Post-Exposure Prophylaxis Review for International Visitors
|
|
|
- Arline Darleen McDaniel
- 5 years ago
- Views:
Transcription
1 Post-Exposure Prophylaxis Review for International Visitors
2 Case Presentation 27 yo nurse presents to Urgent Care for a needlestick 2 days ago from a diabetic lancet. Source patient (SP): 35 yo male known HIV+ (wasn t known at the time) Would you offer her PEP? If so, which agents? What more would you like to know?
3 Case Presentation continued What is her risk for contracting HIV? Are there factors that might affect this risk? How effective is PEP? Is it too late to start PEP? What are the drawbacks of starting PEP? Which regimen(s) should be considered? What follow-up should be arranged?
4
5 Risk Factors for Seroconversion after Needlesticks CDC-sponsored case-control study 33 cases, 665 controls s/p needlestick from confirmed HIV+ SPs AZT only for PEP
6 Risk Factors for Seroconversion Risk Factor Odds Ratio* 95% CI Deep injury Visibly bloody device Device in artery/vein Terminally ill SP AZT PEP *p<0.01 for all NEJM 1997;337:
7 Other Likely Risk Factors Viral Load Glove use 50% decrease in volume of blood transmitted Hollow bore vs solid bore large diameter needles weakly increased risk (p = 0.08) no documented cases to date of seroconversion from suture needles (though 3 from solid sharps) drying conditions tenfold drop in infectivity every 9 hours
8 Other Likely Risk Factors Survivability 10-fold drop in infectivity every 9 hrs Syringes of blood Viable virus at 42 days in 39 degree Fahrenheit 50% At 21 days in 68 degrees 8% At 7 days in 80 degrees - <1% Heimer R J of Substance Use and Misuse, 9/2000
9 NonOccupational Risk Factors Makerere and Columbia U data - Uganda 415 Discordant couples followed 30 months 90 of 415 seroconverted Viral Load below 1,500 copies (n=51) NO SEROCONVERSIONS Circumcised male partners (50/187) NO SEROCONVERSIONS Quinn T, Wawer M, Sewankambo N NEJM 3/30/00 Vol 342
10 Evidence of Efficacy of PEP animal models: high level of protection when started within 24 h multiple studies document reduced vertical transmission with PEP, independent of reduction of maternal viral load OR = 0.19 for AZT use in case-control study cases of seroconversion despite proper PEP imply that efficacy less than 100%
11 Risks of PEP More symptoms, less serious side effects than HIV infected persons on ARV common symptoms: HA, fatigue, malaise, GI disturbances, rash hepatotoxicity, bone marrow, pancreatitis, CNS effects, allergic reactions nevirapine: life threatening hepatotoxicity long-term: unknown
12 Timing of start of PEP? Theoretical considerations Animal data Experience in humans
13
14 Timing of PEP: what s the evidence? animal PEP studies: suggest substantially less effective beyond hours case-control study: most subjects in each group received PEP within 4 hours analysis of PEP failures does not suggest a clear cut-off
15 Timing of PEP: the N of 1 13 yo girl in Italy transfused w/ one unit of blood from donor in the window period seroconversion risk estimated to be virtually 100% 3-drug PEP initiated 50 hours posttransfusion, continued for 9 months no evidence of HIV infection 15 months later Ann Int Med 2000;133:31-4.
16 Timing of PEP Efficacy of PEP thought to wane with time, when is PEP no longer worth it? benefits of PEP risks of PEP exposure time
17 Timing of PEP: CDC Guidelines Initiate as soon as possible (within hours) Interval after which there is no benefit for humans is undefined If appropriate for the exposure, PEP should be started even when the interval since exposure exceeds 36 hours Obtain expert advice when interval has exceeded 36 hours MMWR 1998;47:RR-7.
18 Duration of PEP In animal studies, 3 days or 10 days of PEP inferior to 28 days 4 weeks (28 days) used in case-control study and recommended by CDC guidelines 9 months if you are an Italian girl posttransfusion
19 Back to the Case By report, the SP has never received treatment for his HIV. She does not know his VL or CD4 count, but he looks pretty healthy. The lancet was visibly bloody and stuck her through her glove, causing her to bleed Exam: pinpoint puncture wound on thumb What are your PEP recommendations?
20 PEP Regimens Moving Target Official guidelines versus clinical practice Balance concerns for resistance with toxicity and adherence Guidelines for Occupational and Non occupational exposure currently differ
21 PEP Regimens Basic Regimens two NRTIs simple dosing Expanded Regimens basic regimen plus PI or efavirenz or 3 rd NRTI may be more effective more potential for toxicity adherence more difficult
22 Basic Regimens: AZT/3TC Advantages AZT the best studied agent for PEP, with proven efficacy simple dosage: Combivir, one tab bid well-known & manageable side effects Disadvantages sides effects common, may impair compliance resistance to AZT & 3TC common
23 Expanded Regimens Efavirenz once daily dosing may improve adherence theoretically faster onset of action (does not require phosphorylation) CNS side effects common, can be difficult for health care workers rash common can progress to Stevens - Johnson Syndrome raises concern for acute seroconversion contraindicated in pregnancy
24 Back to the Case After extensive counseling, she decides to take Combivir basic regimen You write the prescription and arrange follow-up
25 Case Number 2 24 yo dental tech splashed in the eye during dental procedure 3 hours ago Source patient: 33 yo female, co-infected with HIV and HCV What more would you like to know?
26 Case number 2 continued Saliva was visibly bloody - in fact, it was mostly blood that splashed her she rinsed out her eye immediately source patient has never taken antiretrovirals, has a CD4 count of about 500 and a viral load of 20,000 last time it was checked. She is 8 weeks pregnant
27 Case number 2 continued What is her risk of contracting HIV? Of HCV? What are your PEP recommendations? How does her pregnancy affect your decision making?
28 Case 2 continued Risk of HIV from mucous membrane exposures: 0.09% (95% CI 0.006% -0.5%) Risk of HCV in this circumstance unknown; thought to be higher than HIV, because risk of HCV in percutaneous exposures, at 1.8%, is higher than that for HIV
29 PEP in Pregnancy Most antiretrovirals class B or C in pregnancy experience with AZT & 3TC largely reassuring avoid efavirenz (anancephaly in monkeys), amprenavir (ossification defects in rabbits), and indinavir (hyperbilirubinemia) theoretically higher risk of vertical transmission with primary HIV infection
30 Case 2 continued You decide on AZT/3TC/Nelfinavir 4 days later she calls complaining of headache, an itchy rash, and URI symptoms what do you do?
31 Case 2 continued Exam: VS: T 99.0 R 14 P 78 BP 134/76 Gen - alert, tired-appearing, no acute distress HEENT - nasal congestion, otherwise benign Neck - 3 ant cervical lymph nodes Lungs, cardiac, abdomen: benign Neuro: nonfocal Skin: urticarial rash on trunk and legs How would you manage her?
32 Primary HIV Infection most patients who contract HIV are symptomatic with seroconversion flu-like or mono-like illness often accompanied by a rash onset typically 3-4 weeks following exposure, but high variability growing evidence that treatment of PHI may have significant long-term benefit
33 Primary HIV Infection - Symptoms Fever 87% Rash 68% Pharyngitis 48% Myalgias 42% Headache 39% Diarrhea 32% Abdominal Pain 32% Arthralgias 29% Nausea/Vomiting 29%
34 Primary HIV Infection - Signs Axillary Temp > % Maculopapular Rash 63% Lymphadenopathy 57% Oral Ulcers 40% Genital Ulcers/Discharge 36% Purulent Sputum 6% Urticarial Rash 6% Meningismus 6%
35 PHI: Diagnostic Testing HIV RNA 1 mil 100,000 10,000 1,000 HIV RNA P24 + Ab + _ HIV-1 Antibodies Exposure Symptoms Days
36 Follow-up HIV Testing 1998 CDC recommendations: HIV Ab at 6 weeks, 3 months, 6 months rare case reports of seroconversion beyond 6 months new guidelines: consider testing at 12 months for serious exposures VL testing not recommended unless Primary HIV Infection (PHI) suspected
37 Hepatitis C Exposure average risk of seroconversion from percutaneous exposure 1.8% same risk factors as for HIV thought to apply gamma globulin not useful early recognition and treatment of HCV infection appears to improve odds of eradication
38 Hepatitis C: follow-up testing HCV Ab test at 6 months consider screening LFTs periodically or if symptomatic note that, unlike HIV, most patients are not symptomatic with acute HCV infection
39 NonOccupational PEP case 34 yo female s/p unprotected, nonconsensual vaginal intercourse with person of unknown HIV status what is her level of risk? what, if any, PEP would you recommend?
40 Exposure risks (average, per episode, from known (+) source) percutaneous (blood) HIV HCV HBV (eag+) HBV (eag-) 0.3% 1.8% 1 40%* %** mucocutaneous (blood).09% 2 receptive anal 0.1-5%*** v. low; unclear insertive anal 0.06% or less 3 v. low; unclear receptive vaginal % 4 v. low; unclear insertive vaginal % 5 v. low; unclear receptive oral-male.06% or less 6 v. low; unclear female-female orogenital contact 4 case reports 7 insertive oral? 1 case report v. low; unclear needle sharing 0.67% 8 very high vertical (no proph.) 24% 5-6% 9 breastfeeding ~ doubles risk of vert.transmission 10 has not been documented 11 *decreases to 2.4% if HBIG & vaccine given **decreases to 0% if HBIG & vaccine given. Hepatitis B vaccines also are 70%-88% effective when given within 1 week after HBV exposure. *** recent studies suggest approx 1% 12
41 npep Case Data is suggestive, but difficult to document failures in US studies MMWR January, 2005 Vol 54/RR-2 pilot study in San Francisco suggests that providing npep, when accompanied by counseling, does not lead to increased risky behavior
42 npep Case, continued Local epidemiology of HIV infections should guide advice on npep Realize that emotions and fear guide decisions in first few days As much as possible try to get HIV testing of SP Balance risk and benefit of treatment
43 PEP: Core Principles Evidence is limited, but suggestive Balancing of risks vs benefits Timing: the sooner the better, but interval beyond which no benefit is unclear 28 days is recommended. Optimal duration unclear Decision making can get very complex when resistance in SP suspected
Blood-Borne Pathogens and Post-Exposure Prophylaxis
 Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
One of your office personnel
 Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
FAMILY HIV CENTER NJ CARES SANE
 HIV, Hepatitis B & C Postexposure Prophylaxis for Sexual Assault Victims Update for Case Managers Susan Burrows-Clark, RN, MSN, CNS, C. 10/17/11 Antiretroviral Postexposure Prophylaxis After Sexual, Injection-Drug
HIV, Hepatitis B & C Postexposure Prophylaxis for Sexual Assault Victims Update for Case Managers Susan Burrows-Clark, RN, MSN, CNS, C. 10/17/11 Antiretroviral Postexposure Prophylaxis After Sexual, Injection-Drug
Occupational HIV exposures are crisis situations demanding immediate, decisive action. Henderson, 2001
 Post-Exposure Care: A Balancing Act Alice C. Thornton, MD Southeast AIDS Training & Education Center Kentucky Local Performance Site University of Kentucky October 24, 2009 Objectives Review the goals
Post-Exposure Care: A Balancing Act Alice C. Thornton, MD Southeast AIDS Training & Education Center Kentucky Local Performance Site University of Kentucky October 24, 2009 Objectives Review the goals
HIV Occupational Transmission and Exposure. Marsh Gelbart 2010
 HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
Management of Workplace Exposure to Blood-borne Pathogens
 Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
Decision Analysis Example
 Decision Analysis Example after Occupational Exposure to Infection after Needlestick Injury Direct inoculation into blood vessels Cutaneous dendritic (Langerhans) cells Delay from injury to infection Initial
Decision Analysis Example after Occupational Exposure to Infection after Needlestick Injury Direct inoculation into blood vessels Cutaneous dendritic (Langerhans) cells Delay from injury to infection Initial
Management of Exposure to Needlestick Injuries & Body Fluids
 Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE
 Sandyford Protocols MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE www.hiv-druginteractions.org If you require information on occupational exposure to blood borne viruses, including HIV, please refer to the
Sandyford Protocols MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE www.hiv-druginteractions.org If you require information on occupational exposure to blood borne viruses, including HIV, please refer to the
Module 1: HIV epidemiology, transmission and prevention
 Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS
 STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
Blood/Body Fluid Exposure Option
 Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Emergency Department Blood/Body Fluid Exposure Instructions
 Emergency Department Blood/Body Fluid Exposure Instructions For employees sent to the Emergency Department after hours to be evaluated for needle stick / body fluid exposure 1. Floor or unit Charge RN
Emergency Department Blood/Body Fluid Exposure Instructions For employees sent to the Emergency Department after hours to be evaluated for needle stick / body fluid exposure 1. Floor or unit Charge RN
0% 0% 0% Parasite. 2. RNA-virus. RNA-virus
 HIV/AIDS and Treatment Manado, Indonesia 16 november HIV [e] EDUCATION HIV is a 1. DNA-virus 2. RNA-virus 3. Parasite 0% 0% 0% DNA-virus RNA-virus Parasite HIV HIV is a RNA-virus. HIV is an RNA virus which
HIV/AIDS and Treatment Manado, Indonesia 16 november HIV [e] EDUCATION HIV is a 1. DNA-virus 2. RNA-virus 3. Parasite 0% 0% 0% DNA-virus RNA-virus Parasite HIV HIV is a RNA-virus. HIV is an RNA virus which
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
43. Guidelines on Needle stick Injury
 43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
Post-Sexual Exposure Prophylaxis (npep)
 Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
Biomedical Prevention in HIV
 Biomedical Prevention in HIV CHART - CCAS-CDC 3 RD Joint Meeting Montego Bay, Jamaica August 21-26,2011 Presented by Tina Hylton-Kong, ERTU-CHART Some Slides from Impact of ART on HIV Transmission Wafaa
Biomedical Prevention in HIV CHART - CCAS-CDC 3 RD Joint Meeting Montego Bay, Jamaica August 21-26,2011 Presented by Tina Hylton-Kong, ERTU-CHART Some Slides from Impact of ART on HIV Transmission Wafaa
Non-occupational HIV Post Exposure Prophylaxis (npep)
 Mountain West AIDS Education and Training Center Non-occupational HIV Post Exposure Prophylaxis (npep) Robert Harrington, M.D. This presentation is intended for educational use only, and does not in any
Mountain West AIDS Education and Training Center Non-occupational HIV Post Exposure Prophylaxis (npep) Robert Harrington, M.D. This presentation is intended for educational use only, and does not in any
Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
 PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
HIV, HBV, AND HCV POSTEXPOSURE MANAGEMENT FOR HEALTHCARE WORKERS. Weerawat Manosuthi Bamrasnaradura Infectious Diseases Institute
 HIV, HBV, AND HCV POSTEXPOSURE MANAGEMENT FOR HEALTHCARE WORKERS Weerawat Manosuthi Bamrasnaradura Infectious Diseases Institute Outline Case scenario of HIV postexposure prophylaxis Risks of and how to
HIV, HBV, AND HCV POSTEXPOSURE MANAGEMENT FOR HEALTHCARE WORKERS Weerawat Manosuthi Bamrasnaradura Infectious Diseases Institute Outline Case scenario of HIV postexposure prophylaxis Risks of and how to
Study finds PEP not 100% effective in preventing HIV infection
 From TreatmentUpdate 152 Study finds PEP not 100% effective in preventing HIV infection Some doctors and nurses who care for PHAs may sustain needle-stick injuries. This raises the possibility that they
From TreatmentUpdate 152 Study finds PEP not 100% effective in preventing HIV infection Some doctors and nurses who care for PHAs may sustain needle-stick injuries. This raises the possibility that they
Clinical Education Initiative OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS. Antonio E. Urbina, MD
 Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
TO DECREASE THE CHANCE OF GETTING
 POST ASSAULT MEDICATIONS Terri Stewart RN Naomi Sugar MD TO DECREASE THE CHANCE OF GETTING Pregnant STDs Chlamydia Gonorrhea Trichomonas Hep B HIV EMERGENCY CONTRACEPTION Plan B Levonorgestrel PLAN B Plan
POST ASSAULT MEDICATIONS Terri Stewart RN Naomi Sugar MD TO DECREASE THE CHANCE OF GETTING Pregnant STDs Chlamydia Gonorrhea Trichomonas Hep B HIV EMERGENCY CONTRACEPTION Plan B Levonorgestrel PLAN B Plan
treatment during pregnancy and breastfeeding
 treatment during pregnancy and breastfeeding Topics covered Introduction. Preventing parent-to-child transmission. AZT as a single therapy. Treatment begun late in pregnancy. Nevirapine for mothers and
treatment during pregnancy and breastfeeding Topics covered Introduction. Preventing parent-to-child transmission. AZT as a single therapy. Treatment begun late in pregnancy. Nevirapine for mothers and
Clinical Case Scenario. HIVeEducation Workshop, Sint Maarten 2009
 Clinical Case Scenario HIVeEducation Workshop, Sint Maarten 2009 Background Mrs. S is a 34 year-old woman who was referred from the VCT center after testing HIV positive three weeks ago. Her husband recently
Clinical Case Scenario HIVeEducation Workshop, Sint Maarten 2009 Background Mrs. S is a 34 year-old woman who was referred from the VCT center after testing HIV positive three weeks ago. Her husband recently
determine need but regimen does not change based on risk factor ED medicine attending meets
 HIV PEP Guidelines after Sexual Assault Harborview Medical Center January 2015 Initial risk assessment and discussion with patient about risk and PEP is by clinician who does exam (SANE, Ob-Gyn resident,
HIV PEP Guidelines after Sexual Assault Harborview Medical Center January 2015 Initial risk assessment and discussion with patient about risk and PEP is by clinician who does exam (SANE, Ob-Gyn resident,
2017 BLOODBORNE PATHOGENS
 2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
SFAF CLINICAL PROTOCOLS
 SFAF CLINICAL PROTOCOLS Page 1 of Supersedes Date: December 31, 2016 Original Date: August 20, 2014 Version: 03 Policy Section: Patient Care Non-Occupational Post Exposure Prophylaxis Program Back ground:
SFAF CLINICAL PROTOCOLS Page 1 of Supersedes Date: December 31, 2016 Original Date: August 20, 2014 Version: 03 Policy Section: Patient Care Non-Occupational Post Exposure Prophylaxis Program Back ground:
HIV and PEP. LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED
 HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
INITIAL EVALUATION AND MANAGEMENT FOLLOWING EXPOSURE TO BLOOD OR BODY FLUIDS
 Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Commonly Asked Questions About Chronic Hepatitis C
 Commonly Asked Questions About Chronic Hepatitis C From the American College of Gastroenterology 1. How common is the hepatitis C virus? The hepatitis C virus is the most common cause of chronic viral
Commonly Asked Questions About Chronic Hepatitis C From the American College of Gastroenterology 1. How common is the hepatitis C virus? The hepatitis C virus is the most common cause of chronic viral
National guidelines for post-exposure prophylaxis after non-occupational exposure to HIV
 National guidelines for post-exposure prophylaxis after non-occupational exposure to HIV These guidelines outline the management of individuals who have been exposed (or suspect they have been exposed)
National guidelines for post-exposure prophylaxis after non-occupational exposure to HIV These guidelines outline the management of individuals who have been exposed (or suspect they have been exposed)
Exposure. Blood. Department of Health & Human Services
 Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Greenwood School District 50 OSHA UPDATE BLOODBORNE PATHOGENS
 Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Jennifer Adams, MD Denver Health. September 28, 2010
 Jennifer Adams, MD Denver Health General Internal Medicine dii and HIV Primary Care September 28, 2010 HIV for PCP s PCP s often think they don t need to know much about HIV: it s managed by specialists
Jennifer Adams, MD Denver Health General Internal Medicine dii and HIV Primary Care September 28, 2010 HIV for PCP s PCP s often think they don t need to know much about HIV: it s managed by specialists
HIV Testing. ECHO Hep C. Judith Feinberg, MD June 22, 2017
 HIV Testing ECHO Hep C Judith Feinberg, MD June 22, 2017 Overview A few basics HIV epidemiology in the US HIV testing Time course of HIV-1 infection symptoms HIV proviral DNA symptoms window period HIV
HIV Testing ECHO Hep C Judith Feinberg, MD June 22, 2017 Overview A few basics HIV epidemiology in the US HIV testing Time course of HIV-1 infection symptoms HIV proviral DNA symptoms window period HIV
Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft:
 Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft: 10-2-2015 Clinical studies demonstrate that when a person without HIV infection takes
Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft: 10-2-2015 Clinical studies demonstrate that when a person without HIV infection takes
Bloodborne Pathogens Across the Continuum of Care Sue Sebazco, Arlington, Texas A Webber Training Teleclass
 Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
EQuIP 5 - This version June 2011 Revision Due June 2014
 Preamble Rockingham Peel Group Non-Occupational Post-Exposure Prophylaxis (NPEP) To Prevent HIV in Western Australia Protocol The purpose of this protocol is to clarify the appropriate use and methods
Preamble Rockingham Peel Group Non-Occupational Post-Exposure Prophylaxis (NPEP) To Prevent HIV in Western Australia Protocol The purpose of this protocol is to clarify the appropriate use and methods
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet. Instructions for Employees/Students:
 MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
The how and why of Acute HIV Infection 1. How do we best diagnosis patients with acute HIV?
 Acute HIV infection Eric Rosenberg, MD Associate Professor of Pathology Director, Clinical Microbiology Laboratory Massachusetts General Hospital Harvard Medical School The how and why of Acute HIV Infection
Acute HIV infection Eric Rosenberg, MD Associate Professor of Pathology Director, Clinical Microbiology Laboratory Massachusetts General Hospital Harvard Medical School The how and why of Acute HIV Infection
Disclosure. Learning Objectives. Epidemiology. Transmission. Risk of Transmission PRE-EXPOSURE PROPHYLAXIS (PREP) FOR HIV PREVENTION 50,000.
 Disclosure PRE-EXPOSURE PROPHYLAXIS (PREP) FOR HIV PREVENTION I have no financial interest in and/or affiliation with any external organizations in relation to this CE program. DaleMarie Vaughan, PharmD
Disclosure PRE-EXPOSURE PROPHYLAXIS (PREP) FOR HIV PREVENTION I have no financial interest in and/or affiliation with any external organizations in relation to this CE program. DaleMarie Vaughan, PharmD
POST-EXPOSURE PROPHYLAXIS, PRE-EXPOSURE PROPHYLAXIS, & TREATMENT OF HIV
 POST-EXPOSURE PROPHYLAXIS, PRE-EXPOSURE PROPHYLAXIS, & TREATMENT OF HIV DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none
POST-EXPOSURE PROPHYLAXIS, PRE-EXPOSURE PROPHYLAXIS, & TREATMENT OF HIV DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none
C 肝職業暴露後之處置 衛福部疾病管制署 中區傳染病防治醫療網 王任賢指揮官
 C 肝職業暴露後之處置 衛福部疾病管制署 中區傳染病防治醫療網 王任賢指揮官 HCV:Structure and Classification Unclassified virus, Member of the flavivirus family (other members yellow fever and dengue) Enveloped single stranded RNA virus Humans
C 肝職業暴露後之處置 衛福部疾病管制署 中區傳染病防治醫療網 王任賢指揮官 HCV:Structure and Classification Unclassified virus, Member of the flavivirus family (other members yellow fever and dengue) Enveloped single stranded RNA virus Humans
Hepatitis STARS Program. Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003
 Hepatitis 2003 STARS Program Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003 Outline n Hepatitis A Epidemiology and screening Transmission n Hepatitis B Epidemiology
Hepatitis 2003 STARS Program Geri Brown, M.D. Associate Professor Department of Internal Medicine October 4, 2003 Outline n Hepatitis A Epidemiology and screening Transmission n Hepatitis B Epidemiology
HIV Update Objectives. Epidemiology. Epidemiology, Transmission and Natural History. Transmission Risk by Exposure. Transmission 9/29/2014
 Objectives HIV Update 2014 Jay Sizemore, MD, MPH Medical Director Chattanooga CARES Assistant Professor UTCOM Chattanooga 2October 2014 Review HIV epidemiology and screening/testing guidelines Discuss
Objectives HIV Update 2014 Jay Sizemore, MD, MPH Medical Director Chattanooga CARES Assistant Professor UTCOM Chattanooga 2October 2014 Review HIV epidemiology and screening/testing guidelines Discuss
The Latest on HIV Testing. Dominika Seidman, MD MAS
 The Latest on HIV Testing Dominika Seidman, MD MAS Disclosures none 2 Learning objectives At the conclusion of this session, participants should be able to Define the window periods for various HIV tests
The Latest on HIV Testing Dominika Seidman, MD MAS Disclosures none 2 Learning objectives At the conclusion of this session, participants should be able to Define the window periods for various HIV tests
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
An International Antiviral Society-USA
 Doug Campos-Outcalt, MD, MPA University of Arizona, Phoenix dougco@email.arizona. edu A look at new guidelines for HIV treatment and prevention Start antiretroviral therapy as soon as possible after HIV
Doug Campos-Outcalt, MD, MPA University of Arizona, Phoenix dougco@email.arizona. edu A look at new guidelines for HIV treatment and prevention Start antiretroviral therapy as soon as possible after HIV
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
PrEP for HIV Prevention. Adult Clinical Guideline from the New York State Department of Health AIDS Institute
 PrEP for HIV Prevention Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the PrEP Guideline Raise awareness of PrEP among healthcare
PrEP for HIV Prevention Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the PrEP Guideline Raise awareness of PrEP among healthcare
Hepatitis C Best Practice Guidelines For Local Health Departments
 Hepatitis C Best Practice Guidelines For Local Health Departments LHDs are responsible for investigating and reporting all physician reported cases of acute hepatitis C (HCV). For clients known to have
Hepatitis C Best Practice Guidelines For Local Health Departments LHDs are responsible for investigating and reporting all physician reported cases of acute hepatitis C (HCV). For clients known to have
Effective Date: 6/10/2013 Review Date: 6/10/2016
 Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Occupational and Non- Occupational HIV Post-exposure Prophylaxis
 Occupational and Non- Occupational HIV Post-exposure Prophylaxis Amy V. Kindrick, MD, MPH National Clinicians Post-Exposure Prophylaxis Hotline (PEPline) University of California, San Francisco San Francisco
Occupational and Non- Occupational HIV Post-exposure Prophylaxis Amy V. Kindrick, MD, MPH National Clinicians Post-Exposure Prophylaxis Hotline (PEPline) University of California, San Francisco San Francisco
PrEP and npep for HIV Prevention. Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine
 PrEP and npep for HIV Prevention Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine Case Study A 26 y/o M presents for routine asymptomatic screening for sexually transmitted infections
PrEP and npep for HIV Prevention Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine Case Study A 26 y/o M presents for routine asymptomatic screening for sexually transmitted infections
Post Exposure Prophylaxis (PEP)
 Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Important Safety Information About Emtricitabine/Tenofovir Disoproxil Fumarate 200 mg/300 mg for HIV-1 Pre-exposure Prophylaxis (PrEP)
 Important Safety Information About Emtricitabine/Tenofovir Disoproxil Fumarate 200 mg/300 mg for HIV-1 Pre-exposure Prophylaxis (PrEP) For Healthcare Providers About Emtricitabine/Tenofovir Disoproxil
Important Safety Information About Emtricitabine/Tenofovir Disoproxil Fumarate 200 mg/300 mg for HIV-1 Pre-exposure Prophylaxis (PrEP) For Healthcare Providers About Emtricitabine/Tenofovir Disoproxil
AMERICAN ACADEMY OF PEDIATRICS. Guidance for the Clinician in Rendering Pediatric Care. Peter L. Havens, MD, and the Committee on Pediatric AIDS
 AMERICAN ACADEMY OF PEDIATRICS CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care Peter L. Havens, MD, and the Committee on Pediatric AIDS Postexposure Prophylaxis in Children and Adolescents
AMERICAN ACADEMY OF PEDIATRICS CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care Peter L. Havens, MD, and the Committee on Pediatric AIDS Postexposure Prophylaxis in Children and Adolescents
Pre and Post Exposure Prophylaxis. Laila AL Dabal MD FRCP MSc Infectious Diseases Unit Dubai Health Authority 15 March 2018
 Pre and Post Exposure Prophylaxis Laila AL Dabal MD FRCP MSc Infectious Diseases Unit Dubai Health Authority 15 March 2018 Indications for Pre and Post Exposure Prophylaxis: occupational and non-occupational
Pre and Post Exposure Prophylaxis Laila AL Dabal MD FRCP MSc Infectious Diseases Unit Dubai Health Authority 15 March 2018 Indications for Pre and Post Exposure Prophylaxis: occupational and non-occupational
Clinical management of non-occupational and occupational exposure to blood borne pathogens. - A Pocket Reference -
 Pocket P.E.P. Clinical management of non-occupational and occupational eposure to blood borne pathogens Development Team: Deborah Yoong, PharmD 1 1, 2, 3 Kevin Gough, MD, MEd 1 Positive Care Clinic, Toronto,
Pocket P.E.P. Clinical management of non-occupational and occupational eposure to blood borne pathogens Development Team: Deborah Yoong, PharmD 1 1, 2, 3 Kevin Gough, MD, MEd 1 Positive Care Clinic, Toronto,
Hepatitis B and C Overview, Outbreaks, and Recommendations. Viral Hepatitis Language. Types of Viral Hepatitis 7/1/2013
 Hepatitis B and C Overview, Outbreaks, and Recommendations Elizabeth Lawlor, MS Healthy Kansans living in safe and sustainable environments. Viral Hepatitis Language Acute infection is when the infection
Hepatitis B and C Overview, Outbreaks, and Recommendations Elizabeth Lawlor, MS Healthy Kansans living in safe and sustainable environments. Viral Hepatitis Language Acute infection is when the infection
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
Postexposure prophylaxis (PEP)
 Postexposure Prophylaxis Against Human Immunodeficiency Virus MICHAEL A. TOLLE, MD, MPH, and HEIDI L. SCHWARZWALD, MD, MPH, Baylor College of Medicine, Houston, Texas Family physicians often encounter
Postexposure Prophylaxis Against Human Immunodeficiency Virus MICHAEL A. TOLLE, MD, MPH, and HEIDI L. SCHWARZWALD, MD, MPH, Baylor College of Medicine, Houston, Texas Family physicians often encounter
Michigan Guidelines: HIV, Syphilis, HBV in Pregnancy
 Michigan Guidelines: HIV, Syphilis, HBV in Pregnancy Presenter: Theodore B. Jones, MD Maternal Fetal Medicine Wayne State University School of Medicine Beaumont Dearborn Hospital HIV, Syphilis, HBV in
Michigan Guidelines: HIV, Syphilis, HBV in Pregnancy Presenter: Theodore B. Jones, MD Maternal Fetal Medicine Wayne State University School of Medicine Beaumont Dearborn Hospital HIV, Syphilis, HBV in
Bloodbourne Pathogens (BBP) Occupational Post-Exposure Chemophrophylaxis
 Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis).
 LTHT Infection Control Policies Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis). This policy covers the immediate actions to
LTHT Infection Control Policies Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis). This policy covers the immediate actions to
Fertility Desires/Management of Serodiscordant HIV + Couples
 Fertility Desires/Management of Serodiscordant HIV + Couples William R. Short, MD, MPH Assistant Professor of Medicine Division Of Infectious Diseases Jefferson Medical College of Thomas Jefferson University
Fertility Desires/Management of Serodiscordant HIV + Couples William R. Short, MD, MPH Assistant Professor of Medicine Division Of Infectious Diseases Jefferson Medical College of Thomas Jefferson University
Exposures at Non-MUSC Clinical Sites
 BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
Bloodborne Pathogens. Penn State University Environmental Health & Safety
 Bloodborne Pathogens Penn State University Environmental Health & Safety Diseases of Concern Hepatitis B (Serum Hepatitis) Hepatitis C (non-a non-b Hepatitis) HIV (Human Immunodeficiency Virus aka the
Bloodborne Pathogens Penn State University Environmental Health & Safety Diseases of Concern Hepatitis B (Serum Hepatitis) Hepatitis C (non-a non-b Hepatitis) HIV (Human Immunodeficiency Virus aka the
PREP IN PRIMARY CARE TRACY SALAMEH RN, BSN, ACRN HIV CLINICAL SPECIALIST DAKOTA AIDS EDUCATION AND TRAINING CENTER
 PREP IN PRIMARY CARE TRACY SALAMEH RN, BSN, ACRN HIV CLINICAL SPECIALIST DAKOTA AIDS EDUCATION AND TRAINING CENTER THE NEED FOR CONTINUED HIV PREVENTION Estimated new HIV infections in the US for the most
PREP IN PRIMARY CARE TRACY SALAMEH RN, BSN, ACRN HIV CLINICAL SPECIALIST DAKOTA AIDS EDUCATION AND TRAINING CENTER THE NEED FOR CONTINUED HIV PREVENTION Estimated new HIV infections in the US for the most
Greater Glasgow and Clyde. Blood Borne Viruses: Some important basic facts
 Greater Glasgow and Clyde Blood Borne Viruses: Some important basic facts Greater Glasgow and Clyde Blood Borne Viruses: Some important basic facts A programme developed by Greater Glasgow and Clyde Health
Greater Glasgow and Clyde Blood Borne Viruses: Some important basic facts Greater Glasgow and Clyde Blood Borne Viruses: Some important basic facts A programme developed by Greater Glasgow and Clyde Health
El Paso - Ambulatory Clinic Policy and Procedure
 Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Needles and Sharps Exposure: How do We Proceed?
 Needles and Sharps Exposure: How do We Proceed? UMAYYA MUSHARRAFIEH,MD AMERICAN UNIVERSITY OF BEIRUT MEDICAL CENTER JUNE 14, 2013 Health care workers who use or may be exposed to needles are at increased
Needles and Sharps Exposure: How do We Proceed? UMAYYA MUSHARRAFIEH,MD AMERICAN UNIVERSITY OF BEIRUT MEDICAL CENTER JUNE 14, 2013 Health care workers who use or may be exposed to needles are at increased
How is it transferred?
 STI s What is a STI? It is a contagious infection that is transferred from one person to another through sexual intercourse or other sexually- related behaviors. How is it transferred? The organisms live
STI s What is a STI? It is a contagious infection that is transferred from one person to another through sexual intercourse or other sexually- related behaviors. How is it transferred? The organisms live
Needlestick and Splash Exposure Flow Chart Page 1 Clinical Practice Guidelines
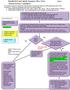 Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
TALKING TO YOUR. DOCTOR ABOUT npep
 TALKING TO YOUR DOCTOR ABOUT npep Please share this with your health provider. If your doctor does not have a great deal of HIV experience, he or she may want to contact a more experienced provider to
TALKING TO YOUR DOCTOR ABOUT npep Please share this with your health provider. If your doctor does not have a great deal of HIV experience, he or she may want to contact a more experienced provider to
Blood and Body Fluid Exposure
 Blood and Body Fluid Exposure Pranavi Sreeramoju, MD, MPH Associate Professor, Medicine Infectious Diseases UT Southwestern Medical Center Chief of Infection Prevention Parkland Health and Hospital System
Blood and Body Fluid Exposure Pranavi Sreeramoju, MD, MPH Associate Professor, Medicine Infectious Diseases UT Southwestern Medical Center Chief of Infection Prevention Parkland Health and Hospital System
Post exposure prophylaxis following exposure to HIV. Paul Benn Mortimer Market Centre, Camden PCT HIVPA study day Tuesday 18 th November 2008 SOAS
 Post exposure prophylaxis following exposure to HIV Paul Benn Mortimer Market Centre, Camden PCT HIVPA study day Tuesday 18 th November 2008 SOAS Overview Hypothesis PEP? Awareness & uptake PEP/PEPSE Ensuring
Post exposure prophylaxis following exposure to HIV Paul Benn Mortimer Market Centre, Camden PCT HIVPA study day Tuesday 18 th November 2008 SOAS Overview Hypothesis PEP? Awareness & uptake PEP/PEPSE Ensuring
BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees
 BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees Buncombe County Public Schools require employees to receive annual training for Bloodborne Pathogens. This online training
BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees Buncombe County Public Schools require employees to receive annual training for Bloodborne Pathogens. This online training
Malaysian Consensus Guidelines on Antiretroviral Therapy Cheng Joo Thye Hospital Raja Permaisuri Bainun Ipoh
 Malaysian Consensus Guidelines on Antiretroviral Therapy 2017 Cheng Joo Thye Hospital Raja Permaisuri Bainun Ipoh Acknowledgement Table of contents Evolution of when to initiate therapy ART improves survival
Malaysian Consensus Guidelines on Antiretroviral Therapy 2017 Cheng Joo Thye Hospital Raja Permaisuri Bainun Ipoh Acknowledgement Table of contents Evolution of when to initiate therapy ART improves survival
Important Safety Information About TRUVADA for a Pre-exposure Prophylaxis (PrEP) Indication. For Healthcare Providers
 Important Safety Information About TRUVADA for a Pre-exposure Prophylaxis (PrEP) Indication For Healthcare Providers About TRUVADA for a PrEP Indication INDICATION AND PRESCRIBING CONSIDERATIONS TRUVADA,
Important Safety Information About TRUVADA for a Pre-exposure Prophylaxis (PrEP) Indication For Healthcare Providers About TRUVADA for a PrEP Indication INDICATION AND PRESCRIBING CONSIDERATIONS TRUVADA,
Obstetric Complications in HIV-Infected Women. Jeanne S. Sheffield, MD Maternal-Fetal Medicine UT Southwestern Medical School
 Obstetric Complications in HIV-Infected Women Jeanne S. Sheffield, MD Maternal-Fetal Medicine UT Southwestern Medical School Obstetric Complications and HIV Obstetric complications are not increased in
Obstetric Complications in HIV-Infected Women Jeanne S. Sheffield, MD Maternal-Fetal Medicine UT Southwestern Medical School Obstetric Complications and HIV Obstetric complications are not increased in
MICROBIOLOGY 211: HIV AND DENTISTRY
 ICROBIOLOGY 211: 2006-2007 Dr. Gillian ccarthy Room 00022 DSB Tel 661 2111 Ext 86122; E-mail: gillian.mccarthy@schulich.uwo.ca HIV AND DENTISTRY OBJECTIVES: The student will be able to discuss - The epidemiology
ICROBIOLOGY 211: 2006-2007 Dr. Gillian ccarthy Room 00022 DSB Tel 661 2111 Ext 86122; E-mail: gillian.mccarthy@schulich.uwo.ca HIV AND DENTISTRY OBJECTIVES: The student will be able to discuss - The epidemiology
Confirmed (Laboratory Tests) Serum positive for IgM anti-hbc or, hepatitis B surface antigen (HbsAg).
 Hepatitis B Hepatitis B is a liver disease that results from infection with the Hepatitis B virus. It can range in severity from a mild illness lasting a few weeks to a serious, lifelong illness. Hepatitis
Hepatitis B Hepatitis B is a liver disease that results from infection with the Hepatitis B virus. It can range in severity from a mild illness lasting a few weeks to a serious, lifelong illness. Hepatitis
TRUVADA for a Pre-exposure Prophylaxis (PrEP) Indication. Training Guide for Healthcare Providers
 TRUVADA for a Pre-exposure Prophylaxis (PrEP) Indication Training Guide for Healthcare Providers About TRUVADA for a PrEP indication to reduce the risk of sexually acquired HIV-1 infection in high-risk
TRUVADA for a Pre-exposure Prophylaxis (PrEP) Indication Training Guide for Healthcare Providers About TRUVADA for a PrEP indication to reduce the risk of sexually acquired HIV-1 infection in high-risk
Knowledge, awareness and compliance among dental professionals regarding percutaneous exposure incidents as occupational hazard
 Original Article Abstract NUJHS Vol. 5, No.4, December 2015, ISSN 2249-7110 Knowledge, awareness and compliance among dental professionals regarding percutaneous exposure incidents as occupational hazard
Original Article Abstract NUJHS Vol. 5, No.4, December 2015, ISSN 2249-7110 Knowledge, awareness and compliance among dental professionals regarding percutaneous exposure incidents as occupational hazard
For. Correctional. Officers. Your. Health Risks. in Correctional Settings. Facts. About HIV
 For Correctional Officers Your Health Risks in Correctional Settings Facts About HIV Working in close quarters with inmates in a correctional facility puts correctional officers (COs) at increased risk
For Correctional Officers Your Health Risks in Correctional Settings Facts About HIV Working in close quarters with inmates in a correctional facility puts correctional officers (COs) at increased risk
Bloodborne Pathogens and Exposure Control
 Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
INITIATING ART IN CHILDREN: Follow the six steps
 INITIATING ART IN CHILDREN: Follow the six steps STEP 1: DECIDE IF THE CHILD HAS CONFIRMED HIV INFECTION Child < 18 months: HIV infection is confirmed if the PCR is positive and the VL is more than 10,000
INITIATING ART IN CHILDREN: Follow the six steps STEP 1: DECIDE IF THE CHILD HAS CONFIRMED HIV INFECTION Child < 18 months: HIV infection is confirmed if the PCR is positive and the VL is more than 10,000
PREVENTION OF HIV IN THE TIMES OF PREP. Daniela Chiriboga, MD Florida Department of Health in Polk County
 PREVENTION OF HIV IN THE TIMES OF PREP Daniela Chiriboga, MD Florida Department of Health in Polk County MAKING THE CASE FOR PREVENTION The Epidemic in Florida Population in 2014: 19.6 million (3 rd in
PREVENTION OF HIV IN THE TIMES OF PREP Daniela Chiriboga, MD Florida Department of Health in Polk County MAKING THE CASE FOR PREVENTION The Epidemic in Florida Population in 2014: 19.6 million (3 rd in
Management of sharps injuries in the healthcare setting
 Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: F:
 University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
Safety Tips from the WorkSafe People
 Blood Borne Pathogens Training HIV/AIDS Hepatitis B Determining Exposure Protecting Yourself Preventing Exposure during an Emergency HIV/AIDS Definition: AIDS stands for Acquired Immune Deficiency Syndrome.
Blood Borne Pathogens Training HIV/AIDS Hepatitis B Determining Exposure Protecting Yourself Preventing Exposure during an Emergency HIV/AIDS Definition: AIDS stands for Acquired Immune Deficiency Syndrome.
Definitions. Appendix A
 Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Management
 01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
