Reviewer #1 (Remarks to the Author)
|
|
|
- Cassandra Baker
- 5 years ago
- Views:
Transcription
1 Reviewer #1 (Remarks to the Author) The authors provide an interesting data set concerning the effects of an ATGL inhibitor on energy balance and indices of insulin action in mice fed a high fat diet. The authors show that ATGL inhibition effectively improves the metabolic profile in mice on HFD and ob/ob mice fed chow by substantially ameliorating obesity, insulin resistance, and liver steatosis. While these are interesting and potentially important observations, the mechanisms involves are complex and somewhat obscure. Many aspects of the phenomenon were recently reported in PNAS. One would hope that a novel chemical inhibitor might provide new mechanistic insights regarding effects on food intake, lipid synthesis, TG handling and glucose metabolism. However, the data seem to be mostly descriptive, and the reasons underlying the fascinating differences between genetic and pharmacological inhibition remain unresolved. Nevertheless, the data do establish a proof of principle for ATGL inhibition. 1) Experiments in figure 1 seem to be contrived to show transient effect, but the design is not strictly relevant to chronic dosing and ad libitum feeding. It would seem difficult to deconvolve the effects of compound on food intake, lipid synthesis, fasting lipid mobilization etc. when administered in the food. The appeal to dose timing and tissue partitioning is speculative. 2) Is the effect of compound reversible? 3) Atglistatin and ATGL KO both reduced white fat pad size of mice on HFD. However, the effects in BAT are highly discordant. The effect of compound on BAT morphology is very striking and is suggestive of activation. Did the authors look at indices of BAT activation, like Ucp1, Cidea, Pgc1a, etc? 4) Measuring Atglistatin levels in adipose tissue and liver does not establish the site of action, as is claimed. The analytical method (Folch extraction) indicates that the compound is highly hydrophobic and the ATGL measured will be that which has partitioned into lipid. In addition, nothing is reported on the PK of Atglistatin, and it seems unlikely that levels of pmol/g are physiologically meaningful. Given the diverse effects on food intake, lipid absorption and clearance, etc. it is not clear what effects are primary and secondary to lipolysis inhibition. 5) The experiments do not test the premise regarding FFA release from adipose tissue. 6) The claim that the lipid lowering effect of Atglistatin depends on the expression of ATGL in the liver, is not demonstrated since ATGL levels in liver specifically were not manipulated nor was ATGL activity measured in the liver. Reviewer #2 (Remarks to the Author) Schweiger et al. report the effects of treatment with an inhibitor of adipose triglyceride lipase (ATGL) on obesity, liver steatosis and insulin resistance. The work is based on the identification of the first ATGL inhibitor by the authors (Mayer et al Nat. Chem. Biol. 9, 785). The article reports the first characterization of the effects of an ATGL inhibitor on several conditions predisposing to diabetes, cardiovascular complications and liver cirrhosis. The work has been carefully conducted with appropriate techniques. As the paper is a preclinical proof of concept for the use of ATGL inhibitors, there are however several points that are important to address. Main points 1. To assess the specificity of ATGL effects, the authors used transgenic mice which express ATGL only in heart and do not die from cardiomyopathy. Using these mice, the authors show that the lower increase of inguinal white adipose tissue weight during high fat diet is due to ATGL. However, some important questions cannot be addressed using heart-rescued ATGL knockout mice. Adipocyte-specific ATGL knock out mice treated with the ATGL inhibitor could be useful to: - prove that the control of fat mass is mediated by adipose ATGL inhibition and activation of PPAR gamma through production of endogenous agonist(s). - demonstrate that the liver phenotype is not due to inhibition of hepatic ATGL. - determine whether the reduction of adipose inflammation is due to ATGL expression in macrophages. 2. As mentioned by the Authors, the data suggest that the decreased fat mass observed in high fat
2 diet-fed ATGL inhibitor-treated mice cannot be entirely explained by reduced food intake and intestinal fat absorption. Yet, no increase in energy expenditure could be observed maybe due to the limitations of indirect calorimetry in capturing moderate changes. The ATGL inhibitor accumulates in white adipose tissue and liver but not in other tissues with ATGL expression (Fig. 5a). The abundance of the inhibitor is not reported in brown adipose tissue. Change in cell size in brown fat (as also reported in white fat in Fig. 1) suggests that the inhibitor accumulates in brown adipose tissue where it could modify thermogenic activity. Treatment of high fat-fed mice with the ATGL inhibitor in a thermoneutral environment may help determining whether brown adipose tissue thermogenesis contribute to the decreased body weight gain. 3. During chronic treatments, assessment of ATGL and HSL protein level and enzymatic activity will document whether the ATGL inhibitor has effects on adipose lipase expression. Other points 1. The concept of inhibition of adipose tissue lipolysis in the treatment of the metabolic syndrome is not a new one. Nicotinic acid, an antilipolytic molecule acting on a GPCR was proposed in the treatment of dyslipidemia 50 years ago. Nicotinic acid and acipimox, a related molecule, have been tested in humans for action on insulin resistance. Several chemical series of inhibitors for another adipose lipase, hormone-sensitive lipase (HSL), have been synthesized with some compounds being tested on metabolic complications. This rationale needs to be mentioned in the introduction section. 2. Dr. Zechner reported at conferences (and maybe published?) that the molecule studied here is a poor inhibitor of human ATGL. This may be mentioned in the therapeutic perspectives of the Discussion section. 3. Fig. 3. LPL and DGAT are assessed as PPARgamma targets. A more complete survey of PPARgamma target genes with known functional PPAR-responsive elements in their promoters may support the conclusion of an inhibition of PPARgamma activity. 4. HOMA-IR is used in Table 1 to assess insulin sensitivity. Use of HOMA-IR is inappropriate in the mouse as the denominator factor of 22.5 used in the equation is human specific. QUICKI index may be used instead. Reviewer #3 (Remarks to the Author) ATGL is the rate-limiting enzyme of first step of lipolysis. Increasing adipose tissue lipolysis activity may increase circulating FFA in serum and lead to insulin resistance and NAFLD. Recent work showed that genetically inhibition of lipolysis could improve insulin sensitivity and protect mice from HFD induced obesity. Here, the authors tried to find whether ATGL inhibitor Atglistatin could act similarly as genetically inhibition. They described many beneficial effects from this drug treatment on HFD mice: plasma FFA is reduced; weight gain of WAT and the whole body is blunted; adipocytes inflammation is decreased; insulin sensitivity is improved by GTT and ITT assays. Surprisingly, the drug also protects mice from HFD-induced liver steatosis. Moreover, the drug-treating effect is better than ATGL genetic deficiency in that ATGL deficiency associated cardiac steatosis and cardiomyopathy is not observed in Atglistatin-treated mice. Overall, Atglistatin could indeed protect mice from HFD induced obesity, IR and liver steatosis based on their data. However, there are several major concerns with this manuscript. 1) As their previous works on genetically knockout ATGL mice show increased body weight and WAT weight in chow condition, what will happen if Atglistatin-treated mice are fed in chow condition? Will it behave similarly? As chronic chow feeding in wild type could also lead to NAFLD and IR, could Atglistatin work well in this case? 2) I noticed that the leptin level reducing remarkably (34.6 vs 3.8) in HFD 5h fasted condition which is shown in Table 1 while both control and ATGLi group food intake showed no significant differences. It is really intriguing to know the leptin level in normal condition, as it is not shown in this table. Basically, leptin regulates appetite effectively in WT mice. May Atglistatin affect leptin signaling pathway? This needs to be illustrated. 3) In oral lipid tolerant test, there is a delayed clearance of post-prandial fat concurred with a sharp reduction of LPL activity. LPL activity is very important to the FA import. Lower LPL activity
3 could result in fewer FA in cells and subsequently the decreased fat content phenotype in adipose tissue, liver and muscle. Since we don't have much information on Atglistatin target specificity, is it possible that Atglistatin also work as LPL inhibitor, besides its inhibition on ATGL? More characters of this drug should be provided to make this clear. 4) The effect of Atglistatin in liver is surprising and intriguing. Since the concentration of Atglistatin is very high in ATGLi liver, the authors should measure the lipolysis activity in liver extracts. 5) In the discussion, the authors want to discuss the paper published in Diabetes, 2009 by Ahmadian et al, which reported that overexpression of ATGL lead to improved insulin sensitivity.
4 Point to point response to the referees: Reviewer #1: We thank the reviewer for the overall positive and constructive criticism. Many aspects of the phenomenon were recently reported in PNAS. One would hope that a novel chemical inhibitor might provide new mechanistic insights regarding effects on food intake, lipid synthesis, TG handling and glucose metabolism. However, the data seem to be mostly descriptive, and the reasons underlying the fascinating differences between genetic and pharmacological inhibition remain unresolved. Nevertheless, the data do establish a proof of principle for ATGL inhibition. We agree with the reviewer that we observed several consistencies between the genetic model of ATGL deficiency and the pharmacological inhibition of ATGL. This accordance confirms the efficacy and target specificity of the inhibitor. However, we also report on some important and unexpected differences between the genetic and pharmacological model. In contrast to findings in global ATGL deficiency, transient inhibition of lipolysis by Atglistatin leads to reduced cardiac and hepatic steatosis, reduced WAT inflammation, and no changes in BAT morphology in mice on a HFD. These beneficial effects upon inhibitor treatment highlight in our view the potential of ATGL as a target to treat obesity and its metabolic consequences. 1) Experiments in figure 1 seem to be contrived to show transient effect, but the design is not strictly relevant to chronic dosing and ad libitum feeding. It would seem difficult to deconvolve the effects of compound on food intake, lipid synthesis, fasting lipid mobilization etc. when administered in the food. The appeal to dose timing and tissue partitioning is speculative. We agree with reviewer that our data does not represent a solid pharmacodynamic study on the inhibitor. However, the transient nature of inhibitor impact is clearly apparent from the fasting experiments presented in Fig. 1. Ex vivo lipolysis assays using fat explants demonstrate that feeding Atglistatin leads to decreased adipose tissue lipolysis whereas fasting of mice for 8 h completely restores FA release. When administered by gavage or by ip. injection, we previously demonstrated that the effect of Atglistatin is transient (Mayer et al., Nat. Chem. Biol., 2013). Twelve hours after a single Atglistatin administration, FA and glycerol levels are similar in treated and untreated animals arguing for a loss of drug efficacy after this time period. We are aware of the fact that ad libitum inhibitor feeding results in a somewhat undefined fluctuation of inhibitor concentrations in blood and tissues and discuss this fact in relation to the observed phenotypes. 2) Is the effect of compound reversible? Previously we demonstrated that Atglistatin is a competitive inhibitor of ATGL (Mayer et al., Nat. Chem. Biol., 2013). Its effect on plasma levels of lipolytic products (FA and glycerol) is reversed upon withdrawal 1
5 of the inhibitor. In the current manuscript, we additionally show that plasma FA levels almost reach control levels already after 5 h fasting. Moreover, using fat explants, we demonstrate that fasting Atglistatin-treated mice reverses its inhibitory effect on adipose tissue lipolysis ex vivo. MS analysis revealed that the compound is not detectable in plasma or tissues of mice fasted for more than 5h (data not shown). Thus we assume that Atglistatin is washed out of the body or degraded, which renders its effects reversible. 3) Atglistatin and ATGL KO both reduced white fat pad size of mice on HFD. However, the effects in BAT are highly discordant. The effect of compound on BAT morphology is very striking and is suggestive of activation. Did the authors look at indices of BAT activation, like Ucp1, Cidea, Pgc1a, etc? The reviewer raises an important point that we addressed with additional experiments displayed in Supplemental Fig. 4. We assessed mrna levels of Ucp-1, Pgc1a and CideA in ibat and found no differences between control and ATGLi animals (Supplemental Fig 4a). Interestingly, UCP1 protein levels were significantly increased in ibat of ATGLi mice (Supplemental Fig 4 b). Despite this increase in UCP1 protein, telemetry sensors implanted in to the abdominal cavity of mice did not reveal differences in core body temperature (Supplemental Fig 4c). To assess whether differences in thermogenesis over an extended period of time contribute to reduced weight gain, we fed mice a HFD in the presence and absence of Atglistatin under thermoneutral conditions (Supplemental Fig 4d-h). We show that ATGLi animals were resistant to diet induced obesity also under thermoneutral conditions indicating that the obesity resistant phenotype is not caused by alterations in BAT activity. 4) Measuring Atglistatin levels in adipose tissue and liver does not establish the site of action, as is claimed. The analytical method (Folch extraction) indicates that the compound is highly hydrophobic and the ATGL measured will be that which has partitioned into lipid. In addition, nothing is reported on the PK of Atglistatin, and it seems unlikely that levels of pmol/g are physiologically meaningful. Given the diverse effects on food intake, lipid absorption and clearance, etc. it is not clear what effects are primary and secondary to lipolysis inhibition. The logp value for Atglistatin is 2.85 making it a highly hydrophobic molecule that presumably binds to cellular lipid and membrane fractions. This also explains why Atglistatin can be efficiently extracted from tissues by the Folch method. We agree with the reviewer that a tissue concentration of Atglistatin in the range of 500 pmol/g (Fig. 5a) is low but assume that the local concentration on LDs may be much higher and explain the efficacy of the inhibitor. This is now discussed in the revised version of the manuscript. With regard to primary and secondary effects of Atglistatin, we conclude that inhibition of ATGL represents the primary effect of the inhibitor and that all other observed effects and phenotypes are secondary to reduced lipolysis (or potential off target effects). 5) The experiments do not test the premise regarding FFA release from adipose tissue. 2
6 The fat pad assay performed in the current study is a well-established in vitro method to measure the FA release from adipose tissue (Schweiger et al., Meth Enzymol, 2014; Jaworski et al., Nat Med, 2009, Kosteli et al., JCI, 2010; Girousse et al., PlosBiol, 2013; ). 6) The claim that the lipid lowering effect of Atglistatin depends on the expression of ATGL in the liver, is not demonstrated since ATGL levels in liver specifically were not manipulated nor was ATGL activity measured in the liver. We agree that the sentence The lipid lowering effect of Atglistatin depends on the expression of ATGL in the liver, as liver samples of AKO/cTg mice that completely lack ATGL in all tissues except cardiac muscle exhibited increased hepatic fat content that could not be reduced by Atglistatin is misleading and changed it to: The lipid lowering effect of Atglistatin is target-specific, because Atglistatin had no effect on the increased hepatic fat content in AKO/cTg mice that lack ATGL in all tissues except cardiac muscle. The contrary results on liver steatosis in ATGLi mice and global as well as liver-specific ATGL knockout models indicates that Atglistatin does not inhibit hepatocyte lipolysis sufficiently (unlike genetic inactivation) to cause TAG accumulation. This conclusion is supported by our finding that TG hydrolase activities in liver extracts of inhibitor treated and untreated mice were identical (Suppl. Fig. 9b). This inability of Atglistatin to inhibit hepatic ATGL and lipolysis may result from increased ATGL enzyme protein levels (Suppl. Fig. 9a), the transient nature of Atglistatin s action (Mayer et al., Nat Chem Biol, 2013), or the compensatory activity of alternative, currently unknown, TG hydrolases. The existence of alternative lipases is corroborated by the relatively small contribution of ATGL to the total lipolytic activity in liver lysates (see attached Fig.1). The various possibilities to explain or findings are discussed in the paper. Reviewer #2 We thank the reviewer for his/her insightful and constructive comments. 1. To assess the specificity of ATGL effects, the authors used transgenic mice which express ATGL only in heart and do not die from cardiomyopathy. Using these mice, the authors show that the lower increase of inguinal white adipose tissue weight during high fat diet is due to ATGL. However, some important questions cannot be addressed using heart-rescued ATGL knockout mice. Adipocyte-specific ATGL knock out mice treated with the ATGL inhibitor could be useful to: (i) prove that the control of fat mass is mediated by adipose ATGL inhibition and activation of PPAR gamma through production of endogenous agonist(s) (ii) demonstrate that the liver phenotype is not due to inhibition of hepatic ATGL. (iii) determine whether the reduction of adipose inflammation is due to ATGL expression in macrophages. 3
7 We agree with the reviewer that experiments with Atglistatin-treated adipose tissue-specific ATGLdeficient mice would additionally validate Atglistatin s target specificity. However, we provide this validation already in global ATGL-deficient mice in the paper and believe that this model is generally more appropriate to delineate ATGL-dependent and ATGL-independent effects of the inhibitor. We believe that the relatively minor additional information gained by a repetition of these experiments in adipose-specific knockout mice does not warrant a considerable further extension of the revision period by several months, which it would take to re-raise the appropriate animals and perform the requested experiments. Moreover, most questions raised by the reviewer can be answered by comparing the phenotypes observed in tissue-specific ATGL deficient animals and Atglistatin-treated mice. ad (1) Schreiber et al., (PNAS 2015) demonstrated that heart-rescued ATGL ko mice are protected from HFD induced obesity due to reduced adipose PPARg activity and fat synthesis as well as decreased calorie intake. Consistent with these findings, Schoiswohl et al. (Endocrinology, 2015) showed that adiposespecific ATGL-deficient animals on a HFD also exhibited reduced weight gain and reduced expression of genes responsible for de novo lipogenesis, lipid uptake, and lipid synthesis (PPARg target genes) in WAT. Finally, we demonstrate in the current study that in accordance with the knockout models ATGL inhibition by Atglisatin also reduces adipose tissue mass by reduced food intake and reduced expression of selected PPARg target genes in WAT (Fig. 3h)of mice on a HFD. Taken together, these data led to our conclusion that the reduced on PPARg target gene expression and decreased fat mass in ATGLi mice is due to the inhibition of ATGL in adipose tissue. This conclusion is reminiscent of a similar outcome in cardiac muscle-specific ATGL-deficient mice, where the lack of ATGL leads to defective PPAR signaling, mitochondrial dysfunction and cardiomyopathy. Evidently, ATGL-mediated lipolysis is a general requirement for effective PPAR function. Whether lipolytic products of ATGL like FAs and DAGs directly act as PPAR ligands or whether more indirect mechanisms (such as FA or DAG conversion into other ligands of PPARs) are responsible for PPAR activation remains to be elucidated. ad (ii)atgl gene deletion in the liver in global or liver-specific ATGL knockout mice causes hepatosteatosis and liver inflammation (Haemmerle, G. et al. Science, 2006; Hoy et al., Endocrinology, 2010; Wu et al., Hepatology, 2011; (LIT.) In contrast, Atglistatin treatment ameliorates hepatic steatosis and inflammation in HFD-fed or ob/ob mice. Similarly as ATGLi mice, adipose-specific ATGL deficientanimals also exhibit reduced hepatic lipid levels and reduced inflammatory marker gene expression (Schoiswohl et al., Endocrinology, 2015). Therefore we assume that the beneficial effect of Atglistatin treatment on liver pathology is not caused by the inhibition of hepatic lipolysis but instead by an inhibition of adipose tissue lipolysis and a concomitant decrease in FA flux from adipose tissue to the liver. This assumption is corroborated by the inability of Atglistatin to lower TG hydrolase activity in the liver of ATGLi animals (Supplemental Fig. 9b). Ad (iii) The reviewer raises an very important point. At this stage, we do not know whether Atglistatin inhibits macrophage ATGL and whether this may cause the antiinflammatory phenotype observed in inhibitor-treated animals. The previous finding that ATGL-deficient macrophages exhibit an M2-like, antiinflammatory phenotype (Aflaki et al, CMLS, 2011), however, potentially support this presumption. Also the fact that, unlike ATGLi mice, adipose-specific ATGL-deficient animals have increased WAT inflammation (F480, cd11c, IL6, TNFa) (Schoiswohl et al, Endocrinology, 2015) argues for a potential antiinflammatory role of the inhibitor via ATGL inhibition in adipose tissue resident macrophages. We believe that the role of Atglistatin in macrophages requires a more extended investigation beyond the 4
8 scope of the current work. However, we consider the role of macrophage ATGL and its potential inhibition by Atglistatin in the context of tissue inflammation in the discussion of the manuscript. 2. As mentioned by the Authors, the data suggest that the decreased fat mass observed in high fat dietfed ATGL inhibitor-treated mice cannot be entirely explained by reduced food intake and intestinal fat absorption. Yet, no increase in energy expenditure could be observed maybe due to the limitations of indirect calorimetry in capturing moderate changes. The ATGL inhibitor accumulates in white adipose tissue and liver but not in other tissues with ATGL expression (Fig. 5a). The abundance of the inhibitor is not reported in brown adipose tissue. Change in cell size in brown fat (as also reported in white fat in Fig. 1) suggests that the inhibitor accumulates in brown adipose tissue where it could modify thermogenic activity. Treatment of high fat-fed mice with the ATGL inhibitor in a thermoneutral environment may help determining whether brown adipose tissue thermogenesis contribute to the decreased body weight gain. We thank the reviewer for raising this important point. In accordance with her/his recommendations, we performed MS analyses and found high concentrations of Atglistatin in ibat (Fig. 5a). We also measured core body temperature in mice using abdominally implanted telemetric sensors but did not observe significant differences in Atglistatin-treated or untreated mice (Supplemental Fig. 4). Finally, we followed the suggestion of the reviewer to study mice at thermoneutral conditions. To assess weight loss independent of reduced food intake we pair-fed the animals. We found that similar as in ambient conditions Atglistatin-fed animals lost more body weight due to fat loss (ibat, iwat, gwat) than pair-fed control mice also in thermoneutrality. Unlike in the genetic knockout model, brown adipocytes became smaller by Atglistatin treatment in thermoneutrality (Supplemental Fig. 4). Together, these data argue against an increase in BAT activity upon Atglistatin feeding that would contribute to decreased body weight gain. 3. During chronic treatments, assessment of ATGL and HSL protein level and enzymatic activity will document whether the ATGL inhibitor has effects on adipose lipase expression. As suggested by the reviewer, we performed Western blot analysis and found that Atglistatin treatment caused an increase in ATGL and a slight decrease in HSL protein abundance in gwat (Supplemental Fig.1). Despite increased cellular ATGL protein levels, adipose tissue explants from ATGLi mice released less FA and glycerol than explants from untreated mice arguing for effective inhibition by Atglistatin (Figure 1). Other points 1. The concept of inhibition of adipose tissue lipolysis in the treatment of the metabolic syndrome is not a new one. Nicotinic acid, an antilipolytic molecule acting on a GPCR was proposed in the treatment of dyslipidemia 50 years ago. Nicotinic acid and acipimox, a related molecule, have been tested in humans for action on insulin resistance. Several chemical series of inhibitors for another adipose lipase, hormone- 5
9 sensitive lipase (HSL), have been synthesized with some compounds being tested on metabolic complications. This rationale needs to be mentioned in the introduction section. We agree and extended the introduction accordingly by adding : Nicotinic acid (niacin) has been used in humans to lower plasma lipids by targeting lipolysis via a G-protein coupled receptor. However, the drug has several off-target side effects limiting its acceptance by patients (Karpe et al., Lancet, 2004). Another approach constitutes the inhibition of either of the two main adipose tissue lipases. To date, only smallmolecule inhibitors for HSL have been tested in mice and this treatment resulted in improved insulin sensitivity but did not affect body weight, fat mass, and WAT inflammation in mice fed a high caloric diet (Girousse et al. Plos Biol, 2013). 2. Dr. Zechner reported at conferences (and maybe published?) that the molecule studied here is a poor inhibitor of human ATGL. This may be mentioned in the therapeutic perspectives of the Discussion section. We include the requested figure (Figure 1 d, e) showing that Atglistatin does not inhibit human ATGL or human adipocyte lipolysis. 3. Fig. 3. LPL and DGAT are assessed as PPARgamma targets. A more complete survey of PPARgamma target genes with known functional PPAR-responsive elements in their promoters may support the conclusion of an inhibition of PPARgamma activity. In accordance with this recommendation, we now show reduced WAT expression of Angptl4, Cd36, and G0s2 as typical additional target genes for PPARγ (Fig. 3h). 4. HOMA-IR is used in Table 1 to assess insulin sensitivity. Use of HOMA-IR is inappropriate in the mouse as the denominator factor of 22.5 used in the equation is human specific. QUICKI index may be used instead. Again an important point that we were happy to address. We calculated quantitative insulin sensitivity check index (QUICKI) for our animals and found a highly significant increase in Atglistatin treated compared to control HFD fed mice, verifying improved insulin sensitivity (included in Table1). Reviewer #3 We thank the reviewer for the thorough review and important input. 1) As their previous works on genetically knockout ATGL mice show increased body weight and WAT weight in chow condition, what will happen if Atglistatin-treated mice are fed in chow condition? Will it 6
10 behave similarly? As chronic chow feeding in wild type could also lead to NAFLD and IR, could Atglistatin work well in this case? We followed the suggestion of the reviewer and performed the chronic feeding of Atglistatin in animals on chow diet. As shown in Supplemental Fig. 7 and Fig. 5h, effects of Atglistatin on body weight gain, fat mass reduction, and reduction in liver fat were similar but less pronounced than in mice on HFD. Consistent with this more moderate effect, we did not observe significant changes in insulin and glucose tolerance or food intake in chow-fed Atglistatin-treated versus untreated mice. 2) I noticed that the leptin level reducing remarkably (34.6 vs 3.8) in HFD 5h fasted condition which is shown in Table 1 while both control and ATGLi group food intake showed no significant differences. It is really intriguing to know the leptin level in normal condition, as it is not shown in this table. Basically, leptin regulates appetite effectively in WT mice. May Atglistatin affect leptin signaling pathway? This needs to be illustrated. As suggested by the reviewer, we measured leptin concentrations in re-fed conditions and found them also significantly reduced in Atglistatin treated animals (Table 1). To answer the reviewer s question on leptin signaling, we performed leptin sensitivity assays (attached Fig. 2). We found both groups (control as well as Atglistatin treated animals) to be identically leptin resistant. Hence, despite markedly reduced leptin levels in ATGLi mice, leptin sensitivity is unaltered compared to untreated animals. We also performed qpcr analysis to assess hypothalamic leptin signaling and found, Agrp and NPY increased; POMPC and CARTPT decreased in ad libitum fed mice (attached Fig. 2). This indicates that ATGLi mice may have increased appetite but still eat less. This counter-intuitive observation adds to the mystery how reduced adipose tissue lipolysis affects food intake, a question that must be thoroughly addressed in future work and cannot be answered by the current study. 3) In oral lipid tolerant test, there is a delayed clearance of post-prandial fat concurred with a sharp reduction of LPL activity. LPL activity is very important to the FA import. Lower LPL activity could result in fewer FA in cells and subsequently the decreased fat content phenotype in adipose tissue, liver and muscle. Since we don't have much information on Atglistatin target specificity, is it possible that Atglistatin also work as LPL inhibitor, besides its inhibition on ATGL? More characters of this drug should be provided to make this clear. We agree that this is a very important point. In a previous publication (Mayer et al, Nat. Chem. Biol., 2013) we investigated the target specificity of Atglistatin and showed that Atglistatin does not directly affect LPL activity. In this work we measured heparin releasable LPL activity from adipose tissue and found it to be drastically reduced. This reduction is presumably due to reduced LPL expression as a result of reduced PPARg signaling and goes along with a downregulation of other PPARg target genes (Fig.3h). 7
11 4) The effect of Atglistatin in liver is surprising and intriguing. Since the concentration of Atglistatin is very high in ATGLi liver, the authors should measure the lipolysis activity in liver extracts. We previously demonstrated that addition of Atglistatin to liver extracts inhibits ATGL activity (Mayer et al., Nat Chem Biol, 2013, Figure attached). As suggested by the reviewer we performed TG hydrolase activity assays from liver extracts of Atglistatin fed animals but did not observe differences to activities found in livers of untreated animals (attached Fig. 1 and Supplemental Fig. 9b). This indicates that in vivo Atglistatin does not efficiently inhibit lipolysis. This inability of Atglistatin to inhibit hepatic ATGL and lipolysis all together may result from increased ATGL enzyme protein levels (Suppl. Fig. 9a), the transient nature of Atgilstatin s action (Mayer et al., Nat Chem Biol, 2013), or the compensatory activity of alternative, currently unknown, TG hydrolases. The existence of alternative lipases is corroborated by the relatively small contribution of ATGL to the total lipolytic activity in liver lysates (see attached Fig.1). The various possibilities to explain or findings are discussed in the paper. 5) In the discussion, the authors want to discuss the paper published in Diabetes, 2009 by Ahmadian et al, which reported that overexpression of ATGL lead to improved insulin sensitivity. We are sorry for this neglect and included the publication of Ahmadian et al. in the discussion of the manuscript. 8
12 Attached Figures Attached Fig. 1:TG hydrolase activity of liver lysates from wild-type and ATGL deficient animals in the presence and in the absence of Atglistatin. Lysates of liver of wild-type (wt) and ATGL-ko mice were subjected for TG hydrolase activity assays in the presence or absence of 40 µm Atglistatin using a substrate containing radiolabeled [9,10-3H(N)]-triolein. After incubation for 1h at 37 C, FA were extracted and quantitated by liquid scintilation counting. Data are presented as mean + S.D. (n=3 for each genotype; **, p < 0.01 for +/- Atglistatin and ##, p < 0.01, for WT vs. ATGL-ko). Attached Fig. 2: Leptin sensitivity and hypothalamic gene expression upon Atglistatin feeding. ATGLi and control mice were fasted for 6 h and re-fed after the injection of 5mg/kg leptin or Tris/Cl as control. At the indicated timepoints food intake was assessed by subtracting food uneaten from the amount of food added to the bottom of cages. Hypothalamic mrna expression was assessed of re-fed mice by RT-qPCR. 9
13 Reviewer #1 (Remarks to the Author) Overall, the revised manuscript is technically sound, the conclusion are well supported, and limitations acknowledged. The main strength of the report is the proof of principle that pharmacologic inhibition of ATGL can have beneficial effects on glucose homeostasis and reduce steatosis in liver and heart in mouse models. The authors acknowledge that the concept of inhibiting adipocyte lipolysis to improve glucose homeostasis and reduce ectopic fat accumulation is not new. On the other hand, the concept that transient,tissue-specific lipase inhibition might be the key to the benefits of ATGL inhibition and explain differences in genetic and pharmacologic models is new and potentially important. Based on this work, it would seem that the benefits of ATGL inhibition in mice relate importantly to unique properties of the inhibitor, including PK, tissue distribution, route of administration, and effects on food intake. However, the mechanisms and sites of action underlying inactivation of ATGL presently remain a matter of informed speculation, and it is uncertain whether these properties can be reproduced in humans. Reviewer #3 (Remarks to the Author) Thanks for properly addressing my comments. The effects of Atglistatin on HFD are both exciting and intriguing.
control kda ATGL ATGLi HSL 82 GAPDH * ** *** WT/cTg WT/cTg ATGLi AKO/cTg AKO/cTg ATGLi WT/cTg WT/cTg ATGLi AKO/cTg AKO/cTg ATGLi iwat gwat ibat
 body weight (g) tissue weights (mg) ATGL protein expression (relative to GAPDH) HSL protein expression (relative to GAPDH) ### # # kda ATGL 55 HSL 82 GAPDH 37 2.5 2. 1.5 1..5 2. 1.5 1..5.. Supplementary
body weight (g) tissue weights (mg) ATGL protein expression (relative to GAPDH) HSL protein expression (relative to GAPDH) ### # # kda ATGL 55 HSL 82 GAPDH 37 2.5 2. 1.5 1..5 2. 1.5 1..5.. Supplementary
Supplemental Information Supplementary Table 1. Tph1+/+ Tph1 / Analyte Supplementary Table 2. Tissue Vehicle LP value
 Supplemental Information Supplementary Table. Urinary and adipose tissue catecholamines in Tph +/+ and Tph / mice fed a high fat diet for weeks. Tph +/+ Tph / Analyte ewat ibat ewat ibat Urine (ng/ml)
Supplemental Information Supplementary Table. Urinary and adipose tissue catecholamines in Tph +/+ and Tph / mice fed a high fat diet for weeks. Tph +/+ Tph / Analyte ewat ibat ewat ibat Urine (ng/ml)
Deficiency in mtorc1-controlled C/EBPβ-mRNA translation improves metabolic health in mice
 Manuscript EMBOR-2014-39837 Deficiency in mtorc1-controlled C/EBPβ-mRNA translation improves metabolic health in mice Laura M. Zidek, Tobias Ackermann, Götz Hartleben, Sabrina Eichwald, Gertrud Kortman,
Manuscript EMBOR-2014-39837 Deficiency in mtorc1-controlled C/EBPβ-mRNA translation improves metabolic health in mice Laura M. Zidek, Tobias Ackermann, Götz Hartleben, Sabrina Eichwald, Gertrud Kortman,
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature12652 Supplementary Figure 1. PRDM16 interacts with endogenous EHMT1 in brown adipocytes. Immunoprecipitation of PRDM16 complex by flag antibody (M2) followed by Western blot analysis
doi:10.1038/nature12652 Supplementary Figure 1. PRDM16 interacts with endogenous EHMT1 in brown adipocytes. Immunoprecipitation of PRDM16 complex by flag antibody (M2) followed by Western blot analysis
Lack of TRPV2 impairs thermogenesis in mouse brown adipose tissue
 Manuscript EMBO-2015-40819 Lack of TRPV2 impairs thermogenesis in mouse brown adipose tissue Wuping Sun, Kunitoshi Uchida, Yoshiro Suzuki, Yiming Zhou, Minji Kim, Yasunori Takayama, Nobuyuki Takahashi,
Manuscript EMBO-2015-40819 Lack of TRPV2 impairs thermogenesis in mouse brown adipose tissue Wuping Sun, Kunitoshi Uchida, Yoshiro Suzuki, Yiming Zhou, Minji Kim, Yasunori Takayama, Nobuyuki Takahashi,
Supplementary Figure 1. DNA methylation of the adiponectin promoter R1, Pparg2, and Tnfa promoter in adipocytes is not affected by obesity.
 Supplementary Figure 1. DNA methylation of the adiponectin promoter R1, Pparg2, and Tnfa promoter in adipocytes is not affected by obesity. (a) Relative amounts of adiponectin, Ppar 2, C/ebp, and Tnf mrna
Supplementary Figure 1. DNA methylation of the adiponectin promoter R1, Pparg2, and Tnfa promoter in adipocytes is not affected by obesity. (a) Relative amounts of adiponectin, Ppar 2, C/ebp, and Tnf mrna
GPR120 *** * * Liver BAT iwat ewat mwat Ileum Colon. UCP1 mrna ***
 a GPR120 GPR120 mrna/ppia mrna Arbitrary Units 150 100 50 Liver BAT iwat ewat mwat Ileum Colon b UCP1 mrna Fold induction 20 15 10 5 - camp camp SB202190 - - - H89 - - - - - GW7647 Supplementary Figure
a GPR120 GPR120 mrna/ppia mrna Arbitrary Units 150 100 50 Liver BAT iwat ewat mwat Ileum Colon b UCP1 mrna Fold induction 20 15 10 5 - camp camp SB202190 - - - H89 - - - - - GW7647 Supplementary Figure
Mobilisation des lipides du tissu adipeux et insulinorésistance. Dominique Langin
 Obesity Research Laboratory Institut Universitaire de France Franco-Czech Laboratory for Clinical Research on Obesity Mobilisation des lipides du tissu adipeux et insulinorésistance Dominique Langin Séminaire
Obesity Research Laboratory Institut Universitaire de France Franco-Czech Laboratory for Clinical Research on Obesity Mobilisation des lipides du tissu adipeux et insulinorésistance Dominique Langin Séminaire
Reviewers' comments: Reviewer #1 (expert in lipid metabolism) Remarks to the Author:
 Reviewers' comments: Reviewer #1 (expert in lipid metabolism) Remarks to the Author: In the manuscript by Ohno et al, the authors set out to identify the enzyme responsible for the ester bond formation
Reviewers' comments: Reviewer #1 (expert in lipid metabolism) Remarks to the Author: In the manuscript by Ohno et al, the authors set out to identify the enzyme responsible for the ester bond formation
SUPPLEMENTARY INFORMATION
 DOI: 10.1038/ncb2211 a! mir-143! b! mir-103/107! let-7a! mir-144! mir-122a! mir-126-3p! mir-194! mir-27a! mir-30c! Figure S1 Northern blot analysis of mir-143 expression dependent on feeding conditions.
DOI: 10.1038/ncb2211 a! mir-143! b! mir-103/107! let-7a! mir-144! mir-122a! mir-126-3p! mir-194! mir-27a! mir-30c! Figure S1 Northern blot analysis of mir-143 expression dependent on feeding conditions.
Supplementary Materials for
 www.sciencesignaling.org/cgi/content/full/8/407/ra127/dc1 Supplementary Materials for Loss of FTO in adipose tissue decreases Angptl4 translation and alters triglyceride metabolism Chao-Yung Wang,* Shian-Sen
www.sciencesignaling.org/cgi/content/full/8/407/ra127/dc1 Supplementary Materials for Loss of FTO in adipose tissue decreases Angptl4 translation and alters triglyceride metabolism Chao-Yung Wang,* Shian-Sen
ANSC/NUTR 601 GENERAL ANIMAL NUTRITION Stearoyl-CoA desaturase, VLDL metabolism, and obesity
 ANSC/NUTR 601 GENERAL ANIMAL NUTRITION Stearoyl-CoA desaturase, VLDL metabolism, and obesity I. Stearoyl coenzyme A desaturase and obesity in rodents A. Stearoyl coenzyme A desaturase (SCD) is the 9 desaturase.
ANSC/NUTR 601 GENERAL ANIMAL NUTRITION Stearoyl-CoA desaturase, VLDL metabolism, and obesity I. Stearoyl coenzyme A desaturase and obesity in rodents A. Stearoyl coenzyme A desaturase (SCD) is the 9 desaturase.
Niacin Metabolism: Effects on Cholesterol
 Niacin Metabolism: Effects on Cholesterol By Julianne R. Edwards For Dr. William R. Proulx, PhD, RD Associate Professor of Nutrition and Dietetics In partial fulfillments for the requirements of NUTR342
Niacin Metabolism: Effects on Cholesterol By Julianne R. Edwards For Dr. William R. Proulx, PhD, RD Associate Professor of Nutrition and Dietetics In partial fulfillments for the requirements of NUTR342
Up-Regulation of Mitochondrial Activity and Acquirement of Brown Adipose Tissue-Like Property in the White Adipose Tissue of Fsp27 Deficient Mice
 Up-Regulation of Mitochondrial Activity and Acquirement of Brown Adipose Tissue-Like Property in the White Adipose Tissue of Fsp27 Deficient Mice Shen Yon Toh 1,2,3., Jingyi Gong 2., Guoli Du 2., John
Up-Regulation of Mitochondrial Activity and Acquirement of Brown Adipose Tissue-Like Property in the White Adipose Tissue of Fsp27 Deficient Mice Shen Yon Toh 1,2,3., Jingyi Gong 2., Guoli Du 2., John
A synergistic anti-obesity effect by a combination of capsinoids and cold temperature through the promotion of beige adipocyte biogenesis
 A synergistic anti-obesity effect by a combination of capsinoids and cold temperature through the promotion of beige adipocyte biogenesis Kana Ohyama, 1,2 Yoshihito Nogusa, 1 Kosaku Shinoda, 2 Katsuya
A synergistic anti-obesity effect by a combination of capsinoids and cold temperature through the promotion of beige adipocyte biogenesis Kana Ohyama, 1,2 Yoshihito Nogusa, 1 Kosaku Shinoda, 2 Katsuya
In The Name Of God. In The Name Of. EMRI Modeling Group
 In The Name Of God In The Name Of God EMRI Modeling Group Cells work together in functionally related groups called tissues Types of tissues: Epithelial lining and covering Connective support Muscle movement
In The Name Of God In The Name Of God EMRI Modeling Group Cells work together in functionally related groups called tissues Types of tissues: Epithelial lining and covering Connective support Muscle movement
Supplementary Figure 1
 Supplementary Figure 1 how HFD how HFD Epi WT p p Hypothalamus p p Inguinal WT T Liver Lean mouse adipocytes p p p p p p Obese mouse adipocytes Kidney Muscle Spleen Heart p p p p p p p p Extracellular
Supplementary Figure 1 how HFD how HFD Epi WT p p Hypothalamus p p Inguinal WT T Liver Lean mouse adipocytes p p p p p p Obese mouse adipocytes Kidney Muscle Spleen Heart p p p p p p p p Extracellular
SUPPLEMENTARY DATA. Nature Medicine: doi: /nm.4171
 SUPPLEMENTARY DATA Supplementary Figure 1 a b c PF %Change - -4-6 Body weight Lean mass Body fat Tissue weight (g).4.3.2.1. PF GC iwat awat BAT PF d e f g week 2 week 3 NEFA (mmol/l) 1..5. PF phsl (Ser565)
SUPPLEMENTARY DATA Supplementary Figure 1 a b c PF %Change - -4-6 Body weight Lean mass Body fat Tissue weight (g).4.3.2.1. PF GC iwat awat BAT PF d e f g week 2 week 3 NEFA (mmol/l) 1..5. PF phsl (Ser565)
Expanded View Figures
 Expanded View Figures A B C D E F G H I J K L Figure EV1. The dysregulated lipid metabolic phenotype of mouse models of metabolic dysfunction is most pronounced in the fasted state. A L Male 12-weeks-old
Expanded View Figures A B C D E F G H I J K L Figure EV1. The dysregulated lipid metabolic phenotype of mouse models of metabolic dysfunction is most pronounced in the fasted state. A L Male 12-weeks-old
Metabolic Syndrome. DOPE amines COGS 163
 Metabolic Syndrome DOPE amines COGS 163 Overview - M etabolic Syndrome - General definition and criteria - Importance of diagnosis - Glucose Homeostasis - Type 2 Diabetes Mellitus - Insulin Resistance
Metabolic Syndrome DOPE amines COGS 163 Overview - M etabolic Syndrome - General definition and criteria - Importance of diagnosis - Glucose Homeostasis - Type 2 Diabetes Mellitus - Insulin Resistance
Regulation of adipose tissue remodeling by peripheral serotonin
 Regulation of adipose tissue remodeling by peripheral serotonin Sangkyu Park Catholic Kwandong University College of Medicine Department of Biochemistry Serotonin (5-HT) is a signaling molecule Hemostasis
Regulation of adipose tissue remodeling by peripheral serotonin Sangkyu Park Catholic Kwandong University College of Medicine Department of Biochemistry Serotonin (5-HT) is a signaling molecule Hemostasis
Targeting of the circadian clock via CK1δ/ε to improve glucose homeostasis in obesity
 Targeting of the circadian clock via CK1δ/ε to improve glucose homeostasis in obesity Peter S. Cunningham, Siobhán A. Ahern, Laura C. Smith, Carla S. da Silva Santos, Travis T. Wager and David A. Bechtold
Targeting of the circadian clock via CK1δ/ε to improve glucose homeostasis in obesity Peter S. Cunningham, Siobhán A. Ahern, Laura C. Smith, Carla S. da Silva Santos, Travis T. Wager and David A. Bechtold
Supplementary Table 2. Plasma lipid profiles in wild type and mutant female mice submitted to a HFD for 12 weeks wt ERα -/- AF-1 0 AF-2 0
 Supplementary Table 1. List of specific primers used for gene expression analysis. Genes Primer forward Primer reverse Hprt GCAGTACAGCCCCAAAATGG AACAAAGTCTGGCCTGTATCCA Srebp-1c GGAAGCTGTCGGGGTAGCGTC CATGTCTTCAAATGTGCAATCCAT
Supplementary Table 1. List of specific primers used for gene expression analysis. Genes Primer forward Primer reverse Hprt GCAGTACAGCCCCAAAATGG AACAAAGTCTGGCCTGTATCCA Srebp-1c GGAAGCTGTCGGGGTAGCGTC CATGTCTTCAAATGTGCAATCCAT
Control 7 d cold 7 d CL
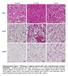 Control 7 d cold 7 d ibat iwat gwat Supplementary Figure 1. Histology of adipose tissues after cold or 3-adrenergic receptor stimulation. C57BL/6J wild-type mice were housed at 4 C or injected daily with
Control 7 d cold 7 d ibat iwat gwat Supplementary Figure 1. Histology of adipose tissues after cold or 3-adrenergic receptor stimulation. C57BL/6J wild-type mice were housed at 4 C or injected daily with
Effect of BI-1 on insulin resistance through regulation of CYP2E1
 Effect of BI-1 on insulin resistance through regulation of CYP2E1 Geum-Hwa Lee 1, Kyoung-Jin Oh 2, 3, Hyung-Ryong Kim 4, Hye-Sook Han 2, Hwa-Young Lee 1, Keun-Gyu Park 5, Ki-Hoan Nam 6, Seung-Hoi Koo 2
Effect of BI-1 on insulin resistance through regulation of CYP2E1 Geum-Hwa Lee 1, Kyoung-Jin Oh 2, 3, Hyung-Ryong Kim 4, Hye-Sook Han 2, Hwa-Young Lee 1, Keun-Gyu Park 5, Ki-Hoan Nam 6, Seung-Hoi Koo 2
PXL770, a novel direct AMPK activator, improves metabolic disorders in a diet-induced mice model of obesity and diabetes
 PXL770, a novel direct AMPK activator, improves metabolic disorders in a diet-induced mice model of obesity and diabetes Sébastien Bolze 1 ; Sophie Hallakou-Bozec 1 ; Michael Roden 2, 3,4 ; Julien Roux
PXL770, a novel direct AMPK activator, improves metabolic disorders in a diet-induced mice model of obesity and diabetes Sébastien Bolze 1 ; Sophie Hallakou-Bozec 1 ; Michael Roden 2, 3,4 ; Julien Roux
University of Groningen. Non-alcoholic fatty liver disease Sheedfar, Fareeba
 University of Groningen Non-alcoholic fatty liver disease Sheedfar, Fareeba IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen Non-alcoholic fatty liver disease Sheedfar, Fareeba IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Interplay between FGF21 and insulin action in the liver regulates metabolism
 Research article Interplay between FGF21 and insulin action in the liver regulates metabolism Brice Emanuelli, 1 Sara G. Vienberg, 1 Graham Smyth, 1 Christine Cheng, 2 Kristin I. Stanford, 1 Manimozhiyan
Research article Interplay between FGF21 and insulin action in the liver regulates metabolism Brice Emanuelli, 1 Sara G. Vienberg, 1 Graham Smyth, 1 Christine Cheng, 2 Kristin I. Stanford, 1 Manimozhiyan
University of California, San Diego La Jolla CA 92093
 AD Award Number: W81XWH-11-1-0131 TITLE: Role of Inflammation and Insulin Resistance in Mouse Models of Breast Cancer PRINCIPAL INVESTIGATOR: Jerrold Olefsky, M.D. CONTRACTING ORGANIZATION: University
AD Award Number: W81XWH-11-1-0131 TITLE: Role of Inflammation and Insulin Resistance in Mouse Models of Breast Cancer PRINCIPAL INVESTIGATOR: Jerrold Olefsky, M.D. CONTRACTING ORGANIZATION: University
Obesity in aging: Hormonal contribution
 Obesity in aging: Hormonal contribution Hormonal issues in obesity and aging Hormonal role in regulation of energy balance Genetic component in hormonal regulation Life style contribution to hormonal changes
Obesity in aging: Hormonal contribution Hormonal issues in obesity and aging Hormonal role in regulation of energy balance Genetic component in hormonal regulation Life style contribution to hormonal changes
Supporting Information
 Supporting Information Charalambous et al. 10.1073/pnas.1406119111 SI Experimental Procedures Serum and Tissue Biochemistry. Enzymatic assay kits were used for determination of plasma FFAs (Roche), TAGs
Supporting Information Charalambous et al. 10.1073/pnas.1406119111 SI Experimental Procedures Serum and Tissue Biochemistry. Enzymatic assay kits were used for determination of plasma FFAs (Roche), TAGs
BEIGE AND BROWN FAT: BASIC BIOLOGY AND NOVEL THERAPEUTICS Dr. Carl Ascoli
 BEIGE AND BROWN FAT: BASIC BIOLOGY AND NOVEL THERAPEUTICS Dr. Carl Ascoli Symposium Co-Chairs: Bruce M. Spiegelman (Harvard/Dana Farber) and Sven Enerbäck (U.Gothenburg) April 17-23, 2015 Snowbird Resort,
BEIGE AND BROWN FAT: BASIC BIOLOGY AND NOVEL THERAPEUTICS Dr. Carl Ascoli Symposium Co-Chairs: Bruce M. Spiegelman (Harvard/Dana Farber) and Sven Enerbäck (U.Gothenburg) April 17-23, 2015 Snowbird Resort,
Mfn2 deletion in brown adipose tissue protects from insulin resistance and impairs thermogenesis
 Article Mfn2 deletion in brown adipose tissue protects from insulin resistance and impairs thermogenesis Kiana Mahdaviani 1,2, Ilan Y Benador 1,2, Shi Su 1, Raffi A Gharakhanian 1, Linsey Stiles 1,2, Kyle
Article Mfn2 deletion in brown adipose tissue protects from insulin resistance and impairs thermogenesis Kiana Mahdaviani 1,2, Ilan Y Benador 1,2, Shi Su 1, Raffi A Gharakhanian 1, Linsey Stiles 1,2, Kyle
Males- Western Diet WT KO Age (wks) Females- Western Diet WT KO Age (wks)
 Relative Arv1 mrna Adrenal 33.48 +/- 6.2 Skeletal Muscle 22.4 +/- 4.93 Liver 6.41 +/- 1.48 Heart 5.1 +/- 2.3 Brain 4.98 +/- 2.11 Ovary 4.68 +/- 2.21 Kidney 3.98 +/-.39 Lung 2.15 +/-.6 Inguinal Subcutaneous
Relative Arv1 mrna Adrenal 33.48 +/- 6.2 Skeletal Muscle 22.4 +/- 4.93 Liver 6.41 +/- 1.48 Heart 5.1 +/- 2.3 Brain 4.98 +/- 2.11 Ovary 4.68 +/- 2.21 Kidney 3.98 +/-.39 Lung 2.15 +/-.6 Inguinal Subcutaneous
ENHANCEMENT OF BROWN ADIPOSE TISSUE DEVELOPMENT IN VIVO BY A NOVEL INSULIN SENSITIZER
 ENHANCEMENT F BRWN ADIPSE TISSUE DEVELPMENT IN VIV BY A NVEL INSULIN SENSITIZER William G. McDonald 1, Serena L. Cole 1, Brian N. Finck 2, Danielle D. Holewa 1, Angela S. Brightwell-Conrad 1, Charles Mackenzie
ENHANCEMENT F BRWN ADIPSE TISSUE DEVELPMENT IN VIV BY A NVEL INSULIN SENSITIZER William G. McDonald 1, Serena L. Cole 1, Brian N. Finck 2, Danielle D. Holewa 1, Angela S. Brightwell-Conrad 1, Charles Mackenzie
Inflammasome-mediated caspase-1 activity Gatekeeper of inflammation in the adipose tissue. Rinke Stienstra
 Inflammasome-mediated caspase-1 activity Gatekeeper of inflammation in the adipose tissue Rinke Stienstra Obesity promotes the development of insulin resistance and type 2 diabetes County-level Estimates
Inflammasome-mediated caspase-1 activity Gatekeeper of inflammation in the adipose tissue Rinke Stienstra Obesity promotes the development of insulin resistance and type 2 diabetes County-level Estimates
Cited4 is a sex-biased mediator of the antidiabetic glitazone response in adipocyte progenitors
 Cited4 is a sex-biased mediator of the antidiabetic glitazone response in adipocyte progenitors Irem Bayindir-Buchhalter, Gretchen Wolff, Sarah Lerch, Tjeerd Sijmonsma, Maximilian Schuster, Jan Gronych,
Cited4 is a sex-biased mediator of the antidiabetic glitazone response in adipocyte progenitors Irem Bayindir-Buchhalter, Gretchen Wolff, Sarah Lerch, Tjeerd Sijmonsma, Maximilian Schuster, Jan Gronych,
A Central Role of MG53 in Metabolic Syndrome. and Type-2 Diabetes
 A Central Role of MG53 in Metabolic Syndrome and Type-2 Diabetes Yan Zhang, Chunmei Cao, Rui-Ping Xiao Institute of Molecular Medicine (IMM) Peking University, Beijing, China Accelerated Aging in China
A Central Role of MG53 in Metabolic Syndrome and Type-2 Diabetes Yan Zhang, Chunmei Cao, Rui-Ping Xiao Institute of Molecular Medicine (IMM) Peking University, Beijing, China Accelerated Aging in China
Molecular pathways linking metabolic inflammation and thermogenesis G. Solinas Summary
 Published in "" which should be cited to refer to this work. Molecular pathways linking metabolic inflammation and thermogenesis G. Solinas http://doc.rero.ch Laboratory of Metabolic Stress Biology, Division
Published in "" which should be cited to refer to this work. Molecular pathways linking metabolic inflammation and thermogenesis G. Solinas http://doc.rero.ch Laboratory of Metabolic Stress Biology, Division
SUPPLEMENTARY DATA. Supplementary Table 1. Primers used in qpcr
 Supplementary Table 1. Primers used in qpcr Gene forward primer (5'-3') reverse primer (5'-3') β-actin AGAGGGAAATCGTGCGTGAC CAATAGTGATGACCTGGCCGT Hif-p4h-2 CTGGGCAACTACAGGATAAAC GCGTCCCAGTCTTTATTTAGATA
Supplementary Table 1. Primers used in qpcr Gene forward primer (5'-3') reverse primer (5'-3') β-actin AGAGGGAAATCGTGCGTGAC CAATAGTGATGACCTGGCCGT Hif-p4h-2 CTGGGCAACTACAGGATAAAC GCGTCCCAGTCTTTATTTAGATA
1.5 ASK1KO fed. fasted 16 hrs w/o water. Fed. 4th. 4th WT ASK1KO N=29, 11(WT), ,5(ASK1KO) ASK1KO ASK1KO **** Time [h]
![1.5 ASK1KO fed. fasted 16 hrs w/o water. Fed. 4th. 4th WT ASK1KO N=29, 11(WT), ,5(ASK1KO) ASK1KO ASK1KO **** Time [h] 1.5 ASK1KO fed. fasted 16 hrs w/o water. Fed. 4th. 4th WT ASK1KO N=29, 11(WT), ,5(ASK1KO) ASK1KO ASK1KO **** Time [h]](/thumbs/87/97258189.jpg) 7: 13: 19: 1: 7: 151117 a 151117 4th 4th b c RQ.95 KO.9.85.8.75.7 light dark light dark.65 7: 19: 7: 19: 7: Means ± SEM, N=6 RQ 1..9.8.7.6.6 KO CL (-) CL (+) ibat weight ratio (/body weight) [%].5.4.3.2.1
7: 13: 19: 1: 7: 151117 a 151117 4th 4th b c RQ.95 KO.9.85.8.75.7 light dark light dark.65 7: 19: 7: 19: 7: Means ± SEM, N=6 RQ 1..9.8.7.6.6 KO CL (-) CL (+) ibat weight ratio (/body weight) [%].5.4.3.2.1
Energy balance. Factors affecting energy input. Energy input vs. Energy output Balance Negative: weight loss Positive: weight gain
 1 Energy balance Energy input vs. Energy output Balance Negative: weight loss Positive: weight gain Special implications Infancy, Illness, Pregnancy & Lactation, Sports Factors affecting energy input neuro-endocrine
1 Energy balance Energy input vs. Energy output Balance Negative: weight loss Positive: weight gain Special implications Infancy, Illness, Pregnancy & Lactation, Sports Factors affecting energy input neuro-endocrine
A microrna-34a/fgf21 Regulatory Axis and Browning of White Fat
 A microrna-34a/fgf21 Regulatory Axis and Browning of White Fat Jongsook Kim Kemper, Ph.D Department of Molecular and Integrative Physiology, University of Illinois at Urbana-Champaign, USA 213 International
A microrna-34a/fgf21 Regulatory Axis and Browning of White Fat Jongsook Kim Kemper, Ph.D Department of Molecular and Integrative Physiology, University of Illinois at Urbana-Champaign, USA 213 International
Adipose tissue dysfunction in obesity. Gijs Goossens, PhD
 Adipose tissue dysfunction in obesity -The role of adipose tissue oxygenation - Gijs Goossens, PhD NUTRIM School of Nutrition and Translational Research in Metabolism Maastricht University Medical Centre
Adipose tissue dysfunction in obesity -The role of adipose tissue oxygenation - Gijs Goossens, PhD NUTRIM School of Nutrition and Translational Research in Metabolism Maastricht University Medical Centre
18s AAACGGCTACCACATCCAAG CCTCCAATGGATCCTCGTTA. 36b4 GTTCTTGCCCATCAGCACC AGATGCAGCAGATCCGCAT. Acc1 AGCAGATCCGCAGCTTG ACCTCTGCTCGCTGAGTGC
 Supplementary Table 1. Quantitative PCR primer sequences Gene symbol Sequences (5 to 3 ) Forward Reverse 18s AAACGGCTACCACATCCAAG CCTCCAATGGATCCTCGTTA 36b4 GTTCTTGCCCATCAGCACC AGATGCAGCAGATCCGCAT Acc1
Supplementary Table 1. Quantitative PCR primer sequences Gene symbol Sequences (5 to 3 ) Forward Reverse 18s AAACGGCTACCACATCCAAG CCTCCAATGGATCCTCGTTA 36b4 GTTCTTGCCCATCAGCACC AGATGCAGCAGATCCGCAT Acc1
ZL ZDF ZDF + E2 *** Visceral (g) ZDF
 Body Weight (g) 4 3 2 1 ** * ZL ZDF 6 8 1 12 14 16 Age (weeks) B * Sub-cutaneous (g) 16 12 8 4 ZL ZDF Visceral (g) 25 2 15 1 5 ZL ZDF Total fat pad weight (g) 4 3 2 1 ZDF ZL Supplemental Figure 1: Effect
Body Weight (g) 4 3 2 1 ** * ZL ZDF 6 8 1 12 14 16 Age (weeks) B * Sub-cutaneous (g) 16 12 8 4 ZL ZDF Visceral (g) 25 2 15 1 5 ZL ZDF Total fat pad weight (g) 4 3 2 1 ZDF ZL Supplemental Figure 1: Effect
NFIL3/E4BP4 controls Type 2 T helper cell cytokine expression
 Manuscript EMBO-2010-75657 NFIL3/E4BP4 controls Type 2 T helper cell cytokine expression Masaki Kashiwada, Suzanne L. Cassel, John D. Colgan and Paul B. Rothman Corresponding author: Paul Rothman, University
Manuscript EMBO-2010-75657 NFIL3/E4BP4 controls Type 2 T helper cell cytokine expression Masaki Kashiwada, Suzanne L. Cassel, John D. Colgan and Paul B. Rothman Corresponding author: Paul Rothman, University
MBB317. Dr D MANGNALL OBESITY. Lecture 2
 MBB317 Dr D MANGNALL OBESITY Lecture 2 When the structure of the insulin receptor was first discovered it was assumed that the active beta subunit tyrosine kinase would phosphorylate some intracellular
MBB317 Dr D MANGNALL OBESITY Lecture 2 When the structure of the insulin receptor was first discovered it was assumed that the active beta subunit tyrosine kinase would phosphorylate some intracellular
FADD is a key regulator of lipid metabolism
 Research Article FADD is a key regulator of lipid metabolism Hongqin Zhuang 1, Xueshi Wang 1, Daolong Zha 1, Ziyi Gan 1, Fangfang Cai 1, Pan Du 1, Yunwen Yang 1, Bingya Yang 1, Xiangyu Zhang 1, Chun Yao
Research Article FADD is a key regulator of lipid metabolism Hongqin Zhuang 1, Xueshi Wang 1, Daolong Zha 1, Ziyi Gan 1, Fangfang Cai 1, Pan Du 1, Yunwen Yang 1, Bingya Yang 1, Xiangyu Zhang 1, Chun Yao
Successful completion of Phase I clinical trial of AMPK activator O304
 Successful completion of Phase I clinical trial of AMPK activator O304 O304 is safe and very well tolerated in young healthy subjects, in middle aged obese subjects, and in type 2 diabetics in combination
Successful completion of Phase I clinical trial of AMPK activator O304 O304 is safe and very well tolerated in young healthy subjects, in middle aged obese subjects, and in type 2 diabetics in combination
General Laboratory methods Plasma analysis: Gene Expression Analysis: Immunoblot analysis: Immunohistochemistry:
 General Laboratory methods Plasma analysis: Plasma insulin (Mercodia, Sweden), leptin (duoset, R&D Systems Europe, Abingdon, United Kingdom), IL-6, TNFα and adiponectin levels (Quantikine kits, R&D Systems
General Laboratory methods Plasma analysis: Plasma insulin (Mercodia, Sweden), leptin (duoset, R&D Systems Europe, Abingdon, United Kingdom), IL-6, TNFα and adiponectin levels (Quantikine kits, R&D Systems
Gut microbiota, metabolic syndrome, obesity and the nutrient sensor pathways
 Gut microbiota, metabolic syndrome, obesity and the nutrient sensor pathways Department of Gastroenterology, Endocrinology & Metabolism Medical University Innsbruck Herbert Tilg Nothing to disclose Fig.
Gut microbiota, metabolic syndrome, obesity and the nutrient sensor pathways Department of Gastroenterology, Endocrinology & Metabolism Medical University Innsbruck Herbert Tilg Nothing to disclose Fig.
Regulation of Lipid Homeostasis: Lipid Droplets
 Regulation of Lipid Homeostasis: Lipid Droplets Bernd Helms Article Brand Recter Hendrik Mertens 1 The Basics I: FAs The Basics II: FA Activation 2 Basics III: TG-FA Interplay. Why? Adipocytes 3 Foam cells
Regulation of Lipid Homeostasis: Lipid Droplets Bernd Helms Article Brand Recter Hendrik Mertens 1 The Basics I: FAs The Basics II: FA Activation 2 Basics III: TG-FA Interplay. Why? Adipocytes 3 Foam cells
Supplemental Information. Increased 4E-BP1 Expression Protects. against Diet-Induced Obesity and Insulin. Resistance in Male Mice
 Cell Reports, Volume 16 Supplemental Information Increased 4E-BP1 Expression Protects against Diet-Induced Obesity and Insulin Resistance in Male Mice Shih-Yin Tsai, Ariana A. Rodriguez, Somasish G. Dastidar,
Cell Reports, Volume 16 Supplemental Information Increased 4E-BP1 Expression Protects against Diet-Induced Obesity and Insulin Resistance in Male Mice Shih-Yin Tsai, Ariana A. Rodriguez, Somasish G. Dastidar,
Desnutrin/ATGL Activates PPARd to Promote Mitochondrial Function for Insulin Secretion in Islet b Cells
 Article Desnutrin/ATGL Activates PPARd to Promote Mitochondrial Function for Insulin Secretion in Islet b Cells Tianyi Tang,,3 Marcia J. Abbott,,3 Maryam Ahmadian,,5 Andressa B. Lopes,,4 Yuhui Wang, and
Article Desnutrin/ATGL Activates PPARd to Promote Mitochondrial Function for Insulin Secretion in Islet b Cells Tianyi Tang,,3 Marcia J. Abbott,,3 Maryam Ahmadian,,5 Andressa B. Lopes,,4 Yuhui Wang, and
HIV VPR alters fat metabolism. Dorothy E Lewis PhD/Ashok Balasubramanyam MD
 HIV VPR alters fat metabolism Dorothy E Lewis PhD/Ashok Balasubramanyam MD Old Dogma for HIV associated lipodystrophy Differentiation Block (PI) Lipoatrophy Apoptosis (NRTI) Stem cell Preadipocyte Adipocyte
HIV VPR alters fat metabolism Dorothy E Lewis PhD/Ashok Balasubramanyam MD Old Dogma for HIV associated lipodystrophy Differentiation Block (PI) Lipoatrophy Apoptosis (NRTI) Stem cell Preadipocyte Adipocyte
Defective Hepatic Autophagy in Obesity Promotes ER Stress and Causes Insulin Resistance
 Cell Metabolism, Volume 11 Supplemental Information Defective Hepatic Autophagy in Obesity Promotes ER Stress and Causes Insulin Resistance Ling Yang, Ping Li, Suneng Fu, Ediz S. Calay, and Gökhan S. Hotamisligil
Cell Metabolism, Volume 11 Supplemental Information Defective Hepatic Autophagy in Obesity Promotes ER Stress and Causes Insulin Resistance Ling Yang, Ping Li, Suneng Fu, Ediz S. Calay, and Gökhan S. Hotamisligil
3-Thia Fatty Acids A New Generation of Functional Lipids?
 Conference on Food Structure and Food Quality 3-Thia Fatty Acids A New Generation of Functional Lipids? Rolf K. Berge rolf.berge@med.uib.no Fatty acids- Essential cellular metabolites Concentrations must
Conference on Food Structure and Food Quality 3-Thia Fatty Acids A New Generation of Functional Lipids? Rolf K. Berge rolf.berge@med.uib.no Fatty acids- Essential cellular metabolites Concentrations must
Effects of growth hormone secretagogue receptor agonist and antagonist in nonobese type 2 diabetic MKR mice
 Effects of growth hormone secretagogue receptor agonist and antagonist in nonobese type 2 diabetic MKR mice Rasha Mosa (MBCHC, M.D, PhD candidate) School of Biomedical Sciences University of Queensland
Effects of growth hormone secretagogue receptor agonist and antagonist in nonobese type 2 diabetic MKR mice Rasha Mosa (MBCHC, M.D, PhD candidate) School of Biomedical Sciences University of Queensland
Food Intake Regulation & the Clock. Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD
 Food Intake Regulation & the Clock Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD Circadian disruption affect multiple organ systems: The diagram provides examples of how circadian disruption
Food Intake Regulation & the Clock Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD Circadian disruption affect multiple organ systems: The diagram provides examples of how circadian disruption
Obesity-associated improvements in metabolic profile through expansion of adipose tissue
 JCI Online First. Published online on August 24, 2007. Research article Obesity-associated improvements in metabolic profile through expansion of adipose tissue Ja-Young Kim, 1 Esther van de Wall, 2 Mathieu
JCI Online First. Published online on August 24, 2007. Research article Obesity-associated improvements in metabolic profile through expansion of adipose tissue Ja-Young Kim, 1 Esther van de Wall, 2 Mathieu
Energy balance. Factors affecting energy input. Energy input vs. Energy output Balance Negative: weight loss Positive: weight gain
 1 Energy balance Energy input vs. Energy output Balance Negative: weight loss Positive: weight gain Special implications Infancy, Illness, Pregnancy & Lactation, Sports Factors affecting energy input neuro-endocrine
1 Energy balance Energy input vs. Energy output Balance Negative: weight loss Positive: weight gain Special implications Infancy, Illness, Pregnancy & Lactation, Sports Factors affecting energy input neuro-endocrine
Myelin suppresses axon regeneration by PIR-B/SHPmediated inhibition of Trk activity
 Manuscript EMBO-2010-76298 Myelin suppresses axon regeneration by PIR-B/SHPmediated inhibition of Trk activity Yuki Fujita, Shota Endo, Toshiyuki Takai and Toshihide Yamashita Corresponding author: Toshihide
Manuscript EMBO-2010-76298 Myelin suppresses axon regeneration by PIR-B/SHPmediated inhibition of Trk activity Yuki Fujita, Shota Endo, Toshiyuki Takai and Toshihide Yamashita Corresponding author: Toshihide
Supplementary Figure 1. DJ-1 modulates ROS concentration in mouse skeletal muscle.
 Supplementary Figure 1. DJ-1 modulates ROS concentration in mouse skeletal muscle. (a) mrna levels of Dj1 measured by quantitative RT-PCR in soleus, gastrocnemius (Gastroc.) and extensor digitorum longus
Supplementary Figure 1. DJ-1 modulates ROS concentration in mouse skeletal muscle. (a) mrna levels of Dj1 measured by quantitative RT-PCR in soleus, gastrocnemius (Gastroc.) and extensor digitorum longus
a b c Physical appearance of mice Lean mass Adipocyte size d e f
 LFD HFD LFD HFD Area under curve (GTT) HFD-VSL#3 LFD HFD Area under curve (ITT) HFD-VSL#3 Liver TG content (% l) HFD-VSL#3 LFD HFD HFD-VSL#3 LFD HFD HFD-VSL#3 LFD HFD HFD + VSL#3 Lean mass (gm) Mean adipocyte
LFD HFD LFD HFD Area under curve (GTT) HFD-VSL#3 LFD HFD Area under curve (ITT) HFD-VSL#3 Liver TG content (% l) HFD-VSL#3 LFD HFD HFD-VSL#3 LFD HFD HFD-VSL#3 LFD HFD HFD + VSL#3 Lean mass (gm) Mean adipocyte
Supplementary Figure S1. Effect of Glucose on Energy Balance in WT and KHK A/C KO
 Supplementary Figure S1. Effect of Glucose on Energy Balance in WT and KHK A/C KO Mice. WT mice and KHK-A/C KO mice were provided drinking water containing 10% glucose or tap water with normal chow ad
Supplementary Figure S1. Effect of Glucose on Energy Balance in WT and KHK A/C KO Mice. WT mice and KHK-A/C KO mice were provided drinking water containing 10% glucose or tap water with normal chow ad
Chapter 2. The Physiology of Fat
 Chapter 2 The Physiology of Fat Obesity, generalized and localized collections of adiposity, has become endemic in the United States. It is estimated that 25-40% of US adult females and 20-25% of adult
Chapter 2 The Physiology of Fat Obesity, generalized and localized collections of adiposity, has become endemic in the United States. It is estimated that 25-40% of US adult females and 20-25% of adult
Activités scientifiques
 Prof. Françoise Rohner-Jeanrenaud Activités scientifiques I. A role for adipose tissue de novo lipogenesis in glucose homeostasis during catch-up growth: A Randle cycle favoring fat storage Catch-up growth
Prof. Françoise Rohner-Jeanrenaud Activités scientifiques I. A role for adipose tissue de novo lipogenesis in glucose homeostasis during catch-up growth: A Randle cycle favoring fat storage Catch-up growth
Supplemental Fig. 1. Relative mrna Expression. Relative mrna Expression WT KO WT KO RT 4 0 C
 Supplemental Fig. 1 A 1.5 1..5 Hdac11 (ibat) n=4 n=4 n=4 n=4 n=4 n=4 n=4 n=4 WT KO WT KO WT KO WT KO RT 4 C RT 4 C Supplemental Figure 1. Hdac11 mrna is undetectable in KO adipose tissue. Quantitative
Supplemental Fig. 1 A 1.5 1..5 Hdac11 (ibat) n=4 n=4 n=4 n=4 n=4 n=4 n=4 n=4 WT KO WT KO WT KO WT KO RT 4 C RT 4 C Supplemental Figure 1. Hdac11 mrna is undetectable in KO adipose tissue. Quantitative
Supplementary Fig. 1 eif6 +/- mice show a reduction in white adipose tissue, blood lipids and normal glycogen synthesis. The cohort of the original
 Supplementary Fig. 1 eif6 +/- mice show a reduction in white adipose tissue, blood lipids and normal glycogen synthesis. The cohort of the original phenotypic screening was n=40. For specific tests, the
Supplementary Fig. 1 eif6 +/- mice show a reduction in white adipose tissue, blood lipids and normal glycogen synthesis. The cohort of the original phenotypic screening was n=40. For specific tests, the
Supplemental Table 1. Plasma NEFA and liver triglyceride levels in ap2-hif1ako and ap2-hif2ako mice under control and high fat diets.
 Supplemental Table 1. Plasma NEFA and liver triglyceride levels in Hif1aKO and Hif2aKO mice under control and high fat diets. Hif1a (n=6) Hif1aK O (n=6) Hif2a Hif2aK O Hif1a (n=5) Hif1aKO (n=5) Hif2a Hif2aK
Supplemental Table 1. Plasma NEFA and liver triglyceride levels in Hif1aKO and Hif2aKO mice under control and high fat diets. Hif1a (n=6) Hif1aK O (n=6) Hif2a Hif2aK O Hif1a (n=5) Hif1aKO (n=5) Hif2a Hif2aK
IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA
 UNIGASTRO Il fegato come centrale metabolica e i fattori di danno oltre ai virus epatitici IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA Dr Elisabetta Bugianesi Divisione di Gastro-Epatologia
UNIGASTRO Il fegato come centrale metabolica e i fattori di danno oltre ai virus epatitici IL METABOLISMO EPATICO DEI CARBOIDRATI IN FISIOLOGIA E PATOLOGIA Dr Elisabetta Bugianesi Divisione di Gastro-Epatologia
Adipose tissue: Roles and function in diabetes and beyond. August 2015; SAGLB.DIA
 Adipose tissue: Roles and function in diabetes and beyond August 2015; SAGLB.DIA.15.07.0398 Acknowledgement The following slides intend to summarise the key points presented during the Banting Medal for
Adipose tissue: Roles and function in diabetes and beyond August 2015; SAGLB.DIA.15.07.0398 Acknowledgement The following slides intend to summarise the key points presented during the Banting Medal for
The Physiology of Weight Regulation: Implications for Effective Clinical Care
 Roundtable on Obesity Solutions The Physiology of Weight Regulation: Implications for Effective Clinical Care Lee M. Kaplan, MD, PhD Obesity, Metabolism & Nutrition Institute Massachusetts General Hospital
Roundtable on Obesity Solutions The Physiology of Weight Regulation: Implications for Effective Clinical Care Lee M. Kaplan, MD, PhD Obesity, Metabolism & Nutrition Institute Massachusetts General Hospital
Gene Polymorphisms and Carbohydrate Diets. James M. Ntambi Ph.D
 Gene Polymorphisms and Carbohydrate Diets James M. Ntambi Ph.D Fatty Acids that Flux into Tissue Lipids are from Dietary Sources or are Made De novo from Glucose or Fructose Glucose Fructose Acetyl-CoA
Gene Polymorphisms and Carbohydrate Diets James M. Ntambi Ph.D Fatty Acids that Flux into Tissue Lipids are from Dietary Sources or are Made De novo from Glucose or Fructose Glucose Fructose Acetyl-CoA
Why Obesity Is A Chronic Disease
 Why Obesity Is A Chronic Disease Arya M Sharma, MD, FRCP(C) Professor of Medicine Chair in Obesity Research & Management University of Alberta Edmonton, AB, Canada www.drsharma.ca Global Obesity Map 2014
Why Obesity Is A Chronic Disease Arya M Sharma, MD, FRCP(C) Professor of Medicine Chair in Obesity Research & Management University of Alberta Edmonton, AB, Canada www.drsharma.ca Global Obesity Map 2014
SCIENCE CHINA Life Sciences. Cidea controls lipid droplet fusion and lipid storage in brown and white adipose tissue
 SCIENCE CHINA Life Sciences Tsinghua Special Issue January 2014 Vol.57 No.1: 107 116 RESEARCH PAPER doi: 10.1007/s11427-013-4585-y Cidea controls lipid droplet fusion and lipid storage in brown and white
SCIENCE CHINA Life Sciences Tsinghua Special Issue January 2014 Vol.57 No.1: 107 116 RESEARCH PAPER doi: 10.1007/s11427-013-4585-y Cidea controls lipid droplet fusion and lipid storage in brown and white
Metabolic Programming. Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD
 Metabolic Programming Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD nutritional stress/stimuli organogenesis of target tissues early period critical window consequence of stress/stimuli are
Metabolic Programming Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD nutritional stress/stimuli organogenesis of target tissues early period critical window consequence of stress/stimuli are
NOTES. Developed by Fabio Comana, MA., MS., All rights Reserved Page 1
 Session 455: Core Essentials in Science Fabio Comana, MA, MS, NASM CPT, CES & PES; ACE CPT & LWMC; ACSM HFS, NSCA CSCS; CISSN National Academy of Sports Medicine fabio.comana@nasm.org NOTES Developed by
Session 455: Core Essentials in Science Fabio Comana, MA, MS, NASM CPT, CES & PES; ACE CPT & LWMC; ACSM HFS, NSCA CSCS; CISSN National Academy of Sports Medicine fabio.comana@nasm.org NOTES Developed by
NASH Bench to Bedside
 NASH Bench to Bedside October 2006 Anna Mae Diehl, M.D. Gastroenterology Division Duke University NonAlcoholic Fatty Liver Disease Common ~1/4-1/3 1/3 US adults Outcome highly variable Course indolent
NASH Bench to Bedside October 2006 Anna Mae Diehl, M.D. Gastroenterology Division Duke University NonAlcoholic Fatty Liver Disease Common ~1/4-1/3 1/3 US adults Outcome highly variable Course indolent
AAV-TBGp-Cre treatment resulted in hepatocyte-specific GH receptor gene recombination
 AAV-TBGp-Cre treatment resulted in hepatocyte-specific GH receptor gene recombination Supplementary Figure 1. Generation of the adult-onset, liver-specific GH receptor knock-down (alivghrkd, Kd) mouse
AAV-TBGp-Cre treatment resulted in hepatocyte-specific GH receptor gene recombination Supplementary Figure 1. Generation of the adult-onset, liver-specific GH receptor knock-down (alivghrkd, Kd) mouse
Metabolic defects underlying dyslipidemia in abdominal obesity
 Metabolic defects underlying dyslipidemia in abdominal obesity Professor Marja-Riitta Taskinen Department of Medicine, Division of Cardiology Helsinki University Hospital, Finland Disclosures: Honorariums/
Metabolic defects underlying dyslipidemia in abdominal obesity Professor Marja-Riitta Taskinen Department of Medicine, Division of Cardiology Helsinki University Hospital, Finland Disclosures: Honorariums/
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION doi:10.1038/nature11464 Supplemental Figure S1. The expression of Vegfb is increased in obese and diabetic mice as compared to lean mice. a-b, Body weight and postprandial blood
SUPPLEMENTARY INFORMATION doi:10.1038/nature11464 Supplemental Figure S1. The expression of Vegfb is increased in obese and diabetic mice as compared to lean mice. a-b, Body weight and postprandial blood
Master class Biomolecular Sciences Molecular Cell Biology.
 Master class Biomolecular Sciences Molecular Cell Biology. 04-09-08: Paul van Bergen en Henegouwen. Clathrin-indep Endocytosis 11-09-08: Willem Stoorvogel. Endocytosis and MHC classii 18-09-08: X-track
Master class Biomolecular Sciences Molecular Cell Biology. 04-09-08: Paul van Bergen en Henegouwen. Clathrin-indep Endocytosis 11-09-08: Willem Stoorvogel. Endocytosis and MHC classii 18-09-08: X-track
Metabolic ER stress and inflammation in white adipose tissue (WAT) of mice with dietary obesity.
 Supplementary Figure 1 Metabolic ER stress and inflammation in white adipose tissue (WAT) of mice with dietary obesity. Male C57BL/6J mice were fed a normal chow (NC, 10% fat) or a high-fat diet (HFD,
Supplementary Figure 1 Metabolic ER stress and inflammation in white adipose tissue (WAT) of mice with dietary obesity. Male C57BL/6J mice were fed a normal chow (NC, 10% fat) or a high-fat diet (HFD,
SUPPLEMENTARY INFORMATION
 DOI: 10.1038/ncb3461 In the format provided by the authors and unedited. Supplementary Figure 1 (associated to Figure 1). Cpeb4 gene-targeted mice develop liver steatosis. a, Immunoblot displaying CPEB4
DOI: 10.1038/ncb3461 In the format provided by the authors and unedited. Supplementary Figure 1 (associated to Figure 1). Cpeb4 gene-targeted mice develop liver steatosis. a, Immunoblot displaying CPEB4
 Targeting Adipose Tissue in Rheumatoid Arthritis TARA study HOFFA L SCAPTIPL 0.1013606 0.270906 0.3759505 0.3373511 0.4050987 0.404667 11.6 DISCUSSIONS The study targeted the serum levels of adipokines
Targeting Adipose Tissue in Rheumatoid Arthritis TARA study HOFFA L SCAPTIPL 0.1013606 0.270906 0.3759505 0.3373511 0.4050987 0.404667 11.6 DISCUSSIONS The study targeted the serum levels of adipokines
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION FOR Liver X Receptor α mediates hepatic triglyceride accumulation through upregulation of G0/G1 Switch Gene 2 (G0S2) expression I: SUPPLEMENTARY METHODS II: SUPPLEMENTARY FIGURES
SUPPLEMENTARY INFORMATION FOR Liver X Receptor α mediates hepatic triglyceride accumulation through upregulation of G0/G1 Switch Gene 2 (G0S2) expression I: SUPPLEMENTARY METHODS II: SUPPLEMENTARY FIGURES
Impacts of prenatal malnutrition and an early obesogenic diet on adipose tissue morphology and gene expression in adult sheep
 Impacts of prenatal malnutrition and an early obesogenic diet on adipose tissue morphology and gene expression in adult sheep Sharmila Ahmad 1, Lise K. Lyngman 1, Rajan Dhakal 1, Morteza Mansouryar 1,
Impacts of prenatal malnutrition and an early obesogenic diet on adipose tissue morphology and gene expression in adult sheep Sharmila Ahmad 1, Lise K. Lyngman 1, Rajan Dhakal 1, Morteza Mansouryar 1,
Thrombin promotes diet-induced obesity through fibrin-driven inflammation
 Thrombin promotes diet-induced obesity through fibrin-driven inflammation Anna K. Kopec, 1 Sara R. Abrahams, 2 Sherry Thornton, 3 Joseph S. Palumbo, 4 Eric S. Mullins, 4 Senad Divanovic, 5 Hartmut Weiler,
Thrombin promotes diet-induced obesity through fibrin-driven inflammation Anna K. Kopec, 1 Sara R. Abrahams, 2 Sherry Thornton, 3 Joseph S. Palumbo, 4 Eric S. Mullins, 4 Senad Divanovic, 5 Hartmut Weiler,
* Author to whom correspondence should be addressed; Tel.: ; Fax:
 Int. J. Mol. Sci. 2014, 15, 6184-6223; doi:10.3390/ijms15046184 Review OPEN ACCESS International Journal of Molecular Sciences ISSN 1422-0067 www.mdpi.com/journal/ijms Obesity and Its Metabolic Complications:
Int. J. Mol. Sci. 2014, 15, 6184-6223; doi:10.3390/ijms15046184 Review OPEN ACCESS International Journal of Molecular Sciences ISSN 1422-0067 www.mdpi.com/journal/ijms Obesity and Its Metabolic Complications:
DOWNLOAD PDF ADIPOSE TISSUE AND ADIPOKINES IN HEALTH AND DISEASE (NUTRITION AND HEALTH)
 Chapter 1 : Adiposity, Adipokines, and Adiposopathy - Sick Fat Explained Adipose Tissue and Adipokines in Health and Disease, Second Edition is a useful resource for physicians interested in adipose tissue
Chapter 1 : Adiposity, Adipokines, and Adiposopathy - Sick Fat Explained Adipose Tissue and Adipokines in Health and Disease, Second Edition is a useful resource for physicians interested in adipose tissue
Supplementary Figure 1: Additional metabolic parameters of obesity mouse models and controls. (a) Body weight, (b) blood glucose and (c) insulin
 Supplementary Figure 1: Additional metabolic parameters of obesity mouse models and controls. (a) Body weight, (b) blood glucose and (c) insulin resistance index of homeostatic model assessment (HOMA IR)
Supplementary Figure 1: Additional metabolic parameters of obesity mouse models and controls. (a) Body weight, (b) blood glucose and (c) insulin resistance index of homeostatic model assessment (HOMA IR)
Supplementary Figure S1
 Lipidomic-based investigation into the regulatory effect of Schisandrin B on palmitic acid level in non-alcoholic steatotic livers Hiu Yee Kwan 1,2, Xuyan Niu 3, Wenlin Dai 4, Tiejun Tong 4, Xiaojuan Chao
Lipidomic-based investigation into the regulatory effect of Schisandrin B on palmitic acid level in non-alcoholic steatotic livers Hiu Yee Kwan 1,2, Xuyan Niu 3, Wenlin Dai 4, Tiejun Tong 4, Xiaojuan Chao
Myocardial lipid accumulation and lipotoxicity in heart failure
 Myocardial lipid accumulation and lipotoxicity in heart failure P. Christian Schulze, MD, PhD New York - Presbyterian Hospital, Columbia University Medical Center, Division of Cardiology, New York, NY,
Myocardial lipid accumulation and lipotoxicity in heart failure P. Christian Schulze, MD, PhD New York - Presbyterian Hospital, Columbia University Medical Center, Division of Cardiology, New York, NY,
FOR REVIEW. BMB Reports - Manuscript Submission. Manuscript Draft. Manuscript Number: BMB
 BMB Reports - Manuscript Submission Manuscript Draft Manuscript Number: BMB-18-095 Title: Insulin Receptor Substrate 2:A Bridge between Hippo and AKT Pathways Article Type: Perspective (Invited Only) Keywords:
BMB Reports - Manuscript Submission Manuscript Draft Manuscript Number: BMB-18-095 Title: Insulin Receptor Substrate 2:A Bridge between Hippo and AKT Pathways Article Type: Perspective (Invited Only) Keywords:
PPARγ in the endothelium regulates metabolic responses to high-fat diet in mice
 Research article PPARγ in the endothelium regulates metabolic responses to high-fat diet in mice Takeshi Kanda, 1 Jonathan D. Brown, 1 Gabriela Orasanu, 1 Silke Vogel, 2 Frank J. Gonzalez, 3 Juliano Sartoretto,
Research article PPARγ in the endothelium regulates metabolic responses to high-fat diet in mice Takeshi Kanda, 1 Jonathan D. Brown, 1 Gabriela Orasanu, 1 Silke Vogel, 2 Frank J. Gonzalez, 3 Juliano Sartoretto,
Improving Access to Quality Medical Care Webinar Series
 Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
SUPPLEMENTARY INFORMATION
 doi: 1.138/nature7221 Brown fat selective genes 12 1 Control Q-RT-PCR (% of Control) 8 6 4 2 Ntrk3 Cox7a1 Cox8b Cox5b ATPase b2 ATPase f1a1 Sirt3 ERRα Elovl3/Cig3 PPARα Zic1 Supplementary Figure S1. stimulates
doi: 1.138/nature7221 Brown fat selective genes 12 1 Control Q-RT-PCR (% of Control) 8 6 4 2 Ntrk3 Cox7a1 Cox8b Cox5b ATPase b2 ATPase f1a1 Sirt3 ERRα Elovl3/Cig3 PPARα Zic1 Supplementary Figure S1. stimulates
Tissue factor-par2 signaling promotes diet-induced obesity and adipose
 Supplementary figures for Tissue factor-par2 signaling promotes diet-induced obesity and adipose inflammation. Leylla Badeanlou 1, Christian Furlan-Freguia 2, Guang Yang 1, Wolfram Ruf 2,3, and Fahumiya
Supplementary figures for Tissue factor-par2 signaling promotes diet-induced obesity and adipose inflammation. Leylla Badeanlou 1, Christian Furlan-Freguia 2, Guang Yang 1, Wolfram Ruf 2,3, and Fahumiya
