperpyrexia. Body temperature fluctuates in a defined normal range (36.6-37.9 C [97.9-100.2
Does This Child Have a Urinary Tract Infection?
 EVIDENCE-BASED EMERGENCY MEDICINE/RATIONAL CLINICAL EXAMINATION ABSTRACT Does This Child Have a Urinary Tract Infection? EBEM Commentator Contact Rupinder Singh Sahsi, BSc, MD Christopher R. Carpenter,
EVIDENCE-BASED EMERGENCY MEDICINE/RATIONAL CLINICAL EXAMINATION ABSTRACT Does This Child Have a Urinary Tract Infection? EBEM Commentator Contact Rupinder Singh Sahsi, BSc, MD Christopher R. Carpenter,
Interval Likelihood Ratios: Another Advantage for the Evidence-Based Diagnostician
 EVIDENCE-BASED EMERGENCY MEDICINE/ SKILLS FOR EVIDENCE-BASED EMERGENCY CARE Interval Likelihood Ratios: Another Advantage for the Evidence-Based Diagnostician Michael D. Brown, MD Mathew J. Reeves, PhD
EVIDENCE-BASED EMERGENCY MEDICINE/ SKILLS FOR EVIDENCE-BASED EMERGENCY CARE Interval Likelihood Ratios: Another Advantage for the Evidence-Based Diagnostician Michael D. Brown, MD Mathew J. Reeves, PhD
PEDIATRICS/ORIGINAL RESEARCH
 PEDIATRICS/ORIGINAL RESEARCH Pneumococcal Bacteremia in Febrile Infants Presenting to the Emergency Department Before and After the Introduction of the Heptavalent Pneumococcal Vaccine Keri L. Carstairs,
PEDIATRICS/ORIGINAL RESEARCH Pneumococcal Bacteremia in Febrile Infants Presenting to the Emergency Department Before and After the Introduction of the Heptavalent Pneumococcal Vaccine Keri L. Carstairs,
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement
 CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
Antimicrobial Stewardship in Community Acquired Pneumonia
 Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Medical Management of childhood UTI and VUR. Dr Patrina HY Caldwell Paediatric Continence Education, CFA 15 th November 2013
 Medical Management of childhood UTI and VUR Dr Patrina HY Caldwell Paediatric Continence Education, CFA 15 th November 2013 Terminology According to the current ICCS terminology guidelines Bladder and
Medical Management of childhood UTI and VUR Dr Patrina HY Caldwell Paediatric Continence Education, CFA 15 th November 2013 Terminology According to the current ICCS terminology guidelines Bladder and
PEDIATRICS/ORIGINAL RESEARCH
 PEDIATRICS/ORIGINAL RESEARCH Comparison of the Test Characteristics of Procalcitonin to C-Reactive Protein and Leukocytosis for the Detection of Serious Bacterial Infections in Children Presenting With
PEDIATRICS/ORIGINAL RESEARCH Comparison of the Test Characteristics of Procalcitonin to C-Reactive Protein and Leukocytosis for the Detection of Serious Bacterial Infections in Children Presenting With
Fever and Infections in Pediatrics
 Fever and Infections in Pediatrics Dr. Todd Twogood 2019 update Big Sky Conference Pediatric Fever and illness The most common reason for children to be taken to the doctor for acute illness Major concern
Fever and Infections in Pediatrics Dr. Todd Twogood 2019 update Big Sky Conference Pediatric Fever and illness The most common reason for children to be taken to the doctor for acute illness Major concern
ARTICLE. Clinical Decision Rule to Identify Febrile Young Girls at Risk for Urinary Tract Infection
 Clinical Decision Rule to Identify Febrile Young Girls at Risk for Urinary Tract Infection Marc H. Gorelick, MD, MSCE; Kathy N. Shaw, MD, MSCE ARTICLE Objective: To develop a clinical prediction rule to
Clinical Decision Rule to Identify Febrile Young Girls at Risk for Urinary Tract Infection Marc H. Gorelick, MD, MSCE; Kathy N. Shaw, MD, MSCE ARTICLE Objective: To develop a clinical prediction rule to
Surveillance report Published: 7 July 2016 nice.org.uk. NICE All rights reserved.
 Surveillance report 2016 Urinary tract infection in under 16s: diagnosis and management (2007) NICE guideline CG54 Surveillance report Published: 7 July 2016 nice.org.uk NICE 2016. All rights reserved.
Surveillance report 2016 Urinary tract infection in under 16s: diagnosis and management (2007) NICE guideline CG54 Surveillance report Published: 7 July 2016 nice.org.uk NICE 2016. All rights reserved.
Bacteremia in Children: Etiologic Agents, Focal Sites, and Risk Factors
 Bacteremia in Children: Etiologic Agents, Focal Sites, and Risk Factors by L. F. Nimri, a M. Rawashdeh, b and M. M. Meqdam a a Department of Applied Biology, and b Department of Pediatrics, Jordan University
Bacteremia in Children: Etiologic Agents, Focal Sites, and Risk Factors by L. F. Nimri, a M. Rawashdeh, b and M. M. Meqdam a a Department of Applied Biology, and b Department of Pediatrics, Jordan University
Diagnostic Value of C - Reactive Protein and Other Hematological Parameters in Neonatal Sepsis
 Diagnostic Value of C - Reactive Protein and Other Hematological Parameters in Neonatal Sepsis Hafadh Jaleel Hussein*, Yusra Fayyadh Alwan** ABSTRACT: BACKGROUND: There have been many attempts to develop
Diagnostic Value of C - Reactive Protein and Other Hematological Parameters in Neonatal Sepsis Hafadh Jaleel Hussein*, Yusra Fayyadh Alwan** ABSTRACT: BACKGROUND: There have been many attempts to develop
Fever without Localizing Signs
 PART II Clinical Syndromes and Cardinal Features of Infectious Diseases: Approach to Diagnosis and Initial Management SECTION B Cardinal Symptom Complexes 14 Fever without Localizing Signs Eugene D. Shapiro
PART II Clinical Syndromes and Cardinal Features of Infectious Diseases: Approach to Diagnosis and Initial Management SECTION B Cardinal Symptom Complexes 14 Fever without Localizing Signs Eugene D. Shapiro
The Value of C-Reactive Protein in Children with Meningitis
 Helmy A. Qurtom, MRCP; Qusay A. Al-Salah, MRCP; Mahmoud M. Lubani, MD; Kamel I. Doudin, MD; Dinesh C. Sharda, FRCP; Areckal I. John, MD From the Department of Pediatrics, Farwania (Drs. Qurtom, Al-Saleh,
Helmy A. Qurtom, MRCP; Qusay A. Al-Salah, MRCP; Mahmoud M. Lubani, MD; Kamel I. Doudin, MD; Dinesh C. Sharda, FRCP; Areckal I. John, MD From the Department of Pediatrics, Farwania (Drs. Qurtom, Al-Saleh,
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A AAP. See American Academy of Pediatrics (AAP) Acyclovir dosing in infants, 185 187 American Academy of Pediatrics (AAP) COFN of, 199 204 Amphotericin
Note: Page numbers of article titles are in boldface type. A AAP. See American Academy of Pediatrics (AAP) Acyclovir dosing in infants, 185 187 American Academy of Pediatrics (AAP) COFN of, 199 204 Amphotericin
UTI are the most common genitourinary disease of childhood. The prevalence of UTI at all ages is girls and 1% of boys.
 UTI are the most common genitourinary disease of childhood. The prevalence of UTI at all ages is girls and 1% of boys. 1-3% of Below 1 yr. male: female ratio is 4:1 especially among uncircumcised males,
UTI are the most common genitourinary disease of childhood. The prevalence of UTI at all ages is girls and 1% of boys. 1-3% of Below 1 yr. male: female ratio is 4:1 especially among uncircumcised males,
