Graves disease may lead to exophthalmos that is
|
|
|
- Reynold Wade
- 5 years ago
- Views:
Transcription
1 Rev Bras Otorrinolaringol 2006;72(2):283-7 REVIEW ARTICLE Orbital endoscopic decompression in Graves Ophthalmopathy Wilma Terezinha Anselmo Lima 1, Mateus Perches 2, Fabiana Cardoso Pereira Valera 3, Ricardo Cassiano Demarco 4 Key words: Graves disease, endoscopic orbital decompression, proptosis. Summary Graves disease may lead to exophthalmos that is cosmetically unacceptable or causes visual loss. This has been managed surgically by external orbital decompression. However, a new minimally invasive endoscopic orbital decompression technique is now possible, with resection of the medial and posterior portion of the orbital limits requiring no cutaneous or gingival incisions. This technique produces decompression comparable to that obtained by external techniques. Endoscopic orbital decompression is a safe and effective procedure for the treatment of thyroid orbitopathy. 1 Associate Professor. 2 MD, Resident of Otorhinolaryngology - Department of Otorhinolaryngology, Ophthalmology and Head and Neck Surgery - FMRP-USP. 3 Assistant physician - University Hospital - Department of Otorhinolaryngology, Ophthalmology and Head and Neck Surgery - FMRP-USP. 4 Assistant physician - University Hospital - Department of Otorhinolaryngology, Ophthalmology and Head and Neck Surgery - FMRP-USP. Mailing Address: Profa. Dra. Wilma T. Anselmo-Lima - Departamento de Oftalmologia e Otorrinolaringologia e Cirurgia de Cabeça e Pescoço do HCFMRP-USP, Avenida Bandeirantes 3900 Ribeirão Preto SP Tel. (0xx16) Fax: (0xx16) Paper submitted to the ABORL-CCF SGP (Management Publications System) on September 8th, 2005, and was approved on the same date. 283
2 INTRODUCTION Graves Ophthalmopathy is an autoimmune disease characterized by deposition of antithyroglobulin immune complexes on the extra-ocular muscles. These complexes induce an inflammatory response through lymphocytes, mast cells and plasmatic cells, causing edema and fibrosis later on, with hypertrophy of the extra-ocular muscles - especially the inferior and middle rectus muscles and orbitary fat. Moreover, there is a stimulation of fibroblast-myogenic activity, resulting in an increase in orbital volume, causing proptosis, mainly. It is more common to women than men, with average age between 20 and 40 years 1-3. The most common clinical signs are proptosis - in different levels of intensity, asymmetrical or bilateral; and diplopia, because of the abnormal and asymmetrical mobility of extra-ocular muscles infiltrated by inflammatory cells. In more severe cases there is keratoconjunctivities, eyelid retraction and corneal ulcerations because of insufficient eyelid closure, and finally, optical neuropathy caused by a compression on the posterior third of ophthalmic nerve, at the orbital apex. Orbital involvement occurs in about 50% of the patients with Graves disease, but only 5 to 10% of these develop severe ophthalmopathy. The disease evolves slowly but progressively until it stabilizes, there are, however, rare cases of spontaneous resolution. Notwithstanding, those patients who develop severe proptosis or optical neuropathy require clinical or surgical treatment. About two-thirds of the patients respond to other treatment modalities, specially if treated in the acute phase, treated with steroids, orbital radiation (which is not efficient for proptosis and diplopia), immunesupressors and plasmapheresis. The acute phase lasts from 6 to 18 months, with orbital inflammation and congestion, increase in intraorbitary volume causing proptosis with anterior shifting of the eye ball. It evolves to a chronic and stable phase which may start from 18 months to 3 years after orbitopathy onset. In this phase, the fibrotic process sets in. The orbitopathy seems to follow a different pathway from the thyroid treatment, and normally does not bear relation with the thyroid abnormalities. It may precede, follow or even occur after hyperthyroidism, or even without clear hyperthyroidism. Surgical treatment for Graves ophthalmopathy is used to treat the consequences of the disease and, therefore, is done during the disease stable phase. It is indicated whenever there are symptoms of ocular surface exposure, optical neuropathy or for cosmetic reasons. It includes repairing strabismus, eyelid retraction and orbital decompression to correct exophthalmia6. The decompression major goals are to open more room to accommodate orbital content, thus reducing orbital tissue pressure; restore vision, allow the functioning of the extra-ocular muscles, eyelid closure and, consequently, reduce proptosis. There are cosmetic improvements. Different approaches have been described for orbital decompression: Lateral orbitotomy, frontal craniotomy, external fronto-ethmoidectomy, orbital transnasal decompression 7-9. Through these approached we may remove the orbital medial or lateral walls, orbital floor, both the floor and medial wall, both floor and lateral wall, and anterior cranial fossa. Walsh-Ogura 7 procedure, which uses a transnasal approach was the one most employed. Through a broad maxillary antrostomy we are able to remove the orbital floor, sparing the infra-orbitary nerve, followed by a transnasal ethmoidectomy and decompression of the medial orbital wall. However, it is an approach associated to Caldwell-Luc s procedure morbidity and may result in inferior shifting of the eye ball, with access limitations for the decompression of the orbital apex. With the development of endoscopic surgery, the transnasal removal of the lamina papyracea has caused proptosis reduction comparable to the results of other approaches, with advantages. Described by Kennedy et al. 10 and Michel et al. 4. It allows excellent view without the need for external incisions, with less morbidity and a more efficient approach for the optical neuropathy. Our goal with this paper is to describe the surgical technique, focusing on its advantages and disadvantages. Preoperative: Basically, besides routine evaluation carried out for any type of surgery, endoscopic assessment and radiology are paramount. Through endoscopy we may see alterations such as septal deviations and the presence of infections, which may be treated clinically or during the surgical procedure. The coronal slice in the CT scan is useful to access how aerated the ethmoid is, the integrity and slope of the ethmoid ceiling, as well as the orbital medial wall (it is important to evaluate the height of the posterior ethmoid sinus and its relation with the maxillary ceiling and determine whether the posterior ethmoid expands posteriorly and superiorly, involving the optical nerve and or the internal carotid artery), the thickness of the orbital floor (the thicker it is, the harder it is to remove it endoscopically through middle meatal antrostomy), the skull base situation. The axial view is useful to show the relation between the posterior ethmoid artery, the optical nerve and the orbital apex. Both views show the hypertrophy of the extrinsic eye muscles (Figure 1). SURGICAL TECHNIQUE Under general anesthesia, the patient is initially positioned in dorsal decubitus, with the head slightly tilted upwards, in 30º. We inject the anesthetic agent on the lateral wall placing cotton balls with vasoconstrictor agents in the nasal cavities. If there is septum deviation 284
3 we correct it prior to the main endoscopic procedure. The orbital decompression (OD) starts in the unciform process incision, with complete ethmoidectomy 11. We proceed with middle meatotomy as broadly as possible, in order to visualize the orbital floor, down to the posterior maxillary wall, enough to accommodate the orbital content and prevent obstructive maxillary sinusitis. We use the 45º endoscope to see the infraorbitary nerve in its canal, along the ceiling of the maxillary sinus, because this nerve represents the lateral limit for bone removal. Following that, we proceed with a transethmoidal sphenoidectomy, and anteriorly, we open the frontal recess. One should pay special attention to Onodi s cells, where the optical nerve may bulge. The anterior limit corresponds to the frontal maxillary process, close to the nasolacrimal duct. The superior limit corresponds to the floor of the anterior cranial fossa, where the ethmoidal arteries represent an important anatomical reference point. Inferiorly, the insertion of the inferior turbinate is the limit. The middle turbinate may be removed in order to optimize the orbital content prolapse. The lamina papyracea is then skeletonized and removed with the periosteum elevator, which easily separates it from the periorbital tissue (Figure 2). The lamina is carefully removed in order to avoid lacerations in the periorbital area, where there may be fat tissue herniations which may impair the periorbital skeletonization. We proceed with the dissection all the way to the posterior ethmoid bundle, close to the optical nerve, where the bone is thicker. Here we find the Zinn annulus, where the extra-ocular muscles are inserted, and certainly the optical nerve path. With the 45º endoscope we remove the orbital floor down to the infra-orbital vascular-nervous bundle, which is our lateral dissection limit. We dissect as posteriorly as possible. Once the periorbit is fully dissected and exposed, we make an incision in order to allow a free fat prolapse from the periorbital tissue. We proceed making two to four longitudinal, postero-anterior and infero-superior periorbital incisions. This sequence reduces the chance of the herniated fat impair the surgeon s view. One should be careful with the superficial unciform process removal in order to avoid penetrating the intraorbitary content. At the end of the procedure there is fat and orbital content extrusion (Figure 3). If necessary, we may proceed with lateral decompression at this stage, because through the medial decompression, it will be easy to expose the lateral bone wall. There is no need for nasal packing. The patient may be discharged on the next day following the procedure, with oral antibiotics (amoxicillin for 10 days) and saline solution nasal spray. DISCUSSION The progress of endoscopic procedures has opened new possibilities for otorhinolaryngologists to work in different areas that were considered difficult, such as dacriocistorrinostomy, orbital decompression and optical nerve decompression, in a safe and minimally invasive way. This technique was first described by Kennedy et al. in the early 90 s 10. The endoscopic approach allows an excellent view for a safe removal of the medial and inferior orbital wall, specially in the regions of the ethmoidal ceiling and orbital apex. The endoscopic orbital decompression is based on a broad middle meatotomy in order to allow broad view of the orbital floor. As to the transantral approach, the endoscopic orbital decompression does not cause hypoesthesia secondary to infra-orbitary nerve lesion, and causes fewer incidences of hypoglobus, thus allowing for a shorter hospital stay when compared to the traditional Walsh-Ogura 7 procedure. It also allows a more effective decompression of the orbit apex, specially indicated in cases of orbital neuropathy. The most difficult surgical step is the removal of the medial portion of the orbital floor, medially to the infraorbitary nerve, due to an excessive thickness that may be present on the floor; however it may be previously evaluated through the CT scan. Bone resections laterally to the infraorbitary cause little proptosis reduction and increase the incidence of hypoglobus and diplopia. Michel et al. 4 also described the bilateral removal of the middle conchae during decompression, aiming at increasing the area for orbit content extrusion. Endoscopically we have been able to achieve variable proptosis retraction, between 3.2 to 4.7 millimeters, as we can see on table 14,10,12,13. However, greater retractions may be reached if external approaches are associated, such as the removal of the lateral orbital wall. Among the disadvantages, we mention a higher incidence of diplopia, which may be surgically corrected later on, and the potential development of sinusitis or secondary mucocele The most frequently reported complications with this procedure are sinusitis or frontal or maxillary mucocele, CSF fistulas, lesion of the nasolacrimal duct, strabismus and diplopia, which may occur in 15 to 60% of Table 1. Reported series of proptosis retraction through endoscopiconly orbital decompression. Series # of orbits Average proptosis reduction Kennedy et al ,7mm Michel et al ,3mm Lund et al ,4mm Metson & Shore ,2mm 285
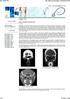
4 Figure 1a. CT scans, axial views (A) of a patient with Graves ophthalmopathy, showing the hypertrophy of the extrinsic ocular muscles. Figure 1b. CT scans, coronal views (B) of a patient with Graves ophthalmopathy, showing the hypertrophy of the extrinsic ocular muscles. Figure 2. Removal of the lamina papyracea in a left side orbital decompression. Figure 3. Extrusion of the orbital content after left side orbit endoscopic decompression. the cases. The latter may have spontaneous resolution in three to four weeks, but it may also appear later on, due to disease progress. In these cases, there is the need for strabismus correction. FINAL COMMENTS In the past this procedure was carried out externally, but currently the orbital decompression may be performed through an endoscopic approach, a minimally invasive procedure, allowing the removal of the infero-medial all without external cuts. It is a safe procedure for the treatment of thyroid orbitopathy, bearing less morbidity, avoiding lesions to the nasolacrimal and nasofrontal duct, or the infraorbitary nerve, allowing a proptosis reduction of 3 to 4 mm. This technique allows a maximum decompression of the orbital apex in cases or orbital neuropathy. However, it is necessary to have a trained surgeon in order to achieve good results and avoid complications. REFERENCES 1. Weetman AP. Thyroid-associated eye disease: Pathophysiology. Lancet 1991; 338: Mc Cord Jr CD. Current trends in orbital decompression. Ophthalmology 1985; 92: Naffizer HC. Progressive exophathalmos following thyroidectomy: Its pathology and treatment. Ann Surg 1931; 94: Michel O. Endoskopish kontrolierte endonasale orbitadekompression beim malignen ophtalmus. Laryngorhinootologie 1991; 70: Shorr N, Baylis HI. Ocular motility problems after orbital decompression for disthyroid ophthalmopathy. Ophthalmology 1982; 89: 286
5 Mc Cord Jr CD. Orbital decompression for Graves disease: Exposure through lateral canthal and inferior fornix incision. Ophthalmology 1981; 88: Walsh TE, Ogura JH. Transantral orbital decompression for malignant exophtalmos. Laryngoscope 1957; 67: Hirsch O. Surgical decompression of exophthalmos. Arch Otolaryngol Head Neck Surg 1950; 51: Sewall EC. Operative control of progressive exophthalmos. Arch Otolaryngol Head Neck Surg 1936; 24: Kennedy DW, Goodstein MZ, Miller NR, Zinreich SJ. Endoscopic transnasal orbital decompression. Arch Otolaryngol Head Neck Surg 1990; 116: Kennedy DW. Functional endoscopic sinus surgery technique. Arch Otolaryngol Head Neck Surg 1985; 111: Lund VJ, Adams G. Orbital decompression for thyroid eye disease: a comparison of external and endoscopic techniques. J Laryngol Otol 1997; 111: Metson R, Shore JW. Endoscopic orbital decompression. Laryngoscope 1994; 104: Henrich DH, Kennedy DW. Endoscopic orbital decompression - Graves disease. In: Stankiewcz JA. Advanced Endocopic Sinnus Surgery. St Louis: Mosby; p Sacks EH, Anand VK, Lisman RD. Orbital decompression: Endoscopic perspective. In: Anand VK, Panje ER. Practical Endoscopic Sinnus Surgery. New York: Mc Graw-Hill; p Hwang PH, Kennedy DW. Endoscopic transnasal orbital decompression. In: Stamm Ac & Draf W. Micro-Endoscopic Surgery of the Paranasal Sinuses And the Skull Base Springer Berlin; p Luxenberger W, Stammberger H, Jebeles JA, Walch C. Endoscopic optic nerve decompression: The Graz experience. The Laryngoscope 1998; 108: De Santo LW. The total rehabilitation of Graves ophthalmopathy. Laryngoscope 1980; 90:
Rhinosinusitis is a severe sickness and may have serious
 Rev Bras Otorrinolaringol 2007;73(5):684-8. ORIGINAL ARTICLE Orbital complications of acute rhinosinusitis: a new classification Antonio Augusto Velasco e Cruz 1, Ricardo Cassiano Demarco 2, Fabiana Cardoso
Rev Bras Otorrinolaringol 2007;73(5):684-8. ORIGINAL ARTICLE Orbital complications of acute rhinosinusitis: a new classification Antonio Augusto Velasco e Cruz 1, Ricardo Cassiano Demarco 2, Fabiana Cardoso
Endoscopic transnasal orbital decompression for thyrotoxic orbitopathy
 Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy
 Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
ORBIT/OPTIC NERVE DECOMPRESSION HISTORICAL PERSPECTIVE
 ORBIT AND OPTIC NERVE DECOMPRESSION Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College HISTORICAL PERSPECTIVE NORMAL AND
ORBIT AND OPTIC NERVE DECOMPRESSION Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College HISTORICAL PERSPECTIVE NORMAL AND
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
PROBLEM RECOMMENDATION
 PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
Mucocele of paranasal sinuses
 From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
Surgery for Exophthalmos
 Surgery for Exophthalmos Frederick S. Rosen, MD, Faculty Advisor: Matthew W. Ryan, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation April 7, 2004 1 Introduction
Surgery for Exophthalmos Frederick S. Rosen, MD, Faculty Advisor: Matthew W. Ryan, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation April 7, 2004 1 Introduction
Transnasal endoscopic approach in the treatment of Graves ophthalmopathy: The value of a medial periorbital strip
 European Annals of Otorhinolaryngology, Head and Neck diseases (2010) 127, 97 103 ORIGINAL CLINICAL RESEARCH Transnasal endoscopic approach in the treatment of Graves ophthalmopathy: The value of a medial
European Annals of Otorhinolaryngology, Head and Neck diseases (2010) 127, 97 103 ORIGINAL CLINICAL RESEARCH Transnasal endoscopic approach in the treatment of Graves ophthalmopathy: The value of a medial
Case Presentation: Indications for orbital decompression in TED: Modern surgical techniques for orbital decompression in TED: Inferomedial
 Case Presentation: Jonathan W. Kim, MD Director, Oculoplastic Surgery Stanford Medical Center 61 year old man with active Graves orbitopathy Visual acuity 20/30 OD 20/50 OS Left RAPD Bilateral optic disc
Case Presentation: Jonathan W. Kim, MD Director, Oculoplastic Surgery Stanford Medical Center 61 year old man with active Graves orbitopathy Visual acuity 20/30 OD 20/50 OS Left RAPD Bilateral optic disc
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
Orbital facia. Periororbital facia Orbital septum Bulbar facia Muscular facia
 Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study
 Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Radiological anatomy of frontal sinus By drtbalu
 2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Transnasal Endoscopic Sinonasal Surgery
 Reda kamel, Cadaveric dissection 1 Transnasal Endoscopic Sinonasal Surgery Cadaver Dissection Guide For Endoscopic Sinus Surgery Cairo University Egypt Reda Kamel Professor of Rhinology Cairo University
Reda kamel, Cadaveric dissection 1 Transnasal Endoscopic Sinonasal Surgery Cadaver Dissection Guide For Endoscopic Sinus Surgery Cairo University Egypt Reda Kamel Professor of Rhinology Cairo University
Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus surgery
 Int J Clin Exp Med 2016;9(6):10317-10321 www.ijcem.com /ISSN:1940-5901/IJCEM0025371 Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus
Int J Clin Exp Med 2016;9(6):10317-10321 www.ijcem.com /ISSN:1940-5901/IJCEM0025371 Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus
Anatomical variations of the sphenopalatine foramen
 Braz J Otorhinolaryngol 2009;75(1):37-41. original article Anatomical study of the sphenopalatine foramen Adriana Bernardini Antunes Scanavine 1, João Adolfo Caldas Navarro 2, Silvia Regina Molinari de
Braz J Otorhinolaryngol 2009;75(1):37-41. original article Anatomical study of the sphenopalatine foramen Adriana Bernardini Antunes Scanavine 1, João Adolfo Caldas Navarro 2, Silvia Regina Molinari de
Ophthalmic complications after surgery for nasal and sinus polyposis
 European Journal of Ophthalmology / Vol. 11 no. 3, 2001 / pp. 218-222 Ophthalmic complications after surgery for nasal and sinus polyposis P. VASSALLO, F. TRANFA, R. FORTE, A. D APONTE, D. STRIANESE, G.
European Journal of Ophthalmology / Vol. 11 no. 3, 2001 / pp. 218-222 Ophthalmic complications after surgery for nasal and sinus polyposis P. VASSALLO, F. TRANFA, R. FORTE, A. D APONTE, D. STRIANESE, G.
Surgery for Exophthalmos April 2004
 TITLE: Surgery for Exophthalmos SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 7, 2004 RESIDENT PHYSICIAN: Frederick S. Rosen, MD FACULTY ADVISOR: Matthew W. Ryan, MD SERIES
TITLE: Surgery for Exophthalmos SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 7, 2004 RESIDENT PHYSICIAN: Frederick S. Rosen, MD FACULTY ADVISOR: Matthew W. Ryan, MD SERIES
Pathophysiology. Surgery for Exophthalmos April 2000
 TITLE: Surgery for Exophthalmos SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 2000 RESIDENT PHYSICIAN: Stephanie Cordes, MD FACULTY ADVISOR: Karen Calhoun, MD SERIES EDITOR:
TITLE: Surgery for Exophthalmos SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: April 2000 RESIDENT PHYSICIAN: Stephanie Cordes, MD FACULTY ADVISOR: Karen Calhoun, MD SERIES EDITOR:
Frontal sinus disease continues to be one of the great
 Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Boundaries Septum Turbinates & Meati Lamellae Drainage Pathways Variants
 The Fastest 20 Minutes in Michelle A. Michel, MD Professor of Radiology and Otolaryngology Medical College of Wisconsin, Milwaukee Overview Nasal cavity Anterior skull base Ostiomeatal complex Frontal
The Fastest 20 Minutes in Michelle A. Michel, MD Professor of Radiology and Otolaryngology Medical College of Wisconsin, Milwaukee Overview Nasal cavity Anterior skull base Ostiomeatal complex Frontal
Reasons for Failure and Surgical Revisions. Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology
 Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
Functional Endoscopic Sinus Surgery
 WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
The surgical approach to the sphenoid sinus continues to
 A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
Skull Base Danger Zones in FESS
 Skull Base Danger Zones in FESS Poster No.: C-2278 Congress: ECR 2014 Type: Educational Exhibit Authors: L. Renza Lozada, R. Carreño Gonzalez, G. Quintana Sanchez, 1 2 1 1 1 2 R. E. Figueroa ; Malaga/ES,
Skull Base Danger Zones in FESS Poster No.: C-2278 Congress: ECR 2014 Type: Educational Exhibit Authors: L. Renza Lozada, R. Carreño Gonzalez, G. Quintana Sanchez, 1 2 1 1 1 2 R. E. Figueroa ; Malaga/ES,
Communication issue - What should the radiologist report before functional endoscopic sinus surgery
 Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
James A. Garrity MD Department of Ophthalmology. Marius N. Stan MD Division of Endocrinology. Mayo Clinic Rochester, MN
 James A. Garrity MD Department of Ophthalmology Marius N. Stan MD Division of Endocrinology Mayo Clinic Rochester, MN Epidemiologic and diagnostic considerations for Graves orbitopathy (GO) 1. How common?
James A. Garrity MD Department of Ophthalmology Marius N. Stan MD Division of Endocrinology Mayo Clinic Rochester, MN Epidemiologic and diagnostic considerations for Graves orbitopathy (GO) 1. How common?
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery
 V Narendrakumar, V Subramanian Original article 10.5005/jp-journals-10013-1259 Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery 1 V Narendrakumar,
V Narendrakumar, V Subramanian Original article 10.5005/jp-journals-10013-1259 Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery 1 V Narendrakumar,
Intranasal location of lacrimal sac in Thai cadavers
 Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
ORIGINAL ARTICLE. Intranasal Localization of the Lacrimal Sac
 ORIGINAL ARTICLE Intranasal Localization of the Lacrimal Sac Mustafa Orhan, MD; Canan Y. Saylam, MD; Raşit Midilli, MD Objective: To optimize the approach to the lacrimal sac during intranasal dacryocystorhinostomy.
ORIGINAL ARTICLE Intranasal Localization of the Lacrimal Sac Mustafa Orhan, MD; Canan Y. Saylam, MD; Raşit Midilli, MD Objective: To optimize the approach to the lacrimal sac during intranasal dacryocystorhinostomy.
Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550013 Volume 1, Issue 3 Case Report Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report Peter Catalano, MD * and Michael
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550013 Volume 1, Issue 3 Case Report Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report Peter Catalano, MD * and Michael
Orbital and Ocular Adnexal Disorders with Red Eyes
 Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS
 From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
1. BRIEF DESCRIPTION OF TRAINING
 RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
Proptosis due to otolaryngology causes a study
 From the SelectedWorks of Balasubramanian Thiagarajan March 29, 2013 Proptosis due to otolaryngology causes a study Balasubramanian Thiagarajan Srikamakshi Kothandaraman Available at: https://works.bepress.com/drtbalu/11/
From the SelectedWorks of Balasubramanian Thiagarajan March 29, 2013 Proptosis due to otolaryngology causes a study Balasubramanian Thiagarajan Srikamakshi Kothandaraman Available at: https://works.bepress.com/drtbalu/11/
Graves Ophthalmopathy Overview. Graves Disease Hyperthyroidism TSIgs (anti-tsh-receptor-abs) Graves Disease 10/22/2010
 Graves Disease Robert Graves Graves Ophthalmopathy Overview Robert C. Kersten Dept. of Ophthalmology UCSF Triad Hyperthyroidism Eye findings Pretibial Myxedema (phalangeal acropachy-1%) Most common auto-immune
Graves Disease Robert Graves Graves Ophthalmopathy Overview Robert C. Kersten Dept. of Ophthalmology UCSF Triad Hyperthyroidism Eye findings Pretibial Myxedema (phalangeal acropachy-1%) Most common auto-immune
ORIGINAL ARTICLE. Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the Anterior Ethmoid
 Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
A comprehensive study on complications of endoscopic sinus surgery
 International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
Chapter Five. 1 of 8 11/3/2008 2:52 PM.
 1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
JMSCR Vol 05 Issue 09 Page September 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
Three-Dimensional Volumetric Display of the Nasal Ostiomeatal Channels and Paranasal Sinuses
 Downloaded from www.ajronline.org by 37.44.202.192 on 12/22/17 from IP address 37.44.202.192. Copyright RRS. For personal use only; all rights reserved Three-Dimensional Volumetric Display of the Nasal
Downloaded from www.ajronline.org by 37.44.202.192 on 12/22/17 from IP address 37.44.202.192. Copyright RRS. For personal use only; all rights reserved Three-Dimensional Volumetric Display of the Nasal
Computed tomography road map of the paranasal sinuses for treatment planning
 Computed tomography road map of the paranasal sinuses for treatment planning Poster No.: C-2607 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Schembri, A. S. Gatt, D. Ellul, J. Brunton; Dundee/UK
Computed tomography road map of the paranasal sinuses for treatment planning Poster No.: C-2607 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Schembri, A. S. Gatt, D. Ellul, J. Brunton; Dundee/UK
Study of success rates in endoscopic dacryocystorhinostomy with and without stenting. dacryocystorhinostomy with and
 Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities
 10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
13/02/1440 بسم ا هلل ا لرحمن ا لر حيم
 بسم ا هلل ا لرحمن ا لر حيم 1 Slowly progressive versus rapidly progressive proptosis by Ali M ISMAIL professor of ophthalmology @SOHAG U H Occuloplastic fellow @NNUH Occuloplastic fellow @Cambridge UH
بسم ا هلل ا لرحمن ا لر حيم 1 Slowly progressive versus rapidly progressive proptosis by Ali M ISMAIL professor of ophthalmology @SOHAG U H Occuloplastic fellow @NNUH Occuloplastic fellow @Cambridge UH
! Women greater than men (4:1)» Typical of other autoimmune diseases
 1 2 3 4 : Overview and Diagnosis Suzanne K. Freitag, M.D. Director, Ophthalmic Plastic Surgery Massachusetts Eye and Ear Infirmary Harvard Medical School! I have no financial disclosures. Learning Objectives!
1 2 3 4 : Overview and Diagnosis Suzanne K. Freitag, M.D. Director, Ophthalmic Plastic Surgery Massachusetts Eye and Ear Infirmary Harvard Medical School! I have no financial disclosures. Learning Objectives!
Lids and Orbits A Patient s Perspective. Dr. Paul Cauchi Consultant Ophthalmologist Southern General and Gartnavel General Hospitals, Glasgow
 Lids and Orbits A Patient s Perspective Dr. Paul Cauchi Consultant Ophthalmologist Southern General and Gartnavel General Hospitals, Glasgow Overview Pathophsiology. Symptoms. Signs. Management. Pathophysiology
Lids and Orbits A Patient s Perspective Dr. Paul Cauchi Consultant Ophthalmologist Southern General and Gartnavel General Hospitals, Glasgow Overview Pathophsiology. Symptoms. Signs. Management. Pathophysiology
1 st International Advanced Sinus Dissection Course, 30 th - 31 st March 2017, Berlin. in Berlin
 1 st International Advanced Sinus Dissection Course, 30 th - 31 st March 2017, Berlin in Berlin Dear colleagues, We are very happy to invite you to the 1 st International Advanced Sinus Dissection Course
1 st International Advanced Sinus Dissection Course, 30 th - 31 st March 2017, Berlin in Berlin Dear colleagues, We are very happy to invite you to the 1 st International Advanced Sinus Dissection Course
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis
 Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
CT OF THE PARANASAL SINUSES : NORMAL ANATOMY, VARIANTS AND PATHOLOGY
 Journal of Optoelectronics and Biomedical Materials Vol.2 Issue 4, October-December 2010, p. 281 289 CT OF THE PARANASAL SINUSES : NORMAL ANATOMY, VARIANTS AND PATHOLOGY AMIT N D DWIVEDI *, KAPIL KUMAR
Journal of Optoelectronics and Biomedical Materials Vol.2 Issue 4, October-December 2010, p. 281 289 CT OF THE PARANASAL SINUSES : NORMAL ANATOMY, VARIANTS AND PATHOLOGY AMIT N D DWIVEDI *, KAPIL KUMAR
Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Mucoceles of the paranasal sinus are epithelial lesions
 Rev Bras Otorrinolaringol. V.70, n.6, 850-4, nov./dec. 2004 ARTIGO DE REVISÃO CASE REPORT Frontoethmoidal mucoceles: a case report and literature review Andy de Oliveira Vicente 1, Adriana Gonzaga Chaves
Rev Bras Otorrinolaringol. V.70, n.6, 850-4, nov./dec. 2004 ARTIGO DE REVISÃO CASE REPORT Frontoethmoidal mucoceles: a case report and literature review Andy de Oliveira Vicente 1, Adriana Gonzaga Chaves
Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases.
 Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases. Akeem O Lasisi* and Aderemi A Adeosun Department of Otorhinolaryngology College of Medicine, University
Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases. Akeem O Lasisi* and Aderemi A Adeosun Department of Otorhinolaryngology College of Medicine, University
Skull Base Volume 12 Month. Patients. Anterior/Midline. Pituitary CSF Leak. Lateral. Craniocervical Junction
 UC SF 2 11/7/2009 Skull Base Surgery in 2009 Ivan El-Sayed MD, FACS Director- Otolaryngology Minimally Invasive Skull Base Surgery Program Department Otolaryngology-Head and Neck Surgery University of
UC SF 2 11/7/2009 Skull Base Surgery in 2009 Ivan El-Sayed MD, FACS Director- Otolaryngology Minimally Invasive Skull Base Surgery Program Department Otolaryngology-Head and Neck Surgery University of
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Imaging of the Paranasal Sinuses
 14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
ORIGINAL ARTICLE RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS.
 RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS. Shrikrishna B H 1, Jyothi A C 2, Sanjay G 3, Sandeep Samson G 4. 1. Associate Professor, Department of
RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS. Shrikrishna B H 1, Jyothi A C 2, Sanjay G 3, Sandeep Samson G 4. 1. Associate Professor, Department of
The advent of high-resolution computerized tomography
 An anatomic classification of the ethmoidal bulla REUBEN C. SETLIFF, III, MD, PETER J. CATALANO, MD, FACS, LISA A. CATALANO, MPH, and CHAD FRANCIS, BA, Sioux Falls, South Dakota, and Burlington, Massachusetts
An anatomic classification of the ethmoidal bulla REUBEN C. SETLIFF, III, MD, PETER J. CATALANO, MD, FACS, LISA A. CATALANO, MPH, and CHAD FRANCIS, BA, Sioux Falls, South Dakota, and Burlington, Massachusetts
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA
 ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
ENDOSCOPIC ENDONASAL SURGERY FOR RESECTION OF BENIGN SINONASAL TUMORS: EXPERIENCE WITH 107 PATIENTS
 Arch Iranian Med 2006; 9 (3): 244 249 Original Article ENDOSCOPIC ENDONASAL SURGERY FOR RESECTION OF BENIGN SINONASAL TUMORS: EXPERIENCE WITH 107 PATIENTS Mohammad-Hossein Baradaranfar MD, Payman Dabirmoghaddam
Arch Iranian Med 2006; 9 (3): 244 249 Original Article ENDOSCOPIC ENDONASAL SURGERY FOR RESECTION OF BENIGN SINONASAL TUMORS: EXPERIENCE WITH 107 PATIENTS Mohammad-Hossein Baradaranfar MD, Payman Dabirmoghaddam
Imaging Anatomy in Revision Sinus Surgery
 Chapter 1 Imaging Anatomy in Revision Sinus Surgery Ramon E. Figueroa 1 Core Messages An intimate knowledge of sinus anatomy and a clear understanding of the baseline postsurgical anatomy are required
Chapter 1 Imaging Anatomy in Revision Sinus Surgery Ramon E. Figueroa 1 Core Messages An intimate knowledge of sinus anatomy and a clear understanding of the baseline postsurgical anatomy are required
Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q
 The British Association of Plastic Surgeons (2004) 57, 37 44 Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q M. Kakibuchi*,
The British Association of Plastic Surgeons (2004) 57, 37 44 Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q M. Kakibuchi*,
Professor Dr.Muhammad Ajmal Dr.Tehmina Nazir. HOLY FAMILY HOSPITAL Rawalpindi
 Professor Dr.Muhammad Ajmal Dr.Tehmina Nazir HOLY FAMILY HOSPITAL Rawalpindi SCHEME OF PRESENTATION PLAIN X-RAYS CT SCAN MRI CONCLUSION IMAGING MODALITIES PLAIN X-RAYS CT SCAN MRI OCCIPITOMENTAL/WATER
Professor Dr.Muhammad Ajmal Dr.Tehmina Nazir HOLY FAMILY HOSPITAL Rawalpindi SCHEME OF PRESENTATION PLAIN X-RAYS CT SCAN MRI CONCLUSION IMAGING MODALITIES PLAIN X-RAYS CT SCAN MRI OCCIPITOMENTAL/WATER
Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision
 THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
Katya A. Shpilberg 1 Simon C. Daniel 1 Amish H. Doshi 1 William Lawson 2 Peter M. Som 1. Neuroradiology/Head and Neck Imaging Original Research
 Neuroradiology/Head and Neck Imaging Original Research Shpilberg et al. CT of Paranasal Sinuses and Nasal Cavity Neuroradiology/Head and Neck Imaging Original Research Katya A. Shpilberg 1 Simon C. Daniel
Neuroradiology/Head and Neck Imaging Original Research Shpilberg et al. CT of Paranasal Sinuses and Nasal Cavity Neuroradiology/Head and Neck Imaging Original Research Katya A. Shpilberg 1 Simon C. Daniel
Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective
 ORIGINAL ARTICLE Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective 1 Dhingra Shruti, 2 Agarwal AK, 3 Passey JC, 4 Kaul JM 1 Resident, Department of Otolaryngology
ORIGINAL ARTICLE Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective 1 Dhingra Shruti, 2 Agarwal AK, 3 Passey JC, 4 Kaul JM 1 Resident, Department of Otolaryngology
Major orbital complications of endoscopic sinus surgery
 598 Moorfields Eye Hospital, London EC1V 2PD, UK C Rene G E Rose R Lenthall I Moseley Correspondence to: Mr G E Rose, Orbital Clinic, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK Accepted 20
598 Moorfields Eye Hospital, London EC1V 2PD, UK C Rene G E Rose R Lenthall I Moseley Correspondence to: Mr G E Rose, Orbital Clinic, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK Accepted 20
Nasal region. cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?
 Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY INFERIOR MAXILLECTOMY Tumours of the hard palate and superior alveolus may be resected by inferior maxillectomy (Figure 1). A Le Fort
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY INFERIOR MAXILLECTOMY Tumours of the hard palate and superior alveolus may be resected by inferior maxillectomy (Figure 1). A Le Fort
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY
 COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
Conventional Sinus Surgery Vs Fess
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K.
 05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
Ophthalmic Manifestations in ENT Diseases & Surgical Procedures
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 11, Issue 4 (Nov.- Dec. 2013), PP 87-92 Ophthalmic Manifestations in ENT Diseases & Surgical Procedures
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 11, Issue 4 (Nov.- Dec. 2013), PP 87-92 Ophthalmic Manifestations in ENT Diseases & Surgical Procedures
Variation in frontal cells in relation to chronic frontal sinusitis
 International Journal of Current Research in Medical Sciences ISSN: 244-71 P-ISJN: A472-04, E -ISJN: A472-01 www.ijcrims.com Original Research Article Volume, Issue 1-2019 DOI: http://dx.doi.org/10.22192/ijcrms.2019.0.01.00
International Journal of Current Research in Medical Sciences ISSN: 244-71 P-ISJN: A472-04, E -ISJN: A472-01 www.ijcrims.com Original Research Article Volume, Issue 1-2019 DOI: http://dx.doi.org/10.22192/ijcrms.2019.0.01.00
January th, 2012
 Basic Endoscopic Sinus Surgery for Residents & Novices and 1st International Advanced Course in Endoscopic Sinus Surgery & Skull Base Surgery January 17-20 th, 2012 January 17 th, 2012: Basic Endoscopic
Basic Endoscopic Sinus Surgery for Residents & Novices and 1st International Advanced Course in Endoscopic Sinus Surgery & Skull Base Surgery January 17-20 th, 2012 January 17 th, 2012: Basic Endoscopic
Contemporary cohort cross-sectional study. Introduction:
 Rev Bras Otorrinolaringol 2008;74(2):207-12. original article Histological Aspects of Rhinosinusal Polyps Luciano Gustavo Ferreira Couto 1, Atílio Maximino Fernades 2, Daniel Ferracioli Brandão 3, Dalisio
Rev Bras Otorrinolaringol 2008;74(2):207-12. original article Histological Aspects of Rhinosinusal Polyps Luciano Gustavo Ferreira Couto 1, Atílio Maximino Fernades 2, Daniel Ferracioli Brandão 3, Dalisio
Case Report Transnasal, Transethmoidal Endoscopic Removal of a Foreign Body in the Medial Extraconal Orbital Space
 Volume 2016, Article ID 1981456, 4 pages http://dx.doi.org/10.1155/2016/1981456 Case Report Transnasal, Transethmoidal Endoscopic Removal of a Foreign Body in the Medial Extraconal Orbital Space Diego
Volume 2016, Article ID 1981456, 4 pages http://dx.doi.org/10.1155/2016/1981456 Case Report Transnasal, Transethmoidal Endoscopic Removal of a Foreign Body in the Medial Extraconal Orbital Space Diego
CT of Maxillofacial Fracture Patterns. CT of Maxillofacial Fracture Patterns
 CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
Maxilla, ORBIT and infratemporal fossa. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion
 THIEME Case Report e105 Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion Paolo Castelnuovo, MD 1,4 Giacomo Fiacchini, MD 2 Francesca Romana Fiorini, MD 3 Iacopo Dallan,
THIEME Case Report e105 Push Pull Technique for the Management of a Selected Superomedial Intraorbital Lesion Paolo Castelnuovo, MD 1,4 Giacomo Fiacchini, MD 2 Francesca Romana Fiorini, MD 3 Iacopo Dallan,
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013
 FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis
 Otolaryngology Head and Neck Surgery (2006) 134, 28-32 ORIGINAL RESEARCH A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis Roee Landsberg, MD, Yoram Segev, MD, Michael Friedman, MD,
Otolaryngology Head and Neck Surgery (2006) 134, 28-32 ORIGINAL RESEARCH A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis Roee Landsberg, MD, Yoram Segev, MD, Michael Friedman, MD,
Anatomy of the orbit. Lay-out. Imaging technique. 3 x 3. brief overview of the basic anatomy of the orbit and its structures
 Anatomy of the orbit Prof. Pia C Sundgren MD, PhD Department of Diagnostic Radiology, Clinical Sciences, Lund University, Sweden Lay-out brief overview of the basic anatomy of the orbit and its structures
Anatomy of the orbit Prof. Pia C Sundgren MD, PhD Department of Diagnostic Radiology, Clinical Sciences, Lund University, Sweden Lay-out brief overview of the basic anatomy of the orbit and its structures
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Anatomic Relations Summary. Done by: Sohayyla Yasin Dababseh
 Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
PRINCIPLES OF ENDOSCOPIC MANAGEMENT OF NASAL AND. Frontier Steven D. Schaefer, MD, FACS
 PRINCIPLES OF ENDOSCOPIC MANAGEMENT OF NASAL AND SKULL : A New Frontier Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York keye and dear Infirmary New York Medical College
PRINCIPLES OF ENDOSCOPIC MANAGEMENT OF NASAL AND SKULL : A New Frontier Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York keye and dear Infirmary New York Medical College
ORIGINAL ARTICLE. Endoscopic ligation of the anterior ethmoidal artery: a cadaver dissection study
 Braz J Otorhinolaryngol. 2011;77(1):33-8. ORIGINAL ARTICLE BJORL Endoscopic ligation of the anterior ethmoidal artery: a cadaver dissection study Bernardo Cunha Araujo Filho 1, Carlos Diógenes Pinheiro-Neto
Braz J Otorhinolaryngol. 2011;77(1):33-8. ORIGINAL ARTICLE BJORL Endoscopic ligation of the anterior ethmoidal artery: a cadaver dissection study Bernardo Cunha Araujo Filho 1, Carlos Diógenes Pinheiro-Neto
FESS imaging - the role of MDCT
 FESS imaging - the role of MDCT Poster No.: C-0179 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Plascak, K. Makaruha, B. Klasic, L. Kavur, V. Vidjak; Zagreb/HR Keywords: Image verification,
FESS imaging - the role of MDCT Poster No.: C-0179 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Plascak, K. Makaruha, B. Klasic, L. Kavur, V. Vidjak; Zagreb/HR Keywords: Image verification,
Research Article Length and Geometric Patterns of the Greater Palatine Canal Observed in Cone Beam Computed Tomography
 International Dentistry Volume 2010, Article ID 292753, 6 pages doi:10.1155/2010/292753 Research Article Length and Geometric Patterns of the Greater Palatine Canal Observed in Cone Beam Computed Tomography
International Dentistry Volume 2010, Article ID 292753, 6 pages doi:10.1155/2010/292753 Research Article Length and Geometric Patterns of the Greater Palatine Canal Observed in Cone Beam Computed Tomography
CT of Maxillofacial Injuries
 CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
The sebaceous glands (glands of Zeis) open directly into the eyelash follicles, ciliary glands (glands of Moll) are modified sweat glands that open
 The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
