What s the Connection?
|
|
|
- Oliver O’Neal’
- 5 years ago
- Views:
Transcription
1 T h e n e w e ng l a nd j o u r na l o f m e dic i n e clinical problem-solving What s the Connection? Aharon E. Sareli, M.D., William J. Janssen, M.D., Daniel Sterman, M.D., Sanjay Saint, M.D., M.P.H., and Reed E. Pyeritz, M.D., Ph.D. In this Journal feature, information about a real patient is presented in stages (boldface type) to an expert clinician, who responds to the information, sharing his or her reasoning with the reader (regular type). The authors commentary follows. From the Department of Medicine, University of Pennsylvania, Philadelphia (A.E.S., D.S., R.E.P.); the Department of Medicine, National Jewish Medical and Research Center, Denver (W.J.J.); and the Ann Arbor Veterans Affairs Health Services Research and Development Center of Excellence and the Department of Internal Medicine, University of Michigan both in Ann Arbor (S.S.). Address reprint requests to Dr. Sareli at the Department of Medicine, Hospital of the University of Pennsylvania, 3400 Spruce St., Philadelphia, PA 19141, or at aharon.sareli@uphs. upenn.edu. N Engl J Med 2008;358: Copyright 2008 Massachusetts Medical Society. A 26-year-old white man presented to our referral hospital with a 1-month history of persistent cough productive of white sputum, which was occasionally tinged with blood. He reported mild pleuritic chest pain but no dyspnea, fever, chills, night sweats, or weight loss. The patient had had no epistaxis or episodes of sinusitis. One week before presentation, his cough had been treated with an empirical course of azithromycin with no resolution of his symptoms. A key feature when evaluating a patient with cough is symptom duration. Acute cough lasts less than 3 weeks and is usually caused by a respiratory tract infection. Cough lasting longer than 8 weeks is considered chronic and is most often due to postnasal drip, asthma, or gastroesophageal reflux disease. Hemoptysis, however, suggests diseases of the airways particularly bronchitis and bronchiectasis, although other causes must also be considered. A young man is unlikely to have bronchogenic carcinoma, although he could have metastatic testicular cancer or bronchial carcinoid. Kaposi s sarcoma involving the airways may cause hemoptysis in patients infected with the human immunodeficiency virus (HIV). Hemoptysis can also arise from the lung parenchyma. Autoimmune disease, cocaine inhalation, and infections (including tuberculosis, bacterial pneumonia, and lung abscess) are potential culprits. A last consideration is that hemoptysis can arise from the pulmonary vasculature as a result of pulmonary embolism, pulmonary arteriovenous malformation, mitral stenosis, and severe left heart failure. Five years before this presentation, the patient had been treated for a right-sided spontaneous pneumothorax. At that time, his hospital course was complicated by multiple chest-tube insertions on the right side, thoracotomy, and pleurodesis. Three years before presentation, he had had left-sided flank pain and was found to have a spontaneous left renal-artery dissection with renal infarction. He had received care elsewhere, and medical records were not available. The patient worked as a graphic designer. He was monogamous and had no risk factors for infection with HIV. He neither smoked nor used illicit drugs. His outpatient medications consisted only of a multivitamin. His mother died at 52 years of age from a presumed pulmonary embolus; the family history was otherwise unremarkable. Since the patient s medical history is notable for two relatively uncommon diagnoses pneumothorax and renal-artery dissection it is tempting to find a single disease that provides a unifying diagnosis for these previous illnesses and the recent hemoptysis. Spontaneous pneumothorax can usually be managed with simple aspiration or tube thoracostomy; that this patient s condition did not respond to the 626
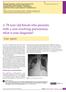
2 usual therapy and required surgical intervention suggests that his pneumothorax occurred as a result of an underlying disease that was not appreciated at the time. Arterial dissection and pneumothorax can occur with Marfan s syndrome, the Ehlers Danlos syndrome, and rarely, homocystinuria. A hypercoagulable state can be seen with the latter and would be consistent with the family history of pulmonary embolism. Pulmonary and bronchial arterial aneurysms can occur in patients with Marfan s syndrome and the Ehlers Danlos syndrome and could explain the hemoptysis. Cocaine use is another possible cause of hemoptysis, pneumothorax, and arterial dissection. It should be investigated despite the patient s report of no substance abuse. A toxicology screen and a careful physical examination with particular focus on the patient s body habitus, skin, joints, and chest will be useful. Attempts should be made to verify the cause of death of the patient s mother and any underlying disease she might have had. The patient appeared comfortable and was in no acute distress. His body habitus appeared normal. The temperature was 36.2 C, the heart rate 63 beats per minute, the respiratory rate 18 breaths per minute, the blood pressure 127/73 mm Hg, and the oxygen saturation 98% while the patient was breathing ambient air. Examination of the abdomen, heart, and neurologic system revealed no abnormalities. On chest examination, the patient had rales and decreased air entry posteriorly in the left lower lung zone. The skin examination revealed no rashes, ecchymoses, or hyperextensibility. The patient had generalized joint hypermobility involving both small and large joints, but there was no joint swelling or synovitis. The findings on lung examination are consistent with consolidation. In the absence of tachypnea, fever, or tachycardia, pneumonia is unlikely. There are no telangiectasias to suggest systemic arteriovenous malformations, and there is no arthritis or other evidence of a collagen vascular disease. Joint hypermobility is a hallmark of Marfan s syndrome. However, there is no mention of arachnodactyly, scoliosis, or anterior chest deformity, findings that would increase the likelihood of Marfan s syndrome. The joint findings could be consistent with the Ehlers Danlos syndrome, but the patient s skin is not hyperextensible. In most cases of the Ehlers Danlos syndrome, the skin appears thin or even transparent. However, skin findings can be subtle in some subtypes of this syndrome, and at this point, I believe that one of these subtypes is the most likely diagnosis. A complete blood count revealed a white-cell count of 5400 per cubic millimeter, with a differential count of 69% granulocytes, 16% lymphocytes, 12% monocytes, 2.5% eosinophils, and 0.1% basophils. The hemoglobin level was 12.3 g per deciliter (7.6 mmol per liter), and the platelet count was 212,000 per cubic millimeter. The serum creatinine level was 1.1 mg per deciliter (97.2 μmol per liter), and the urea nitrogen level was 11 mg per deciliter (3.9 mmol per liter). The results of liver-function tests, the erythrocyte sedimentation rate, and the C-reactive protein level were normal. Testing for HIV was negative. A chest radiograph (Fig. 1) revealed a left lower-lobe cavity with an A B Figure 1. Posterior-Anterior (Panel A) and Lateral (Panel B) Chest Radiographs. A fluid-filled cavity (arrows) in the left lower lobe and adjacent patchy consolidation are shown. There is a small left-sided apical pneumothorax and left hydrothorax (arrowheads). 627
3 T h e n e w e ng l a nd j o u r na l o f m e dic i n e Chest CT (Fig. 2) revealed a left lower-lobe cavity with an air liquid interface as well as a left-sided hydropneumothorax. There was an area of consolidation adjacent to the fluid-containing cavity in the left lower lobe. Subcentimeter nodules with surrounding haziness were seen in the left upper lobe, lingula, and right lower lobe. A left chest tube was placed and drained bloody serosanguineous fluid. The patient received 14 days of intravenous ampicillin sulbactam to treat a presumed lung abscess. Findings from pleural fluid staining as well as cultures for bacteria, fungus, and mycobacteria were negative. The chest tube was removed after 9 days, and the patient was discharged home with close follow-up on a prescribed course of 28 days of oral amoxicillin clavulanate. Figure 2. Chest CT Obtained without Intravenous Contrast Material. The scan shows the left lower-lobe cavity, which is filled with fluid (arrow), and left hydropneumothorax (arrowhead). An area of consolidation is seen adjacent to the fluid-filled cavity in the left lower lobe. Subcentimeter nodules with surrounding haziness were seen in the lingula, left upper lobe, and right lower lobe. air liquid level, small left-sided apical pneumothorax, and left hydrothorax. Lung cavities are air-containing lesions with a wall thickness greater than 4 mm. (In contrast, cysts have thin walls that measure 4 mm or less.) The main causes of cavities include neoplasm, infection, and collagen vascular disease. The patient s age and absence of smoking history make bronchogenic carcinoma unlikely. Lymphoma and metastases may cavitate, but in the absence of other systemic symptoms or examination findings, these possible diagnoses are unlikely. Bacteria and fungi can cause cavities, but generally are associated with fever, leukocytosis, and elevation of the C-reactive protein level. Hydatid disease is another infectious possibility, except that patients are generally quite ill when a cavity ruptures into the pleural space. A primary infection, therefore, seems unlikely. Cavitary nodules can be seen with Wegener s granulomatosis and rheumatoid arthritis, occasionally as the initial manifestation of disease. Septic emboli and thromboemboli may also occasionally cavitate, but the cavities are generally smaller than those here and multiple. Computed tomography (CT) of the chest is warranted. Although the findings on chest CT are consistent with a bacterial abscess, a primary infection is unlikely since the patient does not have any apparent risk factors for aspiration (such as impaired consciousness, dysphagia, or esophageal dysfunction), which is the usual cause of bacterial abscess formation in the lungs. If he does have an infection, it is likely to be with a pathogen that has secondarily occupied a preexisting cavity or an uncommon agent such as a species of rhodococcus or paragonimus, or Entamoeba histolytica. Given the multiple nodules found on the chest CT, I am more concerned about a systemic process than localized infection. Pulmonary vasculitis microscopic polyangiitis, the Churg Strauss syndrome, and Wegener s granulomatosis may cause this radiographic finding. None of these diseases, however, would readily explain the patient s history of spontaneous pneumothorax and renal-artery dissection. The Ehlers Danlos syndrome, as mentioned, could provide us with a unifying diagnosis. Lung cavities can occur with some of the variants of the Ehlers Danlos syndrome, in which spontaneous pneumothorax and arterial dissection are common. At this point, I would order serologic tests and a urinalysis to look for evidence of a collagen vascular disease. I doubt that the patient s lung cavity and nodules will respond to antibiotics, and I would readily proceed with a lung biopsy. The patient returned after 5 weeks for an outpatient chest CT (Fig. 3). He reported that his cough had improved and he no longer had blood-tinged sputum. On chest CT, there appeared to be inter- 628
4 val improvement in the left lower-lobe cavity; however, multiple cavitary pulmonary nodules as well as irregular hazy opacities were noted. The nodules appeared different from those seen on the previous chest CT (obtained 5 weeks earlier). Whereas some nodules had improved or disappeared entirely, new nodules and hazy opacities were visible. Waxing and waning pulmonary nodules can occur with several conditions. Sarcoidosis is one possible diagnosis, but hilar and mediastinal adenopathy would typically be seen in conjunction with waxing and waning nodules in a patient with sarcoidosis. Patients with rheumatoid arthritis can also have cavitary nodules that relapse and remit in concert with systemic disease activity, but the absence of joint manifestations in this case makes this diagnosis unlikely. Whereas the appearance of the pulmonary lesions is consistent with those seen in Wegener s granulomatosis, isolated pulmonary disease is uncommon. Chronic thromboembolic disease can cause waxing and waning pulmonary infiltrates, but the patient s course has been atypical of this condition. The Ehlers Danlos syndrome remains a possibility. Twelve weeks later, the patient presented with massive hemoptysis. Over the preceding 3-week period, hemoptysis (which had transiently resolved after his earlier hospitalization) increased gradually from 5 to 25 ml per day to as much as 200 ml in 1 day. He was readmitted for further treatment. Another chest CT was performed and the results compared with the two previous chest CT scans (obtained 12 and 17 weeks earlier). The rounded opacity in the left lower lobe, noted in the region of the initial fluid-containing cavity, appeared to be unchanged. New cavitary pulmonary nodules as well as irregular hazy opacities (more in the right lung than in the left) were noted. A comparison of the three chest CT scans indicated waxing and waning of individual nodules (Fig. 4). Tests for antinuclear antibody, antineutrophil cytoplasmic antibody, anticardiolipin antibody, anti glomerular basement membrane antibody, anti-ro and anti-la antibodies, anti-jo antibody, anti Scl-70 antibody, and anti smoothmuscle antibody were negative. Levels of complement C3 and C4 were normal. The patient underwent fiberoptic bronchoscopy. No endobronchial lesions were seen. Culture of the lavage fluid was positive for Aspergillus fumigatus. Figure 3. Chest CT Obtained without Intravenous Contrast Material, Showing Interval Improvement of the Left Lower-Lobe Cavity (Arrow), as Well as Bilateral Pulmonary Nodules. Specimens obtained by transbronchial biopsy of the right lower lobe showed hemosiderin-laden macrophages and no evidence of cancer. Massive hemoptysis has developed, which is associated with a high risk of death. Bronchoscopy and high-resolution chest CT may be useful in localizing the site of bleeding. Determining when to perform these procedures depends on the patient s condition and the tempo of the bleeding. It is unlikely that the aspergillus found in the bronchoalveolar lavage is pathogenic. Common risk factors for invasive aspergillosis include severe neutropenia, hematopoietic stem-cell and solid-organ transplantation, HIV infection, and chronic granulomatous disease; the patient has none of these. Aspergillus species are ubiquitous in the environment, and growth in respiratory cultures often represents contamination rather than infection. A lung biopsy is needed for definitive diagnosis. The patient underwent lung biopsy by means of video-assisted thoracoscopic surgery. Left upperlobe and left lower-lobe wedge specimens revealed alveolated lung tissue with emphysematous chang- 629
5 T h e n e w e ng l a nd j o u r na l o f m e dic i n e A B C Figure 4. Chest CT Scans Obtained without Intravenous Contrast Material, at Three Time Points. The CT images shown were obtained at initial presentation (Panel A), 12 weeks after initial presentation (Panel B), and 17 weeks after initial presentation (Panel C). They were taken at similar levels of the chest, higher than the levels of the images in Figures 2 and 3. The scans show waxing and waning nodules with areas of surrounding haziness. Panel A also shows left hydropneumothorax. es; no signs of vasculitis or tumor were seen. The left lower-lobe mass was found to be a well-circumscribed, organizing hematoma. Hemosiderinladen macrophages were noted in the surrounding lung parenchyma (Fig. 5). The lung biopsy is helpful in that aspergillosis and vasculitis have been ruled out. Unfortunately, a diagnosis is still lacking. The challenge is to find a unifying diagnosis that might account for the history of spontaneous pneumothorax and arterial rupture, moderate joint hypermobility, subacute development of hemoptysis, cavitary lung lesions and hemopneumothorax, and histologic evidence of emphysema. A connective-tissue defect that involves the joints, blood vessels, and lung parenchyma must be present. A variant of the Ehlers Danlos syndrome is most likely. The vascular type results from a defect in synthesis or structure of type III procollagen, a critical component of blood-vessel walls and pulmonary parenchyma. Patients with this condition often have arterial rupture and spontaneous pneumothorax. My main concern about the appropriateness of this diagnosis is the absence in this patient of two other common features of the syndrome, namely excessive bruising and thin, translucent skin. A skin sample was submitted for genetic testing. A punch-biopsy specimen of skin was cultured to determine whether either type I or type III collagen, produced by dermal fibroblasts, was abnormal. Type III procollagen showed two bands (rather than one) on polyacrylamide-gel electrophoresis, and therefore, the gene that encodes this peptide, COL3A1, was sequenced. The patient was heterozygous for a missense mutation, confirming the diagnosis of the Ehlers Danlos syndrome type IV (the vascular type). Repeat skin examination was performed in light of the diagnosis and revealed thin, atrophic scars (known as cigarette-paper scars) over the patient s knees and shins at sites of minor trauma. Family members were referred for genetic testing. One year after the diagnosis was established, the patient reported that he was well with the exception of an anterior cruciate ligament tear in the left knee. Commen ta r y The Ehlers Danlos syndromes are a heterogeneous group of heritable disorders of connective tissue. Most of the disorders involve defects in the primary structure or post-translational processing of fibrillar collagen. The six types are differentiated by their clinical features. 1 All types of Ehlers Danlos syndrome share some involvement of both skin and joints. Skin can show easy bruising, hyperextensibility, abnormal thinness, fragility, and dystrophic scarring. Joints can be hypermobile, unstable, or both. The most serious form the Ehlers Danlos syndrome, vascular type is also associated with fragility of the arterial walls and hollow viscera. Spontaneous perforation of the co- 630
6 lon (especially the sigmoid colon) and uterine rupture during labor are recognized causes of death in patients with the syndrome. 2 Ehlers and Danlos independently described the clinical features of the syndrome a century ago, but it was not until the late 1960s that a subgroup of patients with the Ehlers Danlos syndrome who had vascular fragility was identified. Previously called Ehlers Danlos syndrome type IV, this variant is now termed the vascular type. 3 This form of the Ehlers Danlos syndrome results from deficient or defective type III collagen, which is an important component of skin, blood vessels, and organs. The genetic defects primarily involve the gene COL3A1, which encodes type III procollagen. Inheritance is autosomal dominant; patients are heterozygous for one mutant allele. To confirm the diagnosis, fibroblasts cultured from a specimen obtained by skin-punch biopsy are analyzed for production of types I and III collagen. If an abnormality of amount or migration of type III procollagen or collagen is seen, then the COL3A1 gene is analyzed to determine the specific mutation. Once the mutation in the proband is determined, relatives can be screened. 2 Recently, some patients with a phenotype suggestive of the vascular type of Ehlers Danlos syndrome have been found to have mutations in a receptor for transforming growth factor β. 4 Arterial tears are the most serious complication of the Ehlers Danlos syndrome, vascular type. Approximately half of all arterial complications (including tears, dissections, and aneurysms) affect arteries within the abdomen and thorax; the renal artery is commonly affected. 2,5 Pulmonary manifestations include hemoptysis from pulmonary-artery rupture or tears in lung parenchyma, thick-walled cavities resulting from previous lung rupture, pneumothoraxes, bullous lung disease, panacinar emphysema, pulmonary cysts, and bronchiectasis. 6-8 In retrospect, the patient presented with multiple clues to the diagnosis. The medical history included two unusual conditions that are recognized to occur in patients with the vascular type of Ehlers Danlos syndrome: spontaneous renalartery dissection and spontaneous pneumothorax. On initial examination, the patient had joint hypermobility. Skin findings were not initially appreciated, but focused skin examination after Figure 5. Hematoma Surrounded by Lung Parenchyma with Hemosiderin-Laden Macrophages (Arrow) (Hematoxylin and Eosin). the diagnosis was made revealed subtle dystrophic scarring. The patient s hemoptysis, waxing and waning pulmonary cavitary nodules, and wellorganized hematoma on lung biopsy are consistent with pulmonary parenchymal tears, also reported in this syndrome. Although the patient s mother reportedly died of pulmonary embolism, medical records were not available to confirm the diagnosis, and it is possible that she died from a pulmonary manifestation of the Ehlers Danlos syndrome. Both the discussant and the clinical team did what experienced diagnosticians often do when confronted with a patient whose illness does not lend itself to a simple diagnosis: try to find the connection between the present illness and past abnormalities. Only after taking a step back and considering the patient s history did the connection a relatively rare connective-tissue disorder become apparent. Supported by an Advanced Career Development Award from the Health Services Research and Development Program of the Department of Veterans Affairs (to Dr. Saint) and a grant from the American Heart Association (to Dr. Janssen). Dr. Sterman reports receiving consulting fees from Spiration and Alveolus. Dr. Pyeritz reports receiving research support from Genzyme and being deposed or having testified in malpractice suits regarding the vascular type of Ehlers Danlos syndrome. No other potential conflict of interest relevant to this article was reported. We thank Drs. Wallace T. Miller, Jr., and Leslie A. Litzky for their help with the radiologic and pathological findings of this case. 631
7 References 1. Beighton P, De Paepe A, Steinmann B, Tsipouras P, Wenstrup RJ. Ehlers-Danlos syndromes: revised nosology, Villefranche, Am J Med Genet 1998;77: Pepin M, Schwarze U, Superti-Furga A, Byers PH. Clinical and genetic features of Ehlers Danlos syndrome type IV, the vascular type. N Engl J Med 2000;342: [Erratum, N Engl J Med 2001;344: 392.] 3. Pyeritz RE. Ehlers Danlos syndrome. N Engl J Med 2000;342: Loeys BL, Schwarze U, Holm T, et al. Aneurysm syndromes caused by mutations in the TGF-β receptor. N Engl J Med 2006;355: Oderich GS, Panneton JM, Bower TC, et al. The spectrum, management and clinical outcome of Ehlers-Danlos syndrome type IV: a 30-year experience. J Vasc Surg 2005;42: Watanabe A, Kawabata Y, Okada O, et al. Ehlers-Danlos syndrome type IV with few extrathoracic findings: a newly recog- nized point mutation in the COL3A1 gene. Eur Respir J 2002;19: Dowton SB, Pincott S, Demmer L. Respiratory complications of Ehlers-Danlos syndrome type IV. Clin Genet 1996;50: Yost BA, Vogelsang JP, Lie JT. Fatal hemoptysis in Ehlers-Danlos syndrome: old malady with a new curse. Chest 1995;107: Copyright 2008 Massachusetts Medical Society. 632
Ehlers-Danlos Syndrome with Recurrent Spontaneous Pneumothoraces and Cavitary Lesion on Chest X-ray as the Initial Complications
 CASE REPORT Ehlers-Danlos Syndrome with Recurrent Spontaneous Pneumothoraces and Cavitary Lesion on Chest X-ray as the Initial Complications Takashi Ishiguro 1, Noboru Takayanagi 1, Yoshinori Kawabata
CASE REPORT Ehlers-Danlos Syndrome with Recurrent Spontaneous Pneumothoraces and Cavitary Lesion on Chest X-ray as the Initial Complications Takashi Ishiguro 1, Noboru Takayanagi 1, Yoshinori Kawabata
Bjørg J. Abrahamsen, MD ; Mari Ann Kulseth, PhD ; and Benedicte Paus, MD, PhD
 [ Selected Reports ] A 19-Year-Old Man With Relapsing Bilateral Pneumothorax, Hemoptysis, and Intrapulmonary Cavitary Lesions Diagnosed With Vascular Ehlers-Danlos Syndrome and a Novel Missense Mutation
[ Selected Reports ] A 19-Year-Old Man With Relapsing Bilateral Pneumothorax, Hemoptysis, and Intrapulmonary Cavitary Lesions Diagnosed With Vascular Ehlers-Danlos Syndrome and a Novel Missense Mutation
PULMONARY MEDICINE BOARD REVIEW. Financial Conflicts of Interest. Question #1: Question #1 (Cont.): None. Christopher H. Fanta, M.D.
 PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
Lung Cancer - Suspected
 Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
TB Intensive Houston, Texas
 TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
Common things are common, but not always the answer
 Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Pneumothorax: A Rare Presentation of. Pulmonary Mycetoma. Prem Parkash Gupta* Sanjay Fotedar* Dipti Agarwal** Kuldeep Saini* Sarita Magu***
 Pneumothorax: A Rare Presentation of Pulmonary Mycetoma Prem Parkash Gupta* Sanjay Fotedar* Dipti Agarwal** Kuldeep Saini* Sarita Magu*** Departments of *Respiratory Medicine, **Physiology, and ***Radiodiagnosis,
Pneumothorax: A Rare Presentation of Pulmonary Mycetoma Prem Parkash Gupta* Sanjay Fotedar* Dipti Agarwal** Kuldeep Saini* Sarita Magu*** Departments of *Respiratory Medicine, **Physiology, and ***Radiodiagnosis,
COUGH Dr. A m A it i e t sh A g A garwa w l Le L ctu t rer Departm t ent t o f f M e M dic i in i e
 COUGH Dr. Amitesh Aggarwal Lecturer Department of Medicine Cough is an explosive expiration that provides a normal protective mechanism for clearing the tracheobronchial tree of secretions and foreign
COUGH Dr. Amitesh Aggarwal Lecturer Department of Medicine Cough is an explosive expiration that provides a normal protective mechanism for clearing the tracheobronchial tree of secretions and foreign
A Vietnamese woman with a 2-week history of cough
 Delphine Natali 1, Hai Tran Pham 1, Hung Nguyen The 2 delphinenatali@gmail.com Case report A Vietnamese woman with a 2-week history of cough A 52-year-old nonsmoker Vietnamese woman without any past medical
Delphine Natali 1, Hai Tran Pham 1, Hung Nguyen The 2 delphinenatali@gmail.com Case report A Vietnamese woman with a 2-week history of cough A 52-year-old nonsmoker Vietnamese woman without any past medical
Excavated pulmonary nodule: steps to diagnosis?
 Excavated pulmonary nodule: steps to diagnosis? Poster No.: C-1044 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit W. Mnari, M. MAATOUK, A. Zrig, B. Hmida, M. GOLLI; Monastir/ TN Metastases,
Excavated pulmonary nodule: steps to diagnosis? Poster No.: C-1044 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit W. Mnari, M. MAATOUK, A. Zrig, B. Hmida, M. GOLLI; Monastir/ TN Metastases,
A Repeat Case of Idiopathic Spontaneous Hemothorax
 Case Report A Repeat Case of Idiopathic Spontaneous Hemothorax Felix R. Gaw, MD Jack H. Bloch, MD, PhD, FACS Nolan J. Anderson, MD, FACS Spontaneous hemothorax, a collection of blood in the pleural cavity
Case Report A Repeat Case of Idiopathic Spontaneous Hemothorax Felix R. Gaw, MD Jack H. Bloch, MD, PhD, FACS Nolan J. Anderson, MD, FACS Spontaneous hemothorax, a collection of blood in the pleural cavity
HEMOPTYSIS. Prof. G. Zuliani
 HEMOPTYSIS Prof. G. Zuliani HEMOPTYSIS Hemoptysis is the expectoration of blood, that can range from blood-streaking of sputum (Hemoptoe) to the presence of gross blood in the absence of any accompanying
HEMOPTYSIS Prof. G. Zuliani HEMOPTYSIS Hemoptysis is the expectoration of blood, that can range from blood-streaking of sputum (Hemoptoe) to the presence of gross blood in the absence of any accompanying
Lung diseases of Vascular Origin. By: Shefaa Qa qqa
 Lung diseases of Vascular Origin By: Shefaa Qa qqa Pulmonary Hypertension Pulmonary hypertension is defined as a mean pulmonary artery pressure greater than or equal to 25 mm Hg at rest. Based on underlying
Lung diseases of Vascular Origin By: Shefaa Qa qqa Pulmonary Hypertension Pulmonary hypertension is defined as a mean pulmonary artery pressure greater than or equal to 25 mm Hg at rest. Based on underlying
Resident Case Review CHEST. Daria Manos CAR 2016
 Resident Case Review CHEST CAR 2016 Daria Manos Disclosure Speakers bureau, Roche CAR 2016 Daria Manos 1. Recognize common and critical chest radiograph and computed tomography signs and use these clues
Resident Case Review CHEST CAR 2016 Daria Manos Disclosure Speakers bureau, Roche CAR 2016 Daria Manos 1. Recognize common and critical chest radiograph and computed tomography signs and use these clues
A Case of Pediatric Plasma Cell Granuloma
 August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
Pulmonary Aspergillosis
 May 2005 Pulmonary Aspergillosis Nancy Wei, Harvard Medical School, Year III Overview Pulmonary aspergillosis background information Patient presentations Common radiographic findings for each type of
May 2005 Pulmonary Aspergillosis Nancy Wei, Harvard Medical School, Year III Overview Pulmonary aspergillosis background information Patient presentations Common radiographic findings for each type of
Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma
 Article ID: WMC005047 ISSN 2046-1690 Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma Peer review status: No Corresponding Author: Dr. Mohammad Fawad Khattak,
Article ID: WMC005047 ISSN 2046-1690 Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma Peer review status: No Corresponding Author: Dr. Mohammad Fawad Khattak,
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations
 Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
Anatomy. The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs.
 Respiratory System Anatomy The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs. Within the lungs, the bronchi transport air with oxygen to the alveoli on inspiration
Respiratory System Anatomy The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs. Within the lungs, the bronchi transport air with oxygen to the alveoli on inspiration
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
PULMONARY TUBERCULOSIS RADIOLOGY
 PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
Radiological Aspects of Pulmonary Tuberculosis in Immunocompetent Hosts
 Nov 2003 Radiological Aspects of Pulmonary Tuberculosis in Immunocompetent Hosts Josh Rempell, Harvard Medical School Year III Tuberculosis: the captain of all (wo)men of death Overall, one third of the
Nov 2003 Radiological Aspects of Pulmonary Tuberculosis in Immunocompetent Hosts Josh Rempell, Harvard Medical School Year III Tuberculosis: the captain of all (wo)men of death Overall, one third of the
How to Analyse Difficult Chest CT
 How to Analyse Difficult Chest CT Complex diseases are:- - Large lesion - Unusual or atypical pattern - Multiple discordant findings Diffuse diseases are:- - Numerous findings in both sides 3 basic steps
How to Analyse Difficult Chest CT Complex diseases are:- - Large lesion - Unusual or atypical pattern - Multiple discordant findings Diffuse diseases are:- - Numerous findings in both sides 3 basic steps
11/19/2012. The spectrum of pulmonary diseases in HIV-infected persons is broad.
 The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
Bronchial syndrome. Atelectasis Draining bronchus Bronchiectasis
 Bronchial syndrome Atelectasis Draining bronchus Bronchiectasis Etienne Leroy Terquem Pierre L Her SPI / ISP Soutien Pneumologique International / International Support for Pulmonology Atelectasis Consequence
Bronchial syndrome Atelectasis Draining bronchus Bronchiectasis Etienne Leroy Terquem Pierre L Her SPI / ISP Soutien Pneumologique International / International Support for Pulmonology Atelectasis Consequence
Case 1. Background. Presenting Symptoms. Schecter Case1 Differential Diagnosis of TB 1
 TB or Not TB? Case 1 Gisela Schecter, M.D., M.P.H. California Department of Public Health Background 26 year old African American male Born and raised in Bay Area of California Convicted of cocaine trafficking
TB or Not TB? Case 1 Gisela Schecter, M.D., M.P.H. California Department of Public Health Background 26 year old African American male Born and raised in Bay Area of California Convicted of cocaine trafficking
HEMODYNAMIC DISORDERS
 HEMODYNAMIC DISORDERS Normal fluid homeostasis requires vessel wall integrity as well as maintenance of intravascular pressure and osmolarity within certain physiologic ranges. Increases in vascular volume
HEMODYNAMIC DISORDERS Normal fluid homeostasis requires vessel wall integrity as well as maintenance of intravascular pressure and osmolarity within certain physiologic ranges. Increases in vascular volume
100 Chest X Rays for Study Group. by Dr. Suneet Khurana
 100 Chest X Rays for Study Group by Dr. Suneet Khurana Approach to - Chest X Ray (shadow of the viscera on a photographic plate) Gas appears Black Fat appears Dark Grey Water Appears as Light Grey Bone
100 Chest X Rays for Study Group by Dr. Suneet Khurana Approach to - Chest X Ray (shadow of the viscera on a photographic plate) Gas appears Black Fat appears Dark Grey Water Appears as Light Grey Bone
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I. December 5, 2012
 SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
Eosinophils and effusion: a clinical conundrum
 Ruth Sobala, Kevin Conroy, Hilary Tedd, Salem Elarbi kevin.peter.conroy@gmail.com Respiratory Dept, Queen Elizabeth Hospital, Gateshead, UK. Eosinophils and effusion: a clinical conundrum Case report A
Ruth Sobala, Kevin Conroy, Hilary Tedd, Salem Elarbi kevin.peter.conroy@gmail.com Respiratory Dept, Queen Elizabeth Hospital, Gateshead, UK. Eosinophils and effusion: a clinical conundrum Case report A
Let s Talk TB A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year
 A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Barry Rabinovitch, MD, FRCP(C) Author Madhukar Pai, MD, PhD co-author and Series Editor Barry Rabinovitch is an assistant
A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Barry Rabinovitch, MD, FRCP(C) Author Madhukar Pai, MD, PhD co-author and Series Editor Barry Rabinovitch is an assistant
Immune-mediated lung disease. Ian Sabroe
 Immune-mediated lung disease Ian Sabroe It s all immune? Diseases that doesn t have immune involvement? The processes of response to injury and tissue repair are key homeostatic pathways involved in all
Immune-mediated lung disease Ian Sabroe It s all immune? Diseases that doesn t have immune involvement? The processes of response to injury and tissue repair are key homeostatic pathways involved in all
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
Unit II Problem 2 Pathology: Pneumonia
 Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
BELLWORK page 343. Apnea Dyspnea Hypoxia pneumo pulmonary Remember the structures of the respiratory system 1
 BELLWORK page 343 Apnea Dyspnea Hypoxia pneumo pulmonary respiratory system 1 STANDARDS 42) Review case studies that involve persons with respiratory disorders, diseases, or syndromes. Citing information
BELLWORK page 343 Apnea Dyspnea Hypoxia pneumo pulmonary respiratory system 1 STANDARDS 42) Review case studies that involve persons with respiratory disorders, diseases, or syndromes. Citing information
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
General History. 林陳 珠 Female 69 years old 住院期間 : ~ Chief Complaint : sudden loss of conscious 5 minutes in the morning.
 General History 林陳 珠 Female 69 years old 住院期間 : 93.5.8~93.5.15 Chief Complaint : sudden loss of conscious for 2-52 5 minutes in the morning. General History DM under regular medical control for 10 years.
General History 林陳 珠 Female 69 years old 住院期間 : 93.5.8~93.5.15 Chief Complaint : sudden loss of conscious for 2-52 5 minutes in the morning. General History DM under regular medical control for 10 years.
Chapter 22. Pulmonary Infections
 Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW
 SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
Nontuberculous Mycobacterial Lung Disease
 Non-TB Mycobacterial Disease Jeffrey P. Kanne, MD Nontuberculous Mycobacterial Lung Disease Jeffrey P. Kanne, M.D. Consultant Disclosures Perceptive Informatics Royalties (book author) Amirsys, Inc. Wolters
Non-TB Mycobacterial Disease Jeffrey P. Kanne, MD Nontuberculous Mycobacterial Lung Disease Jeffrey P. Kanne, M.D. Consultant Disclosures Perceptive Informatics Royalties (book author) Amirsys, Inc. Wolters
When to suspect Wegener Granulomatosis: A radiologic review
 When to suspect Wegener Granulomatosis: A radiologic review Poster No.: P-0038 Congress: ESTI 2015 Type: Educational Poster Authors: A. Tilve Gómez, R. Díez Bandera, P. Rodríguez Fernández, M. Garcia Vazquez-Noguerol,
When to suspect Wegener Granulomatosis: A radiologic review Poster No.: P-0038 Congress: ESTI 2015 Type: Educational Poster Authors: A. Tilve Gómez, R. Díez Bandera, P. Rodríguez Fernández, M. Garcia Vazquez-Noguerol,
Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program
 Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program History 32 year-old male who presented with a 4 days history of: Productive cough Right sided pleuritic chest
Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program History 32 year-old male who presented with a 4 days history of: Productive cough Right sided pleuritic chest
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Localized Pulmonary Hemorrhage Associated With Massive Hemoptysis: Report of a Case
 113 Localized Pulmonary Hemorrhage Associated With Massive Hemoptysis: Report of a Case Yang-Hao Yu, Te-Chun Hsia, Liang-Wen Hang, Tze-Yi Lin 1, Nan-Yung Hsu 2, Der-Yuan Wang 3 Devision of Pulmonary and
113 Localized Pulmonary Hemorrhage Associated With Massive Hemoptysis: Report of a Case Yang-Hao Yu, Te-Chun Hsia, Liang-Wen Hang, Tze-Yi Lin 1, Nan-Yung Hsu 2, Der-Yuan Wang 3 Devision of Pulmonary and
Α 78-year-old female who presents with a non-resolving pneumonia: what is your diagnosis?
 Evangelia Panagiotidou 1, Serafeim-Chrysovalantis Kotoulas 1, Maria Kilmpasani 2, Nikoleta Pastelli 2, Sofia Akritidou 1, Evangelos Chatzopoulos 1, Vasilis Bikos 1, Vasilios Bagalas 1, Katalin Fekete-Passa
Evangelia Panagiotidou 1, Serafeim-Chrysovalantis Kotoulas 1, Maria Kilmpasani 2, Nikoleta Pastelli 2, Sofia Akritidou 1, Evangelos Chatzopoulos 1, Vasilis Bikos 1, Vasilios Bagalas 1, Katalin Fekete-Passa
Joseph Garland, HMS IV Gillian Lieberman, MD. Round Pneumonia. Joseph Garland, HMS IV Gillian Lieberman, MD
 Round Pneumonia Joseph Garland, HMS IV Case 1: Mr. H Mr. H is a 45-year-old man who presents with a 4 day history of full-body myalgias, headaches and fever to 103 F. He also complains of sharp leftsided
Round Pneumonia Joseph Garland, HMS IV Case 1: Mr. H Mr. H is a 45-year-old man who presents with a 4 day history of full-body myalgias, headaches and fever to 103 F. He also complains of sharp leftsided
Vascular Ehlers- Danlos in the pediatric population
 Vascular Ehlers- Danlos in the pediatric population Shaine A. Morris, MD, MPH Pediatric Cardiology Texas Children s Hospital, Baylor College of Medicine Objectives Learn what Vascular EDS is, and how it
Vascular Ehlers- Danlos in the pediatric population Shaine A. Morris, MD, MPH Pediatric Cardiology Texas Children s Hospital, Baylor College of Medicine Objectives Learn what Vascular EDS is, and how it
Invasive Pulmonary Aspergillosis in
 Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
October 2012 Imaging Case of the Month. Michael B. Gotway, MD Associate Editor Imaging. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
Pneumocystis. Pneumocystis BIOL Summer Introduction. Mycology. Introduction (cont.) Introduction (cont.)
 Introduction Pneumocystis Disclaimer: This lecture slide presentation is intended solely for educational purposes. Many of the images contained herein are the property of the original owner, as indicated
Introduction Pneumocystis Disclaimer: This lecture slide presentation is intended solely for educational purposes. Many of the images contained herein are the property of the original owner, as indicated
Atopic Pulmonary Disease: Findings on Thoracic Imaging
 July 2003 Atopic Pulmonary Disease: Findings on Thoracic Imaging Rebecca G. Breslow Harvard Medical School Year IV Churg-Strauss Syndrome Hypersensitivity Pneumonitis Asthma Atopic Pulmonary Disease Allergic
July 2003 Atopic Pulmonary Disease: Findings on Thoracic Imaging Rebecca G. Breslow Harvard Medical School Year IV Churg-Strauss Syndrome Hypersensitivity Pneumonitis Asthma Atopic Pulmonary Disease Allergic
Aneurysms & a Brief Discussion on Embolism
 Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
Pathology of pulmonary tuberculosis. Dr: Salah Ahmed
 Pathology of pulmonary tuberculosis Dr: Salah Ahmed Is a chronic granulomatous disease, caused by Mycobacterium tuberculosis (hominis) Usually it involves lungs but may affect any organ or tissue Transmission:
Pathology of pulmonary tuberculosis Dr: Salah Ahmed Is a chronic granulomatous disease, caused by Mycobacterium tuberculosis (hominis) Usually it involves lungs but may affect any organ or tissue Transmission:
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids
 Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Pulmonary Alveolar Proteinosis
 January 2001 Pulmonary Alveolar Proteinosis Brady Case, Harvard Medical School 1 Our Patient Nelson is a 40 year-old male who presents with a 6 month history of: progressive dyspnea on exertion dry cough
January 2001 Pulmonary Alveolar Proteinosis Brady Case, Harvard Medical School 1 Our Patient Nelson is a 40 year-old male who presents with a 6 month history of: progressive dyspnea on exertion dry cough
Community Acquired Pneumonia. Abdullah Alharbi, MD, FCCP
 Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA
 Thor-ax (1954), 9, 304. PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA W. J. HANBURY, R. J. R. CURETON, AND G. SIMON From St. Bartholomew's Hospital, London BY (RECEIVED FOR PUBLICATION JUNE
Thor-ax (1954), 9, 304. PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA W. J. HANBURY, R. J. R. CURETON, AND G. SIMON From St. Bartholomew's Hospital, London BY (RECEIVED FOR PUBLICATION JUNE
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550032 Volume 2, Issue 4 Case Report Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke Cheah Wai Hun
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550032 Volume 2, Issue 4 Case Report Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke Cheah Wai Hun
Respiratory Pathology. Kristine Krafts, M.D.
 Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Radiology Pathology Conference
 Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Adi Dagan, Pediatric Pulmonology The Edmond and Lili Safra Children's Hospital, Sheba Medical Center, Ramat-Gan, affiliated to the Sackler Medical
 Adi Dagan, Pediatric Pulmonology The Edmond and Lili Safra Children's Hospital, Sheba Medical Center, Ramat-Gan, affiliated to the Sackler Medical school, Tel-Aviv University, Israel. Case report: 23 yrs
Adi Dagan, Pediatric Pulmonology The Edmond and Lili Safra Children's Hospital, Sheba Medical Center, Ramat-Gan, affiliated to the Sackler Medical school, Tel-Aviv University, Israel. Case report: 23 yrs
Supplemental Figure 1. Gating strategies for flow cytometry and intracellular cytokinestaining
 Supplemental Figure 1. Gating strategies for flow cytometry and intracellular cytokinestaining of PBMCs. Forward scatter area (FSC-A) versus side scatter area (SSC-A) was used to select lymphocytes followed
Supplemental Figure 1. Gating strategies for flow cytometry and intracellular cytokinestaining of PBMCs. Forward scatter area (FSC-A) versus side scatter area (SSC-A) was used to select lymphocytes followed
Lung Cancer Case Study
 Lung Cancer Case Study Presented by s GP Education Programme 2 Part One Initial presentation 60 year old lady, presents with a 6 week history of right sided chest pain. The pain is like a dull ache, but
Lung Cancer Case Study Presented by s GP Education Programme 2 Part One Initial presentation 60 year old lady, presents with a 6 week history of right sided chest pain. The pain is like a dull ache, but
CLINICAL FEATURES IN PULMONARY TUBERCULOSIS
 CLINICAL FEATURES IN PULMONARY TUBERCULOSIS Dr. Amitesh Aggarwal Department of Medicine Tuberculosis Captain of all the Men of Death Great White Plague devastating effect on society 100 years ago one in
CLINICAL FEATURES IN PULMONARY TUBERCULOSIS Dr. Amitesh Aggarwal Department of Medicine Tuberculosis Captain of all the Men of Death Great White Plague devastating effect on society 100 years ago one in
Documentation Tips for Pulmonary/Critical Care
 Documentation Tips for Pulmonary/Critical Care ICD-10 classifications: The HARD WAY! J44 Other chronic obstructive pulmonary disease Includes: asthma with chronic obstructive pulmonary disease chronic
Documentation Tips for Pulmonary/Critical Care ICD-10 classifications: The HARD WAY! J44 Other chronic obstructive pulmonary disease Includes: asthma with chronic obstructive pulmonary disease chronic
Acute and Chronic Lung Disease
 KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
OBJECTIVES. Solitary Solid Spiculated Nodule. What would you do next? Case Based Discussion: State of the Art Management of Lung Nodules.
 Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Tuberculosis - clinical forms. Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases
 Tuberculosis - clinical forms Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases 1 TB DISEASE Primary Post-primary (Secondary) Common primary forms Primary complex Tuberculosis of the intrathoracic
Tuberculosis - clinical forms Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases 1 TB DISEASE Primary Post-primary (Secondary) Common primary forms Primary complex Tuberculosis of the intrathoracic
Radiological syndroms. Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome
 Radiological syndroms Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome Alveolar syndrome Pulmonary architecture : Morphological unit is the lobule 15-25mm
Radiological syndroms Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome Alveolar syndrome Pulmonary architecture : Morphological unit is the lobule 15-25mm
Bronchiectasis: An Imaging Approach
 Bronchiectasis: An Imaging Approach Travis S Henry, MD Associate Professor of Clinical Radiology Cardiac and Pulmonary Imaging Section University of California, San Francisco Large Middle Small 1 Bronchiectasis
Bronchiectasis: An Imaging Approach Travis S Henry, MD Associate Professor of Clinical Radiology Cardiac and Pulmonary Imaging Section University of California, San Francisco Large Middle Small 1 Bronchiectasis
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
Single Lung Cyst Caused by Metastatic Bladder Cancer -A Case Report
 Single Lung Cyst Caused by Metastatic Bladder Cancer -A Case Report *& Jin-Duo ng, Chih-Bin Lin, Min-Shin Kuo', Jen-Jyh Lee The lungs are one of the most common sites of metastases from transitional cell
Single Lung Cyst Caused by Metastatic Bladder Cancer -A Case Report *& Jin-Duo ng, Chih-Bin Lin, Min-Shin Kuo', Jen-Jyh Lee The lungs are one of the most common sites of metastases from transitional cell
Atlas of the Vasculitic Syndromes
 CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C.
 NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C. Past Medical History AIDS/HIV disease Anemia Asthma Bronchitis Cancer Date of last Chest X-ray Diabetes Mellitus, Type I Diabetes Mellitus,
NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C. Past Medical History AIDS/HIV disease Anemia Asthma Bronchitis Cancer Date of last Chest X-ray Diabetes Mellitus, Type I Diabetes Mellitus,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss?
 ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
Pleural effusion as an initial manifestation in a patient with primary pulmonary monoclonal B-cell lymphocyte proliferative disease
 Du et al. Respiratory Research (2018) 19:247 https://doi.org/10.1186/s12931-018-0941-6 LETTER TO THE EDITOR Pleural effusion as an initial manifestation in a patient with primary pulmonary monoclonal B-cell
Du et al. Respiratory Research (2018) 19:247 https://doi.org/10.1186/s12931-018-0941-6 LETTER TO THE EDITOR Pleural effusion as an initial manifestation in a patient with primary pulmonary monoclonal B-cell
A Rare Case of Lymphangioleiomyomatosis in Sri Lanka
 A Rare Case of Lymphangioleiomyomatosis in Sri Lanka Author s Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) Sachini Seneviratne (4) Samadara Nakandala (5) Rathnayake R.M.D.H.M - (1) (2)
A Rare Case of Lymphangioleiomyomatosis in Sri Lanka Author s Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) Sachini Seneviratne (4) Samadara Nakandala (5) Rathnayake R.M.D.H.M - (1) (2)
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Lung Cancer-a primer. Sai Yendamuri, MD Professor and Chair, Dept of Thoracic Surgery,RPCI,Buffalo
 Lung Cancer-a primer Sai Yendamuri, MD Professor and Chair, Dept of Thoracic Surgery,RPCI,Buffalo CLINICAL CATEGORIES THE SOLITARY PULMONARY NODULE MULTIPLE PULMONARY NODULES Differential Diagnosis Malignant
Lung Cancer-a primer Sai Yendamuri, MD Professor and Chair, Dept of Thoracic Surgery,RPCI,Buffalo CLINICAL CATEGORIES THE SOLITARY PULMONARY NODULE MULTIPLE PULMONARY NODULES Differential Diagnosis Malignant
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Brain abscess rupturing into the lateral ventricle causing meningitis: a case report
 Brain abscess rupturing into the lateral ventricle causing meningitis: a case report Endry Martinez, and Judith Berger SBH Health System, 4422 Third Ave, Bronx, NY 10457 Key words: brain abscess, rupture
Brain abscess rupturing into the lateral ventricle causing meningitis: a case report Endry Martinez, and Judith Berger SBH Health System, 4422 Third Ave, Bronx, NY 10457 Key words: brain abscess, rupture
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress THE LAST GASP II: LUNGS AND THORAX David Holt, BVSc, Diplomate ACVS University of Pennsylvania School of Veterinary
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress THE LAST GASP II: LUNGS AND THORAX David Holt, BVSc, Diplomate ACVS University of Pennsylvania School of Veterinary
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT
 Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
10/17/2016. Nuts and Bolts of Thoracic Radiology. Objectives. Techniques
 Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Chapter 16. Lung Abscess. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data
 Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data David Ebler, MD David Skarupa, MD Andrew J. Kerwin, MD, FACS Jhun de Villa, MD Michael S. Nussbaum, MD, FACS J.J. Tepas III, MD, FACS
Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data David Ebler, MD David Skarupa, MD Andrew J. Kerwin, MD, FACS Jhun de Villa, MD Michael S. Nussbaum, MD, FACS J.J. Tepas III, MD, FACS
Langerhans Cell Histiocytosis with Anterior Mediastinum, Pulmonary and Liver Involvement: CT Demonstration
 Chin J Radiol 2002; 27: 191-195 191 Langerhans Cell Histiocytosis with Anterior Mediastinum, Pulmonary and Liver Involvement: CT Demonstration SIU-CHEUNG CHAN 1 MUN-CHING WONG 1 SHIU-FENG HUANG 2 WAN-CHAK
Chin J Radiol 2002; 27: 191-195 191 Langerhans Cell Histiocytosis with Anterior Mediastinum, Pulmonary and Liver Involvement: CT Demonstration SIU-CHEUNG CHAN 1 MUN-CHING WONG 1 SHIU-FENG HUANG 2 WAN-CHAK
Diagnosis of TB: Radiology David Finlay, MD
 TB Intensive Tyler, Texas June 2-4, 2010 Diagnosis of TB: Radiology David Finlay, MD June 3, 2010 2stages stages- Tuberculosis 1. primary infection 2. reactivation, or post primary disease 2 1 Primary
TB Intensive Tyler, Texas June 2-4, 2010 Diagnosis of TB: Radiology David Finlay, MD June 3, 2010 2stages stages- Tuberculosis 1. primary infection 2. reactivation, or post primary disease 2 1 Primary
Dr Rodney Itaki Lecturer Anatomical Pathology Discipline. University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology
 Vasculitis Dr Rodney Itaki Lecturer Anatomical Pathology Discipline University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Disease Spectrum Hypersensitivity vasculitis/microscopic
Vasculitis Dr Rodney Itaki Lecturer Anatomical Pathology Discipline University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Disease Spectrum Hypersensitivity vasculitis/microscopic
Exam 2 Respiratory Disorders
 Exam 2 Respiratory Disorders Common Cold Common Cold Pathology Common Cold Consequences Rhinosinusitis Rhinosinusitis Pathology Rhinosinusitis ostia can close due to Influenza (Flu) Influenza Pathology
Exam 2 Respiratory Disorders Common Cold Common Cold Pathology Common Cold Consequences Rhinosinusitis Rhinosinusitis Pathology Rhinosinusitis ostia can close due to Influenza (Flu) Influenza Pathology
