Re-induction of hyponatremia after rapid overcorrection of hyponatremia reduces mortality in rats
|
|
|
- Noah Hudson
- 6 years ago
- Views:
Transcription
1 original article & 2009 International Society of Nephrology see commentary on page 587 Re-induction of hyponatremia after rapid overcorrection of hyponatremia reduces mortality in rats Fabrice Gankam Kengne 1,2, Alain Soupart 1, Roland Pochet 3, Jean-Pierre Brion 3 and Guy Decaux 1 1 Research Unit for the Study of Hydromineral Metabolism, Faculty of Medicine, Department of General Internal Medicine, Erasme Hospital, Université Libre de Bruxelles, Bruxelles, Belgium; 2 Department of Internal Medicine, University of Texas Southwestern Medical center, Dallas, TX, USA and 3 Laboratory of Histology, Histopathology and Neuroanatomy, Faculty of Medicine, Université Libre de Bruxelles, Bruxelles, Belgium Osmotic demyelination syndrome is a devastating neurologic disorder often seen after the rapid correction of chronic hyponatremia. The permeability of the blood brain barrier is increased in experimental osmotic demyelination, and some have suggested that corticosteroids protect against this disorder by keeping the permeability of the blood brain barrier low. We previously reported that re-lowering of the serum sodium after rapid correction of chronic hyponatremia was beneficial if performed early in the course (12 to 24 h). Here we compared mortality, blood brain barrier permeability, and microglial activation in rats after the rapid correction of chronic hyponatremia. We studied three groups of rats after correction of chronic hyponatremia: and treated them with sodium chloride, with or without dexamethasone; or with sodium chloride followed by re-induction of hyponatremia. We found that treatment with dexamethasone or re-induction of hyponatremia effectively prevented the opening of the blood brain barrier, reduced neurological manifestations, and decreased microglial activation; however, only re-induction of hyponatremia resulted in a significant decrease in mortality 5 days after the correction of chronic hyponatremia. Restoring the permeability of the blood brain barrier to normal levels did not decrease mortality. Our results suggest that after inadvertent rapid correction of hyponatremia, treatment options should favor re-lowering serum sodium. The increased permeability of blood brain barrier seen in osmotic demyelination syndrome may not be a primary pathophysiologic insult of this syndrome. Kidney International (2009) 76, ; doi: /ki ; published online 15 July 2009 KEYWORDS: clinical nephrology; electrolytes; hyponatremia Correspondence: Fabrice Gankam Kengne, Service de Medecine Interne Génerale, Hopital Erasme, 808 Route de Lennik, 1070 Bruxelles, Belgium. fgankamk@ulb.ac.be Received 19 January 2009; revised 5 May 2009; accepted 19 May 2009; published online 15 July 2009 Osmotic demyelination syndrome (ODS) occurs after excessive correction of chronic hyponatremia. 1,2 Histological lesions consist of symmetrical foci of demyelination, with activated microglia infiltration in different regions of the brain. 1,2 The physiopathology of this condition is poorly understood, and as a result, very few interventions have been reported to be beneficial in ODS. 3,4 The development of ODS lesions probably involves complex interactions among blood brain barrier (BBB), brain organic osmolyte fluxes, microglia, and inflammatory cytokines. 4 The permeability of BBB in experimental ODS has been previously investigated and some have postulated that the opening of the BBB, provoked by a rapid correction of chronic hyponatremia, could result in the exposure of the brain to myelinolytic substances and subsequently induce ODS lesions. 5 7 It has recently been suggested that the administration of corticosteroids, such as dexamethasone (DXM), in an animal model of ODS could be beneficial by preventing the opening of BBB. 8 However, the facts that there is an opening of BBB in experimental ODS, that most animals with an open BBB after a rapid correction of hyponatremia will develop ODS, and finally that DEX could be efficacious in ODS because it protects against the opening of BBB, do not necessarily imply that an increase in the permeability of BBB is the initial and priming pathogenic phenomenon in this disorder. In fact, the exact role of this increase in the permeability of BBB is still debatable, as it could either represent the initial and crucial insult or simply a surrogate, secondary marker in the course of the ODS; studies addressing the relationship between BBB permeability and ODS have not fully clarified this issue. Furthermore, the net extent of protection conferred by DXM is controversial Owing to the complex and mostly unknown nature of the phenomenon that induces demyelinative lesions after rapid correction of hyponatremia, few treatment options are available, and there is no consensus on the appropriate treatment strategy in ODS. Our group previously reported a benefit in mortality and neurological manifestations due to ODS, after a re-induction of hyponatremia up to 24 h after 614 Kidney International (2009) 76,
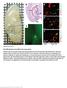
2 F Gankam Kengne et al.: Re-induction of hyponatremia after rapid overcorrection of hyponatremia original article the initial correction in asymptomatic and pauci-symptomatic rats; 12,13 the mechanisms underlying the beneficial effect of serum sodium (SNa) re-lowering are poorly understood and the action of this rescue treatment on BBB and microglial activation has never been investigated. In this work, we aimed at comparing DXM administration and hyponatremia re-induction as preventive treatment options in ODS. We further investigated BBB permeability and microglial activation under both treatments in an attempt to clarify the role of these two components in the pathophysiology of ODS. RESULTS SNa values before and after correction of hyponatremia We used a previously described animal model of ODS (See Figure 1 for experimental protocol). 8,14,15 Along with others, we previously reported that a correction of hyponatremia with a 24-h SNa gradient 425 meq/l was associated with a high incidence of neurological damage. 15 Therefore, to avoid potential bias in survival because of inadequate correction gradient, only rats that had severe hyponatremia (SNa o120 meq/l) and that achieved an SNa gradient X25 meq/l were included in the analysis. Table 1 shows the SNa values in the three groups before and after correction. SNa levels at day 4 were comparable in all groups. In Group 3, the SNa gradient was re-lowered to a mean value of 14 meq/l at the twenty-fourth hour, after a mean gradient of 29 meq/l at the twelth hour. Neurological manifestations and mortality after correction of hyponatremia Table 1 summarizes the outcome of the animals at day 5 (24 h after correction) and at day 10 (5 days after correction). At 24 h after correction of SNa, all rats became severely symptomatic in Group 1; in Group 2, 50% of the animals (8/16) were symptomatic; and in Group 3, only one animal showed neurological signs. DXM administration resulted in a significant reduction in neurological manifestations (P ¼ 0.01). However, animals treated with a re-induction of hyponatremia showed a better clinical status. (P ¼ 0.01, Group 2 vs Group 3) By day 10 of the experiment, all the rats treated with hypertonic saline alone died (two rats were killed at day 7 because they were moribund). Only 3 of 16 rats treated with DXM survived (P ¼ 0.17 for DXM vs NaCl alone), and 15 of 16 rats survived in the group treated with SNa re-lowering. (Po0.001 for SNa re-lowering vs NaCl alone and vs DXM). Figure 2 shows the luxol fast blue staining of myelin in the animals of each group. IgG immunostaining The extent and localization of BBB leakiness in the different groups were analyzed on brain sections immunolabeled for rat IgG. Representative microphotographs of IgG immunostaining carried out on brain slices are shown in Figure 3. In animals treated with DXM or with a re-induction of hyponatremia, only a faint immunostaining for IgG was present around the blood vessels, whereas brain sections of animals corrected with NaCl alone (Figure 3b) showed a massive immunostaining for IgG. BBB permeability Blood brain barrier permeability was quantitatively assessed by Evans blue (EB) dye extravasation (Figure 4), as previously described. 16 The SNa values of the animals used for the EB dye experiment are given in Table 2. As shown in Figure 4, Day 0 Induction of hypona Day 4 Correction of hypona induction of ODS Day 5 Final gradient symptoms analysis Day 10 Mortality analysis Group 1 : n = 12 4 days 5 days Group 2 : n = 16 DXM (2 mg/kg): 0 h 6 h Re-lowering of SNa Group 3 : n = 16 Figure 1 Schematic representation of the experimental protocol used. Hyponatremia was induced by a combination of DDAVP infusion and liquid diet, and was maintained for 4 days. Correction was carried out using intraperitoneal hypertonic NaCl. Rats were allowed to consume food at day 5 after blood sampling and to consume water at day 6. In Group 2, dexamethasone (DXM) was administered 0 and 6 h after correction, whereas in Group 3, serum sodium was re-lowered 12 h after correction. Symptoms and mortality were recorded 1 and 5 days (day 5 and 10, respectively) after correction of hyponatremia in the three groups. HypoNa, hyponatremia; ODS, osmotic demyelination syndrome; SNa, serum sodium. 12 h Kidney International (2009) 76,
3 original article F Gankam Kengne et al.: Re-induction of hyponatremia after rapid overcorrection of hyponatremia Table 1 Serum sodium values (SNas) and clinical data in the three groups of rats measured before (day 4) and after (12 or 24 h) treatment, in the experiment addressing mortality Group 1 NaCl alone (n = 12) Group 2 NaCl+DXM (n = 16) Group 3 NaCl+SNa re-lowering (n = 16) SNa at day 4 (meq/l) 108±2* 107±1* 104±2* SNa 12 h after correction 133±2*,w SNa at 24 h 137±2*,w 136±1*,w 117±2 d-sna at 12 h 29±1* d-sna at 24 h 29±1* 29±1* 14±1 Neurological manifestations at day 5 12/12 8/16 z 1/16 z Mortality at day 10 12/12 13/16 y 1/16 y ANOVA, analysis of variance; DXM, dexamethasone; NaCl, hypertonic NaCl. Data are presented as means±s.e.m. *P = NS between the three groups. w Po 0.01 compared with SNa before the correction (day 4). z P values: Group 1 vs Group 2, o0.01; Group 3 vs Group 2, o0.01; Group 3 vs Group 1, o y P values: Group 1 vs Group 2, NS; Group 3 vs Group 2, o0.001; Group 3 vs Group 1, o w 2 -test and one-way ANOVA were used for statistical analysis. Immunostaining for microglial activation Representative microphotographs of activated microglia immunostaining are shown in Figure 5. We confirmed the intense immunostaining observed in rats corrected with NaCl alone, mostly in the hippocampus, basal ganglia, and deep cortical areas (Figure 5b). In rats treated with DXM (Figure 5c) or with a re-induction of hyponatremia (Figure 5d), moderate immunostaining for activated microglia was also observed. Figure 2 Myelin staining (Luxol Fast Blue/Cresyl Violet). Representative microphotographs of brain sections stained with Luxol Fast Blue and Cresyl Violet for myelin. (a) Rats treated with dexamethasone (2 mg/kg body weight) at 0 and 6 h after the correction. (b) Rats treated with re-induction of hyponatremia. Rats treated with hypertonic saline alone (c) showed massive cortical demyelinative lesions (arrows), characterized as zone of pallor in the deep cortex, compared with uncorrected controls (d). (a and d) At 5 days after correction of chronic hyponatremia. (c) At 3 days after correction of chronic hyponatremia. Bar ¼ 200 mm. CC: corpus callosum. BBB permeability was increased in rats as early as 12 h after correction compared with that in uncorrected rats (Po0.001), and this increased permeability persisted for 24 h after correction. Treatment with DXM or SNa relowering resulted in a significant decrease in BBB permeability 12 h after correction. At 24 h after correction, treatments with DXM and re-induction of hyponatremia had the same protective effect on BBB permeability (Po0.01 compared with rats treated with NaCl alone, P ¼ NS compared with uncorrected control rats). DISCUSSION In these experiments, we found that, compared with rats treated with NaCl alone, rats treated with DXM presented less neurological manifestations 24 h after correction of chronic hyponatremia, but DXM failed to reduce the mortality at 5 days; on the contrary, re-lowering of SNa was efficacious in both reducing neurological manifestations and mortality. We further investigated the opening of BBB and microglial activation with the same treatments. We confirmed the previous findings with regard to the increase in BBB permeability and the protective effect of DXM on that increase (5, 7, 8, and 9). This study also suggests for the first time that a decrease in the permeability of BBB is associated with SNa re-lowering after an inadvertent correction of hyponatremia. As previously suggested, 17 we found that microglial activation occurs after correction of chronic hyponatremia with hypertonic saline alone in the rat model of ODS. This study shows two important points: first of all, our results suggest that re-induction of hyponatremia is more efficient than DXM in the prevention of myelinolysis. This finding has an obvious clinical importance. Previous papers have reported a beneficial effect of corticosteroids in experimental osmotic demyelination 8 11 syndrome and isolated cases reported have echoed these experimental findings. 18 In our study, however, although we confirmed an early protection of DXM from neurological manifestations of ODS, we showed, with a larger series of animals, that DXM does not significantly impact mortality in this experimental 616 Kidney International (2009) 76,
4 F Gankam Kengne et al.: Re-induction of hyponatremia after rapid overcorrection of hyponatremia original article NaCl + DXM NaCl + re-induction of hyponatremia NaCl alone Control Figure 3 Immunoreactivity for IgG in brain of rats of the four different groups. There is a significant increase in IgG reactivity in the cortical and subcortical areas, and in the basal ganglia of rats treated with NaCl alone (arrows) compared with that in all other groups (24 h after correction). DXM, dexamethasone. 4 * EB (µg/gr brain tissue) * 0 Group 4 Uncorrected control Group 1 NACl alone Group 2 NACl + DXM Group 4 Uncorrected control Group 1 NACl alone Group 2 NACl + DXM Group 3 NACl + SNa re 12 h after the correction 24 h after the correction Figure 4 Effect of the different treatments on blood brain barrier (BBB) permeability after rapid correction of hyponatremia. *Po0.01 in Group 1 vs Group 4 (uncorrected controls), and Po0.01 in Group 1 vs Group 2 (rats treated with NaCl alone and NaCl/DXM, respectively) and Group 3 (treated with NaCl and re-induction of hyponatremia), both 12 and 24 h after correction of serum sodium (SNa). P ¼ NS between groups 2, 3, and 4, 12 and 24 h after correction. One-way analysis of variance, followed by Bonferroni LSD, was used for statistical analysis. BBB permeability was quantified using the Evans blue dye method 24 h after correction. Values are mean and s.e.m. (n ¼ 5 6 in each group). There is a striking increase in BBB permeability after rapid correction of hyponatremia. Treatment with DXM or SNa re-lowering resulted in a decrease in the permeability of BBB. DXM, dexamethasone; SNa re k, serum sodium re-lowering. model. In contrast, SNa re-lowering was effective in protecting from both neurological manifestations and death in the animal model of ODS. These later findings are in accordance with our previous experiments, 12,13 and support recent clinical evidence of the protective role of re-induction of hyponatremia in the prevention of ODS in humans Our experiments suggest that the efficacy of DXM in terms of mortality should be considered with caution and that early re-induction of hyponatremia is to be preferred if the patient has been submitted to extensive correction of hyponatremia. Kidney International (2009) 76,
5 original article F Gankam Kengne et al.: Re-induction of hyponatremia after rapid overcorrection of hyponatremia Table 2 Serum sodium values (SNa) in the groups of rats used for EB analysis (data are presented as mean±s.e.m.) 12 h After the correction of SNa 24 h After the correction of SNa Controls Group 1: NaCl alone (n =6) Group 2: NaCl+DXM (n =6) Group 1: NaCl alone (n =5) Group 2: NaCl+DXM (n =5) Group 3: NaCl+SNa re-lowering (n = 5) Group 4: uncorrected controls (n =6) SNa at day 0 (meq/l) 106±1 104±1 102±2 104±2 102±2 104±1 SNa 12 h after correction 135±4 135±2 131±1 SNa at 24 h 133±2 134±1 106±1 d-sna at 12 h 30±2 31±2 29±2 d-sna at 24 h 31±2 30±2 4±2 DXM, dexamethasone; EB, Evans blue stain. P = NS for SNa at day 4 between all groups; P = NS for SNa and dsna at 12 h between all the compared groups; P = NS for SNa and dsna at 24 h between Group 1 and Group 2; Po0.001 for SNa at 24 h between Group 3 and Groups 1 and 2. Figure 5 Immunostaining for microglial activation. Representative microphotograph of activated microglia in the hippocampus of rats of the four different groups. (a) Uncorrected controls. Massive immunoreactivity was observed in rats treated with NaCl alone (b), in rats treated with dexamethasone (DXM) (c), and in those treated with re-induction of hyponatremia (d). On the right, a higher magnification of the hippocampus of a rat treated with NaCl alone (e). Bar ¼ 200 mm. Some differences in experimental design and methodology may account for the discordance between our results and those of previously published experiments. In these reports, particularly worrisome have been the end points studied, the SNa gradient of animals included in the analysis, and the sample size. The other experiments 9 11 mostly addressed the number or severity of lesions in the DXMtreated group compared with that in the control group: some reported 10,11 a decrease in the number of demyelinative lesions in rats treated with corticosteroids or in those that are repeatedly tail transected compared with that in rats treated with hypertonic saline alone, with no significant difference in the number of affected animals (7 of 10 in tail transected and 8 of 10 in steroid treated vs 10 of 10 in control group). Compared with previous papers, we used a larger number of rats (n ¼ 12 16) and we included in the analysis only rats with a large increase of SNa (d-snax25 meq/l/day). By choosing this set point of SNa gradient, we were more likely to disclose any beneficial effect on mortality after treatment with either DXM or hyponatremia re-induction, as such a gradient is invariably associated with a high incidence of neurological manifestations and death. 15 In the previous studies addressing this issue, animals had an SNa gradient of o25 meq/l/day, which could explain the lower mortality rate usually found and a possible overestimation of the protective role of DXM. The second key conclusion from our results is regarding the role of BBB in ODS pathophysiology. Some have hypothesized that the opening of BBB could allow the passage of large blood-borne molecules (IgG and complement) that could damage oligodendrocytes and induce demyelination. 5,6 In other animal models, as well as in in vitro studies, osmotic opening of the BBB has been shown to be involved in the transient modifications of cellular cytoskeletal architecture, leading to a shrinkage of tight junctions of endothelial cells These changes have been related to both the intensity and duration of the osmotic stimulus and involve some proteins of the tight junction complex, such as ZO 1, occluding, and claudin In parallel, various inflammatory stimuli (cytokines and nitric oxide) are known to regulate the permeability of BBB. 26 Some of these inflammatory cytokines are shown to be present in ODS. 17 Taking into account the results of previous experiments, we can hypothesize that the increase in the permeability of BBB in ODS might involve two distinct but overlapping components: one early, reversible osmotic 618 Kidney International (2009) 76,
6 F Gankam Kengne et al.: Re-induction of hyponatremia after rapid overcorrection of hyponatremia original article component mediated by rapid changes in plasma tonicity with the resultant mechanical shrinking of tight junctions of the BBB and a late inflammatory component mediated by the secretion of proinflammatory cytokines after propagation of the osmotic insult. The effect of DXM on BBB has been well characterized in both in vivo and in vitro studies, and DXM has been shown to modulate the changes in tight junctional proteins and other components involved in the regulation of BBB physiology with, as net effect, an increase in the stability of BBB. 27,28 Regarding the re-lowering of SNa, we showed that the permeability of BBB returned to near normal values after the re-induction of hyponatremia; it is likely that the withdrawal of the osmotic insult (by re-induction of hyponatremia) acts on BBB by limiting the consequences of the inflammatory processes triggered by a sustained osmotic stress. Dexamethasone, to a similar extent as SNa re-lowering, prevented the opening of the BBB observed after rapid correction of SNa, but did not significantly affect mortality. This suggests that the opening of the BBB component in ODS is distinct from the initial demyelinative injury. The hypothesis of the marginal contribution of the opening of the BBB as the initial insult causing ODS is further supported by other observations: first, the osmotic opening of BBB has been extensively studied in the clinical setting and has been shown to be transient, 24,25,29 whereas all papers studying this topic with respect to ODS reported a long-lasting opening of the BBB, suggesting that the increased permeability of BBB after 24 h is not related to a mechanical osmotic phenomenon. Second, although lovastatin has been shown to decrease the permeability of BBB in various experimental settings, it has failed to show a significant efficacy in ODS. 17 Third, an increase in the permeability of BBB has been well characterized in other models of neurological injury; yet, such a specific pattern of demyelination does not occur. These facts, when associated with the results of our experiments, strongly imply that the opening of BBB could count as a surrogate marker in ODS resulting from the inflammatory milieu, which is distinct from the priming insult. We showed that rats could still develop ODS and die of it, despite a closed BBB. However, neither our study nor the previous one could fully decipher the exact role of BBB in this disorder, and other experimental approaches are needed to understand how the increased permeability of BBB observed in ODS could be implicated in the complex pathophysiology of this disorder. In summary, although corticosteroids could decrease the permeability of BBB and the neurological symptoms after rapid correction of hyponatremia, this treatment does not result in an increase in the overall survival rate in an experimental model, suggesting that BBB permeability is rather a surrogate marker of secondary phenomenon than initial insult after rapid correction of chronic hyponatremia. Our results are not readily transposable to human practice, and it is important to stress on the fact that the two treatment strategies compared in this study are clinically different, because re-induction of SNa is a rescue maneuver, whereas administration of DXM is strictly preventive. Therefore, both the treatments can be combined for maximal efficacy. Nevertheless, these experiments stress on the fact that re-induction of hyponatremia is an efficacious treatment option after an inadvertent correction of chronic hyponatremia. Our experiments further show how complex the pathophysiology of ODS is. Besides SNa re-lowering, the only interventions that resulted in such a striking reduction in mortality after rapid correction of chronic hyponatremia were myoinositol 30 administration and exogenous or endogenous uremia. 31,32 All these treatments affected the organic osmolyte content of the brain. Indeed, important variations in the organic osmolyte content in the brain have been shown in chronic hyponatremia. 33,34 These imbalances in the buffering potential of the cell could further lead to a poor response to a rapid increase in the tonicity of extracellular space, which could in turn trigger a cellular lesion in oligodendrocytes with secondary inflammation, finally leading to demyelination. MATERIAL AND METHODS Animals Male Wistar rats ( g) were used for all the experiments. The animals were housed in individual cages under conditions of constant temperature (23 1C) and a 12-h/12-h light/dark cycle. They were allowed to adapt for 3 4 days and were fed with standard pelleted chow with ad libitum access to water before the beginning of the experiments. All procedures were performed in accordance with guidelines for animal care at Université Libre de Bruxelles. Induction of hyponatremia In all animals, hyponatremia was induced by previously described methods. 8,14 In brief, an osmotic minipump (Model 2001 Alzet, Palo alto, CA, USA) was filled with desmopressin acetate (0.4 mg/ml) (Ferring, Sweden) and inserted into the back of the animal, which was administered light halothane anesthesia at the beginning of the experiment (Day 0). On the day of the insertion, rats were switched to a liquid diet with a low sodium content (AIN 76, Technilab BMI, Someren, Netherlands). The liquid diet was maintained for a total of 4 days. Correction of hyponatremia After 4 days of liquid feeding (day 4 of the experiment), hyponatremia was rapidly corrected by administration of NaCl 1 M (2 ml/100 g body weight) intraperitoneally in a single dose. Desmopressin infusion was maintained all through the experiment. Pelleted chow was given to the animals on day 5 of the experiment, after blood sampling, for the determination of final 24-h SNa and to avoid incidental re-lowering occurring at day 5; water was given only on day 6. Kidney International (2009) 76,
7 original article F Gankam Kengne et al.: Re-induction of hyponatremia after rapid overcorrection of hyponatremia Blood measurements Blood samples (0.3 ml) were collected by tail transection at days 0 and 1 after administering light anesthesia, for SNa analysis. Electrolyte measurements were determined using MODULAR p800 (Roche Diagnostics, Vilvoorde, Belgium). Evaluation of neurological manifestations and mortality In a first set of experiments (Figure 1), we addressed the effect of DXM and SNa re-lowering in rats after rapid correction of chronic hyponatremia in terms of neurological manifestations and mortality. In these experiments, a total of 44 rats were randomly assigned to three groups depending on the treatment regimen. All groups were studied concurrently. Group 1 (n ¼ 12) consisted of hyponatremic rats, the SNa of which was rapidly corrected with hypertonic saline without further treatment. Group 2 (n ¼ 16) consisted of the DXM-treated group. DXM (Aacidexam, Organon, Brussels, Belgium) was administered subcutaneously at a dose of 2 mg/kg body weight at the time of correction of hyponatremia and 6 h later. This administration scheme has been previously reported to be the most protective in this setting. 8 Group 3 (n ¼ 16) consisted of hyponatremic rats corrected with hypertonic saline, followed by re-induction of hyponatremia 12 h later in asymptomatic rat. Blood samples were taken for serum analysis, and only rats that achieved an SNa gradient of correction X25 meq/l were treated with re-induction of hyponatremia. Hyponatremia was re-induced by an intraperitoneal administration of water (10% of body weight) to achieve a final SNa gradient p20 meq/l over 24 h. 12,13 Groups 1 and 2 included only rats with a 24-h SNa gradient X25 meq/l. This value of SNa gradient has been previously shown to be inevitably associated with brain demyelinative lesions in animals corrected with NaCl alone. 15 Animals were observed for neurological manifestations of ODS 1 day and 5 days after correction of hyponatremia. Rats were considered symptomatic if they showed one of the following: slow or awkward gait, limb weakness and/or paralysis, seizures, severe motor deficits, or a complete inability to move. Immunohistochemistry Animals were killed if they were found to be moribund in their cages; otherwise, all surviving animals at day 10 of the experiment (5 days after correction of chronic hyponatremia) were killed by decapitation. Brain was divided into two hemispheres and was fixed overnight in formalin (10%) before rinsing with phosphate-buffered saline. Specimens were then embedded in paraffin and cut into sagittal sections of 7 mm thickness using a microtome. Immunohistochemical detection of IgG was performed on rat brain sections, as previously described. 5 After deparaffination and rehydration of tissue sections, endogenous peroxidases were blocked (0.3% H 2 O 2 in methanol) and non-specific binding of the antibody was inhibited using appropriate species normal serum at 1/10 ratio. Slides were then incubated with a biotinylated goat anti-rat IgG antibody (1:100; Vector, Burlingame, CA, USA) for 3 h, followed by avidin biotin peroxidase (Vector Labs, Labconsult, Brussels, Belgium) and diaminobenzidine (Dako, Heverlee, Belgium). Immunohistochemistry for activated microglia was performed using a mouse anti-ed1 antibody 16 (1/200, Serotec, Dusseldorf, Germany), followed by a biotinylated horse antimouse antibody (1:100; Vector). Evaluation of BBB by EB dye extravasation In a second set of experiments, EB was used to determine BBB permeability at 12 and 24 h after correction of hyponatremia in the different groups studied, as well as in one group of uncorrected hyponatremic rats serving as controls (Group 4). In each animal, EB solution (Sigma Chemical, St Louis, MO, USA) (2% in saline; 3 ml/kg) was injected intravenously 24 h after rapid correction of chronic hyponatremia and was allowed to circulate for 40 min. The chest was subsequently opened and the brain was transcardially perfused with 100 ml of saline through the left ventricle at 100-mm Hg pressure until an almost colorless perfusion fluid was obtained from the right atrium. Brains were then weighed and placed in 50% trichloroacetic acid solution. After homogenization and centrifugation, 16 the absorbance of the supernatant was analyzed spectrophotometrically at 610 nm and the content of EB, expressed per gram of brain tissue, was calculated using a linear standard curve derived from known amounts of dye. Statistical analysis Results were expressed as mean±s.e.m. The Mann Whitney nonparametric test, Fischer s exact test on proportions, and one-way analysis of variance followed by Bonferroni s LSD were used when appropriate. P values o0.05 were considered to be significant. DISCLOSURE All the authors declared no competing interests. ACKNOWLEDGMENTS We thank Charles Nicaise and Michelle Authelet for their helpful technical assistance. This study was supported by a grant from the Fonds National de la Recherche Scientifique, conventions and , by a grant from foundation Erasme and by a grant from the Belgian PAI/IAP P6/43. Part of this work was presented at the ASN annual meeting November 2008 and at the annual meeting of the Belgian Society of Internal Medicine December REFERENCES 1. Kleinschmidt-DeMasters BK, Norenberg MD. Rapid correction of hyponatremia causes demyelination: relation to central pontine myelinolysis. Science 1981; 211: Kleinschmidt-DeMasters BK, Norenberg MD. Neuropathologic observations in electrolyte-induced myelinolysis in the rat. J Neuropathol Exp Neurol 1982; 41: Kleinschmidt-Demasters BK, Rojiani AM, Filley CM. Central and extrapontine myelinolysis: then and now. J Neuropathol Exp Neurol 2006; 65: Murase T, Sugimura Y, Takefuji S et al. Mechanisms and therapy of osmotic demyelination. Am J Med 2006; 119(7 Suppl 1): S69 S Baker EA, Tian Y, Adler S et al. Blood-brain barrier disruption and complement activation in the brain following rapid correction of chronic hyponatremia. Exp Neurol 2000; 165: Kidney International (2009) 76,
8 F Gankam Kengne et al.: Re-induction of hyponatremia after rapid overcorrection of hyponatremia original article 6. Adler S, Martinez J, Williams DS et al. Positive association between blood brain barrier disruption and osmotically-induced demyelination. Mult Scler 2000; 6: Adler S, Verbalis JG, Williams D. Effect of rapid correction of hyponatremia on the blood-brain barrier of rats. Brain Res 1995; 679: Sugimura Y, Murase T, Takefuji S et al. Protective effect of dexamethasone on osmotic-induced demyelination in rats. Exp Neurol 2005; 192: Ke QH, Liang TB, Yu J et al. A study of the pathogenesis and prevention of central pontine myelinolysis in a rat model. J Int Med Res 2006; 34: Oh MS, Choi KC, Uribarri J et al. Prevention of myelinolysis in rats by DXM or colchicine. Am J Nephrol 1990; 10: Rojiani AM, Prineas JW, Cho ES. Protective effect of steroids in electrolyteinduced demyelination. J Neuropathol Exp Neurol 1987; 46: Soupart A, Penninckx R, Stenuit A et al. Re-induction of hyponatremia improves survival in rats with myelinolysis-related neurologic symptoms. J Neuropathol Exp Neurol 1996; 55: Soupart A, Penninckx R, Crenier L et al. Prevention of brain demyelination in rats after excessive correction of chronic hyponatremia by serum sodium lowering. Kidney Int 1994; 45: Verbalis JG, Drutarosky MD. Adaptation to chronic hypoosmolality in rats. Kidney Int 1988; 34: Soupart A, Stenuit A, Perier O et al. Limits of brain tolerance to daily increments in serum sodium in chronically hyponatraemic rats treated with hypertonic saline or urea: advantages of urea. Clin Sci (Lond) 1991; 80: Uyama O, Okamura N, Yanase M et al. Quantitative evaluation of vascular permeability in the gerbil brain after transient ischemia using Evans blue fluorescence. J Cereb Blood Flow Metab 1988; 8: Takefuji S, Murase T, Sugimura Y et al. Role of microglia in the pathogenesis of osmotic-induced demyelination. Exp Neurol 2007; 204: Takei Y, Akahane C, Ikeda S. Osmotic demyelination syndrome: reversible MRI findings in bilateral cortical lesions. Intern Med 2003; 42: Soupart A, Ngassa M, Decaux G. Therapeutic relowering of the serum sodium in a patient after excessive correction of hyponatremia. Clin Nephrol 1999; 51: Oya S, Tsutsumi K, Ueki K et al. Reinduction of hyponatremia to treat central pontine myelinolysis. Neurology 2001; 57: Perianayagam A, Sterns RH, Silver SM et al. DDAVP is effective in preventing and reversing inadvertent overcorrection of hyponatremia. Clin J Am Soc Nephrol 2008; 3: Lu TS, Chen HW, Huang MH et al. Heat shock treatment protects osmotic stress-induced dysfunction of the blood-brain barrier through preservation of tight junction proteins. Cell Stress Chaperones 2004; 9: Dobrogowska DH, Vorbrodt AW. Immunogold localization of tight junctional proteins in normal and osmotically-affected rat blood-brain barrier. J Mol Histol 2004; 35: Rapoport SI. Osmotic opening of the blood-brain barrier. Ann Neurol 1988; 24: Rapoport SI, Fredericks WR, Ohno K et al. Quantitative aspects of reversible osmotic opening of the blood-brain barrier. Am J Physiol 1980; 238: R421 R Chavarria A, Alcocer-Varela J. Is damage in central nervous system due to inflammation? Autoimmun Rev 2004; 3: Romero IA, Radewicz K, Jubin E et al. Changes in cytoskeletal and tight junctional proteins correlate with decreased permeability induced by dexamethasone in cultured rat brain endothelial cells. Neurosci Lett 2003; 344: Frequin ST, Barkhof F, Lamers KJ et al. The effects of high-dose methylprednisolone on gadolinium-enhanced magnetic resonance imaging and cerebrospinal fluid measurements in multiple sclerosis. J Neuroimmunol 1992; 40: Zünkeler B, Carson RE, Olson J et al. Hyperosmolar blood-brain barrier disruption in baboons: an in vivo study using positron emission tomography and rubidium-82. J Neurosurg 1996; 84: Silver SM, Schroeder BM, Sterns RH et al. Myoinositol administration improves survival and reduces myelinolysis after rapid correction of chronic hyponatremia in rats. J Neuropathol Exp Neurol 2006; 65: Soupart A, Schroëder B, Decaux G. Treatment of hyponatraemia by urea decreases risks of brain complications in rats. Brain osmolyte contents analysis. Nephrol Dial Transplant 2007; 22: Soupart A, Silver S, Schroöeder B et al. Rapid (24-h) reaccumulation of brain organic osmolytes (particularly myo-inositol) in azotemic rats after correction of chronic hyponatremia. J Am Soc Nephrol 2002; 13: Lien YH, Shapiro JI, Chan L. Study of brain electrolytes and organic osmolytes during correction of chronic hyponatremia. Implications for the pathogenesis of central pontine myelinolysis. J Clin Invest 1991; 88: Verbalis JG, Gullans SR. Rapid correction of hyponatremia produces differential effects on brain osmolyte and electrolyte reaccumulation in rats. Brain Res 1993; 606: Kidney International (2009) 76,
Brain Volume Regulation in Response to Hypo-osmolality and Its Correction
 The American Journal of Medicine (2006) Vol 119 (7A), S12 S16 Brain Volume Regulation in Response to Hypo-osmolality and Its Correction Richard H. Sterns, MD,* and Stephen M. Silver, MD Department of Medicine,
The American Journal of Medicine (2006) Vol 119 (7A), S12 S16 Brain Volume Regulation in Response to Hypo-osmolality and Its Correction Richard H. Sterns, MD,* and Stephen M. Silver, MD Department of Medicine,
Workshop CME 22 mars Pr Alain SOUPART Service de Médecine Interne Général Cliniques Universitaires Erasme, Bruxelles
 Workshop CME 22 mars 2013 Pr Alain SOUPART Service de Médecine Interne Général Cliniques Universitaires Erasme, Bruxelles Overcorrection of chronic hyponatremia CASE REPORT I (1) Female 71 year Altered
Workshop CME 22 mars 2013 Pr Alain SOUPART Service de Médecine Interne Général Cliniques Universitaires Erasme, Bruxelles Overcorrection of chronic hyponatremia CASE REPORT I (1) Female 71 year Altered
Prevention of brain demyelination in rats after excessive correction of chronic hyponatremia by serum sodium lowering
 Kidney International, Vol. 45 (1994), pp. 193 200 Prevention of brain demyelination in rats after excessive correction of chronic hyponatremia by serum sodium lowering ALAIN SOUPART, RAYMOND PENNINCKX,
Kidney International, Vol. 45 (1994), pp. 193 200 Prevention of brain demyelination in rats after excessive correction of chronic hyponatremia by serum sodium lowering ALAIN SOUPART, RAYMOND PENNINCKX,
Title:Plasma Exchange Successfully Treats Central Pontine Myelinolysis after Acute Hypernatremia from Intravenous Sodium Bicarbonate Therapy
 Author's response to reviews Title:Plasma Exchange Successfully Treats Central Pontine Myelinolysis after Acute Hypernatremia from Intravenous Sodium Bicarbonate Therapy Authors: Kyung Yoon Chang (cky81@lycos.co.kr)
Author's response to reviews Title:Plasma Exchange Successfully Treats Central Pontine Myelinolysis after Acute Hypernatremia from Intravenous Sodium Bicarbonate Therapy Authors: Kyung Yoon Chang (cky81@lycos.co.kr)
Minocycline Protects against Neurologic Complications of Rapid Correction of Hyponatremia
 SI RESERH Minocycline Protects against Neurologic omplications of Rapid orrection of Hyponatremia Fabrice Gankam-Kengne, lain Soupart, Roland Pochet, Jean Pierre rion, and Guy Decaux Research Unit on Hydromineral
SI RESERH Minocycline Protects against Neurologic omplications of Rapid orrection of Hyponatremia Fabrice Gankam-Kengne, lain Soupart, Roland Pochet, Jean Pierre rion, and Guy Decaux Research Unit on Hydromineral
CASE REPORT. Introduction. Case Report. Hiroshi Ochiai and Eita Uenishi
 doi: 10.2169/internalmedicine.0299-17 http://internmed.jp CASE REPORT Early Relowering of Serum Sodium Concentration Overcomes Disturbances in Consciousness during Hyponatremia Overcorrection and Prevents
doi: 10.2169/internalmedicine.0299-17 http://internmed.jp CASE REPORT Early Relowering of Serum Sodium Concentration Overcomes Disturbances in Consciousness during Hyponatremia Overcorrection and Prevents
Overcorrection of chronic hyponatremia can cause major
 DDAVP Is Effective in Preventing and Reversing Inadvertent Overcorrection of Hyponatremia Anjana Perianayagam,* Richard H. Sterns,* Stephen M. Silver,* Marvin Grieff,* Robert Mayo,* John Hix,* Ruth Kouides*
DDAVP Is Effective in Preventing and Reversing Inadvertent Overcorrection of Hyponatremia Anjana Perianayagam,* Richard H. Sterns,* Stephen M. Silver,* Marvin Grieff,* Robert Mayo,* John Hix,* Ruth Kouides*
Rapid (24-Hour) Reaccumulation of Brain Organic Osmolytes (Particularly myo-inositol) in Azotemic Rats after Correction of Chronic Hyponatremia
 J Am Soc Nephrol 13: 1433 1441, 2002 Rapid (24-Hour) Reaccumulation of Brain Organic Osmolytes (Particularly myo-inositol) in Azotemic Rats after Correction of Chronic Hyponatremia ALAIN SOUPART,* STEPHEN
J Am Soc Nephrol 13: 1433 1441, 2002 Rapid (24-Hour) Reaccumulation of Brain Organic Osmolytes (Particularly myo-inositol) in Azotemic Rats after Correction of Chronic Hyponatremia ALAIN SOUPART,* STEPHEN
Desmopressin to Prevent Rapid Sodium Correction in Severe Hyponatremia: A Systematic Review
 CLINICAL RESEARCH STUDY Desmopressin to Prevent Rapid Sodium Correction in Severe Hyponatremia: A Systematic Review Thomas E. MacMillan, MD, MSc a Terence Tang, MD b,c Rodrigo B. Cavalcanti, MD, MSc a,b
CLINICAL RESEARCH STUDY Desmopressin to Prevent Rapid Sodium Correction in Severe Hyponatremia: A Systematic Review Thomas E. MacMillan, MD, MSc a Terence Tang, MD b,c Rodrigo B. Cavalcanti, MD, MSc a,b
Supplementary Figure 1
 Supplementary Figure 1 The average sigmoid parametric curves of capillary dilation time courses and average time to 50% peak capillary diameter dilation computed from individual capillary responses averaged
Supplementary Figure 1 The average sigmoid parametric curves of capillary dilation time courses and average time to 50% peak capillary diameter dilation computed from individual capillary responses averaged
ACID-BASE AND ELECTROLYTE TEACHING CASE Treating Profound Hyponatremia: A Strategy for Controlled Correction
 ACID-BASE AND ELECTROLYTE TEACHING CASE Treating Profound Hyponatremia: A Strategy for Controlled Correction Richard H. Sterns, MD, John Kevin Hix, MD, and Stephen Silver, MD An alcoholic patient presented
ACID-BASE AND ELECTROLYTE TEACHING CASE Treating Profound Hyponatremia: A Strategy for Controlled Correction Richard H. Sterns, MD, John Kevin Hix, MD, and Stephen Silver, MD An alcoholic patient presented
11 th Annual Cerebrovascular Symposium 5/11-12/2017. Hypertonic Use D E R E K C L A R K
 Hypertonic Use D E R E K C L A R K 1 Outline Types of hyperosmolar therapy Review Cerebral Na Physiology Differences between periphery and BBB Acute phase Subacute phase Chronic changes Hypertonic Saline
Hypertonic Use D E R E K C L A R K 1 Outline Types of hyperosmolar therapy Review Cerebral Na Physiology Differences between periphery and BBB Acute phase Subacute phase Chronic changes Hypertonic Saline
Introduction. Acute sodium overload produces renal tubulointerstitial inflammation in normal rats
 Acute sodium overload produces renal tubulointerstitial inflammation in normal rats MI Roson, et al. Kidney International (2006) Introduction Present by Kanya Bunnan and Wiraporn paebua Tubular sodium
Acute sodium overload produces renal tubulointerstitial inflammation in normal rats MI Roson, et al. Kidney International (2006) Introduction Present by Kanya Bunnan and Wiraporn paebua Tubular sodium
2015 Diagnostic Slide Session
 2015 Diagnostic Slide Session Case 3 R.S. Tashjian, MD A.M. Langer-Gould, MD S. Natarajan, MD B.K. Kleinschmidt-DeMasters, MD H.V. Vinters, MD Disclosures No financial disclosures or conflicts of interest
2015 Diagnostic Slide Session Case 3 R.S. Tashjian, MD A.M. Langer-Gould, MD S. Natarajan, MD B.K. Kleinschmidt-DeMasters, MD H.V. Vinters, MD Disclosures No financial disclosures or conflicts of interest
Where vaptans do and do not fit in the treatment of hyponatremia
 http://www.kidney-international.org & 2012 International Society of Nephrology Where vaptans do and do not fit in the treatment of hyponatremia Anna J. Jovanovich 1 and Tomas Berl 1 1 Division of Renal
http://www.kidney-international.org & 2012 International Society of Nephrology Where vaptans do and do not fit in the treatment of hyponatremia Anna J. Jovanovich 1 and Tomas Berl 1 1 Division of Renal
Neurohypophysis. AVP Receptors. Hyponatremia in Pituitary Disorders 9/29/2016. Lewis S. Blevins, Jr., M.D.
 in Pituitary Disorders Lewis S. Blevins, Jr., M.D. Neurohypophysis AVP secreting neurons in SON and PVN Osmo- and thirst receptors/centers in anterior hypothalamus Ascending pathways from ANS and brainstem
in Pituitary Disorders Lewis S. Blevins, Jr., M.D. Neurohypophysis AVP secreting neurons in SON and PVN Osmo- and thirst receptors/centers in anterior hypothalamus Ascending pathways from ANS and brainstem
Treating the syndrome of inappropriate ADH secretion with isotonic saline
 Q J Med 1998; 91:749 753 Treating the syndrome of inappropriate ADH secretion with isotonic saline W. MUSCH and G. DECAUX1 From the Department of Internal Medicine, Bracops Hospital, Brussels, and 1Department
Q J Med 1998; 91:749 753 Treating the syndrome of inappropriate ADH secretion with isotonic saline W. MUSCH and G. DECAUX1 From the Department of Internal Medicine, Bracops Hospital, Brussels, and 1Department
SATURDAY PRESENTATIONS
 Carolinas Chapter - American Association of Clinical Endocrinologists SATURDAY PRESENTATIONS 2018 Annual Meeting September 7-9, 2018 Kiawah Island Golf Resort Kiawah Island, SC This continuing medical
Carolinas Chapter - American Association of Clinical Endocrinologists SATURDAY PRESENTATIONS 2018 Annual Meeting September 7-9, 2018 Kiawah Island Golf Resort Kiawah Island, SC This continuing medical
Carolinas Chapter - American Association of Clinical Endocrinologists SATURDAY HANDOUTS Annual Meeting
 Carolinas Chapter - American Association of Clinical Endocrinologists SATURDAY HANDOUTS 2018 Annual Meeting September 7-9, 2018 Kiawah Island Golf Resort Kiawah Island, SC This continuing medical education
Carolinas Chapter - American Association of Clinical Endocrinologists SATURDAY HANDOUTS 2018 Annual Meeting September 7-9, 2018 Kiawah Island Golf Resort Kiawah Island, SC This continuing medical education
A Case of Osmotic Demyelination Presenting with Severe Hypernatremia
 Case Report ISSN 1738-5997 (Print) ISSN 2092-9935 (Online) Electrolyte Blood Press 13:30-36, 2015 http://dx.doi.org/10.5049/ebp.2015.13.1.30 A Case of Osmotic Demyelination Presenting with Severe Hypernatremia
Case Report ISSN 1738-5997 (Print) ISSN 2092-9935 (Online) Electrolyte Blood Press 13:30-36, 2015 http://dx.doi.org/10.5049/ebp.2015.13.1.30 A Case of Osmotic Demyelination Presenting with Severe Hypernatremia
Iposodiemia: diagnosi e trattamento
 Iposodiemia: diagnosi e trattamento Enrico Fiaccadori Unita di Fisiopatologia dell Insufficienza Renale Acuta e Cronica Dipartimento di Medicina Clinica e Sperimentale Universita degli Studi di Parma Hyponatremia
Iposodiemia: diagnosi e trattamento Enrico Fiaccadori Unita di Fisiopatologia dell Insufficienza Renale Acuta e Cronica Dipartimento di Medicina Clinica e Sperimentale Universita degli Studi di Parma Hyponatremia
SHORTLY AFTER ITS FIRST DEpiction
 OBSERVATION Seven-Tesla Magnetic Resonance Imaging New Vision of Microvascular Abnormalities in Multiple Sclerosis Yulin Ge, MD; Vahe M. Zohrabian, MD; Robert I. Grossman, MD Background: Although the role
OBSERVATION Seven-Tesla Magnetic Resonance Imaging New Vision of Microvascular Abnormalities in Multiple Sclerosis Yulin Ge, MD; Vahe M. Zohrabian, MD; Robert I. Grossman, MD Background: Although the role
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines
 Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
Dr Francis A. Olaolorun Report on ISN/CAEN category 1A August 2016 research grant Home institution: Host institution:
 Dr Francis. Olaolorun Report on ISN/CEN category 1 ugust 2016 research grant Home institution: Neuroscience Unit, Department of Veterinary natomy, University of Ibadan, Ibadan, Nigeria. Host institution:
Dr Francis. Olaolorun Report on ISN/CEN category 1 ugust 2016 research grant Home institution: Neuroscience Unit, Department of Veterinary natomy, University of Ibadan, Ibadan, Nigeria. Host institution:
Extrapontine Myelinolysis in a Patient with Primary Adrenal Insufficiency
 146 Extrapontine Myelinolysis in a Patient with Primary Adrenal Insufficiency Jr-Wei Wu 1, Pei-Ning Wang 1,3, Jiing-Feng Lirng 2,3, Ruei-Wen Hsu 1, Wei-Ta Chen 1,3 Abstract Purpose: To report the development
146 Extrapontine Myelinolysis in a Patient with Primary Adrenal Insufficiency Jr-Wei Wu 1, Pei-Ning Wang 1,3, Jiing-Feng Lirng 2,3, Ruei-Wen Hsu 1, Wei-Ta Chen 1,3 Abstract Purpose: To report the development
mm Distance (mm)
 b a Magnet Illumination Coverslips MPs Objective 2575 µm 1875 µm 1575 µm 1075 µm 875 µm 545 µm 20µm 2 3 0.5 0.3mm 1 1000 100 10 1 0.1 1000 100 10 1 0.1 Field Induction (Gauss) 1.5 0 5 10 15 20 Distance
b a Magnet Illumination Coverslips MPs Objective 2575 µm 1875 µm 1575 µm 1075 µm 875 µm 545 µm 20µm 2 3 0.5 0.3mm 1 1000 100 10 1 0.1 1000 100 10 1 0.1 Field Induction (Gauss) 1.5 0 5 10 15 20 Distance
The pathophysiology and treatment of hyponatraemic encephalopathy: an update
 Nephrol Dial Transplant (2003) 18: 2486 2491 DOI: 10.1093/ndt/gfg394 Invited Comment The pathophysiology and treatment of hyponatraemic encephalopathy: an update Michael L. Moritz 1 and J. Carlos Ayus
Nephrol Dial Transplant (2003) 18: 2486 2491 DOI: 10.1093/ndt/gfg394 Invited Comment The pathophysiology and treatment of hyponatraemic encephalopathy: an update Michael L. Moritz 1 and J. Carlos Ayus
Supplementary Methods
 1 Supplementary Methods Social Preference Test Subjects Seventy-four Long-Evans, male rats served as subjects (S-rats) in the foodpreference test, with 40 assigned to the CXT-Same (CXT-S) Condition and
1 Supplementary Methods Social Preference Test Subjects Seventy-four Long-Evans, male rats served as subjects (S-rats) in the foodpreference test, with 40 assigned to the CXT-Same (CXT-S) Condition and
TOXIC AND NUTRITIONAL DISORDER MODULE
 TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
All but Vaptans. Pr Guy DECAUX Service de Médecine Interne Général Cliniques Universitaires Erasme, Bruxelles
 All but Vaptans Pr Guy DECAUX Service de Médecine Interne Général Cliniques Universitaires Erasme, Bruxelles [ Na ] = Na + e + K + e TBW 60 y BW 66 kg, TBW ± 33 L, SNa 140 meq/l TBW 1 L SNa: 3% (or 4.2
All but Vaptans Pr Guy DECAUX Service de Médecine Interne Général Cliniques Universitaires Erasme, Bruxelles [ Na ] = Na + e + K + e TBW 60 y BW 66 kg, TBW ± 33 L, SNa 140 meq/l TBW 1 L SNa: 3% (or 4.2
Hematopoietic Stem Cell Transplantation for Adrenoleukodystrophy
 Hematopoietic Stem Cell Transplantation for Adrenoleukodystrophy 2011 NHLBI Pediatric Workshop Sept. 14, 2011 Paul Orchard, M.D. Division of Pediatric Blood and Marrow Transplant University of Minnesota
Hematopoietic Stem Cell Transplantation for Adrenoleukodystrophy 2011 NHLBI Pediatric Workshop Sept. 14, 2011 Paul Orchard, M.D. Division of Pediatric Blood and Marrow Transplant University of Minnesota
1 MS Lesions in T2-Weighted Images
 1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
BIOL 347L Laboratory Three
 Introduction BIOL 347L Laboratory Three Osmosis in potato and carrot samples Osmosis is the movement of water molecules through a selectively permeable membrane into a region of higher solute concentration,
Introduction BIOL 347L Laboratory Three Osmosis in potato and carrot samples Osmosis is the movement of water molecules through a selectively permeable membrane into a region of higher solute concentration,
Supplementary Information
 Supplementary Information Title Degeneration and impaired regeneration of gray matter oligodendrocytes in amyotrophic lateral sclerosis Authors Shin H. Kang, Ying Li, Masahiro Fukaya, Ileana Lorenzini,
Supplementary Information Title Degeneration and impaired regeneration of gray matter oligodendrocytes in amyotrophic lateral sclerosis Authors Shin H. Kang, Ying Li, Masahiro Fukaya, Ileana Lorenzini,
Cerebral Salt Wasting
 Cerebral Salt Wasting Heather A Martin MSN, RN, CNRN, SCRN Swedish Medical Center 1 Disclosures none 2 2 The problem Hyponatremia is the most common disorder of electrolytes encountered in medical practice
Cerebral Salt Wasting Heather A Martin MSN, RN, CNRN, SCRN Swedish Medical Center 1 Disclosures none 2 2 The problem Hyponatremia is the most common disorder of electrolytes encountered in medical practice
SCIRF Award #2016 I-03 PI: Azizul Haque, PhD Grant Title: Neuron-specific Enolase and SCI
 SCIRF Award #2016 I-03 PI: Azizul Haque, PhD Grant Title: Neuron-specific Enolase and SCI 10-month Technical Progress Report Enolase is a multifunctional glycolytic enzyme involved in growth control, hypoxia,
SCIRF Award #2016 I-03 PI: Azizul Haque, PhD Grant Title: Neuron-specific Enolase and SCI 10-month Technical Progress Report Enolase is a multifunctional glycolytic enzyme involved in growth control, hypoxia,
Human Cerebral Osmolytes during Chronic Hyponatremia A Proton Magnetic Resonance Spectroscopy Study
 Human Cerebral Osmolytes during Chronic Hyponatremia A Proton Magnetic Resonance Spectroscopy Study John S. Videen,t Thomas Michaelis, Patrick Pinto,"1 and Brian D. Ross" tmagnetic Resonance Spectroscopy
Human Cerebral Osmolytes during Chronic Hyponatremia A Proton Magnetic Resonance Spectroscopy Study John S. Videen,t Thomas Michaelis, Patrick Pinto,"1 and Brian D. Ross" tmagnetic Resonance Spectroscopy
Workshop on Hyponatremia. Pr Guy DECAUX Service de Médecine Interne Général Cliniques Universitaires Erasme, Bruxelles
 Workshop on Hyponatremia Pr Guy DECAUX Service de Médecine Interne Général Cliniques Universitaires Erasme, Bruxelles CASE REPORT I A 70-year-old female patient is hospitalized because she fall on the
Workshop on Hyponatremia Pr Guy DECAUX Service de Médecine Interne Général Cliniques Universitaires Erasme, Bruxelles CASE REPORT I A 70-year-old female patient is hospitalized because she fall on the
Laura Tormoehlen, M.D. Neurology and EM-Toxicology Indiana University
 Laura Tormoehlen, M.D. Neurology and EM-Toxicology Indiana University Disclosures! No conflicts of interest to disclose Neuroimaging 101! Plain films! Computed tomography " Angiography " Perfusion! Magnetic
Laura Tormoehlen, M.D. Neurology and EM-Toxicology Indiana University Disclosures! No conflicts of interest to disclose Neuroimaging 101! Plain films! Computed tomography " Angiography " Perfusion! Magnetic
Demyelinating Diseases of the Brain
 Department of Radiology University of California San Diego Demyelinating Diseases of the Brain John R. Hesselink, M.D. T1-Weighted Images Normal White Matter Contents Axons with envelope of myelin Neuroglia
Department of Radiology University of California San Diego Demyelinating Diseases of the Brain John R. Hesselink, M.D. T1-Weighted Images Normal White Matter Contents Axons with envelope of myelin Neuroglia
NIH Public Access Author Manuscript Arch Neurol. Author manuscript; available in PMC 2008 November 5.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Neurol. 2008 June ; 65(6): 812 816. doi:10.1001/archneur.65.6.812. 7T MRI: New Vision of Microvascular Abnormalities in Multiple
NIH Public Access Author Manuscript Published in final edited form as: Arch Neurol. 2008 June ; 65(6): 812 816. doi:10.1001/archneur.65.6.812. 7T MRI: New Vision of Microvascular Abnormalities in Multiple
HYPOTHALAMIC ELECTRICAL ACTIVITIES PRODUCED BY FACTORS CAUSING DISCHARGE OF PITUITARY HORMONES
 HYPOTHALAMIC ELECTRICAL ACTIVITIES PRODUCED BY FACTORS CAUSING DISCHARGE OF PITUITARY HORMONES TERUO NAKAYAMA* Institute of Physiology, School of Medicine, University of Nagoya It is known that electrical
HYPOTHALAMIC ELECTRICAL ACTIVITIES PRODUCED BY FACTORS CAUSING DISCHARGE OF PITUITARY HORMONES TERUO NAKAYAMA* Institute of Physiology, School of Medicine, University of Nagoya It is known that electrical
Appendix 1. A. Procedure for preparing histopathology slides. The liver removed and stored immediately in buffered formalin 10 % for
 Appendix 1 A. Procedure for preparing histopathology slides. The liver removed and stored immediately in buffered formalin 10 % for histopathological examination. The tissue fixed for at least 48 hours
Appendix 1 A. Procedure for preparing histopathology slides. The liver removed and stored immediately in buffered formalin 10 % for histopathological examination. The tissue fixed for at least 48 hours
Dr. Dafalla Ahmed Babiker Jazan University
 Dr. Dafalla Ahmed Babiker Jazan University objectives Overview Definition of dehydration Causes of dehydration Types of dehydration Diagnosis, signs and symptoms Management of dehydration Complications
Dr. Dafalla Ahmed Babiker Jazan University objectives Overview Definition of dehydration Causes of dehydration Types of dehydration Diagnosis, signs and symptoms Management of dehydration Complications
APPENDIX 1 ETHICAL CLEARANCE
 APPENDIX 1 ETHICAL CLEARANCE 75 APPENDIX 2 76 PROCEDURE FOR PREPARING OF LIVER HISTOLOGY SLIDES Overview: Histology involves the use of a set of techniques to examine the morphology, architecture and composition
APPENDIX 1 ETHICAL CLEARANCE 75 APPENDIX 2 76 PROCEDURE FOR PREPARING OF LIVER HISTOLOGY SLIDES Overview: Histology involves the use of a set of techniques to examine the morphology, architecture and composition
Complications and management of hyponatremia
 REVIEW C URRENT OPINION Complications and management of hyponatremia Richard H. Sterns and Stephen M. Silver Purpose of review Hyponatremia causes significant morbidity, mortality, and disability. This
REVIEW C URRENT OPINION Complications and management of hyponatremia Richard H. Sterns and Stephen M. Silver Purpose of review Hyponatremia causes significant morbidity, mortality, and disability. This
For nearly 25 years, the treatment of hyponatremia
 The Treatment of Hyponatremia Richard H. Sterns, MD, Sagar U. Nigwekar, MD, and John Kevin Hix, MD Summary: Virtually all investigators now agree that self-induced water intoxication, symptomatic hospital-acquired
The Treatment of Hyponatremia Richard H. Sterns, MD, Sagar U. Nigwekar, MD, and John Kevin Hix, MD Summary: Virtually all investigators now agree that self-induced water intoxication, symptomatic hospital-acquired
Osmotic Demyelination Syndrome Case Report POPOVA RD, KALCHEV EB, VALCHEV GN, KALOYANOVA DV, TENEVA TG, BALEV BD
 Osmotic Demyelination Syndrome Case Report POPOVA RD, KALCHEV EB, VALCHEV GN, KALOYANOVA DV, TENEVA TG, BALEV BD Once upon a time on a Saturday shift u An emergency head CT scan was ordered from the ICU
Osmotic Demyelination Syndrome Case Report POPOVA RD, KALCHEV EB, VALCHEV GN, KALOYANOVA DV, TENEVA TG, BALEV BD Once upon a time on a Saturday shift u An emergency head CT scan was ordered from the ICU
Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences
 Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences Nils Daniel Forkert 1, Dennis Säring 1, Andrea Eisenbeis 2, Frank Leypoldt 3, Jens Fiehler 2, Heinz Handels
Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences Nils Daniel Forkert 1, Dennis Säring 1, Andrea Eisenbeis 2, Frank Leypoldt 3, Jens Fiehler 2, Heinz Handels
Pathophysiology: Regulation of Water Intake and Excretion, Ghent 03/2013. Outline: Regulation of water intake and excretion
 Pathophysiology: Regulation of Water Intake and Excretion, Ghent 03/2013 Daniel G. Bichet, M.D. Université de Montréal Groupe des Protéines Membranaires; Service de néphrologie, Hôpital du Sacré- Cœur
Pathophysiology: Regulation of Water Intake and Excretion, Ghent 03/2013 Daniel G. Bichet, M.D. Université de Montréal Groupe des Protéines Membranaires; Service de néphrologie, Hôpital du Sacré- Cœur
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung
 IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
Progress Report for NJCSCR (Yu-Wen Chang)
 Progress Report for NJCSCR (Yu-Wen Chang) Overall Plan Summary: Traumatic injury to the spinal cord initiates a cascade of degenerative processes, known as secondary injury, which include various inflammatory
Progress Report for NJCSCR (Yu-Wen Chang) Overall Plan Summary: Traumatic injury to the spinal cord initiates a cascade of degenerative processes, known as secondary injury, which include various inflammatory
1.0. FSL NMDAR-fEPSP 0.8. amplitude (mv) Intensity (µa) 2.0 SD FSL Time (ms)
 a 2.5 1. AMPAR-fEPSP slope (mv/ms) 2. 1. NMDAR-fEPSP amplitude (mv).8.6.4.5.2. 2 4 6 8. 1 2 3 4 5 Intensity (µa) Intensity (µa) b 2. PPF Ratio (fepsp2/fepsp1) 1..5. 5 1 2 5 Time (ms) Supplementary Figure
a 2.5 1. AMPAR-fEPSP slope (mv/ms) 2. 1. NMDAR-fEPSP amplitude (mv).8.6.4.5.2. 2 4 6 8. 1 2 3 4 5 Intensity (µa) Intensity (µa) b 2. PPF Ratio (fepsp2/fepsp1) 1..5. 5 1 2 5 Time (ms) Supplementary Figure
Lina AL-Lawama and Tasneem Montaj. Abdullah Nimer. Loai Zghoul
 2 Lina AL-Lawama and Tasneem Montaj Abdullah Nimer Loai Zghoul At the end of this sheet you should be able to understand the general characteristics of action potential and some of its clinical applications
2 Lina AL-Lawama and Tasneem Montaj Abdullah Nimer Loai Zghoul At the end of this sheet you should be able to understand the general characteristics of action potential and some of its clinical applications
Journal of Chemical and Pharmaceutical Research
 Available online www.jocpr.com Journal of Chemical and Pharmaceutical Research ISSN No: 0975-7384 CODEN(USA): JCPRC5 J. Chem. Pharm. Res., 2011, 3(5):468-472 Study on the anticonvulsant activity of Pentazocine
Available online www.jocpr.com Journal of Chemical and Pharmaceutical Research ISSN No: 0975-7384 CODEN(USA): JCPRC5 J. Chem. Pharm. Res., 2011, 3(5):468-472 Study on the anticonvulsant activity of Pentazocine
The pathogenesis of nervous distemper
 Veterinary Sciences Tomorrow - 2004 The pathogenesis of nervous distemper Marc Vandevelde Canine distemper is a highly contagious viral disease of dogs and of all animals in the Canidae, Mustellidae and
Veterinary Sciences Tomorrow - 2004 The pathogenesis of nervous distemper Marc Vandevelde Canine distemper is a highly contagious viral disease of dogs and of all animals in the Canidae, Mustellidae and
Sawada J, Orimoto R, Misu T, Katayama T, Aizawa H, Asanome A, Takahashi K, Saito T, Anei R, Kamada K, Miyokawa N, Takahashi T, Fujihara K, Hasebe N.
 Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
Mult Scler (2014.9) 20(10):1413-1416. A case of pathology-proven neuromyelitis optica spectrum disorder with Sjögren syndrome manifesting aphasia and apraxia due to a localized cerebral white matter lesion.
The Effects of Chemotherapy on Cognitive Behavior and Neurogenesis in an Animal Model of Pre- and Post- Menopausal Females
 The Effects of Chemotherapy on Cognitive Behavior and Neurogenesis in an Animal Model of Pre- and Post- Menopausal Females Samantha Pavlock (Medical Student) Pradeep Bhide and Deirdre McCarthy (Faculty
The Effects of Chemotherapy on Cognitive Behavior and Neurogenesis in an Animal Model of Pre- and Post- Menopausal Females Samantha Pavlock (Medical Student) Pradeep Bhide and Deirdre McCarthy (Faculty
Infection-Associated Neurological Syndromes
 Infection-Associated Neurological Syndromes Anand P, MD PhD Medical Director, BloodCenter of Wisconsin Assistant Professor, Medical College of Wisconsin ASFA Annual Meeting San Antonio, TX, May 8th, 2015
Infection-Associated Neurological Syndromes Anand P, MD PhD Medical Director, BloodCenter of Wisconsin Assistant Professor, Medical College of Wisconsin ASFA Annual Meeting San Antonio, TX, May 8th, 2015
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: van Seters M, van Beurden M, ten Kate FJW, et al. Treatment
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: van Seters M, van Beurden M, ten Kate FJW, et al. Treatment
International Journal of Biological & Medical Research
 Int J Biol Med Res. 213; 4(1): 282-286 Int J Biol Med Res Volume 3, Issue 1, Jan 2 www.biomedscidirect.com BioMedSciDirect Publications Contents lists available at BioMedSciDirect Publications International
Int J Biol Med Res. 213; 4(1): 282-286 Int J Biol Med Res Volume 3, Issue 1, Jan 2 www.biomedscidirect.com BioMedSciDirect Publications Contents lists available at BioMedSciDirect Publications International
Sestrin2 and BNIP3 (Bcl-2/adenovirus E1B 19kDa-interacting. protein3) regulate autophagy and mitophagy in renal tubular cells in. acute kidney injury
 Sestrin2 and BNIP3 (Bcl-2/adenovirus E1B 19kDa-interacting protein3) regulate autophagy and mitophagy in renal tubular cells in acute kidney injury by Masayuki Ishihara 1, Madoka Urushido 2, Kazu Hamada
Sestrin2 and BNIP3 (Bcl-2/adenovirus E1B 19kDa-interacting protein3) regulate autophagy and mitophagy in renal tubular cells in acute kidney injury by Masayuki Ishihara 1, Madoka Urushido 2, Kazu Hamada
Supplementary Methods: Omalizumab Trial This double-blind, randomized, placebo-controlled trial was conducted at the University of Utah Hospital and
 Supplementary Methods: Omalizumab Trial This double-blind, randomized, placebo-controlled trial was conducted at the University of Utah Hospital and Primary Children s Hospital, Salt Lake City, UT, both
Supplementary Methods: Omalizumab Trial This double-blind, randomized, placebo-controlled trial was conducted at the University of Utah Hospital and Primary Children s Hospital, Salt Lake City, UT, both
Nature Neuroscience: doi: /nn Supplementary Figure 1
 Supplementary Figure 1 Quantification of myelin fragments in the aging brain (a) Electron microscopy on corpus callosum is shown for a 18-month-old wild type mice. Myelin fragments (arrows) were detected
Supplementary Figure 1 Quantification of myelin fragments in the aging brain (a) Electron microscopy on corpus callosum is shown for a 18-month-old wild type mice. Myelin fragments (arrows) were detected
Supplementary Figure 1
 Supplementary Figure 1 AAV-GFP injection in the MEC of the mouse brain C57Bl/6 mice at 4 months of age were injected with AAV-GFP into the MEC and sacrificed at 7 days post injection (dpi). (a) Brains
Supplementary Figure 1 AAV-GFP injection in the MEC of the mouse brain C57Bl/6 mice at 4 months of age were injected with AAV-GFP into the MEC and sacrificed at 7 days post injection (dpi). (a) Brains
Cell Culture. The human thyroid follicular carcinoma cell lines FTC-238, FTC-236 and FTC-
 Supplemental material and methods Reagents. Hydralazine was purchased from Sigma-Aldrich. Cell Culture. The human thyroid follicular carcinoma cell lines FTC-238, FTC-236 and FTC- 133, human thyroid medullary
Supplemental material and methods Reagents. Hydralazine was purchased from Sigma-Aldrich. Cell Culture. The human thyroid follicular carcinoma cell lines FTC-238, FTC-236 and FTC- 133, human thyroid medullary
Pediatric Sodium Disorders
 Pediatric Sodium Disorders Guideline developed by Ron Sanders, Jr., MD, MS, in collaboration with the ANGELS team. Last reviewed by Ron Sanders, Jr., MD, MS on May 20, 2016. Definitions, Physiology, Assessment,
Pediatric Sodium Disorders Guideline developed by Ron Sanders, Jr., MD, MS, in collaboration with the ANGELS team. Last reviewed by Ron Sanders, Jr., MD, MS on May 20, 2016. Definitions, Physiology, Assessment,
Hyponatræmia: analysis
 ESPEN Congress Nice 2010 Hyper- and hyponatraemia - serious and iatrogenic problems Hyponatræmia: analysis Mathias Plauth Hyponatremia Case Analysis Mathias Plauth Klinik für Innere Medizin Städtisches
ESPEN Congress Nice 2010 Hyper- and hyponatraemia - serious and iatrogenic problems Hyponatræmia: analysis Mathias Plauth Hyponatremia Case Analysis Mathias Plauth Klinik für Innere Medizin Städtisches
brain ofexperimental animals with chronic hypernatremia (3-
 Study of Brain Electrolytes and Organic Osmolytes during Correction of Chronic Hyponatremia Implications for the Pathogenesis of Central Pontine Myelinolysis Yeong-Hau H. Lien, Joseph 1. Shapiro, and Laurence
Study of Brain Electrolytes and Organic Osmolytes during Correction of Chronic Hyponatremia Implications for the Pathogenesis of Central Pontine Myelinolysis Yeong-Hau H. Lien, Joseph 1. Shapiro, and Laurence
Central pontine myelinolysis: historical and mechanistic considerations
 Metab Brain Dis (2010) 25:97 106 DOI 10.1007/s11011-010-9175-0 ORIGINAL PAPER Central pontine myelinolysis: historical and mechanistic considerations Michael D. Norenberg Received: 18 November 2009 / Accepted:
Metab Brain Dis (2010) 25:97 106 DOI 10.1007/s11011-010-9175-0 ORIGINAL PAPER Central pontine myelinolysis: historical and mechanistic considerations Michael D. Norenberg Received: 18 November 2009 / Accepted:
Hyponatremia with hypoxia: Effects on brain adaptation, perfusion, and histology in rodents
 http://www.kidney-international.org & 26 International Society of Nephrology original article see commentary on page 1291 Hyponatremia with hypoxia: Effects on brain adaptation, perfusion, and histology
http://www.kidney-international.org & 26 International Society of Nephrology original article see commentary on page 1291 Hyponatremia with hypoxia: Effects on brain adaptation, perfusion, and histology
Hyponatraemia: confident diagnosis, effective treatment and avoiding disasters. Dr James Ahlquist Endocrinologist Southend Hospital
 Hyponatraemia: confident diagnosis, effective treatment and avoiding disasters Dr James Ahlquist Endocrinologist Southend Hospital Hyponatraemia: a common electrolyte disorder Electrolyte disorder Prevalence
Hyponatraemia: confident diagnosis, effective treatment and avoiding disasters Dr James Ahlquist Endocrinologist Southend Hospital Hyponatraemia: a common electrolyte disorder Electrolyte disorder Prevalence
R. Pluta, M. Ułamek, and S. Januszewski. relatively high [3] and an e ect of this incidence is irreversible. Summary
![R. Pluta, M. Ułamek, and S. Januszewski. relatively high [3] and an e ect of this incidence is irreversible. Summary R. Pluta, M. Ułamek, and S. Januszewski. relatively high [3] and an e ect of this incidence is irreversible. Summary](/thumbs/88/117553410.jpg) Acta Neurochir (2006) [Suppl] 96: 267 271 6 Springer-Verlag 2006 Printed in Austria Micro-blood-brain barrier openings and cytotoxic fragments of amyloid precursor protein accumulation in white matter
Acta Neurochir (2006) [Suppl] 96: 267 271 6 Springer-Verlag 2006 Printed in Austria Micro-blood-brain barrier openings and cytotoxic fragments of amyloid precursor protein accumulation in white matter
CHAPTER 4 IMMUNOLOGICAL TECHNIQUES
 CHAPTER 4 IMMUNOLOGICAL TECHNIQUES Nitroblue Tetrazolium Chloride (NBT) Reduction test NBT reduction test was evaluated by employing the method described by Hudson and Hay,1989 based upon principle that
CHAPTER 4 IMMUNOLOGICAL TECHNIQUES Nitroblue Tetrazolium Chloride (NBT) Reduction test NBT reduction test was evaluated by employing the method described by Hudson and Hay,1989 based upon principle that
Microglia-derived extracellular vesicles regulate the proliferation and differentiation of oligodendrocyte precursor cells
 University of Turin CNR Institute of Neuroscience Microglia-derived extracellular vesicles regulate the proliferation and differentiation of oligodendrocyte precursor cells Roberta Parolisi Turin, December
University of Turin CNR Institute of Neuroscience Microglia-derived extracellular vesicles regulate the proliferation and differentiation of oligodendrocyte precursor cells Roberta Parolisi Turin, December
HTRF MEASUREMENT OF CYTOKINE RELEASE FROM FRESH BLOOD SAMPLES
 HTRF MEASUREMENT OF CYTOKINE RELEASE FROM FRESH BLOOD SAMPLES APPLICATION NOTE ABSTRACT Cisbio offers a comprehensive line of HTRF cytokine assays to investigate the functional response of immune cells.
HTRF MEASUREMENT OF CYTOKINE RELEASE FROM FRESH BLOOD SAMPLES APPLICATION NOTE ABSTRACT Cisbio offers a comprehensive line of HTRF cytokine assays to investigate the functional response of immune cells.
Cerebral Toxoplasmosis in HIV-Infected Patients. Ahmed Saad,MD,FACP
 Cerebral Toxoplasmosis in HIV-Infected Patients Ahmed Saad,MD,FACP Introduction Toxoplasmosis: Caused by the intracellular protozoan, Toxoplasma gondii. Immunocompetent persons with primary infection
Cerebral Toxoplasmosis in HIV-Infected Patients Ahmed Saad,MD,FACP Introduction Toxoplasmosis: Caused by the intracellular protozoan, Toxoplasma gondii. Immunocompetent persons with primary infection
Cells and viruses. Human isolates (A/Kawasaki/173/01 [H1N1], A/Yokohama/2057/03 [H3N2],
![Cells and viruses. Human isolates (A/Kawasaki/173/01 [H1N1], A/Yokohama/2057/03 [H3N2], Cells and viruses. Human isolates (A/Kawasaki/173/01 [H1N1], A/Yokohama/2057/03 [H3N2],](/thumbs/86/93801604.jpg) Supplementary information Methods Cells and viruses. Human isolates (A/Kawasaki/173/01 [H1N1], A/Yokohama/2057/03 [H3N2], and A/Hong Kong/213/03 [H5N1]) were grown in Madin-Darby canine kidney (MDCK) cells
Supplementary information Methods Cells and viruses. Human isolates (A/Kawasaki/173/01 [H1N1], A/Yokohama/2057/03 [H3N2], and A/Hong Kong/213/03 [H5N1]) were grown in Madin-Darby canine kidney (MDCK) cells
MULTIPLE SCLEROSIS IN Managing the complexity of multiple sclerosis. Olga Ciccarelli and Alan Thompson
 MULTIPLE SCLEROSIS IN 2015 Managing the complexity of multiple sclerosis Olga Ciccarelli and Alan Thompson The application of imaging biomarkers has provided new insights into the mechanisms of damage
MULTIPLE SCLEROSIS IN 2015 Managing the complexity of multiple sclerosis Olga Ciccarelli and Alan Thompson The application of imaging biomarkers has provided new insights into the mechanisms of damage
Dialysis Disequilibrium Syndrome: A Case Report & Concise Review
 ISSN: 2276-7797 Impact Factor 2012 (UJRI): 0.7634 ICV 2012: 5.98 Dialysis Disequilibrium Syndrome: A Case Report & Concise Review By Fahad Aziz Simanta Dutta Misbah Zaeem Research Article Dialysis Disequilibrium
ISSN: 2276-7797 Impact Factor 2012 (UJRI): 0.7634 ICV 2012: 5.98 Dialysis Disequilibrium Syndrome: A Case Report & Concise Review By Fahad Aziz Simanta Dutta Misbah Zaeem Research Article Dialysis Disequilibrium
Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome)
 J Radiol Sci 2012; 37: 45-50 Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome) Chien-Chuan Huang Tai-Yuan Chen Tai-Ching Wu Yu-Kun Tsui Te-Chang Wu Wen-Sheng Tzeng Chien-Jen Lin Department
J Radiol Sci 2012; 37: 45-50 Magnetic Resonance Imaging of Neuromyelitis Optica (Devic s Syndrome) Chien-Chuan Huang Tai-Yuan Chen Tai-Ching Wu Yu-Kun Tsui Te-Chang Wu Wen-Sheng Tzeng Chien-Jen Lin Department
Case Report Chronic Lymphocytic Inflammation with Pontine Perivascular Enhancement Responsive to Steroids, with Cranial and Caudal Extension
 Hindawi Case Reports in Neurological Medicine Volume 2017, Article ID 2593096, 4 pages https://doi.org/10.1155/2017/2593096 Case Report Chronic Lymphocytic Inflammation with Pontine Perivascular Enhancement
Hindawi Case Reports in Neurological Medicine Volume 2017, Article ID 2593096, 4 pages https://doi.org/10.1155/2017/2593096 Case Report Chronic Lymphocytic Inflammation with Pontine Perivascular Enhancement
COLLOID DROPLET FORMATION IN DOG THYROID IN VITRO
 COLLOID DROPLET FORMATION IN DOG THYROID IN VITRO Induction by Dibutyryl Cyclic-AMP I. PASTAN and S. HI. WOLLMAN. Froml the National Institute of Arthritis and Metabolic Diseases and the National Cancer
COLLOID DROPLET FORMATION IN DOG THYROID IN VITRO Induction by Dibutyryl Cyclic-AMP I. PASTAN and S. HI. WOLLMAN. Froml the National Institute of Arthritis and Metabolic Diseases and the National Cancer
Islet viability assay and Glucose Stimulated Insulin Secretion assay RT-PCR and Western Blot
 Islet viability assay and Glucose Stimulated Insulin Secretion assay Islet cell viability was determined by colorimetric (3-(4,5-dimethylthiazol-2-yl)-2,5- diphenyltetrazolium bromide assay using CellTiter
Islet viability assay and Glucose Stimulated Insulin Secretion assay Islet cell viability was determined by colorimetric (3-(4,5-dimethylthiazol-2-yl)-2,5- diphenyltetrazolium bromide assay using CellTiter
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance
 Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
AN E X P E R I M E N T A L METHOD FOR THE EVALUATION OF CONTRAST M E D I A USED IN CEREBRAL ANGIOGRAPHY
 AN E X P E R I M E N T A L METHOD FOR THE EVALUATION OF CONTRAST M E D I A USED IN CEREBRAL ANGIOGRAPHY BYRON M. BLOOR, M.D.,* FRANK R. WRENN, JR., M.D., t AND MAJOR GEORGE J. HAYES, M.C., U.S.A.:~ Division
AN E X P E R I M E N T A L METHOD FOR THE EVALUATION OF CONTRAST M E D I A USED IN CEREBRAL ANGIOGRAPHY BYRON M. BLOOR, M.D.,* FRANK R. WRENN, JR., M.D., t AND MAJOR GEORGE J. HAYES, M.C., U.S.A.:~ Division
Hypo/Hypernatremia. Stuart L. Goldstein MD. Director, Center for Acute Care Nephrology Cincinnati Children s Hospital
 Hypo/Hypernatremia Stuart L. Goldstein MD Director, Center for Acute Care Nephrology Cincinnati Children s Hospital Objectives Understand Fluid cellular shifts Understand maintenance fluid and calculations
Hypo/Hypernatremia Stuart L. Goldstein MD Director, Center for Acute Care Nephrology Cincinnati Children s Hospital Objectives Understand Fluid cellular shifts Understand maintenance fluid and calculations
Supporting Information
 Supporting Information Pang et al. 10.1073/pnas.1322009111 SI Materials and Methods ELISAs. These assays were performed as previously described (1). ELISA plates (MaxiSorp Nunc; Thermo Fisher Scientific)
Supporting Information Pang et al. 10.1073/pnas.1322009111 SI Materials and Methods ELISAs. These assays were performed as previously described (1). ELISA plates (MaxiSorp Nunc; Thermo Fisher Scientific)
Contact: Course outline: Contact for other times.
 Contact: kdelaney@uvic.ca Course outline: http://web.uvic.ca/~kdelaney/b367 Scheduled office hours: 1:00-3:00, M&Th Cunn. 259A Contact kdelaney@uvic.ca for other times. Quiz (0.5 hrs) midterm (1.4 hrs)
Contact: kdelaney@uvic.ca Course outline: http://web.uvic.ca/~kdelaney/b367 Scheduled office hours: 1:00-3:00, M&Th Cunn. 259A Contact kdelaney@uvic.ca for other times. Quiz (0.5 hrs) midterm (1.4 hrs)
An Evaluation of Xylene-free Processing of Tissues From the Central Nervous System Using the PelorisTM Dual Retort Rapid Tissue Processor
 An Evaluation of Xylene-free Processing of Tissues From the Central Nervous System Using the PelorisTM Dual Retort Rapid Tissue Processor Geoffrey Rolls Leica Microsystems, iosystems Division, Melbourne,
An Evaluation of Xylene-free Processing of Tissues From the Central Nervous System Using the PelorisTM Dual Retort Rapid Tissue Processor Geoffrey Rolls Leica Microsystems, iosystems Division, Melbourne,
LIST OF ORGANS FOR HISTOPATHOLOGICAL ANALYSIS:!! Neural!!!!!!Respiratory:! Brain : Cerebrum,!!! Lungs and trachea! Olfactory, Cerebellum!!!!Other:!
 LIST OF ORGANS FOR HISTOPATHOLOGICAL ANALYSIS:!! Neural!!!!!!Respiratory:! Brain : Cerebrum,!!! Lungs and trachea! Olfactory, Cerebellum!!!!Other:! Spinal cord and peripheral nerves! Eyes, Inner ear, nasal
LIST OF ORGANS FOR HISTOPATHOLOGICAL ANALYSIS:!! Neural!!!!!!Respiratory:! Brain : Cerebrum,!!! Lungs and trachea! Olfactory, Cerebellum!!!!Other:! Spinal cord and peripheral nerves! Eyes, Inner ear, nasal
Social stress induces neurovascular pathology promoting depression
 SUPPLEMENTARY INFORMATION Articles https://doi.org/10.1038/s41593-017-0010-3 In the format provided by the authors and unedited. Social stress induces neurovascular pathology promoting depression Caroline
SUPPLEMENTARY INFORMATION Articles https://doi.org/10.1038/s41593-017-0010-3 In the format provided by the authors and unedited. Social stress induces neurovascular pathology promoting depression Caroline
CHRONIC HYPONATREMIA IS A
 ORIGINAL CONTRIBUTION Chronic Hyponatremic Encephalopathy in Postmenopausal Women Association of Therapies With Morbidity and Mortality J. Carlos Ayus, MD Allen I. Arieff, MD CHRONIC HYPONATREMIA IS A
ORIGINAL CONTRIBUTION Chronic Hyponatremic Encephalopathy in Postmenopausal Women Association of Therapies With Morbidity and Mortality J. Carlos Ayus, MD Allen I. Arieff, MD CHRONIC HYPONATREMIA IS A
COPD lungs show an attached stratified mucus layer that separate. bacteria from the epithelial cells resembling the protective colonic
 COPD lungs show an attached stratified mucus layer that separate bacteria from the epithelial cells resembling the protective colonic mucus SUPPLEMENTARY TABLES AND FIGURES Tables S1 S8, page 1 and separate
COPD lungs show an attached stratified mucus layer that separate bacteria from the epithelial cells resembling the protective colonic mucus SUPPLEMENTARY TABLES AND FIGURES Tables S1 S8, page 1 and separate
Subconvulsive Dose of Kainic Acid Transiently Increases the Locomotor Activity of Adult Wistar Rats
 Physiol. Res. 64: 263-267, 2015 SHORT COMMUNICATION Subconvulsive Dose of Kainic Acid Transiently Increases the Locomotor Activity of Adult Wistar Rats V. RILJAK 1, D. MAREŠOVÁ 1, J. POKORNÝ 1, K. JANDOVÁ
Physiol. Res. 64: 263-267, 2015 SHORT COMMUNICATION Subconvulsive Dose of Kainic Acid Transiently Increases the Locomotor Activity of Adult Wistar Rats V. RILJAK 1, D. MAREŠOVÁ 1, J. POKORNÝ 1, K. JANDOVÁ
Pathogenesis of Cervical Myelopathy in Chronic Cervical Cord Compression Model of Rat
 Pathogenesis of Cervical Myelopathy in Chronic Cervical Cord Compression Model of Rat Shigeru Kobayashi,MD,PhD 1, Masafumi Kubota, PT 1, Hisao Iwamoto, MD,PhD 2, Riya Kosaka,MD,PhD 3, Katsuhiko Hayakawa,MD,PhD
Pathogenesis of Cervical Myelopathy in Chronic Cervical Cord Compression Model of Rat Shigeru Kobayashi,MD,PhD 1, Masafumi Kubota, PT 1, Hisao Iwamoto, MD,PhD 2, Riya Kosaka,MD,PhD 3, Katsuhiko Hayakawa,MD,PhD
Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/-
 Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization
 Cell Reports, Volume 9 Supplemental Information VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization Sharon Lim, Yin Zhang, Danfang Zhang, Fang Chen,
Cell Reports, Volume 9 Supplemental Information VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization Sharon Lim, Yin Zhang, Danfang Zhang, Fang Chen,
A case of central pontine myelinolysis in a patient after liver transplantation
 46 A case of central pontine myelinolysis in a patient after liver transplantation Mouloudi E 1 MD, PhD, Papadopoulos S 1, MD, Massa E 1, MD, Giasnetsova T 1, MD, Theodoridou Th 1, MD, Anastasiou A 2,
46 A case of central pontine myelinolysis in a patient after liver transplantation Mouloudi E 1 MD, PhD, Papadopoulos S 1, MD, Massa E 1, MD, Giasnetsova T 1, MD, Theodoridou Th 1, MD, Anastasiou A 2,
Radiologic-Pathologic Correlation of White Matter Disease
 The Neuroradiology Journal 22 (Suppl. 1): 26-32, 2009 www. centauro. it Radiologic-Pathologic Correlation of White Matter Disease J.G. SMIRNIOTOPOULOS 1,2,3,.. SMITH 1,2, E. RUSHING 2,4, F.M. MURPHY 2,
The Neuroradiology Journal 22 (Suppl. 1): 26-32, 2009 www. centauro. it Radiologic-Pathologic Correlation of White Matter Disease J.G. SMIRNIOTOPOULOS 1,2,3,.. SMITH 1,2, E. RUSHING 2,4, F.M. MURPHY 2,
