Mohammad. Renad zakaria ---
|
|
|
- Melissa Paul
- 6 years ago
- Views:
Transcription
1 13 Mohammad Renad zakaria ---
2 Before we start: - I didn t follow the record order, for organizing purposes. - I added extra information from our text box which is Guyton 12 th edition, pages , actually I did so because I felt it needed (since there are things that needed further explanation) so pardon me. - You will find some information in the slides not mention here, so you need to go through them. - I hope you find this sheet easy to understand, it s a difficult one so I tried my best to make it simple so wish you all the best. In the previous lecture: - We talked about male and female reproductive systems in general and we went through some differences between them, in this lecture we may mention some differences. - In females, we said that the oocyte start as oogonia in the uterine life, then this oocyte will sleep (mostly they will degenerate) for at least 10 years (until puberty). When the puberty state initiate, there will be recruitment of the primordial follicles that will end in production of oocyte. Primordial follicle consists of an oocyte surrounded by a single layer of flat, supporting granulosa cells In our lecture we will go through and talk about 3 temporary endocrine glands which haven t consistent pattern of secretions but they are growing, increasing then they will degenerate and because of that we have certain changes in secretions concentration so the homeostasis won t be in the daily basis within a large concept. - Lets carry on what we were talking about in the previous lecture, In general: Somehow when reaching the puberty state we will have developmental aspect of hypothalamic- pituitary (don t mind this now), so more important we end up having follicle stimulating hormone (FSH), this hormone will initiate the recruitment of the primordial germ cells. These follicles will grow until they ovulate and release the oocyte, the oocyte will be picked by the fimbriated end of the fallopian tube and will go through it. 1 P a g e
3 - Also in the previous lecture we said that the primordial follicle has the original oogonia that will give the destined oocyte. We also talked about how the numbers of the follicles decrease in the intrauterine life and the developmental stage. **Let s talk about some histology just for understanding purposes, in adult female, the ovary look like: Figure 1: - The ovary has cortical and medullary areas. - If you look at the cortex you will notice it s just a few millimeters and inside it you will find all primordial germ cells. - So in the core of the ovary ovary you won t see any germ cells since they all reside in the cortex. For explaining purposes please read this extra piece of information: During fetal life, the outer surface of the ovary is covered by a germinal epithelium, which embryologically is derived from the epithelium of the germinal ridges. As the female fetus develops, primordial ova differentiate from this germinal epithelium and migrate into the substance of the ovarian cortex. Each ovum then collects around it a layer of spindle cells from the ovarian stroma (the supporting tissue of the ovary) and causes them to take on epithelioid characteristics; they are then called granulosa cells. The ovum surrounded by a single layer of granulosa cells is called a primordial follicle. The ovum at this stage is still immature, requiring two more cell divisions before it can be fertilized by a sperm. At this time, the ovum is called a primary oocyte. After this primordial follicle stimulated by FSH and then follows growth of additional layers of granulosa cells in some of the follicles; these follicles are known as primary follicles. Guyton. Ch 81, page 987,989 2 P a g e
4 ** So how we start this recruitment? Let s go through the details... - keep in mind that in oogenesis we primary concern about the oocyte but don t neglect the importance of what surrounding the oocyte, this crosstalk is all needed to develop the follicle and we define this crosstalk by maturation. So all the things that we will discuss for now concern to the follicle not the oocyte, be careful!! ** After puberty, the pituitary gland start to secrete FSH in certain concentration that will stimulate certain development on the primordial follicle, it will awaken the oocyte and stimulate the layer around it. These surrounding layers start to develop in term of mitosis and have the ability to secrete some hormones like estrogen which named granulosa cells. FSH, secreted from the anterior pituitary gland, and cause accelerated growth of 6 to 12 primary follicles each month (recruitment). The initial effect is rapid proliferation of the granulosa cells, giving rise to many more layers of these cells and so more estrogen production. Such effect last from 5-14 days. - The functions of FSH been tested by blocking it, so after such a test proceed there will be no more follicle recruitment. - The granulosa cells that have receptor for FSH and go under FSH stimulation produce estrogen, these cells are sensitive to their estrogen production so there is will be increasing in their mitotic function (estrogen by itself a strong mitotic element on these cells). - In the development and recruitment of the follicle there is a mass of cells that developed which named Theca; these cells are capable to produce androgens not estrogen!! So keep in mind the following: The granulosa (follicular) cells are the only ovarian cells that have FSH receptor. FSH produce estrogen from follicle. FSH with estrogen will promote the development of LH receptors on thecal and granulosa cell. So again, we said FSH works on producing estrogen, and LH works on thecal cells to produce androgen. 3 P a g e
5 Physiologically, After few days FSH concentration start to decline which cause reduction in the support of most of the follicles, so no more follicles development and only one follicle will continue to grow. ** But what if we give excess amount of exogenous FSH (pharmacological effect)? We will recruit more follicles and get them out of their primordial stage and maintain them. So in IVF (In Vitro Fertilization) we give FSH for 6-7 days and they maintain it. If we stop given FSH which is pharmacological not physiological there will decline in the follicle recruitment & maintenance. So what accelerate & increase follicles growth is the following: (1) Estrogen is secreted into the follicle and causes the granulosa cells to form increasing numbers of FSH receptors; this causes a positive feedback effect because it makes the granulosa cells even more sensitive to FSH. (2) The pituitary FSH and the estrogens combine to promote LH receptors on the original granulosa cells, thus allowing LH stimulation to occur in addition to FSH stimulation and creating an even more rapid increase in follicular secretion. (3) The increasing estrogens from the follicle plus the increasing LH from the anterior pituitary gland act together to cause proliferation of the follicular thecal cells and increase their secretion as well. ** After the early proliferative phase of growth, lasting for a few days, the mass of granulosa cells secretes a follicular fluid that contains a high concentration of estrogen, Accumulation of this fluid causes an antrum to appear within the mass of granulosa cells (we will have one space)so named the antral follicle, this is stimulated mainly by FSH. Once the antral follicles begin to grow, their growth occurs almost explosively, the ovum itself also enlarges. It s worth to know that estrogen have multiple sources for production: - We have androgens that secreted by adrenal cortex & ovarian thecal cells wich convert to estrogen in the granuluosa cells. - The granulosa cells of the ovaries also produce estrogen. 4 P a g e
6 - Most of this estrogen will go to circulation. ** So we end with rapidly rising pattern of estrogen concentration. ** Lets summarize all these steps as once: High FSH production follicle recruitment & proliferation multi layers of granulosa layers that produce estrogen and thecal cells that produce androgens formation of antral follicle enlargement of this follicle at the end on follicle will formed and the others will involute. If you are interested to know the mechanism of Atresia (which means the degeneration of those ovarian follicles which do not ovulate) and how just one follicle goes out, read page 990. Now let s compare it with the male reproductive system: In male we said that androgen producing from leydig cells, most of it will goes to the circulation and few of it goes to the serotoli cells. In serotoli cells we have small amount of estrogen secretion mainly for local use and most of goes to the circulaton, comparing to females. Let s carry on what we were talking about: So after formation of antral follicle it will increase in size (its diameter will increase up to 10 fold), this will increase pressure inside. Some of the secreted substance has proteolytic activity that lead to weak bond in the wall. The pressure, enlargement and weak bond in the wall all occur under the stimulation of FSH & LH. -The follicle phases are: Primordial follicle primary follicle antral follicle big antral follicle We can call this big follicle, pre ovulatory follicle or big graafian follicle - what will happen If we go to a certain stage where the follicle is around 5-6 millimeters and aspirate the oocyte? The oocyte will continue developing to further stages, when place it in vitro. 5 P a g e
7 **look at the figure below: Figure 2; shows: - Follicular development. - as we said earliar FSH recruit 6-12 follicles only one of them will go under the stages we mention and the other will degenerate, as you know decrease FSH is one of the causes for this to happen. Since the maintaining of FSH maintain the follicles. this is physiological - But if we give exogenous FSH, FSH will maintain and so as the follicle, so more than one follicle will survive & go through these stages. pharmacological effect Estrogen effect: In the blood circulation the levels of the estrogen vary day by day from low amount, high amount and then huge amount, last for 2-4 weeks but not less than 10 days. - The estrogen that enters the circulation will reach the hypothalamus and pituitary which induce the production mainly of FSH & LH, now we concerned more about LH. - We have two hypotheses that explain the mechanism which estrogen stimulates LH production, since we don t really know the mechanism: 1- Continuous progressive increase of exposure to estrogen will alter the responsiveness of the arcuate nucleus in the hypothalamus from suppression to stimulation. 2- We have certain nuclei in the hypothalamus found in deep sleep, but if they expose to continuous rising level of estrogen, they will response in positive feedback. These two hypotheses end in positive feedback in term of LH secretion due to continuous rising level of estrogen. - Such effect called estrogen induced LH surge effect. The increase of LH concentration will reach a certain level. 6 P a g e
8 So what are the effects of LH that increase in this positive feedback? 1-LH will stimulate the thecal cells for more androgen production, so we will end up with more estrogen production. 2- Makes changes in the follicle wall by forming weak bonds. 3- Cause follicle enlargement and increase the pressure inside. All of this will lead to follicle rupture and the release of the oocyte. ** I recommended reading pages 996 and 997 for more explanation on hypothalamus- pituitary relation and this positive feedback mechanism, it s really important to know since I can t put it all in the sheet. So all the things that we went through concern with the follicles not the oocyte, Remember when we said there is crosstalk between the oocyte and its rurrounding. We also explain the fuction of FSH and few about LH on the follicles. What secreted from these follicles needed for further development of the oocytee that concern with resuming the mitotic devision of the oocyte. Now let s go in details about oocyte development: Actually before start talking about it, remember what we took in the 1 st year with doctor Amjad that All eggs are arrested at an early stage (prophase I) of the first meiotic division as a primary oocyte (primordial follicle). Once the follicle rupture and release the oocyte, the first meiotic division takes place in the oocyte. It s important to know that ovulation start with this meiotic devision. If there is no follicle rupture there is no ovulation. - This 1 st meiotic division has criteria s which are: 1- A diploid cell becomes 2 haploid (23 chromosomes) daughter cells, each chromosome has two chromatids. One cell becomes the secondary oocyte the other cell forms the first polar body. 2- So it will give two cells, big one that has most of the cytoplasm (2 nd ry oocyte) and the other small cell has few cytoplasms (polar body). 7 P a g e
9 ## The polar body is a small cytoplasmic exclusion body formed to enclose the excess DNA formed during the oocyte (egg) meiosis and following sperm fertilization. - So the big cell (oocyte) will go out from the ovaries to the fallopian tube. The other cells are essential structure to the ovary. By now we end talking about the first endocrine gland which start from primordial follicle (recruitment) and end with its rupture (ovulation). Special characteristic of it is the progressive rapid increase of estrogen. Ovulation - We know that the typical menstrual cycle is 28 day, at day 14 the ovulation will occur. - And by now you also knew that follicular or proliferative phase (day 4 14). ** Let s review what we said before: The follicle before ovulation is growing under the effect of FSH This Graafian follicle will keep growing under the effect of FSH until part of its wall becomes thin then it will rupture releasing the ovum outside. ** Once the oocyte comes out from the ovary to the pelvic cavity, we have almost seization of all the secretion. The remaining granulosa and thecal cells will change rapidly. Such changes occur due to LH secretion. LH will stimulate these cells to increase their lipid material, cause acute enlargement of these cells and increase their vascularization. So we retain the capacity to produce the two hormones estrogen and progesterone (remember from the beginning we have the ability to produce estrogen). The whole process named luteinization. ** It s worth to know that these granulosa and thecal cells will transform to lutien cells, the total mass of these cells together named corpus luteum. ** In the previous lecture we said that progesterone is a precursor for estrogen, since it s a precursor for all steroid hormones. - The progesterone will be released to the circulation and some estrogen released outside. 8 P a g e
10 So what left in the ovaries will be: 1- Stimulated by ovulation. 2- Maintained by luteinizing hormone LH. 3- Increase secretion of estrogen and progesterone. 4- Change their structure for around 7-10 days then it will start to degenerate. - By 14 days from this, programmed cell deaths (apoptosis) take place and the cells die. - After the death of these cells, progesterone and estrogen level will reach zero. By now we end talking about the 2 nd endocrine gland that start by ovulation and ended by death. It s characterized by increase secretion of estrogen and progesterone. But what about the secondary oocyte with its polar body that completed the 1 st meiotic division? This oocyte surrounded by a cluster of granulosa cells and corona radiata and its polar body, It will survive for 16hours and maximum 24 h (it will live along with the polar body). After that it will degenerate, so degeneration of the oocyte takes place when it completed its1 st meiotic division. This occurs every month unless we have fertilization which will survive and complete the 2 nd meiotic division (that s not important now). ** The figure below summarizes all the stages: Figure 3 9 P a g e
11 ** Look at the figure below that shows the plasma concentrations of the hormones we were talking about; we will go in further details on each hormone: Figure 4 1- Estrogen; will rise (due to the mechanism we explained before) then decline when the apoptosis occur. Estrogen decline in small levels after ovulation since the granulose and thecal cells are no longer there after follicle rupture, so what maintain and keeps it production is the corpus luteum. 2- LH; will increase due to estrogen positive feedback. Then it will decrease suddenly, so it shunts from positive to negative feedback. As you see on the figure the LH increase with estrogen because of positive feedback. Essential for ovulation if not found we will have failure in ovulation. The reduction of LH caused by small amount of estrogen and to lesser extent by progesterone (negative feedback). Corpus luteum may also reduce it in such a mechanism. If you interested read page FSH; as you see in the figure also increase then decline especially after ovulation when follicle recruitment and maintain not needed. Its mechanism of decline follow the mechanism of LH declining. It s essential for development & recruitment of the follicles. 4- Progesterone; its rising level occur after ovulation as we said before. And its decline to the same reason of estrogen when the oocyte go through apoptosis. ** Then this cycle will repeat itself every month, started by increase FSH releasing. 10 P a g e
12 Figure 5;shows: - The different diameters of the follicles through its phases. - It starts with small diameter.1mm and end with follicle with big diameter which is 1 inch. - If we still have FSH, what recruited won t be degenerated. ** For an ovulation to occur we need: 1- LH. 2- Certain structure and volume. 3- Certain developmental pattern. If something wrong happen with one of them, the ovulation won t take place, where the oocyte won t leave the follicle and the follicle will stay in the ovary. Staying of the follicle in the ovary will develop disease such as cysts and tumors. ** In the previous lecture; we talked about FSH & LH regulation, such regulation happen through testerone regulate and inhbin that released from serotoli cells. That was in male reproductive system so what about females? We have what called mullerian inhibitory factor or anti mullerian hormone (AMH). This hormone produced from growing small to medium sized follicle, its FSH independent. AMH function, we don t its exact function but we suggest: It s a developmental marker for the follicle since its express the recruitment. If we have less recruitment and less small to medium size follicle, AMH concentration will be high. 11 P a g e
13 Figure 6; summarizes its function. It s Stable under various conditions like: OCP Pregnancy Menstrual cycle Remember; we said that there is a crosstalk between the oocyte and its surrounding. Actually there is multiple communications you just need what we took. So the take home message is that oocyte sense and receives messages from its surrounding. You need to know this communication is more complex than that but you need to know what we talked before. In the previous lecture we also talked about aromatase and its function and it secreted from serotoli cells in the males. Here in female system you will find aromatase in the granulosa cells which convert androgen to estrogen. Be aware there is no aromatase in thecal cells!! ** Now let s go through hormonal secretion once again: - Why we have rising in FSH & LH? We said that estrogen produced from corpus luteum level will decrease due to cell death, so because of that the inhibition effect of estrogen on LH & FSH will be released, so FSH level will increase. ** So what the time difference between LH surge and ovulation? In IVF, we give them human chorionic gonadotropin which is a glycoprotein that similar mainly to LH & lesser extent to FSH. Once we give it ovulation will take place after h. Physiologically; after the high level of natural LH, ovulation happen in less than one day. 12 P a g e
14 Figure 7: - The high level of FSH will recruit follicles and induce their development. - When the FSH level decrease, all the follicles will degenerate except on which will survive due to rapid increase in size, estrogen secretion and LH surge. - LH surge & FSH will induce ovulation as you see it does occur at the day This is the normal homeostasis, which occurs every month. * We have multi changes of these hormones during the month or in their daily basis, so if you find high level of FSH in certain time (after 17 days of the cycle for example), it will be abnormal and so on. ** With decreasing of estrogen and progesterone level, FSH and LH inhibition will decrease and we will start a rising pattern of FSH & LH to recruit more and new follicles. ** All the estrogen that produced in the follicles by thecal and granulosa cells will be used locally where all enzymes functioning (like aromatase in thecal cells for androgen). What produced from corpus luteum will go to the circulation and some of it will be converted to estrogen. Figure 8; shows: The synthesis of the steroidal hormone progesterone from cholesterol that converted to pregnenolone which will be converted finally to progesterone. 13 P a g e
15 Figure 9; summarizes all the ovarian and hormonal changes let s go through it briefly: The follicle recruitment and increasing of its size start by the stimulation of FSH. Then they start to be responsive to LH and secrete estrogen. Estrogen secretion come from the growing follicles (either thecal or granulosa cells) this rapid increase of estrogen will shift the hypothalamus from negative to positive feedback and we will end up with LH surge that will induce ovulation. No fertilization so the cell will die so will have estrogen suppress so no more activity. Then it will regain activity to produce estrogen and progesterone once more since it s a cycle. - don t mind the uterine cycle for now we will go through it in the next lectures. Figure 10; shows: The production of testosterone in males, Just to show the similarities with estrogen and progesterone. Leydig cells the same as thecal cell Seritoli cells the same as granulosa cell They have receptor for LH that will induce androgen production. They produce estrogen since they have aromatase 1 & P a g e
16 Now let s talk about estrogen and progesterone functions: - We have rising pattern of estrogen, so what its function? Inside the ovaries: 1- It will stimulate mitosis locally in the granulosa cells. 2- It will stimulate the positive feedback of LH. Outside the ovaries: 1- At puberty, increase in size of fallopian tubes, uterus and vagina, external genitalia deposition of fat in mons pubis. Also change vaginal epitheliafrom cuboidal to stratified type endometrium by increase their mitotic division and proliferation of cells and endometrial glands (important in nutrition of fertilized ovum). 2- Its increase the contractility of the uterus. And stimulate mitosis in the endometrial cells, so more cells production and more thickness, that will lead to high numbers of cells found far away from the base that supply them with nutrients and that will cause more capillary infiltration to supply these far cells. We end with decline in estrogen level so we start with estrogen and progesterone release. Progesterone function: 1- Anti estrogenic effect which reduce mitotic activity. 2- Greater metabolic effect on the endometrial cells. The endometrial cells start to produce glycoproteins, proteins and other secretary elements. So more blood flow and the capillaries will increase in length but in limited space, since it occurs in narrow space it will form coils so more blood supply. The endometrial layer increase in thickness due to high blood flow and secreted materials that mean it filled with fluid so we call it spongy endometrium. ** The progesterone level starts to decrease, so the metabolic effect on the endometrial cells starts to decrease. With no more estrogen and progesterone this layers lose its support and start to die. ** Once the endometrial cells die we will have sloughing and bleeding. This blood will leave through the vagina and the menstrual cycle start. Refer to figure 10 for full picture. The way I see it, every life is a pile of good things and bad things. The good things don t always soften the bad things, but vice versa, the bad things don t always spoil the good things and make them unimportant. _Doctor Who 15 P a g e
Chapter 27 The Reproductive System. MDufilho
 Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
Embryology Lecture # 4
 1 Quick Review: Oogenesis : - Oogonia start appear in the ovary when the age of the fetus 1 is th (5 week). - Then the Oogonia transformed into 1ry Oocyte. - 1ry Oocyte is surrounded by a follicle (cover).
1 Quick Review: Oogenesis : - Oogonia start appear in the ovary when the age of the fetus 1 is th (5 week). - Then the Oogonia transformed into 1ry Oocyte. - 1ry Oocyte is surrounded by a follicle (cover).
The reproductive lifespan
 The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
Female Reproductive System. Lesson 10
 Female Reproductive System Lesson 10 Learning Goals 1. What are the five hormones involved in the female reproductive system? 2. Understand the four phases of the menstrual cycle. Human Reproductive System
Female Reproductive System Lesson 10 Learning Goals 1. What are the five hormones involved in the female reproductive system? 2. Understand the four phases of the menstrual cycle. Human Reproductive System
10.7 The Reproductive Hormones
 10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
Reproductive Hormones
 Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Biology of Reproduction- Zool 346 Exam 2
 Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Investigation: The Human Menstrual Cycle Research Question: How do hormones control the menstrual cycle?
 Investigation: The Human Menstrual Cycle Research Question: How do hormones control the menstrual cycle? Introduction: The menstrual cycle (changes within the uterus) is an approximately 28-day cycle that
Investigation: The Human Menstrual Cycle Research Question: How do hormones control the menstrual cycle? Introduction: The menstrual cycle (changes within the uterus) is an approximately 28-day cycle that
Reproduction and Development. Female Reproductive System
 Reproduction and Development Female Reproductive System Outcomes 5. Identify the structures in the human female reproductive system and describe their functions. Ovaries, Fallopian tubes, Uterus, Endometrium,
Reproduction and Development Female Reproductive System Outcomes 5. Identify the structures in the human female reproductive system and describe their functions. Ovaries, Fallopian tubes, Uterus, Endometrium,
Physiology of Male Reproductive System
 Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
CASE 41. What is the pathophysiologic cause of her amenorrhea? Which cells in the ovary secrete estrogen?
 CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
Female Reproductive Physiology. Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF
 Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
9.4 Regulating the Reproductive System
 9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
Reproductive System. Testes. Accessory reproductive organs. gametogenesis hormones. Reproductive tract & Glands
 Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Embryology 3. Spermatogenesis:
 Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara
 Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara 1 Endocrine Control: Three Levels of Integration Hormones of the hypothalamic-anterior pituitary
Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara 1 Endocrine Control: Three Levels of Integration Hormones of the hypothalamic-anterior pituitary
Chapter 46 ~ Animal Reproduction
 Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes
 Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Two important cells in female are the theca cells and the granulose cells. Granulosa cells are affected by the two gonadotropin hormones; FSH and LH.
 1 UGS physiology sheet #13 lecture 3 Dr.Saleem Khresha. Now we will start discussing the female reproductive system Ovarian Steroids Two important cells in female are the theca cells and the granulose
1 UGS physiology sheet #13 lecture 3 Dr.Saleem Khresha. Now we will start discussing the female reproductive system Ovarian Steroids Two important cells in female are the theca cells and the granulose
Mohammad Sha ban. Basheq Jehad. Hamzah Nakhleh
 11 Mohammad Sha ban Basheq Jehad Hamzah Nakhleh Physiology of the reproductive system In physiology, we are concerned with the mechanisms in which the system functions, and how the system responds to different
11 Mohammad Sha ban Basheq Jehad Hamzah Nakhleh Physiology of the reproductive system In physiology, we are concerned with the mechanisms in which the system functions, and how the system responds to different
Hormonal Control of Human Reproduction
 Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
Web Activity: Simulation Structures of the Female Reproductive System
 differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
Reproductive Endocrinology. Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007
 Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
1. During the follicular phase of the ovarian cycle, the hypothalamus releases GnRH.
 1. During the follicular phase of the ovarian cycle, the hypothalamus releases GnRH. 2. This causes the anterior pituitary to secrete small quantities of FSH and LH. 3. At this time, the follicles in the
1. During the follicular phase of the ovarian cycle, the hypothalamus releases GnRH. 2. This causes the anterior pituitary to secrete small quantities of FSH and LH. 3. At this time, the follicles in the
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Chapter 22 The Reproductive System (I)
 Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Animal Science 434! Tonic and Preovulatory Surge of GnRH! Tonic and Preovulatory Surge of GnRH! Lecture 11: The Follicular Phase of the Estrous Cycle!
 Tonic and Preovulatory Surge of GnRH! Animal Science 434! Lecture 11: The Follicular Phase of the Estrous Cycle!! (-)! Hypothalamus! GnRH! Estradiol! (-)! Tonic and Preovulatory Surge of GnRH! Anterior!
Tonic and Preovulatory Surge of GnRH! Animal Science 434! Lecture 11: The Follicular Phase of the Estrous Cycle!! (-)! Hypothalamus! GnRH! Estradiol! (-)! Tonic and Preovulatory Surge of GnRH! Anterior!
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM
 Unit 7B STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the female reproductive tract. 2. Learn the functions of the female reproductive tract. 3.
Unit 7B STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the female reproductive tract. 2. Learn the functions of the female reproductive tract. 3.
Gametogenesis. Omne vivum ex ovo All living things come from eggs.
 Omne vivum ex ovo All living things come from eggs. William Harvery, 1651 Gametogenesis This lecture is the preface, so to speak, to embryology; that is, it introduces the development of the specialized
Omne vivum ex ovo All living things come from eggs. William Harvery, 1651 Gametogenesis This lecture is the preface, so to speak, to embryology; that is, it introduces the development of the specialized
Female reproductive cycle: A Comprehensive Review Rachel Ledden Paper for Bachelors in Science January 20, 2018
 Running head: 1 Female reproductive cycle: A Comprehensive Review Rachel Ledden Paper for Bachelors in Science January 20, 2018 Female reproductive cycle: A Comprehensive Review 2 The reproductive cycle
Running head: 1 Female reproductive cycle: A Comprehensive Review Rachel Ledden Paper for Bachelors in Science January 20, 2018 Female reproductive cycle: A Comprehensive Review 2 The reproductive cycle
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Phases of the Ovarian Cycle
 OVARIAN CYCLE An ovary contains many follicles, and each one contains an immature egg called an oocyte. A female is born with as many as 2 million follicles, but the number is reduced to 300,000 to 400,000
OVARIAN CYCLE An ovary contains many follicles, and each one contains an immature egg called an oocyte. A female is born with as many as 2 million follicles, but the number is reduced to 300,000 to 400,000
Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY
 Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY Gonads Gonads have 2 func7ons Gametogenesis Spermatogenesis Oogenesis Secrete steroid hormones Testosterone Estrogens (3 forms) Estradiol, produced by ovaries,
Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY Gonads Gonads have 2 func7ons Gametogenesis Spermatogenesis Oogenesis Secrete steroid hormones Testosterone Estrogens (3 forms) Estradiol, produced by ovaries,
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure.
 Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
2 - male hormones/ female system
 2 - male hormones/ female system May 7, 2012 5:08 PM I) Testosterone: main androgen (male sex hormone) A) Intro to Testosterone: -steroid hormone produced by interstitial cells in testes -produced in response
2 - male hormones/ female system May 7, 2012 5:08 PM I) Testosterone: main androgen (male sex hormone) A) Intro to Testosterone: -steroid hormone produced by interstitial cells in testes -produced in response
THE MENSTRUAL CYCLE INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY
 THE MENSTRUAL CYCLE INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY REFERENCE Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
THE MENSTRUAL CYCLE INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY REFERENCE Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Reproductive physiology
 Reproductive physiology Sex hormones: Androgens Estrogens Gestagens Learning objectives 86 (also 90) Sex Genetic sex Gonadal sex Phenotypic sex XY - XX chromosomes testes - ovaries external features Tha
Reproductive physiology Sex hormones: Androgens Estrogens Gestagens Learning objectives 86 (also 90) Sex Genetic sex Gonadal sex Phenotypic sex XY - XX chromosomes testes - ovaries external features Tha
The Human Menstrual Cycle
 The Human Menstrual Cycle Name: The female human s menstrual cycle is broken into two phases: the Follicular Phase and the Luteal Phase. These two phases are separated by an event called ovulation. (1)
The Human Menstrual Cycle Name: The female human s menstrual cycle is broken into two phases: the Follicular Phase and the Luteal Phase. These two phases are separated by an event called ovulation. (1)
HANDOUT # 1 GAMETOGENESIS
 Gametogenesis 1 HANDOUT # 1 GAMETOGENESIS Anatomy Department R.A. FADEL Gametogenesis 2 بسم هللا الرحمن الرحيم ت هأ م وى }46 } ا نل و و ا زل و ج و ن و و و و و ن ه و أ ل ه ث وى }45{ إ ول ن أ و ة م ن ان
Gametogenesis 1 HANDOUT # 1 GAMETOGENESIS Anatomy Department R.A. FADEL Gametogenesis 2 بسم هللا الرحمن الرحيم ت هأ م وى }46 } ا نل و و ا زل و ج و ن و و و و و ن ه و أ ل ه ث وى }45{ إ ول ن أ و ة م ن ان
BIOL 2402 Reproductive Systems!
 Dr. Chris Doumen! Female Reproductive Anatomy BIOL 2402 Reproductive Systems! Establishing the Ovarian Cycle During childhood, until puberty Ovaries grow and secrete small amounts of estrogens Estrogen
Dr. Chris Doumen! Female Reproductive Anatomy BIOL 2402 Reproductive Systems! Establishing the Ovarian Cycle During childhood, until puberty Ovaries grow and secrete small amounts of estrogens Estrogen
Reproductive physiology. About this Chapter. Case introduction. The brain directs reproduction 2010/6/29. The Male Reproductive System
 Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
OVARY The surface of the ovary is covered with surface epithelium
 OVARY Cow The ovary, or female gonad, is: 1. an exocrine gland, producing oocytes 2. an endocrine gland, secreting hormones, i.e., estrogen and progesterone OVARY OVARY The surface of the ovary is covered
OVARY Cow The ovary, or female gonad, is: 1. an exocrine gland, producing oocytes 2. an endocrine gland, secreting hormones, i.e., estrogen and progesterone OVARY OVARY The surface of the ovary is covered
REPRODUCTION & GENETICS. Hormones
 REPRODUCTION & GENETICS Hormones http://www.youtube.com/watch?v=np0wfu_mgzo Objectives 2 Define what hormones are; Compare and contrast the male and female hormones; Explain what each hormone in the mail
REPRODUCTION & GENETICS Hormones http://www.youtube.com/watch?v=np0wfu_mgzo Objectives 2 Define what hormones are; Compare and contrast the male and female hormones; Explain what each hormone in the mail
Sample Provincial exam Q s: Reproduction
 Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Ch 28 Lecture Study Guide
 Ch 28 Lecture Study Guide 1. List the characteristics of the reproductive system. Only organ system not essential to life Ensures continued existence of human species Produces, stores, nourishes, and transports
Ch 28 Lecture Study Guide 1. List the characteristics of the reproductive system. Only organ system not essential to life Ensures continued existence of human species Produces, stores, nourishes, and transports
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
The beginning of puberty is marked by the progressive increase in the production of sex hormones.
 Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Bio 12- Ch. 21: Reproductive System
 Bio 12- Ch. 21: Reproductive System 21.1- Male Reproductive System o Male anatomy o Testes and how they relate to sperm production and male sex hormones o Hormone regulation in males 21.2- Female Reproductive
Bio 12- Ch. 21: Reproductive System 21.1- Male Reproductive System o Male anatomy o Testes and how they relate to sperm production and male sex hormones o Hormone regulation in males 21.2- Female Reproductive
Sperm production. Sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
 Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production. Sperm production. Controlling sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
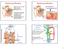 Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Stage 4 - Ovarian Cancer Symptoms
 WELCOME Stage 4 - Ovarian Cancer Symptoms University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad,
WELCOME Stage 4 - Ovarian Cancer Symptoms University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad,
The Reproductive System
 Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Female Reproductive System
 Female Reproductive System (Part A-1) Module 10 -Chapter 12 Overview Female reproductive organs Ovaries Fallopian tubes Uterus and vagina Mammary glands Menstrual cycle Pregnancy Labor and childbirth Menopause
Female Reproductive System (Part A-1) Module 10 -Chapter 12 Overview Female reproductive organs Ovaries Fallopian tubes Uterus and vagina Mammary glands Menstrual cycle Pregnancy Labor and childbirth Menopause
Chapter 36 Active Reading Guide Reproduction and Development
 Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Biology of Reproduction-Biol 326
 Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
2. Which of the following factors does not contribute to ion selectivity?
 General Biology Summer 2014 Exam II Sample Answers 1. Which of the following is TRUE about a neuron at rest? A. The cytosol is positive relative to the outside B. Na+ concentrations are higher inside C.
General Biology Summer 2014 Exam II Sample Answers 1. Which of the following is TRUE about a neuron at rest? A. The cytosol is positive relative to the outside B. Na+ concentrations are higher inside C.
The menstrual cycle. François Pralong
 The menstrual cycle François Pralong Services d Endocrinologie, Diabétologie et Métabolisme, Hôpitaux Universitaires de Genève et Lausanne Centre des Maladies CardioVasculaires et Métaboliques, Lausanne
The menstrual cycle François Pralong Services d Endocrinologie, Diabétologie et Métabolisme, Hôpitaux Universitaires de Genève et Lausanne Centre des Maladies CardioVasculaires et Métaboliques, Lausanne
The menstrual Cycle. François Pralong
 The menstrual Cycle François Pralong Services d Endocrinologie, Diabétologie et Métabolisme, Hôpitaux Universitaires de Genève et Lausanne Centre des Maladies CardioVasculaires et Métaboliques, Lausanne
The menstrual Cycle François Pralong Services d Endocrinologie, Diabétologie et Métabolisme, Hôpitaux Universitaires de Genève et Lausanne Centre des Maladies CardioVasculaires et Métaboliques, Lausanne
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
1. Both asexual and sexual reproduction occur in the animal kingdom
 1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
LeCturer : Maher Hadidi
 lecture # : 1 4 Date : Sybject : LeCturer : Maher Hadidi :t if, Done by: Gametogenesis The process of germ cells formation (gametes) which, involves the chromosomes and cytoplasm of the gametes, to prepare
lecture # : 1 4 Date : Sybject : LeCturer : Maher Hadidi :t if, Done by: Gametogenesis The process of germ cells formation (gametes) which, involves the chromosomes and cytoplasm of the gametes, to prepare
FLASH CARDS. Kalat s Book Chapter 11 Alphabetical
 FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 11 Alphabetical alpha-fetoprotein alpha-fetoprotein Alpha-Fetal Protein (AFP) or alpha-1- fetoprotein. During a prenatal sensitive period, estradiol
FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 11 Alphabetical alpha-fetoprotein alpha-fetoprotein Alpha-Fetal Protein (AFP) or alpha-1- fetoprotein. During a prenatal sensitive period, estradiol
Chapter 26: Reproductive Systems. Male 11/29/2015. Male reproductive system is composed of... BIO 218 Fall Gonads (testes)
 Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Oogenesis. Key Concepts. Female Reproductive Tract
 Oogenesis 1 Key Concepts Female Reproductive Tract Ovary Oogenesis Follicles Ovulation Corpus Luteum Molecular Activity Primordial Germ Cells (PGCs) 2 Female Reproductive Tract Ovary Oviduct Uterus Vagina
Oogenesis 1 Key Concepts Female Reproductive Tract Ovary Oogenesis Follicles Ovulation Corpus Luteum Molecular Activity Primordial Germ Cells (PGCs) 2 Female Reproductive Tract Ovary Oviduct Uterus Vagina
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System
 Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
1 The cell. Checkup Chapter 5. (pp ) 1. Look at the following illustration.
 Checkup Chapter 5 1 The cell (pp. 126 131) 1. Look at the following illustration. a) What three cell components are visible under a light (optical) microscope? Cell membrane Cytoplasm Nucleus b) What is
Checkup Chapter 5 1 The cell (pp. 126 131) 1. Look at the following illustration. a) What three cell components are visible under a light (optical) microscope? Cell membrane Cytoplasm Nucleus b) What is
Endocrine and Reproductive Systems. Chapter 39: Biology II
 Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
Human Reproductive Anatomy The female anatomy first just the reproductive parts:
 Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
REPRODUCTIVE SYSTEM OBJECTIVES
 REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
REPRODUCTIVE CYCLE OF FEMALE MAMMAL
 REPRODUCTIVE CYCLE OF FEMALE MAMMAL Fig. 8-12 Secondary follicles growing follicles increase in number of layers of granulosa cells Tertiary follicles maturing follicles antrum formation fluid filled space
REPRODUCTIVE CYCLE OF FEMALE MAMMAL Fig. 8-12 Secondary follicles growing follicles increase in number of layers of granulosa cells Tertiary follicles maturing follicles antrum formation fluid filled space
The Male Reproductive System
 The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
Chapter 14 The Reproductive System
 Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Student Academic Learning Services Page 1 of 5 Reproductive System Practice
 Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
Cell Divisions. The autosomes represent the whole body. * Male Sex Chromosomes: XY * Female Sex Chromosomes: XX
 Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
REPRODUCTION The diagram below shows a section through seminiferous tubules in a testis.
 1. The diagram below shows a section through seminiferous tubules in a testis. Which cell produces testosterone? 2. A function of the interstitial cells in the testes is to produce A sperm B testosterone
1. The diagram below shows a section through seminiferous tubules in a testis. Which cell produces testosterone? 2. A function of the interstitial cells in the testes is to produce A sperm B testosterone
a. the tail disappears b. they become spermatids c. they undergo capacitation d. they have been stored in the uterus for several days
 (2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
(2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
Unit 5: Cell Cycle, Mitosis, Meiosis & Drug Influence Influence on Nervous System
 Unit 5: Cell Cycle, Mitosis, Meiosis & Drug Influence Influence on Nervous System 1. Which of the following is NOT related to a cell s surface area to volume ratio? a. Cell size b. Number of nuclei c.
Unit 5: Cell Cycle, Mitosis, Meiosis & Drug Influence Influence on Nervous System 1. Which of the following is NOT related to a cell s surface area to volume ratio? a. Cell size b. Number of nuclei c.
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Section 39 1 The Endocrine System (pages )
 Chapter 39 Endocrine and Reproductive Systems 11 What is the function of the parathyroid glands? Section 39 1 The Endocrine System (pages 997 1002) Key Concepts What is the function of the endocrine system?
Chapter 39 Endocrine and Reproductive Systems 11 What is the function of the parathyroid glands? Section 39 1 The Endocrine System (pages 997 1002) Key Concepts What is the function of the endocrine system?
The Cell Life Cycle. S DNA replication, INTERPHASE. G 2 Protein. G 1 Normal THE CELL CYCLE. Indefinite period. synthesis. of histones.
 Mitosis & Meiosis The Cell Life Cycle INTERPHASE G 1 Normal cell functions plus cell growth, duplication of organelles, protein synthesis S DNA replication, synthesis of histones THE CELL CYCLE M G 2 Protein
Mitosis & Meiosis The Cell Life Cycle INTERPHASE G 1 Normal cell functions plus cell growth, duplication of organelles, protein synthesis S DNA replication, synthesis of histones THE CELL CYCLE M G 2 Protein
I. Endocrine System & Hormones Figure 1: Human Endocrine System
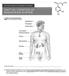 I. Endocrine System & Hormones Figure 1: Human Endocrine System Endocrine System: a) Endocrine glands are ductless since they lack specific vessels for the transport of hormones throughout the body. Instead,
I. Endocrine System & Hormones Figure 1: Human Endocrine System Endocrine System: a) Endocrine glands are ductless since they lack specific vessels for the transport of hormones throughout the body. Instead,
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal
 What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
Section 39 1 The Endocrine System (pages )
 Chapter 39 Endocrine and Reproductive Systems Section 39 1 The Endocrine System (pages 997 1002) Key Concepts What is the function of the endocrine system? How does the endocrine system maintain homeostasis?
Chapter 39 Endocrine and Reproductive Systems Section 39 1 The Endocrine System (pages 997 1002) Key Concepts What is the function of the endocrine system? How does the endocrine system maintain homeostasis?
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase
 Human Sexuality Exam II Review Material Gametogenesis: Oogenesis 1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase 2. Know the relative
Human Sexuality Exam II Review Material Gametogenesis: Oogenesis 1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase 2. Know the relative
to ensure the. Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion of.
 The Reproductive System Fill-In Notes Purpose of life: to ensure the. Stages of Human Development Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion
The Reproductive System Fill-In Notes Purpose of life: to ensure the. Stages of Human Development Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion
The Female Reproductive System
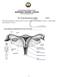 The Female Reproductive System STD X The female reproductive system consists of a pair of ovaries, a pair of oviducts, uterus, a vagina and the outermost part - the vulva. 1 1. Ovaries The ovaries are
The Female Reproductive System STD X The female reproductive system consists of a pair of ovaries, a pair of oviducts, uterus, a vagina and the outermost part - the vulva. 1 1. Ovaries The ovaries are
Spermatogenesis. What is it and what does it look like? How do hormones regulate spermatogenesis?
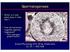 Spermatogenesis What is it and what does it look like? How do hormones regulate spermatogenesis? FSH, androgens, growth factors Animal Physiology (Hill, Wise, Anderson): Ch. 15 435-438 1 Spermatogenesis:
Spermatogenesis What is it and what does it look like? How do hormones regulate spermatogenesis? FSH, androgens, growth factors Animal Physiology (Hill, Wise, Anderson): Ch. 15 435-438 1 Spermatogenesis:
Human Biochemistry. Hormones
 Human Biochemistry Hormones THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM The ENDOCRINE SYSTEM = the organ system that regulates internal environment conditions by secreting hormones into
Human Biochemistry Hormones THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM THE ENDOCRINE SYSTEM The ENDOCRINE SYSTEM = the organ system that regulates internal environment conditions by secreting hormones into
5 15/3/2012. Malik Al-Momani
 5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
Meiosis & Sexual Reproduction. AP Biology
 Meiosis & Sexual Reproduction 2007-2008 Cell division / Asexual reproduction Mitosis produce cells with same information identical daughter cells exact copies clones same amount of DNA same number of chromosomes
Meiosis & Sexual Reproduction 2007-2008 Cell division / Asexual reproduction Mitosis produce cells with same information identical daughter cells exact copies clones same amount of DNA same number of chromosomes
Ch 20: Reproduction. Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition
 Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Reproduction Lecture Spring 2009
 Reproduction Lecture Spring 2009 Slide #2: The term gonads refer to the sex organs. In the male, these are the testes, and the in the female, the ovary. The produce sex cells, or gametes. The male gamete
Reproduction Lecture Spring 2009 Slide #2: The term gonads refer to the sex organs. In the male, these are the testes, and the in the female, the ovary. The produce sex cells, or gametes. The male gamete
