Radiculopathy of C-5 after anterior decompression for cervical myelopathy
|
|
|
- Gladys Gallagher
- 5 years ago
- Views:
Transcription
1 J Neurosurg Spine 3: , 2005 Radiculopathy of C-5 after anterior decompression for cervical myelopathy MINORU IKENAGA, M.D., PH.D., JITSUHIKO SHIKATA M.D., PH.D., AND CHIAKI TANAKA M.D., PH.D. Department of Orthopedic Surgery, Kyoto City Hospital; and Department of Orthopedic Surgery, Yawata Central Hospital, Kyoto, Japan Object. The authors conducted a study to examine the incidence and causes of postoperative C-5 radiculopathy, and they suggest preventive methods for C-5 palsy after anterior corpectomy and fusion. Methods. The authors included in the study 18 patients with postoperative C-5 radiculopathy from 563 patients who underwent anterior decompression and fusion for cervical myelopathy. There were 10 cases of ossification of the posterior longitudinal ligament (OPLL) and eight cases of cervical spondylotic myelopathy (CSM). All patients received conservative treatment. Posttreatment full recovery was present in eight patients, and Grade 3/5 strength was documented in six in whom some weakness remained. Radiographic evaluation revealed that the C3 4 and C4 5 cord compression was significantly more severe in patients with paralysis than in those without paralysis. The incidence of paralysis was higher in patients with OPLL than in those with CSM (chi-square test, p = 0.03). The incidence of paralysis increased in parallel with the number of fusion levels (correlation coefficient r = 0.94). Multivariate analysis revealed that the final manual muscle testing (MMT) value was closely related to the preoperative MMT value (computed t value 4.17; p 0.01) and preoperative Japanese Orthopaedic Association (JOA) score for cervical myelopathty (computed t value, 2.75; p 0.05). Conclusions. Preexisting severe stenosis at C3 4 or C4 5 in patients with OPLL is a risk factor for paralysis. Preoperative muscle weakness and a low JOA score are factors predictive of poor recovery. KEY WORDS anterior fusion cervical spine palsy C-5 palsy cervical myelopathy F OR the treatment of cervical myelopathy, anterior or posterior decompression has been advocated, and both procedures have been reported to yield generally good results. 1,3,4,6,7,9,23,24 Radiculopathy of C-5, however, has been reported as a major complication of both procedures. The development of radiculopathy after decompressive laminoplasty has been intensively studied, 2,5,19,20,21,25 whereas to date there are only a few studies of this complication after anterior decompression. 8,10,12 15,22 Radiculopathy of C-5 after decompression and multilevel corpectomy was noted first in the English literature by Shinomiya, et al. 15 They suggested that it was due to an axial rotation deformity of the cervical spine. They later also reported that the anatomical features of the C-5 nerve root may be a cause of the palsy. 16 Yonenobu, et al., 25 discussed possible causes of postdecompression radiculopathy: C-5 nerve root tethering, the anatomical morphology Abbreviations used in this paper: AP = anteroposterior; CSM = cervical spondylotic myelopathy; CT = computerized tomography; JOA = Japanese Orthopaedic Association; MMT = manual muscle test; MR = magnetic resonance; OPLL = ossification of the posterior longitudinal ligament. 210 of the C-5 root, and the single-nerve innervation to the deltoid muscle. In a 1995 study of a series of anterior corpectomies, Saunders 13 stated that a decompression width greater than 15 mm might increase the incidence of radiculopathy. In our clinic, anterior decompression procedures have been preferred for cervical myelopathy since During a 13-year period ( ), the total number of anterior decompression procedures was 563, representing the largest series yet reported. The purpose of this study was to analyze the incidence and characteristics of C-5 radiculopathy of after anterior decompression and fusion. Clinical Material and Methods Five hundred sixty-three patients with cervical myelopathy underwent anterior decompression and fusion in our hospital from 1989 to There were 353 male and 210 female patients who ranged in age from 11 to 86 years. There were 137 cases of OPLL, 287 cases of CSM, 79 cases of disc herniation, and 60 cases involving other lesions (Table 1). We performed a one-level fusion in 64 patients, two-level fusion in 137, three-level fusion
2 Radiculopathy of C-5 after anterior cervical decompression TABLE 1 Cause of radiculopathy in the overall patient population* Origin No. of Cases cervical spondylosis 328 OPLL 137 disc herniation 79 tumor 9 trauma 8 RA 2 total 563 * RA = rheumatoid arthritis. in 154, four-level fusion in 189, five-level fusion in 17, and six-level fusion in two cases (Table 2). The mean number of fusion levels was 2.9. In the patients in whom the fusion involved more than four disc levels, a plate was not placed; instead, halo vest fixation was used for 6 weeks and Philadelphia collar fixation for the next 6 weeks thereafter. In patients in whom the fusion incorporated one to three disc levels, a plate was implanted for internal fixation, and Philadelphia collar fixation was subsequently instituted for 3 months. Eighteen patients (13 male and five female patients) suffered postoperative motor dominant paralysis in the upper extremities (C-5 radiculopathy) and were included in the study (Table 2). The medical records of these 18 patients were intensively reviewed, and patient age, sex, laterality of the lesion, time of onset, and muscle power were recorded (Table 3). Manual muscle testing (Grades 0 5/5) was performed sequentially to determine recovery after the onset of paralysis. Clinical results were assessed using the JOA tool for measuring cervical myelopathy (JOA score; Table 4). The occupying ratios of ossification (Fig. 1A) at the C3 4, C4 5, and C5 6 disc levels were calculated for the OPLL cases. The AP diameters of the spinal canal (Fig. 1B) at these levels were also measured on preoperative CT myelograms obtained in all OPLL and CSM cases involving fusions across four or more disc levels. The Mann Whitney U-test was used to analyze the incidence of C-5 paralysis depending on the occupying ratio or AP diameter (Table 5). Postoperative anterior expansion of the dura mater and anterior shift of the spinal cord were measured at the C4 5 on pre- and postoperative MR images or CT myelograms available for each patient. The distance between the posterior wall of the spinal canal and the anterior dura and posterior surface of the cord was measured with a caliper (Fig. 2A and B). The decompression width was also measured using the same images. The measurement was made by comparing the pre- and postoperative images of the same slices, and, in cases in which there was difficulty in defining the intraoperative decompression width, by using the follow-up images when the graft was completely incorporated (Fig. 2C). Intergroup statistical analysis between patients with and without C-5 palsy was performed using the Mann Whitney U-test. The relationship of the incidence of paralysis to sex and cause of disease was analyzed using the chi-square test. The statistical difference in the laterality of paralysis was analyzed by binominal distribution analysis. Spearman rank coefficient analysis was used for analysis of the number of fused segments and the AP diameters at the C3 4, C4 5, and C5 6 levels. Multiple regression analysis was performed to identify factors influencing the final MMT value. In statistical analyses significance was set at a 5% level. Operative Technique TABLE 2 Fused levels and incidence of paralysis No. of Levels Fused No. of Cases of Fused Level Cases Paralysis (%) 1 C C C C C C C C6 T C (1.7) C (3.2) C5 T C (6.3) C (6.3) C4 T C (19) C3 T C2 T1 2 0 total (3.2) The operation was performed after induction of general anesthesia, and via a left anterior approach, a discectomy or partial corpectomy was performed using microscopic guidance. The dura mater was exposed by complete or partial resection of the PLL. An anterior cervical plate was implanted in the patients in whom the fusion incorporated fewer than three disc levels (183 cases-116 with Orion plates and 67 Atlantis plates). Autologous fibula or tricortical iliac crest was used for anterior reconstruction. Philadelphia collar fixation was initiated for 2 months postoperatively. For long fusions those crossing four or more disc levels anterior corpectomy, autologous fibula graft placement, and screw fixation (the Shikata technique) were preferred (no plate was used). Instead, we ordered halo vest therapy for the first 6 weeks and Philadelphia collar fixation for the subsequent 4 weeks postoperatively. Results Radiculopathy of C-5 occurred in the 18 patients (10 with OPLL and eight with CSM; Table 3). Weakness was present in the deltoid muscles in all 18, the biceps muscle in 17, and the triceps muscles in two cases right sided, 11 left sided, and one bilaterally (Table 3). The incidence of the paralysis when examined according to sex distribution showed no significant difference 211
3 M. Ikenaga, et al. TABLE 3 Summary of demographic data obtained in 18 patients with postoperative radiculopathy* JOA Score MMT Grade Postop Case Age (yrs), Levels Impaired Onset of Months to No. Sex Lesion Fused Muscles Preop FU Laterality Preop At Onset FU Paralysis Recovery 1 49, M CSM C3 7 D, B lt days , F CSM C3 7 D, B 9 14 lt hrs , M CSM C3 7 D, B, T 6 10 lt days , M CSM C3 7 D, B lt hrs , M CSM C3 7 D, B lt days , F CSM C3 7 D, B lt hrs , F CSM C4 7 D, B rt hrs , M CSM C4 7 D, B rt day , F OPLL C3 7 D, B lt days , F OPLL C3 7 D, B 3 10 lt hrs , M OPLL C2 7 D, B, T 8 14 rt days , M OPLL C2 7 D, B bilat hrs , M OPLL C2 7 D, B 9 9 lt days , M OPLL C3 7 D, B lt hrs , M OPLL C2 6 D, B 12 lt hrs , M OPLL C3 7 D, B rt days , M OPLL C3 6 D rt days , M OPLL C4 7 D, B rt hrs 3 mean days 4.1 * B = biceps; D = deltoid; FU = follow up; T = triceps. (chi-square test, p = 0.40). Its incidence was significantly higher in patients with OPLL than in those with CSM (chi-square test, p = 0.03). Laterality of the paralysis did not show a significant difference (binominal distribution analysis, p = 0.48). There were three cases of five-level fusion, 11 cases of four-level fusion, and four cases of three-level fusion. The overall incidence of palsy was 3.2%, but the incidence increased in parallel with the number of levels fused (correlation coefficient r = 0.94) (Table 2). At onset of weakness MMT of the affected muscles showed Grade 4/5 strength in two cases, 3/5 in nine, 2/5 in four, 1/5 in two, and 0/5 in one. The Spearman rank correlation coefficients showed that the AP diameters at C3 4, C4 5, and C-5 6 were not correlated with the MMT value at onset of the paralysis. Multivariate analysis revealed that the MMT grade at onset did not relate to the age, preoperative paralysis, number of levels fused, preoperative JOA score, or severity of compression at C3 4, C4 5, and C-5 6. The onset of the muscle weakness occurred within 24 hours of surgery in nine cases, 1 day in five, 3 days in two, 7 days in one, and 8 days in one (Table 3). Clearly detailed records of the upper-extremity functional status measured immediately after the operations were not be found in two cases in which the paralysis occurred within 4 hours of surgery. Sensory disturbance was not noted in any cases, but pain around the shoulder girdle was demonstrated in three cases. In one patient, whose paralysis occurred 8 days after the surgery, dull pain around the shoulder girdle preceded the onset of muscle weakness by 1 week. Radiographic evaluation revealed that the occupying ratio at C3 4 and C4 5 was significantly higher in patients with paralysis than in those without paralysis (Table 5). The AP diameter at C3 4 and C4 5 was significantly smaller in patients with paralysis than in those without paralysis (Table 5). Postoperative MR imaging and CT myelography revealed no cases in which the decompression was insufficient. The intergroup postoperative diameter of the dura and the decompression width between patients with and TABLE 4 The JOA scoring system for cervical myelopathy upper-extremity motor function 0 impossible to eat w/ chopsticks or spoon 1 possible to eat w/ spoon but not w/ chopsticks 2 possible to eat w/ chopsticks but inadequate 3 possible to eat w/ chopsticks but awkward 4 normal lower-extremity motor function 0 impossible to walk 1 need cane or aid on flat ground 2 need cane or aid only on stairs 3 possible to walk w/o cane or aid but slowly 4 normal sensory function upper-extremity 0 apparent sensory disturbance 1 minimal sensory disturbance 2 normal lower-extremity 0 apparent sensory disturbance 1 minimal sensory disturbance 2 normal trunk 0 apparent sensory disturbance 1 minimal sensory disturbance 2 normal bladder function 0 urinary retention or incontinence 1 severe dysuria (sense of retention, dribbling, thin stream, protracted micturition) 2 slight dysuria (Pollakiuria, retarded micturition) 3 normal total score for normal
4 Radiculopathy of C-5 after anterior cervical decompression TABLE 5 Summary of occupying ratios and AP diameter stratified by patients with and without paralysis Variable w/ Paralysis w/o Paralysis occupying ratio (%) C3 4* C4 5* C AP diameter (mm) C3 4* C4 5* C *Significant at p FIG. 1. Upper: Occupying ratios of ossification were calculated for the OPLL (ossification of the posterior longitudinal ligament) cases. Lower: The AP diameters of the spinal canal were measured. Illustrative Case Case 15 Presentation and Examination. This 61-year-old man had a 5-year history of left-handed numbness, which had increased 3 months before his visit to our clinic. Physical examination showed hyperreflexia of his extremities and difficulties with fine finger motion of both hands. He also exhibited gait difficulties, which resulted in his need of a handrail when climbing stairs. Preoperative MMT demonstrated normal findings. His preoperative JOA score was 12. Plain x-radiography (Fig. 3A and B) and MR imaging (Fig. 4A and B) revealed C2 5 OPLL predominantly on the left side. Myelography and postmyelograhy CT scanning demonstrated severe cord compression secondary to OPLL (Fig. 5). The occupying ratio in the cord canal was 70 and 80% at C3 4 and C4 5, respectively. Operation. We performed anterior corpectomy and strut fibular graft placement from C-2 to C-6 (Fig. 6A and B). Severe adhesion of the ossified ligament and dura mater without paralysis were not significantly different (Mann Whitney U-test, p = 0.71 and 0.96, respectively). The extent of postoperative anterior shift of the spinal cord was significantly less in the group with paralysis compared with the group without paralysis ( and mm, respectively; Mann Whitney U-test, p 0.01) (Table 6). All patients were treated conservatively. Full recovery occurred in 13 cases. In three patients muscle strength recovered to Grade 3/5 and in two it recovered to Grade 4/5, but weakness remained in these five patients. Recovery was observed within 1 to 11 months (mean 4.1 months) after the onset of paralysis. Incomplete recovery was documented in four of 10 patients with OPLL and in one of eight patients with CSM; however, analysis revealed no statistically significant difference (chi-square test, p = 0.20). In all five cases of incomplete recovery, MMT at onset of paralysis was Grade 2/5 or less, and in all cases in which MMT showed a grade of at least 3/5 at onset, full recovery occurred over time (chi-square test, p = 0.001). Multivariate analysis revealed that the final MMT was closely related to the preoperative counterpart grade (computed t value = 4.17, p 0.01) and preoperative JOA score (computed t value = 2.75, p 0.05; Table 7). FIG. 2. The AP diameter of the dura (a), anterior shift of the spinal cord (b), and decompression width (c) were measured using the postoperative axial images. 213
5 M. Ikenaga, et al. TABLE 6 Summary of postoperative radiological measurements stratified by absence or presence of paralysis* W/ Para- W/O Para- Variable lysis (mm) lysis (mm) p Value AP dural diameter decompression width anterior shift of the spinal cord * Values are presented as the mean standard deviation. was observed intraoperatively. Careful decompression and resection were performed under the microscope. Because of the adhesion, a thin fragment of the ossified ligament was left on the dura mater to prevent leakage of cerebrospinal fluid. Postoperative Course. The numbness and fine finger motion improved postoperatively, and MMT of the upper extremities just after the operation showed Grade 5/5 strength; however, he experienced shoulder and elbow weakness 4 hours after surgery. On the following day, MMT showed Grade 1/5 strength for the deltoid and biceps muscles on his left side. Postoperative radiography and CT scanning revealed complete resection of the ossified PLL, and the decompression appeared perfect (Fig. 7 A and B). A rehabilitation program, including physiotherapy and occupational therapy, commenced on Day 1 after the operation. Active muscle exercises and passive range of motion exercises were initiated with the assistance of a physiotherapist. Passive range of motion exercises involving a pulley were also performed to prevent joint contracture. The rehabilitation programs continued for 3 months. Muscle power recovered gradually to Grade 3/5 in the deltoid and biceps muscles 3 months postoperatively. FIG. 3. Preoperative AP (left) and lateral (right) radiographs revealing C2 5 OPLL. mechanism of C-5 palsy. 19 Yonenobu and associates 25 described five of 180 patients with C-5 palsy. Chiba, et al., 2 reported 16 cases (7.7%) of paralysis in 208 patients who underwent open-door laminoplasties. Minoda, et al., 11 recently reported an incidence of paralysis of 8.9% (four of 45 patients) after midsagittal-splitting laminoplasty. There have been, however, only a few detailed reports concerning C-5 palsy after anterior cervical corpectomy and fusion. Saunders 13 reported an incidence of paralysis of 2.5% (one of 40 patients), Yonenobu and coworkers 25 reported paral- Discussion There have been several reports in which investigators have described the incidence of C-5 palsy after cervical laminoplasty. Tsuzuki and colleagues 20 have stated that C-5 nerve root palsy occurred in 13 (8.4%) of 155 patients, and later they described in detail the pathological TABLE 7 Summary of computed t values of each factor in the multivariate analysis for the final MMT grade Factors Computed t Value preop MMT grade 4.17* age 0.56 preop JOA score 2.75 time needed for recovery 0.09 AP diameter C C C no. of levels fused 1.15 duration before onset of paralysis 0.15 * Significant at p Significant at p FIG. 4. Preoperative sagittal T 1 (left) and T 2 -weighted (right) MR images demonstrating C2 5 OPLL. 214
6 Radiculopathy of C-5 after anterior cervical decompression FIG. 5. Preoperative CT myelograms of the C3 4 (upper) and C4 5 levels (lower) revealing severe cord compression secondary to the ossified ligament predominantly on the left side. ysis in eight of 205 cases, and Wada, et al., 22 reported an incidence of 4% with anterior corpectomy and fusion of 2.5 levels. In our series, the incidence of paralysis tended to increase in parallel with the number of the levels fused, but the incidence of palsy in 563 cases was 3.2% for a mean of 2.9 levels of fusion. This incidence seems to be almost identical to that reported by Wada, et al. (4.4% for a mean of 2.5 levels fused). Numerous investigators have speculated on the cause of the palsy but none has provided unequivocal evidence of its mechanism(s). In 1996, Tsuzuki, et al., 19 postulated that the tethering effect of the nerve rootlet as a mechanism caused postoperative radiculopathy after cervical laminoplasty. This theory, however, does not seem to be applicable to anterior decompression, because the spinal cord tends to move anteriorly after the procedure (Table 6), which implies possible reduction of the tensile force on the rootlet. In our series, the incidence of palsy increased with the number of levels decompressed (Table 2), underscoring the possibility that the extent of anterior dural expansion might have enhanced the incidence. Saunders 13 stated that too much anterior expansion could potentially cause an increase in root traction force. In our series, however, Spearman rank correlation testing revealed that the AP diameters at C3 4 and C4 5 had significant correlation with the number of fusion levels. Therefore, the increased incidence associated with multilevel fusion could be an indirect reflection of the severity of cord compression. Postoperative radiological studies also revealed anterior dural expansion after decompression (Table 6). The values of anterior dural expansion and the values of the decompression widths between patients with and without paralysis did not show any statistical difference. These data, therefore, do not provide sufficient evidence to support strongly Saunders idea that the restriction of the decompression width to less than 15 mm could serve as a preventive tactic for C-5 palsy. Postoperative anterior shift of the spinal cord, however, was significantly restricted in the group with paralysis (p 0.01) and this was thought to implicate intradural spinal cord adhesion as a possible cause of the C-5 palsy because anterior dural expansion with adhesion of the radix ventralis to the dura mater under restricted anterior movement of the spinal cord could generate increased tensile force on the radix ventralis. We were unable to establish ample evidence to prove this hypothesis at this point. Other authors have discussed that palsy may be caused by mechanisms other than the nerve root itself. Minoda, et FIG. 6. Postoperative AP (left) and lateral (right). Anterior C3 5 corpectomy and fusion with a C2 6 fibula graft. 215
7 M. Ikenaga, et al. FIG. 7. Postoperative CT myelograms of the C3 4 (upper) and C4 5 (lower) levels revealing a successful decompression. A thin fragment of the ossified ligament was left on the dura mater. al., 11 stated that C3 4 OPLL was associated with a higher risk of C-5 palsy. The partial disparity between the levels of the spinal cord compression and the segmental levels of neurological impairment implies that the cause of the paralysis is not restricted to the nerve root alone. We found that the cause may also potentially be related to the loss of function of the anterior radicular cells of the spinal cord s gray matter. Analysis of our data also showed that spinal cord compression was significantly more severe at the C3 4 or C4 5 levels in patients with paralysis compared with cases without paralysis. The paralysis occurred on the left side in 12 patients and on the right in seven. Although the difference was not statistically significant, the predominance of the left-sided incidence introduces the suspicion that incomplete decompression or unexpected cord or nerve root damage could be a potential cause of the paralysis. Careful assessment of postoperative CT scans revealed no evidence of insufficient decompression such as a remnant of the ossified PLL or osteophytes at the root canal. Tsuzuki, et al., 19 reported that longitudinal durotomy could be successfully used to treat radiculopathy. In our series, durotomy was not performed, but good recovery occurred in all patients. Conservative therapy seems to have its limitations, especially in cases in which muscle power is less than Grade 2/5 at onset. Durotomy may be a treatment possibility for severe cases, but we as yet have not attempted it. Although conservative treatment was chosen for our cases and the results were favorable, muscle weakness remained in several cases at follow-up examination. Multivariate analysis revealed that the MMT grade at onset of paralysis and preoperative JOA score were closely related with the final MMT grade (Table 7), and patients with a grade of 2/5 or less at onset had a high risk of poor outcome compared with those whose grade was at least 3/5. This suggests surgical treatment of C-5 palsy or prophylactic durotomy is indicated in patients with preoperative MMT-documented weakness. We were unable to identify any single predominant causative factor of C-5 root palsy. The absence of electromyography data are the limitation of the study. We are therefore now planning a new prospective study that includes pre- and postoperative electromyography, which could potentially reveal the pathogenesis of the complication more clearly. In this study, however, we did show the increased risk of C-5 palsy in cases of OPLL in which there was severe compression at C3 4 and C4 5. Our findings also made clear the possible risk of a poor result for the patients with preoperative MMT-documented weakness in the deltoid muscle. Anterior corpectomy and fusion for multilevel cervical myelopathy is somewhat challenging, but its safety and advantages when performed by a well-trained and skillful surgeon have been established. 18 Particularly in cases of cervical stenosis or OPLL with kyphotic alignment, anterior decompression is the treatment of choice. 17,26 In our study, the incidence of postoperative C-5 radiculopathy after the anterior approach was 3.2%; however, there was no deterioration in long tract signs. This incidence of palsy seems not to affect the usefulness of anterior decompression for cervical myelopathy. References 1. Bohlman HH: Cervical spondylosis with moderate to severe myelopathy. A report of seventeen cases treated by Robinson anterior cervical discectomy and fusion. Spine 2: , Chiba K, Toyama Y, Matsumoto M, Maruiwa H, Wantanabe M, Hirabayashi K: Segmental motor paralysis after expansive open-door laminoplasty. Spine 27: , Edwards CC, Heller JG, Murakami H: Corpectomy versus laminoplasty for multilevel cervical myelopathy: an independent matched-cohort analysis. Spine 27: , Hanai K, Inoue Y, Kawai K, Tago K, Itoh Y: Anterior decompression for myelopathy resulting from ossification of the posterior longitudinal ligament. J Bone Joint Surg Br 64: , Hirabayashi K, Satomi K, Ichimura S, Tanaka K, Wakano K, Toyama Y: [Complication of expansive open-door laminoplasty for ossification of the posterior longitudinal ligament in the cervical spine.] Rinsho Seikei Geka 23: , 1988 (Jpn) 6. Hirabayashi K, Watanabe K, Wakano K, Suzuki N, Satomi K, Ishii Y: Expansive open-door laminoplasty for cervical spinal stenotic myelopathy. Spine 8: ,
8 Radiculopathy of C-5 after anterior cervical decompression 7. Kirita Y, Miyazaki K, Hayashi T, Nosaka K, Shima M, Yamamura H, Tamaki S: [Clinical findings and surgical results of the ossification of the posterior longitudinal ligament in the cervical spine.] Rinsho Seikeigeka 10: , 1975 (Jpn) 8. Macdonald RL, Fehlings MG, Tator CH, Lozano A, Fleming JR, Gentili F, et al: Multilevel anterior cervical corpectomy and fibular allograft fusion for cervical myelopathy. J Neurosurg 86: , Matsuoka T, Yamaura I, Kurosa Y, Nakai O, Shindo S, Shinomiya K: Long-term results of the anterior floating method for cervical myelopathy caused by ossification of the posterior longitudinal ligament. Spine 26: , Mayr MT, Subach BR, Comey CH, Rodts GE, Haid RW: Cervical spinal stenosis: outcome after anterior corpectomy, allograft reconstruction, and instrumentation. J Neurosurg (Spine 2) 96:10 16, Minoda Y, Nakamura H, Konishi S, Nagayama R, Suzuki E, Yamao Y, et al: Palsy of the C-5 nerve root after midsagittal-splitting laminoplasty of the cervical spine. Spine 28: , Okada K, Shirasaki N, Hayashi H, Oka S, Hosoya T: Treatment of spondylotic myelopathy by enlargement of the spinal canal anteriorly, followed by arthrodesis. J Bone Joint Surg Am 73: , Saunders RL: On the pathogenesis of the radiculopathy complicating multilevel corpectomy. Neurosurgery 37: , Saunders RL, Bernini PM, Shirreffs TG, Reeves AG: Central corpectomy for cervical spondylotic myelopathy: a consecutive series with long-term follow-up evaluation. J Neurosurg 74: , Shinomiya K, Kurosa Y, Fuchioka M, Furuya K: Clinical study of dissociated motor weakness following anterior cervical decompression surgery. Spine 14: , Shinomiya K, Okawa A, Nakao K, Mochida K, Haro K, Sato T, et al: Morphology of C-5 ventral nerve rootlets as part of dissociated motor loss of deltoid muscle. Spine 19: , Suda K, Abumi K, Ito M, Shono Y, Kaneda K, Fujiya M: Local kyphosis reduces surgical outcomes of expansive open-door laminoplasty for cervical spondylotic myelopathy. Spine 28: , Tani T, Ushida T, Ishida K, Iai H, Noguchi T, Yamamoto H: Relative safety of anterior microsurgical decompression versus laminoplasty for cervical myelopathy with a massive ossified posterior longitudinal ligament. Spine 27: , Tsuzuki N, Abe R, Saiki K, Shongshi L: Extradural tethering effect as one mechanism of radiculopathy complicating posterior decompression of the cervical spinal cord. Spine 21: , Tsuzuki N, Tanaka H, Abe R, Hotta Y, Okai K: [Cervical radiculopathy occurring after the posterior decompression of the cervical spinal cord.] Rinsho Seikei Geka 26: , 1991 (Jpn) 21. Uematsu Y, Tokuhashi Y, Matsuzaki H: Radiculopathy after laminoplasty of the cervical spine. Spine 23: , Wada E, Suzuki S, Kanazawa A, Matsuoka T, Miyamoto S, Yonenobu K: Subtotal corpectomy versus laminoplasty for multilevel cervical spondylotic myelopathy: a long-term follow-up study over 10 years. Spine 26: , Whitecloud TS, LaRocca H: Fibular strut graft in reconstructive surgery of the cervical spine. Spine 1:33 43, Yonenobu K, Hosono N, Iwasaki M, Asano M, Ono K: Laminoplasty versus subtotal corpectomy: a comparative study of results in multisegmental cervical spondylotic myelopathy. Spine 17: , Yonenobu K, Hosono N, Iwasaki M, Asano M, Ono K: Neurologic complications of surgery for cervical compression myelopathy. Spine 16: , Zdeblick TA, Bohlman HH: Cervical kyphosis and myelopathy: treatment by anterior corpectomy and strut-grafting. J Bone Joint Surg Am 71: , 1989 Manuscript received March 24, Accepted in final form June 7, Address reprint requests to: Minoru Ikenaga, M.D., Ph.D., Department of Orthopedic Surgery, Kyoto City Hospital, 1-2 Higashitakada-cho, Mibu, Nakagyo-ku, Kyoto-shi, Kyoto , Japan. taketori@nyc.odn.ne.jp. 217
Yoshifumi Kudo, 1 Tomoaki Toyone, 1 Toshiyuki Shirahata, 1 Tomoyuki Ozawa, 1 Akira Matsuoka, 1 Yoichi Jin, 2 and Katsunori Inagaki 1. 1.
 Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki 3), Masatsune Yamagata 1), Yoshikazu Ikeda 1), Fumitake Nakajima 1)
 Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Rick C. Sasso MD Professor Chief of Spine Surgery Clinical Orthopaedic Surgery Indiana University School of Medicine
 Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy
 THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
Jing Tao Zhang 1, Lin Feng Wang 1, Yue Ju Liu 2, Jun Ming Cao 1, Jie Li 1, Shuai Wang 1 and Yong Shen 1*
 Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Disclosures: T. Yoshii: None. T. Yamada: None. T. Taniyama: None. S. Sotome: None. T. Kato: None. S. Kawabata: None. A. Okawa: None.
 Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty
 Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty Nobuhiro Tanaka 1, 2), Kazuyoshi Nakanishi 2), Naosuke Kamei 2), Toshio Nakamae 2), Shinji Kotaka 2), Yoshinori Fujimoto 1),
Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty Nobuhiro Tanaka 1, 2), Kazuyoshi Nakanishi 2), Naosuke Kamei 2), Toshio Nakamae 2), Shinji Kotaka 2), Yoshinori Fujimoto 1),
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
The Correlation Study of C5 Nerve Root Palsy and Common Body Position in Posterior Total Laminectomy Decompression and Instrumentation
 DOI: 10.5137/1019-5149.JTN.7476-12.1 Received: 30.10.2012 / Accepted: 11.02.2013 Original Investigation The Correlation Study of C5 Nerve Root Palsy and Common Body Position in Posterior Total Laminectomy
DOI: 10.5137/1019-5149.JTN.7476-12.1 Received: 30.10.2012 / Accepted: 11.02.2013 Original Investigation The Correlation Study of C5 Nerve Root Palsy and Common Body Position in Posterior Total Laminectomy
Radiological pathogenesis of cervical myelopathy in 60 consecutive patients with cervical ossi cation of the posterior longitudinal ligament
 Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI /s
 Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Analysis of C5 palsy in cervical myelopathy with massive anterior compression following laminoplasty
 Chen et al. Journal of Orthopaedic Surgery and Research (2018) 13:26 DOI 10.1186/s13018-018-0715-3 RESEARCH ARTICLE Open Access Analysis of C5 palsy in cervical myelopathy with massive anterior compression
Chen et al. Journal of Orthopaedic Surgery and Research (2018) 13:26 DOI 10.1186/s13018-018-0715-3 RESEARCH ARTICLE Open Access Analysis of C5 palsy in cervical myelopathy with massive anterior compression
Op e n-d o o r laminoplasty was developed by Hirabayashi. Risk factors for closure of lamina after open-door laminoplasty.
 J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement
 Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement Thomas T. Lee, M.D., Glen R. Manzano, B.S., and Barth A.
Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement Thomas T. Lee, M.D., Glen R. Manzano, B.S., and Barth A.
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Department of Neurological Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
 online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic resonance imaging study evidence
 See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Cervical myelopathy is a common disease that is
 TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
Lift-up laminoplasty for myelopathy caused by ossification of the posterior longitudinal ligament of the cervical spine
 Original Article Lift-up laminoplasty for myelopathy caused by ossification of the posterior longitudinal ligament of the cervical spine T. Takami, K. Ohata, T. Goto, M. Nishikawa, A. Nishio, N. Tsuyuguchi,
Original Article Lift-up laminoplasty for myelopathy caused by ossification of the posterior longitudinal ligament of the cervical spine T. Takami, K. Ohata, T. Goto, M. Nishikawa, A. Nishio, N. Tsuyuguchi,
Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty
 Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 508534, 5 pages doi:10.1155/2012/508534 Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty Brett
Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 508534, 5 pages doi:10.1155/2012/508534 Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty Brett
Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis
 Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Complex Spine Symposium January 12th, Balgrist University Hospital
 DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
Abstract Study Design Systematic review. Weerasak Singhatanadgige 1 Worawat Limthongkul 1 Frank Valone III 2 Wicharn Yingsakmongkol 1 K.
 702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy
 . 6. Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy WAN Jun, XU Tian-tong*, SHEN Qing-feng, LI Hui-nan and XIA Ying-peng Abstract
. 6. Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy WAN Jun, XU Tian-tong*, SHEN Qing-feng, LI Hui-nan and XIA Ying-peng Abstract
We performed CT myelography in 38 patients
 Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
ORIGINAL PAPER. Department of Orthopedic Surgery, Chubu Rosai Hospital, Nagoya, Japan ABSTRACT
 Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine
 J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire: Part 3. Determination of reliability
 J Orthop Sci (2007) 12:321 326 DOI 10.1007/s00776-007-1131-4 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire: Part 3. Determination of reliability Mitsuru
J Orthop Sci (2007) 12:321 326 DOI 10.1007/s00776-007-1131-4 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire: Part 3. Determination of reliability Mitsuru
ASJ. Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy. Asian Spine Journal.
 Asian Spine Journal 298 Satoshi Clinical Baba et al. Study http://dx.doi.org/10.4184/asj.2016.10.2.298 Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy
Asian Spine Journal 298 Satoshi Clinical Baba et al. Study http://dx.doi.org/10.4184/asj.2016.10.2.298 Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy
Cervical Spine Surgery: Approach related outcome
 Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Original Investigation. Byung-Wan CHOI. INTRODUCTION Ossification of the posterior longitudinal ligament ABSTRACT
 DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review and meta-analysis
 Eur Spine J (201) 22:158 159 DOI 10.1007/s00586-01-2817-2 ORIGINAL ARTICLE Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review
Eur Spine J (201) 22:158 159 DOI 10.1007/s00586-01-2817-2 ORIGINAL ARTICLE Anterior approach versus posterior approach for the treatment of multilevel cervical spondylotic myelopathy: a systemic review
Comparative Effectiveness of Different Types of Cervical Laminoplasty
 Systematic Review 105 Comparative Effectiveness of Different Types of Cervical Laminoplasty John G. Heller 1 Annie L. Raich 2 Joseph R. Dettori 2 K. Daniel Riew 3 1 Department of Orthopaedic Surgery, Emory
Systematic Review 105 Comparative Effectiveness of Different Types of Cervical Laminoplasty John G. Heller 1 Annie L. Raich 2 Joseph R. Dettori 2 K. Daniel Riew 3 1 Department of Orthopaedic Surgery, Emory
Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태
 KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
We have reviewed the cervical spine radiographs
 THE CERVICAL SPINE IN ATHETOID CEREBRAL PALSY A RADIOLOGICAL STUDY OF 180 PATIENTS TAKEO HARADA, SOHEI EBARA, MONZOOR M. ANWAR, ATSUKO OKAWA, ICHIRO KAJIURA, KAZUO HIROSHIMA, KEIRO ONO From Osaka Police
THE CERVICAL SPINE IN ATHETOID CEREBRAL PALSY A RADIOLOGICAL STUDY OF 180 PATIENTS TAKEO HARADA, SOHEI EBARA, MONZOOR M. ANWAR, ATSUKO OKAWA, ICHIRO KAJIURA, KAZUO HIROSHIMA, KEIRO ONO From Osaka Police
Surgical Treatment for Ossification of the Posterior Longitudinal Ligament (OPLL) at the Thoracic Spine: Usefulness of the Posterior Approach
 REVIEW ARTICLE SPINE SURGERY AND RELATED RESEARCH Surgical Treatment for Ossification of the Posterior Longitudinal Ligament (OPLL) at the Thoracic Spine: Usefulness of the Posterior Approach Shigeru Hirabayashi,
REVIEW ARTICLE SPINE SURGERY AND RELATED RESEARCH Surgical Treatment for Ossification of the Posterior Longitudinal Ligament (OPLL) at the Thoracic Spine: Usefulness of the Posterior Approach Shigeru Hirabayashi,
Unanswered Questions. Laminoplasty is best
 Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Spinal Cord (2005) 43, & 2005 International Spinal Cord Society All rights reserved /05 $
 (2005) 43, 503 507 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Case Report Postmortem study of the spinal cord showing snake-eyes appearance due to damage by
(2005) 43, 503 507 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Case Report Postmortem study of the spinal cord showing snake-eyes appearance due to damage by
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up
 Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY
 CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
Laminoplasty for Cervical Myelopathy
 Review Article 187 Manabu Ito 1 Ken Nagahama 2 1 Department of Advanced Medicine for Spine and Spinal Cord Disorders, Hokkaido University Graduate School of Medicine, Sapporo, Japan 2 Department of Orthopaedic
Review Article 187 Manabu Ito 1 Ken Nagahama 2 1 Department of Advanced Medicine for Spine and Spinal Cord Disorders, Hokkaido University Graduate School of Medicine, Sapporo, Japan 2 Department of Orthopaedic
Postoperative C5 Palsy: Conjectured Causes and Effective Countermeasures
 REVIEW ARTICLE SPINE SURGERY AND RELATED RESEARCH Postoperative C5 Palsy: Conjectured Causes and Effective Countermeasures Shigeru Hirabayashi, Tomoaki Kitagawa, Iwao Yamamoto, Kazuaki Yamada and Hirotaka
REVIEW ARTICLE SPINE SURGERY AND RELATED RESEARCH Postoperative C5 Palsy: Conjectured Causes and Effective Countermeasures Shigeru Hirabayashi, Tomoaki Kitagawa, Iwao Yamamoto, Kazuaki Yamada and Hirotaka
Kazunari Takeuchi Æ Toru Yokoyama Æ Atsushi Ono Æ Takuya Numasawa Æ Kanichiro Wada Æ Taito Itabashi Æ Satoshi Toh
 Eur Spine J (2008) 17:415 420 DOI 10.1007/s00586-007-0553-1 ORIGINAL ARTICLE Limitation of activities of daily living accompanying reduced neck mobility after laminoplasty preserving or reattaching the
Eur Spine J (2008) 17:415 420 DOI 10.1007/s00586-007-0553-1 ORIGINAL ARTICLE Limitation of activities of daily living accompanying reduced neck mobility after laminoplasty preserving or reattaching the
Anterior decompression for cervical spondylosis associated with an early form of cervical ossification of the posterior longitudinal ligament
 Neurosurg Focus 12 (1):Article 12, 2002, Click here to return to Table of Contents Anterior decompression for cervical spondylosis associated with an early form of cervical ossification of the posterior
Neurosurg Focus 12 (1):Article 12, 2002, Click here to return to Table of Contents Anterior decompression for cervical spondylosis associated with an early form of cervical ossification of the posterior
Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study
 CLINICAL ARTICLE J Neurosurg Spine 27:627 632, 2017 Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study Takeshi
CLINICAL ARTICLE J Neurosurg Spine 27:627 632, 2017 Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study Takeshi
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Cervical spondylotic myelopathy (CSM) is a progressive
 literature review J Neurosurg Spine 24:77 99, 2016 A systematic review of clinical and surgical predictors of complications following surgery for degenerative cervical myelopathy Lindsay Tetreault, BSc,
literature review J Neurosurg Spine 24:77 99, 2016 A systematic review of clinical and surgical predictors of complications following surgery for degenerative cervical myelopathy Lindsay Tetreault, BSc,
Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for severity scores
 J Orthop Sci (2008) 13:25 31 DOI 10.1007/s00776-007-1194-2 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for
J Orthop Sci (2008) 13:25 31 DOI 10.1007/s00776-007-1194-2 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for
Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
Cervical myelopathy is caused by spinal canal narrowing
 An Original Study Instrumented Open-Door Laminoplasty as Treatment for Cervical Myelopathy in 104 Patients John R. Dimar II, MD, Kelly R. Bratcher, RN, CCRP, Dylan C. Brock, BS, Steven D. Glassman, MD,
An Original Study Instrumented Open-Door Laminoplasty as Treatment for Cervical Myelopathy in 104 Patients John R. Dimar II, MD, Kelly R. Bratcher, RN, CCRP, Dylan C. Brock, BS, Steven D. Glassman, MD,
Key words: Professional Med J 2018;25(8): CERVICAL LAMINOPLASTY
 The Professional Medical Journal DOI: 10.29309/TPMJ/18.4872 1. MBBS Post graduate Trainee, 2. MBBS, FCPS Associate Professor 3. MBBS, FCPS Associate Professor 4. MBBS Honorary Researcher, 5. MBBS, FCPS
The Professional Medical Journal DOI: 10.29309/TPMJ/18.4872 1. MBBS Post graduate Trainee, 2. MBBS, FCPS Associate Professor 3. MBBS, FCPS Associate Professor 4. MBBS Honorary Researcher, 5. MBBS, FCPS
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty
 Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics
 Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Daniel J. Blizzard, MD, MS
 Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament
 Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament - A Multicenter Retrospective Study - Mitsumasa Hayashida,
Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament - A Multicenter Retrospective Study - Mitsumasa Hayashida,
Skip corpectomy in the treatment of multilevel cervical spondylotic myelopathy and ossified posterior longitudinal ligament
 J Neurosurg Spine 12:33 38, 2010 Skip corpectomy in the treatment of multilevel cervical spondylotic myelopathy and ossified posterior longitudinal ligament Technical note Se d a t Da l bay r a k, M.D.,
J Neurosurg Spine 12:33 38, 2010 Skip corpectomy in the treatment of multilevel cervical spondylotic myelopathy and ossified posterior longitudinal ligament Technical note Se d a t Da l bay r a k, M.D.,
ORIGINAL ARTICLE. Introduction SPINE SURGERY AND RELATED RESEARCH
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Cervical Kyphotic Deformity after Laminoplasty in Patients with Cervical Ossification of Posterior Longitudinal Ligament with Normal Sagittal Spinal
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Cervical Kyphotic Deformity after Laminoplasty in Patients with Cervical Ossification of Posterior Longitudinal Ligament with Normal Sagittal Spinal
Comparative study on the effect of anterior and posterior decompression in the treatment of multi-segmental cervical spondylotic myelopathy
 92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA
 AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
Minamide A*, Yoshida M*, Yamada H*, Hashizume H*, NakagawaY*, Iwasaki H*, Tsutsui S*, Hiroyuki Oka H**.
 Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy
 ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 1 Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy V Kumar,
ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 1 Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy V Kumar,
Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine
 Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures
 Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures Guangdong Chen, MD; Zongping Luo, MD, PhD; Badri Nalajala, MD; Tao Liu, MD, PhD; Huilin Yang, MD, PhD abstract Full article available
Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures Guangdong Chen, MD; Zongping Luo, MD, PhD; Badri Nalajala, MD; Tao Liu, MD, PhD; Huilin Yang, MD, PhD abstract Full article available
Recent Surgical Methods of Double-door Laminoplasty of the Cervical Spine (Kurokawa s Method)
 TECHNICAL NOTE SPINE SURGERY AND RELATED RESEARCH Recent Surgical Methods of Double-door Laminoplasty of the Cervical Spine (Kurokawa s Method) Shigeru Hirabayashi Department of Orthopaedic Surgery, Teikyo
TECHNICAL NOTE SPINE SURGERY AND RELATED RESEARCH Recent Surgical Methods of Double-door Laminoplasty of the Cervical Spine (Kurokawa s Method) Shigeru Hirabayashi Department of Orthopaedic Surgery, Teikyo
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Ossification of the posterior longitudinal ligament
 J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years)
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years) Yoshiharu Kawaguchi 1), Masato Nakano 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years) Yoshiharu Kawaguchi 1), Masato Nakano 1),
Novel Classification System of Cervical Myelopathy Based on Symptomatology
 Research Article imedpub Journals www.imedpub.com Journal of Neurology and Neuroscience DOI: 10.21767/2171-6625.1000277 Novel Classification System of Cervical Myelopathy Based on Symptomatology Hisanori
Research Article imedpub Journals www.imedpub.com Journal of Neurology and Neuroscience DOI: 10.21767/2171-6625.1000277 Novel Classification System of Cervical Myelopathy Based on Symptomatology Hisanori
Cervical Spondylotic Myelopathy Associated With Kyphosis or Sagittal Sigmoid Alignment: Outcome After Anterior or Posterior Decompression
 WScJ 1: 38-46, 2010 Clinical article* Cervical Spondylotic Myelopathy Associated With Kyphosis or Sagittal Sigmoid Alignment: Outcome After Anterior or Posterior Decompression Kenzo Uchida, M.D., Ph.D.,
WScJ 1: 38-46, 2010 Clinical article* Cervical Spondylotic Myelopathy Associated With Kyphosis or Sagittal Sigmoid Alignment: Outcome After Anterior or Posterior Decompression Kenzo Uchida, M.D., Ph.D.,
Assessing the sagittal alignment of the cervical
 See the editorial in this issue, pp 518 520. J Neurosurg Spine 11:521 528, 2009 Cervical spondylotic myelopathy associated with kyphosis or sagittal sigmoid alignment: outcome after anterior or posterior
See the editorial in this issue, pp 518 520. J Neurosurg Spine 11:521 528, 2009 Cervical spondylotic myelopathy associated with kyphosis or sagittal sigmoid alignment: outcome after anterior or posterior
Neurological manifestations of thoracic myelopathy in 203 patients
 Neurological manifestations of thoracic myelopathy in 203 patients Shota Takenaka* a, MD; Takashi Kaito b, MD; Noboru Hosono a, MD; Toshitada Miwa c, MD; Takenori Oda d, MD; Shinya Okuda d, MD; Tomoya
Neurological manifestations of thoracic myelopathy in 203 patients Shota Takenaka* a, MD; Takashi Kaito b, MD; Noboru Hosono a, MD; Toshitada Miwa c, MD; Takenori Oda d, MD; Shinya Okuda d, MD; Tomoya
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Synovial cyst of spinal facet
 Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy. Spine January 1, 2009; Volume 34; Issue 1; pp 82-86
 Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy 1 Spine January 1, 2009; Volume 34; Issue 1; pp 82-86 Yukawa, Yasutsugu; Kato, Fumihiko; Ito, Keigo; Horie, Yumiko; Nakashima,
Ten Second Step Test" as a New Quantifiable Parameter of Cervical Myelopathy 1 Spine January 1, 2009; Volume 34; Issue 1; pp 82-86 Yukawa, Yasutsugu; Kato, Fumihiko; Ito, Keigo; Horie, Yumiko; Nakashima,
CMEARTICLE * * * Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed
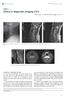 Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion
 Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Misdiagnosis in cervical spondylosis myelopathy.
 Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Abstract Study Design Prospective clinical study.
 812 Technical Report GLOBAL SPINE JOURNAL THIEME Resection of Beak-Type Thoracic Ossification of the Posterior Longitudinal Ligament from a Posterior Approach under Intraoperative Neurophysiological Monitoring
812 Technical Report GLOBAL SPINE JOURNAL THIEME Resection of Beak-Type Thoracic Ossification of the Posterior Longitudinal Ligament from a Posterior Approach under Intraoperative Neurophysiological Monitoring
Narrative Review Cervical Ossified Posterior Longitudinal Ligament
 Narrative Review Cervical Ossified Posterior Longitudinal Ligament Introduction Cervical ossified posterior longitudinal ligament is a common cause of myelopathy. It is frequently encountered in busy spine
Narrative Review Cervical Ossified Posterior Longitudinal Ligament Introduction Cervical ossified posterior longitudinal ligament is a common cause of myelopathy. It is frequently encountered in busy spine
Enlarged anterior cervical diskectomy and fusion in the treatment of severe localised ossification of the posterior longitudinal ligament
 Lei et al. Journal of Orthopaedic Surgery and Research (2016) 11:129 DOI 10.1186/s13018-016-0449-z RESEARCH ARTICLE Open Access Enlarged anterior cervical diskectomy and fusion in the treatment of severe
Lei et al. Journal of Orthopaedic Surgery and Research (2016) 11:129 DOI 10.1186/s13018-016-0449-z RESEARCH ARTICLE Open Access Enlarged anterior cervical diskectomy and fusion in the treatment of severe
ORIGINAL PAPER. Surgical outcomes of decompressive laminoplasty with spinous process osteotomy to treat lumbar spinal stenosis
 Editors Choice ORIGINAL PAPER Nagoya J. Med. Sci. 80. 1 9, 2018 doi:10.18999/nagjms.80.1.1 Surgical outcomes of decompressive laminoplasty with spinous process osteotomy to treat lumbar spinal stenosis
Editors Choice ORIGINAL PAPER Nagoya J. Med. Sci. 80. 1 9, 2018 doi:10.18999/nagjms.80.1.1 Surgical outcomes of decompressive laminoplasty with spinous process osteotomy to treat lumbar spinal stenosis
Appendix: Diagnostic Criteria for OPLL and Diagnosis and Treatment Algorithm
 Appendix: Diagstic Criteria for OPLL and Diagsis and Treatment Algorithm Diagstic Criteria for Ossification of the Posterior Longitudinal Ligament of the Cervical Spine (Proposed by the Committee for Development
Appendix: Diagstic Criteria for OPLL and Diagsis and Treatment Algorithm Diagstic Criteria for Ossification of the Posterior Longitudinal Ligament of the Cervical Spine (Proposed by the Committee for Development
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
ORIGINAL ARTICLE. Introduction SPINE SURGERY AND RELATED RESEARCH
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Radiological Examination of Postoperative Cervical Alignment and Stability in Patients with Dialysis-Associated Spondylosis Excluding Destructive Spondyloarthropathy:
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Radiological Examination of Postoperative Cervical Alignment and Stability in Patients with Dialysis-Associated Spondylosis Excluding Destructive Spondyloarthropathy:
Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates for Cervical Myelopathy
 Original Article Clinics in Orthopedic Surgery 2016;8:399-406 https://doi.org/10.4055/cios.2016.8.4.399 Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates
Original Article Clinics in Orthopedic Surgery 2016;8:399-406 https://doi.org/10.4055/cios.2016.8.4.399 Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates
Thoracic myelopathy secondary to ossification of the spinal ligament
 J Neurosurg 66:11-18, 1987 Thoracic myelopathy secondary to ossification of the spinal ligament KAZUO YONENOBU, M.D., D.Ms., SOHE EBARA, M.D., KEJU FUJWARA, M.D., KAZUO YAMASH TA, M.D., KERO ONO, M.D.,
J Neurosurg 66:11-18, 1987 Thoracic myelopathy secondary to ossification of the spinal ligament KAZUO YONENOBU, M.D., D.Ms., SOHE EBARA, M.D., KEJU FUJWARA, M.D., KAZUO YAMASH TA, M.D., KERO ONO, M.D.,
Case Report Pneumocephalus Associated with Cerebrospinal Fluid Fistula as a Complication of Spinal Surgery: A Case Report
 Case Reports in Medicine Volume 2010, Article ID 328103, 4 pages doi:10.1155/2010/328103 Case Report Pneumocephalus Associated with Cerebrospinal Fluid Fistula as a Complication of Spinal Surgery: A Case
Case Reports in Medicine Volume 2010, Article ID 328103, 4 pages doi:10.1155/2010/328103 Case Report Pneumocephalus Associated with Cerebrospinal Fluid Fistula as a Complication of Spinal Surgery: A Case
Microendoscopic laminotomy versus conventional laminoplasty for cervical spondylotic myelopathy: 5-year follow-up study
 CLINICAL ARTICLE J Neurosurg Spine 27:403 409, 2017 Microendoscopic laminotomy versus conventional laminoplasty for cervical spondylotic myelopathy: 5-year follow-up study Akihito Minamide, MD, PhD, 1
CLINICAL ARTICLE J Neurosurg Spine 27:403 409, 2017 Microendoscopic laminotomy versus conventional laminoplasty for cervical spondylotic myelopathy: 5-year follow-up study Akihito Minamide, MD, PhD, 1
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty
 CASE REPORT SPINE SURGERY AND RELATED RESEARCH Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty Seiichi Odate, Jitsuhiko Shikata and Tsunemitsu
CASE REPORT SPINE SURGERY AND RELATED RESEARCH Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty Seiichi Odate, Jitsuhiko Shikata and Tsunemitsu
En Bloc Cervical Laminoplasty While Preserving the Posterior Structure with Arcocristectomy in Cervical Spondylotic Myelopathy
 DOI: 10.5137/1019-5149.JTN.17440-16.0 Received: 03.03.2016 / Accepted: 05.03.3016 Published Online: 12.08.2016 Original Investigation En Bloc Cervical Laminoplasty While Preserving the Posterior Structure
DOI: 10.5137/1019-5149.JTN.17440-16.0 Received: 03.03.2016 / Accepted: 05.03.3016 Published Online: 12.08.2016 Original Investigation En Bloc Cervical Laminoplasty While Preserving the Posterior Structure
Posterior cervical decompression and fusion for circumferential spondylotic cervical stenosis: Review of 50 consecutive cases
 Journal of Clinical Neuroscience 13 (2006) 23 30 Clinical study Posterior cervical decompression and fusion for circumferential spondylotic cervical stenosis: Review of 50 consecutive cases Lali H.S. Sekhon
Journal of Clinical Neuroscience 13 (2006) 23 30 Clinical study Posterior cervical decompression and fusion for circumferential spondylotic cervical stenosis: Review of 50 consecutive cases Lali H.S. Sekhon
Evaluation of conservative treatment and timing of surgical intervention for mild forms of cervical spondylotic myelopathy
 852 Evaluation of conservative treatment and timing of surgical intervention for mild forms of cervical spondylotic myelopathy LING-DE KONG *, LING-CHEN MENG *, LIN-FENG WANG, YONG SHEN, PAN WANG and ZI-KUN
852 Evaluation of conservative treatment and timing of surgical intervention for mild forms of cervical spondylotic myelopathy LING-DE KONG *, LING-CHEN MENG *, LIN-FENG WANG, YONG SHEN, PAN WANG and ZI-KUN
) ACDF. (Japanese Orthopaedic Association,JOA) ACCF (175.4±12.1ml VS 201.3±80.4ml) ACDF JOA VAS (P=0.000),ACCF :A : X(2015)
 2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion
 Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion SPINE Volume 25, Number 1, pp 41 45 2000, Lippincott Williams & Wilkins, Inc. Jeffrey C. Wang, MD, Paul
Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion SPINE Volume 25, Number 1, pp 41 45 2000, Lippincott Williams & Wilkins, Inc. Jeffrey C. Wang, MD, Paul
Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with and without Instrumentation
 Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
